Prediction of Lung Shunt Fraction for Yttrium-90 Treatment of Hepatic Tumors Using Dynamic Contrast Enhanced MRI with Quantitative Perfusion Processing
Abstract
1. Introduction
2. Materials and Methods
2.1. Patients and MRI Protocols
2.2. Quantitative Perfusion Processing of DCE MRI
2.3. Data Analysis
3. Results
4. Discussion
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Salem, R.; Gabr, A.; Riaz, A.; Mora, R.; Ali, R.; Abecassis, M.; Hickey, R.; Kulik, L.; Ganger, D.; Flamm, S.; et al. Institutional decision to adopt Y90 as primary treatment for hepatocellular carcinoma informed by a 1000-patient 15-year experience. Hepatology 2018, 68, 1429–1440. [Google Scholar] [CrossRef] [PubMed]
- Daher, S.; Massarwa, M.; Benson, A.A.; Khoury, T. Current and future treatment of hepatocellular carcinoma: An updated comprehensive review. J. Clin. Transl. Hepatol. 2018, 6, 69. [Google Scholar] [CrossRef]
- Manchec, B.; Kokabi, N.; Narayanan, G.; Niekamp, A.; Peña, C.; Powell, A.; Schiro, B.; Gandhi, R. Radioembolization of Secondary Hepatic Malignancies. Semin. Interv. Radiol. 2021, 38, 445–452. [Google Scholar] [CrossRef] [PubMed]
- Wehrenberg-Klee, E.; Gandhi, R.T.; Ganguli, S. Patient selection and clinical outcomes of Y90 in hepatocellular carcinoma. Tech. Vasc. Interv. Radiol. 2019, 22, 70–73. [Google Scholar] [CrossRef] [PubMed]
- Lau, W.-Y.; Kennedy, A.S.; Kim, Y.H.; Lai, H.K.; Lee, R.-C.; Leung, T.W.; Liu, C.-S.; Salem, R.; Sangro, B.; Shuter, B.; et al. Patient selection and activity planning guide for selective internal radiotherapy with yttrium-90 resin microspheres. Int. J. Radiat. Oncol. Biol. Phys. 2012, 82, 401–407. [Google Scholar] [CrossRef]
- Vouche, M.; Habib, A.; Ward, T.J.; Kim, E.; Kulik, L.; Ganger, D.; Mulcahy, M.; Baker, T.; Abecassis, M.; Sato, K.T.; et al. Unresectable solitary hepatocellular carcinoma not amenable to radiofrequency ablation: Multicenter radiology-pathology correlation and survival of radiation segmentectomy. Hepatology 2014, 60, 192–201. [Google Scholar] [CrossRef]
- Strigari, L.; Sciuto, R.; Rea, S.; Carpanese, L.; Pizzi, G.; Soriani, A.; Iaccarino, G.; Benassi, M.; Ettorre, G.M.; Maini, C.L. Efficacy and toxicity related to treatment of hepatocellular carcinoma with 90Y-SIR spheres: Radiobiologic considerations. J. Nucl. Med. 2010, 51, 1377–1385. [Google Scholar] [CrossRef]
- Srinivas, S.M.; Natarajan, N.; Kuroiwa, J.; Gallagher, S.; Nasr, E.; Shah, S.N.; DiFilippo, F.P.; A Obuchowski, N.; Bazerbashi, B.; Yu, N.; et al. Determination of radiation absorbed dose to primary liver tumors and normal liver tissue using post-radioembolization 90Y PET. Front. Oncol. 2014, 4, 255. [Google Scholar] [CrossRef]
- Luo, J. Lung Shunt Estimate in Yttrium-90 Microsphere Therapy. J. Interv. Radiol. Nucl. Med. 2017, 2017, 1–3. [Google Scholar]
- Elsayed, M.; Cheng, B.; Xing, M.; Sethi, I.; Brandon, D.; Schuster, D.M.; Bercu, Z.; Galt, J.; Barron, B.; Kokabi, N. Comparison of Tc-99m MAA planar versus SPECT/CT imaging for lung shunt fraction evaluation prior to Y-90 radioembolization: Are we overestimating lung shunt fraction? CardioVascular Interv. Radiol. 2021, 44, 254–260. [Google Scholar] [CrossRef]
- Allred, J.D.; Niedbala, J.; Mikell, J.K.; Owen, D.; Frey, K.A.; Dewaraja, Y.K. The value of 99m Tc-MAA SPECT/CT for lung shunt estimation in 90 Y radioembolization: A phantom and patient study. EJNMMI Res. 2018, 8, 50. [Google Scholar] [CrossRef]
- Ljuboja, D.; Ahmed, M.; Ali, A.; Perez, E.; Subrize, M.W.; Kaplan, R.S.; Sarwar, A. Time-Driven Activity-Based Costing in Interventional Oncology: Cost Measurement and Cost Variability for Hepatocellular Carcinoma Therapies. J. Am. Coll. Radiol. 2021, 18, 1095–1105. [Google Scholar] [CrossRef] [PubMed]
- Marqueen, K.E.; Kim, E.; Ang, C.; Mazumdar, M.; Buckstein, M.; Ferket, B.S. Cost-Effectiveness Analysis of Selective Internal Radiotherapy with Yttrium-90 Versus Sorafenib in Locally Advanced Hepatocellular Carcinoma. JCO Oncol. Pract. 2021, 17, e266–e277. [Google Scholar] [CrossRef] [PubMed]
- Zhou, L.; Zhang, Q.; Spincemaille, P.; Nguyen, T.D.; Morgan, J.; Dai, W.; Li, Y.; Gupta, A.; Prince, M.R.; Wang, Y. Quantitative transport mapping (QTM) of the kidney with an approximate microvascular network. Magn. Reson. Med. 2021, 85, 2247–2262. [Google Scholar] [CrossRef] [PubMed]
- Spincemaille, P.; Zhang, Q.; Nguyen, T.D.; Wang, Y. Vector field perfusion imaging. In Proceedings of the ISMRM Annual Meeting, Honolulu, HI, USA, 22–27 April 2017; p. 3793. [Google Scholar]
- Kety, S.S.; Schmidt, C.F. The Determination of Cerebral Blood Flow in Man by the Use of Nitrous Oxide in Low Concentrations. Am. J. Physiol. 1945, 143, 53–66. [Google Scholar] [CrossRef]
- Kety, S.S. The theory and applications of the exchange of inert gas at the lungs and tissues. Pharm. Rev. 1951, 3, 1–41. [Google Scholar]
- Huang, W.; Zhang, Q.; Wu, G.; Chen, P.P.; Li, J.; Gillen, K.M.; Spincemaille, P.; Chiang, G.C.; Gupta, A.; Wang, Y.; et al. DCE-MRI quantitative transport mapping for noninvasively detecting hypoxia inducible factor-1alpha, epidermal growth factor receptor overexpression, and Ki-67 in nasopharyngeal carcinoma patients. Radiother. Oncol. 2021, 164, 146–154. [Google Scholar] [CrossRef]
- Zhang, Q.; Spincemaille, P.; Drotman, M.; Chen, C.; Eskreis-Winkler, S.; Huang, W.; Zhou, L.; Morgan, J.; Nguyen, T.D.; Prince, M.R.; et al. Quantitative transport mapping (QTM) for differentiating benign and malignant breast lesion: Comparison with traditional kinetics modeling and semi-quantitative enhancement curve characteristics. Magn. Reson. Imaging 2021, 86, 86–93. [Google Scholar] [CrossRef]
- Mitchell, D.G.; Bruix, J.; Sherman, M.; Sirlin, C.B. LI-RADS (Liver Imaging Reporting and Data System): Summary, discussion, and consensus of the LI-RADS Management Working Group and future directions. Hepatology 2015, 61, 1056–1065. [Google Scholar] [CrossRef]
- Camacho, J.C.; Moncayo, V.; Kokabi, N.; Reavey, H.E.; Galt, J.R.; Yamada, K.; Kies, D.D.; Williams, R.S.; Kim, H.S.; Schuster, D.M. 90y radioembolization: Multimodality imaging pattern approach with angiographic correlation for optimized target therapy delivery. Radiographics 2015, 35, 1602–1618. [Google Scholar] [CrossRef]
- Elsayed, M.; Martin, J.; Dabrowiecki, A.; Goldman, D.T.; Faraj, R.; McMahon, J.T.; Kokabi, N.; Duszak, R.; Newsome, J.; Bercu, Z.L. Tc-99m-MAA lung shunt fraction before Y-90 radioembolization is low among patients with non-hepatocellular carcinoma malignancies. Nucl. Med. Commun. 2019, 40, 1154–1157. [Google Scholar] [CrossRef] [PubMed]
- Morani, A.C.; Vicens, R.A.; Wei, W.; Gupta, S.; Vikram, R.; Balachandran, A.; Reed, B.J.; Ma, J.; Qayyum, A.; Szklaruk, J. CAIPIRINHA-VIBE and GRAPPA-VIBE for liver MR imaging at 1.5 T: A comparative in vivo patient study. J. Comput. Assist. Tomogr. 2015, 39, 263. [Google Scholar] [CrossRef] [PubMed]
- Jansen, S.A.; Fan, X.; Karczmar, G.S.; Abe, H.; Schmidt, R.A.; Newstead, G.M. Differentiation between benign and malignant breast lesions detected by bilateral dynamic contrast-enhanced MRI: A sensitivity and specificity study. Magn. Reson. Med. Off. J. Int. Soc. Magn. Reson. Med. 2008, 59, 747–754. [Google Scholar] [CrossRef] [PubMed]
- Sourbron, S. A tracer-kinetic field theory for medical imaging. IEEE Trans. Med. Imaging 2014, 33, 935–946. [Google Scholar] [CrossRef]
- Tofts, P.S.; Brix, G.; Buckley, D.; Evelhoch, J.L.; Henderson, E.; Knopp, M.V.; Larsson, H.B.; Lee, T.-Y.; Mayr, N.A.; Parker, G.; et al. Estimating kinetic parameters from dynamic contrast-enhanced T(1)-weighted MRI of a diffusable tracer: Standardized quantities and symbols. J. Magn. Reson. Imaging 1999, 10, 223–232. [Google Scholar] [CrossRef]
- Jafari, R.; Chhabra, S.; Prince, M.R.; Wang, Y.; Spincemaille, P. Vastly accelerated linear least-squares fitting with numerical optimization for dual-input delay-compensated quantitative liver perfusion mapping. Magn. Reson. Med. 2018, 79, 2415–2421. [Google Scholar] [CrossRef]
- Murase, K. Efficient method for calculating kinetic parameters using T1-weighted dynamic contrast-enhanced magnetic resonance imaging. Magn. Reson. Med. 2004, 51, 858–862. [Google Scholar] [CrossRef]
- Kallehauge, J.F.; Sourbron, S.; Irving, B.; Tanderup, K.; Schnabel, J.A.; Chappell, M. Comparison of linear and nonlinear implementation of the compartmental tissue uptake model for dynamic contrast-enhanced MRI. Magn. Reson. Med. 2017, 77, 2414–2423. [Google Scholar] [CrossRef]
- Ludwig, J.M.; Ambinder, E.M.; Ghodadra, A.; Xing, M.; Prajapati, H.J.; Kim, H.S. Lung shunt fraction prior to yttrium-90 radioembolization predicts survival in patients with neuroendocrine liver metastases: Single-center prospective analysis. Cardiovasc. Interv. Radiol. 2016, 39, 1007–1014. [Google Scholar] [CrossRef]
- Wright, C.L.; Werner, J.D.; Tran, J.M.; Gates, V.L.; Rikabi, A.A.; Shah, M.H.; Salem, R. Radiation pneumonitis following yttrium-90 radioembolization: Case report and literature review. J. Vasc. Interv. Radiol. 2012, 23, 669–674. [Google Scholar] [CrossRef]
- A Ziessman, H.; Thrall, J.H.; Gyves, J.W.; Ensminger, W.D.; E Niederhuber, J.; Tuscan, M.; Walker, S. Quantitative hepatic arterial perfusion scintigraphy and starch microspheres in cancer chemotherapy. J. Nucl. Med. 1983, 24, 871–875. [Google Scholar] [PubMed]
- Leung, W.; Lau, W.; Ho, S.K.; Chan, M.; Leung, N.W.Y.; Lin, J.; Metreweli, C.; Johnson, P.J.; Li, A.K.C. Measuring Lung Shunting in Hepatocellular Carcinoma with Intrahepatic-Arterial Technetium-99m-Macroaggregated Albumin. J. Nucl. Med. 1994, 35, 70–73. [Google Scholar] [PubMed]
- Kim, Y.; Savellano, M.; Savellano, D.; Weissleder, R.; Bogdanov, A., Jr. Measurement of tumor interstitial volume fraction: Method and implication for drug delivery. Magn. Reson. Med. Off. J. Int. Soc. Magn. Reson. Med. 2004, 52, 485–494. [Google Scholar] [CrossRef] [PubMed]
- Zhang, H.; Verkman, A. Microfiberoptic measurement of extracellular space volume in brain and tumor slices based on fluorescent dye partitioning. Biophys. J. 2010, 99, 1284–1291. [Google Scholar] [CrossRef]
- Xu, B.; Spincemaille, P.; Chen, G.; Agrawal, M.; Nguyen, T.D.; Prince, M.R.; Wang, Y. Fast 3D contrast enhanced MRI of the liver using temporal resolution acceleration with constrained evolution reconstruction. Magn. Reson. Med. 2013, 69, 370–381. [Google Scholar] [CrossRef]
- Kim, K.H.; Choi, S.H.; Park, S.H. Feasibility of Quantifying Arterial Cerebral Blood Volume Using Multiphase Alternate Ascending/Descending Directional Navigation (ALADDIN). PLoS ONE 2016, 11, e0156687. [Google Scholar] [CrossRef]
- Duhamel, G.; de Bazelaire, C.; Alsop, D.C. Evaluation of systematic quantification errors in velocity-selective arterial spin labeling of the brain. Magn. Reson. Med. Off. J. Int. Soc. Magn. Reson. Med. 2003, 50, 145–153. [Google Scholar] [CrossRef]
- Wong, E.C.; Cronin, M.; Wu, W.C.; Inglis, B.; Frank, L.R.; Liu, T.T. Velocity-selective arterial spin labeling. Magn. Reson. Med. Off. J. Int. Soc. Magn. Reson. Med. 2006, 55, 1334–1341. [Google Scholar] [CrossRef]
- Jensen, J.H.; Chandra, R. MR imaging of microvasculature. Magn. Reson. Med. 2000, 44, 224–230. [Google Scholar] [CrossRef]
- Kiselev, V.G.; Strecker, R.; Ziyeh, S.; Speck, O.; Hennig, J. Vessel size imaging in humans. Magn. Reson. Med. 2005, 53, 553–563. [Google Scholar] [CrossRef]
- Chakhoyan, A.; Yao, J.; Leu, K.; Pope, W.B.; Salamon, N.; Yong, W.; Lai, A.; Nghiemphu, P.L.; Everson, R.G.; Prins, R.M.; et al. Validation of vessel size imaging (VSI) in high-grade human gliomas using magnetic resonance imaging, image-guided biopsies, and quantitative immunohistochemistry. Sci. Rep. 2019, 9, 2846. [Google Scholar] [CrossRef] [PubMed]
- Wagner, H.N., Jr.; Sabiston, D.C., Jr.; Iio, M.; McAfee, J.G.; Meyer, J.K.; Langan, J.K. Regional Pulmonary Blood Flow in Man by Radioisotope Scanning. JAMA 1964, 187, 601–603. [Google Scholar] [CrossRef]
- Herba, M.J.; Illescas, F.F.; Thirlwell, M.P.; Boos, G.J.; Rosenthall, L.; Atri, M.; Bret, P.M. Hepatic malignancies: Improved treatment with intraarterial Y-90. Radiology 1988, 169, 311–314. [Google Scholar] [CrossRef]
- Ho, S.; Lau, W.Y.; Leung, T.W.T.; Chan, M.; Ngar, Y.K.; Johnson, P.J.; Li, A.K.C. Partition model for estimating radiation doses from yttrium-90 microspheres in treating hepatic tumours. Eur. J. Nucl. Med. 1996, 23, 947–952. [Google Scholar] [CrossRef] [PubMed]
- Giammarile, F.; Therapy, O.A.D.C.T.; Bodei, L.; Chiesa, C.; Flux, G.; Forrer, F.; Kraeber-Bodéré, F.; Brans, B.; Lambert, B.; Konijnenberg, M.; et al. EANM procedure guideline for the treatment of liver cancer and liver metastases with intra-arterial radioactive compounds. Eur. J. Nucl. Med. Mol. Imaging 2011, 38, 1393–1406. [Google Scholar] [CrossRef] [PubMed]
- Wondergem, M.; Smits, M.L.; Elschot, M.; de Jong, H.W.A.M.; Verkooijen, H.M.; van den Bosch, M.A.A.J.; Nijsen, J.F.W.; Lam, M.G.E.H. 99mTc-macroaggregated albumin poorly predicts the intrahepatic distribution of 90Y resin microspheres in hepatic radioembolization. J. Nucl. Med. 2013, 54, 1294–1301. [Google Scholar] [CrossRef] [PubMed]
- Basciano, C.A.; Kleinstreuer, C.; Kennedy, A.S.; Dezarn, W.A.; Childress, E. Computer modeling of controlled microsphere release and targeting in a representative hepatic artery system. Ann. Biomed. Eng. 2010, 38, 1862–1879. [Google Scholar] [CrossRef] [PubMed]
- Roncali, E.; Taebi, A.; Foster, C.; Vu, C.T. Personalized Dosimetry for Liver Cancer Y-90 Radioembolization Using Computational Fluid Dynamics and Monte Carlo Simulation. Ann. Biomed. Eng. 2020, 48, 1499–1510. [Google Scholar] [CrossRef]
- Wang, Y.; Grist, T.M.; Korosec, F.R.; Christy, P.S.; Alley, M.T.; Polzin, J.A.; Mistretta, C.A. Respiratory blur in 3D coronary MR imaging. Magn. Reson. Med. 1995, 33, 541–548. [Google Scholar] [CrossRef]
- Wang, Y.; Ehman, R.L. Retrospective adaptive motion correction for navigator-gated 3D coronary MR angiography. J. Magn. Reson. Imaging Off. J. Int. Soc. Magn. Reson. Med. 2000, 11, 208–214. [Google Scholar] [CrossRef]
- de Rochefort, L.; Liu, T.; Kressler, B.; Liu, J.; Spincemaille, P.; Lebon, V.; Wu, J.; Wang, Y. Quantitative susceptibility map reconstruction from MR phase data using bayesian regularization: Validation and application to brain imaging. Magn. Reson. Med. 2010, 63, 194–206. [Google Scholar] [CrossRef] [PubMed]
- de Rochefort, L.; Nguyen, T.; Brown, R.; Spincemaille, P.; Choi, G.; Weinsaft, J.; Prince, M.R.; Wang, Y. In vivo quantification of contrast agent concentration using the induced magnetic field for time-resolved arterial input function measurement with MRI. Med. Phys. 2008, 35, 5328–5339. [Google Scholar] [CrossRef] [PubMed]
| R (95% CI) | p Value | F Value | |
|---|---|---|---|
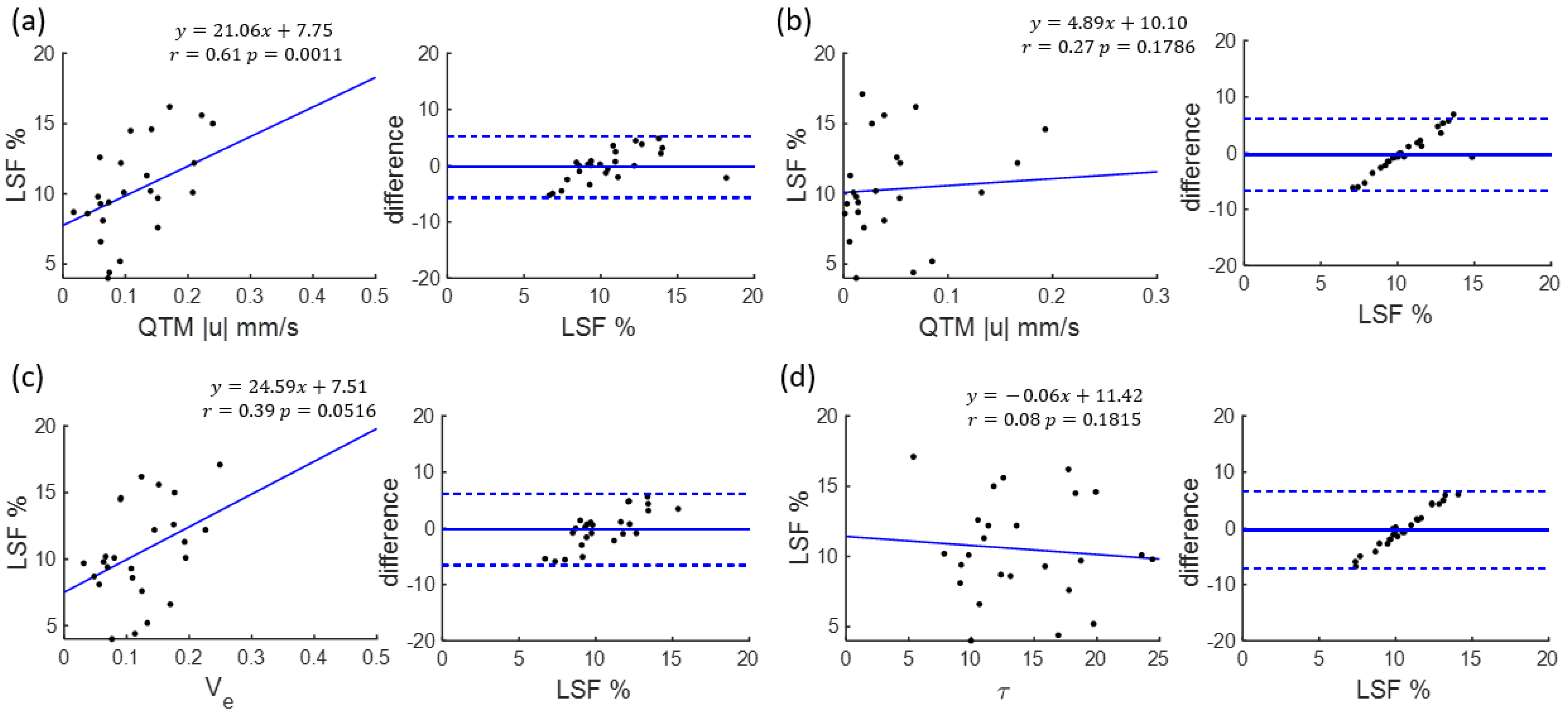
| QTM |u| | 0.6156 (0.4148–0.8164) | 0.0011 | 14.0363 |
| 0.2778 (0.0244–0.5312) | 0.1786 | 1.9251 | |
| 0.3936 (0.1403–0.6469) | 0.0516 | 4.2168 | |
| 0.0883 (−0.0921–0.2687) | 0.1815 | 0.6741 | |
| Tumor volume | 0.2735 (0.0206–0.5264) | 0.1858 | 1.8603 |
| Age | 0.2272 (−0.0180–0.4724) | 0.2749 | 1.2508 |
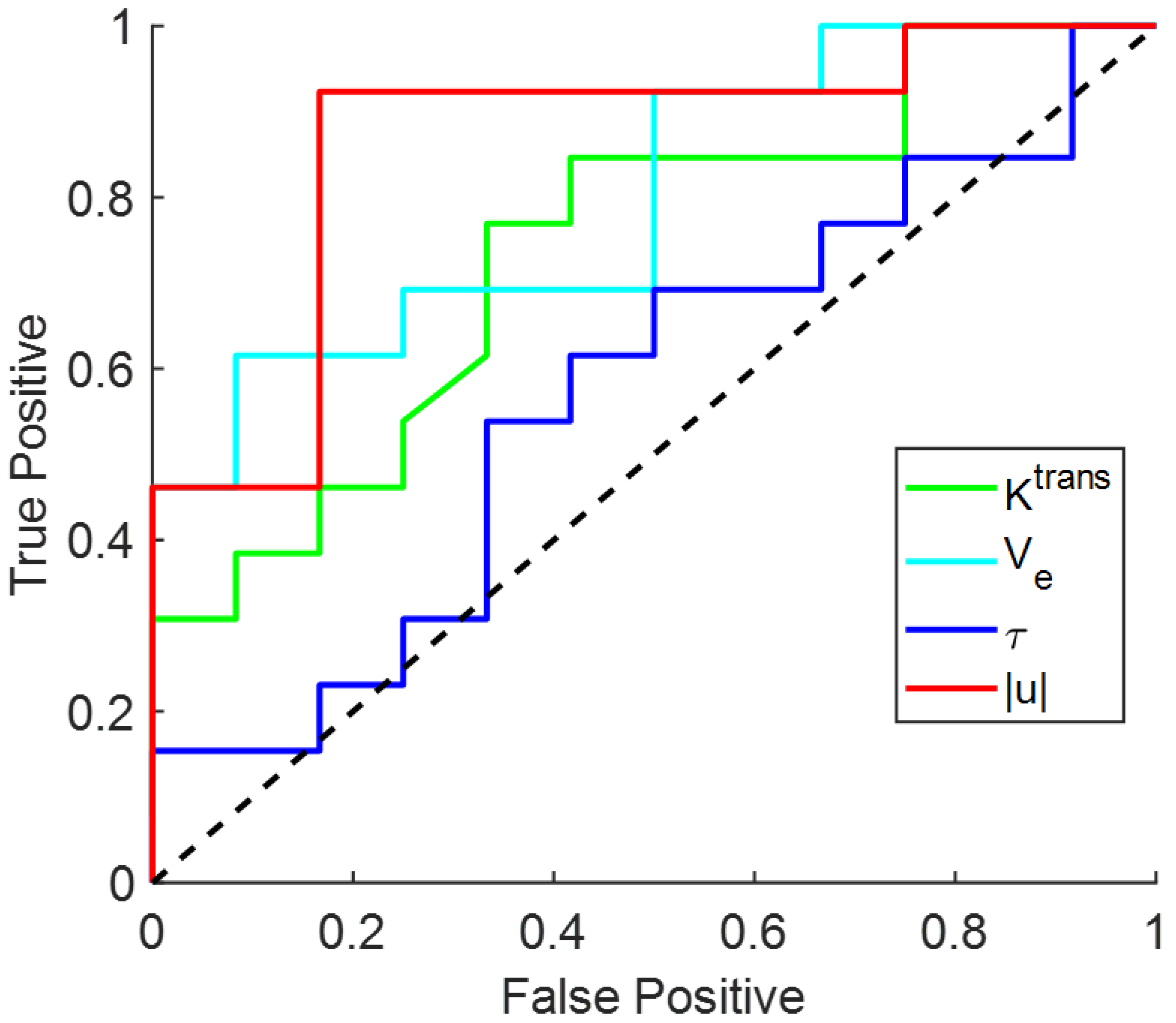
| AUC (95% CI) | Sensitivity (95% CI) | Specificity (95% CI) | |
|---|---|---|---|
| QTM |u| | 0.87 (0.63–0.97) | 0.92 (0.63–1) | 0.83 (0.5–1) |
| 0.74 (0.49–0.90) | 0.77 (0.42–0.93) | 0.67 (0.30–0.89) | |
| 0.80 (0.56–0.93) | 0.62 (0.30–0.85) | 0.92 (0.54–1) | |
| 0.57 (0.32–0.82) | 0.54 (0.23–0.80) | 0.58 (0.29–0.88) | |
| Tumor volume | 0.54 (0.30–0.76) | 0.31 (0.08–0.66) | 0.92 (0.63–1) |
| Age | 0.59 (0.32–0.80) | 0.62 (0.31–0.85) | 0.67 (0.32–0.9) |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2022 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Zhang, Q.; Lee, K.S.; Talenfeld, A.D.; Spincemaille, P.; Prince, M.R.; Wang, Y. Prediction of Lung Shunt Fraction for Yttrium-90 Treatment of Hepatic Tumors Using Dynamic Contrast Enhanced MRI with Quantitative Perfusion Processing. Tomography 2022, 8, 2687-2697. https://doi.org/10.3390/tomography8060224
Zhang Q, Lee KS, Talenfeld AD, Spincemaille P, Prince MR, Wang Y. Prediction of Lung Shunt Fraction for Yttrium-90 Treatment of Hepatic Tumors Using Dynamic Contrast Enhanced MRI with Quantitative Perfusion Processing. Tomography. 2022; 8(6):2687-2697. https://doi.org/10.3390/tomography8060224
Chicago/Turabian StyleZhang, Qihao, Kyungmouk Steve Lee, Adam D. Talenfeld, Pascal Spincemaille, Martin R. Prince, and Yi Wang. 2022. "Prediction of Lung Shunt Fraction for Yttrium-90 Treatment of Hepatic Tumors Using Dynamic Contrast Enhanced MRI with Quantitative Perfusion Processing" Tomography 8, no. 6: 2687-2697. https://doi.org/10.3390/tomography8060224
APA StyleZhang, Q., Lee, K. S., Talenfeld, A. D., Spincemaille, P., Prince, M. R., & Wang, Y. (2022). Prediction of Lung Shunt Fraction for Yttrium-90 Treatment of Hepatic Tumors Using Dynamic Contrast Enhanced MRI with Quantitative Perfusion Processing. Tomography, 8(6), 2687-2697. https://doi.org/10.3390/tomography8060224






