Ornithobacterium rhinotracheale: An Update Review about An Emerging Poultry Pathogen
Abstract
1. Introduction
2. Ornithobacterium rhinotracheale (ORT)
3. Clinical and Pathologic Features
3.1. Mode of Infection and Transmission
3.2. Epidemiology and Prevention
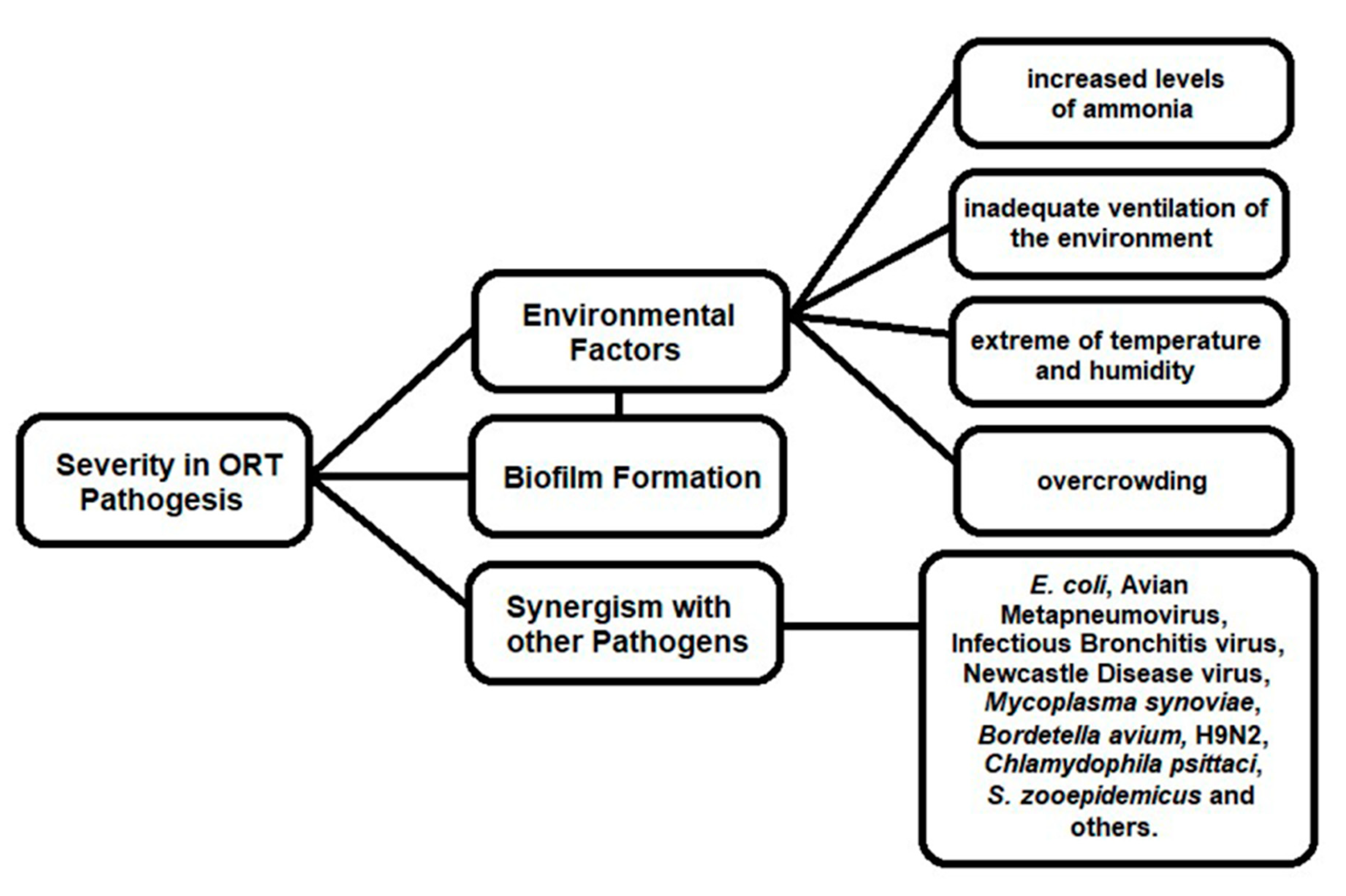
3.3. Clinical Signs and Pathological Lesions
4. Laboratory Diagnosis
4.1. Isolation and Identification
4.2. Serotyping and Detection
5. Genetic Relatedness
6. Treatment
7. Vaccination
8. Conclusions
Author Contributions
Funding
Acknowledgments
Conflicts of Interest
References
- Rubio, A.G.; Salazar, A.R. Identificación de Ornithobacterium Rhinotracheale (ORT) y Metapneumovirus Aviar (MA). Caracterizaçión Epidemiológica em Chile. Boletín Veterinário Oficial. 2010. Available online: https://www2.sag.gob.cl/Pecuaria/bvo/BVO_11_I_semestre_2010/PDF_articulos/identificacion_ORT_MA.pdf (accessed on 23 July 2017).
- Numee, S.; Hauck, R.; Hafez, H.M. Detection and typing of Ornithobacterium rhinotracheale from German poultry flocks. Avian Dis. 2012, 56, 654–658. [Google Scholar] [CrossRef] [PubMed]
- Zehr, E.S.; Bayles, D.O.; Boatwright, W.D.; Tabatabai, L.B.; Register, K.B. Non-contiguous finished genome sequence of Ornithobacterium rhinotracheale strain H06-030791. Stand. Genom. Sci. 2014, 9, 14. [Google Scholar] [CrossRef] [PubMed]
- Pan, Q.; Liu, A.; Zhang, F.; Ling, Y.; Ou, C.; Hou, N.; He, C. Co-infection of broilers with Ornithobacterium rhinotracheale and H9N2 avian influenza virus. BMC Vet. Res. 2012, 8, 104. [Google Scholar] [CrossRef] [PubMed]
- Canal, C.W.; Rocha, S.L.S.; Leão, J.A.; Fallavena, L.C.B.; Oliveira, S.D.; Beltrão, N. Detecção de Ornithobacterium rhinotracheale (ORT) por meio da reação em cadeia da polimerase (PCR). Ciênca Rural Santa Maria 2003, 33, 377–379. [Google Scholar] [CrossRef]
- EFSA European Food Safety Authority Scientific. Opinion on the Use of Animal-Based Measures to Assess Welfare of Broilers. EFSA J. 2012, 10, 2774. Available online: https://efsa.onlinelibrary.wiley.com/doi/epdf/10.2903/j.efsa.2012.2774 (accessed on 10 April 2018).
- Gomes, A.V.S.; Quinteiro-Filho, W.M.; Ribeiro, A.; Ferrazde-Paula, V.; Pinheiro, M.L.; Baskeville, E.; Akamine, A.T.; Astolfi-Ferreira, C.S.; Ferreira, A.J.P.; Palermo-Neto, J. Overcrowding stress decreases macrophage activity and increases Salmonella enteritidis invasion in broiler chickens. Avian Pathol. 2014, 43, 82–90. [Google Scholar] [CrossRef]
- Conway, A. Meat Production: Poultry meat production up 13 million metric tons by 2026. Fig2, Global meat production by species. Poult. Trends 2017, 2017, 22–23. [Google Scholar]
- Patel, J.G.; Pate, B.J.; Patel, S.S.; Raval, S.H.; Parmar, R.S.; Joshi, D.V.; Chauhan, H.C.; Chandel, B.S.; Patel, B.K. Metagenomic of clinically diseased and healthy broiler affected with respiratory disease complex. Data Brief. 2018, 19, 82–85. [Google Scholar] [CrossRef]
- Macagnan, M. Caracterização Fenotípica e Genotípica de Isolados de Ornithobacterium rhinotracheale do Brasil. Rio Grande do Sul, Brasil. Acta Sci. Vet. 2006, 34, 109–110. Available online: https://seer.ufrgs.br/actascientiaeveterinariae/article/view/15119/8908%C2%A7 (accessed on 18 July 2017). [CrossRef]
- Chin, R.P.; Charlton, B.R. Ornithobacteriosis. In A Laboratory Manual for the Isolation, Identification, and Characterization of Avian Pathogens, 5th ed.; Dufour-Zavala, L., Swayne, D.E., Glisson, J.R., Pearson, J.E., Reed, W.M., Jackwood, M.W., Woolcock, P.R., Eds.; The American Association of Avian Pathologists: Madison, WL, USA, 2008; pp. 75–76. ISBN 978-0-9789163-2-9. [Google Scholar]
- Chin, R.P.; van Empel, P.C.M.; Hafez, H.M. Ornithobacterium rhinotracheale infection. In Diseases of Poultry, 13th ed.; Swayne, D.E., Ed.; Wiley-Blackwell: Hoboken, NJ, USA, 2013; pp. 807–858. [Google Scholar]
- World Organisation for Animal Health. O.I.E-Listed Diseases, Infections and Infestations in Force in 2018; OIE: Paris, France, 2018; Available online: http://www.oie.int/en/animal-health-in-the-world/oie-listed-diseases-2018/ (accessed on 31 August 2018).
- Hafez, M.H. Diagnosis of Ornithobacterium rhinotracheale. Int. J. Poult. Sci. 2002, 1, 114–118. [Google Scholar]
- Misirlioğlu, Ö.Z.; Türkyilmaz, S.; Hafez, H.M. Report on isolation and identification of Ornithobacterium rhinotracheale from broiler flocks in Ízmir, Turkey. Arch. Geflügelk. 2006, 70, 134–138. [Google Scholar]
- Cobb, S.P.; Smith, H. The spread of non, O.I.E-listed avian diseases through international trade of chicken meat: An assessment of the risks to New Zealand. Rev. Sci. Tech. Off. Int. Epiz. 2015, 34, 1–44. [Google Scholar]
- Charlton, B.R.; Channing-Santiago, S.E.; Bickford, A.A.; Cardona, C.J.; Chin, R.P.; Cooper, G.L.; Droual, R.; Jeffrey, J.S.; Meteyer, C.U.; Shivaprasad, H.L.; et al. Preliminary characterization of a pleomorphic gram-negative rod associated with avian respiratory disease. J. Vet. Diagn. Investig. 1993, 5, 47–51. [Google Scholar] [CrossRef] [PubMed]
- Van Empel, P.C.M.; Hafez, H.M. Ornithobacterium rhinotracheale: A review. Avian Pathol. 1999, 28, 217–227. [Google Scholar] [CrossRef] [PubMed]
- Van Beek, P.; van Empel, P.C.M.; van den Bosch, G.; Storm, P.; Bongers, J.; du Preez, J. Ademhalingsproblemen, groeivertraging en gewrichtsontsteking bij kalkoenen en vleeskuikens door een Pasteurella-achtige bacterie: Ornithobacterium rhinotracheal e of Taxon 28. Tijdschrift voor Diergeneeskunde 1994, 119, 99–101. [Google Scholar] [PubMed]
- Vandamme, P.; Segers, P.; Vancanneyt, M.; van Hove, K.; Mutters, R.; Hommez, J.; Dewhirst, F.; Paster, B.; Kersters, K.; Falsen, E.; et al. Ornithobacterium rhinotracheale gen. nov., sp. nov., isolated from the avian respiratory tract. Int. J. Syst. Bacteriol. 1994, 44, 24–37. [Google Scholar] [CrossRef]
- De la Rosa-Ramos, M.A.; Muñoz-Solís, K.; Palma-Zepeda, M.; Gutierrez-Castillo, A.C.; Villegas, E.O.L.; Guerra-Infante, F.M.; Castro-Escarpulli, G. Adherence of Ornithobacterium rhinotracheale to chicken embryo lung cells as a pathogenic mechanism. Avian Pathol. 2018, 47, 172–179. [Google Scholar] [CrossRef]
- Churria, C.D.G.; Sansalone, P.L.; Machuca, M.A.; Vigo, G.B.; Sguazza, G.H.; Origlia, J.A.; Píscopo, M.V.; Loyola, M.A.H.; Petruccelli, M.A. Tracheitis in a broiler chicken flock caused by dual infection with Cryptosporidium spp. (Apicomplexa: Cryptosporiidae) and non-hemolytic Ornithobacterium rhinotracheale. Braz. J. Vet. Pathol. 2012, 5, 89–93. [Google Scholar]
- Amonsin, A.; Wellehan, J.F.X.; Li, L.L.; Vandame, P.; Lindeman, C.; Edman, M.; Robinson, R.A.; Kapur, V. Molecular epidemiology of Ornithobacterium rhinotracheale. J. Clin. Microbiol. 1997, 35, 2894–2898. [Google Scholar]
- Gavrilović, O.; Gavrilović, A.; Vidanović, D.; Parunović, J.; Jovanović, M. Comparative pathomorphological, bacteriological and serological examination of broiler breeders and pheasants experimentally infected with Ornithobacterium rhinotracheale. Avian Pathol. 2016, 45, 513–519. [Google Scholar] [CrossRef]
- Sprenger, S.J.; Back, A.; Shaw, D.P.; Nagaraja, K.V.; Roepke, D.C.; Halvorson, D.A. Ornithobacterium rhinotracheale infection in turkeys: Experimental reproduction of the disease. Avian Dis. 1998, 42, 154–161. [Google Scholar] [CrossRef] [PubMed]
- Back, A. Manual de Doenças de Aves, 2th ed.; Editora Integração: Cascavel, Brazil, 2010; pp. 171–173. ISBN 978-85-61806-01-09. [Google Scholar]
- Hauck, R.; Chin, R.P.; Shivaprasad, H.L. Retrospective study on the isolation of Ornithobacterium rhinotracheale from chickens and turkeys in Central California: 294 cases (2000–12). Avian Dis. 2015, 59, 130–137. [Google Scholar] [CrossRef] [PubMed]
- Gavrilović, P.; Jovanović, M.; Živulj, A. Examination of Ornithobacterium rhinotracheale presence and pathomorphological changes in broiler respiratory organs in intensive broiler production. Acta Vet. 2012, 62, 313–323. [Google Scholar]
- Marien, M.; Decostere, A.; Martel, A.; Chiers, K.; Froyman, R.; Nauwynck, H. Synergy between avian pneumovirus and Ornithobacterium rhinotracheale in turkeys. Avian Pathol. 2005, 34, 204–211. [Google Scholar] [CrossRef]
- Tsai, H.J.; Huang, C.W. Phenotypic and molecular characterization of isolates of Ornithobacterium rhinotracheale from chickens and pigeons in Taiwan. Avian Dis. 2006, 50, 502–507. [Google Scholar] [CrossRef]
- Chansiripornchai, N.; Wanasawaeng, W.; Sasipreeyajan, J. Seroprevalence and identification of Ornithobacterium rhinotracheale from broiler and broiler breeder flocks in Thailand. Avian Dis. 2007, 51, 777–780. [Google Scholar] [CrossRef]
- De Haro-Cruz, M.J.; Ixta-Avila, L.; Guerra-Infante, F.M. Adherence of five serovars of Ornithobacterium rhinotracheale to chicken tracheal epithelial cells. Br. Poult. Sci. 2013, 54, 425–429. [Google Scholar] [CrossRef]
- Sharifzadeh, A.; Doosti, A.; Ghasemi, H. Prevalence of Ornithobacterium rhinotracheale at broiler chicken farms in southwest Iran. Bulg. J. Vet. Med. 2011, 3, 179–183. [Google Scholar]
- Walters, J.N. Characterization of Atypical Hemolytic Ornithobacterium rhinotracheale Isolates and Comparison with the Normal Non-Hemolytic Phenotype. Ph.D. Thesis, Virginia Polytechnic Institute and State University, Blacksburg, VA, USA, 2014; 120p. [Google Scholar]
- Patel, J.G.; Pate, B.J.; Joshi, D.V.; Patel, S.S.; Raval, S.H.; Parmar, R.S.; Chauhan, H.C.; Chandel, B.S. Culture based isolation of pathogenic bacteria associated with respiratory disease complex in broiler with special reference to Ornithobacterium rhinotracheale from India. J. Pure Appl. Microbiol. 2017, 11, 1919–1924. [Google Scholar] [CrossRef]
- Mehrabanpour, M.; Bushehri, M.; Mehrabanpour, D. Molecular and serological diagnosis of Newcastle and Ornithobacterium rhinotracheale broiler in chicken in Fars Province, Iran. Int. J. Anim. Vet. Sci. 2017, 4, 3. [Google Scholar]
- Zuo, Z.H.; Zhang, T.Y.; Guo, Y.X.; Chu, J.; Qu, G.G.; Miao, L.Z.; Shen, Z.Q.; He, C. Serosurvey of avian metapneumovirus, Ornithobacterium rhinotracheale, and Chlamydia psittaci and their potential association with avian airsacculitis. Biomed. Environ. Sci. 2018, 31, 403–406. [Google Scholar] [PubMed]
- Chávez, M.C.; León, Y.M.; Ugalde, Y.S.; Cárdenas, N.B.; López, A.M.; Rivero, E.L.; Redondo, A.V. Evidência Sorológica, em Cuba, da Circulação de Ornithobacterium rhinotracheale em Galinhas Poedeiras com Síndrome Respiratória Crônica. XXII Congresso Latino-Americano de Avicultura. 2011. Available online: https://pt.engormix.com/avicultura/artigos/ornitobacterium-rhinotracheale-galinhas-poedeiras-t37346.htm (accessed on 12 October 2017).
- Ha, H.J.; Christensen, N.; Humphrey, S.; Haydon, T.; Bernardi, G.; Rawdon, T. The first of Ornithobacterium rhinotracheale in New Zealand. Avian Dis. 2016, 60, 856–859. [Google Scholar] [CrossRef] [PubMed]
- Canal, C.W.; Leão, J.A.; Rocha, S.L.S.; Macagnan, M.; Lima-Rosa, C.A.V.; Oliveira, S.D.; Back, A. Isolation and characterization of Ornithobacterium rhinotracheale from chickens in Brazil. Res. Vet. Sci. 2005, 78, 225–230. [Google Scholar] [CrossRef] [PubMed]
- Umali, D.V.; Shirota, K.; Sasa, K.; Katoh, H. Characterization of Ornithobacterium rhinotracheale from commercial layer chickens in eastern Japan. Poult. Sci 2018, 97, 24–29. [Google Scholar] [CrossRef]
- Sousa, G.P. Boas Práticas Para Produção de ovos e Legislação de Bem-Estar Animal: Cenário do Município de Bastos/SP. Master’s Thesis, Universidade Estadual Paulista Júlio de Mesquita Filho, São Paulo, Brazil, 2016; 73p. [Google Scholar]
- Vieira, V.A.; Oliveira, N.J.F.; Almeida, A.C.; Pereira, A.A.; Félix, T.M. Práticas de uso de antimicrobianos em rebanhos bovinos em 15 unidades de agricultura familiar no norte de Minas Gerais. Caderno de Ciências Agrárias 2016, 8, 8–15. [Google Scholar]
- Hafez, M.H.; Schulze, D. Examinations on the efficacy of chemical disinfectants on Ornithobacterium rhinotracheale In Vitro. Arch. Geflugelkd. 2003, 67, 153–156. [Google Scholar]
- Hodges, J. Emering boundaries for poultry production: Challenges, dangers and opportunities. Worlds Poult. Sci. J. 2009, 65, 5–21. [Google Scholar] [CrossRef]
- Ellakany, H.F.; Abd-Elhamid, H.S.; Bekhit, A.A.; Elbestawy, A.R.; Abou-Ellif, A.S.; Gado, A.R. Effect of mixed experimental enfection with Ornithobacterium rhinotracheale and Mycoplasma gallisepticum in broiler chickens. Alex. J. Vet. Sci. 2019, 61, 168–178. [Google Scholar]
- Marien, M. Mixed Respiratory Infections in Turkeys, with Emphasis on Avian Metapneumovirus, Ornithobacterium Rhinotracheale, Escherichia Coli and Mycoplasma Gallisepticum. Ph.D. Thesis, Universiteit Gent, Ghent, Belgium, Faculty of Veterinary Medicine, Utrecht, The Netherlands, 2007. [Google Scholar]
- Pan, Q.; Liu, A.; He, C. Co-infection of Ornithobacterium rhinotracheale with Streptococcus zooepidemicus. Avian Dis. 2012, 56, 680–684. [Google Scholar] [CrossRef]
- De la Rosa-Ramos, M.A.; Cruz, M.R.; Villegas, E.O.L.; Castro-Escarpulli, G.; Guerra-Infante, F.M. Conditions that induce biofilm production by Ornithobacterium rhinotracheale. Avian Pathol. 2015, 44, 366–369. [Google Scholar] [CrossRef]
- Kastelic, S.; Berčič, R.L.; Cizelj, I.; Benčina, M.; Makrai, L.; Zorman-Rojs, O.; Narat, M.; Bisgaard, M.; Christensen, H.; Benčina, D. Ornithobacterium rhinotracheale has neuraminidade activity causing desialylation of chicken and turkey serum and tracheal mucus glycoproteins. Vet. Microbiol. 2013, 162, 707–712. [Google Scholar] [CrossRef] [PubMed]
- Zahra, M.; Ferreri, M.; Alkasir, R.; Yin, J.; Han, B.; Su, J. Isolation and characterization of small-colony variants of Ornithobacterium rhinotracheale. J. Clin. Microbiol. 2013, 51, 3228–3236. [Google Scholar] [CrossRef] [PubMed]
- Walters, J.; Evans, R.; Leroith, T.; Sriranganathan, N.; McElroy, A.; Pierson, F.W. Experimental comparison of hemolytic and nonhemolytic Ornithobacterium rhinotracheale field isolates In Vivo. Avian Dis. 2014, 58, 78–82. [Google Scholar] [CrossRef] [PubMed]
- Ozbey, G.; Ongor, H.; Balik, D.T.; Celik, V.; Kilic, A.; Muz, A. Investigations on Ornithobacterium rhinotracheale in broiler flocks in Elazig province located in the East of Turkey. Vet. Med. UZPI 2004, 8, 305–311. [Google Scholar] [CrossRef]
- Mayahi, M.; Gharibi, D.; Ghadimipour, R.; Talazadeh, F. Isolation, identification and antimicrobial sensitivity of Ornithobacterium rhinotracheale in broilers chicken flocks of Khuzestan, Iran. Vet. Res. Forum 2016, 7, 341–346. [Google Scholar]
- Peña-Vargas, E.R.; Vega-Sánchez, V.; Morales-Erasto, V.; Trujillo-Ruís, H.H.; Talavera-Rojas, M. Soriano-Vargas E Serotyping, genotyping, and antimicrobial susceptibility of Ornithobacterium rhinotracheale isolates from Mexico. Avian Dis. 2016, 60, 669–672. [Google Scholar] [CrossRef]
- Szabó, R.; Wehmann, E.; Makrai, L.; Nemes, C.; Gyuris, É.; Thuma, Á.; Maqyar, T. Characterization of Ornithobacterium rhinotracheale field isolates from Hungary. Avian Pathol. 2017, 46, 506–514. [Google Scholar] [CrossRef]
- Umar, S.; Iqbal, M.; Khan, A.H.; Mushtaq, A.; Aqil, K.; Jamil, T.; Asif, S.; Qamar, N.; Shahzad, A.; Younus, M. Ornithobacterium rhinotracheale infection in red wattled lapwings (Vanellus indicus) in Pakistan—A case report. Vet. Arch. 2017, 87, 641–648. [Google Scholar] [CrossRef]
- Siddique, M.; Zia, T.; Rehman, S.U. Outbreak of Ornithobacterium rhinotracheale (ORT) infection in chickens in Pakistan. Archiv für Geflügelkunde Eur. Poult. Sci. 2008, 72, 202–206. [Google Scholar]
- Abujamra, T. Detecção de Agentes Bacterianos Envolvidos nos Quadros de Aerossaculite em Perus Através da Reação em Cadeia Pela Polimerase (PCR). Master’s Thesis, Universidade de São Paulo, São Paulo, Brazil, 2010; 48p. Available online: https://teses.usp.br/teses/disponiveis/10/10134/tde-15122011-113034/en.php (accessed on 31 August 2018).
- Pereira, R.A.; Macagnan, M.; Schwarz, P.; Canal, C.W.; Schmidt, V. Estabelecimento de um Protocolo de Soroaglutinação Rápida (SAR) para Detecção de Anticorpos para Salmonella Typhimurium em Suínos. Ciência Animal Brasileira 2010, 11, 677–682. [Google Scholar]
- Türkyilmaz, S. Isolation and serotyping of Ornithobacterium rhinotracheale from poultry. Turk. J. Vet. Anim. Sci. 2005, 29, 1299–1304. [Google Scholar]
- Numee, S.; Hauck, R.; Hafez, H.M. Influence of different storage media, temperatures and time duration on susceptibility of Ornithobacterium rhinotracheale. Pak. Vet. J. 2012, 32, 438–442. [Google Scholar]
- Van Empel, P.C.M.; van den Bosch, H.; Goovaerts, D.; Storm, P. Experimental infection in turkeys and chickens with Ornithobacterium rhinotracheale. Avian Dis. 1996, 40, 858–864. [Google Scholar] [CrossRef] [PubMed]
- Van Empel, P.C.M. Ornithobacterium rhinotracheale: Current status and control. In Proceedings of the 1st International Symposium on Turkey Diseases, Berlin, Germany, 19–21 February 1998; pp. 129–137. [Google Scholar]
- Hafez, H.M. Current status on the laboratory diagnosis of Ornithobacterium rhinotracheale ‘ORT’ in poultry. Berliner und Münchener Tierärztliche Wochenschrift 1998, 111, 143–145. [Google Scholar]
- Chin, R.; Droual, R. Ornithobacterium rhinotracheale infection. In Diseases of Poultry, 10th ed.; Calnek, B.W., Ed.; Iowa State University Press: Ames, IA, USA, 1997; pp. 1012–1015. [Google Scholar]
- Ryll, M.; Günther, R.; Hafez, M.H.; Hinz, K.H. Isolierung und Differenzierung eines Cytochromoxidase-negativen Ornithobacterium rhinotracheale-stamms aus Puten. Berliner und Münchener Tierärztlichen Wochenschrift 2002, 115, 274–277. [Google Scholar]
- Zehr, E.S.; Bayles, D.O.; Boatwright, W.D.; Tabatabai, L.B.; Register, K.B. Complete genome sequence of Ornithobacterium rhinotracheale strain, O.R.T-UMN 88. Stand. Genom. Sci. 2014, 9, 16. [Google Scholar] [CrossRef]
- Banani, M.; Pourbakhsh, S.A.; Khaki, P. Characterization of Ornithobacterium rhinotracheale isolates from commercial chickens. Arch. Razi Inst. 2001, 52, 27–36. [Google Scholar]
- Montes de Oca-Jimenez, R.; Veja-Sanchez, V.; Morales-Erasto, V.; Salgado-Miranda, C.; Blackall, P.J.; Soriano-Vargas, E. Phylogenetic relationship of Ornithobacterium rhinotracheale strains. J. Vet. Med. Sci. 2018, 80, 869–873. [Google Scholar] [CrossRef]
- Veiga, I.M.B.; Lüschow, D.; Gutzer, S.; Hafez, H.M.; Mühldorfer, K. Phylogenetic relationship of Ornithobacterium rhinotracheale isolated from poultry and diverse avian hosts based on 16S rRNA and rpoB gene analyses. BMC Microbiol. 2019, 19, 1–7. [Google Scholar] [CrossRef]
- Thieme, S.; Mühldorfer, K.; Lüschow, D.; Hafez, H.M. Molecular characterization of the recently emerged poultry pathogen Ornithobacterium rhinotracheale by multilocus sequence typing. PLoS ONE 2016, 11, e0148158. [Google Scholar]
- Devriese, L.A.; Herdt, P.; Haesebrouck, F. Antibiotic sensitivity and resistance in Ornithobacterium rhinotracheale strains from Belgian broiler chickens. Avian Pathol. 2001, 30, 197–200. [Google Scholar] [CrossRef] [PubMed]
- Cauwerts, K.; Herdt, P.; Haesebrouck, F.; Vervloesem, J.; Ducatelle, R. The effect of Ornithobacterium rhinotracheale vaccination of broiler breeder chickens on the performance of their progeny. Avian Pathol. 2002, 31, 619–624. [Google Scholar] [CrossRef] [PubMed]
- Nhung, N.T.; Chansiripornchai, N.; Carrique-Mas, J.J. Antimicrobial resistance in bacterial poultry pathogens: A review. Front. Vet. Sci. 2017, 4, 126. [Google Scholar] [CrossRef] [PubMed]
- Watteyn, A.; Devreese, M.; Plessers, E.; Wyns, H.; Garmyn, A.; Reddy, V.R.; Croubels, S. Efficacy of gamithromycin against Ornithobacterium rhinotracheale in turkey poults pre-infected with avian metapneumovirus. Avian Pathol. 2016, 45, 545–551. [Google Scholar] [CrossRef]
- Soriano, V.E.; Vera, N.A.; Salado, C.R.; Fernández, R.P.; Blackall, P.J. In Vitro susceptibility of Ornithobacterium rhinotracheale to several antimicrobial drugs. Avian Dis. 2003, 47, 476–480. [Google Scholar] [CrossRef]
- Watteyn, A.; Russo, E.; Garmyn, A.; De Baere, S.; Pasmans, F.; Martel, A.; Haesebrouck, F.; Montesissa, C.; De Backer, P.; Croubels, S. Clinical efficacy of florfenicol administered in the drinking water against Ornithobacterium rhinotracheale in turkey housed in different environmental conditions: A pharmacokinetic/pharmacodynamic approach. Avian Pathol. 2013, 42, 474–481. [Google Scholar] [CrossRef][Green Version]
- Van Veen, L.; Hartman, E.; Fabri, T. In Vitro antibiotic sensitivity of strains of Ornithobacterium rhinotracheale isolated in the Netherlands between 1996 and 1999. Vet. Rec. 2001, 149, 611–613. [Google Scholar] [CrossRef]
- Malik, Y.S.; Olsen, K.; Kumar, K.; Goyal, S.M. In Vitro antibiotic resistance profiles of Ornithobacterium rhinotracheale strains from Minnesota turkeys during 1996–2002. Avian Dis. 2003, 47, 588–593. [Google Scholar] [CrossRef]
- Szabó, R.; Wehmann, E.; Magyar, T. Antimicrobial susceptibility of Bordetella avium and Ornithobacterium rhinotracheale strains from wild and domesticated birds in Hungary. Acta Vet. Hung. 2015, 63, 413–424. [Google Scholar] [CrossRef]
- Marien, M.; Decostere, A.; Nauwynck, H.; Froyman, R.; Devriese, L.; Haesebrouck, F. In Vivo selection of reduced enrofloxacin susceptibility in Ornithobacterium rhinotracheale and its resistance-related mutations in gyrA. Microb. Drug Resist. 2006, 12, 140–144. [Google Scholar] [CrossRef]
- Back, A.; Sprenger, S.; Rajashekara, G.; Halvorson, D.A.; Nagaraja, K.V. Antimicrobial sensitivity of Ornithobacterium rhinotracheale isolated from different geographic locations. In Proceedings of the North Central Avian Disease Conference, Des Moines, IA, USA, 29–31 May 1997; Volume 48, pp. 22–24. [Google Scholar]
- Jansen, R.; Chansiripornchai, N.; Gaastra, W.; van Putten, J.P.M. Characterization of plasmid pOR1 from Ornithobacterium rhinotracheale and construction of a shuttle plasmid. Appl. Environ. Microbiol. 2004, 70, 5853–5858. [Google Scholar] [CrossRef] [PubMed]
- Schuijffel, D.F.; Van Empel, P.C.M.; Segers, R.P.A.M.; Van Putten, J.P.M.; Nuijten, P.J.M. Vaccine potencial of recombinate Ornithobacterium rhinotracheale antigens. Vaccine 2006, 24, 1858–1867. [Google Scholar] [CrossRef] [PubMed]
- Schuijffel, D.F.; van Empel, P.C.M.; Pennings, A.M.M.A.; van Putten, J.P.M.; Nuijten, J.P.M. Successful Selection of Cross-Protective Vaccine Candidates for Ornithobacterium rhinotracheale Infection. Infect. Immun. 2005, 73, 6812–6821. [Google Scholar] [CrossRef] [PubMed]
- Van Empel, P.; van den Bosch, H. Vaccination of chickens against Ornithobacterium rhinotracheale infection. Avian Dis. 1998, 42, 572–578. [Google Scholar] [CrossRef] [PubMed]
- Lopes, V.C.; Back, A.; Shin, H.J.; Halvorson, D.A.; Nagaraja, K.V. Development, characterization, and preliminary evaluation of a temperature-sensitive mutant live vaccine in turkeys. Avian Dis. 2002, 46, 162–168. [Google Scholar] [CrossRef]
- Bisshop, S.P.R. The Use of a Bacterin Vaccine in Broiler Breeders in the Control of Ornithobacterium Rhinotracheale in Commercial Broilers. Master’s Thesis, University of Pretoria, Pretoria, South Africa, 2005; p. 112. [Google Scholar]
- Chansiripornchai, N. Molecular Interaction of Ornithobacterium rhinotracheale with Eukaryotic Cells. Ph.D. Thesis, University of Utrecht, Utrecht, The Netherlands, 2004; p. 73. [Google Scholar]
- Gopala Krishna Murthy, T.R.; Dorairajan, N.; Balasubramaniam, G.A.; Manicavasaka Dinakaran, A.; Kalaimathi, R. The effect of vaccination of pullets against Ornithobacterium rhinotracheale infection. Avian Phatol. 2007, 36, 481–485. [Google Scholar] [CrossRef] [PubMed]
- De Herdt, P.; Broeckx, M.; Vankeirsbilck, W.; Van Den Abeele, G.; Van Gorp, S. Improved broiler performance associated with Ornithobacterium rhinotracheale vaccination in breeders. Avian Dis. 2012, 56, 365–368. [Google Scholar] [CrossRef]
- Ellakany, H.F.; Elbestawy, A.R.; Abd-Elhamid, H.S.; Gado, A.R.; Nassar, A.A.; Abdel-Latif, M.A.; Ghanima, I.I.A.; Abd El-Hack, M.E.; Swelum, A.A.; Saadeldin, I.M.; et al. Effect of experimental Ornithobacterium rhinotracheale infection along with live infectious bronchitis vaccination in broiler chickens. Poult. Sci. 2019, 98, 105–111. [Google Scholar] [CrossRef]
| Biochemical Tests | Test Interpretation | Result |
|---|---|---|
| Indol * | Degradation of tryptophan yielding indole. | − |
| Ornithine Decarboxylase | Decarboxylation of ornithine. | − |
| Catalase * | Presence of catalase enzyme by decomposing H2O2 in water and O2. | − |
| Oxidase * | Detect of indophenol production (cytochrome oxidase). | + |
| Fructose | Sucrose fermentation producing fructose and acids. | + |
| Glucose | Fermentation of glucose producing acid or acid and gas. | − |
| Mannitol | Fermentation of mannitol with acid production during the process. | − |
| Maltose | Degradation of maltose generating 2 molecules of glucose. | − |
| Motility | Determination of bacterial motility by means of flagella. | − |
| Triple Sugar Iron (TSI) * | Glucose fermentation and gas production. Fermentation of lactose and/or sucrose. Production of H2S. | − |
| Growth MacConkey | Isolation of gram-negative and inhibition of gram-positive cocci. | − |
| Hemolysis in Blood Agar | Differentiation of hemolysis production. | − |
| Growth in Nutrient Agar | Medium for preliminary culture in bacteriology. | − |
| Voges–Proskauer | Production of acetoin from the fermentation of glucose. | + |
| Urease | Urease enzyme hydrolyzing urea with ammonia formation. | + |
| Βeta-galactosidase * | Fermentation of glucose by the enzyme beta-galactosidase. Difference lactose fermentation delay of lactose non-fermenters. | + |
© 2019 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Barbosa, E.V.; Cardoso, C.V.; Silva, R.d.C.F.; Cerqueira, A.d.M.F.; Liberal, M.H.T.; Castro, H.C. Ornithobacterium rhinotracheale: An Update Review about An Emerging Poultry Pathogen. Vet. Sci. 2020, 7, 3. https://doi.org/10.3390/vetsci7010003
Barbosa EV, Cardoso CV, Silva RdCF, Cerqueira AdMF, Liberal MHT, Castro HC. Ornithobacterium rhinotracheale: An Update Review about An Emerging Poultry Pathogen. Veterinary Sciences. 2020; 7(1):3. https://doi.org/10.3390/vetsci7010003
Chicago/Turabian StyleBarbosa, Eunice Ventura, Clarissa Varajão Cardoso, Rita de Cássia Figueira Silva, Aloysio de Mello Figueiredo Cerqueira, Maíra Halfen Teixeira Liberal, and Helena Carla Castro. 2020. "Ornithobacterium rhinotracheale: An Update Review about An Emerging Poultry Pathogen" Veterinary Sciences 7, no. 1: 3. https://doi.org/10.3390/vetsci7010003
APA StyleBarbosa, E. V., Cardoso, C. V., Silva, R. d. C. F., Cerqueira, A. d. M. F., Liberal, M. H. T., & Castro, H. C. (2020). Ornithobacterium rhinotracheale: An Update Review about An Emerging Poultry Pathogen. Veterinary Sciences, 7(1), 3. https://doi.org/10.3390/vetsci7010003





