The Big Pet Diabetes Survey: Perceived Frequency and Triggers for Euthanasia
Abstract
:1. Introduction
2. Materials and Methods
2.1. Design of Survey
2.2. Recruitment of Respondents
2.3. Statistical Analysis
3. Results
3.1. Results of Univariate Analysis
3.2. Results of Multivariate Analysis
4. Discussion
5. Conclusions
Supplementary Materials
Acknowledgments
Author Contributions
Conflicts of Interest
References
- Niessen, S.J.M.; Powney, S.; Guitian, J.; Niessen, A.P.M.; Pion, P.D.; Shaw, J.A.M.; Church, D.B. Evaluation of a quality-of-life tool for cats with diabetes mellitus. J. Vet. Intern. Med. 2010, 24, 1098–1105. [Google Scholar] [CrossRef] [PubMed]
- Niessen, S.J.M.; Powney, S.; Guitian, J.; Niessen, A.P.M.; Pion, P.D.; Shaw, J.A.M.; Church, D.B. Evaluation of a quality-of-life tool for dogs with diabetes mellitus. J. Vet. Intern. Med. 2012, 26, 953–961. [Google Scholar] [CrossRef] [PubMed]
- Fall, T.; Hamlin, H.H.; Hedhammar, A.; Kämpe, O.; Egenvall, A. Diabetes mellitus in a population of 180,000 insured dogs: incidence, survival and breed distribution. J. Vet. Intern. Med. 2007, 21, 1209–1216. [Google Scholar] [CrossRef] [PubMed]
- O’Neill, D.G.; Gostelow, R.; Orme, C.; Church, D.B.; Niessen, S.J.M.; Verheyen, K.; Brodbelt, D.C. Epidemiology of diabetes mellitus among 193,435 cats attending primary-care veterinary practices in England. J. Vet. Intern. Med. 2016, 30, 964–972. [Google Scholar] [CrossRef] [PubMed]
- Kraus, M.S.; Calvert, C.A.; Jacobs, G.J.; Brown, J. Feline diabetes mellitus: A retrospective mortality study of 55 cats (1982–1994). J. Am. Anim. Hosp. Assoc. 1997, 33, 107–111. [Google Scholar] [CrossRef] [PubMed]
- Goossens, M.M.C.; Nelson, R.W.; Feldman, E.C.; Griffey, S.M. Response to insulin treatment and survival in 104 cats with diabetes mellitus (1985–1995). J. Vet. Intern. Med. 1998, 12, 1–6. [Google Scholar] [CrossRef] [PubMed]
- Callegari, C.; Mercuriali, E.; Hafner, M.; Coppola, L.M.; Guazzetti, S.; Lutz, T.A.; Reusch, C.E.; Zini, E. Survival times and prognostic factors in cats with newly diagnosed diabetes mellitus: 114 cases (2000–2009). J. Am. Vet. Med. Assoc. 2013, 243, 91–95. [Google Scholar] [CrossRef] [PubMed]
- Berendsen, M.; Knol, B.W. Treatment compliance. Tijdschr Diergeneeskd 2002, 127, 548–551. [Google Scholar] [PubMed]
- Rucinsky, R.; Cook, A.; Haley, S.; Nelson, R.; Zoran, D.L.; Poundstone, M. AAHA diabetes management guidelines for dogs and cats. J. Am. Anim. Hosp. Assoc. 2010, 46, 215–224. [Google Scholar] [CrossRef] [PubMed]
- Sparkes, A.H.; Cannon, M.; Church, D.; Fleeman, L.; Harvey, A.; Hoenig, M.; Peterson, M.E.; Reusch, C.E.; Taylor, S.; Rosenberg, D. ISFM consensus guidelines on the practical management of diabetes mellitus in cats. J. Feline Med. Surg. 2017, 17, 235–250. [Google Scholar] [CrossRef] [PubMed]
- Reja, U.; Manfreda, K.L.; Hlebec, V.; Vehovar, V. Open-ended vs close-ended questions in web questionnaires. Metodoloski Zvezki 2003, 19, 159–177. [Google Scholar]
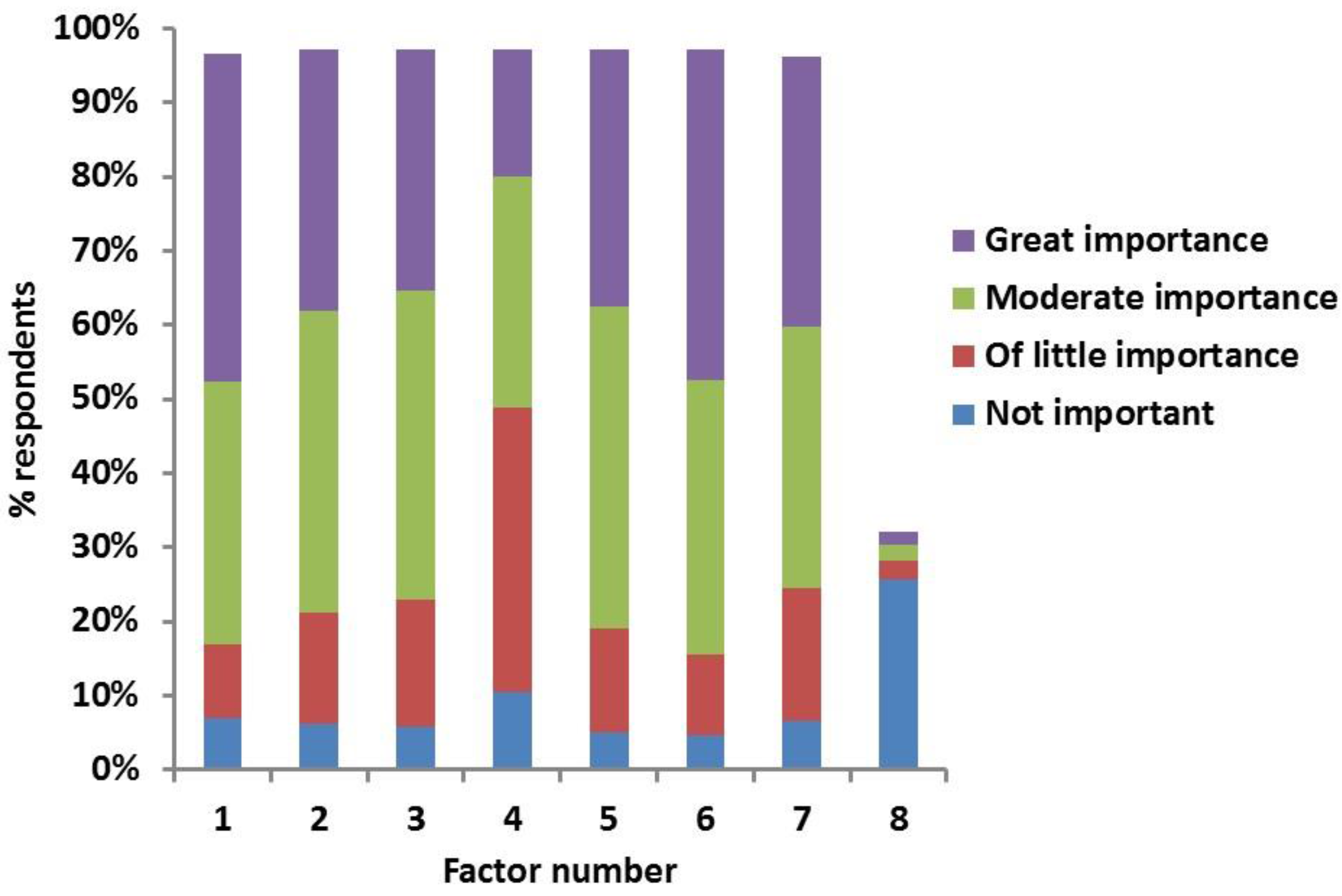
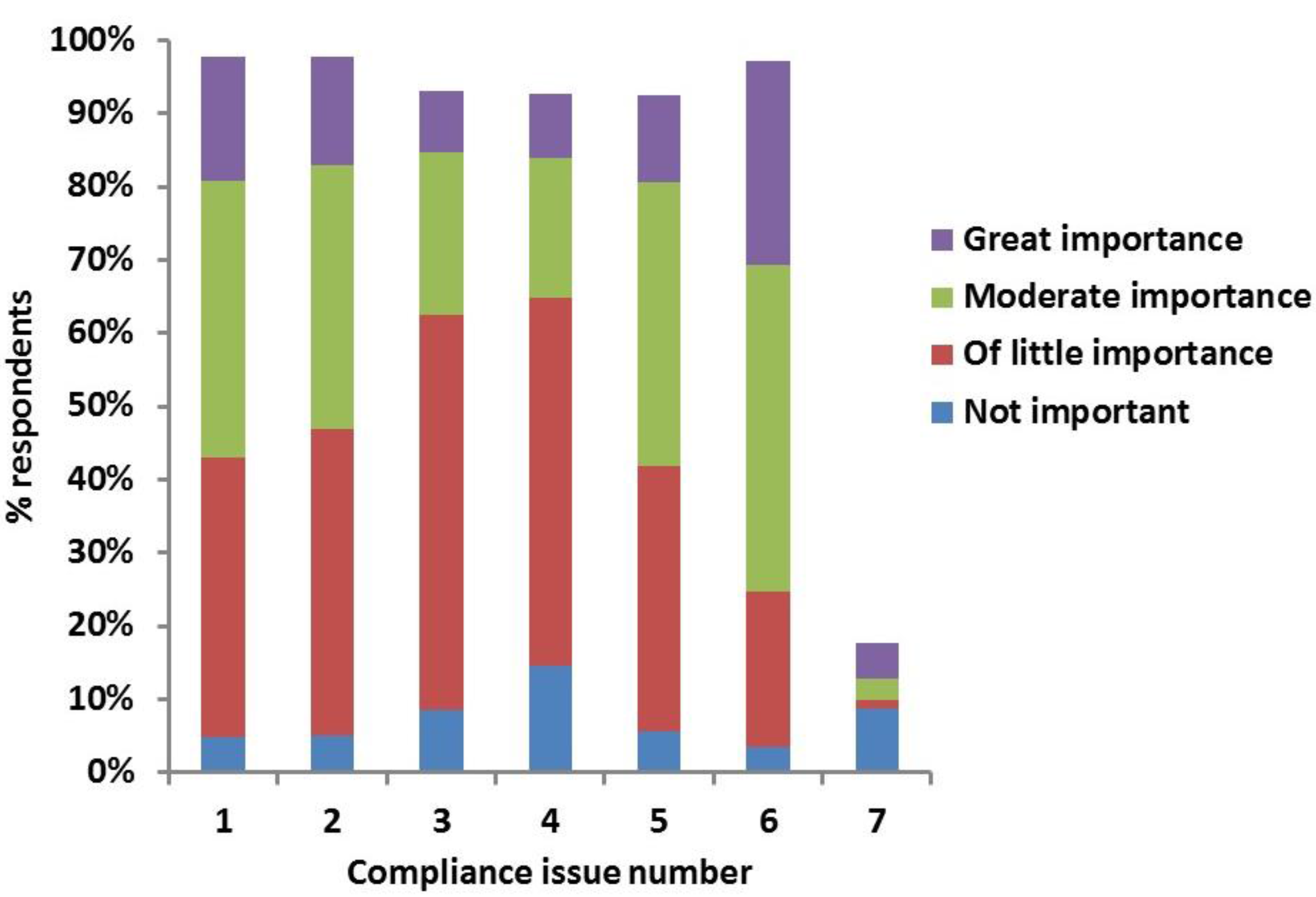
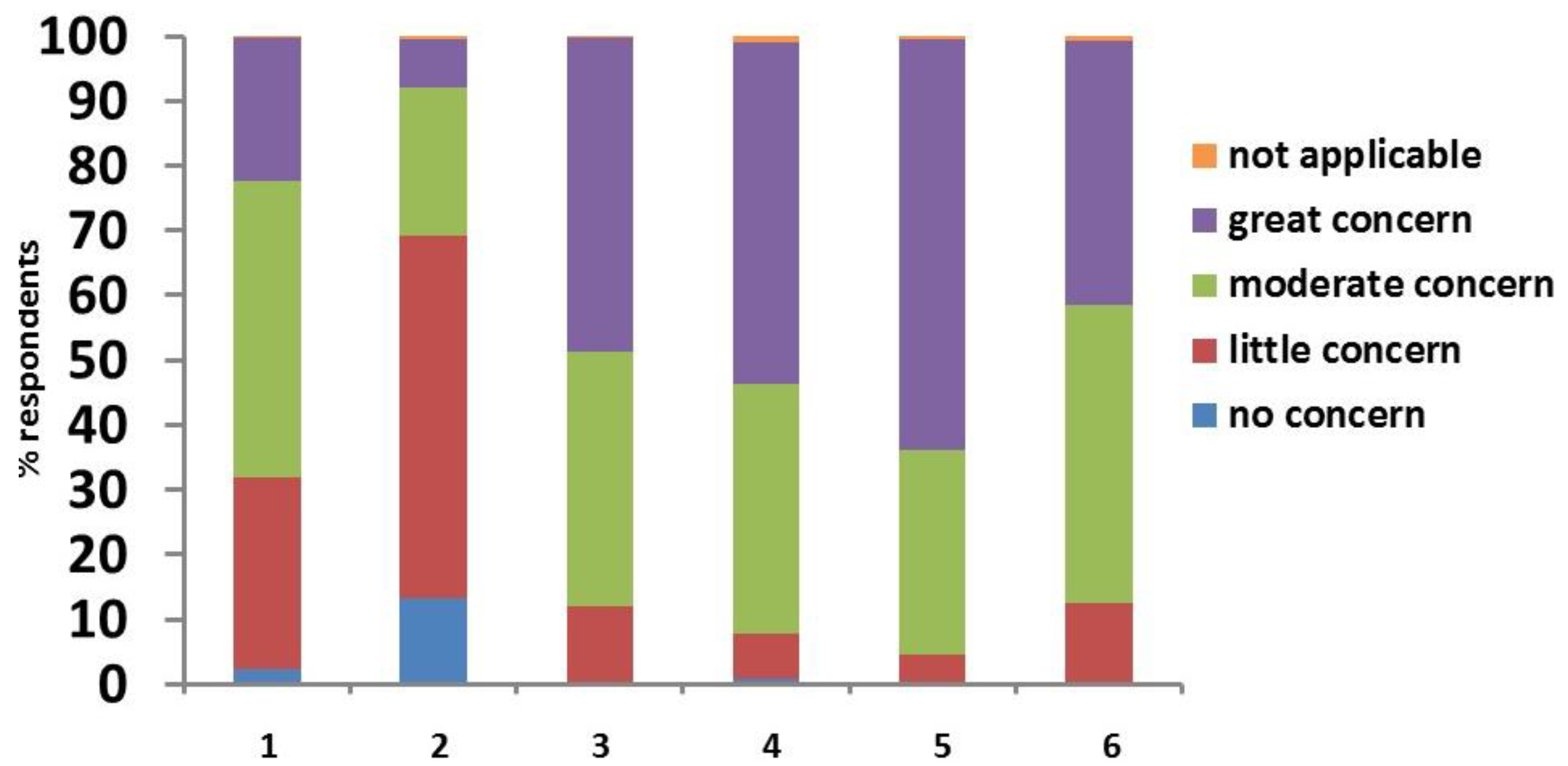

| Country or Region Practicing Clinician | Number of Respondents (%) | Location | Practice Type I | Practice Type II | % Cats and Dogs Insured | DM Diagnoses/Year |
|---|---|---|---|---|---|---|
| USA | 807 (67.8%) | Rural 95 (11.8%) Urban 192 (23.8%) Suburban 509 (63.1%) Other 11 (1.4%) | SA 715 (89.3%) Mixed 62 (7.7%) Other 20 (2.5%) | Private 732 (91.2%) Charity 9 (1.1%) Referral/Uni 37 (4.6%) Other 25 (3.1%) | <20% insured 789 (98%) >20% insured 16 (2%) | Cats: <6: 330 (40.9%) 6–10: 282 (34.9%) >10: 195 (24.2%) Dogs: <6: 492 (61.3%) 6–10: 195 (24.3%) >10: 115 (14.3%) |
| UK and Ireland | 168 (14.1%) | Rural 26 (15.5%) Urban 72 (42.9%) Suburban 67 (39.9%) Other 3 (1.8%) | SA 139 (83.2%) Mixed 26 (15.6%) Other 2 (1.2%) | Private 129 (77.2%) Charity 20 (12%) Referral/Uni 15 (9%) Other 3 (1.8%) | <20% insured 59 (35.1%) >20% insured 109 (64.9%) | Cats: <6: 90 (53.6%) 6–10: 47 (28.0%) >10: 31 (18.5%) Dogs: <6: 97 (58.1%) 6–10: 43 (25.7%) >10: 27 (16.2%) |
| Canada | 93 (7.8%) | Rural 10 (10.8%) Urban 27 (29.0%) Suburban 54 (58%) Other 2 (2.2%) | SA 80 (86%) Mixed 11 (11.8%) Other 2 (2.2%) | Private 82 (88.2%) Charity 3 (3.2%) Referral/Uni 4 (4.3%) Other 4 (4.3%) | <20% insured 90 (96.8%) >20% insured 3 (3.2%) | Cats: <6: 36 (38.7%) 6–10: 36 (38.7%) >10: 21 (22.6%) Dogs: <6: 67 (72.8%) 6–10: 19 (20.4%) >10: 6 (6.5%) |
| Continental Europe | 93 (7.8%) | Rural 13 (14.1%) Urban 46 (50%) Suburban 32 (34.8%) Other 1 (1.1%) | SA 73 (78.5%) Mixed 16 (17.2%) Other 4 (4.3%) | Private 68 (73.1%) Charity 2 (2.2%) Referral/Uni 21 (22.6%) Other 2 (2.2%) | <20% insured 85 (92.4%) >20% insured 7 (7.6%) | Cats: <6: 48 (51.6%) 6–10: 32 (34.4%) >10: 13 (14.0%) Dogs: <6: 69 (74.2%) 6–10: 14 (15.1%) >10: 10 (10.8%) |
| Australia | 29 (2.4%) | Rural 3 (10.3%) Urban 7 (24.1%) Suburban 19 (65.5%) Other 0 (0%) | SA 27 (93.1%) Mixed 2 (6.9%) Other 0 (0%) | Private 24 (82.8%) Charity 1 (3.4%) Referral/Uni 4 (13.8%) Other 0 (0%) | <20% insured 29 (100%) >20% insured 0 (0%) | Cats: <6: 13 (44.8%) 6–10: 11 (37.9%) >10: 5 (17.2%) Dogs: <6: 19 (65.5%) 6–10: 3 (10.3%) >10: 7 (24.1%) |
| Parameter | Unit | Value | |
|---|---|---|---|
| Cats | Dogs | ||
| Proportion of clinicians prescribing twice daily insulin injections | Number (percentage) of clinicians | 980 of 1182 (82.9%) | 946 of 1132 (83.6%) |
| Starting insulin dose | U/kg BW/injection: mean ± SD | 0.45 ± 0.31 | 0.60 ± 0.52 |
| Number of cats/dogs started on new diet at diagnosis | Median number of cats/dogs (IQR) | 9 of 10 (6–10) | 7 of 10 (3–9) |
| Number of cats/dogs started on oral hypoglycaemic drugs at diagnosis | Median number of cats/dogs (IQR) | 0 of 10 (0–0) | 0 of 10 (0–0) |
| Question Number | “Typically, in this practice, out of ten cats or dogs newly diagnosed with diabetes mellitus,….” (second part of the question continued below) | Cats: Median (IQR) | Dogs: Median (IQR) |
|---|---|---|---|
| C1/D1 | “… how many are euthanased on request of the owner at time of diagnosis?” | 1 (0–2) | 1 (0–1) |
| C2/D2 | “…how many are euthanased on request of the owner because of not wanting to treat with insulin injections at time of diagnosis?” | 1 (0–1) | 0 (0–1) |
| C3/D3 | “…and started on insulin injections, in how many is insulin treatment subsequently stopped within 1 month because of lack of success or compliance?” | 0 (0–1) | 0 (0–1) |
| C4/D4 | “…and started on insulin injections, in how many is insulin treatment subsequently stopped within 1 year because of lack of success or compliance?” | 1 (0–2) | 1 (0–2) |
| Question Number | “Typically, in this practice, out of ten cats or dogs newly diagnosed with diabetes mellitus (or their owners),….” (second part of the question continued below) | Cats (Cat Owners): Median (IQR) | Dogs (Dog Owners): Median (IQR) |
|---|---|---|---|
| C5/D5 | “…how many achieve a satisfactory quality of life according to the owner once treatment with insulin injections has been started?” | 8 (7–9) | 8 (7–9) |
| C6/D6 | “…how many of the owners eventually have a satisfactory quality of life and not feel limited in lifestyle because of daily insulin injections?” | 8 (6–9) | 8 (6–9) |
| C7/D7 | “…how many suffer from an apparent hypoglycaemic crisis (suggestive clinical signs OR recorded blood glucose) at some stage during treatment?“ | 2 (1–4) | 2 (1–3) |
| C8/D8 | “…how many will suffer from an episode of keto-acidosis (DKA) after insulin treatment has been initiated?“ | 1 (0–2) | 1 (0–2) |
| 9 | “...how many of the owners report having difficulties fitting in a twice daily injection treatment instead of a once daily injection treatment?” a | 2 (1–4) | |
| Factor | Frequency Euthanasia Newly Diagnosed Diabetic Cats (C1) | Frequency Euthanasia Newly Diagnosed Diabetic Dogs D1 | Frequency Euthanasia Newly Diagnosed Diabetic cats—Not Wanting to Inject C2 | Frequency Euthanasia Newly Diagnosed Diabetic Dogs—Not Wanting to Inject D2 | |||||
|---|---|---|---|---|---|---|---|---|---|
| p-value | OR (95% CI) | p-value | OR (95% CI) | p-value | OR (95% CI) | p-value | OR (95% CI) | ||
| Country | UK and Ireland | 0.331 | 0.75 (0.42–1.34) | 0.188 | 0.67 (0.38–1.21) | 0.290 | 0.72 (0.40–1.32) | 0.828 | 0.93 (0.51–1.72) |
| USA | 0.383 | 0.83 (0.54–1.27) | 0.349 | 0.81 (0.53–1.25) | 0.294 | 0.79 (0.51–1.23) | 0.835 | 0.95 (0.61–1.50) | |
| Canada | 0.001 | 2.68 (1.53–4.67) | 0.050 | 1.75 (1–3.08) | 0.003 | 2.36 (1.34–4.16) | 0.014 | 2.06 (1.15–3.68) | |
| Australia | 0.038 | 2.26 (1.04–4.88) | 0.32 | 2.38 (1.08–5.27) | 0.537 | 1.28 (0.58–2.83) | 0.105 | 1.97 (0.87–4.46) | |
| Cont. Europe a | – | a | – | a | – | a | – | a | |
| Location | Rural | 0.010 | 1.6 (1.12–2.28) | 0.001 | 1.81 (1.26–2.59) | 0.000 | 2.17 (1.51–3.12) | 0.000 | 2.17 (1.51–3.13) |
| Urban | 0.339 | 1.14 (0.87–1.47) | 0.63 | 1.29 (0.99–1.68) | 0.385 | 1.13 (0.86–1.47) | 0.300 | 1.16 (0.88–1.53) | |
| Sub-urban a | – | a | – | a | – | a | – | a | |
| Practice type I | Mixed | 0.009 | 1.69 (1.14–2.50) | 0.02 | 1.59 (1.07–2.35) | 0.987 | 1.00 (0.67–1.51) | 0.312 | 1.23 (0.82–1.85) |
| SA a | – | a | – | a | – | a | – | a | |
| Practice type II | Referral/Uni | 0.032 | 0.6 (0.37–0.96) | 0.439 | 0.83 (0.52–1.33) | 0.015 | 0.54 (0.33–0.89) | 0.560 | 0.86 (0.53–1.41) |
| Charity | 0.424 | 1.3 (0.68–2.5) | 0.101 | 1.72 (0.90–3.31) | 0.129 | 1.69 (0.86–3.33) | 0.597 | 1.2 (0.61–2.37) | |
| Private | – | a | – | a | – | a | – | a | |
| % insured | >20% | 0.693 | 1.11 (0.67–1.82) | 0.809 | 0.94 (0.57–1.56) | 0.988 | 1.00 (0.59–1.68) | 0.562 | 0.86 (0.51–1.45) |
| <20% a | – | a | – | a | – | a | – | a | |
| Factor | Frequency Treatment Stopped Cats <1 Month C3 | Frequency Treatment Stopped Dogs <1 Month D3 | Frequency Treatment Stopped Cats <1 Year C4 | Frequency Treatment Stopped Dogs <1 Year D4 | |||||
|---|---|---|---|---|---|---|---|---|---|
| p-value | OR (95% CI) | p-value | OR (95% CI) | p-value | OR (95% CI) | p-value | OR (95% CI) | ||
| Country | UK and Ireland | 0.017 | 0.47 (0.26–0.88) | 0.026 | 0.48 b (0.25–0.92) | 0.307 | 0.74 (0.41–1.32) | 0.136 | 0.64 (0.36–1.15) |
| USA | 0.033 | 0.61 (0.28–0.94) | 0.148 | 0.71 (0.44–1.13) | 0.614 | 1.12 (0.73–1.71) | 0.490 | 0.86 (0.56–1.32) | |
| Canada | 0.017 | 0.47 (0.43–0.51) | 0.630 | 0.86 (0.61–1.11) | 0.350 | 1.30 (0.79–1.81) | 0.969 | 1.01 (0.45–1.48) | |
| Australia | 0.318 | 0.65 (0.68–2.03) | 0.623 | 0.80 (0.33–1.94) | 0.939 | 1.03 (0.48–2.23) | 0.767 | 1.13 (0.51–2.49) | |
| Cont. Europe a | – | a | – | a | – | a | – | a | |
| Location | Rural | 0.766 | 1.06 (0.72–1.56) | 0.061 | 1.45 (0.98–2.14) | 0.892 | 0.98 (0.69–1.39) | 0.260 | 1.23 (0.86–1.76) |
| Urban | 0.786 | 0.96 (0.72–1.28) | 0.322 | 1.16 (0.86–1.57) | 0.451 | 0.91 (0.70–1.17) | 0.440 | 1.11 (0.85–1.44) | |
| Sub-urban a | – | a | – | a | – | a | – | a | |
| Practice type I | Mixed | 0.155 | 1.35 (0.89–2.05) | 0.149 | 1.37 (0.89–2.09) | 0.012 | 1.64 (1.12–2.41) | 0.01 | 1.67 (1.13–1.47) |
| SA a | – | a | – | a | – | a | – | a | |
| Practice type II | Referral/Uni | 0.404 | 1.23 (0.75–2.01) | 0.367 | 0.78 (0.45–1.34) | 0.045 | 1.59 (1.01–2.49) | 0.232 | 1.32 (0.84–2.09) |
| Charity | 0.023 | 2.18 (1.11–4.27) | 0.002 | 2.93 (1.49–5.78) | 0.028 | 2.05 (1.08–3.87) | 0.047 | 1.92 (1.01–3.66) | |
| Private a | – | a | – | a | – | a | – | a | |
| % insured | >20% | 0.556 | 1.18 (0.68–2.03) | 0.588 | 1.17 (0.66–2.08) | 0.991 | 1.00 (0.61–1.65) | 0.195 | 0.72 (0.43–1.19) |
| <20% a | – | a | – | a | – | a | – | a | |
© 2017 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Niessen, S.J.M.; Hazuchova, K.; Powney, S.L.; Guitian, J.; Niessen, A.P.M.; Pion, P.D.; Shaw, J.A.; Church, D.B. The Big Pet Diabetes Survey: Perceived Frequency and Triggers for Euthanasia. Vet. Sci. 2017, 4, 27. https://doi.org/10.3390/vetsci4020027
Niessen SJM, Hazuchova K, Powney SL, Guitian J, Niessen APM, Pion PD, Shaw JA, Church DB. The Big Pet Diabetes Survey: Perceived Frequency and Triggers for Euthanasia. Veterinary Sciences. 2017; 4(2):27. https://doi.org/10.3390/vetsci4020027
Chicago/Turabian StyleNiessen, Stijn J.M., Katarina Hazuchova, Sonya L. Powney, Javier Guitian, Antonius P.M. Niessen, Paul D. Pion, James A. Shaw, and David B. Church. 2017. "The Big Pet Diabetes Survey: Perceived Frequency and Triggers for Euthanasia" Veterinary Sciences 4, no. 2: 27. https://doi.org/10.3390/vetsci4020027
APA StyleNiessen, S. J. M., Hazuchova, K., Powney, S. L., Guitian, J., Niessen, A. P. M., Pion, P. D., Shaw, J. A., & Church, D. B. (2017). The Big Pet Diabetes Survey: Perceived Frequency and Triggers for Euthanasia. Veterinary Sciences, 4(2), 27. https://doi.org/10.3390/vetsci4020027





