1. Introduction
Although the prevalence of food insecurity has declined as the economy has recovered from the Great Recession that began in December 2007, nearly 16 million US households experienced food insecurity at some point in 2015 [
1]. This means that 12.7% of US households do not have the resources to ensure consistent and dependable access to a healthy diet. Most of these food insecure households (59%) participate in one or more of the federal nutrition assistance programs including the Supplemental Nutrition Assistance Program (SNAP), the National School Lunch Program, and the Special Supplemental Nutrition Program for Women, Infants, and Children (WIC). Of these, SNAP provides most of the nutrition support and SNAP-Ed agencies, an ancillary program, deliver free nutrition education for low-income households based on the Dietary Guidelines for Americans [
2].
Milk, because it is affordable, can fortify the diets of families that experience food insecurity or find a high-quality diet cost-prohibitive [
3,
4,
5,
6,
7,
8,
9]. It is rich in protein and Vitamin B12, as well as under-consumed nutrients such as Vitamin A, Vitamin D, potassium, calcium, and magnesium [
3,
4,
6,
7,
8,
10]. Research has shown that, on average, milk contributes 49.5% of Vitamin D, 25.3% of calcium, 17.1% of Vitamin B12, and 11.6% of potassium to the American diet [
6,
7]. On the other hand, milk is among the top ten sources of saturated fat and calories [
6]. More specifically, based on data from the 2003–2006 National Health & Nutrition Examination Survey, milk was the third leading source of saturated fat and the seventh leading source of calories in the American diet [
6].
Both saturated fat and excess calorie intake are linked to obesity, heart disease, and type 2 diabetes—increasing the burden of chronic disease [
11]. Not surprisingly, these diseases occur more often among populations with limited financial resources. Research shows that adults with income below 130% of the federal poverty level that participate in SNAP are more likely to be overweight or obese and experience more heart disease, stroke, or diabetes than non-participants with higher incomes [
11].
There are small, dietary changes that can significantly reduce the number of calories and the amount of saturated fat consumed without compromising nutritional intake. Nonfat and 1% have the nutritional benefits of high-fat milk but with less saturated fat and fewer calories [
2]. In a study of children (age 2 to 19), researchers concluded that replacing whole and 2% milk with nonfat or 1% milk would significantly reduce the amount of saturated fat and calories consumed at a population level without compromising the nutrient intake of potassium or calcium [
10].
Although not all researchers agree that consumption of saturated fat from dairy increases health risks [
12,
13,
14,
15,
16,
17], the Scientific Advisory Committee for the Dietary Guidelines continues to recommend that low- and nonfat dairy offers key nutrients, but with less saturated fat (a nutrient overconsumed by Americans) [
18]. Subsequently and consistent with its past recommendations [
19,
20], the 2015–2020 Dietary Guidelines [
2] reaffirmed the use of 1% or nonfat milk. These guidelines serve as the basis for federal food and nutrition education programs, such as SNAP-Ed.
Even though low-fat milk is recommended as part of a healthy diet, most Americans consume high-fat milk. The 2003–2004 National Health and Nutrition Examination Survey documented that 74.0% of all milk consumed was whole (32.3%) or 2% milk (41.7%); 1% and nonfat milk together represented 26.0% of all milk consumed (10.4% and 15.6%, respectively) by the general population [
21]. Similarly, low-fat milk sales represented 28.6% of all milk sales for this same time-period, and by 2012, low-fat milk represented barely more than a third of all milk sales (34.4%) [
22].
Not only has low-fat milk use only marginally improved over the past decade, but those with lower household income and less educational attainment are also less likely to use low-fat milk [
23,
24,
25]. In a study examining data from the 1996 National Food Stamp Program Survey, 15.6% of SNAP recipients reported using low-fat milk [
26], a prevalence that is barely half that of the general population [
22]. Low-fat milk use ranges from 38.1% among children and adolescents living in households with income greater than or equal to 350% of the federal poverty level (FPL) to a low of 9.4% among those living in households with income below 130% of the FPL (i.e., eligible to participate in SNAP) [
24].
Americans age two and older consumed about three-fourths of an 8-oz cup of milk each day [
8], which is substantially below the three 8-oz cups of low-fat milk that is recommended for daily consumption by the US Dietary Guidelines [
2]. Moreover, the mean intake of milk gradually declines with age. That is, children consume the most milk, followed by adolescents, and then adults. Yet, unlike the type of milk, income has not been found to be strongly associated with the quantity of milk consumed except among adolescents. Adolescents living in households with an income greater than 350% of FPL consumed significantly more milk than those living in a household with income between 101% and 185% of the FPL [
8].
Notwithstanding the documented disparity in low-fat milk use by socioeconomic status, no peer-reviewed studies have explored the knowledge, attitudes and beliefs of SNAP recipients toward low-fat milk. In one study, women with income higher than the median reported foregoing their taste preference for higher-fat milk to consume low-fat milk, which they perceived as healthier [
27]. These findings were the basis of a series of
1% or Less interventions conducted in the 1990s’ in West Virginia [
28,
29,
30,
31,
32], which were later replicated in California [
33] and Hawaii [
34]. Relying on data collected before and after one of the
1% or Less campaigns [
29], Butterfield and Reger concluded that, in part, positive changes in beliefs about the healthiness (less saturated-fat), taste, and cost of low-fat milk, led to a significant increase in use of low-fat milk [
28].
Maglione and colleagues, building on the findings of Booth-Butterfield and Reger [
28], explored attitudes associated with low-fat milk in Hawaii [
25]. Using a 4-item scale to measure attitudes (taste and health benefits) and a 3-item scale to measure normative beliefs (community, doctor, and friends and family), low-fat milk users had more positive attitudes toward low-fat milk than high-fat milk users, as well as more positive normative beliefs. Applying the transtheoretical model of change to measure intent to use low-fat milk, these researchers posited an intervention promoting low-fat milk could have a population-level impact although intention to change to low-fat milk was modest. Other studies have found that few intended to change the type of milk consumed [
27,
35], and most believed the type of milk currently used was best for them [
35].
Informal interviews conducted in a New York City Latino community revealed whole milk use represented a symbol of prosperity, a belief derived from the practice in some Latin American countries of diluting milk to stretch resources [
36]. A shelf-study in that same community revealed that low-fat milk was available, albeit in smaller quantities than high-fat milk, leading these researchers to conclude that high-fat milk was chosen because it was preferred, not because it was the only choice [
37].
In a more recent study, Bus and Worsley documented that Australian shoppers surveyed understood that whole milk had the most fat and calories but mistakenly believed milk was a good source of iron, Vitamin C, and fiber [
38]. Many believed “reduced-fat milk” was a good source of vitamins and calcium but more believed this about whole milk. Moreover, shoppers rated whole milk as “tasty” and “feels good in the mouth”, and in turn, were more likely to rate reduced-fat milk as “watery” and not “natural”.
In summary, over the past decade, the use of low-fat milk has only marginally improved, and there is a large disparity by socio-economic status. Little is known about the knowledge, attitudes and beliefs contributing to this pattern. The literature suggested that the taste and texture of low-fat milk are barriers to its adoption, and, that among some populations, the rich, thicker texture of whole milk may have symbolic meaning. Evaluation of an intervention implemented in the 1990s suggested that promoting the taste, healthiness (less saturated fat), and cost savings of low-fat milk led to increased consumption. On the other hand, a more recent Australian study suggested that although consumers know that low-fat milk contains less saturated fat, they are unaware or are confused about the nutritional content of milk and the differences between types of milk.
If we are to decrease the difference in milk consumption behaviors of low-income Americans so that it is more consistent with the Dietary Guidelines for Americans [
2], more research is needed to develop a successful intervention promoting low-fat milk consumption. Many behavior change initiatives fail because the program was developed without a clear understanding of the psychographics of the priority audience or the knowledge, perceptions, beliefs, attitudes, and values of those whose behavior we hope to change. Moreover, in comparison to alternate beverage choices, milk is a nutrient-dense food, and promoting low-fat milk, if it came at the cost of less milk consumption, would not further a healthy eating pattern [
10,
39]. This would be particularly disconcerting for a low-income population struggling to afford a nutrient-dense diet and avoiding food insecurity [
40]. Formative research to understand the perspectives of the priority audience reduces the risk of unintended consequences.
This study had three purposes—to establish the type of milk usually purchased by Oklahoma SNAP recipients (a population with income below 130% of the FPL); to identify sociodemographic characteristics associated with low-fat milk consumption among those SNAP recipients; and to understand SNAP recipients’ knowledge, attitudes, and beliefs toward the different types of milk that shape their milk consumption behaviors.
2. Materials and Methods
2.1. Materials
This study is based on a cross-sectional telephone survey of SNAP recipients living in the Oklahoma City media market, which covers 34 of the 77 Oklahoma counties, two of which are considered urban. All procedures were approved by the University of Oklahoma Health Sciences Institutional Review Board. As part of a data sharing agreement, the Oklahoma Department of Human Services provided identifying information including sociodemographic characteristics of the responsible household member of each SNAP household. This information was routinely collected as part of the SNAP application and semi-annual recertification process. Every respondent gave verbal consent to participate in the study.
2.2. Participants
Among those randomly selected to participate, 553 SNAP recipients were reached, and 520 interviews were completed (94.0% completion rate). Respondents were multi-ethnic and included persons identifying as non-Hispanic White (61.2%), Black (20.8%), Hispanic (8.5%), American Indian (8%), and Asian (1.5%). Most were female (66.6%), single (81.8%), and had attained a high school education or less (81.2%). All study participants had been identified as participating in the SNAP program, which means that all were low-income, having household income of no more than 130% of the FPL or receiving annual income of no more than US $26,668 for a family of four. After weighting the sample proportionally based on ethnicity, one difference was observed between the sample and the Oklahoma SNAP population. Survey respondents were more likely to live in rural areas. However, there were no differences in the types of milk usually purchased between rural and urban areas so this is unlikely to bias the results.
2.3. Measures
Measures were selected from the literature, tested for face and content validity, and pre-tested with people similar to the priority audience. Further, these and other questions were used during the formative focus group research [
41], and the ones included in this study had the most probative value. All data were self-reported.
Milk purchasing patterns. Respondents were asked the open-ended question, “Even if you buy or use more than one type of milk, which type of milk do you buy most often for your family”? and were given the opportunity to state what other types of milk were purchased. Responses to both questions were coded as whole, 2%, 1%, nonfat milk, and other (the exact response entered). The survey included three other questions related to milk purchasing patterns, including “How often do you purchase milk?” Open-ended responses were entered as weekly, every two weeks, monthly, and less often. The second question was, “Briefly what is the biggest reason why you usually buy [insert type] milk most often”? (95.3% completion). The third asked whether any changes in the type of milk purchased had been made in the past three months.
Milk nutrition knowledge. A series of 10 true-false questions measured knowledge of general milk nutrition facts. These questions assessed differences in the nutritional attributes of high- and low-fat milk, what types of milk were considered “low-fat”, and awareness of the recommended age to serve children low-fat milk.
Stages of change. High-fat milk users’ intent to change to low-fat milk was assessed by using stages of change constructs based on the Transtheoretical Model (TTM) [
42]. Pre-contemplation was measured with the statements “I would never consider switching to 1% or nonfat milk” and “I have not thought about switching to 1% or nonfat milk”. Contemplation was measured with the statement “I am considering switching to 1% or nonfat milk”. Preparation was measured using the following two options: “I am ready to switch” and “I sometimes use 1% or nonfat milk”.
2.4. Statistical Analysis
Data were analyzed using SPSS Version 20.0. Chi-square test statistics explored bivariate differences in the type of milk usually purchased by sociodemographic variables. A multivariate backward elimination regression model identified sociodemographic characteristics associated with low-fat milk use. A one-way ANOVA compared between-group differences in the mean scores on the milk-nutrition knowledge quiz. The threshold for determining statistical significance was a two-tailed test with 0.05 as the alpha level.
Two coders familiar with the research project independently identified the dominant themes emerging from the open-ended question asking each respondent to explain the reason for purchasing a particular type of milk. Coders began with open coding, assigning themes to ideas and concepts identified in the raw data. These themes were then reviewed for connection and consolidated. While most respondents named only one reason, each theme was coded to ensure that all of the reasons provided were included in the analysis. The themes and concepts that emerged were simple, and there was little coder disagreement.
3. Results
3.1. Milk Consumption Patterns
After excluding those who used other types of milk (1.7%), most SNAP recipients (92.5%) reported usually purchasing high-fat milk (44.6% whole milk and 47.9% purchasing 2% milk) and 7.5% usually purchased low-fat milk (3.9% purchased 1% milk, and 3.6% purchased nonfat milk). In addition, two-thirds of SNAP recipients (67.4%) purchased milk weekly, and 20.0% purchased it every two weeks. Most bought one type of milk (85.3%). Only 4.0% had changed the type of milk usually purchased during the previous three months.
Sociodemographic characteristics were only weakly associated with the type of milk usually purchased among this low-income population. Gender, ethnicity, marital status, residence in a rural or urban area, age, the level of educational attainment, or the presence of a child in the household alone did not significantly differ between high and low-fat milk users. Educational attainment was associated with low-fat milk use if a child lived in the household, Qw = 5.6, df = 1, SE = 0.62, p = 0.02. Among SNAP households with children, 14.6% usually purchased low-fat milk if the head of household had attained some college or more compared with 8% where the head of household had a high school education or less. The odds of using low-fat milk were 4.4 times higher (95% CI 1.3, 14.7) in SNAP households with children present when the head of household had attained some college education. There was no association between educational attainment and low-fat milk use if children did not live in the home, Qw = 0.12, df = 1, SE = 0.59, p = 0.73.
3.2. Milk Nutrition Knowledge
Overall, test scores on the true-false quiz measuring milk-nutrition knowledge were no better than guessing (M = 51.1, SD = 22.2). On the other hand, low-fat milk users (M = 67.4, SD = 23.0) scored significantly higher on the milk-nutrition quiz than high-fat milk users (M = 49.8, SD = 21.6); t(494) = 4.7, p = 0.00. Moreover, there was progressive improvement in milk nutrition knowledge among SNAP recipients with each successive reduction in the fat content of the type of milk consumed, F(1, 492) = 22.9, p = 0.00. Whole milk users had an average score of 46.0 (SD = 21.4), 2% milk users had an average score of 53.2 (SD = 21.3), 1% milk users had an average score of 66.0 (SD = 25.0), and nonfat milk users had an average score of 69.0 (SD = 21.2).
Most SNAP recipients surveyed answered correctly that the fat content differed among the different types of milk (
Table 1). Yet, few understood that 2% milk was not low-fat milk. However, 1% milk users were significantly more likely than high-fat milk users to know that 2% milk was not low-fat milk, X2(1,
n = 479) = 6.2,
p = 0.01. Other differences in milk nutrition knowledge emerged between high- and low-fat milk users. More SNAP recipients who used low-fat milk understood that 1% milk was not watered-down whole milk, X2(1,
n = 496) = 18.5,
p = 0.00. In addition, low-fat milk users had significantly more correct answers than high-fat milk users on questions exploring their general knowledge of the nutrients in the different types of milk—all types of milk have the same amount of calcium, X2(1,
n = 496) = 5.1,
p = 0.02, and the same amount of Vitamin D, X2(1,
n = 497) = 7.6,
p = 0.01. Similarly, low-fat milk users were more likely to understand that 1% milk has the same vitamins and minerals as whole milk, X2(1,
n = 496) = 6.9,
p = 0.01.
3.3. Reasons for the Type of Milk Usually Purchased
SNAP respondents were asked to give an open-ended answer that explained their reasoning for choosing the particular type of milk usually purchased. After organizing these responses into themes, the most common reasons related to the perceived health benefits of milk (41.9%) or its taste (30.2%). Some purchased the type of milk based on habit (7.8%). Very few respondents attributed price as an influential factor (1.2%). Responses coded as “other” were vague or not responsive to the question (14.4%). For example, these responses described how milk was used in the household (e.g., “on cereal” or “in cooking”) or who usually drank the most milk (e.g., “the older girls drink the 2%, and my infant drinks the whole milk”).
However, as illustrated in
Table 2, the reason for the type of milk consumed differed by type. Among SNAP recipients who usually purchased whole milk, taste (49.5%) influenced its purchase more often than health benefits (17.7%), and it was the taste and texture of whole milk that was preferred (
Table 2). As this respondent explained, “It (whole milk) tastes like milk—the rest tastes like colored water”.
For those SNAP recipients who usually purchased whole milk for health-related reasons, most described whole milk as “healthier” with no further explanation. However, when the health benefits were described, many stated whole milk had more vitamins and minerals than lower-fat milk. For example, explanations included “for the Vitamin D” or “It (has) more Vitamin D in it than the other kinds”. Other explanations included “It just feels like I get more vitamins and … high protein”. Similarly, whole milk was believed to be best for children, regardless of age. As explained by one SNAP recipient, “It (whole milk) has more vitamins for my kids”. Other explanations included, “Whole milk is better for the kids because it has more calcium for their bones”.
Other common health-related reasons that were reported included the recommendation of a physician or because of a health condition. When whole milk had been recommended by the children’s pediatrician, it appeared that this recommendation influenced the type of milk used by the whole family. A few described whole milk as “real”, or more “natural”.
For 2% milk users, unlike whole milk users, the perceived health benefits (57.1%) influenced the type of milk chosen most often, not taste (
Table 2). The health benefits cited most often by these SNAP recipients were less fat and fewer calories, usually less fat. About one in four perceived 2% milk as healthier, stating “it’s better for us”, “for health”, and “it’s healthier”. Other themes that emerged were that 2% was recommended by a physician or dietician or that 2% was chosen because of a “health condition” such as being diabetic or lactose intolerant.
Two unique reasons emerged among 2% milk users. For a few SNAP recipients, the health benefits of consuming less fat were valued, but the trade-off between taste and health benefits warranted only moving to 2% milk. One respondent exemplified the balance between taste and health benefits, stating “I basically was trying to cut down on fat. Two percent (2%) milk still tastes good; 1% was a little too weak for me”. Further, at the time of the survey, WIC policies encouraged low-fat milk use but allowed families with children age 2 and older to use vouchers for the purchase of 2%, 1%, and nonfat milk, which led a few SNAP recipients to choose 2% milk because “that was what WIC allowed”.
There was little difference in attitudes between 1% and nonfat milk users. Among those who usually purchased 1% milk, 85.0% said that the biggest reason for this purchase was its health benefits. The frequency increased slightly to 88.2% among nonfat milk users. These SNAP recipients, like many 2% milk users, chose 1% and nonfat milk because they preferred milk with less fat and fewer calories. “Less fat” was expressed as a benefit more often than “fewer calories”.
Habit influenced the type of milk consumed among SNAP recipients who used whole or 2% milk, but not those who used low-fat milk. As these whole and 2% milk users explained, “(it was what) I grew up drinking”, or “It is just the one I always grab”. Deference to maternal figures was also mentioned. For example, one SNAP recipient explained that she used whole milk because that was what her mother had purchased. For other respondents, 2% milk use was a newly formed habit, or at least it was a different type of milk than they had consumed during childhood. For example, one respondent explained, “I just got used to the taste of it. I used to prefer whole milk, but I believe 2% is better for you”.
3.4. Stages of Change
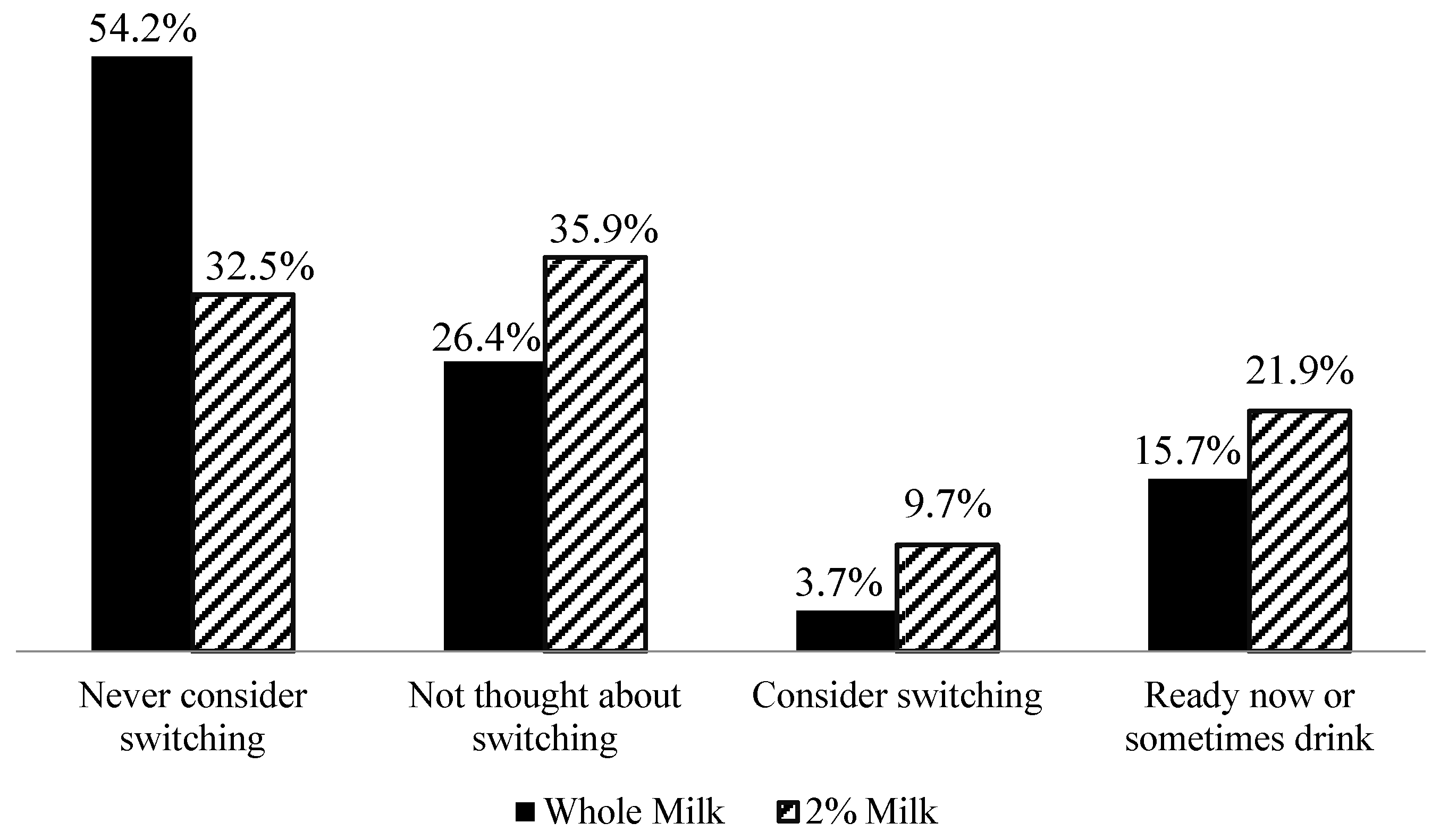
Almost three-fourths (74.2%) of high-fat milk users were in the pre-contemplation stages of the Transtheoretical Model of behavior change theory (
Figure 1). These SNAP recipients answered that they would never consider switching to 1% or non-fat milk (42.7%), or had not thought about switching to 1% or nonfat milk (31.5%). SNAP recipients who reported using 2% milk were more likely to contemplate or sometimes use low-fat milk than those who used whole milk, X2(3,
n = 453) = 23.9,
p = 0.00. Moreover, SNAP recipients with higher scores on the milk nutrition quiz were more likely to be considering or sometimes use low-fat milk, (M = 57.4, SD = 21.6), than those with lower scores, (M = 47.4, SD = 21.1), t(452) = 4.4,
p = 0.00, 95% CI [14.5, 5.5].
4. Discussion
Based on our findings, low-fat milk use among Oklahoma SNAP recipients was remarkably lower than the 34.4% indicated by national milk sales data [
22]. Among this sample of Oklahoma SNAP recipients, 7.5% reported using low-fat milk, a finding comparable to Kitt et al., who found 9.4% of children living in households with income below 130% of the FPL consumed low-fat milk [
24]. Moreover, the evidence revealed only a weak association between low-fat milk use and sociodemographic characteristics.
Rather, this study found that the barriers to changing to low-fat milk were associated with poor milk nutrition knowledge and taste preferences. High-fat milk users understood that the fat content differed between the types of milk but did not know that 2% was not low-fat milk; that 1% milk had the same vitamins and minerals of whole milk; and that 1% and nonfat milk were not watered down.
Past interventions, such as the
1% or Less campaigns of the 1980s and 1990s [
28,
29,
30,
31,
32,
33,
34], promoted reducing saturated fat as the primary benefit of using low-fat milk. Perhaps, at that time, this nutrition fact was not well-known. However in this study, SNAP recipients usually understood that the main difference between the types of milk was the amount of saturated fat, a finding similar to that of Bus and Worsley [
38]. Furthermore, most of the SNAP recipients stated that consuming less saturated fat was the reason they used lower-fat milk (2%, 1% or nonfat milk), suggesting that this was a highly valued benefit, but this alone was not enough for 2% milk users to change to 1% low-fat milk.
Instead, confusion about other milk nutrition facts appeared to be a barrier to adoption of low-fat milk. For example, many believed that 2% milk was low-fat milk, and seemed unaware that choosing 2% milk over whole milk only reduced the saturated fat from 5 g per cup to 3.5 g, a 30% reduction. In comparison, moving from whole to 1% milk reduced the saturated fat to 1.5 g per cup, a 70% reduction. Unfortunately, the nutrition label is either not used or unintelligible to most SNAP recipients. Thus, any promotion must describe the substantial reduction in saturated fat and calories of 1% or nonfat milk, rather than just encouraging the use of “low-fat milk” since this term is not well understood.
Equally, if not more importantly, a barrier to the adoption of low-fat milk was the misperception that low-fat milk had fewer vitamins and minerals than high-fat milk. The reasons given for the usual type of milk purchased revealed low-fat milk was perceived as watery—a diluted milk with fewer of the valued vitamins and minerals of milk, such as calcium and Vitamin D. Answers to specific questions on the milk nutrition quiz reinforced this finding.
Product familiarity is another known motivation for food choice among low-income populations [
43] and our findings indicate that use of higher-fat milks, particularly whole milk, was an entrenched habit among the Oklahoma SNAP population. Many SNAP beneficiaries used the same type of milk as consumed during childhood, and few had changed the type of milk used during the three-month period preceding the study. Similar to Tuorila [
35], most high-fat milk users were not contemplating changing to lower-fat milk.
Regardless, 2% milk users showed more willingness to consider changing to low-fat milk than whole milk users. They valued the benefit of consuming less saturated fat. All of these facts suggest that current 2% milk users will be more receptive to efforts to promote 1% milk consumption.
Previous studies have concluded that price is an influential motive for choosing foods among low-income populations [
43,
44]. Cost savings were also used successfully to promote low-fat milk in the
1% or Less campaigns [
30,
31]. However, low-fat milk usually costs less in Oklahoma than higher fat milk and few SNAP recipients sought out these price savings. Ariely posits that the quality of a product is subjectively discounted when it costs less than similar items [
45]. This study documents that most SNAP recipients believed low-fat milk is inferior to higher-fat milk. It is unclear whether the lower price predictably but irrationally influenced this negative evaluation or whether the price differential is too small to overcome the negative evaluation of low-fat milk. More research is needed to understand why these SNAP recipients were not motivated enough by price to choose 1% or nonfat milk.