Dimethoate Induces DNA Damage and Mitochondrial Dysfunction Triggering Apoptosis in Rat Bone-Marrow and Peripheral Blood Cells
Abstract
1. Introduction
2. Material and Methods
2.1. Chemicals
2.2. Animals—Housing, Acclimatization and Allocation of Groups
2.3. Treatment
2.4. Cytogenetic Assays in Bone Marrow Cells
2.4.1. Micronucleus Test (MNT)
2.4.2. Chromosomal Aberration (CA) Assay
2.5. Comet Assay
2.6. Flow Cytometry Based Measurement
2.6.1. Isolation of WBCs
2.6.2. Cell Cycle Phase Distribution
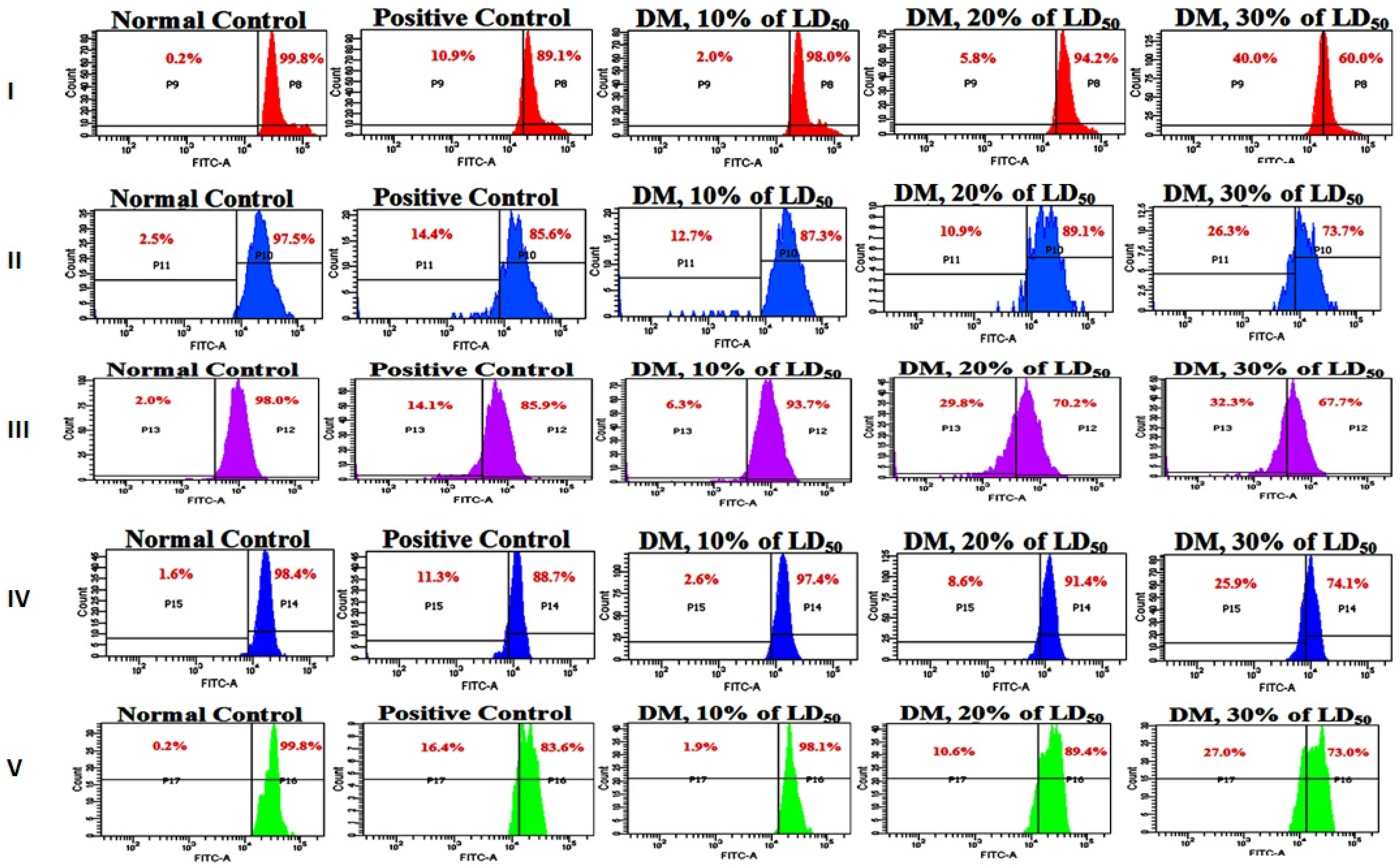
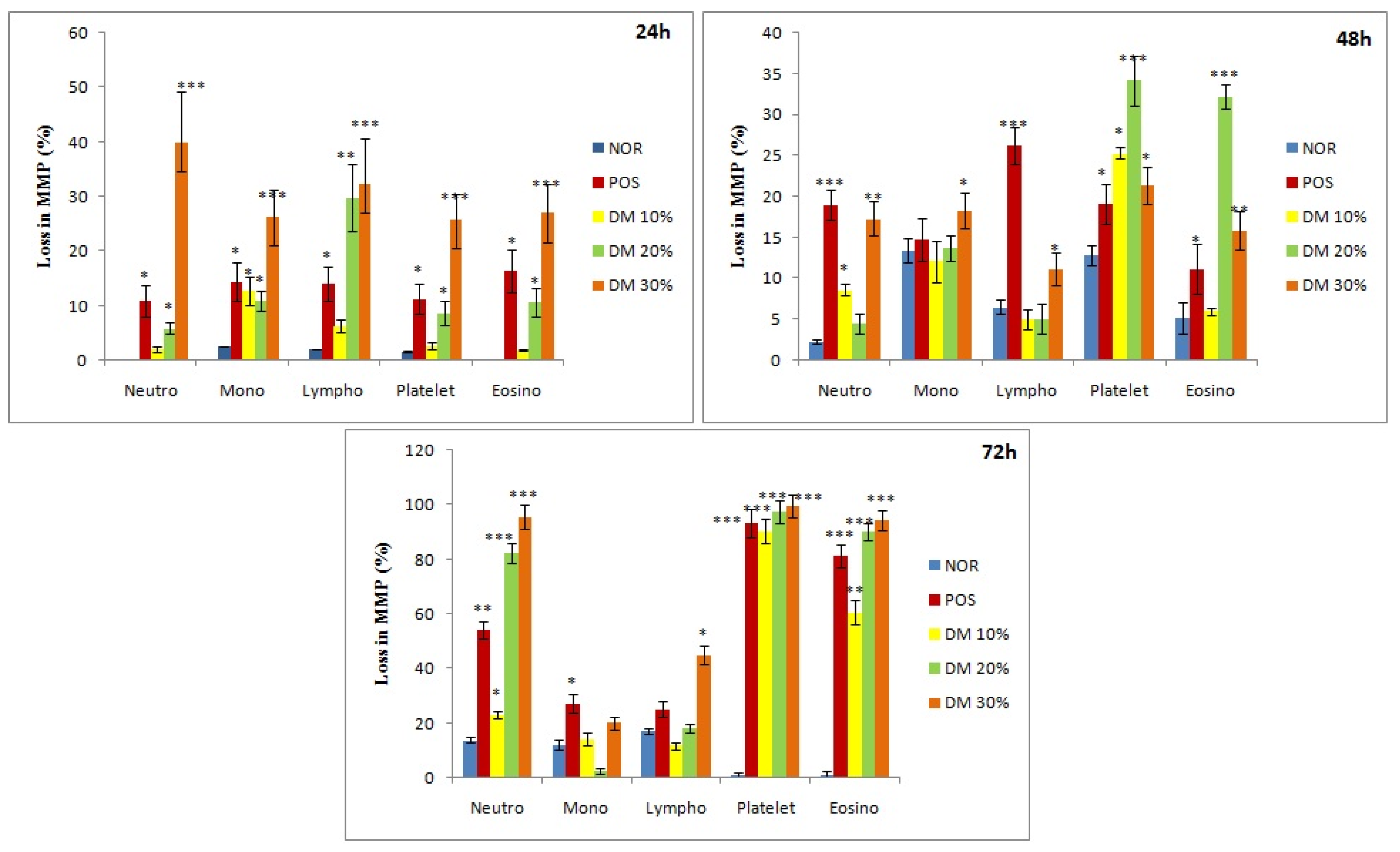
2.6.3. Measurement of Mitochondrial Membrane Potential (Ψm)
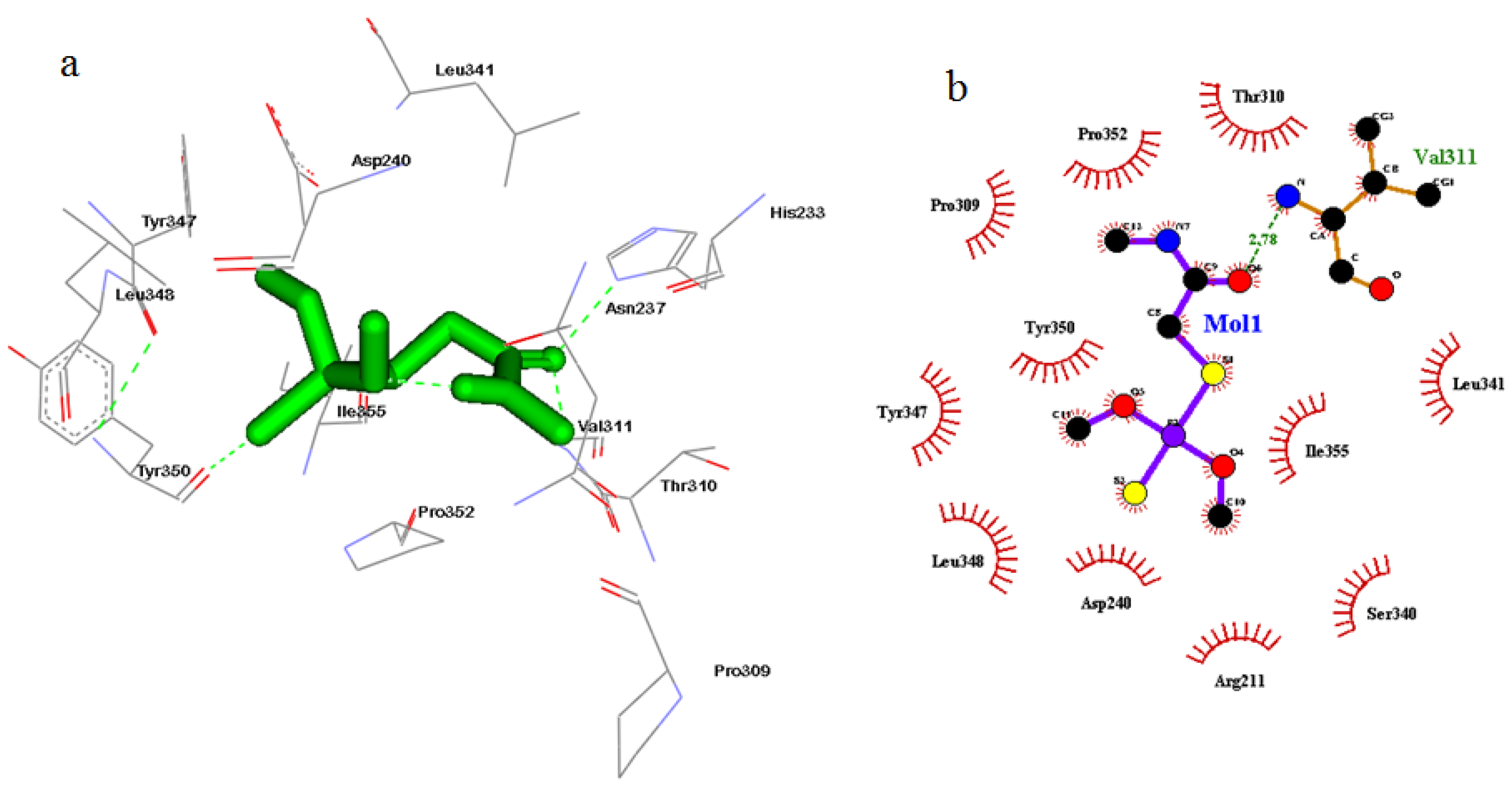
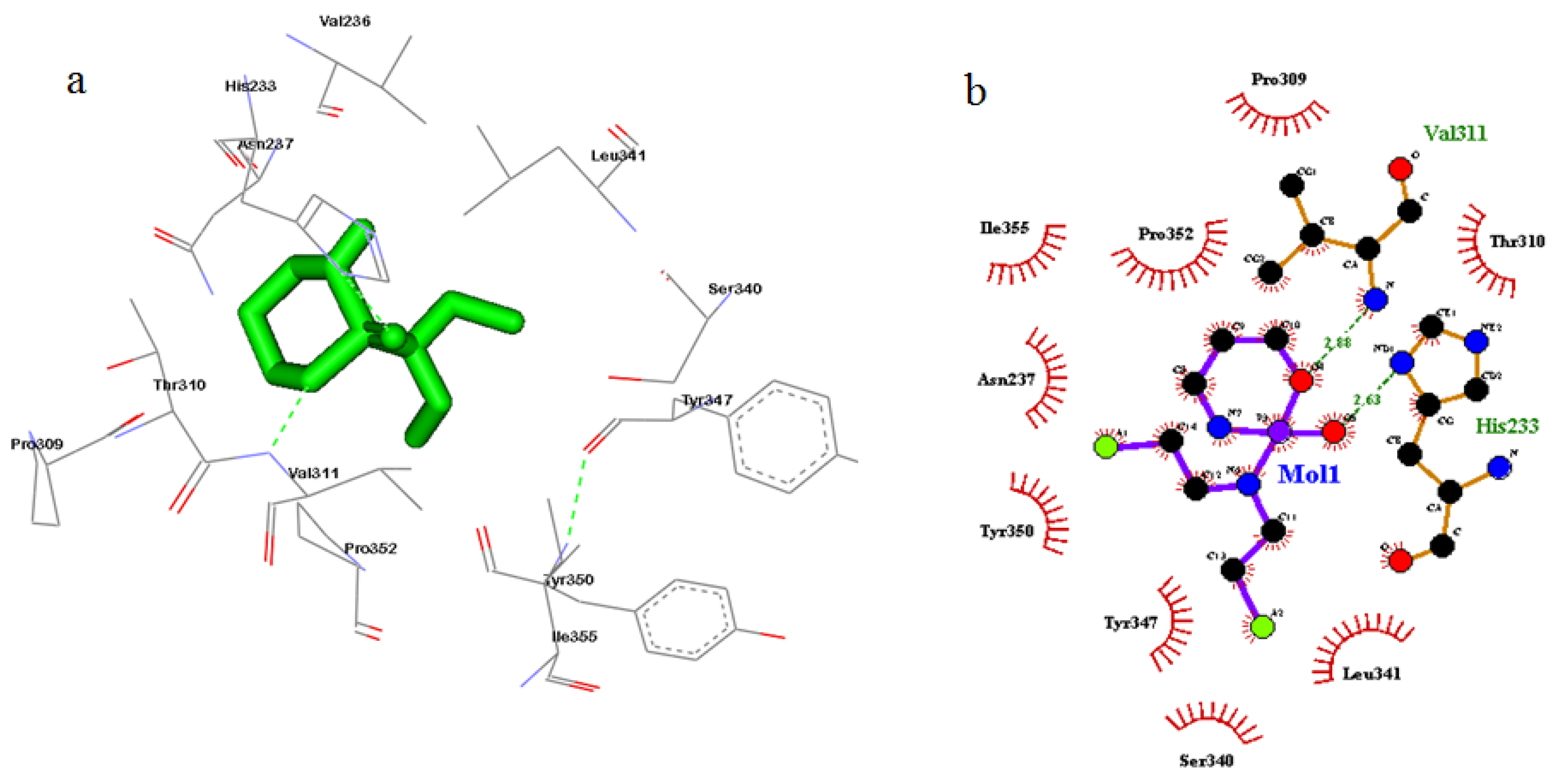
2.7. Molecular Docking Study
2.8. Statistical Analysis
3. Results
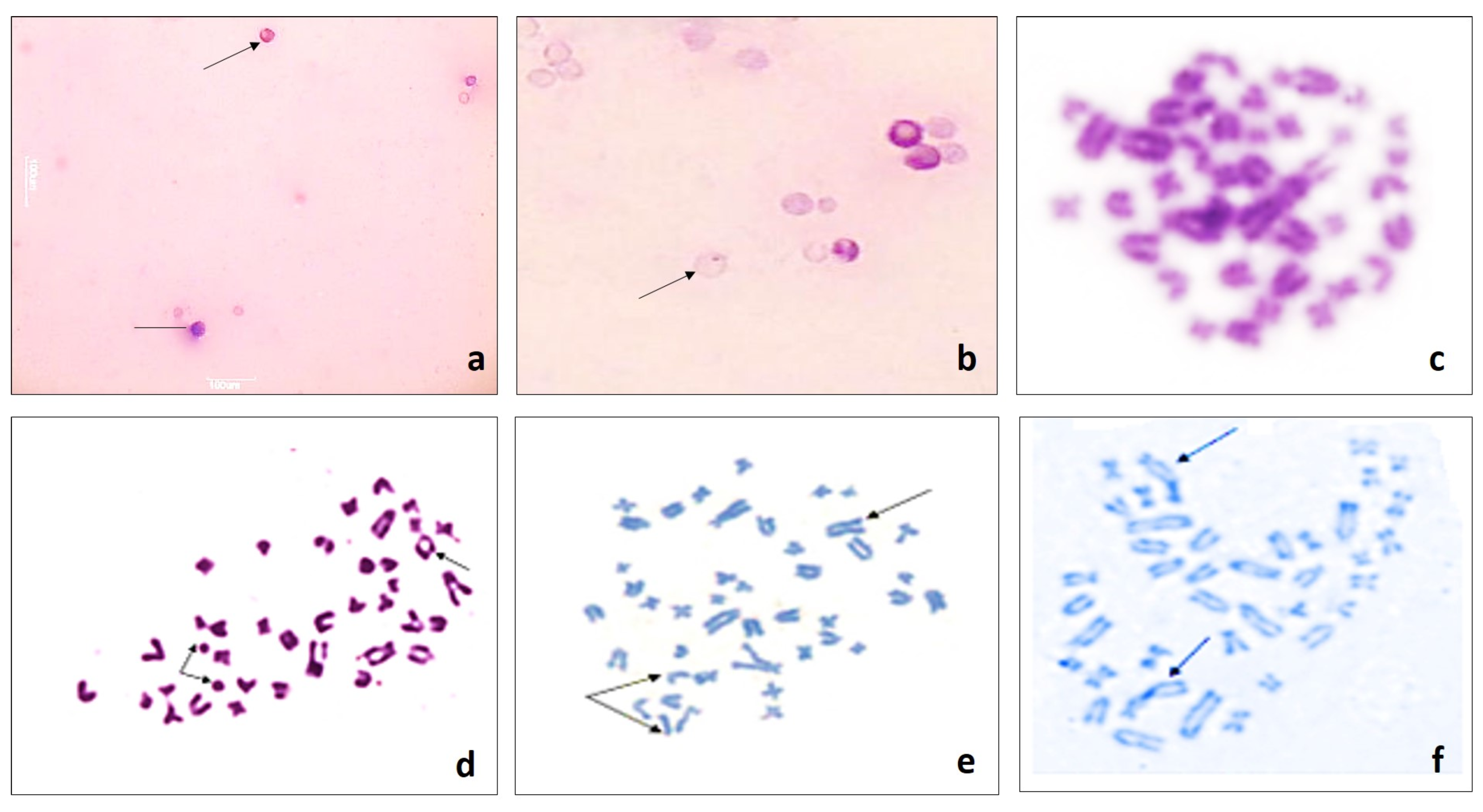
3.1. Micronucleus Test (MNT)
3.2. Chromosomal Aberration (CA)
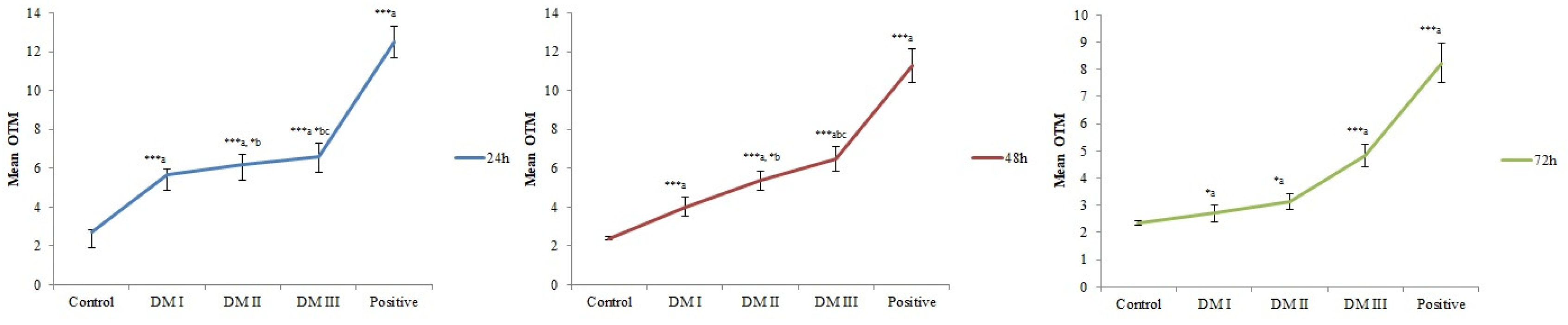
3.3. Comet Assay
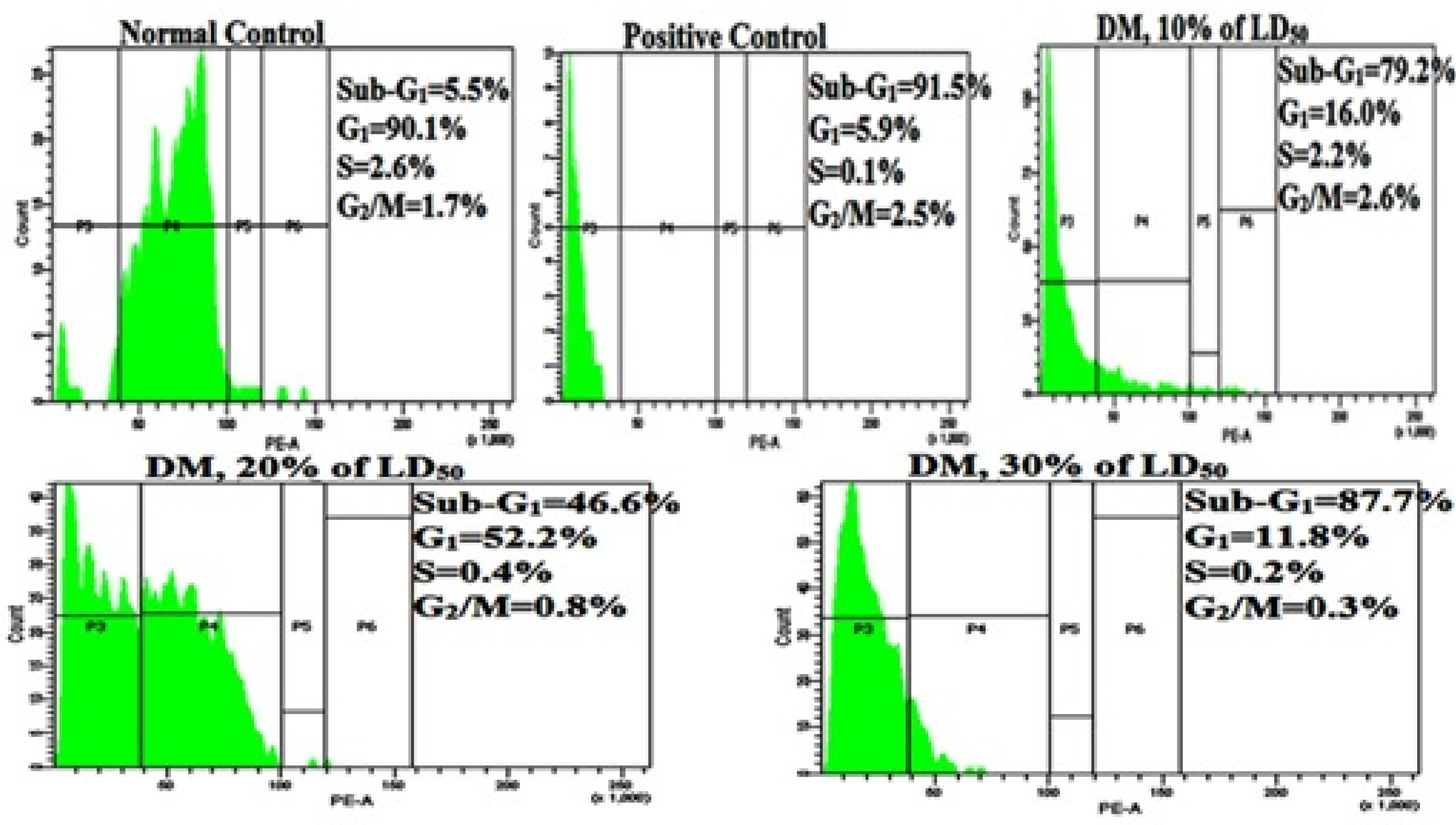
3.4. Cell Cycle Analysis
3.5. Cyclin A2 Inhibition and Cell Cycle Analysis
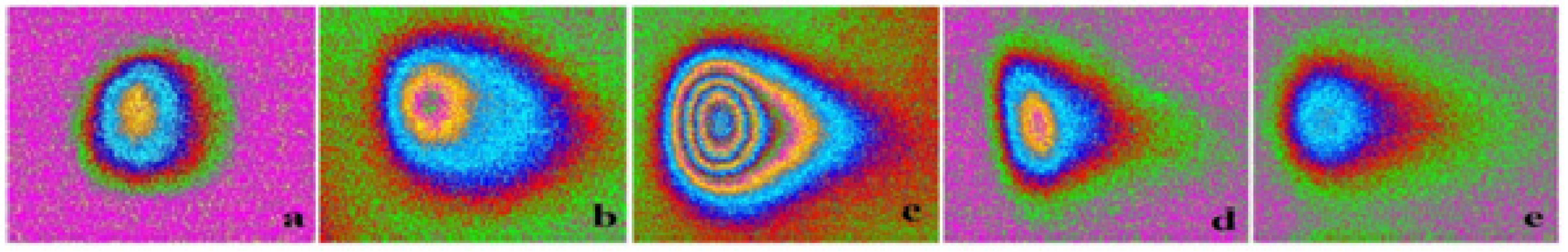
3.6. Analysis of Mitochondrial Membrane Potential
4. Discussion
5. Conclusions
Author Contributions
Funding
Acknowledgments
Conflicts of Interest
References
- Berkowitz, B. Contaminant Geochemistry: Interactions and Transport in the Subsurface Environment, 1st ed.; Springer Science & Business: Berlin/Heidelberg, Germany, 2014. [Google Scholar]
- ATSDR. Petitioned Public Health Assessment: Keil Chemical; Hammond: Lake County, IN, USA, 2001; EPA Facility ID: IND005421755. [Google Scholar]
- IARC. Miscellaneous Pesticides. IARC Monograph Evaluation of Carcinogenic Risk of Chemicals to Humans. IARC Monographs 1983, 30, 1–5424. [Google Scholar]
- Umap, S.A.; Jangde, C.R.; Tiwari, V.; Limsay, R.; Bhandarkar, A.; Jahan, A.; Kurkure, N. Amelioration of Dimethoate-induced toxicity by Morinda citrifolia in Wistar albino rats. Indian J. Vet. Pathol. 2014, 38, 244–249. [Google Scholar] [CrossRef]
- Gallo, M.A.; Lawryk, N.J. Organic Phosphorus Pesticides. In Handbook of Pesticide Toxicology; Hayes, W.J., Jr., Laws, E.R., Eds.; Academic: New York, NY, USA, 1991; Volume 16, pp. 917–1123. [Google Scholar]
- Nazam, N.; Shaikh, S.; Lone, M.I.; Sharma, M.; Ahmad, W. Combined in silico and in vivo studies shed insights into the acute acetylcholinesterase response in rat and human brain. Biotech. Appl. Biochem. 2015, 62, 407–415. [Google Scholar] [CrossRef] [PubMed]
- Horticulture Week Bulletin. 2010. Available online: http://www.hortweek.com/resources/PestsAndDiseases/995126/New-residue level rules mean dimethoate-banned-vegetable-crops/ (accessed on 8 April 2010).
- Gupta, S.; Shukla, D. A case report on severe Dimethoate poisoning: Do we know everything. Ind. J. Appl. Res. 2014, 4, 584–585. [Google Scholar]
- Abhilash, P.C.; Singh, N. Pesticide use and application: An Indian scenario. J. Hazard. Mater. 2009, 165, 1–12. [Google Scholar] [CrossRef]
- Waddell, B.L.; Zahm, S.H.; Baris, D.; Weisenburger, D.D.; Holmes, F.; Burmeister, L.F.; Cantor, K.P.; Blair, A. Agricultural use of organophosphate pesticides and the risk of non-Hodgkin’s lymphoma among male farmers (United States). Cancer Causes Control 2001, 12, 509–517. [Google Scholar] [CrossRef] [PubMed]
- Soldin, O.P.; Nsouli-Maktabi, H.; Genkinger, J.M.; Loffredo, C.A.; Ortega-García, J.A.; Colantino, D.; Barr, D.B.; Luban, N.L.; Shad, A.T.; Nelson, D.; et al. Pediatric acute lymphoblastic leukemia and exposure to pesticides. Drug Monit. 2009, 31, 495–501. [Google Scholar] [CrossRef] [PubMed]
- Bhunya, S.P.; Behera, J. Centromeric sensitivity of mouse chromosomes to the systemic insecticide dimethoate (Rogor). Curr. Sci. 1975, 44, 859–860. [Google Scholar]
- San Sabastion, J.R.; Naismith, R.W.; Matthews, R.J. In Vivo Bone Marrow Cytogenetics Rat Metaphase Analysis: Dimethoate CL 12,880. Unpublished Study Performed for the Dimethoate Task Force, Farmoplast, Milano, Italy; EPA Accession No. 259921; Pharmakon Research International: Waverly PA, USA, 1985. [Google Scholar]
- US EPA. Memorandum on Dimethoate—Assessment of Mutagenicity; TB Proj. No. 7–0037; United States Environmental Protection Agency: Washington, DC, USA, 1987.
- Ayed-Boussema, I.; Rjiba, K.; Mnasri, N.; Moussa, A.; Bacha, H. Genotoxicity evaluation of dimethoate to experimental mice by micronucleus, chromosome aberration tests, and comet assay. Int. J. Toxicol. 2012, 31, 78–85. [Google Scholar] [CrossRef]
- Dolara, P.; Salvadori, M.; Capobianco, T.; Torricelli, F. Sister-chromatid exchanges in human lymphocytes induced by dimethoate, omethoate, deltamethrin, benomyl and their mixture. Mutat. Res. 1992, 283, 113–118. [Google Scholar] [CrossRef]
- Heikal, T.M.; Mossa, A.T.H.; Nawwar, G.A.M.; El-Sherbiny, M.; Ghanem, H.Z. Protective effect of a synthetic antioxidant “Acetyl Gallate Derivative” against dimethoate induced DNA damage and oxidant/antioxidant Status in Male rats. J. Environ. Anal. Toxicol. 2012, 2, 155. [Google Scholar] [CrossRef]
- Saquib, Q.; Attia, S.M.; Siddiqui, M.A.; Aboul-Soud, M.A.; Alkhedhairy, A.A.; Giesy, J.P.; Musarrat, J. Phorate-induced oxidative stress, DNA damage and transcriptional activation of p53 and caspase genes in male Wistar rats. Toxicol. Appl. Pharm. 2012, 259, 54–65. [Google Scholar] [CrossRef] [PubMed]
- Eroglu, H. Toxic nuclear effects of the organophosphorus insecticide Dichlorvos (DDVP) in human peripheral blood lymphocytes. Acta Biol. Hung. 2009, 60, 409–416. [Google Scholar] [CrossRef] [PubMed]
- Tian, Y.; Yamauchi, T. Micronucleus formation in 3-day mouse embryos associated with maternal exposure to chlorpyrifos during the early preimplantation period. Reprod. Toxicol. 2003, 17, 401–405. [Google Scholar] [CrossRef]
- Prasad, S.; Srivatava, S.; Singh, M.; Shukla, Y. Clastogenic effects of glyphosate in bone marrow cells of Swiss albino mice. J. Toxicol. 2009, 2009, 1–6. [Google Scholar] [CrossRef]
- Al-ahmadi, M.S. Cytogenetic effect of chitosan on mitotic chromosomes of root tip cells of Vicia faba. Life Sci. J. 2015, 12, 158–162. [Google Scholar]
- Bhattacharjya, S.; Roy, S.K.; Ganguly, A.; Sarkar, S.; Panda, C.K.; Bhattacharyya, D.; Bhattacharyya, N.P.; Roychowdhury, S. Inhibition of nucleoporin member Nup214expression by miR-133b perturbs mitotic timing and leads to cell death. Mol. Cancer 2015, 14, 42. [Google Scholar] [CrossRef]
- Kang, S.H.; Kwon, J.Y.; Lee, J.K.; Seo, Y.R. Recent advances in in vivo genotoxicity testing: Prediction of carcinogenic potential using comet and micronucleus assay in animal models. J. Cancer Prev. 2013, 18, 277–288. [Google Scholar] [CrossRef]
- Wada, K.; Fukuyama, T.; Nobuaki, N.N.; Matsumoto, K. Assessment of the in vivo genotoxicity of cadmium chloride, chloroform, and d,l-menthol as coded test chemicals using the alkaline comet assay. Mutat. Res. 2015, 786–788, 114–119. [Google Scholar] [CrossRef]
- Musch, A. Exposure: Qualitative and Quantitative Aspects; and Dose–Time–Effect Relationships. In Toxicology Principles and Applications; Niesink, R.J.M., de Vries, J., Hollinger, M.A., Eds.; CRC Press: Boca Raton, FL, USA, 1996; pp. 187–219. [Google Scholar]
- Patlolla, A.K.; Tchounwon, P.B. Cytogenetic evaluation of arsenic trioxide toxicity in Sprague-Dawley rats. Mutat. Res. Genet. Toxicol. Environ. Mutagen. 2005, 587, 126–133. [Google Scholar] [CrossRef]
- OECD. Guideline for the Testing of Chemicals Mammalian Bone Marrow Chromosomal Aberration Test; DRAFT TG 475; OECD: Paris, France, 2013. [Google Scholar]
- Schmid, W. The micronucleus test. Mutat. Res. 1975, 31, 9–15. [Google Scholar] [CrossRef]
- Preston, R.J.; Dean, B.J.; Galloway, S.; Holden, H.; McFee, A.F.; Shelby, M. Mammalian in vivo cytogenetic assays: Analysis of chromosome aberrations in bone marrow cells. Mutat. Res. 1987, 189, 157–165. [Google Scholar] [CrossRef]
- Singh, N.P.; McCoy, M.T.; Tice, R.R.; Schneider, E.L. A simple technique for quantitation of low levels of DNA damage in individual cells. Exp. Cell. Res. 1988, 175, 184–191. [Google Scholar] [CrossRef]
- Herck, V.H.; Baumans, V.; Brandt, C.J.W.M.; Boere, H.A.G.; Hesp, A.P.M.; Van Lith, H.A.; Schurink, M.; Beynen, A.C. Blood sampling from the retro-orbital plexus, the saphenous vein and the tail vein in rats: Comparative effects on selected behavioural and blood variables. Lab. Anim. Refinement Enrich. Forum. Lab. Anim. 2001, 35, 131. [Google Scholar]
- Lone, M.I.; Nazam, N.; Hussain, A.; Singh, S.K.; Dar, A.H.; Najar, R.A.; Al-Qahtani, M.H.; Ahmad, W. Genotoxicity and immunotoxic effects of 1,2-dichloroethane in Wistar rats. J. Environ. Sci. Health C. Environ. Carcinog. Ecotoxicol. Rev. 2016, 34, 169–186. [Google Scholar] [CrossRef] [PubMed]
- Darzynkiewicz, S.; Bruno, G.; Del Bino, W.; Gorczyca, W.; Hotz, M.A.; Lassota, P.; Traganos, F. Features of Apoptotic Cells Measured by Flow Cytometry. Cytometry 1992, 13, 795–808. [Google Scholar] [CrossRef] [PubMed]
- Majeed, R.; Hussain, A.; Sangwan, P.L.; Chinthakindi, P.K.; Khan, I.; Sharma, P.R.; Koul, S.; Saxena, A.K.; Hamid, A. PI3K target based novel cyano derivative of betulinic acid induces its signalling inhibition by down-regulation of pGSK3b and cyclin D1 and potentially checks Cancer cell proliferation. Mol. Carcinog. 2015, 55, 964–976. [Google Scholar] [CrossRef]
- Pharmakon. Micronucleus Test with Dimethoate, CL 12, 880 (Lot #611A). Unpublished Study Performed for the Dimethoate Task Force; Pharmakon Research International, Inc.: Waverly, PA, USA, 1985; EPA Accession No. 257603. [Google Scholar]
- Bakheet, S.A.; Attia, S.M.; AL-Rasheed, N.M.; Al-Harbi, M.M.; Ashour, A.E.; Korashy, H.M.; Abd-Allah, A.R.; Saquib, Q.; Alkhedhairy, A.A.; Musarrat, J. Salubrious effects of dexrazoxane against teniposide-induced DNA damage and programmed cell death in murine marrow cells. Mutagen 2011, 26, 533–543. [Google Scholar] [CrossRef]
- Hartmann, A.; Schumacher, M.; Plappert-Helbig, U.; Lowe, P.J.; Suter, W.; Mueller, L. Use of the alkaline in vivo Comet assay for mechanistic genotoxicity investigations. Mutagen 2003, 19, 51–59. [Google Scholar] [CrossRef]
- Nabeel, M.; Abderrahman, S.; Papini, A. Cytogenetic effect of Arum maculatum extract on the bone marrow cells of mice. Caryologia 2008, 61, 383–387. [Google Scholar] [CrossRef]
- Nazam, N.; Lone, M.I.; Shaikh, S.; Ahmad, W. Assessment of genotoxic potential of an insecticide Dichlorvos using cytogenetic assays. Interdisc. Toxicol. 2013, 6, 101–106. [Google Scholar] [CrossRef] [PubMed]
- Krishna, G.; Hayashi, M. In vivo rodent micronucleus assay: Protocol, conduct and data interpretation. Mutat. Res. 2000, 455, 155–166. [Google Scholar] [CrossRef]
- OECD. Guideline for the Testing of Chemicals Mammalian Erythrocyte Micronucleus Test; DRAFT TG 474; OECD: Paris, France, 2013. [Google Scholar]
- Guerci, A.; Zúniga, L.; Marcos, R. Construction and validation of a dose response curve using the comet assay to determine human radio sensitivity to ionizing radiation. J. Toxicol. Environ. Health Part A 2011, 74, 1087–1093. [Google Scholar] [CrossRef] [PubMed]
- Tice, R.R.; Agurell, E.; Anderson, D. Burlinson, B.; Hartmann, A.; Kobayashi, H.; Miyamae, Y.; Rojas, E.; Ryu, J.C.; Sasaki, Y.F. The single cell gel/comet assay: Guidelines for in vitro and in vivo genetic toxicology testing. Environ. Mol. Mutagen. 2000, 35, 206–221. [Google Scholar] [CrossRef]
- Olive, P.L.; Banath, J.P. The comet assay: A method to measure DNA damage in individual cells. Nat. Protoc. 2006, 1, 23–29. [Google Scholar] [CrossRef]
- Jagetia, A.; Jagetia, G.C.; Jha, S. Naringin, a grapefruit flavanone, protects V79 cells against the bleomycin-induced genotoxicity and decline in survival. J. Appl. Toxicol. 2007, 27, 122–132. [Google Scholar] [CrossRef]
- Schipler, A.; Iliakis, G. DNA double-stranded break complexity levels and their possible contributions to the probability for error-prone processing and repair pathway choice. Nucl. Acids Res. 2013, 41, 7589–7605. [Google Scholar] [CrossRef]
- Li, Y.; Luan, Y.; Qi, X.; Li, M.; Gong, L.; Xue, X.; Wu, X.; Wu, Y.; Chen, M.; Xing, G.; et al. Emodin triggers DNA double-strand breaks by stabilizing topoisomerase II-DNA cleavage complexes and by inhibiting ATP hydrolysis of topoisomerase II. Toxicol. Sci. 2010, 118, 435–443. [Google Scholar] [CrossRef]
- Nazam, N.; Lone, M.I.; Sharma, M.; Khan, A. Biochemical and cytoarchitechtural evaluation of dimethoate intoxication in rat liver and kidney: An in vivo study. IAJPR 2015, 5, 1127–1137. [Google Scholar]
- Banu, S.B.; Danadevi, K.; Rahman, M.F.; Ahuja, Y.R.; Kaiser, J. Genotoxic effect of monocrotophos to sentinel species using comet assay. Food Chem. Toxicol. 2001, 39, 361–366. [Google Scholar] [CrossRef]
- Afford, S.; Randhawa, S. Apoptosis. Mol. Pathol. 2000, 53, 55–63. [Google Scholar] [CrossRef] [PubMed]
- Shaikh, S.; Khan, M.; Biswas, D.; Hameed, N.; Shakil, S. Fetzima (levomilnacipran), a drug for major depressive disorder as a dual inhibitor for human serotonin transporters and beta-site amyloid precursor protein cleaving enzyme-1. CNS Neurol. Disord. Drug Targets 2014, 13, 1427–1431. [Google Scholar]
- Shaikh, S.; Zainab, T.; Rizvi, S.M.D.; Shakil, S. A neuroinformatics study to compare inhibition efficiency of three natural ligands (Fawcettimine, Cernuine and Lycodine) against human brain acetylcholinesterase. Netw. Comput. Neural Syst. 2015, 26, 25–34. [Google Scholar] [CrossRef] [PubMed]
- Verma, A.; Rizvi, S.M.D.; Shaikh, S.; Ansari, M.A.; Shakil, S.; Ghazal, F.; Siddiqui, M.H.; Haneef, M.; Rehman, A. Compounds isolated from Ageratum houstonianum inhibit the activity of matrix metalloproteinases (MMP-2 and MMP-9): An oncoinformatics study. Pharmacogn Mag. 2014, 10, 18–26. [Google Scholar]
- Rizvi, S.M.D.; Shakil, S.; Zeeshan, M.; Khan, M.S.; Shaikh, S.; Biswas, D.; Ahmad, A.; Kamal, M.A. An enzoinformatics study targeting polo-like kinases-1 enzyme: Comparative assessment of anticancer potential of compounds isolated from leaves of Ageratum houstonianum. Pharmacogn Mag. 2014, 10, 14–21. [Google Scholar]
- Yam, C.H.; Fung, T.K.; Poon, R.Y. Cyclin A in cell cycle control and cancer. Cell. Mol. Life Sci. 2002, 59, 1317–1326. [Google Scholar] [CrossRef]
- Lee-MacAry, A.E.; Ross, E.L.; Davies, D.; Laylor, R.; Honeychurch, J.; Glennie, M.J.; Snary, D.; Wilkinson, R.W. Development of a novel flow-cytometric cell-mediated cytotoxicity assay using the fluorophores PKH-26 and TO-PRO-3 iodide. J. Immunol. Methods. 2001, 252, 83–92. [Google Scholar] [CrossRef]
- Wachtel, M.; Schafer, B.W. Targets for cancer therapy in childhood sarcomas. Cancer Treat. Rev. 2010, 36, 318–327. [Google Scholar] [CrossRef]
- Rieder, S.A.; Chauhan, A.; Singh, U.; Nagarkatti, M.; Nagarkatti, P. Cannabinoid induced apoptosis in immune cells as a pathway to immune suppression. Immunobiology 2010, 215, 598–605. [Google Scholar] [CrossRef]
- Munson, A.E.; Sanders, V.M.; Douglas, K.A.; Sain, L.E.; Kauffmann, B.M.; White, L.L., Jr. In vivo assessment of immunotoxicity. Environ. Health Perspect. 1982, 43, 41–52. [Google Scholar] [CrossRef]
- Exline, M.C.; Crouser, E.D. Mitochondrial mechanisms of sepsis induced organ failure. Front. Biosci. 2008, 13, 5030–5041. [Google Scholar] [PubMed]
- Estaquier, J.; Vallette, F.; Vayssiere, J.L.; Mignotte, B. The mitochondrial pathways of apoptosis. Adv. Exp. Med. Biol. 2012, 942, 157–183. [Google Scholar] [PubMed]
- Faddan, N.H.A.; Sayed, D.; Sharkawy, N.A. Apoptosis and mitochondrial membrane potential changes of T lymphocytes from children with Down’s syndrome. Egypt. J. Pediatr. Allergy Immunol. 2010, 8, 35–40. [Google Scholar]
- Moore, P.D.; Patlolla, A.K.; Tchounwou, P. Cytogenetic evaluation of malathion-induced toxicity in Sprague-Dawley rats. Mutat. Res. 2011, 725, 78–82. [Google Scholar] [CrossRef][Green Version]
- Carlson, K.; Ehrich, M. Organophosphorus compound-induced modification of SH-SY5Y human neuroblastoma mitochondrial transmembrane potential. Toxicol. Appl. Pharmacol. 1999, 160, 33–42. [Google Scholar] [CrossRef]
- Gamal-Eldeen, A.M.; Abo-Zeid, M.A.M.; Ahmed, E.F. Anti-genotoxic effect of the Sargassum dentifolium extracts: Prevention of chromosomal aberrations, micronuclei, and DNA fragmentation. Exp. Toxicol. Pathol. 2013, 65, 27–34. [Google Scholar] [CrossRef]
- Lone, M.I.; Nabi, A.; Dar, N.J.; Hussain, A.; Nazam, N.; Hamid, A.; Ahmad, W. Toxicogenetic evaluation of dichlorophene in peripheral blood and in the cells of the immune system using molecular and flow cytometric approaches. Chemosphere 2017, 167, 520–529. [Google Scholar] [CrossRef]
- Alavanja, M.C.R.; Bonner, M.R. Pesticides and human cancers. Cancer Investig. 2005, 23, 700–711. [Google Scholar] [CrossRef]
- Webster, L.R.; McKenzie, G.H.; Moriarty, H.T. Organophosphate-based pesticides and genetic damage implicated in bladder cancer. Cancer Genet. Cytogenet. 2002, 133, 112–117. [Google Scholar] [CrossRef]
- Lerro, C.C.; Koutros, S.; Andreotti, G.; Friesen, M.C.; Alavanja, M.C.; Blair, A.; Hoppin, J.A.; Sandler, D.P.; Lubin, J.H.; Ma, X.; et al. Organophosphate insecticide use and cancer incidence among spouses of pesticide applicators in the Agricultural Health Study. Occup. Environ. Med. 2015, 72, 736–744. [Google Scholar] [CrossRef]
- Bonassi, S.; Hagmar, L.; Stromberg, U.; Montagud, A.H.; Tinnerberg, H.; Forni, A.; Heikkilä, P.; Wanders, S.; Wilhardt, P.; Hansteen, I.L.; et al. Chromosomal aberrations in lymphocytes predict human cancer independently of exposure to carcinogens. Cancer Res. 2000, 60, 1619–1625. [Google Scholar] [PubMed]
| Group and Dose | Exposure (h) | MNPCE (Mean% ± SD) | P/N |
|---|---|---|---|
| Normal Control (Distilled water: 2 ml/kgbw) | 24 | 0.27 ± 0.04 | 0.840 |
| 48 | 0.29 ± 0.07 | 0.844 | |
| 72 | 0.21 ± 0.01 | 0.847 | |
| Positive control (Cyclophosphamide: 40 mg/kgbw) | 24 | 10.6 ± 0.81 *** | 0.604 * |
| 48 | 8.2 ± 0.66 *** | 0.529 ** | |
| 72 | 7.1 ± 0.43 *** | 0.581 ** | |
| Low Dose (DM: 20 mg/kgbw) | 24 | 4.4 ± 0.51 ** | 0.740 * |
| 48 | 4.0 ± 0.44 * | 0.736 * | |
| 72 | 3.6 ± 0.50 * | 0.731 * | |
| Medium Dose (DM: 40 mg/kgbw) | 24 | 5.2 ± 0.58 ** | 0.728 * |
| 48 | 4.8 ± 0.86 ** | 0.715 * | |
| 72 | 4.1 ± 0.73 * | 0.711 * | |
| High Dose (DM: 60 mg/kgbw) | 24 | 5.6 ± 0.70 ** | 0.725 * |
| 48 | 4.9 ± 0.74 ** | 0.721 * | |
| 72 | 3.8 ± 0.80 * | 0.718 * |
| Duration (h) | Group | Structural Aberrations | Total Aberrations | MI | ||||||
|---|---|---|---|---|---|---|---|---|---|---|
| Brk | Del | Frag | Gp | Dcn | Ring | Assoc | (Mean ± SD) | (Mean ± SD) | ||
| 24 | Normal Control | 1 | 0 | 2 | 0 | 0 | 2 | 0 | 0.83 ± 0.40 | 2.65 ± 0.09 |
| Positive Control | 14 | 23 | 26 | 20 | 25 | 8 | 9 | 17.50 ± 3.33 ***,a | 1.52 ± 0.05 **,a | |
| D I | 2 | 4 | 6 | 8 | 8 | 2 | 4 | 5.66 ± 1.03 **,a | 2.19 ± 0.21 *,a | |
| D II | 4 | 4 | 3 | 8 | 12 | 6 | 6 | 5.83 ± 1.69 **,a | 2.16 ± 0.16 *,a | |
| D III | 6 | 6 | 8 | 7 | 10 | 4 | 4 | 7.50 ± 1.15 **,a,*,b | 1.92 ± 0.61 *,a | |
| 48 | Normal Control | 0 | 1 | 1 | 0 | 0 | 0 | 0 | 0.33 ± 0.21 | 2.95 ± 1.06 |
| Positive Control | 12 | 18 | 21 | 16 | 18 | 6 | 7 | 13.66 ± 2.56 ***,a | 1.56 ± 0.05 **,a | |
| D I | 9 | 5 | 12 | 6 | 3 | 6 | 5 | 5.33 ± 1.43 **,a | 2.04 ± 0.15 *,a | |
| D II | 3 | 4 | 16 | 7 | 8 | 5 | 6 | 5.16 ± 1.74 **,a | 1.98 ± 0.08 *,a | |
| D III | 7 | 5 | 14 | 8 | 7 | 9 | 7 | 6.83 ± 1.90 **,a | 1.97 ± 0.12 *,a | |
| 72 | Normal Control | 0 | 0 | 1 | 0 | 0 | 0 | 0 | 0.16 ± 0.14 | 2.71 ± 0.08 |
| Positive Control | 9 | 15 | 19 | 13 | 14 | 3 | 4 | 10.66 ± 2.61 ***,a | 1.63 ± 0.03 **,a | |
| D I | 2 | 4 | 4 | 5 | 2 | 1 | 0 | 2.17 ± 0.83 *,a | 2.07 ± 0.10 *,a | |
| D II | 5 | 2 | 5 | 7 | 2 | 1 | 1 | 2.67 ± 0.75 *,a | 2.05 ± 0.14 *,a | |
| D III | 8 | 3 | 3 | 6 | 2 | 2 | 1 | 3.16 ± 0.71 *,a | 1.95 ± 0.04 *,a | |
| Groups | Time (h) | Olive Tail Moment | Tail Length (µm) |
|---|---|---|---|
| Control | 24 | 0.81 ± 0.16 | 2.69 ± 0.58 |
| 48 | 0.65 ± 0.09 | 2.39 ± 0.52 | |
| 72 | 0.56 ± 0.08 | 2.35 ± 0.49 | |
| Positive | 24 | 12.52 ± 0.81 ***,a | 51.01 ± 3.71 ***,a |
| 48 | 11.28 ± 0.84 ***,a | 40.91 ± 2.86 ***,a | |
| 72 | 8.23 ± 0.73 ***,a | 38.51 ± 1.05 ***,a | |
| DM I | 24 | 5.65 ± 0.33 ***,a | 22.44 ± 2.07 ***,a |
| 48 | 4.01 ± 0.48 ***,a | 19.26 ± 1.00 *,a | |
| 72 | 2.71 ± 0.31 *,a | 16.16 ± 1.35 *,a | |
| DM II | 24 | 6.19 ± 0.52 ***,a,*,b | 24.37 ± 1.66 ***,a,b |
| 48 | 5.35 ± 0.48 ***,a,*,b | 25.07 ± 1.87 ***,a,b | |
| 72 | 3.13 ± 0.28 *,a | 21.12 ± 1.45 ***,a | |
| DM III | 24 | 6.59 ± 0.67 ***,a,b,c | 30.09 ± 2.86 ***,a,b |
| 48 | 6.46 ± 0.64 ***,a,b,c | 27.63 ± 3.12 ***,a,c,**,b | |
| 72 | 4.84 ± 0.41 **,a | 20.37 ± 1.59 *,a,c |
| Groups and Dose | Duration | Sub-G1 | G1 | S | G2/M |
|---|---|---|---|---|---|
| Control | 24 h | 8.46 ± 0.71 | 79.93 ± 2.23 | 7.33 ± 0.89 | 4.16 ± 0.46 |
| 48 h | 9.36 ± 0.82 | 85.81 ± 3.21 | 3.2 ± 0.03 | 2.1 ± 0.36 | |
| 72 h | 5.53 ± 0.72 | 90.14 ± 3.89 | 2.86 ± 0.02 | 1.6 ± 0.04 | |
| Positive | 24 h | 91.3 ± 4.12 ***,a | 6.06 ± 1.26 | 0.2 ± 0.01 | 2.53 ± 0.06 |
| 48 h | 76.3 ± 4.16 ***,a | 21.33 ± 2.41 | 0.06 ± 0.01 | 1.3 ± 0.2 | |
| 72 h | 98.4 ± 6.01 ***,a | 0.87 ± 0.03 | 0.33 ± 0.11 | 0.4 ± 0.02 | |
| DM I | 24 h | 79.2 ± 2.32 ***,a | 15.66 ± 1.28 **,a | 2.2 ± 0.03 | 2.8 ± 0.23 |
| 48 h | 21.13 ± 1.73 *,a | 77.4 ± 3.42 | 0.53 ± 0.22 | 1.1 ± 0.21 | |
| 72 h | 18.9 ± 2.62 *,a | 81.06 ± 4.29 | 0.33 ± 0.02 | 0.43 ± 0.16 | |
| DM II | 24 h | 75.5 ± 3.27 ***,a | 19.1 ± 1.21 **,a | 1.6 ± 0.11 | 2.8 ± 0.05 |
| 48 h | 37.13 ± 2.12 **,a | 57.6 ± 2.02 *,a | 2.4 ± 0.54 | 2.8 ± 0.26 | |
| 72 h | 26.3 ± 2.63 *,a,b | 72.16 ± 4.06 | 0.47 ± 0.14 | 0.8 ± 0.03 | |
| DM III | 24 h | 83.53 ± 5.37 ***,a | 15.2 ± 0.38 ***,a | 0.33 ± 0.11 **,a | 0.83 ± 0.13 **,a |
| 48 h | 39.2 ± 2.38 *,a | 54.83 ± 2.58 *,a | 6.1 ± 0.38 *,a | 0.4 ± 0.11 **,a | |
| 72 h | 37.8 ± 3.01 *,a,b,c | 55.63 ± 1.04 *,a | 5.2 ± 0.25 *,a | 2.3 ± 0.05 |
| Compound | Target | Binding Energy (kcal/mol) | Interacting Amino Acid Residues |
|---|---|---|---|
| Dimethoate | −5.89 | His233, Asn237, Asp240, Pro309, Thr310, Val311, Leu341, Tyr347, Leu348, Tyr350, Pro352, Ile355 | |
| Cyclin A2 | |||
| Cyclophosphamide | −5.82 | His233, Val236, Asn287, Pro309, Thr310, Val311, Ser340, Leu341, Tyr347, Tyr350, Pro352, Ile355 |
© 2020 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Nazam, N.; Lone, M.I.; Hamid, A.; Qadah, T.; Banjar, A.; Alam, Q.; Saeed, M.; Ahmad, W. Dimethoate Induces DNA Damage and Mitochondrial Dysfunction Triggering Apoptosis in Rat Bone-Marrow and Peripheral Blood Cells. Toxics 2020, 8, 80. https://doi.org/10.3390/toxics8040080
Nazam N, Lone MI, Hamid A, Qadah T, Banjar A, Alam Q, Saeed M, Ahmad W. Dimethoate Induces DNA Damage and Mitochondrial Dysfunction Triggering Apoptosis in Rat Bone-Marrow and Peripheral Blood Cells. Toxics. 2020; 8(4):80. https://doi.org/10.3390/toxics8040080
Chicago/Turabian StyleNazam, Nazia, Mohammad Iqbal Lone, Abid Hamid, Talal Qadah, Alaa Banjar, Qamre Alam, Mohd Saeed, and Waseem Ahmad. 2020. "Dimethoate Induces DNA Damage and Mitochondrial Dysfunction Triggering Apoptosis in Rat Bone-Marrow and Peripheral Blood Cells" Toxics 8, no. 4: 80. https://doi.org/10.3390/toxics8040080
APA StyleNazam, N., Lone, M. I., Hamid, A., Qadah, T., Banjar, A., Alam, Q., Saeed, M., & Ahmad, W. (2020). Dimethoate Induces DNA Damage and Mitochondrial Dysfunction Triggering Apoptosis in Rat Bone-Marrow and Peripheral Blood Cells. Toxics, 8(4), 80. https://doi.org/10.3390/toxics8040080







