Sustained Effects on Lung Function in Community Members Following Exposure to Hazardous PM2.5 Levels from Wildfire Smoke
Abstract
1. Introduction
2. Methods
2.1. Study Design
2.2. Study Population
2.3. Particle Exposures
2.4. Study Procedures
2.4.1. Surveys and Participant Screening
2.4.2. Pulmonary Function Tests
2.5. Data Analysis
3. Results
3.1. Cohorts
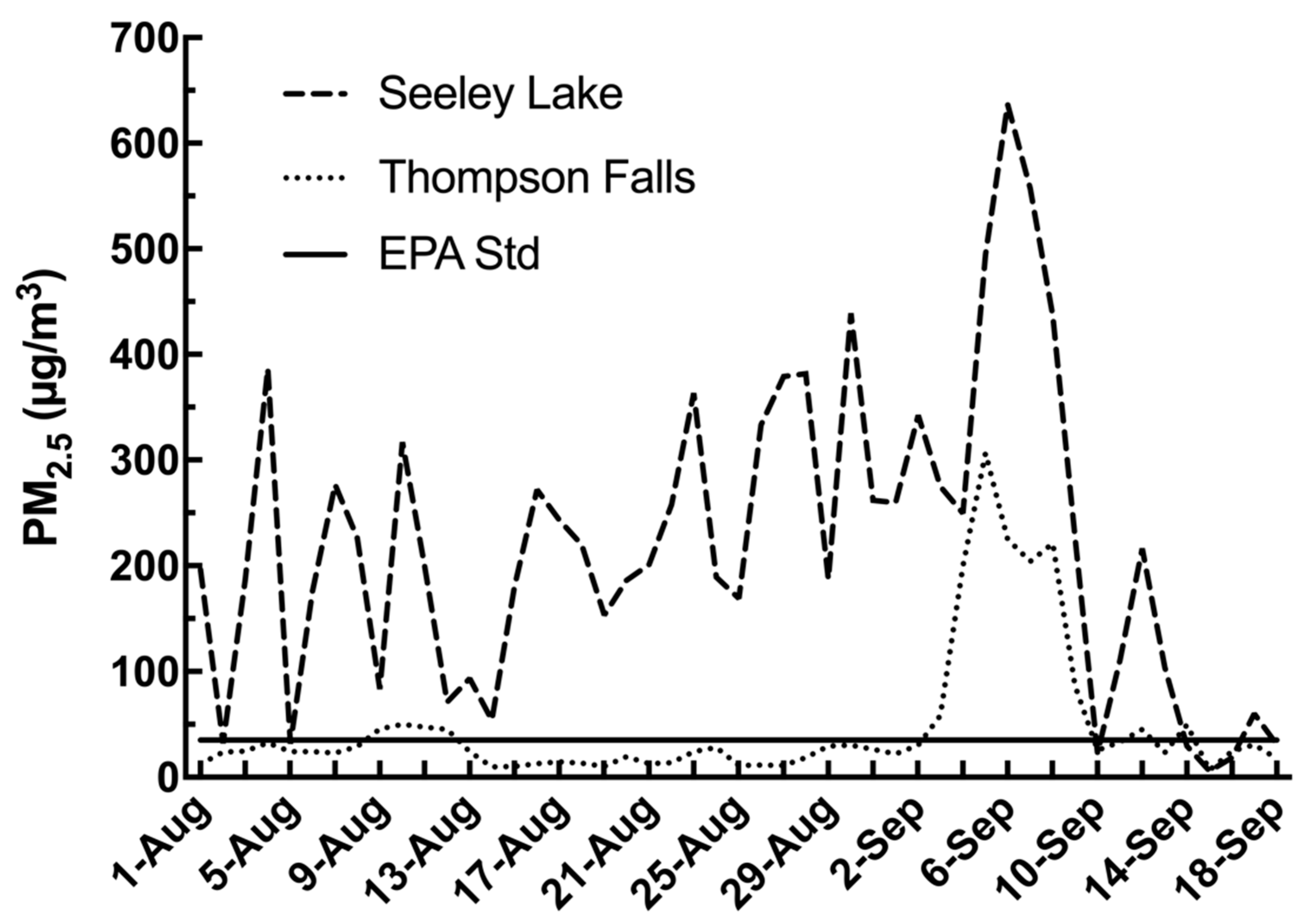
3.2. Exposures
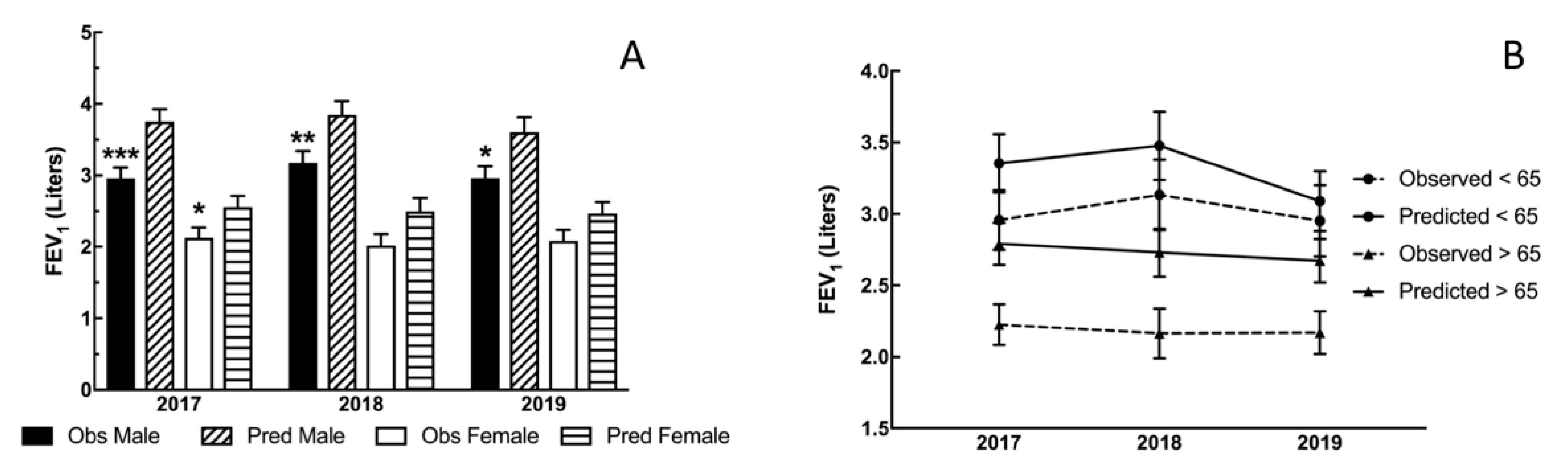
3.3. Lung Function Assessments
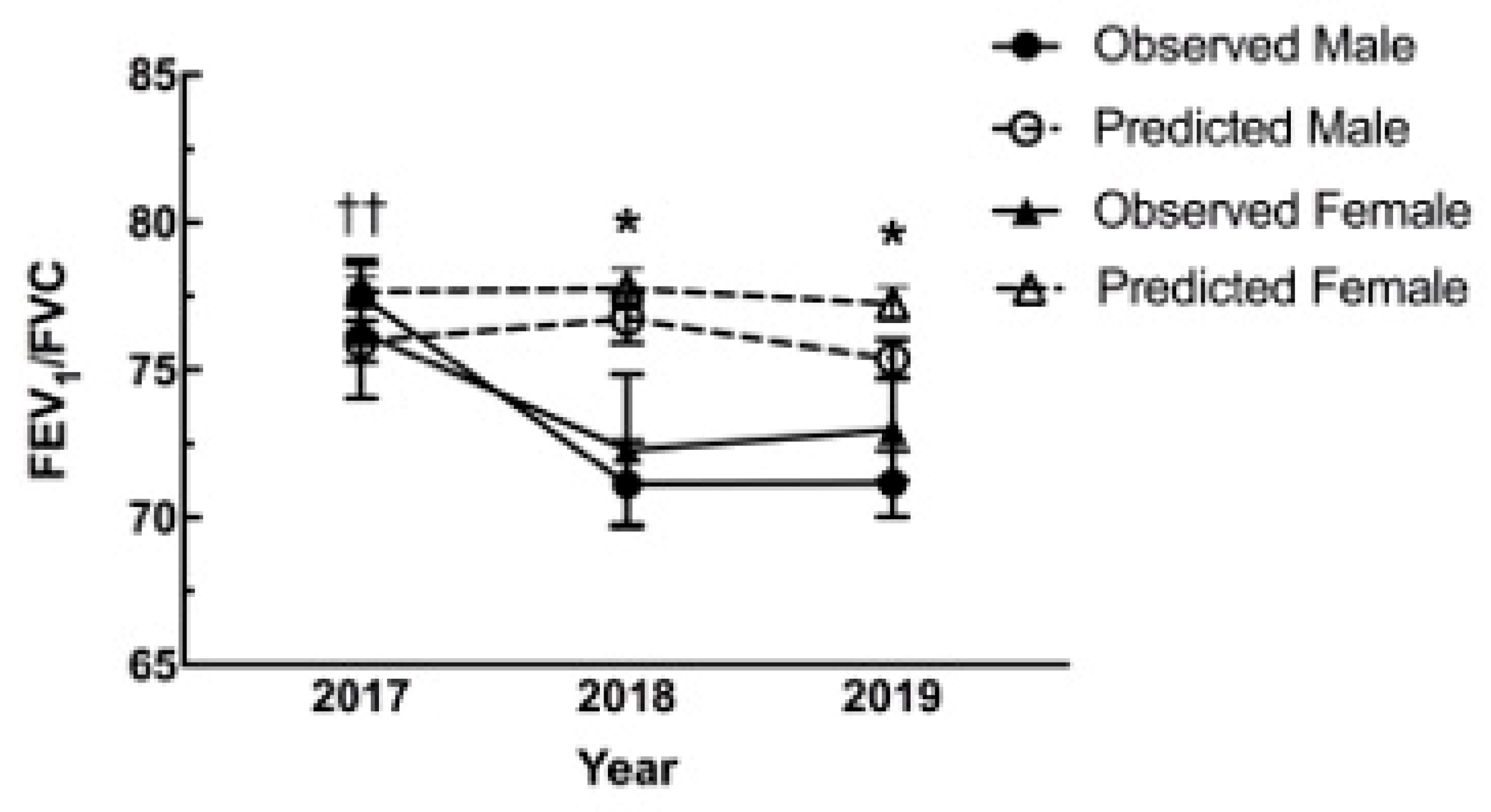
3.3.1. FEV1/FVC Decrease
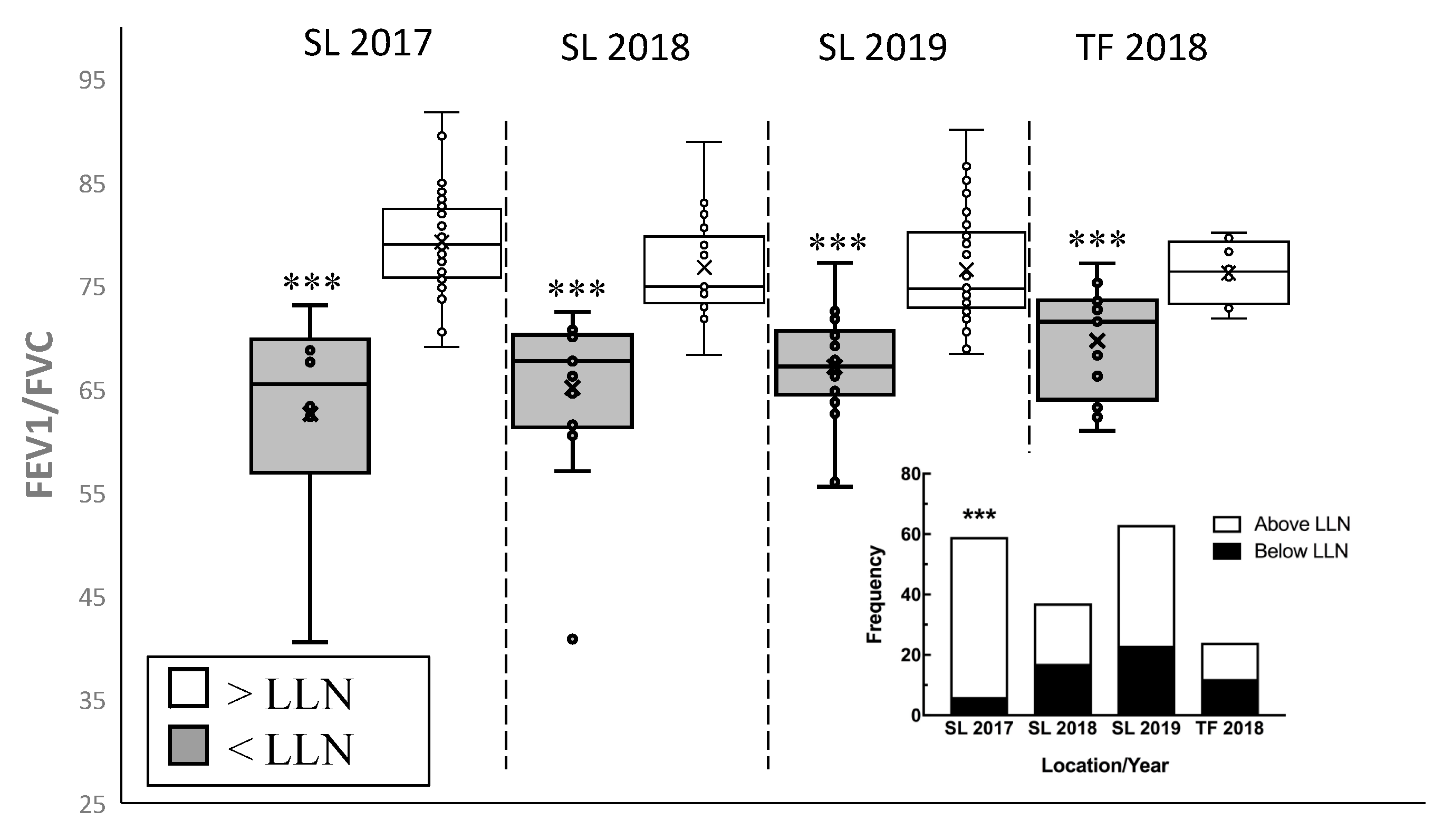
3.3.2. Lower Limit of Normal (LLN)
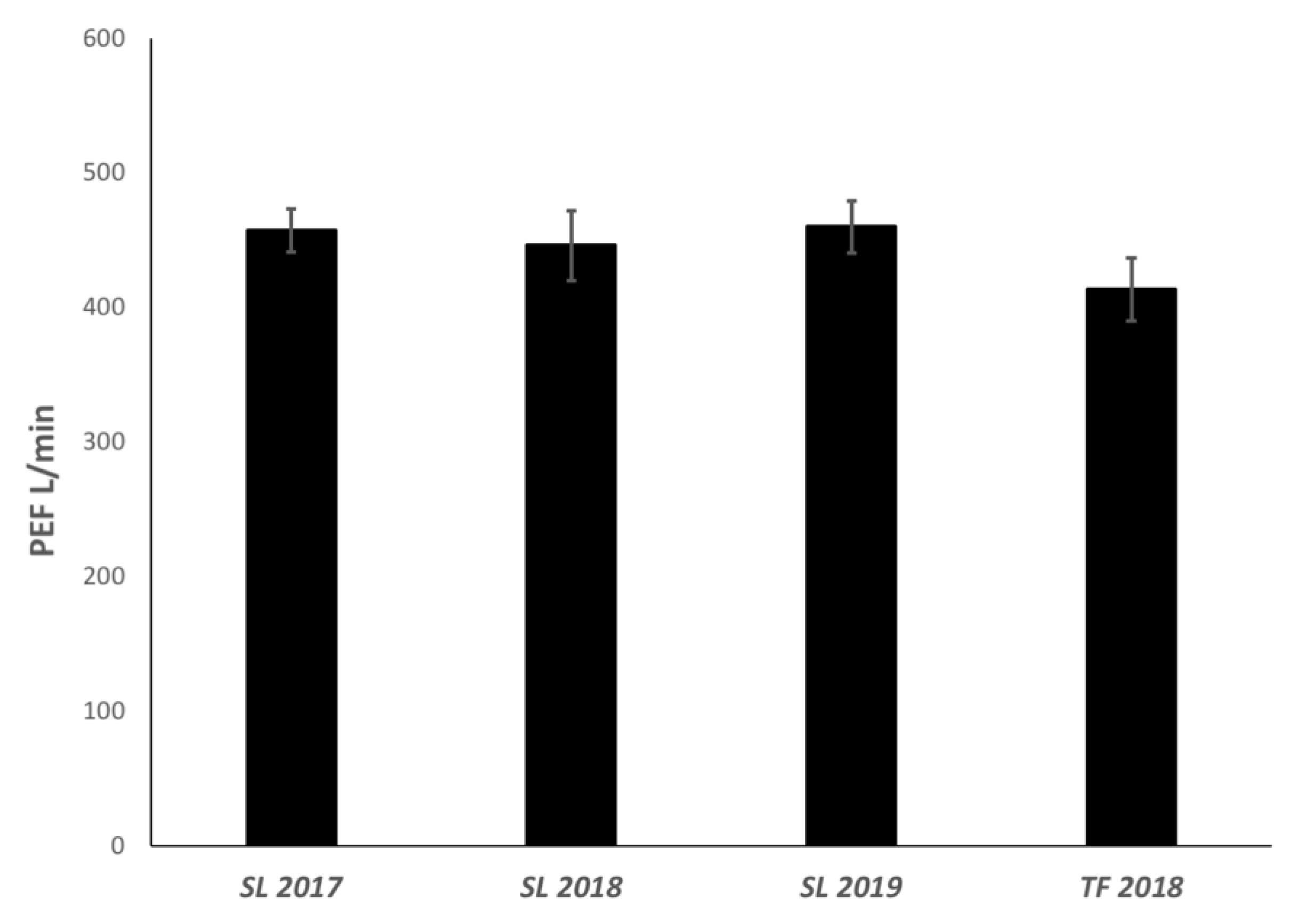
3.3.3. Peak Expiratory Flow
3.3.4. Annual FEV1 Decline
3.4. Covariates
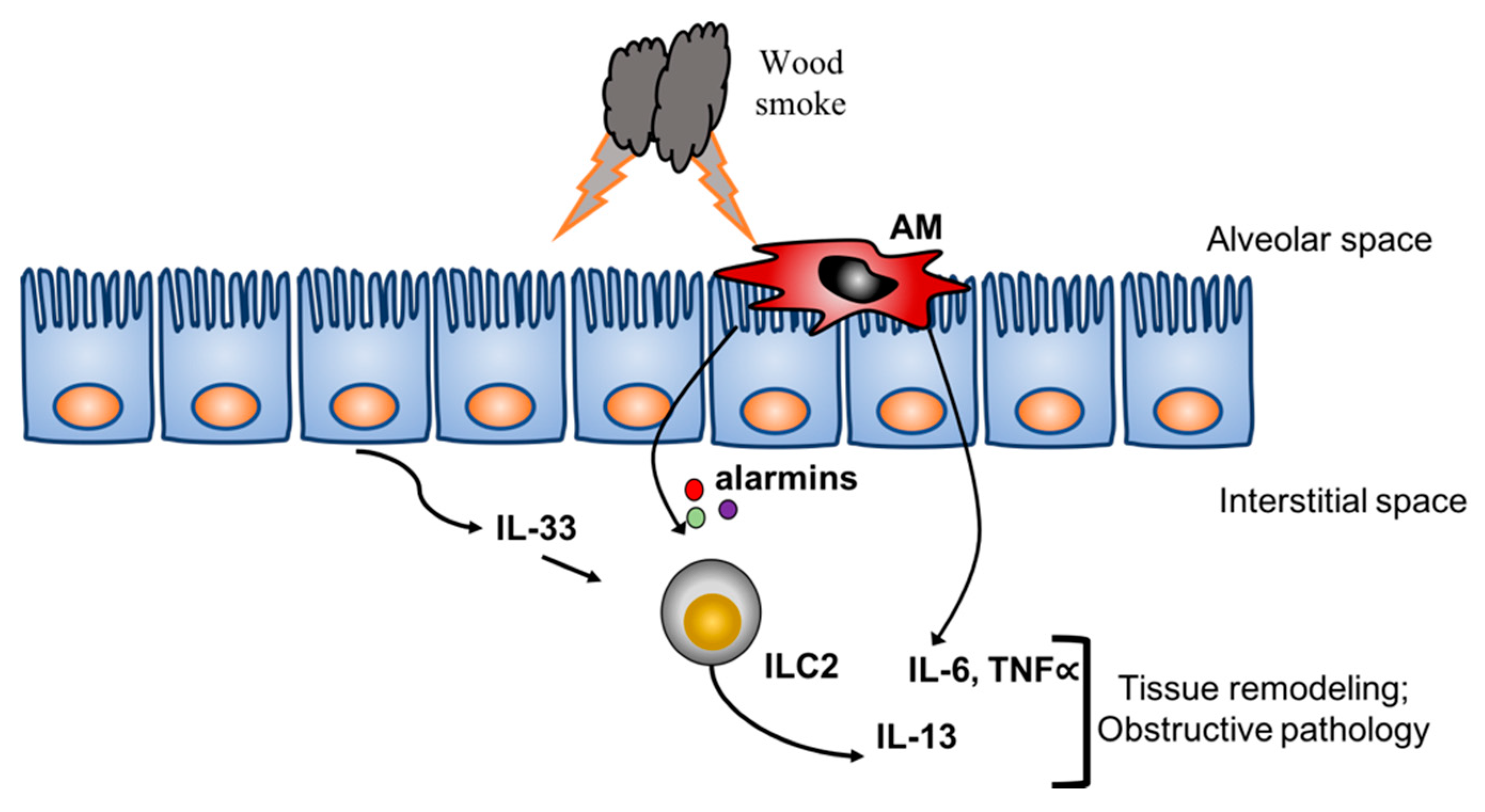
4. Discussion
5. Conclusions
Author Contributions
Funding
Acknowledgments
Conflicts of Interest
References
- Bowman, D.M.J.S.; Balch, J.K.; Artaxo, P.; Bond, W.J.; Carlson, J.M.; Cochrane, M.A.; D’Antonio, C.M.; DeFries, R.S.; Doyle, J.C.; Harrison, S.P.; et al. Fire in the Earth System. Science 2009, 324, 481–484. [Google Scholar] [CrossRef]
- Flannigan, M.D.; Krawchuk, M.A.; De Groot, W.J.; Wotton, B.M.; Gowman, L.M. Implications of changing climate for global wildland fire. Int. J. Wildland Fire 2009, 18, 483–507. [Google Scholar] [CrossRef]
- Black, C.; Tesfaigzi, Y.; Bassein, J.A.; Miller, L.A. Wildfire smoke exposure and human health: Significant gaps in research for a growing public health issue. Environ. Toxicol. Pharmacol. 2017, 55, 186–195. [Google Scholar] [CrossRef] [PubMed]
- Reid, C.E.; Jerrett, M.; Tager, I.B.; Petersen, M.L.; Mann, J.K.; Balmes, J.R. Differential respiratory health effects from the 2008 northern California wildfires: A spatiotemporal approach. Environ. Res. 2016, 150, 227–235. [Google Scholar] [CrossRef]
- Keeley, J.E.; Syphard, A.D. Climate Change and Future Fire Regimes: Examples from California. Geosciences 2016, 6, 37. [Google Scholar] [CrossRef]
- Spracklen, D.V.; Mickley, L.J.; Logan, J.A.; Hudman, R.C.; Yevich, R.; Flannigan, M.D.; Westerling, A.L. Impacts of climate change from 2000 to 2050 on wildfire activity and carbonaceous aerosol concentrations in the western United States. J. Geophys. Res. Space Phys. 2009, 114. [Google Scholar] [CrossRef]
- O’Dell, K.; Ford, B.; Fischer, E.V.; Pierce, J.R. Contribution of Wildland-Fire Smoke to US PM2.5 and Its Influence on Recent Trends. Environ. Sci. Technol. 2019, 53, 1797–1804. [Google Scholar] [CrossRef]
- Holden, Z.A.; Swanson, A.; Luce, C.H.; Jolly, W.M.; Maneta, M.; Oyler, J.W.; Warren, D.A.; Parsons, R.; Affleck, D. Decreasing fire season precipitation increased recent western US forest wildfire activity. Proc. Natl. Acad. Sci. USA 2018, 115, E8349–E8357. [Google Scholar] [CrossRef]
- Westerling, A.L.; Hidalgo, H.G.; Cayan, D.R.; Swetnam, T.W. Warming and Earlier Spring Increase Western U.S. Forest Wildfire Activity. Science 2006, 313, 940–943. [Google Scholar] [CrossRef]
- Westerling, A.L.; Turner, M.; Smithwick, E.A.H.; Romme, W.H.; Ryan, M.G. Continued warming could transform Greater Yellowstone fire regimes by mid-21st century. Proc. Natl. Acad. Sci. USA 2011, 108, 13165–13170. [Google Scholar] [CrossRef]
- Alman, B.L.; Pfister, G.; Hao, H.; Stowell, J.; Hu, X.; Liu, Y.; Strickland, M.J. The association of wildfire smoke with respiratory and cardiovascular emergency department visits in Colorado in 2012: A case crossover study. Environ. Health 2016, 15, 64. [Google Scholar] [CrossRef] [PubMed]
- Cascio, W.E. Wildland fire smoke and human health. Sci. Total. Environ. 2018, 624, 586–595. [Google Scholar] [CrossRef] [PubMed]
- Hutchinson, J.A.; Vargo, J.; Milet, M.; French, N.H.F.; Billmire, M.; Johnson, J.; Hoshiko, S. The San Diego 2007 wildfires and Medi-Cal emergency department presentations, inpatient hospitalizations, and outpatient visits: An observational study of smoke exposure periods and a bidirectional case-crossover analysis. PLoS Med. 2018, 15, e1002601. [Google Scholar] [CrossRef] [PubMed]
- Liu, J.C.; Pereira, G.; Uhl, S.A.; Bravo, M.; Bell, M. A systematic review of the physical health impacts from non-occupational exposure to wildfire smoke. Environ. Res. 2015, 136, 120–132. [Google Scholar] [CrossRef]
- Haikerwal, A.; Akram, M.; Sim, M.R.; Meyer, M.; Abramson, M.J.; Dennekamp, M. Fine particulate matter (PM 2.5) exposure during a prolonged wildfire period and emergency department visits for asthma. Respirology 2015, 21, 88–94. [Google Scholar] [CrossRef]
- Hankinson, J.L.; Odencrantz, J.R.; Fedan, K.B. Spirometric Reference Values from a Sample of the General U.S. Population. Am. J. Respir. Crit. Care Med. 1999, 159, 179–187. [Google Scholar] [CrossRef]
- Quanjer, P.H.; Tammeling, G.J.; Cotes, J.E.; Pedersen, O.F.; Peslin, R.; Yernault, J.C. Lung volumes and forced ventilatory flows. Report Working Party Standardization of Lung Function Tests, European Community for Steel and Coal. Official Statement of the European Respiratory Society. Eur. Respir. J. Suppl. 1993, 16, 5–40. [Google Scholar] [CrossRef]
- CDCP. National Health and Nutrition Examination Survey (NHANES): Respiratory Health Spirometry Procedures Manual; CreateSpace Independent Publishing Platform: Scotts Valley, CA, USA, 2014. [Google Scholar]
- Hart, J.E.; Grady, S.T.; Laden, F.; Coull, B.A.; Koutrakis, P.; Schwartz, J.D.; Moy, M.L.; Garshick, E. Effects of Indoor and Ambient Black Carbon and PM2.5 on Pulmonary Function among Individuals with COPD. Environ. Health Perspect. 2018, 126, 127008. [Google Scholar] [CrossRef]
- Johannson, K.A.; Vittinghoff, E.; Morisset, J.; Wolters, P.J.; Noth, E.M.; Balmes, J.R.; Collard, H.R. Air Pollution Exposure Is Associated with Lower Lung Function, but Not Changes in Lung Function, in Patients with Idiopathic Pulmonary Fibrosis. Chest 2018, 154, 119–125. [Google Scholar] [CrossRef]
- Rohlman, D.; Dixon, H.M.; Kincl, L.D.; Larkin, A.; Evoy, R.; Barton, M.L.; Phillips, A.R.; Peterson, E.; Scaffidi, C.; Herbstman, J.B.; et al. Development of an environmental health tool linking chemical exposures, physical location and lung function. BMC Public Health 2019, 19, 854. [Google Scholar] [CrossRef]
- Quanjer, P.H. Standardized Lung-Function Testing. B Eur. Physiopath. Res. 1983, 19, 1–92. [Google Scholar]
- Sterk, P.J.; Fabbri, L.M.; Quanjer, P.H.; Cockcroft, D.W.; O’Byrne, P.M.; Anderson, S.D.; Juniper, E.; Malo, J.L. Airway responsiveness. Standardized challenge testing with pharmacological, physical and sensitizing stimuli in adults. Report Working Party Standardization of Lung Function Tests, European Community for Steel and Coal. Official Statement of the European Respiratory Society. Eur. Respir. J. Suppl. 1993, 16, 53–83. [Google Scholar] [PubMed]
- Swanney, M.P.; Ruppel, G.; Enright, P.L.; Pedersen, O.F.; Crapo, R.O.; Miller, M.; Jensen, R.L.; Falaschetti, E.; Schouten, J.P.; Hankinson, J.L.; et al. Using the lower limit of normal for the FEV1/FVC ratio reduces the misclassification of airway obstruction. Thorax 2008, 63, 1046–1051. [Google Scholar] [CrossRef] [PubMed]
- Brunekreef, B.; Smit, J.; De Jongste, J.; Neijens, H.; Gerritsen, J.; Postma, D.; Aalberse, R.; Koopman, L.; Kerkhof, M.; Wijga, A.; et al. The Prevention and Incidence of Asthma and Mite Allergy (PIAMA) birth cohort study: Design and first results. Pediatr. Allergy Immunol. 2002, 13, 55–60. [Google Scholar] [CrossRef] [PubMed]
- Zwozdziak, A.; Sówka, I.; Willak-Janc, E.; Kwiecińska, K.; Balińska-Miśkiewicz, W.; Zwozdziak, J. Influence of PM1 and PM2.5 on lung function parameters in healthy schoolchildren—A panel study. Environ. Sci. Pollut. Res. 2016, 23, 23892–23901. [Google Scholar] [CrossRef]
- Van Dijk, W.; Tan, W.; Li, P.; Guo, B.; Li, S.; Benedetti, A.; Bourbeau, J. Clinical Relevance of Fixed Ratio vs Lower Limit of Normal of FEV1/FVC in COPD: Patient-Reported Outcomes From the CanCOLD Cohort. Ann. Fam. Med. 2015, 13, 41–48. [Google Scholar] [CrossRef]
- Morgan, B.W.; Grigsby, M.R.; Siddharthan, T.; Chowdhury, M.; Rubinstein, A.; Gutierrez, L.; Irazola, V.; Miranda, J.J.; Bernabe-Ortiz, A.; Alam, D.; et al. Epidemiology and risk factors of asthma-chronic obstructive pulmonary disease overlap in low- and middle-income countries. J. Allergy Clin. Immunol. 2019, 143, 1598–1606. [Google Scholar] [CrossRef]
- Zeki, A.A.; Flayer, C.H.; Haczku, A. A burning need to redefine airways disease: Biomass smoke exposure identified as a unique risk factor for asthma–chronic obstructive pulmonary disease overlap in low- and middle-income countries. J. Allergy Clin. Immunol. 2019, 143, 1339–1341. [Google Scholar] [CrossRef]
- Flayer, C.H.; Larson, E.D.; Joseph, A.; Kao, S.; Qu, W.; Van Haren, A.; Royer, C.M.; Miller, L.A.; Capitanio, J.P.; Sielecki, T.; et al. Ozone-induced enhancement of airway hyperreactivity in rhesus macaques: Effects of antioxidant treatment. J. Allergy Clin. Immunol. 2020, 145, 312–323. [Google Scholar] [CrossRef]
- Yang, Q.; Ge, M.Q.; Kokalari, B.; Redai, I.G.; Wang, X.; Kemeny, D.M.; Bhandoola, A.; Haczku, A. Group 2 innate lymphoid cells mediate ozone-induced airway inflammation and hyperresponsiveness in mice. J. Allergy Clin. Immunol. 2015, 137, 571–578. [Google Scholar] [CrossRef]
- Sjöberg, L.C.; Nilsson, A.Z.; Lei, Y.; Gregory, J.A.; Adner, M.; Nilsson, G. Interleukin 33 exacerbates antigen driven airway hyperresponsiveness, inflammation and remodeling in a mouse model of asthma. Sci. Rep. 2017, 7, 4219. [Google Scholar] [CrossRef] [PubMed]
- Grubek-Jaworska, H.; Paplińska-Goryca, M.; Hermanowicz-Salamon, J.; Dąbrowska, M.; Grabczak, E.; Stepień, J.; Chazan, R.; Białek-Gosk, K.; Domagała-Kulawik, J. IL-6 and IL-13 in Induced Sputum of COPD and Asthma Patients: Correlation with Respiratory Tests. Respiration 2012, 84, 101–107. [Google Scholar] [CrossRef] [PubMed]
- Rincon, M.; Irvin, C.G. Role of IL-6 in Asthma and Other Inflammatory Pulmonary Diseases. Int. J. Biol. Sci. 2012, 8, 1281–1290. [Google Scholar] [CrossRef] [PubMed]
- Main, L.C.; Wolkow, A.P.; Tait, J.L.; Gatta, P.D.; Raines, J.; Snow, R.; Aisbett, B. Firefighterʼs Acute Inflammatory Response to Wildfire Suppression. J. Occup. Environ. Med. 2020, 62, 145–148. [Google Scholar] [CrossRef]
- Roscioli, E.; Hamon, R.; Lester, S.E.; Jersmann, H.P.A.; Reynolds, P.N.; Hodge, S. Airway epithelial cells exposed to wildfire smoke extract exhibit dysregulated autophagy and barrier dysfunction consistent with COPD. Respir. Res. 2018, 19, 234. [Google Scholar] [CrossRef]
- Fisk, W.J.; Chan, W.R. Health benefits and costs of filtration interventions that reduce indoor exposure to PM2.5 during wildfires. Indoor Air 2016, 27, 191–204. [Google Scholar] [CrossRef]
| Variable | Seeley Lake | Thompson Falls | ||
|---|---|---|---|---|
| 2017 | 2018 | 2019 | 2018 | |
| Participants | 95 | 42 | 62 | 24 |
| Age * (years) | 63 ± 1.5 | 63 ± 2.1 | 64 ± 1.5 | 59 ± 2.5 |
| Sex | ||||
| Male | 44 | 18 | 26 | 5 |
| Female | 51 | 24 | 36 | 19 |
| Race | ||||
| White | 93 | 40 | 60 | 24 |
| Asian | 1 | 1 | 1 | 0 |
| African American | 0 | 0 | 0 | 0 |
| Hispanic | 2 | 1 | 2 | 0 |
| Education | ||||
| Less than High School | 2 | 1 | 1 | 0 |
| High School Diploma or GED | 25 | 11 | 14 | 5 |
| Some College | 27 | 12 | 19 | 7 |
| College Degree | 41 | 16 | 26 | 12 |
| Income | ||||
| Less than $29,999 | 18 | 9 | 11 | 5 |
| $30,000–$74,999 | 52 | 22 | 28 | 15 |
| Greater than $75,000 | 18 | 11 | 18 | 3 |
| n | Clinically Decreased (%) | Average Decrease (mL) | ||
|---|---|---|---|---|
| 2017–2018 | Total | 37 | 19 (50%) | −0.231 ± 0.056 |
| Males | 18 | 8 (44%) | −0.289 ± 0.114 | |
| Females | 19 | 11 (55%) | −0.208 ± 0.060 | |
| 2018–2019 | Total | 30 | 17 (57%) | −0.123 ± 0.029 |
| Males | 14 | 7 (50%) | −0.172 ± 0.043 | |
| Females | 16 | 10 (63%) | −0.135 ± 0.025 | |
© 2020 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Orr, A.; A. L. Migliaccio, C.; Buford, M.; Ballou, S.; Migliaccio, C.T. Sustained Effects on Lung Function in Community Members Following Exposure to Hazardous PM2.5 Levels from Wildfire Smoke. Toxics 2020, 8, 53. https://doi.org/10.3390/toxics8030053
Orr A, A. L. Migliaccio C, Buford M, Ballou S, Migliaccio CT. Sustained Effects on Lung Function in Community Members Following Exposure to Hazardous PM2.5 Levels from Wildfire Smoke. Toxics. 2020; 8(3):53. https://doi.org/10.3390/toxics8030053
Chicago/Turabian StyleOrr, Ava, Cristi A. L. Migliaccio, Mary Buford, Sarah Ballou, and Christopher T. Migliaccio. 2020. "Sustained Effects on Lung Function in Community Members Following Exposure to Hazardous PM2.5 Levels from Wildfire Smoke" Toxics 8, no. 3: 53. https://doi.org/10.3390/toxics8030053
APA StyleOrr, A., A. L. Migliaccio, C., Buford, M., Ballou, S., & Migliaccio, C. T. (2020). Sustained Effects on Lung Function in Community Members Following Exposure to Hazardous PM2.5 Levels from Wildfire Smoke. Toxics, 8(3), 53. https://doi.org/10.3390/toxics8030053




