Potential of MRI in Radiotherapy Mediated by Small Conjugates and Nanosystems
Abstract
:1. Introduction
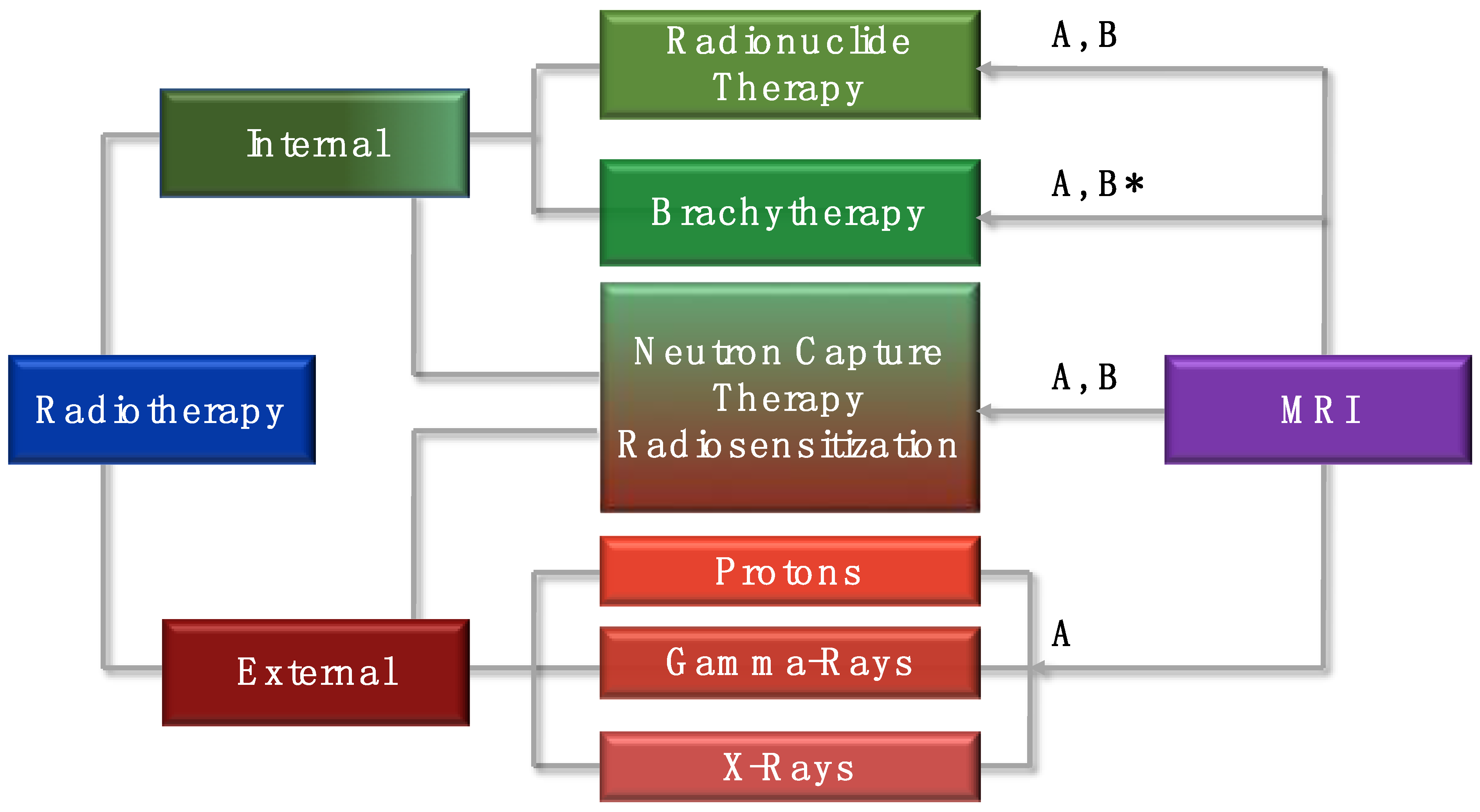
2. The Role of Magnetic Resonance Imaging (MRI) in External Radiation Therapy
2.1. Radiosensitization
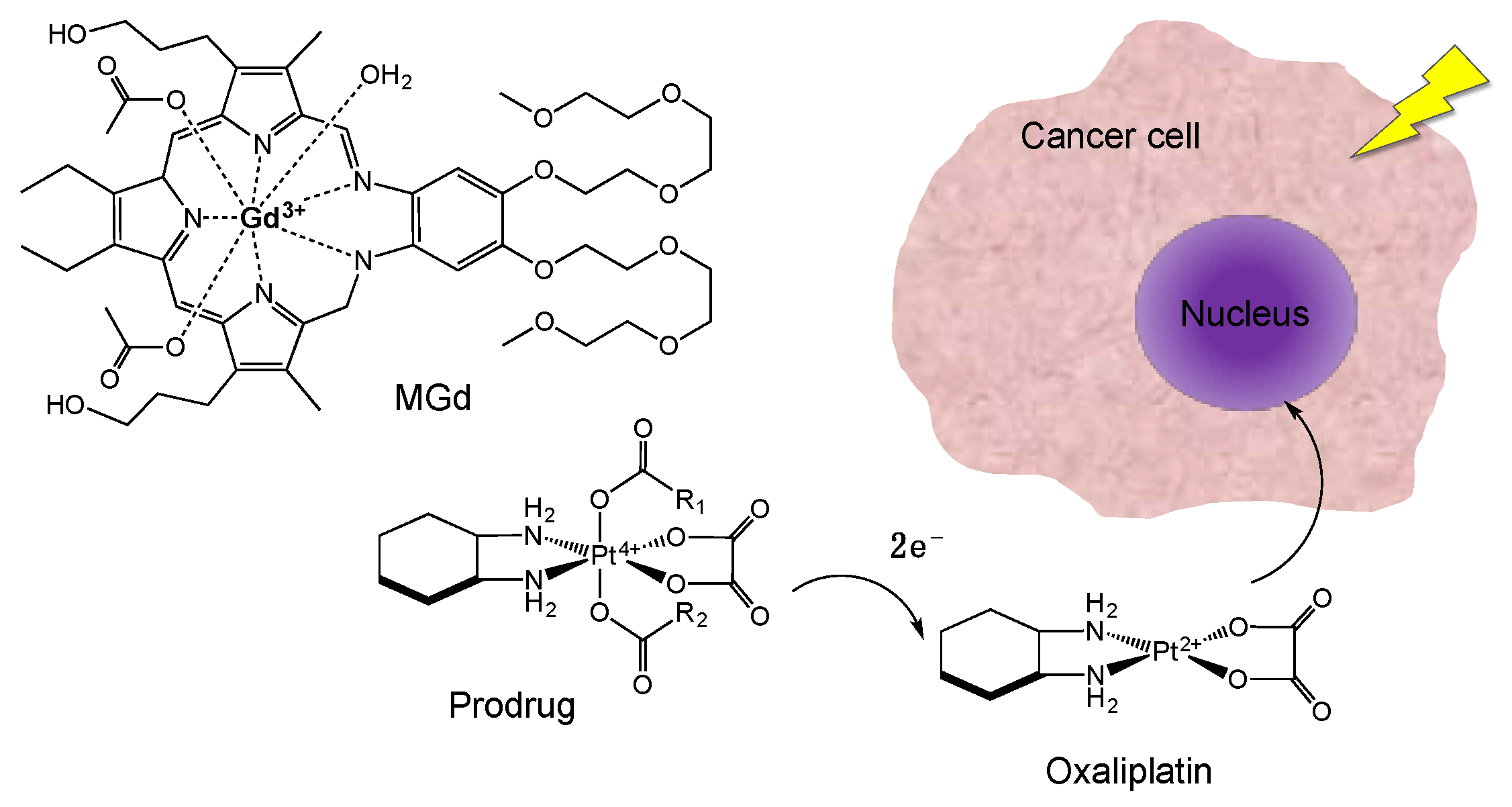
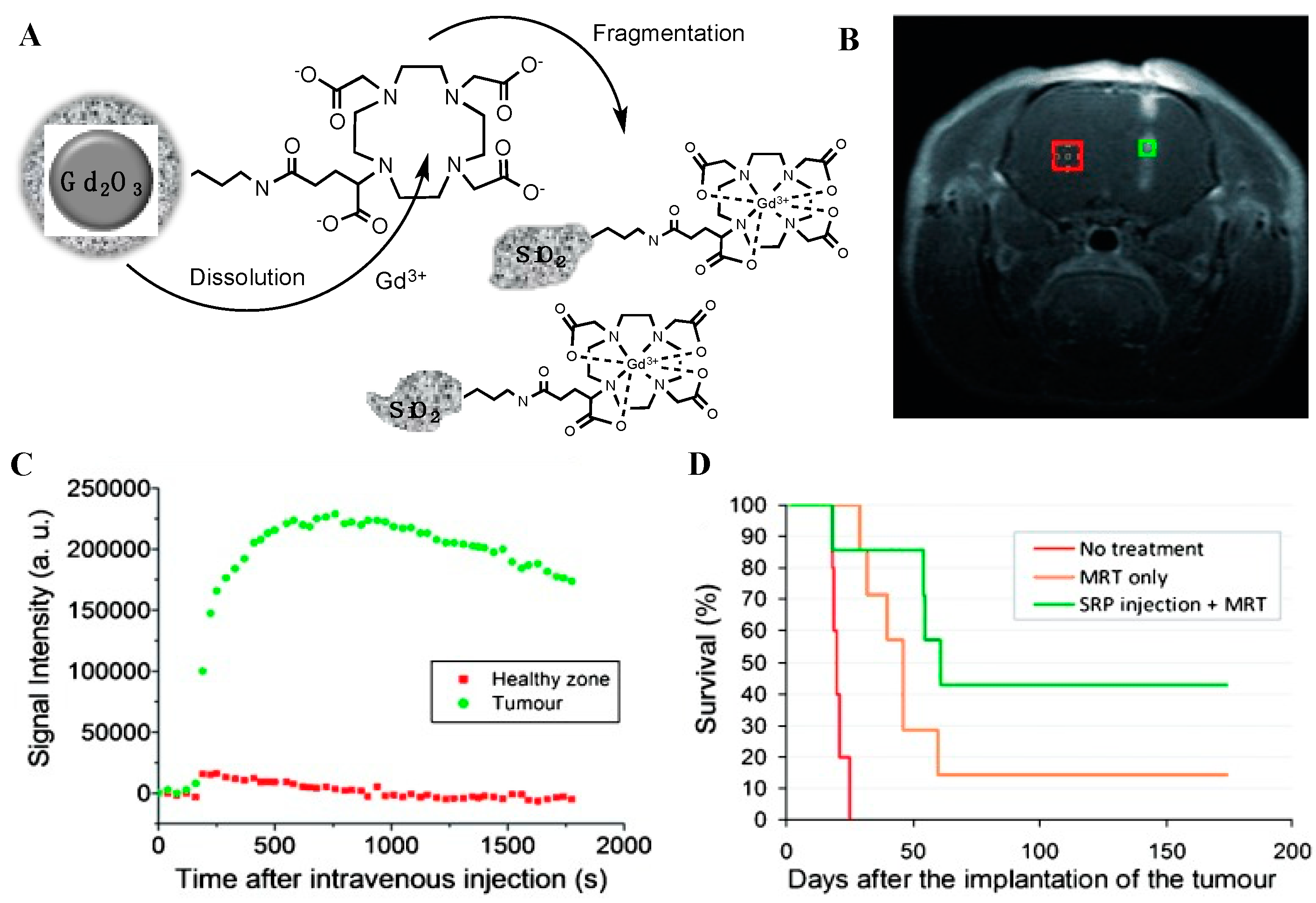
2.1.1. Gadolinium-Based Radiosensitization
2.1.2. Iron Oxide Nanoparticles
3. The Role of MRI in Internal Radionuclide Therapy
4. Neutron Capture Therapy Combined with MRI
5. Conclusions
Author Contributions
Funding
Acknowledgments
Conflicts of Interest
References
- Gaddikeri, S.; Gaddikeri, R.S.; Tailor, T.; Anzai, Y. Dynamic contrast-enhanced MR imaging in head and neck cancer: Techniques and clinical applications. Am. J. Neuroradiol. 2016, 37, 588–595. [Google Scholar] [CrossRef] [PubMed]
- Hoskin, P.J.; Carnell, D.M.; Taylor, N.J.; Smith, R.E.; Stirling, J.J.; Daley, F.M.; Saunders, M.I.; Bentzen, S.M.; Collins, D.J.; d’Arcy, J.A.; et al. Hypoxia in prostate cancer: Correlation of BOLD-MRI with pimonidazole immunohistochemistry—Initial observations. Int. J. Radiat. Oncol. Biol. Phys. 2007, 68, 1065–1071. [Google Scholar] [CrossRef] [PubMed]
- Bostel, T.; Nicolay, N.H.; Grossmann, J.G.; Mohr, A.; Delorme, S.; Echner, G.; Haring, P.; Debus, J.; Sterzing, F. MR-guidance—A clinical study to evaluate a shuttle-based MR-linac connection to provide MR-guided radiotherapy. Radiat. Oncol. 2014, 9, 12. [Google Scholar] [CrossRef] [PubMed]
- Raaymakers, B.W.; Lagendijk, J.J.W.; Overweg, J.; Kok, J.G.M.; Raaijmakers, A.J.E.; Kerkhof, E.M.; van der Put, R.W.; Meijsing, I.; Crijns, S.P.M.; Benedosso, F.; et al. Integrating a 1.5T MRI scanner with a 6 MV accelerator: Proof of concept. Phys. Med. Biol. 2009, 54, N229–N237. [Google Scholar] [CrossRef] [PubMed]
- Torresin, A.; Brambilla, M.G.; Monti, A.F.; Moscato, A.; Brockmann, M.A.; Schad, L.; Attenberger, U.I.; Lohr, F. Review of potential improvements using MRI in the radiotherapy workflow. Z. Med. Phys. 2015, 25, 210–220. [Google Scholar] [CrossRef]
- Kelkar, S.S.; Reineke, T.M. Theranostics: Combining imaging and therapy. Bioconj. Chem. 2011, 22, 1879–1903. [Google Scholar] [CrossRef]
- Veldeman, L.; Madani, I.; Hulstaert, F.; De Meerleer, G.; De Meerleer, G.; De Neve, W. Evidence behind use of intensity-modulated radiotherapy: A systematic review of comparative clinical studies. Lancet Oncol. 2008, 9, 367–375. [Google Scholar] [CrossRef]
- Emami, B.; Sethi, A.; Petruzzelli, G.J. Influence of MRI on target volume delineation and IMRT planning in nasopharyngeal carcinoma. Int. J. Radiat. Oncol. Biol. Phys. 2003, 57, 481–488. [Google Scholar] [CrossRef]
- Caffo, O. Radiosensitization with chemotherapeutic agents. Lung Cancer 2001, 34 (Suppl. 4), S81–S90. [Google Scholar] [CrossRef]
- Wardman, P. Chemical radiosensitizers for use in radiotherapy. Clin. Oncol. 2007, 19, 397–417. [Google Scholar] [CrossRef]
- Castillo, M.H.; Button, T.M.; Doerr, R.; Homs, M.I.; Pruett, C.W.; Pearce, J.I. Effects of radiotherapy on mandibular reconstruction plates. Am. J. Surg. 1988, 156, 261–263. [Google Scholar] [CrossRef]
- Matsudaira, H.; Ueno, A.M.; Furuno, I. Iodine contrast medium sensitizes cultured mammalian cells to X rays but not to γ rays. Radiat. Res. 1980, 84, 144–148. [Google Scholar] [CrossRef]
- Ngoune, R.; Peters, A.; von Elverfeldt, D.; Winkler, K.; Pütz, G. Accumulating nanoparticles by EPR: A route of no return. J. Control. Release 2016, 238, 58–70. [Google Scholar] [CrossRef] [PubMed]
- Jokerst, J.V.; Lobovkina, T.; Zare, R.N.; Gambhir, S.S. Nanoparticle PEGylation for imaging and therapy. Nanomedicine 2011, 6, 715–728. [Google Scholar] [CrossRef]
- Hainfeld, J.F.; Slatkin, D.N.; Smilowitz, H.M. The use of gold nanoparticles to enhance radiotherapy in mice. Phys. Med. Biol. 2004, 49, N309–N315. [Google Scholar] [CrossRef]
- Tóth, E.; Helm, L.; Merbach, A. Relaxivity of Gadolinium(III) Complexes: Theory and Mechanism; John Wiley & Sons Ltd.: Chichester, UK, 2013; pp. 25–81. [Google Scholar]
- Zhang, B.; Liang, L.; Chen, W.; Liang, C.; Zhang, S. An updated study to determine association between gadolinium-based contrast agents and nephrogenic systemic fibrosis. PLoS ONE 2015, 10, e0129720. [Google Scholar] [CrossRef]
- Vergauwen, E.; Vanbinst, A.-M.; Brussaard, C.; Janssens, P.; De Clerck, D.; Van Lint, M.; Houtman, A.C.; Michel, O.; Keymolen, K.; Lefevere, B.; et al. Central nervous system gadolinium accumulation in patients undergoing periodical contrast MRI screening for hereditary tumor syndromes. Hered. Cancer Clin. Pract. 2018, 16, 2. [Google Scholar] [CrossRef]
- Thomas, S.R.; Khuntia, D. Motexafin gadolinium: A promising radiation sensitizer in brain metastasis. Expert Opin. Drug Dis. 2011, 6, 195–203. [Google Scholar] [CrossRef]
- Richards, G.M.; Mehta, M.P. Motexafin gadolinium in the treatment of brain metastases. Expert Opin. Pharmacother. 2007, 8, 351–359. [Google Scholar] [CrossRef]
- Thiabaud, G.; McCall, R.; He, G.; Arambula, J.F.; Siddik, Z.H.; Sessler, J.L. Frontispiece: Activation of platinum(IV) prodrugs by motexafin gadolinium as a redox mediator. Angew. Chem. Int. Ed. 2016, 55, 12626–12631. [Google Scholar] [CrossRef] [PubMed]
- Botta, M.; Tei, L. Relaxivity enhancement in macromolecular and nanosized GdIII-based MRI contrast agents. Eur. J. Inorg. Chem. 2012, 2012, 1945–1960. [Google Scholar] [CrossRef]
- Bazzi, R.; Flores, M.A.; Louis, C.; Lebbou, K.; Zhang, W.; Dujardin, C.; Roux, S.; Mercier, B.; Ledoux, G.; Bernstein, E.; et al. Synthesis and properties of europium-based phosphors on the nanometer scale: Eu2O3, Gd2O3:Eu, and Y2O3:Eu. J. Colloid. Interface Sci. 2004, 273, 191–197. [Google Scholar] [CrossRef]
- Bridot, J.-L.; Dayde, D.; Riviere, C.; Mandon, C.; Billotey, C.; Lerondel, S.; Sabattier, R.; Cartron, G.; Le Pape, A.; Blondiaux, G.; et al. Hybrid gadolinium oxide nanoparticles combining imaging and therapy. J. Mater. Chem. 2009, 19, 2328–2335. [Google Scholar] [CrossRef]
- Mignot, A.; Truillet, C.; Lux, F.; Sancey, L.; Louis, C.; Denat, F.; Boschetti, F.; Bocher, L.; Gloter, A.; Stéphan, O.; et al. A top-down synthesis route to ultrasmall multifunctional Gd-based silica nanoparticles for theranostic applications. Chem. Eur. J. 2013, 19, 6122–6136. [Google Scholar] [CrossRef]
- Le Duc, G.; Roux, S.; Paruta-Tuarez, A.; Dufort, S.; Brauer, E.; Marais, A.; Truillet, C.; Sancey, L.; Perriat, P.; Lux, F.; et al. Advantages of gadolinium based ultrasmall nanoparticles vs. molecular gadolinium chelates for radiotherapy guided by MRI for glioma treatment. Cancer Nanotechnol. 2014, 5, 4. [Google Scholar] [CrossRef]
- Bianchi, A.; Lux, F.; Tillement, O.; Crémillieux, Y. Contrast enhanced lung MRI in mice using ultra-short echo time radial imaging and intratracheally administrated Gd-DOTA-based nanoparticles. Magn. Res. Med. 2012, 70, 1419–1426. [Google Scholar] [CrossRef]
- Detappe, A.; Thomas, E.; Tibbitt, M.W.; Kunjachan, S.; Zavidij, O.; Parnandi, N.; Reznichenko, E.; Lux, F.; Tillement, O.; Berbeco, R. Ultrasmall silica-based bismuth gadolinium nanoparticles for dual magnetic resonance-computed tomography image guided radiation therapy. Nano Lett. 2017, 17, 1733–1740. [Google Scholar] [CrossRef]
- Du, F.; Zhang, L.; Zhang, L.; Zhang, M.; Gong, A.; Tan, Y.; Miao, J.; Gong, Y.; Sun, M.; Ju, H.; et al. Engineered gadolinium-doped carbon dots for magnetic resonance imaging-guided radiotherapy of tumors. Biomaterials 2017, 121, 109–120. [Google Scholar] [CrossRef]
- Mahmoudi, M.; Hosseinkhani, H.; Hosseinkhani, M.; Boutry, S.; Simchi, A.; Journeay, W.S.; Subramani, K.; Laurent, S. Magnetic resonance imaging tracking of stem cells in vivo using iron oxide nanoparticles as a tool for the advancement of clinical regenerative medicine. Chem. Rev. 2011, 111, 253–280. [Google Scholar] [CrossRef]
- Laurent, S.; Forge, D.; Port, M.; Roch, A.; Robic, C.; Vander Elst, L.; Muller, R.N. Magnetic iron oxide nanoparticles: Synthesis, stabilization, vectorization, physicochemical characterizations, and biological applications. Chem. Rev. 2008, 108, 2064–2110. [Google Scholar] [CrossRef]
- Revia, R.A.; Zhang, M. Magnetite nanoparticles for cancer diagnosis, treatment, and treatment monitoring: Recent advances. Mater. Today 2016, 19, 157–168. [Google Scholar] [CrossRef]
- Kohler, N.; Sun, C.; Fichtenholtz, A.; Gunn, J.; Fang, C.; Zhang, M. Methotrexate-immobilized poly(ethylene glycol) magnetic nanoparticles for MR imaging and drug delivery. Small 2006, 2, 785–792. [Google Scholar] [CrossRef]
- Medarova, Z.; Pham, W.; Kim, Y.; Dai, G.P.; Moore, A. In vivo imaging of tumor response to therapy using a dual-modality imaging strategy. Int. J. Cancer 2006, 118, 2796–2802. [Google Scholar] [CrossRef] [PubMed]
- Saberi, A.; Shahbazi-Gahrouei, D.; Abbasian, M.; Fesharaki, M.; Baharlouei, A.; Arab-Bafrani, Z. Gold nanoparticles in combination with megavoltage radiation energy increased radiosensitization and apoptosis in colon cancer HT-29 cells. Int. J. Radiat. Biol. 2017, 93, 315–323. [Google Scholar] [CrossRef]
- Khoshgard, K.; Kiani, P.; Haghparast, A.; Hosseinzadeh, L.; Eivazi, M.T. Radiation dose rate affects the radiosensitization of MCF-7 and HeLa cell lines to X-rays induced by dextran-coated iron oxide nanoparticles. Int. J. Radiat. Biol. 2017, 93, 757–763. [Google Scholar] [CrossRef]
- Khoei, S.; Mahdavi, S.R.; Fakhimikabir, H.; Shakeri-Zadeh, A.; Hashemian, A. The role of iron oxide nanoparticles in the radiosensitization of human prostate carcinoma cell line DU145 at megavoltage radiation energies. Int. J. Radiat. Biol. 2014, 90, 351–356. [Google Scholar] [CrossRef]
- Klein, S.; Sommer, A.; Distel, L.V.; Neuhuber, W.; Kryschi, C. Superparamagnetic iron oxide nanoparticles as radiosensitizer via enhanced reactive oxygen species formation. Biochem. Biophys. Res. Commun. 2012, 425, 393–397. [Google Scholar] [CrossRef] [PubMed]
- Kirakli, E.K.; Takan, G.; Hoca, S.; Müftüler, F.Z.B.; Kılçar, A.Y.; Kamer, S.A. Superparamagnetic iron oxide nanoparticle (SPION) mediated in vitro radiosensitization at megavoltage radiation energies. J. Radioanal. Nucl. Chem. 2018, 315, 595–602. [Google Scholar] [CrossRef]
- Rajaee, A.; Wensheng, X.; Zhao, L.; Wang, S.; Liu, Y.; Wu, Z.; Wang, J.; Si-Shen, F. Multifunctional bismuth ferrite nanoparticles as magnetic localized dose enhancement in radiotherapy and imaging. J. Biomed. Nanotechnol. 2018, 14, 1159–1168. [Google Scholar] [CrossRef] [PubMed]
- Zhao, D.; Sun, X.; Tong, J.; Ma, J.; Bu, X.; Xu, R.; Fan, R. A novel multifunctional nanocomposite C225-conjugated Fe3O4/Ag enhances the sensitivity of nasopharyngeal carcinoma cells to radiotherapy. Acta Biochim. Biophys. Sin. 2012, 44, 678–684. [Google Scholar] [CrossRef] [PubMed]
- Dou, Y.; Li, X.; Yang, W.; Guo, Y.; Wu, M.; Liu, Y.; Li, X.; Zhang, X.; Chang, J. Pb@Au core–satellite multifunctional nanotheranostics for magnetic resonance and computed tomography imaging in vivo and synergetic photothermal and radiosensitive therapy. ACS Appl. Mater. Interfaces 2017, 9, 1263–1272. [Google Scholar] [CrossRef]
- Daou, T.J.; Grenèche, J.M.; Pourroy, G.; Buathong, S.; Derory, A.; Ulhaq-Bouillet, C.; Donnio, B.; Guillon, D.; Begin-Colin, S. Coupling agent effect on magnetic properties of functionalized magnetite-based nanoparticles. Chem. Mater. 2008, 20, 5869–5875. [Google Scholar] [CrossRef]
- Longmire, M.; Choyke, P.L.; Kobayashi, H. Clearance properties of nano-sized particles and molecules as imaging agents: Considerations and caveats. Nanomedicine 2008, 3, 703–717. [Google Scholar] [CrossRef]
- Zagar, T.M.; Oleson, J.R.; Vujaskovic, Z.; Dewhirst, M.W.; Craciunescu, O.I.; Blackwell, K.L.; Prosnitz, L.R.; Jones, E.L. Hyperthermia combined with radiation therapy for superficial breast cancer and chest wall recurrence: A review of the randomised data. Int. J. Hyperther. 2010, 26, 612–617. [Google Scholar] [CrossRef]
- Kratochwil, C.; Bruchertseifer, F.; Giesel, F.L.; Weis, M.; Verburg, F.A.; Mottaghy, F.; Kopka, K.; Apostolidis, C.; Haberkorn, U.; Morgenstern, A. 225Ac-psma-617 for PSMA-targeted alpha-radiation therapy of metastatic castration-resistant prostate cancer. J. Nucl. Med. 2016, 57, 1941–1944. [Google Scholar] [CrossRef]
- Yeong, C.-H.; Cheng, M.-H.; Ng, K.-H. Therapeutic radionuclides in nuclear medicine: Current and future prospects. J. Zhejiang Univ. Sci. B 2014, 15, 845–863. [Google Scholar] [CrossRef]
- Carvalho, D.P.; Ferreira, A.C. The importance of sodium/iodide symporter (NIS) for thyroid cancer management. Arq. Bras. Endocrinol. Metabol. 2007, 51, 672–682. [Google Scholar] [CrossRef]
- Srivastava, S.; Dadachova, E. Recent advances in radionuclide therapy. Semin. Nucl. Med. 2001, 31, 330–341. [Google Scholar] [CrossRef]
- D’Angelo, G.; Sciuto, R.; Salvatori, M.; Sperduti, I.; Mantini, G.; Maini, C.L.; Marian, G. Targeted “bone-seeking” radiopharmaceuticals for palliative treatment of bone metastases: A systematic review and meta-analysis. Q. J. Nucl. Med. Mol. Imaging 2012, 56, 538–543. [Google Scholar]
- Dash, A.; Knapp, F.F.; Pillai, M.R. Targeted radionuclide therapy—An overview. Curr. Radiopharm. 2013, 6, 152–180. [Google Scholar] [CrossRef]
- Pugh, T.J.; Pokharel, S.S. Magnetic resonance imaging in prostate brachytherapy: Evidence, clinical end points to data, and direction forward. Brachytherapy 2017, 16, 659–664. [Google Scholar] [CrossRef]
- Bult, W.; Kroeze, S.G.C.; Elschot, M.; Seevinck, P.R.; Beekman, F.J.; de Jong, H.W.A.M.; Uges, D.R.A.; Kosterink, J.G.W.; Luijten, P.R.; Hennink, W.E.; et al. Intratumoral administration of holmium-166 acetylacetonate microspheres: Antitumor efficacy and feasibility of multimodality imaging in renal cancer. PLoS ONE 2013, 8, e52178. [Google Scholar] [CrossRef]
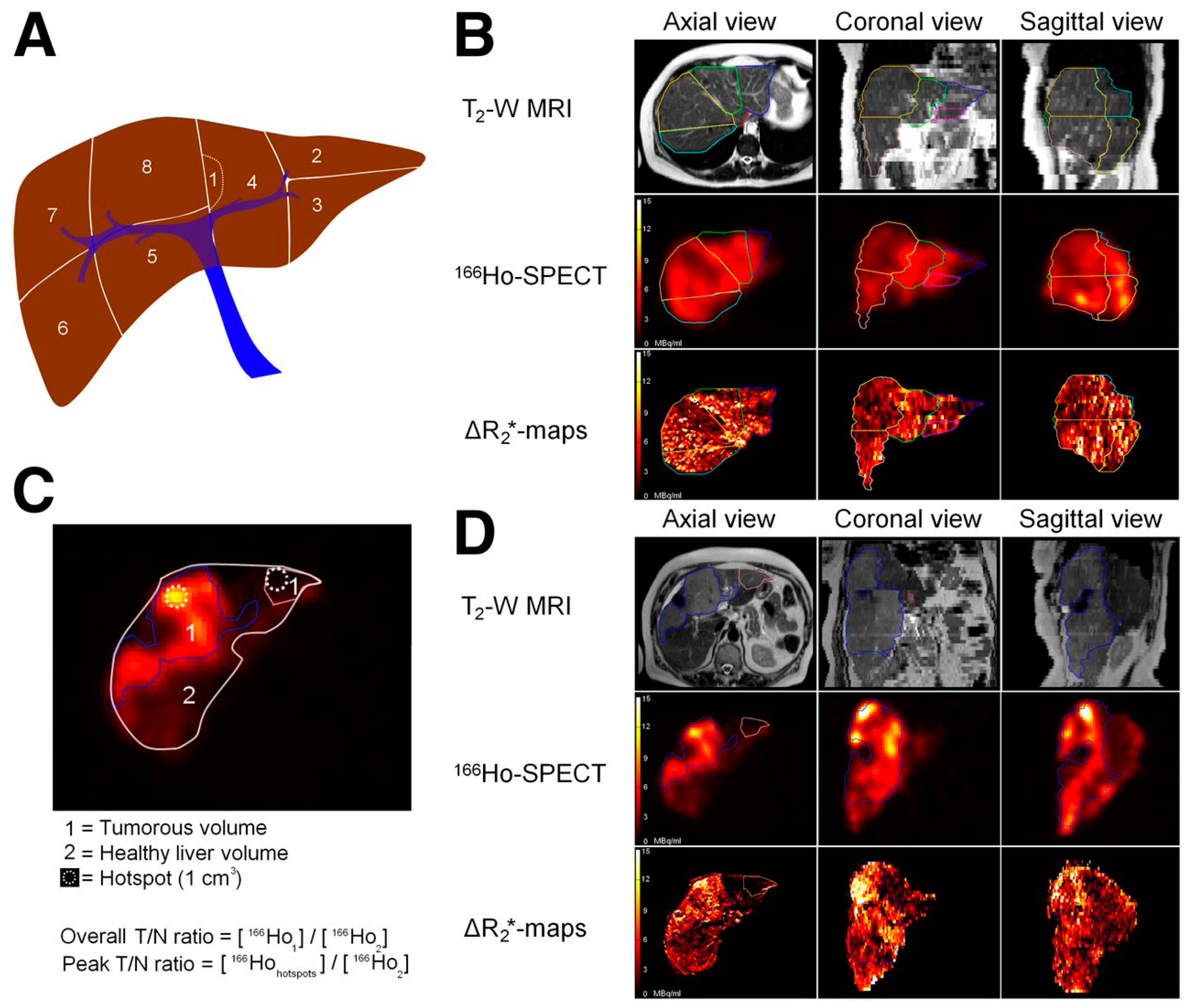
- Smits, M.L.J.; Elschot, M.; van den Bosch, M.A.A.J.; van de Maat, G.H.; van het Schip, A.D.; Zonnenberg, B.A.; Seevinck, P.R.; Verkooijen, H.M.; Bakker, C.J.; de Jong, H.W.A.M.; et al. In vivo dosimetry based on SPECT and MR imaging of 166Ho-microspheres for treatment of liver malignancies. J. Nucl. Med. 2013, 54, 2093–2100. [Google Scholar] [CrossRef]
- Van de Maat, G.H.; Seevinck, P.R.; Elschot, M.; Smits, M.L.J.; de Leeuw, H.; van het Schip, A.D.; Vente, M.A.D.; Zonnenberg, B.A.; de Jong, H.W.A.M.; Lam, M.G.E.H.; et al. MRI-based biodistribution assessment of holmium-166 poly(l-lactic acid) microspheres after radioembolisation. Eur. Radiol. 2013, 23, 827–835. [Google Scholar] [CrossRef]
- Cao, J.; Wang, Y.; Yu, J.; Xia, J.; Zhang, C.; Yin, D.; Häfeli, U.O. Preparation and radiolabeling of surface-modified magnetic nanoparticles with rhenium-188 for magnetic targeted radiotherapy. J. Magn. Magn. Mater. 2004, 277, 165–174. [Google Scholar] [CrossRef]
- Chunfu, Z.; Jinquan, C.; Duanzhi, Y.; Yongxian, W.; Yanlin, F.; Jiajü, T. Preparation and radiolabeling of human serum albumin (HSA)-coated magnetite nanoparticles for magnetically targeted therapy. Appl. Radiat. Isotopes 2004, 61, 1255–1259. [Google Scholar] [CrossRef]
- Zhang, C.; Sun, H.; Xia, J.; Yu, J.; Yao, S.; Yin, D.; Wang, Y. Synthesis of polyacrylamide modified magnetic nanoparticles and radiolabeling with 188Re for magnetically targeted radiotherapy. J. Magn. Magn. Mater. 2005, 293, 193–198. [Google Scholar] [CrossRef]
- Aslan, T.N.; Aşık, E.; Volkan, M. Preparation and labeling of surface-modified magnetoferritin protein cages with a rhenium(I) carbonyl complex for magnetically targeted radiotherapy. RSC Adv. 2016, 6, 8860–8869. [Google Scholar] [CrossRef]
- Radović, M.; Calatayud, M.P.; Goya, G.F.; Ibarra, M.R.; Antić, B.; Spasojević, V.; Nikolić, N.; Janković, D.; Mirković, M.; Vranješ-Đurić, S. Preparation and in vivo evaluation of multifunctional 90Y-labeled magnetic nanoparticles designed for cancer therapy. J. Biomed. Mater. Res. A 2015, 103, 126–134. [Google Scholar] [CrossRef]
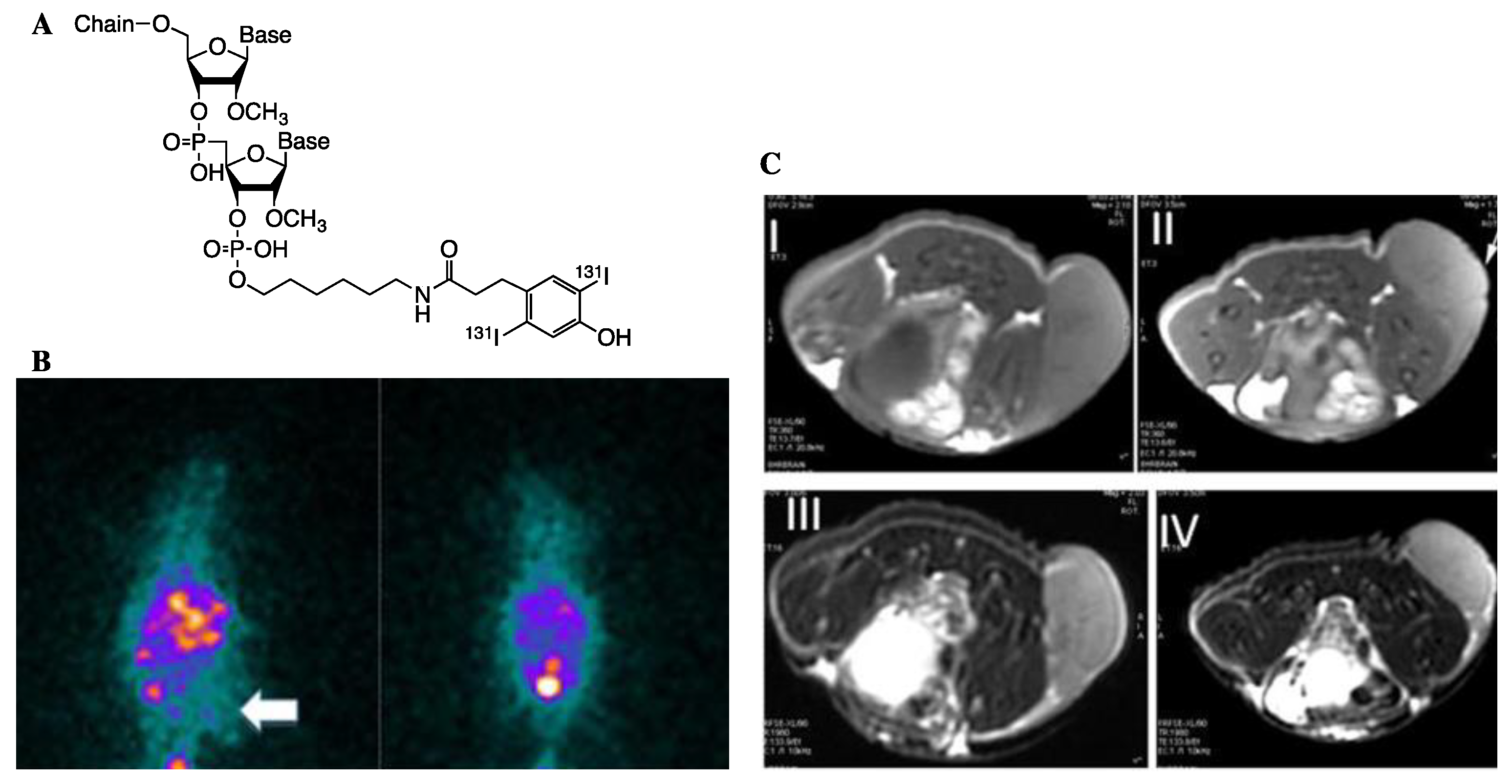
- Chen, J.; Zhu, S.; Tong, L.; Li, J.; Chen, F.; Han, Y.; Zhao, M.; Xiong, W. Superparamagnetic iron oxide nanoparticles mediated 131I-hVGF siRNA inhibits hepatocellular carcinoma tumor growth in nude mice. BMC Cancer 2014, 14, 114. [Google Scholar] [CrossRef]
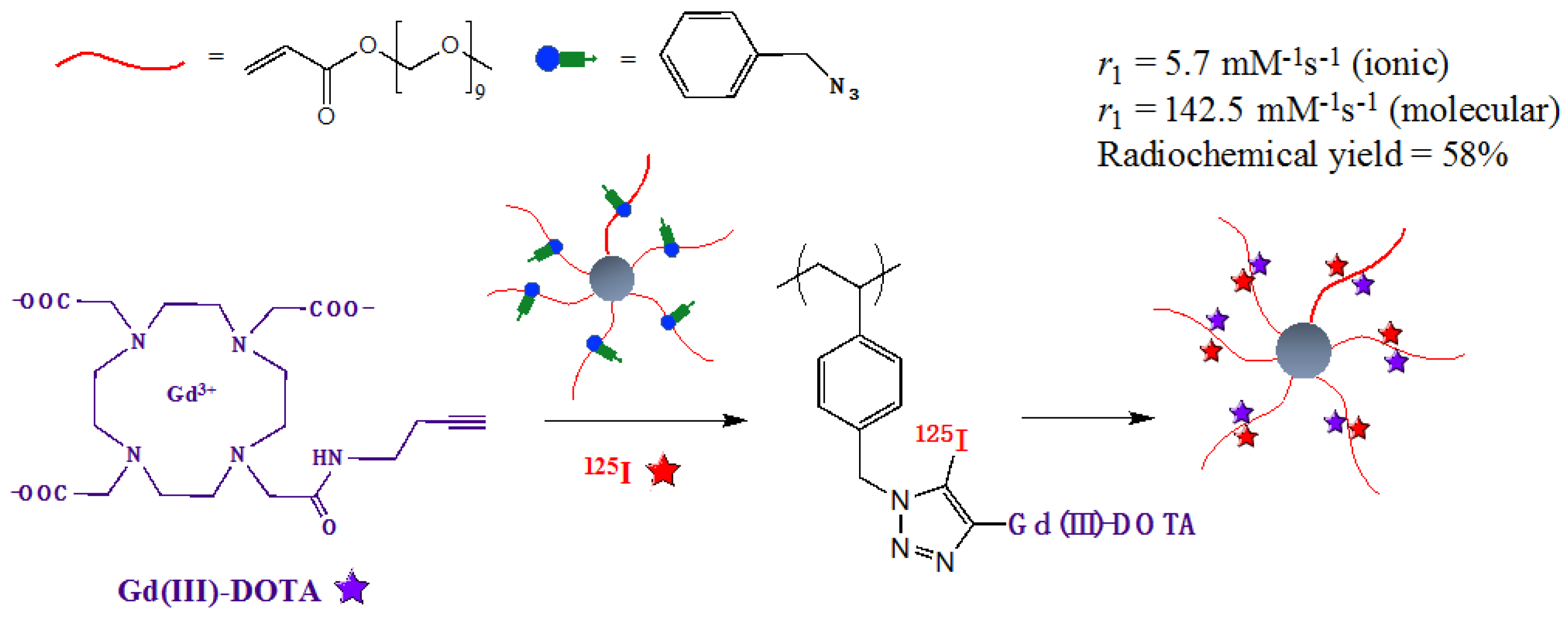
- Esser, L.; Lengkeek, N.A.; Moffat, B.A.; Vu, M.N.; Greguric, I.; Quinn, J.F.; Davis, T.P.; Whittaker, M.R. A tunable one-pot three-component synthesis of an 125I and Gd-labelled star polymer nanoparticle for hybrid imaging with MRI and nuclear medicine. Polym. Chem. 2018, 9, 3528–3535. [Google Scholar] [CrossRef]
- Locher, G.L. Biological effects and therapeutic possibilities of neutrons. Am. J. Roentgenol. 1936, 36, 1–13. [Google Scholar]
- Miyatake, S.-I.; Kawabata, S.; Hiramatsu, R.; Kuroiwa, T.; Suzuki, M.; Kondo, N.; Ono, K. Boron neutron capture therapy for malignant brain tumors. Neurol. Med. Chir. 2016, 56, 361–371. [Google Scholar] [CrossRef]
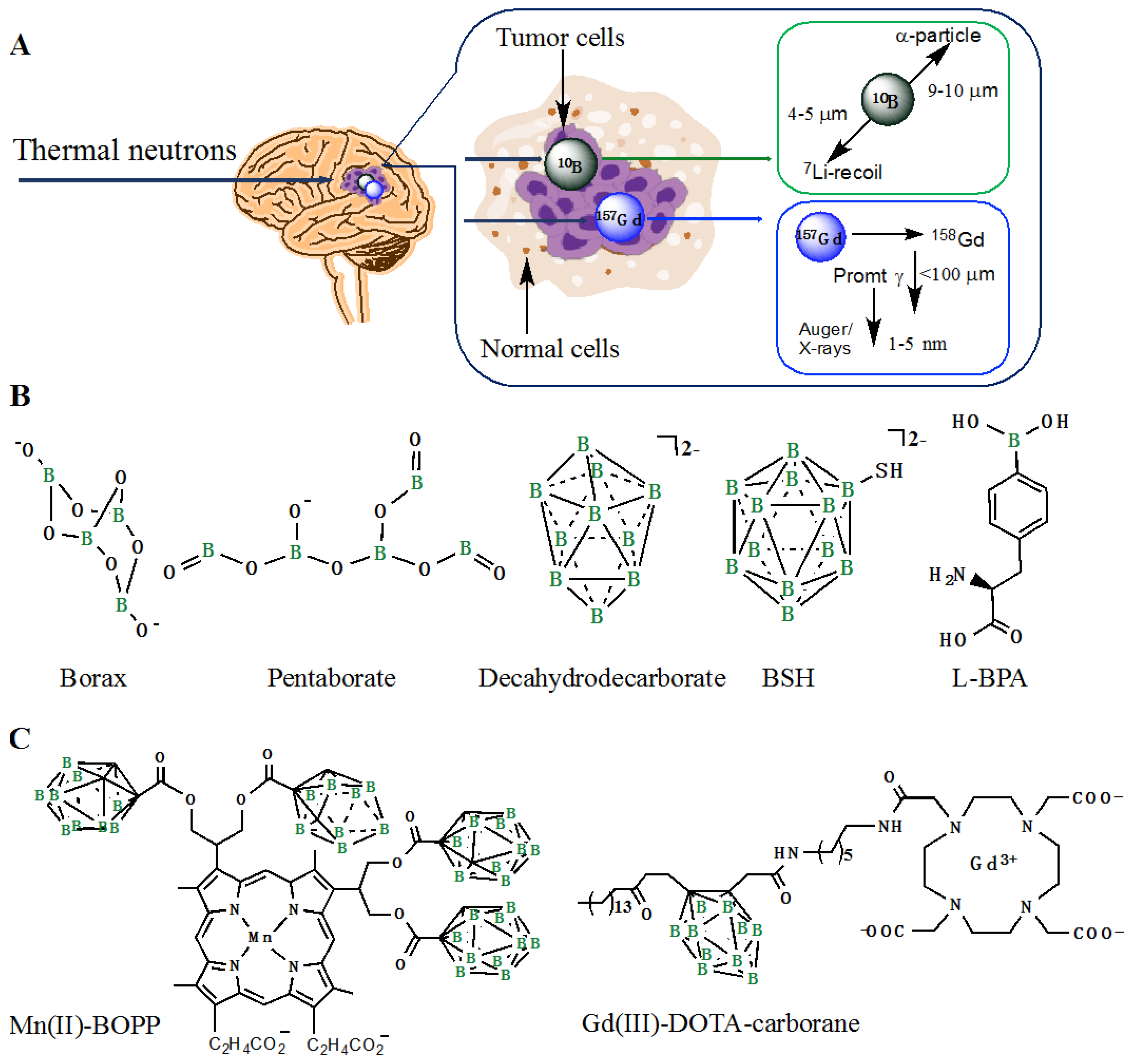
- Barth, R.F.; Coderre, J.A.; Vicente, M.G.H.; Blue, T.E. Boron neutron capture therapy of cancer: Current status and future prospects. Clin. Cancer. Res. 2005, 11, 3987–4002. [Google Scholar] [CrossRef]
- Kabalka, G.W.; Smith, G.T.; Dyke, J.P.; Reid, W.S.; Longford, C.D.; Roberts, T.G.; Kesavulu Reddy, N.; Buonocore, E.; Hübner, K.F. Evaluation of fluorine-18-BPA-fructose for boron neutron capture treatment planning. J. Nucl. Med. 1997, 38, 1762–1767. [Google Scholar]
- Huang, L.R.; Straubinger, R.M.; Kahl, S.B.; Koo, M.-S.; Alletto, J.J.; Mazurchuk, R.; Chau, R.I.; Thamer, S.L.; Fiel, R.J. Boronated metalloporphyrins: A novel approach to the diagnosis and treatment of cancer using contrast-enhanced MR imaging and neutron capture therapy. J. Magn. Reson. Imaging 1993, 3, 351–356. [Google Scholar] [CrossRef]
- Takahashi, K.; Nakamura, H.; Furumoto, S.; Yamamoto, K.; Fukuda, H.; Matsumura, A.; Yamamoto, Y. Synthesis and in vivo biodistribution of BPA-Gd-DTPA complex as a potential MRI contrast carrier for neutron capture therapy. Bioorg. Med. Chem. 2005, 13, 735–743. [Google Scholar] [CrossRef]
- Deagostino, A.; Protti, N.; Alberti, D.; Boggio, P.; Bortolussi, S.; Altieri, S.; Geninatti-Crich, S. Insights into the use of gadolinium and gadolinium/boron-based agents in imaging-guided neutron capture therapy applications. Future Med. Chem. 2016, 8, 899–917. [Google Scholar] [CrossRef]
- Akine, Y.; Tokita, N.; Tokuuye, K.; Satoh, M.; Churei, H.; Le Pechoux, C.; Kobayashi, T.; Kanda, K. Suppression of rabbit VX-2 subcutaneous tumor growth by gadolinium neutron capture therapy. Jpn. J. Cancer Res. 1993, 84, 841–843. [Google Scholar] [CrossRef]
- Khokhlov, V.F.; Yashkin, P.N.; Silin, D.I.; Djorova, E.S.; Lawaczeck, R. Neutron capture therapy with gadopentetate dimeglumine: Experiments on tumor-bearing rats. Acad. Radiol. 1995, 2, 392–398. [Google Scholar] [CrossRef]
- Brugger, R.M.; Shih, J.A. Evaluation of gadolinium-157 as a neutron capture therapy agent. Strahlenther. Onkol. 1989, 165, 153–156. [Google Scholar]
- Tokumitsu, H.; Hiratsuka, J.; Sakurai, Y.; Kobayashi, T.; Ichikawa, H.; Fukumori, Y. Gadolinium neutron-capture therapy using novel gadopentetic acid–chitosan complex nanoparticles: In vivo growth suppression of experimental melanoma solid tumor. Cancer Lett. 2000, 150, 177–182. [Google Scholar] [CrossRef]
- Dewi, N.; Mi, P.; Yanagie, H.; Sakurai, Y.; Morishita, Y.; Yanagawa, M.; Nakagawa, T.; Shinohara, A.; Matsukawa, T.; Yokoyama, K.; et al. In vivo evaluation of neutron capture therapy effectivity using calcium phosphate-based nanoparticles as Gd-DTPA delivery agent. J. Cancer. Res. Clin. Oncol. 2016, 142, 767–775. [Google Scholar] [CrossRef]
| Composition/Coating | Preparation Method | Size (nm) | Radiation Energy | Cell Line | Tested Application | Ref. |
|---|---|---|---|---|---|---|
| Fe3O4/dextran | Co-precipitation | 15 | 6 MV | MCF-7/HeLa | ERT | [36] |
| SPIONs/dextran-NH2 | - 1 | 130 | 6 MV | DU 145 | ERT/MRI | [37] |
| γFe2O3/Fe3O4/citrate | Co-precipitation 3 | 6–20 2 3–10 3 | 120 kV | MCF-7 | ERT | [38] |
| SPIONs/citrate | Co-precipitation | 6–25 | 6 MV | MCF-7/MDAH-2447/MDA-MB-231 | ERT | [39] |
| BiFeO3 | Sol-gel | 30 | 160 kV | MCF-7 | MRI/ERT/CT/HT | [40] |
| Fe3O4/Ag/C225 | Co-precipitation | 102 | 6 MV | CNE | ERT | [41] |
| Fe4[Fe(CN)6]3-Au/ citrate-PEG | Electrostatic absorption | 139 | - | 4T1 | MRI/CT/PTT/ERT | [42] |
| Radio- Nuclide | Half- Life | Decay Mode | Soft Tissue Range (mm) | Product | Most Common Clinical Application 1 |
|---|---|---|---|---|---|
| 166Ho | 26.8 h | β− | 8.5 | 166Er | Hepatic cancer [54] |
| 186Re | 3.7 d | β−/ε | 3.6 | 186Os/186W | Bone metastasis, arthritis |
| 188Re | 17.0 h | β− | 11.0 | 188Os | Bone metastasis, arthritis [59] |
| 89Sr | 50.6 d | β− | 8.0 | 89Y | Bone metastasis |
| 177Lu | 6.7 d | β− | 1.7 | 177Hf | Various cancers |
| 90Y | 64.6 h | β− | 11.0 | 90Zr | Hepatic metastasis [60] |
| 153Sm | 46.3 h | β− | 3.4 | 153Eu | Bone metastasis |
| 165Dy | 2.3 h | β− | 5.7 | 165Ho | Rheumatoid arthritis |
| 32P | 14.3 d | β− | 7.9 | 32S | Cystic craniopharyngioma |
| 223Ra | 11.4 d | α | 0.01 | 219Rn | Bone metastasis |
| 131I | 8.0 d | β− | 2.4 | 131Xe | Thyroid cancer, neuroblastoma [61,62] |
| 125I | 59.4 d | γ/ε | 17.0 | 125Te | Brachytherapy of prostate cancer, postsurgical treatment of brain cancer, uveal melanoma [62] |
© 2019 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Putri Fauzia, R.; Denkova, A.G.; Djanashvili, K. Potential of MRI in Radiotherapy Mediated by Small Conjugates and Nanosystems. Inorganics 2019, 7, 59. https://doi.org/10.3390/inorganics7050059
Putri Fauzia R, Denkova AG, Djanashvili K. Potential of MRI in Radiotherapy Mediated by Small Conjugates and Nanosystems. Inorganics. 2019; 7(5):59. https://doi.org/10.3390/inorganics7050059
Chicago/Turabian StylePutri Fauzia, Retna, Antonia G. Denkova, and Kristina Djanashvili. 2019. "Potential of MRI in Radiotherapy Mediated by Small Conjugates and Nanosystems" Inorganics 7, no. 5: 59. https://doi.org/10.3390/inorganics7050059
APA StylePutri Fauzia, R., Denkova, A. G., & Djanashvili, K. (2019). Potential of MRI in Radiotherapy Mediated by Small Conjugates and Nanosystems. Inorganics, 7(5), 59. https://doi.org/10.3390/inorganics7050059