Interventions for Child Drowning Reduction in the Indian Sundarbans: Perspectives from the Ground
Abstract
1. Introduction
2. Materials and Methods
2.1. Data Collection
2.2. Participants
2.2.1. Community-Level Participants
2.2.2. Government Program Participants
2.2.3. Grassroots Organisations
2.3. Tools and Transcriptions
2.4. Ethics
2.5. Analysis
3. Results
3.1. Considerations for Program Design and Delivery
3.1.1. Acceptability across All Interventions
3.1.2. Affordability
3.1.3. Community Engagement and Ownership
3.1.4. Resources and Skill Set
3.1.5. Social Class
3.2. Intervention-Specific Considerations
3.2.1. Home-Based Barriers
3.2.2. Childcare and Supervision-Based Programs
3.2.3. Swim and Rescue Training
3.2.4. First Responder Program
3.2.5. Indigenous Interventions for Child Safety
3.3. Use of Government Programs in Drowning Intervention Delivery
3.3.1. ASHA Workers
3.3.2. Self-Help Groups
3.3.3. Anganwadi Centres (ICDS Program)
3.3.4. Other Community Programs
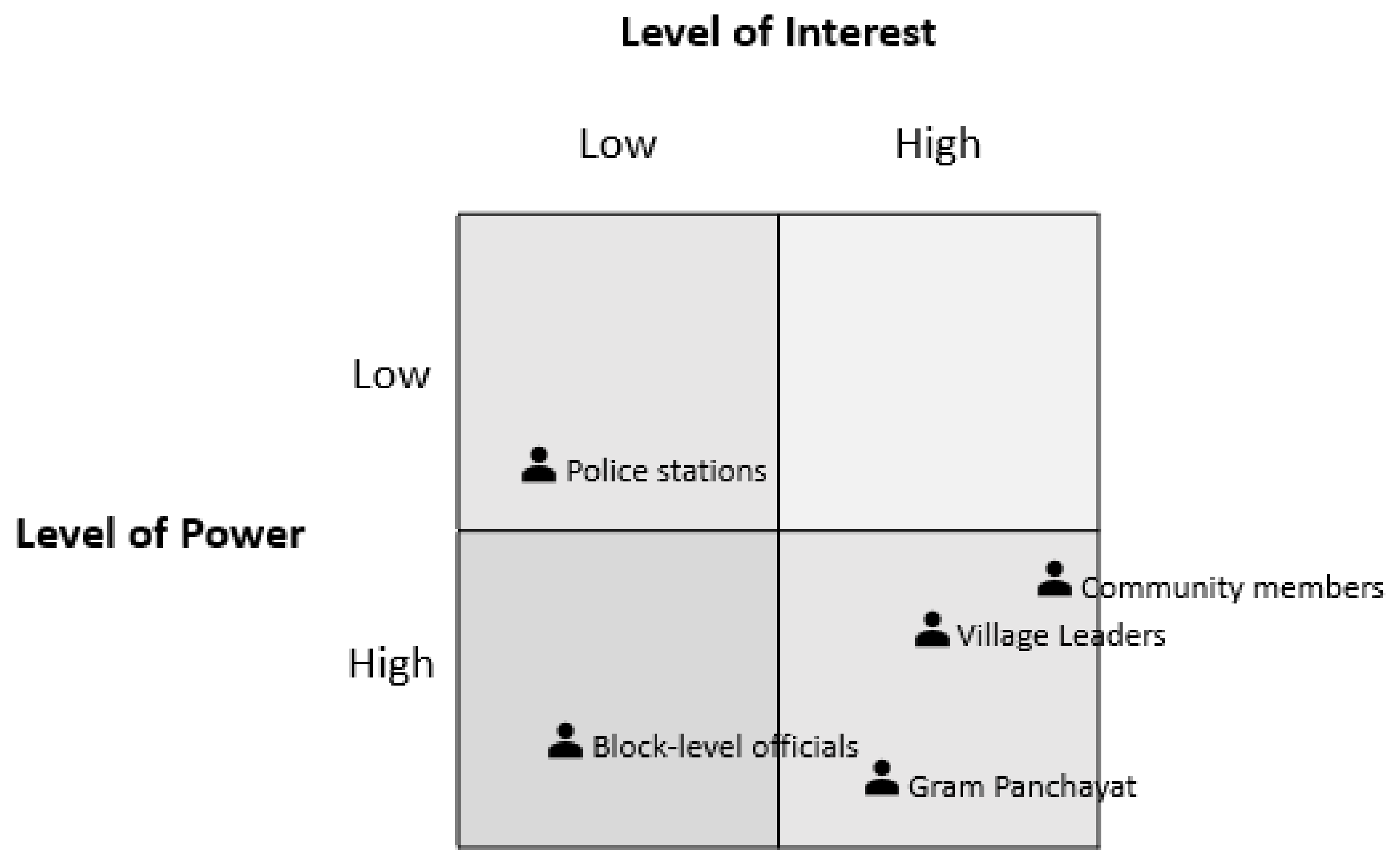
3.4. Stakeholder Analysis
3.4.1. Block-Level Officials
3.4.2. Gram Panchayat
3.4.3. Community Leaders
3.4.4. Local Police Stations
3.4.5. Community Members
3.4.6. Engagement Strategies
4. Discussion
Limitations of This Study
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Acknowledgments
Conflicts of Interest
Data Availability
References
- Meddings, D.; Hyder, A.A.; Ozanne-Smith, J.; Rahman, A. Global Report on Drowning: Preventing a Leading Killer; World Health Organization: Geneva, Switzerland, 2014. [Google Scholar]
- Menon, G.R.; Singh, L.; Sharma, P.; Yadav, P.; Singh, H.; Sati, P.; Begum, R.; Fadel, S.; Watson, L.; Jamison, D.T.; et al. National Burden Estimates of healthy life lost in India, 2017: An analysis using direct mortality data and indirect disability data. Lancet Glob. Health 2019, 7, e1675–e1684. [Google Scholar] [CrossRef]
- Mahadevia Ghimire, K.; Vikas, M. Climate Change–Impact on the Sundarbans: A case study. Int. Sci. J. Environ. Sci. 2012, 2, 7–15. [Google Scholar]
- Kanjilal, B.; Mazumdar, P.G.; Mukherjee, M.; Mondal, S.; Barman, D.; Singh, S.; Mandal, A. Health Care in the Sundarbans (India): Challenges and Plan for a Better Future. Future Health Systems Research Programme; Institute of Health Management Research: Jaipur, India, 2010. [Google Scholar]
- Alonge, O.; Hyder, A.A. Reducing the global burden of childhood unintentional injuries. Arch. Dis. Child. 2014, 99, 62. [Google Scholar] [CrossRef] [PubMed]
- Gupta, M.; Bhaumik, S.; Roy, S.; Panda, R.; Peden, M.; Jagnoor, J. Determining child drowning mortality in the Sundarbans, India: Applying the Community Knowledge Approach. Inj. Prev. 2020. [Google Scholar] [CrossRef]
- Lukaszyk, C.; Mittal, S.; Gupta, M.; Das, R.; Ivers, R.; Jagnoor, J. The impact and understanding of childhood drowning by a community in West Bengal, India, and the suggested preventive measures. Acta Paediatr. 2018, 108. [Google Scholar] [CrossRef]
- Bogart, L.M.; Uyeda, K. Community-Based Participatory Research: Partnering with Communities for Effective and Sustainable Behavioral Health Interventions. Health Psychol. 2009, 28, 391–393. [Google Scholar] [CrossRef]
- Hodge, L.M.; Turner, K.M.T. Sustained Implementation of Evidence-based Programs in Disadvantaged Communities: A Conceptual Framework of Supporting Factors. Am. J. Community Psychol. 2016, 58, 192–210. [Google Scholar] [CrossRef]
- Wight, D.; Wimbush, E.; Jepson, R.; Doi, L. Six steps in quality intervention development (6SQuID). J. Epidemiol. Community Health 2016, 70, 520. [Google Scholar] [CrossRef]
- Puri, S.; Fernandez, S.; Puranik, A.; Anand, D.; Syed, Z.; Patel, A.; Uddin, S.; Thow, A.M. Policy content and stakeholder network analysis for infant and young child feeding in India. BMC Public Health 2017, 17, 461. [Google Scholar] [CrossRef]
- Gruen, R.L.; Elliott, J.H.; Nolan, M.L.; Lawton, P.D.; Parkhill, A.; McLaren, C.J.; Lavis, J.N. Sustainability science: An integrated approach for health-programme planning. Lancet 2008, 372, 1579–1589. [Google Scholar] [CrossRef]
- Uzochukwu, B.; Onwujekwe, O.; Mbachu, C.; Okwuosa, C.; Etiaba, E.; Nyström, M.E.; Gilson, L. The challenge of bridging the gap between researchers and policy makers: Experiences of a Health Policy Research Group in engaging policy makers to support evidence informed policy making in Nigeria. Glob. Health 2016, 12, 67. [Google Scholar] [CrossRef] [PubMed]
- Shiffman, J.; Smith, S. Generation of political priority for global health initiatives: A framework and case study of maternal mortality. Lancet 2007, 370, 9. [Google Scholar] [CrossRef]
- Gupta, M.; Zwi, A.B.; Jagnoor, J. Opportunities for the development of drowning interventions in West Bengal, India: A review of policy and government programs. BMC Public Health 2020, 20, 704. [Google Scholar] [CrossRef] [PubMed]
- Maity, B. Interstate differences in the performance of Anganwadi centres under ICDS scheme. Econ. Polit. Wkly. 2016, 51, 59–66. [Google Scholar]
- Chatterjee, S.; Apartment, M. Self-help groups and economic empowerment of rural women: A case study. Int. J. Educ. Manag. Stud. 2014, 4, 103–107. [Google Scholar]
- Scott, K.; Shanker, S. Tying their hands? Institutional obstacles to the success of the ASHA community Health Worker Programme Rural North India. AIDS Care 2010, 22, 1606–1612. [Google Scholar] [CrossRef]
- Government of West Bengal. State Plan of Action for Children (2014–18); Department of Child Development and Women Development & Social Welfare: West Bengal, India, 2014.
- Tong, A.; Craig, J.; Sainsbury, P. Consolidated criteria for reporting qualitative research (COREQ): A 32-item checklist for interviews and focus groups. Int. J. Qual. Health Care 2007, 19, 349–357. [Google Scholar] [CrossRef]
- NVivo Qualitative Data Analysis Software. Available online: https://www.qsrinternational.com/nvivo-qualitative-data-analysis-software/home (accessed on 25 June 2020).
- Carter, N.; Bryant-Lukosius, D.; DiCenso, A.; Blythe, J.; Neville, A.J. The use of triangulation in qualitative research. Oncol. Nurs. Forum 2014, 41, 545–547. [Google Scholar] [CrossRef]
- Mendelow, A.L. Environmental scanning: The impact of the stakeholder concept. In Proceedings of the Second International Conference on Information Systems, Cambridge, MA, USA, 7–9 December 1981. [Google Scholar]
- World Health Organization. Preventing Drowning: An Implementation Guide; World Health Organization: Geneva, Switzerland, 2017. [Google Scholar]
- Movsisyan, A.; Arnold, L.; Evans, R.; Hallingberg, B.; Moore, G.; O’Cathain, A.; Pfadenhauer, L.M.; Segrott, J.; Rehfuess, E. Adapting evidence-informed complex population health interventions for new contexts: A systematic review of guidance. Implement Sci. 2019, 14, 105. [Google Scholar] [CrossRef]
- Mitchell, R.J.; Ryder, T. Rethinking the public health model for injury prevention. Inj. Prev. 2020, 26, 2. [Google Scholar] [CrossRef]
- Cantwell, N.; Davidson, J.; Elsley, S.; Milligan, I.; Quinn, N. Moving Forward: Implementing the ‘Guidelines for the Alternative Care of Children’; Centre for Excellence for Looked After Children in Scotland: Glasgow, UK, 2012. [Google Scholar]
- United Nations General Assembly. Guidelines for the Alternative Care of Children; United Nations General Assembly: New York, NY, USA, 2010. [Google Scholar]
- Lukaszyk, C.; Ivers, R.Q.; Jagnoor, J. Systematic review of drowning in India: Assessment of burden and risk. Inj. Prev. 2018, 24, 451–458. [Google Scholar] [CrossRef]
- Harvey, B.; Stuart, J.; Swan, T. Evaluation of a Drama-in-Education Programme to Increase AIDS Awareness in South African High Schools: A Randomized Community Intervention Trial. Int. J. STD AIDS 2000, 11, 105–111. [Google Scholar] [CrossRef] [PubMed]
- Gielen, A.C.; Sleet, D. Application of Behavior-Change Theories and Methods to Injury Prevention. Epidemiol. Rev. 2003, 25, 65–76. [Google Scholar] [CrossRef] [PubMed]
- Tankard, M.E.; Paluck, E.L. Norm Perception as a Vehicle for Social Change. Soc. Issues Policy Rev. 2016, 10, 181–211. [Google Scholar] [CrossRef]
- Ryan, R.M.; Patrick, H.; Deci, E.L.; Williams, G.C. Facilitating health behaviour change and its maintenance: Interventions based on self-determination theory. Eur. Health Psychol. 2008, 10, 2–5. [Google Scholar]
- Kwasnicka, D.; Dombrowski, S.U.; White, M.; Sniehotta, F. Theoretical explanations for maintenance of behaviour change: A systematic review of behaviour theories. Health Psychol. Rev. 2016, 10, 277–296. [Google Scholar] [CrossRef] [PubMed]
- Ved, R.; Scott, K.; Gupta, G.; Ummer, O.; Singh, S.; Srivastava, A.; George, A.S. How are gender inequalities facing India’s one million ASHAs being addressed? Policy origins and adaptations for the world’s largest all-female community health worker programme. Hum. Resour. Health 2019, 17, 3. [Google Scholar] [CrossRef]
- Mondal, N.; Murhekar, M.V. Factors associated with low performance of Accredited Social Health Activist (ASHA) regarding maternal care in Howrah district, West Bengal, 2015–16: An unmatched case control study. Clin. Epidemiol. Global Health 2018, 6, 21–28. [Google Scholar] [CrossRef]
- Frieden, T.R. Six Components Necessary for Effective Public Health Program Implementation. Am. J. Public Health 2013, 104, 17–22. [Google Scholar] [CrossRef] [PubMed]
- Abimbola, S. Beyond positive a priori bias: Reframing community engagement in LMICs. Health Promot. Int. 2019, 35, 598–609. [Google Scholar] [CrossRef] [PubMed]
- Bardhan, P.; Mookherjee, D. Pro-poor targeting and accountability of local governments in West Bengal. J. Dev. Econ. 2006, 79, 303–327. [Google Scholar] [CrossRef]
- Odugleh-Koleva, A.; Parrish-Sprowl, J. Universal health coverage and community engagement. Bull. World Health Organ. 2018, 96, 589–664. [Google Scholar] [CrossRef] [PubMed]
- Kok, M.C.; Broerse, J.E.W.; Theobald, S.; Ormel, H.; Dieleman, M.; Taegtmeyer, M. Performance of community health workers: Situating their intermediary position within complex adaptive health systems. Human Resour. Health 2017, 15, 59. [Google Scholar] [CrossRef] [PubMed]
- El Arifeen, S.; Christou, A.; Reichenbach, L.; Osman, F.A.; Azad, K.; Islam, K.S.; Ahmed, F.; Perry, H.B.; Peters, D.H. Community-based approaches and partnerships: Innovations in health-service delivery in Bangladesh. Lancet 2013, 382, 2012. [Google Scholar] [CrossRef]
- Bertone, M.P.; Lagarde, M.; Witter, S. Performance-based financing in the context of the complex remuneration of health workers: Findings from a mixed-method study in rural Sierra Leone. BMC Health Serv. Res. 2016, 16, 286. [Google Scholar] [CrossRef]
- Bracht, N.; Finnegan, J.R., Jr.; Rissel, C.; Weisbrod, R.; Gleaso, J.; Corbett, J.; Veblen-Mortenson, S. Community ownership and program continuation following a health demonstration project. Health Educ. Res. 1994, 9, 243–255. [Google Scholar] [CrossRef]
- Branche, C.; Ozanne-Smith, J.; Oyebite, K.; Hyder, A.A. World Report on Child Injury Prevention; World Health Organization: Geneva, Switzerland, 2008. [Google Scholar]
- Violano, P.; Davis, K.A.; Lane, V.; Lofthouse, R.; Carusone, C. Establishing an Injury Prevention Program to Address Pediatric Pedestrian Collisions. J. Trauma Nurs. 2009, 16, 216–219. [Google Scholar] [CrossRef]
- Cornwall, A.; Jewkes, R. What is participatory research? Soc. Sci. Med. 1995, 41, 1667–1676. [Google Scholar] [CrossRef]
- Douthwaite, B.; Beaulieu, N.; Lundy, M.; Peters, D. Understanding how participatory approaches foster innovation. Int. J. Agric. Sustain. 2009, 7, 42–60. [Google Scholar] [CrossRef]
- Thomas-Slayter, B. Participatory Approaches to Community Change: Building Cooperation through Dialogue and Negotiation Using Participatory Rural Appraisal. In Handbook on Building Cultures of Peace; De Rivera, J., Ed.; Springer: New York, NY, USA, 2009; pp. 333–348. [Google Scholar]

Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2020 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Gupta, M.; Roy, S.; Panda, R.; Konwar, P.; Jagnoor, J. Interventions for Child Drowning Reduction in the Indian Sundarbans: Perspectives from the Ground. Children 2020, 7, 291. https://doi.org/10.3390/children7120291
Gupta M, Roy S, Panda R, Konwar P, Jagnoor J. Interventions for Child Drowning Reduction in the Indian Sundarbans: Perspectives from the Ground. Children. 2020; 7(12):291. https://doi.org/10.3390/children7120291
Chicago/Turabian StyleGupta, Medhavi, Sujoy Roy, Ranjan Panda, Pompy Konwar, and Jagnoor Jagnoor. 2020. "Interventions for Child Drowning Reduction in the Indian Sundarbans: Perspectives from the Ground" Children 7, no. 12: 291. https://doi.org/10.3390/children7120291
APA StyleGupta, M., Roy, S., Panda, R., Konwar, P., & Jagnoor, J. (2020). Interventions for Child Drowning Reduction in the Indian Sundarbans: Perspectives from the Ground. Children, 7(12), 291. https://doi.org/10.3390/children7120291





