Cognitive Assessment and Rehabilitation for Pediatric-Onset Multiple Sclerosis: A Scoping Review
Abstract
1. Introduction
2. Materials and Methods
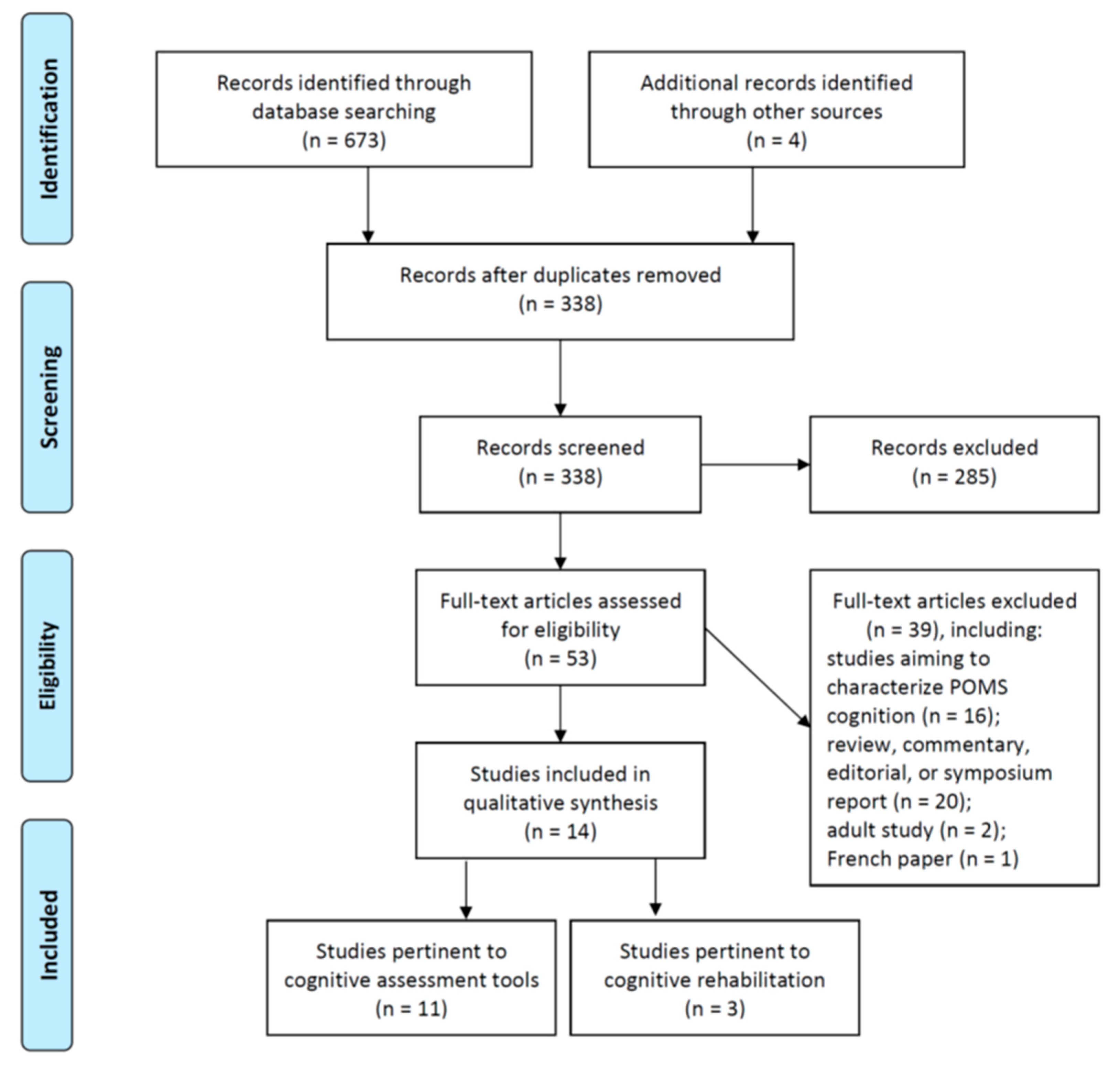
2.1. Literature Search, Screening, and Selection
2.2. Data Charting
3. Results
3.1. Original Studies Evaluating Cognitive Assessment Tools for Pediatric MS
3.2. Original Studies Evaluating Cognitive Rehabilitation for POMS
3.3. Registered Clinical Trials Primarily Focusing on Cognitive Issues in POMS
4. Discussions
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Conflicts of Interest
References
- Waldman, A.; Ness, J.; Pohl, D.; Simone, I.L.; Anlar, B.; Amato, M.P.; Ghezzi, A. Pediatric multiple sclerosis: Clinical features and outcome. Neurology 2016, 87, S74–S81. [Google Scholar] [CrossRef] [PubMed]
- Carotenuto, A.; Moccia, M.; Costabile, T.; Signoriello, E.; Paolicelli, D.; Simone, M.; Lus, G.; Brescia Morra, V.; Lanzillo, R. Associations between cognitive impairment at onset and disability accrual in young people with multiple sclerosis. Sci. Rep. 2019, 9, 18074. [Google Scholar] [CrossRef] [PubMed]
- Wallach, A.I.; Waltz, M.; Casper, T.C.; Aaen, G.; Belman, A.; Benson, L.; Chitnis, T.; Gorman, M.; Graves, J.; Harris, Y.; et al. Cognitive processing speed in pediatric-onset multiple sclerosis: Baseline characteristics of impairment and prediction of decline. Mult. Scler. 2019. [Google Scholar] [CrossRef] [PubMed]
- Julian, L.; Serafin, D.; Charvet, L.; Ackerson, J.; Benedict, R.; Braaten, E.; Brown, T.; O’Donnell, E.; Parrish, J.; Preston, T.; et al. Cognitive impairment occurs in children and adolescents with multiple sclerosis: Results from a United States network. J. Child Neurol. 2013, 28, 102–107. [Google Scholar] [CrossRef]
- Johnen, A.; Elpers, C.; Riepl, E.; Landmeyer, N.C.; Kramer, J.; Polzer, P.; Lohmann, H.; Omran, H.; Wiendl, H.; Gobel, K.; et al. Early effective treatment may protect from cognitive decline in paediatric multiple sclerosis. Eur. J. Paediatr. Neurol. 2019, 23, 783–791. [Google Scholar] [CrossRef]
- Wuerfel, E.; Weddige, A.; Hagmayer, Y.; Jacob, R.; Wedekind, L.; Stark, W.; Gartner, J. Cognitive deficits including executive functioning in relation to clinical parameters in paediatric MS patients. PLoS ONE 2018, 13, e0194873. [Google Scholar] [CrossRef]
- Brenton, J.N.; Koshiya, H.; Woolbright, E.; Goldman, M.D. The Multiple Sclerosis Functional Composite and Symbol Digit Modalities Test as outcome measures in pediatric multiple sclerosis. Mult. Scler. J. Exp. Transl. Clin. 2019, 5, 2055217319846141. [Google Scholar] [CrossRef]
- Kapanci, T.; Rostasy, K.; Hausler, M.G.; Geis, T.; Schimmel, M.; Elpers, C.; Kreth, J.H.; Thiels, C.; Troche, S.J. Evaluating the relationship between psychometric intelligence and cognitive functions in paediatric multiple sclerosis. Mult. Scler. J. Exp. Transl. Clin. 2019, 5, 2055217319894365. [Google Scholar] [CrossRef]
- Amato, M.P.; Goretti, B.; Ghezzi, A.; Hakiki, B.; Niccolai, C.; Lori, S.; Moiola, L.; Falautano, M.; Viterbo, R.G.; Patti, F.; et al. Neuropsychological features in childhood and juvenile multiple sclerosis: Five-year follow-up. Neurology 2014, 83, 1432–1438. [Google Scholar] [CrossRef]
- Charvet, L.E.; O’Donnell, E.H.; Belman, A.L.; Chitnis, T.; Ness, J.M.; Parrish, J.; Patterson, M.; Rodriguez, M.; Waubant, E.; Weinstock-Guttman, B.; et al. Longitudinal evaluation of cognitive functioning in pediatric multiple sclerosis: Report from the US Pediatric Multiple Sclerosis Network. Mult. Scler. 2014, 20, 1502–1510. [Google Scholar] [CrossRef]
- Arksey, H.; O’Malley, L. Scoping studies: Towards a methodological framework. Int. J. Soc. Res. Methodol. 2005, 8, 19–32. [Google Scholar] [CrossRef]
- Tricco, A.C.; Lillie, E.; Zarin, W.; O’Brien, K.K.; Colquhoun, H.; Levac, D.; Moher, D.; Peters, M.D.J.; Horsley, T.; Weeks, L.; et al. PRISMA Extension for Scoping Reviews (PRISMA-ScR): Checklist and Explanation. Ann. Intern Med. 2018, 169, 467–473. [Google Scholar] [CrossRef] [PubMed]
- Portaccio, E.; Goretti, B.; Lori, S.; Zipoli, V.; Centorrino, S.; Ghezzi, A.; Patti, F.; Bianchi, V.; Comi, G.; Trojano, M.; et al. The brief neuropsychological battery for children: A screening tool for cognitive impairment in childhood and juvenile multiple sclerosis. Mult. Scler. 2009, 15, 620–626. [Google Scholar] [CrossRef] [PubMed]
- Falco, F.; Moccia, M.; Chiodi, A.; Carotenuto, A.; D’Amelio, A.; Rosa, L.; Piscopo, K.; Falco, A.; Costabile, T.; Lauro, F.; et al. Normative values of the Rao’s Brief Repeatable Battery in an Italian young adolescent population: The influence of age, gender, and education. Neurol. Sci. 2019, 40, 713–717. [Google Scholar] [CrossRef]
- Smerbeck, A.M.; Parrish, J.; Yeh, E.A.; Hoogs, M.; Krupp, L.B.; Weinstock-Guttman, B.; Benedict, R.H. Regression-based pediatric norms for the brief visuospatial memory test: Revised and the symbol digit modalities test. Clin. Neuropsychol. 2011, 25, 402–412. [Google Scholar] [CrossRef] [PubMed]
- Smerbeck, A.M.; Parrish, J.; Yeh, E.A.; Weinstock-Guttman, B.; Hoogs, M.; Serafin, D.; Krupp, L.; Benedict, R.H. Regression-based norms improve the sensitivity of the National MS Society Consensus Neuropsychological Battery for Pediatric Multiple Sclerosis (NBPMS). Clin. Neuropsychol. 2012, 26, 985–1002. [Google Scholar] [CrossRef] [PubMed]
- Bigi, S.; Marrie, R.A.; Till, C.; Yeh, E.A.; Akbar, N.; Feinstein, A.; Banwell, B.L. The computer-based Symbol Digit Modalities Test: Establishing age-expected performance in healthy controls and evaluation of pediatric MS patients. Neurol. Sci. 2017, 38, 635–642. [Google Scholar] [CrossRef]
- Charvet, L.E.; Beekman, R.; Amadiume, N.; Belman, A.L.; Krupp, L.B. The Symbol Digit Modalities Test is an effective cognitive screen in pediatric onset multiple sclerosis (MS). J. Neurol. Sci. 2014, 341, 79–84. [Google Scholar] [CrossRef]
- Charvet, L.E.; Shaw, M.; Frontario, A.; Langdon, D.; Krupp, L.B. Cognitive impairment in pediatric-onset multiple sclerosis is detected by the Brief International Cognitive Assessment for Multiple Sclerosis and computerized cognitive testing. Mult. Scler. 2018, 24, 512–519. [Google Scholar] [CrossRef]
- Smerbeck, A.M.; Parrish, J.; Serafin, D.; Yeh, E.A.; Weinstock-Guttman, B.; Hoogs, M.; Krupp, L.B.; Benedict, R.H. Visual-cognitive processing deficits in pediatric multiple sclerosis. Mult. Scler. 2011, 17, 449–456. [Google Scholar] [CrossRef]
- Storm Van’s Gravesande, K.; Calabrese, P.; Blaschek, A.; Rostasy, K.; Huppke, P.; Rothe, L.; Mall, V.; Kessler, J.; Kalbe, E. The Multiple Sclerosis Inventory of Cognition for Adolescents (MUSICADO): A brief screening instrument to assess cognitive dysfunction, fatigue and loss of health-related quality of life in pediatric-onset multiple sclerosis. Eur. J. Paediatr. Neurol. 2019, 23, 792–800. [Google Scholar] [CrossRef] [PubMed]
- Hubacher, M.; DeLuca, J.; Weber, P.; Steinlin, M.; Kappos, L.; Opwis, K.; Penner, I.K. Cognitive rehabilitation of working memory in juvenile multiple sclerosis-effects on cognitive functioning, functional MRI and network related connectivity. Restor. Neurol. Neurosci. 2015, 33, 713–725. [Google Scholar] [CrossRef] [PubMed]
- Till, C.; Kuni, B.; De Somma, E.; Yeh, E.A.; Banwell, B. A feasibility study of working memory training for individuals with paediatric-onset multiple sclerosis. Neuropsychol. Rehabil. 2019, 29, 1177–1192. [Google Scholar] [CrossRef] [PubMed]
- Simone, M.; Viterbo, R.G.; Margari, L.; Iaffaldano, P. Computer-assisted rehabilitation of attention in pediatric multiple sclerosis and ADHD patients: A pilot trial. BMC Neurol. 2018, 18, 82. [Google Scholar] [CrossRef] [PubMed]
- Brandstadter, R.; Katz Sand, I.; Sumowski, J.F. Beyond rehabilitation: A prevention model of reserve and brain maintenance in multiple sclerosis. Mult. Scler. 2019, 25, 1372–1378. [Google Scholar] [CrossRef] [PubMed]
- Kalb, R.; Beier, M.; Benedict, R.H.; Charvet, L.; Costello, K.; Feinstein, A.; Gingold, J.; Goverover, Y.; Halper, J.; Harris, C.; et al. Recommendations for cognitive screening and management in multiple sclerosis care. Mult. Scler. 2018, 24, 1665–1680. [Google Scholar] [CrossRef] [PubMed]
- Margoni, M.; Rinaldi, F.; Riccardi, A.; Franciotta, S.; Perini, P.; Gallo, P. No evidence of disease activity including cognition (NEDA-3 plus) in naive pediatric multiple sclerosis patients treated with natalizumab. J. Neurol. 2020, 267, 100–105. [Google Scholar] [CrossRef]
- Duignan, S.; Brownlee, W.; Wassmer, E.; Hemingway, C.; Lim, M.; Ciccarelli, O.; Hacohen, Y. Paediatric multiple sclerosis: A new era in diagnosis and treatment. Dev. Med. Child Neurol. 2019, 61, 1039–1049. [Google Scholar] [CrossRef]
- Amato, M.P.; Morra, V.B.; Falautano, M.; Ghezzi, A.; Goretti, B.; Patti, F.; Riccardi, A.; Mattioli, F. Cognitive assessment in multiple sclerosis-an Italian consensus. Neurol. Sci. 2018, 39, 1317–1324. [Google Scholar] [CrossRef]
- Amato, M.P.; Goretti, B.; Ghezzi, A.; Lori, S.; Zipoli, V.; Portaccio, E.; Moiola, L.; Falautano, M.; De Caro, M.F.; Lopez, M.; et al. Cognitive and psychosocial features of childhood and juvenile MS. Neurology 2008, 70, 1891–1897. [Google Scholar] [CrossRef]
- Bartlett, E.; Shaw, M.; Schwarz, C.; Feinberg, C.; DeLorenzo, C.; Krupp, L.B.; Charvet, L.E. Brief Computer-Based Information Processing Measures are Linked to White Matter Integrity in Pediatric-Onset Multiple Sclerosis. J. Neuroimaging 2019, 29, 140–150. [Google Scholar] [CrossRef] [PubMed]
- Amato, M.P.; Goretti, B.; Ghezzi, A.; Lori, S.; Zipoli, V.; Moiola, L.; Falautano, M.; De Caro, M.F.; Viterbo, R.; Patti, F.; et al. Cognitive and psychosocial features in childhood and juvenile MS: Two-year follow-up. Neurology 2010, 75, 1134–1140. [Google Scholar] [CrossRef] [PubMed]
- Benedict, R.H.; Amato, M.P.; Boringa, J.; Brochet, B.; Foley, F.; Fredrikson, S.; Hamalainen, P.; Hartung, H.; Krupp, L.; Penner, I.; et al. Brief International Cognitive Assessment for MS (BICAMS): International standards for validation. BMC Neurol. 2012, 12, 55. [Google Scholar] [CrossRef] [PubMed]
- Filser, M.; Schreiber, H.; Pottgen, J.; Ullrich, S.; Lang, M.; Penner, I.K. The Brief International Cognitive Assessment in Multiple Sclerosis (BICAMS): Results from the German validation study. J. Neurol. 2018, 265, 2587–2593. [Google Scholar] [CrossRef]
- Toussaint-Duyster, L.C.; Wong, Y.Y.M.; Van der Cammen-van Zijp, M.H.; Van Pelt-Gravesteijn, D.; Catsman-Berrevoets, C.E.; Hintzen, R.Q.; Neuteboom, R.F. Fatigue and physical functioning in children with multiple sclerosis and acute disseminated encephalomyelitis. Mult. Scler. 2018, 24, 982–990. [Google Scholar] [CrossRef]
- Amato, M.P.; Krupp, L.B.; Charvet, L.E.; Penner, I.; Till, C. Pediatric multiple sclerosis: Cognition and mood. Neurology 2016, 87, S82–S87. [Google Scholar] [CrossRef]
- MacAllister, W.S.; Christodoulou, C.; Troxell, R.; Milazzo, M.; Block, P.; Preston, T.E.; Bender, H.A.; Belman, A.; Krupp, L.B. Fatigue and quality of life in pediatric multiple sclerosis. Mult. Scler. 2009, 15, 1502–1508. [Google Scholar] [CrossRef]
- Aaen, G.; Waltz, M.; Vargas, W.; Makhani, N.; Ness, J.; Harris, Y.; Casper, T.C.; Benson, L.; Candee, M.; Chitnis, T.; et al. Acquisition of Early Developmental Milestones and Need for Special Education Services in Pediatric Multiple Sclerosis. J. Child Neurol. 2019, 34, 148–152. [Google Scholar] [CrossRef]
- Mazerolle, E.L.; Wojtowicz, M.A.; Omisade, A.; Fisk, J.D. Intra-individual variability in information processing speed reflects white matter microstructure in multiple sclerosis. Neuroimage Clin. 2013, 2, 894–902. [Google Scholar] [CrossRef]
- Harand, C.; Daniel, F.; Mondou, A.; Chevanne, D.; Creveuil, C.; Defer, G. Neuropsychological management of multiple sclerosis: Evaluation of a supervised and customized cognitive rehabilitation program for self-used at home (SEPIA): Protocol for a randomized controlled trial. Trials 2019, 20, 614. [Google Scholar] [CrossRef]
- Nauta, I.M.; Speckens, A.E.M.; Kessels, R.P.C.; Geurts, J.J.G.; de Groot, V.; Uitdehaag, B.M.J.; Fasotti, L.; de Jong, B.A. Cognitive rehabilitation and mindfulness in multiple sclerosis (REMIND-MS): A study protocol for a randomised controlled trial. BMC Neurol. 2017, 17, 201. [Google Scholar] [CrossRef] [PubMed]
- Hulst, H.E.; Langdon, D.W. Functional training is a senseless strategy in MS cognitive rehabilitation: Strategy training is the only useful approach—NO. Mult. Scler. 2017, 23, 930–932. [Google Scholar] [CrossRef] [PubMed]
- Leavitt, V.M. Functional training is a senseless strategy in MS cognitive rehabilitation: Strategy training is the only useful approach—YES. Mult. Scler. 2017, 23, 928–929. [Google Scholar] [CrossRef] [PubMed]
- Chiaravalloti, N.D.; Genova, H.M.; DeLuca, J. Cognitive rehabilitation in multiple sclerosis: The role of plasticity. Front. Neurol. 2015, 6, 67. [Google Scholar] [CrossRef] [PubMed]
- Charvet, L.E.; Cleary, R.E.; Vazquez, K.; Belman, A.L.; Krupp, L.B. Social cognition in pediatric-onset multiple sclerosis (MS). Mult. Scler. 2014, 20, 1478–1484. [Google Scholar] [CrossRef] [PubMed]
- Ekmekci, O. Pediatric Multiple Sclerosis and Cognition: A Review of Clinical, Neuropsychologic, and Neuroradiologic Features. Behav. Neurol. 2017, 2017, 1463570. [Google Scholar] [CrossRef] [PubMed]
- Lubans, D.; Richards, J.; Hillman, C.; Faulkner, G.; Beauchamp, M.; Nilsson, M.; Kelly, P.; Smith, J.; Raine, L.; Biddle, S. Physical Activity for Cognitive and Mental Health in Youth: A Systematic Review of Mechanisms. Pediatrics 2016, 138. [Google Scholar] [CrossRef] [PubMed]
- Yeh, E.A.; Kinnett-Hopkins, D.; Grover, S.A.; Motl, R.W. Physical activity and pediatric multiple sclerosis: Developing a research agenda. Mult. Scler. 2015, 21, 1618–1625. [Google Scholar] [CrossRef]
- Sandroff, B.M.; Pilutti, L.A.; Benedict, R.H.; Motl, R.W. Association between physical fitness and cognitive function in multiple sclerosis: Does disability status matter? Neurorehabil. Neural Repair 2015, 29, 214–223. [Google Scholar] [CrossRef]
| Author (Year) | Test/Battery | Participants | Subtests and Targeted Cognitive Domains | Main Findings and/or Additional Notes |
|---|---|---|---|---|
| Portaccio et al. (2009) [13] | Brief Neuropsychological Battery for Children (BNBC) | 61 POMS (age 8.8–17.9 years),58 matched HC |
|
|
| Smerbeck et al. (2011) [15] | Brief Visuospatial Memory Test–Revised (BVMTR) | 51 POMS, 4 with ADEM, 92 HC (age 6–17) |
|
|
| SDMT (oral version) | 22 POMS, 3 with ADEM, 92 HC (age 6–17) |
| ||
| Smerbeck et al. (2011) [20] | Brief Visuospatial Memory Test–revised (BVMTR) | 43 POMS (age 9–18), 43 HC (age 9–18) |
|
|
| SDMT (oral version) | 20 POMS (age 9–18), 20 HC (age 8–18) |
|
| |
| Smerbeck et al. (2012) [16] | National MS Society Consensus Neuropsychological Battery for Pediatric Multiple Sclerosis (NBPMS) | 51 POMS (age 9–18), 102 HC (age 5–18) |
|
|
| Charvet et al. (2014) [18] | Symbol Digit Modalities Test (SDMT, oral version) | 70 POMS (70 underwent SDMT, 31 underwent neuropsychological testing), 40 other pediatric neurological diagnoses, 32 HC (note: significant difference in racial distribution between MS and HC) |
|
|
| Bigi et al. (2017) [17] | Computer-Based Symbol Digit Modalities Test (c-SDMT) | 27 POMS (22 female, 81.5%; age 8–18 years), 478 HC (237 female, 49.5%) |
|
|
| Charvet et al. (2018) [19] | Brief International Cognitive Assessment for Multiple Sclerosis battery (BICAMS) | 69 POMS (7–21 years), 66 HC (8–21 years) |
|
|
| Cogstate Brief Battery | 67 POMS, 48 HC | Three speeded processing tasks:
|
| |
| Kapanci et al. (2019) [8] | See subtests column (the study examined the interrelationships of tests tapping processing speed, working memory, and intelligence) | 21 POMS, 21 matched HC |
|
|
| Brenton et al. (2019) [7] | See subtests column | 20 POMS, 40 matched HC |
|
|
| Falco et al. (2019) [14] | Rao’s Brief Repeatable Battery (BRB) | 76 HC (age 14–17) |
|
|
| Storm Van’s Gravesande et al. (2019) [21] | Multiple Sclerosis Inventory of Cognition for Adolescents (MUSICADO) | 106 POMS (age 12–18 years), 210 HC |
|
|
| Author (Year) | Intervention (Duration and Frequency) | Supervision or Coaching | Targeted Cognitive Domain | Study Participants | Comparator Group | Outcome Measures |
|---|---|---|---|---|---|---|
| Hubacher et al. (2015) [22] | computerized training (BrainStim) for 4 weeks (45 min/session, 4 times/week) | supervised by a psychologist once per week | working memory (visuospatial and verbal) | 5 juvenile MS patients (age 12–17 years; 3 females) | Absent | Cognitive measures: working memory (visuospatial and verbal) and attention (alertness) |
| Simone et al. (2018) [24] | computerized training for 3 months (1 h/session, twice/week) | a psychologist called patients every week and met patients and their caregiver/parent every month | attention | 16 POMS patients (age 15.75 ± 1.74 years; 9 females) | Present (nonspecific training) | Neuropsychological performance (using elaborate test battery) |
| Till et al. (2019) [23] | web-based training (Cogmed™) for 5 weeks (<1 h/session, 5 d/week) | weekly telephone support by a trained Cogmed™ Coach | working memory (visuospatial and verbal) | 9 POMS patients (age 19.3 ± 4.1 years; 6 females) | Absent | Feasibility measures: adherence and tolerance; Cognitive measures: working memory, processing speed, visuospatial judgment |
| Author (Year) | Intervention | Effects on Targeted or Related Cognitive Domains | Far Transfer Effect | Sustainability of Effect | Factors Associated with Training Response, and Additional Notes |
|---|---|---|---|---|---|
| Hubacher et al. (2015) [22] | computerized training (BrainStim) for 4 weeks (45 min/session, 4 times/week) | Two (of 5) were responders; both responders showed better WM (visuospatial and verbal), processing speed, and alertness. | Not assessed | Sustained behavioral response at 9 months in both responders | Disease activity and general intelligence may be factors associated with training response. |
| Simone et al. (2018) [24] | computerized training for 3 months (1 h/session, twice/week) | Improved attention, processing speed, and WM. | Improved executive function and visuospatial memory | NA | Not reported |
| Till et al. (2019) [23] | web-based training (Cogmed™) for 5 weeks (<1 h/session, 5 d/week) | Subjective: 8 (out of 9) reported improvement in WM; Objective: medium to large effect size on neuropsychological measures of WM. | Limited | NA | Indicators of feasibility: 6/9 adherence; 8/9 tolerance. The participant who showed the least improvement had the youngest age at disease onset, longest disease duration, highest number of relapses, and lowest normalized brain volume. The participant who did not tolerate the training had the lowest IQ. |
| ClinicalTrials.Gov Identifier | NCT03066752 | NCT03190902 | NCT03933020 |
|---|---|---|---|
| Aim | To study the neural mechanisms underlying cognitive dysfunction | To assess the efficacy of a computerized program for retraining attention | To assess the cognitive impact of a home-based virtual reality videogame exercise program |
| Study period | March~November 2017 | September 2015~April 2016 | May 2019~June 2020 |
| Study type | Observational | Interventional | Interventional |
| Trial design | Prospective case-control | Double blind, randomized clinical trial | Single blind, randomized clinical trial |
| Ages eligible for study | 6~18 years | up to 17 years | 15~25 years |
| Recruitment status | Completed | Completed | Recruiting |
| Enrollment | 10 cases, 10 controls (actual) | 8 cases, 8 controls (actual) | 12 cases, 12 controls (estimated) |
| Principal investigator | E. Ann Yeh | Pietro Iaffaldano | Stephanie Garcia-Tarodo |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2020 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Lin, W.-S.; Lin, S.-J.; Hsu, T.-R. Cognitive Assessment and Rehabilitation for Pediatric-Onset Multiple Sclerosis: A Scoping Review. Children 2020, 7, 183. https://doi.org/10.3390/children7100183
Lin W-S, Lin S-J, Hsu T-R. Cognitive Assessment and Rehabilitation for Pediatric-Onset Multiple Sclerosis: A Scoping Review. Children. 2020; 7(10):183. https://doi.org/10.3390/children7100183
Chicago/Turabian StyleLin, Wei-Sheng, Shan-Ju Lin, and Ting-Rong Hsu. 2020. "Cognitive Assessment and Rehabilitation for Pediatric-Onset Multiple Sclerosis: A Scoping Review" Children 7, no. 10: 183. https://doi.org/10.3390/children7100183
APA StyleLin, W.-S., Lin, S.-J., & Hsu, T.-R. (2020). Cognitive Assessment and Rehabilitation for Pediatric-Onset Multiple Sclerosis: A Scoping Review. Children, 7(10), 183. https://doi.org/10.3390/children7100183





