Stakeholder Engagement in Developing an Electronic Clinical Support Tool for Tobacco Prevention in Adolescent Primary Care
Abstract
:1. Introduction
2. Methods
2.1. Research Setting
2.2. Stakeholders
2.3. The Citizen Scientist Program
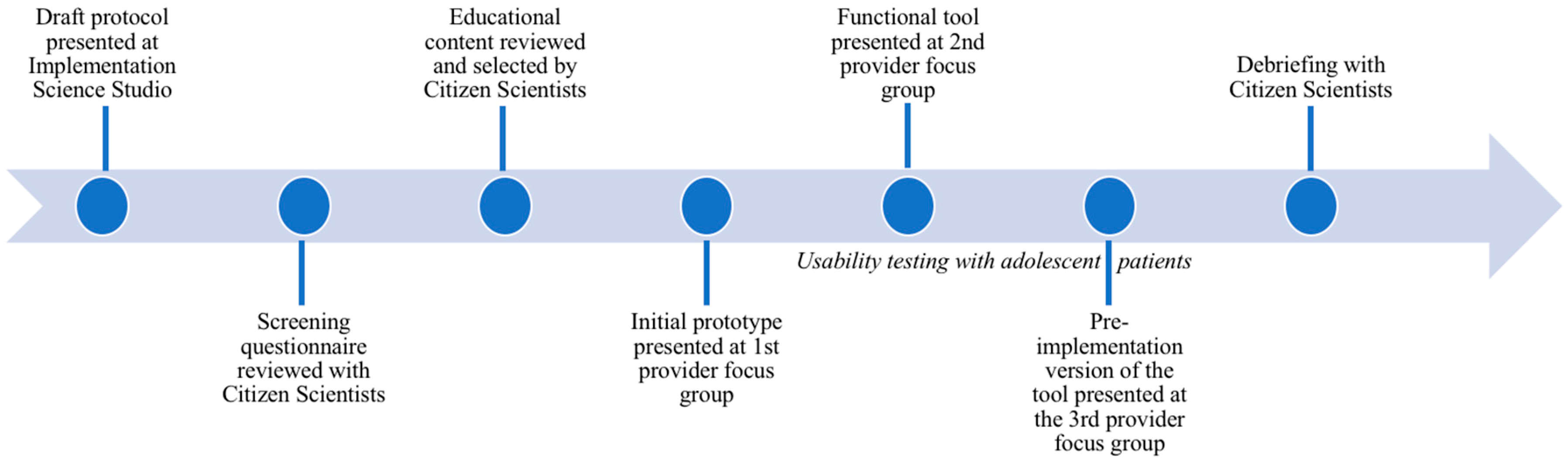
2.4. Step 1: Implementation Science Studio
2.5. Step 2: Consultations with Citizen Scientists
2.6. Step 3: Provider Focus Group Discussions
2.7. Step 4: Patient Interviews
2.8. Step 5: Citizen Scientist Debriefing
2.9. Data Analysis
3. Results
3.1. Intervention Characteristics
3.2. Implementation Science Studio and Citizen Scientist Contributions
3.3. Focus Group Findings
“There could be potentially an office policy that says, ‘This patient is going to go into this room, fills this out.’ And have them do a survey in that area as they are checking in. That could potentially work. But, if we are doing it at the point where the nurses are already with everyone, there could be a pretty big disruption in flow.”
“I think that’s the wave of the future. Why are we filling out forms? They fill out the same thing time and time again. A patient writes on the form, checks these things off, and then I take what they wrote and I type it into the computer... I’m repeating unnecessary work. Wouldn’t it be more efficient it they could type it in? It automatically goes to [the patient portal], automatically populates here every time.”
“I truly see that as an advantage of your process… I think that adolescents are going to feel like their privacy is better protected if they can [do it] on their iPhone, their iPad, or at home prior to the clinic visit. Enter this data, but be reassured and know that it’s going to be protected and kept away from their parent.”
3.4. Patient Interview Findings
“The questions were about teens, which is okay. And then we were asked about the family on the survey. I liked it because it shows how smoking could come from the family members around you. You’re seeing it everywhere you go.”
“Some teenagers, they feel like they don’t want to write so honestly. It all depends on the teenager… They’re not supposed to be doing stuff like that. They’re not supposed to be using tobacco or anything. They’re probably afraid that the person they’re talking to would go tell their parents or something.”
3.5. Debrief Findings
4. Discussion
Supplementary Materials
Author Contributions
Funding
Conflicts of Interest
References
- Moyer, V.A. Primary care interventions to prevent tobacco use in children and adolescents: U.S. Preventive Services Task Force recommendation statement. Ann. Intern. Med. 2013, 159, 552–557. [Google Scholar] [PubMed]
- Patnode, C.D.; O’Connor, E.; Whitlock, E.P.; Perdue, L.A.; Soh, C.; Hollis, J. Primary care-relevant interventions for tobacco use prevention and cessation in children and adolescents: A systematic evidence review for the U.S. Preventive Services Task Force. Ann. Intern. Med. 2013, 158, 253–260. [Google Scholar] [CrossRef] [PubMed]
- Ackard, D.M.; Neumark-Sztainer, D. Health care information sources for adolescents: Age and gender differences on use, concerns, and needs. J. Adolesc. Health 2001, 29, 170–176. [Google Scholar] [CrossRef]
- Marcell, A.V.; Halpern-Felsher, B.L. Adolescents’ health beliefs are critical in their intentions to seek physician care. Prev. Med. (Baltim.) 2005, 41, 118–125. [Google Scholar] [CrossRef] [PubMed]
- Winickoff, J.P.; Tanski, S.E.; McMillen, R.C.; Hipple, B.J.; Friebely, J.; Healey, E.A. A national survey of the acceptability of quitlines to help parents quit smoking. Pediatrics 2006, 117, e695–e700. [Google Scholar] [CrossRef] [PubMed]
- Winickoff, J.P.; Tanski, S.E.; McMillen, R.C.; Ross, K.M.; Lipstein, E.A.; Hipple, B.J.; Friebely, J.; Klein, J.D. Acceptability of testing children for tobacco-smoke exposure: A national parent survey. Pediatrics 2011, 127, 628–634. [Google Scholar] [CrossRef] [PubMed]
- Pbert, L.; Farber, H.; Horn, K.; Lando, H.A.; Muramoto, M.; O’Loughlin, J.; Tanski, S.; Wellman, R.J.; Winickoff, J.P.; Klein, J.D.; et al. State-of-the-art office-based interventions to eliminate youth tobacco use: The past decade. Pediatrics 2015, 135, 734–747. [Google Scholar] [CrossRef] [PubMed]
- Tanski, S.E.; Klein, J.D.; Winickoff, J.P.; Auinger, P.; Weitzman, M. Tobacco counseling at well-child and tobacco-influenced illness visits: Opportunities for improvement. Pediatrics 2003, 111, E162–E167. [Google Scholar] [CrossRef] [PubMed]
- Zapka, J.G.; Fletcher, K.; Pbert, L.; Druker, S.K.; Ockene, J.K.; Chen, L. The perceptions and practices of pediatricians: Tobacco intervention. Pediatrics 1999, 103, e65. [Google Scholar] [CrossRef] [PubMed]
- Arrazola, R.A.; Singh, T.; Corey, C.G.; Husten, C.G.; Neff, L.J.; Apelberg, B.J.; Bunnell, R.E.; Choiniere, C.J.; King, B.A.; Cox, S.; et al. Tobacco Use among Middle and High School Students—United States, 2011–2015. MMWR Morb. Mortal. Wkly. Rep. 2016, 65, 361–367. [Google Scholar] [CrossRef]
- US Department of Health and Human Services. The Health Consequences of Smoking: 50 Years of Progress. A Report of the Surgeon General; US Department of Health and Human Services, Centers for Disease Control and Prevention, National Center for Chronic Disease Prevention and Health Promotion, Office on Smoking and Health: Atlanta, GA, USA, 2014.
- Von Soest, T.; Pedersen, W. Hardcore adolescent smokers? An examination of the hardening hypothesis by using survey data from two Norwegian samples collected eight years apart. Nicotine Tob. Res. 2014, 16. [Google Scholar] [CrossRef] [PubMed]
- Colby, S.M.; Monti, P.M.; Barnett, N.P.; Rohsenow, D.J.; Weissman, K.; Spirito, A.; Woolard, R.H.; Lewander, W.J. Brief motivational interviewing in a hospital setting for adolescent smoking: A preliminary study. J. Consult. Clin. Psychol. 1998, 66, 574–578. [Google Scholar] [CrossRef] [PubMed]
- Colby, S.M.; Monti, P.M.; O’Leary Tevyaw, T.; Barnett, N.P.; Spirito, A.; Rohsenow, D.J.; Riggs, S.; Lewander, W. Brief motivational intervention for adolescent smokers in medical settings. Addict. Behav. 2005, 30, 865–874. [Google Scholar] [CrossRef] [PubMed]
- Zhao, X.; Alexander, T.N.; Hoffman, L.; Jones, C.; Delahanty, J.; Walker, M.; Berger, A.T.; Talbert, E. Youth Receptivity to FDA’s The Real Cost Tobacco Prevention Campaign: Evidence from Message Pretesting. J. Health Commun. 2016, 21, 1153–1160. [Google Scholar] [CrossRef] [PubMed]
- Woolf, S.H.; Zimmerman, E.; Haley, A.; Krist, A.H. Authentic engagement of patients and communities can transform research, practice, and policy. Health Aff. 2016, 35, 590–594. [Google Scholar] [CrossRef] [PubMed]
- Thompson, L.A.; Mercado, R.; Martinko, T.; Acharya, R. Novel Interventions and Assessments Using Patient Portals in Adolescent Research: Confidential Survey Study. J. Med. Intern. Res. 2018, 20, e101. [Google Scholar] [CrossRef] [PubMed]
- Shenkman, E.; Hurt, M.; Hogan, W.; Carrasquillo, O.; Smith, S.; Brickman, A.; Nelson, D. OneFlorida Clinical Research Consortium: Linking a Clinical and Translational Science Institute with a Community-Based Distributive Medical Educational Model. Acad. Med. 2018, 93, 451. [Google Scholar] [CrossRef] [PubMed]
- Proctor, E.; Silmere, H.; Raghavan, R.; Hovmand, P.; Aarons, G.; Bunger, A.; Griffey, R.; Hensley, M. Outcomes for implementation research: Conceptual distinctions, measurement challenges, and research agenda. Adm. Policy Ment. Health Ment. Health Serv. Res. 2011, 38, 65–76. [Google Scholar] [CrossRef] [PubMed]
- Pierce, J.P.; Choi, W.S.; Gilpin, E.A.; Farkas, A.J.; Merritt, R.K. Validation of susceptibility as a predictor of which adolescents take up smoking in the United States. Health Psychol. 1996, 15, 355–361. [Google Scholar] [CrossRef] [PubMed]
- Jackson, C. Cognitive susceptibility to smoking and initiation of smoking during childhood: A longitudinal study. Prev. Med. (Baltim.) 1998, 27, 129–134. [Google Scholar] [CrossRef] [PubMed]
- Glaser, B.G.; Strauss, A.L. The Discovery of Grounded Theory: Strategies for Qualitative Research; Aldine Transaction: New Brunswick, NJ, USA, 1967. [Google Scholar]
- Guest, G.; Macqueen, K.M. An Introduction to Team-Based Qualitative Research. In Handbook for Team-Based Qualitative Research; Rowman & Littlefield Pub Incorporated: Lanham, MF, USA, 2008. [Google Scholar]
- Duke, J.C.; Alexander, T.N.; Zhao, X.; Delahanty, J.C.; Allen, J.A.; MacMonegle, A.J.; Farrelly, M.C. Youth’s awareness of and reactions to the real cost national tobacco public education campaign. PLoS ONE 2015, 10, e0144827. [Google Scholar] [CrossRef] [PubMed]
- American Academy of Pediatrics. Bright Futures. Prevention and Health Promotion for Infants, Children, Adolescents, and Their Families. Available online: https://brightfutures.aap.org/Pages/default.aspx (accessed on 27 September 2017).
- Thompson, L.A.; Martinko, T.; Budd, P.; Mercado, R.; Schentrup, A.M. Meaningful Use of a Confidential Adolescent Patient Portal. J. Adolesc. Health 2016, 58, 134–140. [Google Scholar] [CrossRef] [PubMed]
- Rogers, E.M. Diffusion of Innovations; Macmillian Publishing Co.: New York, NY, USA, 1995. [Google Scholar]
- Stevens, M.M.; Olson, A.L.; Gaffney, C.A.; Tosteson, T.D.; Mott, L.A.; Starr, P. A Pediatric, Practice-Based, Randomized Trial of Drinking and Smoking Prevention and Bicycle Helmet, Gun, and Seatbelt Safety Promotion. Pediatrics 2002, 109, 490–497. [Google Scholar] [CrossRef] [PubMed]
- Hollis, J.F.; Polen, M.R.; Whitlock, E.P.; Lichtenstein, E.; Mullooly, J.P.; Velicer, W.F.; Redding, C.A. Teen Reach: Outcomes from a Randomized, Controlled Trial of a Tobacco Reduction Program for Teens Seen in Primary Medical Care. Pediatrics 2005, 115, 981–989. [Google Scholar] [CrossRef] [PubMed]
- Pbert, L.; Flint, A.J.; Fletcher, K.E.; Young, M.H.; Druker, S.; DiFranza, J.R. Effect of a pediatric practice-based smoking prevention and cessation intervention for adolescents: A randomized, controlled trial. Pediatrics 2008, 121, e738–e747. [Google Scholar] [CrossRef] [PubMed]
- Vidrine, J.I.; Shete, S.; Cao, Y.; Greisinger, A.; Harmonson, P.; Sharp, B.; Miles, L.; Zbikowski, S.M.; Wetter, D.W. Ask-Advise-Connect: A new approach to smoking treatment delivery in health care settings. JAMA Intern. Med. 2013, 173, 458–464. [Google Scholar] [CrossRef] [PubMed]
- Adsit, R.T.; Fox, B.M.; Tsiolis, T.; Ogland, C.; Simerson, M.; Vind, L.M.; Bell, S.M.; Skora, A.D.; Baker, T.B.; Fiore, M.C. Using the electronic health record to connect primary care patients to evidence-based telephonic tobacco quitline services: A closed-loop demonstration project. Transl. Behav. Med. 2014, 4, 324–332. [Google Scholar] [CrossRef] [PubMed]
- Fraser, D.; Christiansen, B.A.; Adsit, R.; Baker, T.B.; Fiore, M.C. Electronic health records as a tool for recruitment of participants’ clinical effectiveness research: Lessons learned from tobacco cessation. Transl. Behav. Med. 2013, 3, 244–252. [Google Scholar] [CrossRef] [PubMed]
- Ramsey, A.; Lanzo, E.; Huston-Paterson, H.; Tomaszewski, K.; Trent, M. Increasing Patient Portal Usage: Preliminary Outcomes From the MyChart Genius Project. J. Adolesc. Health 2018, 62, 29–35. [Google Scholar] [CrossRef] [PubMed]

© 2018 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Salloum, R.G.; Theis, R.P.; Pbert, L.; Gurka, M.J.; Porter, M.; Lee, D.; Shenkman, E.A.; Thompson, L.A. Stakeholder Engagement in Developing an Electronic Clinical Support Tool for Tobacco Prevention in Adolescent Primary Care. Children 2018, 5, 170. https://doi.org/10.3390/children5120170
Salloum RG, Theis RP, Pbert L, Gurka MJ, Porter M, Lee D, Shenkman EA, Thompson LA. Stakeholder Engagement in Developing an Electronic Clinical Support Tool for Tobacco Prevention in Adolescent Primary Care. Children. 2018; 5(12):170. https://doi.org/10.3390/children5120170
Chicago/Turabian StyleSalloum, Ramzi G., Ryan P. Theis, Lori Pbert, Matthew J. Gurka, Maribeth Porter, Diana Lee, Elizabeth A. Shenkman, and Lindsay A. Thompson. 2018. "Stakeholder Engagement in Developing an Electronic Clinical Support Tool for Tobacco Prevention in Adolescent Primary Care" Children 5, no. 12: 170. https://doi.org/10.3390/children5120170
APA StyleSalloum, R. G., Theis, R. P., Pbert, L., Gurka, M. J., Porter, M., Lee, D., Shenkman, E. A., & Thompson, L. A. (2018). Stakeholder Engagement in Developing an Electronic Clinical Support Tool for Tobacco Prevention in Adolescent Primary Care. Children, 5(12), 170. https://doi.org/10.3390/children5120170





