A Trial and Perceptions Assessment of APP-Based Flipped Classroom Teaching Model for Medical Students in Learning Immunology in China
Abstract
:1. Introduction
2. Materials and Methods
2.1. General Information of the Course
2.2. Research Participants
2.3. Ethical Considerations
2.4. Materials of Research
2.5. Curriculum Design and Management
2.6. Evaluation Methods
2.7. Data Analysis
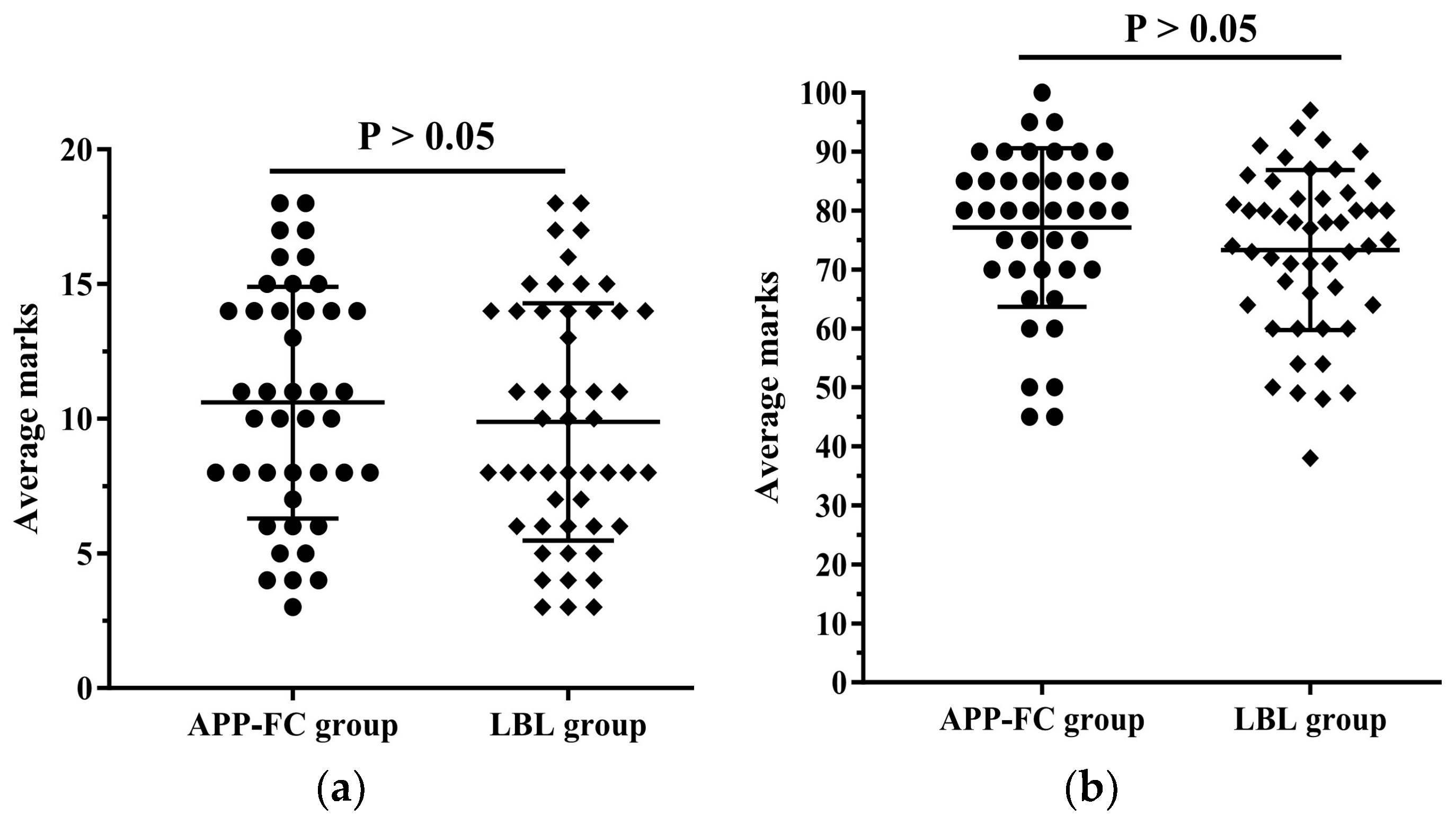
3. Results
4. Discussion
Acknowledgments
Author Contributions
Conflicts of Interest
References
- Ma, X.; Zhang, L.; Luo, Y.; Wang, J.; Yu, H.; Cao, M.; Wu, Y.; Tan, J.; Liang, Y. Establishment of the experimental education system of medical immunology for undergraduate students. Chin. J. Med. Educ. Res. 2016, 15, 394–396. [Google Scholar]
- Ma, X.; Zhang, L.; Wang, J.; Luo, Y.; Liang, Y.; Wu, Y. A perceptions assessment of patient-oriented problem-solving teaching strategy for medical immunology course in Chinese students. J. Balt. Sci. Educ. 2016, 15, 706–711. [Google Scholar]
- Zeng, R.; Xiang, L.-R.; Yue, R.-Z.; Zeng, J.; Wan, X.-H.; Zuo, C. Friend or foe? Flipped classroom for undergraduate electrocardiogram learning: A randomized controlled study. BMC Med. Educ. 2017, 17, 53. [Google Scholar]
- Ying, L.; Yi, Z.; Chuan, C.; Wei, W.; Tingting, C.; Tao, L.; Yonghao, L.; Bingqian, L.; Yu, L.; Lin, L.; et al. Facing the challenges in ophthalmology clerkship teaching: Is flipped classroom the answer. PLoS ONE 2017, 12, e0174829. [Google Scholar]
- Stuart, J.; Rutherford, R.J. Medical student concentration during lectures. Lancet 1978, 2, 514–516. [Google Scholar] [CrossRef]
- Sait, M.S.; Siddiqui, Z.; Ashraf, Y. Advances in medical education and practice: Student perceptions of the flipped classroom. Adv. Med. Educ. Pract. 2017, 8, 317–320. [Google Scholar] [CrossRef] [PubMed]
- Freeman, S.; Eddy, S.L.; McDonough, M.; Smith, M.K.; Okoroafor, N.; Jordt, H.; Wenderoth, M.P. Active learning increases student performance in science, engineering, and mathematics. Proc. Natl. Acad. Sci. USA 2014, 111, 8410–8415. [Google Scholar] [CrossRef] [PubMed]
- Tang, F.; Chen, C.; Zhu, Y.; Zuo, C.; Zhong, Y.; Wang, N.; Zhou, L.; Zou, Y.; Liang, D. Comparison between flipped classroom and lecture-based classroom in ophthalmology clerkship. Med. Educ. Online 2017, 22, 1395679. [Google Scholar] [CrossRef] [PubMed]
- Ma, X.; Luo, Y.; Wang, J.; Zhang, L.; Liang, Y.; Wu, Y.; Yu, H.; Cao, M. Comparison of student perception and performance between case-based learning and lecture-based learning in a clinical laboratory immunology course. J. Lab. Med. 2016, 40, 283–289. [Google Scholar] [CrossRef]
- Zhang, Z.; Liu, W.; Han, J.; Guo, S.; Wu, Y. A trial of patient-oriented problem-solving system for immunology teaching in china: A comparison with dialectic lectures. BMC Med. Educ. 2013, 13. [Google Scholar] [CrossRef] [PubMed]
- Chen, F.; Lui, A.M.; Martinelli, S.M. A systematic review of the effectiveness of flipped classrooms in medical education. Med. Educ. 2017, 51, 585–597. [Google Scholar] [CrossRef] [PubMed]
- Hou, J.; Luo, Y.; Wang, Z.; Meng, Q. Study on the scale and structure of health professional education in Chinas’ colleges and universities from 1998 to 2012. Chin. J. Med. Edu. Res. 2016, 15, 114–121. [Google Scholar]
- Tolks, D.; Schafer, C.; Raupach, T.; Kruse, L.; Sarikas, A.; Gerhardt-Szep, S.; Kllauer, G.; Lemos, M.; Fischer, M.R.; Eichner, B.; et al. An introduction to the inverted/flipped classroom model in education and advanced training in medicine and in the healthcare professions. GMS J. Med. Educ. 2016, 33. [Google Scholar] [CrossRef]
- Tune, J.D.; Sturek, M.; Basile, D.P. Flipped classroom model improves graduate student performance in cardiovascular, respiratory, and renal physiology. Adv. Physiol. Educ. 2013, 37, 316–320. [Google Scholar] [CrossRef] [PubMed]
- Whillier, S.; Lystad, R.P. No differences in grades or level of satisfaction in a flipped classroom for neuroanatomy. J. Chiropr. Educ. 2015, 29, 127–133. [Google Scholar] [CrossRef] [PubMed]
- Deshpande, S.; Chahande, J.; Rathi, A. Mobile learning app: A novel method to teach clinical decision making in prosthodontics. Educ. Health (Abingdon) 2017, 30, 31–34. [Google Scholar] [CrossRef] [PubMed]
- Cheston, C.C.; Flickinger, T.E.; Chisolm, M.S. Social media use in medical education: A systematic review. Acad. Med. 2013, 88, 893–901. [Google Scholar] [CrossRef] [PubMed]
- Lau, C.; Kolli, V. App use in psychiatric education: A medical student survey. Acad. Psychiatry 2016, 41, 68–70. [Google Scholar] [CrossRef] [PubMed]
- Lage, M.; Platt, G.; Treglia, M. Inverting the classroom: A gateway to creating an inclusive learning environment. J. Econ. Educ. 2000, 31, 30–43. [Google Scholar] [CrossRef]
- Van-Vliet, E.A.; Winnips, J.C.; Brouwer, N. Flipped-class pedagogy enhances student metacognition and collaborative-learning strategies in higher education but effect does not persist. CBE-Life Sci. Educ. 2015, 14, 26. [Google Scholar] [CrossRef] [PubMed]
- Medina, M.S.; Castleberry, A.N.; Persky, A.M. Strategies for improving learner metacognition in health professional education. Am. J. Pharm. Educ. 2017, 81, 78. [Google Scholar] [PubMed]
- Persky, A.M.; McLaughlin, J.E. The flipped classroom—From theory to practice in health professional education. Am. J. Pharm. Educ. 2017, 81, 118. [Google Scholar] [PubMed]
- Anderson, H.G., Jr.; Frazier, L.; Anderson, S.L.; Stanton, R.; Gillette, C.; Broedel-Zaugg, K.; Yingling, K. Comparison of pharmaceutical calculations learning outcomes achieved within a traditional lecture or flipped classroom andragogy. Am. J. Pharm. Educ. 2017, 81, 70. [Google Scholar] [PubMed]
- Briz-Ponce, L.; Juanes-Méndez, J.A.; García-Peñalvo, F.J.; Pereira, A. Effects of mobile learning in medical education: A counterfactual evaluation. J. Med. Syst. 2016, 40, 136. [Google Scholar] [CrossRef] [PubMed]
- Zhang, M.W.; Tsang, T.; Cheow, E.; Ho, C.S.; Yeong, N.B.; Ho, R.C. Enabling psychiatrists to be mobile phone app developers: insights into app development methodologies. MIR mHealth uHealth 2014, 2, e53. [Google Scholar] [CrossRef] [PubMed]
- Smeds, M.R.; Thrush, C.R.; Mizell, J.S.; Berry, K.S.; Bentley, F.R. Mobile spaced education for surgery rotation improves national board of medical examiners scores. J. Surg. Res. 2016, 201, 99–104. [Google Scholar] [CrossRef] [PubMed]
- Munson, A.; Pierce, R. Flipping content to improve student examination performance in a pharmacogenomics course. Am. J. Pharm. Educ. 2015, 79, 103. [Google Scholar] [CrossRef] [PubMed]
- Prober, C.G.; Heath, C. Lecture halls without lectures—A proposal for medical education. N. Engl. J. Med. 2012, 366, 1657–1659. [Google Scholar] [CrossRef] [PubMed]
- Fatima, S.S.; Arain, F.M.; Enam, S.A. Flipped classroom instructional approach in undergraduate medical education. Pak. J. Med. Sci. 2017, 33, 1424–1428. [Google Scholar] [CrossRef] [PubMed]
- Girgis, F.; Miller, J.P. Implementation of a “flipped classroom” for neurosurgery resident education. Can. J. Neurol. Sci. 2018, 45, 76–82. [Google Scholar] [CrossRef] [PubMed]

| Characteristics | Application-Based Flipped Classroom (APP-FC) Group | Lecture-Based Learning (LBL) Group |
|---|---|---|
| Number | 42 | 50 |
| Age | 19.4 ± 0.74 | 19.5 ± 0.81 |
| Gender (male/female) | 21/21 | 22/28 |
| Anatomy | 72.02 ± 10.51 | 73.18 ± 8.73 |
| Cellular biology | 79.54 ± 7.64 | 78.16 ± 7.98 |
| Histology and embryology | 80.67 ± 9.67 | 80.32 ± 8.06 |
| Questions | Yes (%) | No (%) | |
|---|---|---|---|
| Compared with traditional lecture-based instruction, do you think: | |||
| 1 | APP-FC should be used by more immunology teachers? | 32 (76%) | 10 (24%) |
| 2 | APP-FC is a more scientific way for medical teaching? | 31 (74%) | 11 (26%) |
| 3 | APP-FC stimulates your interest in learning immunology? | 34 (81%) | 8 (19%) |
| 4 | APP-FC strengthens your intrinsic motivation? | 35 (83%) | 7 (17%) |
| 5 | APP-FC develops your self-directed learning skills? | 34 (81%) | 8 (19%) |
| 6 | APP-FC improves your problem-solving skills? | 33 (79%) | 9 (21%) |
| 7 | APP-FC helps you prepare for immunology exams? | 22 (52%) | 20 (48%) |
| 8 | APP-FC provides benefits in terms of long-term memory? | 31 (74%) | 11 (26%) |
| 9 | APP-FC helps you understand the course objectives? | 22 (52%) | 20 (48%) |
| 10 | I can easily browse lessons according to my own situation any time? | 36 (86%) | 6 (14%) |
| 11 | APP-FC may not bring an increase in workload? | 30 (71%) | 12 (29%) |
| 12 | The delivery of knowledge in an APP-FC is fragmented and unsystematic? | 21 (50%) | 21 (50%) |
| 13 | APP-FC is feasible for the current educational environment? | 30 (71%) | 12 (29%) |
| 14 | APP-FC is an effective teaching model that is worthy of promotion? | 31 (74%) | 11 (26%) |
| Average (%) | 29.4 (70%) | 12.6 (30%) | |
| Question/Statement | APP-FC Teaching Model | Lecture-Based Instruction | t (P) |
|---|---|---|---|
| Increase learning motivation | 4.38 ± 0.73 | 3.90 ± 0.93 | 2.60 (P = 0.011) ▲ |
| Promote self-directed learn skills | 4.67 ± 0.48 | 3.47 ± 1.08 | 6.49 (P = 0.001) ▲ |
| Improve peer interaction | 4.12 ± 0.83 | 3.71 ± 1.06 | 1.94 (P = 0.056) |
| Extend more related knowledge | 3.69 ± 0.98 | 3.88 ± 1.04 | 0.87 (P = 0.389) |
| Help with memorizing basic knowledge | 4.05 ± 0.96 | 3.38 ± 1.28 | 2.68 (P = 0.009) ▲ |
| Enhance problem-solving abilities | 3.90 ± 1.01 | 3.52 ± 0.96 | 2.65 (P = 0.010) ▲ |
| Enhance clinical reasoning abilities | 4.05 ± 0.91 | 3.83 ± 1.03 | 1.01 (P = 0.316) |
| Enhance communication skills | 4.19 ± 0.80 | 3.86 ± 1.13 | 1.55 (P = 0.125) |
| Sum of perception scores (5 × 8 = 40) | 33.05 ± 4.38 | 29.54 ± 5.33 | 3.28 (P = 0.002) ▲ |
© 2018 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Ma, X.; Luo, Y.; Zhang, L.; Wang, J.; Liang, Y.; Yu, H.; Wu, Y.; Tan, J.; Cao, M. A Trial and Perceptions Assessment of APP-Based Flipped Classroom Teaching Model for Medical Students in Learning Immunology in China. Educ. Sci. 2018, 8, 45. https://doi.org/10.3390/educsci8020045
Ma X, Luo Y, Zhang L, Wang J, Liang Y, Yu H, Wu Y, Tan J, Cao M. A Trial and Perceptions Assessment of APP-Based Flipped Classroom Teaching Model for Medical Students in Learning Immunology in China. Education Sciences. 2018; 8(2):45. https://doi.org/10.3390/educsci8020045
Chicago/Turabian StyleMa, Xingming, Yanping Luo, Lifeng Zhang, Jingqiu Wang, Yaling Liang, Hongjuan Yu, Yufeng Wu, Jiying Tan, and Mingqiang Cao. 2018. "A Trial and Perceptions Assessment of APP-Based Flipped Classroom Teaching Model for Medical Students in Learning Immunology in China" Education Sciences 8, no. 2: 45. https://doi.org/10.3390/educsci8020045
APA StyleMa, X., Luo, Y., Zhang, L., Wang, J., Liang, Y., Yu, H., Wu, Y., Tan, J., & Cao, M. (2018). A Trial and Perceptions Assessment of APP-Based Flipped Classroom Teaching Model for Medical Students in Learning Immunology in China. Education Sciences, 8(2), 45. https://doi.org/10.3390/educsci8020045





