Impact of the 2016 Policy Change on the Delivery of MedsCheck Services in Ontario: An Interrupted Time-Series Analysis
Abstract
1. Introduction
2. Materials and Methods
2.1. Study Design
2.2. Data Sources
2.3. Analytical Approach
3. Results
4. Discussion
5. Conclusions
Author Contributions
Funding
Acknowledgments
Conflicts of Interest
References
- Ministry of Health and Long-Term Care. Preventing and Managing Chronic Disease: Ontario’s Framework; Queen’s Printer for Ontario: Toronto, ON, Canada, 2007.
- Institute of Medicine Committee on Identifying and Preventing Medication Errors. Preventing Medication Errors; National Academies Press: Washington, DC, USA, 2007. [Google Scholar]
- Sichieri, K.; Rodrigues, A.R.B.; Takahashi, J.A.; Secoli, S.R.; Nobre, M.R.C.; Mónica, M.A.; Julio, F.G. Mortality associated with the use of inappropriate drugs according Beers criteria: A systematic review. Adv. Pharmacol. Pharm. 2013, 1, 74–84. [Google Scholar]
- Dormann, H.; Criegee-Rieck, M.; Neubert, A.; Egger, T.; Geise, A.; Krebs, S.; Schneider, T.; Levy, M.; Hahn, E.; Brune, K. Lack of awareness of community-acquired adverse drug reactions upon hospital admission: Dimensions and consequences of a dilemma. Drug Saf. 2003, 26, 353–362. [Google Scholar] [CrossRef]
- Tsuyuki, R.T.; Beahm, N.P.; Okada, H.; Al Hamarneh, Y.N. Pharmacists as accessible primary health care providers: Review of the evidence. Can. Pharm. J. 2018, 151, 4–5. [Google Scholar] [CrossRef] [PubMed]
- Schnipper, J.L.; Kirwin, J.L.; Cotugno, M.C.; Wahlstrom, S.A.; Brown, B.A.; Tarvin, E.; Kachalia, A.; Horng, M.; Roy, C.L.; McKean, S.C.; et al. Role of pharmacist counseling in preventing adverse drug events after hospitalization. Arch. Intern. Med. 2006, 166, 565. [Google Scholar] [CrossRef] [PubMed]
- Knudsen, P.; Herborg, H.; Mortensen, A.R.; Knudsen, M.; Hellebek, A. Preventing medication errors in community pharmacy: Frequency and seriousness of medication errors. Qual. Saf. Health Care 2007, 16, 291–296. [Google Scholar] [CrossRef] [PubMed]
- Roberts, A.S.; Benrimoj, S.I.; Chen, T.F.; Williams, K.A.; Hopp, T.R.; Aslani, P. Understanding practice change in community pharmacy: A qualitative study in Australia. Res. Soc. Adm. Pharm. 2005, 1, 546–564. [Google Scholar] [CrossRef] [PubMed]
- Houle, S.K.D.; Carter, C.A.; Tsuyuki, R.T.; Grindrod, K.A. Remunerated patient care services and injections by pharmacists: An international update. Can. Pharm. J. 2019, 152, 92–108. [Google Scholar] [CrossRef] [PubMed]
- Latif, A.; Pollock, K.; Boardman, H.F. Medicines use reviews: A potential resource or lost opportunity for general practice? BMC Fam. Pract. 2013, 14, 57. [Google Scholar] [CrossRef] [PubMed]
- Martin, D.; Miller, A.P.; Quesnel-Vallée, A.; Caron, N.R.; Vissandjée, B.; Marchildon, G.P. Canada’s universal health-care system: Achieving its potential. Lancet 2018, 391, 1718–1735. [Google Scholar] [CrossRef]
- Ontario Ministry of Health and Long-Term Care. The MedsCheck Program Guidebook, 2nd ed.; Queen’s Printer for Ontario: Toronto, ON, Canada, 2008.
- Ontario Ministry of Health and Long-Term Care. Professional Pharmacy Services Guidebook, 3rd ed.; Queen’s Printer for Ontario: Toronto, ON, Cananda, 2016.
- MacCallum, L.; Consiglio, G.; MacKeigan, L.; Dolovich, L.; MacCallum, L. Uptake of community pharmacist-delivered MedsCheck diabetes medication review service in Ontario between 2010 and 2014. Can. J. Diabetes 2017, 41, 253–258. [Google Scholar] [CrossRef]
- Government of Ontario. Central Forms Repository. Available online: http://www.forms.ssb.gov.on.ca/mbs/ssb/forms/ssbforms.nsf?opendatabase&ENV=WWE (accessed on 7 August 2019).
- Canadian Council on Continuing Education in Pharmacy MedsCheck (Diabetes) Ontario. Available online: https://www.cccep.ca/pages/meds_check_diabetes_ontario.html (accessed on 17 May 2019).
- Jandoc, R.; Burden, A.M.; Mamdani, M.; Lévesque, L.E.; Cadarette, S.M. Interrupted time series analysis in drug utilization research is increasing: Systematic review and recommendations. J. Clin. Epidemiol. 2015, 68, 950–956. [Google Scholar] [CrossRef] [PubMed]
- Wagner, A.K.; Soumerai, S.B.; Zhang, F.; Ross-Degnan, D. Segmented regression analysis of interrupted time series studies in medication use research. J. Clin. Pharm. Ther. 2002, 27, 299–309. [Google Scholar] [CrossRef] [PubMed]
- Bernal, J.L.; Cummins, S.; Gasparrini, A. Interrupted time series regression for the evaluation of public health interventions: A tutorial. Int. J. Epidemiol. 2016, 46, 348–355. [Google Scholar]
- Lagarde, M. How to do (or not to do)... Assessing the impact of a policy change with routine longitudinal data. Health Policy Plan. 2012, 27, 76–83. [Google Scholar] [CrossRef] [PubMed]
- Durbin, J.; Watson, G.S. Testing for serial correlation in least squares regression: I. Biometrika 1950, 37, 409–428. [Google Scholar] [PubMed]
- Dickey, D.A.; Fuller, W.A. Distribution of the estimators for autoregressive time series with a unit root. J. Am. Stat. Assoc. 1979, 74, 427–431. [Google Scholar]
- Zhang, F.; Wagner, A.K.; Soumerai, S.B.; Ross-Degnan, D. Methods for estimating confidence intervals in interrupted time series analyses of health interventions. J. Clin. Epidemiol. 2009, 62, 143–148. [Google Scholar] [CrossRef] [PubMed]
- R Core Team. R: A Language and Environment for Statistical Computing; R Foundation for Statistical Computing: Vienna, Austria, 2013. [Google Scholar]
- Dolovich, L.; Consiglio, G.; MacKeigan, L.; Abrahamyan, L.; Pechlivanoglou, P.; Rac, V.E.; Pojskic, N.; Bojarski, E.A.; Su, J.; Krahn, M.; et al. Uptake of the MedsCheck annual medication review service in Ontario community pharmacies between 2007 and 2013. Can. Pharm. J. 2016, 149, 293–302. [Google Scholar] [CrossRef]
- Tracy, C.S.; Upshur, R.E.G. MedsCheck: An opportunity missed. CMAJ 2008, 178, 440. [Google Scholar] [CrossRef]
- Pechlivanoglou, P.; Abrahamyan, L.; Mackeigan, L.; Consiglio, G.P.; Dolovich, L.; Li, P.; Cadarette, S.M.; Rac, V.E.; Shin, J.; Krahn, M. Factors affecting the delivery of community pharmacist-led medication reviews: Evidence from the MedsCheck annual service in Ontario. BMC Health Serv. Res. 2016, 16, 666. [Google Scholar] [CrossRef]
- Ontario Public Drug Programs, Ministry of Health and Long-Term Care. Notice from the Executive Officer: MedsCheck Program Enhancements Standardization. Available online: http://www.health.gov.on.ca/en/pro/programs/drugs/opdp_eo/notices/exec_office_20160704.pdf (accessed on 20 May 2019).
- Ontario Pharmacists Association. MedsCheck Program. Available online: https://www.opatoday.com/professional/resources/for-pharmacists/programs/medscheck (accessed on 2 July 2019).
- Ontario Ministry of Health and Long-Term Care. MedsCheck Resources for Pharmacists—Health Care Professionals. Available online: http://www.health.gov.on.ca/en/pro/programs/drugs/medscheck/resources.aspx (accessed on 2 July 2019).
- Ontario Ministry of Heath and Long-Term Care. Reforming Ontario’s Drug System. Available online: https://news.ontario.ca/mohltc/en/2010/04/reforming-ontarios-drug-system.html (accessed on 29 May 2019).
- Canadian Institute for Health Information; Canadian Patient Safety Institute; Institute for Safe Medication Practices Canada. Medication Reconciliation in Canada: Raising the Bar; Accreditiation Canada: Ottawa, ON, Canada, 2012. [Google Scholar]
- Canadian Institute for Health Information. Prescribed Drug Spending in Canada, 2018: A Focus on Public Drug Programs; Accreditiation Canada: Ottawa, ON, Canada, 2018. [Google Scholar]
- Strauss, M.; Howlett, K. Pharmacies Take Hit as Ontario Cuts Generic Drug Payments Again. Available online: https://www.theglobeandmail.com/globe-investor/pharmacies-take-hit-as-ontario-cuts-generic-drug-payments-again/article4170794/ (accessed on 29 May 2019).
- Ministry of Finance; Ministry of Heath and Long-Term Care. Stronger, Healthier Ontario Act (Budget Measures). 2017. Available online: https://news.ontario.ca/mof/en/2017/05/stronger-healthier-ontario-act-budget-measures-2017.html (accessed on 29 May 2019).
- Barnes, B.; Hincapie, A.L.; Luder, H.; Kirby, J.; Frede, S.; Heaton, P.C. Appointment-based models: A comparison of three model designs in a large chain community pharmacy setting. J. Am. Pharm. Assoc. 2018, 58, 156–162. [Google Scholar] [CrossRef] [PubMed]
- MacCallum, L.; Dolovich, L. Follow-up in community pharmacy should be routine, not extraordinary. Can. Pharm. J. 2018, 151, 79–81. [Google Scholar] [CrossRef] [PubMed]
- Cipolle, R.J.; Strand, L.M.; Morley, P.C. Pharmaceutical Care Practice: The Patient-Centered Approach to Medication Management Services, 3rd ed.; McGraw-Hill Education: New York, NY, USA, 2012. [Google Scholar]
- Ontario Ministry of Health and Long Term Care. MedsCheck at Home. Available online: http://www.health.gov.on.ca/en/pro/programs/drugs/medscheck/medscheck_home.aspx (accessed on 23 May 2019).
- Ontario Long Term Care Association. This Is Long-Term Care 2018; Ontario Long Term Care Association: Toronto, ON, Canada, 2018. [Google Scholar]
- Lipscombe, L.L.; Hux, J.E. Trends in diabetes prevalence, incidence, and mortality in Ontario, Canada 1995–2005: A population-based study. Lancet 2007, 369, 750–756. [Google Scholar] [CrossRef]
- Statistics Canada Diabetes, by Age Group and Sex (Number of Persons). Available online: http://www.statcan.gc.ca/tables-tableaux/sum-som/l01/cst01/health53a-eng.htm (accessed on 22 May 2018).
- Ontario Ministry of Health and Long-Term Care. Diabetes: Strategies for Prevention. Available online: http://www.health.gov.on.ca/en/common/ministry/publications/reports/diabetes/diabetes.aspx (accessed on 22 May 2019).
- Ontario Long Term Care Association. This Is Long-Term Care 2016; Ontario Long Term Care Association: Toronto, ON, Canada, 2016. [Google Scholar]
- Craig, P.; Dieppe, P.; Macintyre, S.; Michie, S.; Nazareth, I.; Petticrew, M.; Medical Research Council guidance. Developing and evaluating complex interventions: The new Medical Research Council guidance. BMJ 2008, 337. [Google Scholar] [CrossRef] [PubMed]
- Bleijenberg, N.; de Man-van Ginkel, J.M.; Trappenburg, J.C.A.; Ettema, R.G.A.; Sino, C.G.; Heim, N.; Hafsteindóttir, T.B.; Richards, D.A.; Schuurmans, M.J. Increasing value and reducing waste by optimizing the development of complex interventions: Enriching the development phase of the Medical Research Council (MRC) Framework. Int. J. Nurs. Stud. 2018, 79, 86–93. [Google Scholar] [CrossRef] [PubMed]
- Drugs and Devices Division: Ministry of Health and Long-Term Care. Proposals to Establish More Efficient Pharmacy Reimbursement Policies. Available online: http://www.health.gov.on.ca/en/pro/programs/drugs/opdp_eo/notices/exec_office_20190426.pdf (accessed on 2 July 2019).
- Office of the Auditor General of Ontario. Chapter 3: Reports on Value-for-Money, 3.09: Ontario Public Drug Programs. 2017 Annual Report Volume 2; Queen’s Printer for Ontario: Toronto, ON, Canada, 2017.
- Ministry of Finance. 2019 Ontario Budget|Chapter 3: Ontario’s Fiscal Plan and Outlook. Available online: http://budget.ontario.ca/2019/chapter-3.html (accessed on 2 July 2019).
- Al-Rashed, S.A.; Wright, D.J.; Roebuck, N.; Sunter, W.; Chrystyn, H. The value of inpatient pharmaceutical counselling to elderly patients prior to discharge. Br. J. Clin. Pharmacol. 2002, 54, 657–664. [Google Scholar] [CrossRef] [PubMed]
- Jack, B.W.; Chetty, V.K.; Anthony, D.; Greenwald, J.L.; Sanchez, G.M.; Johnson, A.E.; Forsythe, S.R.; O’Donnell, J.K.; Paasche-Orlow, M.K.; Manasseh, C.; et al. A reengineered hospital discharge program to decrease rehospitalization: A randomized trial. Ann. Intern. Med. 2009, 150, 178–187. [Google Scholar] [CrossRef] [PubMed]
- Nazar, H.; Nazar, Z.; Portlock, J.; Todd, A.; Slight, S.P. A systematic review of the role of community pharmacies in improving the transition from secondary to primary care. Br. J. Clin. Pharmacol. 2015, 80, 936–948. [Google Scholar] [CrossRef] [PubMed]
- Ali, M.; Schifano, F.; Robinson, P.; Phillips, G.; Doherty, L.; Melnick, P.; Laming, L.; Sinclair, A.; Dhillon, S. Impact of community pharmacy diabetes monitoring and education programme on diabetes management: A randomized controlled study. Diabet. Med. 2012, 29, e326–e333. [Google Scholar] [CrossRef] [PubMed]
- Krass, I.; Armour, C.L.; Mitchell, B.; Brillant, M.; Dienaar, R.; Hughes, J.; Lau, P.; Peterson, G.; Stewart, K.; Taylor, S.; et al. The Pharmacy diabetes care program: Assessment of a community pharmacy diabetes service model in Australia. Diabet. Med. 2007, 24, 677–683. [Google Scholar] [CrossRef]
- Al Hamarneh, Y.N.; Charrois, T.; Lewanczuk, R.; Tsuyuki, R.T. Pharmacist intervention for glycaemic control in the community (the RxING study). BMJ Open 2013, 3, e003154. [Google Scholar] [CrossRef]
- Kallio, S.E.; Kiiski, A.; Airaksinen, M.S.A.; Mäntylä, A.T.; Kumpusalo-Vauhkonen, A.E.J.; Järvensivu, T.P.; Pohjanoksa-Mäntylä, M.K. Community pharmacists’ contribution to medication reviews for older adults: A systematic review. J. Am. Geriatr. Soc. 2018, 66, 1613–1620. [Google Scholar] [CrossRef]
- Jokanovic, N.; Tan, E.C.; Sudhakaran, S.; Kirkpatrick, C.M.; Dooley, M.J.; Ryan-Atwood, T.E.; Bell, J.S. Pharmacist-led medication review in community settings: An overview of systematic reviews. Res. Soc. Adm. Pharm. 2017, 13, 661–685. [Google Scholar] [CrossRef]

| Before October 2016 | Since October 2016 Policy Change |
|---|---|
| Patient Assessment Summary with Pharmacist’s Signature and Date |
|
Specific to MCH
Specific to MCLTC
|
| Service | PIN | Fee |
|---|---|---|
| MedsCheck (MC) 1 | ||
| MC annual | 93899979 | $60 1 |
| MC follow-up | ||
| • Hospital discharge ≤ 2 weeks | 93899981 | |
| • Pharmacist decision | 93899982 | $25 |
| • Physician or nurse practitioner referral | 93899983 | |
| • Planned hospital admission | 93899984 | |
| MedsCheck Diabetes (MCD) 2 | ||
| MCD annual | 93899988 | $75 |
| MCD follow-up | 93899989 | $25 |
| MedsCheck at Home (MCH) 3 | ||
| MCH annual | 93899987 | $150 |
| MedsCheck Long Term Care (MCLTC) 4 | ||
| MCLTC annual | 93899985 | $90 |
| MCLTC quarterly | 93899986 | $50 |
| Service Type | MedsCheck (Annual or Follow-Up) | MedsCheck Diabetes (Annual or Follow-Up) | MedsCheck at Home | MedsCheck Long Term Care (Annual or Quarterly) |
|---|---|---|---|---|
| Number of recipients | 647,740 | 209,060 | 57,583 | 95,191 |
| Number of Service claims | 2,952,434 | 848,911 | 103,591 | 1,084,410 |
| Age, mean (SD) | 58.3 (17.3) | 60.6 (14.2) | 74.4 (16.4) | 82.6 (10.5) |
| Women, % | 52.4 | 45.2 | 62.1 | 64.0 |
| MedsCheck | MedsCheck Diabetes | MedsCheck at Home | MedsCheck Long Term Care | ||||
|---|---|---|---|---|---|---|---|
| Parameter | Annual | Follow-Up | Annual | Follow-Up | Annual | Quarterly | |
| Total Claims | 2,356,615 | 595,819 | 664,483 | 184,428 | 103,591 | 285,403 | 799,007 |
| Monthly Claims | |||||||
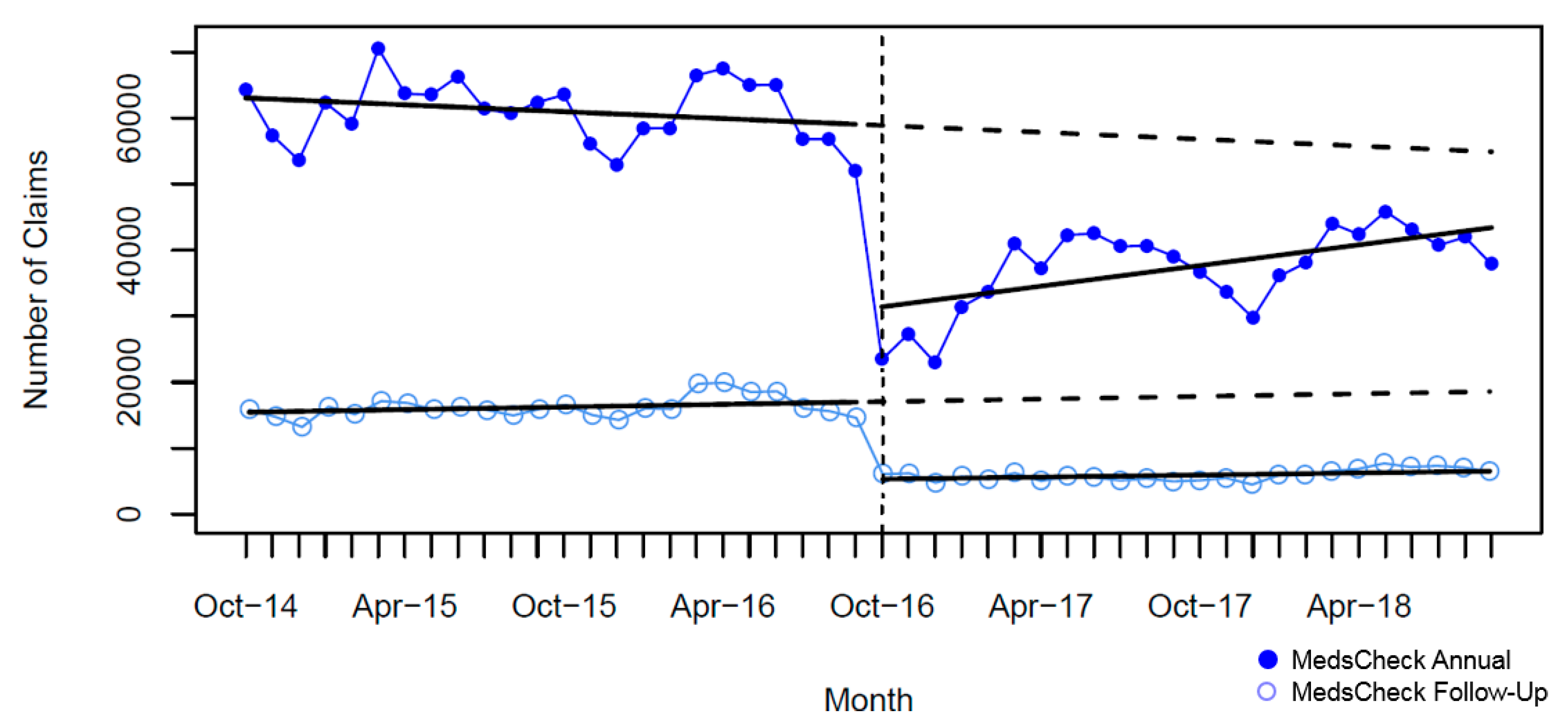
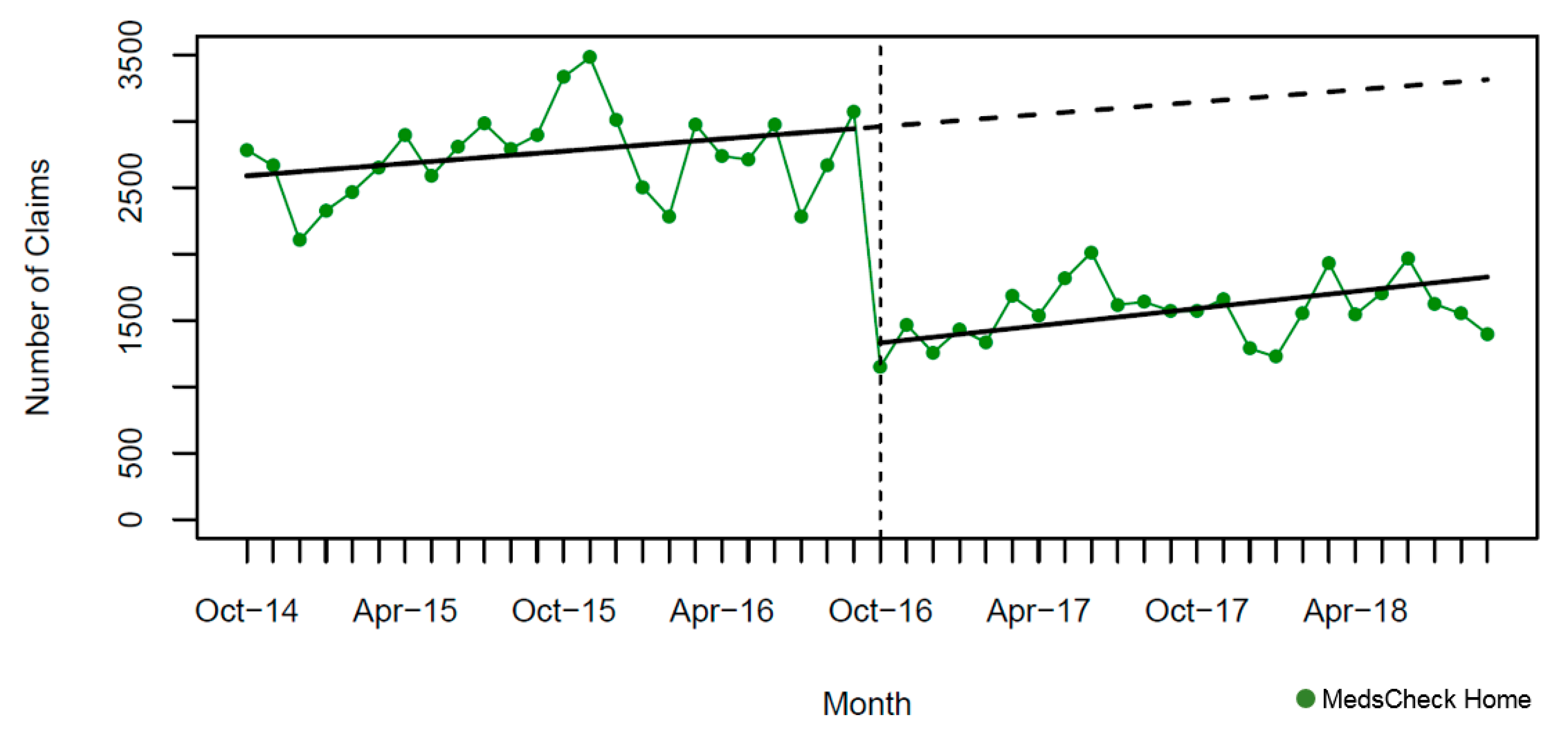
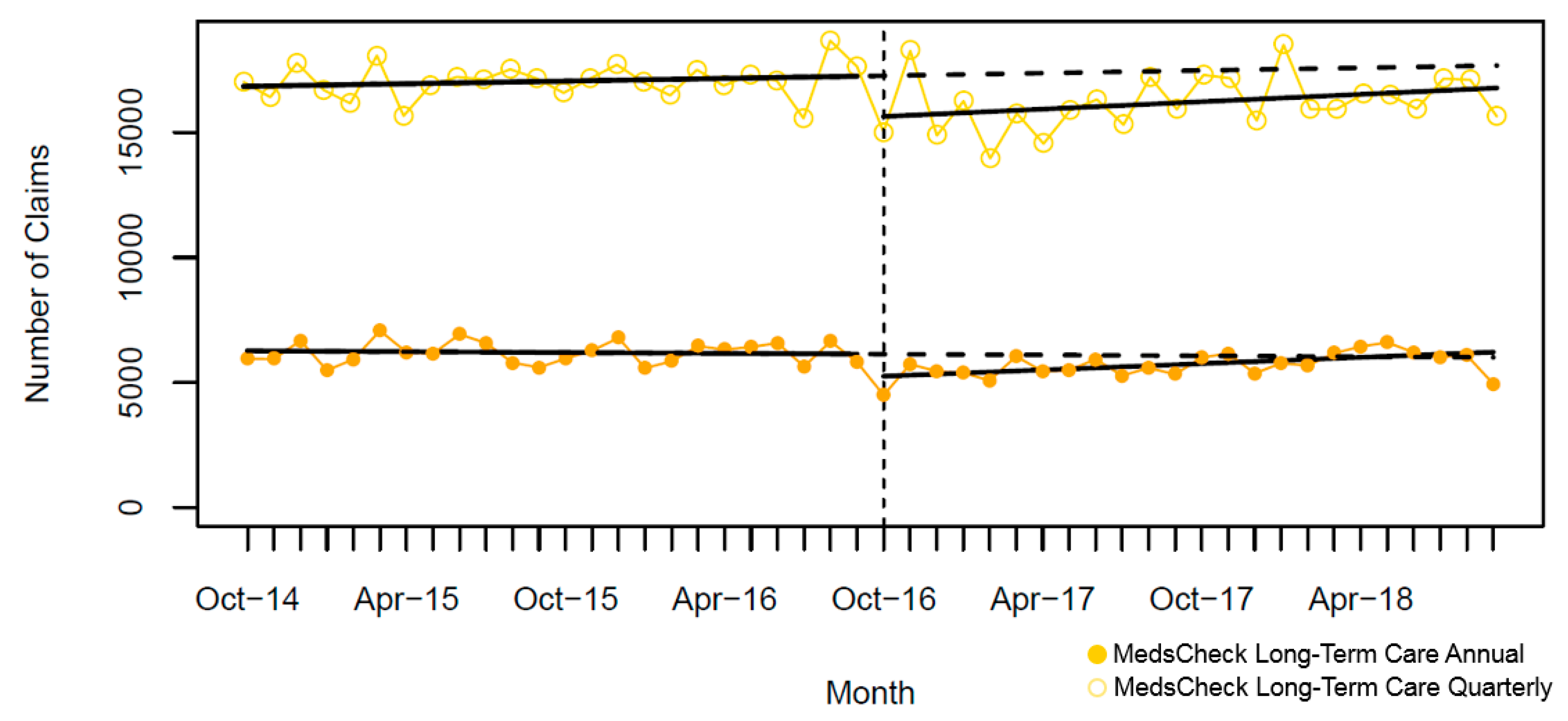
| • Minimum number | 22,973 | 5768 | 4314 | 896 | 1151 | 4493 | 14,000 |
| • Maximum number | 70,554 | 21,353 | 23,443 | 8304 | 3482 | 7074 | 18,687 |
| Results of Segmented Regression Models | |||||||
| Baseline (October 2014), number (95% CI) | 63,223 (60,452, 65,994) | 16,698 (15,826, 17,771) | 18,984 (18,069, 19,899) | 6704 (6157, 7251) | 2575 (2454, 2697) | 6274 (6199, 6349) | 16,848 (16,355, 17,341) |
| Pre-intervention slope, mean monthly claims (95%CI) | −173 (−373, 27) | 67 (−1, 135) | 81 (14, 149) | −19 (−57, 19) | 15 (6, 24) | −6 (−11, −0.3) | 18 (−17, 52) |
| Level Change at Intervention (October 2016) | |||||||
| • Number of claims (95% CI) | −28,167 (−32,034, −24,302) | −11,854 (−13,205, −10,503) | −14,876 (−16,244, −13,508) | −5214 (−5942, −4487) | −1635 (−1828, −1442) | −929 (−1034, −825) | −1656 (−2348, −965) |
| • Relative percent change (95% CI) | −46.7 (−52.9, −40.4) | −64.3 (−71.1, −57.3) | −70.5 (−76.7, −64.3) | −83.2 (−94.3, −72.1) | −55.0 (−61.2, −48.8) | −14.4 (−16.0, −12.8) | −9.4 (−13.2, −5.6) |
| Post-intervention slope, mean monthly claims (95% CI) | 521 (42, 1002) | 52 (−110, 215) | 139 (−17, 296) | 16 (−77, 108) | 22 (4, 40) | 42 (30, 54) | 50 (-33, 132) |
| Relative difference to forecast (September 2018), proportion (95% CI) | −21.0 (−27.7, −14.3) | −61.0 (−67.3, −54.5) | −58.9 (−64.6, −53.2) | −75.8 (−87.7, −63.8) | −44.9 (−50.4, −39.3) | 3.5 (1.8, 5.1) | −5.1 (−8.8, −1.3) |
© 2019 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Shakeri, A.; Dolovich, L.; MacCallum, L.; Gamble, J.-M.; Zhou, L.; Cadarette, S.M. Impact of the 2016 Policy Change on the Delivery of MedsCheck Services in Ontario: An Interrupted Time-Series Analysis. Pharmacy 2019, 7, 115. https://doi.org/10.3390/pharmacy7030115
Shakeri A, Dolovich L, MacCallum L, Gamble J-M, Zhou L, Cadarette SM. Impact of the 2016 Policy Change on the Delivery of MedsCheck Services in Ontario: An Interrupted Time-Series Analysis. Pharmacy. 2019; 7(3):115. https://doi.org/10.3390/pharmacy7030115
Chicago/Turabian StyleShakeri, Ahmad, Lisa Dolovich, Lori MacCallum, John-Michael Gamble, Limei Zhou, and Suzanne M. Cadarette. 2019. "Impact of the 2016 Policy Change on the Delivery of MedsCheck Services in Ontario: An Interrupted Time-Series Analysis" Pharmacy 7, no. 3: 115. https://doi.org/10.3390/pharmacy7030115
APA StyleShakeri, A., Dolovich, L., MacCallum, L., Gamble, J.-M., Zhou, L., & Cadarette, S. M. (2019). Impact of the 2016 Policy Change on the Delivery of MedsCheck Services in Ontario: An Interrupted Time-Series Analysis. Pharmacy, 7(3), 115. https://doi.org/10.3390/pharmacy7030115






