Substantial research has been done on reliability, energy consumption, and security aspects of wireless control. New ideas like IoT-HSNs introduce innovative implementations that require further probing with additional considerations. Not much research can be found on the applications or feasibility studies on real-time control for IoT-HSNs for a variety of reasons, the main reason being the involvement of live subjects.
2.2. IoT-HSN Applications Involving Real-Time Control
It is projected that by 2020, death rates due to cancer might soar by 50%, taking healthcare costs up to 15 million [
5]. Cancer cell monitoring using IoT-HSNs can influence early tumor identification with no biopsy and presents a timely evaluation for early therapy.
Biocompatible nanotubes can be used in the creation of bioactuators and smart biosensors, bone implants on stimulated growth, pointed drug delivery systems, heart attack temperature biosensors, and fabrication of artificial muscles with bioactuators.
Wireless control in IoT-HSNs could have a potential application involving an insulin injection bioactuator that dispenses the correct dose of insulin to a diabetes patient based on inputs from glucose biosensors.
Similar control application can be utilized for Parkinson’s disease (PD) patients. In patients in advanced stages of PD, an unsafe condition called “freezing” or “freezing of gait” is reported [
6]. When a gait-freeze occurs, the patient seems to be stuck and cannot move feet or stand up from a sitting posture. There are no known causes of the ‘freezing’ and the start or end of a gait-freeze cannot be predicted. Such freeze may cause the patient to fall. Freeze episodes happen at random and at varying frequencies across patients. PD patients are given dopaminergic medicines in dose and frequency depending on the patient’s stage of PD. An IoT-HSN control application could use a bioactuator-driven injection system for this medicine as suggested by a measurement and supervisory system.
Related research on Smart Gait [
7] uses biosensors in a smartphone to create an inexpensive gait tracking device. The biosensors measure variability of step length (SL) and step width (SW) to monitor, predict, and possibly prevent falls. Similar application could be in the case of ‘drop foot’ [
8] in which the subject finds it difficult to move or lift the front part of foot causing drag while walking.
Prosthetic implants used in the hip and knee are susceptible to bacterial infections. A flow biosensor in the infected area could sense change in viscosity due to development of bacteria and signal a bioactuator switch in the prosthesis to release stored medicine.
Dakurah et al. [
9] explored a variety of implantable bladder sensors in their work.
In Reference [
10], a wireless bladder volume monitoring system was tested by Hung et al. The system uses a flexible capacitive-based strain sensor to monitor bladder urine volume with respect to changes in the sensor capacitance. The authors used a passive telemetry platform based on inductive coupling to power the sensor in vivo but did not discuss communication and control protocol, limiting themselves to just radio frequency (RF) energization in their work.
For an implantable bladder sensor that uses RF communication, a frequency in the low-MHz region provides a good compromise with respect to bandwidth and tissue absorption [
9]. The approach in Reference [
11] by Liao also focuses on the use of inductive coupling between internal and external coils for power transfer and energizing the in vivo circuitry, limiting the work to the final control element.
For treating chronic wounds, a smart wound dressing platform can be developed on a conformal flexible substrate that has electronics with physical, chemical, and biological modules for monitoring the wound physically and chemically and intervening [
12].
Gastrointestinal lesions and ulcers that require localized medication can benefit from a smart capsule that can release location-specific medication in the GI (gastrointestinal) tract. The smart capsule uses magnetic actuation from an externally worn magnet or an implanted magnetic marker for a proximity fuse that empties the drug reservoir [
13].
In Reference [
14], Gensler et al. tested a wirelessly controlled implantable system for on-demand and pulsatile insulin delivery. The system comprises an implanted magnetically driven pump (MDP), an external control device (ECD), and a mobile app. The MDP consists of a plunger, a barrel, and drug reservoir for infusing the correct amount of insulin when required. The ECD external to the subject’s body can actuate the MDP with an electromagnet that is wirelessly controlled by the mobile app. The system uses Bluetooth protocol between the app and the in vivo MDP. While Bluetooth can be used for a single channel application as a sensing and control protocol, in
Section 2 we discuss why it cannot work satisfactorily for an IoT-HSN with multiple channels.
The correct concentration of oxygen in solid tumors is an important factor that effects the efficacy of radiation therapy. Traditional techniques force patients to breathe an air mixture with higher oxygen content or breath pure oxygen in a pressurized room or tube as in hyperbaric oxygen therapy (HBOT). Maleki et al. [
15] developed an implantable micro-oxygen generator (IMOG) for an in vivo application to place inside a pancreatic tumor. The IMOG was powered with an ultrasonic transducer external to the body through the human body tissue. After it was energized, the device would use water present in the tissue for in situ electrolysis to generate oxygen. The development is significant and apt for in-situ applications. However, the control protocol to handle and energize the ultrasonic power transducer as and when required itself has not been tested by the authors or focused upon in the paper.
Negra et al. [
16] focused on applications and QoS requirements for networks used for remote healthcare monitoring, emergency rescue, disease detection and prevention, rehabilitation, biofeedback, and assisted living.
Zou et al. [
17] mentioned the use of actuators for control of some body functions based on the information received from sensors or a body control unit but did not discuss the actuator or its working in detail.
The article by Movassaghi et al. discussed the importance of improving speed, accuracy, and reliability of communication of sensors and actuators in a body area network [
18]. It also refers to a prior work on a ubiquitous healthcare application proposed by Wang and Park involving an actuator for pumping the right dose of medicine into a subject’s body [
19].
Antonescu and Basagni [
20] briefly mentioned the use of actuators for performing medicine administration on subjects based on sensor information or through user interaction.
In Reference [
21], Madsen et al. briefly discussed the use of an actuator for stimulation and muscle activation, and another real-time application involving injecting insulin into the subject based on a drop in the glucose level.
None of the research work in [
16,
17,
18,
19,
20,
21] discussed anything about bioactuators, their working or design considerations, unlike in the present work. Also, almost none of these approaches discussed the network interface beyond the final control element. There is hardly any published work focusing on the network protocol for such applications or testing the suitability of one for creating a standard.
2.3. Industrial Wireless Control
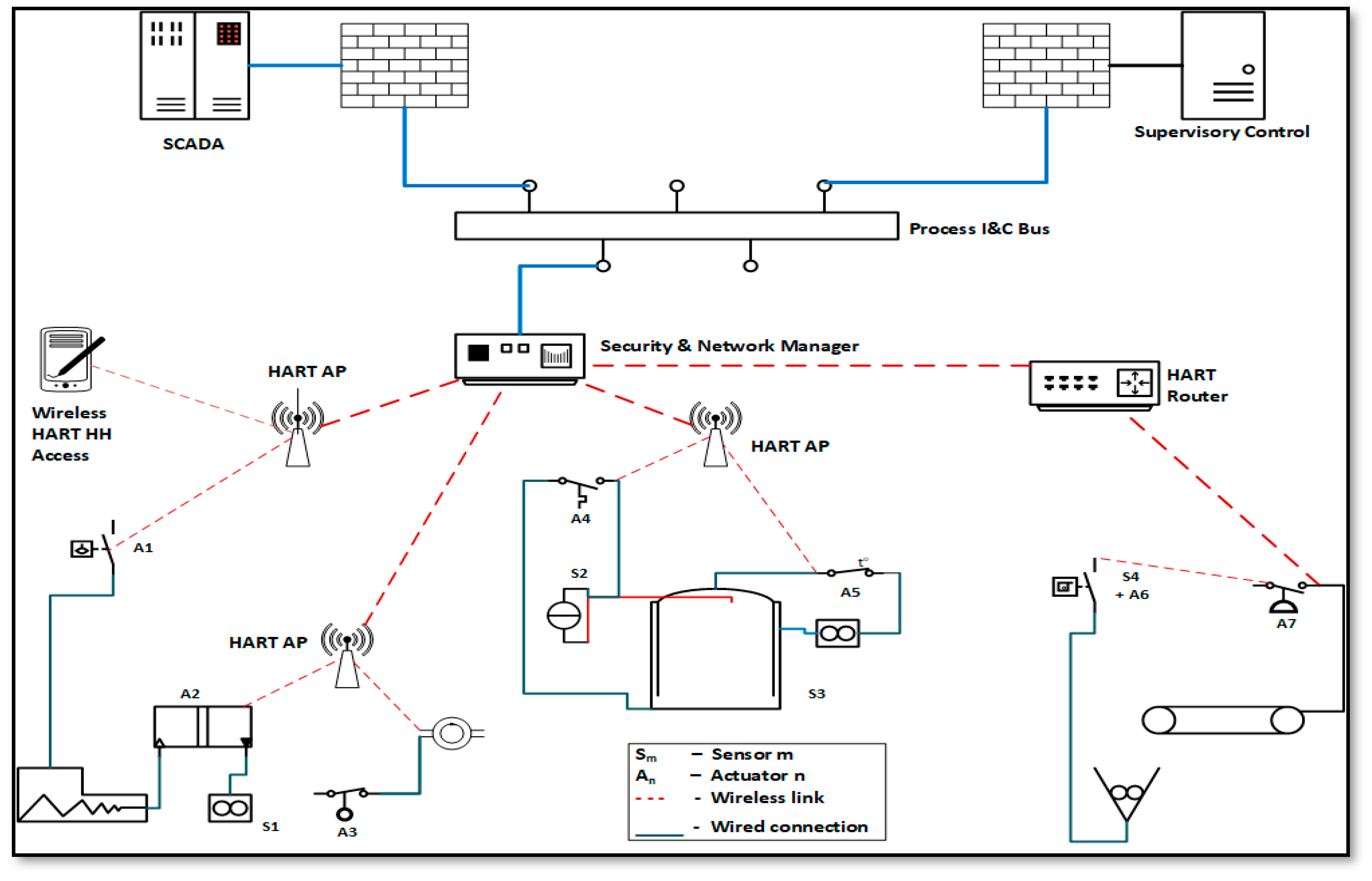
A simple example of an industrial automation application is adjusting the flow rate of the coolant through the cooling jacket surrounding a reactor for a specific, desired outcome. The outcome is to sustain a constant preset temperature for the reactor housing, where jacket temperature is the controlled variable, attained through change in the coolant flow rate, temperature or both. In such a system, all the devices were traditionally connected using wires. A thermal sensor measures the jacket temperature and transmits it to a controller, which uses a special function to decide the adjustment of a valve to manipulate the flow rate of the coolant through the cooling jacket. The controller also transmits the output to control the valve, handles input variations, and generates an alarm for faulty conditions. Sensor data are also archived for future reference. If WSN is used for this application, sensing and action devices will communicate over wireless links with an access point (e.g., a gateway or router), connected to the control station through a wired or wireless system.
Process control applications have stringent requirements and are mostly mission critical. Failure of a critical process control loop can cause accidents and an unscheduled plant shutdown. Researches have indicated the compelling benefits of migrating to wireless sensor technology, but a cautious approach is adopted by process technicians, with initial applications focusing just on process monitoring instead of closed-loop process control, despite wireless control standards being available.
2.3.1. Benefits of Going Wireless
Wireless sensor and control networks are easy to maintain and have no wiring constraints. Wired systems encounter maintenance problems such as physical cable wear, corrosion, cable burns, freezing, wild animal damage, and cost incurred in replacement. Existing wired systems work well with new wireless systems and do not need to be changed completely either. An important consideration is the choice of a right protocol for the application in question.
2.3.2. Evaluating Bluetooth Protocol for Control Applications in an IoT-HSN
Although Bluetooth is a common wireless protocol for short-range personal area networks (PANs), it cannot be used as a process control protocol involving multiple channels in a network due to bandwidth limitations. Newer Bluetooth versions like 3.0 need other technologies like WiFi to attain their full claimed bandwidth and are hence not applicable to pure PAN applications.
While the symbol rate on Bluetooth transmissions is claimed to be 1 megabits per second, the real data rate at an application is much less than that. The achievable data rate on Bluetooth is affected by the packet type. Single-slot packets utilize one 625-microsecond slot and can contain up to 27 bytes, offering a data rate of 108.8 kilobits per second in each direction between the sensors/actuators and the local coordinator station, which could be a smartphone. If five-slot packets are used, they can carry 339 bytes in 3125 microseconds, which theoretically enhances the data rate to 433.9 kilobits per second. To get even better data rates, it is possible to use an asymmetric channel. However, accommodating for higher layer losses (loss of payload bytes due to additions from RFCOMM, L2CAP, and HCI layers) reduces the achievable data rate drastically. As a result of such overheads, applications that just want to connect, transfer data, and disconnect will spend substantial time inquiring, paging, performing service discovery, and configuring links before they can even begin using link bandwidth for data transfer.
Even if the L2CAP packet is split into two high rate DH1 packets with each pair of packets carrying 28 bytes the data rate on air is lowered to 112.2 kilobytes per second. When split across 24 channels, this data rate would dwindle down to 4.7 kbps and would be insufficient for a 24-channel IoT-HSN, going by the QoS indicated in
Table 1. We should also remember that this is the maximum calculated data rate over air. This data rate would reduce while crossing the tissue interface due to body mass and fluids. While any protocols including Bluetooth could end up facing this limitation, Bluetooth would certainly suffer more being low in bandwidth to start with.
As Bluetooth would not be satisfactory for multi-channel IoT-HSN applications, we next examine standard industrial control protocols for suitability.
2.3.3. Evaluating Industrial Process Control Protocols for IoT-HSN Applications
The process control industry uses smart control equipment with in-built diagnostics that offer an enhanced understanding of the process at reduced engineering costs, and without any safety concerns. Industrial WSNs can outperform traditional, wired process control networks by running at higher data transmission speeds. HART (Highway Addressable Remote Transducer) is a popular control protocol with a data rate of 1.2 kbps, the FF (foundation fieldbus) runs at 31.25 kbps [
22] and WirelessHART (based on the IEEE 802.15.4 standard [
23]) tops the chart with 250 kbps with all the data accessible by mobile users too [
24].
Moreover, devices in wired control systems share a single bus, while multiple wireless communications can act simultaneously if there is no mutual radio interference, as put forth by Song et al. [
25]. Also, more wireless sensors/data-points can be used for a better performance.
The reliability of WSNs can be increased by redundancy in equipment and communication channels. Faulty sensors can also be detected and replaced as pointed out by Banerjee et al. [
26].
2.3.4. Wireless Industrial Applications
Working examples of wireless in control include a self-organizing mesh field network used to monitor wellhead annular pressure and heat exchanger pressures on an offshore platform [
27].
Temperature monitoring on a rotating drier to ensure that the proper temperature is reached and maintained during the drying process [
28] is another application where wiring costs are prohibitive and wireless temperature sensors are appropriate.
2.4. HART and WirelessHART
WirelessHART (Highway Addressable Remote Transducer) is one such open-standard wireless networking technology for process automation [
24]. Another such open-standard wireless technology was developed by ISA, the ISA100.11a [
29].
The HART protocol standard for wired, smart instrument-based process-control in the industry has ensured that devices from multiple suppliers work together since the late eighties. The population of HART devices in use is close to 50 million in the world today, totaling up to 75% population of all smart devices deployed. WirelessHART is getting robust and secure and is being tested in IoT applications other than HSN. This is the main reason behind our choice of WirelessHART as the protocol for this evaluation.
2.4.1. WirelessHART Protocol
The HART Field Communications Protocol standard [
22] allows piggybacking of two-way communications on a 4–20 mA standard instrumentation signal while not interfering with the integrity of sensed values.
The current version HART 7 includes a new WirelessHART communication protocol [
24] that targets fixed biosensors, bioactuators, and rotating equipment and has wireless mesh capability with time sync, along with transport and network layers. In addition, the WirelessHART standard leverages other existing standards such as the IEEE-802.15.4 standard [
30], AES-128 encryption [
31], and DDL/EDDL [
32]. The WirelessHART standard provides a 128-bit AES encrypted secure networking technology operating in the 2.4 GHz ISM radio band. It utilizes IEEE 802.15.4 compatible DSSS radios with packet by packet channel hopping [
33] for improving reliability and avoiding interference from metallic plant equipment. It supports high speed piped data communication, block transfers, security with encryption/decryption, event notifications, and advanced diagnostics with very good dynamic performance. The biggest advantage of WirelessHART is that it relieves a user from the tedious manual labor-intensive tasks involved in laying, documentation, and maintaining wiring cables.
WirelessHART devices can be easily scaled up at low cost or seamlessly integrated in no time with a HART wired network due to backward compatibility. WirelessHART mesh is a flexible, adaptive network with self-organizing and self-healing capabilities that can coexist with other wireless networks without issues. It monitors any degradation of communication links and keeps mending and adapting the network for optimal performance. It determines alternative routes around obstacles and keeps hopping channels for routing.
Use of WirelessHART links would help with better management of remote plant areas. Additional diagnostics smoothen out troubleshooting and maintenance of instrumentation loops. Supervisory compliance monitoring in environmental, safety, and health would benefit highly from the use of WirelessHART.
2.4.2. WirelessHART Industrial Applications
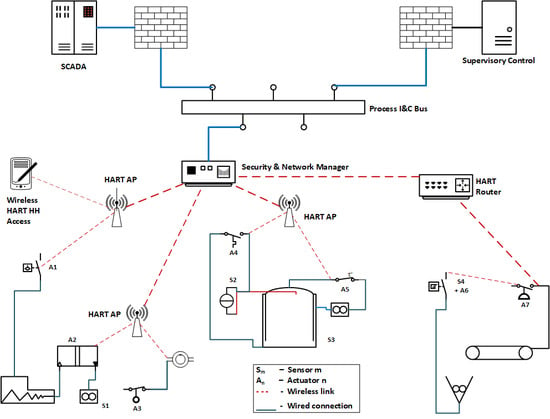
IoT-HSN control applications could possibly use WirelessHART just like an industrial control application does. WirelessHART has an optimal data rate of 250 kbps for handling the relay of both sensor and control data safely. The control design can be redundant to improve the reliability of control.
Figure 1 shows that modeling an industrial control system using WirelessHART is trivial, but we will try to evaluate if WirelessHART could work for an IoT-HSN working on 802.15.6 protocol for possible HSN control applications.