Biophysical and Lipidomic Biomarkers of Cardiac Remodeling Post-Myocardial Infarction in Humans
Abstract
1. Introduction
2. Materials and Methods
2.1. Collection of Human Samples
2.2. Tissue Homogenization and Preparation of the Samples for the Different Studies
2.3. Immunohistochemical Analysis
2.4. Vibrational Characterization
2.5. Differential Scanning Calorimetry
2.6. Lipidomic Analysis of the Heart
2.6.1. Phospholipids and Neutral Lipids
2.6.2. Sphingolipids
2.6.3. UPLC Coupled to HRMS Analysis
2.7. Statistical Analysis
3. Results
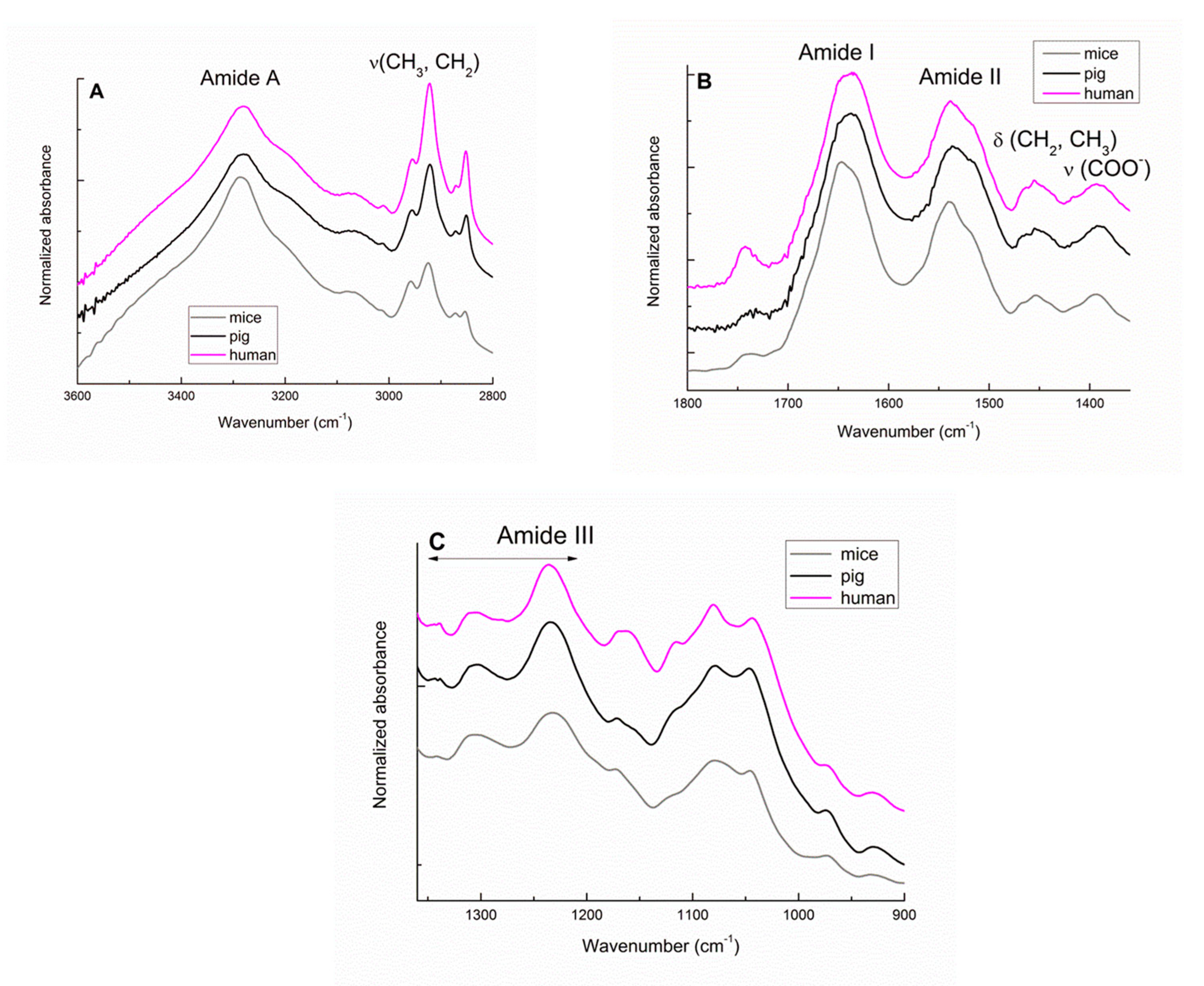
3.1. Identification of the Main FTIR Bands in the Human Heart
3.2. Characterization of the Human Heart Lipidome
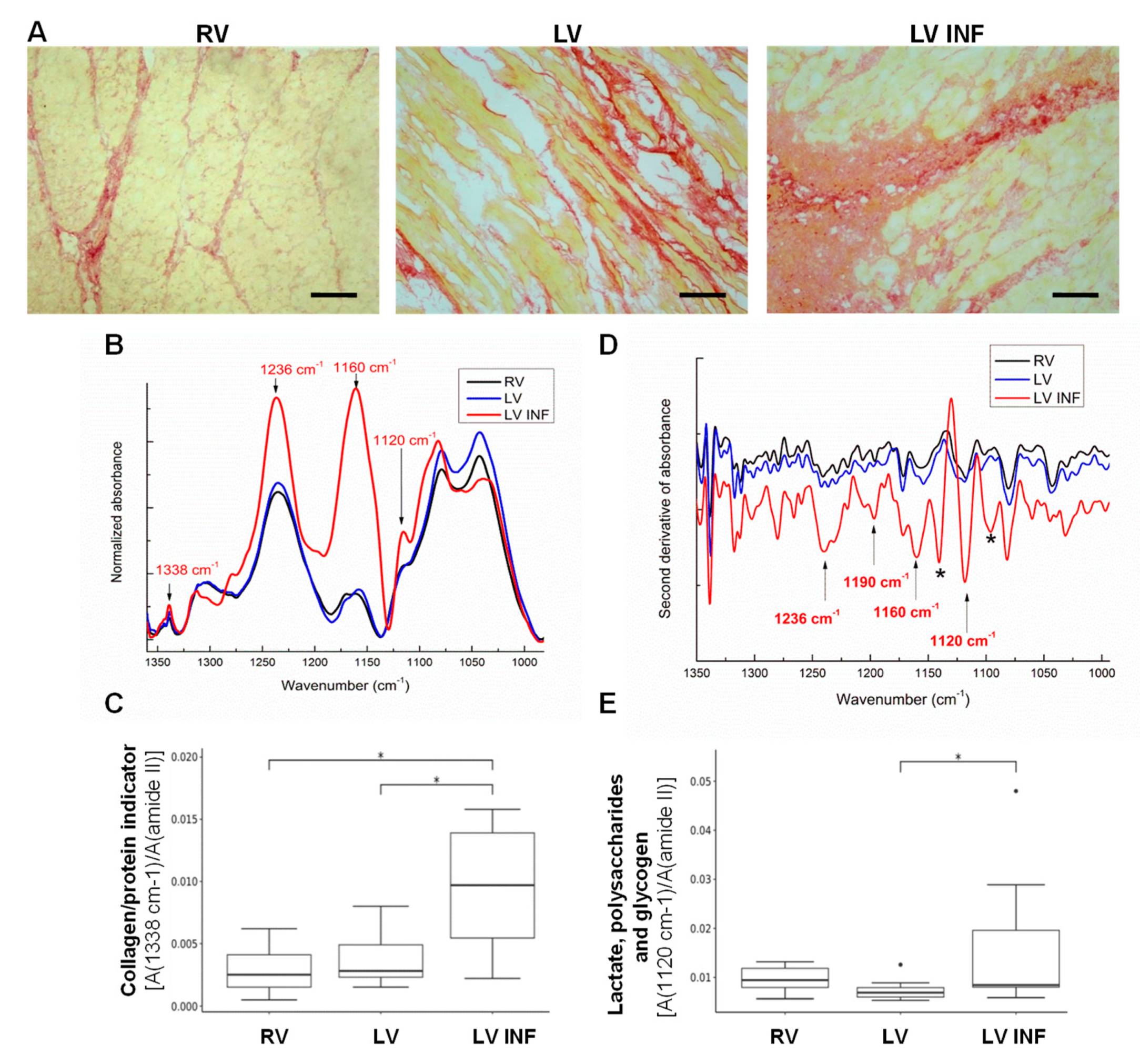
3.3. Identification of the Alterations of the FTIR Bands Related to Myofibers and Structural Extracellular Matrix Proteins in Human LV INF compared to LV and RV
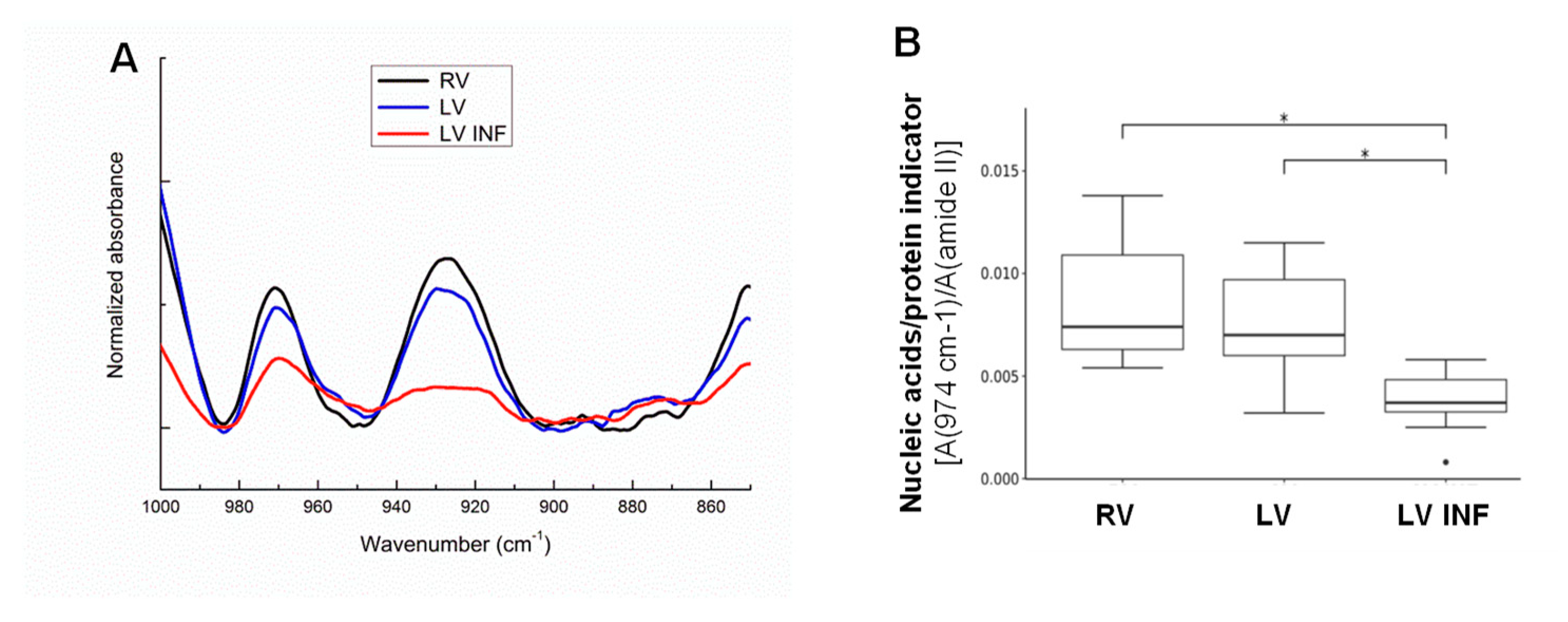
3.4. Identification of the Alterations in the FTIR Bands Corresponding to DNA Response in Human LV INF Compared to LV and RV
3.5. Study of the Hydric Response of Human RV, LV and LV INF
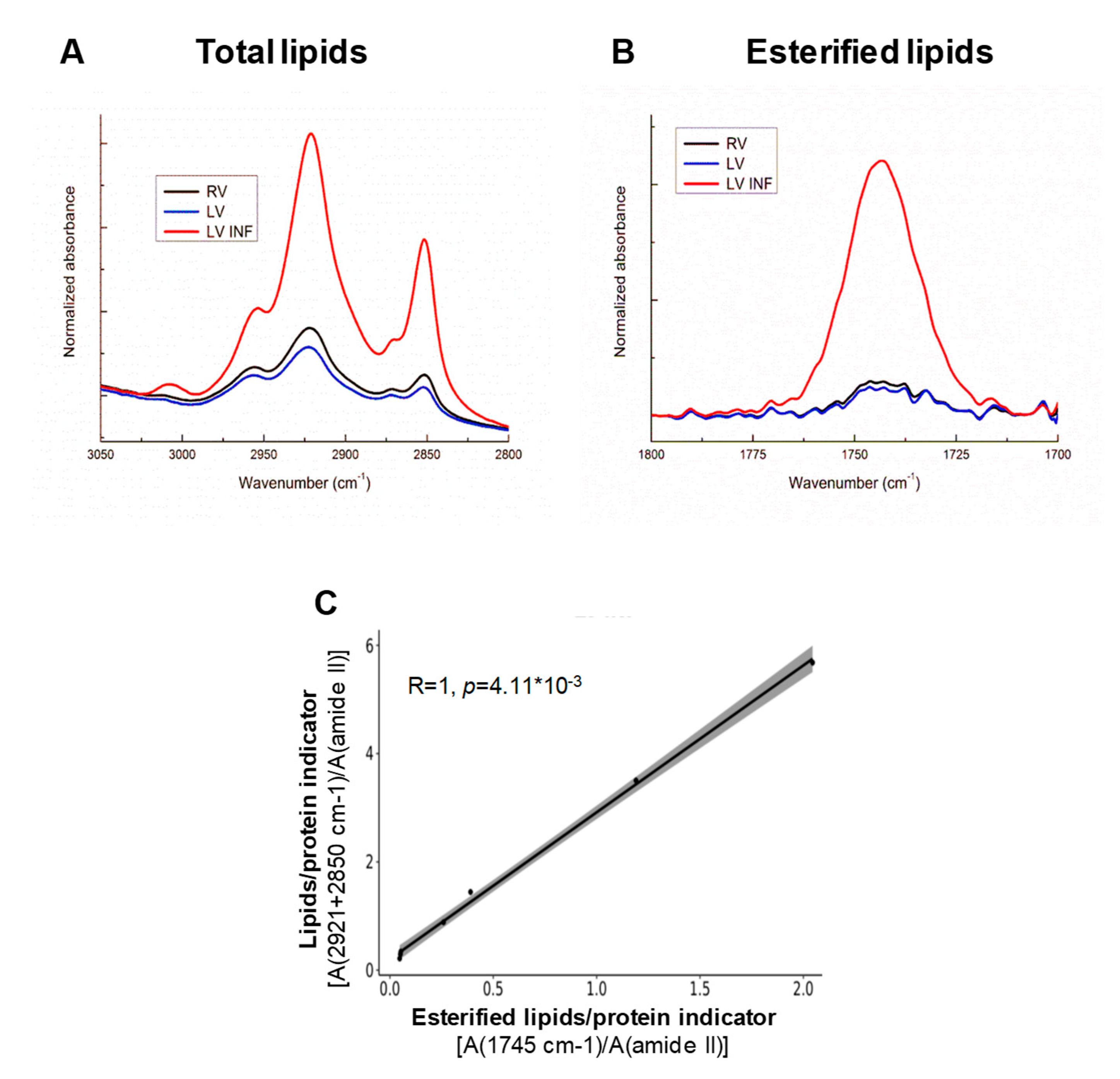
3.6. Study of the Associations between FITR Variables in Human RV, LV and LV INF
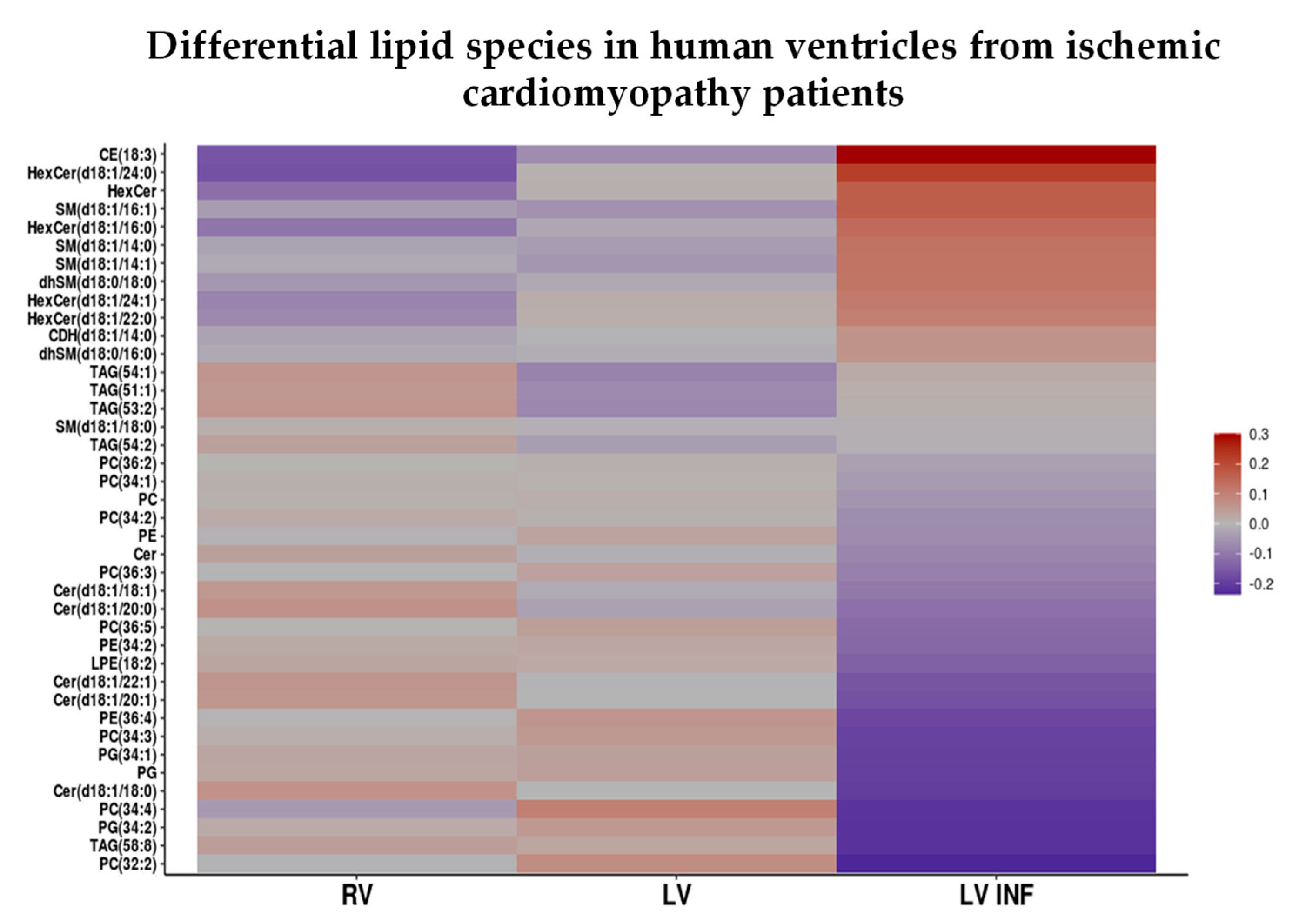
3.7. Identification of the Alterations in Sphingolipids, Glycerophospholipids and Neutral Lipids in Human LV INF Compared to LV and RV
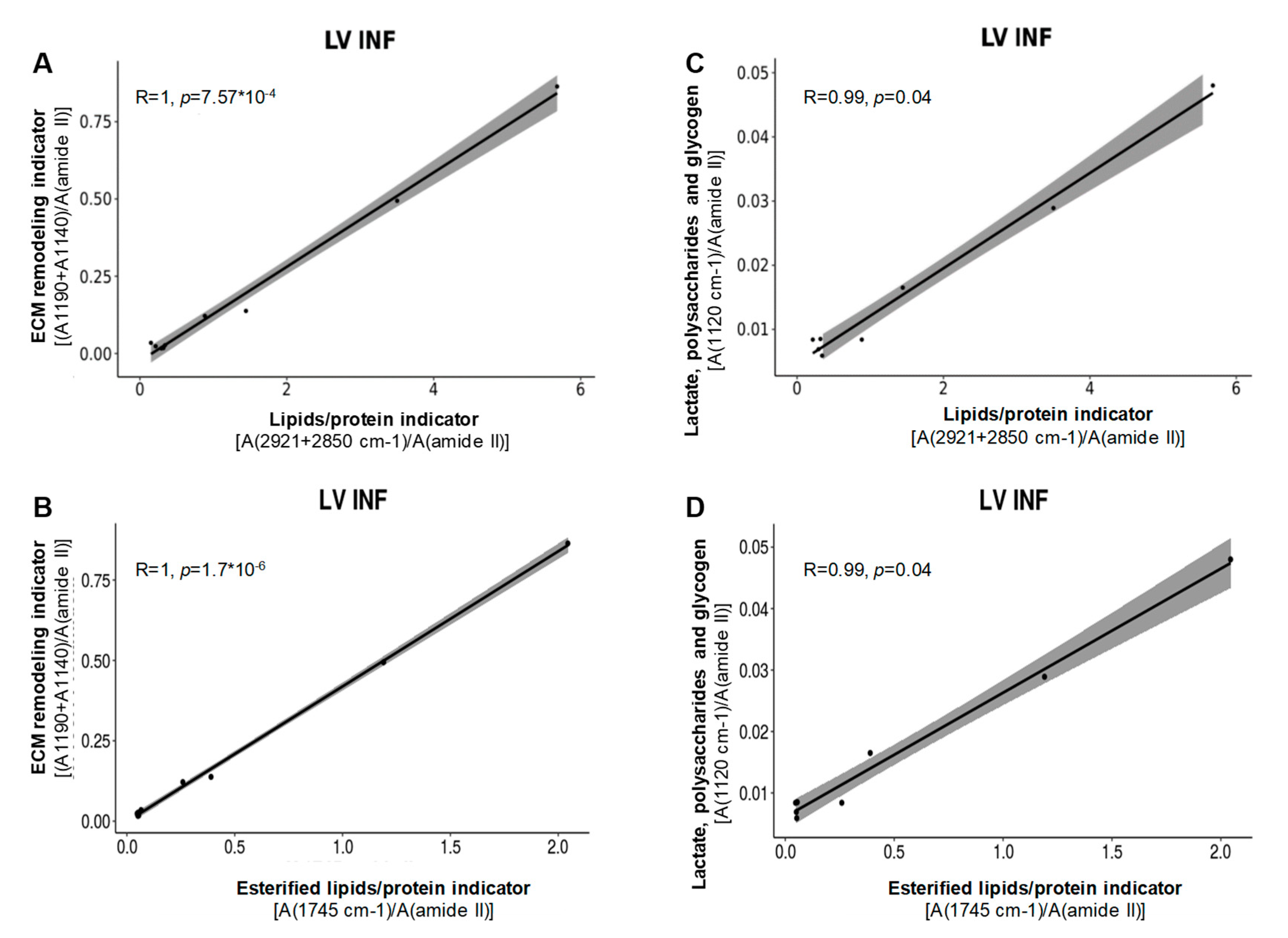
3.8. Study of the Association between FTIR and Lipidomic Variables in RV, LV and LV INF
4. Discussion
5. Conclusions
Limitations of This Study
Supplementary Materials
Author Contributions
Funding
Conflicts of Interest
References
- Pfeffer, M.A.; Braunwald, E. Ventricular remodeling after myocardial infarction. Experimental observations and clinical implications. Circulation 1990, 81, 1161–1172. [Google Scholar] [CrossRef] [PubMed]
- Opie, L.H.; Commerford, P.J.; Gersh, B.J.; Pfeffer, M.A. Controversies in ventricular remodelling. Lancet 2006, 367, 356–367. [Google Scholar] [CrossRef]
- Jugdutt, B.I. Ventricular remodeling after infarction and the extracellular collagen matrix: When is enough enough? Circulation 2003, 108, 1395–1403. [Google Scholar] [CrossRef] [PubMed]
- Samouillan, V.; Revuelta-López, E.; Soler-Botija, C.; Dandurand, J.; Benitez-Amaro, A.; Nasarre, L.; de Gonzalo-Calvo, D.; Bayes-Genis, A.; Lacabanne, C.; Llorente-Cortés, V. Conformational and thermal characterization of left ventricle remodeling post-myocardial infarction. Biochim. Biophys. Acta-Mol. Basis Dis. 2017, 1863, 1500–1509. [Google Scholar] [CrossRef] [PubMed]
- Benitez-Amaro, A.; Samouillan, V.; Jorge, E.; Dandurand, J.; Nasarre, L.; de Gonzalo-Calvo, D.; Bornachea, O.; Amoros-Figueras, G.; Lacabanne, C.; Vilades, D.; et al. Identification of new biophysical markers for pathological ventricular remodelling in tachycardia-induced dilated cardiomyopathy. J. Cell. Mol. Med. 2018, 22, 4197–4208. [Google Scholar] [CrossRef] [PubMed]
- Cheheltani, R.; Rosano, J.M.; Wang, B.; Sabri, A.K.; Pleshko, N.; Kiani, M.F. Fourier transform infrared spectroscopic imaging of cardiac tissue to detect collagen deposition after myocardial infarction. J. Biomed. Opt. 2012, 17, 56014. [Google Scholar] [CrossRef]
- Kong, J.; Yu, S. Fourier Transform Infrared Spectroscopic Analysis of Protein Secondary Structures Protein FTIR Data Analysis and Band Assign- ment. Acta Biochim. Biophys. Sin. 2007, 39, 549–559. [Google Scholar] [CrossRef]
- Amorim, P.A.; Nguyen, T.D.; Shingu, Y.; Schwarzer, M.; Mohr, F.W.; Schrepper, A.; Doenst, T. Myocardial infarction in rats causes partial impairment in insulin response associated with reduced fatty acid oxidation and mitochondrial gene expression. J. Thorac. Cardiovasc. Surg. 2010, 140, 1160–1167. [Google Scholar] [CrossRef]
- Heather, L.C.; Clarke, K. Metabolism, hypoxia and the diabetic heart. J. Mol. Cell. Cardiol. 2011, 50, 598–605. [Google Scholar] [CrossRef]
- Rosenblatt-Velin, N.; Montessuit, C.; Papageorgiou, I.; Terrand, J.; Lerch, R. Postinfarction heart failure in rats is associated with upregulation of GLUT-1 and downregulation of genes of fatty acid metabolism. Cardiovasc. Res. 2001, 52, 407–416. [Google Scholar] [CrossRef]
- Cal, R.; Castellano, J.; Revuelta-López, E.; Aledo, R.; Barriga, M.; Farré, J.; Vilahur, G.; Nasarre, L.; Hove-Madsen, L.; Badimon, L.; et al. Low-density lipoprotein receptor-related protein 1 mediates hypoxia-induced very low density lipoprotein-cholesteryl ester uptake and accumulation in cardiomyocytes. Cardiovasc. Res. 2012, 94, 469–479. [Google Scholar] [CrossRef]
- Cal, R.; Juan-Babot, O.; Brossa, V.; Roura, S.; Gálvez-Montón, C.; Portoles, M.; Rivera, M.; Cinca, J.; Badimon, L.; Llorente-Cortés, V. Low density lipoprotein receptor-related protein 1 expression correlates with cholesteryl ester accumulation in the myocardium of ischemic cardiomyopathy patients. J. Transl. Med. 2012, 10, 160. [Google Scholar] [CrossRef]
- Drevinge, C.; Karlsson, L.O.; Ståhlman, M.; Larsson, T.; Perman Sundelin, J.; Grip, L.; Andersson, L.; Borén, J.; Levin, M.C. Cholesteryl Esters Accumulate in the Heart in a Porcine Model of Ischemia and Reperfusion. PLoS ONE 2013, 8, e61942. [Google Scholar] [CrossRef]
- De Lima, A.D.; Guido, M.C.; Tavares, E.R.; Carvalho, P.O.; Marques, A.F.; de Melo, M.D.T.; Salemi, V.M.C.; Kalil-Filho, R.; Maranhão, R.C. The Expression of Lipoprotein Receptors Is Increased in the Infarcted Area After Myocardial Infarction Induced in Rats With Cardiac Dysfunction. Lipids 2018, 53, 177–187. [Google Scholar] [CrossRef]
- Goldfarb, J.W.; Roth, M.; Han, J. Myocardial fat deposition after left ventricular myocardial infarction: Assessment by using MR water-fat separation imaging. Radiology 2009, 253, 65–73. [Google Scholar] [CrossRef] [PubMed]
- Turer, A.T. Using metabolomics to assess myocardial metabolism and energetics in heart failure. J. Mol. Cell. Cardiol. 2013, 55, 12–18. [Google Scholar] [CrossRef]
- Nam, M.; Jung, Y.; Ryu, D.H.; Hwang, G.S. A metabolomics-driven approach reveals metabolic responses and mechanisms in the rat heart following myocardial infarction. Int. J. Cardiol. 2017, 227, 239–246. [Google Scholar] [CrossRef]
- Feng, L.; Yang, J.; Liu, W.; Wang, Q.; Wang, H.; Shi, L.; Fu, L.; Xu, Q.; Wang, B.; Li, T. Lipid biomarkers in acute myocardial infarction before and after percutaneous coronary intervention by lipidomics analysis. Med. Sci. Monit. 2018, 24, 4175–4182. [Google Scholar] [CrossRef]
- Mundra, P.A.; Barlow, C.K.; Nestel, P.J.; Barnes, E.H.; Kirby, A.; Thompson, P.; Sullivan, D.R.; Alshehry, Z.H.; Mellett, N.A.; Huynh, K.; et al. Large-scale plasma lipidomic profiling identifies lipids that predict cardiovascular events in secondary prevention. JCI Insight 2018, 3. [Google Scholar] [CrossRef]
- Floegel, A.; Kühn, T.; Sookthai, D.; Johnson, T.; Prehn, C.; Rolle-Kampczyk, U.; Otto, W.; Weikert, C.; Illig, T.; von Bergen, M.; et al. Serum metabolites and risk of myocardial infarction and ischemic stroke: A targeted metabolomic approach in two German prospective cohorts. Eur. J. Epidemiol. 2018, 33, 55–66. [Google Scholar] [CrossRef]
- Lewis, G.D.; Asnani, A.; Gerszten, R.E. Application of Metabolomics to Cardiovascular Biomarker and Pathway Discovery. J. Am. Coll. Cardiol. 2008, 52, 117–123. [Google Scholar] [CrossRef] [PubMed]
- Dang, V.T.; Huang, A.; Werstuck, G.H. Untargeted Metabolomics in the Discovery of Novel Biomarkers and Therapeutic Targets for Atherosclerotic Cardiovascular Diseases. Cardiovasc. Hematol. Disord. Targets 2018, 18, 166–175. [Google Scholar] [CrossRef] [PubMed]
- Swedberg, K.; Cleland, J.; Dargie, H.; Drexler, H.; Follath, F.; Komajda, M.; Tavazzi, L.; Smiseth, O.A.; Gavazzi, A.; Haverich, A.; et al. Guidelines for the diagnosis and treatment of chronic heart failure: Executive summary (update 2005). Eur. Heart J. 2005, 26, 1115–1140. [Google Scholar] [CrossRef]
- Kiernan, J.A. Histological and Histochemical Methods: Theory and Practice, 3rd ed.; Butterworth Heinemann: Oxford, UK, 1999; Volume 12, p. 679. [Google Scholar]
- Staniszewska, E.; Malek, K.; Baranska, M. Rapid approach to analyze biochemical variation in rat organs by ATR FTIR spectroscopy. Spectrochim. Acta. A Mol. Biomol. Spectrosc. 2014, 118, 981–986. [Google Scholar] [CrossRef]
- Wang, Q.; Sanad, W.; Miller, L.M.; Voigt, A.; Klingel, K.; Kandolf, R.; Stangl, K.; Baumann, G. Infrared imaging of compositional changes in inflammatory cardiomyopathy. Vib. Spectrosc. 2005, 38, 217–222. [Google Scholar] [CrossRef]
- Simbari, F.; McCaskill, J.; Coakley, G.; Millar, M.; Maizels, R.M.; Fabriás, G.; Casas, J.; Buck, A.H. Plasmalogen enrichment in exosomes secreted by a nematode parasite versus those derived from its mouse host: Implications for exosome stability and biology. J. Extracell. Vesicles 2016, 5, 30741. [Google Scholar] [CrossRef]
- Weber, M.; Mera, P.; Casas, J.; Salvador, J.; Rodríguez, A.; Alonso, S.; Sebastián, D.; Soler-Vázquez, M.C.; Montironi, C.; Recalde, S.; et al. Liver CPT1A gene therapy reduces diet-induced hepatic steatosis in mice and highlights potential lipid biomarkers for human NAFLD. FASEB J. 2020, 34, 11816–11837. [Google Scholar] [CrossRef]
- R Core Team. R: A Language and Environment for Statistical Computing 2020. R Foundation for Statistical Computing: Vienna, Austria. Available online: https://www.R-project.org/ (accessed on 21 October 2020).
- Bozkurt, O.; Severcan, M.; Severcan, F. Diabetes induces compositional, structural and functional alterations on rat skeletal soleus muscle revealed by FTIR spectroscopy: A comparative study with EDL muscle. Analyst 2010, 135, 3110. [Google Scholar] [CrossRef]
- Gough, K.M.; Zelinski, D.; Wiens, R.; Rak, M.; Dixon, I.M.C. Fourier transform infrared evaluation of microscopic scarring in the cardiomyopathic heart: Effect of chronic AT1 suppression. Anal. Biochem. 2003, 316, 232–242. [Google Scholar] [CrossRef]
- Jerônimo, D.P.; de Souza, R.A.; da Silva, F.F.; Camargo, G.L.; Miranda, H.L.; Xavier, M.; Sakane, K.K.; Ribeiro, W. Detection of creatine in rat muscle by FTIR spectroscopy. Ann. Biomed. Eng. 2012, 40, 2069–2077. [Google Scholar] [CrossRef]
- Kirschner, C.; Ofstad, R.; Skarpeid, H.-J.; Høst, V.; Kohler, A. Monitoring of denaturation processes in aged beef loin by Fourier transform infrared microspectroscopy. J. Agric. Food Chem. 2004, 52, 3920–3929. [Google Scholar] [CrossRef]
- Petibois, C.; Gouspillou, G.; Wehbe, K.; Delage, J.-P.; Déléris, G. Analysis of type I and IV collagens by FT-IR spectroscopy and imaging for a molecular investigation of skeletal muscle connective tissue. Anal. Bioanal. Chem. 2006, 386, 1961–1966. [Google Scholar] [CrossRef]
- Zohdi, V.; Wood, B.R.; Pearson, J.T.; Bambery, K.R.; Black, M.J. Evidence of altered biochemical composition in the hearts of adult intrauterine growth-restricted rats. Eur. J. Nutr. 2013, 52, 749–758. [Google Scholar] [CrossRef]
- Belbachir, K.; Noreen, R.; Gouspillou, G.; Petibois, C. Collagen types analysis and differentiation by FTIR spectroscopy. Anal. Bioanal. Chem. 2009, 395, 829–837. [Google Scholar] [CrossRef]
- Wood, B.R. The importance of hydration and DNA conformation in interpreting infrared spectra of cells and tissues. Chem. Soc. Rev. 2016, 45, 1980–1998. [Google Scholar] [CrossRef]
- Yang, T.T.; Weng, S.F.; Zheng, N.; Pan, Q.H.; Cao, H.L.; Liu, L.; Zhang, H.D.; Mu, D.W. Histopathology mapping of biochemical changes in myocardial infarction by Fourier transform infrared spectral imaging. Forensic Sci. Int. 2011, 207, e34–e39. [Google Scholar] [CrossRef] [PubMed]
- Landry, M.R. Thermoporometry by differential scanning calorimetry: Experimental considerations and applications. Thermochim. Acta 2005, 433, 27–50. [Google Scholar] [CrossRef]
- Fathima, N.N.; Kumar, M.P.; Rao, J.R.; Nair, B.U. A DSC investigation on the changes in pore structure of skin during leather processing. Thermochim. Acta 2010, 501, 98–102. [Google Scholar] [CrossRef]
- Mignolet, A.; Derenne, A.; Smolina, M.; Wood, B.R.; Goormaghtigh, E. FTIR spectral signature of anticancer drugs. Can drug mode of action be identified? Biochim. Biophys. Acta-Proteins Proteom. 2016, 1864, 85–101. [Google Scholar] [CrossRef] [PubMed]
- Zhang, D.X.; Fryer, R.M.; Hsu, A.K.; Zou, A.P.; Gross, G.J.; Campbell, W.B.; Li, P.L. Production and metabolism of ceramide in normal and ischemic-reperfused myocardium of rats. Basic Res. Cardiol. 2001, 96, 267–274. [Google Scholar] [CrossRef]
- Wang, H.-Y.J.; Liu, C.B.; Wu, H.-W.; Kuo, S., Jr. Direct profiling of phospholipids and lysophospholipids in rat brain sections after ischemic stroke. Rapid Commun. Mass Spectrom. 2010, 24, 2057–2064. [Google Scholar] [CrossRef]
- Beresewicz, A.; Dobrzyn, A.; Gorski, J. Accumulation of specific ceramides in ischemic/reperfused rat heart; effect of ischemic preconditioning. J. Physiol. Pharmacol. 2002, 53, 371–382. [Google Scholar]
- Bielawska, A.E.; Shapiro, J.P.; Jiang, L.; Melkonyan, H.S.; Piot, C.; Wolfe, C.L.; Tomei, L.D.; Hannun, Y.A.; Umansky, S.R. Ceramide is involved in triggering of cardiomyocyte apoptosis induced by ischemia and reperfusion. Am. J. Pathol. 1997, 151, 1257–1263. [Google Scholar] [PubMed]
- Hadas, Y.; Vincek, A.S.; Youssef, E.; Żak, M.M.; Chepurko, E.; Sultana, N.; Sharkar, M.T.K.; Guo, N.; Komargodski, R.; Kurian, A.A.; et al. Altering sphingolipid metabolism attenuates cell death and inflammatory response after myocardial infarction. Circulation 2020, 141, 916–930. [Google Scholar] [CrossRef] [PubMed]
- Hernández-Corbacho, M.J.; Jenkins, R.W.; Clarke, C.J.; Hannun, Y.A.; Obeid, L.M.; Snider, A.J.; Siskind, L.J. Accumulation of long-chain glycosphingolipids during aging is prevented by caloric restriction. PLoS ONE 2011, 6, e20411. [Google Scholar] [CrossRef]
- Trayssac, M.; Hannun, Y.A.; Obeid, L.M. Role of sphingolipids in senescence: Implication in aging and age-related diseases. J. Clin. Investig. 2018, 128, 2702–2712. [Google Scholar] [CrossRef]
- Laaksonen, R.; Ekroos, K.; Sysi-Aho, M.; Hilvo, M.; Vihervaara, T.; Kauhanen, D.; Suoniemi, M.; Hurme, R.; März, W.; Scharnagl, H.; et al. Plasma ceramides predict cardiovascular death in patients with stable coronary artery disease and acute coronary syndromes beyond LDL-cholesterol. Eur. Heart J. 2016, 37, 1967–1976. [Google Scholar] [CrossRef]
- Wang, D.D.; Toledo, E.; Hruby, A.; Rosner, B.A.; Willett, W.C.; Sun, Q.; Razquin, C.; Zheng, Y.; Ruiz-Canela, M.; Guasch-Ferré, M.; et al. Plasma ceramides, mediterranean diet, and incident cardiovascular disease in the PREDIMED trial (prevención con dieta mediterránea). Circulation 2017, 135, 2028–2040. [Google Scholar] [CrossRef]
- Hazen, S.L.; Ford, D.A.; Gross, R.W. Activation of a membrane-associated phospholipase A2 during rabbit myocardial ischemia which is highly selective for plasmalogen substrate. J. Biol. Chem. 1991, 266, 5629–5633. [Google Scholar]
- Ford, D.A.; Hazen, S.L.; Saffitz, J.E.; Gross, R.W. The rapid and reversible activation of a calcium-independent plasmalogen-selective phospholipase A2 during myocardial ischemia. J. Clin. Investig. 1991, 88, 331–335. [Google Scholar] [CrossRef]
- Chen, W.W.; Chao, Y.J.; Chang, W.H.; Chan, J.F.; Hsu, Y.H.H. Phosphatidylglycerol Incorporates into Cardiolipin to Improve Mitochondrial Activity and Inhibits Inflammation. Sci. Rep. 2018, 8. [Google Scholar] [CrossRef]
- Pokorná, L.; Čermáková, P.; Horváth, A.; Baile, M.G.; Claypool, S.M.; Griač, P.; Malínský, J.; Balážová, M. Specific degradation of phosphatidylglycerol is necessary for proper mitochondrial morphology and function. Biochim. Biophys. Acta 2016, 1857, 34–45. [Google Scholar] [CrossRef]
- Castellano, J.; Aledo, R.; Sendra, J.; Costales, P.; Juan-Babot, O.; Badimon, L.; Llorente-Cortés, V. Hypoxia stimulates low-density lipoprotein receptor-related protein-1 expression through hypoxia-inducible factor-1α in human vascular smooth muscle cells. Arterioscler. Thromb. Vasc. Biol. 2011, 31, 1411–1420. [Google Scholar] [CrossRef]
- Castellano, J.; Farré, J.; Fernandes, J.; Bayes-Genis, A.; Cinca, J.; Badimon, L.; Hove-Madsen, L.; Llorente-Cortés, V. Hypoxia exacerbates Ca(2+)-handling disturbances induced by very low density lipoproteins (VLDL) in neonatal rat cardiomyocytes. J. Mol. Cell. Cardiol. 2011, 50, 894–902. [Google Scholar] [CrossRef]
- Samouillan, V.; Revuelta-López, E.; Dandurand, J.; Nasarre, L.; Badimon, L.; Lacabanne, C.; Llorente-Cortés, V. Cardiomyocyte intracellular cholesteryl ester accumulation promotes tropoelastin physical alteration and degradation: Role of LRP1 and cathepsin S. Int. J. Biochem. Cell Biol. 2014, 55, 209–219. [Google Scholar] [CrossRef]
- Goldberg, I.J.; Reue, K.; Abumrad, N.A.; Bickel, P.E.; Cohen, S.; Fisher, E.A.; Galis, Z.S.; Granneman, J.G.; Lewandowski, E.D.; Murphy, R.; et al. Deciphering the role of lipid droplets in cardiovascular disease. Circulation 2018, 138, 305–315. [Google Scholar] [CrossRef]
- Thiam, A.R.; Beller, M. The why, when and how of lipid droplet diversity. J. Cell Sci. 2017, 130, 315–324. [Google Scholar] [CrossRef]
| ICM (n = 9) | |
|---|---|
| Age (years) | 57.67 ± 12.02 |
| Gender male (%) | 78 |
| Prior Hypertension (%) | 44 |
| Diabetes mellitus (%) | 11 |
| Dislipemia (%) | 75 |
| Perfusion abnormalities * (%) | 72 |
| Echo-Doppler study | |
| Ejection fraction (%) | 29.88 ± 8.90 |
| Intraventricular septum in diastole (mm) | 11.63 ± 4.63 |
| Left ventricular posterior wall in diastole (mm) | 9.53 ± 0.75 |
| Left ventricular end-diastolic diameter (mm) | 60.38 ± 14.15 |
| Left ventricular end-systolic diameter (mm) | 56.25 ± 2.79 |
| Treatment (%) | |
| Diuretics | 89 |
| Angiotensin-converting enzyme inhibitors | 86 |
| β-blockers | 48 |
| Aldosteron antagonists | 71 |
| Digoxin | 49 |
| Statins | 82 |
| Variable | RV | LV | LV INF | p vs. LV | p vs. RV |
|---|---|---|---|---|---|
| SM(d18:1/14:0) | 308.5 ± 77.4 | 309.5 ± 95.9 | 430.5 ± 95.3 | 0.024 | 0.055 |
| SM(d18:1/14:1) | 3 ± 1.2 | 2.8 ± 1 | 3.9 ± 1.4 | 0.029 | 0.096 |
| SM(d18:1/16:1) | 164 ± 39.5 | 160.1 ± 56.8 | 258.8 ± 105.8 | 0.029 | 0.041 |
| SM(d18:1/18:0) | 1199.2 ± 156.3 | 1138.7 ± 128.5 | 1086.2 ± 142.7 | 0.485 | 0.038 |
| Total Cer | 753 ± 261.6 | 592.7 ± 240.1 | 549.5 ± 179.1 | 0.932 | 0.044 |
| Cer(d18:1/18:0) | 30.4 ± 13.5 | 22.9 ± 14.5 | 15 ± 4.9 | 0.115 | 0.029 |
| Cer(d18:1/18:1) | 7.2 ± 2.3 | 5.2 ± 2 | 4.6 ± 1.1 | 0.456 | 0.006 |
| Cer(d18:1/20:0) | 14.5 ± 3.6 | 11.1 ± 4 | 9.6 ± 2.8 | 0.457 | 0.01 |
| Cer(d18:1/20:1) | 4.4 ± 0.8 | 3.4 ± 1.3 | 2.6 ± 0.6 | 0.13 | 0.006 |
| Cer(d18:1/22:1) | 28.7 ± 22.9 | 20.2 ± 16.1 | 17.5 ± 20.1 | 0.804 | 0.018 |
| dhSM(d18:0/16:0) | 179.4 ± 41.3 | 207.5 ± 91.7 | 226.4 ± 65 | 0.931 | 0.029 |
| dhSM(d18:1/18:0) | 46.3 ± 13.4 | 49.5 ± 23.3 | 64.5 ± 16.3 | 0.174 | 0.041 |
| Total HexCer | 48.1 ± 26.6 | 63.9 ± 31.2 | 91.3 ± 36.6 | 0.114 | 0.006 |
| HexCer(d18:1/16:0) | 2.3 ± 1.5 | 3.2 ± 1.7 | 4.4 ± 3.1 | 0.474 | 0.023 |
| HexCer(d18:1/22:0) | 10.9 ± 5.8 | 16.1 ± 13.2 | 16 ± 5.6 | 1 | 0.012 |
| HexCer(d18:1/24:0) | 19.6 ± 10.4 | 25.3 ± 13.6 | 44.3 ± 25.1 | 0.127 | 0.018 |
| HexCer(d18:1/24:1) | 15.5 ± 10.5 | 20 ± 5.6 | 26.7 ± 13.5 | 0.102 | 0.006 |
| Variable | RV | LV | LV INF | p vs. LV | p vs. RV |
|---|---|---|---|---|---|
| Total PC | 54,624.9 ± 11408.6 | 56,737 ± 5670.8 | 48,392.9 ± 4893.7 | 0.012 | 0.335 |
| PC(32:2) | 342.5 ± 146.2 | 389.6 ± 115.9 | 221.1 ± 103.4 | 0.029 | 0.102 |
| PC(34:1) | 14,602.8 ± 2506.6 | 15,143.9 ± 1769.8 | 13,505.1 ± 1492.7 | 0.029 | 0.556 |
| PC(34:2) | 13,397 ± 2572.8 | 13,827.1 ± 1685 | 11,574.9 ± 1501.8 | 0.006 | 0.232 |
| PC(34:3) | 120.7 ± 54.3 | 133.2 ± 46.3 | 71.9 ± 21.8 | 0.012 | 0.049 |
| PC(34:4) | 100.7 ± 52.6 | 133.8 ± 67.5 | 64.7 ± 34.1 | 0.041 | 0.077 |
| PC(36:2) | 4753.8 ± 1047.4 | 4902.2 ± 444.3 | 4439.5 ± 328.1 | 0.025 | 0.698 |
| PC(36:3) | 3650 ± 1035 | 3884.2 ± 936.2 | 2866.5 ± 856.6 | 0.003 | 0.122 |
| PC(36:5) | 391.6 ± 437.5 | 376.8 ± 327.3 | 236.4 ± 269.4 | 0.041 | 0.069 |
| Total PE | 3502.5 ± 1052.4 | 3840.7 ± 914.1 | 2986.4 ± 769 | 0.004 | 0.285 |
| PE(34:2) | 203.1 ± 65.5 | 205.2 ± 47 | 144.1 ± 37.9 | 0.008 | 0.028 |
| PE(36:4) | 1014.5 ± 300.8 | 1309.3 ± 502.6 | 629.4 ± 269.1 | 0.011 | 0.036 |
| LPE(18:2) | 144.7 ± 60.3 | 142.7 ± 43.4 | 95 ± 30.3 | 0.006 | 0.052 |
| Total PG | 538.9 ± 135.4 | 581.8 ± 188.7 | 329.2 ± 152.5 | 0.045 | 0.041 |
| PG(34:1) | 483 ± 121.9 | 523 ± 176.8 | 300.9 ± 139.4 | 0.052 | 0.042 |
| PG(34:2) | 55.9 ± 20.6 | 58.8 ± 19.1 | 28.3 ± 14.9 | 0.028 | 0.047 |
| Variable | RV | LV | LV INF | p vs. LV | p vs. RV |
|---|---|---|---|---|---|
| TAG(58:8) | 2856 ± 1534.1 | 3364.8 ± 3160.3 | 1978.9 ± 1520.3 | 0.018 | 0.075 |
| CE(18:3) | 269.5 ± 248.3 | 352.3 ± 319.7 | 575.9 ± 583.5 | 0.239 | 0.018 |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2020 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Samouillan, V.; Martinez de Lejarza Samper, I.M.; Benitez Amaro, A.; Vilades, D.; Dandurand, J.; Casas, J.; Jorge, E.; de Gonzalo Calvo, D.; Gallardo, A.; Lerma, E.; et al. Biophysical and Lipidomic Biomarkers of Cardiac Remodeling Post-Myocardial Infarction in Humans. Biomolecules 2020, 10, 1471. https://doi.org/10.3390/biom10111471
Samouillan V, Martinez de Lejarza Samper IM, Benitez Amaro A, Vilades D, Dandurand J, Casas J, Jorge E, de Gonzalo Calvo D, Gallardo A, Lerma E, et al. Biophysical and Lipidomic Biomarkers of Cardiac Remodeling Post-Myocardial Infarction in Humans. Biomolecules. 2020; 10(11):1471. https://doi.org/10.3390/biom10111471
Chicago/Turabian StyleSamouillan, Valerie, Ignacio Miguel Martinez de Lejarza Samper, Aleyda Benitez Amaro, David Vilades, Jany Dandurand, Josefina Casas, Esther Jorge, David de Gonzalo Calvo, Alberto Gallardo, Enrique Lerma, and et al. 2020. "Biophysical and Lipidomic Biomarkers of Cardiac Remodeling Post-Myocardial Infarction in Humans" Biomolecules 10, no. 11: 1471. https://doi.org/10.3390/biom10111471
APA StyleSamouillan, V., Martinez de Lejarza Samper, I. M., Benitez Amaro, A., Vilades, D., Dandurand, J., Casas, J., Jorge, E., de Gonzalo Calvo, D., Gallardo, A., Lerma, E., Guerra, J. M., Carreras, F., Leta, R., & Llorente Cortes, V. (2020). Biophysical and Lipidomic Biomarkers of Cardiac Remodeling Post-Myocardial Infarction in Humans. Biomolecules, 10(11), 1471. https://doi.org/10.3390/biom10111471






