Which Role Plays 2-Hydroxybutyric Acid on Insulin Resistance?
Abstract
1. Introduction
1.1. Insulin, a Powerful Molecule
1.2. Insulin Resistance
1.3. Mechanisms Underlying the IR Effect
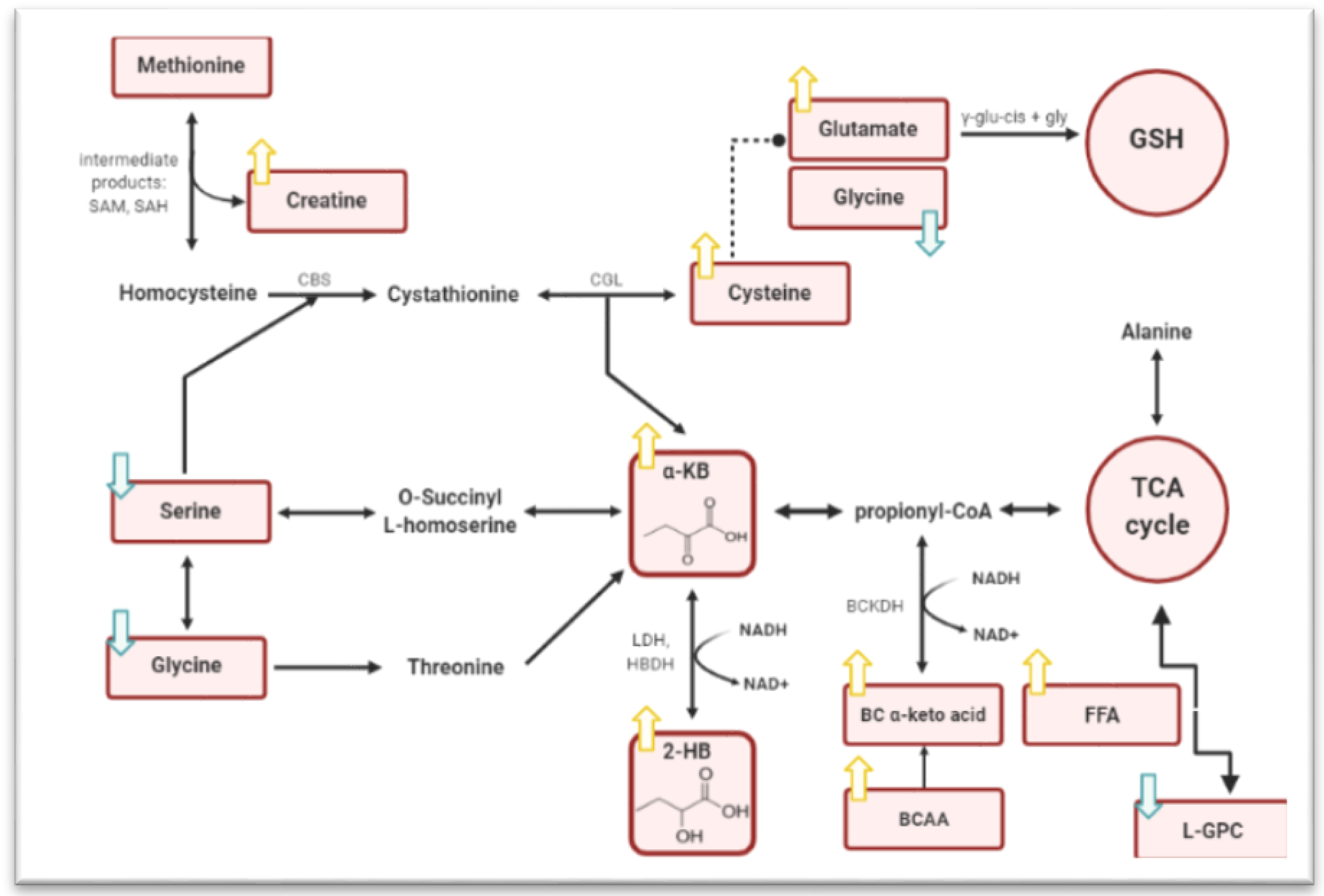
1.4. Biosynthesis of 2HB
1.5. HB Pathways Associated with IR
1.6. A Valuable Biomarker
1.7. Quantification of 2HB
1.8. The Novel Quantification Method, Quantose MQ
2. Results and Discussion
2.1. 2HB
2.2. Relationship between 2HB and Other Metabolites
2.3. Quantose MQ
3. Materials and Methods
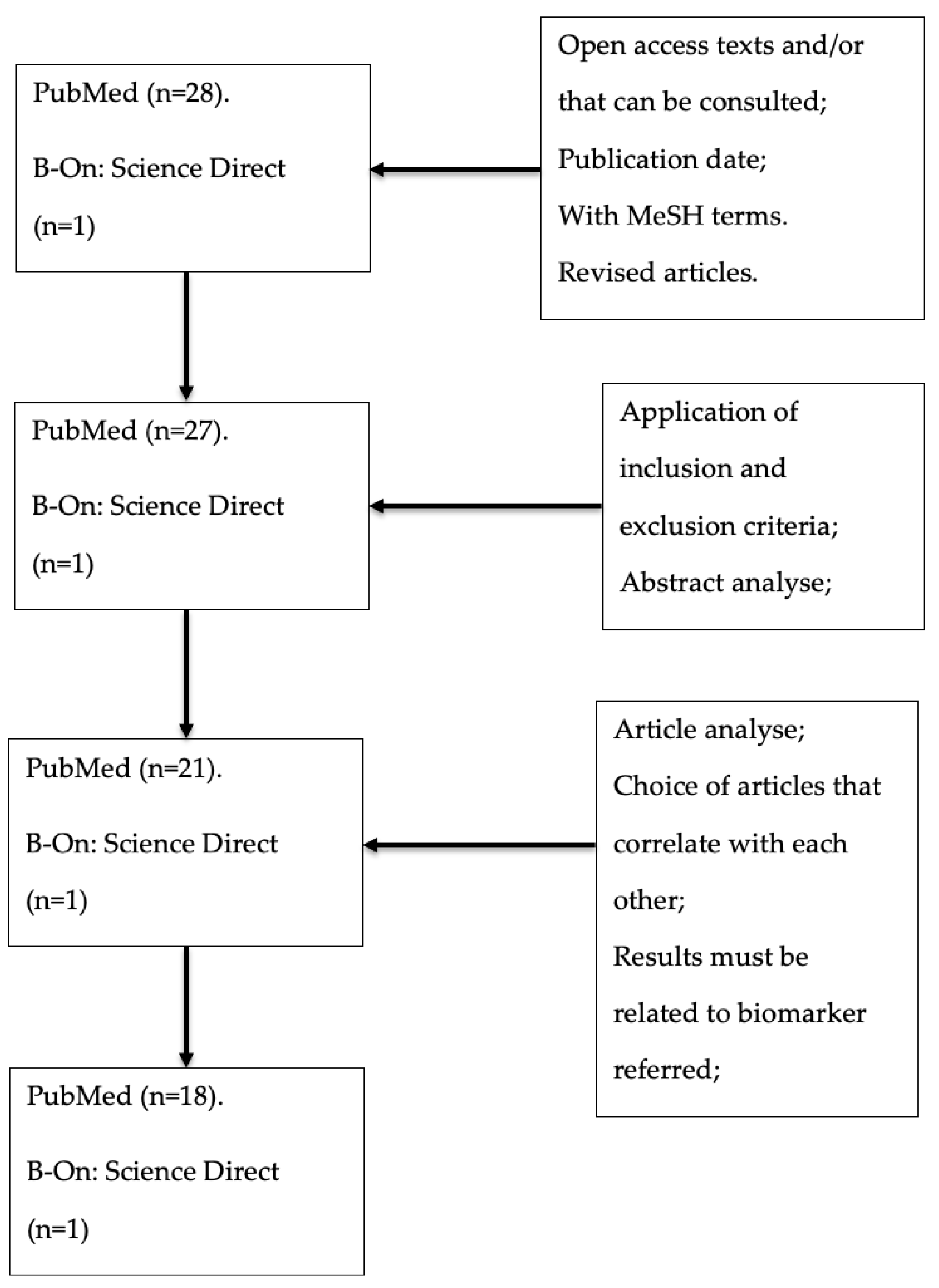
Database Research
4. Conclusions
Author Contributions
Funding
Conflicts of Interest
Abbreviations
| 2HB/α-HB | 2- or α-hydroxybutyric acid |
| 2KB/α-KB | 2- or α-ketobutyrate |
| 3HB/β-HB | 3- or β-hydroxybutyrate |
| BCAA | Branch chain amino acids |
| CNS | Central nervous system |
| CRP | C-reactive protein |
| CSF | Cerebrospinal fluid |
| CVD | Cardiovascular diseases |
| CVS | Cardiovascular system |
| ER | Endoplasmatic reticulum |
| FFA | Free fatty acids |
| G6P | Glucose 6-phosphate |
| GSH | Glutathione (reduced form) |
| HBDH | α-hydroxybutyrate dehydrogenase |
| WGS | Whole genome sequencing |
| XDR | Extensively drug-resistant |
| IGF | Insulin-like growth factors |
| IGT | Impaired Glucose Tolerance |
| IR | Insulin Resistance |
| IRS | Insulin receptor substrate |
| LDH | Lactate dehydrogenase |
| L-GPC | L-linoleoyl-glycerylphosphorylcholine |
| MCP-1 | Monocyte chemotactic protein-1 |
| NAD+ | Nicotinamide adenine dinucleotide |
| NADH | Dihydronicotinamide adenine dinucleotide |
| NIDDM | Non-insulin-dependent diabetes mellitus |
| PI3K | Phosphoinositide 3-kinase |
| PICO | Population, Intervention, Comparison and Outcome |
| PIP2 | y-linositol 4,5-bisphosphate |
| PIP3 | Phosphatidylinositol 3,4,5-trisphosphate |
| PKB | Protein kinase B |
| PTP1B | Protein-tyrosine phosphatase 1b |
| T2D | Type 2 Diabetes Mellitus |
| TNF-α | Tumor necrosis factor-α |
References
- International Diabetes Federation Atlas. 463 People Living with Diabetes Million; The International Diabetes Federation: Brussels, Belgium, 2019; ISBN 9782930229874. [Google Scholar]
- Varvel, S.A.; Pottala, J.V.; Thiselton, D.L.; Caffrey, R.; Dall, T.; Sasinowski, M.; McConnell, J.P.; Warnick, G.R.; Voros, S.; Graham, T.E. Serum α-hydroxybutyrate (α-HB) predicts elevated 1 h glucose levels and early-phase β-cell dysfunction during OGTT. BMJ Open Diabetes Res. Care 2014, 2, e000038. [Google Scholar] [CrossRef]
- Lowe, W.L.; Bain, J.R. “Prediction is very hard, especially about the future”: New biomarkers for type 2 diabetes? Diabetes 2013, 62, 1384–1385. [Google Scholar] [CrossRef] [PubMed]
- Ikmal, S.I.Q.S.; Huri, H.Z.; Vethakkan, S.R.; Ahmad, W.A.W. Potential biomarkers of insulin resistance and atherosclerosis in type 2 diabetes mellitus patients with coronary artery disease. Int. J. Endocrinol. 2013, 2013, 698567. [Google Scholar] [CrossRef]
- Salgado-Bustamante, M.; Rocha-Viggiano, A.K.; Rivas-Santiago, C.; Magaña-Aquino, M.; López, J.A.; López-Hernández, Y. Metabolomics applied to the discovery of tuberculosis and diabetes mellitus biomarkers. Biomark. Med. 2018, 12, 1001–1013. [Google Scholar] [CrossRef]
- Koeppen, B.M.; Stanton, B.A. Berne and Levy Physiology; Elsevier: Amsterdam, The Netherlands, 2017; ISBN 9780323523356. [Google Scholar]
- Liu, M.; Wright, J.; Guo, H.; Xiong, Y.; Arvan, P. Proinsulin entry and transit through the endoplasmic reticulum in pancreatic beta cells. In Vitamins and Hormones; Academic Press Inc.: Cambridge, MA, USA, 2014; Volume 95, pp. 35–62. [Google Scholar]
- Færch, K.; Vistisen, D.; Pacini, G.; Torekov, S.S.; Johansen, N.B.; Witte, D.R.; Jonsson, A.; Pedersen, O.; Hansen, T.; Lauritzen, T.; et al. Insulin resistance is accompanied by increased fasting glucagon and delayed glucagon suppression in individuals with normal and impaired glucose regulation. Diabetes 2016, 65, 3473–3481. [Google Scholar] [CrossRef]
- Weiss, M.; Steiner, D.F.; Philipson, L.H. Insulin Biosynthesis, Secretion, Structure, and Structure-Activity Relationships; MDText.com, Inc.: South Dartmouth, MA, USA, 2000. [Google Scholar]
- Suhre, K.; Meisinger, C.; Döring, A.; Altmaier, E.; Belcredi, P.; Gieger, C.; Chang, D.; Milburn, M.V.; Gall, W.E.; Weinberger, K.M.; et al. Metabolic Footprint of Diabetes: A Multiplatform Metabolomics Study in an Epidemiological Setting. PLoS ONE 2010, 5, e13953. [Google Scholar] [CrossRef] [PubMed]
- Yaribeygi, H.; Farrokhi, F.R.; Butler, A.E.; Sahebkar, A. Insulin resistance: Review of the underlying molecular mechanisms. J. Cell. Physiol. 2019, 234, 8152–8161. [Google Scholar] [CrossRef]
- Copps, K.D.; White, M.F. Regulation of insulin sensitivity by serine/threonine phosphorylation of insulin receptor substrate proteins IRS1 and IRS2. Diabetologia 2012, 55, 2565–2582. [Google Scholar] [CrossRef] [PubMed]
- Bui, D.; Ravasz, D.; Chinopoulos, C. The Effect of 2-Ketobutyrate on Mitochondrial Substrate-Level Phosphorylation. Neurochem. Res. 2019, 44, 2301–2306. [Google Scholar] [CrossRef]
- Ho, C.K.; Sriram, G.; Dipple, K.M. Insulin sensitivity predictions in individuals with obesity and type II diabetes mellitus using mathematical model of the insulin signal transduction pathway. Mol. Genet. Metab. 2016, 119, 288–292. [Google Scholar] [CrossRef]
- Yip, S.C.; Saha, S.; Chernoff, J. PTP1B: A double agent in metabolism and oncogenesis. Trends Biochem. Sci. 2010, 35, 442–449. [Google Scholar] [CrossRef] [PubMed]
- Peraldi, P.; Spiegelman, B. TNF-α and insulin resistance: Summary and future prospects. Mol. Cell. Biochem. 1998, 182, 169–175. [Google Scholar] [CrossRef] [PubMed]
- Dandona, P.; Aljada, A.; Bandyopadhyay, A. Inflammation: The link between insulin resistance, obesity and diabetes. Trends Immunol. 2004, 25, 4–7. [Google Scholar] [CrossRef] [PubMed]
- De Luca, C.; Olefsky, J.M. Inflammation and insulin resistance. FEBS Lett. 2008, 582, 97–105. [Google Scholar] [CrossRef]
- Tilg, H.; Moschen, A.R. Inflammatory mechanisms in the regulation of insulin resistance. Mol. Med. 2008, 14, 222–231. [Google Scholar] [CrossRef]
- Evans, J.L.; Maddux, B.A.; Goldfine, I.D. The molecular basis for oxidative stress-induced insulin resistance. Antioxidants Redox Signal. 2005, 7, 1040–1052. [Google Scholar] [CrossRef]
- Hurrle, S.; Hsu, W.H. The etiology of oxidative stress in insulin resistance. Biomed. J. 2017, 40, 257–262. [Google Scholar] [CrossRef]
- Pan, Y.; Qiao, Q.Y.; Pan, L.H.; Zhou, D.C.; Hu, C.; Gu, H.F.; Fu, S.K.; Liu, X.L.; Jin, H.M. Losartan reduces insulin resistance by inhibiting oxidative stress and enhancing insulin signaling transduction. Exp. Clin. Endocrinol. Diabetes 2015, 123, 170–177. [Google Scholar] [CrossRef]
- Hirosumi, J.; Tuncman, G.; Chang, L.; Görgün, C.Z.; Uysal, K.T.; Maeda, K.; Karin, M.; Hotamisligil, G.S. A central, role for JNK in obesity and insulin resistance. Nature 2002, 420, 333–336. [Google Scholar] [CrossRef]
- Sesti, G. Pathophysiology of insulin resistance. Best Pract. Res. Clin. Endocrinol. Metab. 2006, 20, 665–679. [Google Scholar] [CrossRef] [PubMed]
- Song, X.M.; Lichti, C.F.; Townsend, R.R.; Mueckler, M. Single Point Mutations Result in the Miss-Sorting of Glut4 to a Novel Membrane Compartment Associated with Stress Granule Proteins. PLoS ONE 2013, 8, e68516. [Google Scholar] [CrossRef]
- Gall, W.E.; Beebe, K.; Lawton, K.A.; Adam, K.P.; Mitchell, M.W.; Nakhle, P.J.; Ryals, J.A.; Milburn, M.V.; Nannipieri, M.; Camastra, S.; et al. α-Hydroxybutyrate Is an Early Biomarker of Insulin Resistance and Glucose Intolerance in a Nondiabetic Population. PLoS ONE 2010, 5, e10883. [Google Scholar] [CrossRef] [PubMed]
- Ferrannini, E.; Natali, A.; Camastra, S.; Nannipieri, M.; Mari, A.; Adam, K.P.; Milburn, M.V.; Kastenmüller, G.; Adamski, J.; Tuomi, T.; et al. Early metabolic markers of the development of dysglycemia and type 2 diabetes and their physiological significance. Diabetes 2013, 62, 1730–1737. [Google Scholar] [CrossRef]
- Lin, Z.; Gonçalves, C.M.V.; Dai, L.; Lu, H.-M.; Huang, J.-H.; Ji, H.; Wang, D.-S.; Yi, L.-Z.; Liang, Y.-Z. Exploring metabolic syndrome serum profiling based on gas chromatography mass spectrometry and random forest models. Anal. Chim. Acta 2014, 827, 22–27. [Google Scholar] [CrossRef]
- Xu, F.; Tavintharan, S.; Sum, C.F.; Woon, K.; Lim, S.C.; Ong, C.N. Metabolic signature shift in type 2 diabetes mellitus revealed by mass spectrometry-based metabolomics. J. Clin. Endocrinol. Metab. 2013, 98, E1060–E1065. [Google Scholar] [CrossRef]
- Shantavasinkul, P.C.; Muehlbauer, M.J.; Bain, J.R.; Ilkayeva, O.R.; Craig, D.M.; Newgard, C.B.; Svetkey, L.P.; Shah, S.H.; Torquati, A. Improvement in insulin resistance after gastric bypass surgery is correlated with a decline in plasma 2-hydroxybutyric acid. Surg. Obes. Relat. Dis. 2018, 14, 1126–1132. [Google Scholar] [CrossRef]
- Landaas, S. The formation of 2-hydroxybutyric acid in experimental animals. Clin. Chim. Acta 1975, 58, 23–32. [Google Scholar] [CrossRef]
- Rosalki, S.B.; Wilkinson, J.H. Reduction of α-ketobutyrate by human serum. Nature 1960, 188, 1110–1111. [Google Scholar] [CrossRef]
- Newman, E.B.; Kapoor, V.; Potter, R. Role of L threonine dehydrogenase in the catabolism of threonine and synthesis of glycine by Escherichia coli. J. Bacteriol. 1976, 126, 1245–1249. [Google Scholar] [CrossRef] [PubMed]
- Lord, R.S.; Bralley, J.A. Clinical applications of urinary organic acids. part 1: Detoxification markers. Altern. Med. Rev. 2008, 13, 205–215. [Google Scholar] [PubMed]
- Ragheb, R.; Medhat, A.M. Mechanisms of Fatty Acid-Induced Insulin Resistance in Muscle and Liver. J. Diabetes Metab. 2011, 2, 4. [Google Scholar] [CrossRef]
- Cobb, J.; Gall, W.; Adam, K.P.; Nakhle, P.; Button, E.; Hathorn, J.; Lawton, K.; Milburn, M.; Perichon, R.; Mitchell, M.; et al. A novel fasting blood test for insulin resistance and prediabetes. J. Diabetes Sci. Technol. 2013, 7, 100–110. [Google Scholar] [CrossRef] [PubMed]
- De Souza, C.J.; Eckhardt, M.; Gagen, K.; Dong, M.; Chen, W.; Laurent, D.; Burkey, B.F. Effects of Pioglitazone on Adipose Tissue Remodeling Within the Setting of Obesity and Insulin Resistance. Diabetes 2001, 50, 1863–1871. [Google Scholar] [CrossRef]
- Bouatra, S.; Aziat, F.; Mandal, R.; Guo, A.C.; Wilson, M.R.; Knox, C.; Bjorndahl, T.C.; Krishnamurthy, R.; Saleem, F.; Liu, P.; et al. The Human Urine Metabolome. PLoS ONE 2013, 8, e73076. [Google Scholar] [CrossRef] [PubMed]
- Roux, A.; Xu, Y.; Heilier, J.F.; Olivier, M.F.; Ezan, E.; Tabet, J.C.; Junot, C. Annotation of the human adult urinary metabolome and metabolite identification using ultra high performance liquid chromatography coupled to a linear quadrupole ion trap-orbitrap mass spectrometer. Anal. Chem. 2012, 84, 6429–6437. [Google Scholar] [CrossRef] [PubMed]
- Wishart, D.S.; Lewis, M.J.; Morrissey, J.A.; Flegel, M.D.; Jeroncic, K.; Xiong, Y.; Cheng, D.; Eisner, R.; Gautam, B.; Tzur, D.; et al. The human cerebrospinal fluid metabolome. J. Chromatogr. B Anal. Technol. Biomed. Life Sci. 2008, 871, 164–173. [Google Scholar] [CrossRef]
- Cheng, Y.; Xie, G.; Chen, T.; Qiu, Y.; Zou, X.; Zheng, M.; Tan, B.; Feng, B.; Dong, T.; He, P.; et al. Distinct urinary metabolic profile of human colorectal cancer. J. Proteome Res. 2012, 11, 1354–1363. [Google Scholar] [CrossRef]
- Hoffmann, G.F.; Meier-Augenstein, W.; Stöckler, S.; Surtees, R.; Rating, D.; Nyhan, W.L. Physiology and pathophysiology of organic acids in cerebrospinal fluid. J. Inherit. Metab. Dis. 1993, 16, 648–669. [Google Scholar] [CrossRef] [PubMed]
- Zordoky, B.N.; Sung, M.M.; Ezekowitz, J.; Mandal, R.; Han, B.; Bjorndahl, T.C.; Bouatra, S.; Anderson, T.; Oudit, G.Y.; Wishart, D.S.; et al. Metabolomic fingerprint of heart failure with preserved ejection fraction. PLoS ONE 2015, 10, e0124844. [Google Scholar] [CrossRef]
- Tsuruoka, M.; Hara, J.; Hirayama, A.; Sugimoto, M.; Soga, T.; Shankle, W.R.; Tomita, M. Capillary electrophoresis-mass spectrometry-based metabolome analysis of serum and saliva from neurodegenerative dementia patients. Electrophoresis 2013, 34, 2865–2872. [Google Scholar] [CrossRef]
- Caterino, M.; Ruoppolo, M.; Villani, G.R.D.; Marchese, E.; Costanzo, M.; Sotgiu, G.; Dore, S.; Franconi, F.; Campesi, I. Influence of sex on urinary organic acids: A cross-sectional study in children. Int. J. Mol. Sci. 2020, 21, 582. [Google Scholar] [CrossRef]
- Hušek, P.; Švagera, Z.; Hanzlíková, D.; Řimnáčová, L.; Zahradníčková, H.; Opekarová, I.; Šimek, P. Profiling of urinary amino-carboxylic metabolites by in-situ heptafluorobutyl chloroformate mediated sample preparation and gas chromatography-mass spectrometry. J. Chromatogr. A 2016, 1443, 211–232. [Google Scholar] [CrossRef] [PubMed]
- Loftfield, E.; Vogtmann, E.; Sampson, J.N.; Moore, S.C.; Nelson, H.; Knight, R.; Chia, N.; Sinha, R. Comparison of collection methods for fecal samples for discovery metabolomics in epidemiologic studies. Cancer Epidemiol. Biomark. Prev. 2016, 25, 1483–1490. [Google Scholar] [CrossRef]
- Zierer, J.; Jackson, M.A.; Kastenmüller, G.; Mangino, M.; Long, T.; Telenti, A.; Mohney, R.P.; Small, K.S.; Bell, J.T.; Steves, C.J.; et al. The fecal metabolome as a functional readout of the gut microbiome. Nat. Genet. 2018, 50, 790–795. [Google Scholar] [CrossRef] [PubMed]
- Delgado-Povedano, M.M.; Calderón-Santiago, M.; Priego-Capote, F.; de Castro, M.L. Development of a method for enhancing metabolomics coverage of human sweat by gas chromatography-mass spectrometry in high resolution mode. Anal. Chim. Acta 2016, 905, 115–125. [Google Scholar] [CrossRef] [PubMed]
- Altmaier, E.; Ramsay, S.L.; Graber, A.; Mewes, H.-W.; Weinberger, K.M.; Suhre, K. Bioinformatics Analysis of Targeted Metabolomics—Uncovering Old and New Tales of Diabetic Mice under Medication. Endocrinology 2008, 149, 3478–3489. [Google Scholar] [CrossRef] [PubMed][Green Version]
- López-Trujillo, M.A.; Olivares-Gazca, J.M.; Cantero-Fortiz, Y.; García-Navarrete, Y.I.; Cruz-Mora, A.; Olivares-Gazca, J.C.; Murrieta-Álvarez, I.; León-Peña, A.A.; Ruiz-Delgado, G.J.; Ruiz-Argüelles, G.J. Nonalcoholic Fatty Liver Disease and Thrombocytopenia III: Its Association With Insulin Resistance. Clin. Appl. Thromb. 2019, 25, 4–7. [Google Scholar] [CrossRef]
- Tripathy, D.; Cobb, J.E.; Gall, W.; Adam, K.P.; George, T.; Schwenke, D.C.; Banerji, M.A.; Bray, G.A.; Buchanan, T.A.; Clement, S.C.; et al. A novel insulin resistance index to monitor changes in insulin sensitivity and glucose tolerance: The ACT NOW study. J. Clin. Endocrinol. Metab. 2015, 100, 1855–1862. [Google Scholar] [CrossRef]
- Liu, Y.; Liu, F.-J.; Guan, Z.-C.; Dong, F.-T.; Cheng, J.-H.; Gao, Y.-P.; Li, D.; Yan, J.; Liu, C.-H.; Han, D.-P.; et al. The extracellular domain of Staphylococcus aureus LtaS binds insulin and induces insulin resistance during infection. Nat. Microbiol. 2018, 3, 622–631. [Google Scholar] [CrossRef]
- Saylor, P.J.; Karoly, E.D.; Smith, M.R. Prospective Study of Changes in the Metabolomic Profiles of Men during Their First Three Months of Androgen Deprivation Therapy for Prostate Cancer. Am. Assoc. Cancer Res. 2012, 18, 13. [Google Scholar] [CrossRef]
- Zhang, Q.; Ford, L.A.; Goodman, K.A.; Freed, T.A.; Hauser, D.M.; Conner, J.K.; Vroom, K.E.T.; Toal, D.R. LC–MS/MS method for quantitation of seven biomarkers in human plasma for the assessment of insulin resistance and impaired glucose tolerance. J. Chromatogr. B 2016, 1038, 101–108. [Google Scholar] [CrossRef]
- Metrustry, S.J.; Karhunen, V.; Edwards, M.H.; Menni, C.; Geisendorfer, T.; Huber, A.; Reichel, C.; Dennison, E.M.; Cooper, C.; Spector, T.; et al. Metabolomic signatures of low birthweight: Pathways to insulin resistance and oxidative stress. PLoS ONE 2018, 13, e0194316. [Google Scholar] [CrossRef]
- Ferrannini, E.; Iervasi, G.; Cobb, J.; Ndreu, R.; Nannipieri, M. Insulin resistance and normal thyroid hormone levels: Prospective study and metabolomic analysis. Am. J. Physiol.-Endocrinol. Metab. 2017, 312, 429–436. [Google Scholar] [CrossRef] [PubMed]
- Peddinti, G.; Cobb, J.; Yengo, L.; Froguel, P.; Kravić, J.; Balkau, B.; Tuomi, T.; Aittokallio, T.; Groop, L. Early metabolic markers identify potential targets for the prevention of type 2 diabetes. Diabetologia 2017, 60, 1740–1750. [Google Scholar] [CrossRef]
- Tricò, D.; Prinsen, H.; Giannini, C.; de Graaf, R.; Juchem, C.; Li, F.; Caprio, S.; Santoro, N.; Herzog, R. Elevated α-Hydroxybutyrate and Branched-Chain Amino Acid Levels Predict Deterioration of Glycemic Control in Adolescents. J. Clin. Endocrinol. Metab. 2017, 102, 2473–2481. [Google Scholar] [CrossRef] [PubMed]
- Ruiz-Argüelles, A.; Méndez-Huerta, M.A.; Lozan, C.D.; Ruiz-Argüelles, G.J. Metabolomic profile of insulin resistance in patients with multiple sclerosis is associated to the severity of the disease. Mult. Scler. Relat. Disord. 2018, 25, 316–321. [Google Scholar] [CrossRef] [PubMed]
- Liberati, A.; Altman, D.G.; Tetzlaff, J.; Mulrow, C.; Gøtzsche, P.C.; Ioannidis, J.P.A.; Clarke, M.; Devereaux, P.J.; Kleijnen, J.; Moher, D. The PRISMA Statement for Reporting Systematica Reviews and Meta-Analyses of Studies That Evaluate Healthcare Interventions: Explanation and Elaboration. Br. Med. J. 2009, 339, b2700. [Google Scholar] [CrossRef] [PubMed]
| Study | Principal Metabolites Studied | Correlated Pathologic Conditions | Methodology | Outcomes |
|---|---|---|---|---|
| [29] | 2HB | Insulin resistance (IR) | LC/MS and GC/MS | >levels of 2HB are related to diabetic and IGF patients |
| [28,30,53] | GC/MS | <2HB levels were observed after 6 months of gastric surgery. Furthermore, 2HB was used as inverse biomarker to predict improvement of pathology | ||
| [2] | HPLC and Oral Glucose Tolerance Testing (OGTT) | 2HB can be used to predict hyperglycemia and β-cell dysfunction | ||
| [5] | LC/MS-MS and GC/MS | 2HB showed in urine as a biomarker to T2D | ||
| [54] | IR and prostate cancer | 2HB levels decreased after 3 months beginning treatment | ||
| [26] | IR and Impaired Glucose Tolerance (IGT) | UHPLC-MS/MS and GC/MS | 2HB is an early marker for both IR and impaired glucose regulation | |
| [55] | LC/MS-MS | Applied methodology was efficient to predict IR | ||
| [56] | IR and oxidative stress in low birthweight | Relation between low birthweight and IR | ||
| [57] | IR and dysregulations in thyroid hormone levels | UHPLC-MS/MS | 2HB levels increased in IR, by metabolic overload and oxidative stress | |
| [58] | 2HB and α-tocopherol | IR and cardiovascular risk | UHPLC-MS and GC-MS | Increasing in 2HB and α-tocopherol levels were involved in IR and IGT |
| [3] | 2HB and L-GPC | IR | n.m *** | High levels of 2HB and lower levels of L-GPC were associated with IR and IGT |
| [27] | IR and dysglicemia | HPLC-MS | ||
| [59] | 2HB and Branched-Chain Amino Acids (BCAA) | IR in youth | NMR and OGTT | BCAA and 2HB can predict IR in youth |
| [52] | Quantose MQ mix * | IR and IGT | n.m *** | Improved insulin sensitivity and glucose tolerance, allowing to predict IR |
| [60] | IR and sclerosis multiple | Improved insulin sensitivity and glucose tolerance, allowing to predict IR | ||
| [51] | IR and non-alcoholic fatty liver disease and thrombocytopenia III | HPLC-MS and chemiluminescent microparticles immunoassay (for insulin specific) | Score was elevated in IR patients | |
| [4] | Mix ** | IR associated with atherosclerosis in coronary artery disease | n.m *** | A are a new set of biomarkers for IR and endothelial dysfunction in T2D patients |
| Summary | 2HB | Mainly IR | High throughput technologies (not routine methods) | Higher levels of 2HB is positively associated with IR |
| Inclusion Criteria | Exclusion Criteria |
|---|---|
|
|
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Sousa, A.P.; Cunha, D.M.; Franco, C.; Teixeira, C.; Gojon, F.; Baylina, P.; Fernandes, R. Which Role Plays 2-Hydroxybutyric Acid on Insulin Resistance? Metabolites 2021, 11, 835. https://doi.org/10.3390/metabo11120835
Sousa AP, Cunha DM, Franco C, Teixeira C, Gojon F, Baylina P, Fernandes R. Which Role Plays 2-Hydroxybutyric Acid on Insulin Resistance? Metabolites. 2021; 11(12):835. https://doi.org/10.3390/metabo11120835
Chicago/Turabian StyleSousa, André P., Diogo M. Cunha, Carolina Franco, Catarina Teixeira, Frantz Gojon, Pilar Baylina, and Ruben Fernandes. 2021. "Which Role Plays 2-Hydroxybutyric Acid on Insulin Resistance?" Metabolites 11, no. 12: 835. https://doi.org/10.3390/metabo11120835
APA StyleSousa, A. P., Cunha, D. M., Franco, C., Teixeira, C., Gojon, F., Baylina, P., & Fernandes, R. (2021). Which Role Plays 2-Hydroxybutyric Acid on Insulin Resistance? Metabolites, 11(12), 835. https://doi.org/10.3390/metabo11120835








