Abstract
Cannabis sativa L. plant is currently attracting increasing interest in cosmetics and dermatology. In this review, the biologically active compounds of hemp are discussed. Particularly the complex interactions of cannabinoids with the endocannabinoid system of the skin to treat various conditions (such as acne, allergic contact dermatitis, melanoma, and psoriasis) with clinical data. Moreover, the properties of some cannabinoids make them candidates as cosmetic actives for certain skin types. Hemp seed oil and its minor bioactive compounds such as terpenes, flavonoids, carotenoids, and phytosterols are also discussed for their added value in cosmetic formulation.
1. Introduction
It has already been 6000 years that humans use Cannabis as food, fiber, and medicine [1]. Nowadays, Cannabis has widely spread through the world [1]. It is a predominantly dioecious species, with only male flowers or female flowers [2]. This particularity opened the path to hybridization of the plant, and lead to thousands of cultivars [1]. There is a long taxonomic problem with the classification of the different strains [1]. It is generally accepted to divide the Cannabis sativa L. species into 3 subspecies: “Sativa” refers to strains with a limited amount of THC, “Indica” refers to strains producing principally THC, and “Ruderalis” refers to wild hemp strains [1].
The Cannabis sativa L. plant contains a diversity of bio-active compounds which are promising for topical application in dermatology [3] or as cosmetic ingredients [4,5]. Firstly, because of the high content of cannabinoids, which can modulate diverse inflammatory conditions and immune response via the endocannabinoid system [6]. Secondly, because of the Hemp Seed Oil, which has beneficial properties for the skin [7,8]. And thirdly, because of the diversity of minor bioactive active compounds such as terpenes, flavonoids, carotenoids, phytosterols [9,10,11].
Firstly, this review aims to gather knowledge about the various cannabinoids and their biological actions within and outside the endocannabinoid system. Secondly, to determine the added value of Hemp Seed Oil and its minor constituents compared to other oils for cosmetic formulations or dermatological use.
2. Cannabis sativa L. Botany
Cannabis sativa L. belongs to the Cannabaceae family. It is an annual herb [1]. The plant can reach a height higher than 5 m in the outdoor 6 months growing season, as shown in Figure 1a [12]. The leaves grow on opposite sides of the stem [13]. The leaves, stems, and bracts of the plants are covered by epidermal protuberances called trichomes [1]. There are two types of trichomes: glandular and non-glandular. The non-glandular trichomes are in the bracts, petioles, stipules, leaves, and stems and serve as a defense mechanism against abiotic and biotic stress. The glandular trichomes are responsible for the synthesis of cannabinoids, secondary metabolites, and terpenes in a viscous resin, as shown in Figure 1b [14]. When the days start to shorten, the inflorescence is triggered and buds of flowers develop. Male plants die after the inflorescence while the females remain until winter [1].

Figure 1.
(a) Illustration of Cannabis sativa L. from Heinrich Füllmaurer, 1543 (b) Cannabis sativa L. glandular trichomes, photography by Ethan Budd Russo, reproduced by permission of Wiley-VHCA AG, Zurich, Switzerland [15].
3. The Endocannabinoid System
The endocannabinoid system (ECS), in the skin, is implied in cutaneous function such as cell differentiation modulation, growth and survival, inflammatory and immune responses, nociception, and hair growth. Indeed, dysregulation of the ECS seems to be involved in various skin disease conditions [16]. Two G protein-coupled receptors are involved in the ECS’s regulation: cannabinoid type 1 receptor (CB1) and cannabinoid type 2 receptor (CB2) [17]. In the skin, CB1 is expressed in hair follicular cells, sensory neurons, immune cells, sebaceous glands, and keratinocytes while CB2 is expressed in sensory neurons, immune cells, sebaceous glands, and keratinocytes [18]. The CB1 main activity is the regulation of pain, of excessive neural activity and the extinction of evasive memories in the central nervous system [19]. It has been recently shown that CB1 regulate inflammatory response in various peripheral organs [20,21,22]. As for the skin, activation of CB1 downregulate the production of pro-inflammatory cytokine in keratinocytes, and protects the skin barrier [19]. Activation of CB2 has anti-inflammatory effects in skin; by inhibiting the macrophage 1 polarizations they downregulate pro-inflammatory cytokines [23]. The orphans G-coupled proteins receptors GPR55 and GPR18 can also be activated by some cannabinoids ligands [24,25,26,27]. Further studies are warranted to determine if GPR55 can be officially considered as a CB3 receptor or not. Depending on the target cell, GPR55 can have a pro-inflammatory or anti-inflammatory effects [27]. Nevertheless, its activation promotes human skin tumors and other squamous cell carcinomas [28]. GPR18 was revealed to have anti-inflammatory and anti-nociceptive activity in case of intestinal inflammation [29]. GPR18 is an active inhibitor of apoptosis in melanoma cells [30].
Two endogenous cannabinoids have been studied as the main natural ligands of the ECS, N-arachidonoylethanolamine (AEA), and 2-arachidonoylglycerol (2-AG [31]. AEA is synthesized by phospholipase D, 2-AG is synthesized by diacylglycerol lipase (DAGL), their degradation is mainly controlled by fatty acid amide hydrolase (FAAH), and monoacylglycerol lipase (MAGL) [32]. Palmitoylethanolamide (PEA) is also an endogenous ligand that binds with GPR55 but not with CB1 nor CB2, it has synergistic activity with AEA. PEA is synthesized by N-acyl-phosphatidyl-ethanolamine-selective phospholipase D and its degradation is mainly controlled by FAAH and N-acylethanolamine-hydrolyzing acid amidase (NAAA) [33]. The MAGL, FAAH, and NAAA inhibition has an antipruritic effect [34,35,36].
4. Secondary Cannabinoid Target
Some of the cannabinoids ligands modulate greatly the response of the ECS by the activation of various transient receptor potential ion channels (TRPV1, TRPV2, TRPV3, TRPV4, TRPA1, and TRPM8) [18], of peroxisome proliferator-activated receptor alpha and gamma (PPARα; PPARγ) transcription factors [16], and of serotonin receptors (particularly 5-HT1A, 5-HT2A, and 5-HT3 receptors) [37]. TRP ion channels permit the transit of various cations in the cells when activated by specific ligands [38]. PPAR enables, upon activation by specific ligands, the proliferation of peroxisomes which regulate inflammatory response and lipid metabolism [39].
The sum of these factors may result in synergistic or antagonistic biological effects. Therefore, it is important to take them into account to predict the pharmacological or cosmetic activity of a cannabinoid ligand. The biodynamic effect of these secondary cannabinoid targets and their location in the skin are detailed in Table 1 and illustrated in Figure 2.

Table 1.
Location and biodynamic effects of main secondary targets of cannabinoid ligands.
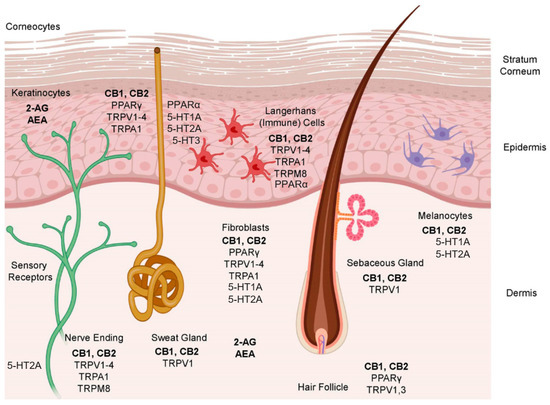
Figure 2.
The repartition of CB1 and CB2, the TRPV1-4 channels, the TRPM8 channel, the PPARs transcription factors, and serotonin 5-HT1A, 5-HT2A, 5-HT3 receptors in skin cells, modificated with the permission of Dove Medical Press, Macclesfield, United Kingdom [61].
5. Cannabinoids
The cannabinoids, which are synthesized in the glandular trichomes [2] of Cannabis sativa L. are exogenous ligands of the ECS [62]. Therefore, they can interact with endocannabinoid receptors and some of the channels and receptors described below [62].
To date, almost 200 cannabinoids have been identified, and a vast majority of them are from Cannabis sativa L. [63]. They are divided into 11 classes: Delta-9 Tetrahydrocannabinol (Δ9-THC) type, Cannabigerol (CBG) type, Cannabinol (CBN) type, Cannabichromene (CBC) type, Cannabitriol (CBT) type, Cannabidiol (CBD) type, Delta-8 Tetrahydrocannabinol (Δ8-THC) type, Cannabielsoin (CBE) type, Cannabicyclol (CBL) type, Cannabinodiol (CBND) type, and miscellaneous type.
The biosynthesis of all these cannabinoids (see Figure 3) originates from Cannabigerolic Acid (CBGA) products by Geranyl Pyrophosphate (GPP) and Olivetolic Acid (OA) or Divarinic Acid (DA), catalyzed by the Cannabigerolic Acid Synthase (CBGAS) enzyme.
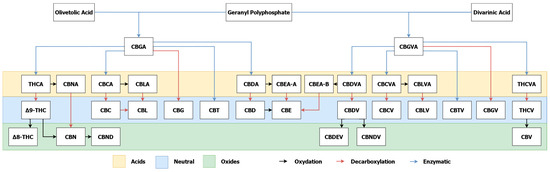
Figure 3.
The Biosynthesis of most known cannabinoids [64,65,66], CBGA: cannabigerolic acid; CBGVA: cannabigerovarinic acid; THCA: tetrahydrocannabinolic acid; Δ9-THC: delta-9 tetrahydrocannabinol; Δ8-THC: delta-8 tetrahydrocannabinol; CBNA: cannabinolic acid; CBN: cannabinol; CBND: cannabinodiol; CBCA: cannabichromenic acid; CBC: cannabichromene; CBLA: cannabicyclolic acid; CBL: cannabicyclol; CBG: cannabigerol; CBT: cannabitriol; CBDA: cannabidiolic acid; CBD: cannabidiol; CBEA-A: cannabielsoin acid A; CBEA-B: cannbielsoin acid B; CBE: cannabielsoin; CBDVA: cannabidivarinic acid; CBDV: cannabidivarin; CBDEV: cannabidielsoinvarin; CBNDV: cannabivarinodiol; CBCVA: cannabichromevarinic acid; CBCV: cannabichromevarin; CBLVA: cannabicyclolvarinic acid; CBLV: cannabicyclolvarin; CBTV: cannabitiolvarin; CBGV: cannabigerovarin; THCVA: tetrahydrocannabivarinic acid; THCV: tetrahydrocannabivarin; CBV: cannabivarin.
Delta-9 Tetrahydrocannabinol (Δ9-THC) is the principal cannabinoid from Cannabis sativa L. Cannabidiol (CBD) is the most abundant non-psychoactive cannabinoid derived from Cannabis sativa L. [1]. Δ9-THC, Δ9-THCA, Δ9-THCV, Δ9-THCVA, CBD, CBDA, CBDV, CBG, CBGA, CBGV, CBC, and CBN have been studied regarding their interaction with the ECS and the secondary cannabinoids targets. The data regarding these interactions is available in Table 2.

Table 2.
Biodynamic effects of 12 cannabinoids.
Moreover, some cannabinoids have specific particularities regarding their biodynamic activity regarding the skin.
CBD and CBG are transcriptional repressors that can control cell differentiation and proliferation in the skin [96]. CBD induces nuclear export and degradation of BACH1, reducing stress oxidation and skin aging [61,97]. CBG is an agonist of α2-adrenoceptor [73,98], it inhibits the endocannabinoid membrane transporter [50,79,82]. CBC is the most potent agonist of the TRPA1 channel [81,82,99]. CBDV is a partial agonist of dopamine D2-like receptors [100]. It has been shown recently that D2-like receptor agonism in the skin, promotes the recovery of the skin barrier and wound healing [101,102,103].
Some of these phytocannabinoids (mainly THC and CBD) have been tested as a treatment against various skin conditions (see Table 3).

Table 3.
Clinical evidence of the therapeutical potential of various cannabinoids.
Cannabinoids exhibit frequently antioxidant, antimicrobial activity, and less frequently a photoprotectant (see Table 4).

Table 4.
Antioxidant, antibacterial and photoprotectant activity of various phytocannabinoids.
Because of its wide range of effects, formulation technologies are being developed to ensure better topical delivery of CBD for medical and cosmetic use [124,125,126,127,128].
6. Hemp Seed Oil
6.1. Generalities
Hemp Seed Oil is extracted from the seeds by cold-pressed extraction or supercritical CO2 for better stability [129]. It represents about 30% of the raw material [130]. The cultivars employed and the growth condition of the plant directly impact the composition of the oil. The oil contains linoleic acid (55.41–59.64%), α-linoleic acid (16.51–20.40%), oleic acid (11.40–15.88%), palmitic acid (6.08–6.82%), and stearic acid (2.34–2.67%) [8]. Furthermore 25–35% of the oil weight are proteins, 10–15% are fibers, and 20–30% are carbohydrates [131]. Certain strains also contain up to 4% of γ-linoleic acid [129]. Sometimes, Hemp Seed Oil can also be classified by saturated, monounsaturated, and poly-unsaturated acids or by omega-3, omega-6, omega-9 acids composition:
- -
- 80.0% poly-unsaturated acids, 10.8% monounsaturated acids, and 9.2% saturated acids [132].
- -
- 59.6% omega-6 acids, 29.7% of omega-3 acids, and 10.8% omega-9 acids [132].
Hemp Seed Oil, as an oil rich in essential fatty acids (ELA), has an action on atopic dermatitis, psoriasis, and particularly acne. Many studies find conflicting results, which indicates that the actions of ELA are dose-dependant and length-dependant [133]. Both α-linolenic acid and linoleic acids reduce UV damage and hyperpigmentation [134]. Clinical evidence highlights the positive hydrating and anti-aging effect of essentials fatty acids on the skin for oral use [135]. A favorable portion of fatty acids in Hemp Seed Oil improves the gliding of a skin care cream and the smoothness of the skin [4,136]. Moreover, Hemp Seed Oil is a non-comedogenic [137] dry oil that does not leave a greasy and sticky layer on the skin [137]. As a result, formulations have been developed with Hemp Seed Oil as long-term moisturizing patches [138] and stable emulsions in sunscreen cosmetics [5,136]. Hemp Seed Oil’s global antioxidant activity can be measured by 2,2-diphenyl-1-picrylhydrazyl (DPPH) and 2,20-azino-bis-(3-ethylbenzthiazoline-6-sulfonic acid) (ABTS) test [130]. DPPH leads to 60–65% scavenging activity and ABTS leads to 40–88% scavenging activity [130,132].
Hemp Seed Oil extraction leads to byproducts of seed paste which can be recycled as a dermo-cosmetic agent by use of eco-friendly processes: Ultrasound-Assisted Extraction or Supercritical Fluid Extraction. These pastes contain 14 bioactive metabolites: seven cannabinoid acid derivates, four lignamides, two amides, and a phenolic acid. The paste showed more than 80% of inhibition for the collagenase enzyme. The global antioxidant activity was measured by DPPH; it is up to 50% of radical scavenging [9].
6.2. Biological Value of the Minor Compounds of Hemp Seed Oil
6.2.1. Essential Fatty Acids
Linoleic acid, α-linoleic acid and γ-linoleic acid are considered ELA. These compounds are required for the wealth being but not synthesized by our body [139]. Because of the competition of omega-6 and omega-3 family acids for the Δ-6 desaturase enzyme, the ratio of their consumption is important. Hemp Seed Oil fits perfectly in the (ω-6/ω-3) ideal ratio which is between 2:1 to 3:1 this ratio [140].
Linoleic acid is involved in the biosynthesis of leukotrienes, endocannabinoids, and arachidonic acid which is the main precursor of prostaglandins. Linoleic acid is also engaged in β-oxidation in the sebaceous gland to synthesize squalene and wax esters. When skin’s linoleic acid levels are low, epidermal barrier function is impaired, the comedone wall becomes permeable to inflammatory substances, resulting in a comedogenic effect [134,141].
α-linoleic acid is a compound in cell and mitochondrial membranes that modifies cell transport and signaling through the lipid layers. The α-linolenic acid metabolites permit the synthesis of the anti-inflammatory prostaglandin and leukotriene [134]. Therefore, α-linoleic acid is involved in barrier function maintenance, the stratum corneum maturation and differentiation, lamellar body formation, lipoxygenase, and pro-inflammatory eicosanoid inhibition, cytokine suppression, inhibition of mast cell degranulation, and modulation of other immune cells [133].
The γ-linoleic acid decreases the production of pro-inflammatory leukotriene B4 by increasing the concentration of dihomo-γ-linoleic acid in the skin [142].
6.2.2. Carotenoids
Hemp Seed Oil contains carotenoids, particularly β-carotene, lutein, and zeaxanthin [7,143]. These carotenoids exhibit antioxidant and UV-filtering properties because of their high solubility in the lipid bilayer membrane [144]. Therefore, β-carotene inhibits the UVB-induced upregulation of pro-inflammatory cytokines, resulting in an anti-inflammatory action [145,146]. Carotenoids improve skin hydration, promote skin regeneration, and stimulate fibroblasts to produce collagen and elastin [137].
6.2.3. Tocopherols
Hemp Seed Oil contains α-tocopherol, β-tocopherol, δ-tocopherol, γ tocopherol [130,147]. γ-tocopherol is the principal isomer with 85-91% of the tocopherols [143]. It is the main antioxidant of the Hemp Seed Oil and is responsible for most of the global antioxidant and anti-aging activities [7].
6.2.4. Phytosterols
Hemp Seed Oil contains phytosterols that inhibit the matrix metalloproteinases. The matrix metalloproteinase action inhibits COL1A1 and COL1A2 genes responsible for collagen synthesis. Therefore phytosterols permit better collagen synthesis and prevent skin aging [148].
6.2.5. Chlorophyll
Chlorophyll is surprisingly high in Hemp Seed Oil, it varies between 100 μg/g to 230 μg/g, depending on the extraction method, which is 11 times higher than in Flax Seed Oil and 88 times higher than in Canola Oil [143]. This component is responsible for the green color of the Hemp Seed Oil. The chlorophyll has beneficial action for wound-healing by promoting tissue growth, and by its antibacterial activity [149]. Therefore, it is an interesting ingredient in topical application against acne [150,151], eczema, and ulcers [152].
6.2.6. Flavonoids
There are 26 flavonoids in Hemp. Orientin, vitexin, luteolin-7-O-glucoside, and apigenin-7-O-glucoside are the main flavonoids in Hemp [153]. It also contains Quercetin which exerts a strong antioxidant effect [154]. There are 3 new flavonoids exclusive to Cannabis called Cannflavins (Cannflavin A, Cannflavin B, and Cannflavin C). Cannflavins are present in the leaves and the flower of Hemp [11]. Cannflavin A’s anti-inflammatory activity is 30 times stronger than Aspirin [155]. This anti-inflammatory effect is explained by the inhibition of the molecular targets microsomal prostaglandin E synthase-1 (mPGES-1) and 5-lipoxygenase (5-LO) [156].
6.2.7. Terpenes
More than 200 terpenes have been identified in Cannabis sativa L. [10]. Terpenes are responsible for the aromatic properties of the plant [157]. Terpenes are secreted and stored inside the glandular trichomes with cannabinoids [158]. The most concentrated terpenes in Cannabis are α-pinene, β-pinene, α-humulene, β-caryophyllene, β-myrcene, limonene, and linalool. Each strain conducts to different chemotypes of terpenes, a strain rarely contains more than 50 terpenes [10,157,158,159,160]. All these compounds have a biodynamic effect [161] (see Table 5.), but β-caryophyllene has the particularity to bind specifically with the CB2.

Table 5.
Biodynamic effect of the main terpenes found in Cannabis sativa L.
6.3. The Entourage Effect
The term «entourage effect» refers to the capacity of two or more cannabinoids or non-cannabinoids to have a better combined synergistic effect than when taken separately [162]. The concept was introduced in 1998 by Mechoulam [163].
Studies consider 4 types of synergies: multi-target effects (each component affects multiple targets), pharmacokinetic effects (components can increase the solubility or the resorption rate of an active), agent interactions affecting bacterial resistance, and modulation of adverse effects and toxicity [164].
The THC and CBD 1:1 combination is the most known case of entourage effect: it alleviates the adverse effects of pure THC [162].
Currently, evidence in favor of an entourage effect of Terpenes or Flavonoids combined with THC is contradictory, further studies are warranted to determine to which extent this concept is relevant [165,166].
7. Conclusions
The cannabinoids contained in Cannabis sativa L. are of dermatological interest for treating most inflammatory skin conditions as well as skin cancer. We now have a better understanding of the endocannabinoid system of the skin and the possible mode of action of cannabinoids. However, the focus of research remains on CBD and THC, which have demonstrated therapeutic value, but at the expense of studying the action of other cannabinoids.
As for their use in cosmetics, CBD, CBC, THCV and CBDV have potential for formulations for acne-prone skin, while CBG and CBGV are promising for regulating sebum production in dry skin. CBN and CBD also appear to be of interest for sunscreens. Almost all cannabinoids have an antibacterial and antioxidant action which is a good added value. Moreover, the immunoregulatory effects of cannabinoids seem interesting for sensitive skin. It should be noted, however, that their safety for regular use has not yet been demonstrated, apart from CBD. Further studies are warranted in this regard.
Hemp Seed Oil is interesting because of its content of flavonoids, terpenes, carotenoids and phytosterols which ensure its anti-inflammatory and anti-aging action. In addition, its ω-6/ω-3 content is ideal for the skin. It is a rapidly absorbed and non-comedogenic oil. It naturally contains tocopherol and chlorophyll. This oil is therefore of interest for formulations for all skin types, especially sensitive skin, and as a sun cream. It has potential for anti-ageing formulations.
Author Contributions
Conceptualization, L.M. and L.R.; methodology, L.R.; validation, L.R.; investigation, L.M.; data curation, L.M.; writing—original draft preparation, L.M.; writing—review and editing, L.M. and L.R.; visualization, L.M.; supervision, L.R.; project administration, L.R. All authors have read and agreed to the published version of the manuscript.
Funding
This research received no external funding.
Institutional Review Board Statement
Not applicable.
Informed Consent Statement
Not applicable.
Data Availability Statement
The data presented in this study are available within the article.
Conflicts of Interest
The authors declare no conflict of interest. The funders had no role in the design of the study; in the collection, analyses, or interpretation of data; in the writing of the manuscript, or in the decision to publish the results.
References
- Small, E. Evolution and Classification of Cannabis sativa (Marijuana, Hemp) in Relation to Human Utilization. Bot. Rev. 2015, 81, 189–294. [Google Scholar] [CrossRef]
- Grof, C.P.L. Cannabis, from plant to pill. Br. J. Clin. Pharmacol. 2018, 84, 2463–2467. [Google Scholar] [CrossRef] [PubMed]
- Sheriff, T.; Lin, M.J.; Dubin, D.; Khorasani, H. The potential role of cannabinoids in dermatology. J. Dermatol. Treat. 2019, 31, 839–845. [Google Scholar] [CrossRef]
- Vogl, C.R.; Mölleken, H.; Lissek-Wolf, G.; Surböck, A.; Kobert, J. Hemp (Cannabis sativa L.) as a resource for green cosmetics: Yield of seed and fatty acid compositions of 20 varieties under the growing conditions of organic farming in Austria. J. Ind. Hemp 2004, 9, 51–68. [Google Scholar] [CrossRef]
- Huang, Y.; Pei, L.; Gu, X.; Wang, J. Study on the Oxidation Products of Hemp Seed Oil and its Application in Cosmetics. Tenside Surfactants Deterg. 2020, 57, 230–236. [Google Scholar] [CrossRef]
- Scheau, C.; Badarau, I.A.; Mihai, L.-G.; Scheau, A.-E.; Costache, D.O.; Constantin, C.; Calina, D.; Caruntu, C.; Costache, R.S.; Caruntu, A. Cannabinoids in the Pathophysiology of Skin Inflammation. Molecules 2020, 25, 652. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Irakli, M.; Tsaliki, E.; Kalivas, A.; Kleisiaris, F.; Sarrou, E.; Cook, C.M. Effect οf Genotype and Growing Year on the Nutritional, Phytochemical, and Antioxidant Properties of Industrial Hemp (Cannabis sativa L.) Seeds. Antioxidants 2019, 8, 491. [Google Scholar] [CrossRef] [Green Version]
- Kiralan, M.; Gül, V.; Kara, S.M. Fatty acid composition of hempseed oils from different locations in Turkey. Span. J. Agric. Res. 2010, 8, 385. [Google Scholar] [CrossRef]
- Michailidis, D.; Angelis, A.; Nikolaou, P.; Mitakou, S.; Skaltsounis, A. Exploitation of Vitis vinifera, Foeniculum vulgare, Cannabis sativa and Punica granatum By-Product Seeds as Dermo-Cosmetic Agents. Molecules 2021, 26, 731. [Google Scholar] [CrossRef]
- Bakro, F.; Jedryczka, M.; Wielgusz, K.; Sgorbini, B.; Inchingolo, R.; Cardenia, V. Simultaneous determination of terpenes and cannabidiol in hemp (Cannabis sativa L.) by fast gas chromatography with flame ionization detection. J. Sep. Sci. 2020, 43, 2817–2826. [Google Scholar] [CrossRef]
- Werz, O.; Seegers, J.; Schaible, A.M.; Weinigel, C.; Barz, D.; Koeberle, A.; Allegrone, G.; Pollastro, F.; Zampieri, L.; Grassi, G.; et al. Cannflavins from hemp sprouts, a novel cannabinoid-free hemp food product, target microsomal prostaglandin E2 synthase-1 and 5-lipoxygenase. PharmaNutrition 2014, 2, 53–60. [Google Scholar] [CrossRef]
- Klumpers, L.; Thacker, D.L. A Brief Background on Cannabis: From Plant to Medical Indications. J. AOAC Int. 2019, 102, 412–420. [Google Scholar] [CrossRef]
- Chandra, S.; Lata, H.; Khan, I.A.; ElSohly, M.A. Cannabis sativa L.: Botany and Horticulture. In Cannabis sativa L.—Botany and Biotechnology; Springer: Cham, Switzerland, 2017; pp. 79–100. [Google Scholar] [CrossRef]
- Addo, P.W.; Brousseau, V.D.; Morello, V.; MacPherson, S.; Paris, M.; Lefsrud, M. Cannabis chemistry, post-harvest processing methods and secondary metabolite profiling: A review. Ind. Crop. Prod. 2021, 170, 113743. [Google Scholar] [CrossRef]
- EB, R. History of cannabis and its preparations in saga, science, and sobriquet. Chem. Biodivers. 2007, 4, 1614–1648. [Google Scholar] [CrossRef]
- Bíró, T.; Tóth, B.I.; Haskó, G.; Paus, R.; Pacher, P. The endocannabinoid system of the skin in health and disease: Novel perspectives and therapeutic opportunities. Trends Pharmacol. Sci. 2009, 30, 411–420. [Google Scholar] [CrossRef] [Green Version]
- del Río, C.; Millán, E.; García, V.; Appendino, G.; DeMesa, J.; Muñoz, E. The endocannabinoid system of the skin. A potential approach for the treatment of skin disorders. Biochem. Pharmacol. 2018, 157, 122–133. [Google Scholar] [CrossRef]
- Caterina, M.J. TRP Channel Cannabinoid Receptors in Skin Sensation, Homeostasis, and Inflammation. ACS Chem. Neurosci. 2014, 5, 1107–1116. [Google Scholar] [CrossRef]
- Tüting, T.; Gaffal, E. Regulatory Role of Cannabinoids for Skin Barrier Functions and Cutaneous. Inflammation 2017, 543–549. [Google Scholar] [CrossRef]
- Mehrpouya-Bahrami, P.; Chitrala, K.N.; Ganewatta, M.S.; Tang, C.; Murphy, E.A.; Enos, R.T.; Velazquez, K.T.; McCellan, J.; Nagarkatti, M.; Nagarkatti, P. Blockade of CB1 cannabinoid receptor alters gut microbiota and attenuates inflammation and diet-induced obesity. Sci. Rep. 2017, 7, 1–16. [Google Scholar] [CrossRef]
- Jorgačević, B.; Vučević, D.; Samardžić, J.; MladenoviĆ, D.; Vesković, M.; Vukićević, D.; Ješić, R.; Radosavljević, T. The Effect of CB1 Antagonism on Hepatic Oxidative/Nitrosative Stress and Inflammation in Nonalcoholic Fatty Liver Disease. Curr. Med. Chem. 2020, 28, 169–180. [Google Scholar] [CrossRef]
- Thapa, D.; Cairns, E.A.; Szczesniak, A.-M.; Kulkarni, P.M.; Straiker, A.J.; Thakur, G.A.; Kelly, M.E.M. Allosteric Cannabinoid Receptor 1 (CB1) Ligands Reduce Ocular Pain and Inflammation. Molecules 2020, 25, 417. [Google Scholar] [CrossRef] [Green Version]
- Du, Y.; Ren, P.; Wang, Q.; Jiang, S.-K.; Zhang, M.; Li, J.-Y.; Wang, L.-L.; Guan, D.-W. Cannabinoid 2 receptor attenuates inflammation during skin wound healing by inhibiting M1 macrophages rather than activating M2 macrophages. J. Inflamm. 2018, 15, 25. [Google Scholar] [CrossRef] [Green Version]
- Prandi, C.; Blangetti, M.; Namdar, D.; Koltai, H. Structure-Activity Relationship of Cannabis Derived Compounds for the Treatment of Neuronal Activity-Related Diseases. Molecules 2018, 23, 1526. [Google Scholar] [CrossRef] [Green Version]
- Guerrero-Alba, R.; Barragan-Iglesias, P.; González-Hernández, A.; Valdez-Moráles, E.E.; Granados-Soto, V.; Condés-Lara, M.; Rodríguez, M.G.; Marichal-Cancino, B.A. Some Prospective Alternatives for Treating Pain: The Endocannabinoid System and Its Putative Receptors GPR18 and GPR55. Front. Pharmacol. 2019, 9, 1496. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Morales, P.; Lago-Fernandez, A.; Hurst, D.P.; Sotudeh, N.; Brailoiu, E.; Reggio, P.H.; Abood, M.E. Jagerovic NTherapeutic Exploitation of GPR18: Beyond the Cannabinoids? J. Med. Chem. 2020, 63, 14216–14227. [Google Scholar] [CrossRef]
- Yang, H.; Zhou, J.; Lehmann, C. GPR55-A putative “type 3” cannabinoid receptor in inflammation. J. Basic Clin. Physiol. Pharmacol. 2016, 27, 297–302. [Google Scholar] [CrossRef] [Green Version]
- Perez-Gomez, E.; Andradas, C.; Flores, J.M.; Quintanilla, M.; Paramio, J.M.; Guzmán, M.; Sanchez, C. The orphan receptor GPR55 drives skin carcinogenesis and is upregulated in human squamous cell carcinomas. Oncogene 2012, 32, 2534–2542. [Google Scholar] [CrossRef] [Green Version]
- Fabisiak, A.; Fabisiak, N.; Mokrowiecka, A.; Malecka-Panas, E.; Jacenik, D.; Kordek, R.; Zielińska, M.; Kieć-Kononowicz, K.; Fichna, J. Novel selective agonist of GPR18, PSB-KK-1415 exerts potent anti-inflammatory and anti-nociceptive activities in animal models of intestinal inflammation and inflammatory pain. Neurogastroenterol. Motil. 2020, 33, e14003. [Google Scholar] [CrossRef]
- Qin, Y.; Verdegaal, E.M.E.; Siderius, M.; Bebelman, J.P.; Smit, M.J.; Leurs, R.; Willemze, R.; Tensen, C.P.; Osanto, S. Quantitative expression profiling of G-protein-coupled receptors (GPCRs) in metastatic melanoma: The constitutively active orphan GPCR GPR18 as novel drug target. Pigment. Cell Melanoma Res. 2011, 24, 207–218. [Google Scholar] [CrossRef]
- Sugiura, T.; Kobayashi, Y.; Oka, S.; Waku, K. Biosynthesis and degradation of anandamide and 2-arachidonoylglycerol and their possible physiological significance. Prostaglandins Leukot. Essent. Fat. Acids 2002, 66, 173–192. [Google Scholar] [CrossRef]
- Di Marzo, V. Endocannabinoids: Synthesis and degradation. Rev. Physiol. Biochem. Pharmacol. 2006, 160, 1–24. [Google Scholar] [CrossRef]
- Petrosino, S.; Di Marzo, V. The pharmacology of palmitoylethanolamide and first data on the therapeutic efficacy of some of its new formulations. Br. J. Pharmacol. 2016, 174, 1349–1365. [Google Scholar] [CrossRef] [PubMed]
- Yesilyurt, O.; Cayirli, M.; Sakin, Y.S.; Seyrek, M.; Akar, A.; Dogrul, A. Systemic and spinal administration of FAAH, MAGL inhibitors and dual FAAH/MAGL inhibitors produce antipruritic effect in mice. Arch. Dermatol. Res. 2016, 308, 335–345. [Google Scholar] [CrossRef] [PubMed]
- Schlosburg, J.E.; Boger, D.L.; Cravatt, B.F.; Lichtman, A.H. Endocannabinoid Modulation of Scratching Response in an Acute Allergenic Model: A New Prospective Neural Therapeutic Target for Pruritus. J. Pharmacol. Exp. Ther. 2009, 329, 314–323. [Google Scholar] [CrossRef] [Green Version]
- Sasso, O.; Summa, M.; Armirotti, A.; Pontis, S.; De Mei, C.; Piomelli, D. The N-Acylethanolamine Acid Amidase Inhibitor ARN077 Suppresses Inflammation and Pruritus in a Mouse Model of Allergic Dermatitis. J. Investig. Dermatol. 2018, 138, 562–569. [Google Scholar] [CrossRef] [Green Version]
- Nordlind, K.; Azmitia, E.; Slominski, A. The skin as a mirror of the soul: Exploring the possible roles of serotonin. Exp. Dermatol. 2008, 17, 301–311. [Google Scholar] [CrossRef]
- Clapham, D.E.; Runnels, L.; Strübing, C. The trp ion channel family. Nat. Rev. Neurosci. 2001, 2, 387–396. [Google Scholar] [CrossRef]
- Rigamonti, E.; Chinetti, G.; Staels, B. Regulation of Macrophage Functions by PPAR-α, PPAR-γ, and LXRs in Mice and Men. Arter. Thromb. Vasc. Biol. 2008, 28, 1050–1059. [Google Scholar] [CrossRef] [Green Version]
- Bagood, M.; Isseroff, R. TRPV1: Role in Skin and Skin Diseases and Potential Target for Improving Wound Healing. Int. J. Mol. Sci. 2021, 22, 6135. [Google Scholar] [CrossRef]
- Muller, C.; Morales, P.; Reggio, P.H. Cannabinoid Ligands Targeting TRP Channels. Front. Mol. Neurosci. 2019, 11, 487. [Google Scholar] [CrossRef]
- Bonchak, J.G.; Swerlick, R.A. Emerging therapies for atopic dermatitis: TRPV1 antagonists. J. Am. Acad. Dermatol. 2018, 78, S63–S66. [Google Scholar] [CrossRef]
- Ishii, T.; Uchida, K.; Hata, S.; Hatta, M.; Kita, T.; Miyake, Y.; Okamura, K.; Tamaoki, S.; Ishikawa, H.; Yamazaki, J. TRPV2 channel inhibitors attenuate fibroblast differentiation and contraction mediated by keratinocyte-derived TGF-β1 in an in vitro wound healing model of rats. J. Dermatol. Sci. 2018, 90, 332–342. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Tóth, K.F.; Ádám, D.; Bíró, T.; Oláh, A. Cannabinoid signaling in the skin: Therapeutic potential of the “c(ut)annabinoid” system. Molecules 2019, 24, 918. [Google Scholar] [CrossRef] [Green Version]
- Cao, X.; Yang, F.; Zheng, J.; Wang, K. Intracellular Proton-mediated Activation of TRPV3 Channels Accounts for the Exfoliation Effect of α-Hydroxyl Acids on Keratinocytes. J. Biol. Chem. 2012, 287, 25905–25916. [Google Scholar] [CrossRef] [Green Version]
- Qu, Y.; Wang, G.; Sun, X.; Wang, K. Inhibition of the Warm Temperature-Activated Ca2+-Permeable Transient Receptor Potential Vanilloid TRPV3 Channel Attenuates Atopic Dermatitis. Mol. Pharmacol. 2019, 96, 393–400. [Google Scholar] [CrossRef]
- Sokabe, T.; Tominaga, M. The TRPV4 cation channel. Commun. Integr. Biol. 2010, 3, 619–621. [Google Scholar] [CrossRef]
- Goswami, R.; Cohen, J.; Sharma, S.; Zhang, D.X.; Lafyatis, R.; Bhawan, J.; Rahaman, S.O. TRPV4 ION Channel Is Associated with Scleroderma. J. Investig. Dermatol. 2017, 137, 962–965. [Google Scholar] [CrossRef] [Green Version]
- Maglie, R.; de Araujo, D.S.M.; Antiga, E.; Geppetti, P.; Nassini, R.; De Logu, F. The Role of TRPA1 in Skin Physiology and Pathology. Int. J. Mol. Sci. 2021, 22, 3065. [Google Scholar] [CrossRef]
- Borrelli, F.; Pagano, E.; Romano, B.; Panzera, S.; Maiello, F.; Coppola, D.; De Petrocellis, L.; Buono, L.; Orlando, P.; Izzo, A.A. Colon carcinogenesis is inhibited by the TRPM8 antagonist cannabigerol, a Cannabis-derived non-psychotropic cannabinoid. Carcinogenesis 2014, 35, 2787–2797. [Google Scholar] [CrossRef] [Green Version]
- Dubrac, S.; Schmuth, M. PPAR-alpha in cutaneous inflammation. Dermato-Endocrinology 2011, 3, 23–26. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Mastrofrancesco, A.; Kovacs, D.; Sarra, M.; Bastonini, E.; Cardinali, G.; Aspite, N.; Camera, E.; Chavatte, P.; Desreumaux, P.; Monteleone, G.; et al. Preclinical Studies of a Specific PPARγ Modulator in the Control of Skin Inflammation. J. Investig. Dermatol. 2014, 134, 1001–1011. [Google Scholar] [CrossRef] [Green Version]
- Ghosh, A.K. Pharmacological activation of PPAR-γ: A potential therapy for skin fibrosis. Int. J. Dermatol. 2020, 60, 376–383. [Google Scholar] [CrossRef] [PubMed]
- Gonzalez, E.G.; Selvi, E.; Balistreri, E.; Akhmetshina, A.; Palumbo, K.; Lorenzini, S.; Lazzerini, P.E.; Montilli, C.; Capecchi, P.L.; Lucattelli, M.; et al. Synthetic cannabinoid ajulemic acid exerts potent antifibrotic effects in experimental models of systemic sclerosis. Ann. Rheum. Dis. 2012, 71, 1545–1551. [Google Scholar] [CrossRef] [Green Version]
- Correia-Sá, I.; Paiva, A.; Carvalho, C.M.; Vieira-Coelho, M.A. Cutaneous endocannabinoid system: Does it have a role on skin wound healing bearing fibrosis? Pharmacol. Res. 2020, 159, 104862. [Google Scholar] [CrossRef] [PubMed]
- Martins, A.M.; Ascenso, A.; Ribeiro, H.M.; Marto, J. Current and Future Therapies for Psoriasis with a Focus on Serotonergic Drugs. Mol. Neurobiol. 2020, 57, 2391–2419. [Google Scholar] [CrossRef] [PubMed]
- Martins, A.M.; Ascenso, A.; Ribeiro, H.M.; Marto, J. The Brain–Skin Connection and the Pathogenesis of Psoriasis: A Review with a Focus on the Serotonergic System. Cells 2020, 9, 796. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Kawana, S.; Kato, Y.; Omi, T. Efficacy of a 5-HT1a receptor agonist in atopic dermatitis. Clin. Exp. Dermatol. 2010, 35, 835–840. [Google Scholar] [CrossRef]
- Sadiq, A.; Menchetti, I.; Shah, A.; Jeschke, M.G.; Belo, C.; Carlos-Alcalde, W.; Hayat, M.Q.; Amini-Nik, S. 5-HT1A Receptor Function Makes Wound Healing a Happier Process. Front. Pharmacol. 2018, 9, 1406. [Google Scholar] [CrossRef]
- Wetterberg, J.; Taher, C.; Azmitia, E.; Elnour, H. Time-dependent modulation of serotonin and its receptors 1A and 2A expression in allergic contact dermatitis. J. Eur. Acad. Dermatol. Venereol. 2011, 25, 1200–1205. [Google Scholar] [CrossRef]
- Baswan, S.M.; Klosner, A.E.; Glynn, K.; Rajgopal, A.; Malik, K.; Yim, S.; Stern, N. Therapeutic Potential of Cannabidiol (CBD) for Skin Health and Disorders. Clin. Cosmet. Investig. Dermatol. 2020, 13, 927–942. [Google Scholar] [CrossRef]
- Dawidowicz, A.L.; Olszowy-Tomczyk, M.; Typek, R. CBG, CBD, Δ9-THC, CBN, CBGA, CBDA and Δ9-THCA as antioxidant agents and their intervention abilities in antioxidant action. Fitoterapia 2021, 152, 104915. [Google Scholar] [CrossRef] [PubMed]
- Johnson, J.V.; Christensen, A.; Morgan, D.; Basso, K.B. Gas chromatography/electron ionization mass spectrometry (GC/EI-MS) for the characterization of phytocannabinoids in Cannabis sativa. Compr. Anal. Chemistry 2020, 90, 235–274. [Google Scholar] [CrossRef]
- Site How Biosynthesis of Cannabinoids Could Impact the Cannabis Industry–New Cannabis Ventures. Available online: https://www.newcannabisventures.com/how-biosynthesis-of-cannabinoids-could-impact-the-cannabis-industry/ (accessed on 12 July 2021).
- Hartsel, J.A.; Eades, J.; Hickory, B.; Makriyannis, A. Cannabis sativa and Hemp. In Nutraceuticals: Efficacy, Safety and Toxicity; Elsevier Inc.: Amsterdam, The Netherlands, 2016; pp. 735–754. ISBN 9780128021477. [Google Scholar]
- Brousseau, V.D.; Wu, B.-S.; MacPherson, S.; Morello, V.; Lefsrud, M. Cannabinoids and Terpenes: How Production of Photo-Protectants Can Be Manipulated to Enhance Cannabis sativa L. Phytochemistry. Front. Plant Sci. 2021, 12. [Google Scholar] [CrossRef]
- Turner, S.E.; Williams, C.M.; Iversen, L.; Whalley, B.J. Molecular Pharmacology of Phytocannabinoids. Phytocannabinoids 2017, 103, 61–101. [Google Scholar] [CrossRef]
- Zagzoog, A.; Mohamed, K.A.; Kim, H.J.J.; Kim, E.D.; Frank, C.S.; Black, T.; Jadhav, P.D.; Holbrook, L.A.; Laprairie, R.B. In vitro and in vivo pharmacological activity of minor cannabinoids isolated from Cannabis sativa. Sci. Rep. 2020, 10, 1–13. [Google Scholar] [CrossRef]
- Palomares, B.; Garrido-Rodriguez, M.; Gonzalo-Consuegra, C.; Gómez-Cañas, M.; Saen-Oon, S.; Soliva, R.; Collado, J.A.; Fernández-Ruiz, J.; Morello, G.; Calzado, M.A.; et al. Δ 9 -Tetrahydrocannabinolic acid alleviates collagen-induced arthritis: Role of PPARγ and CB 1 receptors. Br. J. Pharmacol. 2020, 177, 4034–4054. [Google Scholar] [CrossRef]
- Oláh, A.; Tóth, B.I.; Borbíró, I.; Sugawara, K.; Szöllõsi, A.G.; Czifra, G.; Pál, B.; Ambrus, L.; Kloepper, J.; Camera, E.; et al. Cannabidiol exerts sebostatic and antiinflammatory effects on human sebocytes. J. Clin. Invest. 2014, 124, 3713–3724. [Google Scholar] [CrossRef] [Green Version]
- Steenson, S.; Chambers, L. Cannabidiol: A budding industry! Nutr. Bull. 2019, 44, 228–240. [Google Scholar] [CrossRef]
- Rosenthaler, S.; Pöhn, B.; Kolmanz, C.; Nguyen Huu, C.; Krewenka, C.; Huber, A.; Kranner, B.; Rausch, W.D.; Moldzio, R. Differences in receptor binding affinity of several phytocannabinoids do not explain their effects on neural cell cultures. Neurotoxicol. Teratol. 2014, 46, 49–56. [Google Scholar] [CrossRef]
- Nachnani, R.; Raup-Konsavage, W.M.; Vrana, K.E. The Pharmacological Case for Cannabigerol. J. Pharmacol. Exp. Ther. 2020, 376, 204–212. [Google Scholar] [CrossRef]
- Navarro, G.; Varani, K.; Lillo, A.; Vincenzi, F.; Rivas-Santisteban, R.; Raïch, I.; Reyes-Resina, I.; Ferreiro-Vera, C.; Borea, P.A.; de Medina, V.S.; et al. Pharmacological data of cannabidiol- and cannabigerol-type phytocannabinoids acting on cannabinoid CB1, CB2 and CB1/CB2 heteromer receptors. Pharmacol. Res. 2020, 159, 104940. [Google Scholar] [CrossRef] [PubMed]
- Udoh, M.; Santiago, M.; Devenish, S.; McGregor, I.S.; Connor, M. Cannabichromene is a cannabinoid CB 2 receptor agonist. Br. J. Pharmacol. 2019, 176, 4537–4547. [Google Scholar] [CrossRef]
- dos Santos, R.G.; Hallak, J.E.C.; Crippa, J.A.S. Neuropharmacological Effects of the Main Phytocannabinoids: A Narrative Review. Cannabinoids Neuropsychiatr. Disord. 2020, 1264, 29–45. [Google Scholar] [CrossRef]
- McHugh, D.; Page, J.; Dunn, E.; Bradshaw, H.B. Δ 9-tetrahydrocannabinol and N-arachidonyl glycine are full agonists at GPR18 receptors and induce migration in human endometrial HEC-1B cells. Br. J. Pharmacol. 2012, 165, 2414–2424. [Google Scholar] [CrossRef] [Green Version]
- Zhong, N. Cannabinol Inhibits Proliferation and Induces Cell Cycle Arrest and Apoptosis in Glioblastoma, Hepatocellular Carcinoma and Breast Cancer Cells. Master’s Thesis, University of Lethbridge, Lethbridge, Alta, 2020. [Google Scholar]
- Anavi-Goffer, S.; Baillie, G.; Irving, A.J.; Gertsch, J.; Greig, I.R.; Pertwee, R.G.; Ross, R.A. Modulation of l-α-Lysophosphatidylinositol/GPR55 Mitogen-activated Protein Kinase (MAPK) Signaling by Cannabinoids. J. Biol. Chem. 2012, 287, 91–104. [Google Scholar] [CrossRef] [Green Version]
- Ryberg, E.; Larsson, N.; Sjögren, S.; Hjorth, S.; Hermansson, N.O.; Leonova, J.; Elebring, T.; Nilsson, K.; Drmota, T.; Greasley, P.J. The orphan receptor GPR55 is a novel cannabinoid receptor. Br. J. Pharmacol. 2007, 152, 1092–1101. [Google Scholar] [CrossRef]
- De Petrocellis, L.; Ligresti, A.; Moriello, A.S.; Allarà, M.; Bisogno, T.; Petrosino, S.; Stott, C.G.; Di Marzo, V. Effects of cannabinoids and cannabinoid-enrichedCannabisextracts on TRP channels and endocannabinoid metabolic enzymes. Br. J. Pharmacol. 2011, 163, 1479–1494. [Google Scholar] [CrossRef] [Green Version]
- De Petrocellis, L.; Orlando, P.; Moriello, A.S.; Aviello, G.; Stott, C.; Izzo, A.; Di Marzo, V. Cannabinoid actions at TRPV channels: Effects on TRPV3 and TRPV4 and their potential relevance to gastrointestinal inflammation. Acta Physiol. 2011, 204, 255–266. [Google Scholar] [CrossRef]
- O’Sullivan, S.E. An update on PPAR activation by cannabinoids. Br. J. Pharmacol. 2016, 173, 1899–1910. [Google Scholar] [CrossRef] [Green Version]
- Palomares, B.; Ruiz-Pino, F.; Garrido-Rodriguez, M.; Prados, M.E.; Sánchez-Garrido, M.A.; Velasco, I.; Vazquez, M.J.; Nadal, X.; Ferreiro-Vera, C.; Morrugares, R.; et al. Tetrahydrocannabinolic acid A (THCA-A) reduces adiposity and prevents metabolic disease caused by diet-induced obesity. Biochem. Pharmacol. 2020, 171, 113693. [Google Scholar] [CrossRef] [PubMed]
- D’Aniello, E.; Fellous, T.; Iannotti, F.; Gentile, A.; Allarà, M.; Balestrieri, F.; Gray, R.; Amodeo, P.; Vitale, R.M.; Di Marzo, V. Identification and characterization of phytocannabinoids as novel dual PPARα/γ agonists by a computational and in vitro experimental approach. Biochim. et Biophys. Acta (BBA)-Gen. Subj. 2019, 1863, 586–597. [Google Scholar] [CrossRef] [PubMed]
- Granja, A.G.; Carrillo-Salinas, F.J.; Pagani, A.; Gómez-Cañas, M.; Negri, R.; Navarrete, C.M.; Mecha, M.; Mestre, L.; Fiebich, B.L.; Cantarero, I.; et al. A Cannabigerol Quinone Alleviates Neuroinflammation in a Chronic Model of Multiple Sclerosis. J. Neuroimmune Pharmacol. 2012, 7, 1002–1016. [Google Scholar] [CrossRef] [PubMed]
- O’Sullivan, S.E.; Sun, Y.; Bennett, A.J.; Randall, M.D.; Kendall, D.A. Time-dependent vascular actions of cannabidiol in the rat aorta. Eur. J. Pharmacol. 2009, 612, 61–68. [Google Scholar] [CrossRef] [PubMed]
- Formato, M.; Crescente, G.; Scognamiglio, M.; Fiorentino, A.; Pecoraro, M.T.; Piccolella, S.; Catauro, M.; Pacifico, S. (‒)-Cannabidiolic Acid, a Still Overlooked Bioactive Compound: An Introductory Review and Preliminary Research. Molecules 2020, 25, 2638. [Google Scholar] [CrossRef] [PubMed]
- Braida, D.; Limonta, V.; Malabarba, L.; Zani, A.; Sala, M. 5-HT1A receptors are involved in the anxiolytic effect of Δ9-tetrahydrocannabinol and AM 404, the anandamide transport inhibitor, in Sprague–Dawley rats. Eur. J. Pharmacol. 2007, 555, 156–163. [Google Scholar] [CrossRef] [PubMed]
- Cascio, M.G.; Zamberletti, E.; Marini, P.; Parolaro, D.; Pertwee, R.G. The phytocannabinoid, Δ9-tetrahydrocannabivarin, can act through 5-HT1Areceptors to produce antipsychotic effects. Br. J. Pharmacol. 2015, 172, 1305–1318. [Google Scholar] [CrossRef] [Green Version]
- Rock, E.M.; Sullivan, M.T.; Collins, S.A.; Goodman, H.; Limebeer, C.L.; Mechoulam, R.; Parker, L.A. Evaluation of repeated or acute treatment with cannabidiol (CBD), cannabidiolic acid (CBDA) or CBDA methyl ester (HU-580) on nausea and/or vomiting in rats and shrews. Psychopharmacology 2020, 237, 2621–2631. [Google Scholar] [CrossRef]
- Bolognini, D.; Rock, E.M.; Cluny, N.L.; Cascio, M.G.; Limebeer, C.L.; Duncan, M.; Stott, C.G.; Javid, F.; Parker, L.A.; Pertwee, R.G. Cannabidiolic acid prevents vomiting inSuncus murinusand nausea-induced behaviour in rats by enhancing 5-HT1Areceptor activation. Br. J. Pharmacol. 2013, 168, 1456–1470. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Duggan, P.J. The Chemistry of Cannabis and Cannabinoids. Aust. J. Chem. 2021, 74, 369. [Google Scholar] [CrossRef]
- Russo, E.; Burnett, A.; Hall, B.; Parker, K.K. Agonistic Properties of Cannabidiol at 5-HT1a Receptors. Neurochem. Res. 2005, 30, 1037–1043. [Google Scholar] [CrossRef]
- Xiong, W.; Koo, B.-N.; Morton, R.; Zhang, L. Psychotropic and nonpsychotropic cannabis derivatives inhibit human 5-HT3A receptors through a receptor desensitization-dependent mechanism. Neuroscience 2011, 184, 28–37. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- PPucci, M.; Rapino, C.; Di Francesco, A.; Dainese, E.; D’Addario, C.; Maccarrone, M. Epigenetic control of skin differentiation genes by phytocannabinoids. Br. J. Pharmacol. 2013, 170, 581–591. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Bickers, D.R.; Athar, M. Oxidative Stress in the Pathogenesis of Skin Disease. J. Investig. Dermatol. 2006, 126, 2565–2575. [Google Scholar] [CrossRef] [Green Version]
- Cascio, M.G.; Gauson, L.A.; Stevenson, L.A.; Ross, R.A.; Pertwee, R.G. Evidence that the plant cannabinoid cannabigerol is a highly potent α2-adrenoceptor agonist and moderately potent 5HT1A receptor antagonist. Br. J. Pharmacol. 2010, 159, 129–141. [Google Scholar] [CrossRef] [Green Version]
- Pollastro, F.; Caprioglio, D.; Prete, D.D.; Rogati, F.; Minassi, A.; Taglialatela-Scafati, O.; Munoz, E.; Appendino, G. Cannabichromene. Nat. Prod. Commun. 2018, 13, 1189–1194. [Google Scholar] [CrossRef] [Green Version]
- Zamberletti, E.; Rubino, T.; Parolaro, D. Therapeutic potential of cannabidivarin for epilepsy and autism spectrum disorder. Pharmacol. Ther. 2021, 226, 107878. [Google Scholar] [CrossRef]
- Fuziwara, S.; Suzuki, A.; Inoue, K.; Denda, M. Dopamine D2-Like Receptor Agonists Accelerate Barrier Repair and Inhibit the Epidermal Hyperplasia Induced by Barrier Disruption. J. Investig. Dermatol. 2005, 125, 783–789. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Vaughn, A.R.; Davis, M.J.; Sivamani, R.K.; Isseroff, R.R. A Concise Review of the Conflicting Roles of Dopamine-1 versus Dopamine-2 Receptors in Wound Healing. Molecules 2017, 23, 50. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Parrado, A.C.; Salaverry, L.S.; Mangone, F.M.; Apicella, C.E.; Gentile, T.; Canellada, A.; Rey-Roldán, E.B. Differential Response of Dopamine Mediated by β-Adrenergic Receptors in Human Keratinocytes and Macrophages: Potential Implication in Wound Healing. Neuroimmunomodulation 2017, 24, 282–291. [Google Scholar] [CrossRef]
- Formukong, E.A.; Evans, A.T.; Evans, F.J. Analgesic and antiinflammatory activity of constituents ofCannabis sativa L. Inflammation 1988, 12, 361–371. [Google Scholar] [CrossRef] [PubMed]
- Oláh, A.; Markovics, A.; Szabó-Papp, J.; Szabó, P.T.; Stott, C.; Zouboulis, C.P.D.; Bíró, T. Differential effectiveness of selected non-psychotropic phytocannabinoids on human sebocyte functions implicates their introduction in dry/seborrhoeic skin and acne treatment. Exp. Dermatol. 2016, 25, 701–707. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- ASX/Media Release BTX 1503 acne Phase 2 study results presentation; Philadelphia PA and Syndey Australia. 2019. Available online: https://www.asx.com.au/asxpdf/20191023/pdf/449s36d2bz6vfr.pdf (accessed on 11 August 2021).
- Petrosino, S.; Verde, R.; Vaia, M.; Allarà, M.; Iuvone, T.; Di Marzo, V. Anti-inflammatory Properties of Cannabidiol, a Nonpsychotropic Cannabinoid, in Experimental Allergic Contact Dermatitis. J. Pharmacol. Exp. Ther. 2018, 365, 652–663. [Google Scholar] [CrossRef] [PubMed]
- Kozela, E.; Juknat, A.; Kaushansky, N.; Ben-Nun, A.; Coppola, G.; Vogel, Z. Cannabidiol, a non-psychoactive cannabinoid, leads to EGR2-dependent anergy in activated encephalitogenic T cells. J. Neuroinflammation 2015, 12, 52. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Gaffal, E.; Cron, M.; Glodde, N.; Tüting, T. Anti-inflammatory activity of topical THC in DNFB-mediated mouse allergic contact dermatitis independent of CB1 and CB2 receptors. Allergy 2013, 68, 994–1000. [Google Scholar] [CrossRef]
- Maor, Y.; Yu, J.; Kuzontkoski, P.M.; Dezube, B.J.; Zhang, X.; Groopman, J.E. Cannabidiol Inhibits Growth and Induces Programmed Cell Death in Kaposi Sarcoma-Associated Herpesvirus-Infected Endothelium. Genes Cancer 2012, 3, 512–520. [Google Scholar] [CrossRef] [Green Version]
- Armstrong, J.; Hill, D.S.; McKee, C.S.; Hernandez-Tiedra, S.; Lorente, M.; Lopez-Valero, I.; Anagnostou, M.E.; Babatunde, F.; Corazzari, M.; Redfern, C.; et al. Exploiting Cannabinoid-Induced Cytotoxic Autophagy to Drive Melanoma Cell Death. J. Investig. Dermatol. 2015, 135, 1629–1637. [Google Scholar] [CrossRef] [Green Version]
- Glodde, N.; Jakobs, M.; Bald, T.; Tüting, T.; Gaffal, E. Differential role of cannabinoids in the pathogenesis of skin cancer. Life Sci. 2015, 138, 35–40. [Google Scholar] [CrossRef] [PubMed]
- Simmerman, E.; Qin, X.; Yu, J.C.; Baban, B. Cannabinoids as a Potential New and Novel Treatment for Melanoma: A Pilot Study in a Murine Model. J. Surg. Res. 2019, 235, 210–215. [Google Scholar] [CrossRef]
- Wilkinson, J.D.; Williamson, E. Cannabinoids inhibit human keratinocyte proliferation through a non-CB1/CB2 mechanism and have a potential therapeutic value in the treatment of psoriasis. J. Dermatol. Sci. 2007, 45, 87–92. [Google Scholar] [CrossRef]
- Changoer, L.; Anastassov, G. METHOD TO TREAT PSORIASIS 2019. Available online: https://patentscope.wipo.int/search/en/detail.jsf?docId=US238100786&docAn=16106420 (accessed on 11 August 2021).
- Muscarà, C.; Smeriglio, A.; Trombetta, D.; Mandalari, G.; La Camera, E.; Occhiuto, C.; Grassi, G.; Circosta, C. Antioxidant and antimicrobial activity of two standardized extracts from a new Chinese accession of non-psychotropic Cannabis sativa L. Phytotherapy Res. 2020, 35, 1099–1112. [Google Scholar] [CrossRef]
- Casares, L.; García, V.; Garrido-Rodriguez, M.; Millán, E.; Collado, J.A.; García-Martín, A.; Peñarando, J.; Calzado, M.A.; de la Vega, L.; Muñoz, E. Cannabidiol induces antioxidant pathways in keratinocytes by targeting BACH1. Redox Biol. 2020, 28, 101321. [Google Scholar] [CrossRef] [PubMed]
- Zagórska-Dziok, M.; Bujak, T.; Ziemlewska, A.; Nizioł-Łukaszewska, Z. Positive Effect of Cannabis sativa L. Herb Extracts on Skin Cells and Assessment of Cannabinoid-Based Hydrogels Properties. Molecules 2021, 26, 802. [Google Scholar] [CrossRef] [PubMed]
- Appendino, G.; Gibbons, S.; Giana, A.; Pagani, A.; Grassi, G.; Stavri, M.; Smith, E.; Rahman, M. Antibacterial Cannabinoids from Cannabis sativa: A Structure−Activity Study. J. Nat. Prod. 2008, 71, 1427–1430. [Google Scholar] [CrossRef]
- Wardle, J. Linking Chemical Phenotypes of Different Varieties of Cannabis Sativa to Their Antimicrobial Activities against a Range of Microorganisms. Master’s Thesis, Manchester Metropolitan University, Manchester, UK, September 2019. [Google Scholar]
- Turner, C.E.; ElSohly, M.A. Biological Activity of Cannabichromene, its Homologs and Isomers. J. Clin. Pharmacol. 1981, 21, 283S–291S. [Google Scholar] [CrossRef] [PubMed]
- Karas, J.A.; Wong, L.J.M.; Paulin, O.K.A.; Mazeh, A.C.; Hussein, M.H.; Li, J.; Velkov, T. The Antimicrobial Activity of Cannabinoids. Antibiotics 2020, 9, 406. [Google Scholar] [CrossRef] [PubMed]
- Vacek, J.; Vostalova, J.; Papouskova, B.; Skarupova, D.; Kos, M.; Kabelac, M.; Storch, J. Antioxidant function of phytocannabinoids: Molecular basis of their stability and cytoprotective properties under UV-irradiation. Free. Radic. Biol. Med. 2021, 164, 258–270. [Google Scholar] [CrossRef]
- Millar, S.A.; Maguire, R.F.; Yates, A.S.; O’Sullivan, S.E. Towards Better Delivery of Cannabidiol (CBD). Pharmaceuticals 2020, 13, 219. [Google Scholar] [CrossRef]
- Bruni, N.; Della Pepa, C.; Oliaro-Bosso, S.; Pessione, E.; Gastaldi, D.; Dosio, F. Cannabinoid Delivery Systems for Pain and Inflammation Treatment. Molecules 2018, 23, 2478. [Google Scholar] [CrossRef] [Green Version]
- Casiraghi, A.; Musazzi, U.M.; Centin, G.; Franzè, S.; Minghetti, P. Topical Administration of Cannabidiol: Influence of Vehicle-Related Aspects on Skin Permeation Process. Pharmaceuticals 2020, 13, 337. [Google Scholar] [CrossRef]
- Ali, A.; Akhtar, N. The safety and efficacy of 3% Cannabis seeds extract cream for reduction of human cheek skin sebum and erythema content. Pak. J. Pharm. Sci. 2015, 28, 1389–1395. [Google Scholar]
- Adusumilli, N.C.; Hazuka, E.L.; Friedman, A.J. Nanotechnology to deliver cannabinoids in dermatology. Precis. Nanomed. 2021, 4, 787–794. [Google Scholar] [CrossRef]
- Da Porto, C.; Decorti, D.; Tubaro, F. Fatty acid composition and oxidation stability of hemp (Cannabis sativa L.) seed oil extracted by supercritical carbon dioxide. Ind. Crop. Prod. 2012, 36, 401–404. [Google Scholar] [CrossRef]
- Uluata, S.; Özdemir, N. Antioxidant Activities and Oxidative Stabilities of Some Unconventional Oilseeds. J. Am. Oil Chem. Soc. 2012, 89, 551–559. [Google Scholar] [CrossRef] [Green Version]
- Dąbrowski, G.; Skrajda, M. Frakcja Lipidowa I Białkowa Nasion Konopi Siewnych (C. sativa L.) Oraz Jej Korzystny Wpływ Na Zdrowie Człowieka = Lipid and Protein Fraction of Hemp Seed (C. sativa L.) And Its Beneficial Influence On Human Health. J. Educ. Health Sport. 2016, 6, 357–366. [Google Scholar] [CrossRef]
- Kazlauskienė, D.; Kasparavičienė, G.; Nenortienė, P.; Marksa, M.; Jukilaitytė, J.; Velžienė, S.; Ževžikovas, A. Determination of fatty acid composition and antioxidant activity in vegetable oils. Chemija 2021, 32. [Google Scholar] [CrossRef]
- Balić, A.; Vlašić, D.; Žužul, K.; Marinović, B.; Mokos, Z.B. Omega-3 Versus Omega-6 Polyunsaturated Fatty Acids in the Prevention and Treatment of Inflammatory Skin Diseases. Int. J. Mol. Sci. 2020, 21, 741. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Moore, E.M.; Wagner, C.; Komarnytsky, S. The Enigma of Bioactivity and Toxicity of Botanical Oils for Skin Care. Front. Pharmacol. 2020, 11. [Google Scholar] [CrossRef]
- Wydro, D.M. Omega-3 and 6 Acids in Medicine and Cosmetology. The Effect of Oral Supplementation with Omega-3 and 6 Acids on Skin Condition–Pilot Study. Available online: https://www.researchgate.net/publication/270960751_Kwasy_omega_3_i_6_w_medycynie_i_kosmetologii_Wplyw_doustnej_suplementacji_kwasami_omega-3_i_6_na_kondycje_skory_-_badanie_pilotazowe_Omega-3_and_6_acids_in_medicine_and_cosmetology_The_effect_of_oral_ (accessed on 15 June 2021).
- Pei, L.; Luo, Y.; Gu, X.; Wang, J. Formation, Stability and Properties of Hemp Seed Oil Emulsions for Application in the Cosmetics Industry. Tenside Surfactants Deterg. 2020, 57, 451–459. [Google Scholar] [CrossRef]
- Kurek-górecka, A.; Balwierz, R.; Mizera, P.; Nowak, M.; Żurawska-płaksej, E. L’importance thérapeutique et cosmétique de l ’ huile de chanvre. BioResources 2018, 16, 704–708. [Google Scholar]
- Metwally, S.; Ura, D.P.; Krysiak, Z.J.; Kaniuk, Ł.; Szewczyk, P.K.; Stachewicz, U. Electrospun PCL Patches with Controlled Fiber Morphology and Mechanical Performance for Skin Moisturization via Long-Term Release of Hemp Oil for Atopic Dermatitis. Membranes 2021, 11, 26. [Google Scholar] [CrossRef]
- Nowak, I.; Zielińska, A.K. tłuszczowe w olejach roślinnych i ich znaczenie w kosmetyce. Chemik 2014, 68, 103–110. [Google Scholar]
- Simopoulos, A. The importance of the ratio of omega-6/omega-3 essential fatty acids. Biomed. Pharmacother. 2002, 56, 365–379. [Google Scholar] [CrossRef]
- Cunliffe, W.J.; Holland, D.; Jeremy, A. Comedone formation: Etiology, clinical presentation, and treatment. Clin. Dermatol. 2004, 22, 367–374. [Google Scholar] [CrossRef] [PubMed]
- Callaway, J.; Schwab, U.; Harvima, I.; Halonen, P.; Mykkänen, O.; Hyvönen, P.; Järvinen, T. Efficacy of dietary hempseed oil in patients with atopic dermatitis. J. Dermatol. Treat. 2005, 16, 87–94. [Google Scholar] [CrossRef] [PubMed]
- Liang, J.; Aachary, A.A.; Thiyam-Holländer, U. Hemp Seed Oil: Minor components and oil quality. Lipid Technol. 2015, 27, 231–233. [Google Scholar] [CrossRef]
- Wisniewska, A.; Widomska, J.; Subczynski, W.K. Carotenoid-membrane interactions in liposomes: Effect of dipolar, monopolar, and nonpolar carotenoids. Acta Biochim. Pol. 2006, 53, 475–484. [Google Scholar] [CrossRef]
- Baswan, S.M.; Klosner, A.E.; Weir, C.; Salter-Venzon, D.; Gellenbeck, K.W.; Leveret, J.; Krutmann, J. Role of Ingestible Carotenoids in Skin Protection: A Review of Clinical Evidence. Photodermatol. Photoimmunol. Photomed. 2021. [Google Scholar] [CrossRef]
- Hajizadeh-Sharafabad, F.; Zahabi, E.S.; Malekahmadi, M.; Zarrin, R.; Alizadeh, M. Carotenoids supplementation and inflammation: A systematic review and meta-analysis of randomized clinical trials. Crit. Rev. Food Sci. Nutr. 2021, 1–17. [Google Scholar] [CrossRef]
- Atalay, S.; Jarocka-Karpowicz, I.; Skrzydlewska, E. Antioxidative and Anti-Inflammatory Properties of Cannabidiol. Antioxidants 2019, 9, 21. [Google Scholar] [CrossRef] [Green Version]
- Quirin, K. Phytosterol-Rich Soy Germ and Guggul Extracts Provide Anti-Ageing Benefits. Cosmet. Sci. Technol. 2011, 8, 18–27. [Google Scholar]
- Smith, L.W. The Present Status of topical Chlorophyll Therapy. NY State J. Med. 1995, 14, 2041–2050. [Google Scholar]
- Stephens, T.J.; McCook, J.P.; Herndon, J.H. Pilot Study of Topical Copper Chlorophyllin Complex in Subjects With Facial Acne and Large Pores. J. Drugs Dermatol. 2015, 14, 589–592. [Google Scholar] [PubMed]
- McCook, J.P.; Stephens, T.J.; Jiang, L.I.; Law, R.M.; Gotz, V. Ability of sodium copper chlorophyllin complex to repair photoaged skin by stimulation of biomarkers in human extracellular matrix. Clin. Cosmet. Investig. Dermatol. 2016, 9, 167–174. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Ferreira, V.D.S.; Sant’Anna, C. Impact of culture conditions on the chlorophyll content of microalgae for biotechnological applications. World J. Microbiol. Biotechnol. 2017, 33, 20. [Google Scholar] [CrossRef] [PubMed]
- O’sullivan, S.E. Marijuana and the Cannabinoids, 1st ed.; ElSohly, M.A., Ed.; Humana Press: Totowa, NJ, USA, 2007; ISBN 978-1-58829-456-2. [Google Scholar]
- McPartland, J.M.; Russo, E.B. Cannabis and Cannabis Extracts: Greater than The Sum of Their Parts. In Cannabis Therapeutics in HIV/AIDS; Taylor and Francis Inc.: Abingdon, UK, 2012; pp. 103–132. ISBN 9780203049105. [Google Scholar]
- Barrett, M.; Gordon, D.; Evans, F. Isolation from Cannabis sativa L. of cannflavin—A novel inhibitor of prostaglandin production. Biochem. Pharmacol. 1985, 34, 2019–2024. [Google Scholar] [CrossRef]
- Erridge, S.; Mangal, N.; Salazar, O.; Pacchetti, B.; Sodergren, M.H. Cannflavins–From plant to patient: A scoping review. Fitoterapia 2020, 146, 104712. [Google Scholar] [CrossRef] [PubMed]
- Calvi, L.; Pentimalli, D.; Panseri, S.; Giupponi, L.; Gelmini, F.; Beretta, G.; Vitali, D.; Bruno, M.; Zilio, E.; Pavlovic, R.; et al. Comprehensive quality evaluation of medical Cannabis sativa L. inflorescence and macerated oils based on HS-SPME coupled to GC–MS and LC-HRMS (q-exactive orbitrap®) approach. J. Pharm. Biomed. Anal. 2018, 150, 208–219. [Google Scholar] [CrossRef] [PubMed]
- Pavlovic, R.; Nenna, G.; Calvi, L.; Panseri, S.; Borgonovo, G.; Giupponi, L.; Cannazza, G.; Giorgi, A. Quality Traits of “Cannabidiol Oils”: Cannabinoids Content, Terpene Fingerprint and Oxidation Stability of European Commercially Available Preparations. Molecules 2018, 23, 1230. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Wakshlag, J.J.; Cital, S.; Eaton, S.J.; Prussin, R.; Hudalla, C. Cannabinoid, Terpene, and Heavy Metal Analysis of 29 Over-the-Counter Commercial Veterinary Hemp Supplements. Veter-Med. Res. Rep. 2020, 11, 45–55. [Google Scholar] [CrossRef] [Green Version]
- Leizer, C.; Ribnicky, D.; Poulev, A.; Dushenkov, S.; Raskin, I. The Composition of Hemp Seed Oil and Its Potential as an Important Source of Nutrition. J. Nutraceuticals Funct. Med. Foods 2000, 2, 35–53. [Google Scholar] [CrossRef] [Green Version]
- Hanuš, L.O.; Hod, Y. Terpenes/Terpenoids in Cannabis: Are They Important? Med. Cannabis Cannabinoids 2020, 3, 25–60. [Google Scholar] [CrossRef]
- Anand, U.; Pacchetti, B.; Anand, P.; Sodergren, M.H. Cannabis-based medicines and pain: A review of potential synergistic and entourage effects. Pain Manag. 2021, 11, 395–403. [Google Scholar] [CrossRef] [PubMed]
- Ben-Shabat, S.; Fride, E.; Sheskin, T.; Tamiri, T.; Rhee, M.H.; Vogel, Z.; Bisogno, T.; De Petrocellis, L.; Di Marzo, V.; Mechoulam, R. An entourage effect: Inactive endogenous fatty acid glycerol esters enhance 2-arachidonoyl-glycerol cannabinoid activity. Eur. J. Pharmacol. 1998, 353, 23–31. [Google Scholar] [CrossRef]
- Wagner, H.; Ulrich-Merzenich, G. Synergy research: Approaching a new generation of phytopharmaceuticals. Phytomedicine 2009, 16, 97–110. [Google Scholar] [CrossRef] [PubMed]
- Cogan, P.S. The ‘entourage effect’ or ‘hodge-podge hashish’: The questionable rebranding, marketing, and expectations of cannabis polypharmacy. Expert Rev. Clin. Pharmacol. 2020, 13, 835–845. [Google Scholar] [CrossRef]
- Russo, E.B. Taming THC: Potential cannabis synergy and phytocannabinoid-terpenoid entourage effects. Br. J. Pharmacol. 2011, 163, 1344–1364. [Google Scholar] [CrossRef] [PubMed]
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).