Antimicrobial Resistance in Escherichia coli and Its Correlation with Antimicrobial Use on Commercial Poultry Farms in Bangladesh
Abstract
:1. Introduction
2. Results
2.1. AMR Results
2.2. AMU in Flock Level
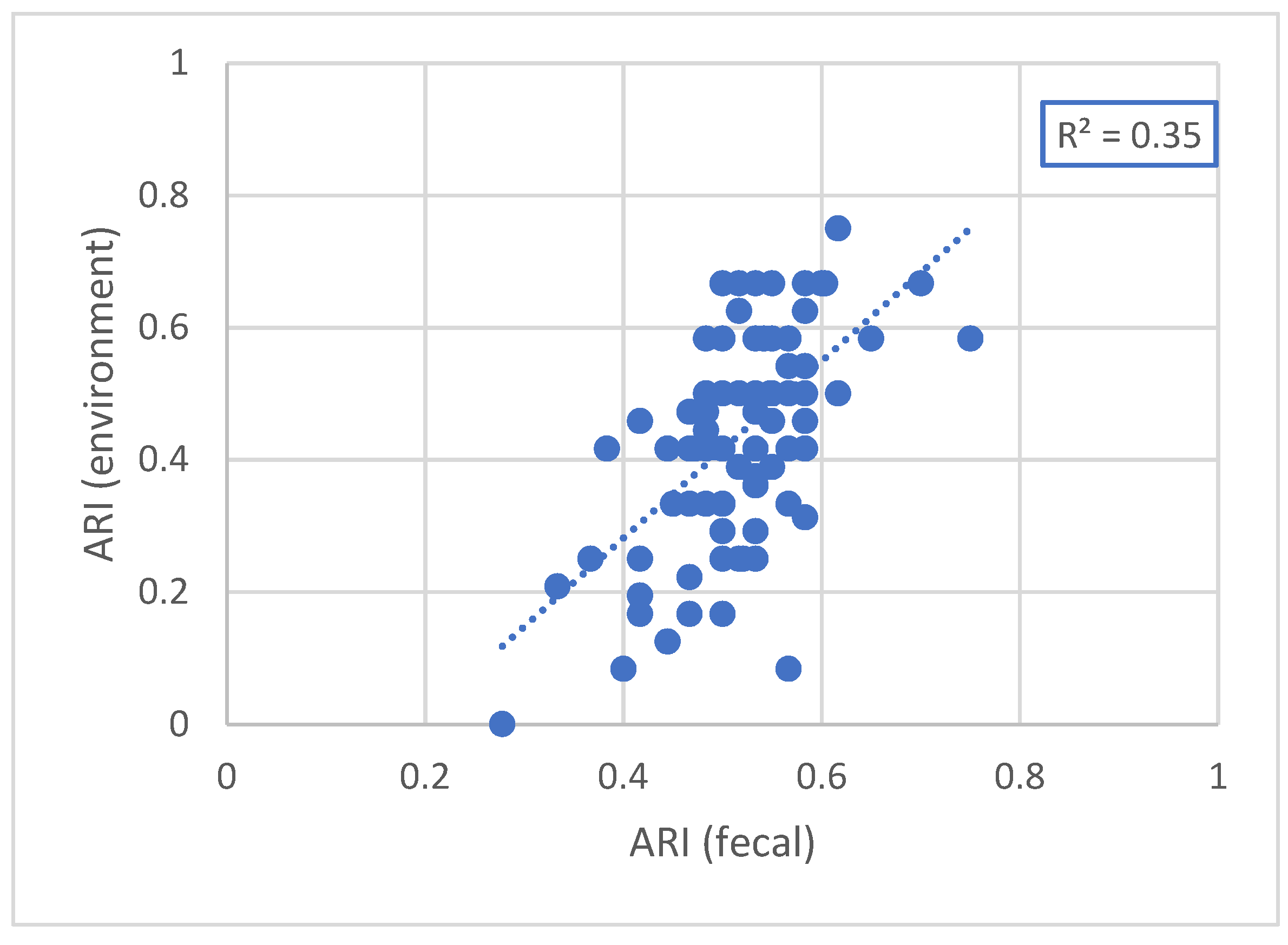
2.3. Linking Antimicrobial Use and Antimicrobial Resistance
3. Discussion
4. Materials and Methods
4.1. Study Design
4.2. AMU
4.3. Data Analysis
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- World Health Organization (WHO). Antibiotic Resistance. 2020. Available online: https://www.who.int/news-room/fact-sheets/detail/antibiotic-resistance (accessed on 17 May 2023).
- World Health Organization (WHO). Global Action Plan on Antimicrobial Resistance. 2015. Available online: https://www.amcra.be/swfiles/files/WHO%20actieplan_90.pdf (accessed on 16 May 2023).
- World Health Organization (WHO). Tripartite and UNEP Support OHHLEP’s Definition of ‘One Health’. 2021. Available online: https://www.who.int/news/item/01-12-2021-tripartite-and-unep-support-ohhlep-s-definition-of-one-health (accessed on 17 May 2023).
- Chereau, F.; Opatowski, L.; Tourdjman, M.; Vong, S. Risk assessment for antibiotic resistance in South East Asia. BMJ 2017, 358, j3393. [Google Scholar] [CrossRef] [PubMed]
- Harbarth, S.; Participants, F.T.W.H.-A.I.R.F.; Balkhy, H.H.; Goossens, H.; Jarlier, V.; Kluytmans, J.; Laxminarayan, R.; Saam, M.; Van Belkum, A.; Pittet, D. Antimicrobial resistance: one world, one fight! Antimicrob. Resist. Infect. Control. 2015, 4, 49. [Google Scholar]
- European Food Safety Authority and European Centre for Disease Prevention Control. EU Summary Report on antimicrobial resistance in zoonotic and indicator bacteria from humans, animals and food in 2013. EFSA J. 2015, 13, 4036. [Google Scholar]
- Marshall, B.M.; Levy, S.B. Food Animals and Antimicrobials: Impacts on Human Health. Clin. Microbiol. Rev. 2011, 24, 718–733. [Google Scholar] [CrossRef]
- Aarestrup, F.M.; Wegener, H.C.; Collignon, P. Resistance in bacteria of the food chain: epidemiology and control strategies. Expert Rev. Anti-Infective Ther. 2008, 6, 733–750. [Google Scholar] [CrossRef]
- Mellata, M. Human and avian extraintestinal pathogenic Escherichia coli: Infections, zoonotic risks, and antibiotic resistance trends. Foodborne Pathog. Dis. 2013, 10, 916–932. [Google Scholar] [CrossRef]
- World Organisation for Animal Health (WOAH). Terrestrial Animal Health Code. Available online: https://www.woah.org/app/uploads/2022/06/a-sixth-annual-report-amu-final.pdf (accessed on 21 May 2023).
- Katakweba, A.A.; Muhairwa, A.P.; Lupindu, A.M.; Damborg, P.; Rosenkrantz, J.T.; Minga, U.M.; Mtambo, M.M.; Olsen, J.E. First report on a randomized investigation of antimicrobial resistance in fecal indicator bacteria from livestock, poultry, and humans in Tanzania. Microb. Drug Resist. 2018, 24, 260–268. [Google Scholar] [CrossRef]
- Odonkor, S.T.; Addo, K.K. Prevalence of multidrug-resistant Escherichia coli isolated from drinking water sources. Int. J. Microbiol. 2018, 2018, 7204013. [Google Scholar] [CrossRef]
- Arsène-Ploetze, F.; Chiboub, O.; Lièvremont, D.; Farasin, J.; Freel, K.C.; Fouteau, S.; Barbe, V. Adaptation in toxic environments: comparative genomics of loci carrying antibiotic resistance genes derived from acid mine drainage waters. Environ. Sci. Pollut. Res. 2017, 25, 1470–1483. [Google Scholar] [CrossRef]
- Department of Livestock Services of Bangladesh. Fish Feed and Animal Feed Act 2010. Bangladesh Government. 2010. Available online: http://extwprlegs1.fao.org/docs/pdf/bgd165024.pdf (accessed on 23 May 2023).
- Directorate General of Health Services (DGHS). National Action Plan: Antimicrobial Resistance Containment in Bangladesh 2017–2022. In: Ministry of Health & Family Welfare, ed. 2017. Available online: https://cdn.who.int/media/docs/default-source/antimicrobial-resistance/amr-spc-npm/nap-library/antimicrobial-resistance-containment-in-bangladesh-2017-2022.pdf?sfvrsn=bfa46b_3&download=true (accessed on 23 May 2023).
- Goutard, F.L.; Bordier, M.; Calba, C.; Erlacher-Vindel, E.; Góchez, D.; de Balogh, K.; Benigno, C.; Kalpravidh, W.; Roger, F.; Vong, S. Antimicrobial policy interventions in food animal production in South East Asia. BMJ 2017, 358, j3544. [Google Scholar] [CrossRef]
- Imam, T.; Gibson, J.S.; Foysal, M.; Das, S.B.; Gupta, S.D.; Fournié, G.; Hoque, M.A.; Henning, J. A Cross-Sectional Study of Antimicrobial Usage on Commercial Broiler and Layer Chicken Farms in Bangladesh. Front. Vet. Sci. 2020, 7, 576113. [Google Scholar]
- Netherlands Enterprise Agency. Poultry sector study Bangladesh. 2020. Available online: https://www.rvo.nl/sites/default/files/2020/12/Poultry%20sector%20study%20Bangladesh.pdf (accessed on 22 May 2023).
- Antunes, P.; Novais, C.; Peixe, L. Food-to-Humans Bacterial Transmission. Microbiol. Spectr. 2020, 8, 161–193. [Google Scholar]
- Tasmim, S.T.; Hasan, M.; Talukder, S.; Mandal, A.K.; Parvin, M.S.; Ali, Y.; Ehsan, A.; Islam, T. Sociodemographic determinants of use and misuse of antibiotics in commercial poultry farms in Bangladesh. IJID Reg. 2023, 7, 146–158. [Google Scholar] [CrossRef] [PubMed]
- Uddin, B.; Alam, M.N.; Hasan, M.; Hossain, S.M.B.; Debnath, M.; Begum, R.; Samad, M.A.; Hoque, S.F.; Chowdhury, S.R.; Rahman, M.; et al. Molecular Detection of Colistin Resistance mcr-1 Gene in Multidrug-Resistant Escherichia coli Isolated from Chicken. Antibiotics 2022, 11, 97. [Google Scholar] [CrossRef] [PubMed]
- Mandal, A.K.; Talukder, S.; Hasan, M.; Tasmim, S.T.; Parvin, M.S.; Ali, Y.; Islam, T. Author response for ‘Epidemiology and antimicrobial resistance of Escherichia coli in broiler chickens, farmworkers, and farm sewage in Bangladesh’. Vet. Med. Sci. 2022, 8, 187–199. [Google Scholar] [CrossRef] [PubMed]
- Nandi, S.; Sultana, M.; Hossain, M. Prevalence and Characterization of Multidrug-Resistant Zoonotic Enterobacter spp. in Poultry of Bangladesh. Foodborne Pathog. Dis. 2013, 10, 420–427. [Google Scholar] [CrossRef]
- Fazal, M.A.; Nath, C.; Islam, M.S.; Hasib, F.Y.; Reza, M.M.B.; Devnath, H.S.; Nahid-Ibn-Rahman, M.; Ahad, A. Isolation and identification of multidrug-resistant Escherichia coli from cattle, sheep, poultry and human in Cumilla, Bangladesh. Malays. J. Microbiol. 2022, 18, 227–234. [Google Scholar]
- Rahman, A.; Khairalla, A. Susceptibility and Multidrug Resistance Patterns of Escherichia coli Isolated from Cloacal Swabs of Live Broiler Chickens in Bangladesh. Pathogens 2019, 8, 118. [Google Scholar]
- Clinical and Laboratory Standards Institute (CLSI), USA. CLSI M100-ED32:2022 Performance Standards for Antimicrobial Susceptibility Testing, 32nd ed. 2022. Available online: https://clsi.org/media/wi0pmpke/m100ed32_sample.pdf (accessed on 15 May 2023).
- Ibrahim, N.; Chantziaras, I.; Mohsin, M.A.S.; Boyen, F.; Fournié, G.; Islam, S.S.; Berge, A.C.; Caekebeke, N.; Joosten, P.; Dewulf, J. Quantitative and qualitative analysis of antimicrobial usage and biosecurity in broilers and Sonali poultry farms in Bangladesh. Prev. Vet. Med. 2023, 217, 105968. [Google Scholar]
- Islam, M.S.; Hossain, M.J.; Sobur, M.A.; Punom, S.A.; Rahman, A.M.M.; Rahman, M.T. A Systematic Review on the Occurrence of Antimicrobial-Resistant Escherichia coli in Poultry and Poultry Environments in Bangladesh between 2010 and 2021. BioMed Res. Int. 2023, 2023, 2425564. [Google Scholar] [CrossRef]
- Al Amin, A.; Hoque, M.N.; Siddiki, A.Z.; Saha, S.; Kamal, M. Antimicrobial resistance situation in animal health of Bangladesh. Vet World 2020, 13, 2713–2727. [Google Scholar] [CrossRef] [PubMed]
- Boyen, F.; Vangroenweghe, F.; Butaye, P.; De Graef, E.; Castryck, F.; Heylen, P.; Vanrobaeys, M.; Haesebrouck, F. Disk prediffusion is a reliable method for testing colistin susceptibility in porcine E. coli strains. Veter- Microbiol. 2010, 144, 359–362. [Google Scholar] [CrossRef] [PubMed]
- World Health Organization (WHO). Integrated Surveillance of Antimicrobial Resistance in Foodborne Bacteria: Application of a One Health Approach: Guidance from the WHO Advisory Group on Integrated Surveillanec of Antimicrobial Resistance (AGISAR); World Health Organization: Geneva, Switzerland, 2017; Available online: https://www.who.int/publications/i/item/9789241515528 (accessed on 25 May 2023).
- Ahmed, S.; Das, T.; Islam, Z.; Herrero-Fresno, A.; Biswas, P.K.; Olsen, J.E. High prevalence of mcr-1-encoded colistin resistance in commensal Escherichia coli from broiler chicken in Bangladesh. Sci. Rep. 2020, 10, 18637. [Google Scholar]
- Ban on All Forms of Combination Drug of Colistin and Ciprofloxacin; Directorate General of Drug Administration: Dhaka, Bangladesh, 2019.
- Circular of All Forms Colistin Ban; Directorate General of Drug Administration: Dhaka, Bangladesh, 2022.
- Parvin, M.S.; Ali, Y.; Mandal, A.K.; Talukder, S.; Islam, T. Sink survey to investigate multidrug resistance pattern of common foodborne bacteria from wholesale chicken markets in Dhaka city of Bangladesh. Sci. Rep. 2022, 12, 10818. [Google Scholar] [PubMed]
- Chantziaras, I.; Boyen, F.; Callens, B.; Dewulf, J. Correlation between veterinary antimicrobial use and antimicrobial resistance in food-producing animals: a report on seven countries. J. Antimicrob. Chemother. 2014, 69, 827–834. [Google Scholar] [CrossRef] [PubMed]
- Judicious Therapeutic Use of Antimicrobials; Association American Veterinary Medical: Schaumburg, IL, USA, 2004.
- More, S.J. European Perspectives on Efforts to Reduce Antimicrobial Usage in Food Animal Production. Ir. Vet. J. 2020, 73, 2. [Google Scholar] [CrossRef] [PubMed]
- Al Azad, M.A.R.; Rahman, M.M.; Amin, R.; Begum, M.I.A.; Fries, R.; Husna, A.; Khairalla, A.S.; Badruzzaman, A.T.M.; El Zowalaty, M.E.; Lampang, K.N.; et al. Prevalence of antimicrobial resistance of Escherichia coli isolated from broiler at Rajshahi region, Bangladesh. Pathogens 2019, 8, 118. [Google Scholar] [CrossRef] [PubMed]
- Schrauwen, E.J.A.; Huizinga, P.; Van Spreuwel, N.; Verhulst, C.; Bergh, M.F.Q.K.-V.D.; Kluytmans, J.A.J.W. High prevalence of the mcr-1 gene in retail chicken meat in the Netherlands in 2015. Antimicrob Resist. Infect Control 2017, 6, 83. [Google Scholar] [CrossRef] [PubMed]
- Lazarus, B.; Paterson, D.L.; Mollinger, J.L.; Rogers, B.A. Do human extraintestinal Escherichia coli infections resistant to expanded-spectrum cephalosporins originate from food-producing animals? A systematic review. Clin. Infect. Dis. 2014, 60, 439–452. [Google Scholar] [CrossRef] [PubMed]
- Collignon, P.J.; McEwen, S.A. One Health—Its Importance in Helping to Better Control Antimicrobial Resistance. Trop. Med. Infect. Dis. 2019, 4, 22. [Google Scholar] [CrossRef]
- Tang, K.L.; Caffrey, N.P.; Nóbrega, D.B.; Cork, S.C.; E Ronksley, P.; Barkema, H.W.; Polachek, A.J.; Ganshorn, H.; Sharma, N.; Kellner, J.D.; et al. Restricting the use of antibiotics in food-producing animals and its associations with antibiotic resistance in food-producing animals and human beings: a systematic review and meta-analysis. Lancet Planet. Health 2017, 1, e316–e327. [Google Scholar] [CrossRef] [PubMed]
- Levy, S.B. Balancing the drug-resistance equation. Trends Microbiol. 1994, 2, 341–342. [Google Scholar] [CrossRef] [PubMed]
- Austin, D.J.; Kristinsson, K.G.; Anderson, R.M. The relationship between the volume of antimicrobial consumption in human communities and the frequency of resistance. Proc. Natl. Acad. Sci. USA 1999, 96, 1152–1156. [Google Scholar] [CrossRef] [PubMed]
- Handel, A.; Regoes, R.R.; Antia, R. The Role of Compensatory Mutations in the Emergence of Drug Resistance. PLoS Comput. Biol. 2006, 2, e137. [Google Scholar] [CrossRef]
- Nilsson, O.; Börjesson, S.; Landén, A.; Bengtsson, B. Vertical transmission of Escherichia coli carrying plasmid-mediated AmpC (pAmpC) through the broiler production pyramid. J. Antimicrob. Chemother. 2014, 69, 1497–1500. [Google Scholar] [CrossRef]
- Davies, J.; Davies, D. Origins and evolution of antibiotic resistance. Microbiol. Mol. Biol. Rev. 2010, 74, 417–433. [Google Scholar] [CrossRef]
- Checkley, W.; Buckley, G.; Gilman, R.H.; Assis, A.M.; Guerrant, R.L.; Morris, S.S.; Mølbak, K.; Valentiner-Branth, P.; Lanata, C.F.; E Black, R.; et al. Multi-country analysis of the effects of diarrhoea on childhood stunting. Leuk. Res. 2008, 37, 816–830. [Google Scholar] [CrossRef]
- Vera, L.; Boyen, F.; Visscher, A.; Vandenbroucke, V.; Vanantwerpen, G.; Govaere, J. Limitations of a chromogenic agar plate for the identifying bacteria isolated from equine endometritis samples. Equine Veter- J. 2018, 51, 266–269. [Google Scholar] [CrossRef]
- European Committee on Antimicrobial Susceptibility Testing (EUCAST). MIC Distributions. 2022. Available online: https://www.eucast.org/mic_distributions_and_ecoffs/ (accessed on 15 May 2023).
- European Committee on Antimicrobial Susceptibility Testing (EUCAST). 2021. Available online: www.eucast.org (accessed on 15 May 2023).
- Cornaglia, G.; Hryniewicz, W.; Jarlier, V.; Kahlmeter, G.; Mittermayer, H.; Stratchounski, L.; Baquero, F. European recommendations for antimicrobial resistance surveillance. Clin. Microbiol. Infect. 2004, 10, 349–383. [Google Scholar] [CrossRef]
- Callens, B.; Persoons, D.; Maes, D.; Laanen, M.; Postma, M.; Boyen, F.; Haesebrouck, F.; Butaye, P.; Catry, B.; Dewulf, J. Prophylactic and metaphylactic antimicrobial use in Belgian fattening pig herds. Prev. Veter- Med. 2012, 106, 53–62. [Google Scholar] [CrossRef]
- European Food Safety Authority (EFSA). Antimicrobial Resistance Remains Commonly Detected in Bacteria in Humans, Animals and Food: EFSA-ECDC Report. 2014. Available online: https://www.efsa.europa.eu/en/press/news/140325 (accessed on 15 May 2023).



 —CLSI breakpoint between susceptible and intermediate,
—CLSI breakpoint between susceptible and intermediate,  —CLSI breakpoint between intermediate and resistant and
—CLSI breakpoint between intermediate and resistant and  —ECOFF value between wild type and non-wild type.
—ECOFF value between wild type and non-wild type.
 —CLSI breakpoint between susceptible and intermediate,
—CLSI breakpoint between susceptible and intermediate,  —CLSI breakpoint between intermediate and resistant and
—CLSI breakpoint between intermediate and resistant and  — ECOFF value between wild type and non-wild type.
— ECOFF value between wild type and non-wild type.| Name of Antibiotics | Number of Farms | No. of Susceptible Isolates | No. of Resistant Isolates | Prevalence of Resistance (%) | p Value | |
|---|---|---|---|---|---|---|
| Ciprofloxacin | Use | 64 | 4 | 311 | 99 | 0.399 |
| No use | 78 | 8 | 368 | 98 | ||
| Ampicillin | Use | 91 | 33 | 422 | 93 | 0.983 |
| No use | 51 | 17 | 219 | 93 | ||
| Tetracycline | Use | 75 | 2 | 361 | 99 | 0.01 |
| No use | 67 | 10 | 318 | 97 | ||
| Trimethoprim | Use | 22 | 7 | 101 | 94 | 0.760 |
| No use | 120 | 32 | 551 | 95 | ||
| Colistin | Use | 80 | 378 | 30 | 7 | 0.570 |
| No use | 62 | 266 | 17 | 6 | ||
| Gentamicin | Use | 8 | 25 | 15 | 38 | 0.02 |
| No use | 134 | 511 | 140 | 22 | ||
| Fluoroquinolones class | Use | 89 | 9 | 485 | 98 | 0.812 |
| No use | 53 | 3 | 194 | 98 | ||
| Sulfonamides class | Use | 101 | 26 | 475 | 95 | 0.829 |
| No use | 41 | 11 | 179 | 94 | ||
| Antimicrobial (Abbreviation) | Concentration Range Tested (mg/L) | Non-Wild-Type Population * (mg/L) | Clinical Breakpoint for Susceptibility # (mg/L) | Clinical Breakpoint for Resistance # (mg/L) |
|---|---|---|---|---|
| Ampicillin (AMP) | 1–64 | ≥8 | ≤8 | ≥32 |
| Cefotaxime (FOT) | 0.25–4 | ≥0.25 | ≤1 | ≥4 |
| Ceftazidime (TAZ) | 0.5–8 | ≥1 | ≤8 | ≥16 |
| Meropenem (MERO) | 0.03–16 | ≥0.06 | ≤1 | ≥4 |
| Nalidixic acid (NAL) | 4–128 | ≥8 | - | ≥32 |
| Ciprofloxacin (CIP) | 0.015–8 | ≥0.06 | ≤0.25 | ≥1 |
| Tetracycline (TET) | 2–64 | ≥8 | ≤4 | ≥16 |
| Colistin (COL) | 1–16 | ≥2 | ≤1 | ≥4 |
| Gentamicin (GEN) | 0.5–32 | ≥2 | ≤4 | ≥16 |
| Trimethoprim (TMP) | 0.25–32 | ≥2 | - | ≥16 |
| Sulfamethoxazole (SMX) | 8–1024 | - | - | ≥512 |
| Chloramphenicol (CHL) | 8–128 | ≥16 | ≤8 | ≥32 |
| Azithromycin (AZI) | 2–64 | ≥16 | - | ≥32 |
| Tigecycline (TGC) | 0.25–8 | ≥0.5 | - | - |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2023 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Ibrahim, N.; Boyen, F.; Mohsin, M.A.S.; Ringenier, M.; Berge, A.C.; Chantziaras, I.; Fournié, G.; Pfeiffer, D.; Dewulf, J. Antimicrobial Resistance in Escherichia coli and Its Correlation with Antimicrobial Use on Commercial Poultry Farms in Bangladesh. Antibiotics 2023, 12, 1361. https://doi.org/10.3390/antibiotics12091361
Ibrahim N, Boyen F, Mohsin MAS, Ringenier M, Berge AC, Chantziaras I, Fournié G, Pfeiffer D, Dewulf J. Antimicrobial Resistance in Escherichia coli and Its Correlation with Antimicrobial Use on Commercial Poultry Farms in Bangladesh. Antibiotics. 2023; 12(9):1361. https://doi.org/10.3390/antibiotics12091361
Chicago/Turabian StyleIbrahim, Nelima, Filip Boyen, Md. Abu Shoieb Mohsin, Moniek Ringenier, Anna Catharina Berge, Ilias Chantziaras, Guillaume Fournié, Dirk Pfeiffer, and Jeroen Dewulf. 2023. "Antimicrobial Resistance in Escherichia coli and Its Correlation with Antimicrobial Use on Commercial Poultry Farms in Bangladesh" Antibiotics 12, no. 9: 1361. https://doi.org/10.3390/antibiotics12091361
APA StyleIbrahim, N., Boyen, F., Mohsin, M. A. S., Ringenier, M., Berge, A. C., Chantziaras, I., Fournié, G., Pfeiffer, D., & Dewulf, J. (2023). Antimicrobial Resistance in Escherichia coli and Its Correlation with Antimicrobial Use on Commercial Poultry Farms in Bangladesh. Antibiotics, 12(9), 1361. https://doi.org/10.3390/antibiotics12091361









