Review of Stratum Corneum Impedance Measurement in Non-Invasive Penetration Application
Abstract
1. Introduction
- Skin impedance model;
- Electrodes for skin impedance measurement;
- Methods and system for impedance measurement;
- Application in penetration promotion treatment.
2. Skin Impedance Model
2.1. Morphology of Human Skin
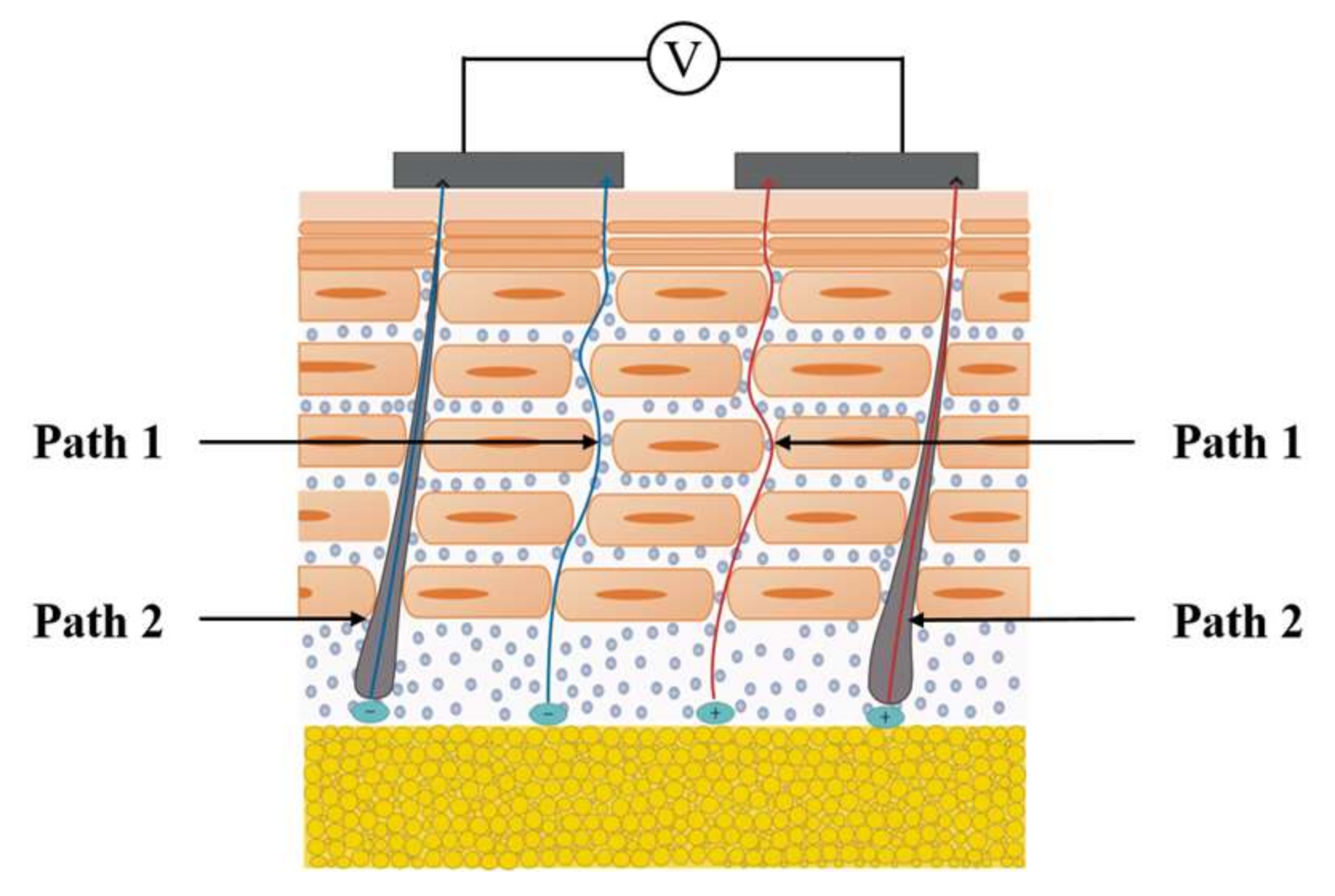
2.2. Physical Principles of Skin Transport
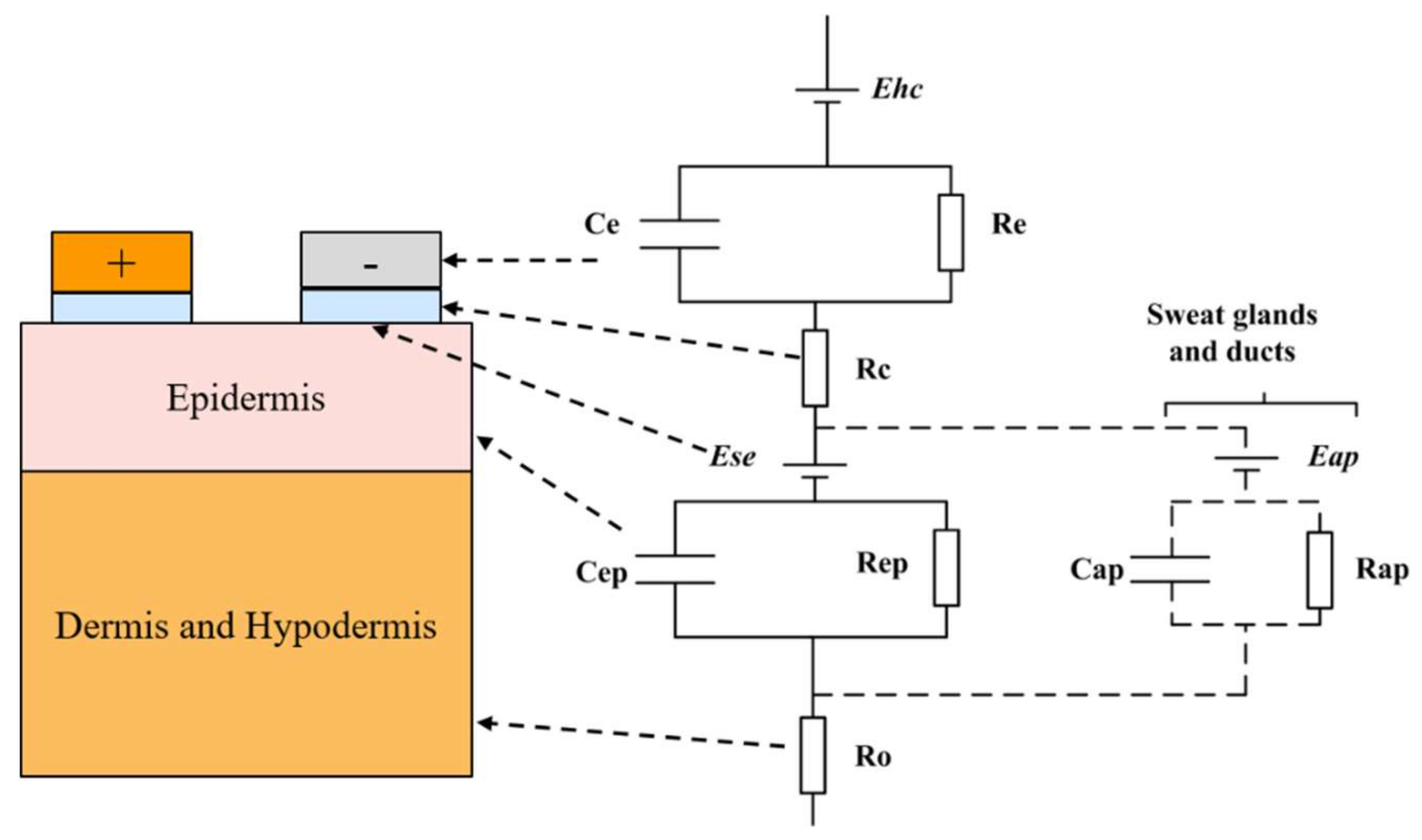
2.3. Skin Impedance Model
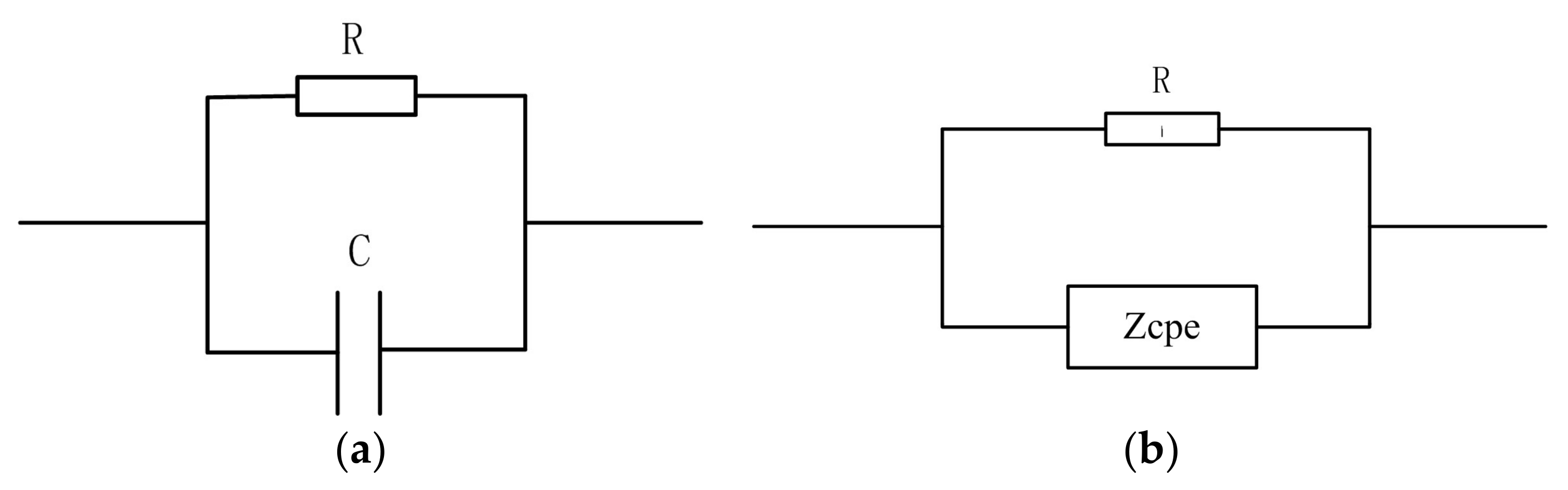
2.3.1. Constant Phase Angle Model
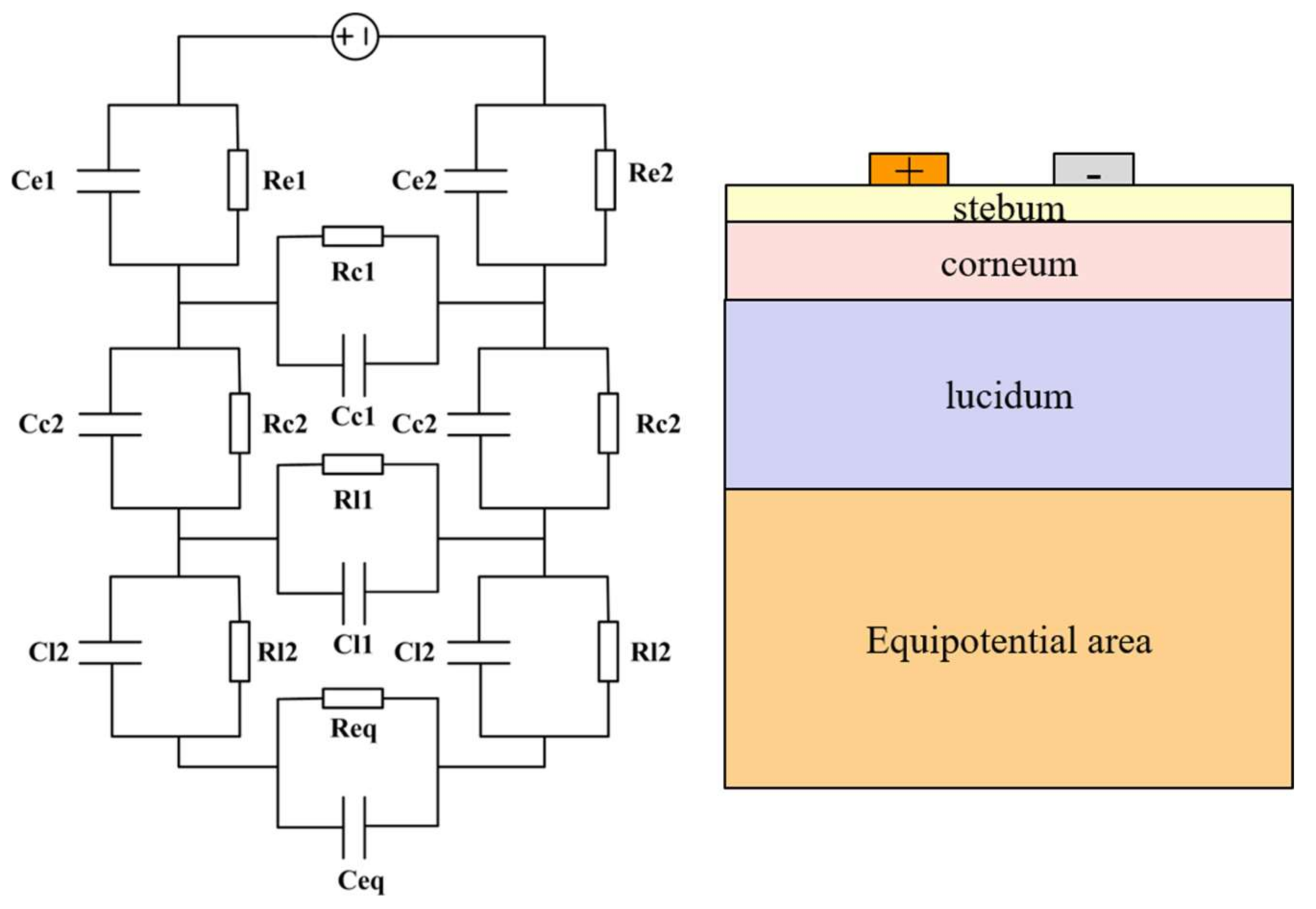
2.3.2. RC Layered Model
3. Electrodes for Skin Impedance Measurement
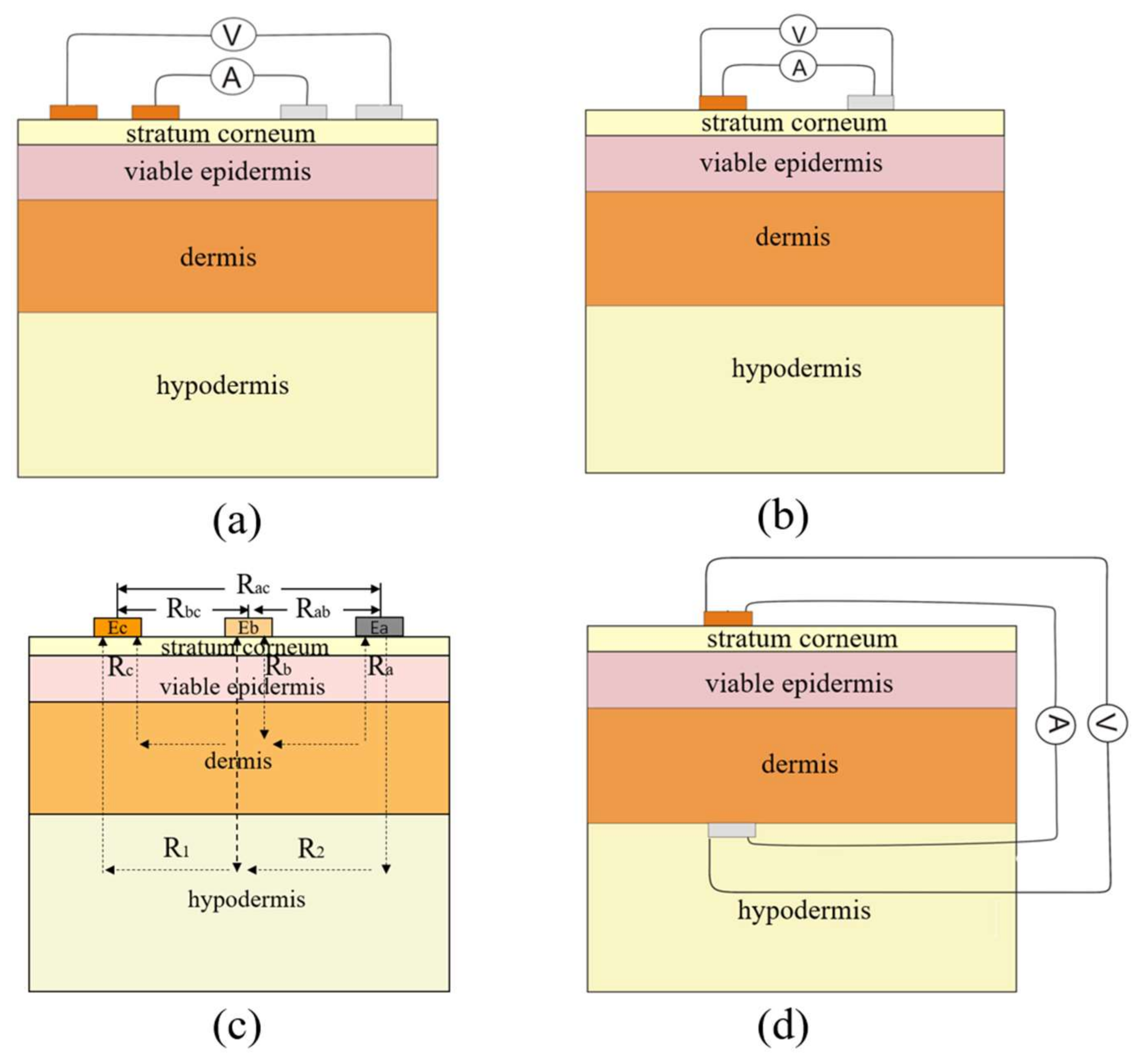
3.1. Types of Electrodes
3.2. Materials of Electrodes
3.2.1. Ag/AgCl
3.2.2. Au
3.2.3. Nanomaterials
3.3. Size and Geometry of Electrodes
4. Methods and System for Impedance Measurement
4.1. Methods for Impedance Measurement
4.2. System for Impedance Measurement
5. Application in Penetration Promotion Treatment
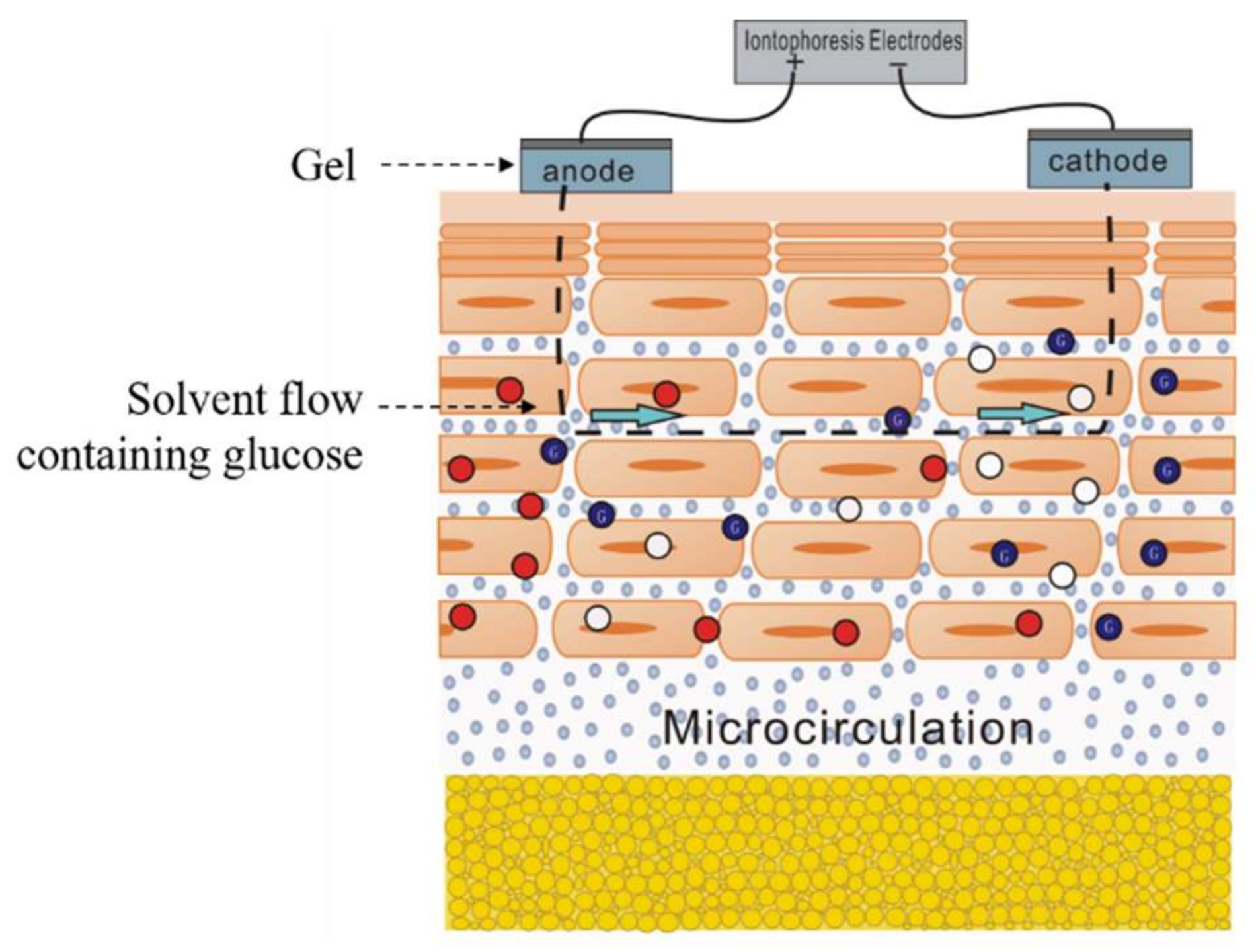
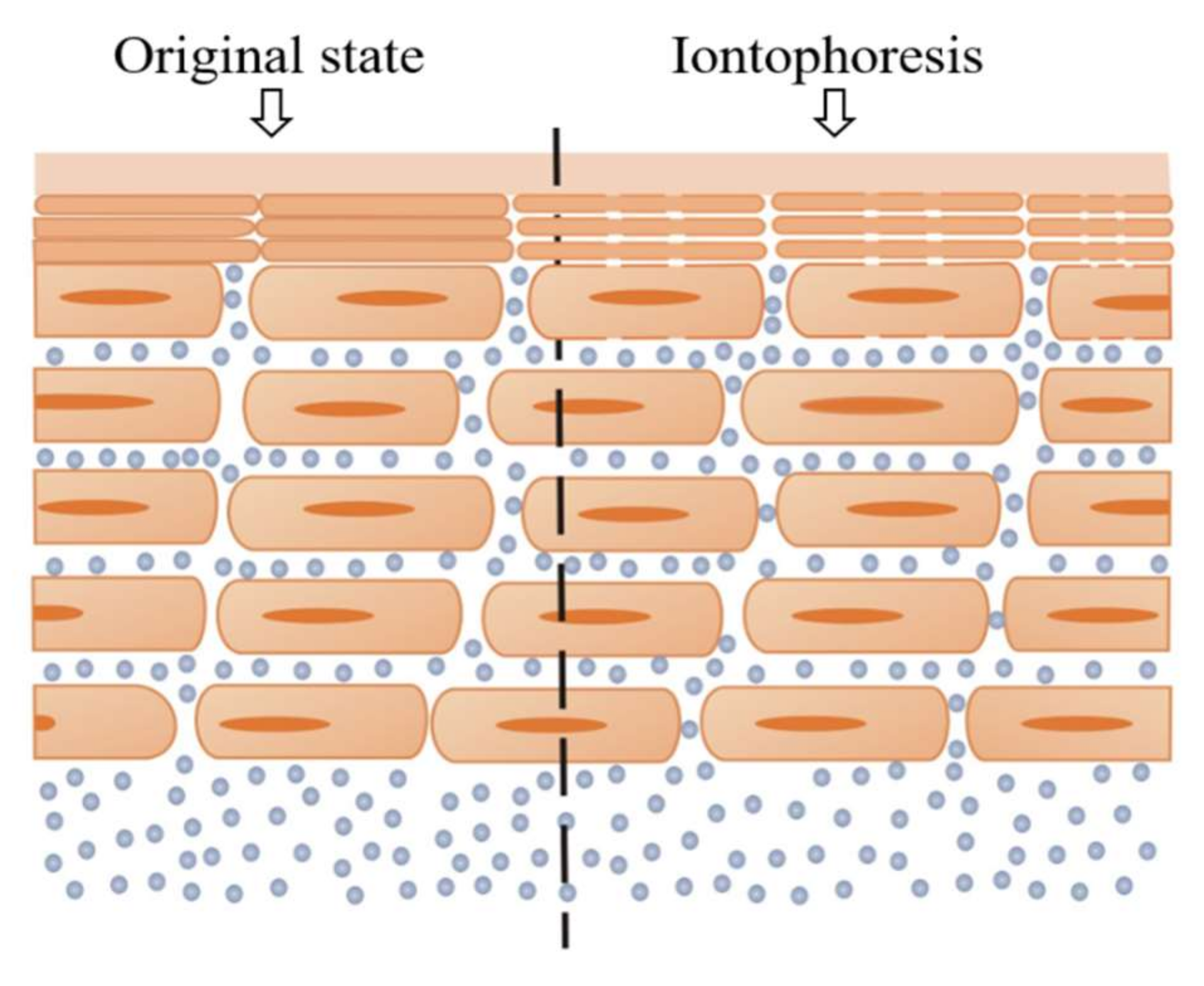
5.1. Iontophoresis
5.2. Electroporation
6. Conclusions and Prospects
- According to the biological structure and frequency response characteristics of the stratum corneum, SC is considered to be the key factor which affects skin transdermal transport ability. Thus, the impedance detection of SC is predicted to be an effective method for assessing skin permeability.
- The future skin impedance model is proposed to be able to express both the layer structure and biological characteristics.
- Micro-electrodes of appropriate size and structure can help to concentrate the working electric field into the target skin layer, which will improve the accuracy of impedance detection.
- Non-symmetric interdigital micro-electrodes are proposed to perform better than symmetric ones because the electric field strengths of non-symmetric electrodes are higher than that of symmetric ones.
- Impedance detection sensors and systems will develop to be more integrated, portable and flexible (skin-like), so as to be more appropriate for long-term and continuous healthcare use.
- Skin impedance could be used as feedback reference for adjusting the stimulation intensity and time for the penetration promoting method to reduce the differences between individual skin permeability.
- The technology of the skin impedance measurement and analysis method could be applied in the fields of cosmetology, dermatological research and so on.
Acknowledgments
Author Contributions
Conflicts of Interest
References
- Gupta, A.; Annu, S.; Batra, P.; Kapoor, R. Bioelectrical Impedance: A Future Health Care Technology. In Proceedings of the IJCA Proceedings on 4th International IT Summit Confluence 2013—The Next Generation Information Technology Summit 2013 (Confluence 2013), Noida, India, 26–27 September 2013; pp. 21–25. [Google Scholar]
- Landaeta, R.G.; Casas, O.; Pallasareny, R. Heart Rate Detection from Plantar Bioimpedance Measurements. IEEE Trans. Biomed. Eng. 2008, 55, 1163–1167. [Google Scholar] [CrossRef] [PubMed]
- Martinsen, O.G.; Clausen, S.; Nysaether, J.B.; Grimnes, S. Utilizing characteristic electrical properties of the epidermal skin layers to detect fake fingers in biometric fingerprint systems—A pilot study. IEEE Trans. Biomed. Eng. 2007, 54, 891–894. [Google Scholar] [CrossRef] [PubMed]
- Weitzen, R.; Epstein, N.; Shoenfeld, Y.; Zimlichman, E. Diagnosing Diseases by Measurement of Electrical Skin Impedance. Ann. N. Y. Acad. Sci. 2007, 1109, 185–192. [Google Scholar] [CrossRef] [PubMed]
- Davies, L.; Chappell, P.; Melvin, T. Modelling the effect of hydration on skin conductivity. Skin Res. Technol. 2016, 23, 363–368. [Google Scholar] [CrossRef] [PubMed][Green Version]
- Kalia, Y.N.; Pirot, F.; Guy, R.H. Homogeneous transport in a heterogeneous membrane: Water diffusion across human stratum corneum in vivo. Biophys. J. 1996, 71, 2692–2700. [Google Scholar] [CrossRef]
- Birgersson, U.; Birgersson, E.; Aberg, P.; Nicander, I.; Ollmar, S. Non-invasive bioimpedance of intact skin: Mathematical modeling and experiments. Physiol. Meas. 2011, 32, 1–18. [Google Scholar] [CrossRef] [PubMed]
- Dujardin, N.; Staes, E.; Kalia, Y.; Clarys, P.; Guy, R.; Préat, V. In vivo assessment of skin electroporation using square wave pulses. J. Control. Release 2002, 79, 219–227. [Google Scholar] [CrossRef]
- Vanbever, R.; Lecouturier, N.; Préat, V. Transdermal delivery of metoprolol by electroporation. Pharm. Res. 1994, 11, 1657–1662. [Google Scholar] [CrossRef] [PubMed]
- Ghosh, S.; Mahadevappa, M.; Mukhopadhyay, J. A 2D electrode-skin model for electrical & contact impedance characterization of Bio Impedance. In Proceedings of the Region 10 Conference (TENCON), Singapore, 22–25 November 2017; pp. 2292–2295. [Google Scholar]
- Clemente, F.; Arpaia, P.; Manna, C. Characterization of human skin impedance after electrical treatment for transdermal drug delivery. Measurement 2013, 46, 3494–3501. [Google Scholar] [CrossRef]
- Mccormick, C.; Heath, D.; Connolly, P. Minimally Invasive Sensing; InTech: Rijeka, Croatia, 2011. [Google Scholar]
- Eastman, R.C.; Chase, H.P.; Buckingham, B.; Hathout, E.H.; Fuller-Byk, L.; Leptien, A.; Van Wyhe, M.M.; Davis, T.L.; Fermi, S.J.; Pechler, H. Use of the GlucoWatch biographer in children and adolescents with diabetes. Pediatr. Diabetes 2002, 3, 127–134. [Google Scholar] [CrossRef] [PubMed]
- Fatouros, D.G.; Am, G.H.G.; van Aelst, A.C.; Koerten, H.K.; Bouwstra, J.A. Visualization studies of human skin in vitro/in vivo under the influence of an electrical field. Eur. J. Pharm. Sci. 2006, 29, 160–170. [Google Scholar] [CrossRef] [PubMed]
- Elias, P.M.; Friend, D.S. The permeability barrier in mammalian epidermis. J. Cell Biol. 1975, 65, 180–191. [Google Scholar] [CrossRef] [PubMed]
- Wilke, K.; Wepf, R.; Keil, F.J.; Wittern, K.P.; Wenck, H.; Biel, S.S. Are sweat glands an alternate penetration pathway? Understanding the morphological complexity of the axillary sweat gland apparatus. Skin Pharmacol. Physiol. 2006, 19, 38–49. [Google Scholar] [CrossRef] [PubMed]
- Schwingenschuh, S.; Scharfetter, H.; Martinsen, O.G.; Boulgaropoulos, B.; Augustin, T.; Tiffner, K.; Dragatin, C.; Raml, R.; Hoefferer, C.; Prandl, E.C. Assessment of skin permeability to topically applied drugs by skin impedance and admittance. Physiol. Meas. 2017, 38, N138–N150. [Google Scholar] [CrossRef] [PubMed]
- Li, D.; Pu, Z.; Liang, W.; Liu, T.; Wang, R.; Yu, H.; Xu, K. Non-invasive measurement of normal skin impedance for determining the volume of the transdermally extracted interstitial fluid. Measurement 2015, 62, 215–221. [Google Scholar] [CrossRef]
- Jayaraman, A.; Kaczmarek, K.A.; Tyler, M.E.; Okpara, U.O. Effect of localized ambient humidity on electrotactile skin resistance. In Proceedings of the IEEE Northeast Bioengineering Conference, Stony Brook, NY, USA, 10–11 March 2007; pp. 110–111. [Google Scholar]
- Kontturi, K.; Murtomäki, L.; Hirvonen, J.; Paronen, P.; Urtti, A. Electrochemical characterization of human skin by impedance spectroscopy: The effect of penetration enhancers. Pharm. Res. 1993, 10, 381–385. [Google Scholar] [CrossRef] [PubMed]
- Ilic, L.; Gowrishankar, T.R.; Vaughan, T.E.; Herndon, T.O.; Weaver, J.C. Spatially constrained skin electroporation with sodium thiosulfate and urea creates transdermal microconduits. J. Control. Release 1999, 61, 185–202. [Google Scholar] [CrossRef]
- White, E.A.; Horne, A.; Runciman, J.; Orazem, M.E.; Navidi, W.C.; Roper, C.S.; Bunge, A.L. On the correlation between single-frequency impedance measurements and human skin permeability to water. Toxicol. In Vitro 2011, 25, 2095–2104. [Google Scholar] [CrossRef] [PubMed]
- Ventrelli, L.; Marsilio Strambini, L.; Barillaro, G. Microneedles for Transdermal Biosensing: Current Picture and Future Direction. Adv. Healthc. Mater. 2015, 4, 2606–2640. [Google Scholar] [CrossRef] [PubMed]
- Jepps, O.G.; Dancik, Y.; Anissimov, Y.G.; Roberts, M.S. Modeling the human skin barrier—Towards a better understanding of dermal absorption. Adv. Drug Deliv. Rev. 2013, 65, 149–151. [Google Scholar] [CrossRef] [PubMed]
- Blair, C. Morphology and thickness of the human stratum corneum. Br. J. Dermatol. 1968, 80, 430–436. [Google Scholar] [CrossRef] [PubMed]
- Yamamoto, T.; Yamamoto, Y. Electrical properties of the epidermal stratum corneum. Med. Biol. Eng. 1976, 14, 151–158. [Google Scholar] [CrossRef] [PubMed]
- Martinsen, Ø.G.; Grimnes, S.; Haug, E. Measuring depth depends on frequency in electrical skin impedance measurements. Skin Res. Technol. 2010, 5, 179–181. [Google Scholar] [CrossRef]
- Wertz, P.W. Lipids and barrier function of the skin. Acta Derm.-Venereol. Suppl. 2000, 208, 7–11. [Google Scholar] [CrossRef]
- Baroni, A.; Buommino, E.; De, G.V.; Ruocco, E.; Ruocco, V.; Wolf, R. Structure and function of the epidermis related to barrier properties. Clin. Dermatol. 2012, 30, 257–262. [Google Scholar] [CrossRef] [PubMed]
- Huclova, S.; Baumann, D.; Talary, M.S.; Fröhlich, J. Sensitivity and specificity analysis of fringing-field dielectric spectroscopy applied to a multi-layer system modelling the human skin. Phys. Med. Biol. 2011, 56, 7777–7793. [Google Scholar] [CrossRef] [PubMed]
- Heard, C.M.; Monk, B.V.; Modley, A.J. Binding of primaquine to epidermal membranes and keratin. Int. J. Pharm. 2003, 257, 237–244. [Google Scholar] [CrossRef]
- Yotsuyanagi, T.; Higuchi, W.I. A two phase series model for the transport of steroids across the fully hydrated stratum corneum. J. Pharm. Pharmacol. 1972, 24, 934–941. [Google Scholar] [CrossRef] [PubMed]
- Siddiqui, O.; Roberts, M.S.; Polack, A.E. Percutaneous absorption of steroids: Relative contributions of epidermal penetration and dermal clearance. J. Pharmacokinet. Pharmacodyn. 1989, 17, 405–424. [Google Scholar] [CrossRef]
- Scheuplein, R.J.; Blank, I.H. Permeability of the skin. Physiol. Rev. 1971, 51, 702–747. [Google Scholar] [CrossRef] [PubMed]
- Mcadams, E.T.; Jossinet, J. Tissue impedance: A historical overview. Physiol. Meas. 1995, 16, A1–A13. [Google Scholar] [CrossRef] [PubMed]
- Hirschorn, B.; Orazem, M.E.; Tribollet, B.; Vivier, V.; Frateur, I.; Musiani, M. Determination of effective capacitance and film thickness from constant-phase-element parameters. Electrochim. Acta 2010, 55, 6218–6227. [Google Scholar] [CrossRef]
- GómezAguilar, F.; BernalAlvarado, J.; RosalesGarcía, J.; GuíaCalderón, M.; CórdovaFraga, T.; SosaAquino, M. Frequency response of an electric equivalent circuit for a skin type system. Rev. Mex. Ing. Biomed. 2011, 32, 93–99. [Google Scholar]
- Rigaud, B.; Morucci, J.P.; Chauveau, N. Bioelectrical impedance techniques in medicine. Part I: Bioimpedance measurement. Second section: Impedance spectrometry. Crit. Rev. Biomed. Eng. 1996, 24, 257–351. [Google Scholar] [PubMed]
- Valentinuzzi, M.E. Bioelectrical impedance techniques in medicine. Part I: Bioimpedance measurement. First section: General concepts. Crit. Rev. Biomed. Eng. 1996, 24, 223–255. [Google Scholar] [PubMed]
- Ivanic, R.; Novotny, I.; Rehacek, V.; Tvarozek, V.; Weis, M. Thin film non-symmetric microelectrode array for impedance monitoring of human skin. Thin Solid Films 2003, 433, 332–336. [Google Scholar] [CrossRef]
- Dudzinski, K.; Dawgul, M.; Pluta, K.; Wawro, B.; Torbicz, W.; Pijanowska, D.G. Spiral concentric two electrode sensor fabricated by direct writing for skin impedance measurements. IEEE Sens. J. 2017, 17, 5306–5314. [Google Scholar] [CrossRef]
- Yao, S.; Zhu, Y. Nanomaterial-Enabled Dry Electrodes for Electrophysiological Sensing: A Review. JOM 2016, 68, 1–11. [Google Scholar] [CrossRef]
- Lopez-Gordo, M.A.; Sanchez-Morillo, D.; Valle, F.P. Dry EEG Electrodes. Sensors 2014, 14, 12847–12870. [Google Scholar] [CrossRef] [PubMed]
- Kalia, Y.N.; Guy, R.H. The electrical characteristics of human skin in vivo. Pharm. Res. 1995, 12, 1605–1613. [Google Scholar] [CrossRef] [PubMed]
- Yokus, M.A.; Jur, J.S. Fabric-Based Wearable Dry Electrodes for Body Surface Biopotential Recording. IEEE Trans. Biomed. Eng. 2015, 63, 423–430. [Google Scholar] [CrossRef] [PubMed]
- Ying, M.; Li, Z.; Chen, J. A flexible dry electrode based on APTES-anchored PDMS substrate for portable ECG acquisition system. Microsyst. Technol. 2016, 22, 1–8. [Google Scholar]
- Cui, J.; Zhang, B.; Duan, J.; Guo, H.; Tang, J. Flexible Pressure Sensor with Ag Wrinkled Electrodes Based on PDMS Substrate. Sensors 2016, 16, 2131. [Google Scholar] [CrossRef] [PubMed]
- Windmiller, J.R.; Wang, J. Wearable Electrochemical Sensors and Biosensors: A Review. Electroanalysis 2013, 25, 29–46. [Google Scholar] [CrossRef]
- Bandodkar, A.J.; Jia, W.; Wang, X.; Ramirez, J.; Wang, J. Tattoo-Based Noninvasive Glucose Monitoring: A Proof-of-Concept Study. Anal. Chem. 2015, 87, 394–398. [Google Scholar] [CrossRef] [PubMed]
- Chen, Y.; Lu, S.; Zhang, S.; Li, Y.; Qu, Z.; Chen, Y.; Lu, B.; Wang, X.; Feng, X. Skin-like biosensor system via electrochemical channels for noninvasive blood glucose monitoring. Sci. Adv. 2017, 3, e1701629. [Google Scholar] [CrossRef] [PubMed]
- Clemente, F.; Romano, M.; Bifulco, P.; Cesarelli, M. EIS measurements for characterization of muscular tissue by means of equivalent electrical parameters. Measurement 2014, 58, 476–482. [Google Scholar] [CrossRef]
- Dudzinski, K.; Dawgul, M.; Wawro, B.; Pijanowska, D.; Torbicz, W. Skin Impedance Measurements by Means of Novel Gold Sensors Fabricated by Direct Writing. Procedia Eng. 2015, 120, 882–886. [Google Scholar] [CrossRef]
- Suni, I.I. Impedance methods for electrochemical sensors using nanomaterials. TrAC Trends Anal. Chem. 2008, 27, 604–611. [Google Scholar] [CrossRef]
- Bhalla, N.; Sathish, S.; Sinha, A.; Shen, A.Q. Large-Scale Nanophotonic Structures for Long-Term Monitoring of Cell Proliferation. Adv. Biosyst. 2018. [Google Scholar] [CrossRef]
- Qi, Y.S.; Tham, S.Y.; Loh, H.S.; Khiew, P.S.; Chiu, W.S.; Tan, M.T.T. One-step green hydrothermal synthesis of biocompatible graphene/TiO2 nanocomposites for enzymeless H2O2 detection and its cytotoxicity effects on human keratinocytes and lung fibroblasts cells. J. Mater. Chem. B 2018. [Google Scholar] [CrossRef]
- Lee, S.M.; Hang, J.B.; Lee, J.H.; Dong, H.B.; Lee, K.H.; Hong, J.S.; Lee, S.H. Self-adhesive epidermal carbon nanotube electronics for tether-free long-term continuous recording of biosignals. Sci. Rep. 2014, 4, 6074. [Google Scholar] [CrossRef] [PubMed]
- Miljković, S.; Tomić, M.; Hut, I.; Pelemis, S. Nanomaterials for Skin Care; Springer: Berlin, Germany, 2018. [Google Scholar]
- Kim, C.; Li, G.; Li, J.; Jong, H.; Ro, C.; Song, Y.; Pak, G.; Im, S. Numerical analysis on effective electric field penetration depth for interdigital impedance sensor. J. Phys. Conf. Ser. 2013, 418, 2020. [Google Scholar] [CrossRef]
- Mamishev, A.V.; Sundara-Rajan, K.; Yang, F.; Du, Y. Interdigital sensors and transducers. Proc. IEEE 2004, 92, 808–845. [Google Scholar] [CrossRef]
- Varshney, M.; Li, Y. Interdigitated array microelectrodes based impedance biosensors for detection of bacterial cells. Biosens. Bioelectron. 2009, 24, 2951–2960. [Google Scholar] [CrossRef] [PubMed]
- Appelboom, G.; Camacho, E.; Abraham, M.E.; Bruce, S.S.; Dumont, E.L.; Zacharia, B.E.; D’Amico, R.; Slomian, J.; Reginster, J.Y.; Bruyère, O. Smart wearable body sensors for patient self-assessment and monitoring. Arch. Public Health 2014, 72, 28. [Google Scholar] [CrossRef] [PubMed]
- Yue, S. The Study on Transdermal Extraction and Prediction of Blood Glucose of Tissue Fluid. Master’s Degree, Tianjin University, Tianjin, China, 2009. [Google Scholar]
- Arpaia, P.; Clemente, F.; Romanucci, C. An instrument for prosthesis osseointegration assessment by electrochemical impedance spectrum measurement. Measurement 2008, 41, 1040–1044. [Google Scholar] [CrossRef]
- Walke, W.; Przondziono, J. Impedance Spectroscopy Study of the Electrochemical Corrosion of Steel Wire Used in Cardiologic Leaders. In Proceedings of the International Conference on Information Technologies in Biomedicine, Goglin, Poland, 11–13 June 2012; pp. 389–397. [Google Scholar]
- Buyin, L.; Zhaoxiang, H.; Hui, X.; Zhijun, L. Designing and implementation of measurement system of impedance spectroscopy analyzer based on AD5933. Microcomput. Inf. 2008, 24, 288–290. [Google Scholar]
- Kaltenbrunner, M.; Sekitani, T.; Reeder, J.; Yokota, T.; Kuribara, K.; Tokuhara, T.; Drack, M.; Schwödiauer, R.; Graz, I.; Bauergogonea, S. An ultra-lightweight design for imperceptible plastic electronics. Nature 2013, 499, 458–463. [Google Scholar] [CrossRef] [PubMed]
- Vosgueritchian, M.; Tok, J.B.H.; Bao, Z. Stretchable LEDs: Light-emitting electronic skin. Nat. Photonics 2013, 7, 769–771. [Google Scholar] [CrossRef]
- Ilievski, F.; Mazzeo, A.D.; Shepherd, R.F.; Chen, X.; Whitesides, G.M. Soft robotics for chemists. Angew. Chem. 2011, 50, 1890–1895. [Google Scholar] [CrossRef] [PubMed]
- Bandodkar, A.J.; Imani, S.; Nunez-Flores, R.; Kumar, R.; Wang, C.; Amv, M.; Wang, J.; Mercier, P.P. Re-usable electrochemical glucose sensors integrated into a smartphone platform. Biosens. Bioelectron. 2017, 101, 181–187. [Google Scholar] [CrossRef] [PubMed]
- Weaver, J.C.; Powell, K.T.; Langer, R.S. Control of Transport of Molecules across Tissue Using Electroporation. U.S. Patent US5019034A, 28 May 1991. [Google Scholar]
- Prausnitz, M.R.; Bose, V.G.; Langer, R.; Weaver, J.C. Electroporation of mammalian skin: A mechanism to enhance transdermal drug delivery. Proc. Natl. Acad. Sci. USA 1993, 90, 10504–10508. [Google Scholar] [CrossRef] [PubMed]
- Alvarez-Román, R.; Naik, A.; Kalia, Y.N.; Fessi, H.; Guy, R.H. Visualization of skin penetration using confocal laser scanning microscopy. Eur. J. Pharm. Biopharm. 2004, 58, 301–316. [Google Scholar] [CrossRef] [PubMed]
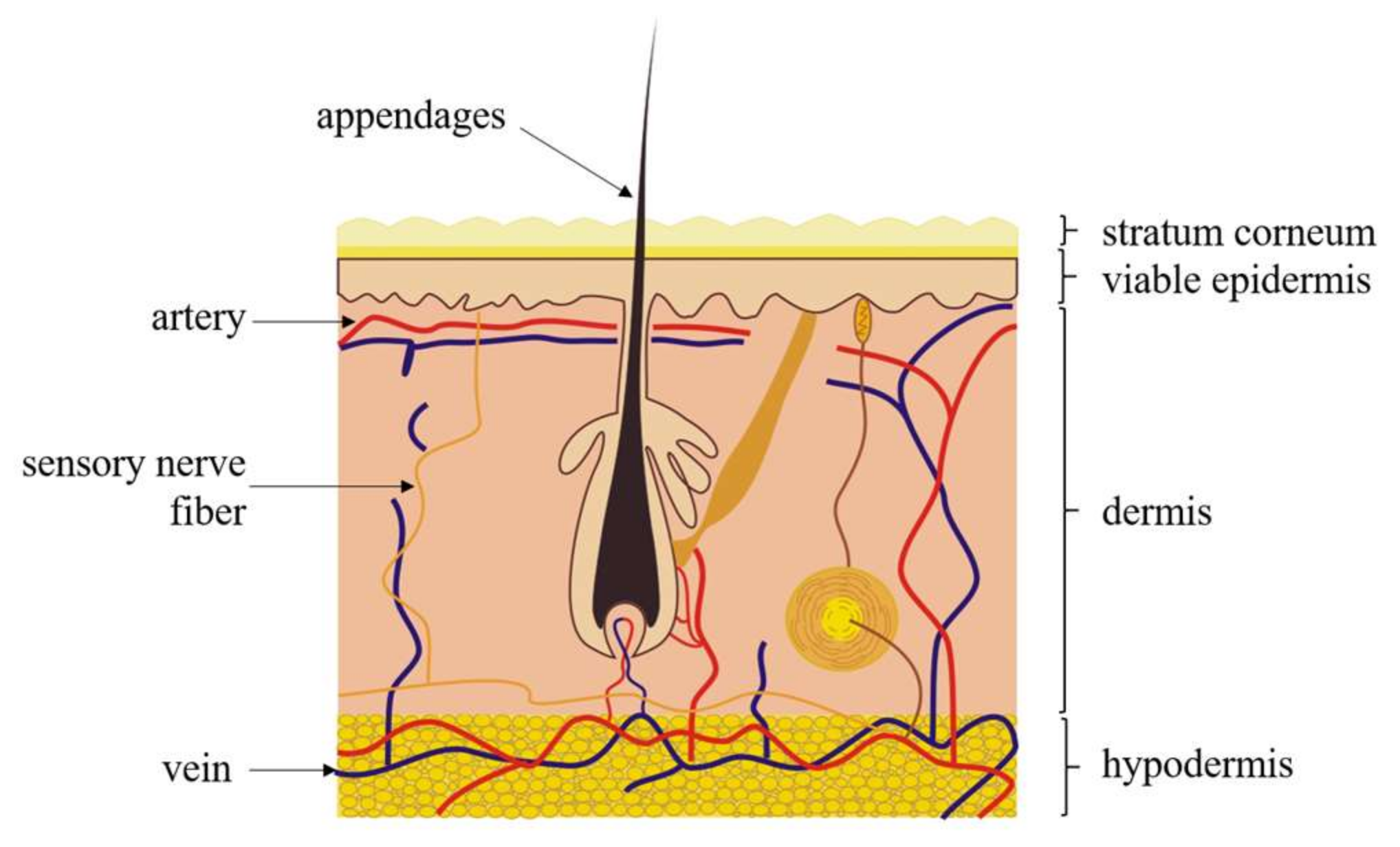
| Stratum Corneum | Viable Epidermis | Dermis | |
|---|---|---|---|
| Composition | Corneocytes embedded in lipid matrix, tightly stacked and overlapping each other | Stratum lucidum, stratum granulosum, stratum spinosum, and stratum basale. | Papillary layer, reticular layer, blood vessel, lymph and nerve system |
| Hydrophilicity | no | yes | yes |
| Impedance | > Ω | > Ω | > Ω |
| Thickness | Tens of microns | 150 μm | 500 μm~2 mm |
| Constant Phase Angle Model | R-C Layered Model | |
|---|---|---|
| Characteristics | Based on the Cole model and RC parallel model, Zcpe is used to characterize its biological property | Based on the layered structure of skin, model is constructed in each layer |
| Parameters | 3 | >20 |
| Accuracy | Not accurate due to the rough model | Ignoring the biological nature of the skin |
| Computation | Small amount | Very large amount |
| Electrodes | Type | Attachment | Size | Advantages | Disadvantages | |
|---|---|---|---|---|---|---|
| Materials | Geometry | |||||
| Ag/AgCl | Bare block electrode | Dry | poor | 2.25 cm2~10 cm2 | Non-disposable, simple and mature fabrication process | Poor attachment |
| Pre-gelled electrode | Wet | good | 0.79 cm2/6 cm2 | Attaches well to skin | Disposable, easily changed by sweat, not suitable for long time use | |
| Electrolyte electrode | Wet | good | UM 1 | Constant humidity and attaches well to skin | Disposable, skin overhydration would greatly change skin impedance | |
| Au | Spiral electrode | Dry | poor | UM | Non-disposable, improves the effective measurement area and is micro-size | Poor attachment |
| Concentric ring electrode | Dry | poor | UM | Non-disposable, simple fabrication process, uniform electric field and distance could be shifted easily | Poor attachment | |
| Interdigital electrode | Dry | poor | a = b = d = 100 µm | Non-disposable, mature theoretical analysis model, widely used | Non-uniform electric field distribution | |
| Nanomaterials (AgNW, Au, CNTs) | Based on the substrate material Polydimethylsiloxane (PDMS), polymide, and textile) | Dry | poor | UM | Non-disposable, biocompatible, stretchable, performs well in the moving state, good mechanical strength, and large contact area | Complicated fabrication process and high cost, only used in laboratory. |
© 2018 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Lu, F.; Wang, C.; Zhao, R.; Du, L.; Fang, Z.; Guo, X.; Zhao, Z. Review of Stratum Corneum Impedance Measurement in Non-Invasive Penetration Application. Biosensors 2018, 8, 31. https://doi.org/10.3390/bios8020031
Lu F, Wang C, Zhao R, Du L, Fang Z, Guo X, Zhao Z. Review of Stratum Corneum Impedance Measurement in Non-Invasive Penetration Application. Biosensors. 2018; 8(2):31. https://doi.org/10.3390/bios8020031
Chicago/Turabian StyleLu, Fei, Chenshuo Wang, Rongjian Zhao, Lidong Du, Zhen Fang, Xiuhua Guo, and Zhan Zhao. 2018. "Review of Stratum Corneum Impedance Measurement in Non-Invasive Penetration Application" Biosensors 8, no. 2: 31. https://doi.org/10.3390/bios8020031
APA StyleLu, F., Wang, C., Zhao, R., Du, L., Fang, Z., Guo, X., & Zhao, Z. (2018). Review of Stratum Corneum Impedance Measurement in Non-Invasive Penetration Application. Biosensors, 8(2), 31. https://doi.org/10.3390/bios8020031





