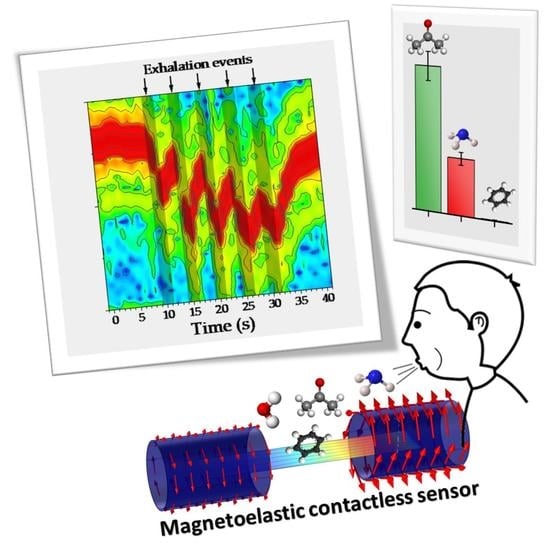
Real-Time Monitoring of Breath Biomarkers with A Magnetoelastic Contactless Gas Sensor: A Proof of Concept
Abstract
1. Introduction
2. Materials and Methods
2.1. Magnetoelastic Sensor Device
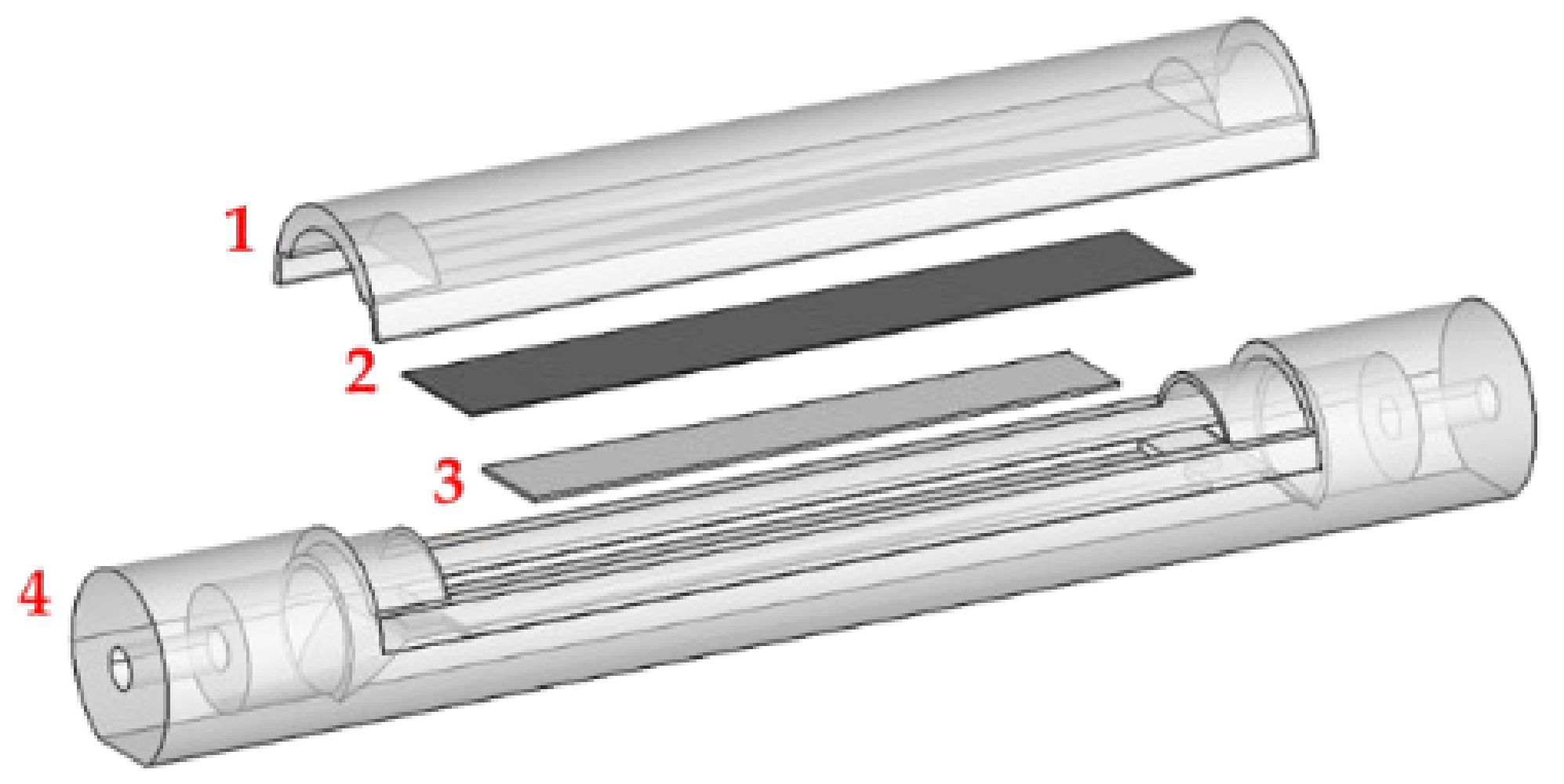
2.2. Sensor Cell
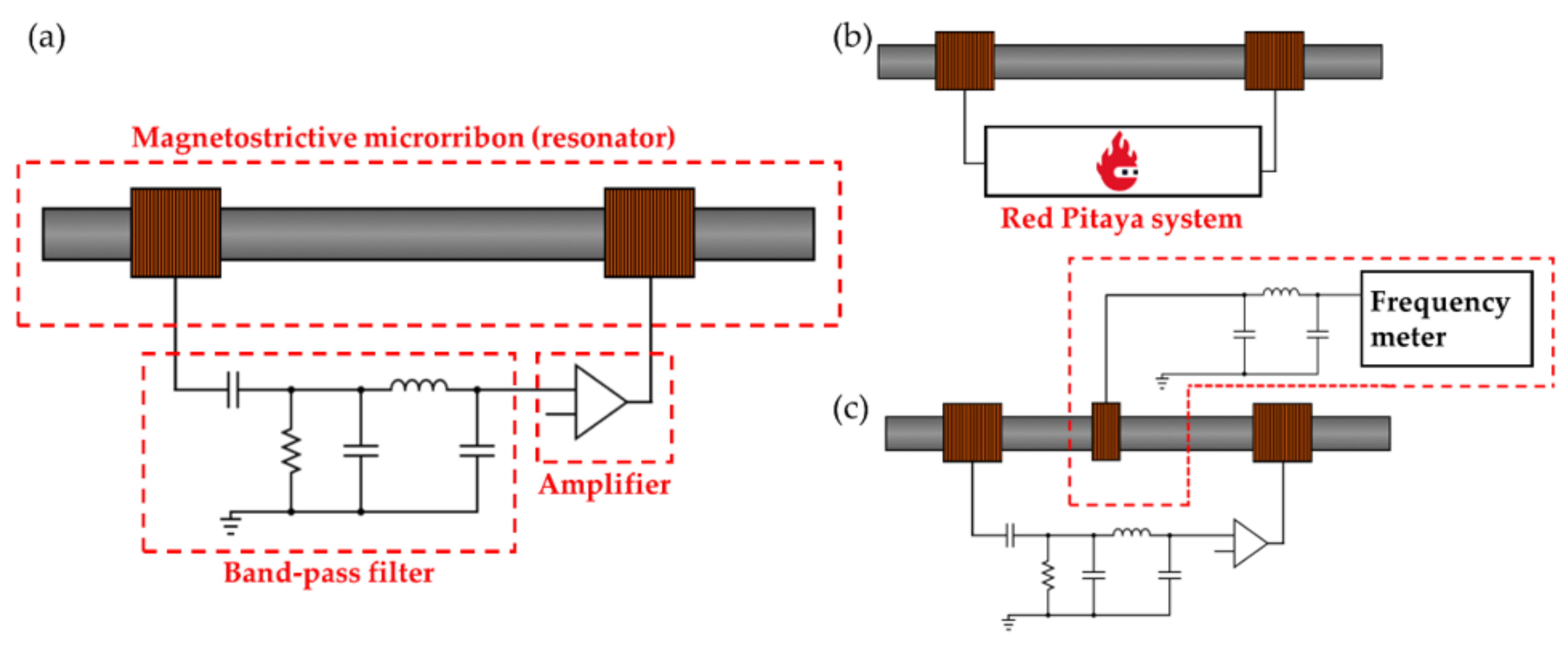
2.3. Magnetoelastic Resonance Oscillator Circuit
- An amplifier;
- A feedback network (magnetostrictive resonator);
- A passive bandpass filter.
2.4. Electrical Characterization and Data Acquisition
2.4.1. Magnetoelastic Resonance Analysis
2.4.2. Q Factor Determination
2.5. Sensors Evaluation
2.6. In-Situ Breath Detection
3. Results and Discussion
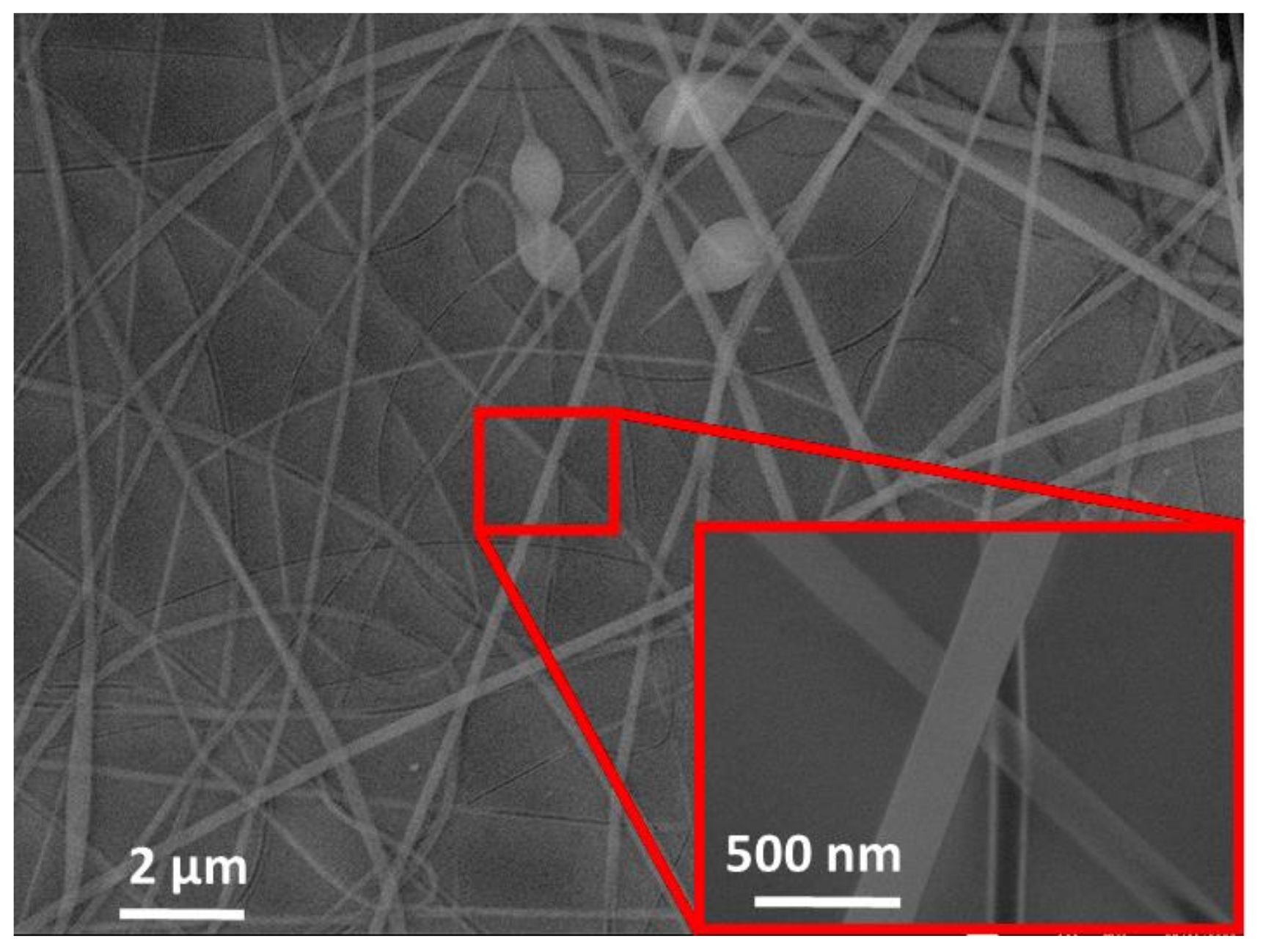
3.1. Sensitive Layer Deposit
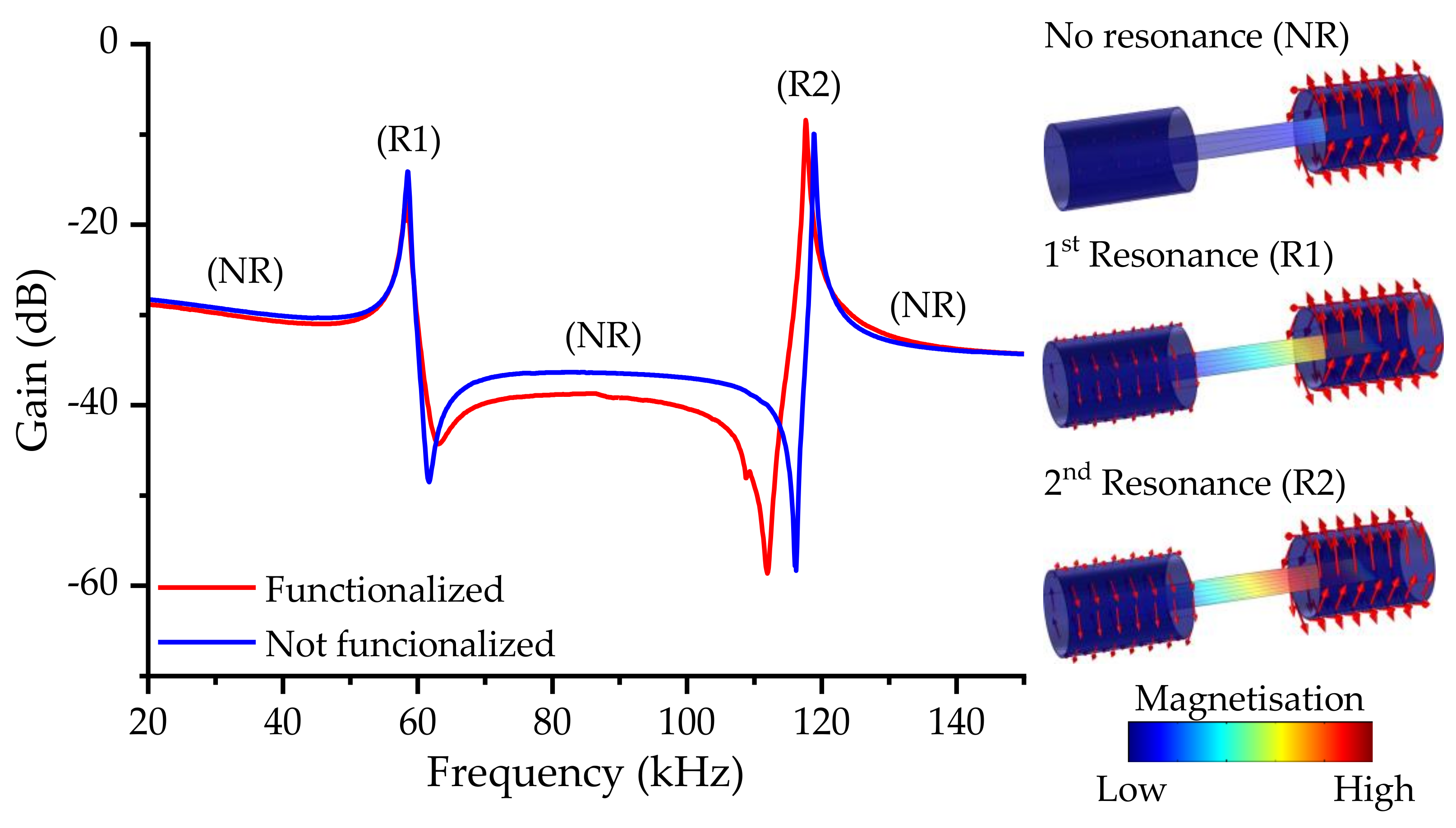
3.2. Magnetoelastic Resonance Characterization
3.3. Gas Response Characterization
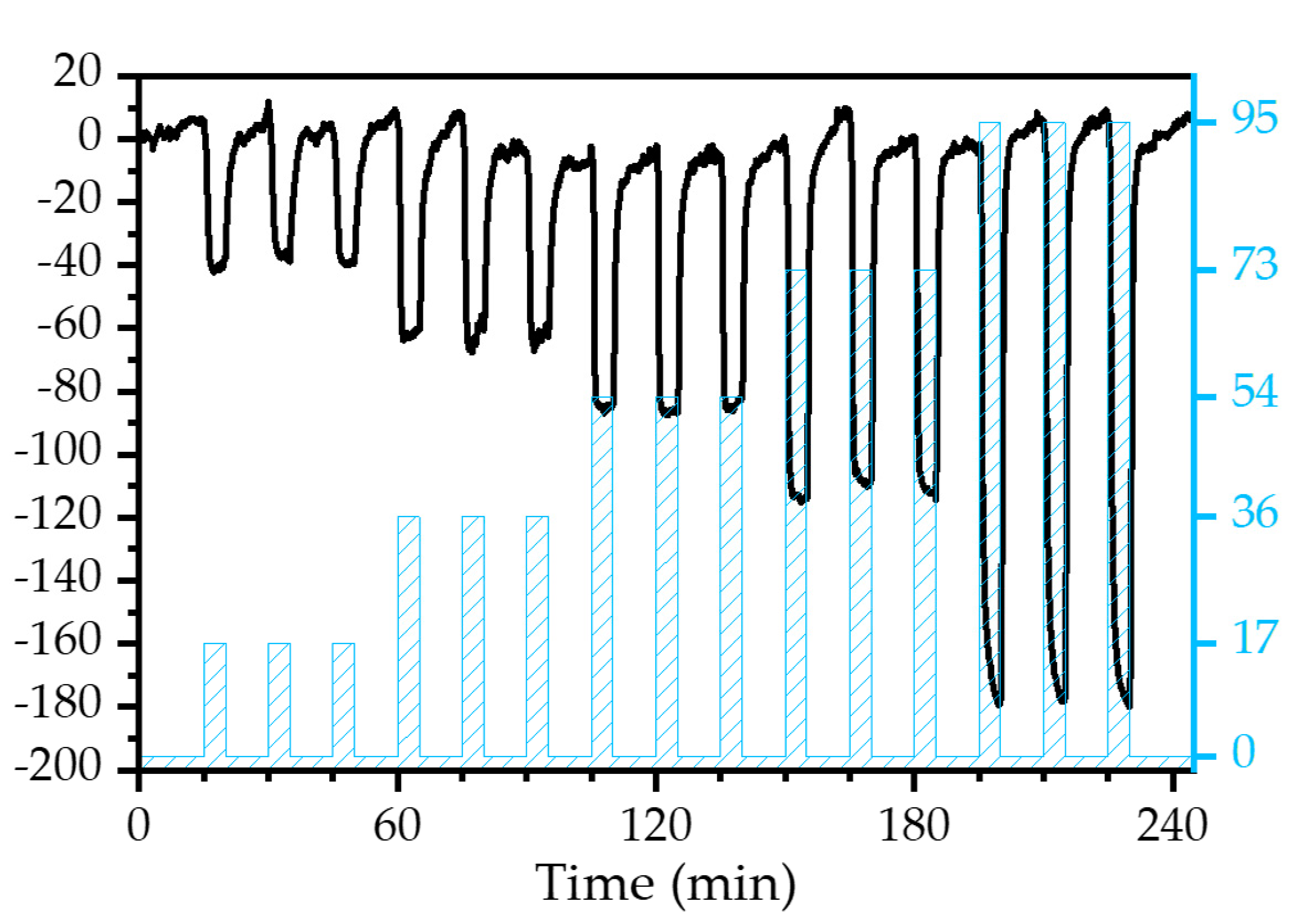
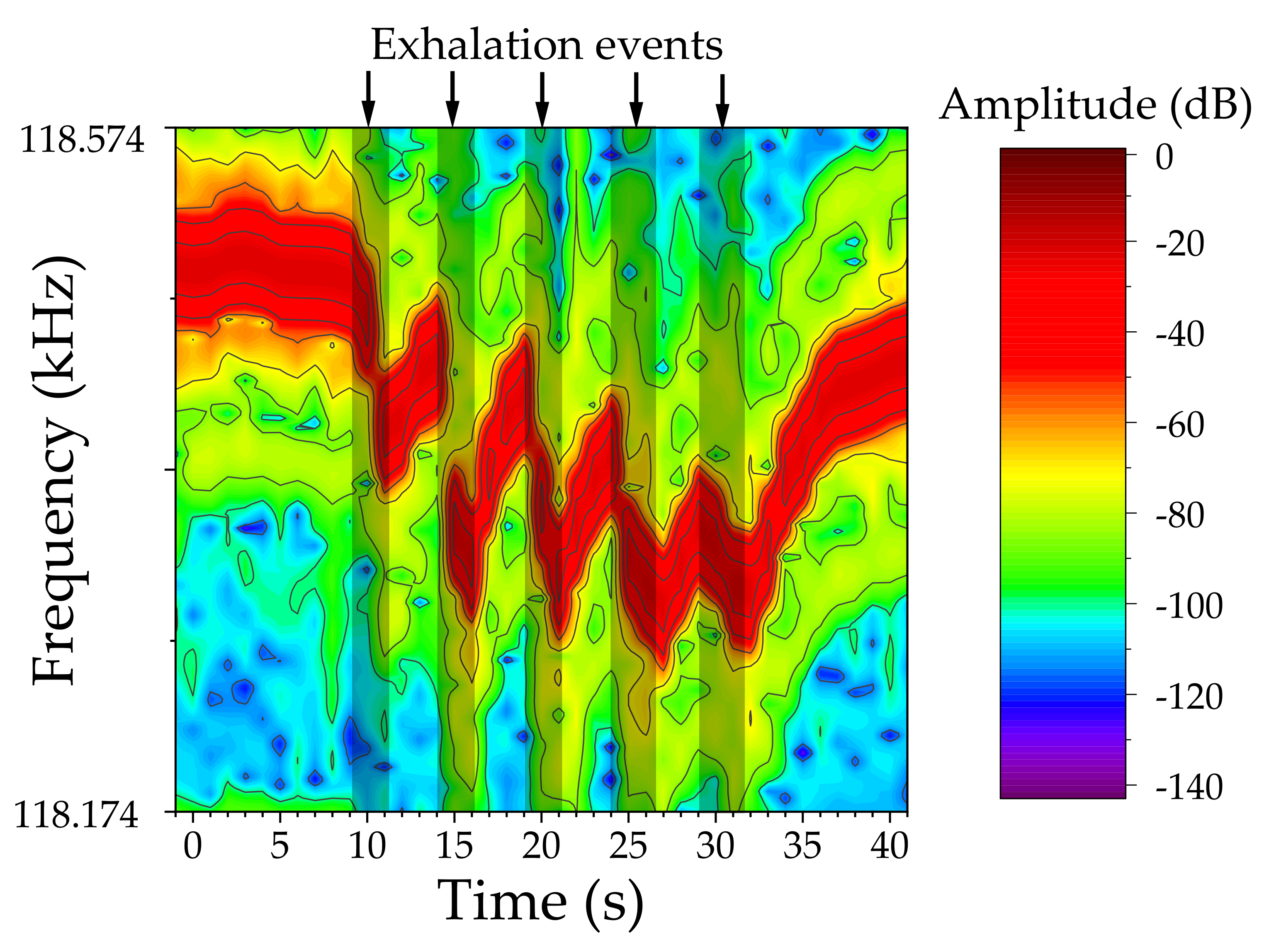
3.3.1. Humidity and Real Breath Monitoring
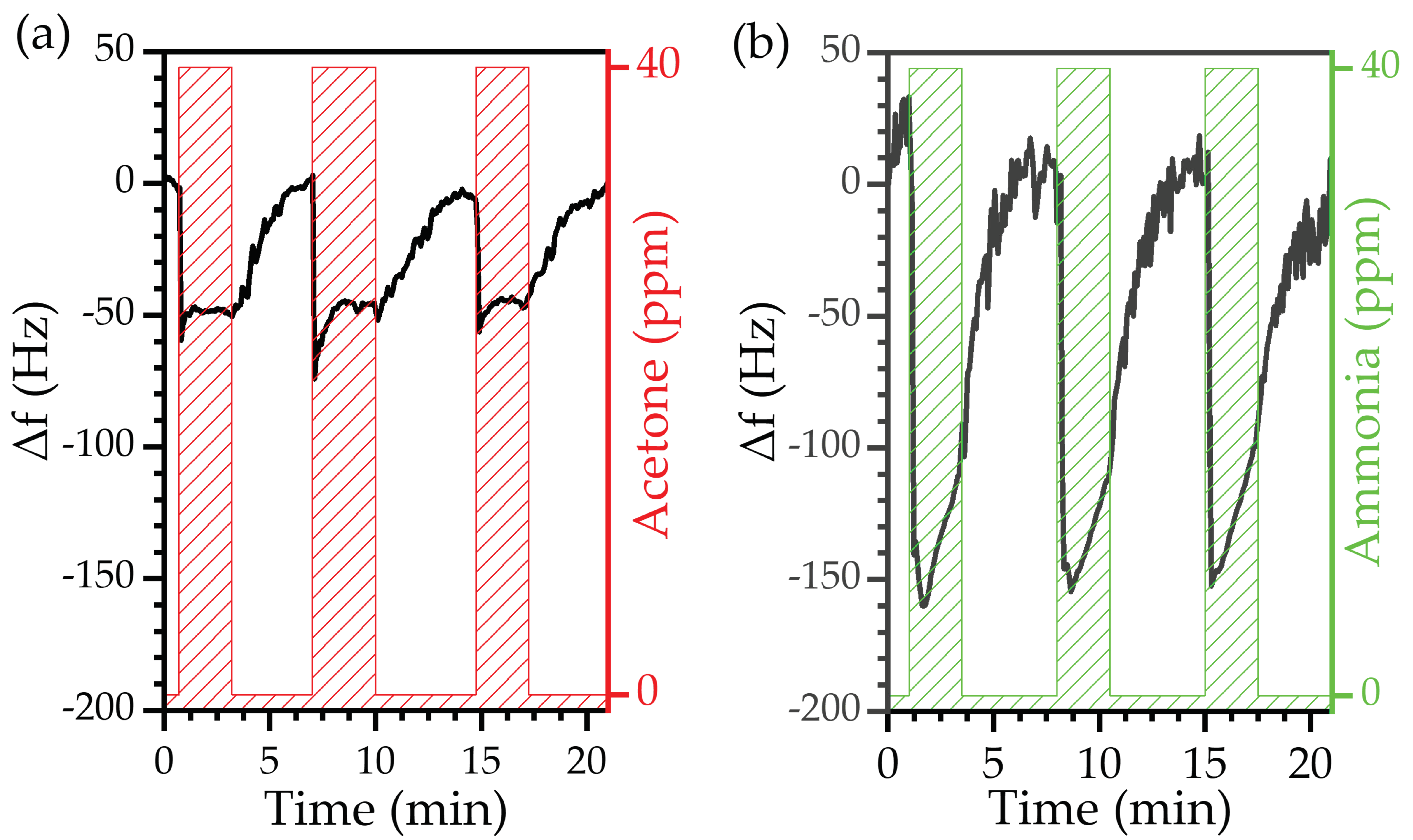
3.3.2. Endogenous Biomarkers: Acetone and Ammonia
3.3.3. Exogeneous Biomarkers: Benzene
4. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- World Health Organization (WHO). Air Quality Guidelines for Europe, 2nd ed.; Theatkston, F., Ed.; WHO Regional Publications: Copenhagen, Denmark, 2000. [Google Scholar]
- Halios, C.H.; Landeg-Cox, C.; Lowther, S.D.; Middleton, A.; Marczylo, T.; Dimitroulopoulou, S. Chemicals in European Residences–Part I: A Review of Emissions, Concentrations and Health Effects of Volatile Organic Compounds (VOCs). Sci. Total Environ. 2022, 839, 156201. [Google Scholar] [CrossRef]
- Wieslander, G.; Norbäck, D.; Björnssonbjörnsson, E.; Janson, C.; Boman, G. Asthma and the Indoor Environment: The Significance of Emission of Formaldehyde and Volatile Organic Compounds from Newly Painted Indoor Surfaces. Swed. Int. Arch Occup. Environ. Health 1997, 69, 115–124. [Google Scholar] [CrossRef]
- Paterson, C.A.; Sharpe, R.A.; Taylor, T.; Morrissey, K. Indoor PM2.5, VOCs and Asthma Outcomes: A Systematic Review in Adults and Their Home Environments. Environ. Res. 2021, 202, 111631. [Google Scholar] [CrossRef]
- Matatagui, D.; López-Sánchez, J.; Peña, A.; Serrano, A.; del Campo, A.; de la Fuente, O.R.; Carmona, N.; Navarro, E.; Marín, P.; del Carmen Horrillo, M. Ultrasensitive NO2 Gas Sensor with Insignificant NH3-Interference Based on a Few-Layered Mesoporous Graphene. Sens. Actuators B Chem. 2021, 335, 129657. [Google Scholar] [CrossRef]
- Khan, M.A.H.; Rao, M.V.; Li, Q. Recent Advances in Electrochemical Sensors for Detecting Toxic Gases: NO2, SO2 and H2S. Sensors 2019, 19, 905. [Google Scholar] [CrossRef]
- Pandey, S.; Nanda, K.K. Au Nanocomposite Based Chemiresistive Ammonia Sensor for Health Monitoring. ACS Sens. 2016, 1, 55–62. [Google Scholar] [CrossRef]
- Liu, W.; Xu, L.; Sheng, K.; Zhou, X.; Dong, B.; Lu, G.; Song, H. A Highly Sensitive and Moisture-Resistant Gas Sensor for Diabetes Diagnosis with Pt@In2O3 Nanowires and a Molecular Sieve for Protection. NPG Asia Mater. 2018, 10, 293–308. [Google Scholar] [CrossRef]
- Nasiri, N.; Clarke, C. Nanostructured Gas Sensors for Medical and Health Applications: Low to High Dimensional Materials. Biosensors 2019, 9, 43. [Google Scholar] [CrossRef]
- Tai, H.; Wang, S.; Duan, Z.; Jiang, Y. Evolution of Breath Analysis Based on Humidity and Gas Sensors: Potential and Challenges. Sens. Actuators B Chem. 2020, 318, 128104. [Google Scholar] [CrossRef]
- Länge, K. Bulk and Surface Acoustic Wave Sensor Arrays for Multi-Analyte Detection: A Review. Sensors 2019, 19, 5382. [Google Scholar] [CrossRef]
- Matatagui, D.; Martí, J.; Fernández, M.J.; Fontecha, J.L.; Gutiérrez, J.; Grcia, I.; Cané, C.; Horrillo, M.C. Chemical Warfare Agents Simulants Detection with an Optimized SAW Sensor Array. Sens. Actuators B Chem. 2011, 154, 199–205. [Google Scholar] [CrossRef]
- Fragoso-Mora, J.R.; Matatagui, D.; Bahos, F.A.; Fontecha, J.; Fernandez, M.J.; Santos, J.P.; Sayago, I.; Gràcia, I.; Horrillo, M.C. Gas Sensors Based on Elasticity Changes of Nanoparticle Layers. Sens. Actuators B Chem. 2018, 268, 93–99. [Google Scholar] [CrossRef]
- di Natale, C.; Macagnano, A.; Martinelli, E.; Paolesse, R.; D’Arcangelo, G.; Roscioni, C.; Finazzi-Agrò, A.; D’Amico, A. Lung Cancer Identification by the Analysis of Breath by Means of an Array of Non-Selective Gas Sensors. Biosens. Bioelectron. 2003, 18, 1209–1218. [Google Scholar] [CrossRef]
- Güntner, A.T.; Abegg, S.; Königstein, K.; Gerber, P.A.; Schmidt-Trucksäss, A.; Pratsinis, S.E. Breath Sensors for Health Monitoring. ACS Sens. 2019, 4, 268–280. [Google Scholar] [CrossRef] [PubMed]
- Kaloumenou, M.; Skotadis, E.; Lagopati, N.; Efstathopoulos, E.; Tsoukalas, D. Breath Analysis: A Promising Tool for Disease Diagnosis—The Role of Sensors. Sensors 2022, 22, 1238. [Google Scholar] [CrossRef] [PubMed]
- Nakhleh, M.K.; Amal, H.; Jeries, R.; Broza, Y.Y.; Aboud, M.; Gharra, A.; Ivgi, H.; Khatib, S.; Badarneh, S.; Har-Shai, L.; et al. Diagnosis and Classification of 17 Diseases from 1404 Subjects via Pattern Analysis of Exhaled Molecules. ACS Nano 2017, 11, 112–125. [Google Scholar] [CrossRef] [PubMed]
- Wallace, L.; Buckley, T.; Pellizzari, E.; Gordon3, S. Breath Measurements as Volatile Organic Compound Biomarkers. Environ. Health Perspect. 1996, 104, 861–869. [Google Scholar]
- Blanchet, L.; Smolinska, A.; Baranska, A.; Tigchelaar, E.; Swertz, M.; Zhernakova, A.; Dallinga, J.W.; Wijmenga, C.; van Schooten, F.J. Factors That Influence the Volatile Organic Compound Content in Human Breath. J. Breath. Res. 2017, 11, 016013. [Google Scholar] [CrossRef] [PubMed]
- Hibbard, T.; Killard, A.J. Breath Ammonia Analysis: Clinical Application and Measurement. Crit. Rev. Anal. Chem. 2011, 41, 21–35. [Google Scholar] [CrossRef]
- Dixit, K.; Fardindoost, S.; Ravishankara, A.; Tasnim, N.; Hoorfar, M. Exhaled Breath Analysis for Diabetes Diagnosis and Monitoring: Relevance, Challenges and Possibilities. Biosensors 2021, 11, 476. [Google Scholar] [CrossRef] [PubMed]
- Kearney, D.J.; Hubbard, T.; Putnam, D. Breath Ammonia Measurement in Helicobacter Pylori Infection. Dig. Dis. Sci. 2002, 47, 2523–2530. [Google Scholar] [CrossRef] [PubMed]
- Narasimhan, L.R.; Goodman, W.; Kumar, C.; Patel, N. Correlation of Breath Ammonia with Blood Urea Nitrogen and Creatinine during Hemodialysis. Proc. Natl. Acad. Sci. USA 2001, 98, 4617–4621. [Google Scholar] [CrossRef] [PubMed]
- MacGregor, G.; Ellis, S.; Andrews, J.; Imrie, M.; Innes, A.; Greening, A.P.; Cunningham, S. Breath Condensate Ammonium Is Lower in Children with Chronic Asthma. Eur. Respir. J. 2005, 26, 271–276. [Google Scholar] [CrossRef]
- Turner, C.; Walton, C.; Hoashi, S.; Evans, M. Breath Acetone Concentration Decreases with Blood Glucose Concentration in Type i Diabetes Mellitus Patients during Hypoglycaemic Clamps. J. Breath. Res. 2009, 3, 046004. [Google Scholar] [CrossRef] [PubMed]
- Wang, D.; Zhang, F.; Prabhakar, A.; Qin, X.; Forzani, E.S.; Tao, N. Colorimetric Sensor for Online Accurate Detection of Breath Acetone. ACS Sens. 2021, 6, 450–453. [Google Scholar] [CrossRef] [PubMed]
- Wang, Z.; Wang, C. Is Breath Acetone a Biomarker of Diabetes? A Historical Review on Breath Acetone Measurements. J Breath. Res. 2013, 7, 037109. [Google Scholar] [CrossRef] [PubMed]
- Simić, M.; Stavrakis, A.K.; Sinha, A.; Premčevski, V.; Markoski, B.; Stojanović, G.M. Portable Respiration Monitoring System with an Embroidered Capacitive Facemask Sensor. Biosensors 2022, 12, 339. [Google Scholar] [CrossRef] [PubMed]
- Ren, L.; Yu, K.; Tan, Y. Applications and Advances of Magnetoelastic Sensors in Biomedical Engineering: A Review. Materials 2019, 12, 1135. [Google Scholar] [CrossRef]
- Rivero, G.; Multigner, M.; Spottorno, J. Magnetic Sensors for Biomedical Applications. In Magnetic Sensors; Kuang, K., Ed.; IntechOpen: London, UK, 2012; pp. 125–150. [Google Scholar]
- Marín, P.; López, M.; Agudo, P.; Vázquez, M.; Hernando, A. Applications of Amorphous Samples Presenting High Magnetomechanical Coupling during the First Stages of Nanocrystallisation Process. Sens Actuators A Phys. 2001, 91, 218–222. [Google Scholar] [CrossRef]
- Marín, P.; Vázquez, M.; Olofinjana, A.; Davies, H.A. Influence of Cu and Nb on Relaxation and Crystallization of Amorphous FeSiB(CuNb) Wires. Nanostruct. Mater. 1998, 10, 299–310. [Google Scholar] [CrossRef]
- Coben, A.F.; Zhukov, A.P.; Pina, E.; Blanco, J.M.; Gonzalez, J.; Barandiaran, J.M. Sensitive Magnetoelastic Properties of Amorphous Ribbon for Magnetoelastic Sensors. J. Magn. Magn. Mater. 2000, 215, 743–745. [Google Scholar] [CrossRef]
- O’Handley, R.C. Modern Magnetic Materials: Principles and Applications; Wiley-Interscience: New York, NY, USA, 2000. [Google Scholar]
- Gutiérrez, J.; Muto, V.; Squire, P.T. Induced Anisotropy and Magnetoelastic Properties in Fe-Rich Metallic Glasses. J. Non Cryst. Solids 2001, 287, 417–420. [Google Scholar] [CrossRef]
- Villari, E. Intorno alle modificazioni del momento magnetico di una verga di ferro e di acciaio, prodotte per la trazione della medesima e pel passaggio di una corrente attraverso la stessa. Il Nuovo Cimento 1864, 20, 317–362. [Google Scholar] [CrossRef]
- Joule, J.P. XVII. On the Effects of Magnetism upon the Dimensions of Iron and Steel Bars. Lond. Edinb. Dublin Philos. Mag. J. Sci. 1847, 30, 76–87. [Google Scholar] [CrossRef]
- Saiz, P.G.; Fernández De Luis, R.; Lasheras, A.; Arriortua, M.I.; Lopes, A.C. Magnetoelastic Resonance Sensors: Principles, Applications, and Perspectives. ACS Sens. 2022, 7, 1248–1268. [Google Scholar] [CrossRef]
- Mungle, C.; Grimes, C.A.; Dreschel, W.R. Magnetic Field Tuning of the Frequency and Temperature Response of a Magnetoelastic Sensor. Sens. Actuators A 2002, 101, 143–149. [Google Scholar] [CrossRef]
- Peña, A.; Matatagui, D.; Marín, P.; Cruz, C.; Horrillo, C. Study of Magnetoelastic Resonance for Chemical Sensors: Ribbons vs. Microwires. In Proceedings of the 2021 13th Spanish Conference on Electron Devices (CDE), Sevilla, Spain, 9–11 June 2021. [Google Scholar] [CrossRef]
- Grimes, C.A.; Kouzoudis, D.; Mungle, C. Simultaneous Measurement of Liquid Density and Viscosity Using Remote Query Magnetoelastic Sensors. Rev. Sci. Instrum. 2000, 71, 3822–3824. [Google Scholar] [CrossRef]
- Atalay, S.; Kolat, V.S.; Bayri, N.; Izgi, T. Magnetoelastic Sensor Studies on Amorphous Magnetic FeSiB Wire and the Application in Viscosity Measurement. J. Supercond. Nov. Magn. 2016, 29, 1551–1556. [Google Scholar] [CrossRef]
- Marín, P.; Marcos, M.; Hernando, A. High Magnetomechanical Coupling on Magnetic Microwire for Sensors with Biological Applications. Appl. Phys. Lett. 2010, 96, 11–14. [Google Scholar] [CrossRef]
- Kouzoudis, D.; Grimes, C.A. The Frequency Response of Magnetoelastic Sensors to Stress and Atmospheric Pressure. Smart Mater. Struct. 2000, 9, 885–889. [Google Scholar] [CrossRef]
- Hernando, A.; Vazquez, M.; Barandiaran, J.M. Metallic Glasses and Sensing Applications. J. Phys. E Sci. Instrum. 1988, 21, 1129–1139. [Google Scholar] [CrossRef]
- Guo, X.; Sang, S.; Guo, J.; Jian, A.; Duan, Q.; Ji, J.; Zhang, Q.; Zhang, W. A Magnetoelastic Biosensor Based on E2 Glycoprotein for Wireless Detection of Classical Swine Fever Virus E2 Antibody. Sci. Rep. 2017, 7, 15626. [Google Scholar] [CrossRef] [PubMed]
- Huang, S.J.; Wang, Y.J.; Cai, Q.Y.; Fang, J. de Detection of Staphylococcus Aureus in Different Liquid Mediums Using Wireless Magnetoelastic Sensor. Chin. J. Anal. Chem. 2010, 38, 105–108. [Google Scholar] [CrossRef]
- Pang, P.; Xiao, X.; Cai, Q.; Yao, S.; Grimes, C.A. A Wireless Magnetoelastic-Sensing Device for in Situ Evaluation of Pseudomonas Aeruginosa Biofilm Formation. Sens. Actuators B Chem. 2008, 133, 473–477. [Google Scholar] [CrossRef]
- Ruan, C.; Zeng, K.; Varghese, O.K.; Grimes, C.A. Magnetoelastic Immunosensors: Amplified Mass Immunosorbent Assay for Detection of Escherichia Coli O157:H7. Anal. Chem. 2003, 75, 6494–6498. [Google Scholar] [CrossRef]
- Gao, X.; Yang, W.; Pang, P.; Liao, S.; Cai, Q.; Zeng, K.; Grimes, C.A. A Wireless Magnetoelastic Biosensor for Rapid Detection of Glucose Concentrations in Urine Samples. Sens. Actuators B Chem. 2007, 128, 161–167. [Google Scholar] [CrossRef]
- Cai, Q.; Zeng, K.; Ruan, C.; Desai, T.A.; Grimes, C.A. A Wireless, Remote Query Glucose Biosensor Based on a PH-Sensitive Polymer. Anal. Chem. 2004, 76, 4038–4043. [Google Scholar] [CrossRef]
- Puckett, L.G.; Barrett, G.; Kouzoudis, D.; Grimes, C.; Bachas, L.G. Monitoring Blood Coagulation with Magnetoelastic Sensors. Biosens. Bioelectron. 2003, 18, 675–681. [Google Scholar] [CrossRef]
- Holmes, H.R.; Tan, E.L.; Ong, K.G.; Rajachar, R.M. Fabrication of Biocompatible, Vibrational Magnetoelastic Materials for Controlling Cellular Adhesion. Biosensors 2012, 2, 57–69. [Google Scholar] [CrossRef] [PubMed]
- Baimpos, T.; Gora, L.; Nikolakis, V.; Kouzoudis, D. Selective Detection of Hazardous VOCs Using Zeolite/Metglas Composite Sensors. Sens. Actuators A Phys. 2012, 186, 21–31. [Google Scholar] [CrossRef]
- Cai, Q.Y.; Jain, M.K.; Grimes, C.A. A Wireless, Remote Query Ammonia Sensor. Sens. Actuators B 2001, 77, 614–619. [Google Scholar] [CrossRef]
- Cai, Q.Y.; Cammers-Goodwin, A.; Grimes, C.A. A Wireless, Remote Query Magnetoelastic CO2 Sensor. J. Environ. Monit. 2000, 2, 556–560. [Google Scholar] [CrossRef]
- Grimes, C.A.; Roy, S.C.; Rani, S.; Cai, Q. Theory, Instrumentation and Applications of Magnetoelastic Resonance Sensors: A Review. Sensors 2011, 11, 2809–2844. [Google Scholar] [CrossRef]
- Sang, S.; Li, Y.; Guo, X.; Zhang, B.; Xue, X.; Zhuo, K.; Zhao, C.; Zhang, W.; Yuan, Z. A Portable Device for Rapid Detection of Human Serum Albumin Using an Immunoglobulin-Coating-Based Magnetoelastic Biosensor. Biosens. Bioelectron. 2019, 141, 111399. [Google Scholar] [CrossRef]
- Ayazi, F.; Kim, C.-J. Institute of Electrical and Electronics Engineers. In Proceedings of the MEMS 2014: The 27th IEEE International Conference on Micro Electro Mechanical Systems, San Francisco, CA, USA, 26–30 January 2014. [Google Scholar]
- Phillips, M.; Herrera, J.; Krishnan, S.; Zain, M.; Greenberg, J.; Cataneo, R.N. Variation in Volatile Organic Compounds in the Breath of Normal Humans. J. Chromatogr. B Biomed. Sci. Appl. 1999, 729, 75–78. [Google Scholar] [CrossRef]
- Jain, M.K.; Schmidt, S.; Ong, G.; Mungle, C.; Grimes, C.A. Magnetoacoustic Remote Query Temperature and Humidity Sensors. Smart Mater. Struct. 2000, 9, 502–510. [Google Scholar] [CrossRef]
- Matatagui, D.; Fernández, M.J.; Santos, J.P.; Fontecha, J.; Sayago, I.; Horrillo, M.C.; Gràcia, I.; Cané, C. Real-Time Characterization of Electrospun PVP Nanofibers as Sensitive Layer of a Surface Acoustic Wave Device for Gas Detection. J. Nanomater. 2014, 2014, 1–8. [Google Scholar] [CrossRef]
- Herrero-Gómez, C.; Marín, P.; Hernando, A. Bias Free Magnetomechanical Coupling on Magnetic Microwires for Sensing Applications. Appl. Phys. Lett. 2013, 103, 142414. [Google Scholar] [CrossRef]
- Apicella, V.; Clemente, C.S.; Davino, D.; Leone, D.; Visone, C. Magneto-Mechanical Optimization and Analysis of a Magnetostrictive Cantilever Beam for Energy Harvesting. J. Magn. Magn. Mater. 2019, 475, 401–407. [Google Scholar] [CrossRef]
- Gonzalez, G. Foundations of Oscillator Circuit Design, 1st ed.; Artech: Morristown, NJ, USA, 2007. [Google Scholar]
- Lopes, A.C.; Sagasti, A.; Lasheras, A.; Muto, V.; Gutiérrez, J.; Kouzoudis, D.; Barandiarán, J.M. Accurate Determination of the Q Quality Factor in Magnetoelastic Resonant Platforms for Advanced Biological Detection. Sensors 2018, 18, 887. [Google Scholar] [CrossRef] [PubMed]
- Sisniega, B.; Gutiérrez, J.; Muto, V.; García-Arribas, A. Improved Determination of q Quality Factor and Resonance Frequency in Sensors Based on the Magnetoelastic Resonance through the Fitting to Analytical Expressions. Materials 2020, 13, 4708. [Google Scholar] [CrossRef]
- Saiz, P.G.; Gandia, D.; Lasheras, A.; Sagasti, A.; Quintana, I.; Fdez-Gubieda, M.L.; Gutiérrez, J.; Arriortua, M.I.; Lopes, A.C. Enhanced Mass Sensitivity in Novel Magnetoelastic Resonators Geometries for Advanced Detection Systems. Sens. Actuators B Chem. 2019, 296, 126612. [Google Scholar] [CrossRef]
- Livingston, J.D. Magnetomechanical Properties of Amorphous Metals. Physica Status Solidi (a) 1982, 70, 591–596. [Google Scholar] [CrossRef]
- Sisniega, B.; Sedano, A.S.; Gutiérrez, J.; García-Arribas, A. Real Time Monitoring of Calcium Oxalate Precipitation Reaction by Using Corrosion Resistant Magnetoelastic Resonance Sensors. Sensors 2020, 20, 2802. [Google Scholar] [CrossRef] [PubMed]
- Hierlernann, A.; Zellers, E.T.; Ricco, A.J. Use of Linear Solvation Energy Relationships for Modeling Responses from Polymer-Coated Acoustic-Wave Vapor Sensors. Anal. Chem. 2001, 73, 3458–3466. [Google Scholar] [CrossRef]
- Song, X.; Hu, R.; Xu, S.; Liu, Z.; Wang, J.; Shi, Y.; Xu, J.; Chen, K.; Yu, L. Highly Sensitive Ammonia Gas Detection at Room Temperature by Integratable Silicon Nanowire Field-Effect Sensors. ACS Appl. Mater. Interfaces 2021, 13, 14377–14384. [Google Scholar] [CrossRef]
- Li, S.; Liu, A.; Yang, Z.; He, J.; Wang, J.; Liu, F.; Lu, H.; Yan, X.; Sun, P.; Liang, X.; et al. Room Temperature Gas Sensor Based on Tin Dioxide@ Polyaniline Nanocomposite Assembled on Flexible Substrate: Ppb-Level Detection of NH3. Sens. Actuators B Chem. 2019, 299, 126970. [Google Scholar] [CrossRef]
- Guo, Z.; Wang, B.; Wang, X.; Li, Y.; Gai, S.; Wu, Y.; Cheng, X. A High-Sensitive Room Temperature Gas Sensor Based on Cobalt Phthalocyanines and Reduced Graphene Oxide Nanohybrids for the Ppb-Levels of Ammonia Detection. RSC Adv. 2019, 9, 37518–37525. [Google Scholar] [CrossRef] [PubMed]
- Kim, K.; Choi, P.G.; Itoh, T.; Masuda, Y. Catalyst-Free Highly Sensitive SnO2 Nanosheet Gas Sensors for Parts per Billion-Level Detection of Acetone. ACS Appl. Mater. Interfaces 2020, 12, 51637–51644. [Google Scholar] [CrossRef] [PubMed]
- Kou, X.; Meng, F.; Chen, K.; Wang, T.; Sun, P.; Liu, F.; Yan, X.; Sun, Y.; Liu, F.; Shimanoe, K.; et al. High-Performance Acetone Gas Sensor Based on Ru-Doped SnO2 Nanofibers. Sens. Actuators B Chem. 2020, 320, 128292. [Google Scholar] [CrossRef]
- Wang, H.; Nie, S.; Li, H.; Ali, R.; Fu, J.; Xiong, H.; Li, J.; Wu, Z.; Lau, W.M.; Mahmood, N.; et al. 3D Hollow Quasi-Graphite Capsules/Polyaniline Hybrid with a High Performance for Room-Temperature Ammonia Gas Sensors. ACS Sens. 2019, 4, 2343–2350. [Google Scholar] [CrossRef] [PubMed]
- Escobedo, P.; Erenas, M.M.; López-Ruiz, N.; Carvajal, M.A.; Gonzalez-Chocano, S.; de Orbe-Payá, I.; Capitán-Valley, L.F.; Palma, A.J.; Martínez-Olmos, A. Flexible Passive near Field Communication Tag for Multigas Sensing. Anal. Chem. 2017, 89, 1697–1703. [Google Scholar] [CrossRef] [PubMed]
- Vásquez Quintero, A.; Molina-Lopez, F.; Smits, E.C.P.; Danesh, E.; van den Brand, J.; Persaud, K.; Oprea, A.; Barsan, N.; Weimar, U.; de Rooij, N.F.; et al. Smart RFID Label with a Printed Multisensor Platform for Environmental Monitoring. Flex. Print. Electron. 2016, 1, 025003. [Google Scholar] [CrossRef]
- Clément, P.; Ramos, A.; Lazaro, A.; Molina-Luna, L.; Bittencourt, C.; Girbau, D.; Llobet, E. Oxygen Plasma Treated Carbon Nanotubes for the Wireless Monitoring of Nitrogen Dioxide Levels. Sens. Actuators B Chem. 2015, 208, 444–449. [Google Scholar] [CrossRef]
- Atalay, S.; Izgi, T.; Kolat, V.S.; Erdemoglu, S.; Inan, O.O. Magnetoelastic Humidity Sensors with TiO2 Nanotube Sensing Layers. Sensors 2020, 20, 425. [Google Scholar] [CrossRef] [PubMed]
- Baimpos, T.; Boutikos, P.; Nikolakis, V.; Kouzoudis, D. A Polymer-Metglas Sensor Used to Detect Volatile Organic Compounds. Sens. Actuators A Phys. 2010, 158, 249–253. [Google Scholar] [CrossRef]





| Techn. | Main approach | Wireless | Analyte | Measurement | Response/Recovery Time | Ref. |
|---|---|---|---|---|---|---|
| CR | Silicon nanowires array | No | NH3/Air–100 ppb | Real time | ~20 s both | [72] |
| CR | Tin dioxide @polyaniline composite | No | NH3/Air–100 ppm | Real time | 125 s/167 s | [73] |
| CR | Cobalt phtalocyanines and reduced graphene oxide nanohybrids | No | NH3/Air–100 ppb | Real time | Response time 45 s, UV light used to speed up recovery | [74] |
| CR | SnO2 nanosheet | No | Acetone/Air–1 ppm | Real time | 40 s/610 s | [75] |
| CR | Ru-doped SnO2 nanofibers | No | Acetone/Air–100 ppm | Real time | 1 s/36 s | [76] |
| CR | Hollow Quasi-Graphite capsules/Polyaniline hybrid | No | NH3/Air–100 ppm | Real time | 34 s/42 s | [77] |
| Opt. | Near Field Communication (NFC) technology, white LED as excitation source | Yes | NH3/N2–0.15% vol | Real time | 5.43 min/6.64 min | [78] |
| Cap. | HF RFID (High-Frequency Radiofrequency Identification) smart label | Yes | NH3/Air–5 ppm | 30 s each measure, 1 min period | ~30 min | [79] |
| CR | RH–20 to 40% | 5.43 min/6.64 min | ||||
| CR | Oxygen plasma-treated carbon nanotubes | Yes | NH3/Air–0–5 ppm | 30 s each measure, 1 min period | ~30 min | [80] |
| ME | TiO2 nanotubes on amorphous ribbon | Yes | RH–20 to 40% | 4 s between each measurement | 5.43 min/6.64 min | [81] |
| ME | BAYHYDROL-110 on Metglas ribbon | Yes | RH–10 to 80% | 1 min between each measurement | Few min | [82] |
| ME | Poly (acrylic acid co-isooctylacrylate) on Metglas ribbon | Yes | NH3/N2–0.8% vol | 1 min between each measurement | ~15 min | [55] |
| RH–0 to 15% | ~1 min/several min | |||||
| ME | PVP nanofiber-functionalized micro ribbon | Yes | RH–17 to 95% | Real time | <2 min | This work |
| Acetone/Air–40 ppm | ||||||
| NH3/Air–40 ppm | ||||||
| Benzene/Air–40 ppm |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2022 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Peña, A.; Aguilera, J.D.; Matatagui, D.; de la Presa, P.; Horrillo, C.; Hernando, A.; Marín, P. Real-Time Monitoring of Breath Biomarkers with A Magnetoelastic Contactless Gas Sensor: A Proof of Concept. Biosensors 2022, 12, 871. https://doi.org/10.3390/bios12100871
Peña A, Aguilera JD, Matatagui D, de la Presa P, Horrillo C, Hernando A, Marín P. Real-Time Monitoring of Breath Biomarkers with A Magnetoelastic Contactless Gas Sensor: A Proof of Concept. Biosensors. 2022; 12(10):871. https://doi.org/10.3390/bios12100871
Chicago/Turabian StylePeña, Alvaro, Juan Diego Aguilera, Daniel Matatagui, Patricia de la Presa, Carmen Horrillo, Antonio Hernando, and Pilar Marín. 2022. "Real-Time Monitoring of Breath Biomarkers with A Magnetoelastic Contactless Gas Sensor: A Proof of Concept" Biosensors 12, no. 10: 871. https://doi.org/10.3390/bios12100871
APA StylePeña, A., Aguilera, J. D., Matatagui, D., de la Presa, P., Horrillo, C., Hernando, A., & Marín, P. (2022). Real-Time Monitoring of Breath Biomarkers with A Magnetoelastic Contactless Gas Sensor: A Proof of Concept. Biosensors, 12(10), 871. https://doi.org/10.3390/bios12100871