COVID-19 and Nanoscience in the Developing World: Rapid Detection and Remediation in Wastewater
Abstract
1. Perspective
2. Conclusions
Author Contributions
Funding
Data Availability Statement
Conflicts of Interest
References
- WHO Organization. WHO Coronavirus Disease (COVID-19) Dashboard. Available online: https://covid19.who.int/ (accessed on 13 July 2020).
- Morawska, L.; Tang, J.W.; Bahnfleth, W.; Bluyssen, P.M.; Boerstra, A.; Buonanno, G.; Cao, J.; Dancer, S.; Floto, A.; Franchimon, F.; et al. How can airborne transmission of COVID-19 indoors be minimised? Environ. Int. 2020, 142, 105832. [Google Scholar] [CrossRef]
- Amirian, E.S. Potential fecal transmission of SARS-CoV-2: Current evidence and implications for public health. Int. J. Infect. Dis. 2020, 95, 363–370. [Google Scholar] [CrossRef] [PubMed]
- Sunkari, E.D.; Korboe, H.M.; Abu, M.; Kizildeniz, T. Sources and routes of SARS-CoV-2 transmission in water systems in Africa: Are there any sustainable remedies? Sci. Total Environ. 2021, 753, 142298. [Google Scholar] [CrossRef]
- Gormley, M.; Aspray, T.J.; Kelly, D.A. COVID-19: Mitigating transmission via wastewater plumbing systems. Lancet Glob. Health 2020, 8, e643. [Google Scholar] [CrossRef]
- Dai, X.; Li, X.; Yang, W.; Dai, L.; Dong, B. Viruses in sewage sludge from wastewater treatment plant: Occurance and potential risk during sludge treatment and disposal. Water Wastewater Eng. 2020, 46, 60–73. [Google Scholar]
- Ahmed, W.; Angel, N.; Edson, J.; Bibby, K.; Bivins, A.; O’Brien, J.W.; Choi, P.M.; Kitajima, M.; Simpson, S.L.; Li, J.; et al. First confirmed detection of SARS-CoV-2 in untreated wastewater in Australia: A proof of concept for the wastewater surveillance of COVID-19 in the community. Sci. Total Environ. 2020, 728, 138764. [Google Scholar] [CrossRef]
- Wurtzer, S.; Marechal, V.; Mouchel, J.-M.; Maday, Y.; Teyssou, R.; Richard, E.; Almayrac, J.L.; Moulin, L. Evaluation of lockdown impact on SARS-CoV-2 dynamics through viral genome quantification in Paris wastewaters. MedRxiv 2020. [Google Scholar] [CrossRef]
- La Rosa, G.; Iaconelli, M.; Mancini, P.; Ferraro, G.B.; Veneri, C.; Bonadonna, L.; Lucentini, L.; Suffredini, E. First detection of SARS-CoV-2 in untreated wastewaters in Italy. Sci. Total Environ. 2020, 736, 139652. [Google Scholar] [CrossRef]
- Medema, G.; Heijnen, L.; Elsinga, G.; Italiaander, R.; Brouwer, A. Presence of SARS-Coronavirus-2 in sewage. MedRxiv 2020. [Google Scholar] [CrossRef]
- Wu, F.; Xiao, A.; Zhang, J.; Gu, X.; Lee, W.L.; Kauffman, K.; Hanage, W.; Matus, M.; Ghaeli, N.; Endo, N.; et al. SARS-CoV-2 titers in wastewater are higher than expected from clinically confirmed cases. MedRxiv 2020, 5. [Google Scholar] [CrossRef]
- Hata, A.; Honda, R.; Hara-Yamamura, H.; Meuchi, Y. Detection of SARS-CoV-2 in wastewater in Japan by multiple molecular assays-implication for wastewater-based epidemiology (WBE). MedRxiv 2020. [Google Scholar] [CrossRef]
- Wang, X.W.; Li, J.; Guo, T.; Zhen, B.; Kong, Q.; Yi, B.; Li, Z.; Song, N.; Jin, M.; Xiao, W.; et al. Concentration and detection of SARS coronavirus in sewage from Xiao Tang Shan Hospital and the 309th Hospital of the Chinese People’s Liberation Army. Water Sci. Technol. 2005, 52, 213–221. [Google Scholar] [CrossRef]
- UNESCO WWAP. World Water Assessment Programme. Available online: http://www.unesco.org/new/en/natural-sciences/environment/water/wwap/ (accessed on 13 July 2020).
- Tabish, T.A.; Hamblin, M.R. Multivalent nanomedicines to treat COVID-19: A slow train coming. Nano Today 2020, 35, 100962. [Google Scholar] [CrossRef] [PubMed]
- Farooq, T.; Adeel, M.; He, Z.; Umar, M.; Shakoor, N.; da Silva, W.; Elmer, W.; White, J.C.; Rui, Y. Nanotechnology and Plant Viruses: An Emerging Disease Management Approach for Resistant Pathogens. ACS Nano 2021. [Google Scholar] [CrossRef] [PubMed]
- Adeel, M.; Farooq, T.; White, J.C.; Hao, Y.; He, Z.; Rui, Y. Carbon-based nanomaterials suppress tobacco mosaic virus (TMV) infection and induce resistance in Nicotiana benthamiana. J. Hazard. Mater. 2021, 404, 124167. [Google Scholar] [CrossRef] [PubMed]
- D’Aoust, P.M.; Mercier, E.; Montpetit, D.; Jia, J.J.; Alexandrov, I.; Neault, N.; Baig, A.T.; Mayne, J.; Zhang, X.; Alain, T.; et al. Quantitative analysis of SARS-CoV-2 RNA from wastewater solids in communities with low COVID-19 incidence and prevalence. Water Res. 2021, 188, 116560. [Google Scholar] [CrossRef] [PubMed]
- Wang, J.; Feng, H.; Zhang, S.; Ni, Z.; Ni, L.; Chen, Y.; Zhuo, L.; Zhong, Z.; Qu, T. SARS-CoV-2 RNA detection of hospital isolation wards hygiene monitoring during the Coronavirus Disease 2019 outbreak in a Chinese hospital. Int. J. Infect. Dis. 2020, 94, 103–106. [Google Scholar] [CrossRef]
- Hokajärvi, A.-M.; Rytkönen, A.; Tiwari, A.; Kauppinen, A.; Oikarinen, S.; Lehto, K.-M.; Kankaanpää, A.; Gunnar, T.; Al-Hello, H.; Blomqvist, S.; et al. The detection and stability of the SARS-CoV-2 RNA biomarkers in wastewater influent in Helsinki, Finland. MedRxiv 2021, 770. [Google Scholar] [CrossRef]
- Westhaus, S.; Weber, F.-A.; Schiwy, S.; Linnemann, V.; Brinkmann, M.; Widera, M.; Greve, C.; Janke, A.; Hollert, H.; Wintgens, T.; et al. Detection of SARS-CoV-2 in raw and treated wastewater in Germany—Suitability for COVID-19 surveillance and potential transmission risks. Sci. Total Environ. 2021, 751, 141750. [Google Scholar] [CrossRef]
- Haramoto, E.; Malla, B.; Thakali, O.; Kitajima, M. First environmental surveillance for the presence of SARS-CoV-2 RNA in wastewater and river water in Japan. Sci. Total Environ. 2020, 737, 140405. [Google Scholar] [CrossRef] [PubMed]
- Sharif, S.; Ikram, A.; Khurshid, A.; Salman, M.; Mehmood, N.; Arshad, Y.; Ahmad, J.; Angez, M.; Alam, M.M.; Rehman, L.; et al. Detection of SARS-Coronavirus-2 in wastewater, using the existing environmental surveillance network: An epidemiological gateway to an early warning for COVID-19 in communities. MedRxiv 2020. [Google Scholar] [CrossRef]
- Nemudryi, A.; Nemudraia, A.; Wiegand, T.; Surya, K.; Buyukyoruk, M.; Vanderwood, K.K.; Wilkinson, R.; Wiedenheft, B. Temporal detection and phylogenetic assessment of SARS-CoV-2 in municipal wastewater. MedRxiv 2020. [Google Scholar] [CrossRef]
- Gehrke, I.; Geiser, A.; Somborn-Schulz, A. Innovations in nanotechnology for water treatment. Nanotechnol. Sci. Appl. 2015, 8, 1–17. [Google Scholar] [CrossRef] [PubMed]
- Amin, M.T.; Alazba, A.A.; Manzoor, U. A Review of Removal of Pollutants from Water/Wastewater Using Different Types of Nanomaterials. Adv. Mater. Sci. Eng. 2014, 2014, 1–24. [Google Scholar] [CrossRef]
- Zodrow, K.; Brunet, L.; Mahendra, S.; Li, D.; Zhang, A.; Li, Q.; Alvarez, P.J. Polysulfone ultrafiltration membranes impregnated with silver nanoparticles show improved biofouling resistance and virus removal. Water Res. 2009, 43, 715–723. [Google Scholar] [CrossRef] [PubMed]
- Quang, D.V.; Sarawade, P.B.; Jeon, S.J.; Kim, S.H.; Kim, J.-K.; Chai, Y.G.; Kim, H.T. Effective water disinfection using silver nanoparticle containing silica beads. Appl. Surf. Sci. 2013, 266, 280–287. [Google Scholar] [CrossRef]
- Hajkova, P.; Spatenka, P.; Horsky, J.; Horska, I.; Kolouch, A. Photocatalytic Effect of TiO2 Films on Viruses and Bacteria. Plasma Process. Polym. 2007, 4, S397–S401. [Google Scholar] [CrossRef]
- Chen, H.; Huang, M.; Liu, Y.; Meng, L.; Ma, M. Functionalized electrospun nanofiber membranes for water treatment: A review. Sci. Total Environ. 2020, 739, 139944. [Google Scholar] [CrossRef]
- Brown, T.D.; Dalton, P.D.; Hutmacher, D.W. Melt electrospinning today: An opportune time for an emerging polymer process. Prog. Polym. Sci. 2016, 56, 116–166. [Google Scholar] [CrossRef]
- Ding, Y.; Hou, H.; Zhao, Y.; Zhu, Z.; Fong, H. Electrospun polyimide nanofibers and their applications. Prog. Polym. Sci. 2016, 61, 67–103. [Google Scholar] [CrossRef]
- Bivins, A.; North, D.; Ahmad, A.; Ahmed, W.; Alm, E.; Been, F.; Bhattacharya, P.; Bijlsma, L.; Boehm, A.B.; Brown, J.; et al. Wastewater-Based Epidemiology: Global Collaborative to Maximize Contributions in the Fight Against COVID-19. Environ. Sci. Technol. 2020, 54, 7754–7757. [Google Scholar] [CrossRef] [PubMed]
- Mao, K.; Zhang, H.; Yang, Z. Can a Paper-Based Device Trace COVID-19 Sources with Wastewater-Based Epidemiology? Environ. Sci. Technol. 2020, 54, 3733–3735. [Google Scholar] [CrossRef] [PubMed]
- Hassard, F.; Lundy, L.; Singer, A.C.; Grimsley, J.; Di Cesare, M. Innovation in wastewater near-source tracking for rapid identification of COVID-19 in schools. Lancet Microbe 2021, 2, e4–e5. [Google Scholar] [CrossRef]
- Tabish, T.A.; Narayan, R.J.; Edirisinghe, M. Rapid and label-free detection of COVID-19 using coherent anti-Stokes Raman scattering microscopy. MRS Commun. 2020, 10, 566–572. [Google Scholar] [CrossRef]
- Moitra, P.; Alafeef, M.; Dighe, K.; Frieman, M.B.; Pan, D. Selective Naked-Eye Detection of SARS-CoV-2 Mediated by N Gene Targeted Antisense Oligonucleotide Capped Plasmonic Nanoparticles. ACS Nano 2020, 14, 7617–7627. [Google Scholar] [CrossRef] [PubMed]
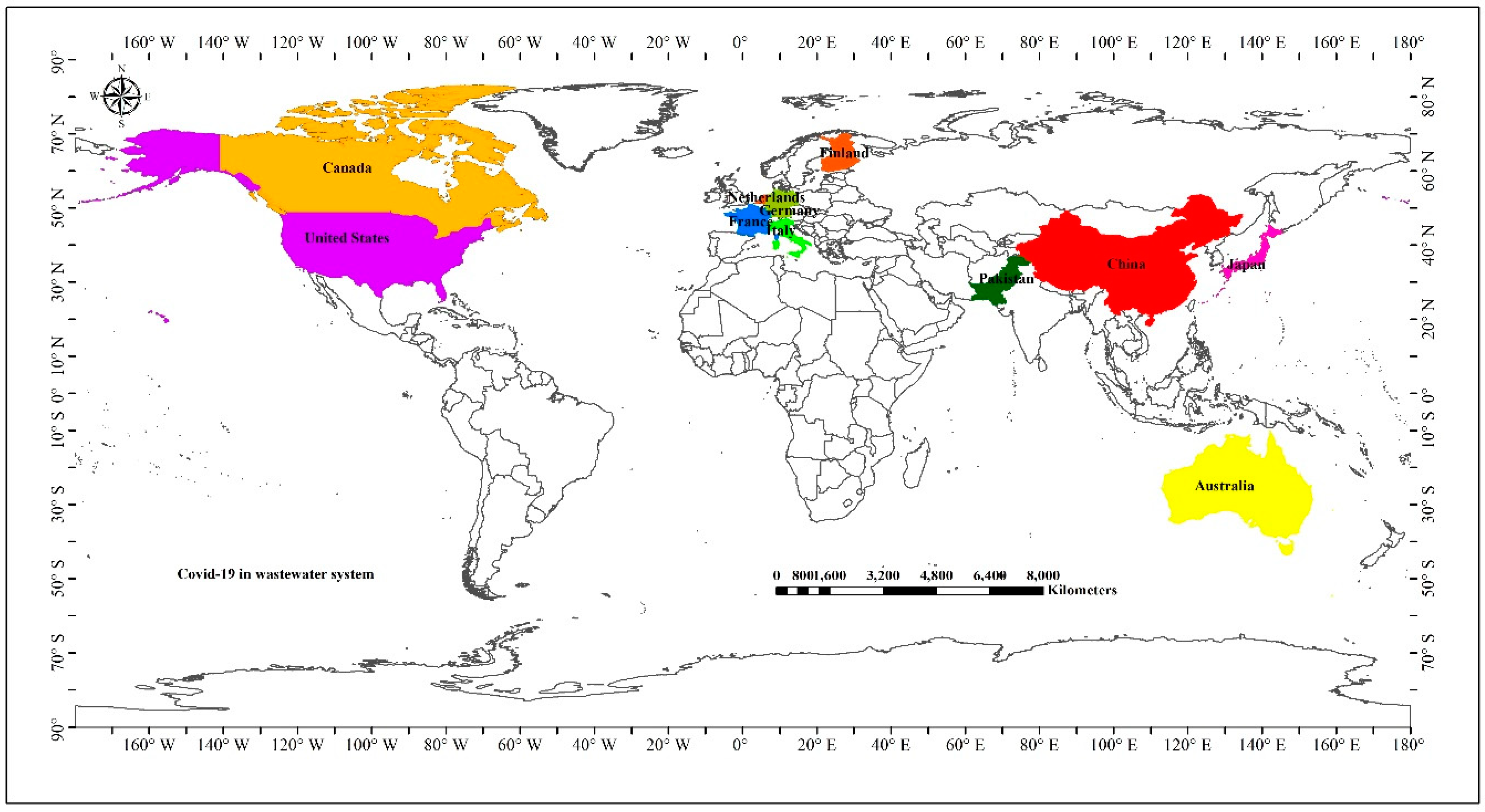
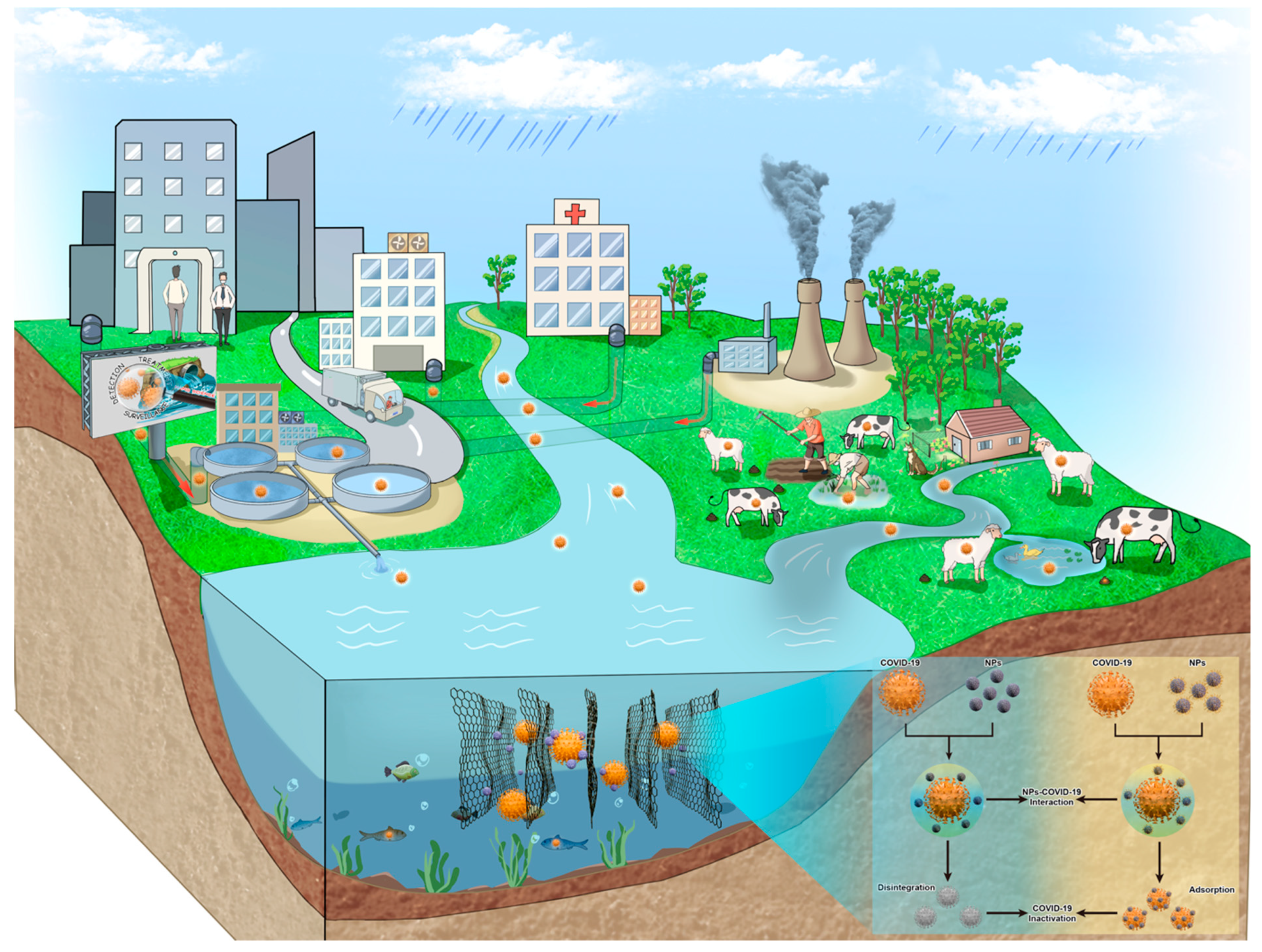

| Country | City/County | Specimen Source | Detection Method | Percentage Detection | Concentration (Copies/L) | Reference |
|---|---|---|---|---|---|---|
| Australia | Brisbane, Queensland | Untreated wastewater | RT-qPCR c, sequencging | 22% (2/9) | 1.2 × 102 | [7] |
| Canada | Ottawa, Gatineau | PCS a | RT-ddPCR, RT-qPCR | 90.6–92.7% (n = 6) | Not available | [18] |
| PGS b | 79.2–82.3% (n = 5) | Not available | ||||
| China | Beijing | Wastewater | RT-qPCR | Not available | Not available | [19] |
| Finland | Helsinki | Wastewater | RT-qPCR | Pellte (78–89%) | Varied according to assay | [20] |
| Supernatent (59–100%) | ||||||
| France | Paris | Treated wastewater | RT-qPCR | 100% (23/23) | >106.5 | [8] |
| Untreated wastewater | RT-qPCR | 75% (6/8) | ~105 | |||
| Germany | North Rhine-Westphalia | Solid phase wastewater d | RT-qPCR, sequencing | Not available | 25 copies/mL | [21] |
| Aqueous phase wastewater e | 1.8 copies/mL | |||||
| Italy | Milan, Rome | Untreated wastewater | RT-qPCR | 50% (6/12) | Not available | [9] |
| Japan | Yamanashi | Secondary-treated wastewater f | RT-qPCR | 20% | 2.4 × 103 | [22] |
| Netherlands | Amsterdam, Utrecht, Amersfoort, Apeldoorn, Tilburg, Schiphol | Untreated wastewater | RT-qPCR | 58% (14/24) | Not available | [10] |
| Pakistan | 38 districts | Untreated wastewater | RT-qPCR | 27% (21/78) | Not available | [23] |
| USA | Massachusett, | Untreated wastewater | RT-qPCR, sequencing | 71% (10/14) | >2 × 105 | [11] |
| Bozeman, Montana | Untreated wastewater | RT-PCR, sequencing | 100% (7/7) | >3 × 104 | [24] |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Adeel, M.; Farooq, T.; Shakoor, N.; Ahmar, S.; Fiaz, S.; White, J.C.; Gardea-Torresdey, J.L.; Mora-Poblete, F.; Rui, Y. COVID-19 and Nanoscience in the Developing World: Rapid Detection and Remediation in Wastewater. Nanomaterials 2021, 11, 991. https://doi.org/10.3390/nano11040991
Adeel M, Farooq T, Shakoor N, Ahmar S, Fiaz S, White JC, Gardea-Torresdey JL, Mora-Poblete F, Rui Y. COVID-19 and Nanoscience in the Developing World: Rapid Detection and Remediation in Wastewater. Nanomaterials. 2021; 11(4):991. https://doi.org/10.3390/nano11040991
Chicago/Turabian StyleAdeel, Muhammad, Tahir Farooq, Noman Shakoor, Sunny Ahmar, Sajid Fiaz, Jason C. White, Jorge L. Gardea-Torresdey, Freddy Mora-Poblete, and Yukui Rui. 2021. "COVID-19 and Nanoscience in the Developing World: Rapid Detection and Remediation in Wastewater" Nanomaterials 11, no. 4: 991. https://doi.org/10.3390/nano11040991
APA StyleAdeel, M., Farooq, T., Shakoor, N., Ahmar, S., Fiaz, S., White, J. C., Gardea-Torresdey, J. L., Mora-Poblete, F., & Rui, Y. (2021). COVID-19 and Nanoscience in the Developing World: Rapid Detection and Remediation in Wastewater. Nanomaterials, 11(4), 991. https://doi.org/10.3390/nano11040991











