Recent Advances in Signaling Pathways Comprehension as Carcinogenesis Triggers in Basal Cell Carcinoma
Abstract
:1. Introduction
2. The Genetic Basis of Basal Cell Carcinoma Initiation and Therapy Resistance
2.1. Genes Involved in Nevoid Basal Cell Carcinoma Syndrome
2.2. Genes Involved in Sporadic BCC
2.3. Genes Linked to Therapy Resistance
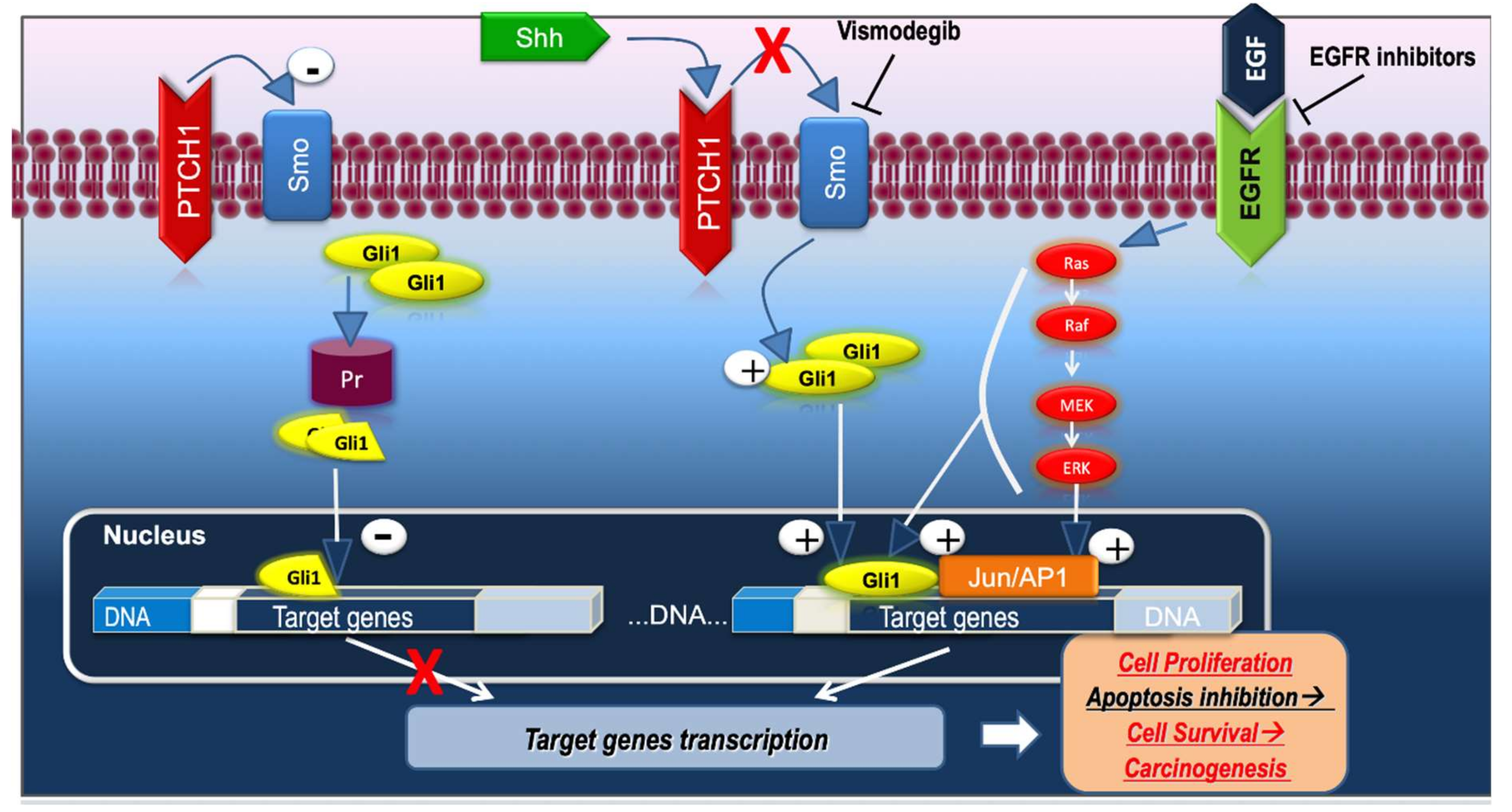
3. Hedgehog Pathway—From Discovery to New Concepts
4. The Role of Inflammation and Immune Response in BCC Pathogenesis
4.1. Tumor Microenvironment in BCC
4.2. The Link between Inflammation and Hh Signaling
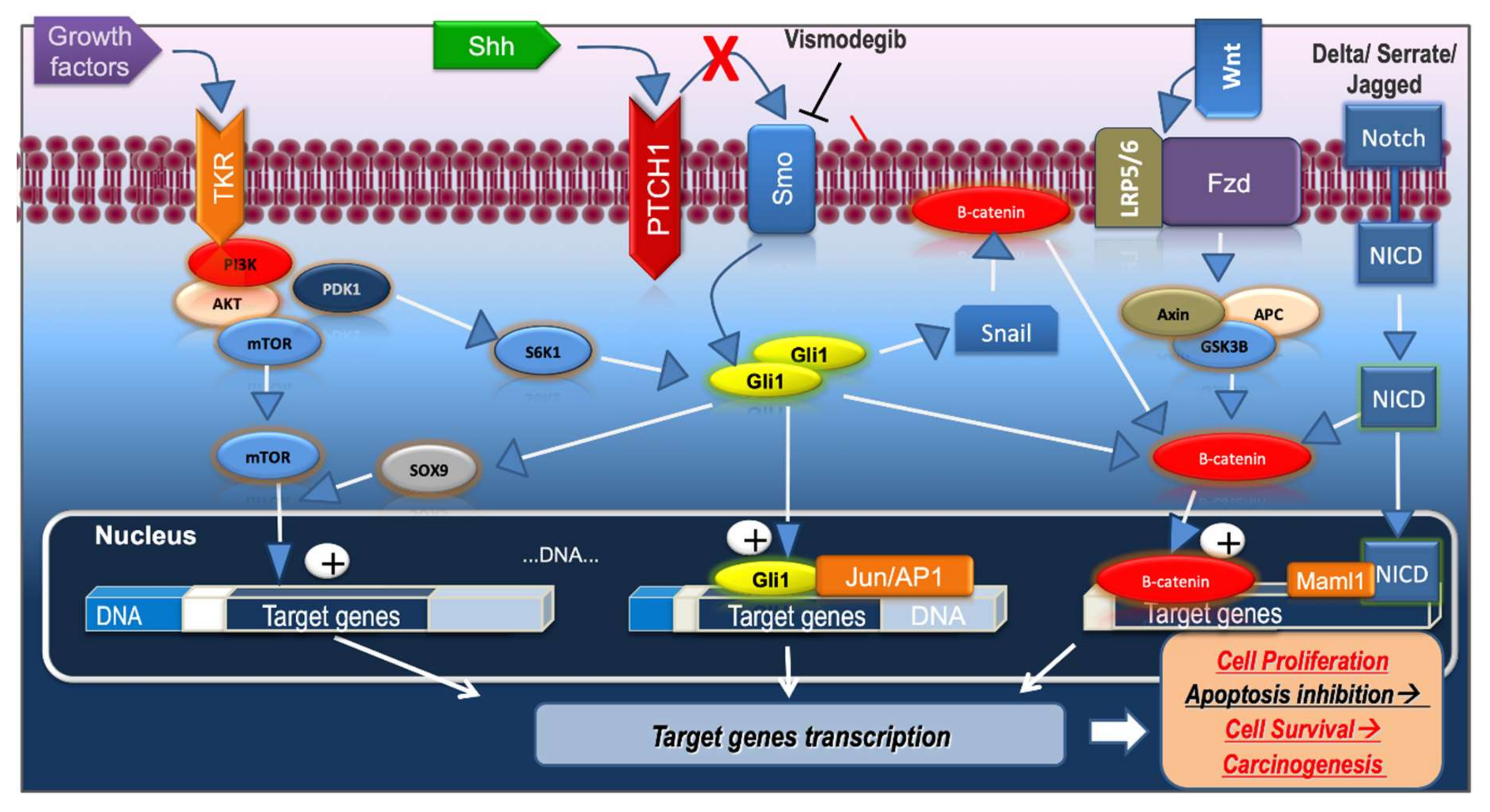
5. Crosstalk between Hh Signaling Pathway and Other Signaling Pathways in BCC
5.1. Wnt/β-Catenin Pathway
5.2. PI3K/AKT/mTOR Pathway
5.3. Hippo-YAP Pathway
5.4. EGFR Pathway
5.5. Vitamin D Pathway
5.6. P53 Pathway
5.7. Notch Pathway
6. Conclusions
Author Contributions
Funding
Conflicts of Interest
References
- Telfer, N.; Colver, G.; Morton, C. British Association of Dermatologists. Guidelines for the management of basal cell carcinoma. Br. J. Dermatol. 2008, 159, 35–48. [Google Scholar] [CrossRef] [PubMed]
- Ghita, M.A.; Caruntu, C.; Rosca, A.E.; Kaleshi, H.; Caruntu, A.; Moraru, L.; Docea, A.O.; Zurac, S.; Boda, D.; Neagu, M.; et al. Reflectance confocal microscopy and dermoscopy for in vivo, non-invasive skin imaging of superficial basal cell carcinoma. Oncol. Lett. 2016, 11, 3019–3024. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Tay, E.Y.-X.; Teoh, Y.-L.; Yeo, M.S.-W. Hedgehog Pathway Inhibitors and Their Utility in Basal Cell Carcinoma: A Comprehensive Review of Current Evidence. Dermatol. Ther. Heidelb. 2018, 9, 33–49. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Situm, M.; Buljan, M.; Bulat, V.; Lugović-Mihić, L.; Bolanča, Z.; Šimić, D. The role of UV radiation in the development of basal cell carcinoma. Coll. Antropol. 2008, 32, 167–170. [Google Scholar]
- Lupu, M.; Caruntu, C.; Popa, M.I.; Voiculescu, V.M.; Zurac, S.; Boda, D. Vascular patterns in basal cell carcinoma: Dermoscopic, confocal and histopathological perspectives (Review). Oncol. Lett. 2019, 17, 4112–4125. [Google Scholar] [CrossRef] [Green Version]
- Crowson, A.N. Basal cell carcinoma: Biology, morphology and clinical implications. Modern Pathol. 2006, 19, S127–S147. [Google Scholar] [CrossRef]
- Rubin, A.I.; Chen, E.H.; Ratner, D. Basal-Cell Carcinoma. N. Engl. J. Med. 2005, 353, 2262–2269. [Google Scholar] [CrossRef]
- Durmaz, C.D.; Evans, G.; Smith, M.J.; Ertop, P.; Akay, B.N.; Tuncalı, T. A Novel PTCH1 Frameshift Mutation Leading to Nevoid Basal Cell Carcinoma Syndrome. Cytogenet. Genome Res. 2018, 154, 57–61. [Google Scholar] [CrossRef] [Green Version]
- Almomani, R.; Khanfar, M.; Bodoor, K.; Al-Qarqaz, F.; Alqudah, M.; Hammouri, H.; Abu-Salah, A.; Haddad, Y.; Al Gargaz, W.; Mohaidat, Z. Evaluation of Patched-1 Protein Expression Level in Low Risk and High Risk Basal Cell Carcinoma Subtypes. Asian Pac. J. Cancer Prev. 2019, 20, 2851–2857. [Google Scholar] [CrossRef]
- Muzio, L.L. Nevoid basal cell carcinoma syndrome (Gorlin syndrome). Orphanet J. Rare Dis. 2008, 3, 32. [Google Scholar] [CrossRef] [Green Version]
- Narang, A.; Maheshwari, C.; Aggarwal, V.; Bansal, P.; Singh, P. Gorlin-Goltz Syndrome with Intracranial Meningioma: Case Report and Review of Literature. World Neurosurg. 2020, 133, 324–330. [Google Scholar] [CrossRef]
- Brinkhuizen, T.; Hurk, V.D.K.; Winnepenninckx, V.J.L.; De Hoon, J.P.; Van Marion, A.M.; Veeck, J.; Van Engeland, M.; Van Steensel, M.A.M. Epigenetic Changes in Basal Cell Carcinoma Affect SHH and WNT Signaling Components. PLoS ONE 2012, 7, e51710. [Google Scholar] [CrossRef]
- Montagna, E.; Lopes, O.S. Molecular Basis of Basal Cell Carcinoma. An. Bras. Dermatol. 2017, 92, 517–520. [Google Scholar] [CrossRef]
- Bonilla, X.; Parmentier, L.; King, B.; Bezrukov, F.; Kaya, G.; Zoete, V.; Seplyarskiy, V.B.; Sharpe, H.J.; McKee, T.; Letourneau, A.; et al. Genomic Analysis Identifies New Drivers and Progression Pathways in Skin Basal Cell Carcinoma. Nat. Genet. 2016, 48, 398–406. [Google Scholar] [CrossRef]
- Heller, E.R.; Gor, A.; Wang, D.; Hu, Q.; Lucchese, A.; Kanduc, D.; Katdare, M.; Liu, S.; Sinha, A.A. Molecular Signatures of Basal Cell Carcinoma Susceptibility and Pathogenesis: A Genomic Approach. Int. J. Oncol. 2013, 42, 583–596. [Google Scholar] [CrossRef]
- Jayaraman, S.S.; Rayhan, D.J.; Hazany, S.; Kolodney, M.S. Mutational Landscape of Basal Cell Carcinomas by Whole-Exome Sequencing. J. Investig. Dermatol. 2014, 134, 213–220. [Google Scholar] [CrossRef] [Green Version]
- Dai, J.; Lin, K.; Huang, Y.; Lu, Y.; Chen, W.-Q.; Zhang, X.-R.; He, B.-S.; Pan, Y.-Q.; Wang, S.-K.; Fan, W.-X. Identification of Critically Carcinogenesis-Related Genes in Basal Cell Carcinoma. OncoTargets Ther. 2018, 11, 6957–6967. [Google Scholar] [CrossRef] [Green Version]
- Sharpe, H.J.; Pau, G.; Dijkgraaf, G.J.; Basset-Séguin, N.; Modrusan, Z.; Januario, T.; Tsui, V.; Durham, A.B.; Dlugosz, A.A.; Haverty, P.M.; et al. Genomic Analysis of Smoothened Inhibitor Resistance in Basal Cell Carcinoma. Cancer Cell 2015, 27, 327–341. [Google Scholar] [CrossRef] [Green Version]
- Atwood, S.X.; Sarin, K.Y.; Whitson, R.J.; Li, J.R.; Kim, G.; Rezaee, M.; Ally, M.S.; Kim, J.; Yao, C.; Chang, A.L.S.; et al. Smoothened Variants Explain the Majority of Drug Resistance in Basal Cell Carcinoma. Cancer Cell 2015, 27, 342–353. [Google Scholar] [CrossRef] [Green Version]
- Sekulic, A.; Migden, M.R.; Oro, A.E.; Dirix, L.; Lewis, K.D.; Hainsworth, J.D.; Solomon, J.A.; Yoo, S.; Arron, S.T.; Friedlander, P.A.; et al. Efficacy and Safety of Vismodegib in Advanced Basal-Cell Carcinoma. N. Engl. J. Med. 2012, 366, 2171–2179. [Google Scholar] [CrossRef] [Green Version]
- Danial, C.; Sarin, K.Y.; Oro, A.E.; Chang, A.L.S. An Investigator-Initiated Open-Label Trial of Sonidegib in Advanced Basal Cell Carcinoma Patients Resistant to Vismodegib. Clin. Cancer Res. 2016, 22, 1325–1329. [Google Scholar] [CrossRef] [Green Version]
- Kim, D.J.; Kim, J.; Spaunhurst, K.; Montoya, J.; Khodosh, R.; Chandra, K.; Fu, T.; Gilliam, A.; Molgó, M.; Beachy, P.A.; et al. Open-Label, Exploratory Phase II Trial of Oral Itraconazole for the Treatment of Basal Cell Carcinoma. J. Clin. Oncol. 2014, 32, 745–751. [Google Scholar] [CrossRef]
- Siu, L.L.; Papadopoulos, K.; Alberts, S.R.; Kirchoff-Ross, R.; Vakkalagadda, B.; Lang, L.; Ahlers, L.M.; Bennett, K.L.; Van Tornout, J.M. A first-in-human, phase I study of an oral hedgehog (HH) pathway antagonist, BMS-833923 (XL139), in subjects with advanced or metastatic solid tumors. J. Clin. Oncol. 2019, 28, 2501. [Google Scholar] [CrossRef]
- Bendell, J.C.; Andre, V.; Ho, A.; Kudchadkar, R.; Migden, M.; Infante, J.; Tiu, R.V.; Pitou, C.; Tucker, T.; Brail, L.; et al. Phase I Study of LY2940680, a Smo Antagonist, in Patients with Advanced Cancer Including Treatment-Naïve and Previously Treated Basal Cell Carcinoma. Clin. Cancer Res. 2018, 24, 2082–2091. [Google Scholar] [CrossRef] [Green Version]
- Jimeno, A.; Weiss, G.J.; Miller, W.H.; Gettinger, S.; Eigl, B.J.C.; Chang, A.L.S.; Dunbar, J.; Devens, S.; Faia, K.; Skliris, G.; et al. Phase I Study of the Hedgehog Pathway Inhibitor IPI-926 in Adult Patients with Solid Tumors. Clin. Cancer Res. 2013, 19, 2766–2774. [Google Scholar] [CrossRef] [Green Version]
- Peukert, S.; He, F.; Dai, M.; Zhang, R.; Sun, Y.; Miller-Moslin, K.; McEwan, M.; Lagu, B.; Wang, K.; Yusuff, N.; et al. Discovery of NVP-LEQ506, a Second-Generation Inhibitor of Smoothened. Chem. Med. Chem. 2013, 8, 1261–1265. [Google Scholar] [CrossRef]
- Hassounah, N.B.; Bunch, T.A.; McDermott, K.M. Molecular Pathways: The Role of Primary Cilia in Cancer Progression and Therapeutics with a Focus on Hedgehog Signaling. Clin. Cancer Res. 2012, 18, 2429–2435. [Google Scholar] [CrossRef] [Green Version]
- Lauth, M.; Bergström, A.; Shimokawa, T.; Toftgård, R. Inhibition of GLI-Mediated Transcription and Tumor Cell Growth by Small-Molecule Antagonists. Proc. Natl. Acad. Sci. USA 2007, 104, 8455–8460. [Google Scholar] [CrossRef] [Green Version]
- Ally, M.S.; Ransohoff, K.; Sarin, K.Y.; Atwood, S.X.; Rezaee, M.; Bailey-Healy, I.; Kim, J.; Beachy, P.A.; Chang, A.L.S.; Oro, A.; et al. Effects of Combined Treatment With Arsenic Trioxide and Itraconazole in Patients With Refractory Metastatic Basal Cell Carcinoma. JAMA Dermatol. 2016, 152, 452–456. [Google Scholar] [CrossRef]
- Jacobsen, A.A.; Aldahan, A.S.; Hughes, O.B.; Shah, V.V.; Strasswimmer, J. Hedgehog Pathway Inhibitor Therapy for Locally Advanced and Metastatic Basal Cell Carcinoma. A Systematic Review and Pooled Analysis of Interventional Studies. JAMA Dermatol. 2016, 152, 816–824. [Google Scholar] [CrossRef] [Green Version]
- Basset-Séguin, N.; Sharpe, H.J.; De Sauvage, F.J. Efficacy of Hedgehog Pathway Inhibitors in Basal Cell Carcinoma. Mol. Cancer Ther. 2015, 14, 633–641. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Whitson, R.J.; Lee, A.; Urman, N.M.; Mirza, A.; Yao, C.Y.; Brown, A.S.; Li, J.R.; Shankar, G.; Fry, M.A.; Atwood, S.X.; et al. Non-Canonical Hedgehog Pathway Activation by MKL1/SRF Promotes Drug-Resistance in Basal Cell Carcinomas. Nat. Med. 2018, 24, 271–281. [Google Scholar] [CrossRef]
- Mahindroo, N.; Punchihewa, C.; Fujii, N. Hedgehog-Gli Signaling Pathway Inhibitors as Anticancer Agents. J. Med. Chem. 2009, 52, 3829–3845. [Google Scholar] [CrossRef] [Green Version]
- Zeng, X.; Ju, D. Hedgehog Signaling Pathway and Autophagy in Cancer. Int. J. Mol. Sci. 2018, 19, 2279. [Google Scholar] [CrossRef] [Green Version]
- Li, C.; Chi, S.; Xie, J. Hedgehog Signaling in Skin Cancers. Cell. Signal. 2011, 23, 1235–1243. [Google Scholar] [CrossRef] [Green Version]
- Sari, I.N.; Phi, L.T.H.; Jun, N.; Wijaya, Y.T.; Lee, S.; Kwon, H.Y. Hedgehog Signaling in Cancer: A Prospective Therapeutic Target for Eradicating Cancer Stem Cells. Cells 2018, 7, 208. [Google Scholar] [CrossRef] [Green Version]
- Gutzmer, R.; Solomon, J.A. Hedgehog Pathway Inhibition for the Treatment of Basal Cell Carcinoma. Target. Oncol. 2019, 14, 253–267. [Google Scholar] [CrossRef]
- Brennan, D.; Chen, X.; Cheng, L.; Mahoney, M.; Riobo, N.A. Noncanonical Hedgehog Signaling. Vitam. Horm. 2012, 88, 55–72. [Google Scholar] [CrossRef] [Green Version]
- Athar, M.; Li, C.; Kim, A.L.; Spiegelman, V.S.; Bickers, D.R. Sonic Hedgehog Signaling in Basal Cell Nevus Syndrome. Cancer Res. 2014, 74, 4967–4975. [Google Scholar] [CrossRef] [Green Version]
- Tang, J.Y. Elucidating the Role of Molecular Signaling Pathways in the Tumorigenesis of Basal Cell Carcinoma. Semin. Cutan. Med. Surg. 2011, 30, S6–S9. [Google Scholar] [CrossRef]
- Lupu, M.; Caruntu, C.; Ghita, M.A.; Voiculescu, V.; Voiculescu, S.; Rosca, A.E.; Caruntu, A.; Moraru, L.; Popa, I.M.; Calenic, B.; et al. Gene Expression and Proteome Analysis as Sources of Biomarkers in Basal Cell Carcinoma. Dis. Markers 2016, 2016, 1–9. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Otsuka, A.; Levesque, M.P.; Dummer, R.; Kabashima, K. Hedgehog Signaling in Basal Cell Carcinoma. J. Dermatol. Sci. 2015, 78, 95–100. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Bakshi, A.; Chaudhary, S.C.; Rana, M.; Elmets, C.A.; Athar, M. Basal Cell Carcinoma Pathogenesis and Therapy Involving Hedgehog Signaling and Beyond. Mol. Carcinog. 2017, 56, 2543–2557. [Google Scholar] [CrossRef]
- Kim, H.S.; Kim, Y.S.; Lee, C.; Shin, M.S.; Kim, J.W.; Jang, B.G. Expression Profile of Sonic Hedgehog Signaling-Related Molecules in Basal Cell Carcinoma. PLoS ONE 2019, 14, e0225511. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Teperino, R.; Aberger, F.; Esterbauer, H.; Riobó, N.; Pospisilik, J.A. Canonical and Non-Canonical Hedgehog Signalling and the Control of Metabolism. Semin. Cell Dev. Biol. 2014, 33, 81–92. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Omland, S.H. Local Immune Response in Cutaneous Basal Cell Carcinoma. Dan. Med. J. 2017, 64, B5412. [Google Scholar]
- Rangwala, S.; Tsai, K.Y. Roles of the Immune System in Skin Cancer. Br. J. Dermatol. 2011, 165, 953–965. [Google Scholar] [CrossRef]
- Kaporis, H.G.; Guttman-Yassky, E.; Lowes, M.A.; Haider, A.S.; Fuentes-Duculan, J.; Darabi, K.; Whynot-Ertelt, J.; Khatcherian, A.; Cardinale, I.; Novitskaya, I.; et al. Human Basal Cell Carcinoma Is Associated with Foxp3+ T cells in a Th2 Dominant Microenvironment. J. Investig. Dermatol. 2007, 127, 2391–2398. [Google Scholar] [CrossRef] [Green Version]
- Omland, S.H.; Nielsen, P.S.; Gjerdrum, L.M.R.; Gniadecki, R. Immunosuppressive Environment in Basal Cell Carcinoma: The Role of Regulatory T Cells. Acta Derm. Venereol. 2016, 96, 917–921. [Google Scholar] [CrossRef] [Green Version]
- Georgescu, S.R.; Tampa, M.; Mitran, C.I.; Mitran, M.I.; Caruntu, C.; Caruntu, A.; Lupu, M.; Matei, C.; Constantin, C.; Neagu, M. Tumour Microenvironment in Skin Carcinogenesis. Adv. Exp. Med. Biol. 2020, 1226, 123–142. [Google Scholar] [CrossRef]
- Nomikos, K.; Lampri, E.; Spyridonos, P.; Bassukas, I.D. Alterations in the Inflammatory Cells Infiltrating Basal Cell Carcinomas during Immunocryosurgery. Arch. Dermatol. Res. 2019, 311, 499–504. [Google Scholar] [CrossRef]
- Hall, E.T.; Fernandez-Lopez, E.; Silk, A.W.; Dummer, R.; Bhatia, S. Immunologic Characteristics of Nonmelanoma Skin Cancers: Implications for Immunotherapy. Am. Soc. Clin. Oncol. Educ. Book 2020, 40, 398–407. [Google Scholar] [CrossRef]
- Pellegrini, C.; Orlandi, A.; Costanza, G.; Di Stefani, A.; Piccioni, A.; Di Cesare, A.; Chiricozzi, A.; Ferlosio, A.; Peris, K.; Fargnoli, M.C. Expression of IL-23/Th17-Related Cytokines in Basal Cell Carcinoma and in the Response to Medical Treatments. PLoS ONE 2017, 12, e0183415. [Google Scholar] [CrossRef]
- Grund-Groeschke, S.; Stockmaier, G.; Aberger, F. Hedgehog/GLI Signaling in Tumor Immunity - New Therapeutic Opportunities and Clinical Implications. Cell Commun. Signal. 2019, 17, 172. [Google Scholar] [CrossRef] [Green Version]
- Otsuka, A.; Dreier, J.; Cheng, P.F.; Nägeli, M.; Lehmann, H.; Felderer, L.; Frew, I.J.; Matsushita, S.; Levesque, M.P.; Dummer, R. Hedgehog Pathway Inhibitors Promote Adaptive Immune Responses in Basal Cell Carcinoma. Clin. Cancer Res. 2015, 21, 1289–1297. [Google Scholar] [CrossRef] [Green Version]
- Okada, F. Inflammation-Related Carcinogenesis: Current Findings in Epidemiological Trends, Causes and Mechanisms. Yonago Acta Med. 2014, 57, 65–72. [Google Scholar]
- Georgescu, S.R.; Mitran, C.I.; Mitran, M.I.; Caruntu, C.; Sarbu, M.I.; Matei, C.; Nicolae, I.; Tocut, S.M.; Popa, M.I.; Tampa, M. New Insights in the Pathogenesis of HPV Infection and the Associated Carcinogenic Processes: The Role of Chronic Inflammation and Oxidative Stress. J. Immunol. Res. 2018, 2018, 5315816. [Google Scholar] [CrossRef] [Green Version]
- Surcel, M.; Constantin, C.; Caruntu, C.; Zurac, S.; Neagu, M. Inflammatory Cytokine Pattern Is Sex-Dependent in Mouse Cutaneous Melanoma Experimental Model. J. Immunol. Res. 2017, 2017, 9212134. [Google Scholar] [CrossRef]
- Multhoff, G.; Molls, M.; Radons, J. Chronic Inflammation in Cancer Development. Front. Immunol. 2012, 2, 98. [Google Scholar] [CrossRef] [Green Version]
- Tampa, M.; Mitran, M.I.; Mitran, C.I.; Sarbu, I.; Matei, C.; Nicolae, I.; Caruntu, A.; Tocut, S.M.; Popa, M.I.; Caruntu, C.; et al. Mediators of Inflammation—A Potential Source of Biomarkers in Oral Squamous Cell Carcinoma. J. Immunol. Res. 2018, 2018, 1061780. [Google Scholar] [CrossRef] [Green Version]
- Sternberg, C.; Gruber, W.; Eberl, M.; Tesanovic, S.; Stadler, M.; Elmer, D.P.; Schlederer, M.; Grund, S.; Roos, S.; Wolff, F.; et al. Synergistic Cross-Talk of Hedgehog and Interleukin-6 Signaling Drives Growth of Basal Cell Carcinoma. Int. J. Cancer 2018, 143, 2943–2954. [Google Scholar] [CrossRef] [Green Version]
- Piérard-Franchimont, C.; Hermanns-Lê, T.; Paquet, P.; Herfs, M.; Delvenne, P.; Piérard, G.E. Hedgehog- and MTOR-Targeted Therapies for Advanced Basal Cell Carcinomas. Future Oncol. 2015, 11, 2997–3002. [Google Scholar] [CrossRef]
- Li, J.; Ji, L.; Chen, J.; Zhang, W.; Ye, Z. Wnt/β-Catenin Signaling Pathway in Skin Carcinogenesis and Therapy. Biomed. Res. Int. 2015, 2015, 964842. [Google Scholar] [CrossRef] [Green Version]
- Noubissi, F.K.; Yedjou, C.G.; Spiegelman, V.S.; Tchounwou, P.B. Cross-Talk between Wnt and Hh Signaling Pathways in the Pathology of Basal Cell Carcinoma. Int. J. Environ. Res. Public Health 2018, 15, 1442. [Google Scholar] [CrossRef] [Green Version]
- Pelullo, M.; Zema, S.; Nardozza, F.; Checquolo, S.; Screpanti, I.; Bellavia, D. Wnt, Notch, and TGF-β Pathways Impinge on Hedgehog Signaling Complexity: An Open Window on Cancer. Front. Genet. 2019, 10, 711. [Google Scholar] [CrossRef] [Green Version]
- Ding, M.; Wang, X. Antagonism between Hedgehog and Wnt Signaling Pathways Regulates Tumorigenicity (Review). Oncol. Lett. 2017, 14, 6327–6333. [Google Scholar] [CrossRef] [Green Version]
- Noubissi, F.K.; Kim, T.; Kawahara, T.N.; Aughenbaugh, W.D.; Berg, E.; Longley, B.J.; Athar, M.; Spiegelman, V.S. Role of CRD-BP in the Growth of Human Basal Cell Carcinoma Cells. J. Investig. Dermatol. 2014, 134, 1718–1724. [Google Scholar] [CrossRef] [Green Version]
- Li, X.; Deng, W.; Lobo-Ruppert, S.; Ruppert, J. Gli1 Acts through Snail and E-Cadherin to Promote Nuclear Signaling by β-Catenin. Oncogene 2007, 26, 4489–4498. [Google Scholar] [CrossRef] [Green Version]
- Lang, C.M.R.; Chan, C.-K.; Veltri, A.; Lien, W.-H. Wnt Signaling Pathways in Keratinocyte Carcinomas. Cancers Basel 2019, 11, 1216. [Google Scholar] [CrossRef] [Green Version]
- Carmo, N.G.D.; Sakamoto, L.H.T.; Pogue, R.; Mascarenhas, C.D.C.; Passos, S.K.; Felipe, M.S.S.; Andrade, R.V.D. Altered Expression of PRKX, WNT3 and WNT16 in Human Nodular Basal Cell Carcinoma. Anticancer Res. 2016, 36, 4545–4552. [Google Scholar] [CrossRef] [Green Version]
- Gerson, S.L.; Caimi, P.F.; William, B.F.; Creger, R.J. Pharmacology and Molecular Mechanisms of Antineoplastic Agents for Hematologic Malignancies. Hematology 2018, 57, 849–912. [Google Scholar] [CrossRef]
- Karayannopoulou, G.; Euvrard, S.; Kanitakis, J. Differential Expression of P-MTOR in Cutaneous Basal and Squamous Cell Carcinomas Likely Explains Their Different Response to MTOR Inhibitors in Organ-Transplant Recipients. Anticancer Res. 2013, 33, 3711–3714. [Google Scholar]
- Pópulo, H.; Lopes, J.M.; Soares, P. The MTOR Signalling Pathway in Human Cancer. Int. J. Mol. Sci. 2012, 13, 1886–1918. [Google Scholar] [CrossRef]
- Fruman, D.A.; Chiu, H.; Hopkins, B.D.; Bagrodia, S.; Cantley, L.C.; Abraham, R.T. The PI3K Pathway in Human Disease. Cell 2017, 170, 605–635. [Google Scholar] [CrossRef] [Green Version]
- Chamcheu, J.C.; Roy, T.; Uddin, M.B.; Banang-Mbeumi, S.; Chamcheu, R.-C.N.; Walker, A.L.; Liu, Y.-Y.; Huang, S. Role and Therapeutic Targeting of the PI3K/Akt/mTOR Signaling Pathway in Skin Cancer: A Review of Current Status and Future Trends on Natural and Synthetic Agents Therapy. Cells 2019, 8, 803. [Google Scholar] [CrossRef] [Green Version]
- Kim, A.L.; Back, J.H.; Chaudhary, S.C.; Zhu, Y.; Athar, M.; Bickers, D.R. SOX9 Transcriptionally Regulates mTOR-Induced Proliferation of Basal Cell Carcinomas. J. Investig. Dermatol. 2018, 138, 1716–1725. [Google Scholar] [CrossRef] [Green Version]
- Eibenschutz, L.; Colombo, D.; Catricalà, C. Everolimus for Compassionate Use in Multiple Basal Cell Carcinomas. Case Rep. Dermatol. Med. 2013, 2013. [Google Scholar] [CrossRef] [Green Version]
- Atwood, S.X.; Whitson, R.J.; Oro, A.E. Advanced Treatment for Basal Cell Carcinomas. Cold Spring Harb. Perspect. Med. 2014, 4. [Google Scholar] [CrossRef]
- Miranda, M.M.; Lowry, W.E. Hip to the Game: YAP/TAZ Is Required for Nonmelanoma Skin Cancers. EMBO J. 2018, 37, e99921. [Google Scholar] [CrossRef]
- Schlegelmilch, K.; Mohseni, M.; Kirak, O.; Pruszak, J.; Rodriguez, J.R.; Zhou, D.; Kreger, B.T.; Vasioukhin, V.; Avruch, J.; Brummelkamp, T.R.; et al. Yap1 Acts Downstream of α-Catenin to Control Epidermal Proliferation. Cell 2011, 144, 782–795. [Google Scholar] [CrossRef] [Green Version]
- Debaugnies, M.; Sánchez-Danés, A.; Rorive, S.; Raphaël, M.; Liagre, M.; Parent, M.-A.; Brisebarre, A.; Salmon, I.; Blanpain, C. YAP and TAZ Are Essential for Basal and Squamous Cell Carcinoma Initiation. EMBO Rep. 2018, 19, e45809. [Google Scholar] [CrossRef]
- Maglic, D.; Schlegelmilch, K.; Dost, A.F.; Panero, R.; Dill, M.T.; Calogero, R.A.; Camargo, F.D. YAP-TEAD Signaling Promotes Basal Cell Carcinoma Development via a c-JUN/AP1 Axis. EMBO J. 2018, 37, e98642. [Google Scholar] [CrossRef]
- Akladios, B.; Reinoso, V.M.; Cain, J.E.; Wang, T.; Lambie, D.L.; Watkins, D.N.; Beverdam, A. Positive Regulatory Interactions between YAP and Hedgehog Signalling in Skin Homeostasis and BCC Development in Mouse Skin in Vivo. PLoS ONE 2017, 12, e0183178. [Google Scholar] [CrossRef] [Green Version]
- Sasaki, T.; Hiroki, K.; Yamashita, Y. The Role of Epidermal Growth Factor Receptor in Cancer Metastasis and Microenvironment. Biomed. Res. Int. 2013, 2013, 546318. [Google Scholar] [CrossRef] [Green Version]
- Florescu, D.E.; Stepan, A.E.; Mărgăritescu, C.; Ciurea, R.N.; Stepan, M.D.; Simionescu, C.E. The Involvement of EGFR, HER2 and HER3 in the Basal Cell Carcinomas Aggressiveness. Rom. J. Morphol. Embryol. 2018, 59, 479–484. [Google Scholar]
- Wieduwilt, M.J.; Moasser, M.M. The Epidermal Growth Factor Receptor Family: Biology Driving Targeted Therapeutics. Cell. Mol. Life Sci. 2008, 65, 1566–1584. [Google Scholar] [CrossRef] [Green Version]
- Willmore-Payne, C.; Holden, J.A.; Layfield, L.J. Detection of EGFR- and HER2-Activating Mutations in Squamous Cell Carcinoma Involving the Head and Neck. Mod. Pathol. 2006, 19, 634–640. [Google Scholar] [CrossRef] [Green Version]
- Avci, C.B.; Kaya, I.; Ozturk, A.; Ay, N.P.O.; Sezgin, B.; Kurt, C.C.; Akyildiz, N.S.; Bozan, A.; Yaman, B.; Akalin, T.; et al. The Role of EGFR Overexpression on the Recurrence of Basal Cell Carcinomas with Positive Surgical Margins. Gene 2019, 687, 35–38. [Google Scholar] [CrossRef]
- Eberl, M.; Klingler, S.; Mangelberger, D.; Loipetzberger, A.; Damhofer, H.; Zoidl, K.; Schnidar, H.; Hache, H.; Bauer, H.-C.; Solca, F.; et al. Hedgehog-EGFR Cooperation Response Genes Determine the Oncogenic Phenotype of Basal Cell Carcinoma and Tumour-Initiating Pancreatic Cancer Cells. EMBO Mol. Med. 2012, 4, 218–233. [Google Scholar] [CrossRef]
- Schnidar, H.; Eberl, M.; Klingler, S.; Mangelberger, R.; Kasper, M.; Hauser-Kronberger, C.; Regl, G.; Kroismayr, R.; Moriggl, R.; Sibilia, M.; et al. Epidermal Growth Factor Receptor Signaling Synergizes with Hedgehog/GLI in Oncogenic Transformation via Activation of the MEK/ERK/JUN Pathway. Cancer Res. 2009, 69, 1284–1292. [Google Scholar] [CrossRef] [Green Version]
- Scarpati, D.V.G.; Perri, F.; Pisconti, S.; Costa, G.; Ricciardiello, F.; Del Prete, S.; Napolitano, A.; Carraturo, M.; Mazzone, S.; Addeo, R. Concomitant Cetuximab and Radiation Therapy: A Possible Promising Strategy for Locally Advanced Inoperable Non-Melanoma Skin Carcinomas. Mol. Clin. Oncol. 2016, 4, 467–471. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Reddy, K.K. Vitamin D Level and Basal Cell Carcinoma, Squamous Cell Carcinoma, and Melanoma Risk. J. Investig. Dermatol. 2013, 133, 589–592. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Neagu, M.; Constantin, C.; Caruntu, C.; Dumitru, C.; Surcel, M.; Zurac, S. Inflammation: A Key Process in Skin Tumorigenesis. Oncol. Lett. 2019, 17, 4068–4084. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Bikle, D.D.; Christakos, S. New Aspects of Vitamin D Metabolism and Action—Addressing the Skin as Source and Target. Nat. Rev. Endocrinol. 2020, 16, 234–252. [Google Scholar] [CrossRef] [PubMed]
- Teichert, A.; Elalieh, H.; Elias, P.; Welsh, J.; Bikle, D.D. Over-Expression of Hedgehog Signaling Is Associated with Epidermal Tumor Formation in Vitamin D Receptor Null Mice. J. Investig. Dermatol. 2011, 131, 2289–2297. [Google Scholar] [CrossRef] [Green Version]
- Linder, B.; Weber, S.; Dittmann, K.; Adamski, J.; Hahn, H.; Uhmann, A. A Functional and Putative Physiological Role of Calcitriol in Patched1/Smoothened Interaction. J. Biol. Chem. 2015, 290, 19614–19628. [Google Scholar] [CrossRef] [Green Version]
- Uhmann, A.; Niemann, H.; Lammering, B.; Henkel, C.; Hess, I.; Nitzki, F.; Fritsch, A.; Prüfer, N.; Rosenberger, A.; Dullin, C.; et al. Antitumoral Effects of Calcitriol in Basal Cell Carcinomas Involve Inhibition of Hedgehog Signaling and Induction of Vitamin D Receptor Signaling and Differentiation. Mol. Cancer Ther. 2011, 10, 2179–2188. [Google Scholar] [CrossRef] [Green Version]
- Albert, B.; Hahn, H. Interaction of Hedgehog and Vitamin D Signaling Pathways in Basal Cell Carcinomas. Adv. Exp. Med. Biol. 2014, 810, 329–341. [Google Scholar] [CrossRef]
- Brinkhuizen, T.; Frencken, K.J.A.; Nelemans, P.J.; Hoff, M.L.S.; Kelleners-Smeets, N.W.J.; Hausen, A.Z.; Van Der Horst, M.P.J.; Rennspiess, D.; Winnepenninckx, V.J.L.; Van Steensel, M.A.M.; et al. The Effect of Topical Diclofenac 3% and Calcitriol 3 Μg/g on Superficial Basal Cell Carcinoma (SBCC) and Nodular Basal Cell Carcinoma (NBCC): A Phase II, Randomized Controlled Trial. J. Am. Acad. Dermatol. 2016, 75, 126–134. [Google Scholar] [CrossRef] [Green Version]
- Shea, C.R.; McNutt, N.S.; Volkenandt, M.; Lugo, J.; Prioleau, P.G.; Albino, A.P. Overexpression of P53 Protein in Basal Cell Carcinomas of Human Skin. Am. J. Pathol. 1992, 141, 25–29. [Google Scholar]
- Golubovskaya, V.M.; Cance, W.G. Targeting the P53 Pathway. Surg. Oncol. Clin. N. Am. 2013, 22, 747–764. [Google Scholar] [CrossRef] [Green Version]
- Mandinova, A.; Lee, S.W. The p53 Pathway as a Target in Cancer Therapeutics: Obstacles and Promise. Sci. Transl. Med. 2011, 3, 64rv1. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Oh, S.-T.; Stark, A.; Reichrath, J. The P53 Signalling Pathway in Cutaneous Basal Cell Carcinoma: An Immunohistochemical Description. Acta Derm. Venereol. 2020, 100, adv00098. [Google Scholar] [CrossRef]
- Tampa, M.; Caruntu, C.; Mitran, M.; Mitran, C.; Sarbu, I.; Rusu, L.-C.; Matei, C.; Constantin, C.; Neagu, M.; Georgescu, S.-R. Markers of Oral Lichen Planus Malignant Transformation. Dis. Markers 2018, 2018, 1959506. [Google Scholar] [CrossRef] [Green Version]
- Wang, G.Y.; Wood, C.N.; Dolorito, J.A.; Libove, E.; Epstein, E.H. Differing Tumor-Suppressor Functions of Arf and P53 in Murine Basal Cell Carcinoma Initiation and Progression. Oncogene 2017, 36, 3772–3780. [Google Scholar] [CrossRef]
- Matheu, A.; Maraver, A.; Serrano, M. The Arf/p53 Pathway in Cancer and Aging. Cancer Res. 2008, 68, 6031–6034. [Google Scholar] [CrossRef] [Green Version]
- Li, Z.J.; Mack, S.C.; Mak, T.H.; Angers, S.; Taylor, M.D.; Hui, C.-C. Evasion of P53 and G2/M Checkpoints Are Characteristic of Hh-Driven Basal Cell Carcinoma. Oncogene 2014, 33, 2674–2680. [Google Scholar] [CrossRef] [Green Version]
- Huang, S.-W.; Chang, S.-H.; Mu, S.-W.; Jiang, H.-Y.; Wang, S.-T.; Kao, J.-K.; Huang, J.-L.; Wu, C.-Y.; Chen, Y.-J.; Shieh, J.-J. Imiquimod Activates P53-Dependent Apoptosis in a Human Basal Cell Carcinoma Cell Line. J. Dermatol. Sci. 2016, 81, 182–191. [Google Scholar] [CrossRef]
- Nowell, C.; Radtke, F. Cutaneous Notch Signaling in Health and Disease. Cold Spring Harb. Perspect. Med. 2013, 3, a017772. [Google Scholar] [CrossRef] [Green Version]
- D’Souza, B.; Meloty-Kapella, L.; Weinmaster, G. Canonical and Non-Canonical Notch Ligands. Curr. Top. Dev. Biol. 2010, 92, 73–129. [Google Scholar]
- Eberl, M.; Mangelberger, R.; Swanson, J.B.; Verhaegen, M.E.; Harms, P.W.; Frohm, M.L.; Dlugosz, A.A.; Wong, S.Y. Tumor Architecture and Notch Signaling Modulate Drug Response in Basal Cell Carcinoma. Cancer Cell 2018, 33, 229–243. [Google Scholar] [CrossRef]
- Shi, F.-T.; Yu, M.; Zloty, D.; Bell, R.H.; Wang, E.; Akhoundsadegh, N.; Leung, G.; Haegert, A.; Carr, N.; Shapiro, J.; et al. Notch Signaling Is Significantly Suppressed in Basal Cell Carcinomas and Activation Induces Basal Cell Carcinoma Cell Apoptosis. Mol. Med. Rep. 2017, 15, 1441–1454. [Google Scholar] [CrossRef] [Green Version]
- Thompson, M.; Nejak-Bowen, K.; Monga, S.P.S. Crosstalk of the Wnt Signaling Pathway. In Targeting the Wnt Pathway in Cancer; Goss, K.H., Kahn, M., Eds.; Springer: New York, NY, USA, 2011; pp. 51–80. [Google Scholar] [CrossRef]
| Target | Therapy Molecule | Reference |
|---|---|---|
| SMO | Vismodegib * | Sekulic et al. [20] |
| SMO | Sonidegib ** | Danial et al. [21] |
| SMO | Itraconazole | Kim et al. [22] |
| SMO | BMS-833923 | Siu et al. [23] |
| SMO | Taladegib | Bendell et al. [24] |
| SMO | Patidegib | Jimeno et al. [25] |
| SMO | NVP-LQ506 | Peukert et al. [26] |
| SHH | Robotnikinin | Hassounah et al. [27] |
| GLI | GANT-58 and GANT-61 | Lauth et al. [28] |
| GLI | Arsenic trioxide | Ally et al. [29] |
© 2020 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Tampa, M.; Georgescu, S.R.; Mitran, C.I.; Mitran, M.I.; Matei, C.; Scheau, C.; Constantin, C.; Neagu, M. Recent Advances in Signaling Pathways Comprehension as Carcinogenesis Triggers in Basal Cell Carcinoma. J. Clin. Med. 2020, 9, 3010. https://doi.org/10.3390/jcm9093010
Tampa M, Georgescu SR, Mitran CI, Mitran MI, Matei C, Scheau C, Constantin C, Neagu M. Recent Advances in Signaling Pathways Comprehension as Carcinogenesis Triggers in Basal Cell Carcinoma. Journal of Clinical Medicine. 2020; 9(9):3010. https://doi.org/10.3390/jcm9093010
Chicago/Turabian StyleTampa, Mircea, Simona Roxana Georgescu, Cristina Iulia Mitran, Madalina Irina Mitran, Clara Matei, Cristian Scheau, Carolina Constantin, and Monica Neagu. 2020. "Recent Advances in Signaling Pathways Comprehension as Carcinogenesis Triggers in Basal Cell Carcinoma" Journal of Clinical Medicine 9, no. 9: 3010. https://doi.org/10.3390/jcm9093010
APA StyleTampa, M., Georgescu, S. R., Mitran, C. I., Mitran, M. I., Matei, C., Scheau, C., Constantin, C., & Neagu, M. (2020). Recent Advances in Signaling Pathways Comprehension as Carcinogenesis Triggers in Basal Cell Carcinoma. Journal of Clinical Medicine, 9(9), 3010. https://doi.org/10.3390/jcm9093010










