Survivorship in Colorectal Cancer: A Cohort Study of the Patterns and Documented Content of Follow-Up Visits
Abstract
:1. Introduction
2. Methods
2.1. Participants
2.2. Period of Follow-Up
2.3. Data Collection and Handling
2.4. Statistical Considerations
3. Results
3.1. Participants
3.2. Survivor Characteristics
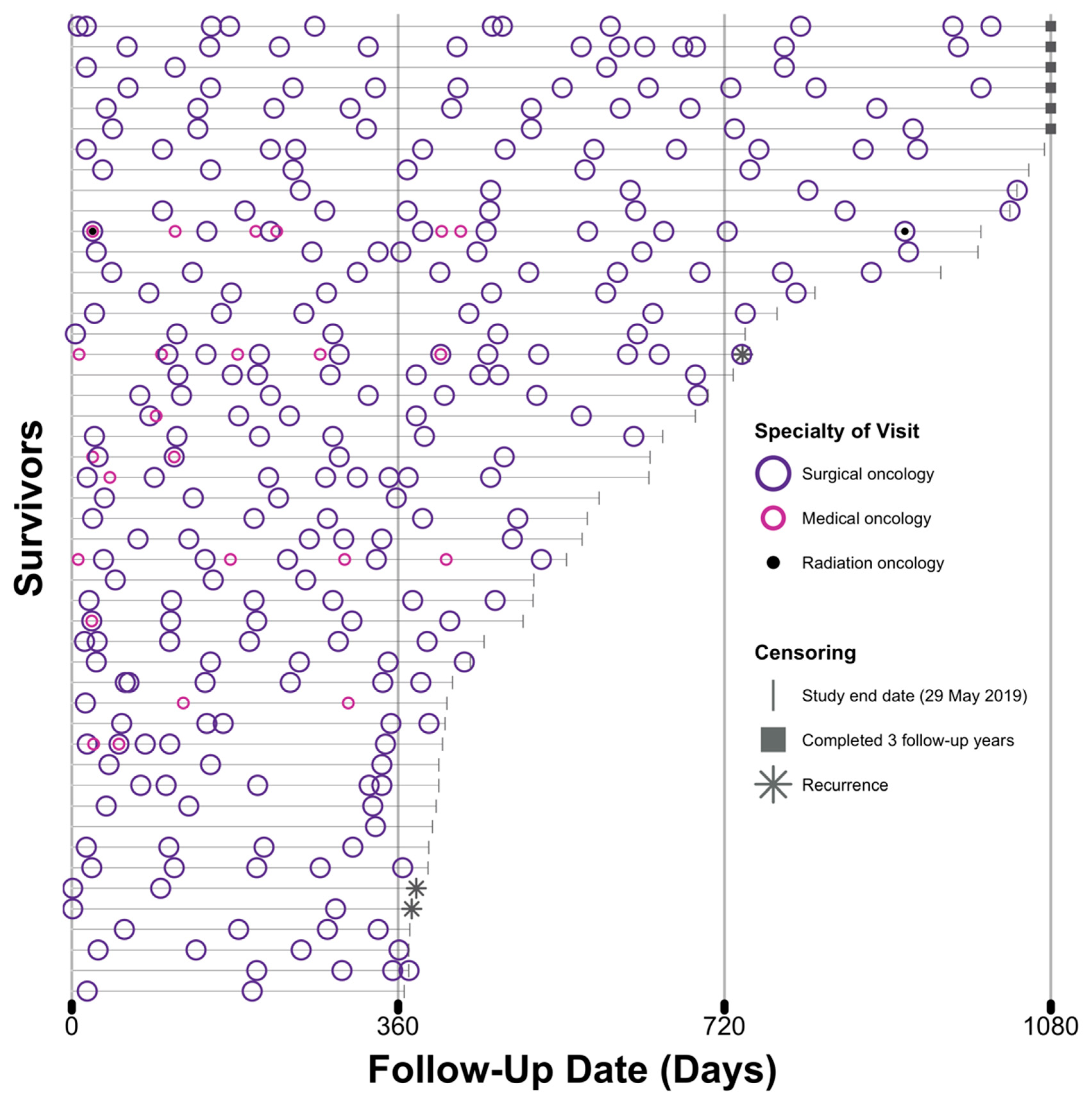
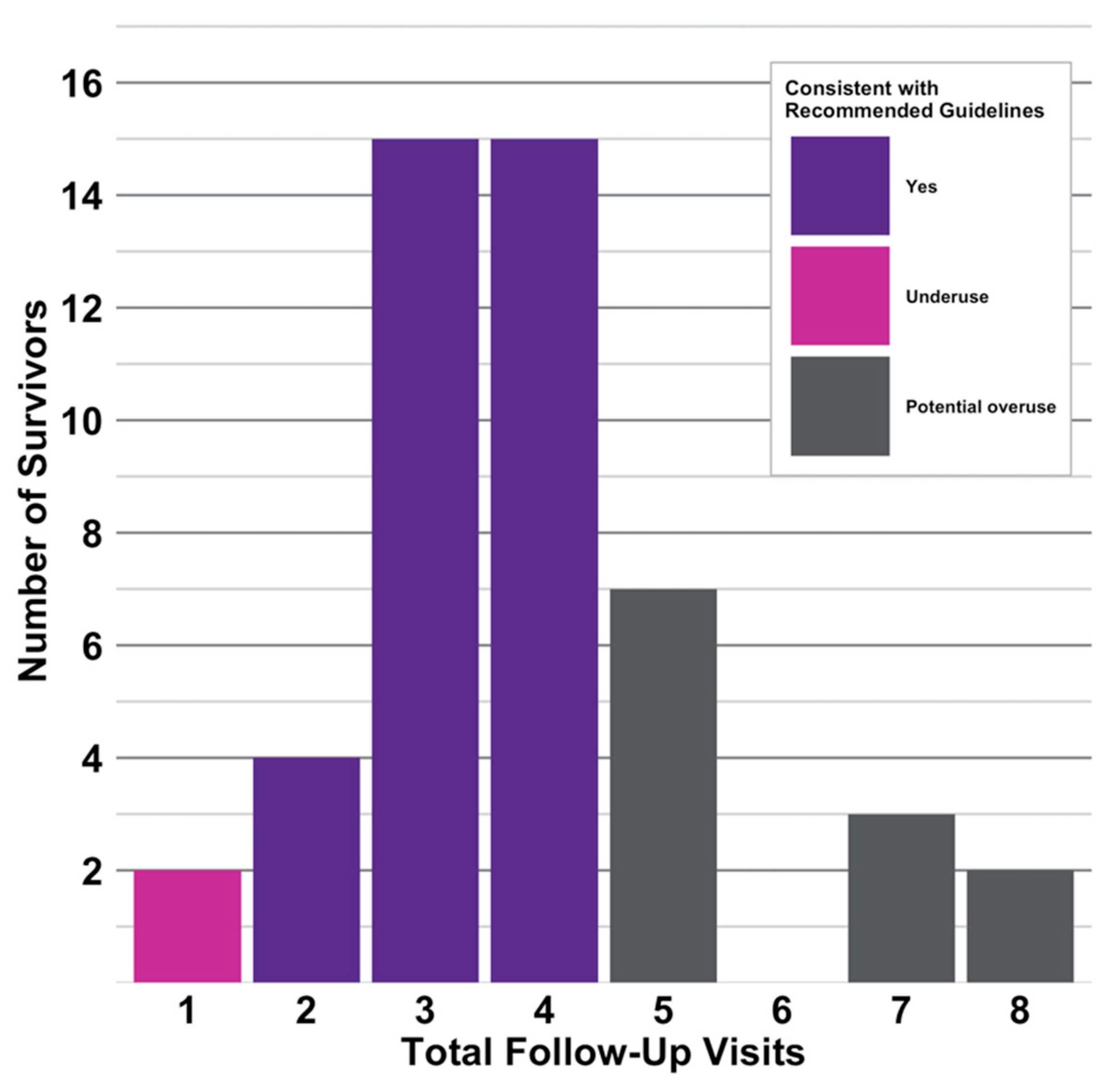
3.3. Patterns of Follow-Up Visits
3.3.1. Patterns of Follow-Up Visits in the First Year
3.3.2. Patterns of Follow-Up Visits in the Second Year
3.3.3. Patterns of Follow-Up Visits in the Third Year
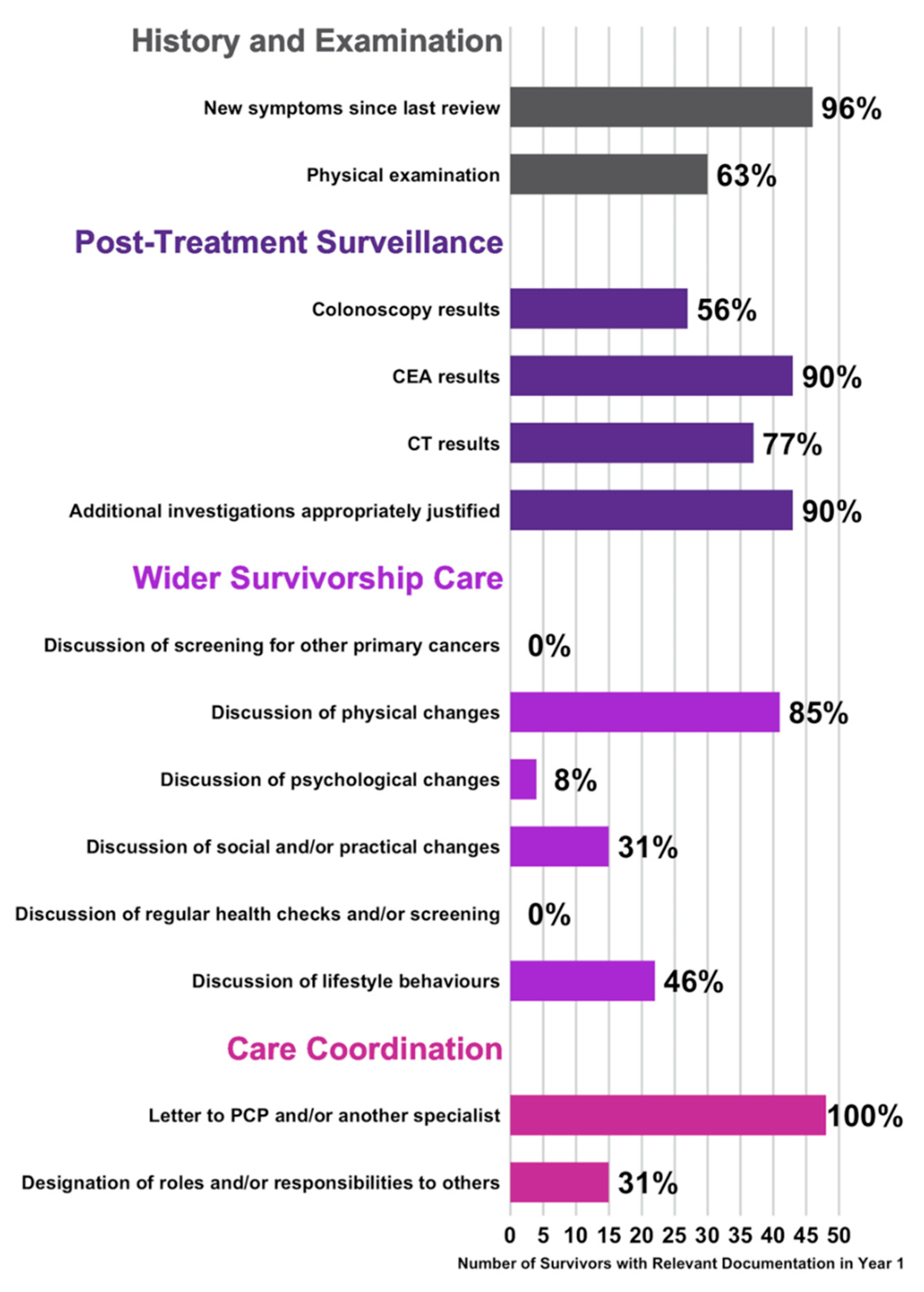
3.4. Documented Content of Follow-Up Visits in the First Year
4. Discussion
Strengths and Limitations
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Acknowledgments
Conflicts of Interest
References
- Australian Institute of Health and Welfare. Cancer data in Australia. Cat. No. Can 122. Available online: https://www.aihw.gov.au/reports/cancer/cancer-data-in-australia (accessed on 30 June 2020).
- Australian Institute of Health and Welfare. Cancer in Australia 2019. Cancer Series no.119. Cat. No. Can 123; AIHW: Canberra, Astralia, 2019. [Google Scholar]
- Chang, G.J.; Kopetz, S. Coordination of care in colon cancer. Cancer 2015, 121, 3201–3202. [Google Scholar] [CrossRef] [PubMed]
- Miller, K.D.; Nogueira, L.; Mariotto, A.B.; Rowland, J.H.; Yabroff, K.R.; Alfano, C.M.; Jemal, A.; Kramer, J.L.; Siegel, R.L. Cancer treatment and survivorship statistics. CA Cancer J. Clin. 2019, 69, 363–385. [Google Scholar]
- Institute of Medicine; National Research Council. From Cancer Patient to Cancer Survivor: Lost in Transition; The National Academies Press: Washington, DC, USA, 2006; p. 534. [Google Scholar]
- Nekhlyudov, L.; Mollica, M.A.; Jacobsen, P.B.; Mayer, D.K.; Shulman, L.N.; Geiger, A.M. Developing a quality of cancer survivorship care framework: Implications for clinical care, research and policy. J. Natl. Cancer Inst. 2019, 111, 1120–1130. [Google Scholar] [CrossRef] [Green Version]
- Jacobs, L.A.; Shulman, L.N. Follow-up care of cancer survivors: Challenges and solutions. Lancet Oncol. 2017, 18, e19–e29. [Google Scholar] [CrossRef]
- El-Shami, K.; Oeffinger, K.C.; Erb, N.L.; Willis, A.; Bretsch, J.K.; Pratt-Chapman, M.L.; Cannady, R.S.; Wong, S.L.; Rose, J.; Barbour, A.L.; et al. American cancer society colorectal cancer survivorship care guidelines. CA Cancer J. Clin. 2015, 65, 428–455. [Google Scholar] [CrossRef]
- University of Texas MD Anderson Cancer Center. Cancer Survivorship Algorithms: Colon Cancer. Available online: https://www.mdanderson.org/content/dam/mdanderson/documents/for-physicians/algorithms/survivorship/survivorship-colon-web-algorithm.pdf (accessed on 4 April 2019).
- University of Texas MD Anderson Cancer Center. Cancer Survivorship Algorithms: Rectal Cancer. Available online: https://www.mdanderson.org/content/dam/mdanderson/documents/for-physicians/algorithms/survivorship/survivorship-rectal-web-algorithm.pdf (accessed on 4 April 2019).
- Members of the Colorectal Cancer Survivorship Group. Follow-Up Care, Surveillance Protocol, and Secondary Prevention Measures for Survivors of Colorectal Rancer; Cancer Care Ontario: Toronto, ON, Canada, 2012. [Google Scholar]
- Leong, K.; Hartley, J.; Karandikar, S. Association of coloproctology of great britain & ireland (ACPGBI): Guidelines for the management of cancer of the colon, rectum and anus-follow up, lifestyle and survivorship. Colorectal Dis. 2017, 19, 67–70. [Google Scholar]
- Cancer Council Australia Colorectal Cancer Guidelines Working Party. Clinical Practice Guidelines for the Prevention, Early Detection and Management of Colorectal Cancer. Available online: https://wiki.cancer.org.au/australia/Guidelines:Colorectal_cancer (accessed on 6 April 2019).
- Meyerhardt, J.A.; Mangu, P.B.; Flynn, P.J.; Korde, L.; Loprinzi, C.L.; Minsky, B.D.; Petrelli, N.J.; Ryan, K.; Schrag, D.H.; Wong, S.L.; et al. Follow-up care, surveillance protocol, and secondary prevention measures for survivors of colorectal cancer: American society of clinical oncology clinical practice guideline endorsement. J. Clin. Oncol. 2013, 31, 4465–4470. [Google Scholar] [CrossRef]
- Institute of Medicine. Delivering High-Quality Cancer Care: Charting a New Course for a System in Crisis; National Academies Press: Washington, DC, USA, 2013. [Google Scholar]
- Carpentier, M.Y.; Vernon, S.W.; Bartholomew, L.K.; Murphy, C.C.; Bluethmann, S.M. Receipt of recommended surveillance among colorectal cancer survivors: A systematic review. J. Cancer Surviv. 2013, 7, 464–483. [Google Scholar] [CrossRef] [Green Version]
- Von Elm, E.; Altman, D.G.; Egger, M.; Pocock, S.J.; Gøtzsche, P.C.; Vandenbroucke, J.P. The strengthening the reporting of observational studies in epidemiology (strobe) statement: Guidelines for reporting observational studies. Lancet 2007, 370, 1453–1457. [Google Scholar] [CrossRef]
- World Health Organization. Icd-10: International Statistical Classification of Diseases and Related Health Problems/World Health Organization; World Health Organization: Geneva, Switzerland, 2004. [Google Scholar]
- Edge, S.B. American joint committee on cancer. AJCC Cancer Staging Handbook: From the AJCC Cancer Staging Manual; Springer: New York, NY, USA, 2010. [Google Scholar]
- Cooper, G.S.; Schultz, L.; Simpkins, J.; Lafata, J.E. The utility of administrative data for measuring adherence to cancer surveillance care guidelines. Med. Care 2007, 45, 66–72. [Google Scholar] [CrossRef]
- Harris, P.A.; Taylor, R.; Thielke, R.; Payne, J.; Gonzalez, N.; Conde, J.G. Research electronic data capture (redcap)—A metadata-driven methodology and workflow process for providing translational research informatics support. J. Biomed. Inf. 2009, 42, 377–381. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- R Core Team. R: A Language and Environment for Statistical Computing; R Foundation for Statistical Computing: Vienna, Austria, 2019; Available online: https://www.R-project.org/ (accessed on 27 April 2019).
- RStudio Team. Rstudio: Integrated Development Environment for R; RStudio, Inc.: Boston, MA, USA, 2018; Available online: http://www.rstudio.com/ (accessed on 28 March 2019).
- Wickham, H. Ggplot2: Elegant Graphics for Data Analysis; Springer-Verlag New York: New York, NY, USA, 2016. [Google Scholar]
- Chang, W. Extrafont: Tools for Using Fonts. R Package Version 0.17. Available online: https://CRAN.R-project.org/package=extrafont (accessed on 21 June 2019).
- Australian bureau of statistics. 1270.0.55.005-Australian Statistical Geography Standard (ASGS): Volume 5-Remoteness Structure. Available online: https://www.abs.gov.au/AUSSTATS/[email protected]/Lookup/1270.0.55.005Main+Features1July%202016?OpenDocument (accessed on 30 June 2019).
- Haggstrom, D.A.; Arora, N.K.; Helft, P.; Clayman, M.L.; Oakley-Girvan, I. Follow-up care delivery among colorectal cancer survivors most often seen by primary and subspecialty care physicians. J. Gen. Intern. Med. 2009, 24, S472–S479. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Fox, J.P.; Jeffery, D.D.; Williams, T.V.; Gross, C.P. Quality of cancer survivorship care in the military health system (tricare). Cancer J. 2013, 19, 1–9. [Google Scholar] [CrossRef] [PubMed]
- Salloum, R.G.; Hornbrook, M.C.; Fishman, P.A.; Ritzwoller, D.P.; O’Keeffe Rossetti, M.C.; Elston Lafata, J. Adherence to surveillance care guidelines after breast and colorectal cancer treatment with curative intent. Cancer 2012, 118, 5644–5651. [Google Scholar] [CrossRef] [Green Version]
- Hu, C.Y.; Delclos, G.L.; Chan, W.; Du, X.L. Post-treatment surveillance in a large cohort of patients with colon cancer. Am. J. Manag. Care 2011, 17, 329–336. [Google Scholar]
- Kupfer, S.S.; Lubner, S.; Coronel, E.; Pickhardt, P.J.; Tipping, M.; Graffy, P.; Keenan, E.; Ross, E.; Li, T.; Weinberg, D.S.; et al. Adherence to postresection colorectal cancer surveillance at national cancer institute-designated comprehensive cancer centers. Cancer Med. 2018, 7, 5351–5358. [Google Scholar] [CrossRef]
- Paulson, E.C.; Veenstra, C.M.; Vachani, A.; Ciunci, C.A.; Epstein, A.J. Trends in surveillance for resected colorectal cancer, 2001–2009. Cancer 2015, 121, 3525–3533. [Google Scholar] [CrossRef] [Green Version]
- Urquhart, R.; Folkes, A.; Porter, G.; Kendell, C.; Cox, M.; Dewar, R.; Grunfeld, E. Population-based longitudinal study of follow-up care for patients with colorectal cancer in nova scotia. J. Oncol. Pract. Am. Soc. Clin. Oncol. 2012, 8, 246–252. [Google Scholar] [CrossRef] [Green Version]
- Frew, G.; Smith, A.; Zutshi, B.; Young, N.; Aggarwal, A.; Jones, P.; Kockelbergh, R.; Richards, M.; Maher, E.J. Results of a quantitative survey to explore both perceptions of the purposes of follow-up and preferences for methods of follow-up delivery among service users, primary care practitioners and specialist clinicians after cancer treatment. Clin. Oncol. 2010, 22, 874–884. [Google Scholar] [CrossRef]
- Jeffery, M.; Hickey, B.E.; Hider, P.N.; See, A.M. Follow-up strategies for patients treated for non-metastatic colorectal cancer. Cochrane Database Syst. Rev. 2016, 11, CD002200. [Google Scholar] [CrossRef]
- Young, J.M.; Durcinoska, I.; de Loyde, K.; Solomon, M.J. Patterns of follow up and survivorship care for people with colorectal cancer in new south wales, australia: A population-based survey. BMC Cancer 2018, 18, 339. [Google Scholar] [CrossRef] [PubMed]
- Dossett, L.A.; Hudson, J.N.; Morris, A.M.; Lee, M.C.; Roetzheim, R.G.; Fetters, M.D.; Quinn, G.P. The primary care provider (PCP)-cancer specialist relationship: A systematic review and mixed-methods meta-synthesis. CA Cancer J. Clin. 2017, 67, 156–169. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Burg, M.A.; Adorno, G.; Lopez, E.D.; Loerzel, V.; Stein, K.; Wallace, C.; Sharma, D.K. Current unmet needs of cancer survivors: Analysis of open-ended responses to the american cancer society study of cancer survivors ii. Cancer 2015, 121, 623–630. [Google Scholar] [CrossRef]
- Lisy, K.; Langdon, L.; Piper, A.; Jefford, M. Identifying the most prevalent unmet needs of cancer survivors in australia: A systematic review. Asia Pac. J. Clin. Oncol. 2019, 15, e68–e78. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Alfano, C.M.; Jefford, M.; Maher, J.; Birken, S.A.; Mayer, D.K. Building personalized cancer follow-up care pathways in the united states: Lessons learned from implementation in England, Northern Ireland, and australia. Am. Soc. Clin. Oncol. Educ. Book. Am. Soc. Clin. Oncol. Annu. Meet. 2019, 39, 625–639. [Google Scholar] [CrossRef]
- Jefford, M.; Emery, J.; Grunfeld, E.; Martin, A.; Rodger, P.; Murray, A.M.; de Abreu Lourenco, R.; Heriot, A.; Phipps-Nelson, J.; Guccione, L.; et al. Score: Shared care of colorectal cancer survivors: Protocol for a randomised controlled trial. Trials 2017, 18, 506. [Google Scholar] [CrossRef]
- Prins, H.; Hasman, A. Appropriateness of icd-coded diagnostic inpatient hospital discharge data for medical practice assessment. A systematic review. Methods Inf. Med. 2013, 52, 3–17. [Google Scholar]

| Sociodemographic | ||
| Age at curative resection (yrs) | ||
| Mean [SD] | 58.9 [14.8] | |
| Median [IQR] | 59 [50, 69] | |
| Min, Max | 28, 88 | |
| Remoteness a | n (%) | |
| RA1 (Major Cities of Australia) | 29 (60.4%) | |
| RA2 (Inner Regional Australia) | 14 (29.2%) | |
| RA3 (Outer Regional Australia) | 5 (10.4%) | |
| Sex | n (%) | |
| Female | 27 (56.3%) | |
| Male | 21 (43.8%) | |
| Smoking status | n (%) | |
| Non-smoker | 29 (60.4%) | |
| Ex-smoker | 11 (22.9%) | |
| Current smoker | 8 (16.7%) | |
| Disease | ||
| Cancer site and treatment | n (%) | |
| Colon | 23 (47.9%) | |
| Surgery only | 13 (56.5%) | |
| Surgery and adjuvant chemotherapy | 9 (39.1%) | |
| Neoadjuvant chemotherapy, surgery and adjuvant chemotherapy | 1 (4.3%) | |
| Rectal | 15 (31.3%) | |
| Neoadjuvant chemoradiotherapy, surgery and adjuvant chemotherapy | 7 (46.7%) | |
| Surgery only | 3 (20%) | |
| Neoadjuvant chemoradiotherapy and surgery | 2 (13.3%) | |
| Neoadjuvant chemoradiotherapy, surgery and adjuvant chemoradiotherapy | 1 (6.7%) | |
| Neoadjuvant radiotherapy and surgery | 1 (6.7%) | |
| Surgery and adjuvant chemotherapy | 1 (6.7%) | |
| Rectosigmoid | 10 (20.8%) | |
| Surgery only | 5 (50%) | |
| Neoadjuvant chemoradiotherapy, surgery and adjuvant chemotherapy | 2 (20%) | |
| Surgery and adjuvant chemotherapy | 2 (20%) | |
| Neoadjuvant chemoradiotherapy and surgery | 1 (10%) | |
| Year of curative resection | n (%) | |
| 2015 | 7 (14.6%) | |
| 2016 | 13 (27.1%) | |
| 2017 | 20 (41.7%) | |
| 2018 | 8 (16.7%) | |
| Cancer grade | n (%) | |
| Low | 41 (85.4%) | |
| High | 7 (14.6%) | |
| Cancer stage b | n (%) | |
| I | 11 (22.9%) | |
| IIA | 12 (25%) | |
| IIB | 1 (2.1%) | |
| IIC | 5 (10.4%) | |
| IIIA | 1 (2.1%) | |
| IIIB | 12 (25%) | |
| IIIC | 6 (12.5%) | |
| Cancer type | n (%) | |
| Adenocarcinoma (NOS) | 36 (75%) | |
| Adenocarcinoma (Usual Type) | 6 (12.5%) | |
| Adenocarcinoma (Mucinous) | 5 (10.4%) | |
| Adenocarcinoma (Colloid) | 1 (2.1%) | |
© 2020 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Garwood, V.; Lisy, K.; Jefford, M. Survivorship in Colorectal Cancer: A Cohort Study of the Patterns and Documented Content of Follow-Up Visits. J. Clin. Med. 2020, 9, 2725. https://doi.org/10.3390/jcm9092725
Garwood V, Lisy K, Jefford M. Survivorship in Colorectal Cancer: A Cohort Study of the Patterns and Documented Content of Follow-Up Visits. Journal of Clinical Medicine. 2020; 9(9):2725. https://doi.org/10.3390/jcm9092725
Chicago/Turabian StyleGarwood, Victoria, Karolina Lisy, and Michael Jefford. 2020. "Survivorship in Colorectal Cancer: A Cohort Study of the Patterns and Documented Content of Follow-Up Visits" Journal of Clinical Medicine 9, no. 9: 2725. https://doi.org/10.3390/jcm9092725





