Effects of Time-Interval since Blood Draw and of Anticoagulation on Platelet Testing (Count, Indices and Impedance Aggregometry): A Systematic Study with Blood from Healthy Volunteers
Abstract
1. Introduction
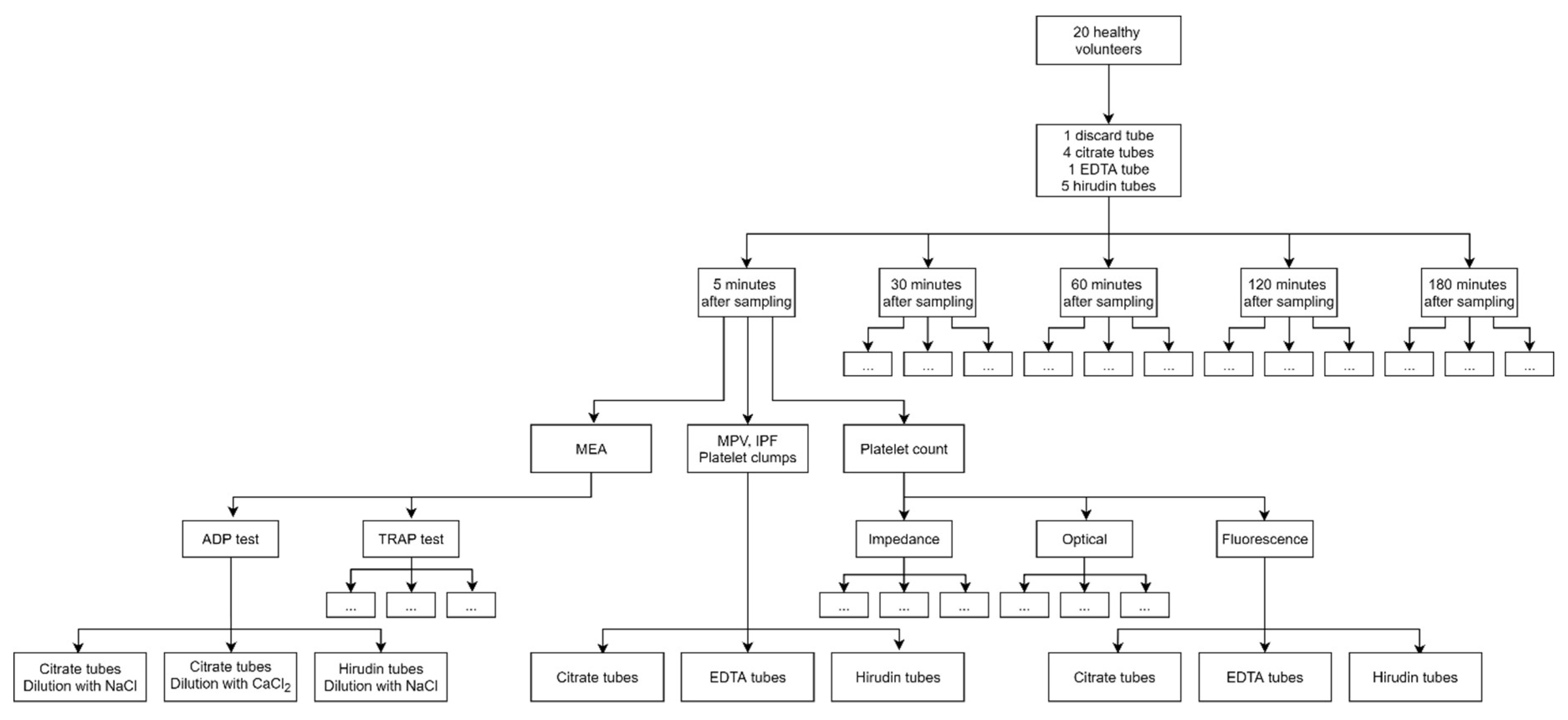
2. Materials and Methods
Statistical Analysis
3. Results
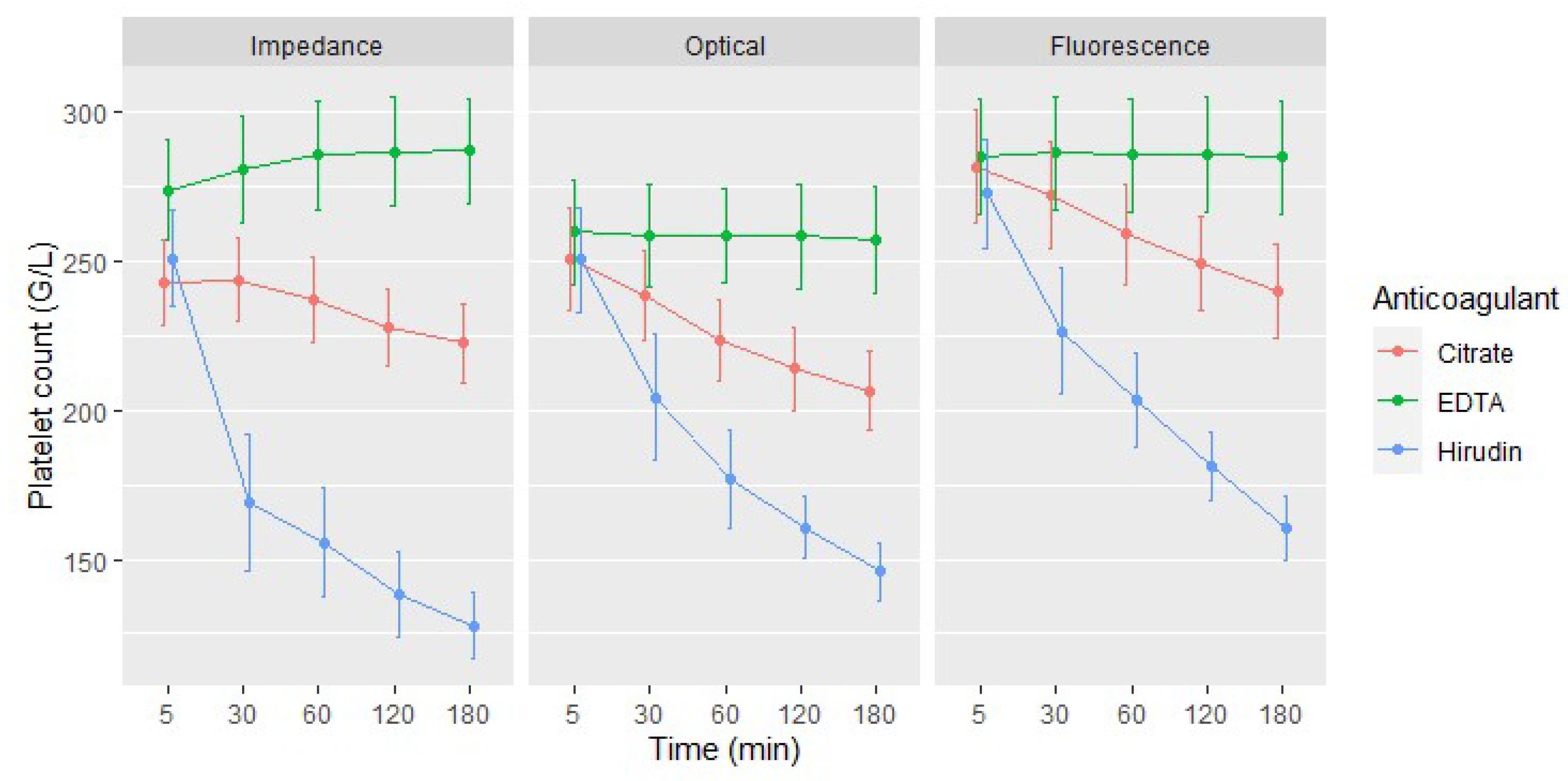
3.1. Platelet Count
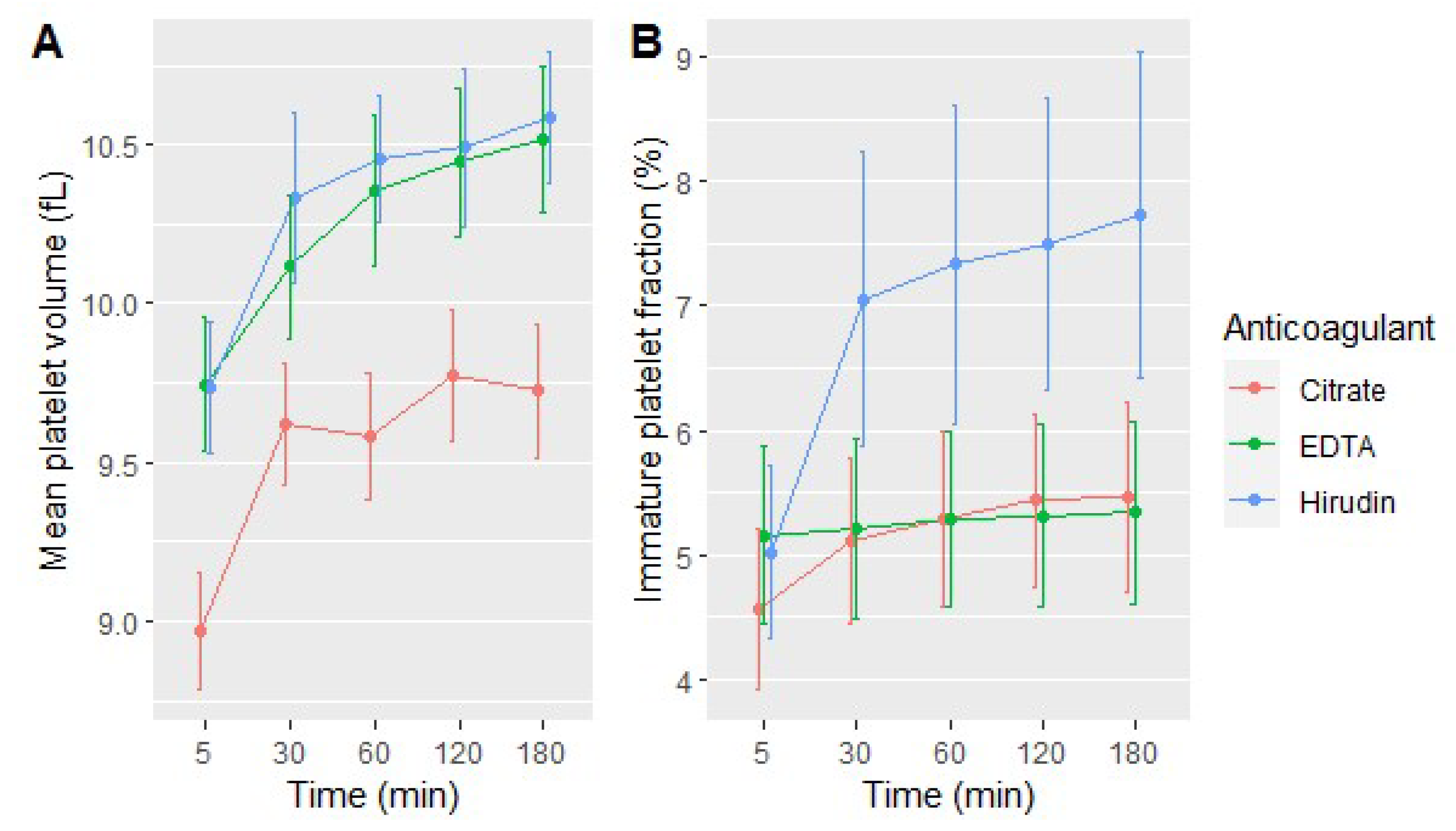
3.2. Platelet Indices
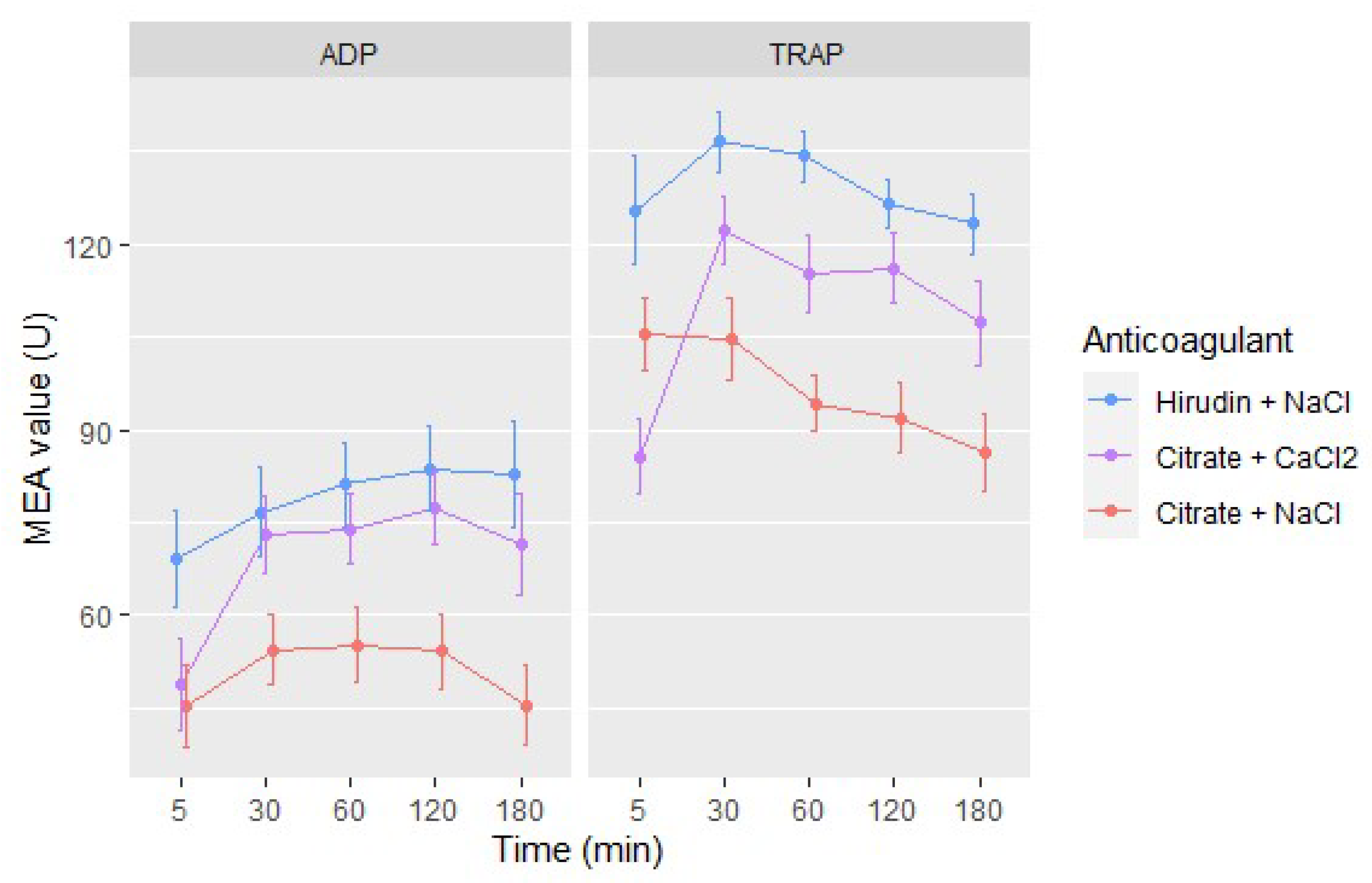
3.3. Platelet Function—MEA
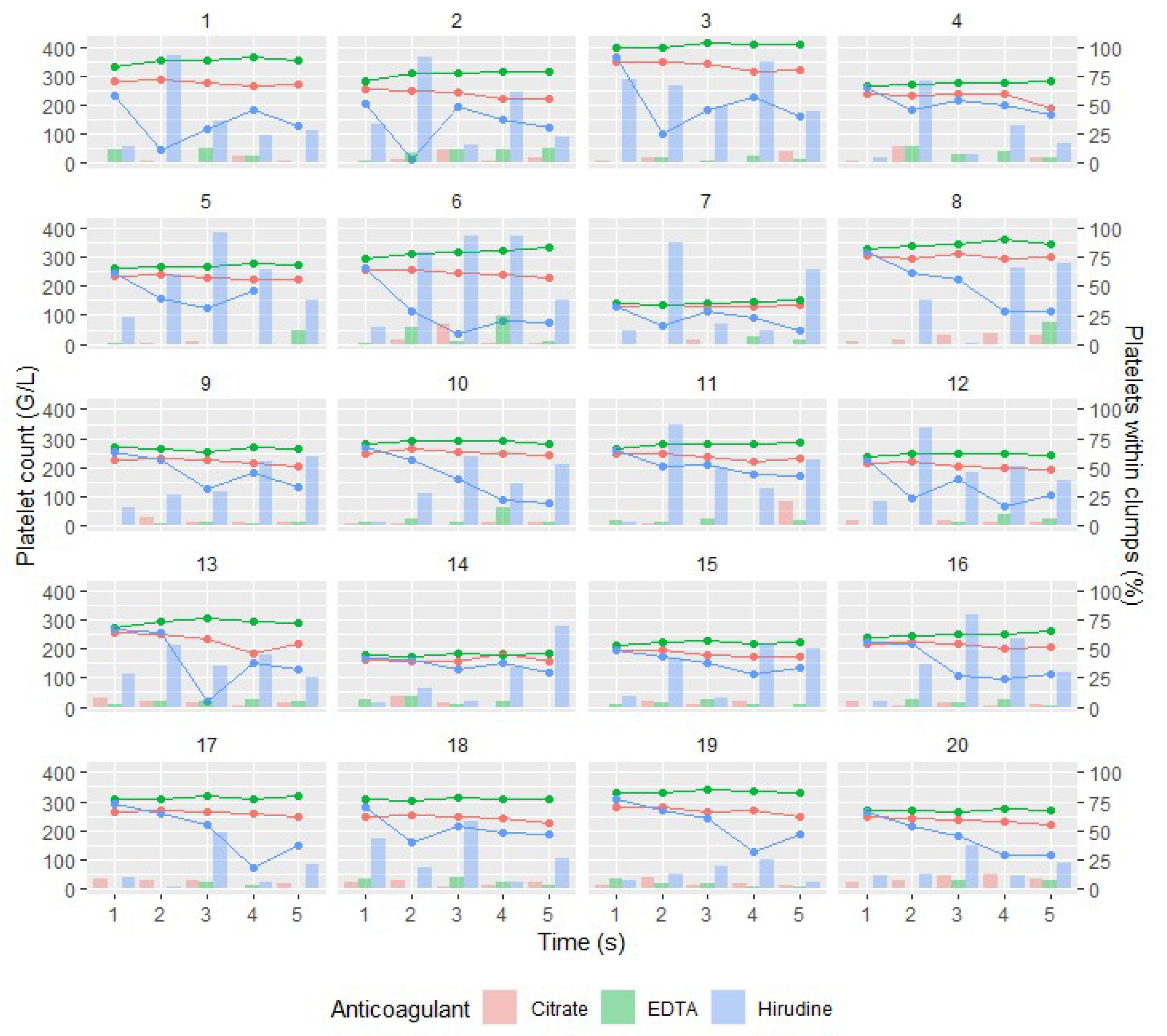
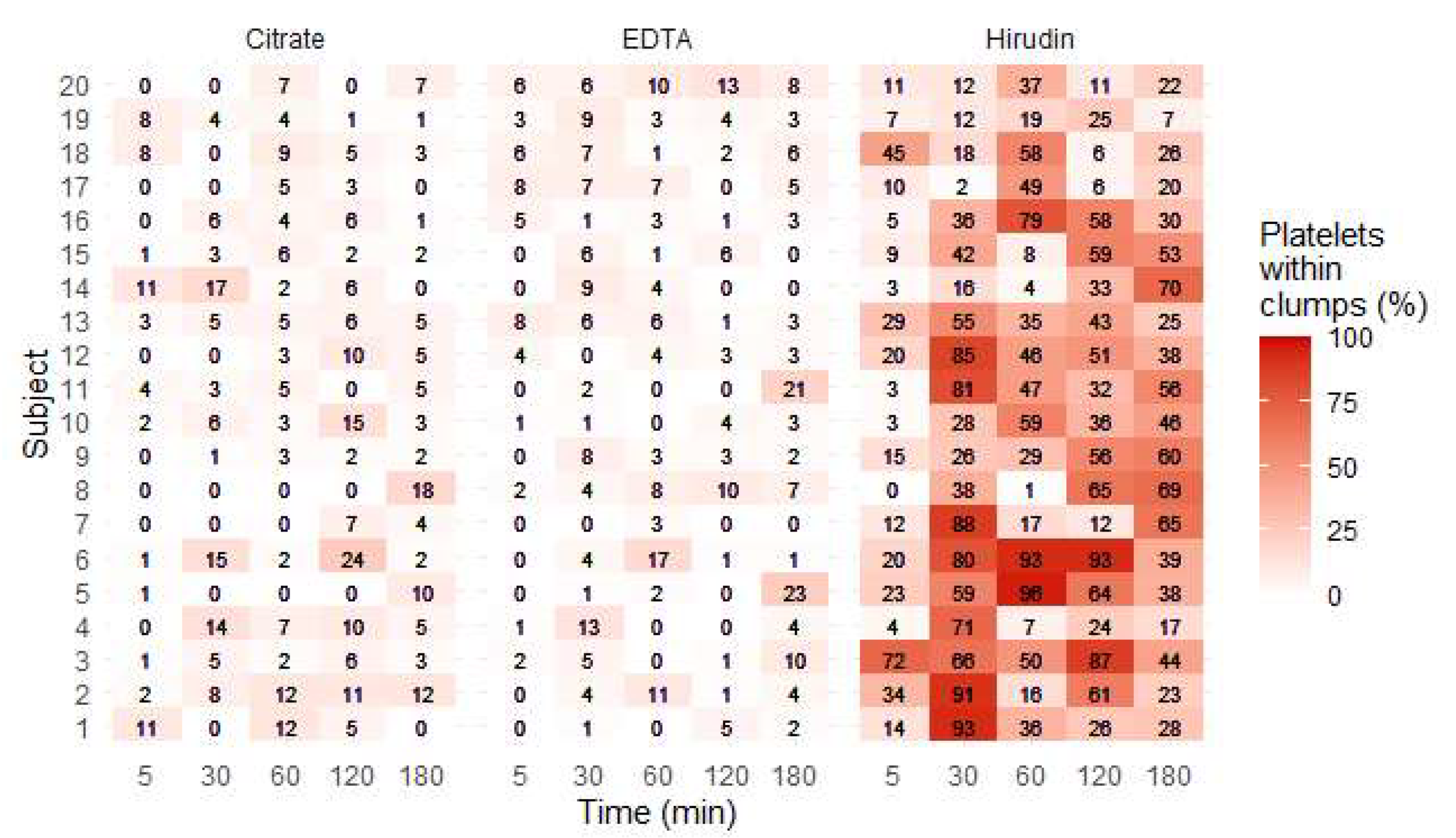
3.4. Platelet Clumps
4. Discussion
4.1. Platelet Clumps
4.2. Platelet Count
4.3. Platelet Indices
4.4. Platelet Function
4.5. Limitations
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Conflicts of Interest
References
- Lance, M.D.; Sloep, M.; Henskens, Y.M.; Marcus, M.A. Mean platelet volume as a diagnostic marker for cardiovascular disease: Drawbacks of preanalytical conditions and measuring techniques. Clin. Appl. Thromb. Hemost. 2012, 18, 561–568. [Google Scholar] [CrossRef] [PubMed]
- Kim, C.H.; Kim, S.J.; Lee, M.J.; Kwon, Y.E.; Kim, Y.L.; Park, K.S.; Ryu, H.J.; Park, J.T.; Han, S.H.; Yoo, T.H.; et al. An increase in mean platelet volume from baseline is associated with mortality in patients with severe sepsis or septic shock. PLoS ONE 2015, 10, e0119437. [Google Scholar] [CrossRef] [PubMed]
- Noris, P.; Klersy, C.; Gresele, P.; Giona, F.; Giordano, P.; Minuz, P.; Loffredo, G.; Pecci, A.; Melazzini, F.; Civaschi, E.; et al. Platelet size for distinguishing between inherited thrombocytopenias and immune thrombocytopenia: A multicentric, real life study. Br. J. Haematol. 2013, 162, 112–119. [Google Scholar] [CrossRef] [PubMed]
- Briggs, C.; Kunka, S.; Hart, D.; Oguni, S.; Machin, S.J. Assessment of an immature platelet fraction (IPF) in peripheral thrombocytopenia. Br. J. Haematol. 2004, 126, 93–99. [Google Scholar] [CrossRef]
- Osei-Bimpong, A. The effect of storage on the clinical utility of the immature platelet fraction. Hematology 2009, 14, 118–121. [Google Scholar] [CrossRef]
- Briggs, C.; Hart, D.; Kunka, S.; Oguni, S.; Machin, S.J. Immature platelet fraction measurement: A future guide to platelet transfusion requirement after haematopoietic stem cell transplantation. Transfus. Med. 2006, 16, 101–109. [Google Scholar] [CrossRef]
- Kong, R.; Trimmings, A.; Hutchinson, N.; Gill, R.; Agarwal, S.; Davidson, S.; Arcari, M. Consensus recommendations for using the Multiplate(R) for platelet function monitoring before cardiac surgery. Int. J. Lab. Hematol. 2015, 37, 143–147. [Google Scholar] [CrossRef]
- Tantry, U.S.; Bonello, L.; Aradi, D.; Price, M.J.; Jeong, Y.H.; Angiolillo, D.J.; Stone, G.W.; Curzen, N.; Geisler, T.; Ten Berg, J.; et al. Consensus and update on the definition of on-treatment platelet reactivity to adenosine diphosphate associated with ischemia and bleeding. J. Am. Coll. Cardiol. 2013, 62, 2261–2273. [Google Scholar] [CrossRef]
- Al Ghaithi, R.; Drake, S.; Watson, S.P.; Morgan, N.V.; Harrison, P. Comparison of multiple electrode aggregometry with lumi-aggregometry for the diagnosis of patients with mild bleeding disorders. J. Thromb. Haemost. 2017, 15, 2045–2052. [Google Scholar] [CrossRef]
- Magnette, A.; Chatelain, M.; Chatelain, B.; Ten Cate, H.; Mullier, F. Pre-analytical issues in the hemostasis laboratory: Guidance for the clinical laboratories. Thromb. J. 2016, 14, 49. [Google Scholar] [CrossRef]
- Baccini, V.; Geneviève, F.; Jacqmin, H.; Chatelain, B.; Girard, S.; Wuilleme, S.; Vedrenne, A.; Guiheneuf, E.; Toussaint-Hacquard, M.; Everaere, F.; et al. Platelet counting: Ugly traps and good advice: Proposals from the French-Speaking Cellular Hematology Group (GFHC). J. Clin. Med. 2020, 9, 808. [Google Scholar] [CrossRef] [PubMed]
- Mahla, E.; Tantry, U.S.; Pruller, F.; Gurbel, P.A. Is There a role for preoperative platelet function testing in patients undergoing cardiac surgery during antiplatelet therapy? Circulation 2018, 138, 2145–2159. [Google Scholar] [CrossRef] [PubMed]
- Taylor, P.M.; Heptinstall, S. The abilities of human blood platelets to bind extracellular calcium and to be aggregated by adenosine diphosphate are related. Br. J. Haematol. 1980, 46, 115–122. [Google Scholar] [CrossRef] [PubMed]
- Johnston, L.R.; Larsen, P.D.; La Flamme, A.C.; Harding, S.A. Methodological considerations for the assessment of ADP induced platelet aggregation using the Multiplate(R) analyser. Platelets 2013, 24, 303–307. [Google Scholar] [CrossRef]
- International Council for Standardization in Haematology, Writing Group; Briggs, C.; Culp, N.; Davis, B.; d’Onofrio, G.; Zini, G. ICSH guidelines for the evaluation of blood cell analysers including those used for differential leucocyte and reticulocyte counting. Int. J. Lab. Hematol. 2014, 36, 613–627. [Google Scholar]
- Tanaka, Y.; Tanaka, Y.; Gondo, K.; Maruki, Y.; Kondo, T.; Asai, S.; Matsushita, H.; Miyachi, H. Performance evaluation of platelet counting by novel fluorescent dye staining in the XN-series automated hematology analyzers. J. Clin. Lab. Anal. 2014, 28, 341–348. [Google Scholar] [CrossRef]
- Fujimoto, K. Principles of measurement in hematology analyzers manufactured by Sysmex Corporation. Sysmex. J. Int. 1999, 99, 31–44. [Google Scholar]
- Wada, A.; Takagi, Y.; Kono, M.; Morikawa, T. Accuracy of a New Platelet Count System (PLT-F) Depends on the Staining Property of Its Reagents. PLoS ONE 2015, 10, e0141311. [Google Scholar] [CrossRef]
- Toth, O.; Calatzis, A.; Penz, S.; Losonczy, H.; Siess, W. Multiple electrode aggregometry: A new device to measure platelet aggregation in whole blood. Thromb. Haemost. 2006, 96, 781–788. [Google Scholar]
- Sibbing, D.; Braun, S.; Jawansky, S.; Vogt, W.; Mehilli, J.; Schömig, A.; Kastrati, A.; von Beckerath, N. Assessment of ADP-induced platelet aggregation with light transmission aggregometry and multiple electrode platelet aggregometry before and after clopidogrel treatment. Thromb. Haemost. 2008, 99, 121–126. [Google Scholar]
- Mackie, I.J.; Jones, R.; Machin, S.J. Platelet impedance aggregation in whole blood and its inhibition by antiplatelet drugs. J. Clin. Pathol. 1984, 3737, 874–878. [Google Scholar] [CrossRef] [PubMed]
- Laird, N.M.; Ware, J.H. Random-effects models for longitudinal data. Biometrics 1982, 38, 963–974. [Google Scholar] [CrossRef]
- Ricos, C.; Cava, F.; Garcia-Lario, J.V.; Hernandez, A.; Iglesias, N.; Jimenez, C.V.; Minchinela, J.; Perich, C.; Simón, M.; Domenech, M.V.; et al. The reference change value: A proposal to interpret laboratory reports in serial testing based on biological variation. Scand. J. Clin. Lab. Investig. 2004, 64, 175–184. [Google Scholar] [CrossRef] [PubMed]
- Coskun, A.; Serteser, M.; Karpuzoglu, H.F.; Unsal, I. How can we evaluate differences between serial measurements on the same sample? A new approach based on within-subject biological variation. Clin. Chem. Lab. Med. 2017, 55, e44–e46. [Google Scholar] [CrossRef] [PubMed]
- R Core Team. R: A Language and Environment for Statistical Computing; R Foundation for Statistical Computing: Vienna, Austria, 2019. [Google Scholar]
- Ts’ao, C.H. Platelet aggregation by ristocetin in EDTA plasma: Extension clumping with high concentrations of EDTA. Hemostasis 1972, 11, 315–319. [Google Scholar] [CrossRef] [PubMed]
- Menssen, H.D.; Melber, K.; Brandt, N.; Thiel, E. The use of hirudin as universal anticoagulant in haematology, clinical chemistry and blood grouping. Clin. Chem. Lab. Med. 2001, 39, 1267–1277. [Google Scholar] [CrossRef] [PubMed]
- Jiang, L.; Xu, C.; Yu, S.; Liu, P.; Luo, D.; Zhou, Q.; Gao, C.; Hu, H. A critical role of thrombin/PAR-1 in ADP-induced platelet secretion and the second wave of aggregation. J. Thromb. Haemost. 2013, 11, 930–940. [Google Scholar] [CrossRef]
- Macey, M.; Azam, U.; McCarthy, D.; Webb, L.; Chapman, E.S.; Okrongly, D.; Zelmanovic, D.; Newland, A. Evaluation of the anticoagulants EDTA and citrate, theophylline, adenosine, and dipyridamole (CTAD) for assessing platelet activation on the ADVIA 120 hematology system. Clin. Chem. 2002, 48, 891–899. [Google Scholar] [CrossRef]
- Védy, S.; Boom, B.; Perez, P.; Schillinger, S.; Ragot, C.; Bakkouch, S.; Puyhardy, J.M. Automatic platelets numbering with citrate as anticoagulant: Is the result valid? Ann. Biol. Clin. (Paris) 2011, 69, 453–458. [Google Scholar] [CrossRef]
- Lance, M.D.; van Oerle, R.; Henskens, Y.M.; Marcus, M.A. Do we need time adjusted mean platelet volume measurements? Lab. Hematol. 2010, 16, 28–31. [Google Scholar] [CrossRef] [PubMed]
- Zhao, T.X. Electrical impedance and haematocrit of human blood with various anticoagulants. Physiol. Meas. 1993, 14, 299–307. [Google Scholar] [CrossRef] [PubMed]
- Nishioka, T.; Yokota, M.; Tsuda, I.; Tatsumi, N. Flow cytometric analysis of platelet activation under calcium ion-chelating conditions. Clin. Lab. Haematol. 2002, 24, 115–119. [Google Scholar] [CrossRef] [PubMed]
- Buttarello, M.; Mezzapelle, G.; Plebani, M. Effect of preanalytical and analytical variables on the clinical utility of mean platelet volume. Clin. Chem. Lab. Med. 2018, 56, 718–725. [Google Scholar] [CrossRef] [PubMed]
- Bessman, J.D.; Williams, L.J.; Gilmer, P.R., Jr. Mean platelet volume. The inverse relation of platelet size and count in normal subjects, and an artifact of other particles. Am. J. Clin. Pathol. 1981, 76, 289–293. [Google Scholar] [CrossRef] [PubMed]
- Jackson, S.R.; Carter, J.M. Platelet volume: Laboratory measurement and clinical application. Blood Rev. 1993, 7, 104–113. [Google Scholar] [CrossRef]
- White, J.G. Effects of ethylenediamine tetracetic acid (EDTA) on platelet structure. Scand J. Haematol. 1968, 55, 241–254. [Google Scholar] [CrossRef]
- Miyazaki, K.; Koike, Y.; Kunishima, S.; Ishii, R.; Danbara, M.; Horie, R.; Yatomi, Y.; Higashihara, M. Immature platelet fraction measurement is influenced by platelet size and is a useful parameter for discrimination of macrothrombocytopenia. Hematology 2015, 2020, 587–592. [Google Scholar] [CrossRef]
- Osei-Bimpong, A.; Saleh, M.; Sola-Visner, M.; Widness, J.; Veng-Pedersen, P. Correction for effect of cold storage on immature platelet fraction. J. Clin. Lab. Anal. 2010, 24, 431–433. [Google Scholar] [CrossRef]
- Maenhout, T.M.; Leus, B.; Bouchier, L.; Dierick, J. Immature platelet fraction (IPF%) in a routine clinical laboratory: (pre)analytical and clinical evaluation. In Proceedings of the Conference of Belgian Society of Clinical Biologists, Liege, Belgium, October 2011. [Google Scholar]
- Anetsberger, A.; Blobner, M.; Haller, B.; Schmid, S.; Umgelter, K.; Hager, T.; Langgartner, C.; Kochs, E.F.; Laugwitz, K.L.; Jungwirth, B.; et al. Immature platelets as a novel biomarker for adverse cardiovascular events in patients after non-cardiac surgery. Thromb. Haemost. 2017, 117, 1887–1895. [Google Scholar] [CrossRef]
- Lee, E.Y.; Kim, S.J.; Song, Y.J.; Choi, S.J.; Song, J. Immature platelet fraction in diabetes mellitus and metabolic syndrome. Thromb. Res. 2013, 132, 692–695. [Google Scholar] [CrossRef]
- Pittens, C.A.; Bouman, H.J.; van Werkum, J.W.; Ten Berg, J.M.; Hackeng, C.M. Comparison between hirudin and citrate in monitoring the inhibitory effects of P2Y12 receptor antagonists with different platelet function tests. J. Thromb. Haemost. 2009, 77, 1929–1932. [Google Scholar] [CrossRef] [PubMed]
- Kalb, M.L.; Potura, L.; Scharbert, G.; Kozek-Langenecker, S.A. The effect of ex vivo anticoagulants on whole blood platelet aggregation. Platelets 2009, 20, 7–11. [Google Scholar] [CrossRef] [PubMed]
- Chapman, K.; Favaloro, E.J. Time dependent reduction in platelet aggregation using the multiplate analyser and hirudin blood due to platelet clumping. Platelets 2018, 29, 305–308. [Google Scholar] [CrossRef] [PubMed]
- Wurtz, M.; Hvas, A.M.; Christensen, K.H.; Rubak, P.; Kristensen, S.D.; Grove, E.L. Rapid evaluation of platelet function using the Multiplate(R) analyzer. Platelets 2014, 25, 628–633. [Google Scholar] [CrossRef] [PubMed]
- Kaiser, A.F.; Neubauer, H.; Franken, C.C.; Kruger, J.C.; Mugge, A.; Meves, S.H. Which is the best anticoagulant for whole blood aggregometry platelet function testing? Comparison of six anticoagulants and diverse storage conditions. Platelets 2012, 23, 359–367. [Google Scholar] [CrossRef]
- Seyfert, U.T.; Haubelt, H.; Vogt, A.; Hellstern, P. Variables influencing Multiplate (TM) whole blood impedance platelet aggregometry and turbidimetric platelet aggregation in healthy individuals. Platelets 2007, 18, 199–206. [Google Scholar] [CrossRef]
- Jilma-Stohlawetz, P.; Ratzinger, F.; Schorgenhofer, C.; Jilma, B.; Quehenberger, P. Effect of preanalytical time-delay on platelet function as measured by multiplate, PFA-100 and VerifyNow. Scand. J. Clin. Lab. Investig. 2016, 76, 249–255. [Google Scholar] [CrossRef]
- Dézsi, D.A.; Merkely, B.; Skopál, J.; Barabás, E.; Várnai, K.; Faluközy, J.; Veress, G.; Alotti, N.; Aradi, D. Impact of test conditions on ADP-induced platelet function results with the multiplate assay: Is further standardization required? J. Cardiovasc. Pharmacol. Ther. 2018, 23, 149–154. [Google Scholar] [CrossRef]
- Harrison, P.; Mackie, I.; Mumford, A.; Briggs, C.; Liesner, R.; Winter, M.; Machin, S.; British Committee for Standards in Haematology. Guidelines for the laboratory investigation of heritable disorders of platelet function. Br. J. Haematol. 2011, 155, 30–44. [Google Scholar] [CrossRef]
- Storey, R.F.; Wilcox, R.G.; Heptinstall, S. Differential effects of glycoprotein IIb/IIIa antagonists on platelet microaggregate and macroaggregate formation and effect of anticoagulant on antagonist potency. Implications for assay methodology and comparison of different antagonists. Circulation 1998, 98, 1616–1621. [Google Scholar] [CrossRef]
- Latger-Cannard, V.; Hoarau, M.; Salignac, S.; Baumgart, D.; Nurden, P.; Lecompte, T. Mean platelet volume: Comparison of three analysers towards standardization of platelet morphological phenotype. Int. J. Lab. Hematol. 2012, 34, 300–310. [Google Scholar] [CrossRef] [PubMed]
- Stissing, T.; Dridi, N.P.; Ostrowski, S.R.; Bochsen, L.; Johansson, P.I. The influence of low platelet count on whole blood aggregometry assessed by Multiplate. Clin. Appl. Thromb. Hemost. 2011, 17, E211–E217. [Google Scholar] [CrossRef] [PubMed]
| 5 min | 30 min (vs. 5 min) | 60 min (vs. 5 min) | 120 min (vs. 5 min) | 180 min (vs. 5 min) | |||||
|---|---|---|---|---|---|---|---|---|---|
| EDTA | 0 | 0.4 (3.8%) (0.3; 0.5) | *** | 0.6 (6.2%) (0.5; 0.7) | *** | 0.7 (7.2%) (0.6; 0.8) | *** | 0.8 (7.9%) (0.7; 0.9) | *** |
| Hirudin | 0 | 0.6 (6.2%) (0.5; 0.7) | *** | 0.7 (7.6%) (0.6; 0.8) | *** | 0.7 (8.0%) (0.6; 0.9) | *** | 0.9 (9.2%) (0.7; 1.0) | *** |
| Citrate | 0 | 0.6 (7.4%) (0.5; 0.8) | *** | 0.6 (6.9%) (0.5; 0.7) | *** | 0.8 (9.0%) (0.7; 0.9) | *** | 0.7 (8.4%) (0.6; 0.9) | *** |
| 5 min | 30 min (vs. 5 min) | 60 min (vs. 5 min) | 120 min (vs. 5 min) | 180 min (vs. 5 min) | |||||
|---|---|---|---|---|---|---|---|---|---|
| EDTA | 0 | 0.1 (1.2%) (−0.5; 0.6) | 0.1 (3.3%) (−0.4; 0.7) | 0.1 (3.1%) (−0.4; 0.7) | 0.2 (4.0%) (−0.4; 0.8) | ||||
| Hirudin | 0 | 2.0 (51.2%) (1.4; 2.6) | *** | 2.3 (58.9%) (1.7; 2.9) | *** | 2.5 (54.8%) (1.9; 3.1) | *** | 2.7 (60.2%) (2.1; 3.1) | *** |
| Citrate | 0 | 0.5 (19.1%) (−0.05; 1.1) | 0.7 (18.5%) (0.1; 1.3) | * | 0.9 (23.4%) (0.3; 1.5) | ** | 0.9 (22.4%) (0.3; 1.5) | ** |
| 5 min (vs. 30 min) | 30 min | 60 min (vs. 30 min) | 120 min (vs. 30 min) | 180 min (vs. 30 min) | ||||||
|---|---|---|---|---|---|---|---|---|---|---|
| ADP | Citrate + NaCl | −9 (−19.9%) (−15; −3) | ** | 0 | 1 (3.0%) (−5; 7) | −0.2 (0.1%) (−6; 6) | −9 (−17.1%) (−15; −3) | ** | ||
| Citrate + CaCl2 | −24 (−35.5%) (−30; −18) | *** | 0 | 1 (2.6%) (−5; 7) | 4 (7.5%) (−2; 10) | −2 (1.0%) (−8; 4) | ||||
| Hirudin | −7 (−10.0%) (−14; −1) | * | 0 | 4 (7.0%) (−2; 10) | 7 (11.6%) (1; 13) | * | 6 (10.0%) (−0.01; 12) | |||
| TRAP | Citrate + NaCl | 1 (1.3%) (−6; 8) | 0 | −10 (−9.2%) (−17; −3) | ** | −13 (−11.8%) (−20; −6) | *** | −18 (−17.2%) (−25; −11) | *** | |
| Citrate + CaCl2 | −36 (−29.5%) (−44; −29) | *** | 0 | −7 (−5.8%) (−14; 0.3) | −6 (−4.9%) (−13; 1) | −15 (−12.1%) (−22; −8) | *** | |||
| Hirudin | −11 (−8.1%) (−18; −4) | ** | 0 | −2 (−1.2%) (−9; 5) | −10 (−6.8%) (−17; −3) | ** | −14 (−9.2%) (−21; −6) | *** |
| 5 min | 30 min | 60 min | 120 min | 180 min | |||||||
|---|---|---|---|---|---|---|---|---|---|---|---|
| ADP | Citrate + CaCl2 (vs. Hirudin) | −20 (−30.3%) (−26; −14) | *** | −4 (−3.0%) (−10; 2) | −7 (−6.3%) (−13; −1) | * | −6 (−6.7%) (−12; −0.4) | * | −11 (−8.3%) (−17; −5) | *** | |
| Citrate + CaCl2 (vs. + NaCl) | 3 (12.0%) (−3; 9) | 19 (41.5%) (13; 25) | *** | 19 (41.9%) (13; 25) | *** | 23 (52.1%) (17; 29) | *** | 26 (76.7%) (20; 32) | *** | ||
| Citrate + NaCl (vs. Hirudin) | −24 (35.5%) (−30; −18) | *** | −22 (−29.2%) (−28; −16) | *** | −26 (−32.3%) (−32; −20) | *** | −29 (−36.0%) (−36; −23) | *** | −37 (−44.6%) (−43; −31) | *** | |
| TRAP | Citrate + CaCl2 (vs. Hirudin) | −40 (−30.1%) (−47; −33) | *** | −14 (−9.9%) (−21; −7) | *** | −19 (−14.0%) (−26; −12) | *** | −11 (−8.0%) (−18; −3) | ** | −15 (−12.3%) (−23; −8) | *** |
| Citrate + CaCl2 (vs. + NaCl) | −20 (17.5%) (−27; −13) | *** | 17 (18.5%) (10; 25) | *** | 21 (23.4%) (14; 28) | *** | 24 (27.9%) (17; 31) | *** | 21 (27.0%) (14; 28) | *** | |
| Citrate + NaCl (vs. Hirudin) | −20 (−14.0%) (−27; −13) | *** | −32 (−23.4%) (−39; −25) | *** | −40 (−29.9%) (−47; −33) | *** | −35 (−27.5%) (−42; −28) | *** | −37 (−29.6%) (−44; −29) | *** |
© 2020 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Hardy, M.; Lessire, S.; Kasikci, S.; Baudar, J.; Guldenpfennig, M.; Collard, A.; Dogné, J.-M.; Chatelain, B.; Jacqmin, H.; Lecompte, T.; et al. Effects of Time-Interval since Blood Draw and of Anticoagulation on Platelet Testing (Count, Indices and Impedance Aggregometry): A Systematic Study with Blood from Healthy Volunteers. J. Clin. Med. 2020, 9, 2515. https://doi.org/10.3390/jcm9082515
Hardy M, Lessire S, Kasikci S, Baudar J, Guldenpfennig M, Collard A, Dogné J-M, Chatelain B, Jacqmin H, Lecompte T, et al. Effects of Time-Interval since Blood Draw and of Anticoagulation on Platelet Testing (Count, Indices and Impedance Aggregometry): A Systematic Study with Blood from Healthy Volunteers. Journal of Clinical Medicine. 2020; 9(8):2515. https://doi.org/10.3390/jcm9082515
Chicago/Turabian StyleHardy, Michael, Sarah Lessire, Sultan Kasikci, Justine Baudar, Maité Guldenpfennig, Adrien Collard, Jean-Michel Dogné, Bernard Chatelain, Hugues Jacqmin, Thomas Lecompte, and et al. 2020. "Effects of Time-Interval since Blood Draw and of Anticoagulation on Platelet Testing (Count, Indices and Impedance Aggregometry): A Systematic Study with Blood from Healthy Volunteers" Journal of Clinical Medicine 9, no. 8: 2515. https://doi.org/10.3390/jcm9082515
APA StyleHardy, M., Lessire, S., Kasikci, S., Baudar, J., Guldenpfennig, M., Collard, A., Dogné, J.-M., Chatelain, B., Jacqmin, H., Lecompte, T., & Mullier, F. (2020). Effects of Time-Interval since Blood Draw and of Anticoagulation on Platelet Testing (Count, Indices and Impedance Aggregometry): A Systematic Study with Blood from Healthy Volunteers. Journal of Clinical Medicine, 9(8), 2515. https://doi.org/10.3390/jcm9082515





