Association between African Dust Transport and Acute Exacerbations of COPD in Miami
Abstract
1. Introduction
2. Materials and Methods
2.1. Study Site
2.2. Study Design and Subjects
2.3. Environmental Data
3. Results
3.1. Subjects and AECOPD Prevalence
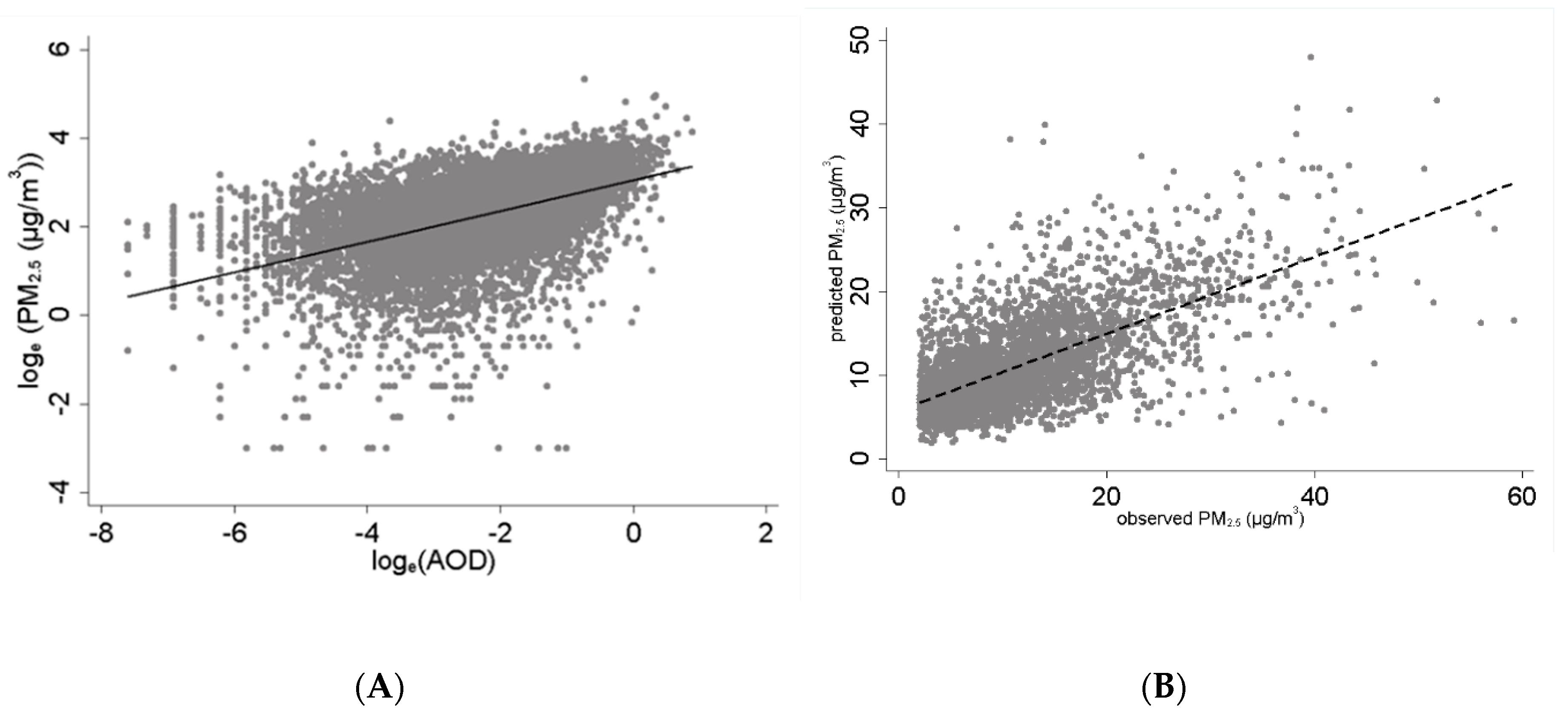
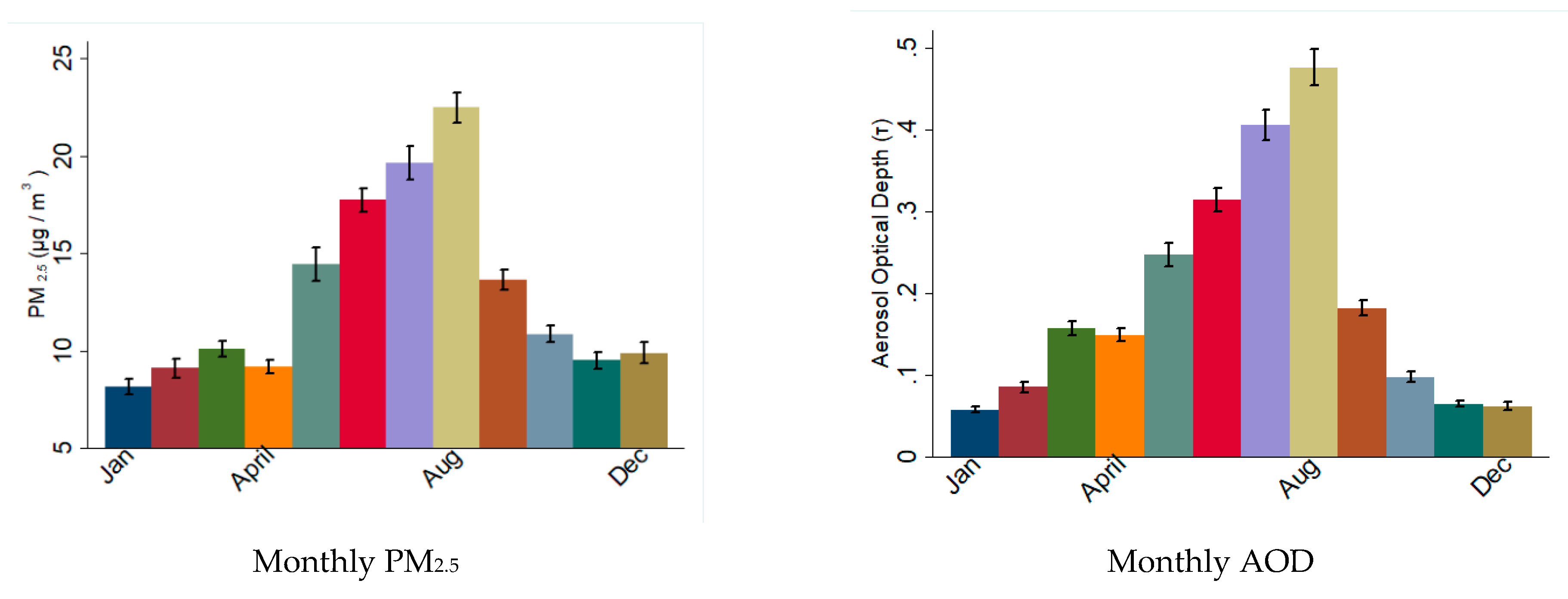
3.2. PM2.5 Exposure
3.3. PM2.5 and AOD during the Dust Outbreak
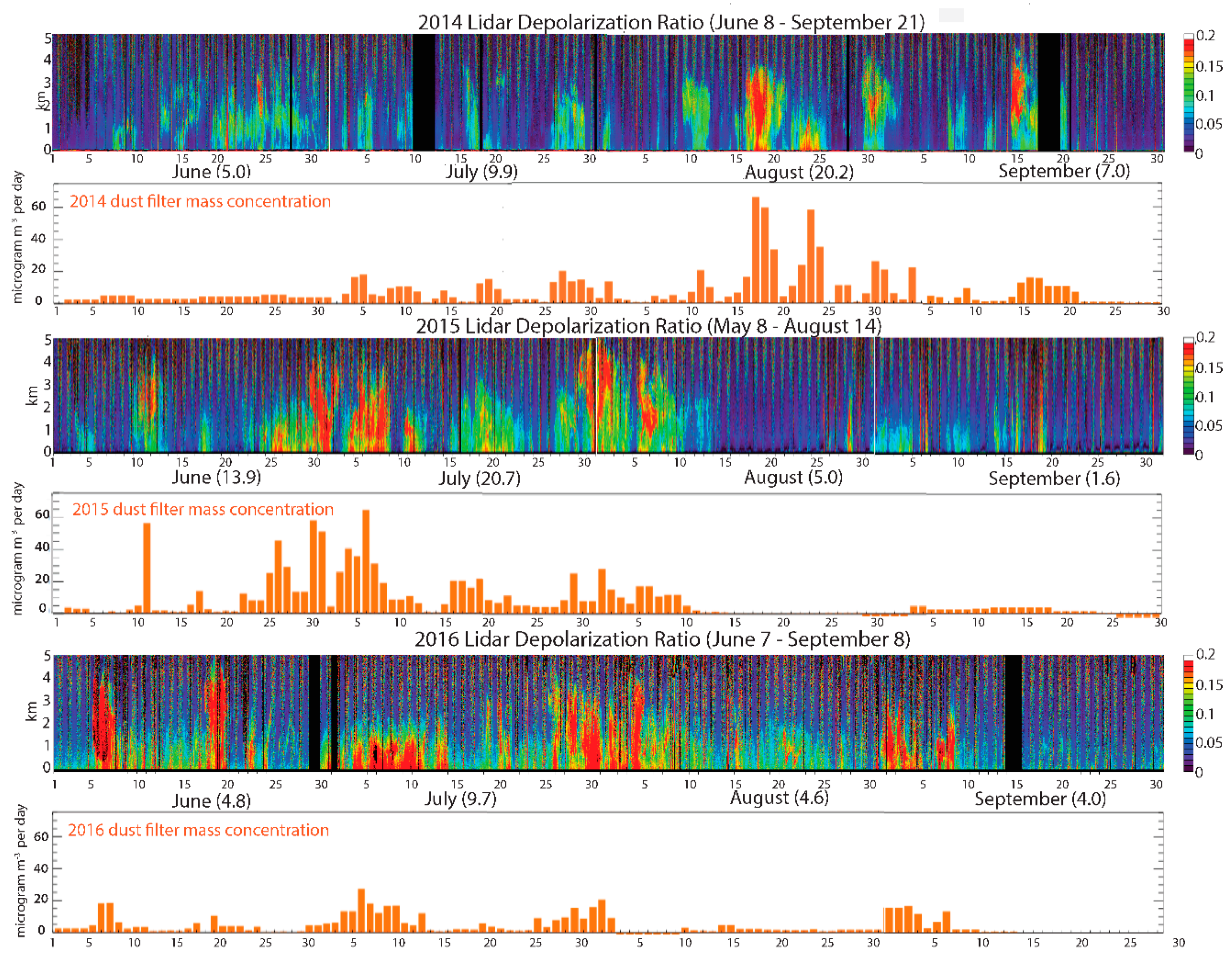
3.4. Dust Outbreak Duration and Intensity
3.5. AECOPD by PM2.5 and Dust Exposure
3.6. AECOPD and 15-Day Time-Lagged Dust Exposure
4. Discussion
5. Conclusions
Author Contributions
Funding
Acknowledgments
Conflicts of Interest
References
- Dransfield, M.T.; Kunisaki, K.M.; Strand, M.J.; Anzueto, A.; Bhatt, S.P.; Bowler, R.P.; Criner, G.J.; Curtis, J.L.; Hanania, N.A.; Nath, H.; et al. Acute exacerbations and lung function loss in smokers with and without chronic obstructive pulmonary disease. Am. J. Respir. Crit. Care Med. 2017, 195, 324–330. [Google Scholar] [CrossRef]
- Seemungal, T.A.; Donaldson, G.C.; Paul, E.A.; Bestall, J.C.; Jeffries, D.J.; Wedzicha, J.A. Effect of exacerbation on quality of life in patients with chronic obstructive pulmonary disease. Am. J. Respir. Crit. Care Med. 1998, 157, 1418–1422. [Google Scholar] [CrossRef]
- Soler-Cataluna, J.J.; Martinez-Garcia, M.A.; Roman Sanchez, P.; Salcedo, E.; Navarro, M.; Ochando, R. Severe acute exacerbations and mortality in patients with chronic obstructive pulmonary disease. Thorax 2005, 60, 925–931. [Google Scholar] [CrossRef]
- Wan, E.S. Examining genetic susceptibility in acute exacerbations of COPD. Thorax 2018, 73, 507–509. [Google Scholar] [CrossRef]
- Arbex, M.A.; de Souza Conceicao, G.M.; Cendon, S.P.; Arbex, F.F.; Lopes, A.C.; Moyses, E.P.; Santiago, S.L.; Saldiva, P.H.; Pereira, L.A.; Braga, A.L. Urban air pollution and chronic obstructive pulmonary disease-related emergency department visits. J. Epidemiol. Community Health 2009, 63, 777–783. [Google Scholar] [CrossRef]
- Choi, J.; Oh, J.Y.; Lee, Y.S.; Min, K.H.; Hur, G.Y.; Lee, S.Y.; Kang, K.H.; Shim, J.J. Harmful impact of air pollution on severe acute exacerbation of chronic obstructive pulmonary disease: Particulate matter is hazardous. Int. J. Chron. Obstruct. Pulmon. Dis. 2018, 13, 1053–1059. [Google Scholar] [CrossRef]
- Li, M.H.; Fan, L.C.; Mao, B.; Yang, J.W.; Choi, A.M.K.; Cao, W.J.; Xu, J.F. Short-term exposure to ambient fine particulate matter increases hospitalizations and mortality in COPD: A systematic review and meta-analysis. Chest 2016, 149, 447–458. [Google Scholar] [CrossRef]
- Kumar, N.; Liang, D.; Comellas, A.; Chu, A.D.; Abrams, T. Satellite-based PM concentrations and their application to COPD in Cleveland, OH. J. Expo. Sci. Environ. Epidemiol. 2013, 23, 637–646. [Google Scholar] [CrossRef]
- Sapey, E.; Stockley, R.A. COPD exacerbations. 2: Aetiology. Thorax 2006, 61, 250–258. [Google Scholar] [CrossRef]
- Ni, L.; Chuang, C.C.; Zuo, L. Fine particulate matter in acute exacerbation of COPD. Front. Physiol. 2015, 6, 294. [Google Scholar] [CrossRef]
- Ling, S.H.; van Eeden, S.F. Particulate matter air pollution exposure: Role in the development and exacerbation of chronic obstructive pulmonary disease. Int. J. Chron. Obstruct. Pulmon. Dis. 2009, 4, 233–243. [Google Scholar]
- Kuhlbusch, T.A.; John, A.C.; Quass, U. Sources and source contributions to fine particles. Biomark. Biochem. Indic. Expo. Response Susceptibility Chem. 2009, 14 (Suppl. 1), 23–28. [Google Scholar] [CrossRef]
- Mirsaeidi, M.; Motahari, H.; Taghizadeh Khamesi, M.; Sharifi, A.; Campos, M.; Schraufnagel, D.E. Climate change and respiratory infections. Ann. Am. Thorac. Soc. 2016, 13, 1223–1230. [Google Scholar] [CrossRef]
- Schweitzer, M.D.; Calzadilla, A.S.; Salamo, O.; Sharifi, A.; Kumar, N.; Holt, G.; Campos, M.; Mirsaeidi, M. Lung health in era of climate change and dust storms. Environ. Res. 2018, 163, 36–42. [Google Scholar] [CrossRef]
- Huneeus, N.; Schulz, M.; Balkanski, Y.; Griesfeller, J.; Prospero, J.; Kinne, S.; Bauer, S.; Boucher, O.; Chin, M.; Dentener, F.; et al. Global dust model intercomparison in AeroCom phase I. Atmos. Chem. Phys. 2011, 11, 7781–7816. [Google Scholar]
- Putaud, J.P.; Van Dingenen, R.; Alastuey, A.; Bauer, H.; Birmili, W.; Cyrys, J.; Flentje, H.; Fuzzi, S.; Gehrig, R.; Hansson, H.C.; et al. A European aerosol phenomenology-3: Physical and chemical characteristics of particulate matter from 60 rural, urban, and kerbside sites across Europe. Atmos. Environ. 2010, 44, 1308–1320. [Google Scholar]
- Prospero, J.M.; Collard, F.X.; Molinie, J.; Jeannot, A. Characterizing the annual cycle of African dust transport to the Caribbean Basin and South America and its impact on the environment and air quality. Glob. Biogeochem. Cycles 2014, 28, 757–773. [Google Scholar]
- Uno, I.; Eguchi, K.; Yumimoto, K.; Takemura, T.; Shimizu, A.; Uematsu, M.; Liu, Z.; Wang, Z.; Hara, Y.; Sugimoto, N. Asian dust transported one full circuit around the globe. Nat. Geosci. 2009, 2, 557–560. [Google Scholar] [CrossRef]
- Prospero, J.M. African dust in America. Geotimes 2001, 46, 24–27. [Google Scholar]
- Prospero, J.M. Long-range transport of mineral dust in the global atmosphere: Impact of African dust on the environment of the southeastern United States. Proc. Natl. Acad. Sci. USA 1999, 96, 3396–3403. [Google Scholar] [CrossRef]
- Prospero, J.M.; Olmez, I.; Ames, M. Al and Fe in PM 2.5 and PM 10 suspended particles in south-central Florida: The impact of the long range transport of African mineral dust. Water Air Soil Pollut. 2001, 125, 291–317. [Google Scholar] [CrossRef]
- WHO. WHO Air Quality Guidelines for Particulate Matter, Ozone, Nitrogen Dioxide and Sulfur Dioxide—Global Update 2005—Summary of Risk Assessment; World Health Organization: Geneva, Switzerland, 2006. [Google Scholar]
- Cardenas, M.; Vallejo, M.; Romano-Riquer, P.; Ruiz-Velasco, S.; Ferreira-Vidal, A.D.; Hermosillo, A.G. Personal exposure to PM2.5 air pollution and heart rate variability in subjects with positive or negative head-up tilt test. Environ. Res. 2008, 108, 1–6. [Google Scholar] [CrossRef]
- Snow, S.J.; De Vizcaya-Ruiz, A.; Osornio-Vargas, A.; Thomas, R.F.; Schladweiler, M.C.; McGee, J.; Kodavanti, U.P. The effect of composition, size, and solubility on acute pulmonary injury in rats following exposure to Mexico city ambient particulate matter samples. J. Toxicol. Environ. Health A 2014, 77, 1164–1182. [Google Scholar] [CrossRef]
- Goudarzi, G.; Daryanoosh, S.M.; Godini, H.; Hopke, P.K.; Sicard, P.; De Marco, A.; Rad, H.D.; Harbizadeh, A.; Jahedi, F.; Mohammadi, M.J.; et al. Health risk assessment of exposure to the Middle-Eastern Dust storms in the Iranian megacity of Kermanshah. Public Health 2017, 148, 109–116. [Google Scholar] [CrossRef]
- Ho, K.F.; Wu, K.C.; Niu, X.; Wu, Y.; Zhu, C.S.; Wu, F.; Cao, J.J.; Shen, Z.X.; Hsiao, T.C.; Chuang, K.J.; et al. Contributions of local pollution emissions to particle bioreactivity in downwind cities in China during Asian dust periods. Environ. Pollut. 2019, 245, 675–683. [Google Scholar] [CrossRef]
- Tam, W.W.; Wong, T.W.; Wong, A.H.; Hui, D.S. Effect of dust storm events on daily emergency admissions for respiratory diseases. Respirology 2012, 17, 143–148. [Google Scholar] [CrossRef]
- EPA. Air Data: Air Quality Data Collected at Outdoor Monitors Across the US. Available online: https://www.epa.gov/outdoor-air-quality-data (accessed on 12 February 2018).
- Levy, R.C.; Remer, L.A.; Mattoo, S.; Vermote, E.F.; Kaufman, Y.J. Second-generation operational algorithm: Retrieval of aerosol properties over land from inversion of Moderate Resolution Imaging Spectroradiometer spectral reflectance. J. Geophys. Res. Atmos. 2007, 112, D13211. [Google Scholar] [CrossRef]
- Kumar, N.; Chu, A.D.; Foster, A.D.; Peters, T.; Willis, R. Satellite remote sensing for developing time and space resolved estimates of ambient particulate in cleveland, OH. Aerosol. Sci. Technol. 2011, 45, 1090–1108. [Google Scholar] [CrossRef]
- Sinha, J.; Kumar, N. Mortality and air pollution effects of air quality interventions in delhi and Beijing. Front. Environ. Sci. 2019, 7, 1–10. [Google Scholar] [CrossRef]
- Liang, D.; Chen, J.; Kumar, N. Local Time Space Kriging. Available online: http://cran.r-project.org/web/packages/ltsk/ (accessed on 10 October 2014).
- Zuidema, P.; Alvarez, C.; Kramer, S.J.; Custals, L.; Izaguirre, M.; Sealy, P.; Prospero, J.M.; Blades, E. Is summer african dust arriving earlier to barbados? The updated long-term in situ dust mass concentration time series from ragged point, barbados, and Miami, Florida. Bull. Am. Meteorol. Soc. 2019, 100, 1981–1986. [Google Scholar]
- Kramer, S.J.; Alvarez, C.; Barkley, A.; Colarco, P.R.; Custals, L.; Delgadillo, R.; Gaston, C.; Govindaraju, R.; Zuidema, P. Apparent dust size discrepancy in aerosol renalysis in north African dust after long-range transport. Atmos. Chem. Phys. 2020. [Google Scholar] [CrossRef]
- Delgadillo, R.; Voss, K.J.; Zuidema, P. Characteristics of optically thin coastal florida cumuli derived from surface-based lidar measurements. J. Geophys. Res. Atmos. 2018, 123, 10591–10605. [Google Scholar]
- STATA. STATA/MP 14.2—Data Analysis and Statistical Software; Stata Corp LP: College Station, TX, USA, 2017. [Google Scholar]
- EPA. National Ambient Air Quality Standards (NAAQS); The Environmental Protection Agency: Research Traingle Park, NC, USA, 2014. [Google Scholar]
- Kanatani, K.T.; Ito, I.; Al-Delaimy, W.K.; Adachi, Y.; Mathews, W.C.; Ramsdell, J.W.; Toyama Asian Desert Dust; Asthma Study Team. Desert dust exposure is associated with increased risk of asthma hospitalization in children. Am. J. Respir. Crit. Care Med. 2010, 182, 1475–1481. [Google Scholar] [CrossRef]
- Ueda, K.; Nitta, H.; Odajima, H. The effects of weather, air pollutants, and Asian dust on hospitalization for asthma in Fukuoka. Environ. Health Prev. Med. 2010, 15, 350–357. [Google Scholar] [CrossRef]
- Chan, C.C.; Chuang, K.J.; Chen, W.J.; Chang, W.T.; Lee, C.T.; Peng, C.M. Increasing cardiopulmonary emergency visits by long-range transported Asian dust storms in Taiwan. Environ. Res. 2008, 106, 393–400. [Google Scholar] [CrossRef]
- Lorentzou, C.; Kouvarakis, G.; Kozyrakis, G.V.; Kampanis, N.A.; Trahanatzi, I.; Fraidakis, O.; Tzanakis, N.; Kanakidou, M.; Agouridakis, P.; Notas, G. Extreme desert dust storms and COPD morbidity on the island of Crete. Int. J. Chronic Obstr. Pulm. Dis. 2019, 14, 1763–1768. [Google Scholar] [CrossRef]
- Middleton, N.; Tozer, P.; Tozer, B. Sand and dust storms: Underrated natural hazards. Disasters 2019, 43, 390–409. [Google Scholar] [CrossRef]
- Boy, J.; Wilcke, W. Tropical Andean forest derives calcium and magnesium from Saharan dust. Glob. Biogeochem. Cycle 2008, 22. [Google Scholar] [CrossRef]
- Swap, R.; Garstang, M.; Greco, S.; Talbot, R.; Kallberg, P. Saharan dust in the Amazon Basin. Tellus B 1992, 44, 133–149. [Google Scholar]
- Crooks, J.L.; Cascio, W.E.; Percy, M.S.; Reyes, J.; Neas, L.M.; Hilborn, E.D. The association between dust storms and daily non-accidental mortality in the United States, 1993–2005. Environ. Health Perspect. 2016, 124, 1735–1743. [Google Scholar] [CrossRef]
- Lee, J.; Jung, H.M.; Kim, S.K.; Yoo, K.H.; Jung, K.S.; Lee, S.H.; Rhee, C.K. Factors associated with chronic obstructive pulmonary disease exacerbation, based on big data analysis. Sci. Rep. 2019, 9, 6679. [Google Scholar] [CrossRef]
- Tseng, C.M.; Chen, Y.T.; Ou, S.M.; Hsiao, Y.H.; Li, S.Y.; Wang, S.J.; Yang, A.C.; Chen, T.J.; Perng, D.W. The effect of cold temperature on increased exacerbation of chronic obstructive pulmonary disease: A nationwide study. PLoS ONE 2013, 8, e57066. [Google Scholar] [CrossRef]
- Middleton, N. Desert dust hazards: A global review. Aeolian Res. 2017, 24, 53–63. [Google Scholar]
- Leys, J.; Heidenreich, S.; Strong, K.; McTanish, G.; Quigley, S. PM10 concentrations and mass transport during “Red Dawn”—Sydney 23 September 2009. Aeolian Res. 2011, 3, 327–342. [Google Scholar]
- Morman, S.A.; Plumlee, G.S. Dust and human health. In Mineral Dust; Springer: Berlin, Germany, 2014; pp. 385–409. [Google Scholar]
- Tong, D.Q.; Wang, J.X.L.; Gill, T.E.; Lei, H.; Wang, B.Y. Intensified dust storm activity and Valley fever infection in the southwestern United States. Geophys. Res. Lett. 2017, 44, 4304–4312. [Google Scholar]
- Woringer, M.; Martiny, N.; Porgho, S.; Bicaba, B.W.; Bar-Hen, A.; Mueller, J.E. Atmospheric dust, early cases, and localized meningitis epidemics in the african meningitis belt: An analysis using high spatial resolution data. Environ. Health Perspect. 2018, 126, 97002. [Google Scholar] [CrossRef]
- Kashima, S.; Yorifuji, T.; Suzuki, E. Are people with a history of disease more susceptible to a short-term exposure to asian dust?: A case-crossover study among the Elderly in Japan. Epidemiology 2017, 28 (Suppl. 1), S60–S66. [Google Scholar] [CrossRef]
- Kotsyfakis, M.; Zarogiannis, S.G.; Patelarou, E. The health impact of Saharan dust exposure. Int. J. Occup. Med. Environ. Health 2019. [Google Scholar] [CrossRef]
- Perez, L.; Tobias, A.; Querol, X.; Kunzli, N.; Pey, J.; Alastuey, A.; Viana, M.; Valero, N.; Gonzalez-Cabre, M.; Sunyer, J. Coarse particles from Saharan dust and daily mortality. Epidemiology 2008, 19, 800–807. [Google Scholar] [CrossRef]
- Sternberg, T.; Edwards, M. Desert dust and health: A central asian review and steppe case study. Int. J. Environ. Res. Public Health 2017, 14, 1342. [Google Scholar] [CrossRef]
- Rizzolo, J.A.; Barbosa, C.G.G.; Borillo, G.C.; Godoi, A.F.L.; Souza, R.A.F.; Andreoli, R.V.; Manzi, A.O.; Sa, M.O.; Alves, E.G.; Pohlker, C.; et al. Soluble iron nutrients in Saharan dust over the central Amazon rainforest. Atmos. Chem. Phys. 2017, 17, 2673–2687. [Google Scholar]
- Prospero, J.M.; Blades, E.; Mathison, G.; Naidu, R. Interhemispheric transport of viable fungi and bacteria from Africa to the Caribbean with soil dust. Aerobiologia 2005, 21, 1–19. [Google Scholar]
- Bozlaker, A.; Prospero, J.M.; Fraser, M.P.; Chellam, S. Quantifying the contribution of long-range saharan dust transport on particulate matter concentrations in Houston, Texas, using detailed elemental analysis. Environ. Sci. Technol. 2013, 47, 10179–10187. [Google Scholar]
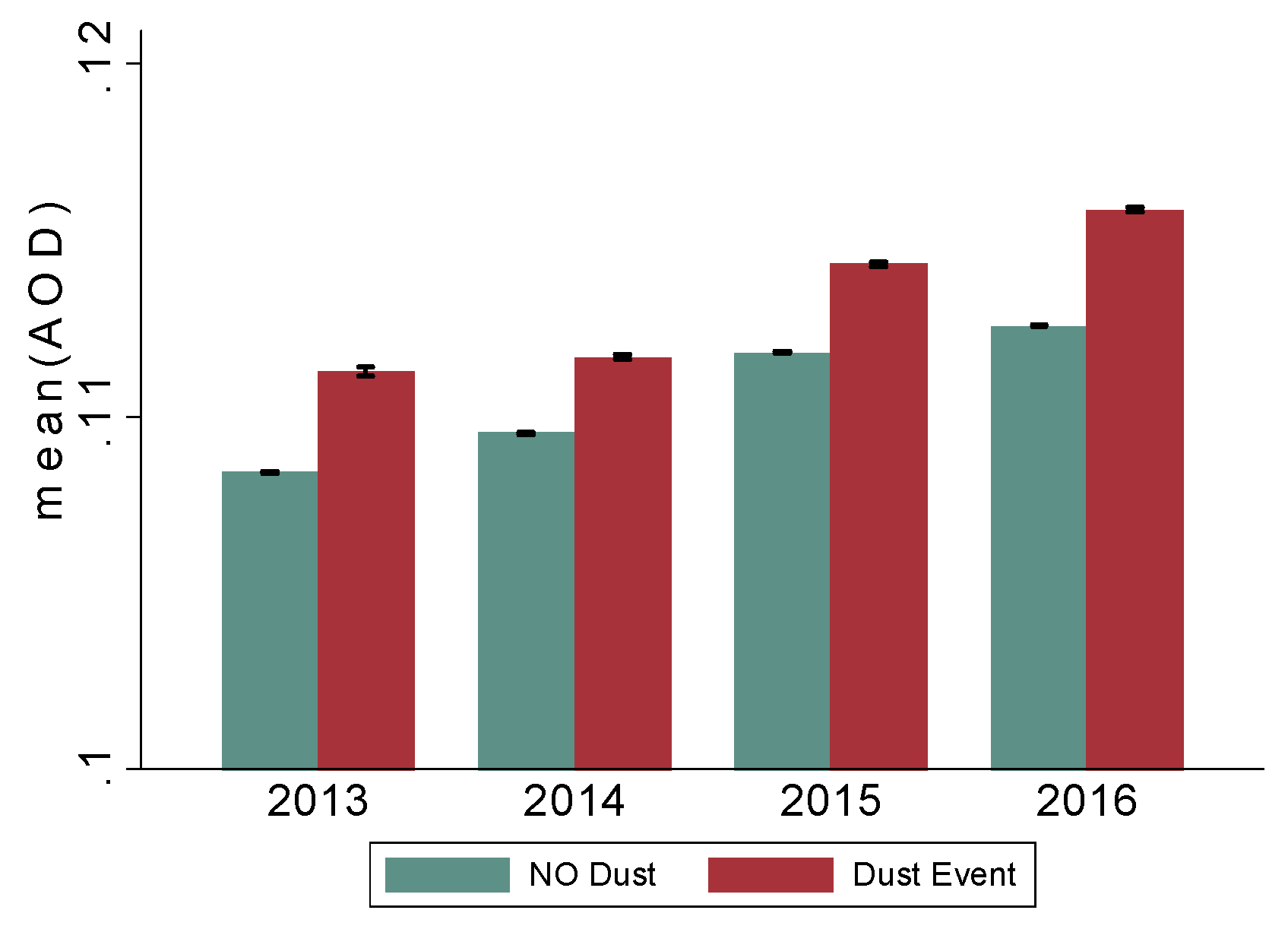
| Variables | Regression Coefficients (95% Confidence Interval in Parenthesis) |
|---|---|
| AOD | 21.44 *** |
| (19.62–23.26) | |
| Season category (0 = October to March, 1 = otherwise) | 0.64 *** |
| (0.17–1.11) | |
| Factor of Meteorological Conditions (dominant variables atmospheric temperature and dew point) | 1.85 *** |
| (1.58–2.12) | |
| Factor of Meteorological Conditions (relative humidity) | –0.69 *** |
| (−0.89–−0.48) | |
| Constant | 7.17 *** |
| (6.81–7.52) | |
| Observations | 4398 |
| R-squared | 0.45 |
| Variable | Factor 1 * | Factor 2 ** | Uniqueness |
|---|---|---|---|
| Wind speed (m/s) | 0.00437 | −0.03431 | 0.7825 |
| Ceiling Height (m) | −0.00381 | 0.02124 | 0.7487 |
| Visibility (m) | 0.00656 | −0.03306 | 0.7531 |
| Dry Bulb Temperature °F | 0.60116 | −0.62288 | 0.0286 |
| Dew Point (°F) | 0.43451 | 0.62488 | 0.0263 |
| Mean sea level pressure (mb) | −0.00650 | −0.00624 | 0.7760 |
| Relative humidity (%) | −0.00762 | 0.57763 | 0.0734 |
| % Variance explained | 55.46 | 38.23 |
| ALL | Subjects without AECOPD * (Controls) | Subjects with at Least 1 AECOPD * | p-Value | |
|---|---|---|---|---|
| N | 296 | 194 | 102 | |
| Age (years) ± 95% confidence interval (CI) | 70.0 ± 8.7 | 69.8 ± 8.9 | 70.3 ± 8.5 | 0.48 |
| Concomitant asthma (%) | 33 (11.1) | 13.1 | 9.4 | 0.33 |
| Number of exacerbations during 4-year study period ± 95% CI | 1.99 ± 3.9 | - | 2.7 ± 5.0 | - |
| Post bronchodilator lung function values | ||||
| FEV1 (L), ± 95% CI | 1.6 ± 1.2 | 1.81 ± 1.7 | 1.42 ± 0.5 | 0.015 |
| FEV1 (%), ± 95% CI | 46.0 ± 17.0 | 48.9 ± 18.0 | 43.2 ±15.5 | 0.006 |
| FVC (L), ± 95% CI | 2.9 ± 0.7 | 3.1 ± 0.7 | 2.8 ± 0.7 | 0.001 |
| FVC (%), ± 95% CI | 68.9 ± 16.3 | 71.3 ± 15.4 | 66.6 ± 16.8 | 0.019 |
| FEV1/FVC (%), ± 95% CI | 51.4 ± 13.4 | 52.6 ± 13.6 | 50.3 ± 13.3 | 0.15 |
| DLCO (%),± 95% CI | 53.1 ± 15.3 | 53.9 ± 14.7 | 52.2 ± 15.8 | 0.37 |
| GROUP | AECOPD Events | Number of Subjects | Events in Miami Catchment Area | Total | |
|---|---|---|---|---|---|
| NO | YES | ||||
| Controls | 0 | 194 | 28 | 166 | 194 |
| Cases | 1 | 42 | 6 | 36 | 42 |
| 2 | 19 | 4 | 34 | 38 | |
| ≥3 | 41 | 6 | 227 | 233 | |
| Total | 296 | 44 | 463 | 507 | |
| During No Dust Event | Dust Event Intensity * | Total | |||
|---|---|---|---|---|---|
| ≤0.10 (Low) | 0.11–0.15 (Medium) | ≥0.15 (High) | |||
| Miami Catchment (n = 1,322,344) | |||||
| Aerosol Optical Depth (AOD) | 0.162 | 0.198 | 0.246 | 0.241 | 0.168 |
| (0.161–0.162) | (0.196–0.199) | (0.244–0.247) | (0.240–0.242) | (0.168–0.169) | |
| Surface Temperature (°C) | 21.0 | 22.6 | 22.3 | 23.1 | 21.2 |
| (21.0–21.0) | (22.5–22.6) | (22.3–22.3) | (23.1–23.1) | (21.2–21.2) | |
| Dew Point (°C) | 17.6 | 19.3 | 18.7 | 19.9 | 17.8 |
| (17.6–17.6) | (19.3–19.4) | (18.7–18.8) | (19.9–19.9) | (17.8–17.8) | |
| Relative Humidity (%) | 77.6 | 78.4 | 76.9 | 78.5 | 77.7 |
| (77.6–77.6) | (78.3–78.5) | (76.8–76.9) | (78.4–78.5) | (77.6–77.7) | |
| Particulate Matter ≤ 2.5 µm (PM2.5) (µg/m3) | 10.3 | 12.0 | 12.9 | 13.1 | 10.5 |
| (10.3–10.3) | (11.9–12.0) | (12.9–13.0) | (13.0–13.1) | (10.5–10.5) | |
| Florida excluding Miami Catchment Area (n = 7,648,441) | |||||
| Aerosol Optical Depth (AOD) | 0.124 | 0.175 | 0.201 | 0.189 | 0.130 |
| (0.124–0.124) | (0.175–0.176) | (0.201–0.202) | (0.189–0.189) | (0.130–0.130) | |
| Surface Temperature (°C) | 21.0 | 22.2 | 21.5 | 22.4 | 21.1 |
| (21.0–21.0) | (22.1–22.2) | (21.5–21.5) | (22.4–22.4) | (21.1–21.1) | |
| Dew Point (°C) | 17.6 | 18.9 | 18.1 | 19.2 | 17.7 |
| (17.6–17.6) | (18.9–18.9) | (18.1–18.1) | (19.2–19.2) | (17.7–17.7) | |
| Relative Humidity (%) | 77.4 | 78.2 | 77.7 | 78.4 | 77.4 |
| (77.4–77.4) | (78.1–78.2) | (77.7–77.8) | (78.4–78.5) | (77.4–77.5) | |
| Particulate Matter ≤ 2.5 µm (PM2.5) (µg/m3) | 9.5 | 11.4 | 11.7 | 11.7 | 9.6 |
| (9.5–9.5) | (11.4–11.4) | (11.7–11.7) | (11.7–11.7) | (9.6–9.6) | |
| Florida (n = 8,970,785) | |||||
| Aerosol Optical Depth (AOD) | 0.130 | 0.179 | 0.209 | 0.197 | 0.136 |
| (0.130–0.130) | (0.178–0.179) | (0.209–0.210) | (0.197–0.197) | (0.135–0.136) | |
| Surface Temperature (°C) | 21.0 | 22.2 | 21.6 | 22.5 | 21.1 |
| (21.0–21.0) | (22.2–22.2) | (21.6–21.6) | (22.5–22.5) | (21.1–21.1) | |
| Dew Point (°C) | 17.6 | 19.0 | 18.2 | 19.3 | 17.7 |
| (17.6–17.6) | (19.0–19.0) | (18.2–18.3) | (19.3–19.3) | (17.7–17.7) | |
| Relative Humidity (%) | 77.4 | 78.2 | 77.6 | 78.4 | 77.5 |
| (77.4–77.4) | (78.2–78.2) | (77.5–77.6) | (78.4–78.5) | (77.5–77.5) | |
| Particulate Matter ≤ 2.5 µm (PM2.5) (µg/m3) | 9.6 | 11.5 | 11.9 | 11.9 | 9.8 |
| (9.6–9.6) | (11.4–11.5) | (11.9–11.9) | (11.9–11.9) | (9.8–9.8) | |
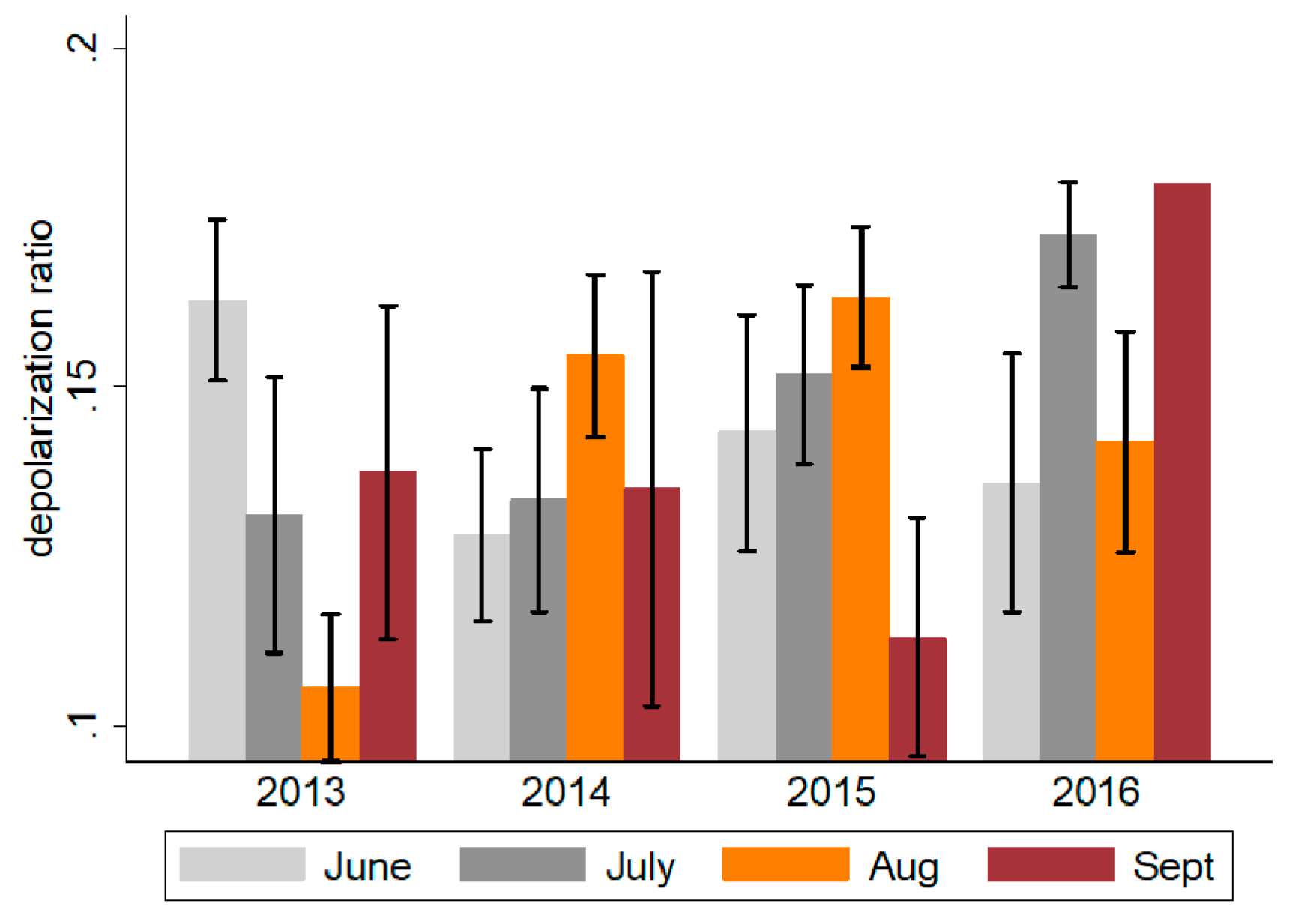
| 2013 | 2014 | 2015 | 2016 | |
|---|---|---|---|---|
| June | 0.16 | 0.13 | 0.14 | 0.14 |
| (0.15–0.17) | (0.12–0.14) | (0.13–0.16) | (0.12–0.15) | |
| 7 days | 16 days | 15 days | 17 days | |
| July | 0.13 | 0.13 | 0.15 | 0.17 |
| (0.11–0.15) | (0.12–0.15) | (0.14–0.17) | (0.16–0.18) | |
| 9 days | 9 days | 20 days | 23 days | |
| August | 0.11 | 0.15 | 0.16 | 0.14 |
| (0.09–0.12) | (0.14–0.17) | (0.15–0.17) | (0.13–0.16) | |
| 9 days | 17 days | 9 days | 20 days | |
| September | 0.14 | 0.14 | 0.11 | 0.18 |
| (0.11–0.16) | (0.10–0.17) | (0.10–0.13) | (0.18–0.18) | |
| 4 days | 6 days | 10 days | 8 days | |
| Total | 0.13 | 0.14 | 0.14 | 0.16 |
| (0.12–0.14) | (0.13–0.15) | (0.14–0.15) | (0.15–0.16) | |
| 29 days | 48 days | 54 days | 68 days |
| Variables | 2+ AECOPD | |||||
|---|---|---|---|---|---|---|
| Model 1 | Model 2 | Model 3 | Model 4 | Model 5 | Model 6 | |
| Age (year) | 1.002 | 1.034 *** | 1.040 *** | 1.001 | 1.038 *** | 1.001 |
| (0.970–1.035) | (1.009–1.059) | (1.014–1.066) | (0.968–1.035) | (1.012–1.065) | (0.968–1.035) | |
| Asthma status (YES = 1, 0 otherwise) | 0.842 | 1.405 | 1.6 | 0.907 | 1.548 | 1.123 |
| (0.264–2.689) | (0.717–2.756) | (0.793–3.224) | (0.278–2.964) | (0.756–3.172) | (0.349–3.611) | |
| Smoking status (1 = Active, 0 otherwise) | 2.110 * | 1.942 ** | 1.998 ** | 2.051 | 2.007 ** | 2.112 |
| (0.891–4.996) | (1.069–3.529) | (1.087–3.671) | (0.849–4.952) | (1.066–3.779) | (0.831–5.367) | |
| Lung function (FEV1/FVC) | 1.008 | 1.002 | 1 | 1.006 | 0.998 | 0.999 |
| (0.980–1.036) | (0.982–1.021) | (0.981–1.020) | (0.978–1.035) | (0.978–1.018) | (0.972–1.028) | |
| One-day lag PM2.5 (µg/m3) | 1.139 *** | 1.124 *** | 1.122 *** | |||
| (1.083–1.197) | (1.068–1.184) | (1.061–1.185) | ||||
| One-day lag ambient temperature (°C) | 1.121 *** | 1.059 | 1.103 ** | 1.062 | ||
| (1.033–1.217) | (0.960–1.169) | (1.015–1.198) | (0.961–1.173) | |||
| One-day lag dust exposure (LIDAR intensity) | 5.777 *** | 5.222 *** | 4.955 *** | |||
| (2.084–16.010) | (2.077–13.126) | (1.826–13.449) | ||||
| Constant | 0.028 ** | 0.002 *** | 0.022 *** | 0.010 *** | 0.002 *** | 0.011 ** |
| (0.001–0.525) | (0.000–0.036) | (0.003–0.165) | (0.000–0.327) | (0.000–0.039) | (0.000–0.385) | |
| Observations | 169 | 308 | 308 | 169 | 308 | 169 |
| Variables | ≥2 AECOPD | |||||
|---|---|---|---|---|---|---|
| Model 1 | Model 2 | Model 3 | Model 4 | Model 5 | Model 6 | |
| Age (year) | 0.999 | 1.034 ** | 1.038 *** | 0.996 | 1.035 ** | 0.994 |
| (0.968–1.032) | (1.005–1.064) | (1.010–1.066) | (0.961–1.032) | (1.006–1.065) | (0.960–1.030) | |
| Asthma status (YES = 1, 0 = otherwise) | 1.213 | 1.931 | 2.201 ** | 1.587 | 2.028 * | 1.78 |
| (0.374–3.937) | (0.869–4.289) | (1.077–4.498) | (0.426–5.910) | (0.903–4.558) | (0.480–6.603) | |
| Smoking status (1 = Active, 0 = otherwise) | 1.795 | 1.882 * | 1.784 * | 1.749 | 1.827 * | 1.714 |
| (0.761–4.232) | (0.955–3.709) | (0.953–3.341) | (0.692–4.422) | (0.916–3.644) | (0.678–4.330) | |
| Lung function (FEV1/FVC) | 1.005 | 0.998 | 1.001 | 1.002 | 0.997 | 0.998 |
| (0.979–1.032) | (0.977–1.020) | (0.981–1.021) | (0.974–1.031) | (0.975–1.020) | (0.970–1.027) | |
| One-day lag PM2.5 (µg/m3) | 1.146 *** | 1.111 *** | 1.109 *** | |||
| (1.090–1.205) | (1.050–1.175) | (1.045–1.176) | ||||
| One-day lag ambient temperature (°C) | 1.315 *** | 1.214 *** (1.096–1.344) | 1.301 *** | 1.214 *** | ||
| (1.174–1.473) | (1.161–1.457) | (1.096–1.345) | ||||
| One-day lag dust exposure (LIDAR intensity) | 1.741 *** | 1.581 ** | 1.808 ** | |||
| (1.176–2.578) | (1.041–2.401) | (1.003–3.261) | ||||
| Constant | 0.025 ** | 0.000 *** | 0.016 *** | 0.000 *** | 0.000 *** | 0.001 *** |
| (0.001–0.541) | (0.000–0.001) | (0.002–0.139) | (0.000–0.030) | (0.000–0.001) | (0.000–0.037) | |
| Observations | 169 | 308 | 308 | 169 | 308 | 169 |
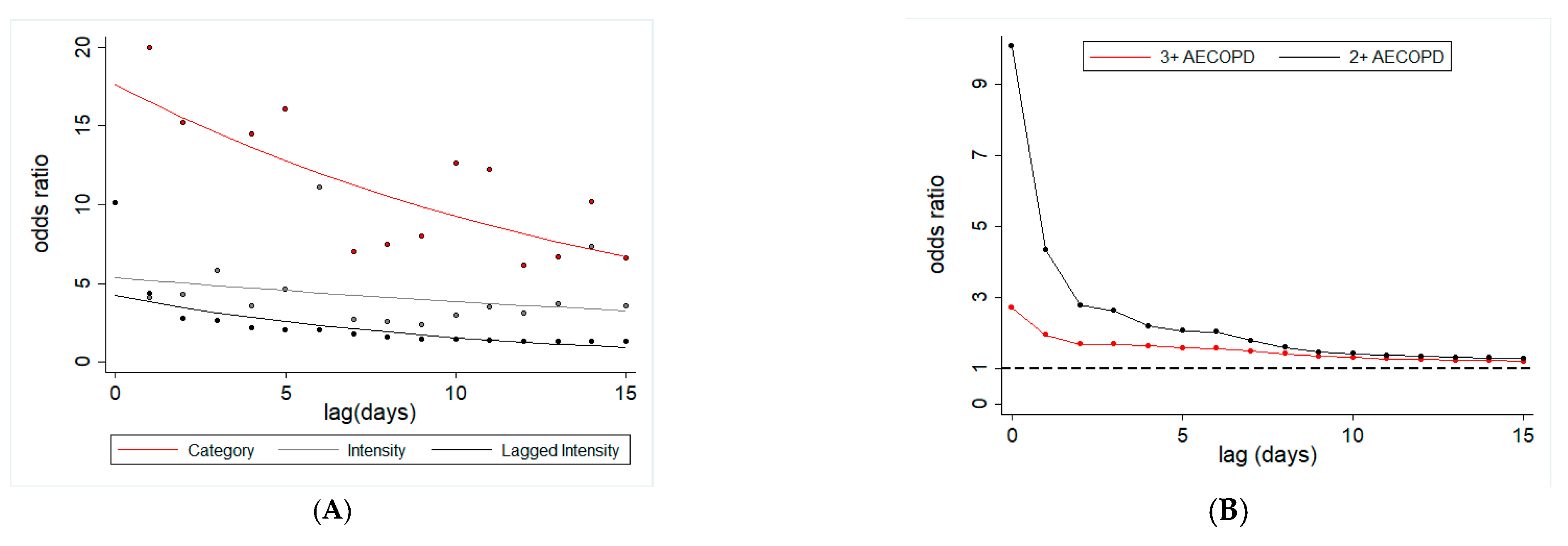
| Lag (day) | Odds Ratio for AECOPD | |||||
|---|---|---|---|---|---|---|
| ≥2 AECOPD | ≥3AECOPD | |||||
| Dust Event (0 = Yes, 1 = No) | Dust Intensity | Distributed Lag | Dust Event (0 = Yes, 1 = No) | Dust Intensity | Distributed Lag | |
| 0 | NA | 10.074 *** | 10.074 *** | 7.781 *** | 2.717 *** | 2.717 *** |
| (2.241–45.292) | (2.241–45.292) | (2.274–26.621) | (1.460–5.057) | (1.460–5.057) | ||
| 1 | 19.930 *** | 4.116 *** | 4.340 *** | 5.859 *** | 2.193 *** | 1.948 *** |
| (2.621–151.548) | (1.700–9.963) | (1.634–11.529) | (1.991–17.242) | (1.373–3.501) | (1.259–3.014) | |
| 2 | 15.162 ** | 4.269 *** | 2.791 ** | 5.959 *** | 2.589 *** | 1.684 *** |
| (1.895–121.291) | (1.502–12.131) | (1.247–6.247) | (1.675–21.204) | (1.496–4.482) | (1.238–2.291) | |
| 3 | NA | 5.800 *** | 2.632 ** | 21.066 *** | 3.603 *** | 1.685 *** |
| (2.152–15.634) | (1.225–5.654) | (2.850–155.729) | (1.825–7.114) | (1.239–2.292) | ||
| 4 | 14.443 *** | 3.578 *** | 2.201 *** | 19.903 *** | 3.566 *** | 1.639 *** |
| (1.921–108.593) | (1.489–8.597) | (1.321–3.667) | (2.649–149.532) | (1.733–7.339) | (1.276–2.106) | |
| 5 | 16.062 *** | 4.585 *** | 2.065 *** | 10.155 *** | 3.800 *** | 1.586 *** |
| (2.154–119.792) | (1.600–13.139) | (1.244–3.430) | (2.259–45.661) | (1.648–8.765) | (1.245–2.021) | |
| 6 | NA | 11.080 *** | 2.032 *** | 20.757 *** | 5.433 *** | 1.570 *** |
| (2.084–58.915) | (1.247–3.310) | (2.571–167.581) | (1.721–17.153) | (1.229–2.007) | ||
| 7 | 7.021 *** | 2.714 ** | 1.781 *** | 5.862 *** | 2.570 *** | 1.490 *** |
| (1.611–30.601) | (1.160–6.354) | (1.188–2.671) | (1.661–20.692) | (1.282–5.150) | (1.186–1.873) | |
| 8 | 7.475 *** | 2.558 ** | 1.601 *** | 6.226 *** | 2.487 *** | 1.416 *** |
| (1.725–32.395) | (1.218–5.370) | (1.131–2.264) | (1.790–21.654) | (1.316–4.701) | (1.150–1.744) | |
| 9 | 7.956 *** | 2.345 *** | 1.461 *** | 6.646 *** | 2.178 *** | 1.346 *** |
| (1.843–34.346) | (1.272–4.322) | (1.118–1.911) | (1.918–23.037) | (1.250–3.794) | (1.127–1.609) | |
| 10 | 12.621 ** | 2.936 ** | 1.416 *** | 7.408 ** | 2.352 ** | 1.313 *** |
| (1.541–103.354) | (1.068–8.070) | (1.124–1.784) | (1.508–36.396) | (1.080–5.119) | (1.118–1.543) | |
| 11 | 12.186 ** | 3.477 ** | 1.376 *** | 4.442 ** | 2.249 ** | 1.277 *** |
| (1.558–95.288) | (1.058–11.423) | (1.117–1.695) | (1.160–17.019) | (1.100–4.597) | (1.105–1.476) | |
| 12 | 6.153 ** | 3.127 ** | 1.343 *** | 4.986 ** | 2.502 ** | 1.256 *** |
| (1.393–27.186) | (1.284–7.614) | (1.112–1.623) | (1.389–17.897) | (1.184–5.288) | (1.096–1.440) | |
| 13 | 6.635 ** | 3.660 ** | 1.315 *** | 5.409 *** | 2.885 ** | 1.237 *** |
| (1.507–29.212) | (1.357–9.868) | (1.105–1.566) | (1.515–19.309) | (1.269–6.560) | (1.086–1.409) | |
| 14 | 10.165 ** | 7.322 ** | 1.300 *** | 6.164 ** | 3.366 ** | 1.222 *** |
| (1.317–78.442) | (1.171–45.791) | (1.103–1.533) | (1.314–28.903) | (1.194–9.487) | (1.079–1.384) | |
| 15 | NA | 3.553 ** | 1.282 *** | 5.495 *** | 2.823 *** | 1.208 *** |
| (1.343–9.400) | (1.090–1.507) | (1.566–19.280) | (1.291–6.173) | (1.069–1.364) | ||
© 2020 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Gutierrez, M.P.; Zuidema, P.; Mirsaeidi, M.; Campos, M.; Kumar, N. Association between African Dust Transport and Acute Exacerbations of COPD in Miami. J. Clin. Med. 2020, 9, 2496. https://doi.org/10.3390/jcm9082496
Gutierrez MP, Zuidema P, Mirsaeidi M, Campos M, Kumar N. Association between African Dust Transport and Acute Exacerbations of COPD in Miami. Journal of Clinical Medicine. 2020; 9(8):2496. https://doi.org/10.3390/jcm9082496
Chicago/Turabian StyleGutierrez, Miguel Pardinas, Paquita Zuidema, Mehdi Mirsaeidi, Michael Campos, and Naresh Kumar. 2020. "Association between African Dust Transport and Acute Exacerbations of COPD in Miami" Journal of Clinical Medicine 9, no. 8: 2496. https://doi.org/10.3390/jcm9082496
APA StyleGutierrez, M. P., Zuidema, P., Mirsaeidi, M., Campos, M., & Kumar, N. (2020). Association between African Dust Transport and Acute Exacerbations of COPD in Miami. Journal of Clinical Medicine, 9(8), 2496. https://doi.org/10.3390/jcm9082496





