Importance of Footwear Outsole Rigidity in Improving Spatiotemporal Parameters in Patients with Diabetes and Previous Forefoot Ulcerations
Abstract
1. Introduction
2. Methods
2.1. Subjects
2.2. Clinical Evaluation
2.3. Shoe Conditions
2.4. Experimental Procedures
2.4.1. Kinematic Analyses
2.4.2. Comfort Assessment
2.4.3. Data Analyses
2.5. Main Outcome
2.6. Secondary Outcomes
2.7. Statistical Analyses
3. Results
4. Discussion
5. Conclusions
Author Contributions
Funding
Acknowledgments
Conflicts of Interest
References
- Armstrong, D.G.; Boulton, A.J.M.; Bus, S.A. Diabetic Foot Ulcers and Their Recurrence. N. Engl. J. Med. 2017, 376, 2367–2375. [Google Scholar] [CrossRef] [PubMed]
- Lavery, L.A.; Armstrong, D.G.; Wunderlich, R.P.; Tredwell, J.; Boulton, A.J. Diabetic foot syndrome: Evaluating the prevalence and incidence of foot pathology in Mexican Americans and non-Hispanic whites from a diabetes disease management cohort. Diabetes Care 2003, 26, 1435–1438. [Google Scholar] [CrossRef] [PubMed]
- Walsh, J.W.; Hoffstad, O.J.; Sullivan, M.O.; Margolis, D.J. Association of diabetic foot ulcer and death in a population-based cohort from the United Kingdom. Diabet. Med. 2016, 33, 1493–1498. [Google Scholar] [CrossRef]
- Lavery, L.A.; Hunt, N.A.; Ndip, A.; Lavery, D.C.; van Houtum, W.; Boulton, A.J. Impact of chronic kidney disease on survival after amputation in individuals with diabetes. Diabetes Care 2010, 33, 2365–2369. [Google Scholar] [CrossRef] [PubMed]
- American Diabetes Association. Economic costs of diabetes in the U.S. in 2017. Diabetes Care 2018, 41, 917–928. [Google Scholar] [CrossRef] [PubMed]
- Prompers, L.; Huijberts, M.; Apelqvist, J.; Jude, E.; Piaggesi, A.; Bakker, K.; Edmons, M.; Holstein, P.; Jirkovska, A.; Mauricio, D.; et al. High prevalence of ischaemia, infection and serious comorbidity in patients with diabetic foot disease in Europe. Baseline results from the Eurodiale study. Diabetologia 2007, 50, 18–25. [Google Scholar] [CrossRef]
- Van Schie, C.H.; Vermigli, C.; Carrington, A.L.; Boulton, A. Muscle weakness and foot deformities in diabetes: Relationship to neuropathy and foot ulceration in caucasian diabetic men. Diabetes Care 2004, 27, 1668–1673. [Google Scholar] [CrossRef]
- Van Netten, J.J.; Lazzarini, P.A.; Armstrong, D.G.; Bus, S.A.; Fitridge, R.; Harding, K.; Kinnear, E.; Mälone, M.; Menz, H.B.; Perrin, B.M.; et al. Diabetic Foot Australia guideline on footwear for people with diabetes. J. Foot Ankle Res. 2018, 11, 2. [Google Scholar] [CrossRef]
- Bus, S.A.; Waaijman, R.; Arts, M.; de Haart, M.; Busch-Westbroek, T.; van Baal, J.; Nollet, F. Effect of custom-made footwear on foot ulcer recurrence in diabetes: A multicenter randomized controlled trial. Diabetes Care 2013, 36, 4109–4116. [Google Scholar] [CrossRef]
- Bus, S.A.; Monteiro-Soares, M.; Rasmussen, A.; Raspovic, A.; Sacco, I.; van Netten, J.J. International Working Group on the Diabetic Foot (IWGDF). Guidelines on the prevention of foot ulcers in persons with diabetes (IWGDF 2019 update). Diabetes Metab. Res. Rev. 2020, 36, e3269. [Google Scholar]
- American Diabetes Association. Microvascular Complications and Foot Care. Diabetes Care. 2017, 40, 88–98. [Google Scholar] [CrossRef] [PubMed]
- López-Moral, M.; Lázaro-Martínez, J.L.; García-Morales, E.; García-Álvarez, Y.; Alvaro-Afonso, F.J.; Molines-Barroso, R.J. Clinical efficacy of therapeutic footwear with a rigid rocker sole in the prevention of recurrence in patients with diabetes mellitus and diabetic polyneuropathy: A randomized clinical trial. PLoS ONE. 2019, 14, 0219537. [Google Scholar] [CrossRef] [PubMed]
- Reints, R.; Hijmans, J.M.; Burgerhof, J.G.M.; Postema, K.; Verkerke, G.J. Effects of flexible and rigid rocker profiles on in-shoe pressure. Gait Posture. 2017, 58, 287–293. [Google Scholar] [CrossRef] [PubMed]
- Lin, S.Y.; Su, P.F.; Chung, C.H.; Hsia, C.C.; Chang, C.H. Stiffness Effects in Rocker-Soled Shoes: Biomechanical Implications. PLoS ONE 2017, 12, 0169151. [Google Scholar] [CrossRef]
- Sawacha, Z.; Spolaor, F.; Guarneri, G.; Contessa, P.; Carraro, E.; Venturin, A.; Venturin, A.; Avogaro, A.; Cobelli, C. Abnormal muscle activation during gait in diabetes patients with and without neuropathy. Gait Posture 2012, 35, 101–105. [Google Scholar] [CrossRef]
- Fernando, M.; Crowther, R.; Lazzarini, P.; Sangla, K.; Cunningham, M.; Buttner, P.; Golledge, J. Biomechanical characteristics of peripheral diabetic neuropathy: A systematic review and meta-analysis of findings from the gait cycle, muscle activity and dynamic barefoot plantar pressure. Clin. Biomech. 2013, 28, 831–845. [Google Scholar] [CrossRef]
- Hinchliffe, R.J.; Forsythe, R.O.; Apelqvist, J.; Boyko, E.J.; Fitridge, R.; Pio Hong, J.; Katsanos, K.; Mills, J.L.; Nikol, S.; Reekers, J.; et al. International Working Group on the Diabetic Foot (IWGDF). Guidelines on diagnosis, prognosis, and management of peripheral artery disease in patients with a foot ulcer and diabetes (IWGDF 2019 update). Diabetes Metab. Res. Rev. 2020, 36, e3276. [Google Scholar] [CrossRef]
- Richard, J.L.; Reilhes, L.; Buvry, S.; Goletto, M.; Faillie, J.L. Screening patients at risk for diabetic foot ulceration: A comparison between measurement of vibration perception threshold and 10-g monofilament test. Int. Wound J. 2014, 11, 147–151. [Google Scholar] [CrossRef]
- Lázaro-Martínez, J.L.; Aragón-Sánchez, J.; Alvaro-Afonso, F.J.; García-Morales, E.; García-Álvarez, Y.; Molines-Barroso, R.J. The best way to reduce reulcerations: If you understand biomechanics of the diabetic foot, you can do it. Int. J. Low Extrem. Wounds. 2014, 13, 294–319. [Google Scholar] [CrossRef]
- Molines-Barroso, R.J.; Lázaro-Martínez, J.L.; Aragón-Sánchez, F.J.; Alvaro-Afonso, F.J.; García-Morales, E.; García-Álvarez, Y. Forefoot ulcer risk is associated with foot type in patients with diabetes and neuropathy. Diabetes Res. Clin. Pract. 2016, 114, 93–98. [Google Scholar] [CrossRef]
- Redmond, A.C.; Crosbie, J.; Ouvrier, R.A. Development and validation of a novel rating system for scoring standing foot posture: The Foot Posture Index. Clin. Biomech. 2006, 21, 89–98. [Google Scholar] [CrossRef]
- Chiu, M.C.; Wu, H.C.; Chang, L.Y. Gait speed and gender effects on center of pressure progression during normal walking. Gait Posture 2013, 37, 43–48. [Google Scholar] [CrossRef] [PubMed]
- Cohen, J. A power primer. Psychol. Bull. 1992, 112, 155–159. [Google Scholar] [CrossRef] [PubMed]
- Rao, S.; Saltzman, C.; Yack, H.J. Ankle ROM and stiffness measured at rest and during gait in individuals with and without diabetic sensory neuropathy. Gait Posture 2006, 24, 295–301. [Google Scholar] [CrossRef] [PubMed]
- Raspovic, A. Gait characteristics of people with diabetes-related peripheral neuropathy, with and without a history of ulceration. Gait Posture. 2013, 38, 723–728. [Google Scholar] [CrossRef] [PubMed]
- Nuesch, C.; Overberg, J.A.; Schwameder, H.; Pagenstert, G.; Mundermann, A. Repeatability of spatiotemporal, plantar pressure and force parameters during treadmill walking and running. Gait Posture 2018, 62, 117–123. [Google Scholar] [CrossRef] [PubMed]
- Karimi, M.T. The Evaluation of Foot Rockers on the Kinematic Parameters of Individuals With Diabetes. Foot Ankle Spec. 2018, 11, 322–329. [Google Scholar] [CrossRef] [PubMed]
- Jarl, G.; Lundqvist, L.O. Adherence to wearing therapeutic shoes among people with diabetes: A systematic review and reflections. Patient Prefer. Adherence 2016, 8, 1521–1528. [Google Scholar] [CrossRef]
- Waaijman, R.; Keuenkamp, R.; de Haart, M.; Polomski, W.P.; Nollet, F.; Bus, S.A. Adherence to wearing prescription custom—Made footwear in patient with diabetes at high risk for foot ulceration. Diabetes Care 2013, 36, 1613–1618. [Google Scholar] [CrossRef]

| Baseline Characteristics | Patients (n = 24) |
|---|---|
| Male n (%) | 17 (70.8) |
| Female n (%) | 7 (29.2) |
| Type 1 DM n (%) | 3 (12.5) |
| Type 2 DM n (%) | 21 (87.5) |
| Retinopathy n (%) | 15 (62.5) |
| Nephropathy n (%) | 1 (4.2) |
| Foot deformity n (%) | 22 (85) |
| Diabetic polyneuropathy (%) | 24 (100) |
| Mean age ± SD (years) | 62.5 ± 8.8 |
| Body mass index (kg/cm2), mean ± SD | 27.3 ± 4.6 |
| Glycated hemoglobin mmol/mol (%), mean ± SD | 53 (7.03) ± 1.15 |
| Diabetes mellitus (years), mean ± SD | 21.3 ± 14.1 |
| Foot Characteristics | n = 48 feet |
| Hallux abductus valgus n (%) | 6 (12.5) |
| Hammer toes n (%) | 37 (77.1) |
| Taylor bunion n (%) | 14 (29.2) |
| Previous amputation n (%) | 28 (58.3) |
| Previous DFU n (%) | 39 (81.3) |
| Interphalangeal joint of the hallux n (%) | 2 (5.2) |
| First MTH n (%) | 13 (33.3) |
| Second MTH n (%) | 11 (28.2) |
| Fourth MTH n (%) | 8 (20.5) |
| Fifth MTH n (%) | 5 (12.8) |
| Foot Posture Index (FPI), mean ± SD | 1.6 ± 4.8 |
| Neutral n (%) | 26 (54.2) |
| Pronated n (%) | 6 (12.5) |
| Supinated n (%) | 16 (33.3) |
| Barefoot maximal mean pressure in the forefoot (kPa), mean ± SD | 757.2 ± 357.8 |
| Barefoot force time integral in the forefoot (kPa/s), mean ± SD | 244.52 ± 156.65 |
| n = 24 Patients | Left Foot n = 24 | Right Foot n = 24 | ||
|---|---|---|---|---|
| Previous Amputation | Foot Posture Index | Previous Amputation | Foot Posture Index | |
| Patient 01 | 3rd MTH | −3 | - | −9 |
| Patient 02 | - | 2 | 5th MTH | 0 |
| Patient 03 | 2nd MTH | 0 | - | 0 |
| Patient 04 | - | 6 | - | 2 |
| Patient 05 | - | 5 | 1st MTH | 6 |
| Patient 06 | 2nd MTH | 7 | - | 3 |
| Patient 07 | 1st MTH | 10 | 4th MTH | 8 |
| Patient 08 | 4th MTH | 9 | - | 4 |
| Patient 09 | - | 3 | - | 2 |
| Patient 10 | 2nd and 4th MTH | −2 | - | −3 |
| Patient 11 | - | −5 | - | −2 |
| Patient 12 | 3rd MTH | 5 | 1st MTH | 8 |
| Patient 13 | - | 0 | - | −4 |
| Patient 14 | - | −1 | - | −1 |
| Patient 15 | - | 2 | 1st MTH | 6 |
| Patient 16 | 2nd MTH | −2 | - | −2 |
| Patient 17 | 1st MTH | 3 | 5th MTH | −6 |
| Patient 18 | 5th MTH | 5 | 2nd MTH | 0 |
| Patient 19 | 2nd MTH | 10 | 5th MTH | 7 |
| Patient 20 | 1st MTH | 4 | - | −2 |
| Patient 21 | 1st MTH | 4 | 3rd MTH | 6 |
| Patient 22 | 2nd MTH | 5 | 2nd toe | 0 |
| Patient 23 | 1st MTH | 4 | - | −2 |
| Patient 24 | 5th MTH | −2 | 3rd MTH | −12 |
| Foot Type | ||||
|---|---|---|---|---|
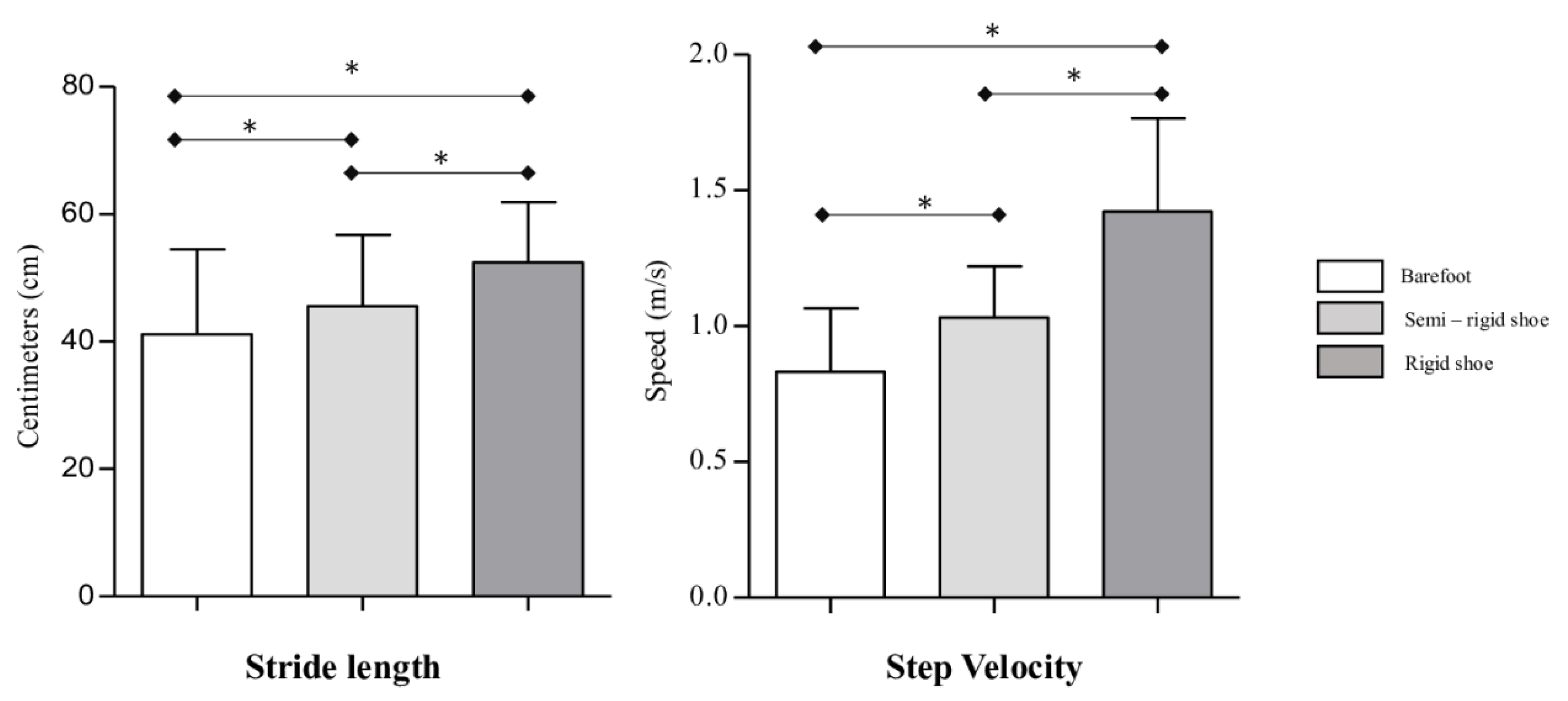
| Stride Length (cm) | Neutral | Pronated | Supinated | P-Value |
| Semirigid condition | 21.7 | 11.42 | 34.31 | 0.001 * |
| Rigid condition | 21.71 | 14.33 | 32.84 | 0.007 * |
© 2020 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
López-Moral, M.; Molines-Barroso, R.J.; Álvaro-Afonso, F.J.; Uccioli, L.; Senneville, E.; Lázaro-Martínez, J.L. Importance of Footwear Outsole Rigidity in Improving Spatiotemporal Parameters in Patients with Diabetes and Previous Forefoot Ulcerations. J. Clin. Med. 2020, 9, 907. https://doi.org/10.3390/jcm9040907
López-Moral M, Molines-Barroso RJ, Álvaro-Afonso FJ, Uccioli L, Senneville E, Lázaro-Martínez JL. Importance of Footwear Outsole Rigidity in Improving Spatiotemporal Parameters in Patients with Diabetes and Previous Forefoot Ulcerations. Journal of Clinical Medicine. 2020; 9(4):907. https://doi.org/10.3390/jcm9040907
Chicago/Turabian StyleLópez-Moral, Mateo, Raúl Juan Molines-Barroso, Francisco Javier Álvaro-Afonso, Luigi Uccioli, Eric Senneville, and José Luis Lázaro-Martínez. 2020. "Importance of Footwear Outsole Rigidity in Improving Spatiotemporal Parameters in Patients with Diabetes and Previous Forefoot Ulcerations" Journal of Clinical Medicine 9, no. 4: 907. https://doi.org/10.3390/jcm9040907
APA StyleLópez-Moral, M., Molines-Barroso, R. J., Álvaro-Afonso, F. J., Uccioli, L., Senneville, E., & Lázaro-Martínez, J. L. (2020). Importance of Footwear Outsole Rigidity in Improving Spatiotemporal Parameters in Patients with Diabetes and Previous Forefoot Ulcerations. Journal of Clinical Medicine, 9(4), 907. https://doi.org/10.3390/jcm9040907









