A Scoping Review of The Efficacy of Virtual Reality and Exergaming on Patients of Musculoskeletal System Disorder
Abstract
1. Introduction
2. Materials and Methods
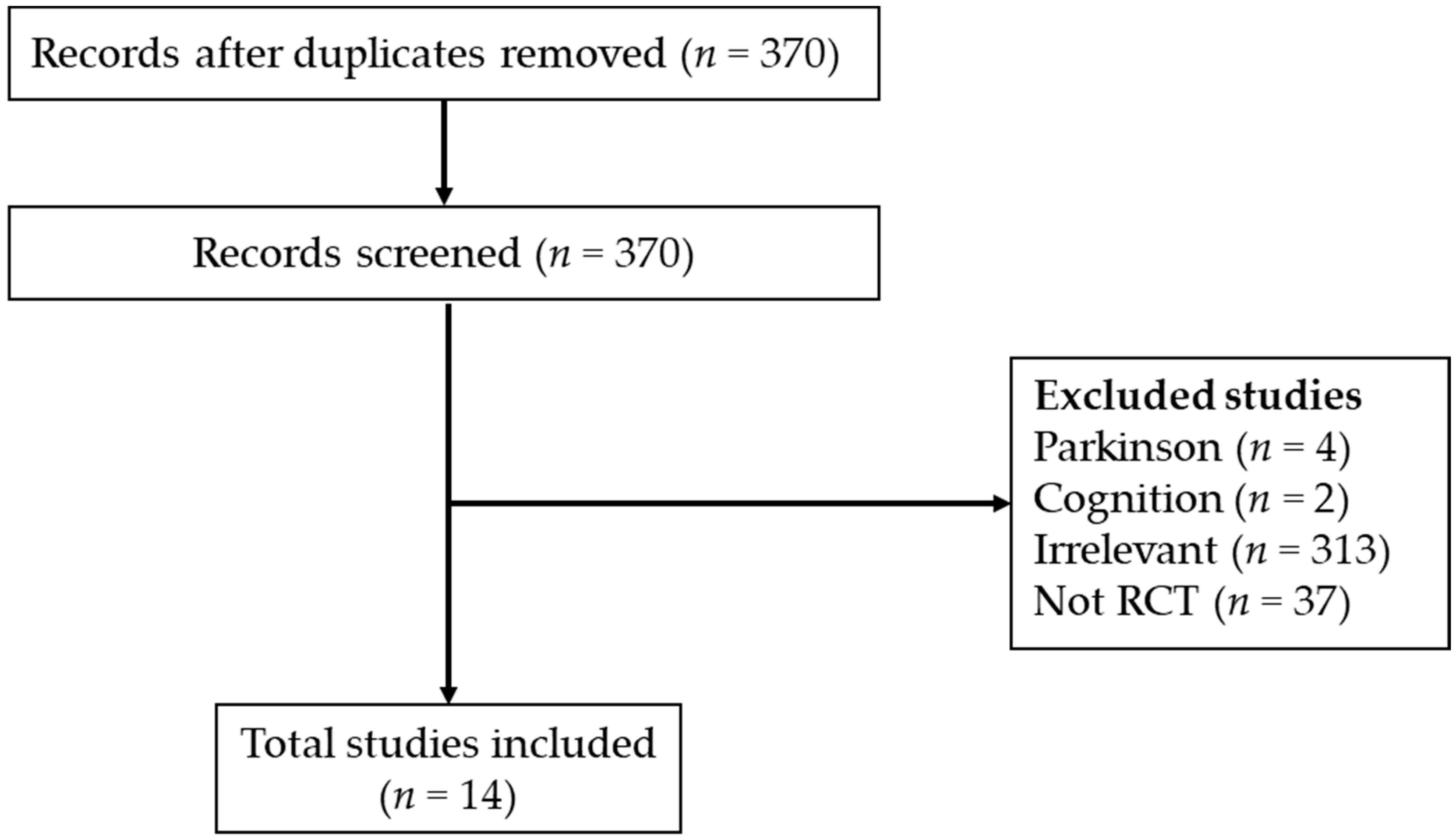
2.1. Determination and Selection of Articles
2.2. Data Extraction and Quality Assessment
3. Result
3.1. Quality of the Included Studies
3.2. Description of Included Studies
3.3. Virtual Reality Resources Choosing
3.4. Heterogeneity of Included RCT
3.5. Effect of Virtual Reality versus Other Interventions
3.6. Effect of Virtual Reality Versus No Intervention
3.7. Effect of Virtual Reality on Acute and Chronic Musculoskeletal Pain
4. Discussion
Limitations
5. Conclusions
Acknowledgements
Conflicts of Interest
References
- Burdea, G.C.; Coiffet, P. Virtual Reality Technology, 2nd ed.; Wiley-IEEE Press: Hoboken, NJ, USA, 2003. [Google Scholar]
- Wang, P.; Wu, P.; Wang, J.; Chi, H.-L.; Wang, X. A Critical Review of the Use of Virtual Reality in Construction Engineering Education and Training. Int. J. Environ. Res. Public Health 2018, 15, 1204. [Google Scholar] [CrossRef] [PubMed]
- Levac, D.; Glegg, S.; Colquhoun, H.; Miller, P.; Noubary, F. Virtual Reality and Active Videogame-Based Practice, Learning Needs, and Preferences: A Cross-Canada Survey of Physical Therapists and Occupational Therapists. Games Health J. 2017, 6, 217–228. [Google Scholar] [CrossRef] [PubMed]
- Levac, D.E.; Miller, P.E. Integrating virtual reality video games into practice: Clinicians’ experiences. Physiother. Theory Pract. 2013, 29, 504–512. [Google Scholar] [CrossRef] [PubMed]
- Barton, G.J.; Hawken, M.B.; Foster, R.J.; Holmes, G.; Butler, P.B. The effects of virtual reality game training on trunk to pelvis coupling in a child with cerebral palsy. J. Neuroeng. Rehabil. 2013, 10, 15. [Google Scholar] [CrossRef] [PubMed]
- Broeren, J.; Rydmark, M.; Sunnerhagen, K.S. Virtual reality and haptics as a training device for movement rehabilitation after stroke: A single-case study. Arch. Phys. Med. Rehabil. 2004, 85, 1247–4250. [Google Scholar] [CrossRef] [PubMed]
- Chang, Y.J.; Chen, S.F.; Huang, J.D. A Kinect-based system for physical rehabilitation: A pilot study for young adults with motor disabilities. Res. Dev. Disabil. 2011, 32, 2566–2570. [Google Scholar] [CrossRef] [PubMed]
- Deutsch, J.E. Use of a low-cost, commercially available gaming console (Wii) for rehabilitation of an adolescent with cerebral palsy. Phys. Ther. 2008, 88, 1196. [Google Scholar] [CrossRef] [PubMed]
- Dos Santos Mendes, F.A.; Pompeu, J.E.; Modenesi Lobo, A.; Guedes da Silva, K.; Oliveira Tde, P.; Peterson Zomignani, A.; Pimentel Piemonte, M.E. Motor learning, retention and transfer after virtual-reality-based training in Parkinson’s disease—Effect of motor and cognitive demands of games: A longitudinal, controlled clinical study. Physiotherapy 2012, 98, 217–223. [Google Scholar] [CrossRef]
- Fischer, H.C.; Stubblefield, K.; Kline, T.; Luo, X.; Kenyon, R.V.; Kamper, D.G. Hand rehabilitation following stroke: A pilot study of assisted finger extension training in a virtual environment. Top. Stroke Rehabil. 2007, 14, 1–12. [Google Scholar] [CrossRef]
- Sevick, M.; Eklund, E.; Mensch, A.; Foreman, M.; Standeven, J.; Engsberg, J. Using Free Internet Videogames in Upper Extremity Motor Training for Children with Cerebral Palsy. Behav. Sci. 2016, 6, 10. [Google Scholar] [CrossRef]
- Bonnechere, B.; Jansen, B.; Omelina, L.; Van Sint Jan, S. The use of commercial video games in rehabilitation: A systematic review. Int. J. Rehabil. Res. 2016, 39, 277–290. [Google Scholar] [CrossRef]
- The Definition of Musculoskeletal Disorders. 15 February 2018. Available online: https://www.who.int/news-room/fact-sheets/detail/musculoskeletal-conditions (accessed on 03 April 2019).
- Fung, V.; Ho, A.; Shaffer, J.; Chung, E.; Gomez, M. Use of Nintendo Wii Fit in the rehabilitation of outpatients following total knee replacement: A preliminary randomised controlled trial. Physiotherapy 2012, 98, 183–188. [Google Scholar] [CrossRef] [PubMed]
- Huang, M.C.; Lee, S.H.; Yeh, S.C.; Chan, R.C.; Rizzo, A.; Xu, W.; Wu, H.L.; Lin, S.H. Intelligent Frozen Shoulder Rehabilitation. IEEE Intell. Syst. 2014, 29, 22–28. [Google Scholar] [CrossRef]
- Koo, K.-I.; Park, D.K.; Youm, Y.S.; Cho, S.D.; Hwang, C.H. Enhanced Reality Showing Long-Lasting Analgesia after Total Knee Arthroplasty: Prospective, Randomized Clinical Trial. Sci. Rep. 2018, 8, 2343. [Google Scholar] [CrossRef] [PubMed]
- Sarig Bahat, H.; Croft, K.; Carter, C.; Hoddinott, A.; Sprecher, E.; Treleaven, J. Remote kinematic training for patients with chronic neck pain: A randomised controlled trial. Eur. Spine J. 2017, 27, 1309–1323. [Google Scholar] [CrossRef] [PubMed]
- Sarig Bahat, H.; Takasaki, H.; Chen, X.; Bet-Or, Y.; Treleaven, J. Cervical kinematic training with and without interactive VR training for chronic neck pain—A randomized clinical trial. Man. Ther. 2015, 20, 68–78. [Google Scholar] [CrossRef] [PubMed]
- Scapin, S.; Echevarria-Guanilo, M.E.; Boeira Fuculo Junior, P.R.; Goncalves, N.; Rocha, P.K.; Coimbra, R. Virtual Reality in the treatment of burn patients: A systematic review. Burns 2018, 44, 1403–1416. [Google Scholar] [CrossRef]
- Hoffman, H.G.; Patterson, D.R.; Carrougher, G.J. Use of virtual reality for adjunctive treatment of adult burn pain during physical therapy: A controlled study. Clin. J. Pain 2000, 16, 244–250. [Google Scholar] [CrossRef]
- Arlati, S.; Colombo, V.; Ferrigno, G.; Sacchetti, R.; Sacco, M. Virtual reality-based wheelchair simulators: A scoping review. Assist. Technol. 2019, 1–12. [Google Scholar] [CrossRef]
- Pekyavas, N.O.; Ergun, N. Comparison of virtual reality exergaming and home exercise programs in patients with subacromial impingement syndrome and scapular dyskinesis: Short term effect. Acta Orthop. Traumatol. Turc. 2017, 51, 238–242. [Google Scholar] [CrossRef]
- Thomas, J.S.; France, C.R.; Applegate, M.E.; Leitkam, S.T.; Walkowski, S. Feasibility and Safety of a Virtual Reality Dodgeball Intervention for Chronic Low Back Pain: A Randomized Clinical Trial. J. Pain 2016, 17, 1302–1317. [Google Scholar] [CrossRef] [PubMed]
- Kim, S.S.; Min, W.K.; Kim, J.H.; Lee, B.H. The Effects of VR-based Wii Fit Yoga on Physical Function in Middle-aged Female LBP Patients. J. Phys. Ther. Sci. 2014, 26, 549–552. [Google Scholar] [CrossRef] [PubMed]
- Yilmaz Yelvar, G.; ırak1, Y.C.; Dalkılınc, M.; Demir, Y.P.; Guner, Z.; Boydak, A.E. Is physiotherapy integrated virtual walking effective on pain, function, and kinesiophobia in patients with non-specific low-back pain? Randomised controlled trial. Eur. Spine J. 2017, 26, 538–545. [Google Scholar] [CrossRef] [PubMed]
- Martinho, N.M.; Silva, V.R.; Marques, J.; Carvalho, L.C.; Iunes, D.H.; Botelho, S. The effects of training by virtual reality or gym ball on pelvic floor muscle strength in postmenopausal women: A randomized controlled trial. Braz. J. Phys. Ther. 2016, 20, 248–257. [Google Scholar] [CrossRef] [PubMed]
- Jeffs, D.; Dorman, D.; Brown, S.; Files, A.; Graves, T.; Kirk, E.; Meredith-Neve, S.; Sanders, J.; White, B.; Swearingen, C.J. Effect of virtual reality on adolescent pain during burn wound care. J. Burn Care Res. 2014, 35, 395–408. [Google Scholar] [CrossRef]
- Kipping, B.; Rodger, S.; Miller, K.; Kimble, R.M. Virtual reality for acute pain reduction in adolescents undergoing burn wound care: A prospective randomized controlled trial. Burns 2012, 38, 650–657. [Google Scholar] [CrossRef]
- Jin, C.; Feng, Y.; Ni, Y.; Shan, Z. Virtual reality intervention in postoperative rehabilitation after total knee arthroplasty: A prospective and randomized controlled clinical trial. Int. J. Clin. Exp. Med. 2018, 11, 6119–6124. [Google Scholar]
- Punt, I.M.; Ziltener, J.L.; Monnin, D.; Allet, L. Wii Fit exercise therapy for the rehabilitation of ankle sprains: Its effect compared with physical therapy or no functional exercises at all. Scand. J. Med. Sci. Sports 2016, 26, 816–823. [Google Scholar] [CrossRef]
- Tubach, F.; Ravaud, P.; Baron, G.; Falissard, B.; Logeart, I.; Bellamy, N.; Bombardier, C.; Felson, D.; Hochberg, M.; van der Heijde, D.; et al. Evaluation of clinically relevant changes in patient reported outcomes in knee and hip osteoarthritis: The minimal clinically important improvement. Ann. Rheum. Dis. 2005, 64, 29–33. [Google Scholar] [CrossRef]
- Treede, R.D.; Rief, W.; Barke, A.; Aziz, Q.; Bennett, M.I.; Benoliel, R.; Cohen, M.; Evers, S.; Finnerup, N.B.; First, M.B.; et al. A classification of chronic pain for ICD-11. Pain 2015, 156, 1003–1007. [Google Scholar] [CrossRef]
- Carpenter, D.M.; Nelson, B.W. Low back strengthening for the prevention and treatment of low back pain. Med. Sci. Sports Exerc. 1999, 31, 18–24. [Google Scholar] [CrossRef] [PubMed]
- Sharar, S.R.; Alamdari, A.; Hoffer, C.; Hoffman, H.G.; Jensen, M.P.; Patterson, D.R. Circumplex Model of Affect: A Measure of Pleasure and Arousal During Virtual Reality Distraction Analgesia. Games Health J. 2016, 5, 197–202. [Google Scholar] [CrossRef] [PubMed]
- Mosadeghi, S.; Reid, M.W.; Martinez, B.; Rosen, B.T.; Spiegel, B.M. Feasibility of an Immersive Virtual Reality Intervention for Hospitalized Patients: An Observational Cohort Study. JMIR Ment. Health 2016, 3, e28. [Google Scholar] [CrossRef] [PubMed]
- Pourmand, A.; Davis, S.; Marchak, A.; Whiteside, T.; Sikka, N. Virtual Reality as a Clinical Tool for Pain Management. Curr. Pain Headache Rep. 2018, 22, 53. [Google Scholar] [CrossRef] [PubMed]
- Garrett, B.; Taverner, T.; Masinde, W.; Gromala, D.; Shaw, C.; Negraeff, M. A rapid evidence assessment of immersive virtual reality as an adjunct therapy in acute pain management in clinical practice. Clin. J. Pain 2014, 30, 1089–1098. [Google Scholar] [CrossRef] [PubMed]
- Jones, T.; Moore, T.; Choo, J. The Impact of Virtual Reality on Chronic Pain. PLoS ONE 2016, 11, e0167523. [Google Scholar] [CrossRef] [PubMed]
- Chan, E.; Foster, S.; Sambell, R.; Leong, P. Clinical efficacy of virtual reality for acute procedural pain management: A systematic review and meta-analysis. PLoS ONE 2018, 13, e0200987. [Google Scholar] [CrossRef] [PubMed]
- Hoffman, H.G.; Patterson, D.R.; Seibel, E.; Soltani, M.; Jewett-Leahy, L.; Sharar, S.R. Virtual reality pain control during burn wound debridement in the hydrotank. Clin. J. Pain 2008, 24, 299–304. [Google Scholar] [CrossRef]
- Morris, L.D.; Louw, Q.A.; Crous, L.C. Feasibility and potential effect of a low-cost virtual reality system on reducing pain and anxiety in adult burn injury patients during physiotherapy in a developing country. Burns 2010, 36, 659–664. [Google Scholar] [CrossRef] [PubMed]
- Maani, C.V.; Hoffman, H.G.; Morrow, M.; Maiers, A.; Gaylord, K.; McGhee, L.L.; DeSocio, P.A. Virtual reality pain control during burn wound debridement of combat-related burn injuries using robot-like arm mounted VR goggles. J. Trauma 2011, 71, S125–S130. [Google Scholar] [CrossRef]
- Junginger, B.; Baessler, K.; Sapsford, R.; Hodges, P.W. Effect of abdominal and pelvic floor tasks on muscle activity, abdominal pressure and bladder neck. Int. Urogynecol. J. 2010, 21, 69–77. [Google Scholar] [CrossRef] [PubMed]
- Hibbs, A.E.; Thompson, K.G.; French, D.; Wrigley, A.; Spears, I. Optimizing Performance by Improving Core Stability and Core Strength. Sports Med. 2008, 38, 995–1008. [Google Scholar] [CrossRef] [PubMed]
- Park, M.; Im, H.; Kim, D.Y. Feasibility and user experience of virtual reality fashion stores. Fash. Text. 2018, 5, 1–17. [Google Scholar] [CrossRef]
| Huang et al. 2014 [15] | Pekyavas et al. 2017 [22] | Bahat et al. 2015 [18] | Bahat et al. 2017 [17] | Kim et al. 2014 [24] | Thomas et al. 2016 [23] | Yilmaz Yelvar et al. 2017 [25] | Martinho et al. 2016 [26] | Kipping et al. 2012 [28] | Jeffs et al. 2014 [27] | Fung et al. 2012 [14] | Koo et al. 2018 [16] | Jin et al. 2018 [29] | Punt et al. 2016 [30] | |
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| 2014 | 2017 | 2015 | 2017 | 2014 | 2016 | 2017 | 2016 | 2012 | 2014 | 2012 | 2018 | 2018 | 2016 | |
| Taiwan | Turkey | Australia | Australia | Korea | America | Turkey | Brazil | Australia | America | Canada | Korea | China | Switzerland | |
| Eligibility criteria | Y | N | Y | N | N | Y | Y | Y | Y | Y | Y | Y | Y | Y |
| Random allocation | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y |
| Concealed allocation | N | N | Y | Y | N | Y | N | Y | Y | Y | N | Y | N | Y |
| Baseline comparability | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y |
| Blind subjects | N | N | N | N | N | N | N | N | N | Y | N | N | N | N |
| Blind therapists | N | N | N | N | N | N | N | N | N | N | N | N | N | N |
| Blind assessors | Y | N | Y | Y | N | N | Y | N | N | N | Y | Y | N | Y |
| Adequate follow-up | Y | Y | Y | N | Y | Y | Y | N | Y | Y | Y | N | Y | N |
| Intention-to-treat analysis | Y | N | N | Y | N | N | N | Y | Y | N | N | N | N | Y |
| Between-group comparisons | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y |
| Point estimates and variability | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | N | Y | Y | Y |
| Total score (0~10) | 7/10 | 5/10 | 7/10 | 7/10 | 5/10 | 6/10 | 6/10 | 6/10 | 7/10 | 7/10 | 5/10 | 6/10 | 5/10 | 7/10 |
| Title | Author | Part | Design | Participant (number) | Intervention | Exercise Mode (Frequency or Intensity) | Outcome Measures | |
|---|---|---|---|---|---|---|---|---|
| Age (years) = mean (SD) | ||||||||
| Intelligent Frozen Shoulder Rehabilitation | Huang et al. 2014 [15] | Frozen shoulder | RCT | frozen shoulder syndrome > 3 months | 20 min/time, 2 times/week (Total 4 weeks) | ROM, CMS assessment | ||
| E | n = 20 Age (years) = 60.65 (11.84) | Hot pack + ultrasonic + VR | ||||||
| C | n = 20 Age (years) = 61.45 (12.84) | Hot pack + ultrasonic + traditional exercise training | ||||||
| Comparison of virtual reality exergaming and home exercise programs in patients with subacromial impingement syndrome and scapular dyskinesis: Short term effect | Pekyavas et al. 2017 [22] | subacromial impingement syndrome(SAIS) & scapular dyskinesis | RCT | 18–60 years old; Type II SAIS | VAS(rest, activity, night), SPADI, Neer, Hawkins, SRT, SAT, LSST1-3 | |||
| None rotator cuff problem | ||||||||
| E | n = 15 Age (years) = 40.33 (13.20) | VR + control period (after 6 weeks) | VR: 45 min/day, twice a week, for 6 weeks; Control: 1 month for home exercise | |||||
| C | n = 15 Age (years) = 40.60 (11.77) | Exercise + control period (after 6 weeks) | Exercise: 45 min/day, twice a week, for 6 weeks; Control: 1 month for home exercise | |||||
| Cervical Kinematic Training with and without Interactive VR Training for Chronic Neck Pain—a Randomized Clinical Trial | Bahat et al. 2015 [18] | Chronic neck pain | RCT | Neck pain > 3 months, NDI > 10% | VAS, Neck Disability Index, TSK, ROM, Peak velocity, mean velocity, TIP%, Sway SD, Accuracy, Eyes closed balance, singer leg stance, step test | |||
| E | n = 16 Age (years) = 40.63 (14.18) | VR + kinematic training | Total 30 min, at least 3 times a week, for 5 weeks | |||||
| C | n = 16 Age (years) = 41.13 (12.59) | kinematic training (using laser point) | ||||||
| Remote kinematic training for patients with chronic neck pain: a randomized controlled trial | Bahat et al. 2017 [17] | Chronic neck pain | RCT | Neck pain > 3 months, NDI > 12% | Neck Disability Index, Peak velocity, mean velocity, VAS, EQ5D, TSK, NVP, TTP%, Accuracy, ROM, GPE | |||
| VR | n = 30 Age (years) = 48 (9.5) | VR | 1 set 5 min, 20 min/day, 4 times/week, for 4 weeks | |||||
| Laser | n = 30 Age (years) = 48 (12.5) | Laser point training | ||||||
| C | n = 30 Age (years) = 48 (13) | Not receive any treatment | ||||||
| The Effects of VR-Based Wii Fit Yoga on Physical Function in Middle-Aged Female LBP Patients | Kim et al. 2014 [24] | LBP | RCT | LBP > 2 months | VAS, pressure algometer, ODI, RMDQ, FBQ | |||
| E | n = 15 Age (years) = 44.33 | VR | 30 min/session, 3 session/week, for 4 weeks (1 session had 7 exercise program. 3 min of exercise and 1 min of rest) | |||||
| C | n = 15 Age (years) = 50.46 | Trunk stabilizing exercise + physical therapy | 2 sets (30 min), 1set included 10 repetitions, physical therapy 30 min | |||||
| Feasibility and Safety of a Virtual Reality Dodgeball Intervention for Chronic Low Back Pain: A Randomized Clinical Trial | Thomas et al. 2016 [23] | LBP | RCT | 18–50 years old with LBP > 3 months | pain and harm, lumbar spine flexion ROM | |||
| kinesiophobia ≥35 | ||||||||
| E | n = 26 Age (years) = 23.9 (6.8) | VR | 3 days (<48 h) | |||||
| C | n = 26 Age (years) = 26.7 (8.5) | Not receive any treatment | ||||||
| Is physiotherapy integrated virtual walking effective on pain, function, and kinesiophobia in patients with non-specific low-back pain? Randomised controlled trial | Yilmaz Yelvar et al. 2017 [25] | LBP | RCT | non-specific LBP for longer than 2 months | VAS, ODI, TKS, TUG, and 6MWT scores | |||
| E | n = 23 Age (years) = 46.27 (10.93) | VR + Traditional physical therapy | 5 times/week, for 2 weeks | |||||
| C | n = 23 Age (years) = 52.81 (11.53) | Traditional physical therapy | 5 times/week, for 2 weeks | |||||
| The effects of training by virtual reality or gym ball on pelvic floor muscle strength in postmenopausal women: a randomized controlled trial | Martinho et al. 2016 [26] | Pelvic floor muscle | RCT | >50 years old women | Maximum strength, average strength, endurance | |||
| >1 year postmenopausal phase | ||||||||
| APT-VR | n = 30 Age (years) = 61.9 (8.6) | Abdominopelvic training by VR | 1 session 5 min with 90 s resting, for 10 session. Twice a week, for 5 weeks | |||||
| PFMT-GB | n = 30 Age (years) = 61 (8.5) | Pelvic floor muscle training using a gym ball | 4 series of 10 fast & sustained (8 s maintain with 16 s resting), each exercise 5 times, twice a week, for 5 weeks | |||||
| Virtual reality for acute pain reduction in adolescents undergoing burn wound care: A prospective randomized controlled trial | Kipping et al. 2012 [28] | Burn wound | RCT | 11–18 years old | VAS, FLACC scale | |||
| burn wound Total Body Surface Area (TBSA) > 1% | ||||||||
| E | n = 20 Age (years) = 12.6 (1.3) | VR | Dressing period (3–58 min), only 1 time | |||||
| C | n = 21 Age (years) = 13.5 (1.8) | Another distraction way or no distraction | ||||||
| Effect of Virtual Reality on Adolescent Pain During Burn Wound Care | Jeffs et al. 2014 [27] | Burn wound | RCT | 10–17 years old | Adolescent Pediatric Pain Tool, Spielberger State-Trait Anxiety InventoryFor Children, Pre-Procedure Questionnaire, Post-Procedure Questionnaire | |||
| standard care | n = 10 Age (years) = 18.9 (2.8) | standard care | Dressing period only 1 time | |||||
| passive distraction | n = 10 Age (years) = 12.6 (2.1) | passive distraction watching a movie | ||||||
| virtual reality | n = 8 Age (years) = 14.8 (2.0) | virtual reality | ||||||
| Use of Nintendo Wii Fit™ in the Rehabilitation of Outpatients Following Total Knee Replacement: a Preliminary Randomized Controlled Trial | Fung et al. 2012 [14] | TKR | RCT | requiring twice-weekly physiotherapy treatment for TKR rehabilitation | active knee flexion/extension ROM, 2 min walk test, NPRS, ABCS, LEFS | |||
| Full lower extremity weight bearing | ||||||||
| E | n = 27 Age (years) = 67.9 (9.5) | physiotherapy + VR | physiotherapy (45 min), 15 min VR until discharge | |||||
| C | n = 23 Age (years) = 68.2 (12.8) | physiotherapy + lower extremity exercise | physiotherapy (45 min), 15 min lower extremity exercise until discharge | |||||
| Enhanced Reality Showing Long-Lasting Analgesia after Total Knee Arthroplasty: Prospective, Randomized Clinical Trial | Koo et al. 2018 [16] | TKR | RCT | Full term | n = 20 Age (years) = 63.7 (5.09) | VR + physiotherapy for 2 weeks | VR + PT: 5 days/week, for 2 weeks | VAS, WOMAC, 6 min walk test, Timed-stands test |
| Half term | n = 22 Age (years) = 65.0 (6.97) | VR + physiotherapy for 1 week before physiotherapy for 1 week | VR + PT for 1 week | |||||
| Virtual reality intervention in postoperative rehabilitation after total knee arthroplasty: a prospective and randomized controlled clinical trial | Jin et al. 2018 [29] | TKR | RCT | E | n = 33 Age (years) = 66.45 (3.49) | VR(begin 2nd days for TKA) + conventional rehabilitation | three sets of 30 repetitions | WOMAC, HSS, VAS, ROM. |
| C | n = 33 Age (years) = 66.30 (4.41) | conventional rehabilitation | three sets of 30 repetitions | |||||
| Wii Fit™ Exercise Therapy for the Rehabilitation of Ankle Sprains: Its Effect Compared with Physical Therapy or No Functional Exercises at All | Punt et al. 2016 [30] | Ankle sprain | RCT | 18–64 years old | FAAM-ADL, FAAM-sport, VAS-rest, VAS-walk | |||
| Grade I or II lateral ankle sprain | ||||||||
| requiring 4 weeks RICE and can pain free movement | ||||||||
| VR | n = 30 Age (years) = 34.7 (10.7) | VR | 30 min/time, 2 times/week, for 6 weeks | |||||
| Physiotherapy | n = 30 Age (years) = 34.7 (11.3) | modalities, joint mobilization, muscle strengthening, proprioceptive exercise | 30 min/time, 9 times/6 weeks | |||||
| C | n = 30 Age (years) = 33.5 (9.5) | Not receive any treatment | - | |||||
| Study | Outcome Measure | Mean Difference between VR Groups and Another Intervention | Significance of Difference between Groups | |
|---|---|---|---|---|
| Huang et al. 2014 [15] | ROM | 8% | Between groups p < 0.05 | |
| CMS | NA | Between groups p < 0.05 | ||
| Pekyavas et al. 2017 [22] | Neer | post-intervention/1 month follow-up | NA | p = 0.02 |
| SRT | post-intervention/1 month follow-up | NA | p = 0.01 | |
| SAT | post-intervention/1 month follow-up | NA | p = 0.047 | |
| VAS (rest, activity, night) | post-intervention/1 month follow-up | NA | - | |
| SPADI | post-intervention/1 month follow-up | NA | - | |
| Hawkins | post-intervention/1 month follow-up | NA | - | |
| LSST1-3 | post-intervention/1 month follow-up | NA | - | |
| Bahat et al. 2015 [18] | cervical flexion ROM | post-intervention | NA | Between groups p < 0.05 |
| 3 months follow-up | NA | - | ||
| Global Perceived change | post-intervention | NA | - | |
| 3 months follow-up | NA | Between groups p < 0.05 | ||
| VAS | post-intervention/3 months follow-up | NA | - | |
| NDI | post-intervention/3 months follow-up | NA | - | |
| TSK | post-intervention/3 months follow-up | NA | - | |
| Velocity | post-intervention/3 months follow-up | NA | - | |
| TIP% | post-intervention/3 months follow-up | NA | - | |
| Accuracy | post-intervention/3 months follow-up | NA | - | |
| sway SD | post-intervention/3 months follow-up | NA | - | |
| Eyes closed balance | post-intervention/3 months follow-up | NA | - | |
| singer leg stance | post-intervention/3 months follow-up | NA | - | |
| Bahat et al. 2017 [17] | Vmean (F,LR) | Post-pre intervention | NA | Between groups p < 0.05 |
| Vpeak (LR) | Post-pre intervention | NA | Between groups p < 0.05 | |
| Vmean (F,E,LR) | 3 months follow up-pre intervention | NA | Between groups p < 0.05 | |
| Vpeak (E,LR) | 3 months follow up-pre intervention | NA | Between groups p < 0.05 | |
| VAS | Post-pre/3 months-pre | NA | Between groups p < 0.05 | |
| EQ5D | Post-pre/3 months-pre | NA | Between groups p < 0.05 | |
| Accuracy (F,RR,LR) | Post-pre intervention | NA | Between groups p < 0.05 | |
| Accuracy (F) | 3 months follow up-pre intervention | NA | Between groups p < 0.05 | |
| TTP% | Post-pre/3 months-pre | NA | Between groups p < 0.05 | |
| ROM | Post-pre/3 months-pre | NA | - | |
| NDI | Post-pre/3 months-pre | NA | - | |
| TSK | Post-pre/3 months-pre | NA | - | |
| NVP | Post-pre/3 months-pre | NA | - | |
| GPE | Post-pre/3 months-pre | NA | - | |
| Kim et al. 2014 [24] | VAS | NA | Between groups p < 0.05 | |
| Pressure algometer | NA | |||
| ODI | NA | |||
| FBQ | NA | |||
| RMDQ | NA | - | ||
| Yilmaz Yelvar et al. 2017 [25] | VAS | NA | Between groups p < 0.05 | |
| TKS | NA | |||
| TUG | NA | |||
| 6 MWT scores | NA | |||
| Martinho et al. 2016 [26] | Maximum strength | −0.08 | p = 0.1 | |
| average strength | 0.01 | p = 0.6 | ||
| Endurance | 1.83 | p = 0.007 | ||
| Jeffs et al. 2014 [27] | Pain | 23.7 | p = 0.029 | |
| Fung et al. 2012 [14] | Active knee flexion ROM | −0.33 | - | |
| Active knee extension ROM | −0.6 | - | ||
| 2 min walk test | 2.68 | - | ||
| NPPS | 16.84 | - | ||
| ABCS | 14.11 | - | ||
| LEFS | 31.85 | - | ||
| Koo et al. 2018 [16] | VAS | NA | - | |
| WOMAC | NA | - | ||
| 6 min walk test | NA | - | ||
| Timed-stands test | NA | - | ||
| Jin et al. 2018 [29] | VAS (at 3, 5, 7 days after TKR) | NA | p < 0.05 | |
| WOMAC (at 1, 3, 6 months after TKR) | NA | p < 0.05 | ||
| HSS (at 1, 3, 6 months after TKR) | NA | p < 0.05 | ||
| Punt et al. 2016 [30] | FAAM-ADL | NA | - | |
| FAAM-sport | NA | - | ||
| VAS-rest | NA | - | ||
| VAS-walk | NA | - | ||
| Study | Outcome Measure | Mean Difference between VR Groups and Control Group | Significance of Difference between Groups |
|---|---|---|---|
| Bahat et al. 2017 [17] | NDI | NA | Between groups p < 0.05 |
| velocity | NA | ||
| TTP% (F,LR) | NA | ||
| Accuracy (F,RR) | NA | ||
| ROM | NA | - | |
| EQ5D | NA | - | |
| TSK | NA | - | |
| NVP | NA | - | |
| Thomas et al. 2016 [23] | ROM | NA | - |
| Pain | NA | - | |
| Kipping et al. 2012 [28] | VAS | NA | - |
| FLACC (dressing removal) | NA | Between groups p < 0.05 | |
| Punt et al. 2016 [30] | FAAM-ADL | NA | - |
| FAAM-sport | NA | - | |
| VAS-rest | NA | - | |
| VAS-walk | NA | - |
© 2019 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Lin, H.-T.; Li, Y.-I.; Hu, W.-P.; Huang, C.-C.; Du, Y.-C. A Scoping Review of The Efficacy of Virtual Reality and Exergaming on Patients of Musculoskeletal System Disorder. J. Clin. Med. 2019, 8, 791. https://doi.org/10.3390/jcm8060791
Lin H-T, Li Y-I, Hu W-P, Huang C-C, Du Y-C. A Scoping Review of The Efficacy of Virtual Reality and Exergaming on Patients of Musculoskeletal System Disorder. Journal of Clinical Medicine. 2019; 8(6):791. https://doi.org/10.3390/jcm8060791
Chicago/Turabian StyleLin, Hui-Ting, Yen-I Li, Wen-Pin Hu, Chun-Cheng Huang, and Yi-Chun Du. 2019. "A Scoping Review of The Efficacy of Virtual Reality and Exergaming on Patients of Musculoskeletal System Disorder" Journal of Clinical Medicine 8, no. 6: 791. https://doi.org/10.3390/jcm8060791
APA StyleLin, H.-T., Li, Y.-I., Hu, W.-P., Huang, C.-C., & Du, Y.-C. (2019). A Scoping Review of The Efficacy of Virtual Reality and Exergaming on Patients of Musculoskeletal System Disorder. Journal of Clinical Medicine, 8(6), 791. https://doi.org/10.3390/jcm8060791






