Knowledge Assessment of E-Bug Assisted Antimicrobial Resistance Education Module in Class VII School Students of South Indian Coastal Town of Manipal
Abstract
:1. Introduction
Global Initiatives against AMR and Education as Stewardship Strategy in Children from an Indian Viewpoint
2. Materials and Methods
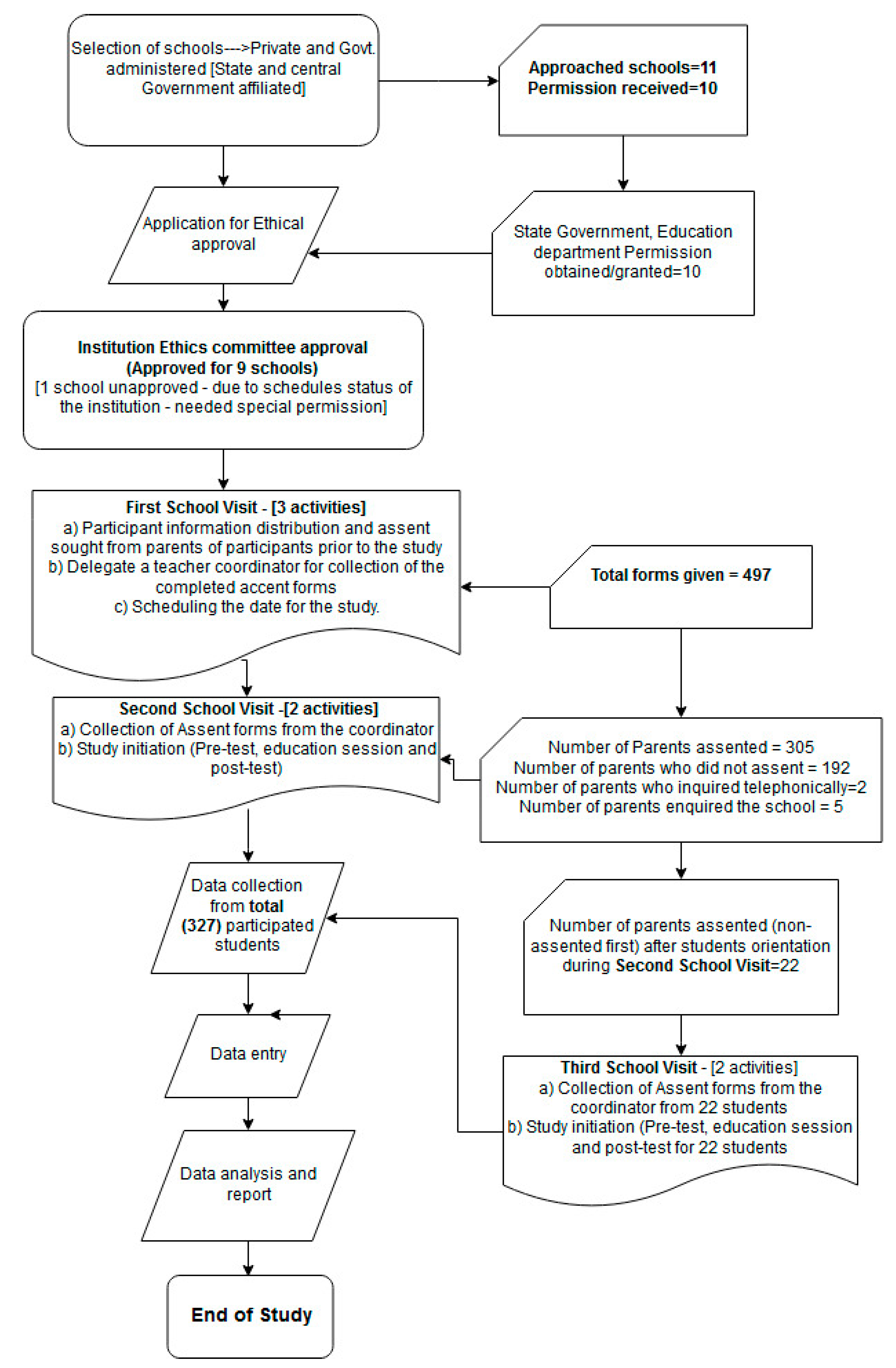
2.1. Selection of Study Participants and Criteria
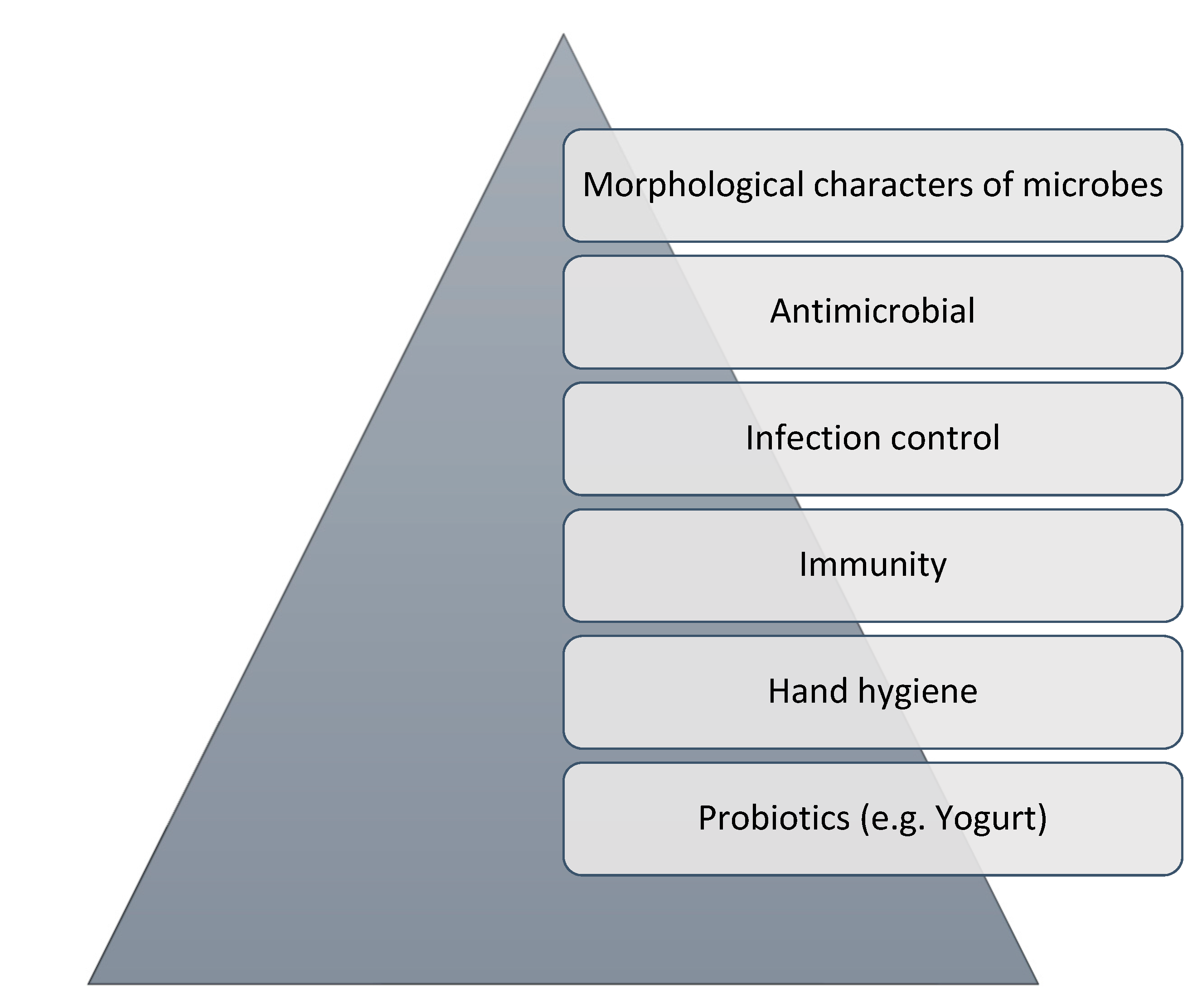
2.2. Educational Intervention Module
2.3. Statistical Analysis
3. Results
4. Discussion
5. Conclusions
Author Contributions
Funding
Acknowledgments
Conflicts of Interest
References
- World Health Organization. Global Antimicrobial Resistance Surveillance System—Manual for Early Implementation. Available online: https://www.who.int/antimicrobial-resistance/publications/surveillance-system-manual/en/ (accessed on 14 December 2018).
- McNulty, C.A.M.; Lecky, D.M.; Farrell, D.; Kostkova, P.; Adriaenssens, N.; Herotová, T.K.; Holt, J.; Touboul, P.; Merakou, K.; Koncan, R.; et al. Overview of e-bug: An antibiotic and hygiene educational resource for schools. J. Antimicrob. Chemother. 2011, 66, v3–v12. [Google Scholar] [CrossRef] [PubMed]
- Marquet, K.; Liesenborgs, A.; Bergs, J.; Vleugels, A.; Claes, N. Incidence and outcome of inappropriate in-hospital empiric antibiotics for severe infection: A systematic review and meta-analysis. Crit. Care 2015, 19, 63. [Google Scholar] [CrossRef]
- Pulcini, C.; Gyssens, I.C. How to educate prescribers in antimicrobial stewardship practices. Virulence 2013, 4, 192–202. [Google Scholar] [CrossRef] [PubMed]
- Essack, S.; Bell, J.; Shephard, A. Community pharmacists—Leaders for antibiotic stewardship in respiratory tract infection. J. Clin. Pharm. Ther. 2018, 43, 302–307. [Google Scholar] [CrossRef]
- Ghafur, A.; Mathai, D.; Muruganathan, A.; Jayalal, J.; Kant, R.; Chaudhary, D.; Prabhash, K.; Abraham, O.C.; Gopalakrishnan, R.; Ramasubramanian, V.; et al. The Chennai declaration: A roadmap to tackle the challenge of antimicrobial resistance. Indian J. Cancer 2013, 50, 71–73. [Google Scholar] [CrossRef]
- Walia, K.; Ohri, V.C.; Mathai, D. Antimicrobial stewardship programme (AMSP) practices in India. Indian J. Med. Res. 2015, 142, 130–138. [Google Scholar] [CrossRef]
- Deo, M.G. Doctor population ratio for India—The reality. Indian J. Med. Res. 2013, 137, 632–635. [Google Scholar]
- Singh, S.; Badaya, S. Health care in rural India: A lack between need and feed. South Asian J. Cancer 2014, 3, 143–144. [Google Scholar] [CrossRef]
- Ahmad, A.; Patel, I.; Parimilakrishnan, S.; Mohanta, G.P.; Chung, H.; Chang, J. The role of pharmacoeconomics in current Indian healthcare system. J. Res. Pharm. Pract. 2013, 2, 3–9. [Google Scholar] [CrossRef]
- Lecky, D.M.; McNulty, C.A.M.; Adriaenssens, N.; Herotová, T.K.; Holt, J.; Kostkova, P.; Merakou, K.; Koncan, R.; Olczak-Pienkowska, A.; Avô, A.B.; et al. Development of an educational resource on microbes, hygiene and prudent antibiotic use for junior and senior school children. J. Antimicrob. Chemother. 2011, 66, v23–v31. [Google Scholar] [CrossRef]
- Fonseca, M.J.; Santos, C.L.; Costa, P.; Lencastre, L.; Tavares, F. Increasing awareness about antibiotic use and resistance: A hands-on project for high school students. PLoS ONE 2012, 7, e44699. [Google Scholar] [CrossRef] [PubMed]
- Scalas, D.; Roana, J.; Mandras, N.; Cuccu, S.; Banche, G.; Marra, E.S.; Collino, N.; Piersigilli, G.; Allizond, V.; Tullio, V.; et al. The Microbiological@mind project: A public engagement initiative of Turin University bringing microbiology and health education into primary schools. Int. J. Antimicrob. Agents 2017, 50, 588–592. [Google Scholar] [CrossRef] [PubMed]
- European Commission. EU Guidelines for the Prudent Use of Antimicrobials in Human Health. Available online: https://ec.europa.eu/health/amr/sites/amr/files/amr_guidelines_prudent_use_en.pdf (accessed on 10 January 2019).
- Bush, P.J.; Hardon, A.P. Towards rational medicine use: Is there a role for children? Soc. Sci. Med. 1990, 31, 1043–1050. [Google Scholar] [CrossRef]
- Kotwani, A.; Wattal, C.; Joshi, P.; Holloway, K. Knowledge and perceptions on antibiotic use and resistance among high school students and teachers in New Delhi, India: A qualitative study. Indian J. Pharmacol. 2016, 48, 365–371. [Google Scholar] [CrossRef] [PubMed]
- Azevedo, M.M.; Pinheiro, C.; Yaphe, J.; Baltazar, F. Assessing the impact of a school intervention to promote students’ knowledge and practices on correct antibiotic use. Int. J. Environ. Res. Public Health 2013, 10, 2920–2931. [Google Scholar] [CrossRef] [PubMed]
- Gawai, P.P.; Taware, S.A.; Chatterjee, A.S.; Thakur, H.P. A cross sectional descriptive study of hand washing knowledge and practices among primary school children in Mumbai, Maharashtra, India. Int. J. Community Med. Public Health 2016, 3, 2958–2966. [Google Scholar] [CrossRef]
- Simonneaux, L. A study of pupils’ conceptions and reasoning in connection with ‘microbes’, as a contribution to research in biotechnology education. Int. J. Sci. Educ. 2000, 22, 619–644. [Google Scholar] [CrossRef]
- Onwubiko, N.E.; Helenchinyeaka, A. Isolation and identification of bacterial contaminants from door handles in a tertiary institution in Umuahia, Abia State, Nigeria. Niger. J. Microbiol. 2015, 29, 3139–3147. [Google Scholar]
- Byrne, J. Models of micro-organisms: Children’s knowledge and understanding of micro-organisms from 7 to 14 years old. Int. J. Sci. Educ. 2011, 33, 1927–1961. [Google Scholar] [CrossRef]
- Jones, M.G.; Rua, M.J. Conceptions of germs: Expert to novice understandings of microorganisms. Electron. J. Sci. Educ. 2006, 10, 3. [Google Scholar]
- Lecky, D.M.; McNulty, C.A.M.; Touboul, P.; Herotova, T.K.; Beneš, J.; Dellamonica, P.; Verlander, N.Q.; Kostkova, P.; Weinberg, J. Evaluation of e-bug, an educational pack, teaching about prudent antibiotic use and hygiene, in the Czech Republic, France and England. J. Antimicrob. Chemother. 2010, 65, 2674–2684. [Google Scholar] [CrossRef] [PubMed]
- Young, V.L.; Rajapandian, V.; Eley, C.V.; Hoekstra, B.A.; Lecky, D.M.; McNulty, C.A. Monitoring web site usage of e-bug: A hygiene and antibiotic awareness resource for children. JMIR Res. Protoc. 2015, 4, e131. [Google Scholar] [CrossRef] [PubMed]
- Hale, A.R.; Young, V.L.; Grand, A.; McNulty, C.A.M. Can gaming increase antibiotic awareness in Children? A mixed-methods approach. JMIR Serious Games 2017, 5, e5. [Google Scholar] [CrossRef] [PubMed]
| Description | N | % | |
|---|---|---|---|
| Total Schools (9) | School 1 students | 87 | 26.6 |
| School 2 students | 29 | 8.9 | |
| School 3 students | 14 | 4.3 | |
| School 4 students | 11 | 3.4 | |
| School 5 students | 40 | 12.2 | |
| School 6 students | 47 | 14.4 | |
| School 7 students | 14 | 4.3 | |
| School 8 students | 27 | 8.3 | |
| School 9 students | 58 | 17.7 | |
| Gender (overall) | Male | 160 | 48.9 |
| Female | 167 | 51.1 | |
| School Type | Private | 221 | 67.6 |
| Government | 81 | 24.8 | |
| Charitable | 25 | 7.6 | |
| School Syllabus | State | 251 | 76.8 |
| CBSE | 76 | 23.2 | |
| Questions | Correct (%) | Incorrect (%) | p-Value @ | |
|---|---|---|---|---|
| Q1: Antimicrobials are used to kill bacteria | Pre | 85.0 | 15.0 | <0.001 * |
| Post | 93.9 | 6.1 | ||
| Q2: You should always finish your course of antimicrobials | Pre | 77.1 | 22.9 | <0.001 * |
| Post | 93.0 | 7.0 | ||
| Q3: We should always cover our coughs and sneezes | Pre | 92.0 | 8.0 | 0.869 |
| Post | 92.4 | 7.6 | ||
| Q4: All microbes on our hands are good for us | Pre | 92.0 | 8.0 | 0.086 |
| Post | 95.1 | 4.9 | ||
| Q5: We should only wash our hands once a day | Pre | 92.4 | 7.6 | 0.011 * |
| Post | 96.0 | 4.0 | ||
| Q6: Some microbes can make us ill | Pre | 89.3 | 10.7 | 0.238 |
| Post | 91.7 | 8.3 | ||
| Q7: We use some microbes to make bread and yogurt | Pre | 49.8 | 50.2 | <0.001 * |
| Post | 84.1 | 15.9 | ||
| Q8: You can pick-up microbes from door handles | Pre | 51.4 | 48.6 | <0.001 * |
| Post | 75.2 | 24.8 | ||
| Q9: Microbes can multiply very fast | Pre | 84.1 | 15.9 | <0.001 * |
| Post | 95.1 | 4.9 | ||
| Q10: If you cannot see a microbe, it is not there. | Pre | 70.6 | 29.4 | <0.001 * |
| Post | 85.0 | 15.0 | ||
| Questions | School 1 (n) | School 2 (n) | School 3 (n) | School 4 (n) | School 5 (n) | School 6 (n) | School 7 (n) | School 8 (n) | School 9 (n) | Overall % (Correct) $ | p-Value |
|---|---|---|---|---|---|---|---|---|---|---|---|
| Q1 | 86 | 29 | 14 | 10 | 28 | 45 | 14 | 27 | 54 | 93.9 | <0.001 # |
| Q2 | 82 | 27 | 14 | 11 | 34 | 46 | 12 | 26 | 52 | 93.0 | 0.248 |
| Q3 | 84 | 27 | 14 | 10 | 28 | 46 | 13 | 27 | 53 | 92.4 | <0.001 # |
| Q4 | 83 | 28 | 14 | 9 | 36 | 46 | 14 | 27 | 54 | 95.1 | 0.223 |
| Q5 | 83 | 29 | 14 | 9 | 39 | 45 | 12 | 27 | 56 | 96.0 | 0.114 |
| Q6 | 77 | 27 | 12 | 11 | 37 | 46 | 13 | 24 | 53 | 91.7 | 0.692 |
| Q7 | 66 | 28 | 13 | 11 | 33 | 41 | 13 | 25 | 45 | 84.1 | 0.057 |
| Q8 | 59 | 22 | 11 | 10 | 42 | 32 | 12 | 24 | 42 | 75.2 | 0.191 |
| Q9 | 81 | 27 | 14 | 11 | 39 | 47 | 12 | 24 | 56 | 95.1 | 0.243 |
| Q10 | 72 | 27 | 11 | 9 | 31 | 47 | 8 | 26 | 47 | 84.0 | <0.001 # |
© 2019 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Fernandes, R.; Naik, S.; Bhat, A.-G.; Shetty, R.; Hande, M.-H.; Ghafur, A.; Rao, M.; Kunhikatta, V.; Pathiraj, J.-P.-K. Knowledge Assessment of E-Bug Assisted Antimicrobial Resistance Education Module in Class VII School Students of South Indian Coastal Town of Manipal. J. Clin. Med. 2019, 8, 84. https://doi.org/10.3390/jcm8010084
Fernandes R, Naik S, Bhat A-G, Shetty R, Hande M-H, Ghafur A, Rao M, Kunhikatta V, Pathiraj J-P-K. Knowledge Assessment of E-Bug Assisted Antimicrobial Resistance Education Module in Class VII School Students of South Indian Coastal Town of Manipal. Journal of Clinical Medicine. 2019; 8(1):84. https://doi.org/10.3390/jcm8010084
Chicago/Turabian StyleFernandes, Reona, Swathi Naik, Archana-Gururaj Bhat, Rashmi Shetty, Manjunatha-H Hande, Abdul Ghafur, Mahadev Rao, Vijayanarayana Kunhikatta, and John-Preshanth-Kumar Pathiraj. 2019. "Knowledge Assessment of E-Bug Assisted Antimicrobial Resistance Education Module in Class VII School Students of South Indian Coastal Town of Manipal" Journal of Clinical Medicine 8, no. 1: 84. https://doi.org/10.3390/jcm8010084
APA StyleFernandes, R., Naik, S., Bhat, A.-G., Shetty, R., Hande, M.-H., Ghafur, A., Rao, M., Kunhikatta, V., & Pathiraj, J.-P.-K. (2019). Knowledge Assessment of E-Bug Assisted Antimicrobial Resistance Education Module in Class VII School Students of South Indian Coastal Town of Manipal. Journal of Clinical Medicine, 8(1), 84. https://doi.org/10.3390/jcm8010084






