Perioperative Goal-Directed Therapy during Kidney Transplantation: An Impact Evaluation on the Major Postoperative Complications
Abstract
:1. Introduction
2. Materials and Methods
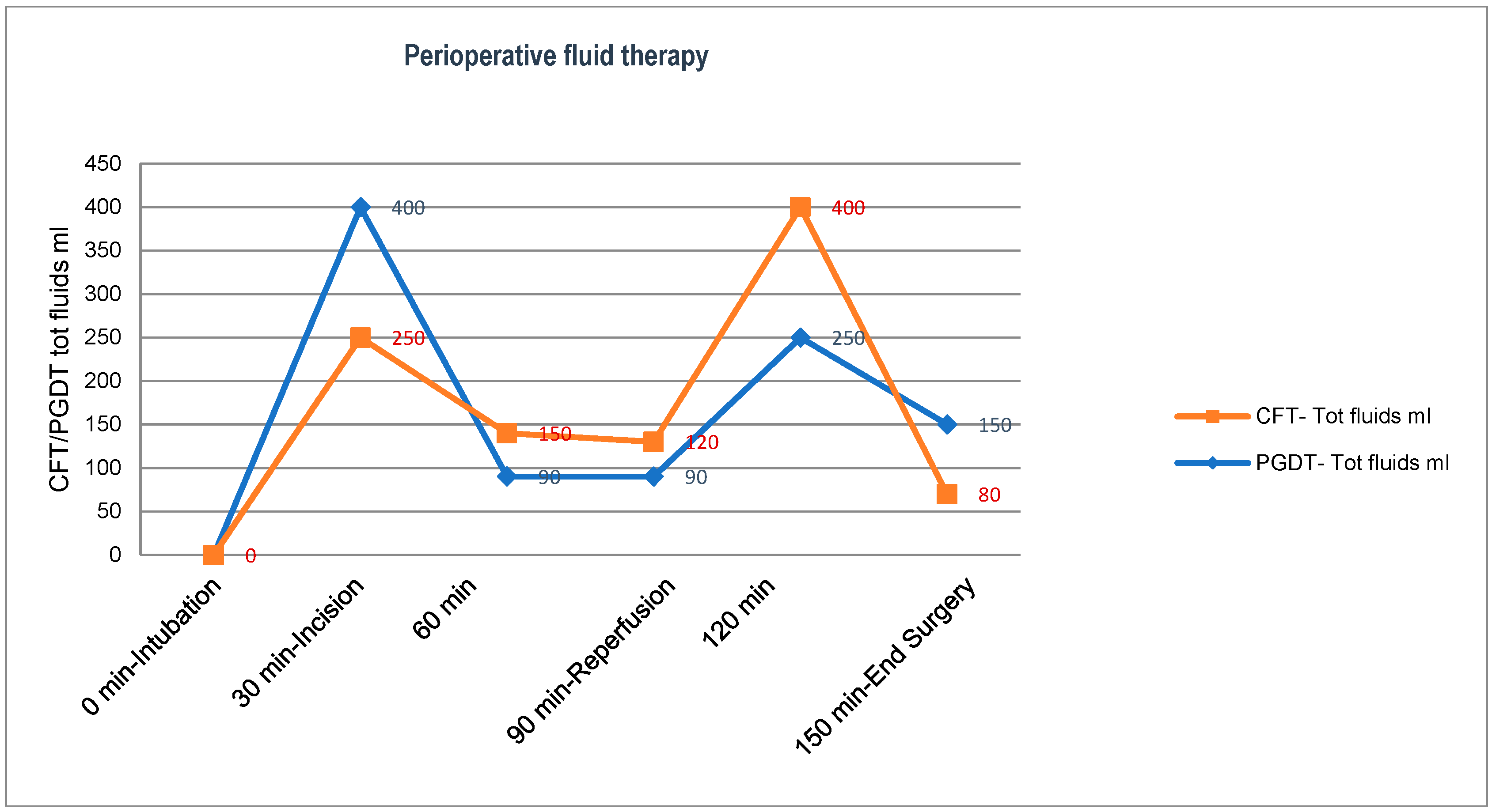
2.1. Intraoperative Phase
2.2. Postoperative Phase
2.3. Statistical Analysis
3. Results
4. Discussion
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Conflicts of Interest
Abbreviations
| ACS | acute coronary syndromes |
| AF | atrial fibrillation |
| AKI | acute kidney injury |
| ASA | American Society of Anesthesiology |
| ATG | anti thymocyte globulin |
| BIS | bispectral index |
| BMI | body mass index |
| BUN | blood urea nitrogen |
| CFT. | conventional fluid therapy |
| CI | cardiac index |
| CIT | cold ischemia time |
| CyA | cyclosporine |
| CV | cardiovascular |
| CVP | central venous pressure |
| DBP | diastolic blood pressure |
| DGF. | delayed graft function |
| ECG. | electrocardiogram |
| ESRD. | end stage renal disease |
| EtCO2 | end tidal CO2 |
| EVE | everolimus |
| GI | gastrointestinal |
| HR | heart rate |
| ICU. | intensive care unit |
| IBP | invasive blood pressure |
| IQR | interquartile range |
| IVCCI | inferior vena cava collapsibility index |
| LOS | length of stay |
| MAC | minimum alveolar concentration |
| MAP | mean arterial pressure |
| MPA | mycophenolic acid |
| NaCl | 0.9% normal saline 0.9% |
| NIBP | non-invasive blood pressure |
| NICE | National Institute of Health and Care Excellence |
| NRS | numeric rating scale |
| NS | not significative |
| PCWP | pulmonary capillary wedge pressure |
| PGDT. | perioperative goal directed therapy |
| PONV | postoperative nausea and vomiting |
| PPV | pulse pressure variation |
| RA | ringer acetate |
| RR | respiratory rate |
| SBP | systolic blood pressure |
| SpO2 | peripheral saturation of oxygen |
| Ster | steroids |
| SV | stroke volume |
| SVI | stroke volume index |
| SPV | systolic pressure variation |
| SVV | stroke volume variation |
| SVR/SVRI | systemic vascular resistance index |
| TAC | tacrolimus |
| v | train of four |
References
- Diaz, G.; O’Connor, M. Cardiovascular and renal complications in patients receiving a solid-organ transplant. Curr. Opin. Crit. Care 2011, 17, 382–389. [Google Scholar] [CrossRef] [PubMed]
- Collins, A.J.; Foley, R.N.; Chavers, B.; Gilbertson, D.; Herzog, C.; Ishani, A.; Johansen, K.; Kasiske, B.L.; Kutner, N.; Liu, J.; et al. US Renal Data System 2013 Annual Data Report. Am. J. Kidney Dis. 2014, 63, A7. [Google Scholar] [CrossRef] [PubMed]
- Neale, J.; Smith, A.C. Cardiovascular risk factors following renal transplant. World J. Transplant. 2015, 5, 183–195. [Google Scholar] [CrossRef]
- Farrugia, D.; Cheshire, J.; Begaj, I.; Khosla, S.; Ray, D.; Sharif, A. Death within the first year after kidney transplantation—An observational cohort study. Transpl. Int. 2014, 27, 262–270. [Google Scholar] [CrossRef] [PubMed]
- Ojo, A.O. Cardiovascular complications after kidney transplantation and their prevention. Transplantation 2006, 82, 603–611. [Google Scholar] [CrossRef] [PubMed]
- Zeyneloglu, P. Respiratory complications after solid-organ transplantation. Exp. Clin. Transplant. 2015, 13, 115–125. [Google Scholar] [PubMed]
- Canet, E.; Osman, D.; Lambert, J.; Guitton, C.; Heng, A.E.; Argaud, L.; Klouche, K.; Mourad, G.; Legendre, C.; Timsit, J.F.; et al. Acute respiratory failure in kidney transplant recipients: A multicenter study. Crit. Care 2011, 15, R91. [Google Scholar] [CrossRef]
- Santos, F.; Guimaraes, J.; Araujo, A.M.; Nunes, C.S.; Casal, M. Deceased-donor Kidney Transplantation: Predictive Factors and Impact on Postoperative Outcome. Transplant. Proc. 2015, 47, 933–937. [Google Scholar] [CrossRef]
- Yee, J.; Parasuraman, R.; Narins, R.G. Selective review of key perioperative renal-electrolyte disturbances in chronic renal failure patients. Chest 1999, 115, 149S–157S. [Google Scholar] [CrossRef]
- Calixto Fernandes, M.H.; Schricker, T.; Magder, S.; Hatzakorzian, R. Perioperative fluid management in kidney transplantation: A black box. Crit. Care 2018, 22, 14. [Google Scholar] [CrossRef]
- Veroux, M.; Grosso, G.; Corona, D.; Mistretta, A.; Giaquinta, A.; Giuffrida, G.; Sinagra, N.; Veroux, P. Age is an important predictor of kidney transplantation outcome. Nephrol. Dial. Transplant. 2012, 27, 1663–1671. [Google Scholar] [CrossRef] [PubMed]
- Toth, M.; Reti, V.; Gondos, T. Effect of recipients’ peri-operative parameters on the outcome of kidney transplantation. Clin. Transplant. 1998, 12, 511–517. [Google Scholar] [PubMed]
- Chappell, D.; Jacob, M.; Hofmann-Kiefer, K.; Conzen, P.; Rehm, M. A rational approach to perioperative fluid management. Anesthesiology 2008, 109, 723–740. [Google Scholar] [CrossRef] [PubMed]
- Spiro, M.D.; Eilers, H. Intraoperative care of the transplant patient. Anesthesiol. Clin. 2013, 31, 705–721. [Google Scholar] [CrossRef] [PubMed]
- Schnuelle, P.; Johannes van der Woude, F. Perioperative fluid management in renal transplantation: A narrative review of the literature. Transpl. Int. 2006, 19, 947–959. [Google Scholar] [CrossRef] [PubMed]
- Othman, M.M.; Ismael, A.Z.; Hammouda, G.E. The impact of timing of maximal crystalloid hydration on early graft function during kidney transplantation. Anesth. Analg. 2010, 110, 1440–1446. [Google Scholar] [CrossRef] [PubMed]
- Chaumont, M.; Racape, J.; Broeders, N.; El Mountahi, F.; Massart, A.; Baudoux, T.; Hougardy, J.M.; Mikhalsky, D.; Hamade, A.; Le Moine, A.; et al. Delayed Graft Function in Kidney Transplants: Time Evolution, Role of Acute Rejection, Risk Factors, and Impact on Patient and Graft Outcome. J. Transplant. 2015, 2015, 163757. [Google Scholar] [CrossRef]
- De Gasperi, A.; Narcisi, S.; Mazza, E.; Bettinelli, L.; Pavani, M.; Perrone, L.; Grugni, C.; Corti, A. Perioperative fluid management in kidney transplantation: Is volume overload still mandatory for graft function? Transplant. Proc. 2006, 38, 807–809. [Google Scholar] [CrossRef]
- Ciapetti, M.; di Valvasone, S.; di Filippo, A.; Cecchi, A.; Bonizzoli, M.; Peris, A. Low-dose dopamine in kidney transplantation. Transplant. Proc. 2009, 41, 4165–4168. [Google Scholar] [CrossRef]
- Brienza, N.; Giglio, M.T.; Marucci, M.; Fiore, T. Does perioperative hemodynamic optimization protect renal function in surgical patients? A meta-analytic study. Crit. Care Med. 2009, 37, 2079–2090. [Google Scholar] [CrossRef]
- Kumar, A.; Anel, R.; Bunnell, E.; Habet, K.; Zanotti, S.; Marshall, S.; Neumann, A.; Ali, A.; Cheang, M.; Kavinsky, C.; et al. Pulmonary artery occlusion pressure and central venous pressure fail to predict ventricular filling volume, cardiac performance, or the response to volume infusion in normal subjects. Crit. Care Med. 2004, 32, 691–699. [Google Scholar] [CrossRef] [PubMed]
- Marik, P.E.; Cavallazzi, R. Does the central venous pressure predict fluid responsiveness? An updated meta-analysis and a plea for some common sense. Crit. Care Med. 2013, 41, 1774–1781. [Google Scholar] [CrossRef] [PubMed]
- Marik, P.E.; Baram, M.; Vahid, B. Does central venous pressure predict fluid responsiveness? A systematic review of the literature and the tale of seven mares. Chest 2008, 134, 172–178. [Google Scholar] [CrossRef] [PubMed]
- Chamos, C.; Vele, L.; Hamilton, M.; Cecconi, M. Less invasive methods of advanced hemodynamic monitoring: Principles, devices, and their role in the perioperative hemodynamic optimization. Perioper. Med. 2013, 2, 19. [Google Scholar] [CrossRef] [PubMed]
- Headley, J.M. Arterial pressure-based technologies: A new trend in cardiac output monitoring. Crit. Care Nurs. Clin. N. Am. 2006, 18, 179–187. [Google Scholar] [CrossRef] [PubMed]
- Toyoda, D.; Fukuda, M.; Iwasaki, R.; Terada, T.; Sato, N.; Ochiai, R.; Kotake, Y. The comparison between stroke volume variation and filling pressure as an estimate of right ventricular preload in patients undergoing renal transplantation. J. Anesth. 2015, 29, 40–46. [Google Scholar] [CrossRef]
- Cannesson, M.; Ramsingh, D.; Rinehart, J.; Demirjian, A.; Vu, T.; Vakharia, S.; Imagawa, D.; Yu, Z.; Greenfield, S.; Kain, Z. Perioperative goal-directed therapy and postoperative outcomes in patients undergoing high-risk abdominal surgery: A historical-prospective, comparative effectiveness study. Crit. Care 2015, 19, 261. [Google Scholar] [CrossRef]
- Grosso, G.; Corona, D.; Mistretta, A.; Zerbo, D.; Sinagra, N.; Giaquinta, A.; Cimino, S.; Ekser, B.; Giuffrida, G.; Leonardi, A.; et al. Delayed graft function and long-term outcome in kidney transplantation. Transplant. Proc. 2012, 44, 1879–1883. [Google Scholar] [CrossRef] [PubMed]
- Abramowicz, D.; Cochat, P.; Claas, F.H.; Heemann, U.; Pascual, J.; Dudley, C.; Harden, P.; Hourmant, M.; Maggiore, U.; Salvadori, M.; et al. European Renal Best Practice Guideline on kidney donor and recipient evaluation and perioperative care. Nephrol. Dial. Transplant. 2015, 30, 1790–1797. [Google Scholar] [CrossRef]
- Kumar, A.; Cannon, C.P. Acute coronary syndromes: Diagnosis and management, part I. Mayo Clin. Proc. 2009, 84, 917–938. [Google Scholar] [CrossRef]
- Delville, M.; Sabbah, L.; Girard, D.; Elie, C.; Manceau, S.; Piketty, M.; Martinez, F.; Mejean, A.; Legendre, C.; Sberro-Soussan, R. Prevalence and predictors of early cardiovascular events after kidney transplantation: Evaluation of pre-transplant cardiovascular work-up. PLoS ONE 2015, 10, e0131237. [Google Scholar] [CrossRef]
- Marik, P.E.; Cavallazzi, R.; Vasu, T.; Hirani, A. Dynamic changes in arterial waveform derived variables and fluid responsiveness in mechanically ventilated patients: A systematic review of the literature. Crit. Care Med. 2009, 37, 2642–2647. [Google Scholar] [CrossRef] [PubMed]
- Hamilton, M.A.; Cecconi, M.; Rhodes, A. A systematic review and meta-analysis on the use of preemptive hemodynamic intervention to improve postoperative outcomes in moderate and high-risk surgical patients. Anesth. Analg. 2011, 112, 1392–1402. [Google Scholar] [CrossRef]
- Scheeren, T.W.; Wiesenack, C.; Gerlach, H.; Marx, G. Goal-directed intraoperative fluid therapy guided by stroke volume and its variation in high-risk surgical patients: A prospective randomized multicentre study. J. Clin. Monit. Comput. 2013, 27, 225–233. [Google Scholar] [CrossRef] [PubMed]
- Giglio, M.T.; Marucci, M.; Testini, M.; Brienza, N. Goal-directed haemodynamic therapy and gastrointestinal complications in major surgery: A meta-analysis of randomized controlled trials. Br. J. Anaesth. 2009, 103, 637–646. [Google Scholar] [CrossRef] [PubMed]
- Corcoran, T.; Rhodes, J.E.; Clarke, S.; Myles, P.S.; Ho, K.M. Perioperative fluid management strategies in major surgery: A stratified meta-analysis. Anesth. Analg. 2012, 114, 640–651. [Google Scholar] [CrossRef] [PubMed]
- Stoumpos, S.; Jardine, A.G.; Mark, P.B. Cardiovascular morbidity and mortality after kidney transplantation. Transpl. Int. 2015, 28, 10–21. [Google Scholar] [CrossRef]
- Perico, N.; Cattaneo, D.; Sayegh, M.H.; Remuzzi, G. Delayed graft function in kidney transplantation. Lancet 2004, 364, 1814–1827. [Google Scholar] [CrossRef]
- Gill, J.; Dong, J.; Rose, C.; Gill, J.S. The risk of allograft failure and the survival benefit of kidney transplantation are complicated by delayed graft function. Kidney Int. 2016, 89, 1331–1336. [Google Scholar] [CrossRef]
- Ojo, A.O.; Wolfe, R.A.; Held, P.J.; Port, F.K.; Schmouder, R.L. Delayed graft function: Risk factors and implications for renal allograft survival. Transplantation 1997, 63, 968–974. [Google Scholar] [CrossRef]
- De Gasperi, A.; Feltracco, P.; Ceravola, E.; Mazza, E. Pulmonary complications in patients receiving a solid-organ transplant. Curr. Opin. Crit. Care 2014, 20, 411–419. [Google Scholar] [CrossRef] [PubMed]
| Characteristics | PGDT | CFT | p-Value |
|---|---|---|---|
| N | 33 | 33 | |
| Age (years) | 50 ± 9.7 | 53 ± 10 | 0.638 |
| Sex (M/F) | 20/13 | 19/14 | 0.732 |
| BMI (kg/m2) | 24.8 ± 5 | 24.3 ± 4.2 | 0.443 |
| Waiting list (months) | 23.9 ± 18.1 | 27.1 ± 21.4 | 0.434 |
| Recipient cause of ESRD (n) | |||
| Polycystic kidney disease | 10 (33.3%) | 9 (27.3%) | 0.543 |
| Diabetes | 8 (24.3%) | 3 (9%) | <0.05 |
| Other/unknown | 15 (45.4%) | 21 (63.6%) | <0.05 |
| Pre-transplant dialysis (months) | 40.4 ± 32.1 | 46.7 ± 32 | 0.328 |
| Hemodialysis/peritoneal dialysis | 26/7 | 30/2 | 0.184 |
| Recipient comorbidities (n) | |||
| Hypertension | 30 (90%) | 28 (84.8%) | 0.543 |
| Previous acute myocardial infarction | 5 (15.1%) | 4 (12.1%) | 0.388 |
| Donor age (yr) | 51.7 ± 16 | 52.1 ± 15.7 | 0.264 |
| Donor Comorbidities (n) | |||
| Hypertension | 12 (36.3%) | 11 (33.3%) | 0.953 |
| Diabetes | 7 (21.2%) | 1 (3%) | <0.05 |
| Donor intensive care unit stay | 5.2 ± 2.1 | 5.2 ± 3.5 | 0.825 |
| Terminal serum creatinine (mg/dL) | 0.8 ± 0.2 | 0.7 ± 0.2 | 0.896 |
| Cold ischemia time (min) | 822 ± 370.2 | 744 ± 376.1 | 0.243 |
| Operative time (min) | 148.2 ± 71.7 | 157.9 ± 46.1 | 0.723 |
| Immunosuppression (n) | |||
| Induction | 18 (54.5%) | 17 (51.5%) | 0.742 |
| Tac + MPA + Ster | 25 (75.7%) | 24 (72.7%) | 0.456 |
| CyA + MPA + Ster | 3 (9%) | 2 (6%) | 0.765 |
| Ever + Tac + Ster | 5 (15.1%) | 7 (21.2%) | 0.523 |
| Blood loss (mL) | 300 ± 122 | 322 ± 142 | 0.221 |
| DGF | 4 (12.1%) | 11 (32.5%) | <0.05 |
| Duration of DGF (days) | 3.2 ± 1.2 | 8.3 ± 3.5 | <0.05 |
| Acute rejection | 1 (3%) | 1 (3%) | 1 |
| Postoperative hospital stay (days) | 14.5 ± 6.1 | 13.6 ± 16.5 | 0.321 |
| Mean 7-day serum creatinine (mg/dL) | 2.23 | 2.85 | <0.05 |
| Mean 30-day serum creatinine (mg/dL) | 1.35 | 1.55 | <0.05 |
| Intraoperative | PGDT Group | CFT Group | p Value |
|---|---|---|---|
| SBP/DBP | 114 ± 10/61 ± 7 mmHg | 109 ± 8/61 ± 5 mmHg | 0.3/0.2 |
| MAP | 78 ± 2 mmHg | 77 ± 2 mmHg | 0.2 |
| SVI | 51 ± 4 mL/min/m2 | / | / |
| CI | 4.2 L/min/m2 | / | / |
| Tot fluids (median-IQR) | 980 (700) mL | 1000 (250) mL | 0.2 |
| RA/NaCl 0.9% | 830 vs. 150 mL (85% vs. 15%) | 800 vs. 200 mL (80% vs. 20%) | / |
| Urine output (median-IQR) | 100 (650) mL | 100 (400) mL | 0.09 |
| CFT Group | PGDT Group | p Value | |||||
|---|---|---|---|---|---|---|---|
| Average Values | T1 | T2 | T3 | T1 | T2 | T3 | T1/T2/T3 |
| Serum Creatinine, mg/dL | 5.5 ± 2.5 | 5.4 ± 2.4 | 2.8 ± 1.4 | 7.7 ± 3.1 | 6.4 ± 3.1 | 2.2 ± 1.5 | <0.05/0.08/<0.05 |
| Blood Urea Nitrogen, mg/dL | 143 ± 47 | 143 ± 47 | 132 ± 47 | 125 ± 50 | 140 ± 50 | 140 ± 54 | 0.06/0.4/0.3 |
| Serum potassium, mmol/L | 4.3 ± 0.5 | 4.3 ± 0.6 | 4.1 ± 0.3 | 4.5 ± 0.8 | 4.1 ± 0.7 | 4.2 ± 0.6 | 0.07/0.1/0.4 |
| SpO2 % | 95 ± 2 | 96 ± 1.8 | 97 ± 1.5 | 95 ± 2 | 95 ± 2.1 | 98 ± 1.8 | 0.5/0.09/0.07 |
| NIBP | 131 ± 17/74 ± 10 | 129 ± 14/74 ± 12 | 131 ± 14/73 ± 9 | 134 ± 19/75 ± 12 | 135 ± 16/75 ± 9 | 135 ± 17/77 ± 10 | 0.2–0.3/0.06–0.3/0.2–0.06 |
| Heart rate, bpm | 83 ± 8.2 | 82 ± 9.6 | 80 ± 7.1 | 81 ± 11 | 82 ± 11 | 77 ± 10 | 0.1/0.4/0.06 |
| Urinary output, mL/h | 131 ± 66 | 131 ± 65 | 95 ± 47 | 125 ± 120 | 119 ± 68 | 97 ± 46 | 0.1/0.06/0.2 |
| CV Complications ACS | Complications+ (T3) | Complications− (T3) | CV Complications− Congestive Failure | Complications+ (T3) | Complications− (T3) |
|---|---|---|---|---|---|
| PGDT (n) | 1 (3%) | 32 (97%) | PGDT (n) | 0 (0%) | 33 (100%) |
| CFT (n) | 6 (18.2%) | 27 (81.8%) | CFT (n) | 1 (3%) | 32 (97%) |
| Total (n) | 7 (9%) | 59 (91%) | Total (n) | 1 (1.5%) | 65 (98.5%) |
| Chi-square Fisher’s exact test | p < 0.05 | / | Chi-square Fisher’s exact test | p > 0.05 | / |
| Pulmonary Complications RDS | Complications+ (T3) | Complications− (T3) | Pulmonary Complications Pneumonia | Complications+ (T3) | Complication− (T3) |
|---|---|---|---|---|---|
| PGDT (n) | 0 (0%) | 33 (100%) | PGDT (n) | 1 (3%) | 32 (97%) |
| CFT (n) | 1 (3%) | 32 (97%) | CFT (n) | 0 (0%) | 33 (100%) |
| Total (n) | 1 (1.5%) | 65 (98.5%) | Total (n) | 1 (1.5%) | 65 (98.5%) |
| Chi-square Fisher’s exact test | p > 0.05 | / | Chi-square Fisher’s exact test | p > 0.05 | / |
| DGF/Hemodialysis | Complications+ (T3) | Complication− (T3) | GI Complications Postoperative Ileus | Complications+ (T2) | Complications (T2) |
|---|---|---|---|---|---|
| PGDT (n) | 4 (12.1%) | 29 (87.9%) | PGDT (n) | 3 (9.1%) | 30 (90.9%) |
| CFT (n) | 11 (33%) | 22 (67%) | CFT (n) | 26 (78.8%) | 7 (21.2%) |
| Total (n) | 15 (23%) | 51 (77%) | Total (n) | 29 (43.9%) | 37 (56.1%) |
| Chi-square Fisher’s exact test | p < 0.05 | / | Chi-square Fisher’s exact test | p < 0.01 | / |
| 30-Day Morbidity | Cardiovascular Complications | Renal Complications | Pulmonary Complications |
|---|---|---|---|
| PGDT | 0 (0%) | 1 (3%) | 0 (0%) |
| CFT | 2 (6%) | 1 (3%) | 1 (3%) |
| Total | 2 (6%) | 2 (6%) | 1 (3%) |
| / | p > 0.05 | p > 0.05 | p > 0.05 |
© 2019 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Cavaleri, M.; Veroux, M.; Palermo, F.; Vasile, F.; Mineri, M.; Palumbo, J.; Salemi, L.; Astuto, M.; Murabito, P. Perioperative Goal-Directed Therapy during Kidney Transplantation: An Impact Evaluation on the Major Postoperative Complications. J. Clin. Med. 2019, 8, 80. https://doi.org/10.3390/jcm8010080
Cavaleri M, Veroux M, Palermo F, Vasile F, Mineri M, Palumbo J, Salemi L, Astuto M, Murabito P. Perioperative Goal-Directed Therapy during Kidney Transplantation: An Impact Evaluation on the Major Postoperative Complications. Journal of Clinical Medicine. 2019; 8(1):80. https://doi.org/10.3390/jcm8010080
Chicago/Turabian StyleCavaleri, Marco, Massimiliano Veroux, Filippo Palermo, Francesco Vasile, Mirko Mineri, Joseph Palumbo, Lorenzo Salemi, Marinella Astuto, and Paolo Murabito. 2019. "Perioperative Goal-Directed Therapy during Kidney Transplantation: An Impact Evaluation on the Major Postoperative Complications" Journal of Clinical Medicine 8, no. 1: 80. https://doi.org/10.3390/jcm8010080
APA StyleCavaleri, M., Veroux, M., Palermo, F., Vasile, F., Mineri, M., Palumbo, J., Salemi, L., Astuto, M., & Murabito, P. (2019). Perioperative Goal-Directed Therapy during Kidney Transplantation: An Impact Evaluation on the Major Postoperative Complications. Journal of Clinical Medicine, 8(1), 80. https://doi.org/10.3390/jcm8010080





