Comparison of LC-MS and LC-DAD Methods of Detecting Abused Piperazine Designer Drugs
Abstract
1. Introduction
2. Materials and Methods
2.1. Reagents and Solvents
2.2. Instrumentation
2.3. Chromatographic Conditions for LC-MS
2.4. Chromatographic Conditions for LC-DAD
2.5. LC-MS Analysis—Preparation of Calibration Samples
2.6. Biological Samples Preparation
2.7. LC-DAD Analysis—Preparation of Samples for Calibration
2.8. LC-DAD Analysis—Validation of the Method
2.9. LC-DAD Analysis—Linearity of the Method
2.10. LC-DAD Analysis—Analytical Limits
2.11. LC-DAD Analysis—Method Repeatability
3. Results
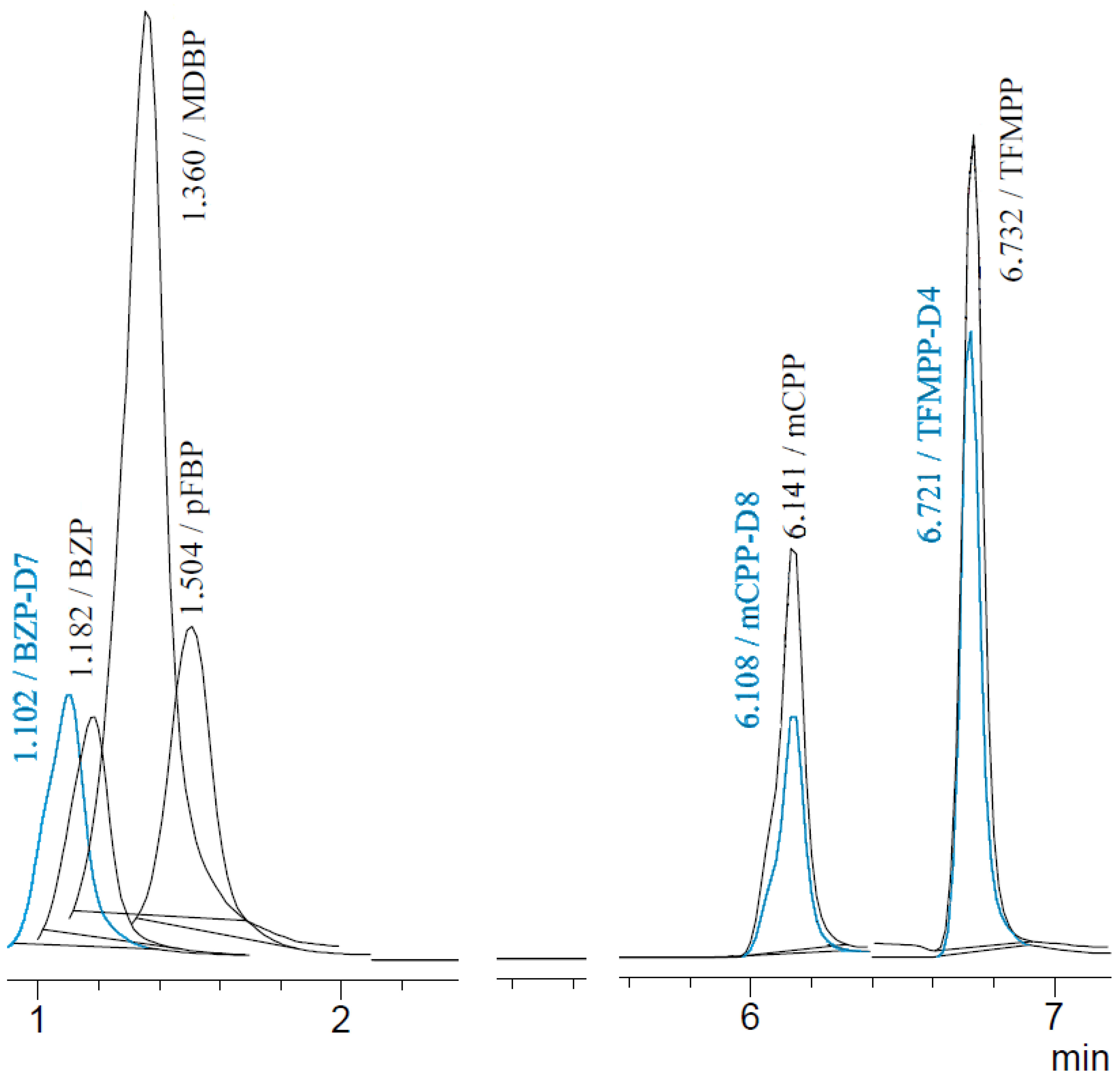
3.1. LC-MS Method—MRM Transitions and Chromatographic Separation
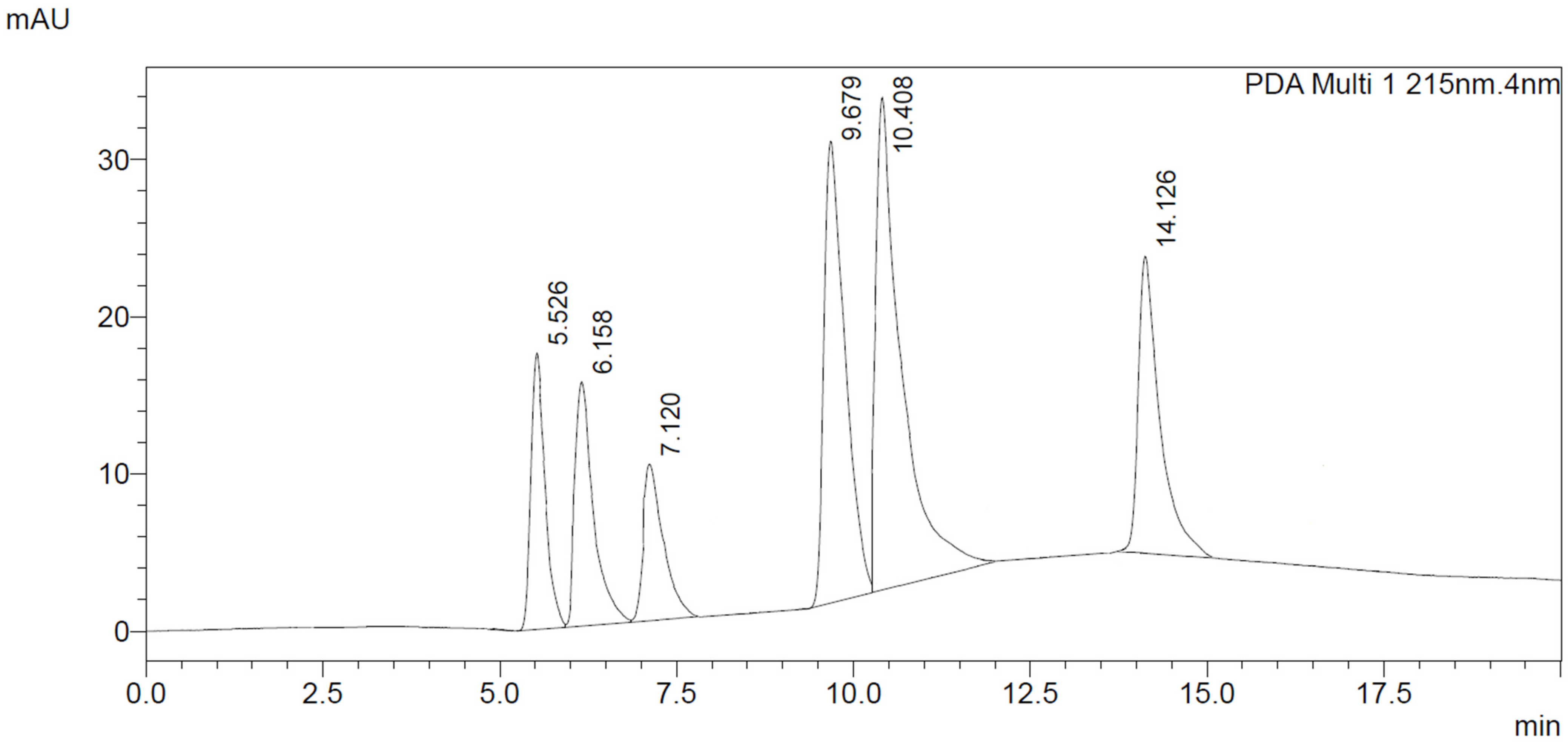
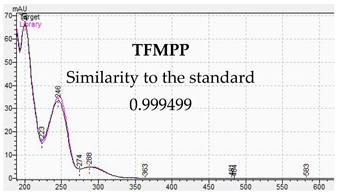
3.2. LC-DAD Method—UV-VIS Spectra and Chromatographic Separation
3.3. Validation of the LC-DAD Method (Measuring Range, Linearity, Repeatability, LOD and LOQ)
4. Discussion
4.1. LC-MS Method
4.2. LC-DAD Method
4.3. Comparison of LC-MS and LC-DAD Methods
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Conflicts of Interest
References
- Bertol, E.; Vaiano, F.; Mari, F.; Di Milia, M.G.; Bua, S.; Supuran, C.T.; Carta, F. Advances in new psychoactive substances identification: The U.R.I.To.N. Consortium. Enzym. J. Inhib. Med. Chem. 2017, 32, 841–849. [Google Scholar] [CrossRef] [PubMed]
- Shafi, A.; Berry, A.J.; Sumnall, H.; Wood, D.M.; Tracy, D.K. New psychoactive substances: A review and updates. Ther. Adv. Psychopharmacol. 2020, 10, 2045125320967197. [Google Scholar] [CrossRef]
- Vaiano, F.; Bertol, E.; Mineo, M.; Pietrosemoli, L.; Rubicondo, J.; Supuran, C.T.; Carta, F. Development of a New LC-MS/MS Screening Method for Detection of 120 NPS and 43 Drugs in Blood. Separations 2021, 8, 221. [Google Scholar] [CrossRef]
- Luethi, D.; Liechti, M.E. Designer drugs: Mechanism of action and adverse effects. Arch. Toxicol. 2020, 94, 1085–1133. [Google Scholar] [CrossRef]
- Giorgetti, A.; Pascali, J.P.; Fais, P.; Pelletti, G.; Gabbin, A.; Franchetti, G.; Cecchetto, G.; Viel, G. Molecular Mechanisms of Action of Novel Psychoactive Substances (NPS). A New Threat for Young Drug Users with Forensic-Toxicological Implications. Life 2021, 11, 440. [Google Scholar] [CrossRef] [PubMed]
- Varì, M.R.; Mannocchi, G.; Tittarelli, R.; Campanozzi, L.L.; Nittari, G.; Feola, A.; Ronchi, F.U.; Ricci, G. New Psychoactive Substances: Evolution in the Exchange of Information and Innovative Legal Responses in the European Union. Int. J. Environ. Res. Public Health 2020, 17, 8704. [Google Scholar] [CrossRef] [PubMed]
- Wadsworth, E.; Drummond, C.; Deluca, P. The Dynamic Environment of Crypto Markets: The Lifespan of New Psychoactive Substances (NPS) and Vendors Selling NPS. Brain Sci. 2018, 8, 46. [Google Scholar] [CrossRef] [PubMed]
- Madras, B.K. The Growing Problem of New Psychoactive Substances (NPS). In Neuropharmacology of New Psychoactive Substances (NPS); Current Topics in Behavioral Neurosciences; Springer: Berlin/Heidelberg, Germany, 2017; Volume 32, pp. 1–18. [Google Scholar] [CrossRef]
- Caccia, S. N-dealkylation of arylpiperazine derivatives: Disposition and metabolism of the 1-aryl-piperazines formed. Curr. Drug Metab. 2007, 8, 612–622. [Google Scholar] [CrossRef] [PubMed]
- Arbo, M.D.; Bastos, M.L.; Carmo, H.F. Piperazine compounds as drugs of abuse. Drug Alcohol Dep. 2012, 122, 174–185. [Google Scholar] [CrossRef]
- Kersten, B.P.; McLaughlin, M.E. Toxicology and management of novel psychoactive drugs. J. Pharm. 2015, 28, 50–65. [Google Scholar] [CrossRef] [PubMed]
- Ren, Y.; Du, J.; Du, X.; Xin, G.; Chang, J.; Zhou, H.; Hao, H. A novel analytical method of TFMPP and mCPP in fluids of drug addicts using LLE-GC/NPD. Technol. Health Care 2019, 27, 67–84. [Google Scholar] [CrossRef] [PubMed]
- Cohen, B.M.; Butler, R. BZP-party pills: A review of research on benzylpiperazine as a recreational drug. Int. J. Drug Policy 2011, 22, 95–101. [Google Scholar] [CrossRef] [PubMed]
- Dias da Silva, D.; Silva, M.J.; Moreira, P.; Martins, M.J.; Valente, M.J.; Carvalho, F.; Bastos, M.L.; Carmo, H. In vitro hepatotoxicity of ‘Legal X’: The combination of 1-benzylpiperazine (BZP) and 1-(m-trifluoromethylphenyl)piperazine (TFMPP) triggers oxidative stress, mitochondrial impairment and apoptosis. Arch. Toxicol. 2017, 91, 1413–1430. [Google Scholar] [CrossRef] [PubMed]
- Swortwood, M.J.; Boland, D.M.; De Caprio, A.P. Determination of 32 cathinone derivatives and other designer drugs in serum by comprehensive LC-QQQ-MS/MS analysis. Anal. Bioanal. Chem. 2013, 405, 1383–1397. [Google Scholar] [CrossRef] [PubMed]
- Bell, C.; George, C.; Kicman, A.T.; Traynor, A. Development of a rapid LC-MS/MSmethod for direct urinalysis of designer drugs. Drug Test. Anal. 2011, 3, 496–504. [Google Scholar] [CrossRef] [PubMed]
- Schep, L.J.; Slaughter, R.J.; Vale, J.A.; Beasley, D.M.G.; Gee, P. The clinical toxicology of the designer “party pills” benzylpiperazine and trifluoromethylphenylpiperazine. Clin. Toxicol. 2011, 49, 131–141. [Google Scholar] [CrossRef]
- Staack, R.F.; Maurer, H.H. New designer drug 1-(3,4-methylenedioxybenzyl) piperazine (MDBP): Studies on its metabolism and toxicological detection in rat urine using gas chromatography/mass spectrometry. J. Mass Spectrom. 2004, 39, 255–261. [Google Scholar] [CrossRef] [PubMed]
- Welz, A.; Koba, M. Piperazine derivatives as dangerous abused compounds. Acta Pharm. 2020, 70, 423–441. [Google Scholar] [CrossRef] [PubMed]
- Dolan, S.B.; Shetty, R.A.; Forster, M.J.; Gatch, M.B. Impure but not inactive: Behavioral pharmacology of dibenzylpiperazine, a common by-product of benzylpiperazine synthesis. J. Psychopharmacol. 2018, 32, 802–810. [Google Scholar] [CrossRef] [PubMed]
- Hondebrink, L.; Zwartsen, A.; Westerink, R.H.S. Effect fingerprinting of new psychoactive substances (NPS): What can we learn from in vitro data? Pharmacol. Ther. 2018, 182, 193–224. [Google Scholar] [CrossRef] [PubMed]
- Welz, A.; Koba, M.; Kośliński, P.; Siódmiak, J. Rapid Targeted Method of Detecting Abused Piperazine Designer Drugs. J. Clin. Med. 2021, 10, 5813. [Google Scholar] [CrossRef]
- Orsolini, L.; Papanti, G.D.; De Berardis, D.; Guirguis, A.; Corkery, J.M.; Schifano, F. The “Endless Trip” among the NPS Users: Psychopathology and Psychopharmacology in the Hallucinogen-Persisting Perception Disorder. A Systematic Review. Front. Psychiatry 2017, 8, 240. [Google Scholar] [CrossRef] [PubMed]
- Katz, D.P.; Deruiter, J.; Bhattacharya, D.; Ahuja, M.; Bhattacharya, S.; Clark, C.R. Benzylpiperazine: “A messy drug”. Drug Alcohol Dep. 2016, 164, 1–7. [Google Scholar] [CrossRef] [PubMed]
- Lau, T.; LeBlanc, R.; Botch-Jones, S. Stability of Synthetic Piperazines in Human Whole Blood. J. Anal. Toxicol. 2018, 42, 88–98. [Google Scholar] [CrossRef]
- Elliott, S. Current awareness of piperazines: Pharmacology and toxicology. Drug Test. Anal. 2011, 3, 430–438. [Google Scholar] [CrossRef]
- Smith, C.D.; Robert, S. ‘Designer drugs’: Update on the management of novel psychoactive substance misuse in the acute care setting. Clin. Med. 2014, 14, 409–415. [Google Scholar] [CrossRef] [PubMed]
- Simmler, L.D.; Rickli, A.; Schramm, Y.; Hoener, M.C.; Liechti, M.E. Pharmacological profiles of aminoindanes, piperazines, and pipradrol derivatives. Biochem. Pharmacol. 2014, 88, 237–244. [Google Scholar] [CrossRef]
- Wood, D.M.; Button, J.; Lidder, S.; Ramsey, J.; Holt, D.W.; Dargan, P.I. Dissociative and sympathomimetic toxicity associated with recreational use of 1-(3-Trifluoromethylphenyl)piperazine (TFMPP) and 1-Benzylpiperazine (BZP). J. Med. Toxicol. 2008, 4, 254–257. [Google Scholar] [CrossRef] [PubMed]
- Staack, R.F.; Theobald, D.S.; Paul, L.D.; Springer, D.; Kraemer, T.; Maurer, H.H. In vivo metabolism of the new designer drug 1-(4-methoxyphenyl)piperazine (MeOPP) in rat and identification of the human cytochrome P450 enzymes responsible for the major metabolic step. Xenobiotica 2004, 34, 179–192. [Google Scholar] [CrossRef]
- Kumar, H.K.; Yathirajan, H.S.; Chinthal, C.H.; Foro, S.; Glidewell, C. Crystal structures of the recreational drug N-(4-meth¬oxy¬phen¬yl)piperazine (MeOPP) and three of its salts. Acta Crystallogr. Crystallogr. Commun. 2020, 76, 488–495. [Google Scholar] [CrossRef] [PubMed]
- Musselman, M.E.; Hampton, J.P. “Not for Human Consumption”: A Review of Emerging Designer Drugs. Pharmacother. J. Hum. Pharmacol. Drug Ther. 2014, 34, 745–757. [Google Scholar] [CrossRef]
- Berney-Meyer, L.; Putt, T.; Schollum, J.; Walker, R. Nephrotoxicity of recreational party drugs. Nephrology 2012, 17, 99–103. [Google Scholar] [CrossRef] [PubMed]
- Lecompte, Y.; Roussel, O.; Perrin, M. 1-benzylpiperazine (BZP) and 1-(3 trifluoromethylphenyl)piperazine (TFMPP): Emergence of two agents which lead to misuse. Ann. Pharm. Fr. 2008, 66, 85–91. [Google Scholar] [CrossRef]
- Tancer, M.E.; Johanson, C.E. The subjective effects of MDMA and mCPP in moderate MDMA users. Drug Alcohol Dep. 2001, 65, 97–101. [Google Scholar] [CrossRef]
- Luethi, D.; Liechti, M.E. Monoamine Transporter and Receptor Interaction Profiles in Vitro Predict Reported Human Doses of Novel Psychoactive Stimulants and Psychedelics. Int. J. Neuropsychopharmacol. 2018, 21, 926–931. [Google Scholar] [CrossRef] [PubMed]
- Gaillard, Y.P.; Cuquel, A.C.; Boucher, A.; Romeuf, L.; Bevalot, F.; Prevosto, J.M.; Menard, J.M. A Fatality Following Ingestion of the Designer Drug Meta-Chlorophenylpiperazine (mCPP) in an Asthmatic—HPLC-MS/MS Detection in Biofluids and Hair. J. For. Sci. 2013, 58, 263–269. [Google Scholar] [CrossRef] [PubMed]
- Lee, H.; Wang, G.Y.; Curley, L.E.; Sollers, J.J.; Kydd, R.R.; Kirk, I.J.; Russell, B.R. Acute effects of BZP, TFMPP and the combination of BZP and TFMPP in comparison to dexamphetamine on an auditory oddball task using electroencephalography: A single-dose study. Psychopharmacology 2016, 233, 863–871. [Google Scholar] [CrossRef] [PubMed]
- Staack, R.F.; Maurer, H.H. Toxicological detection of the new designer drug 1-(4-methoxyphenyl)piperazine and its metabolites in urine and differentiation from an intake of structurally related medicaments using gas chromatography-mass spectrometry. J. Chromatogr. B Analyt. Technol. Biomed. Life Sci. 2003, 798, 333–342. [Google Scholar] [CrossRef]
- Welz, A.; Koba, M. Piperazine derivatives in designer drugs—Compounds of great popularity and high risk for human health. Farm. Pol. 2017, 73, 487–494. [Google Scholar]
- Boumrah, Y.; Rosset, M.; Lecompte, Y.; Bouanani, S.; Khimeche, K.; Dahmani, A. Development of a targeted GC/MS screening method and validation of an HPLC/DAD quantification method for piperazines-amphetamines mixtures in seized material. Egypt. J. Forensic Sci. 2014, 4, 90–99. [Google Scholar] [CrossRef]
- Arbo, M.D.; Silva, R.; Barbosa, D.J.; Dias da Silva, D.; Rossato, L.G.; Bastos, M.L.; Carmo, H. Piperazine designer drugs induce toxicity in cardiomyoblast h9c2 cells through mitochondrial impairment. Toxicol. Lett. 2014, 229, 178–189. [Google Scholar] [CrossRef]
- Zwartsen, A.; Korte, T.; Nacken, P.; Lange, D.W.; Westerink, R.H.S.; Hondebrink, L. Cardiotoxicity screening of illicit drugs and new psychoactive substances (NPS) in human iPSC-derived cardiomyocytes using microelectrode array (MEA) recordings. J. Mol. Cell. Cardiol. 2019, 136, 102–112. [Google Scholar] [CrossRef]
- Dias-da-Silva, D.; Arbo, M.D.; Valente, M.J.; Bastos, M.L.; Carmo, H. Hepatotoxicity of piperazine designer drugs: Comparison of different in vitro models. Toxicol. Vitr. 2015, 29, 987–996. [Google Scholar] [CrossRef] [PubMed]
- Persona, K.; Polus, A.; Góralska, J.; Gruca, A.; Dembińska-Kieć, A.; Piekoszewski, W. An In Vitro Study of the Neurotoxic Effects of N-Benzylpiperazine: A Designer Drug of Abuse. Neurotox. Res. 2016, 29, 558–568. [Google Scholar] [CrossRef][Green Version]
- Zwartsen, A.; Hondebrink, L.; Westerink, R.H.S. Neurotoxicity screening of new psychoactive substances (NPS): Effects on neuronal activity in rat cortical cultures using microelectrode arrays (MEA). Neurotoxicology 2018, 66, 87–97. [Google Scholar] [CrossRef] [PubMed]
- Min, C.R.; Kim, M.J.; Park, Y.J.; Kim, H.R.; Lee, S.Y.; Chung, K.H.; Oh, S.M. Estrogenic effects and their action mechanism of the major active components of party pill drugs. Toxicol. Lett. 2012, 214, 339–347. [Google Scholar] [CrossRef]
- Campbell, H.; Cline, W.; Evans, M.; Lloyd, J.; Peck, A.W. Comparison of the effects of dexamphetamine and 1-benzylpiperazine in former addicts. Eur. J. Clin. Pharmacol. 1973, 6, 170–176. [Google Scholar] [CrossRef]
- Scotton, W.J.; Hill, L.J.; Williams, A.C.; Barnes, N.M. Serotonin Syndrome: Pathophysiology, Clinical Features, Management, and Potential Future Directions. Int. J. Tryptophan Res. 2019, 12, 1178646919873925. [Google Scholar] [CrossRef] [PubMed]
- European Monitoring Centre for Drugs and Drug Addiction (EMCDDA). European Drug Report: Trends and Developments; MDMA, New Psychoactive Substances; Publications Office of the European Union: Luxembourg, 2021; pp. 24–27. Available online: https://www.emcdda.europa.eu/system/files/publications/13838/TDAT21001ENN.pdf (accessed on 9 October 2021).
- Wang, L.; Zhang, Y.; Du, X.; Ding, T.; Gong, W.; Liu, F. Review of antidepressants in clinic and active ingredients of traditional Chinese medicine targeting 5-HT1A receptors. Biomed. Pharmacother. 2019, 120, 109408. [Google Scholar] [CrossRef]
- Ulenberg, S.; Belka, M.; Bączek, T. Comparison of MLR, OPLS, and SVM as potent chemometric techniques used to estimate in vitro metabolic stability. J. Chemom. 2016, 30, 177–181. [Google Scholar] [CrossRef]
- Caccia, S.; Conti, I.; Notarnicola, A. In-vivo metabolism in the rat and mouse of antrafenine to 1-m-trifluoromethylphenylpiperazine. J. Pharm. Pharmacol. 1985, 37, 75–77. [Google Scholar] [CrossRef]
- Encinar, J.A.; Menendez, J.A. Potential Drugs Targeting Early Innate Immune Evasion of SARS-Coronavirus 2 via 2′-O-Methylation of Viral RNA. Viruses 2020, 12, 525. [Google Scholar] [CrossRef]
- Welz, A.; Breś-Targowska, A. Coronavirus—Current medical and social problem. Farm. Pol. 2020, 76, 259–268. [Google Scholar] [CrossRef]
- Dotevall, G.; Groll, E. Controlled clinical trial of mepiprazole in irritable bowel syndrome. Br. Med. J. 1974, 4, 16–18. [Google Scholar] [CrossRef][Green Version]
- Khouzam, H.R. A review of trazodone use in psychiatric and medical conditions. Postgrad. Med. 2017, 129, 140–148. [Google Scholar] [CrossRef]
- Soe, K.K.; Lee, M.Y. Arrhythmias in Severe Trazodone Overdose. Am. J. Case Rep. 2019, 20, 1949–1955. [Google Scholar] [CrossRef]
- Avila, J.D. Fatal Cerebral Edema, Seizures, and Hyponatremia after Trazodone Overdose. Clin. Neuropharmacol. 2017, 40, 221–223. [Google Scholar] [CrossRef]
- De Meester, A.; Carbutti, G.; Gabriel, L.; Jacques, J.M. Fatal overdose with trazodone: Case report and literature review. Acta Clin. Belg. 2001, 56, 258–261. [Google Scholar] [CrossRef]
- Stanaszek, R.; Lechowicz, W. Determination of trazodone and its metabolite 1-(3- chlorophenyl)piperazine (mCPP) in hair by the high performance liquid chromatography method coupled with mass spectrometry (HPLC-ESI-MS). Probl. Forensic Sci. 2006, 66, 131–139. [Google Scholar]
- Logan, B.K.; Costantino, A.G.; Rieders, E.F.; Sanders, D. Trazodone, meta-chlorophenylpiperazine (an hallucinogenic drug and trazodone metabolite), and the hallucinogen trifluoromethylphenylpiperazine cross-react with the EMIT®II ecstasy immunoassay in urine. J. Anal. Toxicol. 2010, 34, 587–589. [Google Scholar] [CrossRef]
- Ishida, M.; Otani, K.; Kaneko, S.; Ohkubo, T.; Osanai, T.; Yasui, N.; Mihara, K.; Higuchi, H.; Sugawara, K. Effects of various factors on steady state plasma concentrations of trazodone and its active metabolite m-chlorophenylpiperazine. Int. Clin. Psychopharmacol. 1995, 10, 143–146. [Google Scholar] [CrossRef] [PubMed]
- Staack, R.S.; Maurer, H.H. Piperazine-derived designer drug 1-(3-chlorophenyl)piperazine (mCPP): GC-MS studies on its metabolism and its toxicological detection in rat urine including analytical differentiation from its precursor drugs trazodone and nefazodone. J. Anal. Toxicol. 2003, 27, 560–568. [Google Scholar] [CrossRef] [PubMed]
- Buch, J. Urapidil, a dual-acting antihypertensive agent: Current usage considerations. Adv. Ther. 2010, 27, 426–443. [Google Scholar] [CrossRef]
- Andreu, I.; Mayorga, C.; Miranda, M.A. Metabolomics in drug intolerance. Curr. Drug Metab. 2009, 10, 947–955. [Google Scholar] [CrossRef]
- Durand, F.; Samuel, D.; Bernuau, J.; Saliba, F.; Pariente, E.A.; Marion, S.; Benhamou, J.P.; Bizmut, H. Fipexide-induced fulminant hepatitis. Report of three cases with emergency liver transplantation. J. Hepatol. 1992, 15, 144–146. [Google Scholar] [CrossRef]
- Sleno, L.; Staack, R.F.; Varesio, E.; Hopfgartner, G. Investigating the in vitro metabolism of fipexide: Characterization of reactive metabolites using liquid chromatography/mass spectrometry. Rapid Commun. Mass Spectrom. 2007, 21, 2301–2311. [Google Scholar] [CrossRef]
- Tang, M.; Ching, C.K.; Tse, M.L.; Ng, C.; Lee, C.; Chong, Y.K.; Wong, W.; Mak, T.W. Surveillance of emerging drugs of abuse in Hong Kong: Validation of an analytical tool. Hong Kong Med. J. 2015, 21, 114–123. [Google Scholar] [CrossRef] [PubMed]
- Niebel, A.; Krumbiegel, F.; Hartwig, S.; Parr, M.K.; Tsokos, M. Detection and quantification of synthetic cathinones and selected piperazines in hair by LC-MS/MS. Forensic Sci. Med. Pathol. 2020, 16, 32–42. [Google Scholar] [CrossRef]
- Nieddu, M.; Trignano, C.; Burrai, L.; Pirisi, M.A.; Boatto, G. Cross-reactivities of 41 new amphetamine designer drugs to EMIT immunoassays. Forensic. Toxicol. 2013, 31, 133–137. [Google Scholar] [CrossRef]
- Nieddu, M.; Burrai, L.; Trignano, C.; Boatto, G. Cross-reactivities of 39 new amphetamine designer drugs on three abuse drugs urinary screening tests. Forensic. Toxicol. 2014, 32, 132–138. [Google Scholar] [CrossRef]
- Wohlfarth, A.; Weinmann, W.; Dresen, S. LC-MS/MS screening method for designer amphetamines, tryptamines, and piperazines in serum. Anal. Bioanal. Chem. 2010, 396, 2403–2414. [Google Scholar] [CrossRef]
- Concheiro, M.; Castaneto, M.; Kronstrand, R.; Huestis, M.A. Simultaneous determination of 40 novel psychoactive stimulants in urine by liquid chromatography-high resolution mass spectrometry and library matching. J. Chromatogr. A 2015, 1397, 32–42. [Google Scholar] [CrossRef] [PubMed]
- Paul, M.; Ippisch, J.; Herrmann, C.; Guber, S.; Schultis, W. Analysis of new designer drugs and common drugs of abuse in urine by a combined targeted and untargeted LC-HR-QTOFMS approach. Anal. Bioanal. Chem. 2014, 406, 4425–4441. [Google Scholar] [CrossRef]
- Montesano, C.; Sergi, M.; Moro, M.; Napoletano, S.; Romolo, F.S.; Del Carlo, M.; Compagnone, D.; Curini, R. Screening of methylenedioxyamphetamine and piperazine-derived designer drugs in urine by LC–MS/MS using neutral loss and precursor ion scan. J. Mass Spectrom. 2013, 48, 49–59. [Google Scholar] [CrossRef]
- Dickson, A.J.; Vorce, S.P.; Holler, J.M.; Lyons, T.P. Detection of 1- Benzylpiperazine, 1-(3-Trifluoromethylphenyl)-piperazine, and 1-(3-Chlorophenyl)-piperazine in 3,4-Methylenedioxymethamphetamine-Positive Urine Samples. J. Anal. Toxicol. 2010, 34, 464–469. [Google Scholar] [CrossRef][Green Version]
- Strano Rossi, S.; Odoardi, S.; Gregori, A.; Peluso, G.; Ripani, L.; Ortar, G.; Serpelloni, G.; Romolo, F.S. An analytical approach to the forensic identification of different classes of new psychoactive substances (NPSs) in seized materials. Rapid Commun. Mass Spectrom. 2014, 28, 1904–1916. [Google Scholar] [CrossRef]
- Maurer, H.H. Position of chromatographic techniques in screening for detection of drugs or poisons in clinical and forensic toxicology and/or doping control. Clin. Chem. Lab. Med. 2004, 42, 1310–1324. [Google Scholar] [CrossRef]
- Scientific Working Group for Forensic Toxicology (SWGTOX). Standard Practices for Method Validation in Forensic Toxicology. J. Anal. Toxicol. 2013, 37, 452–474. [Google Scholar] [CrossRef]
- Tan, A.; Hussain, S.; Musuku, A.; Massé, R. Internal standard response variations during incurred sample analysis by LC–MS/MS: Case by case trouble shooting. J. Chromatogr. B Analyt. Technol. Biomed. Life Sci. 2009, 877, 3201–3209. [Google Scholar] [CrossRef]
- Avery, M.J. Quantitative characterization of differential ion suppression on liquid chromatography/atmospheric pressure ionization mass spectrometric bioanalytical methods. Rapid Commun. Mass Spectrom. 2003, 17, 197–201. [Google Scholar] [CrossRef]
- Stokvis, E.; Rosing, H.; Beijnen, J.H. Stable isotopically labeled internal standards in quantitative bioanalysis using liquid chromatography/mass spectrometry: Necessity or not? Rapid Commun. Mass Spectrom. 2005, 19, 401–407. [Google Scholar] [CrossRef] [PubMed]
- Matuszewski, B.K. Standard line slopes as a measure of a relative matrix effect in quantitative HPLC-MS bioanalysis. J. Chromatogr. B. 2006, 830, 293–300. [Google Scholar] [CrossRef] [PubMed]
- Nicolò, A.D.; Cantù, M.; D’Avolio, A. Matrix effect management in liquid chromatography mass spectrometry: The internal standard normalized matrix effect. Bioanalysis 2017, 9, 1093–1105. [Google Scholar] [CrossRef]
- De Boer, D.; Bosman, I.J.; Hidvégi, E.; Manzoni, C.; Benkö, A.A.; Dos Reys, L.J.; Maes, R.A. Piperazine-like compounds: A new group of designer drugs-of-abuse on the European market. Forensic Sci. Int. 2001, 121, 47–56. [Google Scholar] [CrossRef]

PIPERAZINE | |
| Benzylpiperazine Derivatives | Phenylpiperazine Derivatives |
| BZP N-benzylpiperazine  | mCPP 1-(3-chlorophenyl)piperazine 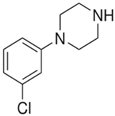 |
| MDBP 1-(3,4-methylenedioxybenzyl)piperazine  | TFMPP 1-(3-trifluoromethylphenyl)piperazine  |
| pFBP 1-(4-fluorobenzyl)piperazine 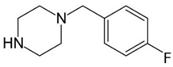 | pFPP 1-(4-parafluorophenyl)piperazine 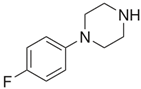 |
| DBZP 1,4-dibenzylpiperazine 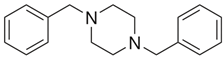 | MeOPP 1-(4-methoxyphenyl)piperazine 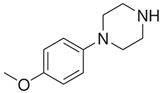 |
| Compound | Precursor Ion (m/z) | Fragmentation Patterns (m/z) | ||
|---|---|---|---|---|
BZP | 177.3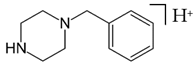 | 90.95 | 64.95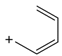 | 86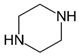 |
| C11H16N2 | [C11H16N2]+ | [C7H7]+ | [C5H5]+ | [C4H10N2] |
MDBP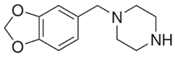 | 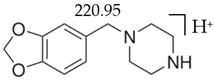 | 135.00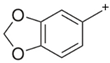 | 76.9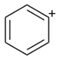 | 86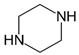 |
| C12H16N202 | [C12H16N202]+ | [C8H7O2]+ | [C6H5]+ | [C4H10N2] |
pFBP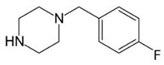 | 195 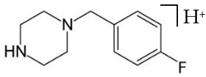 | 108.90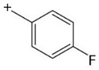 | 83.00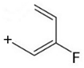 | 86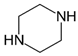 |
| C11H15FN2 | [C11H15FN2]+ | [C7H6F]+ | [C5H4F]+ | [C4H10N2] |
mCPP | 197.05 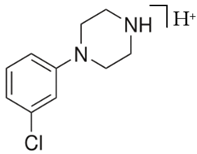 | 153.95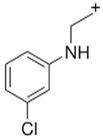 | 117.95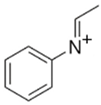 | 44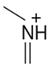 |
| C10H13ClN2 | [C10H13ClN2]+ | [C8H9ClN]+ | [C8H8N]+ | [C2H5N]+ |
TFMPP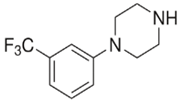 | 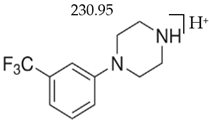 | 187.95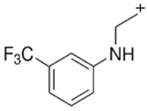 | 118.10 | 44 |
| C11H13F3N2 | [C11H13F3N2]+ | [C9H9F3N]+ | [C8H8N]+ | [C2H5N]+ |
| Compound Name | Mobile Phase Composition: BF70/MeOH20/ACN10 | |||||
|---|---|---|---|---|---|---|
| BF 20 mM | BF 100 mM | |||||
| tR (pH 2.7) | tR (pH 3.6) | tR (pH 4.1) | tR (pH 4.6) | tR (pH 6.0) | tR (pH 6.0) | |
| BPZ | 3.036 | 3.659 | 3.832 | 3.857 | 4.032 | 3.985 |
| MDBP | 3.065 | 3.775 | 3.979 | 4.009 | 4.187 | 4.135 |
| pFBP | 3.359 | 4.192 | 4.392 | 4.423 | 4.632 | 4.560 |
| mCPP | 5.215 | 5.235 | 5.309 | 5.320 | 5.736 | 5.591 |
| TFMPP | 8.216 | 8.249 | 8.368 | 8.561 | 9.707 | 9.382 |
| Compound Name | Mobile Phase Composition: BF85/MeOH10/ACN5 | ||||
|---|---|---|---|---|---|
| BF 20 mM | BF 100 mM | ||||
| tR (pH 3.6) | tR (pH 4.1) | tR (pH 4.6) | tR (pH 6.0) | tR (pH 6.0) | |
| BPZ | 4.996 | 5.702 | 6.024 | 6.472 | 6.588 |
| MDBP | 5.437 | 6.438 | 6.859 | 7.477 | 7.534 |
| pFBP | 6.417 | 7.380 | 7.775 | 8.340 | 8.433 |
| mCPP | 11.763 | 11.835 | 12.015 | 12.654 | 12.791 |
| TFMPP | 23.663 | 23.680 | 24.569 | 26.783 | 27.257 |
| Analytes | Internal Standard | Linear Range (ng/mL) | Regression Equation | R2 | Analytes LOD (ng/mL) | Analytes LOQ (ng/mL) |
|---|---|---|---|---|---|---|
| BZP | Pentedrone | 500–7000 | y = 0.0001x − 0.0235 | 0.9984 | 150 | 450 |
| MDBP | Pentedrone | 500–7000 | y = 0.0006x − 0.0397 | 0.9917 | 110 | 330 |
| pFBP | Pentedrone | 500–7000 | y = 0.0027x − 0.3238 | 0.9941 | 100 | 300 |
| mCPP | Pentedrone | 500–7000 | y = 0.0005x + 0.0645 | 0.9919 | 150 | 450 |
| TFMPP | Pentedrone | 500–7000 | y = 0.0006x − 0.0884 | 0.9961 | 140 | 420 |
| Analytes | Level | Daily Accuracy for tR, n = 12 CV (%) | Daily Accuracy for AUC, n = 12 CV (%) | Accuracy between Days for tR CV (%) | Accuracy between Days for AUC CV (%) |
|---|---|---|---|---|---|
| BPZ | LQC | 0.24 | 1.42 | 0.64 | 9.64 |
| MQC | 0.14 | 1.18 | 0.49 | 5.04 | |
| HQC | 0.12 | 1.56 | 0.44 | 7.75 | |
| MDBP | LQC | 0.23 | 3.12 | 0.38 | 4.06 |
| MQC | 0.14 | 2.20 | 0.47 | 3.51 | |
| HQC | 0.11 | 1.20 | 0.40 | 5.07 | |
| pFBP | LQC | 0.11 | 1.74 | 0.26 | 10.31 |
| MQC | 0.03 | 0.76 | 0.05 | 5.73 | |
| HQC | 0.07 | 1.92 | 0.11 | 1.69 | |
| mCPP | LQC | 0.04 | 0.95 | 1.32 | 2.24 |
| MQC | 0.04 | 1.07 | 1.27 | 1.20 | |
| HQC | 0.04 | 1.00 | 1.34 | 2.47 | |
| TFMPP | LQC | 0.05 | 2.34 | 0.84 | 4.65 |
| MQC | 0.34 | 1.13 | 1.26 | 3.11 | |
| HQC | 0.04 | 1.20 | 1.44 | 3.47 |
| Identification of Piperazine Designer Drug in Urine | Identification of Piperazine Designer Drugs in Serum |
|---|---|
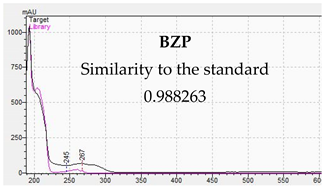 | 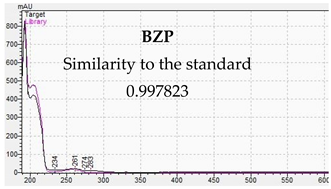 |
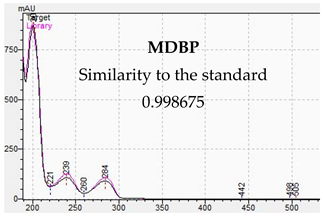 | 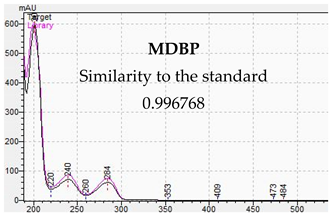 |
 | 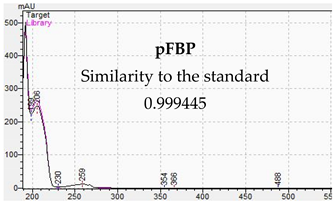 |
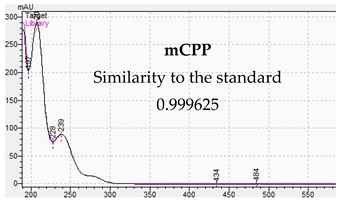 | 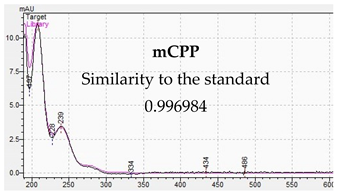 |
 |  |
| Analytes | Internal Standard | Urine | Serum | ||||
|---|---|---|---|---|---|---|---|
| Average 1000 ng | Standard Deviation | %CV | Average 1000 ng | Standard Deviation | %CV | ||
| BPZ | BZP-D7 | 1183.70 | 14.47 | 1.18 | 1120.88 | 9.71 | 0.87 |
| MDBP | BZP-D7 | 1021.15 | 7.70 | 0.75 | 983.20 | 11.25 | 1.14 |
| pFBP | BZP-D7 | 973.34 | 13.08 | 1.34 | 1006.45 | 16.52 | 1.64 |
| mCPP | mCPP-D8 | 1095.33 | 8.11 | 0.74 | 1146.73 | 18.71 | 1.63 |
| TFMPP | TFMPP-D4 | 996.96 | 1.61 | 0.16 | 1013.00 | 27.61 | 2.73 |
| Elements of the Measuring System and Work Parameters | LC-MS Method | LC-DAD Method |
|---|---|---|
| Liquid chromatograph | LCMS-8045, Shimadzu | LC-DAD, Shimadzu |
| Mobile phase | A: Water (0.1%FA) B: Methanol (0.1%FA) | A: 20 mM phosphate buffer B: Acetonitrile C: Methanol |
| Column | Synergi Hydro-RP C18 4 μm; 2.00 × 150 mm | Xterra RP C18 5 μm; 4.6 × 150 mm |
| Injection volume | 5 μL | 10 μL |
| Analysis time | 15 min | 20 min |
| Compound | Mass Spectra from LC-MS | UV/VIS Spectra from LC-DAD |
|---|---|---|
| BZP | 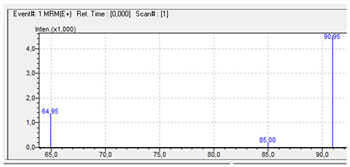 | 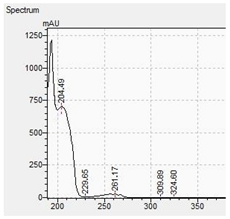 |
| MDBP | 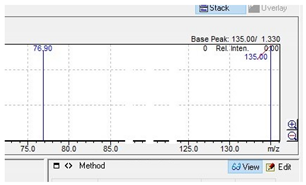 | 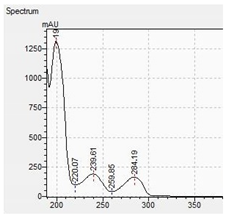 |
| pFBP | 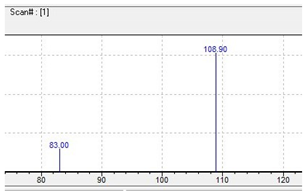 |  |
| mCPP | 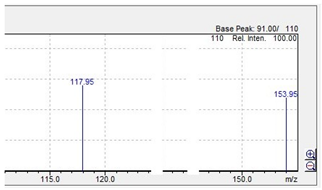 | 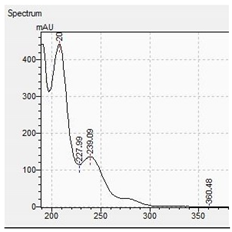 |
| TFMPP | 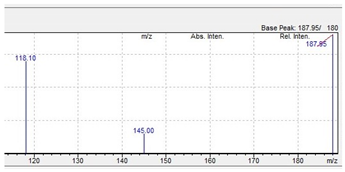 | 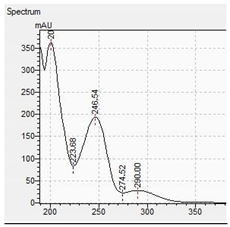 |
| General Name of Therapeutic Drug | Pharmacological Classification | Piperazine Derivatives as Metabolite | References |
|---|---|---|---|
| Antrafenine | Analgesic | TFMPP | [17,53,54] |
| Trazodone | Antidepressant | mCPP | [57,58,59,60,62] |
| Nefazodone | Antidepressant | mCPP | [10,26] |
| Etoperidone | Antidepressant | mCPP | [10,26] |
| Enziprazole | Antidepressant | mCPP | [10,26] |
| Mepiprazole | Tranquilizer | mCPP | [10,26,56] |
| Urapidil | Antihypertensive | MeOPP | [26,65] |
| Fipexide (withdrawn from the treatment) | Nootropic | MDBP | [66,67] |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2022 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Welz, A.; Koba, M.; Kośliński, P.; Siódmiak, J. Comparison of LC-MS and LC-DAD Methods of Detecting Abused Piperazine Designer Drugs. J. Clin. Med. 2022, 11, 1758. https://doi.org/10.3390/jcm11071758
Welz A, Koba M, Kośliński P, Siódmiak J. Comparison of LC-MS and LC-DAD Methods of Detecting Abused Piperazine Designer Drugs. Journal of Clinical Medicine. 2022; 11(7):1758. https://doi.org/10.3390/jcm11071758
Chicago/Turabian StyleWelz, Anna, Marcin Koba, Piotr Kośliński, and Joanna Siódmiak. 2022. "Comparison of LC-MS and LC-DAD Methods of Detecting Abused Piperazine Designer Drugs" Journal of Clinical Medicine 11, no. 7: 1758. https://doi.org/10.3390/jcm11071758
APA StyleWelz, A., Koba, M., Kośliński, P., & Siódmiak, J. (2022). Comparison of LC-MS and LC-DAD Methods of Detecting Abused Piperazine Designer Drugs. Journal of Clinical Medicine, 11(7), 1758. https://doi.org/10.3390/jcm11071758






