Fast-Track Programs in Total Hip and Knee Replacement at Swedish Hospitals—Influence on 2-Year Risk of Revision and Mortality
Abstract
1. Introduction
2. Material and Methods
2.1. Ethics
2.2. Informed Consent
2.3. Definition of Cohorts
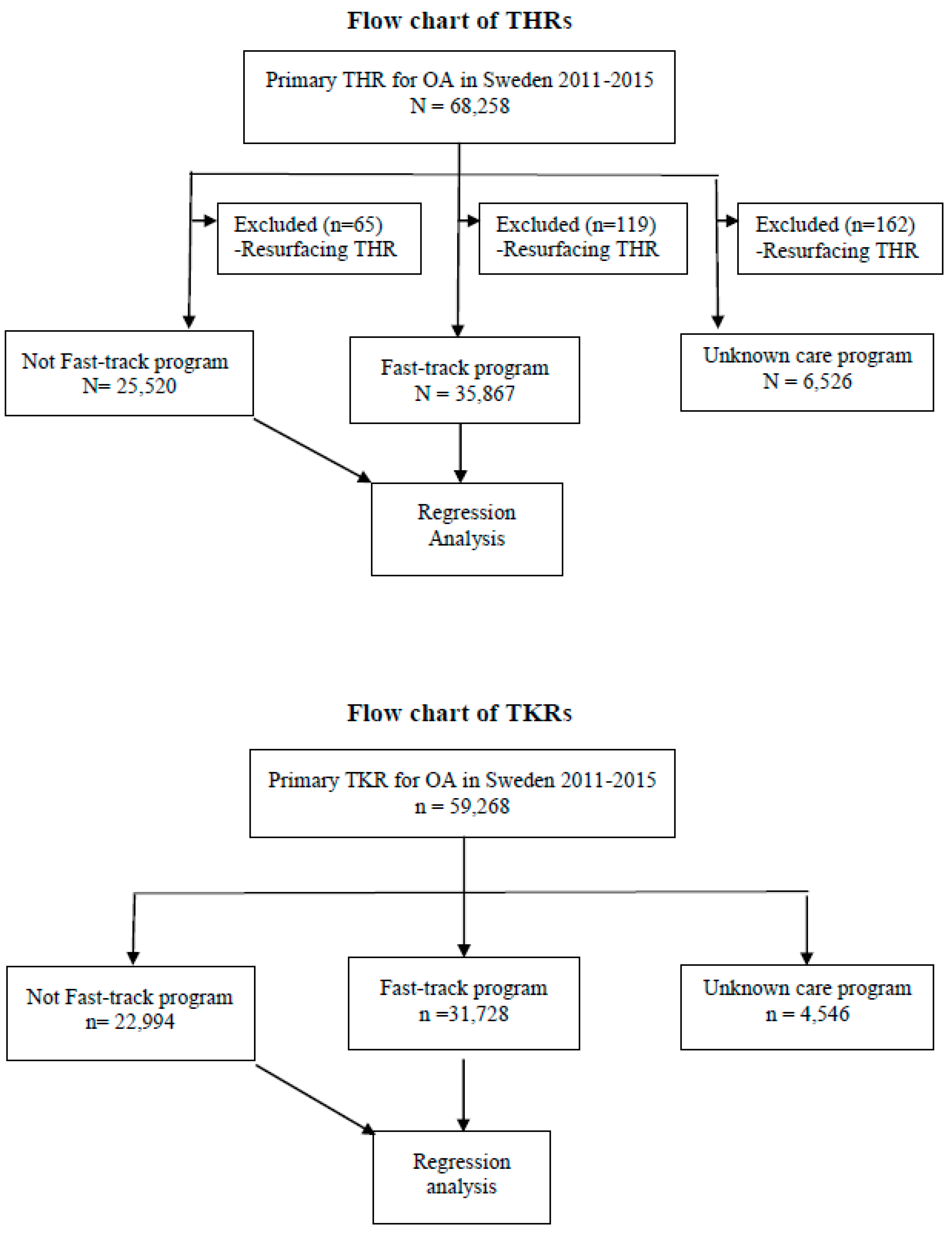
2.4. Data Source and Patient Selection
2.5. Exposure and Outcome
2.6. Statistics and Data Analysis
3. Results
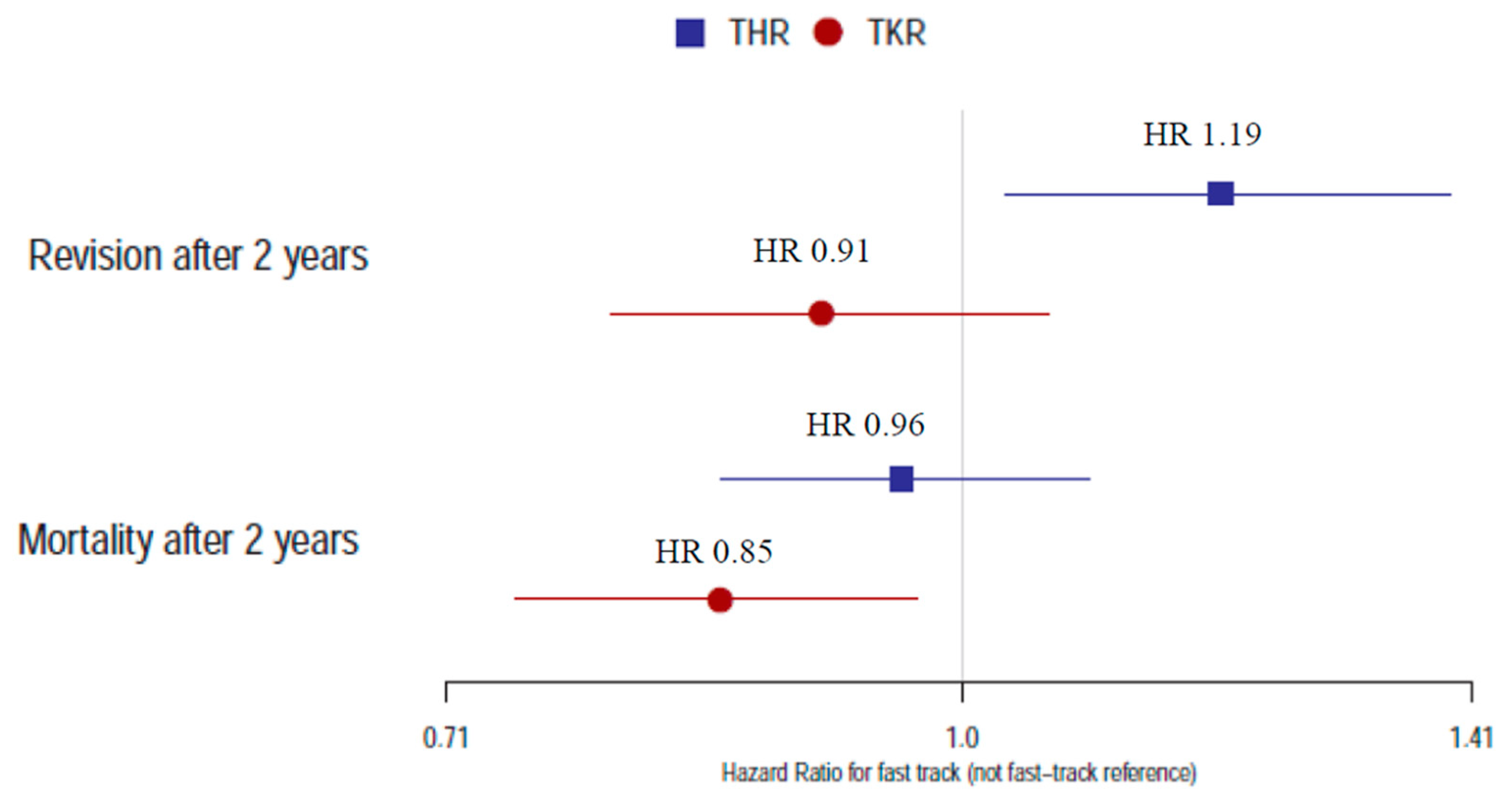
3.1. Cohort Characteristics and Revisions after THR
3.2. Cohort Characteristics and Revisions after TKR
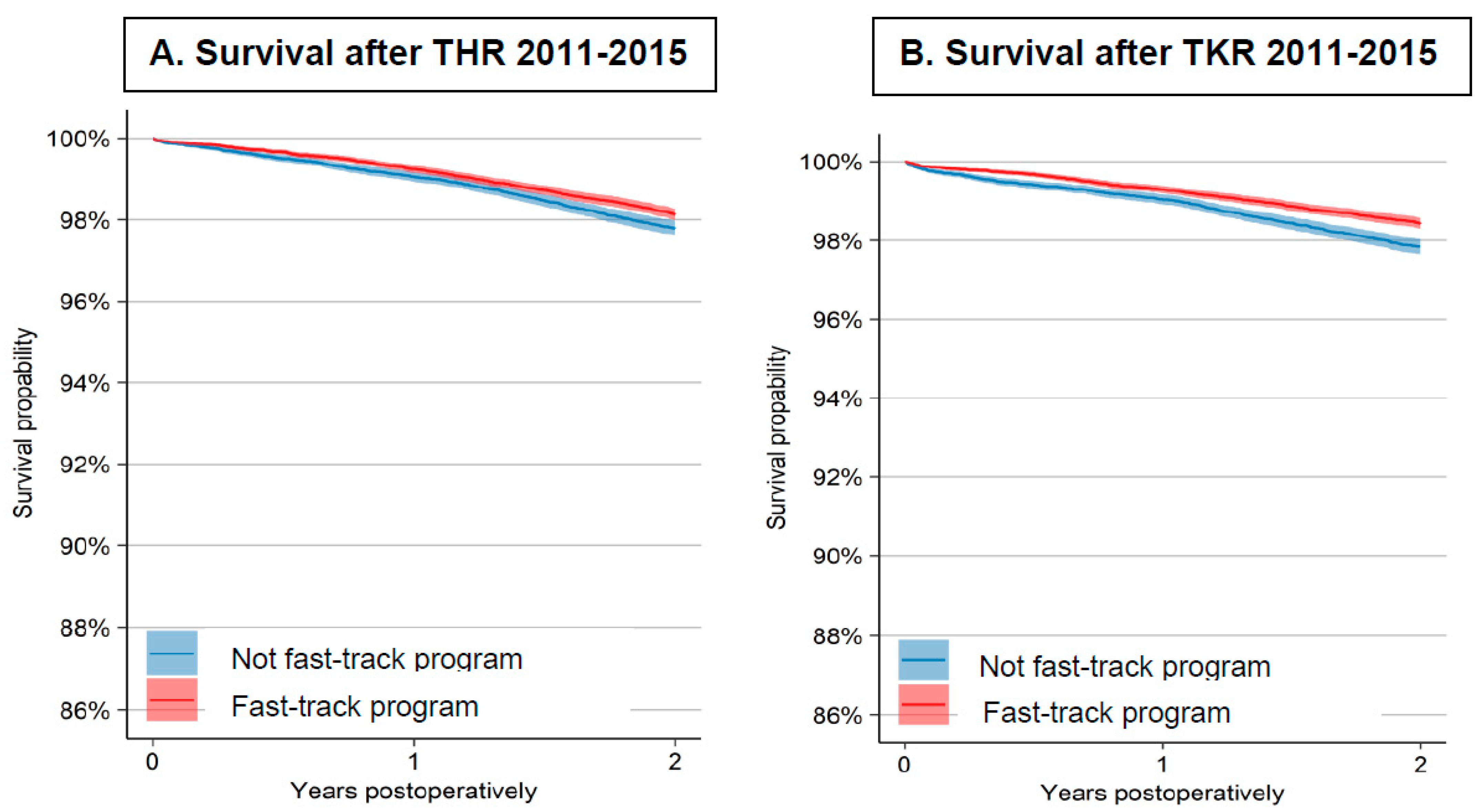
3.3. Mortality
4. Discussion
Strengths and Limitations
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Wainwright, T.W.; Kehlet, H. Fast-track hip and knee arthroplasty—have we reached the goal? Acta Orthop. 2019, 90, 3–5. [Google Scholar] [CrossRef] [PubMed]
- Amlie, E.; Lerdal, A.; Gay, C.L.; Høvik, Ø.; Nordsletten, L.; Dimmen, S. A Trend for Increased Risk of Revision Surgery due to Deep Infection following Fast-Track Hip Arthroplasty. Adv. Orthop. 2016, 2016, 1–7. [Google Scholar] [CrossRef] [PubMed][Green Version]
- Pamilo, K.J.; Torkki, P.; Peltola, M.; Pesola, M.; Remes, V.; Paloneva, J. Reduced length of uninterrupted institutional stay after implementing a fast-track protocol for primary total hip replacement. Acta Orthop. 2017, 89, 10–16. [Google Scholar] [CrossRef] [PubMed]
- Hartog, Y.M.D.; Mathijssen, N.M.C.; Vehmeijer, S.B.W. Reduced length of hospital stay after the introduction of a rapid recovery protocol for primary THA procedures. Acta Orthop. 2013, 84, 444–447. [Google Scholar] [CrossRef] [PubMed]
- Glassou, E.N.; Pedersen, A.B.; Hansen, T.B. Risk of re-admission, reoperation, and mortality within 90 days of total hip and knee arthroplasty in fast-track departments in Denmark from 2005 to 2011. Acta Orthop. 2014, 85, 493–500. [Google Scholar] [CrossRef] [PubMed]
- Pedersen, A.B.; Baron, J.A.; Overgaard, S.; Johnsen, S.P. Short- and long-term mortality following primary total hip replacement for osteoarthritis: A Danish nationwide epidemiological study. J. Bone Joint Surg. Br. 2011, 93, 172–177. [Google Scholar] [CrossRef]
- Khan, S.K.; Malviya, A.; Muller, S.D.; Carluke, I.; Partington, P.F.; Emmerson, K.P.; Reed, M.R. Reduced short-term complications and mortality following Enhanced Recovery primary hip and knee arthroplasty: Results from 6000 consecutive procedures. Acta Orthop. 2013, 85, 26–31. [Google Scholar] [CrossRef]
- Savaridas, T.; Serrano-Pedraza, I.; Khan, S.K.; Martin, K.; Malviya, A.; Reed, M.R. Reduced medium-term mortality following primary total hip and knee arthroplasty with an enhanced recovery program. Acta Orthop. 2013, 84, 40–43. [Google Scholar] [CrossRef]
- Berg, U. Fast-Track Programs in Total Hip and Knee Replacement at Swedish Hospitals-Influences on Safety, Outcome and Patients’ Experiences. Ph.D. Thesis, Institute of Clinical Sciences, University of Gothenburg, Gothenburg, Sweden, 8 May 2020. [Google Scholar]
- Kärrhom, J.; Rogmark, C.; Naucler, E.; Nåtman, J.; Vinblad, J.; Mohaddes, M.; Rolfson, O. Swedish Hip Arthroplasty Register Annual Report 2019; The Swedish Hip Arthroplasty Register: Gothenburg, Sweden, 2020. [Google Scholar] [CrossRef]
- Berg, U.; Bülow, E.; Sundberg, M.; Rolfson, O. No increase in readmissions or adverse events after implementation of fast-track program in total hip and knee replacement at 8 Swedish hospitals: An observational before-and-after study of 14,148 total joint replacements 2011–2015. Acta Orthop. 2018, 89, 522–527. [Google Scholar] [CrossRef] [PubMed]
- Kärrhom, J.; Rogmark, C.; Naucler, E.; Vinblad, J.; Mohaddes, M.; Rolfson, O. Swedish Hip Arthroplasty Register Annual Report 2018; The Swedish Hip Arthroplasty Register: Gothenburg, Sweden, 2019. [Google Scholar] [CrossRef]
- Robertsson, O.; Ranstam, J.; Sundberg, M.; W-Dahl, A.; Lidgren, L. The Swedish knee arthroplasty register: A review. Bone Joint Res. 2014, 3, 217–222. [Google Scholar] [CrossRef] [PubMed]
- Vehmeijer, S.B.W.; Husted, H.; Kehlet, H. Outpatient total hip and knee arthroplasty. Acta Orthop. 2018, 89, 141–144. [Google Scholar] [CrossRef] [PubMed]
- Ho, J.; Meis, J.F.; Nabuurs-Franssen, M.; Voss, A. Hip and knee arthroplasty: Quo vadis? Antimicrob. Resist. Infect. Control. 2015, 4, 19. [Google Scholar] [CrossRef] [PubMed]
- Jorgensen, C.C.; Kehlet, H. Fall-related admissions after fast-track total hip and knee arthroplasty—Cause of concern or consequence of success? Clin. Interv. Aging 2013, 8, 1569–1577. [Google Scholar] [CrossRef] [PubMed]
- Lalmohamed, A.; Vestergaard, P.; de Boer, A.; Leufkens, H.G.; van Staa, T.P.; de Vries, F. Changes in mortality patterns following total hip or knee arthroplasty over the past two decades: A nationwide cohort study. Arthritis Rheumatol. 2014, 66, 311–318. [Google Scholar] [CrossRef] [PubMed]
- Deng, Q.-F.; Gu, H.-Y.; Peng, W.-Y.; Zhang, Q.; Huang, Z.-D.; Zhang, C.; Yu, Y.-X. Impact of enhanced recovery after surgery on postoperative recovery after joint arthroplasty: Results from a systematic review and meta-analysis. Postgrad. Med. J. 2018, 94, 678–693. [Google Scholar] [CrossRef] [PubMed]
- Petersen, P.B.; Kehlet, H.; Jørgensen, C.C. On behalf of the Lundbeck Foundation Center for Fast-track Hip and Knee Replacement Collaborative Group Myocardial infarction following fast-track total hip and knee arthroplasty—incidence, time course, and risk factors: A prospective cohort study of 24,862 procedures. Acta Orthop. 2018, 89, 603–609. [Google Scholar] [CrossRef] [PubMed]
- Jorgensen, C.C.; Kehlet, H. Early thromboembolic events ≤ 1week after fast-track total hip and knee arthroplasty. Thromb. Res. 2016, 138, 37–42. [Google Scholar] [CrossRef] [PubMed]
- Pedersen, A.B.; Mehnert, F.; Sorensen, H.T.; Emmeluth, C.; Overgaard, S.; Johnsen, S.P. The risk of venous thromboembolism, myocardial infarction, stroke, major bleeding and death in patients undergoing total hip and knee replacement: A 15-year retrospective cohort study of routine clinical practice. Bone Joint J. 2014, 96, 479–485. [Google Scholar] [CrossRef] [PubMed]
- Jørgensen, C.; Kehlet, H. On behalf of the Lundbeck Foundation Centre for Fast-track Hip and Knee Replacement Collaborative Group Time course and reasons for 90-day mortality in fast-track hip and knee arthroplasty. Acta Anaesthesiol. Scand. 2017, 61, 436–444. [Google Scholar] [CrossRef] [PubMed]

| Variable | Definition | Non-Fast-Track | Fast-Track |
|---|---|---|---|
| THR | n | 25,585 | 35,986 |
| Age (years) | mean (SD) | 68.6 (10.4) | 68.2 (10.2) |
| Female sex | n (%) | 14,761 (57.7) | 20,250 (56.3) |
| BMI | mean (SD) | 27.6 (4.6) | 27.3 (4.4) |
| ASA class | I-II (%) | 20,779 (82.7) | 29,989 (85.3) |
| III-IV (%) | 4341 (17.3) | 5168 (14.7) | |
| Fixation | Cemented (%) | 17,825 (69.7) | 22,154 (61.6) |
| Hybrid (%) | 408 (1.6) | 1243 (3.5) | |
| Uncemented (%) | 4404 (17.2) | 7123 (19.8) | |
| Reverse hybrid (%) | 2882 (11.3) | 5326 (14.8) | |
| Incision | Direct lateral (%) | 9187 (35.9) | 19,403 (53.9) |
| Posterior (%) | 15,995 (62.5) | 16,573 (46.1) | |
| Other (%) | 402 (1.6) | 5 (0.0) | |
| TKR | n | 23,036 | 31,686 |
| Age (years) | mean (SD) | 69.6 (9.1) | 68.7 (8.9) |
| Female gender | n (%) | 13,372 (58.0) | 17,910 (56.5) |
| BMI | mean (SD) | 29.3 (4.7) | 28.9 (4.5) |
| ASA class | I-II (%) | 18,826 (81.8) | 26,735 (84.5) |
| III-IV (%) | 4174 (18.2) | 4890 (15.5) | |
| Fixation | Cemented (%) | 22,284 (96.8) | 29,568 (93.4) |
| Patella resurfacing | No resurfacing (%) | 22,210 (96.4) | 31,106 (98.2) |
| Variable | Definition | Non-Fast-Track | Fast-Track |
|---|---|---|---|
| THR | n | 25,520 | 35,867 |
| Revision <2 years | n (%) | 335 (1.3) | 565 (1.6) |
| Reason of revision | PJI or suspected PJI, n (%) | 174 (0.7) | 300 (0.8) |
| Aseptic loosening, n (%) | 43 (0.2) | 74 (0.2) | |
| Dislocation, n (%) | 61 (0.2) | 102 (0.3) | |
| Fracture, n (%) | 38 (0.1) | 65 (0.2) | |
| Other reasons, n (%) | 19 (0.1) | 24 (0.1) | |
| TKR | n | 23,036 | 31,686 |
| Revision < 2 years | n (%) | 405 (1.8) | 434 (1.4) |
| Reason of revision | PJI or suspected PJI | 217 (0.9) | 221 (0.7) |
| Aseptic loosening | 36 (0.2) | 37 (0.1) | |
| Patellar problems | 71 (0.3) | 60 (0.2) | |
| Instability | 42 (0.2) | 66 (0.2) | |
| Other reasons | 39 (0.2) | 49 (0.2) |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Berg, U.; W-Dahl, A.; Nilsdotter, A.; Nauclér, E.; Sundberg, M.; Rolfson, O. Fast-Track Programs in Total Hip and Knee Replacement at Swedish Hospitals—Influence on 2-Year Risk of Revision and Mortality. J. Clin. Med. 2021, 10, 1680. https://doi.org/10.3390/jcm10081680
Berg U, W-Dahl A, Nilsdotter A, Nauclér E, Sundberg M, Rolfson O. Fast-Track Programs in Total Hip and Knee Replacement at Swedish Hospitals—Influence on 2-Year Risk of Revision and Mortality. Journal of Clinical Medicine. 2021; 10(8):1680. https://doi.org/10.3390/jcm10081680
Chicago/Turabian StyleBerg, Urban, Annette W-Dahl, Anna Nilsdotter, Emma Nauclér, Martin Sundberg, and Ola Rolfson. 2021. "Fast-Track Programs in Total Hip and Knee Replacement at Swedish Hospitals—Influence on 2-Year Risk of Revision and Mortality" Journal of Clinical Medicine 10, no. 8: 1680. https://doi.org/10.3390/jcm10081680
APA StyleBerg, U., W-Dahl, A., Nilsdotter, A., Nauclér, E., Sundberg, M., & Rolfson, O. (2021). Fast-Track Programs in Total Hip and Knee Replacement at Swedish Hospitals—Influence on 2-Year Risk of Revision and Mortality. Journal of Clinical Medicine, 10(8), 1680. https://doi.org/10.3390/jcm10081680






