A Systematic Review on Detraining Effects after Balance and Fall Prevention Interventions
Abstract
:1. Introduction
2. Materials and Methods
2.1. Information Sources and Search Strategy
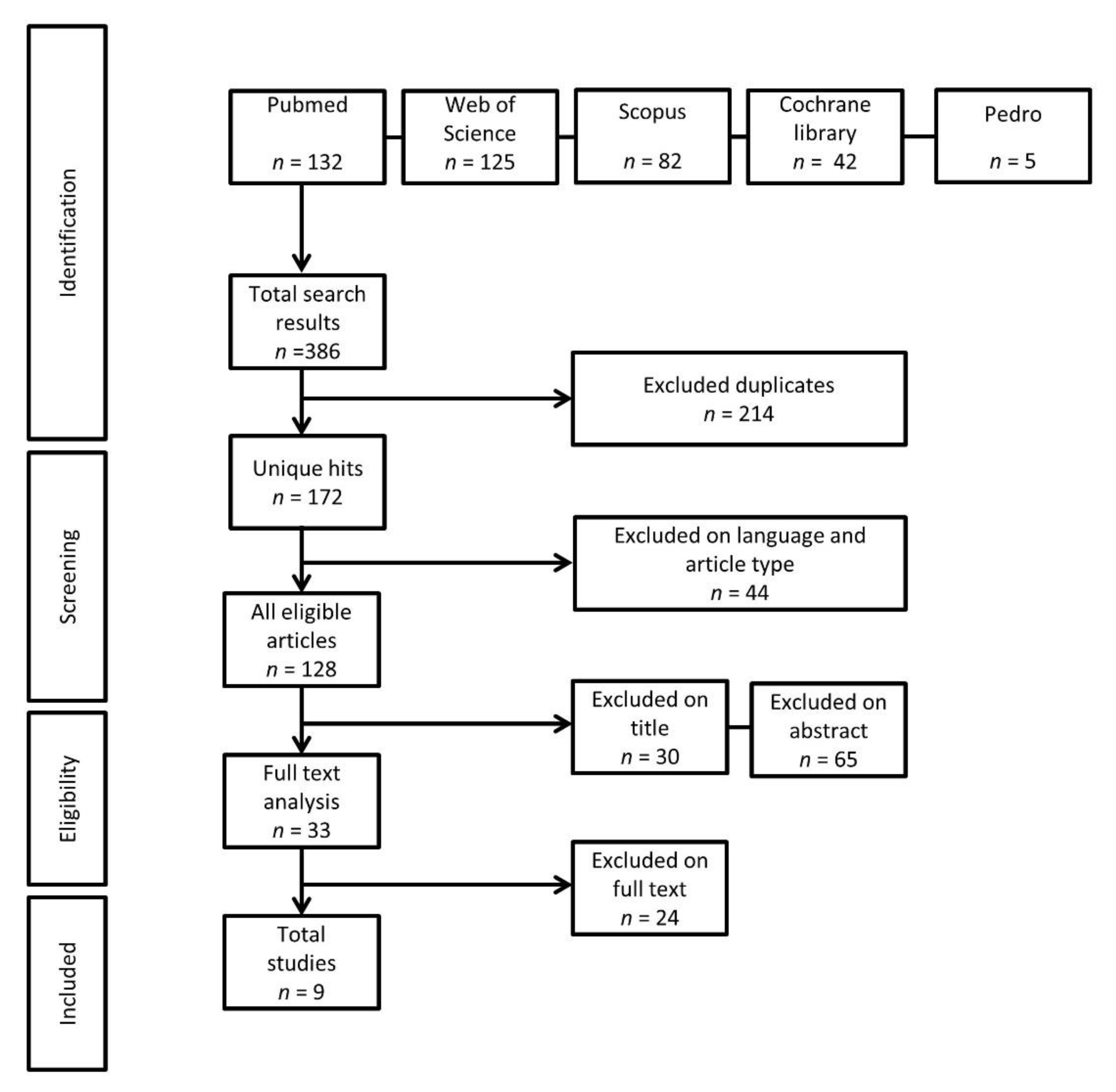
2.2. Eligibility Criteria and Study Selection
2.3. Data Extraction
2.4. Quality Assessment
3. Results
3.1. Effects of Detraining
3.2. Quality Assessment
4. Discussion
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- World Health Organization. World Report on Ageing and Health; World Health Organization: Luxembourg, 2015; ISBN 9780874216561. [Google Scholar]
- Campbell, A.J.; Reinken, J.; Allan, B.C.; Martinez, G.S. Falls in Old Age: A Study of Frequency and Related Clinical Factors. Age Ageing 1981, 10, 264–270. [Google Scholar] [CrossRef]
- World Health Organization. WHO Global Report on Falls Prevention in Older Age; World Health Organization: Geneva, Switzerland, 2007; ISBN 9789241563. [Google Scholar]
- Papalia, G.F.; Papalia, R.; Diaz Balzani, L.A.; Torre, G.; Zampogna, B.; Vasta, S.; Fossati, C.; Alifano, A.M.; Denaro, V. The Effects of Physical Exercise on Balance and Prevention of Falls in Older People: A Systematic Review and Meta-Analysis. J. Clin. Med. 2020, 9, 2595. [Google Scholar] [CrossRef]
- Sherrington, C.; Fairhall, N.J.; Wallbank, G.K.; Tiedemann, A.; Michaleff, Z.A.; Howard, K.; Clemson, L.; Hopewell, S.; Lamb, S.E. Exercise for Preventing Falls in Older People Living in the Community. Cohrane Database Syst. Rev. 2019, 1, CD012424. [Google Scholar] [CrossRef]
- Mujika, I.; Padilla, S. Detraining: Loss of Training-Induced Physiological and Performance Adaptations. Part I. Sport. Med. 2000, 30, 79–87. [Google Scholar] [CrossRef]
- Lemmer, J.T.; Hurlbut, D.E.; Martel, G.F.; Tracy, B.L.; Ivey, F.M.; Metter, E.J.; Fozard, J.L.; Fleg, J.L.; Hurley, B.F. Age and Gender Responses to Strength Training and Detraining. Med. Sci. Sports Exerc. 2000, 32, 1505–1512. [Google Scholar] [CrossRef]
- Mujika, I.; Padilla, S. Muscular Characteristics of Detraining in Humans. Med. Sci. Sports Exerc. 2001, 33, 1297–1303. [Google Scholar] [CrossRef]
- Lesinski, M.; Hortobágyi, T.; Muehlbauer, T.; Gollhofer, A.; Granacher, U. Dose-Response Relationships of Balance Training in Healthy Young Adults: A Systematic Review and Meta-Analysis. Sport. Med. 2015, 45, 557–576. [Google Scholar] [CrossRef] [PubMed]
- Park, S.-H. Tools for Assessing Fall Risk in the Elderly: A Systematic Review and Meta-Analysis. Aging Clin. Exp. Res. 2018, 30, 1–16. [Google Scholar] [CrossRef] [PubMed]
- Moher, D. Preferred Reporting Items for Systematic Reviews and Meta-Analyses: The PRISMA Statement. Ann. Intern. Med. 2009, 151, 264. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Crowe, M.; Sheppard, L. A General Critical Appraisal Tool: An Evaluation of Construct Validity. Int. J. Nurs. Stud. 2011, 48, 1505–1516. [Google Scholar] [CrossRef] [PubMed]
- Crowe, M.; Sheppard, L.; Campbell, A. Reliability Analysis for a Proposed Critical Appraisal Tool Demonstrated Value for Diverse Research Designs. J. Clin. Epidemiol. 2012, 65, 375–383. [Google Scholar] [CrossRef]
- Van Andel, S.; Cole, M.H.; Pepping, G.-J. A Systematic Review on Perceptual-Motor Calibration to Changes in Action Capabilities. Hum. Mov. Sci. 2017, 51, 59–71. [Google Scholar] [CrossRef] [PubMed]
- Abbasi, A.; Sadeghi, H.; Tabrizi, H.B.; Bagheri, K.; Ghasemizad, A.; Asl, A.K. Effect of Whole Body Vibration, Aquatic Balance and Combined Training on Neuromuscular Performance, Balance and Walking Ability in Male Elderly Able-Bodied Individual. World Appl. Sci. J. 2011, 15, 84–91. [Google Scholar]
- Ansai, J.H.; Aurichio, T.R.; Gonçalves, R.; Rebelatto, J.R. Effects of Two Physical Exercise Protocols on Physical Performance Related to Falls in the Oldest Old: A Randomized Controlled Trial. Geriatr. Gerontol. Int. 2016, 16, 492–499. [Google Scholar] [CrossRef] [PubMed]
- Harvey, J.A.; Chastin, S.F.M.; Skelton, D.A. Breaking Sedentary Behaviour Has the Potential to Increase/Maintain Function in Frail Older Adults. J. Frailty Sarcopenia Falls 2018, 3, 26–34. [Google Scholar] [CrossRef] [PubMed]
- Ritzmann, R.; Freyler, K.; Kümmel, J.; Gruber, M.; Belavy, D.L.; Felsenberg, D.; Gollhofer, A.; Kramer, A.; Ambrecht, G. High Intensity Jump Exercise Preserves Posture Control, Gait, and Functional Mobility during 60 Days of Bed-Rest: An RCT Including 90 Days of Follow-Up. Front. Physiol. 2018, 9, 1713. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Sherk, K.A.; Bemben, D.A.; Brickman, S.E.; Bemben, M.G. Effects of Resistance Training Duration on Muscular Strength Retention 6-Month Posttraining in Older Men and Women. J. Geriatr. Phys. Ther. 2012, 35, 20–27. [Google Scholar] [CrossRef]
- Sun, W.; Wang, L.; Zhang, C.; Song, Q.; Gu, H.; Mao, D. Detraining Effects of Regular Tai Chi Exercise on Postural Control Ability in Older Women: A Randomized Controlled Trial. J. Exerc. Sci. Fit. 2018, 16, 55–61. [Google Scholar] [CrossRef]
- Toulotte, C.; Thevenon, A.; Fabre, C. Effects of Training and Detraining on the Static and Dynamic Balance in Elderly Fallers and Non-Fallers: A Pilot Study. Disabil. Rehabil. 2006, 28, 125–133. [Google Scholar] [CrossRef]
- Vogler, C.M.; Menant, J.C.; Sherrington, C.; Ogle, S.J.; Lord, S.R. Evidence of Detraining after 12-Week Home-Based Exercise Programs Designed to Reduce Fall-Risk Factors in Older People Recently Discharged from Hospital. Arch. Phys. Med. Rehabil. 2012, 93, 1685–1691. [Google Scholar] [CrossRef]
- Zhang, C.; Sun, W.; Yu, B.; Song, Q.; Mao, D. Effects of Exercise on Ankle Proprioception in Adult Women during 16 Weeks of Training and Eight Weeks of Detraining. Res. Sport. Med. 2015, 23, 102–113. [Google Scholar] [CrossRef]
- Hurvitz, E.A.; Richardson, J.K.; Werner, R.A.; Ruhl, A.M.; Dixon, M.R. Unipedal Stance Testing as an Indicator of Fall Risk among Older Outpatients. Arch. Phys. Med. Rehabil. 2000, 81, 587–591. [Google Scholar] [CrossRef]
- Nordin, E.; Lindelöf, N.; Rosendahl, E.; Jensen, J.; Lundin-olsson, L. Prognostic Validity of the Timed Up-and-Go Test, a Modified Get-Up-and-Go Test, Staff’s Global Judgement and Fall History in Evaluating Fall Risk in Residential Care Facilities. Age Ageing 2008, 37, 442–448. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Chow, R.B.; Lee, A.; Kane, B.G.; Jacoby, J.L.; Barraco, R.D.; Dusza, S.W.; Meyers, M.C.; Greenberg, M.R. Effectiveness of the “Timed Up and Go” (TUG) and the Chair Test as Screening Tools for Geriatric Fall Risk Assessment in the ED. Am. J. Emerg. Med. 2019, 37, 457–460. [Google Scholar] [CrossRef] [PubMed]
- Khosla, S.; Riggs, B.L. Pathophysiology of Age-Related Bone Loss and Osteoporosis. Endocrinol. Metab. Clin. N. Am. 2005, 34, 1015–1030. [Google Scholar] [CrossRef] [PubMed]
- Davis, M.G.; Fox, K.R. Physical Activity Patterns Assessed by Accelerometry in Older People. Eur. J. Appl. Physiol. 2007, 100, 581–589. [Google Scholar] [CrossRef] [PubMed]
| Participants (N at Study Onset) | Training Duration | Training Intensity | Detraining Duration | Type of Intervention | Outcome Measures | Effect of Training | Effect of Detraining | Notes | |
|---|---|---|---|---|---|---|---|---|---|
| Abbasi et al. [15] | Age: 70 ± 9.6 years (n = 60) | 8 weeks | 3 × 60 min per week | 8 weeks, measured at 4, 6, and 8 weeks | Aquatic balance (AB) training | 5 × STS | Significantly improved | Improvements retained at 8 w | Attrition information: No mention of dropout rate |
| TUG | Significantly improved | Improvements retained at 8 w | |||||||
| Whole-body vibration (WBV) training | 5 × STS | Significantly improved | Returned to baseline at 6 w detraining | ||||||
| TUG | Significantly improved | Returned to baseline at 6 w detraining | |||||||
| Combined AB and WBV | 5 × STS | Significantly improved | Improvements retained at 8 w | ||||||
| TUG | Significantly improved | Improvements retained at 8 w | |||||||
| Ansai et al. [16] | Age: 82.4 ± 2.4 years (n = 69) | 16 weeks | 3 × 60 min per week | 6 weeks | Multicomponent training, containing aerobic, strength, and balance component | 5 × STS | No significant improvement | Effects following “intention to treat” principle. Some effects were found in “high adherence” group. Attrition information: n = 1 participant dropped out before the post-test and 3 were lost to follow-up. | |
| Balance tests | No significant improvement | ||||||||
| TUG | No significant improvement | ||||||||
| Resistance training | 5 × STS | No significant improvement | |||||||
| Balance tests | No significant improvement | ||||||||
| TUG | No significant improvement | ||||||||
| Harvey et al. [17] | Age: 78.4 ± 6.9 years (n = 23) | 10 weeks | 3 × 40 min total | 4 weeks | Motivational interview and retrospective feedback, one group with and one group without real time feedback | Chair sit and reach | No significant improvement | Only main effects between baseline and retention test reported. No effects of intervention itself. Attrition information: n = 13 participants completed the program. | |
| 30 s STS | Significantly improved | ||||||||
| BST | No significant improvement | ||||||||
| TUG | Significantly improved | ||||||||
| Sedentary behavior | No significant improvement | ||||||||
| Ritzmann et al. [18] | Age: 30 ± 7 years (n = 23) | 60 days head tilted down bedrest | Full bedrest | One-leg stance sway | 30–105% decrease | No training intervention/detraining study, but study showing effects of bedrest on healthy subjects. Attrition information: one participant reallocated to full bedrest for medical reasons. n = 0 participants dropped out. | |||
| One-leg stance co-contraction | Increased co-contraction | ||||||||
| 10 m walk test | Significant decreases | ||||||||
| TUG | 20–40% decrease | ||||||||
| 10 × STS | 20–80% decrease | ||||||||
| Bedrest with in total 48–3 min jump sessions | One-leg stance sway | No significant decrease | |||||||
| One-leg stance co-contraction | No significant decrease | ||||||||
| 10 m walk test | Most variables unchanged | ||||||||
| TUG | No significant decrease | ||||||||
| 10 × STS | No significant decrease | ||||||||
| Sherk et al. [19] | Age: 64.5 ± 0.5 years (n = 69) | 40 or 80 weeks | 2 or 3 times per week | 6 months | Resistance training 40 weeks | Upper body 1RM strength | 52% increase | About 15% decrease | Detraining values visually assessed from Figure 3 in [19]. Attrition information: n = 69 participants returned for 6 month follow-up. |
| Lower body 1RM strength | 71% increase | About 9% decrease | |||||||
| Resistance training 80 weeks | Upper body 1RM strength | 22% increase | About 4% decrease | ||||||
| Lower body 1RM strength | 33% increase | No visible change | |||||||
| Sun et al. [20] | Age: 64.2 ± 3.18 years (n = 48) | 16 weeks | 5 × 60 min times per week | 8 weeks | Tai Chi | Eyes open single leg stance variables | 7/7 variables significantly improved | 7/7 variables remain significantly different from baseline after 8 w detraining | No intention to treat data. Only participants who completed the program are reported 25% drop outs not. Reporte dattrition information: n = 36 participants completed the study. |
| Eyes closed single leg stance variables | 7/7 variables significantly improved | 5/7 variables remain significantly different from baseline after 8 w detraining | |||||||
| Brisk Walking | Eyes open single leg stance variables | 7/7 variables significantly improved | 4/7 variables remain significantly different from baseline after 8 w detraining | ||||||
| Eyes closed single leg stance variables | 7/7 variables significantly improved | 5/7 variables remain significantly different from baseline after 8 w detraining | |||||||
| Toulotte et al. [21] | Faller-group age: 71.1 ± 5.0 years (n = 16) | 12 weeks | 2 × 60 min per week | 12 weeks | Low-intensity balance program | 30 s one-leg stance test eyes open | Significantly improved | Significant decrease | Attrition information: No mention of dropout rate. |
| 30 s one-leg stance test eye closed | Significantly improved | Significant decrease | |||||||
| Gait variables single task | 5/5 variables significantly improved | 0/5 variables stay on post-intervention value after 12 w detraining | |||||||
| Gait variables dual task | 5/5 variables significantly improved | 1/5 variables stay on post-intervention value after 12 w detraining | |||||||
| Non-faller-group age: 68.4 ± 4.5 years (n = 8) | 12 weeks | 2 × 60 min per week | 12 weeks | Low-intensity balance program | 30 s one-leg stance test eyes open | Significantly improved | Significant decrease | ||
| 30 s one-leg stance test eyes closed | No significant improvement | Significant decrease | |||||||
| Gait variables single task | 5/5 variables significantly improved | 1/5 variables stay on post-intervention value after 12 w detraining | |||||||
| Gait variables dual task | 5/5 variables significantly improved | 0/5 variables stay on post-intervention value after 12 w detraining | |||||||
| Vogler et al. [22] | Age: 80 ± 7 years (n = 180 in 3 groups) | 12 weeks | 3 times per week | 12 weeks | Weight-bearing functional exercise | Physiological Profile Assessment | Visibly improved compared to controls | Not different from controls at 12 w detraining | Control condition: social visits. Direct post-intervention data not reported, differences reported here are visually assessed from Figure 2 in [22]. Attrition information: no difference in adherence between groups, n = 9 participants dropped out before the end of the 12 w training phase and n = 6 participants were lost to the 24 w follow-up. |
| Maximal balance range | Visibly improved compared to controls | Not different from controls at 12 w detraining | |||||||
| Coordinated stability | Visibly improved compared to controls | Significantly improved compared to controls | |||||||
| Seated resistance exercise | Physiological Profile Assessment | Visibly improved compared to controls | Not different from controls at 12 w detraining | ||||||
| Maximal balance range | Visually not different from controls | ||||||||
| Coordinated stability | Visually not different from controls | ||||||||
| Zhang et al. [23] | Age: 62.01 ± 4.40 years (n =60) | 16 weeks | 5 × 60 min times per week | 8 weeks | Tai Chi | Plantar flexion proprioception | Significantly improved | Improvements retained at 8 w | Attrition information: n = 52 participants completed the study. |
| Dorsal flexion proprioception | Significantly improved | Improvements retained at 8 w | |||||||
| Inversion proprioception | No significant improvement compared to baseline | ||||||||
| Eversion proprioception | No significant improvement compared to baseline | ||||||||
| Brisk walking | Plantar flexion proprioception | Significantly improved | Returned to baseline at 4 w detraining | ||||||
| Dorsal flexion proprioception | No significant improvement compared to baseline | ||||||||
| Inversion proprioception | No significant improvement compared to baseline | ||||||||
| Eversion proprioception | No significant improvement compared to baseline |
| Preliminaries | Introduction | Design | Sampling | Data Collection | Ethical Matters | Results | Discussion | Total | |
|---|---|---|---|---|---|---|---|---|---|
| Abbasi et al. [15] | 3 | 4 | 4 | 0 | 2 | 3 | 3 | 3 | 22 M |
| Ansai et al. [16] | 3 | 4 | 5 | 4 | 4 | 4 | 4 | 3 | 31 H |
| Harvey et al. [17] | 3 | 3 | 5 | 2 | 5 | 5 | 3 | 4 | 30 H |
| Ritzmann et al. [18] | 4 | 5 | 5 | 4 | 5 | 5 | 5 | 4 | 37 VH |
| Sherk et al. [19] | 4 | 4 | 2 | 3 | 5 | 5 | 3 | 3 | 29 H |
| Sun et al. [20] | 2 | 2 | 4 | 3 | 5 | 5 | 5 | 4 | 30 H |
| Toulotte et al. [21] | 4 | 3 | 5 | 3 | 3 | 4 | 3 | 5 | 30 H |
| Vogler et al. [22] | 3 | 5 | 3 | 5 | 5 | 5 | 3 | 4 | 33V H |
| Zhang et al. [23] | 4 | 4 | 4 | 3 | 4 | 4 | 4 | 2 | 29 H |
| Mean values | 3.3 | 3.8 | 4.1 | 3.0 | 4.2 | 4.4 | 3.7 | 3.6 | 30.1 |
| Standard deviation | 0.71 | 0.97 | 1.05 | 1.41 | 1.09 | 0.73 | 0.87 | 0.88 | 3.95 |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Modaberi, S.; Saemi, E.; Federolf, P.A.; van Andel, S. A Systematic Review on Detraining Effects after Balance and Fall Prevention Interventions. J. Clin. Med. 2021, 10, 4656. https://doi.org/10.3390/jcm10204656
Modaberi S, Saemi E, Federolf PA, van Andel S. A Systematic Review on Detraining Effects after Balance and Fall Prevention Interventions. Journal of Clinical Medicine. 2021; 10(20):4656. https://doi.org/10.3390/jcm10204656
Chicago/Turabian StyleModaberi, Shaghayegh, Esmaeel Saemi, Peter A. Federolf, and Steven van Andel. 2021. "A Systematic Review on Detraining Effects after Balance and Fall Prevention Interventions" Journal of Clinical Medicine 10, no. 20: 4656. https://doi.org/10.3390/jcm10204656
APA StyleModaberi, S., Saemi, E., Federolf, P. A., & van Andel, S. (2021). A Systematic Review on Detraining Effects after Balance and Fall Prevention Interventions. Journal of Clinical Medicine, 10(20), 4656. https://doi.org/10.3390/jcm10204656







