Peripheral Arterial Stiffness in Acute Pulmonary Embolism and Pulmonary Hypertension at Short-Term Follow-Up
Abstract
1. Introduction
2. Materials and Methods
2.1. Study Population
2.2. Right Heart Catheterization
2.3. Echocardiographic Assessment
2.4. Cardio-Ankle Vascular Index (CAVI)
2.5. Statistical Analysis
3. Results
4. Discussion
5. Conclusions
6. Limitations
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
Abbreviations
| ABI | ankle-brachial index |
| CAVI | cardio ankle vascular index |
| CO | Cardiac output |
| CTEPH | Chronic thromboembolic pulmonary hypertension |
| DBP | diastolic blood pressure |
| IP-10 | y-interferon-induced protein |
| PAWP | pulmonary artery wedge pressure |
| IPAH | idiopathic pulmonary arterial hypertension |
| LV | left ventricle |
| PE | Pulmonary embolism |
| LVEF | left ventricle ejection fraction |
| MCP-1 | monocyte chemotactic protein-1 |
| mPAP | mean pulmonary artery pressure |
| PH | Pulmonary Hypertension |
| NYHA/WHO | New York Heart Association/World Health Organization |
| PA | pulmonary arterial |
| PAH | pulmonary arterial hypertension |
| PASP | pulmonary artery systolic pressure |
| PVR | pulmonary vascular resistance |
| PWV | pulse wave velocity |
| RAP | right atrial pressure |
| RHC | right heart catheterization |
| RV | right ventricle |
| SBP | systolic blood pressure |
| TAPSE | Tricuspid annular plane systolic excursion |
References
- Delcroix, M.; Kerr, K.; Fedullo, P. Chronic Thromboembolic Pulmonary Hypertension. Epidemiology and Risk Factors. Ann. Am. Thorac. Soc. 2016, 13 (Suppl. 3), S201–S206. [Google Scholar] [CrossRef]
- Ende-Verhaar, Y.M.; Cannegieter, S.C.; Vonk Noordegraaf, A.; Delcroix, M.; Pruszczyk, P.; Mairuhu, A.T.; Huisman, M.V.; Klok, F.A. Incidence of chronic thromboembolic pulmonary hypertension after acute pulmonary embolism: A contemporary view of the published literature. Eur. Respir. J. 2017, 49, 1601792. [Google Scholar] [CrossRef]
- Kim, N.H.; Delcroix, M.; Jais, X.; Madani, M.M.; Matsubara, H.; Mayer, E.; Ogo, T.; Tapson, V.F.; Ghofrani, H.A.; Jenkins, D.P. Chronic thromboembolic pulmonary hypertension. Eur. Respir. J. 2019, 53, 1801915. [Google Scholar] [CrossRef]
- Sista, A.K.; Klok, F.A. Late outcomes of pulmonary embolism: The post-PE syndrome. Thromb. Res. 2018, 164, 157–162. [Google Scholar] [CrossRef]
- Bonderman, D.; Jakowitsch, J.; Adlbrecht, C.; Schemper, M.; Kyrle, P.A.; Schönauer, V.; Exner, M.; Klepetko, W.; Kneussl, M.P.; Maurer, G.; et al. Medical conditions increasing the risk of chronic thromboembolic pulmonary hypertension. Thromb. Haemost. 2005, 93, 512–516. [Google Scholar] [CrossRef] [PubMed]
- Lang, I.; Kerr, K. Risk factors for chronic thromboembolic pulmonary hypertension. Proc. Am. Thorac. Soc. 2006, 3, 568–570. [Google Scholar] [CrossRef]
- Jaïs, X.; Ioos, V.; Jardim, C.; Sitbon, O.; Parent, F.; Hamid, A.; Fadel, E.; Dartevelle, P.; Simonneau, G.; Humbert, M. Splenectomy and chronic thromboembolic pulmonary hypertension. Thorax 2005, 60, 1031–1034. [Google Scholar] [CrossRef] [PubMed]
- Morris, T.A. Why acute pulmonary embolism becomes chronic thromboembolic pulmonary hypertension: Clinical and genetic insights. Curr. Opin. Pulm. Med. 2013, 19, 422–429. [Google Scholar] [CrossRef] [PubMed]
- Bonderman, D.; Turecek, P.L.; Jakowitsch, J.; Weltermann, A.; Adlbrecht, C.; Schneider, B.; Kneussl, M.; Rubin, L.J.; Kyrle, P.A.; Klepetko, W.; et al. High prevalence of elevated clotting factor VIII in chronic thromboembolic pulmonary hypertension. Thromb. Haemost. 2003, 90, 372–376. [Google Scholar] [CrossRef] [PubMed]
- Auger, W.R.; Permpikul, P.; Moser, K.M. Lupus anticoagulant, heparin use, and thrombocytopenia in patients with chronic thromboembolic pulmonary hypertension: A preliminary report. Am. J. Med. 1995, 99, 392–396. [Google Scholar] [CrossRef]
- Lang, I.M.; Pesavento, R.; Bonderman, D.; Yuan, J.X. Risk factors and basic mechanisms of chronic thromboembolic pulmonary hypertension: A current understanding. Eur. Respir. J. 2013, 41, 462–468. [Google Scholar] [CrossRef]
- Bonderman, D.; Wilkens, H.; Wakounig, S.; Schäfers, H.J.; Jansa, P.; Lindner, J.; Simkova, I.; Martischnig, A.M.; Dudczak, J.; Sadushi, R.; et al. Risk factors for chronic thromboembolic pulmonary hypertension. Eur. Respir. J. 2009, 33, 325–331. [Google Scholar] [CrossRef] [PubMed]
- Guérin, L.; Couturaud, F.; Parent, F.; Revel, M.P.; Gillaizeau, F.; Planquette, B.; Pontal, D.; Guégan, M.; Simonneau, G.; Meyer, G.; et al. Prevalence of chronic thromboembolic pulmonary hypertension after acute pulmonary embolism. Prevalence of CTEPH after pulmonary embolism. Thromb. Haemost. 2014, 112, 598–605. [Google Scholar] [CrossRef]
- Nishiyama, K.H.; Saboo, S.S.; Tanabe, Y.; Jasinowodolinski, D.; Landay, M.J.; Kay, F.U. Chronic pulmonary embolism: Diagnosis. Cardiovasc. Diagn. Ther. 2018, 8, 253–271. [Google Scholar] [CrossRef] [PubMed]
- Gopalan, D.; Delcroix, M.; Held, M. Diagnosis of chronic thromboembolic pulmonary hypertension. Eur. Respir. Rev. 2017, 26, 160108. [Google Scholar] [CrossRef]
- Ribeiro, A.; Lindmarker, P.; Johnsson, H.; Juhlin-Dannfelt, A.; Jorfeldt, L. Pulmonary embolism: One-year follow-up with echocardiography doppler and five-year survival analysis. Circulation 1999, 99, 1325–1330. [Google Scholar] [CrossRef] [PubMed]
- Konstantinides, S.V.; Meyer, G.; Becattini, C.; Bueno, H.; Geersing, G.J.; Harjola, V.P.; Huisman, M.V.; Humbert, M.; Jennings, C.S.; Jiménez, D.; et al. 2019 ESC Guidelines for the diagnosis and management of acute pulmonary embolism developed in collaboration with the European Respiratory Society (ERS). Eur. Heart J. 2020, 41, 543–603. [Google Scholar] [CrossRef] [PubMed]
- Shirai, K.; Utino, J.; Otsuka, K.; Takata, M. A novel blood pressure-independent arterial wall stiffness parameter; cardio-ankle vascular index (CAVI). J. Atheroscler. Thromb. 2006, 13, 101–107. [Google Scholar] [CrossRef]
- Galiè, N.; Humbert, M.; Vachiery, J.L.; Gibbs, S.; Lang, I.; Torbicki, A.; Simonneau, G.; Peacock, A.; Vonk Noordegraaf, A.; Beghetti, M.; et al. 2015 ESC/ERS Guidelines for the diagnosis and treatment of pulmonary hypertension: The Joint Task Force for the Diagnosis and Treatment of Pulmonary Hypertension of the European Society of Cardiology (ESC) and the European Respiratory Society (ERS): Endorsed by: Association for European Paediatric and Congenital Cardiology (AEPC), International Society for Heart and Lung Transplantation (ISHLT). Eur. Heart J. 2016, 37, 67–119. [Google Scholar] [CrossRef]
- Williams, B.; Mancia, G.; Spiering, W.; Agabiti Rosei, E.; Azizi, M.; Burnier, M.; Clement, D.L.; Coca, A.; De Simone, G.; Dominiczak, A.; et al. ESC/ESH Guidelines for the management of arterial hypertension. Eur. Heart J. 2018, 39, 3021–3104. [Google Scholar] [CrossRef]
- Poscia, R.; Ghio, S.; D’Alto, M.; Vitulo, P.; Mulè, M.; Albera, C.; Parisi, F.; Badagliacca, R.; Fedele, F.; Vizza, C.D. ‘Real-life’ information on pulmonary arterial hypertension: The iPHnet Project. Curr. Med. Res. Opin. 2014, 30, 2409–2414. [Google Scholar] [CrossRef]
- Vizza, C.D.; Letizia, C.; Sciomer, S.; Naeije, R.; Della Rocca, G.; Di Roma, A.; Musarò, S.; Quattrucci, S.; Gaudio, C.; Battagliese, A.; et al. Increased plasma levels of adrenomedullin, a vasoactive peptide, in patients with end-stage pulmonary disease. Regul. Pept. 2005, 124, 187–193. [Google Scholar] [CrossRef]
- Badagliacca, R.; Poscia, R.; Pezzuto, B.; Papa, S.; Nona, A.; Mancone, M.; Mezzapesa, M.; Nocioni, M.; Sciomer, S.; Valli, G.; et al. Pulmonary arterial dilatation in pulmonary hypertension: Prevalence and prognostic relevance. Cardiology 2012, 121, 76–82. [Google Scholar] [CrossRef]
- Lang, R.M.; Bierig, M.; Devereux, R.B.; Flachskampf, F.A.; Foster, E.; Pellikka, P.A.; Picard, M.H.; Roman, M.J.; Seward, J.; Shanewise, J.S.; et al. Recommendations for chamber quantification: A report from the American Society of Echocardiography’s Guidelines and Standards Committee and the Chamber Quantification Writing Group, developed in conjunction with the European Association of Echocardiography, a branch of the European Society of Cardiology. J. Am. Soc. Echocardiogr. 2005, 18, 1440–1463. [Google Scholar] [CrossRef] [PubMed]
- Sciomer, S.; Badagliacca, R.; Fedele, F. Pulmonary hypertension: Echocardiographic assessment. Ital. Heart J. 2005, 6, 840–845. [Google Scholar]
- Badagliacca, R.; Papa, S.; Valli, G.; Pezzuto, B.; Poscia, R.; Manzi, G.; Giannetta, E.; Sciomer, S.; Palange, P.; Naeije, R.; et al. Echocardiography Combined With Cardiopulmonary Exercise Testing for the Prediction of Outcome in Idiopathic Pulmonary Arterial Hypertension. Chest 2016, 150, 1313–1322. [Google Scholar] [CrossRef]
- Badagliacca, R.; Reali, M.; Poscia, R.; Pezzuto, B.; Papa, S.; Mezzapesa, M.; Nocioni, M.; Valli, G.; Giannetta, E.; Sciomer, S.; et al. Right Intraventricular Dyssynchrony in Idiopathic, Heritable, and Anorexigen-Induced Pulmonary Arterial Hypertension: Clinical Impact and Reversibility. JACC Cardiovasc. Imaging 2015, 8, 642–652. [Google Scholar] [CrossRef] [PubMed]
- Badagliacca, R.; Pezzuto, B.; Papa, S.; Poscia, R.; Manzi, G.; Pascaretta, A.; Miotti, C.; Luongo, F.; Scoccia, G.; Ciciarello, F.; et al. Right Ventricular Strain Curve Morphology and Outcome in Idiopathic Pulmonary Arterial Hypertension. JACC Cardiovasc. Imaging 2021, 14, 162–172. [Google Scholar] [CrossRef] [PubMed]
- Badagliacca, R.; Papa, S.; Valli, G.; Pezzuto, B.; Poscia, R.; Reali, M.; Manzi, G.; Giannetta, E.; Berardi, D.; Sciomer, S.; et al. Right ventricular dyssynchrony and exercise capacity in idiopathic pulmonary arterial hypertension. Eur. Respir. J. 2017, 49, 1601419. [Google Scholar] [CrossRef]
- Badagliacca, R.; Raina, A.; Ghio, S.; D’Alto, M.; Confalonieri, M.; Correale, M.; Corda, M.; Paciocco, G.; Lombardi, C.; Mulè, M.; et al. Influence of various therapeutic strategies on right ventricular morphology, function and hemodynamics in pulmonary arterial hypertension. J. Heart Lung Transplant. 2018, 37, 365–375. [Google Scholar] [CrossRef]
- Yambe, M.; Tomiyama, H.; Hirayama, Y.; Gulniza, Z.; Takata, Y.; Koji, Y.; Motobe, K.; Yamashina, A. Arterial stiffening as a possible risk factor for both atherosclerosis and diastolic heart failure. Hypertens. Res. 2004, 27, 625–631. [Google Scholar] [CrossRef] [PubMed]
- Shirai, K.; Hiruta, N.; Song, M.; Kurosu, T.; Suzuki, J.; Tomaru, T.; Miyashita, Y.; Saiki, A.; Takahashi, M.; Suzuki, K.; et al. Cardio-ankle vascular index (CAVI) as a novel indicator of arterial stiffness: Theory, evidence and perspectives. J. Atheroscler. Thromb. 2011, 18, 924–938. [Google Scholar] [CrossRef] [PubMed]
- Stuart, E.A. Matching Methods for Causal Inference: A Review and a Look Forward. Statist. Sci. 2010, 25, 1–21. [Google Scholar] [CrossRef]
- Casazza, F.; Becattini, C.; Bongarzoni, A.; Cuccia, C.; Roncon, L.; Favretto, G.; Zonzin, P.; Pignataro, L.; Agnelli, G. Clinical features and short term outcomes of patients with acute pulmonary embolism. The Italian Pulmonary Embolism Registry (IPER). Thromb. Res. 2012, 130, 847–852. [Google Scholar] [CrossRef] [PubMed]
- Yambe, T.; Yoshizawa, M.; Saijo, Y.; Yamaguchi, T.; Shibata, M.; Konno, S.; Nitta, S.; Kuwayama, T. Brachio-ankle pulse wave velocity and cardio-ankle vascular index (CAVI). Biomed. Pharmacother. 2004, 58 (Suppl. 1), S95–S98. [Google Scholar] [CrossRef]
- Townsend, R.R.; Wilkinson, I.B.; Schiffrin, E.L.; Avolio, A.P.; Chirinos, J.A.; Cockcroft, J.R.; Heffernan, K.S.; Lakatta, E.G.; McEniery, C.M.; Mitchell, G.F.; et al. American Heart Association Council on Hypertension. Recommendations for Improving and Standardizing Vascular Research on Arterial Stiffness: A Scientific Statement from the American Heart Association. Hypertension 2015, 66, 698–722. [Google Scholar] [CrossRef]
- Schillaci, G.; Battista, F.; D’Abbondanza, M.; Pucci, G. The impact of the cardio-ankle vascular index on left ventricular structure and function. Eur. Heart J. Suppl. 2017, 19 (Suppl. B), B30–B34. [Google Scholar] [CrossRef][Green Version]
- Hayashi, K.; Yamamoto, T.; Takahara, A.; Shirai, K. Clinical assessment of arterial stiffness with cardio-ankle vascular index: Theory and applications. J. Hypertens. 2015, 33, 1742–1757, discussion 1757. [Google Scholar] [CrossRef] [PubMed]
- Radchenko, G.D.; Zhyvylo, I.O.; Titov, E.Y.; Sirenko, Y.M. Systemic Arterial Stiffness in New Diagnosed Idiopathic Pulmonary Arterial Hypertension Patients. Vasc. Health Risk Manag. 2020, 16, 29–39. [Google Scholar] [CrossRef]
- Sznajder, M.; Dzikowska-Diduch, O.; Kurnicka, K.; Roik, M.; Wretowski, D.; Pruszczyk, P.; Kostrubiec, M. Increased systemic arterial stiffness in patients with chronic thromboembolic pulmonary hypertension. Cardiol. J. 2020, 27, 742–748. [Google Scholar] [CrossRef]
- Laurent, S.; Cockcroft, J.; Van Bortel, L.; Boutouyrie, P.; Giannattasio, C.; Hayoz, D.; Pannier, B.; Vlachopoulos, C.; Wilkinson, I.; Struijker-Boudier, H. European Network for Non-invasive Investigation of Large Arteries. Expert consensus document on arterial stiffness: Methodological issues and clinical applications. Eur. Heart J. 2006, 27, 2588–2605. [Google Scholar] [CrossRef] [PubMed]
- McEniery, C.M.; Yasmin; Hall, I.R.; Qasem, A.; Wilkinson, I.B.; Cockcroft, J.R.; ACCT Investigators. Normal vascular aging: Differential effects on wave reflection and aortic pulse wave velocity: The Anglo-Cardiff Collaborative Trial (ACCT). J. Am. Coll. Cardiol. 2005, 46, 1753–1760. [Google Scholar] [CrossRef] [PubMed]
- Simon, A.C.; Levenson, J.; Bouthier, J.; Safar, M.E.; Avolio, A.P. Evidence of early degenerative changes in large arteries in human essential hypertension. Hypertension 1985, 7, 675–680. [Google Scholar] [CrossRef]
- Watahiki, M.; Horinaka, S.; Ishimitsu, T.; Toyoda, S.; Inoue, T. Comparing the Heart–Thigh and Thigh–Ankle Arteries with the Heart–Ankle Arterial Segment for Arterial Stiffness Measurements. Vasc. Health Risk Manag. 2020, 16, 561–570. [Google Scholar] [CrossRef] [PubMed]
- Mahmud, A.; Feely, J. Arterial Stiffness Is Related to Systemic Inflammation in Essential Hypertension. Hypertension 2005, 46, 1118–1122. [Google Scholar] [CrossRef]
- Stewart, L.K.; Nordenholz, K.E.; Courtney, M.; Kabrhel, C.; Jones, A.E.; Rondina, M.T.; Diercks, D.B.; Klinger, J.R.; Kline, J.A. Comparison of acute and convalescent biomarkers of inflammation in patients with acute pulmonary embolism treated with systemic fibrinolysis vs. placebo. Blood Coagul. Fibrinolysis 2017, 28, 675–680. [Google Scholar] [CrossRef]
- Jezovnik, M.K.; Poredos, P. Idiopathic venous thrombosis is related to systemic inflammatory response and to increased levels of circulating markers of endothelial dysfunction. Int. Angiol. 2010, 29, 226–231. [Google Scholar]
- Smeeth, L.; Cook, C.; Thomas, S.; Hall, A.J.; Hubbard, R.; Vallance, P. Risk of deep vein thrombosis and pulmonary embolism after acute infection in a community setting. Lancet 2006, 367, 1075–1079. [Google Scholar] [CrossRef]
- Zabini, D.; Heinemann, A.; Foris, V.; Nagaraj, C.; Nierlich, P.; Bálint, Z.; Kwapiszewska, G.; Lang, I.M.; Klepetko, W.; Olschewski, H.; et al. Comprehensive analysis of inflammatory markers in chronic thromboembolic pulmonary hypertension patients. Eur. Respir. J. 2014, 44, 951–962. [Google Scholar] [CrossRef] [PubMed]
- Pezzuto, B.; Badagliacca, R.; Poscia, R.; Ghio, S.; D’Alto, M.; Vitulo, P.; Mulè, M.; Albera, C.; Volterrani, M.; Fedele, F.; et al. Circulating biomarkers in pulmonary arterial hypertension: Update and future direction. J. Heart Lung Transplant. 2015, 34, 282–305. [Google Scholar] [CrossRef]
- Voelkel, N.F.; Cool, C.; Lee, S.D.; Wright, L.; Geraci, M.W.; Tuder, R.M. Primary pulmonary hypertension between inflammation and cancer. Chest 1998, 114 (Suppl. 3), 225S–230S. [Google Scholar] [CrossRef]
- Tamby, M.C.; Chanseaud, Y.; Humbert, M.; Fermanian, J.; Guilpain, P.; Garcia-de-la-Peña-Lefebvre, P.; Brunet, S.; Servettaz, A.; Weill, B.; Simonneau, G.; et al. Anti-endothelial cell antibodies in idiopathic and systemic sclerosis associated pulmonary arterial hypertension. Thorax 2005, 60, 765–772. [Google Scholar] [CrossRef]
- Yanai-Landau, H.; Amital, H.; Bar-Dayan, Y.; Levy, Y.; Gur, H.; Lin, H.C.; Alosachie, I.J.; Peter, J.B.; Shoenfeld, Y. Autoimmune aspects of primary pulmonary hypertension. Pathobiology 1995, 63, 71–75. [Google Scholar] [CrossRef]
- Vizza, C.D.; Letizia, C.; Badagliacca, R.; Poscia, R.; Pezzuto, B.; Gambardella, C.; Nona, A.; Papa, S.; Marcon, S.; Mancone, M.; et al. Relationship between baseline ET-1 plasma levels and outcome in patients with idiopathic pulmonary hypertension treated with bosentan. Int. J. Cardiol. 2013, 167, 220–224. [Google Scholar] [CrossRef] [PubMed]
- Calabrò, P.; Limongelli, G.; Maddaloni, V.; Vizza, C.D.; D’Alto, M.; D’Alessandro, R.; Poscia, R.; Argiento, P.; Ziello, B.; Badagliacca, R.; et al. Analysis of endothelin-1 and endothelin-1 receptor A gene polymorphisms in patients with pulmonary arterial hypertension. Intern. Emerg. Med. 2012, 7, 425–430. [Google Scholar] [CrossRef] [PubMed]
- Stefanantoni, K.; Sciarra, I.; Vasile, M.; Badagliacca, R.; Poscia, R.; Pendolino, M.; Alessandri, C.; Vizza, C.D.; Valesini, G.; Riccieri, V. Elevated serum levels of macrophage migration inhibitory factor and stem cell growth factor β in patients with idiopathic and systemic sclerosis associated pulmonary arterial hypertension. Reumatismo 2015, 66, 270–276. [Google Scholar] [CrossRef]
- Quarck, R.; Nawrot, T.; Meyns, B.; Delcroix, M. C-reactive protein: A new predictor of adverse outcome in pulmonary arterial hypertension. J. Am. Coll. Cardiol. 2009, 53, 1211–1218. [Google Scholar] [CrossRef]
- Pussadhamma, B.; Suwannakrua, W.; Toparkngarm, P.; Wongvipaporn, C.; Foocharoen, C.; Nanagara, R. Relationship between Peripheral Arterial Stiffness and Estimated Pulmonary Pressure by Echocardiography in Systemic Sclerosis. Acta Cardiol. Sin. 2017, 33, 514–522. [Google Scholar] [CrossRef] [PubMed]
- Lang, I.M.; Madani, M. Update on chronic thromboembolic pulmonary hypertension. Circulation 2014, 130, 508–518. [Google Scholar] [CrossRef] [PubMed]
- Klok, F.A.; Dzikowska-Diduch, O.; Kostrubiec, M.; Vliegen, H.W.; Pruszczyk, P.; Hasenfuß, G.; Huisman, M.V.; Konstantinides, S.; Lankeit, M. Derivation of a clinical prediction score for chronic thromboembolic pulmonary hypertension after acute pulmonary embolism. J. Thromb. Haemost. 2016, 14, 121–128. [Google Scholar] [CrossRef] [PubMed]
- Radchenko1, G.D.; Sirenko, Y.M. Prognostic Significance of Systemic Arterial Stiffness Evaluated by Cardio-Ankle Vascular Index in Patients with Idiopathic Pulmonary Hypertension. Vasc. Health Risk Manag. 2021, 17, 77–93. [Google Scholar] [CrossRef] [PubMed]
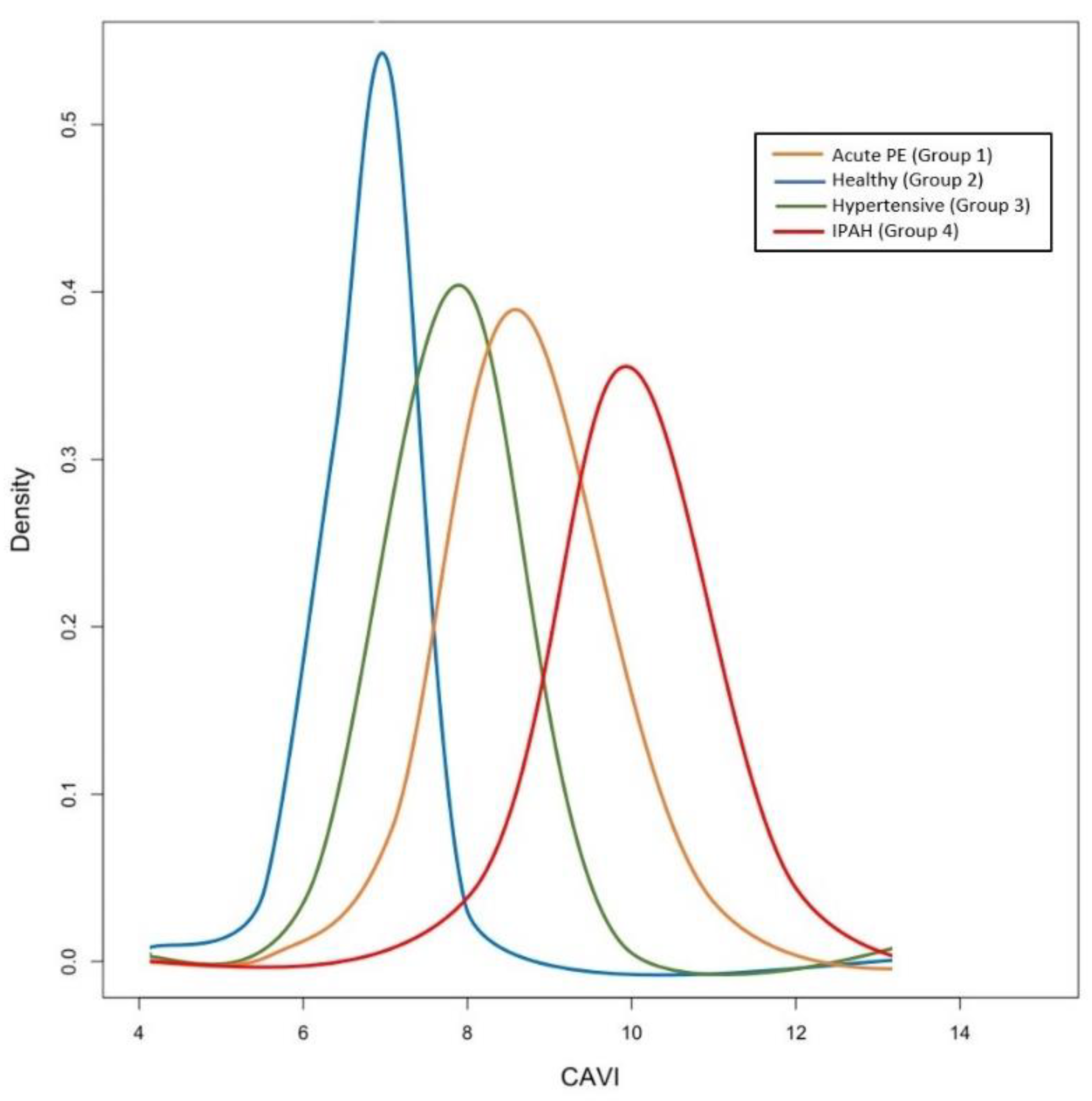
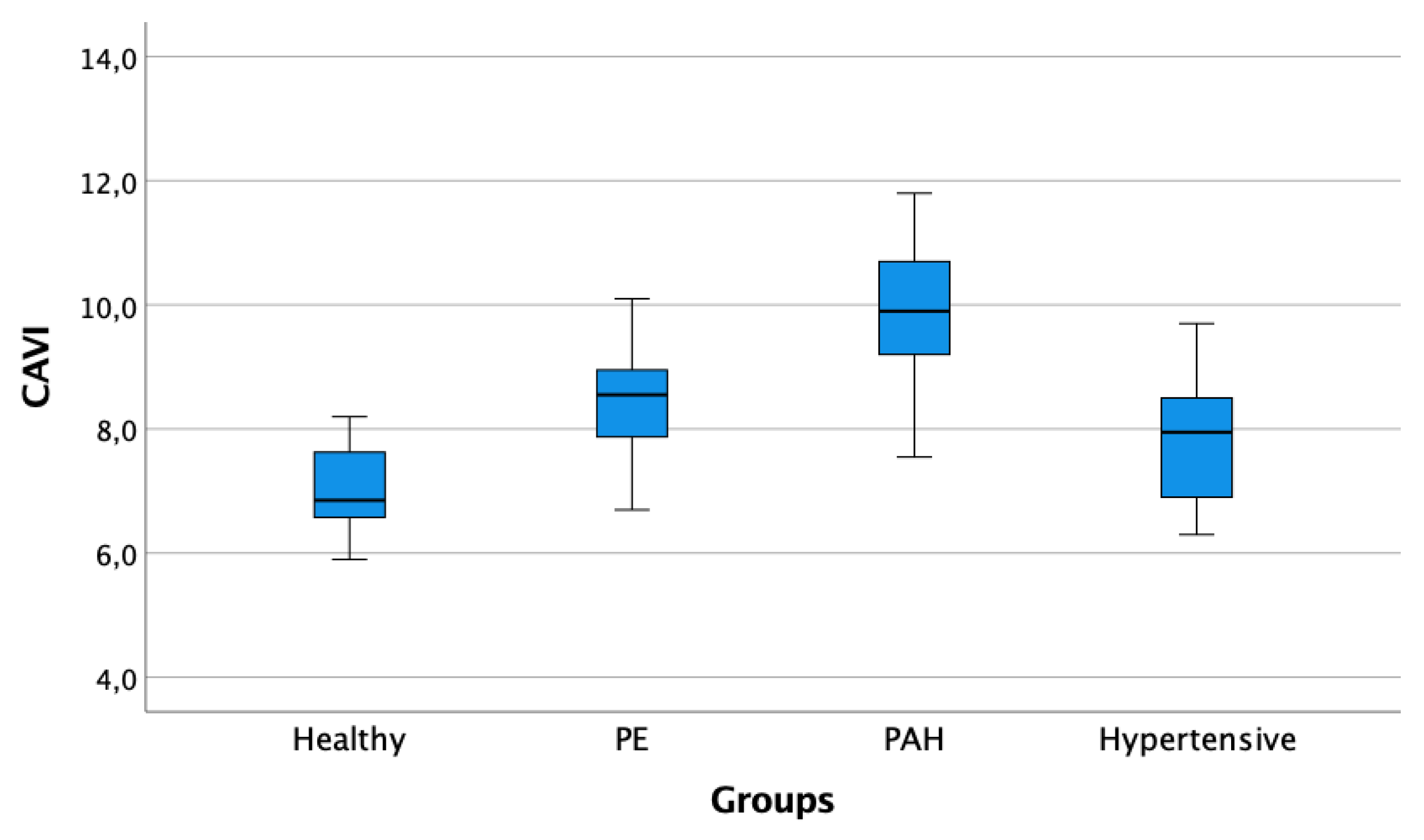
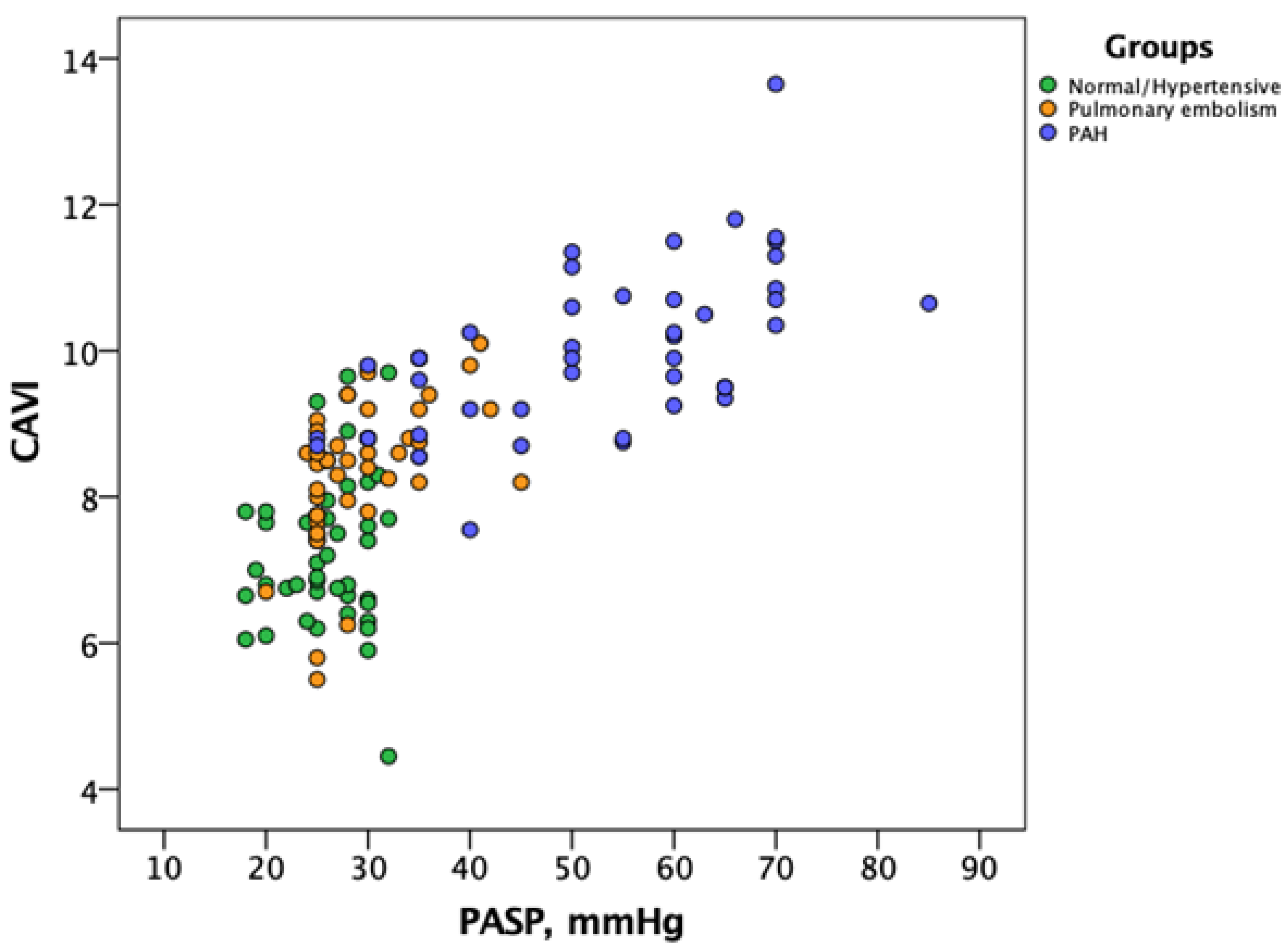
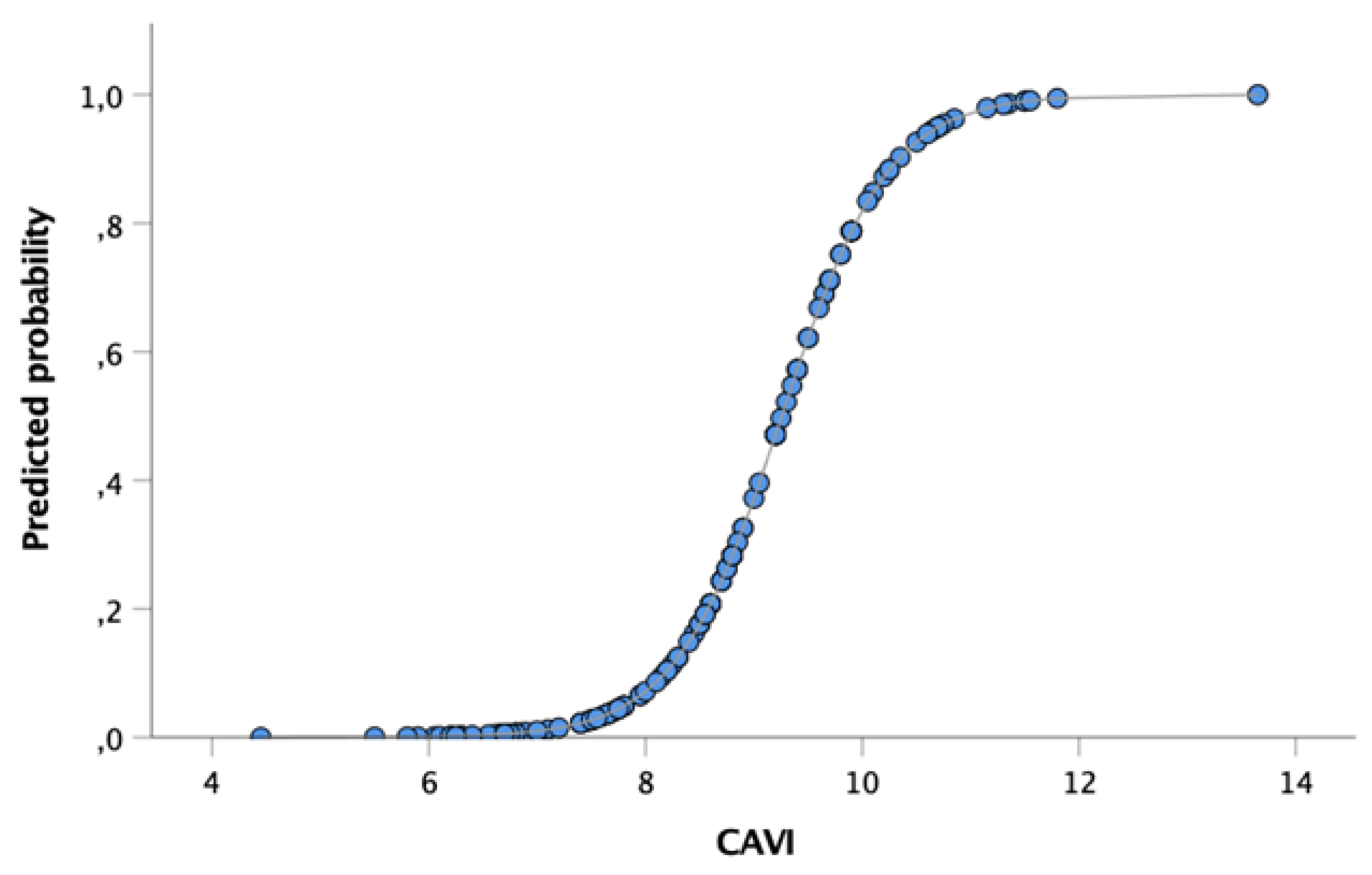
| Acute PE | Healthy | Hypertensive | IPAH | |
|---|---|---|---|---|
| Patients, n | 40 | 40 | 40 | 45 |
| Age, years | 69 ± 15 | 67 ± 12 | 69 ± 13 | 67 ± 11 |
| Gender, F:M, n | 22:18 | 21:19 | 20:20 | 23:22 |
| Height, cm | 163 ± 9 | 165 ± 8 | 164 ± 9 | 163 ± 10 |
| Weight, Kg | 68 ± 12 | 66 ± 10 | 70 ± 11 | 68 ± 9 |
| Comorbidities, n (%) | ||||
| Smoking | 7 (17.5%) | 6 (15%) | 8 (20%) | 0 (0%) |
| Hypercholesterolemia | 10 (25%) | 4 (10%) | 11 (27.5%) | 6 (13.3%) |
| Diabetes mellitus | 6 (15%) | 0 (0%) | 5 (12.5%) | 4 (8.8%) |
| systemic hypertension | 12 (30%) | 0 (0%) | 40 (100%) | 0 (0%) |
| Risk factors for PE, n (%) | ||||
| immobilization >3 days, % | 10 (25%) | 0 (0%) | 0 (0%) | 0 (0%) |
| previous VTE, % | 9 (22.5%) | 0 (0%) | 0 (0%) | 0 (0%) |
| history of cancer | 6 (15%) | 0 (0%) | 0 (0%) | 0 (0%) |
| NYHA/WHO, n (%) | 2.6 ± 0.6 | 1.0 | 1.5 ± 0.7 | 2.5 ± 1.4 |
| I | 7 (17.5%) | 40 (100%) | 32 (80%) | 5 (11.1%) |
| II | 13 (32.5%) | 0 (0%) | 8 (20%) | 18 (40%) |
| III | 16 (40%) | 0 (0%) | 0 (0%) | 18 (40%) |
| IV | 4 (10%) | 0 (0%) | 0 (0%) | 4 (8.9%) |
| SBP, mmHg | 117 ± 18 | 115 ± 12 | 140 ± 14 | 110 ± 13 |
| DBP, mmHg | 71 ± 9 | 66 ± 7 | 89 ± 8 | 68 ± 8 |
| HR, b/m | 84 ± 13 | 79 ± 6 | 80 ± 7 | 80 ± 11 |
| CAVI | 8.6 (7.8; 9.0) | 6.9 (6.6; 7.7) | 7.9 (6.8; 8.5) | 9.9 (9.2; 10.7) |
| Echocardiography * | ||||
| LVEDd (mm) | 48.2 ± 4.3 | 47.8 ± 3.8 | 49.1 ± 4.3 | 43.5 ± 4.3 |
| LVEDA (cm2) | 38.8 ± 2.5 | 40.1 ± 4.8 | 42.1 ± 5.8 | 30.8 ± 4.7 |
| LVESA (cm2) | 19.4 ± 4.4 | 20.3 ± 4.3 | 21.5 ± 5.2 | 17.6 ± 4.4 |
| LA area, (cm2) | 18.2 ± 3.1 | 15.2 ± 2.4 | 21.5 ± 3.2 | 13.6 ± 3.4 |
| LVEF, % | 56 ± 5 | 58 ± 4 | 57 ± 4 | 56 ± 4 |
| TAPSE, mm | 20.2 ± 3.3 | 24.5 ± 2.8 | 25.1 ± 2.7 | 16.9 ± 3.2 |
| RA area, cm2 | 20.1 ± 2.8 | 13.3 ± 2.5 | 14.1 ± 2.7 | 26.2 ± 6.6 |
| PASP, mmHg, n (%) | ||||
| ≥40 | 8 (20%) | 0 (0%) | 0 (0%) | 45 (100%) |
| RV/LV ratio, n (%) | ||||
| 1 | 2 (5%) | 0 (0%) | 0 (0%) | 18 (40%) |
| >1 | 3 (7.5%) | 0 (0%) | 0 (0%) | 27 (60%) |
| <1 | 35 (87.5%) | 40 (100%) | 40 (100%) | 0 (0%) |
| Acute PE | CTEPH | p | |
|---|---|---|---|
| Patients, n | 40 | 4 | |
| Age, years | 69 ± 15 | 70 ± 4.2 | ns |
| Gender, F:M, n | 22:18 | 2:2 | ns |
| Height, cm | 163 ± 9 | 162 ± 8 | ns |
| Weight, Kg | 68 ± 12 | 71 ± 5.6 | ns |
| WHO, n (%) | 2.6 ± 0.6 | 2.5 ± 0.7 | ns |
| I | 7 (17.5%) | 0 (0%) | |
| II | 13 (32.5%) | 1 (25%) | |
| III | 16 (40%) | 3 (75%) | |
| IV | 4 (10%) | 0 (0%) | |
| CAVI | 8.6 (7.8; 9.0) | 9.75 (9.4; 10.1) | <0.01 |
| Echocardiography * | |||
| TAPSE, mm | 20 ± 3 | 17.5 ± 3.5 | <0.01 |
| RA area, cm2 | 20 ± 2.8 | 23.5 ± 3.5 | <0.01 |
| PASP, mmHg, n (%) | |||
| ≥40 | 8 (20%) | 4 (100%) | <0.01 |
| RV/LV ratio, n (%) | <0.01 | ||
| 1 | 2 (5%) | 1 (25%) | |
| >1 | 3 (7.5%) | 3 (75%) | |
| <1 | 35 (87.5%) | 0 (0%) |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Papa, S.; Miotti, C.; Manzi, G.; Scoccia, G.; Luongo, F.; Toto, F.; Malerba, C.; Cedrone, N.; Canuti, E.S.; Caputo, A.; et al. Peripheral Arterial Stiffness in Acute Pulmonary Embolism and Pulmonary Hypertension at Short-Term Follow-Up. J. Clin. Med. 2021, 10, 3008. https://doi.org/10.3390/jcm10143008
Papa S, Miotti C, Manzi G, Scoccia G, Luongo F, Toto F, Malerba C, Cedrone N, Canuti ES, Caputo A, et al. Peripheral Arterial Stiffness in Acute Pulmonary Embolism and Pulmonary Hypertension at Short-Term Follow-Up. Journal of Clinical Medicine. 2021; 10(14):3008. https://doi.org/10.3390/jcm10143008
Chicago/Turabian StylePapa, Silvia, Cristiano Miotti, Giovanna Manzi, Gianmarco Scoccia, Federico Luongo, Federica Toto, Claudia Malerba, Nadia Cedrone, Elena Sofia Canuti, Annalisa Caputo, and et al. 2021. "Peripheral Arterial Stiffness in Acute Pulmonary Embolism and Pulmonary Hypertension at Short-Term Follow-Up" Journal of Clinical Medicine 10, no. 14: 3008. https://doi.org/10.3390/jcm10143008
APA StylePapa, S., Miotti, C., Manzi, G., Scoccia, G., Luongo, F., Toto, F., Malerba, C., Cedrone, N., Canuti, E. S., Caputo, A., Manguso, G., Valentini, S., Sciomer, S., Ciciarello, F., Benedetti, G., Fedele, F., Vizza, C. D., & Badagliacca, R. (2021). Peripheral Arterial Stiffness in Acute Pulmonary Embolism and Pulmonary Hypertension at Short-Term Follow-Up. Journal of Clinical Medicine, 10(14), 3008. https://doi.org/10.3390/jcm10143008






