Coverage and Timeliness of Birth Dose Vaccination in Sub-Saharan Africa: A Systematic Review and Meta-Analysis
Abstract
1. Introduction
2. Materials and Methods
2.1. Data Sources and Searches
2.2. Eligibility Criteria
2.3. Data Extraction
2.4. Statistical Analysis
3. Results
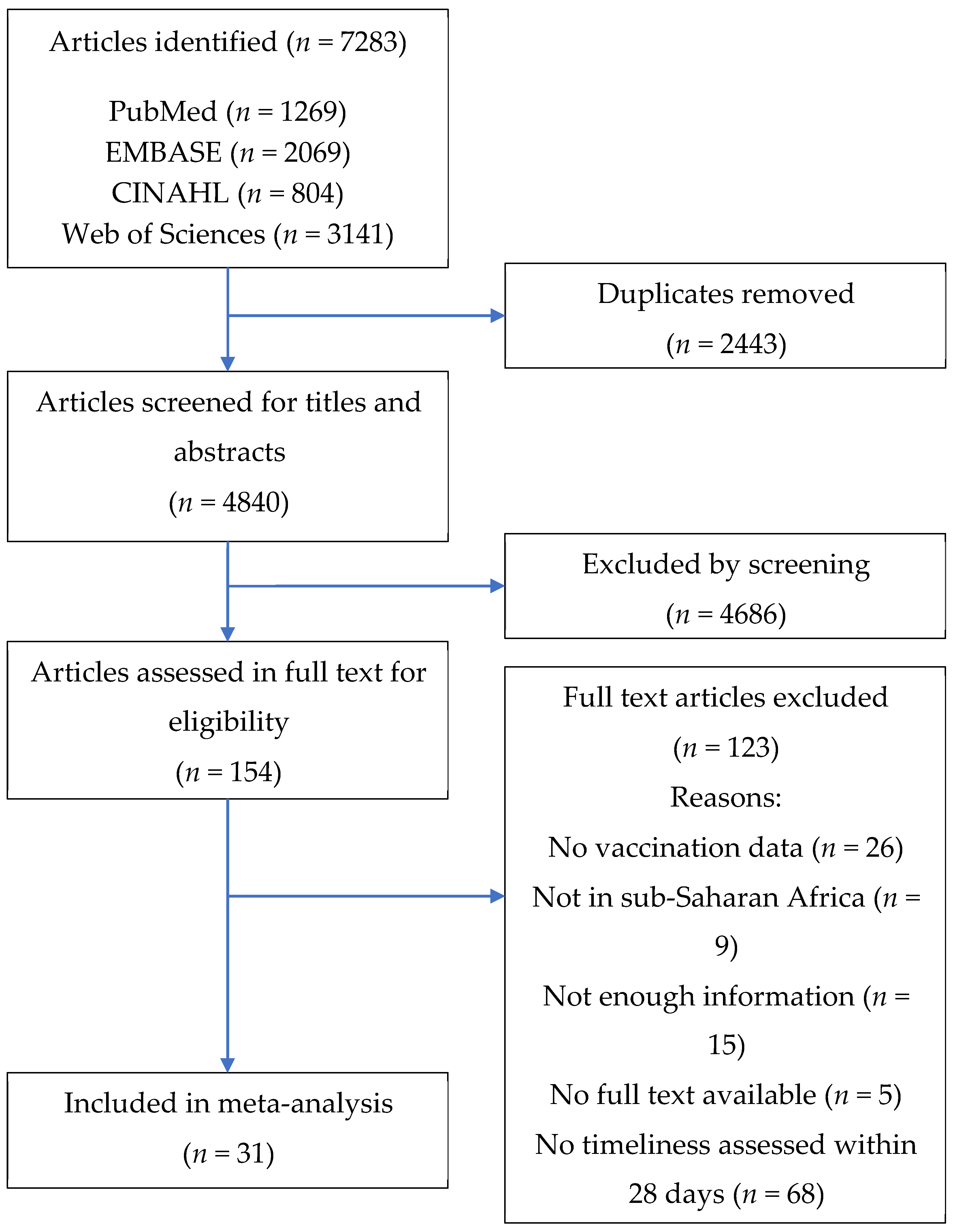
3.1. Study Selection
3.2. Study Characteristics
3.3. Risk of Bias
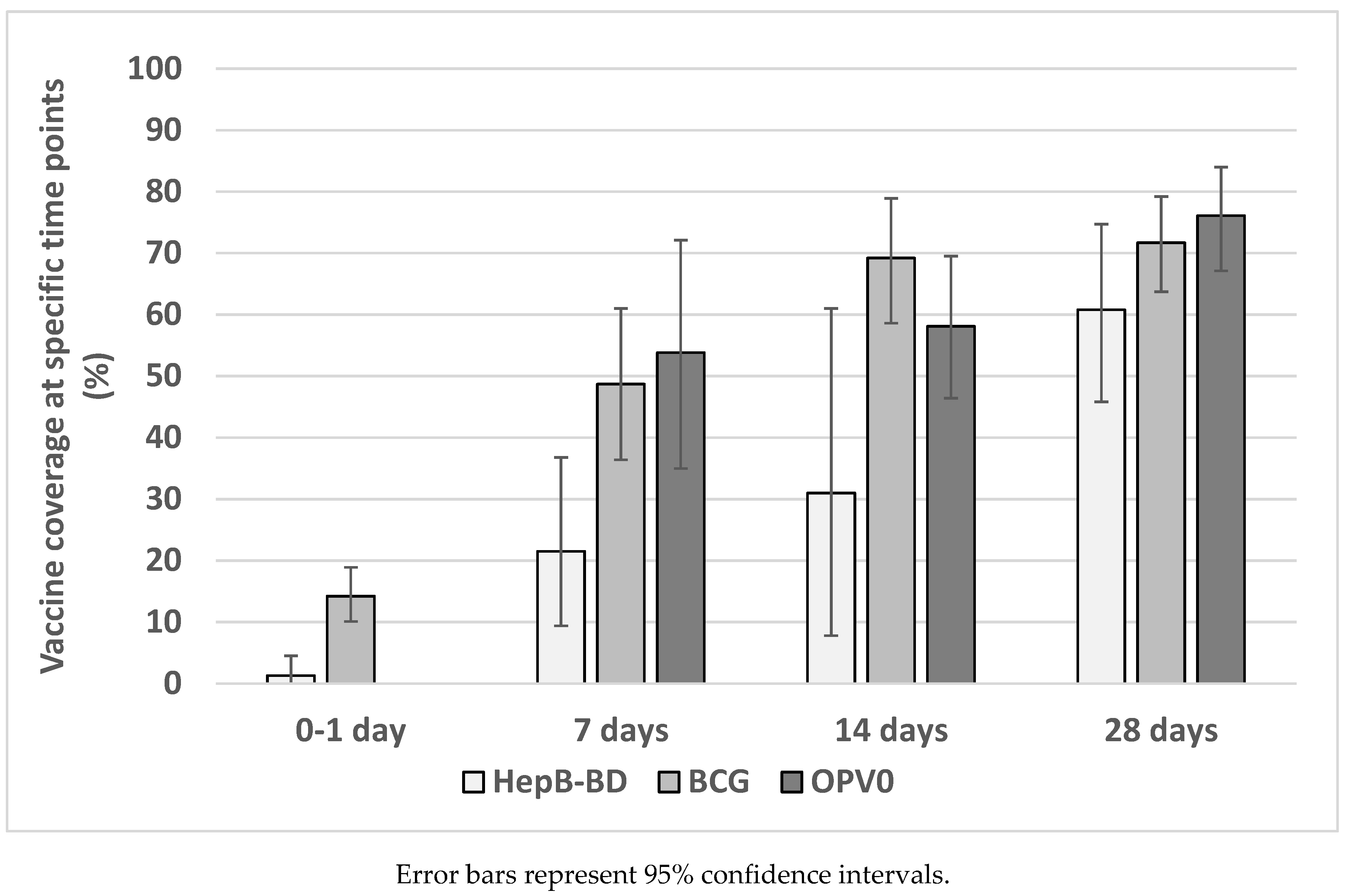
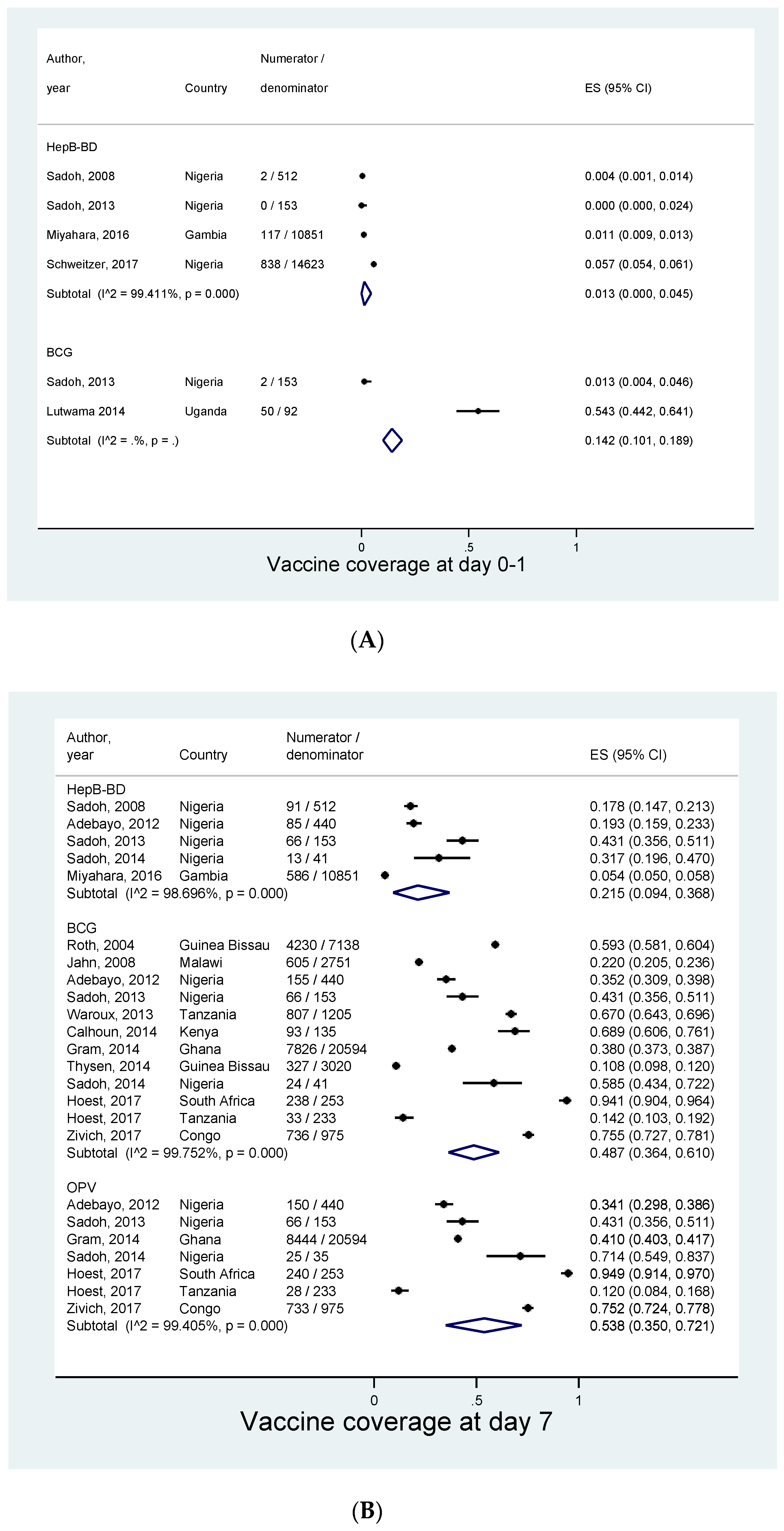
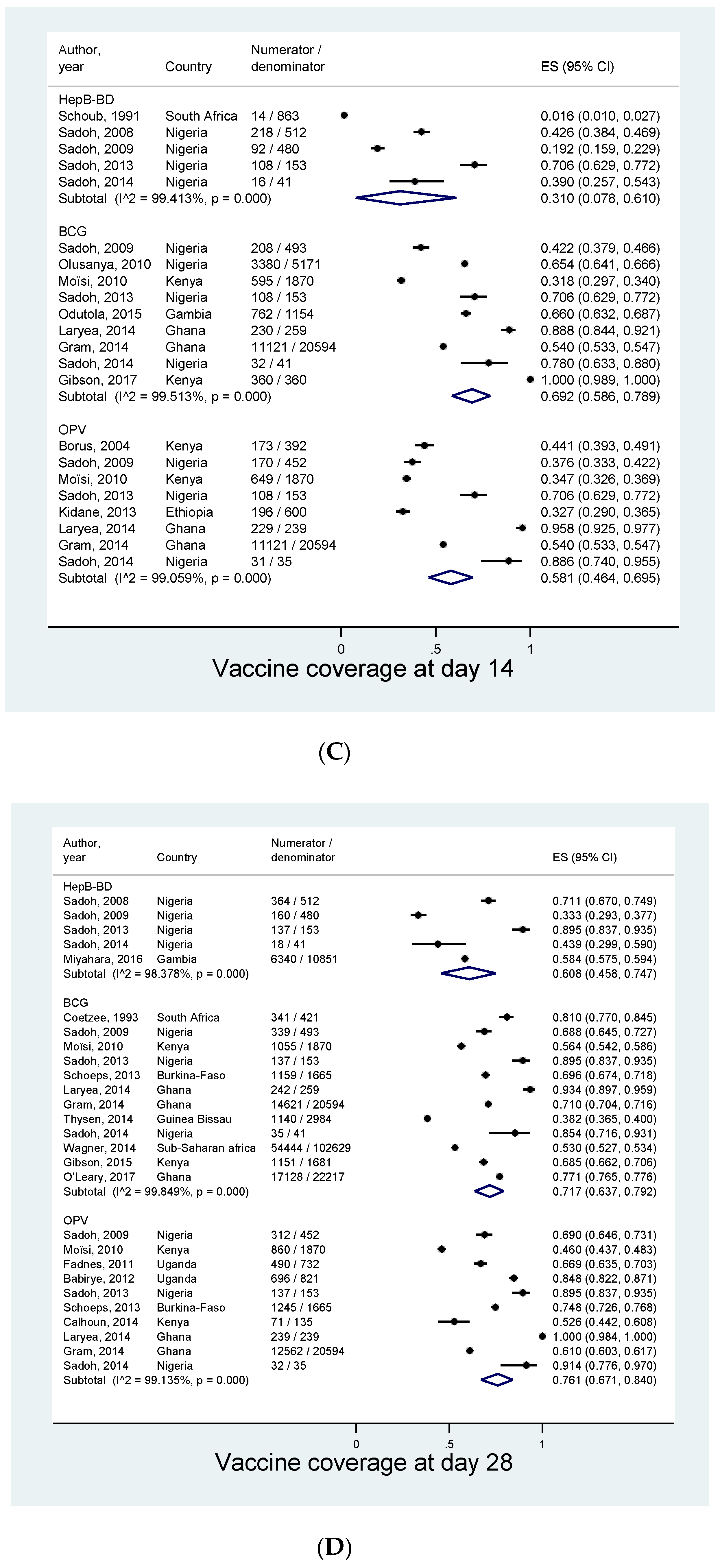
3.4. Coverage and Timeliness of Birth Dose Vaccines
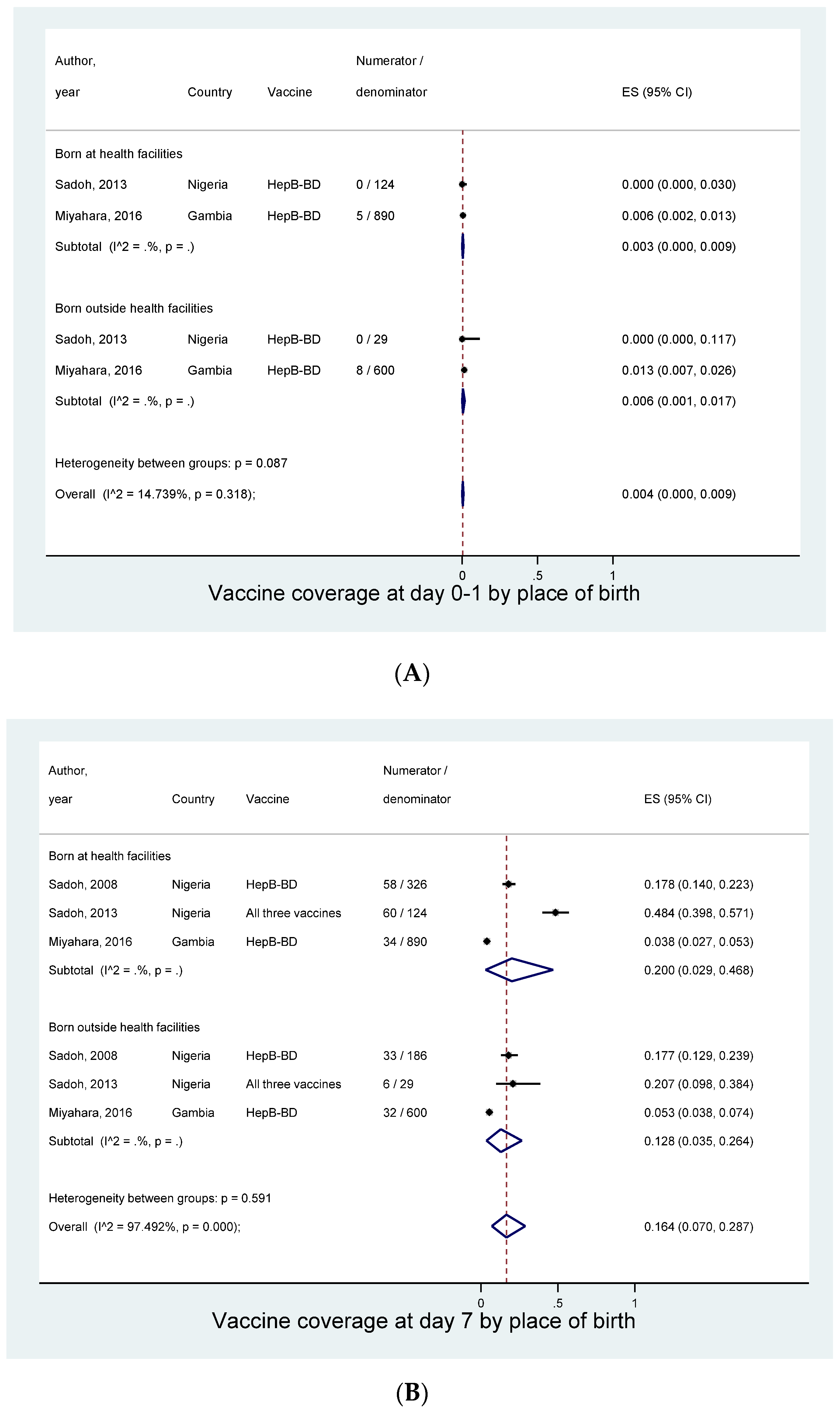
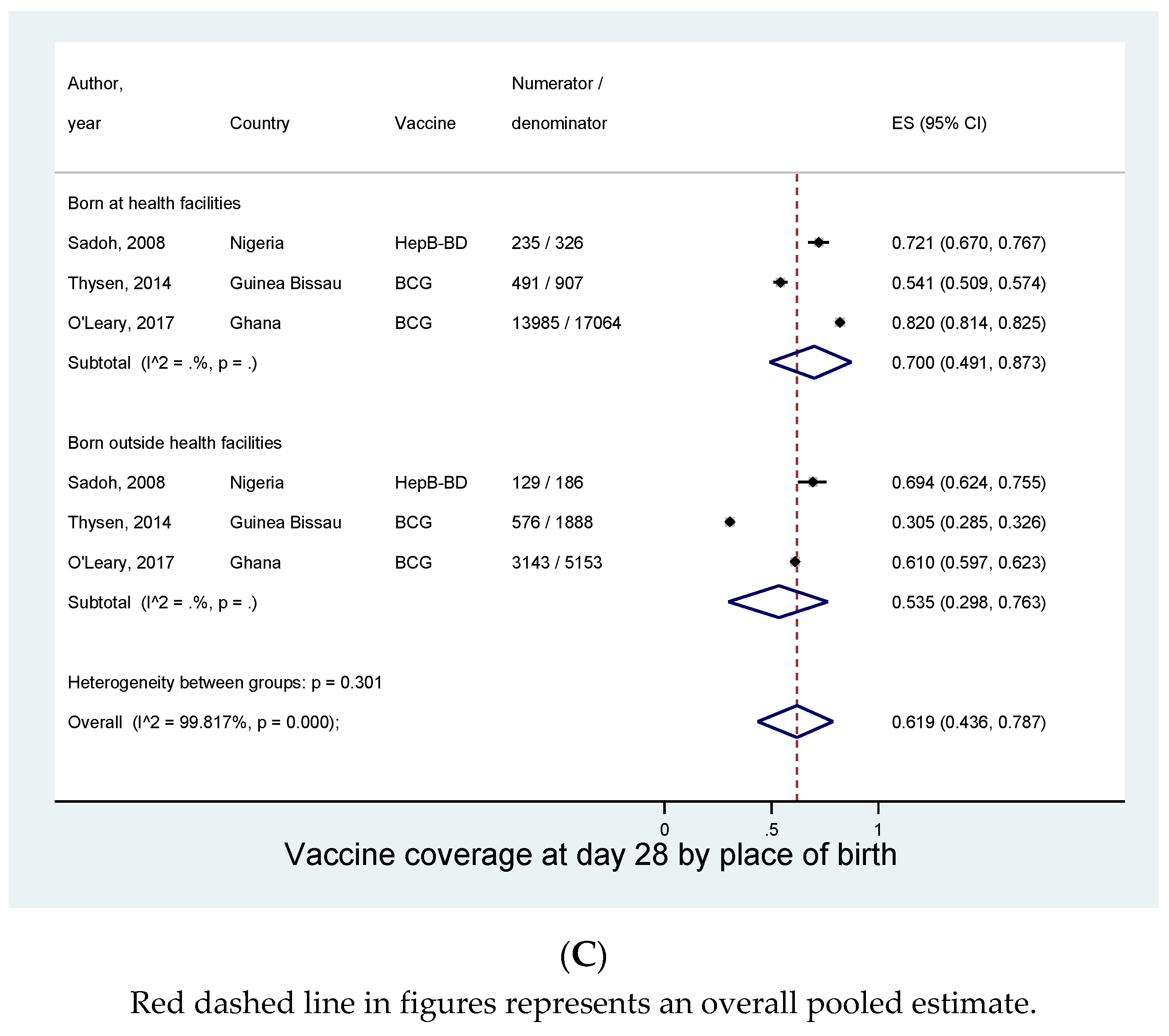
3.5. Subgroup Analysis
4. Discussion
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Acknowledgments
Conflicts of Interest
References
- Andre, F.; Booy, R.; Bock, H.L.; Clemens, J.; Datta, S.K.; John, T.J.; Lee, B.W.; Lolekha, S.; Peltola, H.; Ruff, T.A.; et al. Vaccination greatly reduces disease, disability, death and inequity worldwide. Bull. World Heal. Organ. 2008, 86, 140–146. [Google Scholar] [CrossRef] [PubMed]
- Lee, L.A.; Franzel, L.; Atwell, J.; Datta, S.D.; Friberg, I.K.; Goldie, S.J.; Reef, S.E.; Schwalbe, N.; Simons, E.; Strebel, P.M.; et al. The estimated mortality impact of vaccinations forecast to be administered during 2011–2020 in 73 countries supported by the GAVI Alliance. Vaccine 2013, 31, B61–B72. [Google Scholar] [CrossRef] [PubMed]
- World Health Organization. BCG Vaccines: WHO Position Paper-February 2018; The Weekly Epidemiological Record (WER): Geneva, Switzerland, 2018; Volume 93, pp. 73–96. [Google Scholar]
- World Health Organization. Polio Vaccines: WHO Position Paper-March 2016; The Weekly Epidemiological Record (WER): Geneva, Switzerland, 2016; Volume 91, pp. 145–168. [Google Scholar]
- World Health Organization. Hepatitis B Vaccines: WHO Position Paper-July 2017; The Weekly Epidemiological Record (WER): Geneva, Switzerland, 2017; Volume 27, pp. 369–392. [Google Scholar]
- Roy, P.; Vekemans, J.; Clark, A.; Sanderson, C.; Harris, R.C.; White, R.G. Potential effect of age of BCG vaccination on global paediatric tuberculosis mortality: A modelling study. Lancet Glob. Heal. 2019, 7, e1655–e1663. [Google Scholar] [CrossRef]
- Higgins, J.P.T.; Soares-Weiser, K.; Lopez-Lopez, J.; Kakourou, A.; Chaplin, K.; Christensen, H.; Martin, N.K.; Sterne, J.A.; Reingold, A.L. Association of BCG, DTP, and measles containing vaccines with childhood mortality: Systematic review. BMJ 2016, 355, i5170. [Google Scholar] [CrossRef]
- Lund, N.; Andersen, A.; Hansen, A.S.K.; Jepsen, F.S.; Barbosa, A.; Biering-Sørensen, S.; Rodrigues, A.; Ravn, H.; Aaby, P.; Benn, C.S. The Effect of Oral Polio Vaccine at Birth on Infant Mortality: A Randomized Trial. Clin. Infect. Dis. 2015, 61, 1504–1511. [Google Scholar] [CrossRef]
- World Bank. Mortality Rate, Infant (per 1000 Live Births) | Data [Internet]. 2018. Available online: https://data.worldbank.org/indicator/SP.DYN.IMRT.IN (accessed on 29 March 2020).
- World Health Organization. WHO Vaccine-Preventable Diseases: Monitoring System. 2019 Global Summary [Internet]. 2019. Available online: http://apps.who.int/immunizationmonitoring/globalsummary/schedules (accessed on 29 March 2020).
- World Health Organization. Global and Regional Immunization Profile. African Region. [Internet]. 2019. Available online: https://www.who.int/immunization/monitoring_surveillance/data/AFR/en/ (accessed on 29 March 2020).
- Clark, A.; Sanderson, C. Timing of children’s vaccinations in 45 low-income and middle-income countries: An analysis of survey data. Lancet 2009, 373, 1543–1549. [Google Scholar] [CrossRef]
- World Health Organization. WHO/UNICEF Joint Reporting Process [Internet]. 2019. Available online: https://www.who.int/immunization/monitoring_surveillance/routine/reporting/en/ (accessed on 29 March 2020).
- Liberati, A.; Altman, D.G.; Tetzlaff, J.; Mulrow, C.; Gøtzsche, P.C.; Ioannidis, J.P.A.; Clarke, M.; Devereaux, P.J.; Kleijnen, J.; Moher, D. The PRISMA statement for reporting systematic reviews and meta-analyses of studies that evaluate health care interventions: Explanation and elaboration. J. Clin. Epidemiol. 2009, 62, e1–e34. [Google Scholar] [CrossRef]
- Egger, M.; Smith, G.D.; Altman, D. Systematic Reviews in Health Care: Meta-Analysis in Context; Wiley-Blackwell: Oxford, UK, 2001; p. 512. [Google Scholar]
- Nyaga, V.N.; Arbyn, M.; Aerts, M. Metaprop: A Stata command to perform meta-analysis of binomial data. Arch. Public Heal. 2014, 72, 1–10. [Google Scholar] [CrossRef] [PubMed]
- Freeman, M.F.; Tukey, J.W. Transformations Related to the Angular and the Square Root. Ann. Math. Stat. 1950, 21, 607–611. [Google Scholar] [CrossRef]
- DerSimonian, R.; Laird, N. Meta-analysis in clinical trials. Control. Clin. Trials 1986, 7, 177–188. [Google Scholar] [CrossRef]
- Wagner, Z.; Szilagyi, P.G.; Sood, N. Comparative performance of public and private sector delivery of BCG vaccination: Evidence from Sub-Saharan Africa. Vaccine 2014, 32, 4522–4528. [Google Scholar] [CrossRef] [PubMed]
- Coetzee, D.J.; Ferrinho, P.; Reinach, S.G. A vaccination survey using the EPI methodology ot evaluate the impact of a child health outreach programme in an urban area of South Africa. Bull. World Heal. Organ. 1993, 71, 33–39. [Google Scholar]
- Roth, A.; Jensen, H.; Garly, M.-L.; Djana, Q.; Martins, C.; Sodemann, M.; Rodrigues, A.; Aaby, P. Low birth weight infants and Calmette-Guérin bacillus vaccination at birth: Community study from Guinea-Bissau. Pediatr. Infect. Dis. J. 2004, 23, 544–550. [Google Scholar] [CrossRef] [PubMed]
- Jahn, A.; Floyd, S.; Mwinuka, V.; Mwafilaso, J.; Mwagomba, D.; Mkisi, R.E.; Katsulukuta, A.; Khunga, A.; Crampin, A.; Branson, K.; et al. Ascertainment of childhood vaccination histories in northern Malawi. Trop. Med. Int. Heal. 2008, 13, 129–138. [Google Scholar] [CrossRef]
- Moïsi, J.C.; Kabuka, J.; Mitingi, R.; Levine, O.S.; Scott, J.A.G. Spatial and socio-demographic predictors of time-to-immunization in a rural area in Kenya: Is equity attainable? Vaccine 2010, 28, 5725–5730. [Google Scholar] [CrossRef] [PubMed]
- Fadnes, L.T.; Jackson, D.; Engebretsen, I.M.S.; Zembe-Mkabile, W.; Sanders, D.; Sommerfelt, H.; Tylleskär, T. Vaccination coverage and timeliness in three South African areas: A prospective study. BMC Public Heal. 2011, 11, 404. [Google Scholar] [CrossRef]
- Adebayo, B.E.; Oladokun, R.E.; Akinbami, F.O. Immunization Coverage in A Rural Community in Southwestern Nigeria. J. Vaccines Vaccin. 2012, 3, 1–6. [Google Scholar] [CrossRef]
- Babirye, J.N.; Engebretsen, I.M.S.; Makumbi, F.; Fadnes, L.T.; Wamani, H.; Tylleskär, T.; Nuwaha, F. Timeliness of Childhood Vaccinations in Kampala Uganda: A Community-Based Cross-Sectional Study. PLoS ONE 2012, 7, e35432. [Google Scholar] [CrossRef]
- Schoeps, A.; Ouedraogo, N.; Kagone, M.; Sié, A.; Muller, O.; Becher, H. Socio-demographic determinants of timely adherence to BCG, Penta3, measles, and complete vaccination schedule in Burkina Faso. Vaccine 2013, 32, 96–102. [Google Scholar] [CrossRef] [PubMed]
- Waroux, O.L.P.D.; Schellenberg, J.R.A.; Manzi, F.; Mrisho, M.; Shirima, K.; Mshinda, H.; Alonso, P.; Tanner, M. Timeliness and completeness of vaccination and risk factors for low and late vaccine uptake in young children living in rural southern Tanzania. Int. Heal. 2013, 5, 139–147. [Google Scholar] [CrossRef] [PubMed]
- Calhoun, L.M.; van Eijk, A.M.; Lindblade, K.A.; Odhiambo, F.O.; Wilson, M.L.; Winterbauer, E.; Slutsker, L.; Hamel, M.J. Determinants and Coverage of Vaccination in Children in Western Kenya from a 2003 Cross-Sectional Survey. Am. J. Trop. Med. Hyg. 2014, 90, 234–241. [Google Scholar] [CrossRef][Green Version]
- Gram, L.; Soremekun, S.; Asbroek, A.T.; Manu, A.; O’Leary, M.; Hill, Z.; Danso, S.; Amenga-Etego, S.; Owusu-Agyei, S.; Kirkwood, B.R. Socio-economic determinants and inequities in coverage and timeliness of early childhood immunisation in rural Ghana. Trop. Med. Int. Heal. 2014, 19, 802–811. [Google Scholar] [CrossRef]
- Laryea, D.O.; Parbie, E.A.; Frimpong, E. Timeliness of childhood vaccine uptake among children attending a tertiary health service facility-based immunisation clinic in Ghana. BMC Public Heal. 2014, 14, 90. [Google Scholar] [CrossRef] [PubMed]
- Sadoh, A.E.; Ofili, A. Hepatitis B infection among Nigerian children admitted to a children’s emergency room. Afr. Heal. Sci. 2014, 14, 377–383. [Google Scholar] [CrossRef][Green Version]
- Thysen, S.M.; Byberg, S.; Pedersen, M.; Rodrigues, A.; Ravn, H.; Martins, C.; Benn, C.S.; Aaby, P.; Fisker, A.B. BCG coverage and barriers to BCG vaccination in Guinea-Bissau: An observational study. BMC Public Heal. 2014, 14, 1037. [Google Scholar] [CrossRef]
- Odutola, A.; Afolabi, M.; Ogundare, E.O.; Lowe-Jallow, Y.N.; Worwui, A.; Okebe, J.; Ota, M. Risk factors for delay in age-appropriate vaccinations among Gambian children. BMC Heal. Serv. Res. 2015, 15, 346. [Google Scholar] [CrossRef] [PubMed]
- Lutwama, F.; Kagina, B.M.; Wajja, A.; Waiswa, F.; Mansoor, N.; Kirimunda, S.; Hughes, E.J.; Kiwanuka, N.; Joloba, M.; Musoke, P.; et al. Distinct T-Cell Responses When BCG Vaccination Is Delayed From Birth to 6 Weeks of Age in Ugandan Infants. J. Infect. Dis. 2013, 209, 887–897. [Google Scholar] [CrossRef] [PubMed]
- Gibson, D.G.; Ochieng, B.; Kagucia, E.W.; Obor, D.; Odhiambo, F.; O’Brien, K.L.; Feikin, D.R. Individual level determinants for not receiving immunization, receiving immunization with delay, and being severely underimmunized among rural western Kenyan children. Vaccine 2015, 33, 6778–6785. [Google Scholar] [CrossRef]
- Miyahara, R.; Jasseh, M.; Gomez, P.; Shimakawa, Y.; Greenwood, B.; Keita, K.; Ceesay, S.; D’Alessandro, U.; Roca, A. Barriers to timely administration of birth dose vaccines in The Gambia, West Africa. Vaccine 2016, 34, 3335–3341. [Google Scholar] [CrossRef]
- O’Leary, M.; Edmond, K.; Floyd, S.; Hurt, L.; Shannon, C.; Thomas, G.; Newton, S.; Kirkwood, B.; Thomas, S. Neonatal vaccination of low birthweight infants in Ghana. Arch. Dis. Child. 2016, 102, 145–151. [Google Scholar] [CrossRef]
- Gibson, D.G.; Ochieng, B.; Kagucia, E.W.; Were, J.; Hayford, K.; Moulton, L.H.; Levine, O.S.; Odhiambo, F.; O’Brien, K.L.; Feikin, D.R. Mobile phone-delivered reminders and incentives to improve childhood immunisation coverage and timeliness in Kenya (M-SIMU): A cluster randomised controlled trial. Lancet Glob. Heal. 2017, 5, e428–e438. [Google Scholar] [CrossRef]
- Schweitzer, A.; Akmatov, M.K.; Krause, G. Hepatitis B vaccination timing: Results from demographic health surveys in 47 countries. Bull. World Heal. Organ. 2017, 95, 199–209. [Google Scholar] [CrossRef] [PubMed]
- Zivich, P.N.; Kiketa, L.; Kawende, B.; Lapika, B.; Yotebieng, M. Vaccination Coverage and Timelines Among Children 0–6 Months in Kinshasa, the Democratic Republic of Congo: A Prospective Cohort Study. Matern. Child Heal. J. 2017, 21, 1055–1064. [Google Scholar] [CrossRef]
- Schoub, B.D.; Johnson, S.; McAnerney, J.M.; Blackburn, N.; Kew, M.C.; McCutcheon, J.P.; Carlier, N.D. Integration of hepatitis B vaccination into rural African primary health care programmes. BMJ 1991, 302, 313–316. [Google Scholar] [CrossRef] [PubMed][Green Version]
- Sadoh, A.E.; Eregie, C. Age at presentation for infant immunization in Nigeria: Implications for hepatitis B immunization. Public Heal. 2008, 122, 1318–1320. [Google Scholar] [CrossRef] [PubMed]
- Sadoh, A.E.; Eregie, C.O. Timeliness and Completion Rate of Immunization among Nigerian Children Attending a Clinic-based Immunization Service. J. Heal. Popul. Nutr. 2009, 27, 391–395. [Google Scholar] [CrossRef]
- Olusanya, B.O. Pattern and determinants of BCG immunisation delays in a sub-Saharan African community. Heal. Res. Policy Syst. 2010, 8, 1. [Google Scholar] [CrossRef] [PubMed]
- E Sadoh, A.; E Sadoh, W.; Uduebor, J.; Ekpebe, P.; Iguodala, O. Factors contributing to delay in commencement of immunisation in Nigerian infants. Tanzan J. Health Res. 2013, 15, 1–8. [Google Scholar] [CrossRef] [PubMed][Green Version]
- Borus, P.K. Missed opportunities and inappropriately given vaccines reduce immunisation coverage in facilities that serve slum areas of Nairobi. East Afr. Med. J. 2004, 81, 124–129. [Google Scholar] [CrossRef] [PubMed][Green Version]
- Kidanne, L.; Bisrat, F.; Dinku, B.; Lynch, M.; Fantahun, M. Newborn tracking for polio birth dose vaccination in pastoralist and semi-pastoralist CORE Group Polio Project implementation districts (woredas) in Ethiopia. Ethiop. Med. J. 2013, 51, 1–12. [Google Scholar] [PubMed]
- Hoest, C.; Seidman, J.C.; Lee, G.; A Platts-Mills, J.; Ali, A.; Olortegui, M.P.; Bessong, P.O.; Chandyo, R.; Babji, S.; Mohan, V.R.; et al. Vaccine coverage and adherence to EPI schedules in eight resource poor settings in the MAL-ED cohort study. Vaccine 2016, 35, 443–451. [Google Scholar] [CrossRef] [PubMed]
- Shimakawa, Y.; Yan, H.-J.; Tsuchiya, N.; Bottomley, C.; Hall, A.J. Association of Early Age at Establishment of Chronic Hepatitis B Infection with Persistent Viral Replication, Liver Cirrhosis and Hepatocellular Carcinoma: A Systematic Review. PLoS ONE 2013, 8, e69430. [Google Scholar] [CrossRef]
- Shimakawa, Y.; Lemoine, M.; Njai, H.F.; Bottomley, C.; Ndow, G.; Goldin, R.D.; Jatta, A.; Jeng-Barry, A.; Wegmüller, R.; Moore, S.E.; et al. Natural history of chronic HBV infection in West Africa: A longitudinal population-based study from The Gambia. Gut 2015, 65, 2007–2016. [Google Scholar] [CrossRef] [PubMed]
- Nayagam, S.; Shimakawa, Y.; Lemoine, M. Mother-to-child transmission of hepatitis B: What more needs to be done to eliminate it around the world? J. Viral Hepat. 2020, 27, 342–349. [Google Scholar] [CrossRef] [PubMed]
- A Guerra, F.; Guerra, F.A. Delays in Immunization Have Potentially Serious Health Consequences. Pediatr. Drugs 2007, 9, 143–148. [Google Scholar] [CrossRef] [PubMed]
- Moturi, E.; Tevi-Benissan, C.; Hagan, J.; Shendale, S.; Mayenga, D.; Murokora, D.; Patel, M.; Hennessey, K.; Mihigo, R. Implementing a Birth Dose of Hepatitis B Vaccine in Africa: Findings from Assessments in 5 Countries. J. Immunol. Sci. 2018, 2, 31–40. [Google Scholar] [CrossRef]
- UNICEF. Global Delivery Care Coverage and Treands. Percentage of Births Assisted by a Skilled Birth Attendant, by Country, 2014–2019. [Internet]. 2020. Available online: https://data.unicef.org/topic/maternal-health/delivery-care/ (accessed on 29 March 2020).
- Allison, R.D.; Patel, M.K.; Tohme, R.A. Hepatitis B vaccine birth dose coverage correlates worldwide with rates of institutional deliveries and skilled attendance at birth. Vaccine 2017, 35, 4094–4098. [Google Scholar] [CrossRef]
- Scott, N.; Palmer, A.; Morgan, C.; Lesi, O.; Spearman, C.W.; Sonderup, M.; E Hellard, M. Cost-effectiveness of the controlled temperature chain for the hepatitis B virus birth dose vaccine in various global settings: A modelling study. Lancet Glob. Heal. 2018, 6, e659–e667. [Google Scholar] [CrossRef]
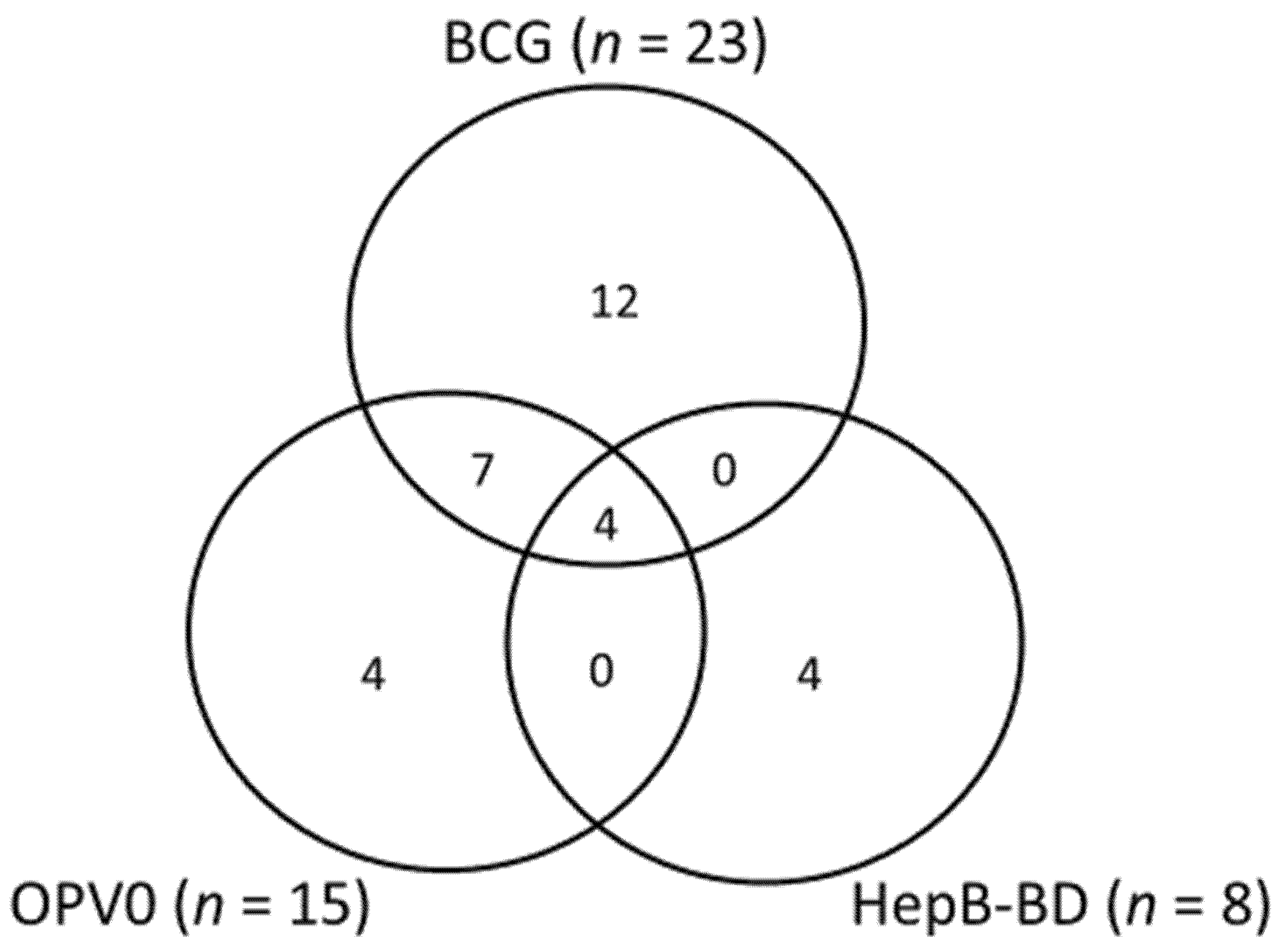
| Author, Year, Reference | Country | Study Design | Study Setting | % Ascertained | Vaccine Assessed | Time Points Assessed (days) | Total No. of Infants Assessed |
|---|---|---|---|---|---|---|---|
| Studies using vaccination cards only | |||||||
| Coetzee, 1993 [20] | South Africa | Cross-sectional | Population | 88.0% | BCG | 28 | 421 |
| Roth, 2004 [21] | Guinea Bissau | Retrospective cohort | Hospital | 84.2% | BCG | 7 | 7138 |
| Jahn, 2008 [22] | Malawi | Cross-sectional | Population | 78.0% | BCG | 7 | 2751 |
| Moisi, 2010 [23] | Kenya | Cross-sectional | Population | 86.2% | BCG, OPV0 | 14/28 | 1870 |
| Fadnes, 2011 [24] | Uganda | Prospective cohort | Hospital | 98.0% | OPV0 | 28 | 732 |
| Adebayo, 2012 [25] | Nigeria | Cross-sectional | Population | N/R | BCG, OPV0, HepB-BD | 7 | 440 |
| Babirye, 2012 [26] | Uganda | Cross-sectional | Population | 91.2% | OPV0 | 28 | 821 |
| Schoeps, 2013 [27] | Burkina Faso | Cross-sectional | Population | N/R | BCG, OPV0 | 28 | 1665 |
| Waroux, 2013 [28] | Tanzania | Cross-sectional | Population | 59.0% | BCG | 7 | 1205 |
| Calhoun, 2014 [29] | Kenya | Retrospective cohort | Population | 55.3% | BCG, OPV0 | 7/28 | 135 |
| Gram, 2014 [30] | Ghana | Prospective cohort | Population | N/R | BCG, OPV0 | 7/14/28 | 20,594 |
| Laryea, 2014 [31] | Ghana | Cross-sectional | Hospital | N/R | BCG, OPV0 | 14/28 | 259 |
| Sadoh, 2014 [32] | Nigeria | Cross-sectional | Hospital | 27.3% | BCG, OPV0, HepB-BD | 7/14/28 | 41 |
| Thysen, 2014 [33] | Guinea Bissau | Cross-sectional | Population | 85.0% | BCG | 7/28 | 3020 |
| Wagner, 2014 [19] | Sub-Saharan Africa * | Cross-sectional | Population | N/R | BCG | 28 | 102,629 |
| Odutola, 2015 [34] | The Gambia | Cross-sectional | Hospital | N/R | BCG | 14 | 1154 |
| Lutwama 2014 [35] | Uganda | Cross-sectional | Hospital | N/R | BCG | 0–1 | 92 |
| Gibson, 2015 [36] | Kenya | Cross-sectional | Population | 63.9% | BCG | 28 | 1681 |
| Miyahara, 2016 [37] | The Gambia | Cross-sectional | Population | 99.8% | HepB-BD | 0–1/7/28 | 10,851 |
| O’Leary, 2017 [38] | Ghana | Prospective cohort | Population | 96.5% | BCG | 28 | 22,217 |
| Gibson, 2017 [39] | Kenya | Prospective cohort | Population | N/R | BCG | 14 | 360 |
| Schweitzer, 2017 [40] | Nigeria | Cross-sectional | Population | N/R | HepB-BD | 0–1 | 14,623 |
| Zivich, 2017 [41] | Congo | Prospective cohort | Hospital | 93.5% | BCG, OPV0 | 7 | 975 |
| Studies using clinical records only | |||||||
| Schoub, 1991 [42] | South Africa | Prospective cohort | Hospital | N/R | HepB-BD | 14 | 863 |
| Sadoh, 2008 [43] | Nigeria | Retrospective cohort | Hospital | N/R | HepB-BD | 0–1/7/14/ 28 | 512 |
| Sadoh, 2009 [44] | Nigeria | Retrospective cohort | Population | N/R | BCG, OPV0, HepB-BD | 14/28 | 493 |
| Olusanya, 2010 [45] | Nigeria | Cross-sectional | Hospital | 68.9% | BCG | 14 | 5171 |
| Sadoh, 2013 [46] | Nigeria | Cross-sectional | Hospital | N/R | BCG, OPV0, HepB-BD | 0–1/7/14/ 28 | 153 |
| Studies using both vaccination cards and clinical records | |||||||
| Borus, 2004 [47] | Kenya | Cross-sectional | Hospital | N/R | OPV0 | 14 | 392 |
| Kidane, 2013 [48] | Ethiopia | Cross-sectional | Population | N/R | OPV0 | 14 | 600 |
| Hoest, 2017 [49] | South Africa and Tanzania | Prospective cohort | Population | N/R | BCG, OPV0 | 7 | 253 |
© 2020 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Bassoum, O.; Kimura, M.; Tal Dia, A.; Lemoine, M.; Shimakawa, Y. Coverage and Timeliness of Birth Dose Vaccination in Sub-Saharan Africa: A Systematic Review and Meta-Analysis. Vaccines 2020, 8, 301. https://doi.org/10.3390/vaccines8020301
Bassoum O, Kimura M, Tal Dia A, Lemoine M, Shimakawa Y. Coverage and Timeliness of Birth Dose Vaccination in Sub-Saharan Africa: A Systematic Review and Meta-Analysis. Vaccines. 2020; 8(2):301. https://doi.org/10.3390/vaccines8020301
Chicago/Turabian StyleBassoum, Oumar, Moe Kimura, Anta Tal Dia, Maud Lemoine, and Yusuke Shimakawa. 2020. "Coverage and Timeliness of Birth Dose Vaccination in Sub-Saharan Africa: A Systematic Review and Meta-Analysis" Vaccines 8, no. 2: 301. https://doi.org/10.3390/vaccines8020301
APA StyleBassoum, O., Kimura, M., Tal Dia, A., Lemoine, M., & Shimakawa, Y. (2020). Coverage and Timeliness of Birth Dose Vaccination in Sub-Saharan Africa: A Systematic Review and Meta-Analysis. Vaccines, 8(2), 301. https://doi.org/10.3390/vaccines8020301





