Pediatric Traumatic Brain Injury in the United States: Rural-Urban Disparities and Considerations
Abstract
1. Introduction
2. Methods
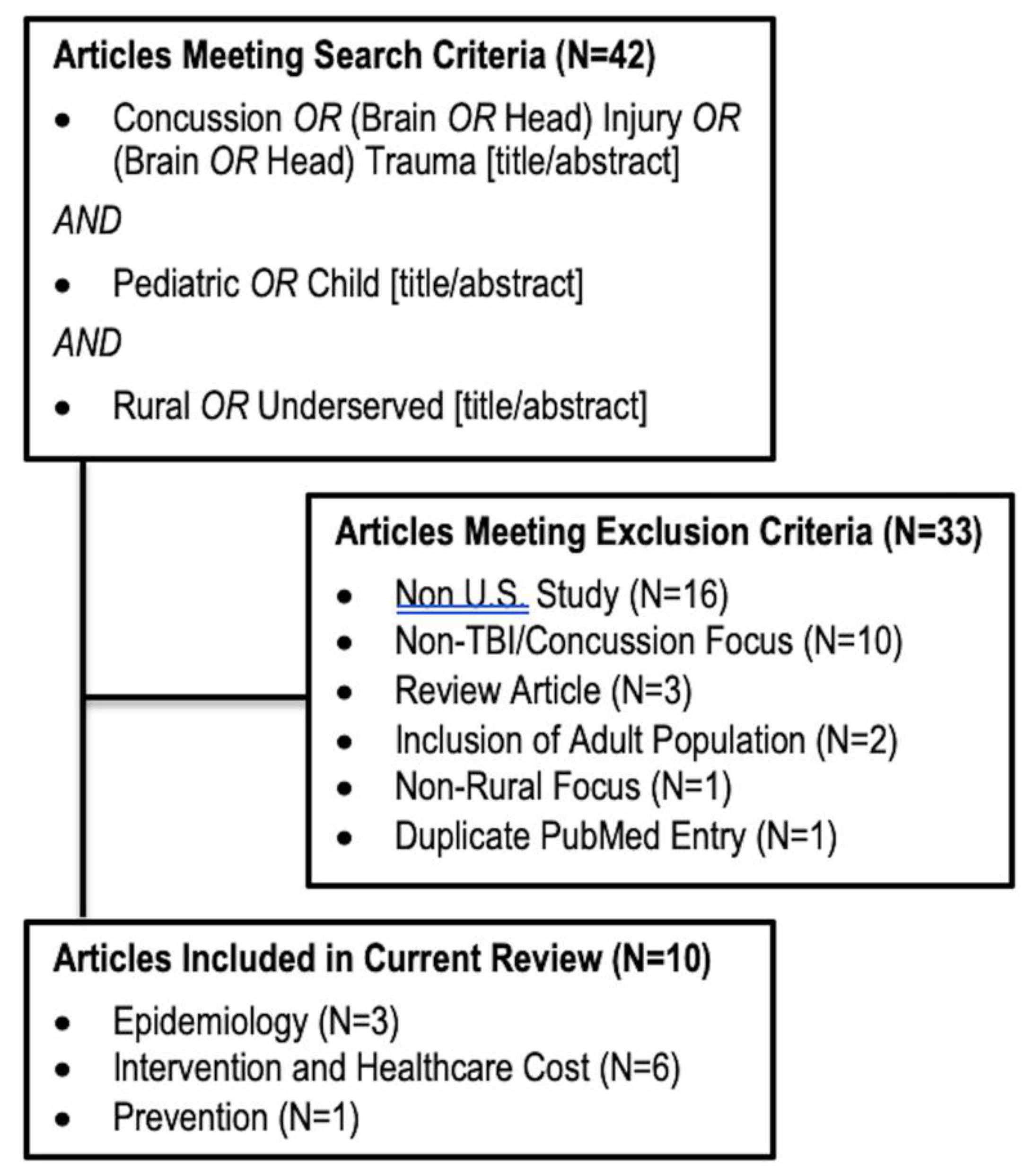
2.1. Study Selection
2.2. Study Analyses
3. Results
3.1. Epidemiology
3.1.1. Oregon Trauma Registry Study
3.1.2. Pediatric Health Information System Study
3.1.3. Minnesota Olmsted County Skull Fracture Study
3.2. Intervention and Healthcare Cost
3.2.1. MarketScan Insurance Claims Study: Utilization of Healthcare Services and Cost in Mild TBI
3.2.2. North Dakota Emergency Medical Services Study: Suboptimal Triage to Care Facility in Moderate to Severe TBI
3.2.3. Utah Trauma Performance Measures Study: Predictors of Suboptimal Triage and Transfer in Severe Trauma
3.2.4. Iowa Emergency Department Transfer Study: Potentially Avoidable ED Transfers in TBI
3.2.5. Texas Urban vs. Rural Designation Study: Injury Severity and Outcomes in Severe TBI
3.2.6. Oregon Parental Focus Group Study: Survivor Impact after Neurocritical Care
3.2.7. Georgia Bicycle Helmet Study: Pre- and Post-Mandate Adherence
3.3. Included Studies
4. Discussion
4.1. Epidemiology
4.2. Intervention and Healthcare Cost
4.3. Prevention
4.4. Limitations
5. Conclusions
Author Contributions
Conflicts of Interest
References
- Feigin, V.L.; Theadom, A.; Barker-Collo, S.; Starkey, N.J.; McPherson, K.; Kahan, M.; Dowell, A.; Brown, P.; Parag, V.; Kydd, R.; et al. Incidence of traumatic brain injury in New Zealand: a population-based study. Lancet Neurol. 2013, 12, 53–64. [Google Scholar] [CrossRef]
- Cuthbert, J.P.; Harrison-Felix, C.; Corrigan, J.D.; Kreider, S.; Bell, J.M.; Coronado, V.G.; Whiteneck, G.G. Epidemiology of adults receiving acute inpatient rehabilitation for a primary diagnosis of traumatic brain injury in the United States. J. Head Trauma Rehabil. 2015, 30, 122–135. [Google Scholar] [CrossRef] [PubMed]
- Hyder, A.A.; Wunderlich, C.A.; Puvanachandra, P.; Gururaj, G.; Kobusingye, O.C. The impact of traumatic brain injuries: a global perspective. NeuroRehabilitation 2007, 22, 341–353. [Google Scholar] [CrossRef] [PubMed]
- Chen, C.; Peng, J.; Sribnick, E.A.; Zhu, M.; Xiang, H. Trend of Age-Adjusted Rates of Pediatric Traumatic Brain Injury in U.S. Emergency Departments from 2006 to 2013. Int. J. Environ. Res. Public Health 2018, 15, 1171. [Google Scholar] [CrossRef]
- Leading Causes of Death Reports, National and Regional, 1999–2013. Available online: http://webappa.cdc.gov/cgi-bin/broker.exe (accessed on 31 October 2019).
- Cnossen, M.C.; Winkler, E.A.; Yue, J.K.; Okonkwo, D.O.; Valadka, A.; Steyerberg, E.W.; Lingsma, H.; Manley, G.T. Development of a Prediction Model for Post-Concussive Symptoms following Mild Traumatic Brain Injury: A TRACK-TBI Pilot Study. J. Neurotrauma 2017, 34, 2396–2409. [Google Scholar] [CrossRef]
- McMahon, P.; Hricik, A.; Yue, J.K.; Puccio, A.M.; Inoue, T.; Lingsma, H.F.; Beers, S.R.; Gordon, W.A.; Valadka, A.B.; Manley, G.T.; et al. Symptomatology and functional outcome in mild traumatic brain injury: results from the prospective TRACK-TBI study. J. Neurotrauma 2014, 31, 26–33. [Google Scholar] [CrossRef]
- Johnstone, B.; Price, T.; Bounds, T.; Schopp, L.H.; Schootman, M.; Schumate, D. Rural/urban differences in vocational outcomes for state vocational rehabilitation clients with TBI. NeuroRehabilitation 2003, 18, 197–203. [Google Scholar] [CrossRef]
- Beedasy, J. Rural Designations and Geographic Access to Tertiary Healthcare in Idaho. Online J. Rural Res. Policy 2010, 5. Available online: https://doi.org/10.4148/ojrrp.v5i2.191 (accessed on 31 October 2019). [CrossRef]
- Chan, L.; Hart, L.G.; Goodman, D.C. Geographic access to health care for rural Medicare beneficiaries. J. Rural Health 2006, 22, 140–146. [Google Scholar] [CrossRef]
- Byrne, R.W.; Bagan, B.T.; Slavin, K.V.; Curry, D.; Koski, T.R.; Origitano, T.C. Neurosurgical emergency transfers to academic centers in Cook County: a prospective multicenter study. Neurosurgery 2008, 62, 709–716. [Google Scholar] [CrossRef]
- Ewbank, C.; Sheckter, C.C.; Warstadt, N.M.; Pirrotta, E.A.; Curtin, C.; Newton, C.; Wang, N.E. Variations in access to specialty care for children with severe burns. Am. J. Emerg. Med. 2019, 158401. [Google Scholar] [CrossRef] [PubMed]
- Upadhyayula, P.S.; Yue, J.K.; Yang, J.; Birk, H.S.; Ciacci, J.D. The Current State of Rural Neurosurgical Practice: An International Perspective. J. Neurosci. Rural Pract. 2018, 9, 123. [Google Scholar] [CrossRef] [PubMed]
- Yue, J.K.; Rick, J.W.; Morrissey, M.R.; Taylor, S.R.; Deng, H.; Suen, C.G.; Vassar, M.J.; Cnossen, M.C.; Lingsma, H.F.; Yuh, E.L.; et al. Preinjury employment status as a risk factor for symptomatology and disability in mild traumatic brain injury: A TRACK-TBI analysis. NeuroRehabilitation 2018, 43, 169–182. [Google Scholar] [CrossRef] [PubMed]
- Yue, J.K.; Winkler, E.A.; Sharma, S.; Vassar, M.J.; Ratcliff, J.J.; Korley, F.K.; Seabury, S.A.; Ferguson, A.R.; Lingsma, H.F.; Deng, H.; et al. Temporal profile of care following mild traumatic brain injury: predictors of hospital admission, follow-up referral and six-month outcome. Brain Inj. 2017, 31, 1820–1829. [Google Scholar] [CrossRef] [PubMed]
- Leonhard, M.J.; Wright, D.A.; Fu, R.; Lehrfeld, D.P.; Carlson, K.F. Urban/Rural disparities in Oregon pediatric traumatic brain injury. Inj Epidemiol 2015, 2, 32. [Google Scholar] [CrossRef]
- Stewart, T.C.; Gilliland, J.; Fraser, D.D. An epidemiologic profile of pediatric concussions: identifying urban and rural differences. J. Trauma Acute Care Surg. 2014, 76, 736–742. [Google Scholar] [CrossRef]
- Loftus, K.V.; Rhine, T.; Wade, S.L.; Pomerantz, W.J. Characterization of children hospitalized with traumatic brain injuries after building falls. Inj Epidemiol 2018, 5, 15. [Google Scholar] [CrossRef]
- Nelson, E.L.; Melton, L.J., 3rd; Annegers, J.F.; Laws, E.R.; Offord, K.P. Incidence of skull fractures in Olmsted County, Minnesota. Neurosurgery 1984, 15, 318–324. [Google Scholar] [CrossRef]
- Graves, J.M.; Mackelprang, J.L.; Moore, M.; Abshire, D.A.; Rivara, F.P.; Jimenez, N.; Fuentes, M.; Vavilala, M.S. Rural-urban disparities in health care costs and health service utilization following pediatric mild traumatic brain injury. Health Serv. Res. 2019, 54, 337–345. [Google Scholar] [CrossRef]
- Poltavski, D.; Muus, K. Factors associated with incidence of “inappropriate” ambulance transport in rural areas in cases of moderate to severe head injury in children. J. Rural Health 2005, 21, 272–277. [Google Scholar] [CrossRef]
- Gleich, S.J.; Bennett, T.D.; Bratton, S.L.; Larsen, G.Y. Pediatric trauma transport performance measures in a mountain state: adherence and outcomes. J. Trauma 2011, 71, 1016–1022. [Google Scholar] [CrossRef] [PubMed]
- Mohr, N.M.; Harland, K.K.; Shane, D.M.; Miller, S.L.; Torner, J.C. Potentially Avoidable Pediatric Interfacility Transfer Is a Costly Burden for Rural Families: A Cohort Study. Acad. Emerg. Med. 2016, 23, 885–894. [Google Scholar] [CrossRef] [PubMed]
- Robertson, B.D.; McConnel, C.E. Town-level comparisons may be an effective alternative in comparing rural and urban differences: a look at accidental traumatic brain injuries in North Texas children. Rural Remote Health 2011, 11, 1521. [Google Scholar] [PubMed]
- Williams, C.N.; Eriksson, C.; Piantino, J.; Hall, T.; Moyer, D.; Kirby, A.; McEvoy, C. Long-term Sequelae of Pediatric Neurocritical Care: The Parent Perspective. Pediatr. Crit. Care Med. 2018, 7, 173–181. [Google Scholar]
- Sacks, J.J.; Kresnow, M.; Houston, B.; Russell, J. Bicycle helmet use among American children, 1994. Inj. Prev. 1996, 2, 258–262. [Google Scholar] [CrossRef]
- Gilchrist, J.; Schieber, R.A.; Leadbetter, S.; Davidson, S.C. Police enforcement as part of a comprehensive bicycle helmet program. Pediatrics 2000, 106, 6–9. [Google Scholar] [CrossRef]
- McCauley, S.R.; Wilde, E.A.; Anderson, V.A.; Bedell, G.; Beers, S.R.; Campbell, T.F.; Chapman, S.B.; Ewing-Cobbs, L.; Gerring, J.P.; Gioia, G.A.; et al. Recommendations for the use of common outcome measures in pediatric traumatic brain injury research. J. Neurotrauma 2012, 29, 678–705. [Google Scholar] [CrossRef]
- Bell, M.J.; Kochanek, P.M. Pediatric traumatic brain injury in 2012: the year with new guidelines and common data elements. Crit. Care Clin. 2013, 29, 223–238. [Google Scholar] [CrossRef]
- Stein, M.B.; Jain, S.; Giacino, J.T.; Levin, H.; Dikmen, S.; Nelson, L.D.; Vassar, M.J.; Okonkwo, D.O.; Diaz-Arrastia, R.; Robertson, C.S.; et al. Risk of Posttraumatic Stress Disorder and Major Depression in Civilian Patients After Mild Traumatic Brain Injury: A TRACK-TBI Study. JAMA Psychiatry 2019, 76, 249–258. [Google Scholar] [CrossRef]
- De Koning, M.E.; Scheenen, M.E.; Van Der Horn, H.J.; Spikman, J.M.; Van Der Naalt, J. From “miserable minority” to the “fortunate few”: the other end of the mild traumatic brain injury spectrum. Brain Inj. 2018, 32, 540–543. [Google Scholar] [CrossRef]
- Boake, C.; McCauley, S.R.; Pedroza, C.; Levin, H.S.; Brown, S.A.; Brundage, S.I. Lost productive work time after mild to moderate traumatic brain injury with and without hospitalization. Neurosurgery 2005, 56, 994–1003. [Google Scholar] [PubMed]
- de Koning, M.E.; Scheenen, M.E.; van der Horn, H.J.; Hageman, G.; Roks, G.; Spikman, J.M.; van der Naalt, J. Non-Hospitalized Patients with Mild Traumatic Brain Injury: The Forgotten Minority. J. Neurotrauma 2017, 34, 257–261. [Google Scholar] [CrossRef] [PubMed]
| Epidemiological Studies | ||||
| Author | Study Type | Description | Results | Conclusions |
| Leonhard et al. 2015 | Retrospective cohort study | 2794 pediatric TBI cases in rural vs. metropolitan areas abstracted from Oregon Trauma Registry 2009–2012. | Rural children had higher annualized rates of TBI incidence than metropolitan children (107 vs. 71 per 100,000) and a 2-fold increase in odds of mortality following TBI (OR 1.8, 1.04–3.3) adjusting for demographic factors. | Rural patients have greater TBI incidence and worse outcomes. Missing data is a pervasive problem for rural cases. |
| Loftus et al. 2010 | Retrospective cohort study | 23,813 pediatric hospitalization abstracted from Pediatric Health Information systems between 2009–2014. | Rural children sustaining building falls were more likely to have serious/severe TBI compared to urban children (58.9% vs. 53.6%; p < 0.01) | Rural children sustaining TBI due to falls sustain more severe injuries than urban children. |
| Nelson et al. 1984 | Retrospective cohort study | 3598 head trauma cases reported from rural Olmsted County, Minnesota | Higher incidence of TBI caused by MVA (39% vs. 26%) or occupational injury (8% vs. 4%) as compared to Urban Rochester MN. Younger patients (ages 0–5) had greater incidence of concomitant fracture with TBI. | Younger children were more likely to suffer complex TBI. MVA and occupational injuries are the most prominent mechanisms of injury. |
| Intervention and Healthcare Cost | ||||
| Author | Study Type | Description | Results | Conclusions |
| Gleich et al. 2011 | Retrospective cohort study | 412 patients abstracted from Primary Children’s Medical Center (PCMC) database from 2006 to 2009. | 50% of pediatric TBI cases were transferred and triaged from original hospital in <2 h. Factors associated with delayed triage included: less severe head injury, greater distance from hospital, primary chest/abdominal injuries. Outcomes did not differ between patients transferred <2 h and those transferred >2 h. | Patients sustaining severe head injuries were more likely to be transferred within the 2-hour practice guideline. The effect this has on outcomes is unclear. |
| Graves et al. 2019 | Retrospective cohort study | 387,846 mild TBI cases abstracted from MarketScan Commercial Claims and Encounters Data 2007–2011 | Healthcare costs for pediatric mild TBI was $2778 for rural patients and $2499 for urban patients (p < 0.01). Urban children utilized more speech therapy and mental health services than rural children. Rural children utilized more PT/OT. | TBI costs are greater for rural patients. Rural patients use of more PT/OT services but less mental health and speech therapy services requires further examination. |
| Mohr et al. 2016 | Retrospective cohort study | 2,117,317 rural pediatric ED admissions between 2004–2013 were assessed for potentially avoidable transfers. | Isolated traumatic brain injury without extra-axial bleeding was frequently identified as a potentially avoidable transfer and incurred an additional cost of $1455 to patients. | Creating best practice guidelines can minimize cost to patient and the healthcare system while maintaining or improving outcomes. |
| Poltavski et al. 2005 | Retrospective cohort study | 156 cases of pediatric head injuries with GCS ≤ 12 in North Dakota from 1995 to 2000. | Mistriage, defined as transportation of pediatric patients with moderate to severe TBI to a non-trauma center occurred more frequently in winter and if the child was Native American. Distance to trauma center and shorter distance to receiving facility also corresponded with rates of mistriage. | Distance and race are two key issues that should be addressed in policy aimed at optimizing triage of pediatric TBI patients. |
| Robertson et al. 2011 | Retrospective cohort study | 444 patients treated at Children’s Medical Center Dallas classified into urban city, large town, small town, or isolated town based off of commuting area codes | Isolated town TBI patients had higher injury severity scores (ISS; 17 vs. 15), and longer hospital stays (7 vs. 5 days) than urban city patients. | Rural pediatric TBI are generally more severe than urban areas. |
| Williams et al. 2018 | Focus group study | 16 parent caretakers of pediatric patients with TBI or other neurologic insults assessed in 4 focus group sessions. | Pediatric neurocritical care has an immense and long-lasting effect on families and survivors. 89% of patients require ongoing medical attention, 33% require psychological counseling and 56% require at-school aid. Rural settings have limited resources compounding financial burdens for families. | Outcome optimization for pediatric TBI patients requires long-term support for survivors and their families |
| Prevention | ||||
| Author | Study Type | Description | Results | Conclusions |
| Gilchrist et al. 2000 | Prospective observational study | In April 1997, 580 students from kindergarten to 7th grade received bicycle helmets and education and were observationally followed. | Observed helmet use rose from 0% pre-intervention to 45% post-intervention. Police impounded bikes of helmetless riders. Two-years after study initiation helmet use was observed at 54% | Education and enforcement can create behavioral changes that can mitigate pediatric TBI. |
© 2020 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Yue, J.K.; Upadhyayula, P.S.; Avalos, L.N.; Cage, T.A. Pediatric Traumatic Brain Injury in the United States: Rural-Urban Disparities and Considerations. Brain Sci. 2020, 10, 135. https://doi.org/10.3390/brainsci10030135
Yue JK, Upadhyayula PS, Avalos LN, Cage TA. Pediatric Traumatic Brain Injury in the United States: Rural-Urban Disparities and Considerations. Brain Sciences. 2020; 10(3):135. https://doi.org/10.3390/brainsci10030135
Chicago/Turabian StyleYue, John K., Pavan S. Upadhyayula, Lauro N. Avalos, and Tene A. Cage. 2020. "Pediatric Traumatic Brain Injury in the United States: Rural-Urban Disparities and Considerations" Brain Sciences 10, no. 3: 135. https://doi.org/10.3390/brainsci10030135
APA StyleYue, J. K., Upadhyayula, P. S., Avalos, L. N., & Cage, T. A. (2020). Pediatric Traumatic Brain Injury in the United States: Rural-Urban Disparities and Considerations. Brain Sciences, 10(3), 135. https://doi.org/10.3390/brainsci10030135






