Comparison of Intensity- and Polarization-based Contrast in Amyloid-beta Plaques as Observed by Optical Coherence Tomography
Abstract
:Featured Application
Abstract
1. Introduction
2. Materials and Methods
2.1. Brain Samples
2.2. OCT and Data Acquisition
2.3. Histology
2.4. Data Processing and Statistical Analysis
3. Results
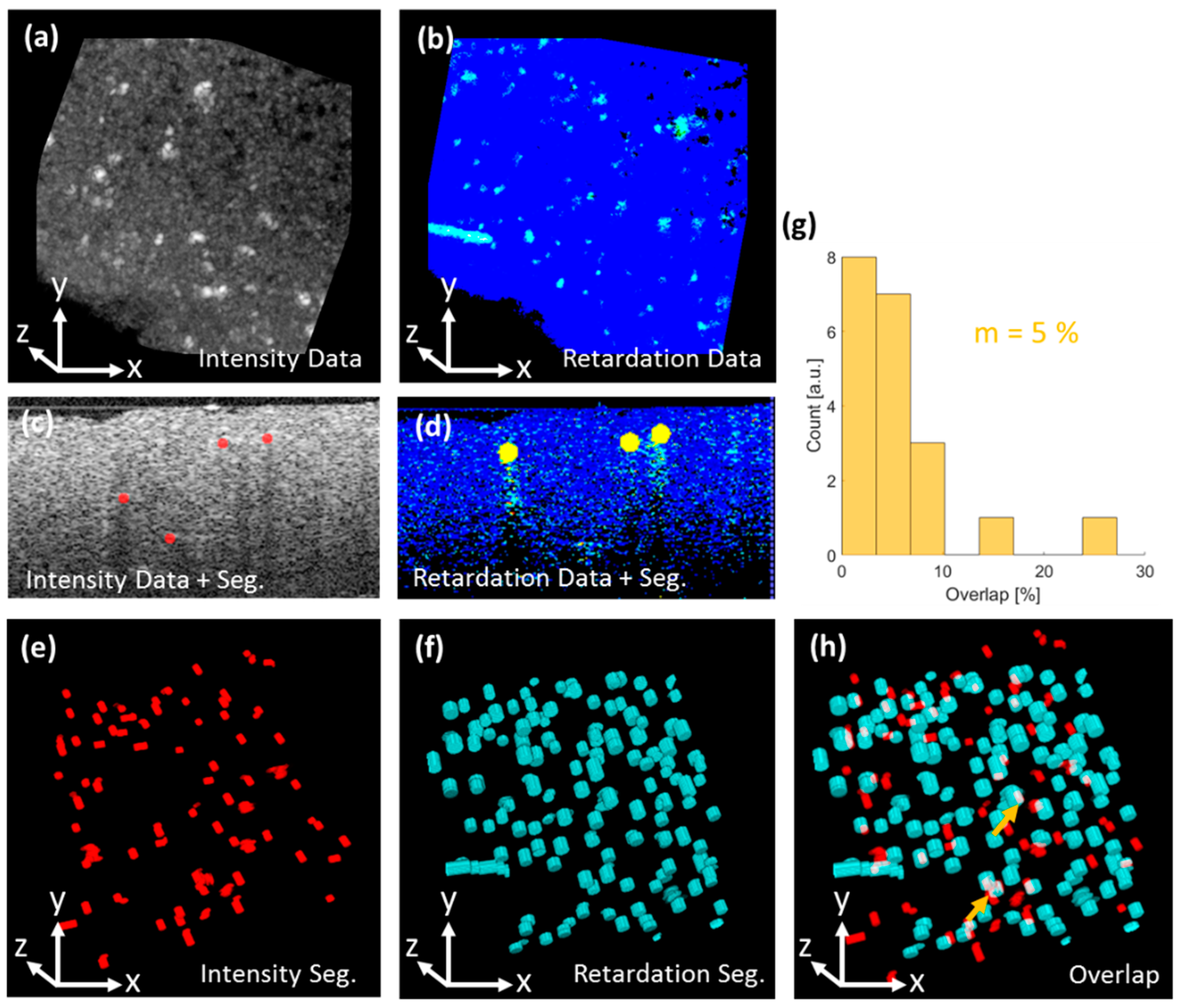
3.1. Appearance of Plaques in Intensity and Retardation OCT Images
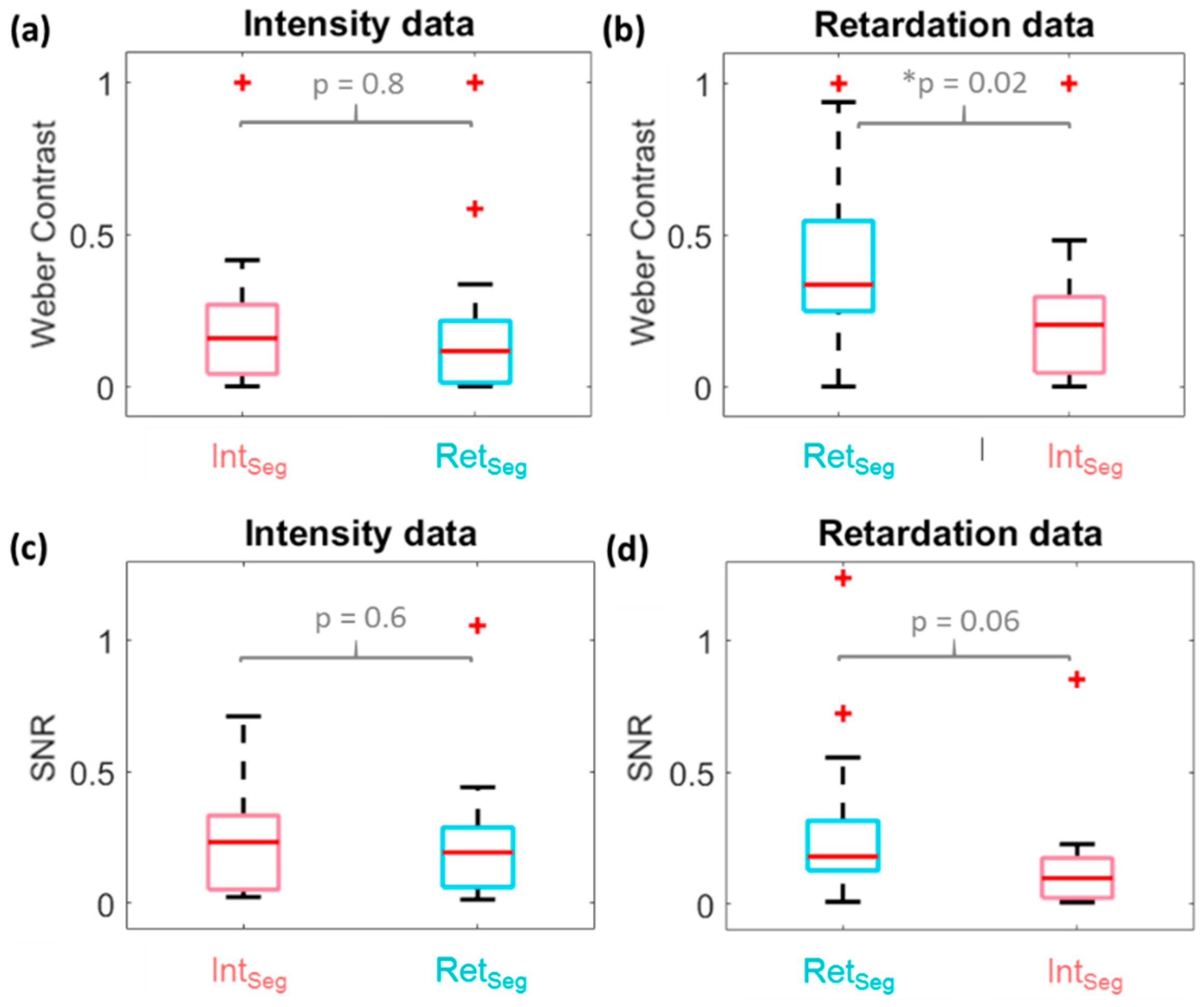
3.2. Comparison of Segmentation and Image Contrast
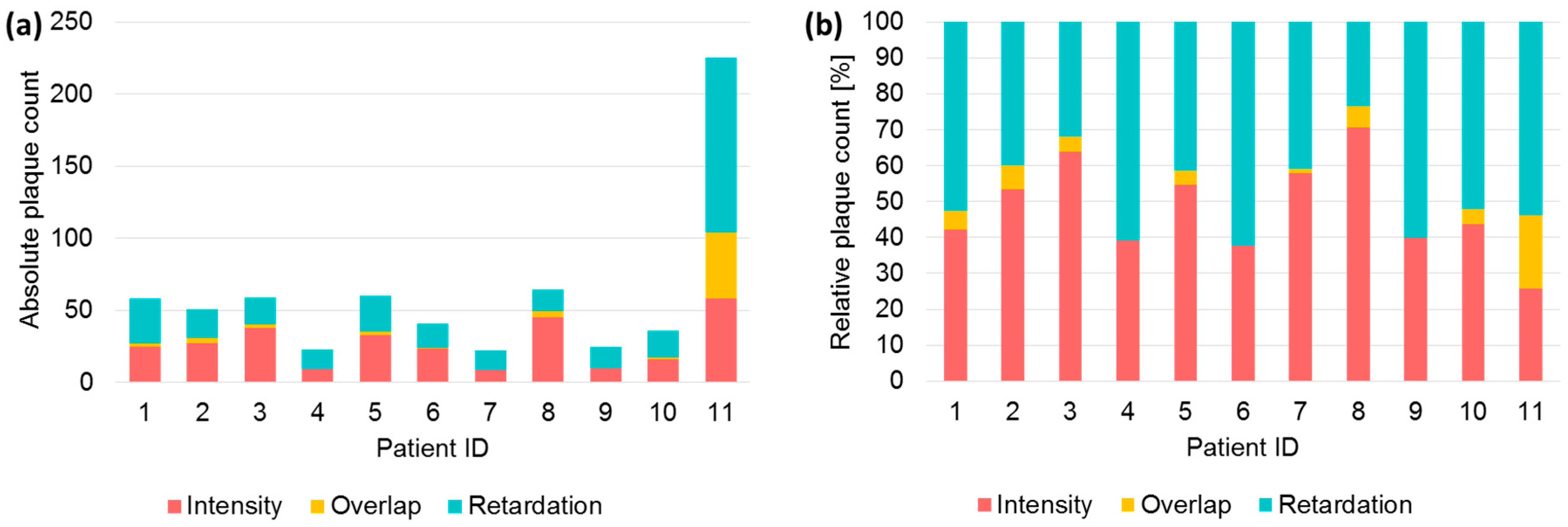
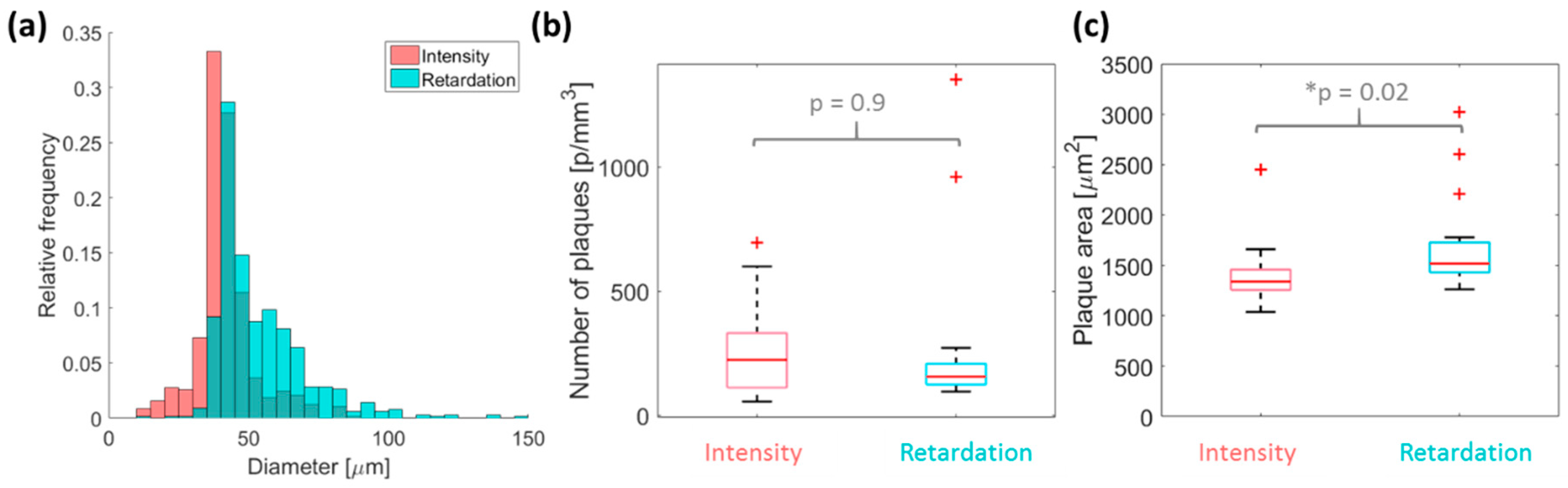
3.3. Evaluation of Plaque Load and Size Using Multicontrast OCT
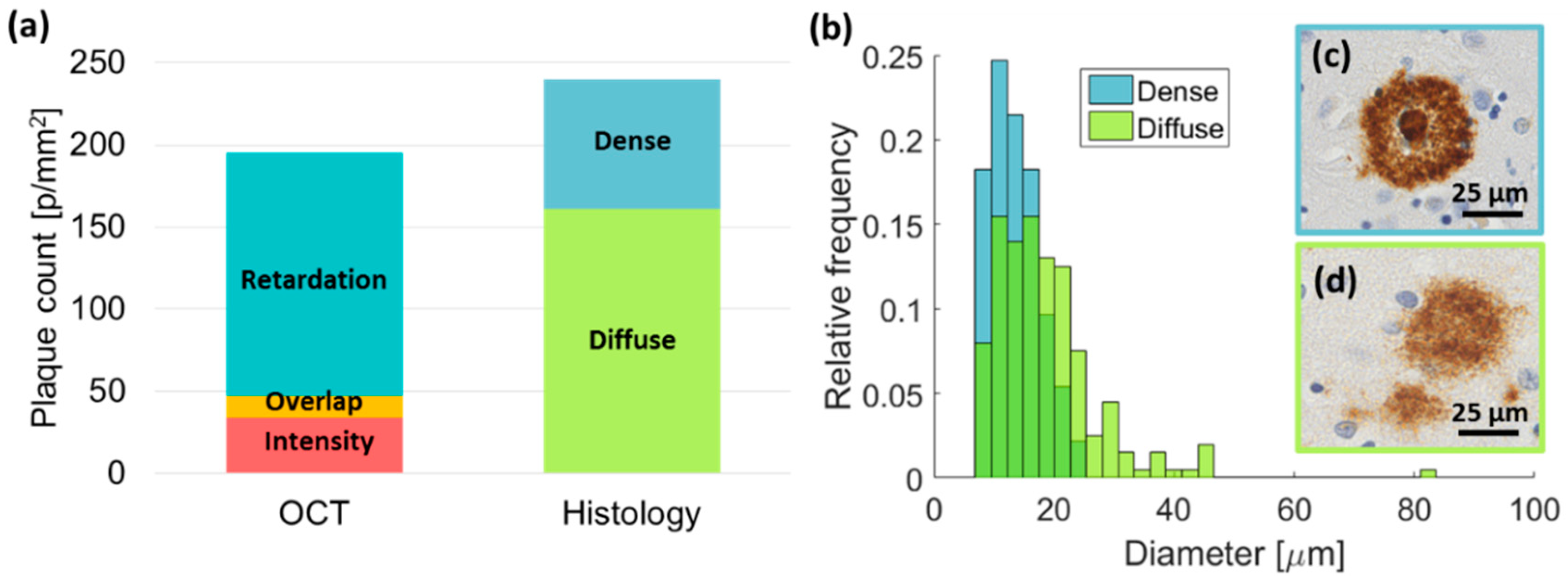
3.4. Comparison to Histology
4. Discussion
5. Conclusions
Author Contributions
Funding
Acknowledgments
Conflicts of Interest
References
- Alzheimer’s Association. 2019 Alzheimer’s Disease Facts and Figures. Alzheimer’s Dement. 2019, 15, 321–387. [Google Scholar] [CrossRef]
- Winblad, B.; Amouyel, P.; Andrieu, S.; Ballard, C.; Bryane, C.; Brodaty, H.; Cedazo-Minguez, A.; Dubois, B.; Edvardsson, D. Defeating Alzheimer’s Disease and Other Dementias: A Priority for European Science and Society. Lancet Neurol. 2016, 15, 455–532. [Google Scholar] [CrossRef]
- Scheltens, P.; Blennow, K.; Breteler, M.M.B.; Strooper, B.; Frisoni, G.B.; Salloway, S.; Flier, W.M. Alzheimer’s Disease. Lancet 2016, 388, 505–517. [Google Scholar] [CrossRef]
- Prince, M.; Bryce, R.; Albanese, E.; Wimo, A.; Ribeiro, W.; Ferri, C.P. The Global Prevalence of Dementia: A Systematic Review and Metaanalysis. Alzheimer’s Dement. 2013, 9, 63–75. [Google Scholar] [CrossRef]
- Ferri, C.; Prince, M.; Brayne, C.; Brodaty, H.; Fratiglioni, L.; Ganguli, M.; Hall, K.; Hasegawa, K.; Hendrie, H.; Scazufca, M. Global Prevalence of Dementia: A Delphi Consensus Study. Lancet 2005, 366, 2112–2117. [Google Scholar] [CrossRef]
- Janus, C.; Westaway, D. Transgenic Mouse Models of Alzheimer’s Disease. Physiol. Behav. 2001, 73, 873–886. [Google Scholar] [CrossRef]
- Arnold, S.E.; Hyman, B.T.; Flory, J.; Damasio, A.R.; Van Hoesen, G.W. The Topographical and Neuroanatomical Distribution of Neurofibrillary Tangles and Neuritic Plaques in the Cerebral Cortex of Patients with Alzheimer’s Disease. Cereb. Cortex 1991, 1, 103–116. [Google Scholar] [CrossRef]
- Hyman, B.; Van Hoesen, G.W.; Damasio, A.R.; Barnes, C.L. Alzheimer’s Disease: Cell-Specific Pathology Isolates the Hippocampal Formation. Science 1984, 225, 1168–1170. [Google Scholar] [CrossRef]
- Horn, R.; Ostertun, B.; Frica, M.; Solymosi, L.; Steudel, A.; Möllev, H.J. Atrophy of Hippocampus in Patients with Alzheimer’s Disease and Other Diseases with Memory Impairment. Dement. Geriatr. Cogn. Disord. 1996, 7, 182–186. [Google Scholar] [CrossRef]
- Bahmanyar, S.; Higgins, G.A.; Goldgaber, D.; Lewis, D.A.; Morrison, J.H.; Wilson, M.C.; Shankar, S.K.; Gajdusek, D.C. Localization of Amyloid Beta Protein Messenger RNA in Brains from Patients with Alzheimer’s Disease. Science 1987, 237, 77–80. [Google Scholar] [CrossRef]
- Whitehouse, P.J.; Price, D.L.; Struble, R.G.; Clark, A.W.; Coyle, J.T.; Delon, M.R. Alzheimer’s Disease and Senile Dementia: Loss of Neurons in the Basal Forebrain. Science 1982, 215, 1237–1239. [Google Scholar] [CrossRef]
- Morrison, J.H.; Hof, P.R. Life and Death of Neurons in the Aging Brain. Science 2002, 278, 412–419. [Google Scholar] [CrossRef]
- Bondi, M.W.; Edmonds, E.C.; Salmon, D.P. Alzheimer’s Disease: Past, Present, and Future. J. Int. Neuropsychol. Soc. 2017, 23, 818–831. [Google Scholar] [CrossRef]
- Reitz, C.; Brayne, C.; Mayeux, R. Epidemiology of Alzheimer Disease. Nat. Rev. Neurol. 2011, 7, 137–152. [Google Scholar] [CrossRef]
- Hampel, H.; Bürger, K.; Teipel, S.J.; Bokde, A.L.W.; Zetterberg, H.; Blennow, K. Core Candidate Neurochemical and Imaging Biomarkers of Alzheimer’s Disease. Alzheimer’s Dement. 2008, 4, 38–48. [Google Scholar] [CrossRef]
- Lane, C.A.; Hardy, J.; Schott, J.M. Alzheimer’s Disease. Eur. J. Neurol. 2018, 25, 59–70. [Google Scholar] [CrossRef]
- Funato, H.; Yoshimura, M.; Kusui, K.; Tamaoka, A.; Ishikawa, K.; Ohkoshi, N.; Namekata, K.; Okeda, R.; Ihara, Y. Quantitation of Amyloid Beta-Protein in the Cortex during Aging and in Alzheimer’s Disease. Am. J. Pathol. 1998, 152, 1633–1640. [Google Scholar]
- Ikeda, S.; Allsop, D.; Glenner, G. Morphology and Distribution of Plaque and Related Deposits in the Brains of Alzheimer’s Disease and Control Cases. An Immunohistochemical Study Using Amyloid Beta-Protein Antibody. Lab. Investig. 1989, 60, 113–122. [Google Scholar]
- Baumann, B.; Woehrer, A.; Ricken, G.; Augustin, M.; Mitter, C.; Pircher, M.; Kovacs, G.G.; Hitzenberger, C.K. Visualization of Neuritic Plaques in Alzheimer’s Disease by Polarization-Sensitive Optical Coherence Microscopy. Sci. Rep. 2017, 7, 43477. [Google Scholar] [CrossRef]
- Taylor, D.L.; Allen, R.D.; Benditt, E.P. Determination of the Polarization Optical Properties of the Amyloid Congo Red Complex by Phase Modulation Microspectrophotometry. J. Histochem. Cytochem. 1974, 22, 1105–1112. [Google Scholar] [CrossRef]
- Ross, M.H.; Pawlina, W. Histology; Lippincott Williams & Wilkins: Philadelphia, PA, USA, 2006. [Google Scholar]
- Schulz, G.; Crooijmans, H.J.A.; Germann, M.; Scheffler, K.; Müller-Gerbl, M.; Müller, B. Three-Dimensional Strain Fields in Human Brain Resulting from Formalin Fixation. J. Neurosci. Methods 2011, 202, 17–27. [Google Scholar] [CrossRef]
- Gal, A.A.; Cagle, P.T. The 100-Year Anniversary of the Description of the Frozen Section Procedure. J. Am. Med. Assoc. 2005, 294, 3135–3137. [Google Scholar] [CrossRef]
- Ratnavelu, N.D.; Brown, A.P.; Mallett, S.; Scholten, R.J.P.M.; Patel, A.; Founta, C.; Galaal, K.; Cross, P.; Naik, R. Intraoperative Frozen Section Analysis for the Diagnosis of Early Stage Ovarian Cancer in Suspicious Pelvic Masses. Cochrane Database Syst. Rev. 2016. [Google Scholar] [CrossRef]
- Drexler, W.; Fujimoto, J.G. Optical Coherence Tomography: Technology and Applications; Springer Science & Business Media: Berlin, Germany, 2008. [Google Scholar]
- Thomas, D.; Duguid, G. Optical Coherence Tomography—A Review of the Principles and Contemporary Uses in Retinal Investigation. Eye 2004, 18, 561–570. [Google Scholar] [CrossRef]
- Gora, M.J.; Suter, M.J.; Tearney, G.J.; Li, X. Endoscopic Optical Coherence Tomography: Technologies and Clinical Applications. Biomed. Opt. Express 2017, 8, 2405–2444. [Google Scholar] [CrossRef]
- Baumann, B. Advanced Optical Methods for Brain Imaging; Springer: Singapore, 2019; p. 5. [Google Scholar] [CrossRef]
- Olsen, J.; Holmes, J.; Jemec, G.B.E. Advances in Optical Coherence Tomography in Dermatology—A Review. J. Biomed. Opt. 2018, 23, 040901. [Google Scholar] [CrossRef]
- Hee, M.R.M.; Huang, D.; Swanson, E.A.E.; Fujimoto, J.G.J.G. Polarization-Sensitive Low-Coherence Reflectometer for Birefringence Characterization and Ranging. J. Opt. Soc. Am. B 1992, 9, 903–908. [Google Scholar] [CrossRef]
- De Boer, J.; Hitzenberger, C.K.; Yasuno, Y. Polarization Sensitive Optical Coherence Tomography: A Review of Technology and Applications. Biomed. Opt. Express 2017, 8, 1838–1873. [Google Scholar] [CrossRef]
- Lichtenegger, A.; Harper, D.J.; Augustin, M.; Eugui, P.; Muck, M.; Gesperger, J.; Hitzenberger, C.K.; Woehrer, A.; Baumann, B. Spectroscopic Imaging with Spectral Domain Visible Light Optical Coherence Microscopy in Alzheimer’s Disease Brain Samples. Biomed. Opt. Express 2017, 8, 4007–4025. [Google Scholar] [CrossRef]
- Lichtenegger, A.; Muck, M.; Eugui, P.; Harper, D.J.; Augustin, M.; Leskovar, K.; Hitzenberger, C.K.; Woehrer, A.; Baumann, B. Assessment of Pathological Features in Alzheimer’s Disease Brain Tissue with a Large Field-of-View Visible-Light Optical Coherence Microscope. Neurophotonics 2018, 5, 035002. [Google Scholar] [CrossRef]
- Bolmont, T.; Bouwens, A.; Pache, C.; Dimitrov, M.; Berclaz, C.; Villiger, M.; Wegenast-Braun, B.M.; Lasser, T.; Fraering, P.C. Label-Free Imaging of Cerebral Amyloidosis with Extended-Focus Optical Coherence Microscopy. J. Neurosci. 2012, 32, 14548–14556. [Google Scholar] [CrossRef]
- Marchand, P.J.; Bouwens, A.; Szlag, D.; Hguyen, D.; Descloux, A.; Sison, M.; Coquoz, S.; Extermann, J.; Lasser, T. Visible Spectrum Extended-Focus Optical Coherence Microscopy for Label-Free Sub-Cellular Tomography. Biomed. Opt. Express 2017, 8, 3343–3359. [Google Scholar] [CrossRef]
- Eugui, P.; Lichtenegger, A.; Augustin, M.; Harper, D.J.; Muck, M.; Roetzer, T.; Wartak, A.; Konegger, T.; Widhalm, G.; Baumann, B. Beyond Backscattering: Optical Neuroimaging by BRAD. Biomed. Opt. Express 2018, 9, 2467–2494. [Google Scholar] [CrossRef]
- Schindelin, J.; Arganda-Carreras, I.; Frise, E.; Kaynig, V.; Longair, M.; Pietzsch, T.; Preibisch, S.; Rueden, C.; Saalfeld, S.; Schmid, B.; Cardona, A. Fiji—An Open Source Platform for Biological Image Analysis. Nat. Methods 2013, 9, 676. [Google Scholar] [CrossRef]
- Thévenaz, P.; Ruttimann, U.E.; Unser, M. A Pyramid Approach to Subpixel Registration Based on Intensity. IEEE Trans. Image Process. 1998, 7, 27–41. [Google Scholar] [CrossRef]
- Yushkevich, P.A.; Piven, J.; Hazlett, H.C.; Smith, R.G.; Ho, S.; Gee, J.C.; Gerig, G. User-Guided 3D Active Contour Segmentation of Anatomical Structures: Significantly Improved Efficiency and Reliability. Neuroimage 2006, 31, 1116–1128. [Google Scholar] [CrossRef]
- Bolte, S.; Cordeliéres, F.P. A Guided Tour into Subcellular Colocalization Analysis in Light Microscopy. J. Microsc. 2006, 224, 213–232. [Google Scholar] [CrossRef]
- Götzinger, E.; Pircher, M.; Baumann, B.; Schmoll, T.; Sattmann, H.; Leitgeb, R.A.; Hitzenberger, C.K. Speckle Noise Reduction in High Speed Polarization Sensitive Spectral Domain Optical Coherence Tomography. Opt. Express 2011, 19, 14568–14584. [Google Scholar] [CrossRef]
- Lozzi, A.; Agrawal, A.; Boretsky, A.; Welle, C.G.; Hammer, D.X. Image Quality Metrics for Optical Coherence Angiography. Biomed. Opt. Express 2015, 6, 2435–2447. [Google Scholar] [CrossRef]
- Jin, L.-W.; Claborn, K.A.; Kurimoto, M.; Geday, M.A.; Maezawa, I.; Sohraby, F.; Estrada, M.; Kaminksy, W.; Kahr, B. Imaging Linear Birefringence and Dichroism in Cerebral Amyloid Pathologies. Proc. Natl. Acad. Sci. USA 2003, 100, 15294–15298. [Google Scholar] [CrossRef]
- Dudeffant, C.; Vandesquille, M.; Herbert, K.; Garin, C.M.; Alves, S.; Blanchard, V.; Comoy, E.E.; Petit, F.; Dhenain, M. Contrast-Enhanced MR Microscopy of Amyloid Plaques in Five Mouse Models of Amyloidosis and in Human Alzheimer’s Disease Brains. Sci. Rep. 2017, 7, 4955. [Google Scholar] [CrossRef]
- Selkoe, D.J.; Hardy, J. The Amyloid Hypothesis of Alzheimer’s Disease at 25 Years. EMBO Mol. Med. 2016, 8, 595–608. [Google Scholar] [CrossRef]
- Arbor, S.C.; LaFontaine, M.; Cumbay, M. Amyloid-Beta Alzheimer Targets - Protein Processing, Lipid Rafts, and Amyloid-Beta Pores. Yale J. Biol. Med. 2016, 89, 5–21. [Google Scholar]
- Iwadare, T.; Mori, H.; Ishiguro, K.; Takeishi, M. Dimensional Changes of Tissues in the Course of Processing. J. Microsc. 1984, 136, 323–327. [Google Scholar] [CrossRef]
- Fox, C.H.; Johnson, F.B.; Whiting, J.; Roller, P.P. Formaldehyde Fixation. J. Histochem. Cytochem. 1985, 33, 845–853. [Google Scholar] [CrossRef]
- Fercher, A.F.; Drexler, W.; Hitzenberger, C.K.; Lasser, T. Optical Coherence Tomography—Principles and Applications. Rep. Prog. Phys. 2003, 66, 239–303. [Google Scholar] [CrossRef]


© 2019 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Gesperger, J.; Lichtenegger, A.; Roetzer, T.; Augustin, M.; Harper, D.J.; Eugui, P.; Merkle, C.W.; Hitzenberger, C.K.; Woehrer, A.; Baumann, B. Comparison of Intensity- and Polarization-based Contrast in Amyloid-beta Plaques as Observed by Optical Coherence Tomography. Appl. Sci. 2019, 9, 2100. https://doi.org/10.3390/app9102100
Gesperger J, Lichtenegger A, Roetzer T, Augustin M, Harper DJ, Eugui P, Merkle CW, Hitzenberger CK, Woehrer A, Baumann B. Comparison of Intensity- and Polarization-based Contrast in Amyloid-beta Plaques as Observed by Optical Coherence Tomography. Applied Sciences. 2019; 9(10):2100. https://doi.org/10.3390/app9102100
Chicago/Turabian StyleGesperger, Johanna, Antonia Lichtenegger, Thomas Roetzer, Marco Augustin, Danielle J. Harper, Pablo Eugui, Conrad W. Merkle, Christoph K. Hitzenberger, Adelheid Woehrer, and Bernhard Baumann. 2019. "Comparison of Intensity- and Polarization-based Contrast in Amyloid-beta Plaques as Observed by Optical Coherence Tomography" Applied Sciences 9, no. 10: 2100. https://doi.org/10.3390/app9102100
APA StyleGesperger, J., Lichtenegger, A., Roetzer, T., Augustin, M., Harper, D. J., Eugui, P., Merkle, C. W., Hitzenberger, C. K., Woehrer, A., & Baumann, B. (2019). Comparison of Intensity- and Polarization-based Contrast in Amyloid-beta Plaques as Observed by Optical Coherence Tomography. Applied Sciences, 9(10), 2100. https://doi.org/10.3390/app9102100







