Treatment Selection for Early to Intermediate Hepatocellular Carcinoma
Abstract
1. Introduction
2. Application of RFA in HCC Treatment Guidelines
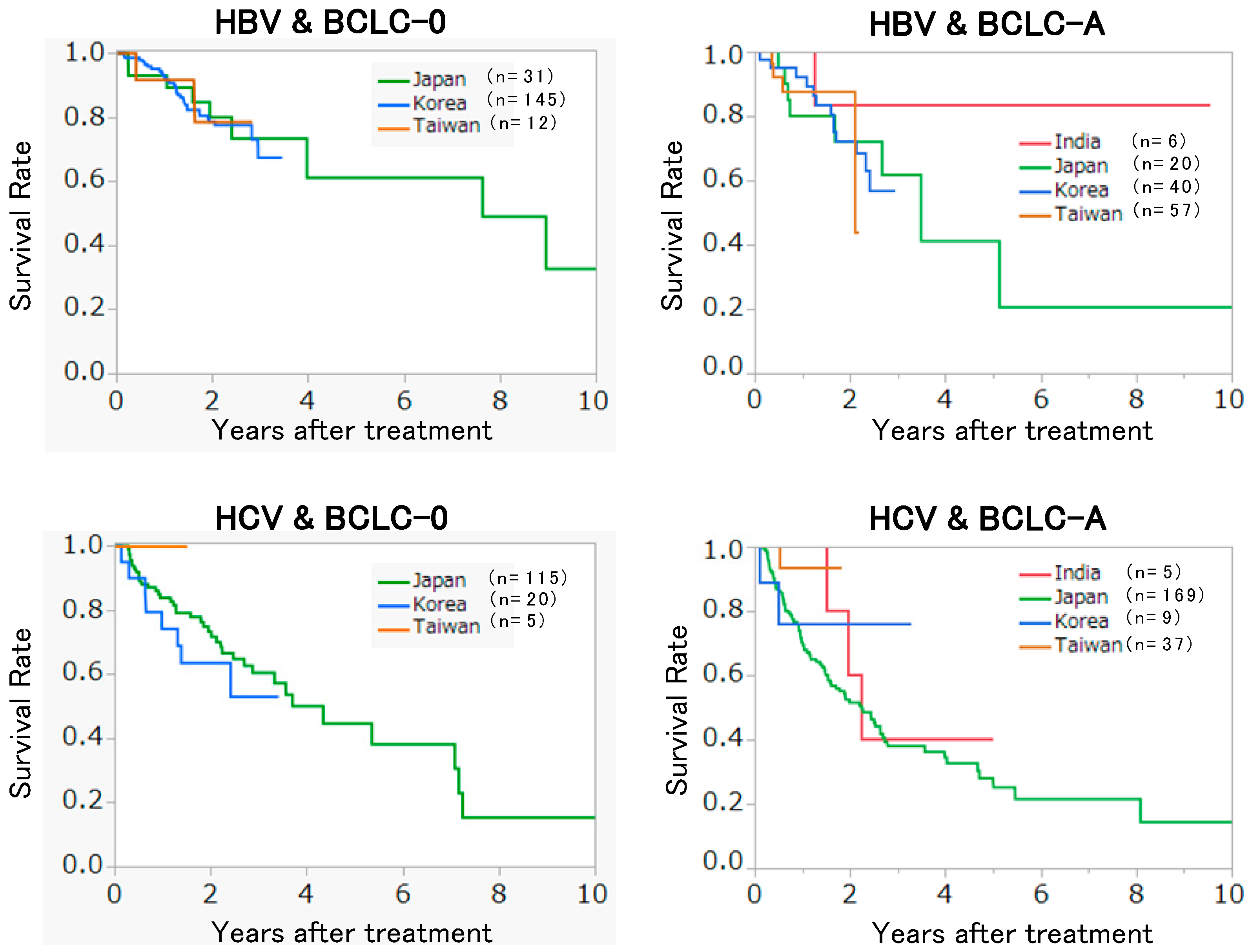
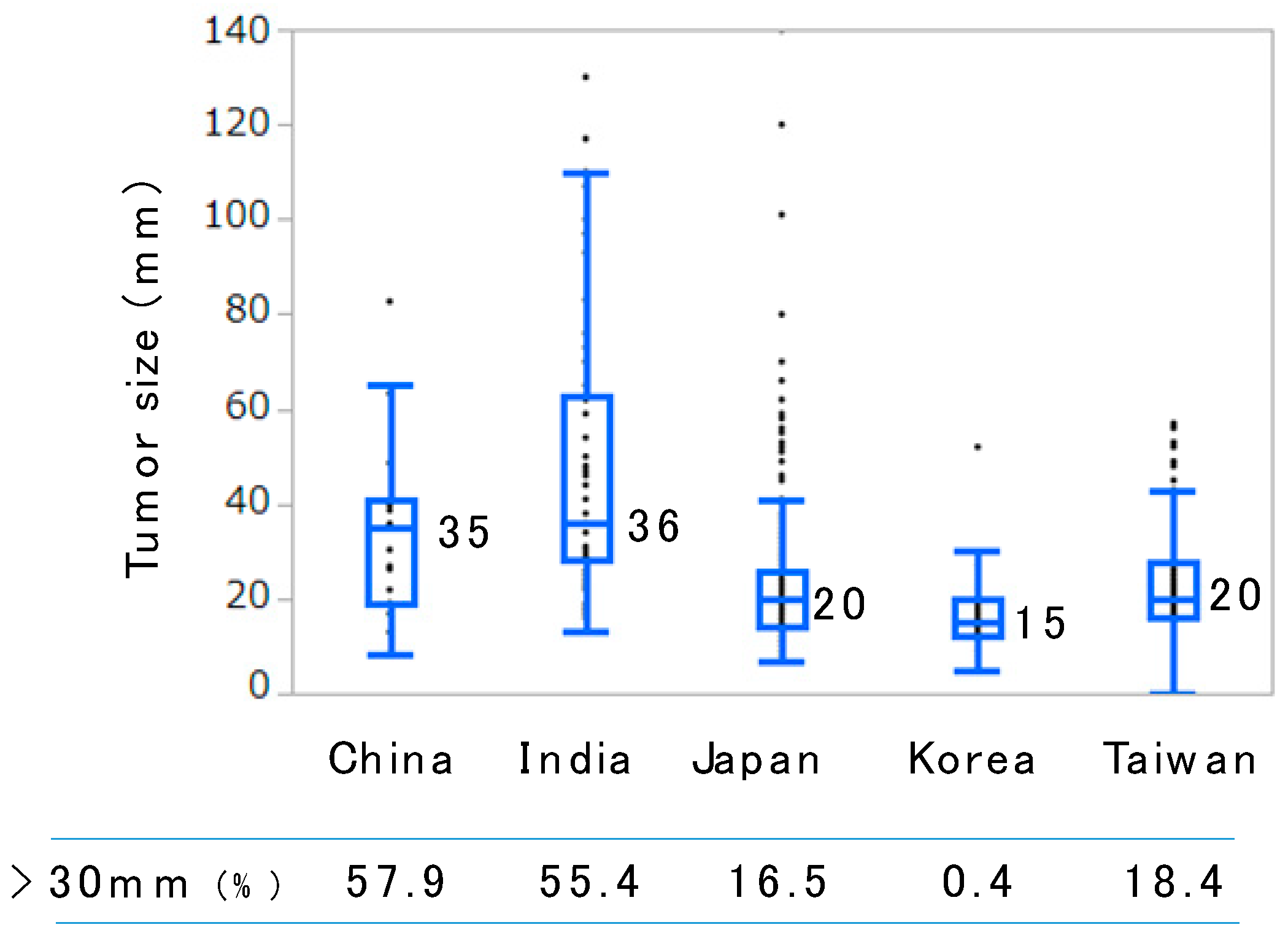
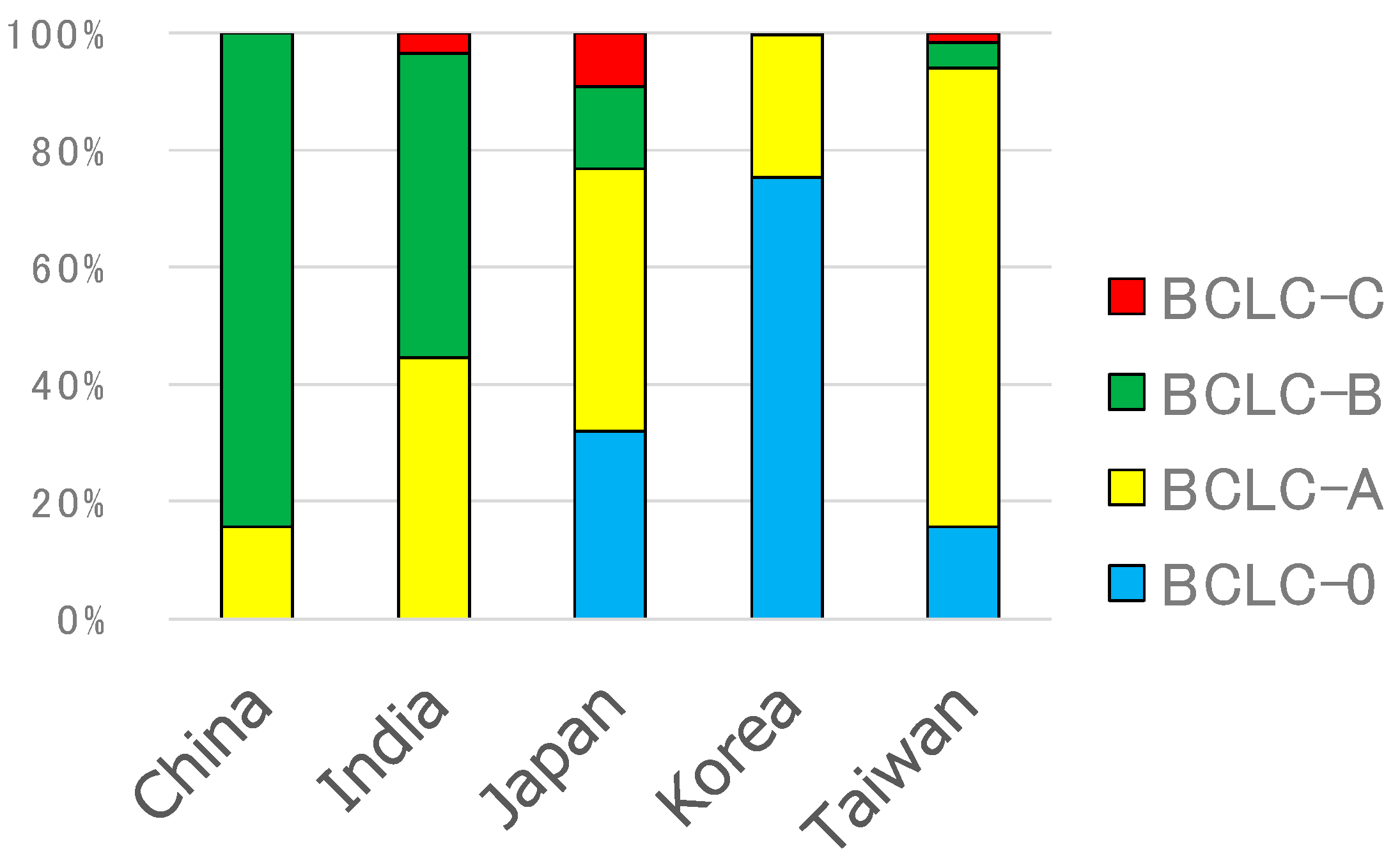
3. Current Status of RFA in Asia
4. RFA for Intermediate-Stage HCC
5. Application of Molecular Target Agents for the Treatment of Intermediate-Stage HCC
6. Application of Hepatic Arterial Infusion Chemotherapy (HAIC)
7. Future Perspectives
Author Contributions
Funding
Acknowledgments
Conflicts of Interest
References
- Ferlay, J.; Colombet, M.; Soerjomataram, I.; Mathers, C.; Parkin, D.M.; Pineros, M.; Znaor, A.; Bray, F. Estimating the global cancer incidence and mortality in 2018: GLOBOCAN sources and methods. Int. J. Cancer 2019, 144, 1941–1953. [Google Scholar] [CrossRef]
- Tateishi, R.; Koike, K. Changing etiology of hepatocellular carcinoma. J. Gastroenterol. 2020, 55, 125–126. [Google Scholar] [CrossRef] [PubMed]
- Nouso, K.; Kobayashi, Y.; Nakamura, S.; Kobayashi, S.; Toshimori, J.; Kuwaki, K.; Hagihara, H.; Onishi, H.; Miyake, Y.; Ikeda, F.; et al. Evolution of prognostic factors in hepatocellular carcinoma in Japan. Aliment. Pharmacol. Ther. 2010, 31, 407–414. [Google Scholar] [CrossRef] [PubMed]
- Omata, M.; Cheng, A.L.; Kokudo, N.; Kudo, M.; Lee, J.M.; Jia, J.; Tateishi, R.; Han, K.H.; Chawla, Y.K.; Shiina, S.; et al. Asia-Pacific clinical practice guidelines on the management of hepatocellular carcinoma: A 2017 update. Hepatol. Int. 2017, 11, 317–370. [Google Scholar] [CrossRef] [PubMed]
- Xie, D.Y.; Ren, Z.G.; Zhou, J.; Fan, J.; Gao, Q. Critical appraisal of Chinese 2017 guideline on the management of hepatocellular carcinoma. Hepatobiliary Surg. Nutr. 2017, 6, 387–396. [Google Scholar] [CrossRef] [PubMed]
- EASL Clinical Practice Guidelines: Management of hepatocellular carcinoma. J. Hepatol. 2018, 69, 182–236. [CrossRef] [PubMed]
- Management consensus guideline for hepatocellular carcinoma: 2016 updated by the Taiwan Liver Cancer Association and the Gastroenterological Society of Taiwan. J. Formos. Med Assoc. 2018, 117, 381–403. [CrossRef] [PubMed]
- Heimbach, J.K.; Kulik, L.M.; Finn, R.S.; Sirlin, C.B.; Abecassis, M.M.; Roberts, L.R.; Zhu, A.X.; Murad, M.H.; Marrero, J.A. AASLD guidelines for the treatment of hepatocellular carcinoma. Hepatology 2018, 67, 358–380. [Google Scholar] [CrossRef] [PubMed]
- Marrero, J.A.; Kulik, L.M.; Sirlin, C.B.; Zhu, A.X.; Finn, R.S.; Abecassis, M.M.; Roberts, L.R.; Heimbach, J.K. Diagnosis, Staging, and Management of Hepatocellular Carcinoma: 2018 Practice Guidance by the American Association for the Study of Liver Diseases. Hepatology 2018, 68, 723–750. [Google Scholar] [CrossRef]
- 2018 Korean Liver Cancer Association-National Cancer Center Korea Practice Guidelines for the Management of Hepatocellular Carcinoma. Korean J. Radiol. 2019, 20, 1042–1113. [CrossRef]
- Kokudo, N.; Takemura, N.; Hasegawa, K.; Takayama, T.; Kubo, S.; Shimada, M.; Nagano, H.; Hatano, E.; Izumi, N.; Kaneko, S.; et al. Clinical practice guidelines for hepatocellular carcinoma: The Japan Society of Hepatology 2017 (4th JSH-HCC guidelines) 2019 update. Hepatol. Res. 2019, 49, 1109–1113. [Google Scholar] [CrossRef] [PubMed]
- Wakuta, A.; Nouso, K.; Kariyama, K.; Nishimura, M.; Kishida, M.; Wada, N.; Mizushima, T.; Higashi, T.; Tanimoto, M. Radiofrequency ablation for the treatment of hepatocellular carcinoma with decompensated cirrhosis. Oncology 2011, 81, 39–44. [Google Scholar] [CrossRef] [PubMed]
- Hoffmann, R.; Rempp, H.; Syha, R.; Ketelsen, D.; Pereira, P.L.; Claussen, C.D.; Clasen, S. Transarterial chemoembolization using drug eluting beads and subsequent percutaneous MR-guided radiofrequency ablation in the therapy of intermediate sized hepatocellular carcinoma. Eur. J. Radiol. 2014, 83, 1793–1798. [Google Scholar] [CrossRef] [PubMed]
- Yin, X.; Zhang, L.; Wang, Y.H.; Zhang, B.H.; Gan, Y.H.; Ge, N.L.; Chen, Y.; Li, L.X.; Ren, Z.G. Transcatheter arterial chemoembolization combined with radiofrequency ablation delays tumor progression and prolongs overall survival in patients with intermediate (BCLC B) hepatocellular carcinoma. BMC Cancer 2014, 14, 849. [Google Scholar] [CrossRef]
- Kariyama, K.; Wakuta, A.; Nishimura, M.; Kishida, M.; Oonishi, A.; Ohyama, A.; Nouso, K.; Kudo, M. Percutaneous Radiofrequency Ablation for Intermediate-Stage Hepatocellular Carcinoma. Oncology 2015, 89 (Suppl. 2), 19–26. [Google Scholar] [CrossRef] [PubMed]
- Azuma, S.; Asahina, Y.; Nishimura-Sakurai, Y.; Kakinuma, S.; Kaneko, S.; Nagata, H.; Goto, F.; Ootani, S.; Kawai-Kitahata, F.; Taniguchi, M.; et al. Efficacy of additional radiofrequency ablation after transcatheter arterial chemoembolization for intermediate hepatocellular carcinoma. Hepatol. Res. 2016, 46, 312–319. [Google Scholar] [CrossRef]
- Nouso, K.; Kariyama, K.; Nakamura, S.; Oonishi, A.; Wakuta, A.; Oyama, A.; Ako, S.; Dohi, C.; Wada, N.; Morimoto, Y.; et al. Application of radiofrequency ablation for the treatment of intermediate-stage hepatocellular carcinoma. J. Gastroenterol. Hepatol. 2017, 32, 695–700. [Google Scholar] [CrossRef] [PubMed]
- Endo, K.; Kuroda, H.; Oikawa, T.; Okada, Y.; Fujiwara, Y.; Abe, T.; Sato, H.; Sawara, K.; Takikawa, Y. Efficacy of combination therapy with transcatheter arterial chemoembolization and radiofrequency ablation for intermediate-stage hepatocellular carcinoma. Scand. J. Gastroenterol. 2018, 53, 1575–1583. [Google Scholar] [CrossRef] [PubMed]
- Espinosa, W.; Liu, Y.W.; Wang, C.C.; Lin, C.C.; Wang, J.H.; Lu, S.N.; Hung, C.H. Combined resection and radiofrequency ablation versus transarterial embolization for intermediate-stage hepatocellular carcinoma: A propensity score matching study. J. Formos. Med Assoc. 2018, 117, 197–203. [Google Scholar] [CrossRef]
- Liu, F.; Chen, M.; Mei, J.; Xu, L.; Guo, R.; Lin, X.; Zhang, Y.; Peng, Z. Transarterial Chemoembolization Combined with Radiofrequency Ablation in the Treatment of Stage B1 Intermediate Hepatocellular Carcinoma. J. Oncol. 2019, 2019, 6298502. [Google Scholar] [CrossRef]
- Kariyama, K.; Nouso, K.; Wakuta, A.; Oonishi, A.; Toyoda, H.; Tada, T.; Hiraoka, A.; Tsuji, K.; Itobayashi, E.; Ishikawa, T.; et al. Treatment of Intermediate-Stage Hepatocellular Carcinoma in Japan: Position of Curative Therapies. Liver Cancer 2020, 9, 41–49. [Google Scholar] [CrossRef] [PubMed]
- Bolondi, L.; Burroughs, A.; Dufour, J.F.; Galle, P.R.; Mazzaferro, V.; Piscaglia, F.; Raoul, J.L.; Sangro, B. Heterogeneity of patients with intermediate (BCLC B) Hepatocellular Carcinoma: Proposal for a subclassification to facilitate treatment decisions. Semin Liver Dis. 2012, 32, 348–359. [Google Scholar] [PubMed]
- Llovet, J.M.; Ricci, S.; Mazzaferro, V.; Hilgard, P.; Gane, E.; Blanc, J.F.; de Oliveira, A.C.; Santoro, A.; Raoul, J.L.; Forner, A.; et al. Sorafenib in advanced hepatocellular carcinoma. N. Engl. J. Med. 2008, 359, 378–390. [Google Scholar] [CrossRef]
- Kudo, M.; Finn, R.S.; Qin, S.; Han, K.H.; Ikeda, K.; Piscaglia, F.; Baron, A.; Park, J.W.; Han, G.; Jassem, J.; et al. Lenvatinib versus sorafenib in first-line treatment of patients with unresectable hepatocellular carcinoma: A randomised phase 3 non-inferiority trial. Lancet 2018, 391, 1163–1173. [Google Scholar] [CrossRef]
- Zhu, A.X.; Kang, Y.K.; Yen, C.J.; Finn, R.S.; Galle, P.R.; Llovet, J.M.; Assenat, E.; Brandi, G.; Pracht, M.; Lim, H.Y.; et al. Ramucirumab after sorafenib in patients with advanced hepatocellular carcinoma and increased alpha-fetoprotein concentrations (REACH-2): A randomised, double-blind, placebo-controlled, phase 3 trial. Lancet Oncol. 2019, 20, 282–296. [Google Scholar] [CrossRef]
- Kudo, M.; Ueshima, K.; Chan, S.; Minami, T.; Chishina, H.; Aoki, T.; Takita, M.; Hagiwara, S.; Minami, Y.; Ida, H.; et al. Lenvatinib as an Initial Treatment in Patients with Intermediate-Stage Hepatocellular Carcinoma Beyond Up-To-Seven Criteria and Child-Pugh A Liver Function: A Proof-Of-Concept Study. Cancers 2019, 11, 1084. [Google Scholar] [CrossRef] [PubMed]
- Nouso, K.; Miyahara, K.; Uchida, D.; Kuwaki, K.; Izumi, N.; Omata, M.; Ichida, T.; Kudo, M.; Ku, Y.; Kokudo, N.; et al. Effect of hepatic arterial infusion chemotherapy of 5-fluorouracil and cisplatin for advanced hepatocellular carcinoma in the Nationwide Survey of Primary Liver Cancer in Japan. Br. J. Cancer 2013, 109, 1904–1907. [Google Scholar] [CrossRef]
- Kudo, M.; Ueshima, K.; Yokosuka, O.; Ogasawara, S.; Obi, S.; Izumi, N.; Aikata, H.; Nagano, H.; Hatano, E.; Sasaki, U.; et al. Sorafenib Plus Low-Dose Cisplatin and Fluorouracil Hepatic Arterial Infusion Chemotherapy Versus Sorafenib Alone in Patients with Advanced Hepatocellular Carcinoma (SILIUS): A Randomised, Open Label, Phase 3 Trial. Lancet Gastroenterol. Hepatol. 2018, 3, 424–432. [Google Scholar] [CrossRef]
- Terashima, T.; Yamashita, T.; Arai, K.; Kawaguchi, K.; Kitamura, K.; Yamashita, T.; Sakai, Y.; Mizukoshi, E.; Honda, M.; Kaneko, S. Response to chemotherapy improves hepatic reserve for patients with hepatocellular carcinoma and Child–Pugh B cirrhosis. Cancer Sci. 2016, 107, 1263–1269. [Google Scholar] [CrossRef]
| Authors | Pt No. | Intervention | Results |
|---|---|---|---|
| Azuma, et al. [16] | n = 59 | TACE + RFA to the nodules with poor lipiodol retention | Better PFS, OS than TACE |
| Yin, et al. [14] | n = 211 | TACE + RFA to the nodules with easy to ablation | Better PFS, OS than TACE |
| Hoffmann, et al. [13] | n = 20 | DC beads + RFA | Effective and Safe |
| Nouso, et al. [17] | n = 167 | RFA to all nodules | Better OS than TACE |
| Endo, et al. [18] | n = 92 | TACE + RFA | Better PFS, OS than TACE (especially AFP < 100 ng/mL) |
| Kariyama, et al. [15] | n = 627 | RFA | Better OS than TACE in B1/B2 stages |
| Liu, et al. [20] | n = 404 (B1 stage) | TACE + RFA | Better OS and PFS |
© 2020 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Nouso, K.; Ohki, T.; Yamashita, T.; Takaki, H.; Liu, C.-A.; Kang, T.W.; Lee, D.H.; Lee, S.J.; Kulkarni, S.; Shree, D.; et al. Treatment Selection for Early to Intermediate Hepatocellular Carcinoma. Appl. Sci. 2020, 10, 4607. https://doi.org/10.3390/app10134607
Nouso K, Ohki T, Yamashita T, Takaki H, Liu C-A, Kang TW, Lee DH, Lee SJ, Kulkarni S, Shree D, et al. Treatment Selection for Early to Intermediate Hepatocellular Carcinoma. Applied Sciences. 2020; 10(13):4607. https://doi.org/10.3390/app10134607
Chicago/Turabian StyleNouso, Kazuhiro, Takamasa Ohki, Tatsuya Yamashita, Haruyuki Takaki, Chien-Au Liu, Tae Wook Kang, Dong Ho Lee, So Jung Lee, Suyash Kulkarni, Deepa Shree, and et al. 2020. "Treatment Selection for Early to Intermediate Hepatocellular Carcinoma" Applied Sciences 10, no. 13: 4607. https://doi.org/10.3390/app10134607
APA StyleNouso, K., Ohki, T., Yamashita, T., Takaki, H., Liu, C.-A., Kang, T. W., Lee, D. H., Lee, S. J., Kulkarni, S., Shree, D., & Tanaka, M. (2020). Treatment Selection for Early to Intermediate Hepatocellular Carcinoma. Applied Sciences, 10(13), 4607. https://doi.org/10.3390/app10134607






