Effect of Mindful Hypnotherapy on Psychological Distress: A Systematic Review and Meta-Analysis
Abstract
1. Introduction
2. Materials and Methods
2.1. Eligibility Criteria
2.2. Study Selection and Data Extraction
2.3. Risk of Bias Assessment
2.4. Quality of Evidence Assessment
2.5. Statistical Analysis
3. Results
3.1. Study Inclusion
3.2. Participant Characteristics
3.3. Intervention Characteristics
3.4. Data Synthesis from Meta-Analysis
3.4.1. Psychological Distress
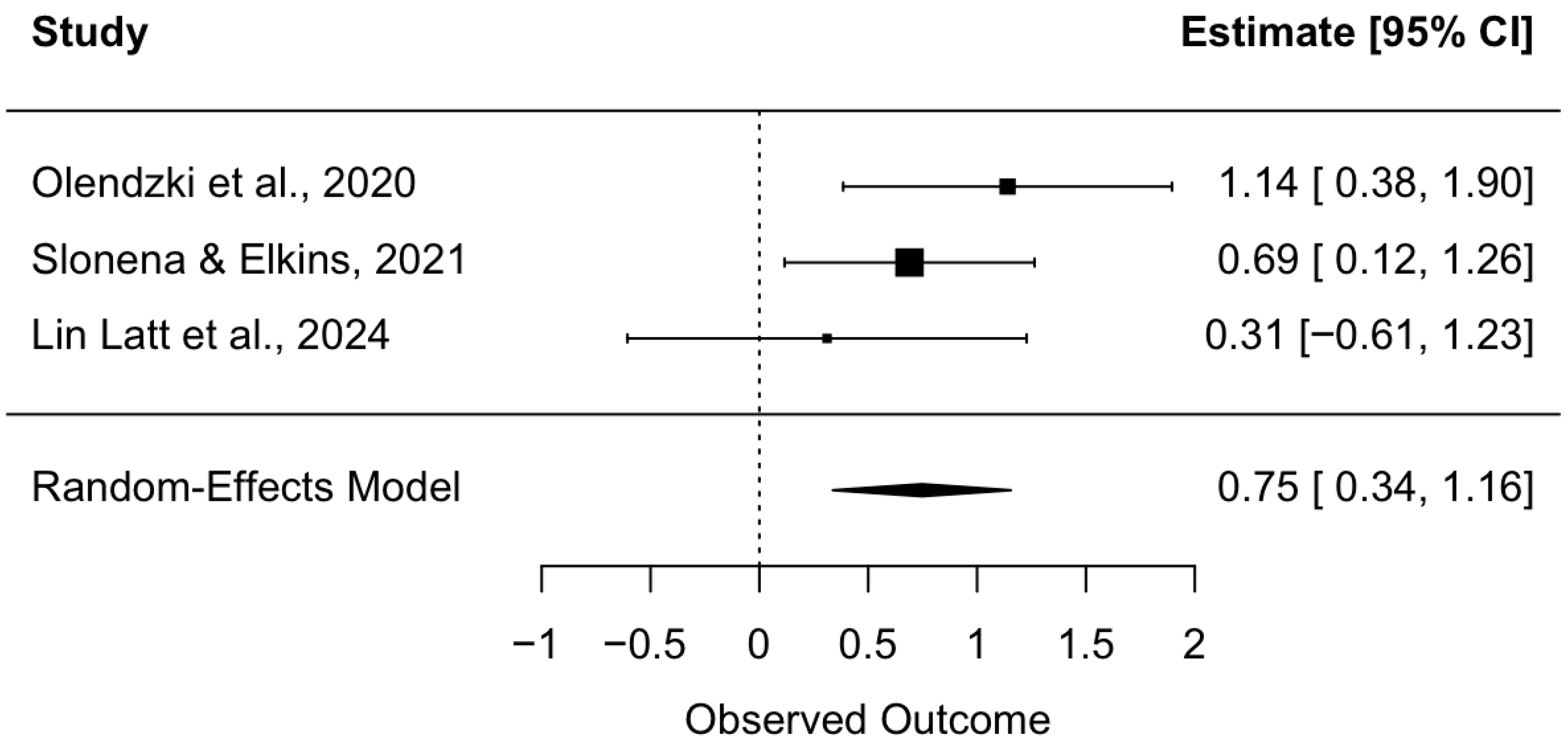
3.4.2. Stress
3.4.3. Mindfulness
3.5. Risk of Bias and Quality Assessment
4. Discussion
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Arvidsdotter, T., Marklund, B., Kylén, S., Taft, C., & Ekman, I. (2016). Understanding persons with psychological distress in primary health care. Scandinavian Journal of Caring Sciences, 30(4), 687–694. [Google Scholar] [CrossRef]
- Baer, R. A. (2003). Mindfulness training as a clinical intervention: A conceptual and empirical review. Clinical Psychology: Science and Practice, 10(2), 125–143. [Google Scholar] [CrossRef]
- Benzeval, M., & Judge, K. (2001). Income and health: The time dimension. Social Science & Medicine, 52(9), 1371–1390. [Google Scholar] [CrossRef]
- Bishop, S. R., Lau, M., Shapiro, S., Carlson, L., Anderson, N. D., Carmody, J., Segal, Z. V., Abbey, S., Speca, M., Velting, D., & Devins, G. (2004). Mindfulness: A proposed operational definition. Clinical Psychology: Science and Practice, 11(3), 230–241. [Google Scholar] [CrossRef]
- Bowles, N. I., Davies, J. N., & Van Dam, N. T. (2022). Dose–response relationship of reported lifetime meditation practice with mental health and wellbeing: A cross-sectional study. Mindfulness, 13(10), 2529–2546. [Google Scholar] [CrossRef]
- Britton, W. B., Lindahl, J. R., Cooper, D. J., Canby, N. K., & Palitsky, R. (2021). Defining and measuring meditation-related adverse effects in mindfulness-based programs. Clinical Psychological Science, 9(6), 1185–1204. [Google Scholar] [CrossRef] [PubMed]
- Chittleborough, C. R., Winefield, H., Gill, T. K., Koster, C., & Taylor, A. W. (2011). Age differences in associations between psychological distress and chronic conditions. International Journal of Public Health, 56(1), 71–80. [Google Scholar] [CrossRef]
- Cohen, J. (1988). Statistical power analysis for the behavioral sciences (2nd ed.). Erlbaum. [Google Scholar]
- Cumpston, M., Li, T., Page, M. J., Chandler, J., Welch, V. A., Higgins, J. P., & Thomas, J. (2019). Updated guidance for trusted systematic reviews: A new edition of the cochrane handbook for systematic reviews of interventions. Cochrane Database of Systematic Reviews, 2019(10), ED000142. [Google Scholar] [CrossRef] [PubMed]
- Elkins, G. R., Barabasz, A. F., Council, J. R., & Spiegel, D. (2015). Advancing research and practice: The revised APA division 30 definition of hypnosis. American Journal of Clinical Hypnosis, 57(4), 378–385. [Google Scholar] [CrossRef]
- Elkins, G. R., & Olendzki, N. (2019). Mindful hypnotherapy: The basics for clinical practice. Springer Publishing Company. [Google Scholar]
- Elkins, G. R., Roberts, R. L., & Simicich, L. (2018). Mindful self-hypnosis for self-care: An integrative model and illustrative case example. American Journal of Clinical Hypnosis, 61(1), 45–56. [Google Scholar] [CrossRef]
- Gispert, R., Rajmil, L., Schiaffino, A., & Herdman, M. (2003). Sociodemographic and health-related correlates of psychiatric distress in a general population. Social Psychiatry and Psychiatric Epidemiology, 38(12), 677–683. [Google Scholar] [CrossRef]
- Goldberg, S. B., Tucker, R. P., Greene, P. A., Davidson, R. J., Wampold, B. E., Kearney, D. J., & Simpson, T. L. (2018). Mindfulness-based interventions for psychiatric disorders: A systematic review and meta-analysis. Clinical Psychology Review, 59, 52–60. [Google Scholar] [CrossRef]
- Guyatt, G. H., Oxman, A. D., Schünemann, H. J., Tugwell, P., & Knottnerus, A. (2011). GRADE guidelines: A new series of articles in the Journal of Clinical Epidemiology. Journal of Clinical Epidemiology, 64(4), 380–382. [Google Scholar] [CrossRef] [PubMed]
- Hidderley, M., & Holt, M. (2004). A pilot randomized trial assessing the effects of autogenic training in early stage cancer patients in relation to psychological status and immune system responses. European Journal of Oncology Nursing: The Official Journal of European Oncology Nursing Society, 8(1), 61–65. [Google Scholar] [CrossRef] [PubMed]
- Higgins, J. P., & Thompson, S. G. (2002). Quantifying heterogeneity in a meta-analysis. Statistics in Medicine, 21, 1539–1558. [Google Scholar] [CrossRef]
- Hofmann, S. G., Sawyer, A. T., Witt, A. A., & Oh, D. (2010). The effect of mindfulness-based therapy on anxiety and depression: A meta-analytic review. Journal of Consulting and Clinical Psychology, 78(2), 169. [Google Scholar] [CrossRef]
- Horwitz, A. V. (2007). Distinguishing distress from disorder as psychological outcomes of stressful social arrangements. Health, 11(3), 273–289. [Google Scholar] [CrossRef]
- Hölzel, B. K., Lazar, S. W., Gard, T., Schuman-Olivier, Z., Vago, D. R., & Ott, U. (2011). How does mindfulness meditation work? Proposing mechanisms of action from a conceptual and neural perspective. Perspectives on Psychological Science, 6(6), 537–559. [Google Scholar] [CrossRef]
- Jensen, M. P., Mendoza, M. E., Ehde, D. M., Patterson, D. R., Molton, I. R., Dillworth, T. M., Gertz, K. J., Chan, J., Hakimian, S., Battalio, S. L., & Ciol, M. A. (2020). Effects of hypnosis, cognitive therapy, hypnotic cognitive therapy, and pain education in adults with chronic pain: A randomized clinical trial. Pain, 161(10), 2284–2298. [Google Scholar] [CrossRef] [PubMed]
- Kabat-Zinn, J., Massion, A. O., Kristeller, J., Peterson, L. G., Fletcher, K. E., Pbert, L., Lenderking, W. R., & Santorelli, S. F. (1992). Effectiveness of a meditation-based stress reduction program in the treatment of anxiety disorders. American Journal of Psychiatry, 149(7), 936–943. [Google Scholar] [CrossRef]
- Karo, M., Simorangkir, L., Daryanti Saragih, I., Suarilah, I., & Tzeng, H. (2024). Effects of mindfulness-based interventions on reducing psychological distress among nurses: A systematic review and meta-analysis of randomized controlled trials. Journal of Nursing Scholarship, 56(2), 319–330. [Google Scholar] [CrossRef] [PubMed]
- Khazraee, H., Bakhtiari, M., Kianimoghadam, A. S., & Ghorbanikhah, E. (2023a). The effectiveness of mindful hypnotherapy on depression, self-compassion, and psychological inflexibility in females with major depressive disorder: A single-blind, randomized clinical trial. International Journal of Clinical and Experimental Hypnosis, 71(1), 63–78. [Google Scholar] [CrossRef]
- Khazraee, H., Bakhtiari, M., Kianimoghadam, A. S., & Ghorbanikhah, E. (2023b). The effectiveness of mindful hypnotherapy on difficulties in emotion regulation, mindfulness, and mental health in patients with major depressive disorder. Journal of Education and Health Promotion, 12(1), 365. [Google Scholar] [CrossRef]
- Khoury, B., Lecomte, T., Fortin, G., Masse, M., Therien, P., Bouchard, V., Chapleau, M.-A., Paquin, K., & Hofmann, S. G. (2013). Mindfulness-based therapy: A comprehensive meta-analysis. Clinical Psychology Review, 33(6), 763–771. [Google Scholar] [CrossRef]
- Kuriyama, S., Nakaya, N., Ohmori-Matsuda, K., Shimazu, T., Kikuchi, N., Kakizaki, M., Sone, T., Sato, F., Nagai, M., Sugawara, Y., Akhter, M., Higashiguchi, M., Fukuchi, N., Takahashi, H., Hozawa, A., & Tsuji, I. (2009). Factors associated with psychological distress in a community-dwelling Japanese population: The Ohsaki cohort 2006 study. Journal of Epidemiology, 19(6), 294–302. [Google Scholar] [CrossRef] [PubMed]
- Lin Latt, C. M., Alldredge, C. T., Williams, S., Vinson, M., Seiba Moris, J., & Elkins, G. R. (2024). Mindful self-hypnosis combined with resistance training to reduce perceived stress and improve other psychological factors in female college students. International Journal of Clinical and Experimental Hypnosis, 72(3), 254–273. [Google Scholar] [CrossRef]
- Lomas, T., Cartwright, T., Edginton, T., & Ridge, D. (2015). A qualitative analysis of experiential challenges associated with meditation practice. Mindfulness, 6(4), 848–860. [Google Scholar] [CrossRef]
- Lynn, S. J., Kirsch, I., & Hallquist, M. N. (2008). Social cognitive theories of hypnosis. Oxford University Press. [Google Scholar] [CrossRef]
- Lynn, S. J., Surya Das, L., Hallquist, M. N., & Williams, J. C. (2006). Mindfulness, acceptance, and hypnosis: Cognitive and clinical perspectives. International Journal of Clinical and Experimental Hypnosis, 54(2), 143–166. [Google Scholar] [CrossRef] [PubMed]
- Miller, J. J., Fletcher, K., & Kabat-Zinn, J. (1995). Three-year follow-up and clinical implications of a mindfulness meditation-based stress reduction intervention in the treatment of anxiety disorders. General Hospital Psychiatry, 17(3), 192–200. [Google Scholar] [CrossRef]
- Olendzki, N., Elkins, G. R., Slonena, E., Hung, J., & Rhodes, J. R. (2020). Mindful hypnotherapy to reduce stress and increase mindfulness: A randomized controlled pilot study. International Journal of Clinical and Experimental Hypnosis, 68(2), 151–166. [Google Scholar] [CrossRef]
- Page, M. J., McKenzie, J. E., Bossuyt, P. M., Boutron, I., Hoffmann, T. C., Mulrow, C. D., Shamseer, L., Tetzlaff, J. M., Akl, E. A., Brennan, S. E., Chou, R., Glanville, J., Grimshaw, J. M., Hróbjartsson, A., Lalu, M. M., Li, T., Loder, E. W., Mayo-Wilson, E., McDonald, S., … Moher, D. (2021). The PRISMA 2020 statement: An updated guideline for reporting systematic reviews. The BMJ, 372, n71. [Google Scholar] [CrossRef]
- Park, S., Sato, Y., Takita, Y., Tamura, N., Ninomiya, A., Kosugi, T., Sado, M., Nakagawa, A., Takahashi, M., Hayashida, T., & Fujisawa, D. (2020). Mindfulness-cased cognitive therapy for psychological distress, fear of cancer recurrence, fatigue, spiritual well-being, and quality of life in patients with breast cancer—A randomized controlled trial. Journal of Pain and Symptom Management, 60(2), 381–389. [Google Scholar] [CrossRef]
- Phongsavan, P., Chey, T., Bauman, A., Brooks, R., & Silove, D. (2006). Social capital, socio-economic status and psychological distress among Australian adults. Social Science & Medicine, 63(10), 2546–2561. [Google Scholar] [CrossRef]
- Ridner, S. H. (2004). Psychological distress: Concept analysis. Journal of Advanced Nursing, 45(5), 536–545. [Google Scholar] [CrossRef]
- Slonena, E. E., & Elkins, G. R. (2021). Effects of a brief mindful hypnosis intervention on stress reactivity: A randomized active control study. International Journal of Clinical and Experimental Hypnosis, 69(4), 453–467. [Google Scholar] [CrossRef]
- Sterne, J. A. C., Savović, J., Page, M. J., Elbers, R. G., Blencowe, N. S., Boutron, I., Cates, C. J., Cheng, H.-Y., Corbett, M. S., Eldridge, S. M., Emberson, J. R., Hernán, M. A., Hopewell, S., Hróbjartsson, A., Junqueira, D. R., Jüni, P., Kirkham, J. J., Lasserson, T., Li, T., … Higgins, J. P. T. (2019). RoB 2: A revised tool for assessing risk of bias in randomised trials. BMJ, 366, l4898. [Google Scholar] [CrossRef]
- Stoerkel, E., Bellanti, D., Paat, C., Peacock, K., Aden, J., Setlik, R., Walter, J., & Inman, A. (2018). Effectiveness of a self-care toolkit for surgical breast cancer patients in a military treatment facility. Journal of Alternative and Complementary Medicine, 24(9–10), 916–925. [Google Scholar] [CrossRef] [PubMed]
- Taylor, S., Abramowitz, J. S., & McKay, D. (2012). Non-adherence and non-response in the treatment of anxiety disorders. Journal of Anxiety Disorders, 26(5), 583–589. [Google Scholar] [CrossRef] [PubMed]
- Teasdale, J. D., Segal, Z. V., Williams, J. M. G., Ridgeway, V. A., Soulsby, J. M., & Lau, M. A. (2000). Prevention of relapse/recurrence in major depression by mindfulness-based cognitive therapy. Journal of Consulting and Clinical Psychology, 68(4), 615–623. [Google Scholar] [CrossRef] [PubMed]
- Viertiö, S., Kiviruusu, O., Piirtola, M., Kaprio, J., Korhonen, T., Marttunen, M., & Suvisaari, J. (2021). Factors contributing to psychological distress in the working population, with a special reference to gender difference. BMC Public Health, 21, 611. [Google Scholar] [CrossRef]
- von Hippel, P. T. (2015). The heterogeneity statistic I 2 can be biased in small meta-analyses. BMC Medical Research Methodology, 15(1), 35. [Google Scholar] [CrossRef] [PubMed]




| Study ID | Groups | Sponsorship Source | Total N | Retention | Reported Outcomes in Study |
|---|---|---|---|---|---|
| Olendzki et al. (2020) | Mindful hypnotherapy intervention, waitlist control | None reported | 42 | 71.4% (30/42 completed) | Stress, psychological distress, mindfulness |
| Slonena and Elkins (2021) | Brief mindful hypnotherapy, cognitive training control | None reported | 55 | 92.7% (51/55 completed) | Stress, mindfulness, psychological distress |
| Khazraee et al. (2023a) | Mindful hypnotherapy intervention, waitlist control | Taleghani Hospital Research Development Committee, Shahid Beheshti University of Medical Sciences, Tehran, Iran (Grant Number: 28489) | 34 | 91.2.2% (31/34 completed) | Depression, mindfulness |
| Khazraee et al. (2023b) | Mindful hypnotherapy, waitlist control | Taleghani Hospital Research Development Committee, Shahid Beheshti University of Medical Sciences, Tehran, Iran (Grant Number: 28489) | 34 | 91.2% (31/34 completed) | Mindfulness |
| Lin Latt et al. (2024) | Mindful self-hypnotherapy + resistance training, resistance training only, waitlist control | None reported | 44 | 68.2% (30/44 completed) | Stress, psychological distress, mindfulness |
| Study ID | Mean Age (Years) | Gender | Race | Participants Allocated to Intervention |
|---|---|---|---|---|
| Olendzki et al. (2020) | 19.6 | 35 (83.3%) female | White = 28 (66.7%); Hispanic/Latino = 8 (19.0%); Mixed race/ethnicity = 3 (7.1%); Black = 2 (4.8%); Asian = 2 (4.8%) | 22 |
| Slonena and Elkins (2021) | 19.5 | 43 (78.2%) female | White = 34 (61.8%); Hispanic/Latino = 10 (18.2); Asian = 8 (14.5); Black = 2 (3.6%); Native American/Alaskan Native = 1 (1.8%) | 33 |
| Khazraee et al. (2023a) | 32.06 | 34 (100%) female | Persian = 34 (100%) | 17 |
| Khazraee et al. (2023b) | 32.06 | 34 (100%) female | Persian = 34 (100%) | 17 |
| Lin Latt et al. (2024) | 21 | 44 (100%) female | White = 11 (30.4%); Black = 5 (16.7%); Hispanic/Latino = 7 (23.3%); Asian = 7 (23.3%) | 16 |
| Study ID | Study Aims | Intervention Sessions | Comparator | Home Practice | Inclusion Criteria | Exclusion Criteria |
|---|---|---|---|---|---|---|
| Olendzki et al. (2020) | (1) Investigate feasibility of MH; (2) investigate impact of MH on stress, psychological distress, and mindfulness compared to WLC | 8 weekly, 1 h, in-person sessions | Waitlist control | Instructed to practice daily using home practice CD | (1) Proficiency in English; (2) at least 18 years of age; (3) self-identify as being highly stressed, as indicated by a score of 50% or higher on a visual analog scale measuring overall stress | (1) Diagnostic indicators or a history of borderline personality disorder, psychosis, or schizophrenia |
| Slonena and Elkins (2021) | (1) Investigate impact of a brief MH intervention on stress reactivity relative to an active control condition; (2) compare brief MH intervention to active control in relaxation, mindfulness, intervention satisfaction, and home practice adherence | 2 weekly in-person sessions | Cognitive training (active control) | Instructed to listen to audio recording daily for one week | (1) At least 18 years of age; (2) proficient in English; (3) no prior experience with mindfulness or clinical hypnosis; (4) score > 18 on PSS | (1) Individuals with diagnostic indicators or a history of borderline personality disorder or psychosis; (2) those currently in psychotherapy treatment for major depressive disorder |
| Khazraee et al. (2023a) | Investigate the effectiveness of MH for depression, self-compassion, and psychological inflexibility in females with MDD | 8 weekly, 1 h, in-person sessions | Waitlist control | Given daily practice audio recordings based on the content presented that week | (1) Score > 28 on BDI-II, indicating severe levels of depression; (2) diagnosis of MDD, according to the DSM-5; (3) between 18 and 50 years old; (4) having at the least a diploma from a high school/secondary school; (5) if receiving psychiatric medication, the dosage and type of medication were stable in the last three months before the start of the study and remained steady during the study period; (6) available for 8 weekly sessions | (1) Unwillingness to continue treatment; (2) serious suicidal thoughts and any plan(s) to attempt suicide; (3) receiving psychological interventions in the last 6 months; (4) participation in another psychological intervention at the same time as study; (5) recent substance abuse; (6) diagnostic indicators or history of borderline personality disorder, bipolar disorder, psychosis, or schizophrenia |
| Khazraee et al. (2023b) | Investigate the effectiveness of MH intervention on difficulties in emotion regulation, mindfulness, and mental health in patients with MDD | 8 weekly, 1 h, in-person sessions | Waitlist control | Given audio recording of session material | (1) Score > 28 on BDI-II, indicating severe levels of depression; (2) diagnosis of MDD, according to the DSM-5; (3) between 18 and 50 years old; (4) having at the least a diploma from a high school/secondary school; (5) if receiving psychiatric medication, the dosage and type of medication were stable in the last three months before the start of the study and remained steady during the study period; (6) available for 8 weekly sessions | (1) Unwillingness to continue treatment; (2) serious suicidal thoughts and any plan(s) to attempt suicide; (3) receiving psychological interventions in the last 6 months; (4) participation in another psychological intervention at the same time as study; (5) recent substance abuse; (6) diagnostic indicators or history of borderline personality disorder, bipolar disorder, psychosis, or schizophrenia |
| Lin Latt et al. (2024) | (1) Investigate impact of mindful self-hypnotherapy combined with resistance training on perceived stress as measured by the PSS; (2) investigate whether this combination can improve psychological well-being and strength gains | 5 min hypnotherapy before and after the 15 RT sessions which occurred 3× per week for five weeks. A total of 5 sessions were performed with a supervisor, and 10 were performed on their own | Resistance training only (active control) and waitlist control | Given two self-guided 45–60 min sessions | (1) Full-time college students; (2) between 18 and 29 years old; (3) able to perform resistance training w/o health complications; (4) no previous experience of regular physical exercise in the past 6 months | (1) Previous diagnosis of serious psychiatric illnesses (e.g., bipolar disorder, borderline personality disorder, psychosis, or schizophrenia); (2) diagnosis of major depressive disorder in the past 5 years; (3) current substance use (including smoking cigarettes); (4) if participants were taking anti-anxiety or anti-depressant medication, they were asked to not change their dose for one month prior to and during the intervention; to not use additional hypnosis or meditation during the intervention; and to not begin taking supplements that could impact strength throughout the course of the intervention |
| Hedges’ g | 95% CI | p | Q | P | I2 | |
|---|---|---|---|---|---|---|
| Observing | 0.849 | 0.1866, 1.5110 | 0.012 | 10.07 | 0.02 | 67.76% |
| Describing | 0.649 | 0.2228, 1.0762 | 0.0029 | 4.05 | 0.26 | 27.96% |
| Acting with Awareness | 0.890 | 0.529, 1.252 | <0.0001 | 1.72 | 0.63 | 0.0% |
| Nonjudging | 0.95 | 0.1704, 1.7367 | 0.017 | 10.93 | 0.01 | 76.31% |
| Nonreactivity | 1.18 | 0.096, 2.266 | 0.03 | 9.04 | 0.01 | 79.37% |
| Patient or population: Adults aged 18 years of age or older Intervention: Mindful hypnotherapy interventions Comparator: Active, waitlist, or treatment as usual control Outcome: Symptoms of psychological distress; mindfulness Study design: Randomized control trials | ||||
| Outcomes | Effect size Hedges’ g | Significance | N participants | Quality of evidence (GRADE) |
| Psychological distress PDP, SUDS | Hedges’ g = 0.61, 95% CI [0.10, 1.12] | p = 0.018 | 141 | ⊕⊕⊖⊖ Low 1,2,3,4 |
| Stress PSS, WSI-SF | Hedges’ g = 0.75, 95% CI [0.34, 1.16] | p = 0.0003 | 175 | ⊕⊕⊖⊖ Low 1,2,3,4 |
| Mindfulness AAQ-II, FFMQ, KIMS | Hedges’ g = 1.38, 95% CI [0.83, 1.92] | p < 0.001 | 209 | ⊕⊕⊕⊖ Moderate 1,3,4,5,6,7 |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2026 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license.
Share and Cite
Padilla, V.J.; Muñiz, V.; Scheffrahn, K.; Elkins, G. Effect of Mindful Hypnotherapy on Psychological Distress: A Systematic Review and Meta-Analysis. Behav. Sci. 2026, 16, 107. https://doi.org/10.3390/bs16010107
Padilla VJ, Muñiz V, Scheffrahn K, Elkins G. Effect of Mindful Hypnotherapy on Psychological Distress: A Systematic Review and Meta-Analysis. Behavioral Sciences. 2026; 16(1):107. https://doi.org/10.3390/bs16010107
Chicago/Turabian StylePadilla, Victor Julián, Vanessa Muñiz, Katherine Scheffrahn, and Gary Elkins. 2026. "Effect of Mindful Hypnotherapy on Psychological Distress: A Systematic Review and Meta-Analysis" Behavioral Sciences 16, no. 1: 107. https://doi.org/10.3390/bs16010107
APA StylePadilla, V. J., Muñiz, V., Scheffrahn, K., & Elkins, G. (2026). Effect of Mindful Hypnotherapy on Psychological Distress: A Systematic Review and Meta-Analysis. Behavioral Sciences, 16(1), 107. https://doi.org/10.3390/bs16010107





