Population Perspectives on Impact of the COVID-19 Pandemic on Essential Health Services—Behavioral Insights from the Federation of Bosnia and Herzegovina
Abstract
1. Introduction
2. Methods
2.1. Study Design, Population, and Data Collection
2.2. Data Analysis
2.3. Ethical Considerations
3. Results
3.1. Demographic Characteristics
Access to Care
3.2. Out-of-Pocket Expenses for Health Care
3.3. Postponements of Health Care
3.4. Mental Health
3.5. Satisfaction with Health Care
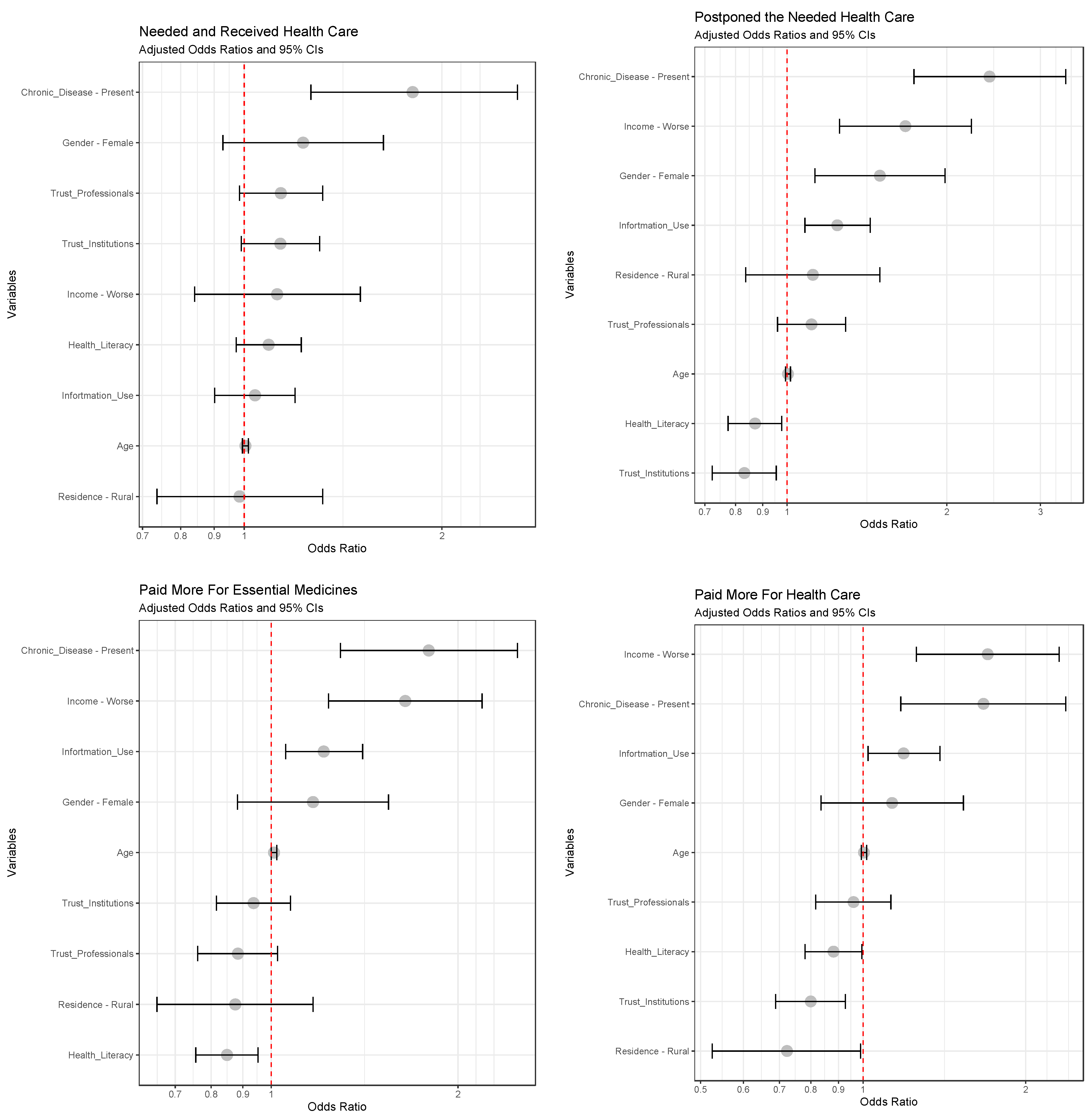
3.6. Predictors of Need and Access to Health Care
4. Discussion
4.1. Main Findings
4.2. Interpretation and Comparison with Published Literature
4.3. Study Limitations
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
Disclaimer
Open Access Statement
References
- WHO. WHO Coronavirus (COVID-19) Dashboard. Available online: https://covid19.who.int/ (accessed on 10 December 2021).
- WHO. Second Round of the National Pulse Survey on Continuity of Essential Health Services during the COVID-19 Pandemic. 2021. Available online: https://www.who.int/publications/i/item/WHO-2019-nCoV-EHS-continuity-survey-2021.1 (accessed on 10 December 2021).
- Bilinski, A.; Emanuel, E.J. COVID-19 and Excess All-Cause Mortality in the US and 18 Comparison Countries. JAMA 2020, 324, 2100–2102. [Google Scholar] [CrossRef] [PubMed]
- Karlinsky, A.; Kobak, D. Tracking excess mortality across countries during the COVID-19 pandemic with the World Mortality Dataset. Elife 2021, 10, e69336. [Google Scholar] [CrossRef] [PubMed]
- Kontis, V.; Bennett, J.E.; Rashid, T.; Parks, R.M.; Pearson-Stuttard, J.; Guillot, M.; Asaria, P.; Zhou, B.; Battaglini, M.; Corsetti, G.; et al. Magnitude, demographics and dynamics of the effect of the first wave of the COVID-19 pandemic on all-cause mortality in 21 industrialized countries. Nat. Med. 2020, 26, 1919–1928. [Google Scholar] [CrossRef]
- Tanne, J.H. Covid-19: At least two thirds of 225 000 excess deaths in US were due to virus. BMJ 2020, 371, m3948. [Google Scholar] [CrossRef] [PubMed]
- WHO. National Pulse Survey on Continuity of Essential Health Services during the COVID-19 Pandemic. 2020. Available online: https://www.who.int/teams/integrated-health-services/monitoring-health-services/national-pulse-survey-on-continuity-of-essential-health-services-during-the-covid-19-pandemic (accessed on 10 December 2021).
- Institute for Public Health, Federation of Bosnia and Herzegovina. Health Statistics Annual Report, Federation of Bosnia and Herzegovina 2019; Institute for Public Health, Federation of Bosnia and Herzegovina: Sarajevo, Bosnia and Herzegovina, 2019. [Google Scholar]
- Institute for Public Health, Federation of Bosnia and Herzegovina. Health Statistics Annual Report, Federation of Bosnia and Herzegovina 2020; Institute for Public Health, Federation of Bosnia and Herzegovina: Sarajevo, Bosnia and Herzegovina, 2020. [Google Scholar]
- Betsch, C.; Wieler, L.H.; Habersaat, K.; on behalf of the COSMO group. Monitoring behavioural insights related to COVID-19. Lancet 2020, 395, 1255–1256. [Google Scholar] [CrossRef]
- Cilovic-Lagarija, S.; Hasanica, N.; Mulic, M.; Radojicic, M.; Brankovic, S.; Pilav, A.; Huseinagic, S.; Musa, S. An Overview of Human Resources and Capacity in Health Care Institutions in the Federation of Bosnia and Herzegovina in the Context of Responding to the COVID 19 Pandemic. Mater. Sociomed. 2021, 33, 56–59. [Google Scholar] [CrossRef]
- Institute for Public Health FB&H. Health Status of the Population and Health Care in FB&H in 2018. 2018. Available online: http://www.zzjzfbih.ba/wp-content/uploads/2018/10/Zdravstveno-2017 (accessed on 10 December 2021).
- WHO. Survey Tool and Guidance: Behavioural Insights on COVID-19, 29 July 2020 (produced by the WHO European Region). 2020. Available online: https://www.euro.who.int/en/health-topics/health-determinants/behavioural-and-cultural-insights-for-health/tools-and-resources/who-tool-for-behavioural-insights-on-covid-19/survey-tool-and-guidance-behavioural-insights-on-covid-19-produced-by-the-who-european-region (accessed on 10 December 2021).
- CDC. The National Health Interview Survey (NHIS). 2020. Available online: https://www.cdc.gov/nchs/nhis/index.htm (accessed on 10 December 2021).
- Šeila Cilović Lagarija, E.K.; Hasanica, N.; Begagić, S.; Džubur-Alić, A.; Lisica, D. A Study of Patient Satisfaction With Healthcare in Zenica-Doboj Canton. Southeast. Eur. Med. J. 2020, 4, 129–135. [Google Scholar]
- Spasojevic, N.; Hrabac, B.; Huseinagic, S. Patient’s Satisfaction with Health Care: A Questionnaire Study of Different Aspects of Care. Mater. Sociomed. 2015, 27, 220–224. [Google Scholar] [CrossRef]
- Team, R.C. R: A Language and Environment for Statistical Computing. Available online: https://www.r-project.org/ (accessed on 10 December 2021).
- ICC. ICC/ESOMAR International Code on Market and Social Research. Available online: https://iccwbo.org/publication/iccesomar-international-code-on-market-and-social-research (accessed on 10 December 2021).
- WHO. Bosnia and Herzegovina: Assessing Health Systems Capacity to Manage Large Influx of Refugees and Migrants. 2020. Available online: https://www.euro.who.int/en/publications/abstracts/bosnia-and-herzegovina-assessing-health-systems-capacity-to-manage-large-influx-of-refugees-and-migrants-2020 (accessed on 10 December 2021).
- Hukic, M.; Ponjavic, M.; Tahirovic, E.; Karabegovic, A.; Ferhatbegovic, E.; Travar, M.; Serdarevic, F. SARS-CoV-2 virus outbreak and the emergency public health measures in Bosnia and Herzegovina: January–July, 2020. Bosn. J. Basic Med. Sci. 2021, 21, 111–116. [Google Scholar] [CrossRef]
- Toromanovic, S.; Masic, I.; Novo, A.; Pilav, A.; Jokic, I. Health Care System in federation of Bosnia and Herzegovina. Mater. Socio Med. 2006, 18, 212–218. [Google Scholar]
- Universal Health Coverage Collaborators. Measuring universal health coverage based on an index of effective coverage of health services in 204 countries and territories, 1990–2019: A systematic analysis for the Global Burden of Disease Study 2019. Lancet 2020, 396, 1250–1284. [Google Scholar] [CrossRef]
- Eurostat. Healthcare Personnel Statistics—Physicians. Available online: https://ec.europa.eu/eurostat/statistics-explained/pdfscache/37382.pdf (accessed on 10 December 2021).
- Rossi, R.; Socci, V.; Pacitti, F.; Mensi, S.; Di Marco, A.; Siracusano, A.; Di Lorenzo, G. Mental Health Outcomes Among Healthcare Workers and the General Population During the COVID-19 in Italy. Front. Psychol. 2020, 11, 608986. [Google Scholar] [CrossRef] [PubMed]
- Shaukat, N.; Ali, D.M.; Razzak, J. Physical and mental health impacts of COVID-19 on healthcare workers: A scoping review. Int. J. Emerg. Med. 2020, 13, 40. [Google Scholar] [CrossRef]
- Chew, N.W.S.; Lee, G.K.H.; Tan, B.Y.Q.; Jing, M.; Goh, Y.; Ngiam, N.J.H.; Yeo, L.L.L.; Ahmad, A.; Ahmed Khan, F.; Napolean Shanmugam, G.; et al. A multinational, multicentre study on the psychological outcomes and associated physical symptoms amongst healthcare workers during COVID-19 outbreak. Brain. Behav. Immun. 2020, 88, 559–565. [Google Scholar] [CrossRef] [PubMed]
- Gomez-Ochoa, S.A.; Franco, O.H.; Rojas, L.Z.; Raguindin, P.F.; Roa-Diaz, Z.M.; Wyssmann, B.M.; Guevara, S.L.R.; Echeverria, L.E.; Glisic, M.; Muka, T. COVID-19 in Health-Care Workers: A Living Systematic Review and Meta-Analysis of Prevalence, Risk Factors, Clinical Characteristics, and Outcomes. Am. J. Epidemiol. 2021, 190, 161–175. [Google Scholar] [CrossRef] [PubMed]
- WHO. Health Workforce Policy and Management in the Context of the COVID-19 Pandemic Response: Interim Guidance. 3 December 2020. Available online: https://apps.who.int/iris/handle/10665/337333 (accessed on 10 December 2021).
- WHO. Health Workers in Focus: Policies and Practices for Successful Public Response to COVID-19 Vaccination: Strategic Considerations for Member States in the WHO European Region (2021) (produced by WHO/Europe). 2020. Available online: https://www.euro.who.int/en/health-topics/health-determinants/behavioural-and-cultural-insights-for-health/tools-and-resources/health-workers-in-focus-policies-and-practices-for-successful-public-response-to-covid-19-vaccination-strategic-considerations-for-member-states-in-the-who-european-region-2021-produced-by-whoeurope (accessed on 10 December 2021).
- CDC. Strategies to Mitigate Healthcare Personnel Staffing Shortages. 2021. Available online: https://www.cdc.gov/coronavirus/2019-ncov/hcp/mitigating-staff-shortages.html (accessed on 10 December 2021).
- GBD. Bosnia and Herzegovina Country Profile. Available online: http://www.healthdata.org/bosnia-and-herzegovina (accessed on 10 December 2021).
- WHO. The Impact of the COVID-19 Pandemic on Noncommunicable Disease Resources and Services: Results of a Rapid Assessment; WHO: Geneva, Switzerland, 2020. [Google Scholar]
- WHO. Living Guidance for Clinical Management of COVID-19. 2021. Available online: https://www.who.int/publications/i/item/WHO-2019-nCoV-clinical-2021-2 (accessed on 10 December 2021).
- Clark, A.; Jit, M.; Warren-Gash, C.; Guthrie, B.; Wang, H.H.X.; Mercer, S.W.; Sanderson, C.; McKee, M.; Troeger, C.; Ong, K.L.; et al. Global, regional, and national estimates of the population at increased risk of severe COVID-19 due to underlying health conditions in 2020: A modelling study. Lancet Glob. Health 2020, 8, e1003–e1017. [Google Scholar] [CrossRef] [PubMed]
- Chudasama, Y.V.; Gillies, C.L.; Zaccardi, F.; Coles, B.; Davies, M.J.; Seidu, S.; Khunti, K. Impact of COVID-19 on routine care for chronic diseases: A global survey of views from healthcare professionals. Diabetes Metab. Syndr. 2020, 14, 965–967. [Google Scholar] [CrossRef]
- Katzmarzyk, P.T.; Salbaum, J.M.; Heymsfield, S.B. Obesity, noncommunicable diseases, and COVID-19: A perfect storm. Am. J. Hum. Biol. 2020, 32, e23484. [Google Scholar] [CrossRef]
- Sheldon, T.A.; Wright, J. Twin epidemics of covid-19 and non-communicable disease. BMJ 2020, 369, m2618. [Google Scholar] [CrossRef]
- NCD Alliance. A Global NCD Agenda for Resilience and Recovery from COVID-19. NCD Alliance. 2021. Available online: https://ncdalliance.org/sites/default/files/NCDA%20Resilience%20and%20Recovery.pdf (accessed on 10 December 2021).
- Kardas, P.; van Boven, J.F.M.; Pinnock, H.; Menditto, E.; Wettermark, B.; Tsiligianni, I.; Agh, T.; ENABLE collaborators. Disparities in European healthcare system approaches to maintaining continuity of medication for non-communicable diseases during the COVID-19 outbreak. Lancet Reg. Health Eur. 2021, 4, 100099. [Google Scholar] [CrossRef]
- WHO. Maintaining Essential Health Services: Operational Guidance for the COVID-19 Context, Interim Guidance. 2020. Available online: https://www.who.int/publications/i/item/WHO-2019-nCoV-essential_health_services-2020.2 (accessed on 10 December 2021).
- Musa, S.; Cilovic-Lagarija, S.; Kavazovic, A.; Bosankic-Cmajcanin, N.; Stefanelli, A.; Scott, N.A.; Scherzer, M.; Kiss, Z.; Habersaat, K.B. COVID-19 Risk Perception, Trust in Institutions and Negative Affect Drive Positive COVID-19 Vaccine Intentions. Int. J. Public Health 2022, 67, 1604231. [Google Scholar] [CrossRef] [PubMed]
- Maddock, J.; Parsons, S.; Di Gessa, G.; Green, M.J.; Thompson, E.J.; Stevenson, A.J.; Kwong, A.S.; McElroy, E.; Santorelli, G.; Silverwood, R.J.; et al. Inequalities in healthcare disruptions during the COVID-19 pandemic: Evidence from 12 UK population-based longitudinal studies. BMJ Open 2022, 12, e064981. [Google Scholar]
- Gausman, J.; Langer, A. Sex and Gender Disparities in the COVID-19 Pandemic. J. Womens Health (Larchmt.) 2020, 29, 465–466. [Google Scholar] [CrossRef] [PubMed]
- Chmielewska, B.; Barratt, I.; Townsend, R.; Kalafat, E.; van der Meulen, J.; Gurol-Urganci, I.; O’Brien, P.; Morris, E.; Draycott, T.; Thangaratinam, S.; et al. Effects of the COVID-19 pandemic on maternal and perinatal outcomes: A systematic review and meta-analysis. Lancet Glob. Health 2021, 9, e759–e772. [Google Scholar] [CrossRef] [PubMed]
- Thornton, J. COVID-19: Millions of women and children at risk as visits to essential services plummet. BMJ 2020, 369, m2171. [Google Scholar] [CrossRef]
- Beth Prusaczyk, B.C.; Morrow-Howell, N.; Lenze, E. Disruptions to Care and the Use of Telehealth Among Older Adults During the COVID-19 Pandemic. Innov. Aging 2020, 4 (Suppl. S1), 943. [Google Scholar] [CrossRef]
- IHME. Estimation of Excess Mortality Due to COVID-19. 2021. Available online: http://www.healthdata.org/special-analysis/estimation-excess-mortality-due-covid-19-and-scalars-reported-covid-19-deaths (accessed on 10 December 2021).
- Studies IfF. COVID-19 and Disruptions to the Health and Social Care of Older People in England. 2020. Available online: https://ifs.org.uk/publications/15160 (accessed on 10 December 2021).
- Mujkic, S.; Marinkovic, V. Critical Appraisal of Reimbursement List in Bosnia and Herzegovina. Front Pharm. 2017, 8, 129. [Google Scholar] [CrossRef]
- WHO. Spending on Health in Europe: Entering a New Era. 2021. Available online: https://apps.who.int/iris/bitstream/handle/10665/340910/9789289055079-eng.pdf (accessed on 10 December 2021).
- El-Khatib, Z.; Otu, A.; Neogi, U.; Yaya, S. The Association between Out-of-Pocket Expenditure and COVID-19 Mortality Globally. J. Epidemiol. Glob. Health 2020, 10, 192–193. [Google Scholar] [CrossRef]

| Variable Name | Sex of Respondents (n, %) | |||
|---|---|---|---|---|
| Males 514 (48%) | Females 554 (52%) | Total 1068 | p-Value | |
| Access to health care | ||||
| Needed and received care (n, % Yes) | 314/514 (61%) | 372/554 (67%) | 686/1068 (64%) | 0.046 |
| Way of not getting needed care (n, % Yes) | ||||
| Postponed visit to the family doctor | 100/200 (50%) | 97/182 (53%) | 197/382 (52%) | 0.588 |
| Postponed planned surgery | 32/200 (16%) | 27/182 (15%) | 59/382 (15%) | 0.863 |
| Not able to book an appointment at family doctor, specialist, hospital | 107/200 (54%) | 99/182 (54%) | 206/382 (54%) | 0.942 |
| Needed medication was not available | 36/200 (18%) | 33/182 (18%) | 69/382 (18%) | 1 |
| Other | 65/200 (33%) | 57/182 (31%) | 122/382 (32%) | 0.891 |
| Increased out-of-pocket expenses for medicines (n, % Yes) | 188/483 (39%) | 225/530 (42%) | 413/1013 (41%) | 0.281 |
| Increased out-of-pocket expenses for health services (n, % Yes) | 137/479 (29%) | 166/523 (32%) | 303/1002 (30%) | 0.312 |
| Postponements of care | ||||
| Postponed medical care (n, % Yes) | 165/514 (32%) | 239/554 (43%) | 404/1068 (38%) | <0.001 |
| Main reason for postponement (n, % Yes) * | ||||
| Condition was not serious enough | 129/165 (78%) | 202/239 (85%) | 331/404 (82%) | 0.135 |
| No appointment/long waiting time | 122/165 (74%) | 154/239 (64%) | 276/404 (68%) | 0.056 |
| Facility was closed | 67/165 (41%) | 70/239 (29%) | 137/404 (34%) | 0.024 |
| Fear of infection with SARS-CoV-2 | 108/165 (65%) | 168/239 (70%) | 276/404 (68%) | 0.358 |
| Other | 42/165 (25%) | 47/239 (20%) | 89/404 (22%) | 0.208 |
| Mental health | ||||
| Taking prescription medication to help with emotions, concentration, behavior, or mental health (n, % Yes) | 63/493 (13%) | 94/539 (17%) | 157/1032 (15%) | 0.046 |
| Receiving counselling or therapy from a mental health professional in past 9 months (n, % Yes) | 30/498 (6%) | 33/541 (6%) | 63/1039 (6%) | 1 |
| Currently receiving counselling or therapy from a mental health professional (n, % Yes) | 22/496 (4%) | 22/544 (4%) | 44/1040 (4%) | 0.874 |
| Variable Name | Residence of Respondents (n, %) | |||
|---|---|---|---|---|
| Rural 398 (37%) | Urban 670 (63%) | Total 1068 | p-Value | |
| Access to health care | ||||
| Needed and received care (n, % Yes) | 258/398 (65%) | 428/670 (64%) | 686/1068 (64%) | 0.806 |
| Way of not getting needed care (n, % Yes) | ||||
| Postponed visit to the family doctor | 70/140 (50%) | 127/242 (52%) | 197/382 (52%) | 0.718 |
| Postponed planned surgery | 16/140 (11%) | 43/242 (18%) | 59/382 (15%) | 0.132 |
| Not able to book an appointment at family doctor, specialist, hospital | 76/140 (54%) | 130/242 (54%) | 206/382 (54%) | 1 |
| Needed medication was not available | 18/140 (13%) | 51/242 (21%) | 69/382 (18%) | 0.061 |
| Other | 47/140 (34%) | 75/242 (31%) | 122/382 (32%) | 0.684 |
| Increased out-of-pocket expenses for medicines (n, % Yes) | 149/379 (39%) | 264/634 (42%) | 413/1013 (41%) | 0.507 |
| Increased out-of-pocket expenses for health services (n, % Yes) | 99/377 (26%) | 204/625 (33%) | 303/1002 (30%) | 0.040 |
| Postponements of care | ||||
| Postponed medical care (n, % Yes) | 156/398 (39%) | 248/670 (37%) | 404/1068 (38%) | 0.519 |
| Main reason for postponement (n, % Yes) | ||||
| Condition was not serious enough | 125/156 (80%) | 206/248 (83%) | 331/404 (82%) | 0.539 |
| No appointment/long waiting time | 104/156 (67%) | 172/248 (69%) | 276/404 (68%) | 0.649 |
| Facility was closed | 57/156 (37%) | 80/248 (32%) | 137/404 (34%) | 0.437 |
| Fear of infection with SARS-CoV-2 | 104/156 (67%) | 172/248 (69%) | 276/404 (68%) | 0.649 |
| Other | 31/156 (20%) | 58/248 (23%) | 89/404 (22%) | 0.480 |
| Mental health | ||||
| Taking prescription medication to help with emotions, concentration, behavior, or mental health (n, % Yes) | 48/382 (13%) | 109/650 (17%) | 157/1032 (15%) | 0.084 |
| Receiving counselling or therapy from a mental health professional in past 9 months (n, % Yes) | 22/390 (6%) | 41/649 (6%) | 63/1039 (6%) | 0.758 |
| Currently receiving counselling or therapy from a mental health professional (n, % Yes) | 18/389 (5%) | 26/651 (4%) | 44/1040 (4%) | 0.740 |
| Variable Name | Chronic Disease Present (n, %) | |||
|---|---|---|---|---|
| No 731 (76%) | Yes 237 (24%) | Total 968 | p-Value | |
| Access to health care | ||||
| Needed and received care (n, % Yes) | 447/731 (61%) | 178/237 (75%) | 625/968 (65%) | <0.001 |
| Way of not getting needed care (n, % Yes) | ||||
| Postponed visit to the family doctor | 138/284 (49%) | 37/59 (63%) | 175/343 (51%) | 0.067 |
| Postponed planned surgery | 41/284 (14%) | 10/59 (17%) | 51/343 (15%) | 0.770 |
| Not able to book an appointment at family doctor, specialist, hospital | 141/284 (50%) | 44/59 (75%) | 185/343 (54%) | <0.001 |
| Needed medication was not available | 47/284 (17%) | 12/59 (20%) | 59/343 (17%) | 0.608 |
| Other | 89/284 (31%) | 19/59 (32%) | 108/343 (31%) | 1 |
| Increased out-of-pocket expenses for medicines (n, % Yes) | 245/691 (35%) | 124/233 (53%) | 369/924 (40%) | <0.001 |
| Increased out-of-pocket expenses for health services (n, % Yes) | 184/690 (27%) | 85/220 (39%) | 269/910 (30%) | <0.001 |
| Postponements of care | ||||
| Postponed medical care (n, % Yes) | 229/731 (31%) | 130/237 (55%) | 359/968 (37%) | <0.001 |
| Main reason for postponement (n, % Yes) | ||||
| Condition was not serious enough | 199/229 (87%) | 96/130 (74%) | 295/359 (82%) | 0.003 |
| No appointment/long waiting time | 152/229 (66%) | 92/130 (71%) | 244/359 (68%) | 0.459 |
| Facility was closed | 74/229 (32%) | 49/130 (38%) | 123/359 (34%) | 0.360 |
| Fear of infection with SARS-CoV-2 | 155/229 (68%) | 87/130 (67%) | 242/359 (67%) | 0.975 |
| Other | 47/229 (21%) | 30/130 (23%) | 77/359 (21%) | 0.665 |
| Mental health | ||||
| Taking prescription medication to help with emotions, concentration, behavior, or mental health (n, % Yes) | 87/713 (12%) | 53/229 (23%) | 140/942 (15%) | <0.001 |
| Receiving counselling or therapy from a mental health professional in past 9 months (n, % Yes) | 35/711 (5%) | 20/235 (9%) | 55/946 (6%) | 0.061 |
| Currently receiving counselling or therapy from a mental health professional (n, % Yes) | 27/710 (4%) | 13/235 (6%) | 40/945 (4%) | 0.34 |
| Variable Name | Age Group of Respondents (n, %) | ||||
|---|---|---|---|---|---|
| 18–34 Years 327 (31%) | 35–54 Years 473 (44%) | 55+ Years 268 (25%) | Total 1068 | p-Value | |
| Access to health care | |||||
| Needed and received care (n, % Yes) | 191/327 (58%) | 316/473 (67%) | 179/268 (67%) | 686/1068 (64%) | 0.031 |
| Way of not getting needed care (n, % Yes) | |||||
| Postponed visit to the family doctor | 64/136 (47%) | 90/157 (57%) | 43/89 (48%) | 197/382 (52%) | 0.168 |
| Postponed planned surgery | 21/136 (15%) | 25/157 (16%) | 13/89 (15%) | 59/382 (15%) | 0.963 |
| Not able to book an appointment at family doctor, specialist, hospital | 61/136 (45%) | 91/157 (58%) | 54/89 (61%) | 206/382 (54%) | 0.028 |
| Needed medication was not available | 26/136 (19%) | 21/157 (13%) | 22/89 (25%) | 69/382 (18%) | 0.078 |
| Other | 32/136 (24%) | 52/157 (33%) | 38/89 (43%) | 122/382 (32%) | 0.010 |
| Increased out-of-pocket expenses for medicines (n, % Yes) | 99/303 (33%) | 196/453 (43%) | 118/257 (46%) | 413/1013 (41%) | 0.002 |
| Increased out-of-pocket expenses for health services (n, % Yes) | 76/305 (25%) | 141/442 (32%) | 86/255 (34%) | 303/1002 (30%) | 0.046 |
| Postponements of care | |||||
| Postponed medical care (n, % Yes) | 103/327 (31%) | 185/473 (39%) | 116/268 (43%) | 404/1068 (38%) | 0.010 |
| Main reason for postponement (n, % Yes) | |||||
| Condition was not serious enough | 88/103 (85%) | 154/185 (83%) | 89/116 (77%) | 331/404 (82%) | 0.202 |
| No appointment/long waiting time | 71/103 (69%) | 122/185 (66%) | 83/116 (72%) | 276/404 (68%) | 0.589 |
| Facility was closed | 42/103 (41%) | 61/185 (33%) | 34/116 (29%) | 137/404 (34%) | 0.189 |
| Fear of infection with SARS-CoV-2 | 72/103 (70%) | 126/185 (68%) | 78/116 (67%) | 276/404 (68%) | 0.912 |
| Other | 22/103 (21%) | 35/185 (19%) | 32/116 (28%) | 89/404 (22%) | 0.207 |
| Mental health | |||||
| Taking prescription medication to help with emotions, concentration, behavior, or mental health (n, % Yes) | 37/314 (12%) | 74/459 (16%) | 46/259 (18%) | 157/1032 (15%) | 0.108 |
| Receiving counselling or therapy from a mental health professional in past 9 months (n, % Yes) | 20/312 (6%) | 32/466 (7%) | 11/261 (4%) | 63/1039 (6%) | 0.340 |
| Currently receiving counselling or therapy from a mental health professional (n, % Yes) | 14/307 (5%) | 20/469 (4%) | 10/264 (4%) | 44/1040 (4%) | 0.900 |
| Score | Gender | Residence | Age Group | Chronic Disease | Total | |||||
|---|---|---|---|---|---|---|---|---|---|---|
| Males | Females | Urban | Rural | 18–34 | 35–54 | 55+ | YES | NO | ||
| Mean Score (95% CI) | 3.2 (3.1–3.3) | 3.2 (3.1–3.4) | 3.2 (3.1–3.4) | 3.2 (3.1–3.3) | 3.2 (3.1–3.4) | 3.2 (3.1–3.3) | 3.2 (3.1–3.4) | 3.3 (3.1–3.4) | 3.3 (3.1–3.4) | 3.2 (3.2–3.3) |
| p-value | 0.745 | 0.810 | 0.947 | 0.936 | ||||||
| Predictor | Needed and Received Health Care | Postponed the Needed Health Care | Increased Expenses for Essential Medicines | Increased Expenses for Health Care | ||||
|---|---|---|---|---|---|---|---|---|
| OR (95% CI) | p-value | OR (95% CI) | p-Value | OR (95% CI) | p-value | OR (95% CI) | p-Value | |
| Age | 1.01 (1.002–1.02) | 0.016 | 1.01 (1.002–1.02) | <0.01 | 1.01 (1.01–1.02) | <0.01 | 1.01 (1.004–1.02) | 0.04 |
| Sex | ||||||||
| Female (vs. Male) | 1.3 (1.03–1.7) | 0.039 | 1.6 (1.2–2.1) | <0.001 | 1.2 (0.9–1.5) | 0.254 | 1.2 (0.9–1.5) | 0.28 |
| Education | ||||||||
| Primary/HS (vs. College) | 1.08 (0.81–1.44) | 0.569 | 0.85 (0.64–1.13) | 0.282 | 0.83 (0.62–1.1) | 0.205 | 0.51 (0.38–0.69) | <0.001 |
| Residence | ||||||||
| Rural (vs. Urban) | 1.04 (0.8–1.35) | 0.756 | 1.1 (0.84–1.4) | 0.477 | 0.91 (0.7–1.2) | 0.466 | 0.73 (0.55–0.98) | 0.035 |
| Income | ||||||||
| Worse (vs. Same/improved) | 1.09 (0.78–1.31) | 0.946 | 1.8 (1.4–2.3) | <0.001 | 1.9 (1.5–2.5) | <0.001 | 1.8 (1.4–2.4) | <0.001 |
| Chronic disease | ||||||||
| Present (vs. No) | 1.91 (1.38–2.66) | <0.001 | 2.7 (2–3.6) | <0.001 | 2.1 (1.5–2.8) | <0.001 | 1.7 (1.3–2.4) | <0.001 |
| Health Literacy | ||||||||
| Point increase (7-point scale) | 1.2 (1.1–1.4) | <0.001 | 0.9 (0.82–0.98) | 0.025 | 0.85 (0.77–0.93) | <0.01 | 0.82 (0.74–0.9) | <0.001 |
| Information Use | ||||||||
| Point increase (7-point scale) | 1.2 (1.1–1.4) | <0.001 | 1.1 (1.04–1.2) | <0.01 | 1.03 (0.96–1.1) | 0.393 | 0.97 (0.89–1.06) | 0.484 |
| Trust in Professionals | ||||||||
| Point increase (7-point scale) | 1.3 (1.2–1.4) | <0.001 | 1.08 (1.01–1.2) | 0.032 | 0.95 (0.88–1.03) | 0.251 | 0.92 (0.84–0.99) | 0.038 |
| Trust in Institutions | ||||||||
| Point increase (8-point scale) | 1.3 (1.2–1.4) | <0.001 | 0.95 (0.88–1.04) | 0.302 | 0.92 (0.85–0.99) | 0.047 | 0.82 (0.75–0.9) | <0.001 |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2022 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Cilović-Lagarija, Š.; Musa, S.; Hasanica, N.; Čerkez, G.; Palo, M.; Majdan, M.; Scherzer, M.; Habersaat, K.B.; Smallwood, C.; Tahirukaj, A.; et al. Population Perspectives on Impact of the COVID-19 Pandemic on Essential Health Services—Behavioral Insights from the Federation of Bosnia and Herzegovina. Behav. Sci. 2022, 12, 495. https://doi.org/10.3390/bs12120495
Cilović-Lagarija Š, Musa S, Hasanica N, Čerkez G, Palo M, Majdan M, Scherzer M, Habersaat KB, Smallwood C, Tahirukaj A, et al. Population Perspectives on Impact of the COVID-19 Pandemic on Essential Health Services—Behavioral Insights from the Federation of Bosnia and Herzegovina. Behavioral Sciences. 2022; 12(12):495. https://doi.org/10.3390/bs12120495
Chicago/Turabian StyleCilović-Lagarija, Šeila, Sanjin Musa, Nino Hasanica, Goran Čerkez, Mirza Palo, Marek Majdan, Martha Scherzer, Katrine Bach Habersaat, Catherine Smallwood, Ardita Tahirukaj, and et al. 2022. "Population Perspectives on Impact of the COVID-19 Pandemic on Essential Health Services—Behavioral Insights from the Federation of Bosnia and Herzegovina" Behavioral Sciences 12, no. 12: 495. https://doi.org/10.3390/bs12120495
APA StyleCilović-Lagarija, Š., Musa, S., Hasanica, N., Čerkez, G., Palo, M., Majdan, M., Scherzer, M., Habersaat, K. B., Smallwood, C., Tahirukaj, A., & Nitzan, D. (2022). Population Perspectives on Impact of the COVID-19 Pandemic on Essential Health Services—Behavioral Insights from the Federation of Bosnia and Herzegovina. Behavioral Sciences, 12(12), 495. https://doi.org/10.3390/bs12120495





