Commensal Neisseria Are Shared between Sexual Partners: Implications for Gonococcal and Meningococcal Antimicrobial Resistance
Abstract
1. Introduction
2. Results
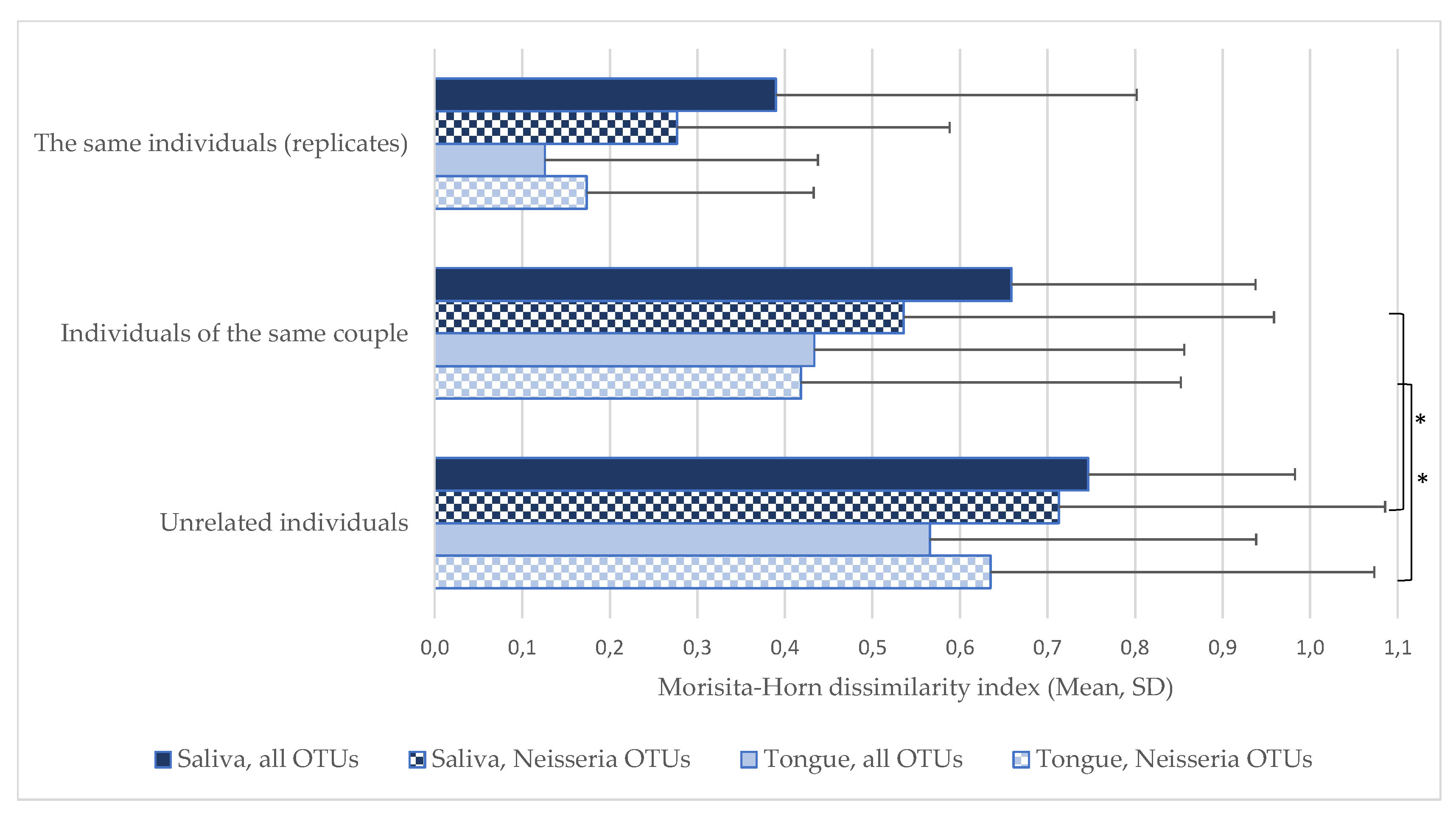
- A high pairwise similarity (an MHi value close to zero) between duplicate samples of an individual’s tongue surface (MHi 0.17) and saliva (MHi 0.28) indicated that sampling was reproducible at the level of the genus Neisseria (Figure 1).
- Partners’ oral Neisseria communities sampled after a 10-second kiss were not more similar than before the kiss (saliva: average MHi 0.55 before versus 0.53 after, p = 0.704; surface of the tongue: average MHi 0.39 before versus 0.45 after, p = 0.597; Figure 1). Therefore, samples before and after kissing were combined in the subsequent analyses.
- Partners’ oral Neisseria communities were more similar compared to unrelated individuals. This was found for saliva (average MHi 0.54 versus 0.71, respectively, p = 0.005) and for samples of the tongue surface (average MHi 0.42 versus 0.63, respectively, p = 0.006; Figure 1).
3. Discussion
4. Materials and Methods
4.1. Sample Collection and Processing
4.2. Availability of Data and Materials
4.3. Assessment of Community Similarity
4.4. Statistical Analysis
4.5. Ethics Approval and Consent to Participate
Author Contributions
Funding
Conflicts of Interest
Abbreviations
| AMR | antimicrobial resistance |
| MSM | men who have sex with men |
| OTU | operational taxonomic unit |
| MHi | Morisita–Horn index |
References
- Wi, T.; Lahra, M.M.; Ndowa, F.; Bala, M.; Dillon, J.A.R.; Ramon-Pardo, P.; Eremin, S.R.; Bolan, G.; Unemo, M. Antimicrobial resistance in Neisseria gonorrhoeae: Global surveillance and a call for international collaborative action. PLoS Med. 2017, 14, e1002344. [Google Scholar] [CrossRef]
- Verma, D.; Garg, P.K.; Dubey, A.K. Insights into the human oral microbiome. Arch. Microbiol. 2018, 200, 525–540. [Google Scholar] [CrossRef]
- Sâez, J.A.; Carmen, N.; Vinde, M.A. Multicolonization of human nasopharynx due to Neisseria spp. Int. Microbiol. 1998, 1, 59–63. [Google Scholar] [CrossRef]
- Dong, H.V.; Pham, L.Q.; Nguyen, H.T.; Nguyen, M.X.B.; Nguyen, T.V.; May, F.; Le, G.M.; Klausner, J.D. Decreased Cephalosporin Susceptibility of Oropharyngeal Neisseria Species in Antibiotic-using Men Who Have Sex With Men in Hanoi, Vietnam. Clin. Infect. Dis. 2019. [Google Scholar] [CrossRef]
- Lewis, D.A. The role of core groups in the emergence and dissemination of antimicrobial-resistant N gonorrhoeae. Sex. Transm. Infect. 2013, 89. [Google Scholar] [CrossRef]
- Zhang, L.; Regan, D.G.; Chow, E.P.; Gambhir, M.; Cornelisse, V.; Grulich, A.; Ong, J.; Lewis, D.A.; Hocking, J.; Fairley, C.K. Neisseria gonorrhoeae Transmission among Men Who Have Sex with Men: An Anatomical Site-Specific Mathematical Model Evaluating the Potential Preventive Impact of Mouthwash. Sex. Transm. Dis. 2017, 44, 586–592. [Google Scholar] [CrossRef]
- Fairley, C.K.; Cornelisse, V.J.; Hocking, J.S.; Chow, E.P.F. Models of gonorrhoea transmission from the mouth and saliva. Lancet Infect. Dis. 2019, 1–7. [Google Scholar] [CrossRef]
- Kenyon, C. We need to consider collateral damage to resistomes when we decide how frequently to screen for chlamydia/gonorrhoea in PrEP cohorts. AIDS 2019, 33, 155–157. [Google Scholar] [CrossRef]
- Tully, J.; Viner, R.M.; Coen, P.G.; Stuart, J.M.; Zambon, M.; Peckham, C.; Booth, C.; Klein, N.; Kaczmarski, E.; Booy, R. Risk and protective factors for meningococcal disease in adolescents: Matched cohort study. Br. Med. J. 2006, 332, 445–448. [Google Scholar] [CrossRef]
- Mandal, S.; Wu, H.M.; MacNeil, J.R.; Machesky, K.; Garcia, J.; Plikaytis, B.D.; Quinn, K.; King, L.; Schmink, S.E.; Wang, X.; et al. Prolonged university outbreak of meningococcal disease associated with a serogroup B strain rarely seen in the United States. Clin. Infect. Dis. 2013, 57, 344–348. [Google Scholar] [CrossRef]
- Stanwell-Smith, R.E.; Stuart, J.M.; Hughes, A.O.; Robinson, P.; Griffin, M.B.; Cartwright, K. Smoking, the environment and meningococcal disease: A case control study. Epidemiol. Infect. 1994, 112, 315–328. [Google Scholar] [CrossRef]
- McMillan, M.; Walters, L.; Mark, T.; Lawrence, A.; Leong, L.E.; Sullivan, T.; Rogers, G.B.; Andrews, R.M.; Marshall, H.S. B Part of It study: A longitudinal study to assess carriage of Neisseria meningitidis in first year university students in South Australia. Hum. Vaccines Immunother. 2019, 15, 987–994. [Google Scholar] [CrossRef]
- Van Ravenhorst, M.B.; Bijlsma, M.W.; van Houten, M.A.; Struben, V.M.; Anderson, A.S.; Eiden, J.; Hao, L.; Jansen, K.U.; Jones, H.; Kitchin, N.; et al. Meningococcal carriage in Dutch adolescents and young adults; a cross-sectional and longitudinal cohort study. Clin. Microbiol. Infect. 2017, 23, 573.e1–573.e7. [Google Scholar] [CrossRef]
- Neal, K.R.; Nguyen-Van-Tam, J.S.; Jeffrey, N.; Slack, R.C.; Madeley, R.J.; Ait-Tahar, K.; Job, K.; Wale, M.C.; Ala’aldeen, D.A. Changing carriage rate of Neisseria meningitidis among university students during the first week of term: Cross sectional study. Bmj 2000, 320, 846–849. [Google Scholar] [CrossRef][Green Version]
- Marshall, H.S.; McMillan, M.; Koehler, A.; Lawrence, A.; Sullivan, T.; MacLennan, J.M.; Maiden, M.C.; Ladhani, S.N.; Ramsay, M.; Trotter, C.; et al. Impact of meningococcal B vaccine on meningococcal carriage in adolescents. N. Engl. J. Med. 2019, 318–327, in Press. [Google Scholar] [CrossRef]
- Hallqvist, L.; Lindgren, S. Gonorrhoea of the throat at a venereological clinic incidence and results of treatment. Sex. Transm. Infect. 1975, 51, 395–397. [Google Scholar] [CrossRef]
- Hutt, D.M.; Judson, F.N. Epidemiology and treatment of oropharyngeal gonorrhea. Ann. Intern. Med. 1986, 104, 655–658. [Google Scholar] [CrossRef]
- Chow, E.P.; Lee, D.; Tabrizi, S.N.; Phillips, S.; Snow, A.; Cook, S.; Howden, B.P.; Petalotis, I.; Bradshaw, C.S.; Chen, M.Y.; et al. Detection of Neisseria gonorrhoeae in the pharynx and saliva: Implications for gonorrhoea transmission. Sex. Transm. Infect. 2016, 92, 347–349. [Google Scholar] [CrossRef]
- Chow, E.P.; Cornelisse, V.J.; Read, T.R.; Lee, D.; Walker, S.; Hocking, J.S.; Chen, M.Y.; Bradshaw, C.S.; Fairley, C.K. Saliva use as a lubricant for anal sex is a risk factor for rectal gonorrhoea among men who have sex with men, a new public health message: A cross-sectional survey. Sex. Transm. Infect. 2016. [Google Scholar] [CrossRef]
- Templeton, D.J.; Jin, F.; McNally, L.P.; Imrie, J.C.; Prestage, G.P.; Donovan, B.; Cunningham, P.H.; Kaldor, J.M.; Kippax, S.; Grulich, A.E. Prevalence, incidence and risk factors for pharyngeal gonorrhoea in a community-based HIV-negative cohort of homosexual men in Sydney, Australia. Sex. Transm. Infect. 2010, 86, 90–96. [Google Scholar] [CrossRef]
- Cornelisse, V.J.; Walker, S.; Phillips, T.; Hocking, J.S.; Bradshaw, C.S.; Lewis, D.A.; Prestage, G.P.; Grulich, A.E.; Fairley, C.K.; Chow, E.P. Risk factors for oropharyngeal gonorrhoea in men who have sex with men: An age-matched case-control study. Sex. Transm. Infect. 2018, 94, 359–364. [Google Scholar] [CrossRef]
- Chow, E.P.F.; Cornelisse, V.J.; Williamson, D.A.; Priest, D.; Hocking, J.S.; Bradshaw, C.S.; Read, T.R.H.; Chen, M.Y.; Howden, B.P.; Fairley, C.K. Kissing may be an important and neglected risk factor for oropharyngeal gonorrhoea: A cross-sectional study in men who have sex with men. Sex. Transm. Infect. 2019, 95. [Google Scholar] [CrossRef]
- Cornelisse, V.J.; Zhang, L.; Law, M.; Chen, M.Y.; Bradshaw, C.S.; Bellhouse, C.; Fairley, C.K.; Chow, E.P. Concordance of gonorrhoea of the rectum, pharynx and urethra in same-sex male partnerships attending a sexual health service in Melbourne, Australia. BMC Infect. Dis. 2018, 18. [Google Scholar] [CrossRef]
- Song, J.; Lauber, C.; Costello, E.K.; Lozupone, C.A.; Humphrey, G.; Berg-Lyons, D.; Caporaso, J.G.; Knights, D.; Clemente, J.C.; Nakielny, S.; et al. Cohabiting family members share microbiota with one another and with their dogs. eLife 2013, 2013, 1–22. [Google Scholar] [CrossRef]
- Abeles, S.R.; Jones, M.B.; Santiago-Rodriguez, T.M.; Ly, M.; Klitgord, N.; Yooseph, S.; Nelson, K.E.; Pride, D.T. Microbial diversity in individuals and their household contacts following typical antibiotic courses. Microbiome 2016, 4, 1–12. [Google Scholar] [CrossRef]
- Kort, R.; Caspers, M.; van de Graaf, A.; van Egmond, W.; Keijser, B.; Roeselers, G. Shaping the oral microbiota through intimate kissing. Microbiome 2014, 2, 1–8. [Google Scholar] [CrossRef]
- Marangoni, A.; Marziali, G.; Salvo, M.; D’Antuono, A.; Gaspari, V.; Foschi, C.; Re, M.C. Mosaic structure of the penA gene in the oropharynx of men who have sex with men negative for gonorrhoea. Int. J. STD AIDS 2020. [Google Scholar] [CrossRef]
- Igawa, G.; Yamagishi, Y.; Lee, K.I.I.; Dorin, M.; Shimuta, K.; Suematsu, H.; Nakayama, S.I.I.; Mikamo, H.; Unemo, M.; Ohnishi, M.; et al. Neisseria cinerea with high ceftriaxone MIC Is a source of ceftriaxone and cefixime resistance-mediating penA sequences in Neisseria gonorrhoeae. Antimicrob. Agents Chemother. 2018, 62, 1–5. [Google Scholar] [CrossRef]
- Wadsworth, C.B.; Arnold, B.J.; Sater, M.R.A.; Grad, Y.H. Azithromycin Resistance through Interspecific Acquisition of an Epistasis-Dependent Efflux Pump Component and Transcriptional Regulator in Neisseria gonorrhoeae. mBio 2018, 9, 1–17. [Google Scholar] [CrossRef]
- Furuya, R.; Onoye, Y.; Kanayama, A.; Saika, T.; Iyoda, T.; Tatewaki, M.; Matsuzaki, K.; Kobayashi, I.; Tanaka, M. Antimicrobial resistance in clinical isolates of Neisseria subflava from the oral cavities of a Japanese population. J. Infect. Chemother. 2007, 13, 302–304. [Google Scholar] [CrossRef]
- Kenyon, C.R.; Schwartz, I.S. Effects of sexual network connectivity and antimicrobial drug use on antimicrobial resistance in neisseria gonorrhoeae. Emerg. Infect. Dis. 2018, 24, 1195–1203. [Google Scholar] [CrossRef] [PubMed]
- Trinh, P.; Zaneveld, J.R.; Safranek, S.; Rabinowitz, P.M. One Health Relationships Between Human, Animal, and Environmental Microbiomes: A Mini-Review. Front. Public Health 2018, 6, 1–9. [Google Scholar] [CrossRef] [PubMed]
- Kenyon, C. How actively should we screen for chlamydia and gonorrhoea in MSM and other high-ST-prevalence populations as we enter the era of increasingly untreatable infections? A viewpoint. J. Med. Microbiol. 2019, 68, 132–135. [Google Scholar] [CrossRef] [PubMed]
- Tan, D.H.; Hull, M.W.; Yoong, D.; Tremblay, C.; O’Byrne, P.; Thomas, R.; Kille, J.; Baril, J.G.; Cox, J.; Giguere, P.; et al. Canadian guideline on HIV pre-exposure prophylaxis and nonoccupational postexposure prophylaxis. CMAJ 2017, 189, E1448–E1458. [Google Scholar] [CrossRef] [PubMed]
- Australian Sexually Transmitted Infection & HIV Testing Guidelines 2019 for Asymptomatic Men Who Have Sex with Men. Available online: http://www.sti.guidelines.org.au (accessed on 18 March 2020).
- Ridpath, A.D.; Chesson, H.; Marcus, J.L.; Kirkcaldy, R.D.; Torrone, E.A.; Aral, S.O.; Bernstein, K.T. Screening Peter to Save Paul: The Population-Level Effects of Screening Men Who Have Sex with Men for Gonorrhea and Chlamydia. Sex. Transm. Dis. 2018, 45, 623–625. [Google Scholar] [CrossRef] [PubMed]
- Kenyon, C.; Buyze, J.; Spiteri, G.; Cole, M.J.; Unemo, M. Population-Level Antimicrobial Consumption Is Associated With Decreased Antimicrobial Susceptibility in Neisseria gonorrhoeae in 24 European Countries: An Ecological Analysis. J. Infect. Dis. 2019, 8. [Google Scholar] [CrossRef]
- Wind, C.M.; De Vries, E.; Schim Van Der Loeff, M.F.; Van Rooijen, M.S.; Van Dam, A.P.; Demczuk, W.H.; Martin, I.; De Vries, H.J. Decreased Azithromycin Susceptibility of Neisseria gonorrhoeae Isolates in Patients Recently Treated with Azithromycin. Clin. Infect. Dis. 2017, 65, 37–45. [Google Scholar] [CrossRef]
- Chow, E.P.; Walker, S.; Hocking, J.S.; Bradshaw, C.S.; Chen, M.Y.; Tabrizi, S.N.; Howden, B.P.; Law, M.G.; Maddaford, K.; Read, T.R.; et al. A multicentre double-blind randomised controlled trial evaluating the efficacy of daily use of antibacterial mouthwash against oropharyngeal gonorrhoea among men who have sex with men: The OMEGA (Oral Mouthwash use to Eradicate GonorrhoeA) study protocol. BMC Infect. Dis. 2017, 17, 456. [Google Scholar] [CrossRef]
- Paynter, J.; Goodyear-Smith, F.; Morgan, J.; Saxton, P.; Black, S.; Petousis-Harris, H. Effectiveness of a group b outer membrane vesicle meningococcal vaccine in preventing hospitalization from gonorrhea in New Zealand: A retrospective cohort study. Vaccines 2019, 7, 5. [Google Scholar] [CrossRef]
- Horn, H.S. Measurement of “Overlap” in Comparative Ecological Studies. Am. Nat. 1966, 100, 419–424. [Google Scholar] [CrossRef]
© 2020 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Van Dijck, C.; Laumen, J.G.E.; Manoharan-Basil, S.S.; Kenyon, C. Commensal Neisseria Are Shared between Sexual Partners: Implications for Gonococcal and Meningococcal Antimicrobial Resistance. Pathogens 2020, 9, 228. https://doi.org/10.3390/pathogens9030228
Van Dijck C, Laumen JGE, Manoharan-Basil SS, Kenyon C. Commensal Neisseria Are Shared between Sexual Partners: Implications for Gonococcal and Meningococcal Antimicrobial Resistance. Pathogens. 2020; 9(3):228. https://doi.org/10.3390/pathogens9030228
Chicago/Turabian StyleVan Dijck, Christophe, Jolein G. E. Laumen, Sheeba S. Manoharan-Basil, and Chris Kenyon. 2020. "Commensal Neisseria Are Shared between Sexual Partners: Implications for Gonococcal and Meningococcal Antimicrobial Resistance" Pathogens 9, no. 3: 228. https://doi.org/10.3390/pathogens9030228
APA StyleVan Dijck, C., Laumen, J. G. E., Manoharan-Basil, S. S., & Kenyon, C. (2020). Commensal Neisseria Are Shared between Sexual Partners: Implications for Gonococcal and Meningococcal Antimicrobial Resistance. Pathogens, 9(3), 228. https://doi.org/10.3390/pathogens9030228




