Disease Manifestation and Viral Sequences in a Bonobo More Than 30 Years after Papillomavirus Infection
Abstract
1. Introduction
2. Materials and Methods
2.1. Sample Acquisition
2.2. Histological and Immunohistochemical Examinations
2.3. PCR-Based Detection of PpPV1
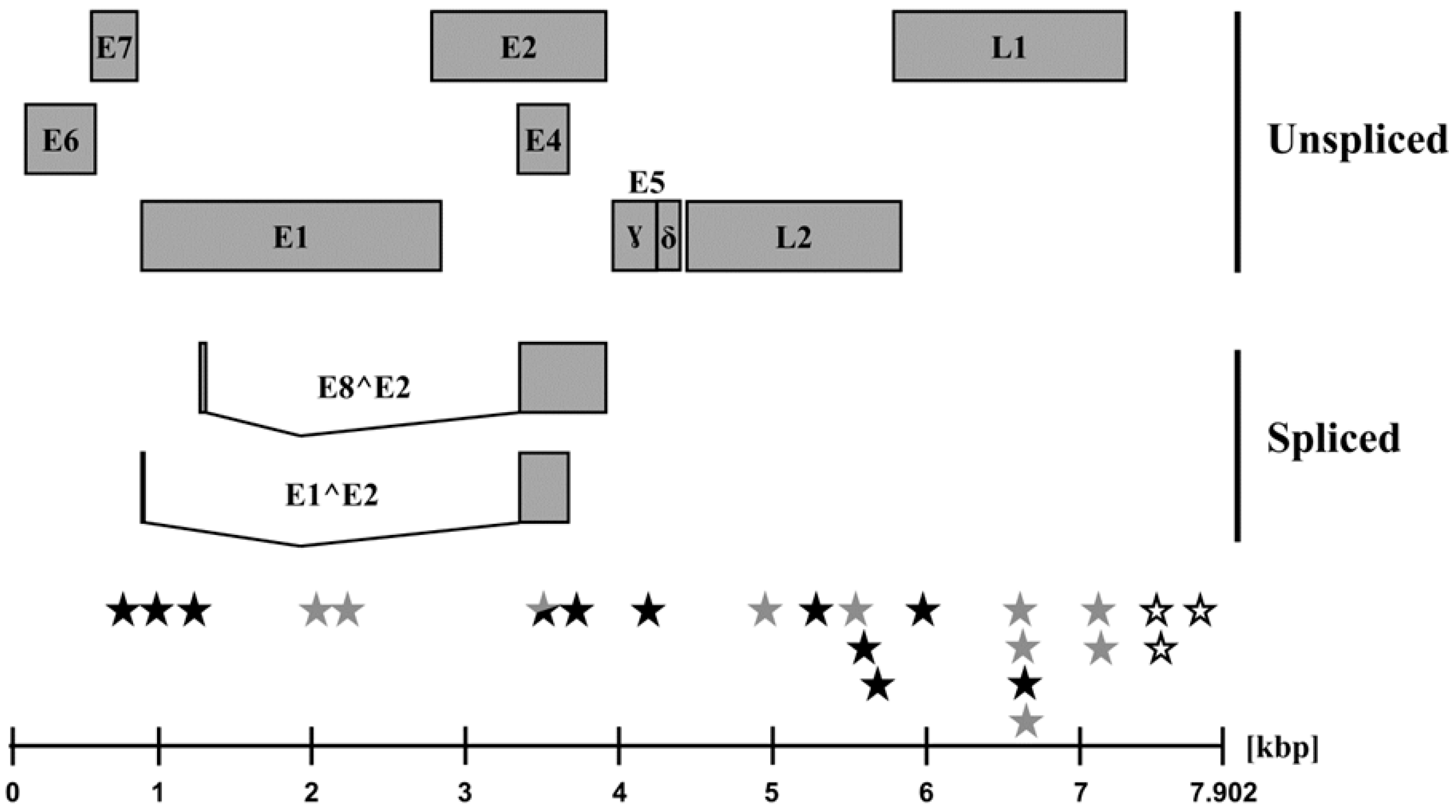
2.4. Amplification and Sequencing of DNA Fragments Covering the Whole PpPV1 Genome
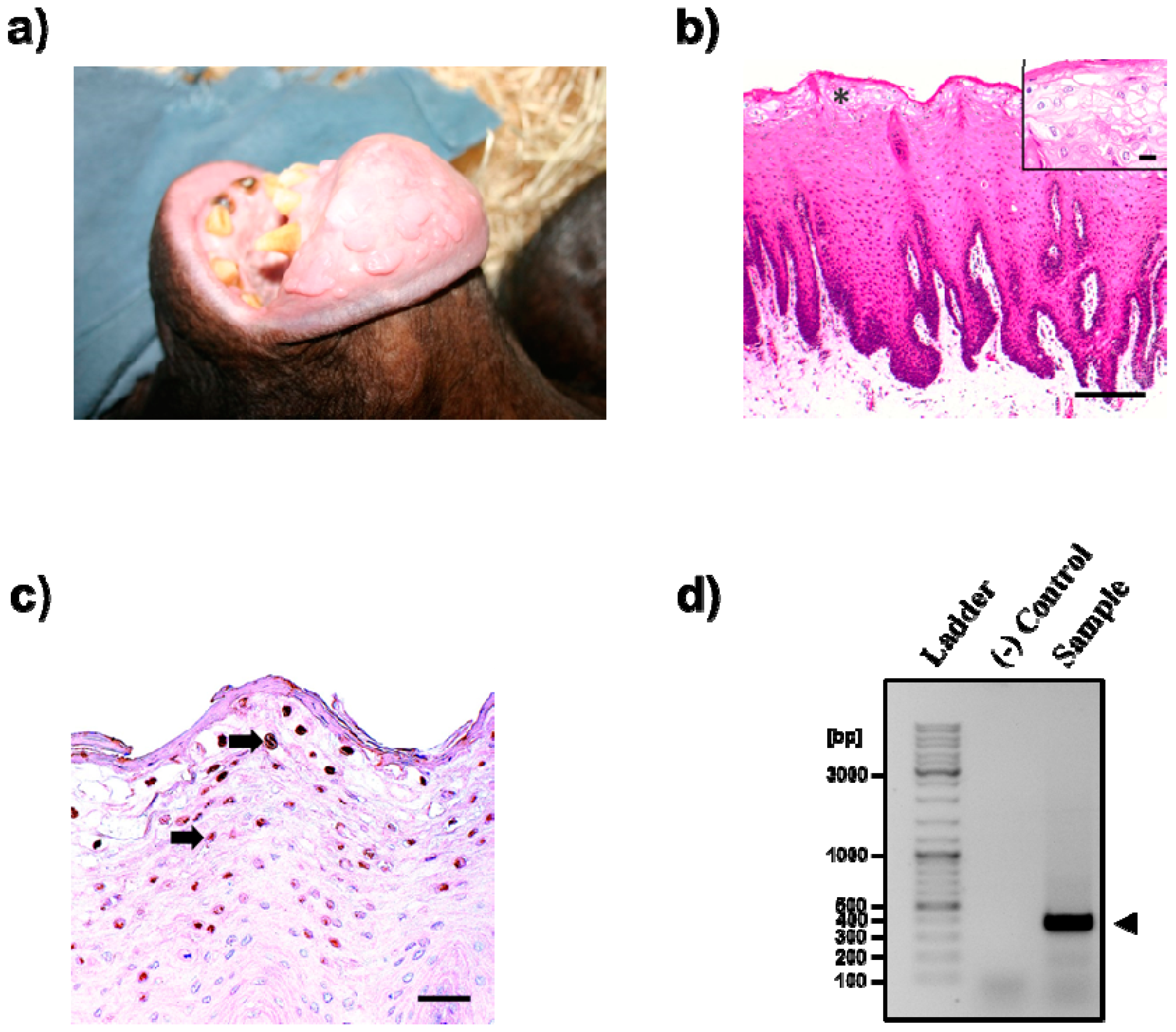
3. Results
4. Discussion
5. Conclusions
Author Contributions
Funding
Acknowledgments
Conflicts of Interest
References
- ICTV. Current Taxonomy Release. Available online: https://talk.ictvonline.org/taxonomy/ (accessed on 21 June 2018).
- Doorbar, J.; Quint, W.; Banks, L.; Bravo, I.G.; Stoler, M.; Broker, T.R.; Stanley, M.A. The biology and life-cycle of human papillomaviruses. Vaccine 2012, 30 (Suppl. 5), F55–F70. [Google Scholar] [CrossRef] [PubMed]
- Prabhu, S.R.; Wilson, D.F. Human papillomavirus and oral disease—Emerging evidence: A review. Aust. Dent. J. 2013, 58, 2–10. [Google Scholar] [CrossRef] [PubMed]
- Witkop, C.J., Jr.; Niswander, J.D. Focal Epithelial Hyperplasia in Central and South American Indians and Ladinos. Oral. Surg. Oral Med. Oral Pathol. 1965, 20, 213–217. [Google Scholar] [CrossRef]
- Ledesma-Montes, C.; Mendez-Mendoza, A. Unusually high incidence of multifocal epithelial hyperplasia in children of the Nahuatl population of Mexico. Indian J. Dermatol. Venereol. Leprol. 2017, 83, 663–666. [Google Scholar] [CrossRef] [PubMed]
- Clausen, F.P.; Mogeltoft, M.; Roed-Petersen, B.; Pindborg, J.J. Focal epithelial hyperplasia of the oral mucosa in a south-west Greenlandic population. Scand. J. Dent. Res. 1970, 78, 287–294. [Google Scholar] [CrossRef] [PubMed]
- Jarvis, A.; Gorlin, R.J. Focal epithelial hyperplasia in an Eskimo population. Oral Surg. Oral Med. Oral Pathol. 1972, 33, 227–228. [Google Scholar] [CrossRef]
- Akoglu, G.; Metin, A.; Ceylan, G.G.; Emre, S.; Akpolat, D.; Sungu, N. Focal epithelial hyperplasia associated with human papillomavirus 13 and common human leukocyte antigen alleles in a Turkish family. Int. J. Dermatol. 2015, 54, 174–178. [Google Scholar] [CrossRef]
- Garcia-Corona, C.; Vega-Memije, E.; Mosqueda-Taylor, A.; Yamamoto-Furusho, J.K.; Rodriguez-Carreon, A.A.; Ruiz-Morales, J.A.; Salgado, N.; Granados, J. Association of HLA-DR4 (DRB1*0404) with human papillomavirus infection in patients with focal epithelial hyperplasia. Arch. Dermatol. 2004, 140, 1227–1231. [Google Scholar] [CrossRef]
- Said, A.K.; Leao, J.C.; Fedele, S.; Porter, S.R. Focal epithelial hyperplasia—An update. J. Oral Pathol. Med. 2013, 42, 435–442. [Google Scholar] [CrossRef]
- Beaudenon, S.; Praetorius, F.; Kremsdorf, D.; Lutzner, M.; Worsaae, N.; Pehau-Arnaudet, G.; Orth, G. A new type of human papillomavirus associated with oral focal epithelial hyperplasia. J. Investig. Dermatol. 1987, 88, 130–135. [Google Scholar] [CrossRef]
- Pfister, H.; Hettich, I.; Runne, U.; Gissmann, L.; Chilf, G.N. Characterization of human papillomavirus type 13 from focal epithelial hyperplasia Heck lesions. J. Virol. 1983, 47, 363–366. [Google Scholar] [PubMed]
- Van Ranst, M.; Fuse, A.; Fiten, P.; Beuken, E.; Pfister, H.; Burk, R.D.; Opdenakker, G. Human papillomavirus type 13 and pygmy chimpanzee papillomavirus type 1: Comparison of the genome organizations. Virology 1992, 190, 587–596. [Google Scholar] [CrossRef]
- Van Ranst, M.; Fuse, A.; Sobis, H.; De Meurichy, W.; Syrjanen, S.M.; Billiau, A.; Opdenakker, G. A papillomavirus related to HPV type 13 in oral focal epithelial hyperplasia in the pygmy chimpanzee. J. Oral Pathol. Med. 1991, 20, 325–331. [Google Scholar] [CrossRef] [PubMed]
- Ramos-Vara, J.A. Technical aspects of immunohistochemistry. Vet. Pathol. 2005, 42, 405–426. [Google Scholar] [CrossRef] [PubMed]
- Forslund, O.; Antonsson, A.; Nordin, P.; Stenquist, B.; Hansson, B.G. A broad range of human papillomavirus types detected with a general PCR method suitable for analysis of cutaneous tumours and normal skin. J. Gen. Virol. 1999, 80 Pt 9, 2437–2443. [Google Scholar] [CrossRef]
- Li, J.; Pan, Y.; Xu, Z.; Wang, Q.; Hang, D.; Shen, N.; Liu, M.; Zhang, C.; Abliz, A.; Deng, Q.; et al. Improved detection of human papillomavirus harbored in healthy skin with FAP6085/64 primers. J. Virol. Methods 2013, 193, 633–638. [Google Scholar] [CrossRef] [PubMed]
- Tamura, K.; Stecher, G.; Peterson, D.; Filipski, A.; Kumar, S. MEGA6: Molecular Evolutionary Genetics Analysis version 6.0. Mol. Biol. Evol. 2013, 30, 2725–2729. [Google Scholar] [CrossRef] [PubMed]
- Gonzalez-Losa Mdel, R.; Barrera, E.S.; Herrera-Pech, V.; Conde-Ferraez, L.; Puerto-Solis, M.; Ayora-Talavera, G. Epidemiology of oral HPV in the oral mucosa in women without signs of oral disease from Yucatan, Mexico. Braz. J. Microbiol. 2015, 46, 301–306. [Google Scholar] [CrossRef]
- Smith, E.M.; Ritchie, J.M.; Summersgill, K.F.; Hoffman, H.T.; Wang, D.H.; Haugen, T.H.; Turek, L.P. Human papillomavirus in oral exfoliated cells and risk of head and neck cancer. J. Natl. Cancer Inst. 2004, 96, 449–455. [Google Scholar] [CrossRef]
- Sundberg, J.P.; Shima, A.L.; Adkison, D.L. Oral papillomavirus infection in a pygmy chimpanzee (Pan paniscus). J. Vet. Diagn. Investig. 1992, 4, 70–74. [Google Scholar] [CrossRef]
- Van der Weele, P.; Meijer, C.; King, A.J. Whole-Genome Sequencing and Variant Analysis of Human Papillomavirus 16 Infections. J. Virol. 2017, 91. [Google Scholar] [CrossRef] [PubMed]
- Mirabello, L.; Clarke, M.A.; Nelson, C.W.; Dean, M.; Wentzensen, N.; Yeager, M.; Cullen, M.; Boland, J.F.; Workshop, N.H.; Schiffman, M.; et al. The Intersection of HPV Epidemiology, Genomics and Mechanistic Studies of HPV-Mediated Carcinogenesis. Viruses 2018, 10, 80. [Google Scholar] [CrossRef] [PubMed]
- Biryukov, J.; Meyers, C. Superinfection Exclusion between Two High-Risk Human Papillomavirus (HPV) Types During a Co-Infection. J. Virol. 2018, JVI.01993-17. [Google Scholar] [CrossRef] [PubMed]
- Ahola, H.; Stenlund, A.; Moreno-Lopez, J.; Pettersson, U. Sequences of bovine papillomavirus type 1 DNA--functional and evolutionary implications. Nucleic Acids Res. 1983, 11, 2639–2650. [Google Scholar] [CrossRef] [PubMed]
- Bravo, I.G.; Felez-Sanchez, M. Papillomaviruses: Viral evolution, cancer and evolutionary medicine. Evol. Med. Public Health 2015, 2015, 32–51. [Google Scholar] [CrossRef] [PubMed]
- Kukimoto, I.; Maehama, T.; Sekizuka, T.; Ogasawara, Y.; Kondo, K.; Kusumoto-Matsuo, R.; Mori, S.; Ishii, Y.; Takeuchi, T.; Yamaji, T.; et al. Genetic variation of human papillomavirus type 16 in individual clinical specimens revealed by deep sequencing. PLoS ONE 2013, 8, e80583. [Google Scholar] [CrossRef]
- Dube Mandishora, R.S.; Gjotterud, K.S.; Lagstrom, S.; Stray-Pedersen, B.; Duri, K.; Chin’ombe, N.; Nygard, M.; Christiansen, I.K.; Ambur, O.H.; Chirenje, M.Z.; et al. Intra-host sequence variability in human papillomavirus. Papillomavirus Res 2018, 5, 180–191. [Google Scholar] [CrossRef]
- Hirose, Y.; Onuki, M.; Tenjimbayashi, Y.; Mori, S.; Ishii, Y.; Takeuchi, T.; Tasaka, N.; Satoh, T.; Morisada, T.; Iwata, T.; et al. Within-Host Variations of Human Papillomavirus Reveal APOBEC Signature Mutagenesis in the Viral Genome. J. Virol. 2018, 92, JVI.00017-18. [Google Scholar] [CrossRef]
| Name | Sequence (5′–3′) |
|---|---|
| PpPV1_1F | CAGCTCAGAAGAAGATGAGG |
| PpPV1_1R | CTTAGTAATACTAACAATAGC |
| PpPV1_2F | TGCATCATAGTGTGTCTGAGG |
| PpPV1_2R | TTCTGTCAAAAGGGAATGG |
| PpPV1_3F | TAGAAAACATAAATCGTTAGC |
| PpPV1_3R | CCTGTGCAAGGGTGGTTGTGG |
| PpPV1_4F | AGCAAAGTTATATGTTCTCC |
| PpPV1_4R | CTGCGAGGCCTACTATGTGC |
| PpPV1_5F | TTACTGCATATTAGAACTGG |
| PpPV1_5R | CGTCCACCAATATGTTTGCC |
| PpPV1_6F | GGCTATAACGTCTAGGCGTGG |
| PpPV1_6R | ACACCTGAACATTGTGTGCC |
| PpPV1_7F | GTTTGGTGTGGGCCTGTATAGG |
| PpPV1_7R | AAACTGAGACCTGCATAAGG |
| PpPV1_8F | TTTAGAAGAATGGAACTTTGG |
| PpPV1_8R | GAAACCGTTTTCGGTCCCTCC |
| PpPV1_9F | AATCCTTTTTGGCTACCAGC |
| PpPV1_9R | ATGTCCGATCCTGTACAGTCC |
| Primer For | Primer Rev | Amplicon | Amplicon Size (bp) | Genome Region (nt) |
|---|---|---|---|---|
| PpPV1_1F | PpPV1_1R | 1a | 1055 | 618–1672 |
| PpPV1_2R | 1b | 2005 | 618–2622 | |
| PpPV1_2F | PpPV1_2R | 2a | 1062 | 1561–2622 |
| PpPV1_3R | 2b | 1825 | 1561–3385 | |
| PpPV1_3F | PpPV1_3R | 3a | 909 | 2477–3385 |
| PpPV1_4R | 3b | 1914 | 2477–4390 | |
| PpPV1_4F | PpPV1_4R | 4a | 1102 | 3289–4390 |
| PpPV1_5R | 4b | 2038 | 3289–5326 | |
| PpPV1_5F | PpPV1_5R | 5a | 1046 | 4281–5326 |
| PpPV1_6R | 5b | 1989 | 4281–6269 | |
| PpPV1_6F | PpPV1_6R | 6a | 1036 | 5234–6269 |
| PpPV1_7R | 6b | 1843 | 5234–7076 | |
| PpPV1_7F | PpPV1_7R | 7a | 1051 | 6026–7076 |
| PpPV1_8R | 7b | 1927 | 6026–50 | |
| PpPV1_8F | PpPV1_8R | 8a | 1020 | 6933–50 |
| PpPV1_9R | 8b | 1728 | 6933–758 | |
| PpPV1_9F | PpPV1_9R | 9a | 912 | 7749–758 |
| PpPV1_1R | 9b | 1826 | 7749–1672 |
| Genome | Genetic Element | Open Reading Frame | ||||
|---|---|---|---|---|---|---|
| Position (nt) | Effect (nt) a | Position (nt) | Position (aa) | Effect (aa) b | Codon c | |
| 711 | G711C | E7 | 180 | 60 | Q60H | CAx |
| 861 | A861G | E1 | 28 | 10 | K10E | xAG |
| 1170 | A1170C | E1 | 337 | 113 | I113L | xTA |
| 1964 | T1964C | E1 | 1131 | 377 | silent (F) | TTx |
| 2172 | A2172C | E1 | 1339 | 447 | silent (R) | xGG |
| 3472 d | C3472G | E2 | 751 | 251 | R251G | xGA |
| 3666 e | C3666A | E2 | 945 | 315 | D315E | GAx |
| 3472 d | C3472G | E4 | 189 | 63 | silent (L) | CTx |
| 3472 d | C3472G | E1^E4 | 165 | 55 | silent (L) | CTx |
| 3666 e | C3472G | E8^E2 | 187 | 63 | R187G | xGA |
| 3472 d | C3666A | E8^E2 | 381 | 127 | D381E | GAx |
| 4136 | G4136C | E5ɣ | 237 | 79 | L79F | TTx |
| 4883 | C4883A | L2 | 516 | 172 | silent (P) | CCx |
| 5217 | G5217A | L2 | 850 | 284 | V284I | xTA |
| 5477 | G5477A | L2 | 1110 | 370 | silent (S) | TCx |
| 5523 | A5523C | L2 | 1156 | 386 | K386Q | xAG |
| 5613 | G5613A | L2 | 1246 | 416 | C416Y | TxT |
| 5900 | G5900A | L1 | 155 | 52 | R52K | AxA |
| 6543 | G6543A | L1 | 798 | 266 | silent (E) | GAx |
| 6549 | A6549T | L1 | 804 | 268 | silent (I) | ATx |
| 6555 | A6555C | L1 | 810 | 270 | E270D | GAx |
| 6573 | G6573T | L1 | 828 | 276 | silent (G) | GGx |
| 7071 | C7071T | L1 | 1326 | 442 | silent (L) | CTx |
| 7089 | T7089C | L1 | 1344 | 448 | silent (N) | AAx |
| 7443 | G7443C | URR | n.a. | n.a. | n.a. | n.a. |
| 7469 | A7469C | URR | n.a. | n.a. | n.a. | n.a. |
| 7726 | C7726G | URR | n.a. | n.a. | n.a. | n.a. |
© 2019 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Hoffmann, M.; Schütze, E.; Bernhard, A.; Schlaphoff, L.; Kaul, A.; Schöniger, S.; Pöhlmann, S. Disease Manifestation and Viral Sequences in a Bonobo More Than 30 Years after Papillomavirus Infection. Pathogens 2019, 8, 13. https://doi.org/10.3390/pathogens8010013
Hoffmann M, Schütze E, Bernhard A, Schlaphoff L, Kaul A, Schöniger S, Pöhlmann S. Disease Manifestation and Viral Sequences in a Bonobo More Than 30 Years after Papillomavirus Infection. Pathogens. 2019; 8(1):13. https://doi.org/10.3390/pathogens8010013
Chicago/Turabian StyleHoffmann, Markus, Enrika Schütze, Andreas Bernhard, Lennart Schlaphoff, Artur Kaul, Sandra Schöniger, and Stefan Pöhlmann. 2019. "Disease Manifestation and Viral Sequences in a Bonobo More Than 30 Years after Papillomavirus Infection" Pathogens 8, no. 1: 13. https://doi.org/10.3390/pathogens8010013
APA StyleHoffmann, M., Schütze, E., Bernhard, A., Schlaphoff, L., Kaul, A., Schöniger, S., & Pöhlmann, S. (2019). Disease Manifestation and Viral Sequences in a Bonobo More Than 30 Years after Papillomavirus Infection. Pathogens, 8(1), 13. https://doi.org/10.3390/pathogens8010013






