The New Precision Stewards?
Abstract
1. Introduction
2. Lessons Learned: ELSI and Precision Medicine
2.1. A National Investment in Multidisciplinary Inquiry
2.2. Assessing Understanding and Attitudes
2.2.1. Human Genomics
2.2.2. Pathogen Genomics
2.3. Health Equity
2.3.1. Human Genomics
2.3.2. Pathogen Genomics
2.4. Data Governance
2.4.1. Human Genomics
2.4.2. Pathogen Genomics
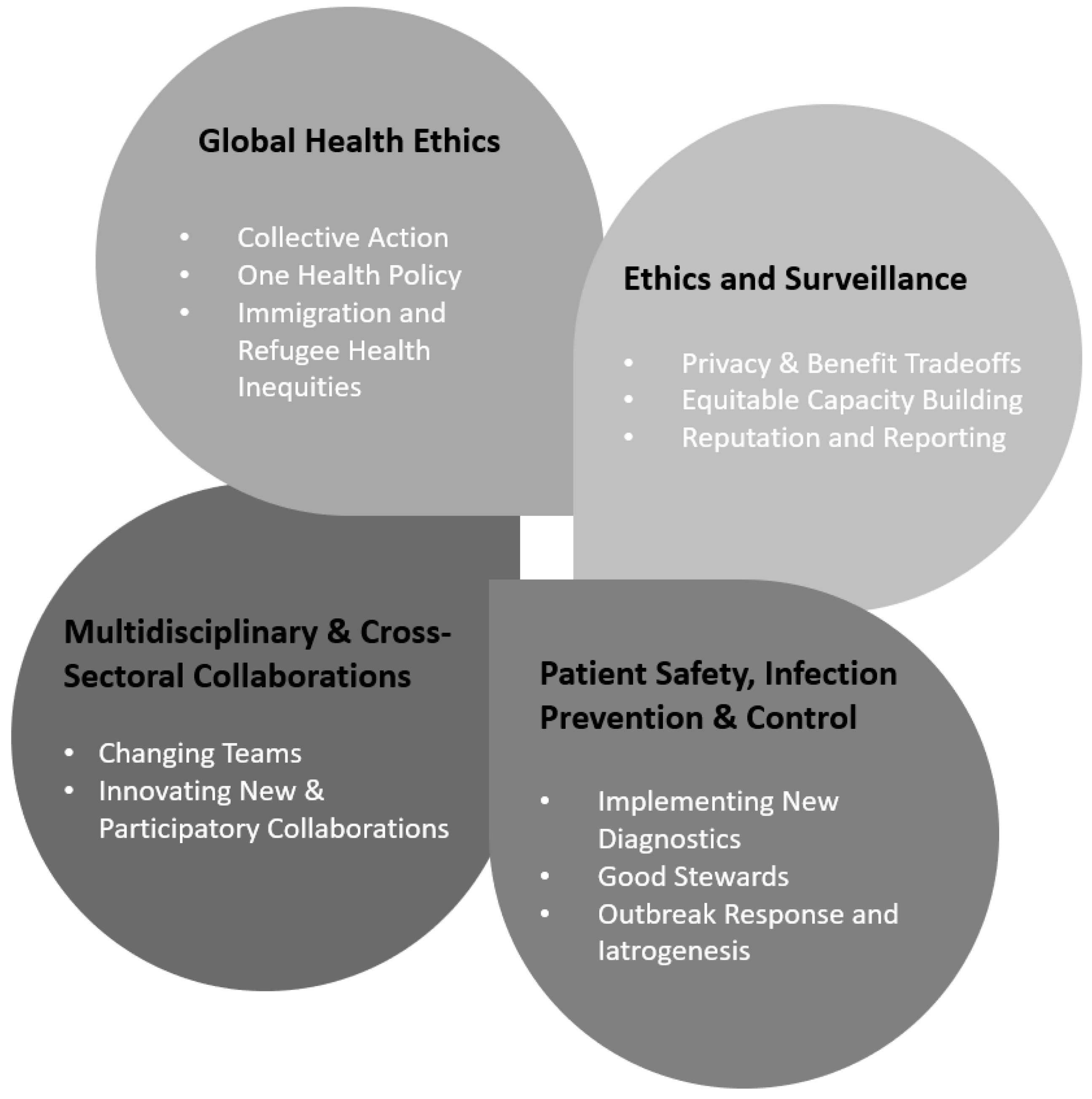
3. AMR Is Distinct: Toward an ELSI of Precision Antimicrobial Stewardship
3.1. Global Health Ethics
3.1.1. Collective Action
3.1.2. One Health Policy
3.1.3. Global Health Justice
3.1.4. Immigration and Refugee Health Inequities
3.2. Precision Health Surveillance
3.2.1. Equitable Capacity Building
3.2.2. Reputation and Reporting
3.3. Ethics, Patient Safety, and Precision Infection Prevention and Control
3.3.1. Implementing New Diagnostics
3.3.2. Good Stewards
3.3.3. Outbreak Response and Iatrogenesis
3.4. Multidisciplinary and Cross-Sectoral Collaborations
3.4.1. Changing Teams
3.4.2. Innovating New and Participatory Collaborations
4. Conclusions: Advancing an ELSI Precision Stewardship Agenda
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Bowater, L. Antimicrobial stewardship: The role of scientists? J. Antimicrob. Chemother. 2015, 70, 1925–1927. [Google Scholar] [CrossRef]
- Ladner, J.T.; Grubaugh, N.D.; Pybus, O.G.; Andersen, K.G. Precision epidemiology for infectious disease control. Nat. Med. 2019, 25, 206–211. [Google Scholar] [CrossRef]
- Afshinnekoo, E.; Chou, C.; Alexander, N.; Ahsanuddin, S.; Schuetz, A.N.; Mason, C.E. Precision Metagenomics: Rapid Metagenomic Analyses for Infectious Disease Diagnostics and Public Health Surveillance. J. Biomol. Tech. 2017, 28, 40–45. [Google Scholar] [CrossRef] [PubMed]
- Armstrong, G.L.; MacCannell, D.R.; Taylor, J.; Carleton, H.A.; Neuhaus, E.B.; Bradbury, R.S.; Posey, J.E.; Gwinn, M. Pathogen Genomics in Public Health. N. Engl. J. Med. 2019, 381, 2569–2580. [Google Scholar] [CrossRef] [PubMed]
- Carlet, J.; Pulcini, C.; Piddock, L.J.V. Antibiotic resistance: A geopolitical issue. Clin. Microbiol. Infect. 2014, 20, 949–953. [Google Scholar] [CrossRef]
- Lorencatto, F.; Charani, E.; Sevdalis, N.; Tarrant, C.; Davey, P. Driving sustainable change in antimicrobial prescribing practice: How can social and behavioural sciences help? J. Antimicrob. Chemother. 2018, 73, 2613–2624. [Google Scholar] [CrossRef] [PubMed]
- Smith, R. Antimicrobial resistance is a social problem requiring a social solution. BMJ 2015, 350, h2682. [Google Scholar] [CrossRef] [PubMed]
- Tompson, A.C.; Chandler, C.I. Addressing antibiotic use: Insights from social science around the world. Lond. Sch. Hyg. Trop. Med. 2021. [Google Scholar] [CrossRef]
- Thornber, K.; Pitchforth, E. Communicating antimicrobial resistance: The need to go beyond human health. JAC Antimicrob. Resist. 2021, 3, dlab096. [Google Scholar] [CrossRef]
- O’Neill, J. Review on Antimicrobial Resistance. In Tackling a Global Health Crisis: Initial Steps; WellcomeTrust, Government of the United Kingdom: London, UK, 2015. Available online: https://wellcomecollection.org/works/bfepg7pb (accessed on 20 April 2022).
- Broom, A.; Kenny, K.; Prainsack, B.; Broom, J. Antimicrobial resistance as a problem of values? Views from three continents. Crit. Public Health 2020, 31, 451–463. [Google Scholar] [CrossRef]
- Littmann, J.; Viens, A.M. The Ethical Significance of Antimicrobial Resistance. Public Health Ethics 2015, 8, 209–224. [Google Scholar] [CrossRef]
- Parsonage, B.; Hagglund, P.K.; Keogh, L.; Wheelhouse, N.; Brown, R.E.; Dancer, S.J. Control of Antimicrobial Resistance Requires an Ethical Approach. Front. Microbiol. 2017, 8, 2124. [Google Scholar] [CrossRef]
- Munthe, C.; Nijsingh, N.; de Fine Licht, K.; Larsson, D.G.J. Health-related Research Ethics and Social Value: Antibiotic Resistance Intervention Research and Pragmatic Risks. Bioethics 2019, 33, 335–342. [Google Scholar] [CrossRef] [PubMed]
- Gilbert, G.L.; Kerridge, I. The politics and ethics of hospital infection prevention and control: A qualitative case study of senior clinicians’ perceptions of professional and cultural factors that influence doctors’ attitudes and practices in a large Australian hospital. BMC Health Serv. Res. 2019, 19, 212. [Google Scholar] [CrossRef]
- Dyar, O.J.; Huttner, B.; Schouten, J.; Pulcini, C. What is antimicrobial stewardship? Clin. Microbiol. Infect. 2017, 23, 793–798. [Google Scholar] [CrossRef] [PubMed]
- Krockow, E.M.; Colman, A.M.; Chattoe-Brown, E.; Jenkins, D.R.; Perera, N.; Mehtar, S.; Tarrant, C. Balancing the risks to individual and society: A systematic review and synthesis of qualitative research on antibiotic prescribing behaviour in hospitals. J. Hosp. Infect. 2019, 101, 428–439. [Google Scholar] [CrossRef]
- Anomaly, J. Combating Resistance: The Case for a Global Antibiotics Treaty. Public Health Ethics 2010, 3, 13–22. [Google Scholar] [CrossRef]
- Podolsky, S.H. The evolving response to antibiotic resistance (1945–2018). Palgr. Commun. 2018, 4, 124. [Google Scholar] [CrossRef]
- Littmann, J.; Rid, A.; Buyx, A. Tackling anti-microbial resistance: Ethical framework for rational antibiotic use. Eur. J. Public Health 2018, 28, 359–363. [Google Scholar] [CrossRef]
- Antoine-Moussiaux, N.; Janssens de Bisthoven, L.; Leyens, S.; Assmuth, T.; Keune, H.; Jakob, Z.; Huge, J.; Vanhove, M.P.M. The good, the bad and the ugly: Framing debates on nature in a One Health community. Sustain. Sci. 2019, 14, 1729–1738. [Google Scholar] [CrossRef]
- Kahn, L.H. One Health and the Politics of Antimicrobial Resistance; Johns Hopkins University: Baltimore, MD, USA, 2016. [Google Scholar]
- Hoffman, S.J.; Outterson, K.; Røttingen, J.-A.; Cars, O.; Clift, C.; Rizvi, Z.; Rotberg, F.; Tomson, G.; Zorzet, A. An international legal framework to address antimicrobial resistance. Bull. World Health Organ. 2015, 93, 66. [Google Scholar] [CrossRef]
- Giubilini, A. Antibiotic resistance as a tragedy of the commons: An ethical argument for a tax on antibiotic use in humans. Bioethics 2019, 33, 776–784. [Google Scholar] [CrossRef]
- Viens, A.M.; Littmann, J. Is Antimicrobial Resistance a Slowly Emerging Disaster? Public Health Ethics 2015, 8, 255–265. [Google Scholar] [CrossRef]
- Littman, J.; Viens, A.; Silva, D.S. The Super-Wicked Problem of Antimicrobial Resistance. In Ethics and Drug Resistance: Collective Responsibility for Global Public Health; Jamrozik, E., Selgelid, M., Eds.; Springer: Cham, Switzerland, 2020; Volume 5. [Google Scholar]
- Lu, J.; Sheldenkar, A.; Lwin, M.O. A decade of antimicrobial resistance research in social science fields: A scientometric review. Antimicrob. Resist. Infect. Control 2020, 9, 178. [Google Scholar] [CrossRef]
- Frid-Nielsen, S.S.; Rubin, O.; Baekkeskov, E. The state of social science research on antimicrobial resistance. Soc. Sci. Med. 2019, 242, 112596. [Google Scholar] [CrossRef]
- National Institutes of Health Studies of the Ethical, Legal, and Social Implications (ELSI) of Human Microbiome Research (R01). Available online: https://grants.nih.gov/grants/guide/rfa-files/RFA-RM-08-030.html (accessed on 16 June 2022).
- Institute of Medicine; Committee on the Social and Ethical Impacts of Developments in Biomedicine. Society’s Choices: Social and Ethical Decision Making in Biomedicine; Bulger, R.E., Bobby, E.M., Fineberg, H.V., Eds.; The National Academies Press: Washington, DC, USA, 1995; p. 560. Available online: https://nap.nationalacademies.org/catalog/4771/societys-choices-social-and-ethical-decision-making-in-biomedicine (accessed on 12 May 2022).
- ELSIhub. Available online: https://elsihub.org/ (accessed on 11 August 2021).
- American Society of Human Genetics. Public Attitudes Toward Genetics & Genomics Research: Literature and Polling Review Report. January 2020. Available online: https://www.ashg.org/wp-content/uploads/2020/01/2020-Public-Views-Genetics-Literature-Review.pdf (accessed on 11 August 2022).
- Condit, C.M. Public attitudes and beliefs about genetics. Annu. Rev. Genom. Hum. Genet. 2010, 11, 339–359. [Google Scholar] [CrossRef]
- Heine, S.J.; Dar-Nimrod, I.; Cheung, B.Y.; Proulx, T. Essentially biased: Why people are fatalistic about genes. In Advances in Experimental Social Psychology; Academic Press: Cambridge, MA, 2017; Volume 55, pp. 137–192. [Google Scholar]
- Condit, C.M. Laypeople Are Strategic Essentialists, Not Genetic Essentialists. Hastings Cent. Rep. 2019, 49, S27–S37. [Google Scholar] [CrossRef]
- Rasouly, H.M.; Cuneo, N.; Marasa, M.; DeMaria, N.; Chatterjee, D.; Thompson, J.J.; Fasel, D.A.; Wynn, J.; Chung, W.K.; Appelbaum, P.; et al. GeneLiFT: A novel test to facilitate rapid screening of genetic literacy in a diverse population undergoing genetic testing. J. Genet. Couns. 2021, 30, 742–754. [Google Scholar] [CrossRef]
- Veilleux, S.; Bouffard, M. Knowledge and understanding of pharmacogenomic testing among patients and health care professionals: A scoping review. Patient Educ. Couns. 2019, 102, 2001–2009. [Google Scholar] [CrossRef]
- Ha, V.T.D.; Frizzo-Barker, J.; Chow-White, P. Adopting clinical genomics: A systematic review of genomic literacy among physicians in cancer care. BMC Med. Genom. 2018, 11, 18. [Google Scholar] [CrossRef]
- Vears, D.F.; Minion, J.T.; Roberts, S.J.; Cummings, J.; Machirori, M.; Blell, M.; Budin-Ljosne, I.; Cowley, L.; Dyke, S.O.M.; Gaff, C.; et al. Return of individual research results from genomic research: A systematic review of stakeholder perspectives. PLoS ONE 2021, 16, e0258646. [Google Scholar] [CrossRef]
- Gualano, M.R.; Gili, R.; Scaioli, G.; Bert, F.; Siliquini, R. General population’s knowledge and attitudes about antibiotics: A systematic review and meta-analysis. Pharmacoepidemiol. Drug Saf. 2015, 24, 2–10. [Google Scholar] [CrossRef] [PubMed]
- Cespedes, A.; Larson, E. Knowledge, attitudes, and practices regarding antibiotic use among Latinos in the United States: Review and recommendations. Am. J. Infect. Control 2006, 34, 495–502. [Google Scholar] [CrossRef] [PubMed]
- Friedman, D.B.; Kanwat, C.P.; Headrick, M.L.; Patterson, N.J.; Neely, J.C.; Smith, L.U. Importance of prudent antibiotic use on dairy farms in South Carolina: A pilot project on farmers’ knowledge, attitudes and practices. Zoonoses Public Health 2007, 54, 366–375. [Google Scholar] [CrossRef] [PubMed]
- Cantarero-Arévalo, L.; Hallas, M.P.; Kaae, S. Parental knowledge of antibiotic use in children with respiratory infections: A systematic review. Int. J. Pharm. Pract. 2017, 25, 31–49. [Google Scholar] [CrossRef]
- Srinivasan, A.; Song, X.; Richards, A.; Sinkowitz-Cochran, R.; Cardo, D.; Rand, C. A Survey of Knowledge, Attitudes, and Beliefs of House Staff Physicians from Various Specialties Concerning Antimicrobial Use and Resistance. Arch. Intern. Med. 2004, 164, 1451–1456. [Google Scholar] [CrossRef]
- Carter, E.J.; Greendyke, W.G.; Furuya, E.Y.; Srinivasan, A.; Shelley, A.N.; Bothra, A.; Saiman, L.; Larson, E.L. Exploring the nurses’ role in antibiotic stewardship: A multisite qualitative study of nurses and infection preventionists. Am. J. Infect. Control 2018, 46, 492–497. [Google Scholar] [CrossRef]
- Harris, A.; Chandramohan, S.; Awali, R.A.; Grewal, M.; Tillotson, G.; Chopra, T. Physicians’ attitude and knowledge regarding antibiotic use and resistance in ambulatory settings. Am. J. Infect. Control 2019, 47, 864–868. [Google Scholar] [CrossRef]
- Bishop, C.; Yacoob, Z.; Knobloch, M.J.; Safdar, N. Community pharmacy interventions to improve antibiotic stewardship and implications for pharmacy education: A narrative overview. Res. Soc. Adm. Pharm. 2019, 15, 627–631. [Google Scholar] [CrossRef]
- Chahine, E.B.; El-Lababidi, R.M.; Sourial, M. Engaging Pharmacy Students, Residents, and Fellows in Antimicrobial Stewardship. J. Pharm. Pract. 2015, 28, 585–591. [Google Scholar] [CrossRef]
- McGuckin, M.; Govednik, J.; Hyman, D.; Black, B. Public reporting of health care-associated infection rates: Are consumers aware and engaged? Am. J. Med. Qual. 2014, 29, 83–85. [Google Scholar] [CrossRef] [PubMed]
- Longtin, Y.; Sax, H.; Leape, L.L.; Sheridan, S.E.; Donaldson, L.; Pittet, D. Patient participation: Current knowledge and applicability to patient safety. Mayo Clin. Proc. 2010, 85, 53–62. [Google Scholar] [CrossRef]
- Wikler, D. Can we learn from eugenics? J. Med. Ethics 1999, 25, 183–194. [Google Scholar] [CrossRef]
- Garver, K.L.; Garver, B. The Human Genome Project and eugenic concerns. Am. J. Hum. Genet. 1994, 54, 148–158. Available online: https://www.ncbi.nlm.nih.gov/pubmed/8279465 (accessed on 25 April 2022). [PubMed]
- Rothstein, M.A. GINA at Ten and the Future of Genetic Nondiscrimination Law. Hastings Cent. Rep. 2018, 48, 5–7. [Google Scholar] [CrossRef] [PubMed]
- Hudson, K.L.; Rothenberg, K.H.; Andrews, L.B.; Kahn, M.J.; Collins, F.S. Genetic discrimination and health insurance: An urgent need for reform. Science 1995, 270, 391–393. [Google Scholar] [CrossRef]
- Caulfield, T.; Burningham, S.; Joly, Y.; Master, Z.; Shabani, M.; Borry, P.; Becker, A.; Burgess, M.; Calder, K.; Critchley, C.; et al. A review of the key issues associated with the commercialization of biobanks. J. Law Biosci. 2014, 1, 94–110. [Google Scholar] [CrossRef]
- Cho, M. Patently unpatentable: Implications of the Myriad court decision on genetic diagnostics. Trends Biotechnol. 2010, 28, 548–551. [Google Scholar] [CrossRef] [PubMed]
- Meagher, K.M.; McGowan, M.L.; Settersten, R.A., Jr.; Fishman, J.R.; Juengst, E.T. Precisely Where Are We Going? Charting the New Terrain of Precision Prevention. Annu. Rev. Genom. Hum. Genet. 2017, 18, 369–387. [Google Scholar] [CrossRef]
- Sabatello, M.; Juengst, E. Genomic Essentialism: Its Provenance and Trajectory as an Anticipatory Ethical Concern. Hastings Cent. Rep. 2019, 49, S10–S18. [Google Scholar] [CrossRef]
- Hindorff, L.A.; Bonham, V.L.; Brody, L.C.; Ginoza, M.E.C.; Hutter, C.M.; Manolio, T.A.; Green, E.D. Prioritizing diversity in human genomics research. Nat. Rev. Genet. 2018, 19, 175–185. [Google Scholar] [CrossRef] [PubMed]
- Juengst, E.T.; Flatt, M.A.; Settersten, R.A., Jr. Personalized genomic medicine and the rhetoric of empowerment. Hastings Cent. Rep. 2012, 42, 34–40. [Google Scholar] [CrossRef]
- Kass, N.E.; Medley, A.M.; Natowicz, M.R.; Hull, S.C.; Faden, R.R.; Plantinga, L.; Gostin, L.O. Access to health insurance: Experiences and attitudes of those with genetic versus non-genetic medical conditions. Am. J. Med. Genet. A 2007, 143A, 707–717. [Google Scholar] [CrossRef]
- Koski, C.A. The Human Genome Project: An examination of its challenge to the technological imperative. New Genet. Soc. 2005, 24, 265–281. [Google Scholar] [CrossRef]
- Landeweerd, L.; Townend, D.; Mesman, J.; Van Hoyweghen, I. Reflections on different governance styles in regulating science: A contribution to ‘Responsible Research and Innovation’. Life Sci. Soc. Policy 2015, 11, 8. [Google Scholar] [CrossRef]
- Liegl, M.; Boden, A.; Buscher, M.; Oliphant, R.; Kerasidou, X. Designing for ethical innovation: A case study on ELSI co-design in emergency. Int. J. Hum. Comput. Stud. 2016, 95, 80–95. [Google Scholar] [CrossRef]
- Heyman, G.; Cars, O.; Bejarano, M.T.; Peterson, S. Access, excess, and ethics—Towards a sustainable distribution model for antibiotics. Ups. J Med. Sci. 2014, 119, 134–141. [Google Scholar] [CrossRef]
- Millar, M. Can antibiotic use be both just and sustainable. or only more or less so? J. Med. Ethics 2011, 37, 153–157. [Google Scholar] [CrossRef]
- Klein, E.Y.; Van Boeckel, T.P.; Martinez, E.M.M.; Pant, S.; Gandra, S.; Levin, S.A.; Goossens, H.; Laxminarayan, R. Global increase and geographic convergence in antibiotic consumption between 2000 and 2015. Proc. Natl. Acad. Sci. USA 2018, 115, E3463–E3470. [Google Scholar] [CrossRef] [PubMed]
- Clift, C.; Salisbury, D.M. Enhancing the role of vaccines in combatting antimicrobial resistance. Vaccine 2017, 35, 6591–6593. [Google Scholar] [CrossRef] [PubMed]
- Wauters, A.; Van Hoyweghen, I. Global trends on fears and concerns of genetic discrimination: A systematic literature review. J. Hum. Genet. 2016, 61, 275–282. [Google Scholar] [CrossRef] [PubMed]
- Contreras, J.L. COVID-19 as an example of why genomic sequence data should remain patent ineligible. In COVID-19 Policy Playbook: Legal Recommendations for a Safer, More Equitable Future; Burris, S., de Guia, S., Gable, L., Levin, D.E., Parmet, W.E., Terry, N.P., Eds.; Public Health Law Watch: Boston, MA, USA, 2021. [Google Scholar]
- Lázaro-Muñoz, G.; Conley, J.M.; Davis, A.M.; Prince, A.E.; Cadigan, R.J. Which Results to Return: Subjective Judgments in Selecting Medically Actionable Genes. Genet. Test. Mol. Biomark. 2017, 21, 184–194. [Google Scholar] [CrossRef]
- McArthur, A.G.; Wright, G.D. Bioinformatics of antimicrobial resistance in the age of molecular epidemiology. Curr. Opin. Microbiol. 2015, 27, 45–50. [Google Scholar] [CrossRef] [PubMed]
- Jia, B.; Raphenya, A.R.; Alcock, B.; Waglechner, N.; Guo, P.; Tsang, K.K.; Lago, B.A.; Dave, B.M.; Pereira, S.; Sharma, A.N.; et al. CARD 2017: Expansion and model-centric curation of the comprehensive antibiotic resistance database. Nucleic Acids Res. 2017, 45, D566–D573. [Google Scholar] [CrossRef] [PubMed]
- Gupta, S.K.; Padmanabhan, B.R.; Diene, S.M.; Lopez-Rojas, R.; Kempf, M.; Landraud, L.; Rolain, J.M. ARG-ANNOT, a new bioinformatic tool to discover antibiotic resistance genes in bacterial genomes. Antimicrob. Agents Chemother. 2014, 58, 212–220. [Google Scholar] [CrossRef] [PubMed]
- Zankari, E.; Allesoe, R.; Joensen, K.G.; Cavaco, L.M.; Lund, O.; Aarestrup, F.M. PointFinder: A novel web tool for WGS-based detection of antimicrobial resistance associated with chromosomal point mutations in bacterial pathogens. J. Antimicrob. Chemother. 2017, 72, 2764–2768. [Google Scholar] [CrossRef]
- Goldenberg, A.; Brothers, K. Misplaced Trust: Building Research Relationships in the Age of Biorepository Networks. Am. J. Bioeth. 2018, 18, 21–23. [Google Scholar] [CrossRef]
- Bezuidenhout, L.; Chakauya, E. Hidden concerns of sharing research data by low/middle-income country scientists. Glob. Bioeth. 2018, 29, 39–54. [Google Scholar] [CrossRef]
- Yozwiak, N.L.; Schaffner, S.F.; Sabeti, P.C. Data sharing: Make outbreak research open access. Nature 2015, 518, 477–479. [Google Scholar] [CrossRef] [PubMed]
- CDC. Antibiotic Resistance Threats in the United States, 2019; Centers for Disease Control and Prevention: Atlanta, GA, USA, 2019.
- Burnham, J.P.; Olsen, M.A.; Kollef, M.H. Re-estimating annual deaths due to multidrug-resistant organism infections. Infect. Control. Hosp. Epidemiol. 2019, 40, 112–113. [Google Scholar] [CrossRef]
- Rump, B.; Timen, A.; Verweij, M.; Hulscher, M. Experiences of carriers of multidrug-resistant organisms: A systematic review. Clin. Microbiol. Infect. 2019, 25, 274–279. [Google Scholar] [CrossRef]
- Goldsack, J.C.; DeRitter, C.; Power, M.; Spencer, A.; Taylor, C.L.; Kim, S.F.; Kirk, R.; Drees, M. Clinical, patient experience and cost impacts of performing active surveillance on known methicillin-resistant Staphylococcus aureus positive patients admitted to medical-surgical units. Am. J. Infect. Control 2014, 42, 1039–1043. [Google Scholar] [CrossRef] [PubMed]
- Catalano, G.; Houston, S.H.; Catalano, M.C.; Butera, A.S.; Jennings, S.M.; Hakala, S.M.; Burrows, S.L.; Hickey, M.G.; Duss, C.V.; Skelton, D.N.; et al. Anxiety and depression in hospitalized patients in resistant organism isolation. South. Med. J. 2003, 96, 141–146. [Google Scholar] [CrossRef] [PubMed]
- Sengupta, A.; Rand, C.; Perl, T.M.; Milstone, A.M. Knowledge, awareness, and attitudes regarding methicillin-resistant Staphylococcus aureus among caregivers of hospitalized children. J. Pediatr. 2011, 158, 416–421. [Google Scholar] [CrossRef] [PubMed]
- Skyman, E.; Lindahl, B.; Bergbom, I.; Sjostrom, H.T.; Ahren, C. Being Met as marked—Patients’ experiences of being infected with community-acquired methicillin-resistant Staphylococcus aureus (MRSA). Scand. J. Caring Sci. 2016, 30, 813–820. [Google Scholar] [CrossRef] [PubMed]
- Andersson, H.; Lindholm, C.; Fossum, B. MRSA—Global threat and personal disaster: Patients’ experiences. Int. Nurs. Rev. 2011, 58, 47–53. [Google Scholar] [CrossRef] [PubMed]
- Baekkeskov, E.; Rubin, O.; Munkholm, L.; Zaman, W. Antimicrobial Resistance as a Global Health Crisis. In Oxford Research Encyclopedia of Politics; Oxford University Press: Oxford, UK, 2020; Available online: https://oxfordre.com/politics/view/10.1093/acrefore/9780190228637.001.0001/acrefore-9780190228637-e-1626 (accessed on 15 September 2021).
- Landecker, H. Antibiotic Resistance and the Biology of History. Body Soc. 2016, 22, 19–52. [Google Scholar] [CrossRef] [PubMed]
- Mendelson, M.; Sharland, M.; Mpundu, M. Antibiotic resistance: Calling time on the ‘silent pandemic’. JAC Antimicrob. Resist. 2022, 4, dlac016. [Google Scholar] [CrossRef] [PubMed]
- Abimbola, S.; Otieno, M.; Cole, J. Reducing the Use of Antimicrobials as a Solution to the Challenge of Antimicrobial Resistance (AMR): Approaching an Ethical Dilemma through the Lens of Planetary Health. Challenges 2021, 12, 23. [Google Scholar] [CrossRef]
- Kirchhelle, C.; Atkinson, P.; Broom, A.; Chuengsatiansup, K.; Ferreira, J.P.; Fortane, N.; Frost, I.; Gradmann, C.; Hinchliffe, S.; Hoffman, S.J.; et al. Setting the standard: Multidisciplinary hallmarks for structural, equitable and tracked antibiotic policy. BMJ Glob. Health 2020, 5, e003091. [Google Scholar] [CrossRef]
- Wallinga, D.; Kar, A.; Klein, E. New Data: Animal vs. Human Antibiotic Use Remains Lopsided. In Expert Blog; Natural Resources Defense Council: New York, NY, USA, 2020; Available online: https://www.nrdc.org/experts/david-wallinga-md/most-human-antibiotics-still-going-us-meat-production (accessed on 27 June 2022).
- Van Boeckel, T.P.; Brower, C.; Gilbert, M.; Grenfell, B.T.; Levin, S.A.; Robinson, T.P.; Teillant, A.; Laxminarayan, R. Global trends in antimicrobial use in food animals. Proc. Natl. Acad. Sci. USA 2015, 112, 5649–5654. [Google Scholar] [CrossRef] [PubMed]
- Manyi-Loh, C.; Mamphweli, S.; Meyer, E.; Okoh, A. Antibiotic Use in Agriculture and Its Consequential Resistance in Environmental Sources: Potential Public Health Implications. Molecules 2018, 23, 795. [Google Scholar] [CrossRef]
- Ferguson, C. Animal agriculture is not the cause of antibiotic resistance. The Baltimore Sun. 16 May 2019. Available online: https://www.baltimoresun.com/opinion/readers-respond/bs-ed-rr-agriculture-antibiotic-resistance-20190516-story.html (accessed on 23 June 2022).
- McKernan, C.; Benson, T.; Farrell, S.; Dean, M. Antimicrobial use in agriculture: Critical review of the factors influencing behaviour. JAC-Antimicrob. Resist. 2021, 3, dlab178. [Google Scholar] [CrossRef] [PubMed]
- Ahmed, S.A.; Barış, E.; Go, D.S.; Lofgren, H.; Osorio-Rodarte, I.; Thierfelder, K. Assessing the global poverty effects of antimicrobial resistance. World Dev. 2018, 111, 148–160. [Google Scholar] [CrossRef]
- Keshavjee, S.; Farmer, P.E. Tuberculosis, drug resistance, and the history of modern medicine. N. Engl. J. Med. 2012, 367, 931–936. [Google Scholar] [CrossRef] [PubMed]
- Pareek, M.; Greenaway, C.; Noori, T.; Munoz, J.; Zenner, D. The impact of migration on tuberculosis epidemiology and control in high-income countries: A review. BMC Med. 2016, 14, 48. [Google Scholar] [CrossRef] [PubMed]
- Stegger, M.; Wirth, T.; Andersen, P.S.; Skov, R.L.; De Grassi, A.; Simoes, P.M.; Tristan, A.; Petersen, A.; Aziz, M.; Kiil, K.; et al. Origin and evolution of European community-acquired methicillin-resistant Staphylococcus aureus. mBio 2014, 5, e01044-14. [Google Scholar] [CrossRef]
- Uhlemann, A.-C.; McAdam, P.R.; Sullivan, S.B.; Knox, J.R.; Khiabanian, H.; Rabadan, R.; Davies, P.R.; Fitzgerald, J.R.; Lowy, F.D.; Daum, R.; et al. Evolutionary Dynamics of Pandemic Methicillin-Sensitive Staphylococcus aureus ST398 and Its International Spread via Routes of Human Migration. mBio 2017, 8, e01375-16. [Google Scholar] [CrossRef]
- Lonnroth, K.; Mor, Z.; Erkens, C.; Bruchfeld, J.; Nathavitharana, R.R.; van der Werf, M.J.; Lange, C. Tuberculosis in migrants in low-incidence countries: Epidemiology and intervention entry points. Int. J. Tuberc. Lung Dis. 2017, 21, 624–637. [Google Scholar] [CrossRef] [PubMed]
- Kamenshchikova, A.; Wolffs, P.F.G.; Hoebe, C.J.; Penders, J.; Horstman, K. Complex narratives of health, stigma and control: Antimicrobial resistance screening among non-hospitalized refugees. Soc. Sci. Med. 2018, 212, 43–49. [Google Scholar] [CrossRef] [PubMed]
- Langmuir, A.D. The surveillance of communicable diseases of national importance. N. Engl. J. Med. 1963, 268, 182–192. [Google Scholar] [CrossRef] [PubMed]
- Lee, L.M.; Steven, M.; Teutsch, M.; Stephen, B.; Thacker, M.S.; Louis, M.E.S. Principles and Practice of Public Health Surveillance; Oxford University Press: New York, NY, USA, 2010. [Google Scholar]
- Jackson, C.; Gardy, J.L.; Shadiloo, H.C.; Silva, D.S. Trust and the ethical challenges in the use of whole genome sequencing for tuberculosis surveillance: A qualitative study of stakeholder perspectives. BMC Med. Ethics 2019, 20, 43. [Google Scholar] [CrossRef]
- McClelland, A.; Guta, A.; Gagnon, M. The rise of molecular HIV surveillance: Implications on consent and criminalization. Crit. Public Health 2020, 30, 487–493. [Google Scholar] [CrossRef]
- Molldrem, S.; Smith, A.K.J. Reassessing the Ethics of Molecular HIV Surveillance in the Era of Cluster Detection and Response: Toward HIV Data Justice. AJOB 2020, 20, 10–23. [Google Scholar] [CrossRef]
- WHO Global Antimicrobial Resistance and Use Surveillance System (GLASS). Available online: https://www.who.int/initiatives/glass (accessed on 12 February 2020).
- Gostin, L.O.; Lazzarini, Z. Human Rights and Public Health in the AIDS Pandemic; Oxford University Press: New York, NY, USA, 1997. [Google Scholar]
- Warmbrod, K.L.; West, R.; Frieman, M.; George, D.; Martin, E.; Rivers, C. Staying Ahead of the Variants: Policy Recommendations to Identify and Manage. Current and Future Variants of Concern; Johns Hopkins Center for Health Security: Baltimore, MD, USA, 2021. [Google Scholar]
- Jaillard, M.; van Belkum, A.; Cady, K.C.; Creely, D.; Shortridge, D.; Blanc, B.; Barbu, E.M.; Dunne, W.M., Jr.; Zambardi, G.; Enright, M.; et al. Correlation between phenotypic antibiotic susceptibility and the resistome in Pseudomonas aeruginosa. Int. J. Antimicrob. Agents 2017, 50, 210–218. [Google Scholar] [CrossRef] [PubMed]
- Boyce, T.; Murray, E.; Holmes, A. What are the drivers of the UK media coverage of meticillin-resistant Staphylococcus aureus, the inter-relationships and relative influences? J. Hosp. Infect. 2009, 73, 400–407. [Google Scholar] [CrossRef] [PubMed]
- The Lancet. MRSA: How politicians are missing the point. Lancet 2005, 365, 1203. [Google Scholar] [CrossRef]
- Anderson, M.; Schulze, K.; Cassini, A.; Plachouras, D.; Mossialos, E. A governance framework for development and assessment of national action plans on antimicrobial resistance. Lancet Infect. Dis. 2019, 19, e371–e384. [Google Scholar] [CrossRef]
- Thakur, M.; Kumar, V. Expanding antimicrobial resistance and shrinking antibiotic arsenal: Phytochemicals—A ray of hope. MGM J. Med. Sci. 2019, 6, 191–193. [Google Scholar] [CrossRef]
- Bookstaver, P.B.; Nimmich, E.B.; Smith, T.J.; Justo, J.A.; Kohn, J.; Hammer, K.L.; Troficanto, C.; Albrecht, H.A.; Al-Hasan, M.N. Cumulative Effect of an Antimicrobial Stewardship and Rapid Diagnostic Testing Bundle on Early Streamlining of Antimicrobial Therapy in Gram-Negative Bloodstream Infections. Antimicrob. Agents Chemother. 2017, 61, e00189-17. [Google Scholar] [CrossRef] [PubMed]
- Foster, R.A.; Kuper, K.; Lu, Z.K.; Bookstaver, P.B.; Bland, C.M.; Mahoney, M.V. Pharmacists’ Familiarity with and Institutional Utilization of Rapid Diagnostic Technologies for Antimicrobial Stewardship. Infect. Control Hosp. Epidemiol. 2017, 38, 863–866. [Google Scholar] [CrossRef] [PubMed]
- Cash, R.A. Ethical issues in adapting new technologies for rapid diagnosis. Indian J. Med. Ethics 2013, 10, 254–255. [Google Scholar] [CrossRef] [PubMed]
- Burchett, H.E.; Leurent, B.; Baiden, F.; Baltzell, K.; Bjorkman, A.; Bruxvoort, K.; Clarke, S.; DiLiberto, D.; Elfving, K.; Goodman, C.; et al. Improving prescribing practices with rapid diagnostic tests (RDTs): Synthesis of 10 studies to explore reasons for variation in malaria RDT uptake and adherence. BMJ Open 2017, 7, e012973. [Google Scholar] [CrossRef] [PubMed]
- Paul, M.; Dickstein, Y.; Raz-Pasteur, A. Antibiotic de-escalation for bloodstream infections and pneumonia: Systematic review and meta-analysis. Clin. Microbiol. Infect. 2016, 22, 960–967. [Google Scholar] [CrossRef]
- Campion, M.; Scully, G. Antibiotic Use in the Intensive Care Unit: Optimization and De-Escalation. J. Intensive Care Med. 2018, 33, 647–655. [Google Scholar] [CrossRef] [PubMed]
- Olivier, C.; Williams-Jones, B.; Godard, B.; Mikalson, B.; Ozdemir, V. Personalized medicine, bioethics and social responsibilities: Re-thinking the pharmaceutical industry to remedy inequities in patient care and international health. Curr. Pharm. Person. Med. 2008, 6, 108–120. [Google Scholar] [CrossRef][Green Version]
- Munthe, C.; Nijsingh, N. Cutting red tape to manage public health threats: An ethical dilemma of expediting antibiotic drug innovation. Bioethics 2019, 33, 785–791. [Google Scholar] [CrossRef] [PubMed]
- Selgelid, M.J. Research Priorities, Profits, and Public Goods: The Case of Drug Resistant Disease. In Business Ethics of Innovation; Hanekamp, G., Wütscher, F., Eds.; Springer: Berlin/Heidelberg, Germany, 2007; pp. 27–38. [Google Scholar]
- Krockow, E.M.; Tarrant, C. The international dimensions of antimicrobial resistance: Contextual factors shape distinct ethical challenges in South Africa, Sri Lanka and the United Kingdom. Bioethics 2019, 33, 756–765. [Google Scholar] [CrossRef]
- Renwick, M.J.; Brogan, D.M.; Mossialos, E. A systematic review and critical assessment of incentive strategies for discovery and development of novel antibiotics. J. Antibiot. 2016, 69, 73–88. [Google Scholar] [CrossRef] [PubMed]
- Littmann, J.; Buyx, A.; Cars, O. Antibiotic resistance: An ethical challenge. Int. J. Antimicrob. Agents 2015, 46, 359–361. [Google Scholar] [CrossRef]
- Gilbert, G.L.; Kerridge, I. Hospital Infection Prevention and Control (IPC) and Antimicrobial Stewardship (AMS): Dual Strategies to Reduce Antibiotic Resistance (ABR) in Hospitals. In Ethics and Drug Resistance: Collective Responsibility for Global Public Health; Jamrozik, E., Selgelid, M., Eds.; Springer International Publishing: Cham, Switzerland, 2020; pp. 89–108. [Google Scholar]
- Broom, A.; Broom, J.; Kirby, E. Cultures of resistance? A Bourdieusian analysis of doctors’ antibiotic prescribing. Soc. Sci. Med. 2014, 110, 81–88. [Google Scholar] [CrossRef]
- Lawati, M.H.A.; Dennis, S.; Short, S.D.; Abdulhadi, N.N. Patient safety and safety culture in primary health care: A systematic review. BMC Fam. Pract. 2018, 19, 104. [Google Scholar] [CrossRef]
- Sammer, C.E.; Lykens, K.; Singh, K.P.; Mains, D.A.; Lackan, N.A. What is patient safety culture? A review of the literature. J. Nurs. Scholarsh. 2010, 42, 156–165. [Google Scholar] [CrossRef]
- Quainoo, S.; Coolen, J.P.M.; van Hijum, S.; Huynen, M.A.; Melchers, W.J.G.; van Schaik, W.; Wertheim, H.F.L. Whole-Genome Sequencing of Bacterial Pathogens: The Future of Nosocomial Outbreak Analysis. Clin. Microbiol. Rev. 2017, 30, 1015–1063. [Google Scholar] [CrossRef]
- Bougnoux, M.-E.; Brun, S.; Zahar, J.-R. Healthcare-associated fungal outbreaks: New and uncommon species, New molecular tools for investigation and prevention. Antimicrob. Resist. Infect. Control 2018, 7, 45. [Google Scholar] [CrossRef]
- Angeletti, S.; Dicuonzo, G.; Lo Presti, A.; Cella, E.; Crea, F.; Avola, A.; Vitali, M.A.; Fagioni, M.; De Florio, L. MALDI-TOF Mass spectrometry and blakpc gene phylogenetic analysis of an outbreak of carbapenem-resistant K. pneumoniae strains. New Microbiol. 2015, 38, 541–550. Available online: https://www.ncbi.nlm.nih.gov/pubmed/26485012 (accessed on 8 January 2020). [PubMed]
- Lee, S.E.; Scott, L.D.; Dahinten, V.S.; Vincent, C.; Lopez, K.D.; Park, C.G. Safety Culture, Patient Safety, and Quality of Care Outcomes: A Literature Review. West. J. Nurs. Res. 2019, 41, 279–304. [Google Scholar] [CrossRef]
- Institute of Medicine. Committee on Quality of Health Care in America. In To Err Is Human: Building a Safer Health System; Kohn, L.T., Corrigan, J.M., Donaldson, M.S., Eds.; National Academies Press (US): Washington, DC, USA, 2000. [Google Scholar]
- Sorrell, J.M. Ethics: Ethical issues with medical errors: Shaping a culture of safety in healthcare. OJIN Online J. Issues Nurs. 2017, 22. [Google Scholar] [CrossRef]
- Sharpe, V.A.; Faden, A.I. Medical Harm: Historical, Conceptual and Ethical Dimensions of Iatrogenic Illness; Cambridge University Press: Cambridge, UK, 1998. [Google Scholar]
- Singh, H.; Carayon, P. A Roadmap to Advance Patient Safety in Ambulatory Care. JAMA 2020, 324, 2481–2482. [Google Scholar] [CrossRef]
- Dekker, S.W.; Leveson, N.G. The systems approach to medicine: Controversy and misconceptions. BMJ Qual. Saf. 2015, 24, 7–9. [Google Scholar] [CrossRef]
- Khan, N.; Ahmad, I.; Ilyas, M. Impact of ethical leadership on organizational safety performance: The mediating role of safety culture and safety consciousness. Ethics Behav. 2018, 28, 628–643. [Google Scholar] [CrossRef]
- Barlam, T.F.; Cosgrove, S.E.; Abbo, L.M.; MacDougall, C.; Schuetz, A.N.; Septimus, E.J.; Srinivasan, A.; Dellit, T.H.; Falck-Ytter, Y.T.; Fishman, N.O.; et al. Implementing an Antibiotic Stewardship Program: Guidelines by the Infectious Diseases Society of America and the Society for Healthcare Epidemiology of America. Clin. Infect. Dis. 2016, 62, e51–e77. [Google Scholar] [CrossRef] [PubMed]
- Manning, M.L.; Pfeiffer, J.; Larson, E.L. Combating antibiotic resistance: The role of nursing in antibiotic stewardship. Am. J. Infect. Control 2016, 44, 1454–1457. [Google Scholar] [CrossRef]
- Sakeena, M.H.F.; Bennett, A.A.; McLachlan, A.J. Enhancing pharmacists’ role in developing countries to overcome the challenge of antimicrobial resistance: A narrative review. Antimicrob. Resist. Infect. Control. 2018, 7, 63. [Google Scholar] [CrossRef]
- Van Goethem, N.; Struelens, M.J.; De Keersmaecker, S.C.J.; Roosens, N.H.C.; Robert, A.; Quoilin, S.; Van Oyen, H.; Devleesschauwer, B. Perceived utility and feasibility of pathogen genomics for public health practice: A survey among public health professionals working in the field of infectious diseases, Belgium, 2019. BMC Public Health 2020, 20, 1318. [Google Scholar] [CrossRef]
- Oakley, J. The Virtuous Physician and Antimicrobial Prescribing Policy and Practice. In Ethics and Drug Resistance: Collective Responsibility for Global Public Health; Jamrozik, E., Selgelid, M., Eds.; Springer International Publishing: Cham, Switzerland, 2020; pp. 125–140. [Google Scholar]
- Charani, E.; Castro-Sanchez, E.; Sevdalis, N.; Kyratsis, Y.; Drumright, L.; Shah, N.; Holmes, A. Understanding the determinants of antimicrobial prescribing within hospitals: The role of “prescribing etiquette”. Clin. Infect. Dis. 2013, 57, 188–196. [Google Scholar] [CrossRef]
- Fynbo, L.; Jensen, C.S. Antimicrobial stigmatization: Public health concerns about conventional pig farming and pig farmers’ experiences with stigmatization. Soc. Sci. Med. 2018, 201, 1–8. [Google Scholar] [CrossRef]
- Mitchell, J.; Cooke, P.; Ahorlu, C.; Arjyal, A.; Baral, S.; Carter, L.; Dasgupta, R.; Fieroze, F.; Fonseca-Braga, M.; Huque, R.; et al. Community engagement: The key to tackling Antimicrobial Resistance (AMR) across a One Health context? Glob. Public Health 2021, 1–18. Available online: https://www.ncbi.nlm.nih.gov/pubmed/34882505 (accessed on 15 July 2022). [CrossRef]
- Bakhit, M.; Del Mar, C.; Gibson, E.; Hoffmann, T. Exploring patients’ understanding of antibiotic resistance and how this may influence attitudes towards antibiotic use for acute respiratory infections: A qualitative study in Australian general practice. BMJ Open 2019, 9, e026735. [Google Scholar] [CrossRef]
- King, A.J.; Wald, D.M.; Coberley, D.D.; Dahlstrom, M.F.; Plummer, P.J. Science communication challenges about antimicrobial resistance in animal agriculture: Insights from stakeholders. JAC Antimicro. 2022, 4, dlac032. [Google Scholar] [CrossRef]
| Framing of AMR | Source | Title | Quote |
|---|---|---|---|
| Stewardship | Broom et al. 2020. [11] | Antimicrobial resistance as a problem of values? Views from three continents | “The move from de-contextualised information (data) to social action is highly dependent upon various forms of social relations, power dynamics, and the institutionalisation of professional and political practice.” |
| Global health justice | Hoffman et al. 2015. [23] | An international legal framework to address antimicrobial resistance | “To avert millions of deaths caused by treatable infections, access to antimicrobials should be scaled-up for the many people worldwide who cannot obtain or afford such drugs.” |
| Collective action problem | Giubilini 2019. [24] | Antibiotic resistance as a tragedy of the commons: An ethical argument for a tax on antibiotic use in humans | “Antibiotic effectiveness is a common good, or a common pool resource. These types of goods are defined, among other things, by the fact that each individual who enjoys them contributes to their erosion.” |
| Slowly emerging epidemic | Viens and Littmann. 2015. [25] | Is Antimicrobial Resistance a Slowly Emerging Disaster? | “Whether terms such as disaster or pandemic are contested concepts or reflect different health issue prioritizations, how we define and use technical terms matters. We should be very wary of people who throw such terms around so capriciously as synonyms for public health problems that are important, urgent or serious.” |
| One Health policy | Antoine-Moussiax et al. 2019. [21] | The good, the bad and the ugly: framing debates on nature in a One Health community | “While each positionally objective view may be useful, when considered separately, they may lead to mistakes due to the biased perspective of the position. The main issue is not to assess the impact of logically equivalent (i.e., having the same truth-value that is, being verified by the same facts) framings on decision-making, but to deal with descriptions having different truth-values (i.e., being verified by different facts and actors).” |
| Wicked problem | Littmann, Viens & Silva. 2020. [26] | The Super-Wicked Problem of Antimicrobial Resistance | “To put it another way, through framing AMR as a super-wicked problem, we not only acknowledge that previous approaches are unlikely to be sustainable in the long run, but we are also forced to ask what sort of values and norms could justify new policy options that would not only be effective but also ethical. This is all the more relevant because understanding AMR as more than a scientific or technical issue is a relatively new perspective.” |
| Shared Domains | ELSI and Human Genetics | ELSI and Resistance Genetics |
|---|---|---|
| Understanding and attitudes | Genetic determinism | Views on immunity, infections |
| Familiarity and expectations | Implementation barriers and facilitators | |
| Genetic literacy | Cross-sectional affected stakeholders | |
| Disclosing to third parties | Communicability | |
| Health equity | Insurance discrimination | Global health policy |
| Information and empowerment | Access and excess interrelatedness | |
| Eugenics | Disparities of disease burden | |
| Commercialization | Drug-development pipeline | |
| Race, essentialism, genetics | Laboratory and research capacity | |
| Data governance | Privacy and identifiability | Surveillance and privacy |
| Data sharing | Global health collaborations | |
| Reciprocity | Local trust | |
| Broad consent | Data for action | |
| Utilization and sustainability |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2022 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Meagher, K.M.; Watson, S.; Suh, G.A.; Virk, A. The New Precision Stewards? J. Pers. Med. 2022, 12, 1308. https://doi.org/10.3390/jpm12081308
Meagher KM, Watson S, Suh GA, Virk A. The New Precision Stewards? Journal of Personalized Medicine. 2022; 12(8):1308. https://doi.org/10.3390/jpm12081308
Chicago/Turabian StyleMeagher, Karen M., Sara Watson, Gina A. Suh, and Abinash Virk. 2022. "The New Precision Stewards?" Journal of Personalized Medicine 12, no. 8: 1308. https://doi.org/10.3390/jpm12081308
APA StyleMeagher, K. M., Watson, S., Suh, G. A., & Virk, A. (2022). The New Precision Stewards? Journal of Personalized Medicine, 12(8), 1308. https://doi.org/10.3390/jpm12081308







