Making Radiomics More Reproducible across Scanner and Imaging Protocol Variations: A Review of Harmonization Methods
Abstract
:1. Introduction
- Have scanner and protocol variations affected the reproducibility of radiomic features/images? If yes, the how significant was the change?
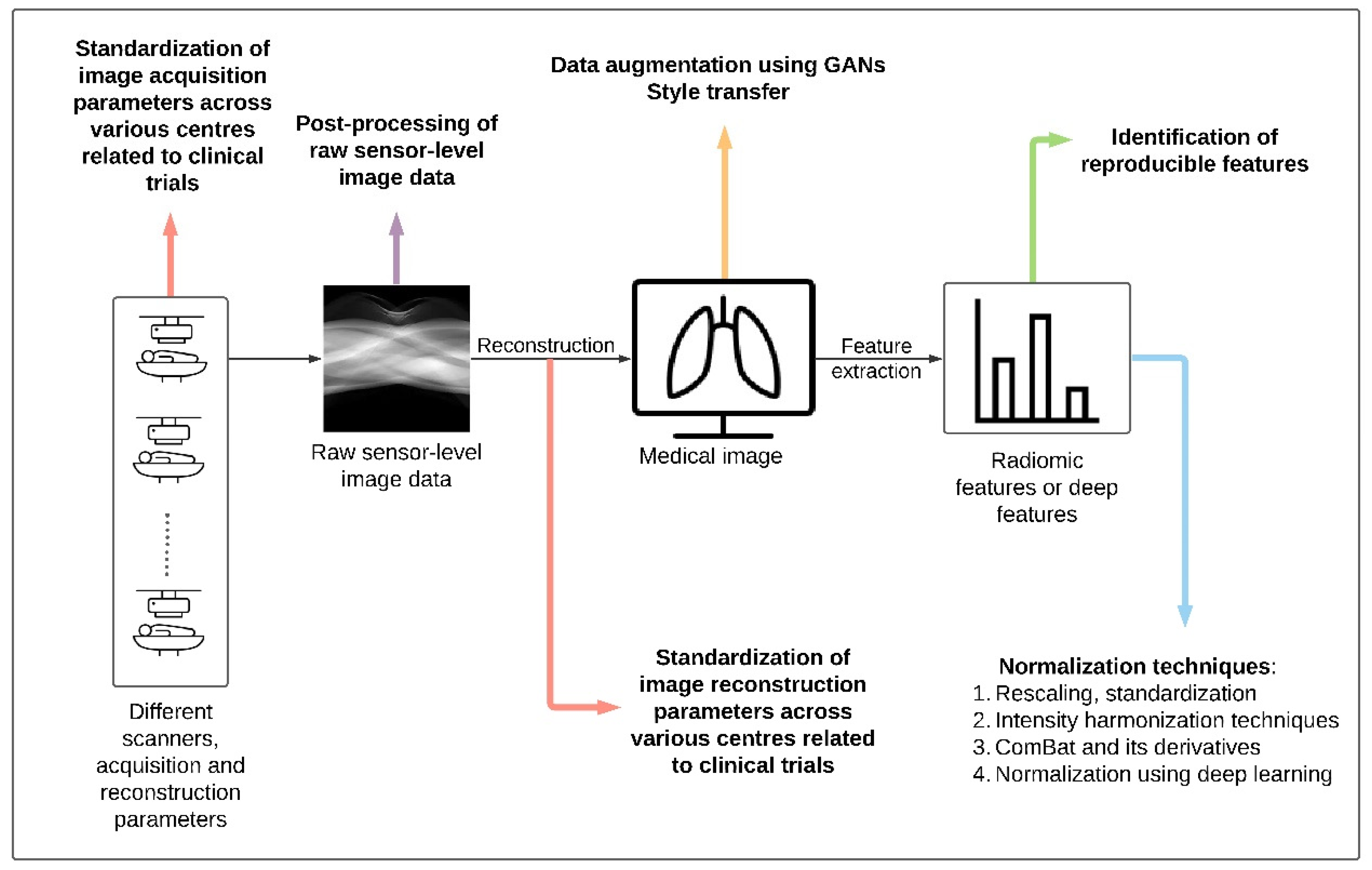
- Various harmonization methods were identified in previous work. Can they be categorized into domains (image and feature)? Furthermore, can the methods be applied at different stages of medical imaging (Figure 2)?
- What are the latest developments in the field of radiomics to make radiomics more reproducible?
- Are there non-medical studies performed to harmonize images/features? What are the different types of methods?
- What are the advantages, disadvantages and challenges of various harmonization methods?
2. Image Domain Harmonization
2.1. Standardization of Image Acquisition and Reconstruction Parameters across Various Centers Related to Clinical Trials
2.2. Post-Processing of Raw Sensor-Level Image Data
2.3. Data Augmentation Using GANs
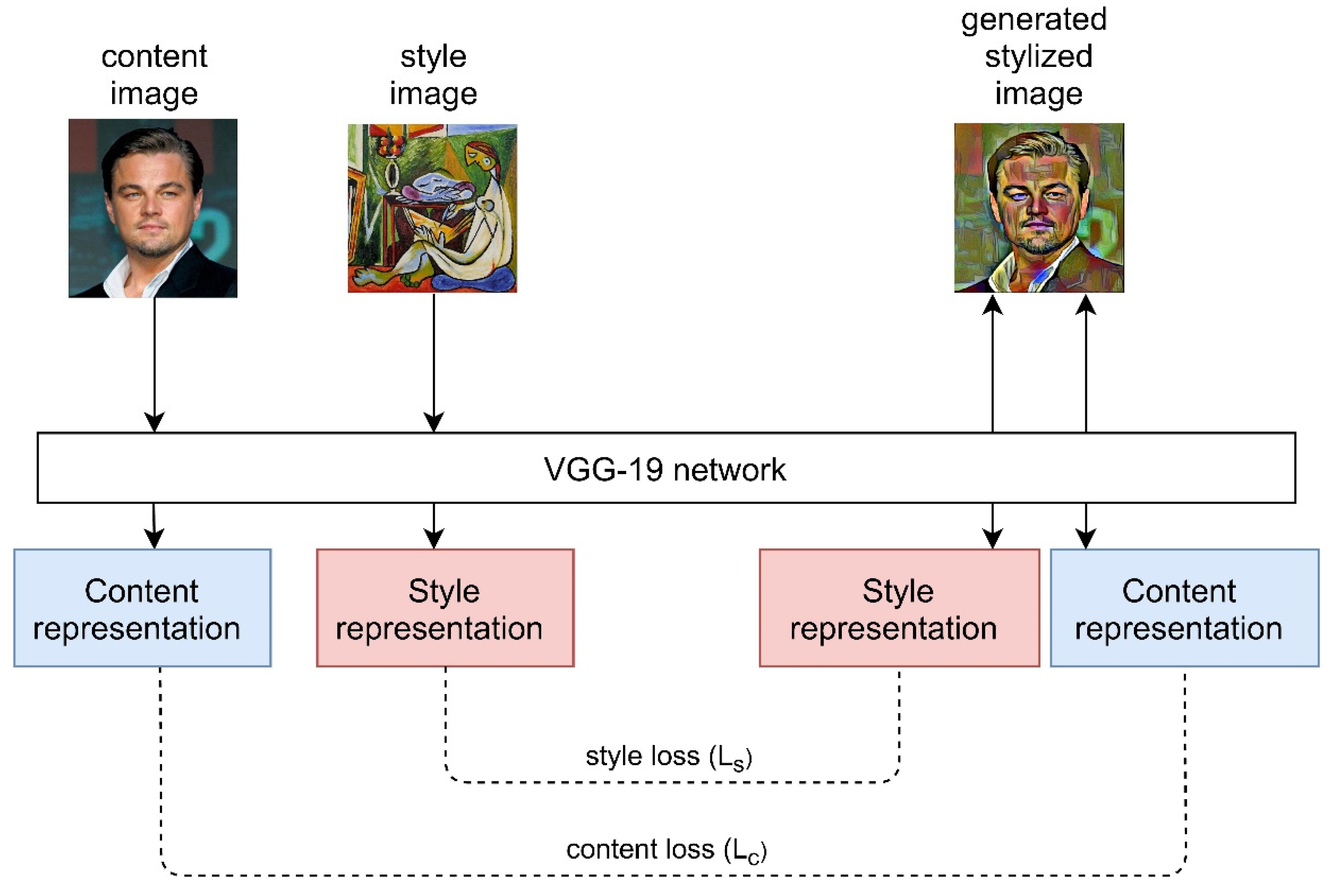
2.4. Style Transfer
3. Feature Domain Harmonization
3.1. Focusing on Reproducible Features (Identification of Reproducible Features)
3.2. Normalization Techniques
3.2.1. Statistical Normalization
3.2.2. Intensity Harmonization Techniques
3.2.3. ComBat Method and Its Derivatives
3.2.4. Normalization Using Deep Learning
4. Discussion
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Aerts, H.J.W.L.; Velazquez, E.R.; Leijenaar, R.T.H.; Parmar, C.; Grossmann, P.; Carvalho, S.; Bussink, J.; Monshouwer, R.; Haibe-Kains, B.; Rietveld, D.; et al. Decoding tumour phenotype by noninvasive imaging using a quantitative radiomics approach. Nat. Commun. 2014, 5, 4006. [Google Scholar] [CrossRef]
- Hood, L.; Friend, S.H. Predictive, personalized, preventive, participatory (P4) cancer medicine. Nat. Rev. Clin. Oncol. 2011, 8, 184–187. [Google Scholar] [CrossRef]
- Lambin, P.; Rios-Velazquez, E.; Leijenaar, R.; Carvalho, S.; van Stiphout, R.G.P.M.; Granton, P.; Zegers, C.M.L.; Gillies, R.; Boellard, R.; Dekker, A.; et al. Radiomics: Extracting more information from medical images using advanced feature analysis. Eur. J. Cancer 2012, 48, 441–446. [Google Scholar] [CrossRef] [Green Version]
- Lambin, P.; Leijenaar, R.T.H.; Deist, T.M.; Peerlings, J.; de Jong, E.; van Timmeren, J.; Sanduleanu, S.; Larue, R.; Even, A.; Jochems, A.; et al. Radiomics: The bridge between medical imaging and personalized medicine. Nat. Rev. Clin. Oncol. 2017, 14, 749–762. [Google Scholar] [CrossRef]
- Kumar, V.; Gu, Y.; Basu, S.; Berglund, A.; Eschrich, S.A.; Schabath, M.B.; Forster, K.; Aerts, H.J.; Dekker, A.; Fenstermacher, D.; et al. Radiomics: The process and the challenges. Magn. Reson. Imaging 2012, 30, 1234–1248. [Google Scholar] [CrossRef] [Green Version]
- Refaee, T.; Wu, G.; Ibrahim, A.; Halilaj, I.; Leijenaar, R.T.; Rogers, W.; Gietema, H.A.; Hendriks, L.E.; Lambin, P.; Woodruff, H.C. The Emerging Role of Radiomics in COPD and Lung Cancer. Respiration 2020, 99, 99–107. [Google Scholar] [CrossRef]
- Liu, Z.; Wang, S.; Dong, D.; Wei, J.; Fang, C.; Zhou, X.; Sun, K.; Li, L.; Li, B.; Wang, M.; et al. The Applications of Radiomics in Precision Diagnosis and Treatment of Oncology: Opportunities and Challenges. Theranostics 2019, 9, 1303–1322. [Google Scholar] [CrossRef]
- Schoolman, H.M.; Bernstein, L.M. Computer use in diagnosis, prognosis, and therapy. Science 1978, 200, 926–931. [Google Scholar] [CrossRef] [Green Version]
- Zerka, F.; Barakat, S.; Walsh, S.; Bogowicz, M.; Leijenaar, R.T.H.; Jochems, A.; Miraglio, B.; Townend, D.; Lambin, P. Systematic Review of Privacy-Preserving Distributed Machine Learning From Federated Databases in Health Care. JCO Clin. Cancer Inform. 2020, 4, 184–200. [Google Scholar] [CrossRef]
- Gillies, R.J.; Kinahan, P.E.; Hricak, H. Radiomics: Images Are More than Pictures, They Are Data. Radiology 2016, 278, 563–577. [Google Scholar] [CrossRef] [Green Version]
- Roelofs, E.; Persoon, L.; Nijsten, S.; Wiessler, W.; Dekker, A.; Lambin, P. Benefits of a clinical data warehouse with data mining tools to collect data for a radiotherapy trial. Radiother. Oncol. 2013, 108, 174–179. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Roelofs, E.; Dekker, A.; Meldolesi, E.; van Stiphout, R.G.; Valentini, V.; Lambin, P. International data-sharing for radiotherapy research: An open-source based infrastructure for multicentric clinical data mining. Radiother. Oncol. 2014, 110, 370–374. [Google Scholar] [CrossRef] [Green Version]
- Miotto, R.; Li, L.; Kidd, B.; Dudley, J.T. Deep Patient: An Unsupervised Representation to Predict the Future of Patients from the Electronic Health Records. Sci. Rep. 2016, 6, 26094. [Google Scholar] [CrossRef]
- Nead, K.T.; Gaskin, G.; Chester, C.; Swisher-McClure, S.; Dudley, J.T.; Leeper, N.J.; Shah, N.H. Androgen Deprivation Therapy and Future Alzheimer’s Disease Risk. J. Clin. Oncol. 2016, 34, 566–571. [Google Scholar] [CrossRef] [Green Version]
- Gatenby, R.A.; Grove, O.; Gillies, R.J. Quantitative Imaging in Cancer Evolution and Ecology. Radiology 2013, 269, 8–14. [Google Scholar] [CrossRef] [Green Version]
- Van Timmeren, J.E.; Cester, D.; Tanadini-Lang, S.; Alkadhi, H.; Baessler, B. Radiomics in medical imaging—“How-to” guide and critical reflection. Insights Imaging 2020, 11, 91. [Google Scholar] [CrossRef]
- Alzubaidi, L.; Zhang, J.; Humaidi, A.J.; Al-Dujaili, A.; Duan, Y.; Al-Shamma, O.; Santamaría, J.; Fadhel, M.A.; Al-Amidie, M.; Farhan, L. Review of deep learning: Concepts, CNN architectures, challenges, applications, future directions. J. Big Data 2021, 8, 53. [Google Scholar] [CrossRef]
- Limkin, E.J.; Sun, R.; Dercle, L.; Zacharaki, E.I.; Robert, C.; Reuzé, S.; Schernberg, A.; Paragios, N.; Deutsch, E.; Ferté, C. Promises and challenges for the implementation of computational medical imaging (radiomics) in oncology. Ann. Oncol. 2017, 28, 1191–1206. [Google Scholar] [CrossRef]
- Vickers, A.J. Prediction Models: Revolutionary in Principle, But Do They Do More Good Than Harm? J. Clin. Oncol. 2011, 29, 2951–2952. [Google Scholar] [CrossRef]
- Foy, J.J.; Al-Hallaq, H.; Grekoski, V.; Tran, T.; Guruvadoo, K.; Iii, S.G.A.; Sensakovic, W.F. Harmonization of radiomic feature variability resulting from differences in CT image acquisition and reconstruction: Assessment in a cadaveric liver. Phys. Med. Biol. 2020, 65, 205008. [Google Scholar] [CrossRef]
- Andrearczyk, V.; Depeursinge, A.; Müller, H. Neural network training for cross-protocol radiomic feature standardization in computed tomography. J. Med. Imaging 2019, 6, 024008. [Google Scholar] [CrossRef]
- Perone, C.S.; Ballester, P.; Barros, R.; Cohen-Adad, J. Unsupervised domain adaptation for medical imaging segmentation with self-ensembling. NeuroImage 2019, 194, 1–11. [Google Scholar] [CrossRef] [Green Version]
- Andrearczyk, V.; Oreiller, V.; Jreige, M.; Vallières, M.; Castelli, J.; ElHalawani, H.; Boughdad, S.; Prior, J.O.; Depeursinge, A. Overview of the HECKTOR Challenge at MICCAI 2020: Automatic Head and Neck Tumor Segmentation in PET/CT. In 3D Head and Neck Tumor Segmentation in PET/CT Challenge; Springer: Cham, Switzerland, 2020; pp. 1–21. [Google Scholar]
- Zhao, B.; Tan, Y.; Tsai, W.Y.; Schwartz, L.H.; Lu, L. Exploring Variability in CT Characterization of Tumors: A Preliminary Phantom Study. Transl. Oncol. 2014, 7, 88–93. [Google Scholar] [CrossRef] [Green Version]
- Caramella, C.; Allorant, A.; Orlhac, F.; Bidault, F.; Asselain, B.; Ammari, S.; Jaranowski, P.; Moussier, A.; Balleyguier, C.; Lassau, N.; et al. Can we trust the calculation of texture indices of CT images? A phantom study. Med. Phys. 2018, 45, 1529–1536. [Google Scholar] [CrossRef] [PubMed]
- Berenguer, R.; Pastor-Juan, M.D.R.; Canales-Vazquez, J.; Castro-García, M.; Villas, M.V.; Legorburo, F.M.; Sabater, S. Radiomics of CT Features May Be Nonreproducible and Redundant: Influence of CT Acquisition Parameters. Radiology 2018, 288, 407–415. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Mackin, D.; Fave, X.; Zhang, L.; Fried, D.; Yang, J.; Taylor, B.; Rodriguez-Rivera, E.; Dodge, C.; Jones, A.K.; Court, L. Measuring Computed Tomography Scanner Variability of Radiomics Features. Investig. Radiol. 2015, 50, 757–765. [Google Scholar] [CrossRef]
- Cameron, A.; Khalvati, F.; Haider, M.A.; Wong, A. MAPS: A Quantitative Radiomics Approach for Prostate Cancer Detection. IEEE Trans. Biomed. Eng. 2016, 63, 1145–1156. [Google Scholar] [CrossRef] [PubMed]
- Parmar, C.; Grossmann, P.; Bussink, J.; Lambin, P.; Aerts, H.J.W.L. Machine Learning methods for Quantitative Radiomic Biomarkers. Sci. Rep. 2015, 5, 13087. [Google Scholar] [CrossRef]
- Wibmer, A.; Hricak, H.; Gondo, T.; Matsumoto, K.; Veeraraghavan, H.; Fehr, D.; Zheng, J.; Goldman, D.; Moskowitz, C.; Fine, S.W.; et al. Haralick texture analysis of prostate MRI: Utility for differentiating non-cancerous prostate from prostate cancer and differentiating prostate cancers with different Gleason scores. Eur. Radiol. 2015, 25, 2840–2850. [Google Scholar] [CrossRef]
- Peng, Y.; Jiang, Y.; Yang, C.; Brown, J.B.; Antic, T.; Sethi, I.; Schmid-Tannwald, C.; Giger, M.; Eggener, S.E.; Oto, A. Quantitative Analysis of Multiparametric Prostate MR Images: Differentiation between Prostate Cancer and Normal Tissue and Correlation with Gleason Score—A Computer-aided Diagnosis Development Study. Radiology 2013, 267, 787–796. [Google Scholar] [CrossRef]
- Cattell, R.; Chen, S.; Huang, C. Robustness of radiomic features in magnetic resonance imaging: Review and a phantom study. Vis. Comput. Ind. Biomed. Art 2019, 2, 1–16. [Google Scholar] [CrossRef] [PubMed]
- Jimenez-Del-Toro, O.; Aberle, C.; Bach, M.; Schaer, R.; Obmann, M.M.; Flouris, K.; Konukoglu, E.; Stieltjes, B.; Müller, H.; Depeursinge, A. The Discriminative Power and Stability of Radiomics Features with Computed Tomography Variations: Task-based analysis in an anthropomorphic 3D-printed CT phantom. Investig. Radiol. 2021. [Google Scholar] [CrossRef] [PubMed]
- Yang, F.; Simpson, G.; Young, L.; Ford, J.; Dogan, N.; Wang, L. Impact of contouring variability on oncological PET radiomics features in the lung. Sci. Rep. 2020, 10, 369. [Google Scholar] [CrossRef]
- Pavic, M.; Bogowicz, M.; Würms, X.; Glatz, S.; Finazzi, T.; Riesterer, O.; Roesch, J.; Rudofsky, L.; Friess, M.; Veit-Haibach, P.; et al. Influence of inter-observer delineation variability on radiomics stability in different tumor sites. Acta Oncol. 2018, 57, 1070–1074. [Google Scholar] [CrossRef] [Green Version]
- Traverso, A.; Kazmierski, M.; Welch, M.L.; Weiss, J.; Fiset, S.; Foltz, W.D.; Gladwish, A.; Dekker, A.; Jaffray, D.; Wee, L.; et al. Sensitivity of radiomic features to inter-observer variability and image pre-processing in Apparent Diffusion Coefficient (ADC) maps of cervix cancer patients. Radiother. Oncol. 2020, 143, 88–94. [Google Scholar] [CrossRef] [Green Version]
- Depeursinge, A.; Yanagawa, M.; Leung, A.N.; Rubin, D.L. Predicting adenocarcinoma recurrence using computational texture models of nodule components in lung CT. Med. Phys. 2015, 42, 2054–2063. [Google Scholar] [CrossRef] [Green Version]
- Granzier, R.W.Y.; Verbakel, N.M.H.; Ibrahim, A.; Van Timmeren, J.E.; Van Nijnatten, T.J.A.; Leijenaar, R.T.H.; Lobbes, M.B.I.; Smidt, M.L.; Woodruff, H.C. MRI-based radiomics in breast cancer: Feature robustness with respect to inter-observer segmentation variability. Sci. Rep. 2020, 10, 14163. [Google Scholar] [CrossRef]
- Zwanenburg, A.; Vallières, M.; Abdalah, M.A.; Aerts, H.J.W.L.; Andrearczyk, V.; Apte, A.; Ashrafinia, S.; Bakas, S.; Beukinga, R.J.; Boellaard, R.; et al. The Image Biomarker Standardization Initiative: Standardized Quantitative Radiomics for High-Throughput Image-based Phenotyping. Radiology 2020, 295, 328–338. [Google Scholar] [CrossRef] [Green Version]
- Da-Ano, R.; Visvikis, D.; Hatt, M. Harmonization strategies for multicenter radiomics investigations. Phys. Med. Biol. 2020, 65, 24TR02. [Google Scholar] [CrossRef]
- Papadimitroulas, P.; Brocki, L.; Chung, N.C.; Marchadour, W.; Vermet, F.; Gaubert, L.; Eleftheriadis, V.; Plachouris, D.; Visvikis, D.; Kagadis, G.C.; et al. Artificial intelligence: Deep learning in oncological radiomics and challenges of interpretability and data harmonization. Phys. Med. 2021, 83, 108–121. [Google Scholar] [CrossRef]
- Mottet, N.; Bellmunt, J.; Bolla, M.; Briers, E.; Cumberbatch, M.G.; De Santis, M.; Fossati, N.; Gross, T.; Henry, A.M.; Joniau, S.; et al. EAU-ESTRO-SIOG Guidelines on Prostate Cancer. Part 1: Screening, Diagnosis, and Local Treatment with Curative Intent. Eur. Urol. 2017, 71, 618–629. [Google Scholar] [CrossRef] [PubMed]
- Cornford, P.; Bellmunt, J.; Bolla, M.; Briers, E.; De Santis, M.; Gross, T.; Henry, A.M.; Joniau, S.; Lam, T.B.; Mason, M.D.; et al. EAU-ESTRO-SIOG Guidelines on Prostate Cancer. Part II: Treatment of Relapsing, Metastatic, and Castration-Resistant Prostate Cancer. Eur. Urol. 2017, 71, 630–642. [Google Scholar] [CrossRef] [PubMed]
- Pötter, R.; Haie-Meder, C.; Van Limbergen, E.; Barillot, I.; De Brabandere, M.; Dimopoulos, J.; Dumas, I.; Erickson, B.; Lang, S.; Nulens, A.; et al. Recommendations from gynaecological (GYN) GEC ESTRO working group (II): Concepts and terms in 3D image-based treatment planning in cervix cancer brachytherapy—3D dose volume parameters and aspects of 3D image-based anatomy, radiation physics, radiobiology. Radiother. Oncol. 2006, 78, 67–77. [Google Scholar] [CrossRef]
- Boellaard, R.; Delgado-Bolton, R.; Oyen, W.J.G.; Giammarile, F.; Tatsch, K.; Eschner, W.; Verzijlbergen, F.J.; Barrington, S.F.; Pike, L.C.; Weber, W.A.; et al. FDG PET/CT: EANM procedure guidelines for tumour imaging: Version 2.0. Eur. J. Nucl. Med. Mol. Imaging 2015, 42, 328–354. [Google Scholar] [CrossRef] [PubMed]
- Pfaehler, E.; Van Sluis, J.; Merema, B.B.; van Ooijen, P.; Berendsen, R.C.; Van Velden, F.H.; Boellaard, R. Experimental Multicenter and Multivendor Evaluation of the Performance of PET Radiomic Features Using 3-Dimensionally Printed Phantom Inserts. J. Nucl. Med. 2020, 61, 469–476. [Google Scholar] [CrossRef]
- Yu, J.B.; Beck, T.F.; Anscher, M.S.; Baschnagel, A.M.; Brock, K.K.; Carlson, D.J.; Dominello, M.M.; Kimple, R.J.; Knisely, J.P.; Mendonca, M.S.; et al. Analysis of the 2017 American Society for Radiation Oncology (ASTRO) Research Portfolio. Int. J. Radiat. Oncol. Biol. Phys. 2019, 103, 297–304. [Google Scholar] [CrossRef]
- Luh, J.Y.; Albuquerque, K.V.; Cheng, C.; Ermoian, R.P.; Nabavizadeh, N.; Parsai, H.; Roeske, J.C.; Weiss, S.E.; Wynn, R.B.; Yu, Y.; et al. ACR–ASTRO Practice Parameter for Image-guided Radiation Therapy (IGRT). Am. J. Clin. Oncol. 2020, 43, 459–468. [Google Scholar] [CrossRef]
- Carré, A.; Klausner, G.; Edjlali, M.; Lerousseau, M.; Briend-Diop, J.; Sun, R.; Ammari, S.; Reuzé, S.; Andres, E.A.; Estienne, T.; et al. Standardization of brain MR images across machines and protocols: Bridging the gap for MRI-based radiomics. Sci. Rep. 2020, 10, 12340. [Google Scholar] [CrossRef]
- Schick, U.; Lucia, F.; Dissaux, G.; Visvikis, D.; Badic, B.; Masson, I.; Pradier, O.; Bourbonne, V.; Hatt, M. MRI-derived radiomics: Methodology and clinical applications in the field of pelvic oncology. Br. J. Radiol. 2019, 92, 20190105. [Google Scholar] [CrossRef]
- Sachs, P.B.; Hunt, K.; Mansoubi, F.; Borgstede, J. CT and MR Protocol Standardization across a Large Health System: Providing a Consistent Radiologist, Patient, and Referring Provider Experience. J. Digit. Imaging 2016, 30, 11–16. [Google Scholar] [CrossRef] [Green Version]
- Center for Drug Evaluation and Research. Clinical Trial Imaging Endpoint Process Standards. 2020. Available online: https://www.fda.gov/regulatory-information/search-fda-guidance-documents/clinical-trial-imaging-endpoint-process-standards-guidance-industry (accessed on 12 April 2021).
- Chung, C.; Kalpathy-Cramer, J.; Knopp, M.V.; Jaffray, D.A. In the Era of Deep Learning, Why Reconstruct an Image at All? J. Am. Coll. Radiol. 2021, 18, 170–173. [Google Scholar] [CrossRef]
- De Man, Q.; Haneda, E.; Claus, B.; Fitzgerald, P.; De Man, B.; Qian, G.; Shan, H.; Min, J.; Sabuncu, M.; Wang, G. A two-dimensional feasibility study of deep learning-based feature detection and characterization directly from CT sinograms. Med. Phys. 2019, 46, e790–e800. [Google Scholar] [CrossRef] [PubMed]
- Gao, Y.; Tan, J.; Liang, Z.; Li, L.; Huo, Y. Improved computer-aided detection of pulmonary nodules via deep learning in the sinogram domain. Vis. Comput. Ind. Biomed. Art 2019, 2, 1–9. [Google Scholar] [CrossRef] [PubMed]
- Lee, H.; Huang, C.; Yune, S.; Tajmir, S.H.; Kim, M.; Do, S. Machine Friendly Machine Learning: Interpretation of Computed Tomography without Image Reconstruction. Sci. Rep. 2019, 9, 15540. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Szegedy, C.; Vanhoucke, V.; Ioffe, S.; Shlens, J.; Wojna, Z. Rethinking the Inception Architecture for Computer Vision. In Proceedings of the IEEE Computer Society Conference on Computer Vision and Pattern Recognition, Las Vegas, NV, USA, 26 June–1 July 2016; pp. 2818–2826. [Google Scholar] [CrossRef] [Green Version]
- Gallardo-Estrella, L.; Lynch, D.A.; Prokop, M.; Stinson, D.; Zach, J.; Judy, P.F.; Van Ginneken, B.; Van Rikxoort, E.M. Normalizing computed tomography data reconstructed with different filter kernels: Effect on emphysema quantification. Eur. Radiol. 2016, 26, 478–486. [Google Scholar] [CrossRef]
- Lambin, P.; Woodruff, H. Method of Performing Radiomics Analysis on Image Data. Application No.: N2028271; Ref: P129643NL01, 21 May 2021. [Google Scholar]
- Ravishankar, S.; Ye, J.C.; Fessler, J.A. Image Reconstruction: From Sparsity to Data-Adaptive Methods and Machine Learning. Proc. IEEE Inst. Electr. Electron. Eng. 2019, 108, 86–109. [Google Scholar] [CrossRef] [Green Version]
- St-Jean, S.; Viergever, M.A.; Leemans, A. Harmonization of diffusion MRI datasets with adaptive dictionary learning. Hum. Brain Mapp. 2020, 41, 4478–4499. [Google Scholar] [CrossRef]
- Dewey, B.E.; Zhao, C.; Reinhold, J.C.; Carass, A.; Fitzgerald, K.C.; Sotirchos, E.S.; Saidha, S.; Oh, J.; Pham, D.L.; Calabresi, P.A.; et al. DeepHarmony: A deep learning approach to contrast harmonization across scanner changes. Magn. Reson. Imaging 2019, 64, 160–170. [Google Scholar] [CrossRef]
- Guha, I.; Nadeem, S.A.; You, C.; Zhang, X.; Levy, S.M.; Wang, G.; Torner, J.C.; Saha, P.K. Deep learning based high-resolution reconstruction of trabecular bone microstructures from low-resolution CT scans using GAN-CIRCLE. Proc. SPIE Int. Soc. Opt. Eng. 2020, 11317, 113170U. [Google Scholar] [CrossRef]
- Zhu, J.-Y.; Park, T.; Isola, P.; Efros, A.A. Unpaired Image-to-Image Translation Using Cycle-Consistent Adversarial Networks. In Proceedings of the 2017 IEEE International Conference on Computer Vision (ICCV), Venice, Italy, 22–29 October 2017. [Google Scholar]
- Zhao, F.; the UNC/UMN Baby Connectome Project Consortium; Wu, Z.; Wang, L.; Lin, W.; Xia, S.; Shen, D.; Li, G. Harmonization of Infant Cortical Thickness Using Surface-to-Surface Cycle-Consistent Adversarial Networks. Med. Image Comput. Comput. Assist. Interv. 2019, 11767, 475–483. [Google Scholar] [CrossRef]
- Kim, T.; Cha, M.; Kim, H.; Lee, J.K.; Kim, J. Learning to Discover Cross-Domain Relations with Generative Adversarial Networks. arXiv 2017, arXiv:1703.05192. [Google Scholar]
- Yi, Z.; Zhang, H.; Tan, P.; Gong, M. Dualgan: Unsupervised dual learning for image-to-image translation. In Proceedings of the IEEE International Conference on Computer Vision, Cambridge, MA, USA, 20–23 June 2017; pp. 2849–2857. [Google Scholar]
- Goodfellow, I. NIPS 2016 Tutorial: Generative Adversarial Networks. arXiv 2016, arXiv:1701.00160. [Google Scholar]
- Goodfellow, I.; Pouget-Abadie, J.; Mirza, M.; Xu, B.; Warde-Farley, D.; Ozair, S.; Courville, A.C.; Bengio, Y. Generative Adversarial Nets Ian. In Mining of Massive Datasets; Cambridge University Press: Cambridge, UK, 2014. [Google Scholar]
- Yan, C.; Lin, J.; Li, H.; Xu, J.; Zhang, T.; Chen, H.; Woodruff, H.C.; Wu, G.; Zhang, S.; Xu, Y.; et al. Cycle-Consistent Generative Adversarial Network: Effect on Radiation Dose Reduction and Image Quality Improvement in Ultralow-Dose CT for Evaluation of Pulmonary Tuberculosis. Korean J. Radiol. 2021, 22, 983–993. [Google Scholar] [CrossRef] [PubMed]
- Moyer, D.; Steeg, G.V.; Tax, C.M.W.; Thompson, P.M. Scanner invariant representations for diffusion MRI harmonization. Magn. Reson. Med. 2020, 84, 2174–2189. [Google Scholar] [CrossRef] [Green Version]
- Mirzaalian, H.; de Pierrefeu, A.; Savadjiev, P.; Pasternak, O.; Bouix, S.; Kubicki, M.; Westin, C.F.; Shenton, M.E.; Rathi, Y. Harmonizing Diffusion MRI Data across Multiple Sites and Scanners. In Lecture Notes in Computer Science; Springer: Berlin/Heidelberg, Germany, 2015; pp. 12–19. [Google Scholar]
- Mirzaalian, H.; Ning, L.; Savadjiev, P.; Pasternak, O.; Bouix, S.; Michailovich, O.; Grant, G.; Marx, C.; Morey, R.; Flashman, L.; et al. Inter-site and inter-scanner diffusion MRI data harmonization. NeuroImage 2016, 135, 311–323. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Tax, C.M.; Grussu, F.; Kaden, E.; Ning, L.; Rudrapatna, U.; Evans, C.J.; St-Jean, S.; Leemans, A.; Koppers, S.; Merhof, D.; et al. Cross-scanner and cross-protocol diffusion MRI data harmonisation: A benchmark database and evaluation of algorithms. NeuroImage 2019, 195, 285–299. [Google Scholar] [CrossRef]
- Goodfellow, I.; Pouget-Abadie, J.; Mirza, M.; Xu, B.; Warde-Farley, D.; Ozair, S.; Courville, A.C.; Bengio, Y. Generative Adversarial Networks. arXiv 2014, arXiv:1406.2661. [Google Scholar] [CrossRef]
- Zhong, J.; Wang, Y.; Li, J.; Xue, X.; Liu, S.; Wang, M.; Gao, X.; Wang, Q.; Yang, J.; Li, X. Inter-site harmonization based on dual generative adversarial networks for diffusion tensor imaging: Application to neonatal white matter development. Biomed. Eng. Online 2020, 19, 1–18. [Google Scholar] [CrossRef] [Green Version]
- Ronneberger, O.; Fischer, P.; Brox, T. U-Net: Convolutional networks for biomedical image segmentation. In Proceedings of the International Conference on Medical Image Computing and Computer-Assisted Intervention, Granada, Spain, 16–20 September 2015; Springer: Berlin/Heidelberg, Germany, 2015; pp. 234–241. [Google Scholar] [CrossRef] [Green Version]
- Modanwal, G.; Vellal, A.; Buda, M.; Mazurowski, M.A. MRI image harmonization using cycle-consistent generative adversarial network. In Medical Imaging 2020: Computer-Aided Diagnosis; International Society for Optics and Photonics: Bellingham, WA, USA, 2020; p. 1131413. [Google Scholar]
- Cackowski, S.; Barbier, E.L.; Dojat, M.; Christen, T. comBat versus cycleGAN for multi-center MR images harmonization. Proc. Mach. Learn. Res. 2021, 1–15, under review. [Google Scholar]
- You, C.; Cong, W.; Vannier, M.W.; Saha, P.K.; Hoffman, E.; Wang, G.; Li, G.; Zhang, Y.; Zhang, X.; Shan, H.; et al. CT Super-Resolution GAN Constrained by the Identical, Residual, and Cycle Learning Ensemble (GAN-CIRCLE). IEEE Trans. Med. Imaging 2020, 39, 188–203. [Google Scholar] [CrossRef] [Green Version]
- Arjovsky, M.; Chintala, S.; Bottou, L. Wasserstein GAN. arXiv 2017, arXiv:1701.07875. [Google Scholar]
- Chen, Y.; Shi, F.; Christodoulou, A.G.; Xie, Y.; Zhou, Z.; Li, D. Efficient and Accurate MRI Super-Resolution Using a Generative Adversarial Network and 3D Multi-level Densely Connected Network. In International Conference on Medical Image Computing and Computer-Assisted Intervention; Metzler, J.B., Ed.; Springer: Cham, Switzerland, 2018; pp. 91–99. [Google Scholar]
- Park, J.; Hwang, D.; Kim, K.Y.; Kang, S.K.; Kim, Y.K.; Lee, J.S. Computed tomography super-resolution using deep convolutional neural network. Phys. Med. Biol. 2018, 63, 145011. [Google Scholar] [CrossRef] [PubMed]
- Yu, H.; Liu, D.; Shi, H.; Wang, Z.; Wang, X.; Cross, B.; Bramler, M.; Huang, T.S. Computed tomography super-resolution using convolutional neural networks. In Proceedings of the 2017 IEEE International Conference on Image Processing (ICIP), Beijing, China, 17–20 September 2017; pp. 3944–3948. [Google Scholar]
- Chaudhari, A.S.; Fang, Z.; Kogan, F.; Wood, J.; Stevens, K.J.; Gibbons, E.K.; Lee, J.H.; Gold, G.E.; Hargreaves, B.A. Super-resolution musculoskeletal MRI using deep learning. Magn. Reson. Med. 2018, 80, 2139–2154. [Google Scholar] [CrossRef] [PubMed]
- Wolterink, J.M.; Leiner, T.; Viergever, M.A.; Isgum, I. Generative Adversarial Networks for Noise Reduction in Low-Dose CT. IEEE Trans. Med. Imaging 2017, 36, 2536–2545. [Google Scholar] [CrossRef]
- Wei, L.; Lin, Y.; Hsu, W. Using a Generative Adversarial Network for CT Normalization and Its Impact on Radiomic Features. In Proceedings of the 2020 IEEE 17th International Symposium on Biomedical Imaging (ISBI), Iowa City, IA, USA, 3–7 April 2020; pp. 844–848. [Google Scholar]
- Miyato, T.; Kataoka, T.; Koyama, M.; Yoshida, Y. Spectral Normalization for Generative Adversarial Networks. arXiv 2018, arXiv:1802.05957. [Google Scholar]
- Castiglioni, I.; Rundo, L.; Codari, M.; Di Leo, G.; Salvatore, C.; Interlenghi, M.; Gallivanone, F.; Cozzi, A.; D’Amico, N.C.; Sardanelli, F. AI applications to medical images: From machine learning to deep learning. Phys. Med. 2021, 83, 9–24. [Google Scholar] [CrossRef] [PubMed]
- Chatterjee, A. Method of Processing Medical Images by an Analysis System for Enabling Radiomics Signature Analysis. Patent No. P127348NL00, 23 October 2020. [Google Scholar]
- Rosin, P.; Collomosse, J. Image and Video-Based Artistic Stylisation; Springer Science & Business Media: Berlin/Heidelberg, Germany, 2012. [Google Scholar]
- Kyprianidis, J.E.; Collomosse, J.; Wang, T.; Isenberg, T. State of the “Art”: A Taxonomy of Artistic Stylization Techniques for Images and Video. IEEE Trans. Vis. Comput. Graph. 2012, 19, 866–885. [Google Scholar] [CrossRef] [Green Version]
- Semmo, A.; Isenberg, T.; Döllner, J. Neural style transfer: A paradigm shift for image-based artistic rendering? In Proceedings of the Symposium on Non-Photorealistic Animation and Rendering, Los Angeles, CA, USA, 29–30 July 2017; Association for Computing Machinery: New York, NY, USA, 2017; pp. 1–13. [Google Scholar]
- Jing, Y.; Yang, Y.; Feng, Z.; Ye, J.; Yu, Y.; Song, M. Neural Style Transfer: A Review. IEEE Trans. Vis. Comput. Graph. 2020, 26, 3365–3385. [Google Scholar] [CrossRef] [Green Version]
- Hertzmann, A. Painterly rendering with curved brush strokes of multiple sizes. In Proceedings of the 25th Annual Conference on Computer Graphics and Interactive Techniques, Orlando, FL, USA, 19–24 July 1998; pp. 453–460. [Google Scholar]
- Kolliopoulos, A. Image Segmentation for Stylized Non-Photorealistic Rendering and Animation. Available online: https://citeseerx.ist.psu.edu/viewdoc/download?doi=10.1.1.113.3711&rep=rep1&type=pdf (accessed on 24 March 2021).
- Gooch, B.; Coombe, G.; Shirley, P. Artistic Vision: Painterly rendering using computer vision techniques. In Proceedings of the 2nd International Symposium on Non-Photorealistic Animation and Rendering, Annecy, France, 3–5 June 2002; Association for Computing Machinery: New York, NY, USA, 2002; p. 83. [Google Scholar]
- Hertzmann, A.; Jacobs, C.E.; Oliver, N.; Curless, B.; Salesin, D.H. Image analogies. In Proceedings of the 28th annual conference on Computer graphics and interactive techniques—SIGGRAPH ’01, Los Angeles, CA, USA, 28 July–1 August 2001; pp. 327–340. [Google Scholar]
- Winnemöller, H.; Olsen, S.C.; Gooch, B. Real-time video abstraction. ACM Trans. Graph. 2006, 25, 1221–1226. [Google Scholar] [CrossRef]
- Gooch, B.; Reinhard, E.; Gooch, A. Human facial illustrations: Creation and psychophysical evaluation. ACM Trans. Graph. 2004, 23, 27–44. [Google Scholar] [CrossRef]
- Gatys, L.A.; Ecker, A.S.; Bethge, M. Image Style Transfer Using Convolutional Neural Networks. In Proceedings of the IEEE Conference on Computer Vision and Pattern Recognition, Las Vegas, NV, USA, 27–30 June 2016; pp. 2414–2423. [Google Scholar]
- Simonyan, K.; Zisserman, A. Very deep convolutional networks for large-scale image recognition. arXiv 2014, arXiv:1409.1556. [Google Scholar]
- Gatys, L.A.; Ecker, A.S.; Bethge, M. Texture synthesis using convolutional neural networks. arXiv 2015, arXiv:1505.07376. [Google Scholar]
- Li, Y.; Wang, N.; Liu, J.; Hou, X. Demystifying Neural Style Transfer. In Proceedings of the Twenty-Sixth International Joint Conference on Artificial Intelligence, Melbourne, Australia, 19–25 August 2017; pp. 2230–2236. [Google Scholar]
- Gretton, A.; Borgwardt, K.M.; Rasch, M.J. A kernel two-sample test. J. Mach. 2012, 13, 723–773. [Google Scholar]
- Xu, Z.; Wilber, M.J.; Fang, C.; Hertzmann, A.; Jin, H. Learning from Multi-domain Artistic Images for Arbitrary Style Transfer. arXiv 2018, arXiv:1805.09987. [Google Scholar]
- Wilber, M.J.; Fang, C.; Jin, H.; Hertzmann, A.; Collomosse, J.; Belongie, S. BAM! The Behance Artistic Media Dataset for Recognition beyond Photography. In Proceedings of the 2017 IEEE International Conference on Computer Vision (ICCV), Venice, Italy, 22–29 October 2017; pp. 1211–1220. [Google Scholar]
- Huang, X.; Belongie, S. Arbitrary Style Transfer in Real-Time with Adaptive Instance Normalization. In Proceedings of the 2017 IEEE International Conference on Computer Vision (ICCV), Venice, Italy, 22–29 October 2017; pp. 1501–1510. [Google Scholar]
- Johnson, J.; Alahi, A.; Fei-Fei, L. Perceptual Losses for Real-Time Style Transfer and Super-Resolution. In Computer Vision—ECCV 2016; Springer: Cham, Switzerland, 2016; pp. 694–711. [Google Scholar] [CrossRef] [Green Version]
- Li, Y.; Fang, C.; Yang, J.; Wang, Z.; Lu, X.; Yang, M. Universal Style Transfer via Feature Transforms. arXiv 2017, arXiv:1705.08086. [Google Scholar]
- Yang, S.; Kim, E.Y.; Ye, J.C. Continuous Conversion of CT Kernel using Switchable CycleGAN with AdaIN. arXiv 2020, arXiv:2011.13150. [Google Scholar]
- Kim, B.; Ye, J.C. Mumford–Shah Loss Functional for Image Segmentation with Deep Learning. IEEE Trans. Image Process. 2020, 29, 1856–1866. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Villani, C. Optimal Transport: Old and New; Springer Science & Business Media: Berlin/Heidelberg, Germany, 2008. [Google Scholar]
- Peyré, G.; Cuturi, M. Computational Optimal Transport: With Applications to Data Science. Found. Trends Mach. Learn. 2019, 11, 355–607. [Google Scholar] [CrossRef]
- Liu, M.; Maiti, P.; Thomopoulos, S.I.; Zhu, A.; Chai, Y.; Kim, H.; Jahanshad, N. Style Transfer Using Generative Adversarial Networks for Multi-Site MRI Harmonization. bioRxiv 2021. [Google Scholar] [CrossRef]
- Armanious, K.; Jiang, C.; Fischer, M.; Küstner, T.; Nikolaou, K.; Gatidis, S.; Yang, B. MedGAN: Medical Image Translation using GANs. arXiv 2018, arXiv:1806.06397. [Google Scholar] [CrossRef]
- Clancy, T.; Milanko, B. Applications of Cyclic Invariant Style Transfers in Medical Imaging. 2019. Available online: https://benmilanko.com/projects/chestgan/style_transfers_in_medical_imaging.pdf (accessed on 24 March 2021).
- Isola, P.; Zhu, J.-Y.; Zhou, T.; Efros, A.A. Image-to-Image Translation with Conditional Adversarial Networks. arXiv 2016, arXiv:1611.07004. [Google Scholar]
- Wang, C.; Xu, C.; Wanga, C.; Tao, D. Perceptual Adversarial Networks for Image-to-Image Transformation. IEEE Trans. Image Process. 2018, 27, 4066–4079. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Fetty, L.; Bylund, M.; Kuess, P.; Heilemann, G.; Nyholm, T.; Georg, D.; Löfstedt, T. Latent space manipulation for high-resolution medical image synthesis via the StyleGAN. Z. Med. Phys. 2020, 30, 305–314. [Google Scholar] [CrossRef] [PubMed]
- Ma, C.; Ji, Z.; Gao, M. Neural Style Transfer Improves 3D Cardiovascular MR Image Segmentation on Inconsistent Data. In International Conference on Medical Image Computing and Computer-Assisted Intervention; Springer: Cham, Switzerland, 2019; pp. 128–136. [Google Scholar]
- Xu, Y.; Li, Y.; Shin, B.-S. Medical image processing with contextual style transfer. Hum. Cent. Comput. Inf. Sci. 2020, 10, 1–16. [Google Scholar] [CrossRef]
- Nishar, H.; Chavanke, N.; Singhal, N. Histopathological Stain Transfer Using Style Transfer Network with Adversarial Loss. In International Conference on Medical Image Computing and Computer-Assisted Intervention; Springer: Cham, Switzerland, 2020; pp. 330–340. [Google Scholar]
- Ganesh, A.; Vasanth, N.R.; George, K. Staining of Histopathology Slides Using Image Style Transfer Algorithm. In Proceedings of the 2018 IEEE Symposium Series on Computational Intelligence (SSCI), Bengaluru, India, 18–21 November 2018; pp. 1254–1260. [Google Scholar]
- Nyíri, T.; Kiss, A. Style Transfer for Dermatological Data Augmentation. In Proceedings of the SAI Intelligent Systems Conference; Springer: Cham, Switzerland, 2020; pp. 915–923. [Google Scholar]
- Yamashita, R.; Long, J.; Banda, S.; Shen, J.; Rubin, D. Learning domain-agnostic visual representation for computational pathology using medically-irrelevant style transfer augmentation. arXiv 2021, arXiv:2102.01678. [Google Scholar]
- Shiri, I.; Rahmim, A.; Ghafarian, P.; Geramifar, P.; Abdollahi, H.; Bitarafan-Rajabi, A. The impact of image reconstruction settings on 18F-FDG PET radiomic features: Multi-scanner phantom and patient studies. Eur. Radiol. 2017, 27, 4498–4509. [Google Scholar] [CrossRef]
- Vuong, D.; Tanadini-Lang, S.; Huellner, M.W.; Veit-Haibach, P.; Unkelbach, J.; Andratschke, N.; Kraft, J.; Guckenberger, M.; Bogowicz, M. Interchangeability of radiomic features between [18F]-FDG PET/CT and [18F]-FDG PET/MR. Med. Phys. 2019, 46, 1677–1685. [Google Scholar] [CrossRef]
- Bailly, C.; Bodet-Milin, C.; Couespel, S.; Necib, H.; Kraeber-Bodéré, F.; Ansquer, C.; Carlier, T. Revisiting the Robustness of PET-Based Textural Features in the Context of Multi-Centric Trials. PLoS ONE 2016, 11, e0159984. [Google Scholar] [CrossRef]
- Pfaehler, E.; Beukinga, R.J.; De Jong, J.R.; Slart, R.H.J.A.; Slump, C.H.; Dierckx, R.A.J.O.; Boellaard, R. Repeatability of 18 F- FDG PET radiomic features: A phantom study to explore sensitivity to image reconstruction settings, noise, and delineation method. Med. Phys. 2019, 46, 665–678. [Google Scholar] [CrossRef] [Green Version]
- Van Timmeren, J.E.; Carvalho, S.; Leijenaar, R.T.H.; Troost, E.G.C.; Van Elmpt, W.; De Ruysscher, D.; Muratet, J.-P.; Denis, F.; Schimek-Jasch, T.; Nestle, U.; et al. Challenges and caveats of a multi-center retrospective radiomics study: An example of early treatment response assessment for NSCLC patients using FDG-PET/CT radiomics. PLoS ONE 2019, 14, e0217536. [Google Scholar] [CrossRef]
- Orlhac, F.; Soussan, M.; Maisonobe, J.-A.; Garcia, C.A.; Vanderlinden, B.; Buvat, I. Tumor Texture Analysis in 18F-FDG PET: Relationships Between Texture Parameters, Histogram Indices, Standardized Uptake Values, Metabolic Volumes, and Total Lesion Glycolysis. J. Nucl. Med. 2014, 55, 414–422. [Google Scholar] [CrossRef] [Green Version]
- Cortes-Rodicio, J.; Sanchez-Merino, G.; Garcia-Fidalgo, M.; Tobalina-Larrea, I. Identification of low variability textural features for heterogeneity quantification of 18F-FDG PET/CT imaging. Rev. Española Med. Nucl. Imagen Mol. 2016, 35, 379–384. [Google Scholar] [CrossRef]
- Nyflot, M.J.; Yang, F.; Byrd, D.; Bowen, S.R.; Sandison, G.A.; Kinahan, P. Quantitative radiomics: Impact of stochastic effects on textural feature analysis implies the need for standards. J. Med. Imaging 2015, 2, 041002. [Google Scholar] [CrossRef] [Green Version]
- Galavis, P.; Hollensen, C.; Jallow, N.; Paliwal, B.; Jeraj, R. Variability of textural features in FDG PET images due to different acquisition modes and reconstruction parameters. Acta Oncol. 2010, 49, 1012–1016. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Van Velden, F.H.P.; Kramer, G.M.; Frings, V.; Nissen, I.A.; Mulder, E.R.; de Langen, A.J.; Hoekstra, O.S.; Smit, E.F.; Boellaard, R. Repeatability of Radiomic Features in Non-Small-Cell Lung Cancer [18F]FDG-PET/CT Studies: Impact of Reconstruction and Delineation. Mol. Imaging Biol. 2016, 18, 788–795. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Leijenaar, R.T.; Nalbantov, G.; Carvalho, S.; Van Elmpt, W.J.; Troost, E.G.; Boellaard, R.; Aerts, H.J.; Gillies, R.J.; Lambin, P. The effect of SUV discretization in quantitative FDG-PET Radiomics: The need for standardized methodology in tumor texture analysis. Sci. Rep. 2015, 5, 11075. [Google Scholar] [CrossRef]
- Shiri, I.; Rahmim, A.; Abdollahi, H.; Ghafarian, P.; Bitarafan, A.; Ay, M. Radiomics texture features variability and reproducibility in advance image reconstruction setting of oncological PET/CT. Eur. J. Nucl. Med. Mol. Imaging 2016, 43, S150. [Google Scholar]
- Yan, J.; Chu-Shern, J.L.; Loi, H.Y.; Khor, L.K.; Sinha, A.K.; Quek, S.T.; Tham, I.W.; Townsend, D.W. Impact of Image Reconstruction Settings on Texture Features in 18F-FDG PET. J. Nucl. Med. 2015, 56, 1667–1673. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Belli, M.L.; Mori, M.; Broggi, S.; Cattaneo, G.M.; Bettinardi, V.; Dell’Oca, I.; Fallanca, F.; Passoni, P.; Vanoli, E.G.; Calandrino, R.; et al. Quantifying the robustness of [18F]FDG-PET/CT radiomic features with respect to tumor delineation in head and neck and pancreatic cancer patients. Phys. Med. 2018, 49, 105–111. [Google Scholar] [CrossRef] [PubMed]
- Desseroit, M.C.; Tixier, F.; Weber, W.A. Reliability of PET/CT shape and heterogeneity features in functional and morpho-logic components of non–small cell lung cancer tumors: A repeatability analysis in a prospective multicentre cohort. J. Nucl. 2017, 58, 406–411. [Google Scholar] [CrossRef]
- Orlhac, F.; Soussan, M.; Chouahnia, K.; Martinod, E.; Buvat, I. 18F-FDG PET-Derived Textural Indices Reflect Tissue-Specific Uptake Pattern in Non-Small Cell Lung Cancer. PLoS ONE 2015, 10, e0145063. [Google Scholar] [CrossRef] [PubMed]
- Ger, R.B.; Meier, J.; Pahlka, R.B.; Gay, S.; Mumme, R.; Fuller, C.D.; Li, H.; Howell, R.M.; Layman, R.R.; Stafford, R.J.; et al. Effects of alterations in positron emission tomography imaging parameters on radiomics features. PLoS ONE 2019, 14, e0221877. [Google Scholar] [CrossRef] [PubMed]
- Leijenaar, R.T.H.; Carvalho, S.; Velazquez, E.R.; Van Elmpt, W.J.C.; Parmar, C.; Hoekstra, O.S.; Hoekstra, C.J.; Boellaard, R.; Dekker, A.; Gillies, R.; et al. Stability of FDG-PET Radiomics features: An integrated analysis of test-retest and inter-observer variability. Acta Oncol. 2013, 52, 1391–1397. [Google Scholar] [CrossRef] [Green Version]
- Prayer, F.; Hofmanninger, J.; Weber, M.; Kifjak, D.; Willenpart, A.; Pan, J.; Röhrich, S.; Langs, G.; Prosch, H. Variability of computed tomography radiomics features of fibrosing interstitial lung disease: A test-retest study. Methods 2021, 188, 98–104. [Google Scholar] [CrossRef] [PubMed]
- Zhovannik, I.; Bussink, J.; Traverso, A.; Shi, Z.; Kalendralis, P.; Wee, L.; Dekker, A.; Fijten, R.; Monshouwer, R. Learning from scanners: Bias reduction and feature correction in radiomics. Clin. Transl. Radiat. Oncol. 2019, 19, 33–38. [Google Scholar] [CrossRef] [Green Version]
- Balagurunathan, Y.; Gu, Y.; Wang, H.; Kumar, V.; Grove, O.; Hawkins, S.; Kim, J.; Goldgof, D.B.; Hall, L.O.; Gatenby, R.A.; et al. Reproducibility and Prognosis of Quantitative Features Extracted from CT Images. Transl. Oncol. 2014, 7, 72–87. [Google Scholar] [CrossRef] [Green Version]
- Al-Kadi, O.S. Assessment of texture measures susceptibility to noise in conventional and contrast enhanced computed tomography lung tumour images. Comput. Med. Imaging Graph. 2010, 34, 494–503. [Google Scholar] [CrossRef] [Green Version]
- Lee, J.; Steinmann, A.; Ding, Y.; Lee, H.; Owens, C.; Wang, J.; Yang, J.; Followill, D.; Ger, R.; MacKin, D.; et al. Radiomics feature robustness as measured using an MRI phantom. Sci. Rep. 2021, 11, 3973. [Google Scholar] [CrossRef]
- Peerlings, J.; Woodruff, H.C.; Winfield, J.M.; Ibrahim, A.; Van Beers, B.E.; Heerschap, A.; Jackson, A.; Wildberger, J.E.; Mottaghy, F.M.; DeSouza, N.M.; et al. Stability of radiomics features in apparent diffusion coefficient maps from a multi-centre test-retest trial. Sci. Rep. 2019, 9, 48. [Google Scholar] [CrossRef] [Green Version]
- Traverso, A.; Wee, L.; Dekker, A.; Gillies, R. Repeatability and Reproducibility of Radiomic Features: A Systematic Review. Int. J. Radiat. Oncol. Biol. Phys. 2018, 102, 1143–1158. [Google Scholar] [CrossRef] [Green Version]
- Su, C.; Jiang, J.; Zhang, S.; Shi, J.; Xu, K.; Shen, N.; Zhang, J.; Li, L.; Zhao, L.; Zhang, J.; et al. Radiomics based on multicontrast MRI can precisely differentiate among glioma subtypes and predict tumour-proliferative behaviour. Eur. Radiol. 2019, 29, 1986–1996. [Google Scholar] [CrossRef]
- Han, Y.; Xie, Z.; Zang, Y.; Zhang, S.; Gu, D.; Zhou, M.; Gevaert, O.; Wei, J.; Li, C.; Chen, H.; et al. Non-invasive genotype prediction of chromosome 1p/19q co-deletion by development and validation of an MRI-based radiomics signature in lower-grade gliomas. J. Neuro-Oncol. 2018, 140, 297–306. [Google Scholar] [CrossRef]
- Liu, Z.; Zhang, X.-Y.; Ying-Shi, S.; Wang, L.; Zhu, H.-T.; Tang, Z.; Wang, S.; Li, X.-T.; Tian, J.; Sun, Y.-S. Radiomics Analysis for Evaluation of Pathological Complete Response to Neoadjuvant Chemoradiotherapy in Locally Advanced Rectal Cancer. Clin. Cancer Res. 2017, 23, 7253–7262. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Horvat, N.; Veeraraghavan, H.; Khan, M.; Blazic, I.; Zheng, J.; Capanu, M.; Sala, E.; Garcia-Aguilar, J.; Gollub, M.J.; Petkovska, I. MR Imaging of Rectal Cancer: Radiomics Analysis to Assess Treatment Response after Neoadjuvant Therapy. Radiology 2018, 287, 833–843. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Nie, K.; Shi, L.; Chen, Q.; Hu, X.; Jabbour, S.K.; Yue, N.; Niu, T.; Sun, X. Rectal Cancer: Assessment of Neoadjuvant Chemoradiation Outcome based on Radiomics of Multiparametric MRI. Clin. Cancer Res. 2016, 22, 5256–5264. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Min, X.; Li, M.; Dong, D.; Feng, Z.; Zhang, P.; Ke, Z.; You, H.; Han, F.; Ma, H.; Tian, J.; et al. Multi-parametric MRI-based radiomics signature for discriminating between clinically significant and insignificant prostate cancer: Cross-validation of a machine learning method. Eur. J. Radiol. 2019, 115, 16–21. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Viswanath, S.E.; Chirra, P.V.; Yim, M.; Rofsky, N.M.; Purysko, A.S.; Rosen, M.A.; Bloch, B.N.; Madabhushi, A. Comparing radiomic classifiers and classifier ensembles for detection of peripheral zone prostate tumors on T2-weighted MRI: A multi-site study. BMC Med. Imaging 2019, 19, 1–12. [Google Scholar] [CrossRef]
- Rai, R.; Holloway, L.C.; Brink, C.; Field, M.; Christiansen, R.L.; Sun, Y.; Barton, M.B.; Liney, G.P. Multicenter evaluation of MRI-based radiomic features: A phantom study. Med. Phys. 2020, 47, 3054–3063. [Google Scholar] [CrossRef]
- Chatterjee, A.; Vallieres, M.; Dohan, A.; Levesque, I.R.; Ueno, Y.; Saif, S.; Reinhold, C.; Seuntjens, J. Creating Robust Predictive Radiomic Models for Data From Independent Institutions Using Normalization. IEEE Trans. Radiat. Plasma Med. Sci. 2019, 3, 210–215. [Google Scholar] [CrossRef]
- Haga, A.; Takahashi, W.; Aoki, S.; Nawa, K.; Yamashita, H.; Abe, O.; Nakagawa, K. Standardization of imaging features for radiomics analysis. J. Med. Investig. 2019, 66, 35–37. [Google Scholar] [CrossRef]
- Crombé, A.; Kind, M.; Fadli, D.; Le Loarer, F.; Italiano, A.; Buy, X.; Saut, O. Intensity harmonization techniques influence radiomics features and radiomics-based predictions in sarcoma patients. Sci. Rep. 2020, 10, 15496. [Google Scholar] [CrossRef] [PubMed]
- Nyúl, L.G.; Udupa, J.K. On standardizing the MR image intensity scale. Magn. Reson. Med. 1999, 42, 1072–1081. [Google Scholar] [CrossRef]
- Nyul, L.; Udupa, J.; Zhang, X. New variants of a method of MRI scale standardization. IEEE Trans. Med. Imaging 2000, 19, 143–150. [Google Scholar] [CrossRef] [PubMed]
- Wang, L.; Lai, H.-M.; Barker, G.; Miller, D.H.; Tofts, P. Correction for variations in MRI scanner sensitivity in brain studies with histogram matching. Magn. Reson. Med. 1998, 39, 322–327. [Google Scholar] [CrossRef] [PubMed]
- Masson, I.; Da-Ano, R.; Lucia, F.; Doré, M.; Castelli, J.; de Monsabert, C.G.; Ramée, J.; Sellami, S.; Visvikis, D.; Hatt, M.; et al. Statistical harmonization can improve the development of a multicenter CT-based radiomic model predictive of nonresponse to induction chemotherapy in laryngeal cancers. Med. Phys. 2021, 48, 4099–4109. [Google Scholar] [CrossRef]
- Lucia, F.; Visvikis, D.; Vallières, M.; Desseroit, M.-C.; Miranda, O.; Robin, P.; Bonaffini, P.A.; Alfieri, J.; Masson, I.; Mervoyer, A.; et al. External validation of a combined PET and MRI radiomics model for prediction of recurrence in cervical cancer patients treated with chemoradiotherapy. Eur. J. Nucl. Med. Mol. Imaging 2019, 46, 864–877. [Google Scholar] [CrossRef] [PubMed]
- Johnson, W.; Li, C.; Rabinovic, A. Adjusting batch effects in microarray expression data using empirical Bayes methods. Biostatistics 2006, 8, 118–127. [Google Scholar] [CrossRef]
- Fortin, J.-P.; Parker, D.; Tunç, B.; Watanabe, T.; Elliott, M.A.; Ruparel, K.; Roalf, D.R.; Satterthwaite, T.D.; Gur, R.C.; Gur, R.E.; et al. Harmonization of multi-site diffusion tensor imaging data. NeuroImage 2017, 161, 149–170. [Google Scholar] [CrossRef]
- Orlhac, F.; Frouin, F.; Nioche, C.; Ayache, N.; Buvat, I. Validation of a Method to Compensate Multicenter Effects Affecting CT Radiomics. Radiology 2019, 291, 53–59. [Google Scholar] [CrossRef] [Green Version]
- Orlhac, F.; Boughdad, S.; Philippe, C.; Stalla-Bourdillon, H.; Nioche, C.; Champion, L.; Soussan, M.; Frouin, F.; Frouin, V.; Buvat, I. A Postreconstruction Harmonization Method for Multicenter Radiomic Studies in PET. J. Nucl. Med. 2018, 59, 1321–1328. [Google Scholar] [CrossRef]
- Da-Ano, R.; Masson, I.; Lucia, F.; Doré, M.; Robin, P.; Alfieri, J.; Rousseau, C.; Mervoyer, A.; Reinhold, C.; Castelli, J.; et al. Performance comparison of modified ComBat for harmonization of radiomic features for multicenter studies. Sci. Rep. 2020, 10, 10248. [Google Scholar] [CrossRef] [PubMed]
- Vetter, T.R.; Schober, P. Agreement Analysis: What He Said, She Said Versus You Said. Anesth. Analg. 2018, 126, 2123–2128. [Google Scholar] [CrossRef]
- Ibrahim, A.; Primakov, S.; Beuque, M.; Woodruff, H.; Halilaj, I.; Wu, G.; Refaee, T.; Granzier, R.; Widaatalla, Y.; Hustinx, R.; et al. Radiomics for precision medicine: Current challenges, future prospects, and the proposal of a new framework. Methods 2021, 188, 20–29. [Google Scholar] [CrossRef] [PubMed]
- Lin, L.I.-K. A Concordance Correlation Coefficient to Evaluate Reproducibility. Biometrics 1989, 45, 255–268. [Google Scholar] [CrossRef]
- Mackin, D.; Fave, X.; Zhang, L.; Fried, D.; Yang, J.; Taylor, B.; Rodriguez-Rivera, E.; Dodge, C.; Jones, A.K.; Court, L. Data from credence cartridge radiomics phantom CT scans. Cancer Imaging Arch. 2017, 10, K9. [Google Scholar]
- Ibrahim, A.; Refaee, T.; Leijenaar, R.T.H.; Primakov, S.; Hustinx, R.; Mottaghy, F.M.; Woodruff, H.C.; Maidment, A.D.A.; Lambin, P. The application of a workflow integrating the variable reproducibility and harmonizability of radiomic features on a phantom dataset. PLoS ONE 2021, 16, e0251147. [Google Scholar] [CrossRef] [PubMed]
- Ibrahim, A.; Refaee, T.; Primakov, S.; Barufaldi, B.; Acciavatti, R.; Granzier, R.; Hustinx, R.; Mottaghy, F.; Woodruff, H.; Wildberger, J.; et al. The effects of in-plane spatial resolution on CT-based radiomic features’ stabil-ity with and without ComBat harmonization. Cancers 2021, 13, 1848. [Google Scholar] [CrossRef]
- Ibrahim, A.; Refaee, T.; Primakov, S.; Barufaldi, B.; Acciavatti, R.J.; Granzier, R.W.Y.; Hustinx, R.; Mottaghy, F.M.; Woodruff, H.C.; Wildberger, J.E.; et al. Reply to Orlhac, F.; Buvat, I. Comment on “Ibrahim et al. The Effects of In-Plane Spatial Resolution on CT-Based Radiomic Features’ Stability with and without ComBat Harmonization. Cancers 2021, 13, 1848”. Cancers 2021, 13, 3080. [Google Scholar] [CrossRef]
- Mackin, D.; Fave, X.; Zhang, L.; Yang, J.; Jones, A.K.; Ng, C.S.; Court, L. Harmonizing the pixel size in retrospective computed tomography radiomics studies. PLoS ONE 2017, 12, e0178524. [Google Scholar] [CrossRef] [Green Version]
- Rozantsev, A.; Salzmann, M.; Fua, P. Beyond Sharing Weights for Deep Domain Adaptation. IEEE Trans. Pattern Anal. Mach. Intell. 2019, 41, 801–814. [Google Scholar] [CrossRef] [Green Version]
- Sun, B.; Saenko, K. Deep CORAL: Correlation Alignment for Deep Domain Adaptation. In Computer Vision—ECCV 2016 Workshops; Springer International Publishing: Cham, Switzerland, 2016; pp. 443–450. [Google Scholar]
- Sun, B.; Feng, J.; Saenko, K. Return of Frustratingly Easy Domain Adaptation. In Proceedings of the AAAI Conference on Artificial Intelligence, Phoenix, AZ, USA, 12–17 February 2016. [Google Scholar]
- Saenko, K.; Kulis, B.; Fritz, M.; Darrell, T. Adapting Visual Category Models to New Domains. In Computer Vision—ECCV 2010; Springer: Berlin/Heidelberg, Germany, 2010; pp. 213–226. [Google Scholar]
- Ganin, Y.; Ustinova, E.; Ajakan, H.; Germain, P.; Larochelle, H.; Laviolette, F.; Marchand, M.; Lempitsky, V. Domain-Adversarial Training of Neural Networks. In Domain Adaptation in Computer Vision Applications; Springer: Cham, Switzerland, 2017; pp. 189–209. [Google Scholar]
- Tzeng, E.; Hoffman, J.; Darrell, T.; Saenko, K. Simultaneous Deep Transfer across Domains and Tasks. In Proceedings of the 2015 IEEE International Conference on Computer Vision (ICCV), Istanbul, Turkey, 2–5 August 2015. [Google Scholar]
- Dinsdale, N.K.; Jenkinson, M.; Namburete, A.I. Deep learning-based unlearning of dataset bias for MRI harmonisation and confound removal. NeuroImage 2021, 228, 117689. [Google Scholar] [CrossRef] [PubMed]
- Welch, M.L.; McIntosh, C.; Haibe-Kains, B.; Milosevic, M.; Wee, L.; Dekker, A.; Huang, S.H.; Purdie, T.; O’Sullivan, B.; Aerts, H.J.; et al. Vulnerabilities of radiomic signature development: The need for safeguards. Radiother. Oncol. 2019, 130, 2–9. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Rizzo, S.; Botta, F.; Raimondi, S.; Origgi, D.; Fanciullo, C.; Morganti, A.G.; Bellomi, M. Radiomics: The facts and the challenges of image analysis. Eur. Radiol. Exp. 2018, 2, 36. [Google Scholar] [CrossRef] [PubMed]
| Standardization of Image Acquisition and Reconstruction Parameters across Various Centers Related to Clinical Trials | |||
|---|---|---|---|
| Reference | Data | Variation Across | Summary |
| Mottet et al. [42] Cornford et al. [43] (ESTRO) | CT and MRI images (prostate cancer) | NA | Provided guidelines procedures and methods for image-guided radiation therapy (IGRT) in prostate cancer |
| Boellaard et al. [45] (EARL) | PET imaging | Scan acquisition, image processing, image interpretation | Provides guideline/regulations for oncology |
| Luh et al. [48] (ASTRO) | NA | NA | Developed a ‘practice parameter’ for IGRT, and provided quality assurance standards, personnel qualifications, indications and guided documentation for imaging |
| Sachs et al. [51] | CT and MRI images | CT and MRI protocols | Reduced the number of MRI protocols from 168 to 66 and CT protocols from 248 to 97 across scanners and centers by selecting an appropriate clinical-driven protocol and standardization process |
| Center for Drug Evaluation and Research (FDA) [52] | NA | Image acquisition parameters | Provided guidelines to focus on image acquisition in clinical trials conducted to support authorization of drugs and biological products |
| Post-Processing of Raw Image Data | |||
|---|---|---|---|
| Reference | Data | Variation Across | Summary |
| Lee et al. [56] | Raw sinogram CT data (head and whole-body) | Acquisition parameters in terms of projections and detector like sinograms | Investigated the performance of a CNN for classifying raw CT data in sinogram-space to identify body region and detect intracranial hemorrhage |
| Gallardo-Estrella et al. [58] | Reconstructed CT images (emphysema in lungs) | Reconstruction kernels | Proposed a method to reduce variability due to different reconstruction kernels in CT images by decomposing each CT scan into a set of frequency bands and the energy in each frequency band is scaled to a reference value iteratively. |
| Data Augmentation Using GANs | |||
|---|---|---|---|
| Reference | Data | Variation Across | Summary |
| Zhong et al. [76] | MRI images (neonatal brains) | Scanners, acquisition protocols | Utilized a dual GAN, with U-Net as the backbone to harmonize the diffusion tensor imaging (DTI) derived metrics on neonatal brains |
| Modanwal et al. [78] | MRI images (breast) | Scanners | Utilized a cycleGAN to perform intensity harmonization on MRI breast images obtained from two different scanners |
| Cackowski et al. [79] | MRI images (brain) | Scanners, acquisition protocols | Conducted a comparative study was conducted by Cackowski et al. [79] between ComBat and cycleGAN to harmonize multi-centric MRI images |
| Guha et al. [63] | CT images (trabecular bone (Tb) microstructures) | Scanners | Conducted a study that transforms low-resolution (LR) CT scans of trabecular (Tb) bone microstructures into high-resolution (HR) CT scans, obtained from two scanners (LR from Siemens FLASH and HR from Siemens FORCE; paired images), using GAN-CIRCLE [80] |
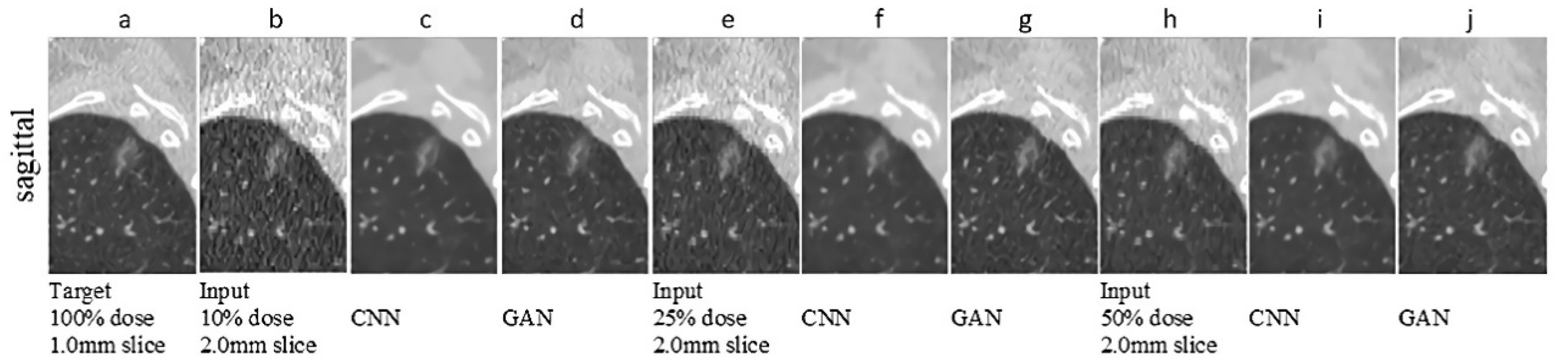
| Wei et al. [87] | CT images (chest) | Dosage, slices thickness | Utilized a 3D GAN to normalize CT images to classify and detect pulmonary nodules |
| Style Transfer | |||
|---|---|---|---|
| Reference | Data | Variation Across | Summary |
| Gatys et al. [101] | Non-medical images (mostly artistic images) | NA | Utilized a CNN to perform neural style transfer using Gram matrix |
| Li et al. [104] | Non-medical images (mostly artistic images) | NA | Treated neural style transfer as a domain adaptation problem and proved that matching Gram matrices of filter responses is equivalent to minimizing MMD [105] |
| Xu et al. [106] | Non-medical images (mostly artistic images) | NA | Combined the concepts of original neural style transfer with the concept of adversarial training for arbitrary style transfer from multi-domain images |
| Yang et al. [111] | CT images (head, facial bone) | Reconstruction kernels | Investigated the effects of different kernels on CT images and proposed an unsupervised image style transfer method by utilizing a cycleGAN with AdaIN [108] that works on unpaired images |
| Liu et al. [115] | MRI images (chest) | Multi-center datasets, image acquisition parameters | Harmonized MRI images from multiple arbitrary sites using a style transferable GAN entailing cycle consistency, style and adversarial losses. |
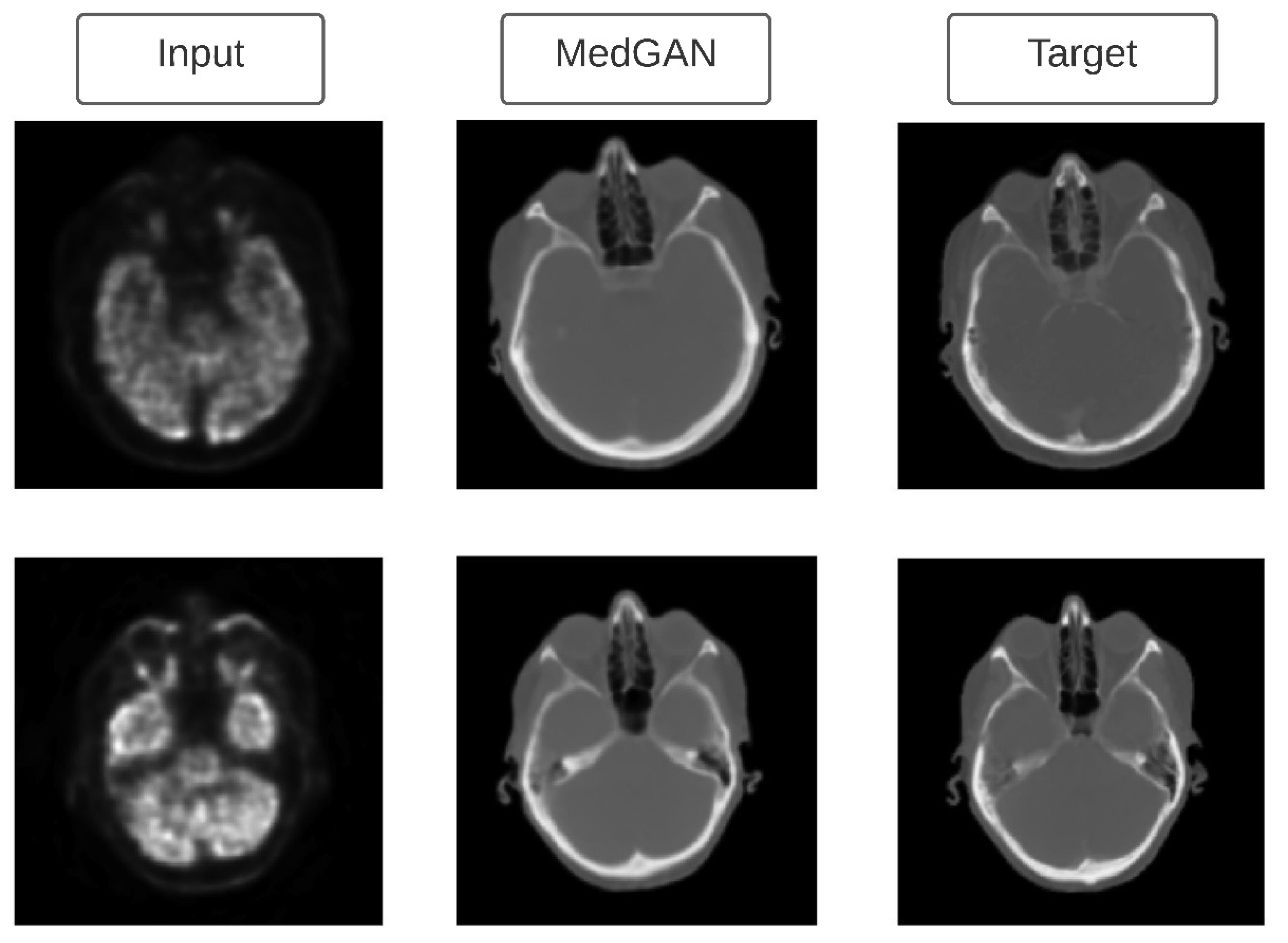
| Armanious et al. [116] | PET, CT images (brain) | Multi-modal dataset | Developed MedGAN architecture which consists of a cascade of UNet blocks to obtain sharper translated images (CasNet) along with Gatys et al.’s [101] style transfer losses. |
| Clancy and Milanko [117] | X-rays (chest) | Healthy and unhealthy patients | Utilized the cycleGAN with adversarial losses to perform style transfer. |
| Fetty et al. [120] | MRI, CT images (pelvic malignancies) | Multi-model dataset | Used StyleGAN with baseline GAN architecture and AdaIN method for transferring style across images. |
| Focusing on Reproducible Features (Identification of Reproducible Features) | |||
|---|---|---|---|
| Reference | Data | Variation Across | Summary |
| Shiri et al. [127] | PET/CT phantom | Image reconstruction settings, scanners | Reproducibility and variability of radiomic features were evaluated using the coefficient of variation (COV) |
| Bailly et al. [129] | PET scans (gastro-entero-pancreatic neuroendocrine tumors) | Multi-centric trials (acquisition and reconstruction parameters) | Analyzed the reproducibility of textural features in PET scans across different acquisition and reconstruction parameters in the context of multi-center trials |
| Prayer et al. [145] | CT scans (fibrosing interstitial lung disease (fILD)) | Scanners, test-retest study | Investigated the inter-and intra-scanner repeatability and reproducibility of computed tomography (CT) radiomic features (radiomic feature) of fILD |
| Lee et al. [149] | MRI scans (phantom, brain lesions) | Scanners, scanning protocol | Investigated the reproducibility of MRI radiomic features across different MRI scanners and scanning protocol parameters |
| Peerlings et al. [150] | MRI scans (ovarian cancer, colorectal liver metastasis) | Vendors, field strengths | Extracted stable parametric MRI radiomic features with a minimum concordance correlation coefficient of 0.85 between data derived from 61 patients’ test and retest apparent diffusion coefficient maps |
| Statistical Normalization | |||
|---|---|---|---|
| Reference | Data | Variation Across | Summary |
| Chatterjee et al. [160] | MRI images (endometrial cancer) | Multi-center datasets | Investigated the effect of applying rescaling and standardization as normalization transformations in MRI images obtained from two different institutes. These transformations were applied separately on balanced training and testing sets rather than applying normalization for the entire dataset |
| Haga et al. [161] | CT images (non-small cell lung cancer (NSCLC)) | Multi-centric datasets | Used z-score normalization to standardize the radiomic features extracted from CT images of NSCLC patients from The University of Tokyo Hospital and TCIA (the Cancer Imaging Archive) |
| Intensity Harmonization Techniques | |||
|---|---|---|---|
| Reference | Data | Variation Across | Summary |
| Crombé et al. [162] | MRI images (sarcoma) | Multi-centric datasets | Performed IHT (standard normalization, z-score normalization, standardization per signal intensities of healthy tissue, histogram matching and ComBat harmonization) as a post-processing method on T2-weighted MRI images of sarcoma patients to enhance the MFS (metastatic-relapse-free survival) predictive models |
| Masson et al. [166] | Contrast enhanced CT images | Multicenteric dataset | Applied histogram equalization (enhancing the contrast by flattening the histogram) on images to normalize intensity scales to pre-process images prior to applying ComBat harmonization method on top of it. |
| ComBat Method and Its Derivatives | |||
|---|---|---|---|
| Reference | Data | Variation Across | Summary |
| Fortin et al. [169] | DTI data | Acquisition and reconstruction parameters | Used ComBat to harmonize cortical thickness measurements calculated on DTI data to remove variations in feature values attributed to differences in acquisition and reconstruction parameters. |
| Orlhac et al. [170] | CT scans(phantom [180], lung cancer) | Multi-centric dataset | Investigated the potential of ComBat to correct for the variations of CT radiomic features extracted from scans collected from different centers. |
| Orlhac et al. [171] | PET scans | Acquisition parameters | Investigated the potential of ComBat to harmonize radiomic features extracted from PET scans acquired differently |
| Ibrahim et al. [174] | Phantom CT [176] | Acquisition and reconstruction parameters | Proposed a framework that guides the use of ComBat in radiomics analyses to assess the performance of ComBat |
| Ibrahim et al. [177] | Phantom CT [176] | Imaging protocols, vendors | Investigated the reproducibility of radiomic features in a pairwise manner and performed ComBat harmonization on it. |
| Ibrahim et al. [178,179] | Phantom CT | In-plane resolution | Performed pairwise comparisons between the scans and reported that radiomic features are affected differently by the degree of variation within a single reconstruction parameter (in-plane resolution). |
| Normalization Using Deep Learning | |||
|---|---|---|---|
| Reference | Data | Variation Across | Summary |
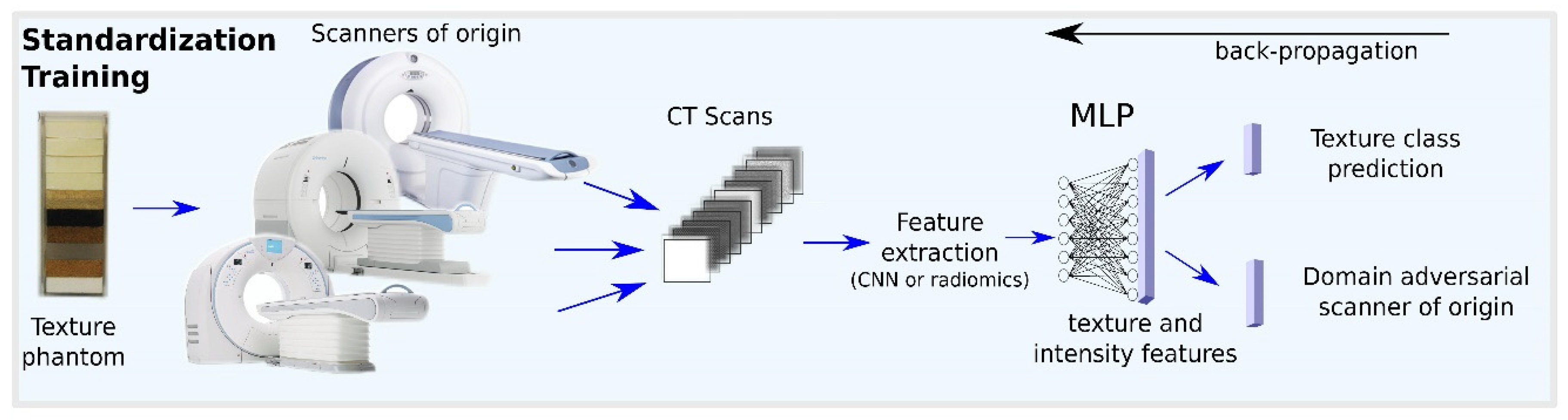
| Andrearczyk et al. [21] | Phantom CT [27] | Acquisition and reconstruction parameters | Proposed a DL-based technique trained on phantom data to normalize various types of features including hand-crafted and deep features using a simple neural network to learn a non-linear normalization transformation |
| Rozantsev et al. [181] | Non-medical images | Synthetic, real image domains | Adapted divergence-based approaches for domain adaptation by using a two-stream CNN architecture (one in the source domain with synthetic images and the other in the target domain with real images) with unshared weights |
| Sun and Saenko [182] | Non-medical images | Different image domain in Office dataset [184] | Adapted divergence-based approaches for domain adaptation by using DeepCORAL [183] architecture |
| Dinsdale et al. [187] | MRI images (neuro) | Multi-centric dataset | Adapted the framework as in [186] and utilized an iterative update approach that aimed to generate scanner-invariant (i.e., harmonized features) representations of MRI neuroimages while evaluating the main task (segmentation). |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Mali, S.A.; Ibrahim, A.; Woodruff, H.C.; Andrearczyk, V.; Müller, H.; Primakov, S.; Salahuddin, Z.; Chatterjee, A.; Lambin, P. Making Radiomics More Reproducible across Scanner and Imaging Protocol Variations: A Review of Harmonization Methods. J. Pers. Med. 2021, 11, 842. https://doi.org/10.3390/jpm11090842
Mali SA, Ibrahim A, Woodruff HC, Andrearczyk V, Müller H, Primakov S, Salahuddin Z, Chatterjee A, Lambin P. Making Radiomics More Reproducible across Scanner and Imaging Protocol Variations: A Review of Harmonization Methods. Journal of Personalized Medicine. 2021; 11(9):842. https://doi.org/10.3390/jpm11090842
Chicago/Turabian StyleMali, Shruti Atul, Abdalla Ibrahim, Henry C. Woodruff, Vincent Andrearczyk, Henning Müller, Sergey Primakov, Zohaib Salahuddin, Avishek Chatterjee, and Philippe Lambin. 2021. "Making Radiomics More Reproducible across Scanner and Imaging Protocol Variations: A Review of Harmonization Methods" Journal of Personalized Medicine 11, no. 9: 842. https://doi.org/10.3390/jpm11090842
APA StyleMali, S. A., Ibrahim, A., Woodruff, H. C., Andrearczyk, V., Müller, H., Primakov, S., Salahuddin, Z., Chatterjee, A., & Lambin, P. (2021). Making Radiomics More Reproducible across Scanner and Imaging Protocol Variations: A Review of Harmonization Methods. Journal of Personalized Medicine, 11(9), 842. https://doi.org/10.3390/jpm11090842








