Diagnostic Performance of Different Simulated Low-Dose Levels in Patients with Suspected Cervical Abscess Using a Third-Generation Dual-Source CT Scanner
Abstract
1. Introduction
2. Materials and Methods
2.1. Imaging Protocol
2.2. Low-Dose Simulation
2.3. Radiation Dose
2.4. Subjective Image Analysis
2.5. Objective Image Analysis
2.6. Reference Standard
2.7. Statistics
3. Results
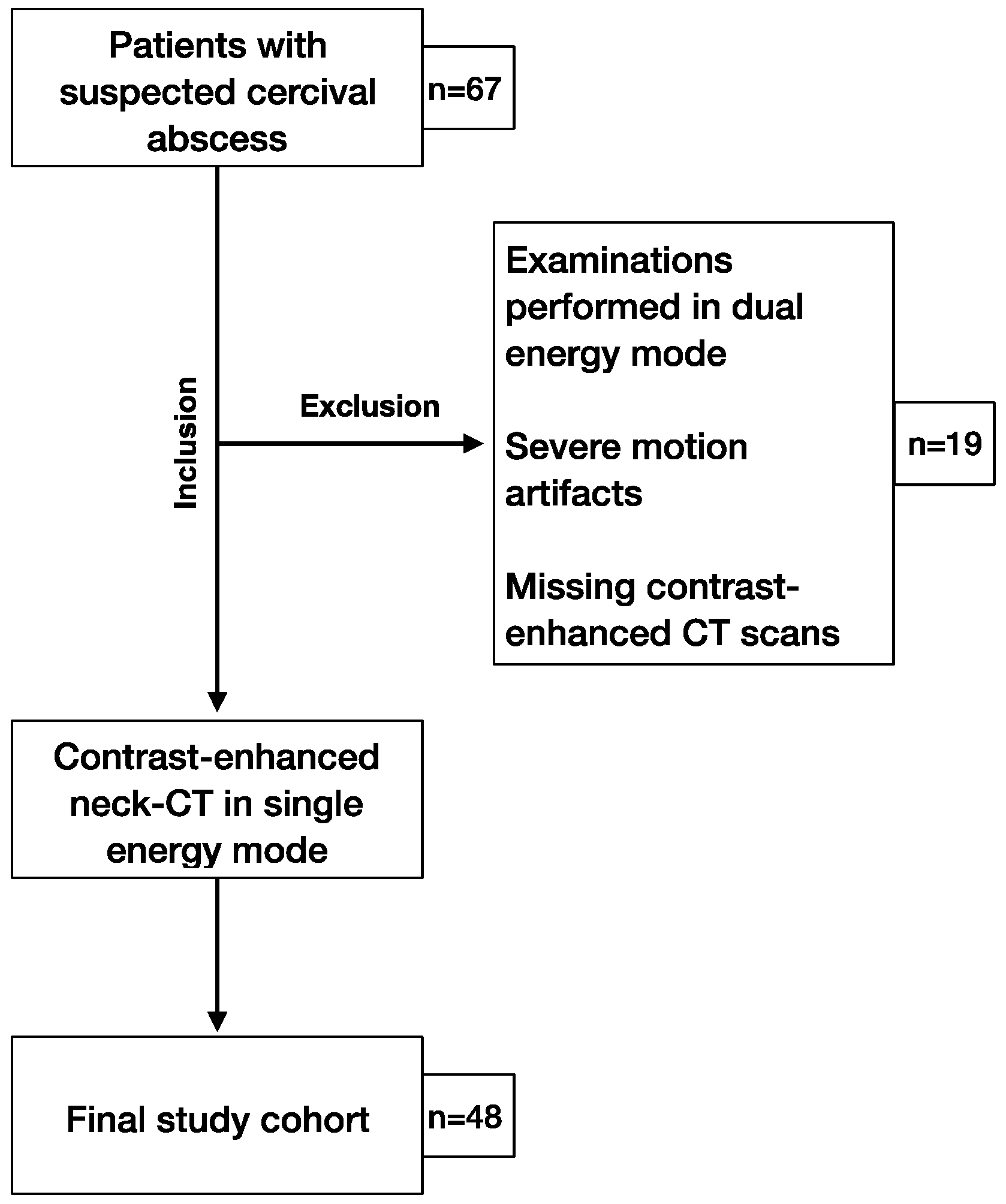
3.1. General Results
3.2. Radiation Dose
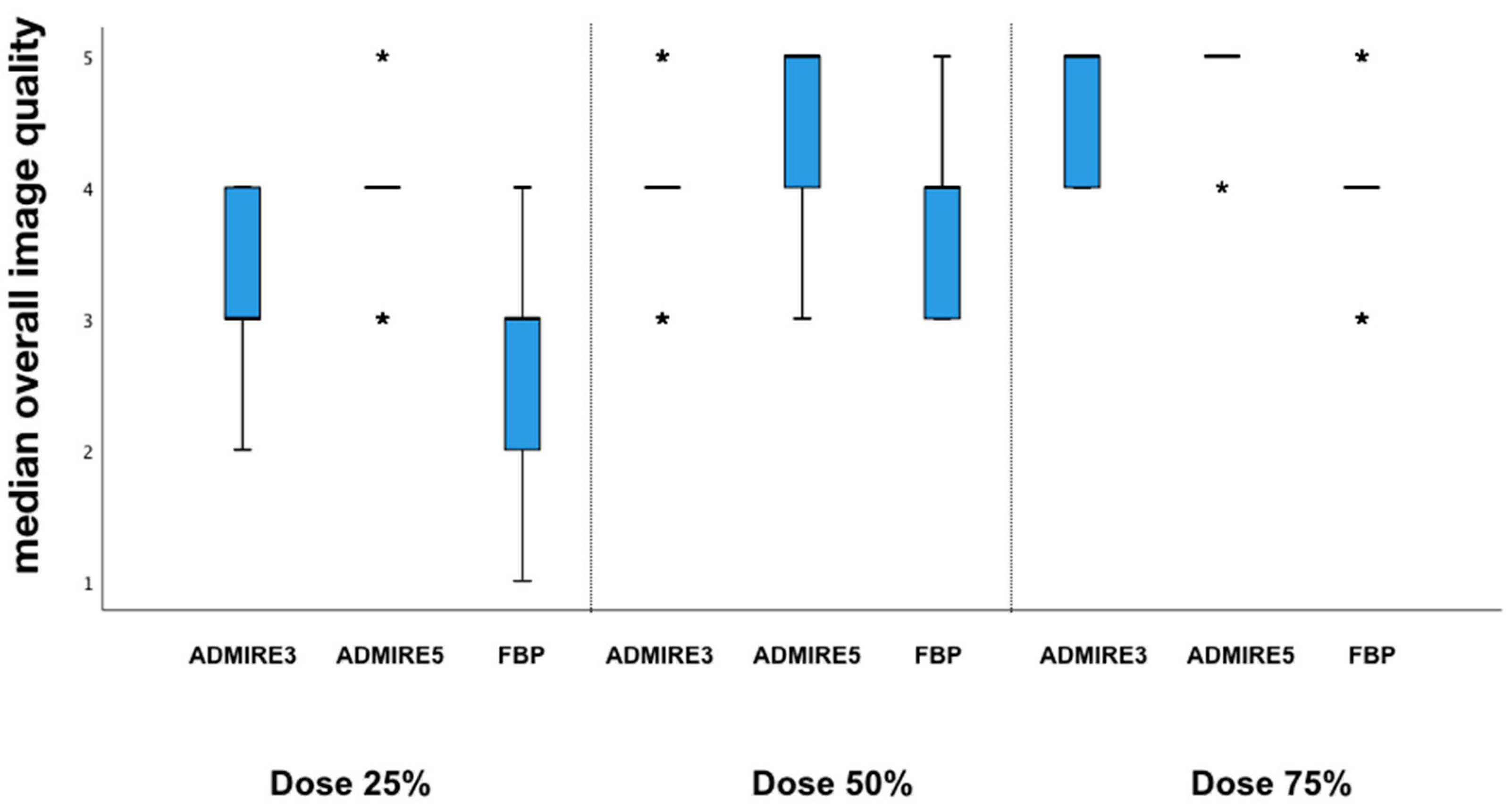
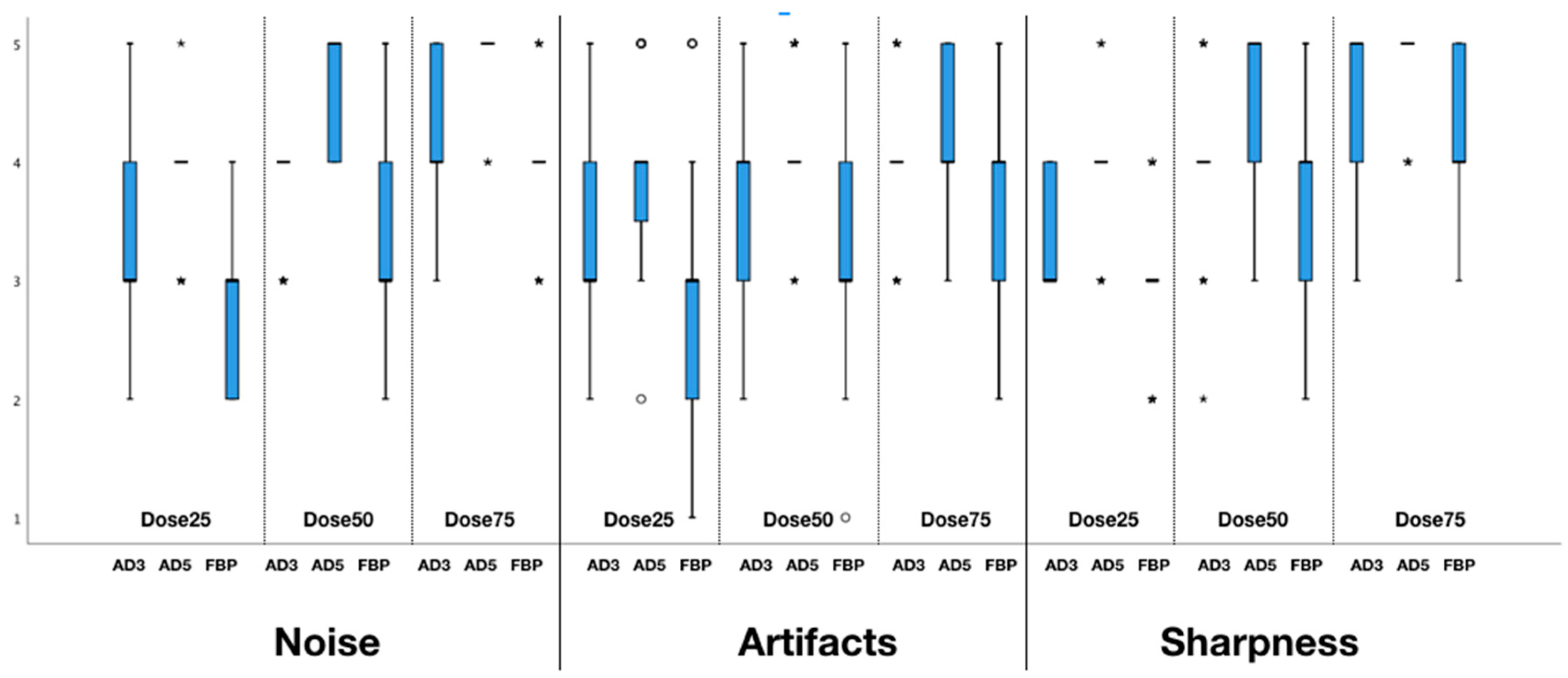
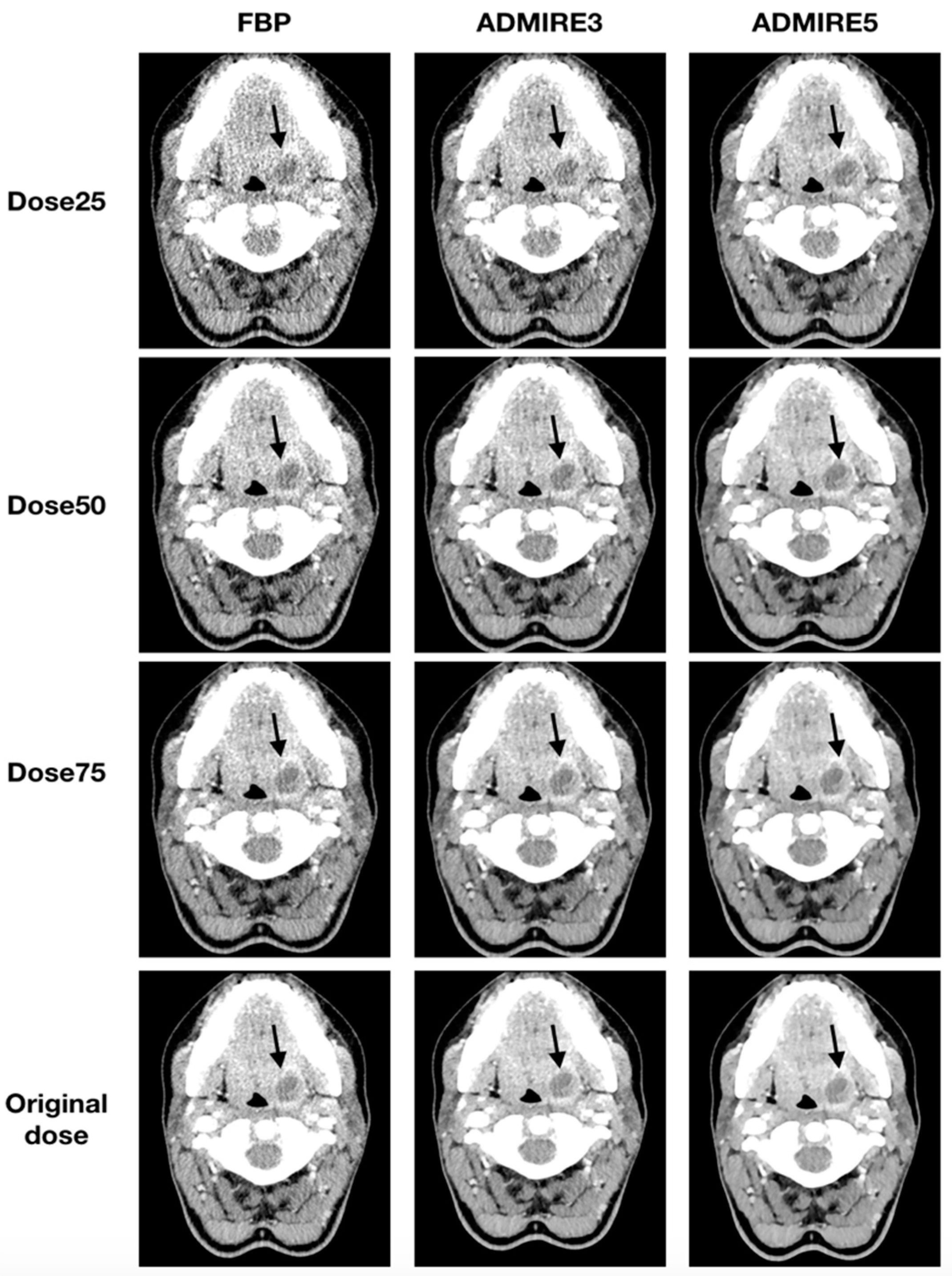
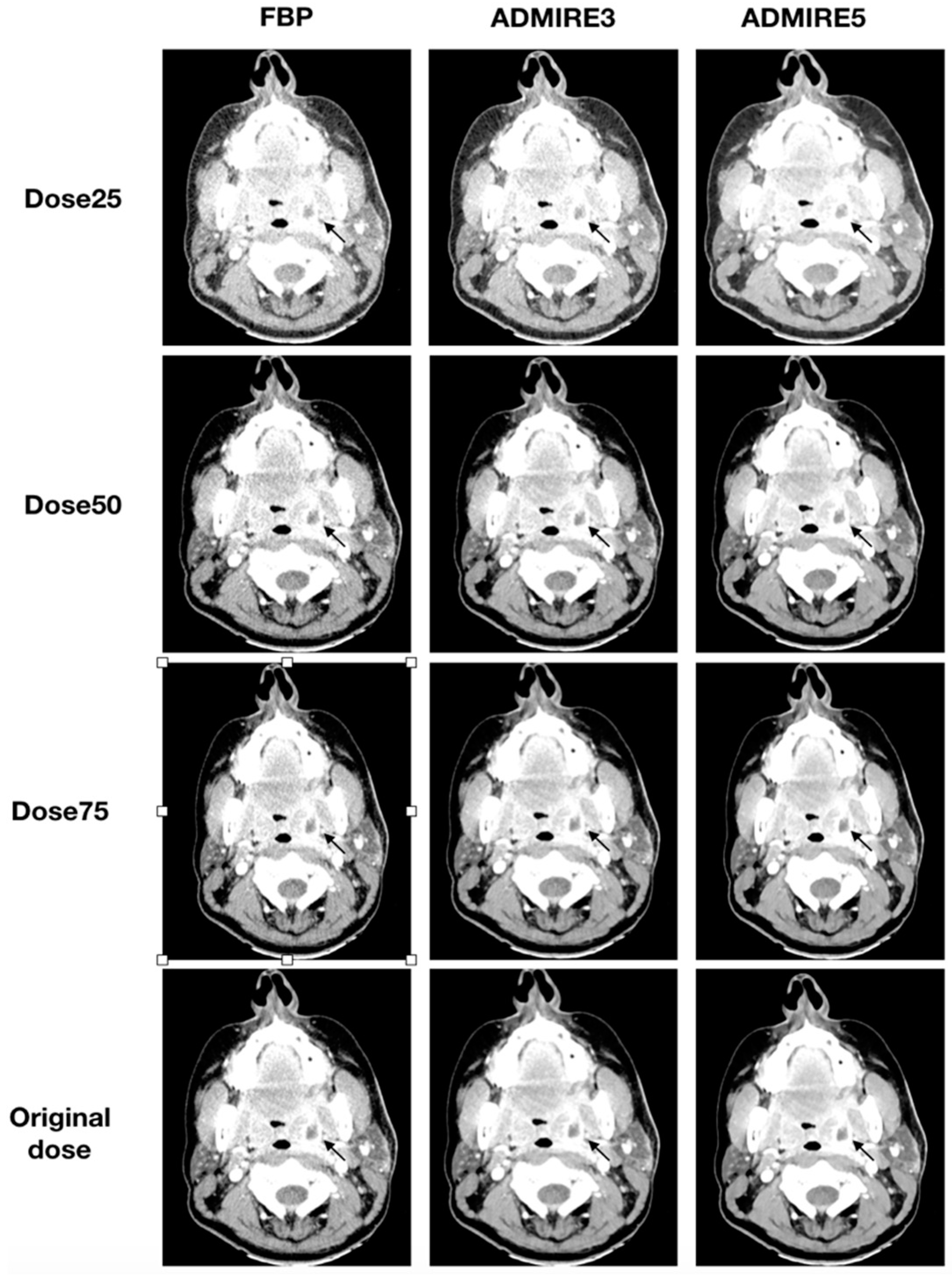
3.3. Subjective Image Analysis
3.4. Objective Image Analysis
3.5. Diagnostic Accuracy
4. Discussion
Author Contributions
Funding
Conflicts of Interest
References
- Celakovsky, P.; Kalfert, D.; Tucek, L.; Mejzlik, J.; Vrbacky, A.; Matousek, P.; Stanikova, L.; Hoskova, T.; Pasz, A. Deep neck infections: Risk factors for mediastinal extension. Eur. Arch. Otorhinolaryngol. 2014, 271, 1679–1683. [Google Scholar] [CrossRef] [PubMed]
- Parhiscar, A.; Har-El, G. Deep Neck Abscess: A Retrospective Review of 210 Cases. Ann. Otol. Rhinol. Laryngol. 2001, 110, 1051–1054. [Google Scholar] [CrossRef] [PubMed]
- Wang, B.; Gao, B.-L.; Xu, G.-P.; Xiang, C. Images of deep neck space infection and the clinical significance. Acta Radiol. 2014, 55, 945–951. [Google Scholar] [CrossRef] [PubMed]
- Wippold, F.J., II. Head and neck imaging: The role of CT and MRI. J. Magn. Reson. Imaging 2007, 25, 453–465. [Google Scholar] [CrossRef]
- Page, C.; Biet, A.; Zaatar, R.; Strunski, V. Parapharyngeal abscess: Diagnosis and treatment. Eur. Arch. Otorhinolaryngol. 2008, 265, 681–686. [Google Scholar] [CrossRef]
- Miracle, A.; Mukherji, S. Conebeam CT of the Head and Neck, Part 2: Clinical Applications. Am. J. Neuroradiol. 2009, 30, 1285–1292. [Google Scholar] [CrossRef]
- Risberg, S.; Engfeldt, P.; Hugosson, S. Incidence of peritonsillar abscess and relationship to age and gender: Retrospective study. Scand. J. Infect. Dis. 2008, 40, 792–796. [Google Scholar] [CrossRef]
- Berrington de Gonzalez, A.; Mahesh, M.; Kim, K.-P.; Bhargavan, M.; Lewis, R.; Mettler, F.; Land, C. Projected cancer risks from computed tomographic scans performed in the United States in 2007. Arch. Intern. Med. 2009, 169, 2071–2077. [Google Scholar] [CrossRef]
- Brenner, D.J. Slowing the Increase in the Population Dose Resulting from CT Scans. Radiat. Res. 2010, 174, 809–815. [Google Scholar] [CrossRef]
- Scholtz, J.-E.; Hüsers, K.; Kaup, M.; Albrecht, M.; Beeres, M.; Bauer, R.; Schulz, B.; Vogl, T.; Wichmann, J. Evaluation of image quality and dose reduction of 80 kVp neck computed tomography in patients with suspected peritonsillar abscess. Clin. Radiol. 2015, 70, e67–e73. [Google Scholar] [CrossRef]
- Scholtz, J.-E.; Wichmann, J.L.; Hüsers, K.; Albrecht, M.H.; Beeres, M.; Bauer, R.W.; Vogl, T.J.; Bodelle, B. Third-generation dual-source CT of the neck using automated tube voltage adaptation in combination with advanced modeled iterative reconstruction: Evaluation of image quality and radiation dose. Eur. Radiol. 2016, 26, 2623–2631. [Google Scholar] [CrossRef] [PubMed]
- Weiss, J.; Maurer, M.; Ketelsen, D.; Notohamiprodjo, M.; Zinsser, D.; Wichmann, J.L.; Nikolaou, K.; Bamberg, F.; Othman, A.E. Effect of reduced z-axis scan coverage on diagnostic performance and radiation dose of neck computed tomography in patients with suspected cervical abscess. PLoS ONE 2017, 12, e0180671. [Google Scholar] [CrossRef] [PubMed]
- Vachha, B.; Brodoefel, H.; Wilcox, C.; Hackney, D.B.; Moonis, G. Radiation dose reduction in soft tissue neck CT using adaptive statistical iterative reconstruction (ASIR). Eur. J. Radiol. 2013, 82, 2222–2226. [Google Scholar] [CrossRef] [PubMed]
- Haubenreisser, H.; Meyer, M.; Sudarski, S.; Allmendinger, T.; Schoenberg, S.O.; Henzler, T. Unenhanced third-generation dual-source chest CT using a tin filter for spectral shaping at 100 kVp. Eur. J. Radiol. 2015, 84, 1608–1613. [Google Scholar] [CrossRef]
- Mangold, S.; De Cecco, C.N.; Wichmann, J.L.; Canstein, C.; Varga-Szemes, A.; Caruso, D.; Fuller, S.R.; Bamberg, F.; Nikolaou, K.; Schoepf, U.J. Effect of automated tube voltage selection, integrated circuit detector and advanced iterative reconstruction on radiation dose and image quality of 3rd generation dual-source aortic CT angiography: An intra-individual comparison. Eur. J. Radiol. 2016, 85, 972–978. [Google Scholar] [CrossRef]
- Kataria, B.; Althén, J.N.; Smedby, Ö.; Persson, A.; Sökjer, H.; Sandborg, M. Assessment of image quality in abdominal CT: Potential dose reduction with model-based iterative reconstruction. Eur. Radiol. 2018, 28, 2464–2473. [Google Scholar] [CrossRef]
- Solomon, J.B.; Marin, D.; Choudhury, K.R.; Patel, B.; Samei, E. Effect of Radiation Dose Reduction and Reconstruction Algorithm on Image Noise, Contrast, Resolution, and Detectability of Subtle Hypoattenuating Liver Lesions at Multidetector CT: Filtered Back Projection versus a Commercial Model-based Iterative Reconstruction Algorithm. Radiology 2017, 284, 777–787. [Google Scholar] [CrossRef]
- Ellmann, S.; Kammerer, F.; Allmendinger, T.; Brand, M.; Janka, R.; Hammon, M.; Lell, M.M.; Uder, M.; Kramer, M. Dose reduction potential of iterative reconstruction algorithms in neck CTA—a simulation study. Dentomaxillofac. Radiol. 2016, 45, 20160228. [Google Scholar] [CrossRef]
- Kramer, M.; Ellmann, S.; Allmendinger, T.; Eller, A.; Kammerer, F.; May, M.S.; Baigger, J.F.; Uder, M.; Lell, M.M. Computed Tomography Angiography of Carotid Arteries and Vertebrobasilar System: A Simulation Study for Radiation Dose Reduction. Medicine 2015, 94, e1058. [Google Scholar] [CrossRef]
- Strahlenschutz, B.F. Bekanntmachung der Aktualisierten Diagnostischen Referenzwerte für Diagnostische und Interventionelle Röntgenanwendungen. (In German). Available online: https://www.bfs.de/SharedDocs/Downloads/BfS/DE/fachinfo/ion/drw-roentgen.pdf?__blob=publicationFile&v=1. (accessed on 22 June 2016).
- Scholtz, J.-E.; Kaup, M.; Hüsers, K.; Albrecht, M.H.; Bodelle, B.; Metzger, S.C.; Kerl, J.M.; Bauer, R.W.; Lehnert, T.; Vogl, T.J.; et al. Advanced Modeled Iterative Reconstruction in Low-Tube-Voltage Contrast-Enhanced Neck CT: Evaluation of Objective and Subjective Image Quality. Am. J. Neuroradiol. 2015, 37, 143–150. [Google Scholar] [CrossRef]
- Brito, T.P.; Hazboun, I.M.; Fernandes, F.L.; Bento, L.R.; Zappelini, C.E.M.; Chone, C.T.; Crespo, A.N. Deep neck abscesses: Study of 101 cases. Braz. J. Otorhinolaryngol. 2017, 83, 341–348. [Google Scholar] [CrossRef] [PubMed]
- Gaddikeri, S.; Andre, J.B.; Benjert, J.; Hippe, D.S.; Anzai, Y. Impact of Model-Based Iterative Reconstruction on Image Quality of Contrast-Enhanced Neck CT. Am. J. Neuroradiol. 2014, 36, 391–396. [Google Scholar] [CrossRef] [PubMed]
- Bodelle, B.; Klein, E.; Naguib, N.N.; Bauer, R.W.; Kerl, J.M.; Al-Butmeh, F.; Wichmann, J.; Ackermann, H.; Lehnert, T.; Vogl, T.J.; et al. Acute Intracranial Hemorrhage in CT: Benefits of Sinogram-Affirmed Iterative Reconstruction Techniques. Am. J. Neuroradiol. 2014, 35, 445–449. [Google Scholar] [CrossRef] [PubMed]
- May, M.S.; Wust, W.; Brand, M.; Stahl, C.; Allmendinger, T.; Schmidt, B.; Uder, M.; Lell, M.M. Dose reduction in abdominal computed tomography: Intraindividual comparison of image quality of full-dose standard and half-dose iterative reconstructions with dual-source computed tomography. Investig. Radiol. 2011, 46, 465–470. [Google Scholar] [CrossRef]
- Vardhanabhuti, V.; Riordan, R.D.; Mitchell, G.R.; Hyde, C.; Roobottom, C.A. Image comparative assessment using iterative reconstructions: Clinical comparison of low-dose abdominal/pelvic computed tomography between adaptive statistical, model-based iterative reconstructions and traditional filtered back projection in 65 patients. Investig. Radiol. 2014, 49, 209–216. [Google Scholar] [CrossRef] [PubMed]
- Ellmann, S.; Kammerer, F.; Allmendinger, T.; Hammon, M.; Janka, R.; Lell, M.; Uder, M.; Kramer, M. Advanced Modeled Iterative Reconstruction (ADMIRE) Facilitates Radiation Dose Reduction in Abdominal CT. Acad. Radiol. 2018, 25, 1277–1284. [Google Scholar] [CrossRef] [PubMed]
- Gordic, S.; Desbiolles, L.; Stolzmann, P.; Gantner, L.; Leschka, S.; Husarik, D.B.; Alkadhi, H. Advanced modelled iterative reconstruction for abdominal CT: Qualitative and quantitative evaluation. Clin. Radiol. 2014, 69, e497–e504. [Google Scholar] [CrossRef] [PubMed]
- Tao, S.; Rajendran, K.; McCollough, C.H.; Leng, S. Feasibility of multi-contrast imaging on dual-source photon counting detector (PCD) CT: An initial phantom study. Med. Phys. 2019, 46, 4105–4115. [Google Scholar] [CrossRef] [PubMed]

| Variables | n (%)/Mean ± SD |
|---|---|
| Patients | 48 |
| Age (years) Sex (M/F) | 45.5 ± 17.7 33 (68.8%)/15 (31.2%) |
| Clinical diagnosis | Cervical abscess (n = 35) Peritonsillar (n = 28) Parapharyngeal (n = 7) Other pathologies (n = 12) Parotitis (n = 4) Tonsillitis (n = 3) Lymphadenitis colli (n = 2) Pharyngitis (n = 1) Sialadenitis (n = 1) Odontogenic inflammation (n = 1) No pathology (n = 1) |
| Dose25 | Dose50 | Dose75 | |||||||
|---|---|---|---|---|---|---|---|---|---|
| AD3 | AD5 | FBP | AD3 | AD5 | FBP | AD3 | AD5 | FBP | |
| Signal-to-noise ratio | |||||||||
| 4.4 ±1.7 5.7 ± 2.4 | 5.9 ± 2.3 7.5 ± 2.9 | 3.0 ± 1.0 4.5 ± 1.6 | 5.5 ± 1.9 6.8 ± 2.6 | 7.3 ± 2.9 8.6 ± 3.5 | 4.0 ± 1.4 5.3 ± 1.9 | 6.3 ± 2.4 7.5 ± 2.9 | 8.4 ± 3.2 9.3 ± 4.3 | 4.7 ± 1.7 5.9 ± 2.2 |
| Contrast-to-noise ratio | |||||||||
| 7.9 ± 3.5 9.4 ± 4.6 | 11.1 ± 4.9 13.1 ± 6.4 | 6.1 ± 2.2 7.3 ± 3.0 | 10.4 ± 3.3 12.2 ± 4.2 | 14.6 ± 8.3 16.9 ± 9.1 | 7.9 ± 2.5 9.2 ± 3.3 | 12.3 ± 4.6 14.5 ± 6.0 | 15.7 ± 5.9 18 ± 7.8 | 9.3 ± 2.9 10.9 ± 3.9 |
| Dose (Recon Mode) and Reader 1–3 | Sensitivity % (95% CI) | Specificity % (95% CI) | PPV % (95% CI) | NPV % (95% CI) |
|---|---|---|---|---|
| Dose 25 | ||||
| AD3, AD5 | 100 (88–100) | 100 (88–100) | 100 (73–100) | 100 (87–100) |
| FBP: | ||||
| Reader 1 | 88.6 (72–96) | 92.3 (62–99) | 96.9 (82–99) | 75 (47–91) |
| Reader 2 | 91.4 (76–98) | 100 (72–100) | 100 (87–100) | 81.3 (54–95) |
| Reader 3 | 94.3 (80–99) | 100 (72–100) | 100 (87–100) | 86.7 (58–98) |
| Dose 50 | ||||
| AD3, AD5, FBP | ||||
| Reader 1–3 | 100 (88–100) | 100 (72–100) | 100 (88–100) | 100 (72–100) |
| Dose 75 | ||||
| AD3, AD5, FBP | ||||
| (Reader 1–3) | 100 (88–100) | 100 (72–100) | 100 (88–100) | 100 (72–100) |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2020 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Winkelmann, M.T.; Afat, S.; Walter, S.S.; Stock, E.; Schwarze, V.; Brendlin, A.; Kolb, M.; Artzner, C.P.; Othman, A.E. Diagnostic Performance of Different Simulated Low-Dose Levels in Patients with Suspected Cervical Abscess Using a Third-Generation Dual-Source CT Scanner. Diagnostics 2020, 10, 1072. https://doi.org/10.3390/diagnostics10121072
Winkelmann MT, Afat S, Walter SS, Stock E, Schwarze V, Brendlin A, Kolb M, Artzner CP, Othman AE. Diagnostic Performance of Different Simulated Low-Dose Levels in Patients with Suspected Cervical Abscess Using a Third-Generation Dual-Source CT Scanner. Diagnostics. 2020; 10(12):1072. https://doi.org/10.3390/diagnostics10121072
Chicago/Turabian StyleWinkelmann, Moritz T., Saif Afat, Sven S. Walter, Eva Stock, Vincent Schwarze, Andreas Brendlin, Manuel Kolb, Christoph P. Artzner, and Ahmed E. Othman. 2020. "Diagnostic Performance of Different Simulated Low-Dose Levels in Patients with Suspected Cervical Abscess Using a Third-Generation Dual-Source CT Scanner" Diagnostics 10, no. 12: 1072. https://doi.org/10.3390/diagnostics10121072
APA StyleWinkelmann, M. T., Afat, S., Walter, S. S., Stock, E., Schwarze, V., Brendlin, A., Kolb, M., Artzner, C. P., & Othman, A. E. (2020). Diagnostic Performance of Different Simulated Low-Dose Levels in Patients with Suspected Cervical Abscess Using a Third-Generation Dual-Source CT Scanner. Diagnostics, 10(12), 1072. https://doi.org/10.3390/diagnostics10121072






