Abstract
Nonalcoholic fatty liver disease (NAFLD) is one of the most common causes of chronic liver disease. As the second stage of developing steatosis, nonalcoholic hepatitis (NASH) carries the risk of fibrosis, cirrhosis, and hepatocellular carcinoma. Sarcopenia is defined as a condition characterized by a decrease in muscle mass and functional decline. Both NAFLD and sarcopenia are global problems. The pathophysiological mechanisms that link the two entities of the disease are insulin resistance, inflammation, nutritional deficiencies, impairment of myostatin and adiponectin, or physical inactivity. Furthermore, disorders of the gut-liver axis appear to induce the process of developing NAFLD and sarcopenia. The correlations between NAFLD and sarcopenia appear to be bidirectional, so the main objective of the review was to determine the cause-and-effect relationship between the two diseases.
1. Introduction
Nonalcoholic fatty liver disease (NAFLD) is one of the most prevalent liver diseases worldwide [1]. It is estimated that a quarter of the population is affected [2]. NAFLD is determined by liver steatosis that is not related to alcohol consumption [3]. Due to the severity of the disease, two stages of the disease can be distinguished [4]. The first is nonalcoholic fatty liver (NAFL), which is not associated with inflammation and fibrosis [5]. The next stage is nonalcoholic steatohepatitis (NASH). It is associated with inflammatory infiltration, the possibility of developing fibrosis and cirrhosis, and hepatocellular carcinoma (HCC) [6]. The term MAFLD, which describes steatohepatic disease associated with metabolic dysfunction, is increasingly appearing in scientific reports. Metabolic dysfunction-associated fatty liver disease (MAFLD) is said to emphasize the association between the coexistence of liver steatosis and various components of metabolic syndrome. Importantly, MAFLD, unlike NAFLD, does not exclude alcohol abuse [7].
Sarcopenia is a condition characterized by a decrease in muscle mass, a decrease in muscle function, and a loss of physical fitness. Sarcopenia can be divided into primary and secondary. Primary sarcopenia is closely related to the physiological process of aging. Secondary sarcopenia, on the other hand, is associated with chronic diseases but also with dietary errors and physical inactivity [8,9]. It is estimated to occur in 11–50% of patients older than 80 years of age. The global trend toward aging has made sarcopenia a worldwide problem [10]. A study was conducted on 15,132 individuals from the Korean population to determine the association between NAFLD and sarcopenia. Sarcopenia has been shown to be associated with a higher risk of NAFLD, regardless of the presence of obesity [11]. Another study was conducted in the United States of America (USA) with 11,325 participants. The researchers identified NAFLD based on the presence of hepatic steatosis on ultrasound. The prevalence of NAFLD was shown to be more common in patients with sarcopenia than without sarcopenia [12]. In addition, it appears that an increase in muscle mass may have an effect on inhibiting the development of NAFLD [13]. When analyzing all the data, it is difficult to determine whether sarcopenia is a result of NAFLD or its risk factor. Therefore, the main purpose of the review is to identify factors that are associated with both sarcopenia and non-alcoholic fatty liver disease.
2. Nonalcoholic Fatty Liver Disease (NAFLD)
NAFLD is one of the most frequently diagnosed chronic liver diseases [14,15]. It is considered the leading cause of mortality, taking into account all liver-related pathologies [16]. NAFLD is a broad and collective term that describes a spectrum of liver diseases resulting from causes other than excessive alcohol consumption [17]. NAFLD includes liver steatosis in >5% of all hepatocyte cells. Liver steatosis itself is referred to in medical nomenclature as nonalcoholic fatty liver (NAFL). The next stage in which inflammation occurs along with liver cell damage is called nonalcoholic steatohepatitis (NASH) [18]. NASH can eventually lead to the development of organ fibrosis and cirrhosis [19].
Importantly, the liver is an organ that accounts for 15% of oxygen consumption in the human body. It follows that hepatocytes are cells rich in mitochondria [20]. It has been observed that in mouse models with NAFLD, there is a decrease in mitochondrial ATP-synthesizing respiration. This appears to occur because the mitochondria are unable to oxidize sufficient fatty acids [21,22]. Impaired mitochondrial function can induce oxidative stress. Consequently, it promotes inflammation and predisposes to NAFLD [23]. It appears that preventing NAFLD progression and restoring liver function can be achieved by focusing on improving mitochondrial activity. There are recent indications that the ketogenic diet can induce improvements in mitochondrial function through stimulation of mitochondriogenesis and bioenergetic pathways [24,25].
In the final stage, impaired liver function can induce liver failure, which requires organ transplantation [26]. In 2009, NASH represented about 10% of liver transplants in the United States [27]. Approximately 30–40% of patients with NAFLD have been reported to develop NASH [28]. Furthermore, patients with NAFLD have an increased risk of extrahepatic complications, including cardiovascular disease and malignancies [29,30]. Currently, the prevalence of NAFLD is estimated to be around 25% in the general population [31]. The number of patients with NAFLD in the United States is estimated to increase from 83.1 million in 2015 to 100.9 million in 2030 [32]. The analyses show that NAFLD can develop in 70% of overweight individuals and up to 90% of those with established obesity [33]. Asians, on the other hand, have been found to accumulate fat in hepatocytes more rapidly than normal-weight individuals [34]. The number of patients with NASH is also expected to increase due to the aging process, as is the expected increase in the prevalence of diabetes among the elderly [32]. Furthermore, the percentage of children diagnosed with hepatic steatosis has increased in recent years [35].
Recently, researchers have pointed out that the name NAFLD does not emphasize the role of the metabolic syndrome in the overall pathogenesis as well as the complications of liver disease. Therefore, a new definition has been proposed, which is MAFLD, or metabolic steatohepatic disease. This definition defines an independent disease entity and excludes the criterion of alcohol abuse [36]. Many studies show a reciprocal correlation between NAFLD and metabolic disorders, which indicates that NAFLD may be a cause but also a consequence of extrahepatic metabolic diseases [37,38]. In patients with established NAFLD, it is very common to find the coexistence of one or more components of metabolic syndrome (MS), such as dyslipidaemia, hypertension, insulin resistance (IR), and diabetes [39,40]. It is widely believed that NAFLD is one of the hepatic manifestations of MS [41]. Importantly, the mechanism of interaction between MS and NAFL may be bilateral. Consequently, NAFLD increases the possibility of MS [42]. The coexistence of NAFLD with MS is correlated with an increased risk of cardiovascular disease and type 2 diabetes. On the contrary, no such correlations were found in patients with NAFLD without concomitant MS [43]. On the other hand, Baratta et al. showed that patients with liver steatosis have an increased risk of cardiovascular disease, and this risk is further increased in patients with already established organ fibrosis [44]. Importantly, patients without established excess body weight have also been shown to have a higher rate of cardiovascular events [45]. Another study showed that NAFLD, regardless of predisposing factors, increases the risk of myocardial infarction [46]. In addition, there are meta-analyses that confirm that the presence of NAFLD is associated with cardiovascular disease [47,48].
There is a lack of approved drugs to treat NAFL and NASH [49]. The European Association for the Study of the Liver (EASL) recommends that patients make lifestyle modifications. Focusing especially on physical activity and changes in eating habits. In recent years, the Mediterranean diet has been proposed and may be beneficial for patients with NAFLD [50]. Adherence to a Mediterranean diet for 6 months resulted in a decrease in intrahepatic fat and an improvement in the state of the MS trait [51]. The reduction in weight in overweight or obese individuals with established NAFLD resulted in a greater improvement in liver function and increased insulin sensitivity compared to healthy overweight individuals [52]. Interventions such as lifestyle changes appear to be the most important and effective for preventing and controlling NAFL without developing NASH and fibrosis [53]. A weight loss of 7–10% appears to have beneficial effects in patients with NAFLD, regardless of diet composition [54]. However, many scientific societies recommend the Mediterranean diet as the recommended dietary pattern [55]. Softic et al. show that fructose has a greater effect on obesity and insulin resistance compared to glucose. Especially when combined with a high-fat diet [56]. In addition, it appears that a high-carbohydrate or fat-only-focused diet is not sufficient to induce NAFLD. It has been suggested that it is the combination of different nutrients that stimulates the induction of liver disease [57]. In addition, the introduction of physical activity helps maintain muscle mass and strength, especially in middle-aged and older individuals [58].
Therefore, it is necessary to undertake research that will help determine the exact quantitative and qualitative composition of diet and physical activity intensity that will enable a reduction in the risk of NAFLD while also halting the progression of the disease.
3. Sarcopenia
Sarcopenia is defined as muscle failure and is defined by a low index of measurements such as strength, quantity, quality of muscle, and physical capacity [59]. Sarcopenia is divided into primary and secondary. The primary is related to age and is a natural process such as aging, and no other significant cause can be identified [60]. Secondary, on the other hand, is due to systemic diseases, physical inactivity, or nutritional errors [61]. In addition, sarcopenic obesity is referred to in the literature. It is defined as the co-occurrence of obesity and sarcopenia [15]. Sarcopenia is a multifactorial disease. The main risk factors for sarcopenia include older age, female sex, low levels of physical activity, and the presence of chronic diseases [62]. Oxidative stress, chronic inflammation, inadequate caloric intake, and neuromuscular junction degeneration overlap to cause the progression of sarcopenia [63,64]. Decreased muscle mass plays an important role in the induction of IR and metabolic syndrome. Sarcopenia is often associated with cardiometabolic disorders such as cardiovascular disease and diabetes [65]. Han et al. showed that both sarcopenia and cardiovascular disease can be associated with similar risk factors such as hypertension, diabetes, dyslipidemia, and metabolic syndrome [66]. The effect of sarcopenia and the amount of muscle mass in liver disease is also increasingly being studied [67].
It is estimated that sarcopenia is diagnosed in about 29% of elderly people living in healthcare facilities, with those aged ≥80 years estimated to have sarcopenia in 11–50% of them [68]. Sarcopenia contributes to an increased risk of falls and disability, increased hospitalizations, and mortality [69,70]. In some sense, primary sarcopenia is inevitable, but its severity depends on the amount of physical activity, hormonal balance, the ability to synthesize and regenerate proteins, or early developmental influences [71]. Sarcopenia appears to be a physiological process, as it begins between the ages of 30 and 40 and is found to increase after the age of 60 [72]. The physiological changes that occur with aging can have important implications in terms of decreased muscle mass and reduced functionality. These changes include low-level chronic systemic inflammation and increased concentrations of reactive oxygen species (ROS) [73]. Ageing causes an increase in oxidative stress, which negatively affects mitochondrial function [74]. When mitochondrial function and structure are disrupted, redox balance is impaired. As a consequence, cell function is impaired, and, thus, health deteriorates [75]. Ageing is associated with ROS production but also with impaired endogenous antioxidant enzyme production in muscle and brain. This process can induce sarcopenia [76,77,78]. Additionally, elevated inflammatory mediators are found in the elderly. These include interleukin 6 (IL-6), tumor necrosis factor α (TNF-α), and C-reactive protein (CRP) [79]. In addition, naturally occurring aging causes an imbalance between the anabolic and catabolic mechanisms of muscle proteins [80]. Insufficient calorie and protein intake leads to a reduction in muscle mass and function [72]. In women after menopause, the concentration of sex hormones decreases, among other estrogen [81]. Patients with sarcopenia often experience a reduced quality of life, most often resulting from a decrease in physical fitness. This lower quality of life can, therefore, hinder patient communication [82]. Hsu et al. showed that in adults with established obesity, a high-protein diet combined with physical activity can improve strength, muscle function, and exercise capacity [83]. Similarly, Seo et al. showed that resistance training in older women with diagnosed sarcopenia improves muscle quality and functional capacity [84]. Resistance training appears to be used in prevention and as a form of therapy for sarcopenia in adults and the elderly [85,86,87].
4. NAFLD and Sarcopenia: Common Factors
Patients with sarcopenia have poorer recurrence-free survival (RFS) in early-stage intrahepatic recurrent hepatocellular carcinoma [88]. Its severity increases with the progression of the underlying disease. In patients with cirrhosis, its prevalence is estimated to be around 60% [89,90]. Its incidence depends on the ethical background, the severity of liver disease, and the selected criteria for its diagnosis [91]. Furthermore, sarcopenia has been identified as a predisposing factor to the severity of NAFLD [92]. Its presence is associated with an increased risk of NAFLD, but also with the appearance of advanced organ fibrosis [93,94]. Lee et al. came to similar conclusions. In their study, they showed that sarcopenia is correlated with organ fibrosis in patients with NAFLD. Importantly, this association was independent of IR and obesity [95]. Similarly, Koo et al. observed a correlation between fibrosis, NAFLD, and sarcopenia, further indicating that this relationship was not dependent on systemic inflammation [96]. Tantai et al. found that sarcopenia associated with cirrhosis could increase the risk of death by two times. Furthermore, mortality increased with the severity and duration of sarcopenia [97]. Studies show that the presence of sarcopenia in patients with cirrhosis generates an increased incidence of infections, prolonged hospitalization after organ transplantation, and increased hyperammonemia and visible liver encephalopathy [98,99,100]. In addition, sarcopenia generates metabolic disorders that include impaired glucose tolerance, impaired ammonia, and amino acid metabolism. Also, it affects bone structure. Sarcopenia and osteoporosis that occur at the same time are defined as osteosarcopenia [101]. Saeki et al. studied the prevalence of osteosarcopenia in 291 patients with chronic liver disease. Osteosarcopenia was found in 16.8% of patients [102]. Patients with coexisting sarcopenia and NAFLD have reduced creatinine production, which causes problems in estimating renal function in these patients [103]. In cirrhosis, factors such as hyperammonemia, hypogonadism, and branched-chain amino acid (BCAA) deficiency appear to influence the development and progression of sarcopenia [104]. In addition, nutritional disorders, insulin resistance, lipid disorders, and a disturbed gut microbiota [105]. Both the risk of NAFL and sarcopenia increases with age, and both conditions are a major public health problem and a burden on health care [98,106]. Many studies indicate associations between the presence of sarcopenia and NAFLD. However, they very often lack an analysis of factors that may interfere with the final results. Undoubtedly, lifestyle, which is defined by factors such as nutrition and physical activity but also economic and social factors, has a huge impact on the final analyses. The complexity of these factors makes them difficult to measure unambiguously. As a result, it is difficult to adjust to them. The research is presented in Table 1.

Table 1.
Studies on the association between sarcopenia and NAFLD.
4.1. Insulin Resistance
NAFLD and sarcopenia share common pathophysiological mechanisms. These include IR, systemic inflammation, impairment of myostatin and adiponectin function, catabolic factor production, nutritional deficiencies, and physical inactivity [12,110]. This is shown in Figure 1.
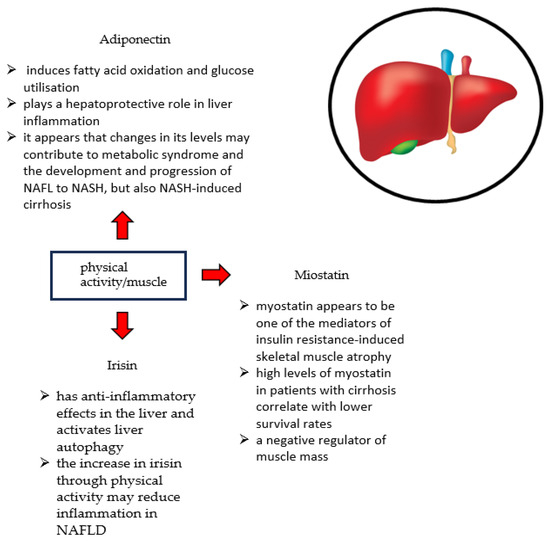
Figure 1.
The relationship between muscle, myokines, and liver.
Studies show that IR is a pathological condition that can induce NAFLD and sarcopenia [111,112,113]. IR is a situation in which the physiological response of target skeletal muscle cells to insulin is disrupted and the body’s carbohydrate metabolism is impaired, thus enhancing the development of sarcopenia. IR appears to induce sarcopenia by affecting various physiological processes in the body. These include decreased synthesis of skeletal muscle proteins and increased catabolism, increased expression of forkhead box O (FOXO) family proteins, and the autophagy process that occurs in skeletal muscle [114]. Patients with NAFLD appear to be prone to sarcopenia despite a high body mass index (BMI) [15]. Furthermore, impaired gluconeogenesis caused by hyperinsulinemia promotes proteolysis and decreases protein synthesis. This situation, with age, can promote sarcopenia [115]. On the other hand, a decrease in muscle mass exacerbates IR. This is due to the fact that skeletal muscle is the primary insulin-responsive organ [116]. Hyperinsulinemia associated with IR causes inhibition of β-oxidation of fats in the liver and an increase in the binding protein of the sterol regulatory element 1c (SREBP-1c). This results in the accumulation of triacylglycerols and free fatty acids in the organ [117]. Smith et al., in their study, showed that de novo lipogenesis in the liver is responsible for the regulation of intrahepatic triglycerides and that increased glucose and insulin levels induce de novo lipogenesis [118]. Importantly, NAFLD can also induce IR. It appears that this may be due to the action of hepatokines such as fibroblast growth factor (FGF)-21 and fetuin-A, which are produced by the liver in response to oxidative stress [119].
4.2. Myosteatosis
Patients with liver disease, especially cirrhosis, can simultaneously experience a situation in which fat mass increases and skeletal muscle mass is reduced. This condition can be referred to as “sarcopenic obesity”. It appears that inflammation, insulin resistance, and vitamin D deficiency may be associated with sarcopenic obesity in the Korean population [120]. In addition, sarcopenic obesity is associated with higher morbidity and mortality than these individuals separately [15]. Importantly, loss of muscle mass characterized by both a decrease in muscle size and an increase in intermuscular fat is defined as myosteatosis. Infiltration of adipose tissue into skeletal muscle is associated with metabolic abnormalities and reduced muscle mobility and strength. Its severity increases with the age of the patient [121,122]. The presence of myosteatosis is correlated with a high mortality risk, but also with IR [123]. Hsieh et al. showed that advanced myosteatosis is associated with the early progression of NASH and liver fibrosis [124]. Nachit et al. propose myosteatosis as a non-invasive marker for the detection of NASH [125].
4.3. Inflammation
Sarcopenia and NAFLD are also related to systemic inflammation. The accumulation of lipids promotes the secretion of pro-inflammatory cytokines from adipose tissue. This results in ROS induction. This occurs through impaired mitochondrial function, which consequently initiates lipid peroxidation. Interleukin-6 (IL-6), tumor necrosis factor-α (TNF-α), and transforming growth factor-β (TGF-β) are among the cytokines that generate low-grade chronic inflammation [109,126]. Patients with NAFLD also show elevated levels of TNF-α. TNF-α, in turn, is responsible for stimulating nuclear factor κB, which is involved in the development of NAFLD but also induces muscle catabolism [127,128]. In addition, TNF-α participates in the activation of de novo lipogenesis, which ultimately causes lipid accumulation in the liver [129]. In sarcopenia, the main pro-inflammatory cytokines include TNF-α, IL-6, and interleukin-1 (IL-1) [130]. Hong et al. showed that patients with sarcopenia have higher levels of CRP compared to patients without sarcopenia. In addition, they found that CRP levels showed a negative correlation with the index of liver function and skeletal muscle mass. These findings may indicate that inflammation is involved in the pathogenesis of NAFLD as well as sarcopenia [107]. Patients with NAFLD have excessive oxidation of free fatty acids (FFA); consequently, this promotes the formation of ROS. These, in turn, cause lipid peroxidation and the production of pro-inflammatory cytokines. In addition, liver-produced hepatokines are produced by the liver (e.g., fetuin A and B, selenoprotein P), which, due to their multidirectional functions, affect IR, lipid metabolism, protein catabolism, and sarcopenia. These broad-spectrum functions of hepatokines may explain the relationship between adipose tissue, muscle tissue, and the liver [131].
4.4. Vitamin D
Vitamin D deficiencies may increase the risk of developing sarcopenia [132]. Vitamin D is responsible for the increase in muscle fiber size, but it also increases their strength and endurance [133]. Furthermore, it is involved in cell differentiation and the proper functioning of the immune system, as well as in the regulation of cardiovascular and calcium-phosphate homeostasis [134]. In the elderly, vitamin D deficiency is common and a worldwide problem. In this group of people, it is usually due to low exposure to the sun and chronic diseases such as renal failure and malabsorption [135]. Recently, a correlation has been confirmed between vitamin D deficiency and the progression of fibrosis in chronic liver disease [136,137,138]. The prevalence of vitamin D deficiency is estimated to be found in 64% to 92% of patients with chronic liver disease [139]. The causes of these deficiencies appear to include a lower supply of exogenous vitamin D (both from the diet and low sun exposure), impaired absorption, decreased synthesis of vitamin D binding protein (VDBP), but also impaired hydroxylation in the liver and increased catabolism of 25(OH)D [140]. Izadi et al. showed an inverse relationship between 25(OH)D levels and aspartate aminotransferase (AST) and alanine aminotransferase (ALT) [141]. In addition, Wang et al. showed a positive correlation between vitamin D levels and irisin levels in women with sarcopenia [142]. Studies on vitamin D supplementation in patients with NAFLD are conflicting, so further research is needed in this area [143,144,145,146].
4.5. Physical Activity
Physical activity induces the production of anti-inflammatory cytokines while inhibiting the production of pro-inflammatory cytokines. Physical exertion also increases muscle protein synthesis and glucose uptake, which reduces the risk of sarcopenia [147]. On the contrary, lack of exercise can induce chronic inflammation, IR, and oxidative stress, resulting in disease exacerbation in patients with NAFLD and sarcopenia [148]. Additionally, physical inactivity results in reduced energy consumption and reduced muscle mass. The result is a fatty liver and obesity [149]. Furthermore, physical activity can contribute to a decrease in the secretion of fetuin A, which is responsible for the promotion of IR in the muscle and liver, but also increase the secretion of the inhibitor myostatin [150]. Increasing physical activity in sarcopenic patients can help reduce the risk of progression of IR [147]. Iwanaga et al. showed that physical activity based on electrical neuromuscular stimulation reduces the severity of IR by lowering IL-6 and selenoprotein levels [151]. Physical activity associated with building muscle mass plays an important role in reducing the risk of chronic diseases. Physical training has the potential to act as a therapy for lifestyle-related diseases. These include cardiovascular disease, cancer, type 2 diabetes, and dementia [152]. In addition, exercise-induced IL-6 can promote and enhance lipolysis [153]. Given these mechanisms, analyses confirm that low physical activity is associated with a higher risk of NAFLD [118,154]. Ageing, fat, and IR accumulation alter the signaling pathways for growth hormone (GH) and insulin-like growth factor 1 (IGF-1). Consequently, this leads to a decrease in muscle mass synthesis [155]. Cabrera et al. showed that induced NAFLD mice show an association of reduced IGF-1 with reductions in muscle mass and muscle strength. The authors also suggest a link between reduced IGF-1 and the pathogenesis of NAFLD-associated sarcopenia [108]. The study by Foong et al. showed that the intensity and amount of physical activity had an independent dose-response relationship with lower limb strength and percent lean body mass. These results suggest that increased physical activity in the elderly is necessary to maintain body weight with age [156]. In addition, in another study, Foong et al. suggest that increased physical activity may be necessary for weight reduction in older adults [157]. Importantly, physical activity is a key factor in the development of sarcopenia. Physical activity is responsible for skeletal muscle synthesis; its absence can result in the development of IR [15,62]. Furthermore, physical activity can be a major confounding factor in many studies, so it seems important to carefully analyze its presence and intensity in the patients studied.
4.6. Myokines
Skeletal muscles not only belong to the musculoskeletal system but also play an important secretory role [158]. Skeletal muscles secrete myokines, including Il-6, irisin, myostatin, and adiponectin. They play a role in the regulation of glucose and fatty acid metabolism. Disturbed levels of these myokines resulting from decreased muscle mass can cause fat accumulation in the liver [93]. The relationship between muscle, myockines, and liver is shown in Figure 1.
In patients with liver disease, hepatocyte dysfunction, impaired urea cycle, constipation, and intestinal dysbiosis contribute to hyperammonemia. The increased absorption of ammonia by skeletal muscle contributes to the development of sarcopenia. Muscle hyperammonemia results in increased myostatin expression and decreased activation of nuclear factor kappa B (Nf-B). As a result, impaired muscle protein synthesis occurs [159]. Myostatin is a negative regulator of muscle mass, which plays a key role in the development and maintenance of skeletal muscle mass [160]. Mutations or genetic disorders resulting in myostatin atrophy cause skeletal muscle hypertrophy [161]. Myostatin appears to be one of the mediators of insulin resistance-induced skeletal muscle atrophy [103,162]. In addition, in patients with cirrhosis, significantly elevated levels of ammonia can increase myostatin expression. Hyperammonemia appears to be an important inducer of sarcopenia by affecting the increase in myostatin [163]. Nishikawa et al. showed that high myostatin levels in patients with cirrhosis were correlated with lower survival rates [164]. In contrast, irisin is a myokine that is produced in response to exercise. It is responsible for fat-browning and thermogenesis [165]. Additionally, it exhibits anti-inflammatory effects in the liver and activates liver autophagy [166]. In addition, Zhao et al. showed that irisin is associated with sarcopenia in patients with cirrhosis [167]. Kosmalski et al. suggest that irisin can be used as a diagnostic marker for NAFLD, as it is associated with biochemical and anthropometric parameters related to liver function [168]. Wu et al. showed that irisin treatment can reduce age-related skeletal muscle fibrosis [169]. On the contrary, Zhu et al. have shown that increasing irisin levels through physical activity can reduce inflammation in NAFLD [170]. Adiponectin is one of the most common adipokines in human plasma. It is produced and secreted primarily by white adipose tissue [171]. Adiponectin induces fatty acid oxidation and glucose utilization [172]. In addition, it exhibits anti-inflammatory effects. In liver inflammation, it plays a hepatoprotective role [173]. It appears that changes in their levels can contribute to the development of MS, the development and progression of NAFL to NASH, and also NASH-induced cirrhosis [174,175]. The myokines described above are shown in Table 2.

Table 2.
Myokines.
4.7. Intestinal Microbiota
The intestine is directly connected to the liver through the portal vein [176]. These organs interact with each other through multiple pathways and are thus involved in the induction and progression of many diseases [177]. Intestinal bacteria and their metabolites can enter the liver through the portal vein, through which they can influence liver disease processes [178]. Dysfunction of the gut-liver axis contributes to the pathogenesis of NAFLD through processes such as disruption of the intestinal barrier and intestinal translocation, as well as the inflammatory response of the liver [179]. Disruption of the gut microbiota in cirrhosis contributes to hyperammonemia. This, in turn, plays a key role in the induction of sarcopenia and IR [180]. Furthermore, in cirrhosis, intestinal dysbiosis is associated with reduced intestinal bacterial diversity, reduced antioxidant activity, and endotoxemia. This in turn is associated with chronic inflammation, mitochondrial dysfunction, and IR, which can cause the progression of cirrhosis and sarcopenia [181]. Furthermore, recent indications suggest that amino acids synthesized by the gut microbiota may be involved in the occurrence of sarcopenia [182]. Obese people are found to have an increased risk of dysbiosis and increased lipopolysaccharide (LPS) production. In turn, LPS causes skeletal muscle damage via the gut-liver-muscle axis. Consequently, LPS and obesity play a role in the induction of sarcopenia [183]. Fecal microbiota transplantation can be used in the future to treat NAFLD. It seems that fecal microbiota transplantation has a positive effect on gut microbiota disorders in these patients [184]. Furthermore, a combination of nutritional modification and increased physical activity contributes to a reduction in the intestinal dysbiosis characteristic of patients with NAFLD [185].
5. Conclusions
Many factors are shown to be common in the pathophysiology of NAFLD and sarcopenia. Given existing studies, it is impossible to say whether sarcopenia is a risk factor or a consequence of NAFLD. However, there is undoubtedly a link between the two due to the presence of common pathophysiological factors. More studies are needed to clearly define the cause-and-effect relationship between these entities so that it will be easier to select prevention and therapy for these patients. In addition, it is worth noting the introduction of physical activity that is tailored to the patient’s capabilities, as well as dietary modifications depending on the patient’s comorbidities and dietary preferences. Ultimately, there is a lack of data that clearly identifies lifestyle changes as adjunctive therapies for primary treatment in patients with NAFLD associated with sarcopenia.
Author Contributions
Conceptualization, K.F., S.J.-C. and R.F.; writing—original draft preparation, K.F., S.J.-C. and R.F.; writing—review and editing, K.F., S.J.-C. and R.F.; supervision, R.F. All authors have read and agreed to the published version of the manuscript.
Funding
This research received no external funding.
Institutional Review Board Statement
Not applicable.
Informed Consent Statement
Not applicable.
Data Availability Statement
No new data were created or analyzed in this study. Data sharing is not applicable to this article.
Conflicts of Interest
The authors declare no conflict of interest.
References
- Younossi, Z.M.; Koenig, A.B.; Abdelatif, D.; Fazel, Y.; Henry, L.; Wymer, M. Global epidemiology of nonalcoholic fatty liver disease-Meta-analytic assessment of prevalence, incidence, and outcomes. Hepatology 2016, 64, 73–84. [Google Scholar] [CrossRef] [PubMed]
- Guo, X.; Yin, X.; Liu, Z.; Wang, J. Non-Alcoholic Fatty Liver Disease (NAFLD) Pathogenesis and Natural Products for Prevention and Treatment. Int. J. Mol. Sci. 2022, 23, 15489. [Google Scholar] [CrossRef] [PubMed]
- Chalasani, N.; Younossi, Z.; Lavine, J.E.; Diehl, A.M.; Brunt, E.M.; Cusi, K.; Charlton, M.; Sanyal, A.J. The diagnosis and management of non-alcoholic fatty liver disease: Practice Guideline by the American Association for the Study of Liver Diseases, American College of Gastroenterology, and the American Gastroenterological Association. Hepatology 2012, 55, 2005–2023. [Google Scholar] [CrossRef] [PubMed]
- Sveinbjornsson, G.; Ulfarsson, M.O.; Thorolfsdottir, R.B.; Jonsson, B.A.; Einarsson, E.; Gunnlaugsson, G.; Rognvaldsson, S.; Arnar, D.O.; Baldvinsson, M.; Bjarnason, R.G.; et al. Multiomics study of nonalcoholic fatty liver disease. Nat. Genet. 2022, 54, 1652–1663. [Google Scholar] [CrossRef] [PubMed]
- Day, C.P.; James, O.F. Steatohepatitis: A tale of two “hits”? Gastroenterology 1998, 114, 842–845. [Google Scholar] [CrossRef] [PubMed]
- Rinella, M.E. Nonalcoholic fatty liver disease: A systematic review. JAMA 2015, 313, 2263–2273. [Google Scholar] [CrossRef] [PubMed]
- Eslam, M.; Newsome, P.N.; Sarin, S.K.; Anstee, Q.M.; Targher, G.; Romero-Gomez, M.; Zelber-Sagi, S.; Wong, V.W.S.; Dufour, J.F.; Schattenberg, J.M.; et al. A new definition for metabolic dysfunction-associated fatty liver disease: An international expert consensus statement. J. Hepatol. 2020, 73, 202–209. [Google Scholar] [CrossRef] [PubMed]
- Liu, C.; Cheung, W.-H.; Li, J.; Kwoon-Ho Chow, S.; Yu, J.; Hei Wong, S.; Ip, M.; Yiu Sung, J.J.; Yeung Wong, R.M. Understanding the gut microbiota and sarcopenia: A systematic revie. JCSM 2021, 12, 1393–1407. [Google Scholar] [CrossRef]
- Noce, A.; Marrone, G.; Ottaviani, E.; Guerriero, C.; Di Daniele, F.; Pietroboni Zaitseva, A.; Di Daniele, N. Uremic Sarcopenia and Its Possible Nutritional Approach. Nutrients 2021, 13, 147. [Google Scholar] [CrossRef]
- Kim, S.H.; Jeong, J.B.; Kang, J.; Ahn, D.W.; Kim, J.W.; Kim, B.G.; Lee, K.L.; Oh, S.; Yoon, S.H.; Park, S.J.; et al. Association between sarcopenia level and metabolic syndrome. PLoS ONE 2021, 16, e0248856. [Google Scholar] [CrossRef]
- Lee, Y.-H.; Jung, K.S.; Kim, S.U.; Yoon, H.J.; Yun, Y.J.; Lee, B.W.; Kang, E.S.; Han, K.H.; Lee, H.C.; Cha, B.S. Sarcopaenia is associated with NAFLD independently of obesity and insulin resistance: Nationwide surveys (KNHANES 2008–2011). J. Hepatol. 2015, 63, 486–493. [Google Scholar] [CrossRef] [PubMed]
- Wijarnpreecha, K.; Kim, D.; Raymond, P.; Scribani, M.; Ahmed, A. Associations between sarcopenia and nonalcoholic fatty liver disease and advanced fibrosis in the USA. Eur. J. Gastroenterol. Hepatol. 2019, 31, 1121–1128. [Google Scholar] [CrossRef] [PubMed]
- Kim, G.; Lee, S.E.; Lee, Y.B.; Jun, J.E.; Ahn, J.; Bae, J.C.; Jin, S.M.; Hur, K.Y.; Jee, J.H.; Lee, M.K.; et al. Relationship Between Relative Skeletal Muscle Mass and Nonalcoholic Fatty Liver Disease: A 7-Year Longitudinal Study. Hepatology 2018, 68, 1755–1768. [Google Scholar] [CrossRef]
- Younossi, Z.M.; Stepanova, M.; Younossi, Y.; Golabi, P.; Mishra, A.; Rafiq, N.; Henry, L. Epidemiology of chronic liver diseases in the USA in the past three decades. Gut 2020, 69, 564–568. [Google Scholar] [CrossRef] [PubMed]
- Iwaki, M.; Kobayashi, T.; Nogami, A.; Saito, S.; Nakajima, A.; Yoneda, M. Impact of Sarcopenia on Non-Alcoholic Fatty Liver Disease. Nutrients 2023, 15, 891. [Google Scholar] [CrossRef]
- Whalley, S.; Puvanachandra, P.; Desai, A.; Kennedy, H. Hepatology outpatient service provision in secondary care: A study of liver disease incidence and resource costs. Clin. Med. 2007, 7, 119–124. [Google Scholar] [CrossRef] [PubMed]
- Nassir, F. NAFLD: Mechanisms, Treatments, and Biomarkers. Biomolecules 2022, 12, 824. [Google Scholar] [CrossRef]
- Wong, R.J.; Aguilar, M.; Cheung, R.; Perumpail, R.B.; Harrison, S.A.; Younossi, Z.M.; Ahmed, A. Nonalcoholic steatohepatitis is the second leading etiology of liver disease among adults awaiting liver transplantation in the United States. Gastroenterology 2015, 148, 547–555. [Google Scholar] [CrossRef]
- Pouwels, S.; Sakran, N.; Graham, Y.; Leal, A.; Pintar, T.; Yang, W.; Kassir, R.; Singhal, R.; Mahawar, K.; Ramnarain, D. Non-alcoholic fatty liver disease (NAFLD): A review of pathophysiology, clinical management and effects of weight loss. BMC Endocr. Disord. 2022, 22, 63. [Google Scholar] [CrossRef]
- Shum, M.; Ngo, J.; Shirihai, O.S.; Liesa, M. Mitochondrial oxidative function in NAFLD: Friend or foe? Mol. Metab. 2021, 50, 101134. [Google Scholar] [CrossRef]
- Arruda, A.; Pers, B.; Parlakgül, G.; Güney, E.; Inouye, K.; Hotamisligil, G.S. Chronic enrichment of hepatic endoplasmic reticulum–mitochondria contact leads to mitochondrial dysfunction in obesity. Nat. Med. 2014, 20, 1427–1435. [Google Scholar] [CrossRef] [PubMed]
- Boland, M.L.; Laker, R.C.; Mather, K.; Nawrocki, A.; Oldham, S.; Boland, B.B.; Lewis, H.; Conway, J.; Naylor, J.; Guionaud, S.; et al. Resolution of NASH and hepatic fibrosis by the GLP-1R and GCGR dual-agonist cotadutide via modulating mitochondrial function and lipogenesis. Nat. Metab. 2020, 2, 413–431. [Google Scholar] [CrossRef] [PubMed]
- Mansouri, A.; Gattolliat, C.-H.; Asselach, T. Mitochondrial Dysfunction and Signaling in Chronic Liver Diseases. Gastroenterology 2018, 155, 629–647. [Google Scholar] [CrossRef] [PubMed]
- Paoli, A.; Cerullo, G. Investigating the Link between Ketogenic Diet, NAFLD, Mitochondria, and Oxidative Stress: A Narrative Review. Antioxidants 2023, 12, 1065. [Google Scholar] [CrossRef] [PubMed]
- Ilyas, Z.; Perna, S.; Alalwan, T.A.; Zahid, M.N.; Spadaccini, D.; Gasparri, C.; Peroni, G.; Faragli, A.; Alogna, A.; La Porta, E.; et al. The Ketogenic Diet: Is It an Answer for Sarcopenic Obesity? Nutrients 2022, 14, 620. [Google Scholar] [CrossRef] [PubMed]
- Caussy, C.; Soni, M.; Cui, J.; Bettencourt, R.; Schork, N.; Chen, C.H.; Al Ikhwan, M.; Bassirian, S.; Cepin, S.; Gonzalez, M.P.; et al. Familial NAFLD Cirrhosis Research Consortium. Nonalcoholic fatty liver disease with cirrhosis increases familial risk for advanced fibrosis. J. Clin. Investig. 2017, 127, 2697–2704. [Google Scholar] [CrossRef] [PubMed]
- Charlton, M.R.; Burns, J.M.; Pedersen, R.A.; Watt, K.D.; Heimbach, J.K.; Dierkhising, R.A. Frequency and outcomes of liver transplantation for nonalcoholic steatohepatitis in the United States. Gastroenterology 2011, 141, 1249–1253. [Google Scholar] [CrossRef]
- Ekstedt, M.; Franzén, L.E.; Mathiesen, U.L.; Thorelius, L.; Holmqvist, M.; Bodemar, G.; Kechagias, S. Long-term follow-up of patients with NAFLD and elevated liver enzymes. Hepatology 2006, 44, 865–873. [Google Scholar] [CrossRef]
- Lindenmeyer, C.C.; McCullough, A.J. The Natural History of Nonalcoholic Fatty Liver Disease-An Evolving View. Clin. Liver Dis. 2018, 22, 11–21. [Google Scholar] [CrossRef]
- Rinella, M.E.; Sanyal, A.J. Management of NAFLD: A stage-based approach. Nat. Rev. Gastroenterol. Hepatol. 2016, 13, 196–205. [Google Scholar] [CrossRef]
- Friedman, S.L.; Neuschwander-Tetri, B.A.; Rinella, M.; Sanyal, A.J. Mechanisms of NAFLD development and therapeutic strategies. Nat. Med. 2018, 24, 908–922. [Google Scholar] [CrossRef] [PubMed]
- Estes, C.; Razavi, H.; Loomba, R.; Younossi, Z.; Sanyal, A.J. Modeling the epidemic of nonalcoholic fatty liver disease demonstrates an exponential increase in burden of disease. Hepatology 2018, 67, 123–133. [Google Scholar] [CrossRef] [PubMed]
- Younossi, Z.M. Non-alcoholic fatty liver disease—A global public health perspective. J. Hepatol. 2019, 70, 531–544. [Google Scholar] [CrossRef] [PubMed]
- Younes, R.; Bugianesi, E. NASH in Lean Individuals. Semin. Liver Dis. 2019, 39, 86–95. [Google Scholar] [CrossRef] [PubMed]
- Nobili, V.; Alisi, A.; Valenti, L.; Miele, L.; Feldstein, A.E.; Alkhouri, N. NAFLD in children: New genes, new diagnostic modalities and new drugs. Nat. Rev. Gastroenterol. Hepatol. 2019, 16, 517–530. [Google Scholar] [CrossRef] [PubMed]
- Eslam, M.; Sanyal, A.J.; George, J. International Consensus Panel. MAFLD: A Consensus-Driven Proposed Nomenclature for Metabolic Associated Fatty Liver Disease. Gastroenterology 2020, 158, 1999–2014. [Google Scholar] [CrossRef] [PubMed]
- Adams, L.A.; Anstee, Q.M.; Tilg, H.; Targher, G. Non-alcoholic fatty liver disease and its relationship with cardiovascular disease and other extrahepatic diseases. Gut 2017, 66, 1138–1153. [Google Scholar] [CrossRef] [PubMed]
- Lonardo, A.; Nascimbeni, F.; Mantovani, A.; Targher, G. Hypertension, diabetes, atherosclerosis and NASH: Cause or consequence? J. Hepatol. 2018, 68, 335–352. [Google Scholar] [CrossRef]
- Dixon, J.B.; Bhathal, P.S.; O’Brien, P.E. Nonalcoholic fatty liver disease: Predictors of nonalcoholic steatohepatitis and liver fibrosis in the severely obese. Gastroenterology 2001, 121, 91–100. [Google Scholar] [CrossRef]
- Huang, P.L. A comprehensive definition for metabolic syndrome. Dis. Model. Mech. 2009, 2, 231–237. [Google Scholar] [CrossRef]
- Tarantino, G.; Finelli, C. What about non-alcoholic fatty liver disease as a new criterion to define metabolic syndrome? World J. Gastroenterol. 2013, 19, 3375–3384. [Google Scholar] [CrossRef] [PubMed]
- Allen, A.M.; Therneau, T.M.; Larson, J.J.; Coward, A.; Somers, V.K.; Kamath, P.S. Nonalcoholic fatty liver disease incidence and impact on metabolic burden and death: A 20 year-community study. Hepatology 2018, 67, 1726–1736. [Google Scholar] [CrossRef] [PubMed]
- Käräjämäki, A.J.; Bloigu, R.; Kauma, H.; Kesäniemi, Y.A.; Koivurova, O.P.; Perkiömäki, J.; Huikuri, H.; Ukkola, O. Non-alcoholic fatty liver disease with and without metabolic syndrome: Different long-term outcomes. Metabolism 2017, 66, 55–63. [Google Scholar] [CrossRef] [PubMed]
- Baratta, F.; Pastori, D.; Angelico, F.; Balla, A.; Paganini, A.M.; Cocomello, N.; Ferro, D.; Violi, F.; Sanyal, A.J.; Del Ben, M. Nonalcoholic Fatty Liver Disease and Fibrosis Associated With Increased Risk of Cardiovascular Events in a Prospective Study. Clin. Gastroenterol. Hepatol. 2020, 18, 2324–2331. [Google Scholar] [CrossRef] [PubMed]
- Yoshitaka, H.; Hamaguchi, M.; Kojima, T.; Fukuda, T.; Ohbora, A.; Fukui, M. Nonoverweight nonalcoholic fatty liver disease and incident cardiovascular disease: A post hoc analysis of a cohort study. Medicine 2017, 96, e6712. [Google Scholar] [CrossRef] [PubMed]
- Hyun Sinn, D.; Kang, D.; Chang, Y.; Ryu, S.; Cho, S.J.; Paik, S.W.; Song, Y.B.; Pastor-Barriuso, R.; Guallar, E.; Cho, J.; et al. Non-alcoholic fatty liver disease and the incidence of myocardial infarction: A cohort study. JGHF 2020, 35, 833–839. [Google Scholar] [CrossRef]
- Wu, S.; Wu, F.; Ding, Y.; Hou, J.; Bi, J.; Zhang, Z. Association of non-alcoholic fatty liver disease with major adverse cardiovascular events: A systematic review and meta-analysis. Sci. Rep. 2016, 6, 33386. [Google Scholar] [CrossRef]
- Targher, G.; Byrne, C.D.; Lonardo, A.; Zoppini, G.; Barbui, C. Non-alcoholic fatty liver disease and risk of incident cardiovascular disease: A meta-analysis. J. Hepatol. 2016, 65, 589–600. [Google Scholar] [CrossRef]
- Sanyal, A.J.; Friedman, S.L.; McCullough, A.J.; Dimick-Santos, L.; American Association for the Study of Liver Diseases; United States Food and Drug Administration. Challenges and opportunities in drug and biomarker development for nonalcoholic steatohepatitis: Findings and recommendations from an American Association for the Study of Liver Diseases-U.S. Food and Drug Administration Joint Workshop. Hepatology 2015, 61, 1392–1405. [Google Scholar] [CrossRef]
- Godos, J.; Federico, A.; Dallio, M.; Scazzina, F. Mediterranean diet and nonalcoholic fatty liver disease: Molecular mechanisms of protection. Int. J. Food Sci. Nutr. 2017, 68, 18–27. [Google Scholar] [CrossRef]
- Montemayor, S.; Mascaró, C.M.; Ugarriza, L.; Casares, M.; Llompart, I.; Abete, I.; Zulet, M.Á.; Martínez, J.A.; Tur, J.A.; Bouzas, C. Adherence to Mediterranean Diet and NAFLD in Patients with Metabolic Syndrome: The FLIPAN Study. Nutrients 2022, 14, 3186. [Google Scholar] [CrossRef] [PubMed]
- Schübel, R.; Nonnenmacher, T.; Sookthai, D.; Gonzalez Maldonado, S.; Sowah, S.A.; von Stackelberg, O.; Schlett, C.L.; Grafetstätter, M.; Nabers, D.; Johnson, T.; et al. Similar Weight Loss Induces Greater Improvements in Insulin Sensitivity and Liver Function among Individuals with NAFLD Compared to Individuals without NAFLD. Nutrients 2019, 11, 544. [Google Scholar] [CrossRef] [PubMed]
- Xu, X.; Poulsen, K.L.; Wu, L.; Liu, S.; Miyata, T.; Song, Q.; Wei, Q.; Zhao, C.; Lin, C.; Yang, J. Targeted therapeutics and novel signaling pathways in non-alcohol-associated fatty liver/steatohepatitis (NAFL/NASH). Signal Transduct. Target. Ther. 2022, 7, 287. [Google Scholar] [CrossRef] [PubMed]
- Chalasani, N.; Younossi, Z.; Lavine, J.E.; Charlton, M.; Cusi, K.; Rinella, M.; Harrison, S.A.; Brunt, E.M.; Sanyal, A.J. The diagnosis and management of nonalcoholic fatty liver disease: Practice guidance from the American Association for the Study of Liver Diseases. Clin. Liver Dis. 2018, 11, 81. [Google Scholar] [CrossRef] [PubMed]
- Semmler, G.; Datz, C.; Reiberger, T.; Trauner, M. Diet and exercise in NAFLD/NASH: Beyond the obvious. Liver Int. 2021, 41, 2249–2268. [Google Scholar] [CrossRef] [PubMed]
- Softic, S.; Gupta, M.K.; Wang, G.X.; Fujisaka, S.; O’Neill, B.T.; Rao, T.N.; Willoughby, J.; Harbison, C.; Fitzgerald, K.; Ilkayeva, O.; et al. Divergent effects of glucose and fructose on hepatic lipogenesis and insulin signaling. J. Clin. Investig. 2017, 127, 4059–4074. [Google Scholar] [CrossRef] [PubMed]
- Eng, J.M.; Estall, J.L. Diet-Induced Models of Non-Alcoholic Fatty Liver Disease: Food for Thought on Sugar, Fat, and Cholesterol. Cells 2021, 10, 1805. [Google Scholar] [CrossRef]
- Cruz-Jentoft, A.J.; Dawson Hughes, B.; Scott, D.; Sanders, K.M.; Rizzoli, R. Nutritional strategies for maintaining muscle mass and strength from middle age to later life: A narrative review. Maturitas 2020, 13, 57–64. [Google Scholar] [CrossRef]
- Cruz-Jentoft, A.J.; Bahat, G.; Bauer, J.; Boirie, Y.; Bruyère, O.; Cederholm, T.; Cooper, C.; Landi, F.; Rolland, Y.; Sayer, A.A.; et al. Writing Group for the European Working Group on Sarcopenia in Older People 2 (EWGSOP2), and the Extended Group for EWGSOP2. Sarcopenia: Revised European consensus on definition and diagnosis. Age Ageing 2019, 48, 16–31. [Google Scholar] [CrossRef]
- Muscaritoli, M.; Anker, S.D.; Argilés, J.; Aversa, Z.; Bauer, J.M.; Biolo, G.I.A.N.N.I.; Boirie, Y.; Bosaeus, I.; Cederholm, T.; Costelli, P.; et al. Consensus definition of sarcopenia, cachexia and pre-cachexia: Joint document elaborated by Special Interest Groups (SIG) “cachexia-anorexia in chronic wasting diseases” and “nutrition in geriatrics”. Clin. Nutr. 2010, 29, 154–159. [Google Scholar] [CrossRef]
- Sasaki, K.I.; Fukumoto, Y. Sarcopenia as a comorbidity of cardiovascular disease. J. Cardiol. 2022, 79, 596–604. [Google Scholar] [CrossRef] [PubMed]
- Papadopoulou, S.K. Sarcopenia: A Contemporary Health Problem among Older Adult Populations. Nutrients 2020, 12, 1293. [Google Scholar] [CrossRef] [PubMed]
- Marty, E.; Liu, Y.; Samuel, A.; Or, O.; Lane, J. A review of sarcopenia: Enhancing awareness of an increasingly prevalent disease. Bone 2017, 105, 276–286. [Google Scholar] [CrossRef] [PubMed]
- Hashemi, R.; Shafiee, G.; Motlagh, A.D.; Pasalar, P.; Esmailzadeh, A.; Siassi, F.; Larijani, B.; Heshmat, R. Sarcopenia and its associated factors in Iranian older individuals: Results of SARIR study. Arch. Gerontol. Geriatr. 2016, 66, 18–22. [Google Scholar] [CrossRef] [PubMed]
- Kalyani, R.R.; Corriere, M.; Ferrucci, L. Age-related and disease-related muscle loss: The effect of diabetes, obesity, and other diseases. Lancet Diabetes Endocrinol. 2014, 2, 819–829. [Google Scholar] [CrossRef] [PubMed]
- Kim, Y.; Han, B.D.; Han, K.; Shin, K.E.; Lee, H.; Kim, T.R.; Cho, K.H.; Kim, D.H.; Kim, Y.H.; Kim, H.; et al. Optimal cutoffs for low skeletal muscle mass related to cardiovascular risk in adults: The Korea National Health and Nutrition Examination Survey 2009–2010. Endocrine 2015, 50, 424–433. [Google Scholar] [CrossRef]
- Kamimura, H.; Sato, T.; Natsui, K.; Kobayashi, T.; Yoshida, T.; Kamimura, K.; Tsuchiya, A.; Murayama, T.; Yokoyama, J.; Kawai, H.; et al. Molecular Mechanisms and Treatment of Sarcopenia in Liver Disease: A Review of Current Knowledge. Int. J. Mol. Sci. 2021, 22, 1425. [Google Scholar] [CrossRef]
- Cruz-Jentoft, A.J.; Landi, F.; Schneider, S.M.; Zúñiga, C.; Arai, H.; Boirie, Y.; Chen, L.K.; Fielding, R.A.; Martin, F.C.; Michel, J.P.; et al. Prevalence of and interventions for sarcopenia in ageing adults: A systematic review. Report of the International Sarcopenia Initiative (EWGSOP and IWGS). Age Ageing 2014, 43, 748–759. [Google Scholar] [CrossRef]
- Senior, H.E.; Henwood, T.R.; Beller, E.M.; Mitchell, G.K.; Keogh, J.W. Prevalence and risk factors of sarcopenia among adults living in nursing homes. Maturitas 2015, 82, 418–423. [Google Scholar] [CrossRef]
- Cruz-Jentoft, A.J.; Baeyens, J.P.; Bauer, J.M.; Boirie, Y.; Cederholm, T.; Landi, F.; Martin, F.C.; Michel, J.P.; Rolland, Y.; Schneider, S.M.; et al. European Working Group on Sarcopenia in Older People. Sarcopenia: European consensus on definition and diagnosis: Report of the European Working Group on Sarcopenia in Older People. Age Ageing 2010, 39, 412–423. [Google Scholar] [CrossRef]
- Shi, Y.; Zhou, L.; Yan, E.; Yang, L.; Yang, C.; Liu, C. Sarcopenia and perioperative management of elderly surgical patients. Front. Biosci. 2021, 26, 882–894. [Google Scholar] [CrossRef]
- Dhillon, R.J.; Hasni, S. Pathogenesis and Management of Sarcopenia. Clin. Geriatr. Med. 2017, 33, 17–26. [Google Scholar] [CrossRef]
- Dalle, S.; Rossmeislova, L.; Koppo, K. The Role of Inflammation in Age-Related Sarcopenia. Front. Physiol. 2017, 12, 1045. [Google Scholar] [CrossRef]
- Carter, H.N.; Chen, C.C.; Hood, D.A. Mitochondria, muscle health, and exercise with advancing age. Physiology 2015, 30, 208–223. [Google Scholar] [CrossRef]
- Brown, J.L.; Rosa-Caldwell, M.E.; Lee, D.E.; Blackwell, T.A.; Brown, L.A.; Perry, R.A.; Haynie, W.S.; Hardee, J.P.; Carson, J.A.; Wiggs, M.P. Mitochondrial degeneration precedes the development of muscle atrophy in progression of cancer cachexia in tumour-bearing mice. J. Cachexia Sarcopenia Muscle 2017, 8, 926–938. [Google Scholar] [CrossRef]
- Liguori, I.; Russo, G.; Curcio, F.; Bulli, G.; Aran, L.; Della-Morte, D.; Gargiulo, G.; Testa, G.; Cacciatore, F.; Bonaduce, D.; et al. Oxidative stress, aging, and diseases. Clin. Interv. Aging 2018, 26, 757–772. [Google Scholar] [CrossRef]
- Alway, S.E.; Mohamed, J.S.; Myers, M.J. Mitochondria Initiate and Regulate Sarcopenia. Exerc. Sport. Sci. Rev. 2017, 45, 58–69. [Google Scholar] [CrossRef]
- Romanello, V.; Sandri, M. Mitochondrial Quality Control and Muscle Mass Maintenance. Front. Physiol. 2016, 12, 422. [Google Scholar] [CrossRef]
- Tchkonia, T.; Zhu, Y.; van Deursen, J.; Campisi, J.; Kirkland, J.L. Cellular senescence and the senescent secretory phenotype: Therapeutic opportunities. J. Clin. Investig. 2013, 123, 966–972. [Google Scholar] [CrossRef]
- Ali, S.; Garcia, J.M. Sarcopenia, cachexia and aging: Diagnosis, mechanisms and therapeutic options—A mini-review. Gerontology. 2014, 60, 294–305. [Google Scholar] [CrossRef]
- Kalinkovich, A.; Livshits, G. Sarcopenia--The search for emerging biomarkers. Ageing Res. Rev. 2015, 22, 58–71. [Google Scholar] [CrossRef]
- Ohara, D.G.; Pegorari, M.S.; Oliveira Dos Santos, N.L.; de Fátima Ribeiro Silva, C.; Monteiro, R.L.; Matos, A.P.; Jamami, M. Respiratory Muscle Strength as a Discriminator of Sarcopenia in Community-Dwelling Elderly: A Cross-Sectional Study. J. Nutr. Health Aging 2018, 22, 952–958. [Google Scholar] [CrossRef]
- Hsu, K.J.; Chien, K.Y.; Tsai, S.C.; Tsai, Y.S.; Liao, Y.H.; Chen, J.J.; Chen, Y.R.; Chen, C.N. Effects of Exercise Alone or in Combination with High-Protein Diet on Muscle Function, Aerobic Capacity, and Physical Function in Middle-Aged Obese Adults: A Randomized Controlled Trial. J. Nutr. Health Aging 2021, 25, 727–734. [Google Scholar] [CrossRef]
- Seo, M.-W.; Jung, S.-W.; Kim, S.-W.; Lee, J.-M.; Jung, H.C.; Song, J.-K. Effects of 16 Weeks of Resistance Training on Muscle Quality and Muscle Growth Factors in Older Adult Women with Sarcopenia: A Randomized Controlled Trial. Int. J. Environ. Res. Public Health 2021, 18, 6762. [Google Scholar] [CrossRef]
- Chiang, F.-Y.; Chen, J.-R.; Lee, W.-J.; Yang, S.-C. Effects of Milk or Soy Milk Combined with Mild Resistance Exercise on the Muscle Mass and Muscle Strength in Very Old Nursing Home Residents with Sarcopenia. Foods 2021, 10, 2581. [Google Scholar] [CrossRef]
- Peng, L.N.; Yu, P.C.; Hsu, C.C.; Tseng, S.H.; Lee, W.J.; Lin, M.H.; Hsiao, F.Y.; Chen, L.K. Sarcojoint®, the branched-chain amino acid-based supplement, plus resistance exercise improved muscle mass in adults aged 50 years and older: A double-blinded randomized controlled trial. Exp. Gerontol. 2022, 157, 111644. [Google Scholar] [CrossRef]
- Takeuchi, I.; Yoshimura, Y.; Shimazu, S.; Jeong, S.; Yamaga, M.; Koga, H. Effects of branched-chain amino acids and vitamin D supplementation on physical function, muscle mass and strength, and nutritional status in sarcopenic older adults undergoing hospital-based rehabilitation: A multicenter randomized controlled trial. Geriatr. Gerontol. Int. 2019, 19, 12–17. [Google Scholar] [CrossRef]
- Doi, S.; Yasuda, S.; Matsuo, Y.; Sakata, T.; Nishiwada, S.; Nagai, M.; Nakamura, K.; Terai, T.; Kohara, Y.; Sho, M. Clinical impact of sarcopenia in early-stage intrahepatic recurrent hepatocellular carcinoma: An association with impaired host immunity. Langenbecks Arch. Surg. 2023, 408, 433. [Google Scholar] [CrossRef]
- Chen, H.W.; Dunn, M.A. Arresting Frailty and Sarcopenia in Cirrhosis:Future Prospects. Clin. Liver Dis. 2018, 11, 52–57. [Google Scholar] [CrossRef]
- Bhanji, R.A.; Carey, E.J.; Yang, L.; Watt, K.D. The Long Winding Road to Transplant: How Sarcopenia and Debility Impact Morbidity and Mortality on the Waitlist. Clin. Gastroenterol. Hepatol. 2017, 15, 1492–1497. [Google Scholar] [CrossRef]
- Puri, P.; Dhiman, R.K.; Taneja, S.; Tandon, P.; Merli, M.; Anand, A.C.; Arora, A.; Acharya, S.K.; Benjamin, J.; Chawla, Y.K.; et al. Nutrition in Chronic Liver Disease: Consensus Statement of the Indian National Association for Study of the Liver. J. Clin. Exp. Hepatol. 2021, 11, 97–143. [Google Scholar] [CrossRef]
- Zhao, Z.H.; Zou, J.; Huang, X.; Fan, Y.C.; Wang, K. Assessing causal relationships between sarcopenia and nonalcoholic fatty liver disease: A bidirectional Mendelian randomization study. Front. Nutr. 2022, 9, 971913. [Google Scholar] [CrossRef]
- Li, A.A.; Kim, D.; Ahmed, A. Association of sarcopenia and NAFLD: An overview. Clin. Liver Dis. 2020, 16, 73–76. [Google Scholar] [CrossRef]
- Petta, S.; Ciminnisi, S.; Di Marco, V.; Cabibi, D.; Cammà, C.; Licata, A.; Marchesini, G.; Craxì, A. Sarcopenia is associated with severe liver fibrosis in patients with non-alcoholic fatty liver disease. Aliment. Pharmacol. Ther. 2017, 45, 510–518. [Google Scholar] [CrossRef]
- Lee, Y.H.; Kim, S.U.; Song, K.; Park, J.Y.; Ahn, S.H.; Lee, B.W.; Kang, E.S.; Cha, B.S.; Han, K.H. Sarcopenia is associated with significant liver fibrosis independently of obesity and insulin resistance in nonalcoholic fatty liver disease: Nationwide surveys (KNHANES 2008-2011). Hepatology 2016, 63, 776–786. [Google Scholar] [CrossRef]
- Koo, B.K.; Kim, D.; Joo, S.K.; Kim, J.H.; Chang, M.S.; Kim, B.G.; Lee, K.L.; Kim, W. Sarcopenia is an independent risk factor for non-alcoholic steatohepatitis and significant fibrosis. J. Hepatol. 2017, 66, 123–131. [Google Scholar] [CrossRef]
- Tantai, X.; Liu, Y.; Yeo, Y.H.; Praktiknjo, M.; Mauro, E.; Hamaguchi, Y.; Engelmann, C.; Zhang, P.; Jeong, J.Y.; Van Vugt, J.L.A.; et al. Effect of sarcopenia on survival in patients with cirrhosis: A meta-analysis. J. Hepatol. 2022, 76, 588–599. [Google Scholar] [CrossRef]
- Schiavo, L.; Busetto, L.; Cesaretti, M.; Zelber-Sagi, S.; Deutsch, L.; Iannelli, A. Nutritional issues in patients with obesity and cirrhosis. World J. Gastroenterol. 2018, 24, 3330–3346. [Google Scholar] [CrossRef]
- Tandon, P.; Montano-Loza, A.J.; Lai, J.C.; Dasarathy, S.; Merli, M. Sarcopenia and frailty in decompensated cirrhosis. J. Hepatol. 2021, 75, 147-S162. [Google Scholar] [CrossRef]
- Cleasby, M.E.; Jamieson, P.M.; Atherton, P.J. Insulin resistance and sarcopenia: Mechanistic links beetween common co-morbidities. J. Endocrinol. 2016, 229, R67–R81. [Google Scholar] [CrossRef]
- Saeki, C.; Tsubota, A. Influencing Factors and Molecular Pathogenesis of Sarcopenia and Osteosarcopenia in Chronic Liver Disease. Life 2021, 11, 899. [Google Scholar] [CrossRef] [PubMed]
- Saeki, C.; Kanai, T.; Nakano, M.; Oikawa, T.; Torisu, Y.; Abo, M.; Saruta, M.; Tsubota, A. Relationship between Osteosarcopenia and Frailty in Patients with Chronic Liver Disease. J. Clin. Med. 2020, 9, 2381. [Google Scholar] [CrossRef] [PubMed]
- Ichikawa, T.; Miyaaki, H.; Miuma, S.; Motoyoshi, Y.; Yamashima, M.; Yamamichi, S.; Koike, M.; Takahashi, Y.; Honda, T.; Yajima, H.; et al. Indices calculated by serum creatinine and cystatin C as predictors of liver damage, muscle strength and sarcopenia in liver disease. Biomed. Rep. 2020, 12, 89–98. [Google Scholar] [CrossRef] [PubMed]
- Yang, Y.J.; Kim, D.J. An Overview of the Molecular Mechanisms Contributing to Musculoskeletal Disorders in Chronic Liver Disease: Osteoporosis, Sarcopenia, and Osteoporotic Sarcopenia. Int. J. Mol. Sci. 2021, 22, 2604. [Google Scholar] [CrossRef] [PubMed]
- Kumar, R.; Prakash, S.S.; Priyadarshi, R.N.; Anand, U. Sarcopenia in Chronic Liver Disease: A Metabolic Perspective. J. Clin. Transl. Hepatol. 2022, 28, 1213–1222. [Google Scholar] [CrossRef] [PubMed]
- Hamaguchi, M.; Kojima, T.; Ohbora, A.; Takeda, N.; Fukui, M.; Kato, T. Aging is a risk factor of nonalcoholic fatty liver disease in premenopausal women. World J. Gastroenterol. 2012, 18, 237–243. [Google Scholar] [CrossRef]
- Hong, H.C.; Hwang, S.Y.; Choi, H.Y.; Yoo, H.J.; Seo, J.A.; Kim, S.G.; Kim, N.H.; Baik, S.H.; Choi, D.S.; Choi, K.M. Relationship between sarcopenia and nonalcoholic fatty liver disease: The Korean Sarcopenic Obesity Study. Hepatology 2014, 59, 1772–1778. [Google Scholar] [CrossRef] [PubMed]
- Cabrera, D.; Ruiz, A.; Cabello-Verrugio, C.; Brandan, E.; Estrada, L.; Pizarro, M.; Solis, N.; Torres, J.; Barrera, F.; Arrese, M. Diet-Induced Nonalcoholic Fatty Liver Disease Is Associated with Sarcopenia and Decreased Serum Insulin-Like Growth Factor-1. Dig. Dis. Sci. 2016, 61, 3190–3198. [Google Scholar] [CrossRef]
- Han, J.W.; Kim, D.I.; Nam, H.C.; Chang, U.I.; Yang, J.M.; Song, D.S. Association between serum tumor necrosis factor-α and sarcopenia in liver cirrhosis. Clin. Mol. Hepatol. 2022, 28, 219–231. [Google Scholar] [CrossRef]
- Merli, M.; Dasarathy, S. Sarcopenia in non-alcoholic fatty liver disease: Targeting the real culprit? J. Hepatol. 2015, 63, 309–311. [Google Scholar] [CrossRef]
- Rasmussen, B.B.; Fujita, S.; Wolfe, R.R.; Mittendorfer, B.; Roy, M.; Rowe, V.L.; Volpi, E. Insulin resistance of muscle protein metabolism in aging. FASEB J. 2006, 20, 768–769. [Google Scholar] [CrossRef] [PubMed]
- Takamura, T.; Misu, H.; Ota, T.; Kaneko, S. Fatty liver as a consequence and cause of insulin resistance: Lessons from type 2 diabetic liver. Endocr. J. 2012, 59, 745–763. [Google Scholar] [CrossRef] [PubMed]
- Guillet, C.; Boirie, Y. Insulin resistance: A contributing factor to age-related muscle mass loss?La résistance à l’insuline: Un facteur contribuant à la fonte protéique musculaire liée à l’âge? Diabetes Metab. 2005, 31 (Suppl. S1), 5S20–5S26. [Google Scholar] [CrossRef] [PubMed]
- Liu, Z.J.; Zhu, C.F. Causal relationship between insulin resistance and sarcopenia. Diabetol. Metab. Syndr. 2023, 15, 46. [Google Scholar] [CrossRef] [PubMed]
- Joo, S.K.; Kim, W. Interaction between sarcopenia and nonalcoholic fatty liver disease. Clin. Mol. Hepatol. 2023, 29, S68–S78. [Google Scholar] [CrossRef] [PubMed]
- Srikanthan, P.; Hevener, A.L.; Karlamangla, A.S. Sarcopenia exacerbates obesity-associated insulin resistance and dysglycemia: Findings from the National Health and Nutrition Examination Survey III. PLoS ONE 2010, 26, e10805. [Google Scholar] [CrossRef] [PubMed]
- Zhai, Y.; Xiao, Q. The Common Mechanisms of Sarcopenia and NAFLD. Biomed. Res. Int. 2017, 2017, 6297651. [Google Scholar] [CrossRef] [PubMed]
- Smith, G.I.; Shankaran, M.; Yoshino, M.; Schweitzer, G.G.; Chondronikola, M.; Beals, J.W.; Okunade, A.L.; Patterson, B.W.; Nyangau, E.; Field, T.; et al. Insulin resistance drives hepatic de novo lipogenesis in nonalcoholic fatty liver disease. J. Clin. Investig. 2020, 2, 1453–1460. [Google Scholar] [CrossRef]
- Kucukoglu, O.; Sowa, J.P.; Mazzolini, G.D.; Syn, W.K.; Canbay, A. Hepatokines and adipokines in NASH-related hepatocellular carcinoma. J. Hepatol. 2021, 74, 442–457. [Google Scholar] [CrossRef]
- Kim, T.N.; Park, M.S.; Lim, K.I.; Choi, H.Y.; Yang, S.J.; Yoo, H.J.; Kang, H.J.; Song, W.; Choi, H.; Baik, S.H.; et al. Relationships between sarcopenic obesity and insulin resistance, inflammation, and vitamin D status: The Korean Sarcopenic Obesity Study. Clin. Endocrinol. 2013, 78, 525–532. [Google Scholar] [CrossRef]
- Cespiati, A.; Meroni, M.; Lombardi, R.; Oberti, G.; Dongiovanni, P.; Fracanzani, A.L. Impact of Sarcopenia and Myosteatosis in Non-Cirrhotic Stages of Liver Diseases: Similarities and Differences across Aetiologies and Possible Therapeutic Strategies. Biomedicines 2022, 10, 182. [Google Scholar] [CrossRef] [PubMed]
- Correa-de-Araujo, R.; Addison, O.; Miljkovic, I. Myosteatosis in the Context of Skeletal Muscle Function Deficit: An Interdisciplinary Workshop at the National Institute on Aging. Front. Physiol. 2020, 7, 963. [Google Scholar] [CrossRef]
- Montano-Loza, A.J.; Angulo, P.; Meza-Junco, J. Sarcopenic obesity and myosteatosis are associated with higher mortality in patients with cirrhosis. J. Cachexia Sarcopenia Muscle 2016, 7, 126–135. [Google Scholar] [CrossRef] [PubMed]
- Hsieh, Y.-C.; Kyoung Joo, S.; Ko, B.K.; Lin, H.C.; Lee, D.H.; Chang, M.S.; Park, J.H.; So, Y.H.; Kim, W. Myosteatosis, but not Sarcopenia, Predisposes NAFLD Subjects to Early Steatohepatitis and Fibrosis Progression. Hepatology 2023, 21, 388–397. [Google Scholar] [CrossRef] [PubMed]
- Nachit, M.; De Rudder, M.; Thissen, J.P.; Schakman, O.; Bouzin, C.; Horsmans, Y.; Vande Velde, G.; Leclercq, I.A. Myosteatosis rather than sarcopenia associates with non-alcoholic steatohepatitis in non-alcoholic fatty liver disease preclinical models. J. Cachexia Sarcopenia Muscle 2021, 12, 144–158. [Google Scholar] [CrossRef] [PubMed]
- Beyer, I.; Mets, T.; Bautmans, I. Chronic low-grade inflammation and age-related sarcopenia. Curr. Opin. Clin. Nutr. Metab. Care 2012, 15, 12–22. [Google Scholar] [CrossRef] [PubMed]
- Wree, A.; Kahraman, A.; Gerken, G.; Canbay, A. Obesity affects the liver—the link between adipocytes and hepatocytes. Digestion. 2011, 83, 124–133. [Google Scholar] [CrossRef]
- Yuan, S.; Liu, H.; Yuan, D.; Xu, J.; Chen, Y.; Xu, X.; Xu, F.; Liang, H. PNPLA3 I148M mediates the regulatory effect of NF-kB on inflammation in PA-treated HepG2 cells. J. Cell Mol. Med. 2020, 24, 1541–1552. [Google Scholar] [CrossRef]
- Chen, T.; Zhang, X.; Zhu, G.; Liu, H.; Chen, J.; Wang, Y.; He, X. Quercetin inhibits TNF-α induced HUVECs apoptosis and inflammation via downregulating NF-kB and AP-1 signaling pathway in vitro. Medicine 2020, 99, e22241. [Google Scholar] [CrossRef]
- Jimenez-Gutierrez, G.E.; Martínez-Gómez, L.E.; Martínez-Armenta, C.; Pineda, C.; Martínez-Nava, G.A.; Lopez-Reyes, A. Molecular Mechanisms of Inflammation in Sarcopenia: Diagnosis and Therapeutic Update. Cells 2022, 11, 2359. [Google Scholar] [CrossRef]
- Mikolasevic, I.; Pavic, T.; Kanizaj, T.; Bender, D.; Domislovic, V.; Krznaric, Z. Nonalcoholic Fatty Liver Disease and Sarcopenia: Where Do We Stand? Gastroenterol. Hepatol. 2020, 2020, 8859719. [Google Scholar] [CrossRef] [PubMed]
- Visser, M.; Deeg, D.J.; Lips, P. Longitudinal Aging Study Amsterdam. Low vitamin D and high parathyroid hormone levels as determinants of loss of muscle strength and muscle mass (sarcopenia): The Longitudinal Aging Study Amsterdam. J. Clin. Endocrinol. Metab. 2003, 88, 5766–5772. [Google Scholar] [CrossRef] [PubMed]
- Shuler, F.D.; Wingate, M.K.; Moore, G.H.; Giangarra, C. Sports health benefits of vitamin d. Sports Health 2012, 4, 496–501. [Google Scholar] [CrossRef] [PubMed]
- Christakos, S.; Dhawan, P.; Verstuyf, A.; Verlinden, L.; Carmeliet, G. Vitamin D: Metabolism, Molecular Mechanism of Action, and Pleiotropic Effects. Physiol. Rev. 2016, 96, 365–408. [Google Scholar] [CrossRef] [PubMed]
- Remelli, F.; Vitali, A.; Zurlo, A.; Volpato, S. Vitamin D Deficiency and Sarcopenia in Older Persons. Nutrients 2019, 11, 2861. [Google Scholar] [CrossRef] [PubMed]
- Sun, S.; Xu, M.; Zhuang, P.; Chen, G.; Dong, K.; Dong, R.; Zheng, S. Effect and mechanism of vitamin D activation disorder on liver fibrosis in biliary atresia. Sci. Rep. 2021, 11, 19883. [Google Scholar] [CrossRef] [PubMed]
- Eliades, M.; Spyrou, E.; Agrawal, N.; Lazo, M.; Brancati, F.L.; Potter, J.J.; Koteish, A.A.; Clark, J.M.; Guallar, E.; Hernaez, R. Meta-analysis: Vitamin D and non-alcoholic fatty liver disease. Aliment. Pharmacol. Ther. 2013, 38, 246–254. [Google Scholar] [CrossRef]
- Liu, T.; Xu, L.; Chen, F.H.; Zhou, Y.B. Association of serum vitamin D level and nonalcoholic fatty liver disease: A meta-analysis. Eur. J. Gastroenterol. Hepatol. 2020, 32, 140–147. [Google Scholar] [CrossRef]
- Pop, T.L.; Sîrbe, C.; Benţa, G.; Mititelu, A.; Grama, A. The Role of Vitamin D and Vitamin D Binding Protein in Chronic Liver Diseases. Int. J. Mol. Sci. 2022, 23, 10705. [Google Scholar] [CrossRef]
- Stokes, C.S.; Volmer, D.A.; Grünhage, F.; Lammert, F. Vitamin D in chronic liver disease. Liver Int. 2013, 33, 338–352. [Google Scholar] [CrossRef]
- Izadi, A.; Aliasghari, F.; Gargari, B.P.; Ebrahimi, S. Strong association between serum Vitamin D and Vaspin Levels, AIP, VAI and liver enzymes in NAFLD patients. Int. J. Vitam. Nutr. Res. 2020, 90, 59–66. [Google Scholar] [CrossRef] [PubMed]
- Wang, Y.; Gu, Y.; Huang, J.; Wu, H.; Meng, G.; Zhang, Q.; Liu, L.; Zhang, S.; Wang, X.; Zhang, J.; et al. Serum vitamin D status and circulating irisin levels in older adults with sarcopenia. Front. Nutr. 2022, 7, 1051870. [Google Scholar] [CrossRef] [PubMed]
- Barchetta, I.; Del Ben, M.; Angelico, F.; Di Martino, M.; Fraioli, A.; La Torre, G.; Saulle, R.; Perri, L.; Morini, S.; Tiberti, C.; et al. No effects of oral vitamin D supplementation on non-alcoholic fatty liver disease in patients with type 2 diabetes: A randomized, double-blind, placebo-controlled trial. BMC Med. 2016, 29, 92. [Google Scholar] [CrossRef]
- Dasarathy, J.; Varghese, R.; Feldman, A.; Khiyami, A.; McCullough, A.J.; Dasarathy, S. Patients with Nonalcoholic Fatty Liver Disease Have a Low Response Rate to Vitamin D Supplementation. J. Nutr. 2017, 147, 1938–1946. [Google Scholar] [CrossRef] [PubMed]
- Papapostoli, I.; Lammert, F.; Stokes, C.S. Effect of Short-Term Vitamin D Correction on Hepatic Steatosis as Quantified by Controlled Attenuation Parameter (CAP). J. Gastrointestin Liver Dis. 2016, 25, 175–181. [Google Scholar] [CrossRef] [PubMed]
- Alarfaj, S.J.; Bahaa, M.M.; Yassin, H.A.; El-Khateeb, E.; Kotkata, F.A.; El-Gammal, M.A.; Elberri, A.I.; Habba, E.; Zien El-Deen, E.E.; Khrieba, M.O.; et al. A randomized placebo-controlled, double-blind study to investigate the effect of a high oral loading dose of cholecalciferol in non-alcoholic fatty liver disease patients, new insights on serum STAT-3 and hepassocin. Eur. Rev. Med. Pharmacol. Sci. 2023, 27, 7607–7619. [Google Scholar] [CrossRef] [PubMed]
- Steffl, M.; Bohannon, R.W.; Sontakova, L.; Tufano, J.J.; Shiells, K.; Holmerova, I. Relationship between sarcopenia and physical activity in older people: A systematic review and meta-analysis. Clin. Interv. Aging 2017, 12, 835–845. [Google Scholar] [CrossRef]
- Lang, T.; Streeper, T.; Cawthon, P.; Baldwin, K.; Taaffe, D.R.; Harris, T.B. Sarcopenia: Etiology, clinical consequences, intervention, and assessment. Osteoporos. Int. 2010, 21, 543–559. [Google Scholar] [CrossRef]
- Biolo, G.; Cederholm, T.; Muscaritoli, M. Muscle contractile and metabolic dysfunction is a common feature of sarcopenia of aging and chronic diseases: From sarcopenic obesity to cachexia. Clin. Nutr. 2014, 33, 737–748. [Google Scholar] [CrossRef]
- De Fre, C.H.; De Fre, M.A.; Kwanten, W.J.; Op de Beeck, B.J.; Van Gaal, L.F.; Francque, S.M. Sarcopenia in patients with non-alcoholic fatty liver disease: Is it a clinically significant entity? Obes. Rev. 2019, 20, 353–363. [Google Scholar] [CrossRef]
- Iwanaga, S.; Hashida, R.; Takano, Y.; Bekki, M.; Nakano, D.; Omoto, M.; Nago, T.; Kawaguchi, T.; Matsuse, H.; Torimura, T.; et al. Hybrid Training System Improves Insulin Resistance in Patients with Nonalcoholic Fatty Liver Disease: A Randomized Controlled Pilot Study. Tohoku J. Exp. Med. 2020, 252, 23–32. [Google Scholar] [CrossRef] [PubMed]
- Severinsen, M.C.K.; Pedersen, B.K. Muscle-Organ Crosstalk: The Emerging Roles of Myokines. Endocr. Rev. 2020, 1, 594–609. [Google Scholar] [CrossRef] [PubMed]
- Pedersen, B.K.; Febbraio, M.A. Muscle as an endocrine organ: Focus on muscle-derived interleukin-6. Physiol. Rev. 2008, 88, 1379–1406. [Google Scholar] [CrossRef] [PubMed]
- Kim, J.A.; Choi, K.M. Sarcopenia and fatty liver disease. Hepatol. Int. 2019, 13, 674–687. [Google Scholar] [CrossRef]
- Berryman, D.E.; Glad, C.A.; List, E.O.; Johannsson, G. The GH/IGF-1 axis in obesity: Pathophysiology and therapeutic considerations. Nat. Rev. Endocrinol. 2013, 9, 346–356. [Google Scholar] [CrossRef]
- Foong, Y.C.; Chherawala, N.; Aitken, D.; Scott, D.; Winzenberg, T.; Jones, G. Accelerometer-determined physical activity, muscle mass, and leg strength in community-dwelling older adults. J. Cachexia Sarcopenia Muscle 2016, 7, 275–283. [Google Scholar] [CrossRef]
- Foong, Y.C.; Aitken, D.; Winzenberg, T.; Otahal, P.; Scott, D.; Jones, G. The association between physical activity and reduced body fat lessens with age—results from a cross-sectional study in community-dwelling older adults. Exp. Gerontol. 2014, 55, 107–112. [Google Scholar] [CrossRef]
- Pedersen, B.K. Muscle as a secretory organ. Compr. Physiol. 2013, 3, 1337–1362. [Google Scholar] [CrossRef]
- Qiu, J.; Thapaliya, S.; Runkana, A.; Yang, Y.; Tsien, C.; Mohan, M.L.; Narayanan, A.; Eghtesad, B.; Mozdziak, P.E.; McDonald, C.; et al. Hyperammonemia in cirrhosis induces transcriptional regulation of myostatin by an NF-κB-mediated mechanism. Proc. Natl. Acad. Sci. USA 2013, 5, 18162–18167. [Google Scholar] [CrossRef]
- Kang, M.J.; Moon, J.W.; Lee, J.O.; Kim, J.H.; Jung, E.J.; Kim, S.J.; Oh, J.Y.; Wu, S.W.; Lee, P.R.; Park, S.H.; et al. Metformin induces muscle atrophy by transcriptional regulation of myostatin via HDAC6 and FoxO3a. J. Cachexia Sarcopenia Muscle 2022, 13, 605–620. [Google Scholar] [CrossRef]
- Pasteuning-Vuhman, S.; Boertje-van der Meulen, J.W.; van Putten, M.; Overzier, M.; Ten Dijke, P.; Kiełbasa, S.M.; Arindrarto, W.; Wolterbeek, R.; Lezhnina, K.V.; Ozerov, I.V.; et al. New function of the myostatin/activin type I receptor (ALK4) as a mediator of muscle atrophy and muscle regeneration. FASEB J. 2017, 31, 238–255. [Google Scholar] [CrossRef] [PubMed]
- Roy, B.; Curtis, M.E.; Fears, L.S.; Nahashon, S.N.; Fentress, H.M. Molecular Mechanisms of Obesity-Induced Osteoporosis and Muscle Atrophy. Front. Physiol. 2016, 29, 439. [Google Scholar] [CrossRef] [PubMed]
- Kim, Y. Emerging Treatment Options for Sarcopenia in Chronic Liver Disease. Life 2021, 11, 250. [Google Scholar] [CrossRef] [PubMed]
- Nishikawa, H.; Enomoto, H.; Ishii, A.; Iwata, Y.; Miyamoto, Y.; Ishii, N.; Yuri, Y.; Hasegawa, K.; Nakano, C.; Nishimura, T. Elevated serum myostatin level is associated with worse survival in patients with liver cirrhosis. J. Cachexia Sarcopenia Muscle 2017, 8, 915–925. [Google Scholar] [CrossRef] [PubMed]
- Armandi, A.; Rosso, C.; Caviglia, G.P.; Ribaldone, D.G.; Bugianesi, E. The Impact of Dysmetabolic Sarcopenia Among Insulin Sensitive Tissues: A Narrative Review. Front. Endocrinol. 2021, 10, 716533. [Google Scholar] [CrossRef]
- Chen, C.-L.; Lin, Y.-C. Autophagy Dysregulation in Metabolic Associated Fatty Liver Disease: A New Therapeutic Target. Int. J. Mol. Sci. 2022, 23, 10055. [Google Scholar] [CrossRef]
- Zhao, M.; Zhou, X.; Yuan, C.; Li, R.; Ma, Y.; Tang, X. Association between serum irisin concentrations and sarcopenia in patients with liver cirrhosis: A cross-sectional study. Sci. Rep. 2020, 30, 16093. [Google Scholar] [CrossRef]
- Kosmalski, M.; Drzewoski, J.; Szymczak-Pajor, I.; Zieleniak, A.; Mikołajczyk-Solińska, M.; Kasznicki, J.; Śliwińska, A. Irisin Is Related to Non-Alcoholic Fatty Liver Disease (NAFLD). Biomedicines 2022, 10, 2253. [Google Scholar] [CrossRef]
- Wu, Y.; Wu, Y.; Yu, J.; Zhang, Y.; Li, Y.; Fu, R.; Sun, Y.; Zhao, K.; Xiao, Q. Irisin ameliorates D-galactose-induced skeletal muscle fibrosis via the PI3K/Akt pathway. Eur. J. Pharmacol. 2023, 939, 175476. [Google Scholar] [CrossRef]
- Zhu, W.; Sahar, N.E.; Javaid, H.M.A.; Pak, E.S.; Liang, G.; Wang, Y.; Ha, H.; Huh, J.Y. Exercise-Induced Irisin Decreases Inflammation and Improves NAFLD by Competitive Binding with MD2. Cells 2021, 10, 3306. [Google Scholar] [CrossRef]
- Choi, H.M.; Doss, H.M.; Kim, K.S. Multifaceted Physiological Roles of Adiponectin in Inflammation and Diseases. Int. J. Mol. Sci. 2020, 21, 1219. [Google Scholar] [CrossRef] [PubMed]
- Shih, P.-H.; Shiue, S.-J.; Chen, C.-N.; Cheng, S.-W.; Lin, H.-Y.; Wu, L.-W.; Wu, M.-S. Fucoidan and Fucoxanthin Attenuate Hepatic Steatosis and Inflammation of NAFLD through Modulation of Leptin/Adiponectin Axis. Mar. Drugs 2021, 19, 148. [Google Scholar] [CrossRef] [PubMed]
- Takemura, Y.; Ouchi, N.; Shibata, R.; Aprahamian, T.; Kirber, M.T.; Summer, R.S.; Kihara, S.; Walsh, K. Adiponectin modulates inflammatory reactions via calreticulin receptor-dependent clearance of early apoptotic bodies. J. Clin. Investig. 2007, 117, 375–386. [Google Scholar] [CrossRef] [PubMed]
- Shabalala, S.C.; Dludla, S.C.; Mabasa, L.; Kappo, A.P.; Basson, A.K.; Pheiffer, C.; Johnson, R. The effect of adiponectin in the pathogenesis of non-alcoholic fatty liver disease (NAFLD) and the potential role of polyphenols in the modulation of adiponectin signaling. Biomed. Pharmacother. 2020, 131, 110785. [Google Scholar] [CrossRef] [PubMed]
- Dong, Z.; Zhuang, Q.; Ye, X.; Ning, M.; Wu, S.; Lu, L.; Wan, X. Adiponectin Inhibits NLRP3 Inflammasome Activation in Nonalcoholic Steatohepatitis via AMPK-JNK/ErK1/2-NFκB/ROS Signaling Pathways. Front. Med. 2020, 7, 546445. [Google Scholar] [CrossRef] [PubMed]
- Kubes, P.; Jenne, C. Immune Responses in the Liver. Annu. Rev. Immunol. 2018, 36, 247–277. [Google Scholar] [CrossRef]
- Milosevic, I.; Vujovic, A.; Barac, A.; Djelic, M.; Korac, M.; Radovanovic Spurnic, A.; Gmizic, I.; Stevanovic, O.; Djordjevic, V.; Lekic, N.; et al. Gut-Liver Axis, Gut Microbiota, and Its Modulation in the Management of Liver Diseases: A Review of the Literature. Int. J. Mol. Sci. 2019, 20, 395. [Google Scholar] [CrossRef]
- Wiest, R.; Albillos, A.; Trauner, M.; Bajaj, J.S.; Jalan, R. Targeting the gut-liver axis in liver disease. J. Hepatol. 2017, 67, 1084–1103. [Google Scholar] [CrossRef]
- Kolodziejczyk, A.A.; Zheng, D.; Shibolet, O.; Elinav, E. The role of the microbiome in NAFLD and NASH. EMBO Mol. Med. 2019, 11, e9302. [Google Scholar] [CrossRef]
- Ahluwalia, V.; Betrapally, N.S.; Hylemon, P.B.; White, M.B.; Gillevet, P.M.; Unser, A.B.; Fagan, A.; Daita, K.; Heuman, D.M.; Zhou, H.; et al. Impaired Gut-Liver-Brain Axis in Patients with Cirrhosis. Sci. Rep. 2016, 6, 26800. [Google Scholar] [CrossRef]
- Nishikawa, H.; Enomoto, H.; Nishiguchi, S.; Iijima, H. Sarcopenic Obesity in Liver Cirrhosis: Possible Mechanism and Clinical Impact. Int. J. Mol. Sci. 2021, 22, 1917. [Google Scholar] [CrossRef] [PubMed]
- Gojda, J.; Cahova, M. Gut Microbiota as the Link between Elevated BCAA Serum Levels and Insulin Resistance. Biomolecules 2021, 11, 1414. [Google Scholar] [CrossRef] [PubMed]
- Kawamura, N.; Ohnuki, Y.; Matsuo, I.; Suita, K.; Ishikawa, M.; Mototani, Y.; Shiozawa, K.; Ito, A.; Yagisawa, Y.; Hayakawa, Y.; et al. Effects of chronic Porphyromonas gingivalis lipopolysaccharide infusion on skeletal muscles in mice. J. Physiol. Sci. 2019, 69, 503–511. [Google Scholar] [CrossRef] [PubMed]
- Xue, L.; Deng, Z.; Luo, W.; He, X.; Chen, Y. Effect of Fecal Microbiota Transplantation on Non-Alcoholic Fatty Liver Disease: A Randomized Clinical Trial. Front. Cell. Infect. Microbiol. 2022, 12, 759306. [Google Scholar] [CrossRef]
- Calabrese, F.M.; Disciglio, V.; Franco, I.; Sorino, P.; Bonfiglio, C.; Bianco, A.; Campanella, A.; Lippolis, T.; Pesole, P.L.; Polignano, M.; et al. A Low Glycemic Index Mediterranean Diet Combined with Aerobic Physical Activity Rearranges the Gut Microbiota Signature in NAFLD Patients. Nutrients 2022, 14, 1773. [Google Scholar] [CrossRef]
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2023 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
