Non-Surgical Locoregional Therapies Alone or in Combination with Systemic Therapy in Patients with Hepatocellular Carcinoma
Simple Summary
Abstract
1. Introduction
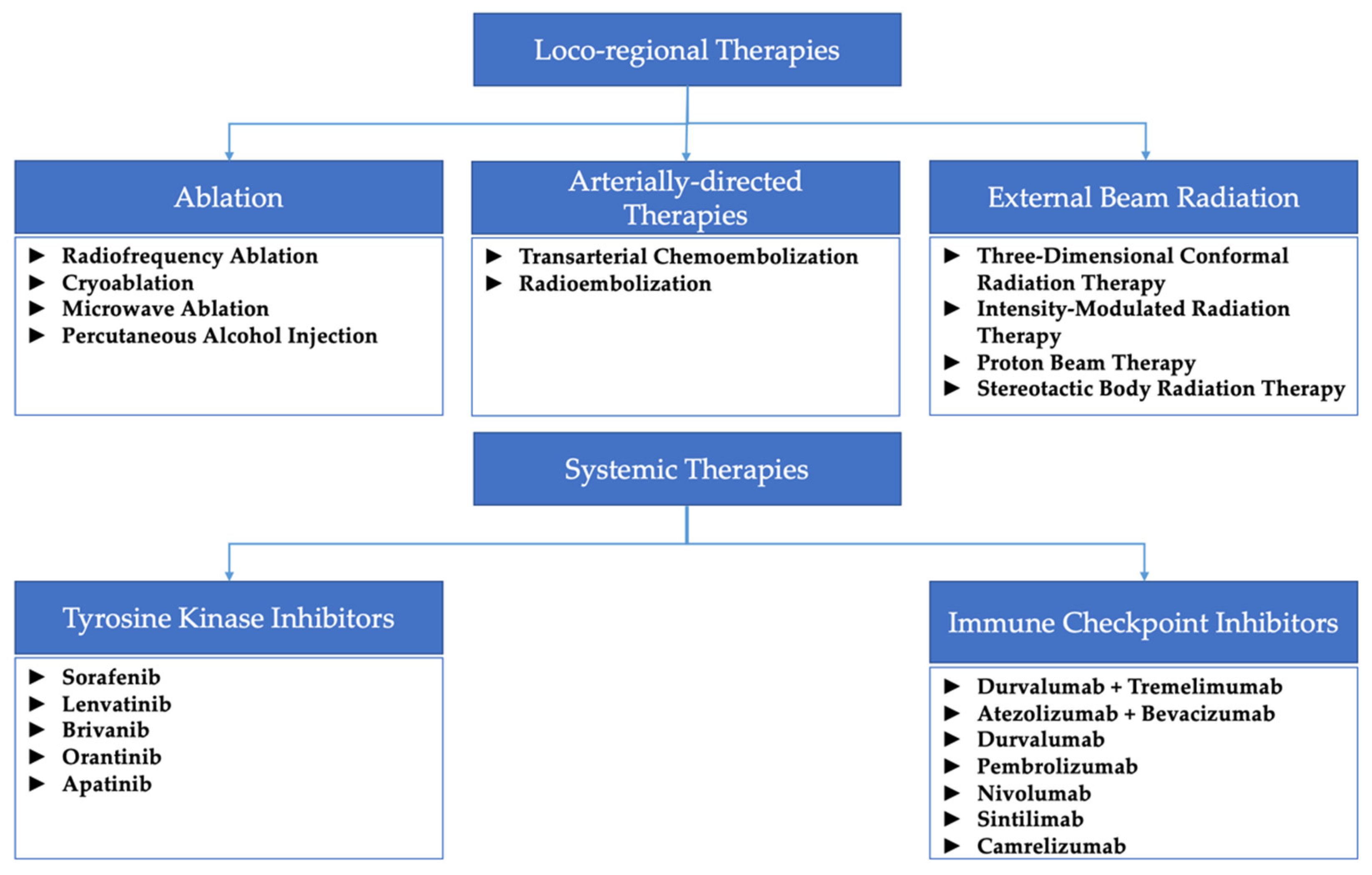
2. Locoregional Therapies
2.1. Ablation
2.1.1. Radiofrequency Ablation
2.1.2. Cryoablation
2.1.3. Microwave Ablation
2.1.4. Percutaneous Alcohol Injection
2.2. Arterially Directed Therapies
2.2.1. Transarterial Chemoembolization
2.2.2. Radioembolization
2.3. External Beam Radiation Therapy
2.3.1. Three-Dimensional Conformal Radiation Therapy
2.3.2. Intensity-Modulated Radiation Therapy
2.3.3. Proton Beam Therapy
2.3.4. Stereotactic Body Radiation Therapy
| Study | Treatment Arms | Primary Endpoints | Outcomes | p-Value |
|---|---|---|---|---|
| Hong et al. [62] | PBT (n = 83) | LC (2 years) | 94.8% (HCC); 94.1% (ICC) | NA |
| OS (2 years) | 63.2% (HCC); 46.5% (ICC) | |||
| Sanford et al. [66] | PBT (n = 49) vs. IMRT/VMAT (n = 84) | OS (median) | 31 vs. 14 months | p = 0.008 |
| Tao et al. [74] | Ablative RT (n = 19) vs. RT (n = 60) | OS (3 years) | 73% vs. 38% | p = 0.017 |
| LC (3 years) | 78% vs. 45% | p = 0.04 | ||
| Hilal et al. [73] | Ablative RT (n = 14) vs. non-ablative RT (n = 31) | LC (1 year) | 91.7% vs. 75.2% | p = 0.038 |
| OS (median) | 28 vs. 7 months | p = 0.044 | ||
| NRG-GI003 NCT03186898 a | Photon RT vs. proton RT (n = 186) | OS | Ongoing |
3. Combination Therapies
| Randomized Controlled Trial | Treatment Arms | Primary Endpoints | Outcomes | p-Value |
|---|---|---|---|---|
| Locoregional therapies | ||||
| PRECISION V [34] | TACE (n = 108) vs. DEB-TACE (n = 93) | Tumor response at 6 months | 22.2% vs. 26.9% | p = 0.11 |
| Treatment-related adverse events within 30 days of a procedure | 19.4% vs. 20.4% | p = 0.86 | ||
| PRECISION ITALIA [96] | TACE (n = 88) vs. DEB-TACE (n = 89) | OS (2 years) | 55.4% vs. 56.8% | p = 0.949 |
| Systemic therapies alone | ||||
| IMbrave150 [5] | Atezolizumab + bevacizumab (n = 336) vs. sorafenib (n = 165) | OS (1 year) | 67.2% vs. 54.6% | p < 0.001 |
| PFS (median) | 6.8 vs. 4.3 months | p < 0.001 | ||
| HIMALAYA [7] | Tremelimumab + durvalumab (n = 393) vs. sorafenib (n = 389) | OS (median) | 16.4 vs. 13.8 months | p = 0.0035 |
| Durvalumab (n = 389) vs. sorafenib (n = 389) noninferiority | OS (median) | 16.6 vs. 13.8 months | p = 0.0035 | |
| LEAP-002 c [81] | Lenvatinib + pembrolizumab vs. lenvatinib alone | OS (median) | 21.2 vs. 19.0 months | p = 0.0227 |
| PFS (median) | 8.2 vs. 8.0 months | p = 0.0466 | ||
| Systemic therapies in combination with locoregional therapies | ||||
| SPACE [82] | DEB-TACE + sorafenib (n = 154) vs. DEB-TACE + placebo (n = 153) | Time to tumor progression | 169 vs. 166 days | p = 0.072 |
| TACE 2 [83] | DEB-TACE + sorafenib (n = 157) vs. DEB-TACE + placebo (n = 156) | PFS (median) | 238.0 vs. 235.0 days | p = 0.94 |
| BRISK-TA [84] | TACE + brivanib (n = 249) vs. TACE + placebo (n = 253) | OS (median) | 26.4 vs. 26.1 months | p = 0.5280 |
| ORIENTAL [85] | TACE+ orantinib (n = 444) vs. TACE + placebo (n = 444) | OS (median) | 31.1 vs. 32.3 months | p = 0.435 |
| TACTICS [86] | TACE+ sorafenib (n = 80) vs. TACE alone (n = 76) | PFS (median) | 25.2 vs. 13.5 months | p = 0.006 |
| RTOG-1112 [93] NCT01730937 | Sorafenib + SBRT (n = 85) vs. sorafenib alone (n = 92) | OS (median) | 15.8 vs. 12.3 months | p = 0.0554 |
| NCT04857684 a | Atezolizumab + bevacizumab + SBRT (n = 20) | Proportion of patients with grade 3–4 treatment-related adverse events | ||
| NCT05096715 b | Atezolizumab + bevacizumab + SBRT (n = 20) | Dose-limiting toxicity rate | ||
| NCT05377034 b | Atezolizumab + bevacizumab + SIRT-Y-90 (n = 88) vs. SIRT-Y-90 + placebo (n = 88) | BORR | ||
| NCT04541173 a | Atezolizumab + bevacizumab + TARE-Y-90 vs. TARE-Y-90 alone (n = 128) | PFS | ||
| NCT04712643 a | Atezolizumab + bevacizumab + TACE vs. TACE alone (n = 342) | TACE PFS OS | ||
| NCT04913480 a | Durvalumab + SBRT (n = 37) | PFS (1 year) | ||
| NCT04167293 a | Sintilimab (n = 58) + SBRT vs. SBRT alone (n = 58) | PFS (24 weeks) | ||
| NCT04387695 a | Sorafenib + SBRT + TACE vs. sorafenib alone (n= 54) | PFS (12 weeks) | ||
| EMERALD-3 NCT05301842 a | Durvalumab + tremelimumab + TACE +/− lenvatinib vs. TACE alone (n = 525) | PFS | ||
| LEAP-012 NCT04246177 a | Lenvatinib + pembrolizumab + TACE vs. TACE + placebo + placebo (n = 950) | PFS OS | ||
| NCT05286320 a | Lenvatinib + pembrolizumab + SBRT (n = 27) | Safety rate ORR | ||
4. Ongoing Clinical Trials
5. Conclusions
Author Contributions
Funding
Conflicts of Interest
References
- Sung, H.; Ferlay, J.; Siegel, R.L.; Laversanne, M.; Soerjomataram, I.; Jemal, A.; Bray, F. Global Cancer Statistics 2020: GLOBOCAN Estimates of Incidence and Mortality Worldwide for 36 Cancers in 185 Countries. CA Cancer J. Clin. 2021, 71, 209–249. [Google Scholar] [CrossRef] [PubMed]
- Soni, P.D.; Palta, M. Stereotactic Body Radiation Therapy for Hepatocellular Carcinoma: Current State and Future Opportunities. Dig. Dis. Sci. 2019, 64, 1008–1015. [Google Scholar] [CrossRef] [PubMed]
- Balogh, J.; Victor, D., 3rd; Asham, E.H.; Burroughs, S.G.; Boktour, M.; Saharia, A.; Li, X.; Ghobrial, R.M.; Monsour, H.P., Jr. Hepatocellular carcinoma: A review. J. Hepatocell. Carcinoma 2016, 3, 41. [Google Scholar] [CrossRef] [PubMed]
- Benson, A.B.; D’Angelica, M.I.; Abbott, D.E.; Anaya, D.A.; Anders, R.; Are, C.; Bachini, M.; Borad, M.; Brown, D.; Burgoyne, A.; et al. Hepatobiliary Cancers, Version 2.2021, NCCN Clinical Practice Guidelines in Oncology. J. Natl. Compr. Canc. Netw. 2021, 19, 541–565. [Google Scholar] [CrossRef]
- Finn, R.S.; Qin, S.; Ikeda, M.; Galle, P.R.; Ducreux, M.; Kim, T.-Y.; Kudo, M.; Breder, V.; Merle, P.; Kaseb, A.O.; et al. Atezolizumab plus Bevacizumab in Unresectable Hepatocellular Carcinoma. N. Engl. J. Med. 2020, 382, 1894–1905. [Google Scholar] [CrossRef]
- Kudo, M.; Finn, R.S.; Qin, S.; Han, K.-H.; Ikeda, K.; Piscaglia, F.; Baron, A.; Park, J.-W.; Han, G.; Jassem, J.; et al. Lenvatinib versus sorafenib in first-line treatment of patients with unresectable hepatocellular carcinoma: A randomised phase 3 non-inferiority trial. Lancet 2018, 391, 1163–1173. [Google Scholar] [CrossRef]
- Abou-Alfa, G.K.; Lau, G.; Kudo, M.; Chan, S.L.; Kelley, R.K.; Furuse, J.; Sukeepaisarnjaroen, W.; Kang, Y.-K.; Van Dao, T.; De Toni, E.N.; et al. Tremelimumab plus Durvalumab in Unresectable Hepatocellular Carcinoma. NEJM Évid. 2022, 1. [Google Scholar] [CrossRef]
- Kim, N.; Cheng, J.; Jung, I.; Der Liang, J.; Shih, Y.L.; Huang, W.-Y.; Kimura, T.; Lee, V.H.; Zeng, Z.C.; Zhenggan, R.; et al. Stereotactic body radiation therapy vs. radiofrequency ablation in Asian patients with hepatocellular carcinoma. J. Hepatol. 2020, 73, 121–129. [Google Scholar] [CrossRef]
- Shen, P.-C.; Chang, W.-C.; Lo, C.-H.; Yang, J.-F.; Lee, M.-S.; Dai, Y.-H.; Lin, C.-S.; Fan, C.-Y.; Huang, W.-Y. Comparison of Stereotactic Body Radiation Therapy and Transarterial Chemoembolization for Unresectable Medium-Sized Hepatocellular Carcinoma. Int. J. Radiat. Oncol. 2019, 105, 307–318. [Google Scholar] [CrossRef]
- Sapir, E.; Tao, Y.; Schipper, M.J.; Bazzi, L.; Novelli, P.M.; Devlin, P.; Owen, D.; Cuneo, K.C.; Lawrence, T.S.; Parikh, N.D.; et al. Stereotactic Body Radiation Therapy as an Alternative to Transarterial Chemoembolization for Hepatocellular Carcinoma. Int. J. Radiat. Oncol. 2017, 100, 122–130. [Google Scholar] [CrossRef]
- European Association for the Study of the Liver. EASL clinical practice guidelines: Management of hepatocellular carcinoma. J. Hepatol. 2018, 69, 182–236. [Google Scholar] [CrossRef] [PubMed]
- Marrero, J.A.; Kulik, L.M.; Sirlin, C.B.; Zhu, A.X.; Finn, R.S.; Abecassis, M.M.; Roberts, L.R.; Heimbach, J.K. Diagnosis, S taging, and M anagement of H epatocellular C arcinoma: 2018 P ractice G uidance by the A merican A ssociation for the S tudy of L iver D iseases. Hepatology 2018, 68, 723–750. [Google Scholar] [CrossRef] [PubMed]
- Curley, S.A.; Izzo, F.; Ellis, L.M.; Vauthey, J.N.; Vallone, P. Radiofrequency Ablation of Hepatocellular Cancer in 110 Patients With Cirrhosis. Ann. Surg. 2000, 232, 381–391. [Google Scholar] [CrossRef] [PubMed]
- Kudo, M. Radiofrequency Ablation for Hepatocellular Carcinoma: Updated Review in 2010. Oncology 2010, 78, 113–124. [Google Scholar] [CrossRef]
- Horvat, N.; de Oliveira, A.I.; de Oliveira, B.C.; Araujo-Filho, J.A.B.; El Homsi, M.; Elsakka, A.; Bajwa, R.; Martins, G.L.P.; Elsayes, K.M.; Menezes, M.R. Local-Regional Treatment of Hepatocellular Carcinoma: A Primer for Radiologists. Radiographics 2022, 42, 1670–1689. [Google Scholar] [CrossRef] [PubMed]
- Laimer; Schullian, P.; Bale, R. Stereotactic Thermal Ablation of Liver Tumors: 3D Planning, Multiple Needle Approach, and Intraprocedural Image Fusion Are the Key to Success-A Narrative Review. Biology 2021, 10, 644. [Google Scholar] [CrossRef]
- Schullian, P.; Johnston, E.W.; Putzer, D.; Eberle, G.; Laimer, G.; Bale, R. Stereotactic radiofrequency ablation of subcardiac hepatocellular carcinoma: A case-control study. Int. J. Hyperth. 2019, 36, 875–884. [Google Scholar] [CrossRef]
- Hu, K.-Q. Advances in Clinical Application of Cryoablation Therapy for Hepatocellular Carcinoma and Metastatic Liver Tumor. J. Clin. Gastroenterol. 2014, 48, 830–836. [Google Scholar] [CrossRef]
- Llovet, J.M.; De Baere, T.; Kulik, L.; Haber, P.K.; Greten, T.F.; Meyer, T.; Lencioni, R. Locoregional therapies in the era of molecular and immune treatments for hepatocellular carcinoma. Nat. Rev. Gastroenterol. Hepatol. 2021, 18, 293–313. [Google Scholar] [CrossRef]
- Chen, L.; Ren, Y.; Sun, T.; Cao, Y.; Yan, L.; Zhang, W.; Ouyang, T.; Zheng, C. The efficacy of radiofrequency ablation versus cryoablation in the treatment of single hepatocellular carcinoma: A population-based study. Cancer Med. 2021, 10, 3715–3725. [Google Scholar] [CrossRef]
- Wang, C.; Wang, H.; Yang, W.; Hu, K.; Xie, H.; Hu, K.; Bai, W.; Dong, Z.; Lu, Y.; Zeng, Z.; et al. Multicenter randomized controlled trial of percutaneous cryoablation versus radiofrequency ablation in hepatocellular carcinoma. Hepatology 2015, 61, 1579–1590. [Google Scholar] [CrossRef] [PubMed]
- Yang, Y.; Zhang, Y.; Wu, Y.; Chen, J.; Liang, B.; Chen, Q.; Wang, Q.; Lyu, J.; Li, Y.; Mu, F.; et al. Efficacy and Safety of Percutaneous Argon-Helium Cryoablation for Hepatocellular Carcinoma Abutting the Diaphragm. J. Vasc. Interv. Radiol. 2020, 31, 393–400. [Google Scholar] [CrossRef]
- Liang, P.; Wang, Y. Microwave ablation of hepatocellular carcinoma. Oncology 2007, 72 (Suppl. 1), 124–131. [Google Scholar] [CrossRef] [PubMed]
- Tan, W.; Deng, Q.; Lin, S.; Wang, Y.; Xu, G. Comparison of microwave ablation and radiofrequency ablation for hepatocellular carcinoma: A systematic review and meta-analysis. Int. J. Hyperth. 2019, 36, 263–271. [Google Scholar] [CrossRef] [PubMed]
- Shen, Q.; Wang, N.; Wu, P.P.; Tan, B.B.; Qian, G.J. Comparison of percutaneous microwave ablation with radiofrequency ablation for hepatocellular carcinoma adjacent to major vessels: A retrospective study. J. Cancer Res. Ther. 2022, 18, 329–335. [Google Scholar]
- Ding, J.; Jing, X.; Liu, J.; Wang, Y.; Wang, F.; Du, Z. Complications of thermal ablation of hepatic tumours: Comparison of radiofrequency and microwave ablative techniques. Clin. Radiol. 2013, 68, 608–615. [Google Scholar] [CrossRef] [PubMed]
- Livraghi, T.; Giorgio, A.; Marin, G.; Salmi, A.; De Sio, I.; Bolondi, L.; Pompili, M.; Brunello, F.; Lazzaroni, S.; Torzilli, G. Hepatocellular carcinoma and cirrhosis in 746 patients: Long-term results of percutaneous ethanol injection. Radiology 1995, 197, 101–108. [Google Scholar] [CrossRef]
- Orlando, A.; Leandro, G.; Olivo, M.; Andriulli, A.; Cottone, M. Radiofrequency Thermal Ablation vs. Percutaneous Ethanol Injection for Small Hepatocellular Carcinoma in Cirrhosis: Meta-Analysis of Randomized Controlled Trials. Am. J. Gastroenterol. 2009, 104, 514–524. [Google Scholar] [CrossRef]
- Giorgio, A.; Di Sarno, A.; De Stefano, G.; Scognamiglio, U.; Farella, N.; Mariniello, A.; Esposito, V.; Coppola, C.; Giorgio, V. Percutaneous radiofrequency ablation of hepatocellular carcinoma compared to percutaneous ethanol injection in treatment of cirrhotic patients: An Italian randomized controlled trial. Anticancer. Res. 2011, 31, 2291–2295. [Google Scholar]
- Yang, P.; Li, N. Efficacy of percutaneous ethanol injection versus radiofrequency ablation for single hepatocellular carcinoma no larger than 5 cm. J. Int. Med. Res. 2022, 50, 1–12. [Google Scholar] [CrossRef]
- Reig, M.; Forner, A.; Rimola, J.; Ferrer-Fàbrega, J.; Burrel, M.; Garcia-Criado, Á.; Kelley, R.K.; Galle, P.R.; Mazzaferro, V.; Salem, R.; et al. BCLC strategy for prognosis prediction and treatment recommendation Barcelona Clinic Liver Cancer (BCLC) staging system: The 2022 update. J. Hepatol. 2021, 76, 681–693. [Google Scholar] [CrossRef] [PubMed]
- Imai, N. Transarterial chemoembolization for hepatocellular carcinoma: A review of techniques. World J. Hepatol. 2014, 6, 844–850. [Google Scholar] [CrossRef] [PubMed]
- Forner, A.; Gilabert, M.; Bruix, J.; Raoul, J.-L. Treatment of intermediate-stage hepatocellular carcinoma. Nat. Rev. Clin. Oncol. 2014, 11, 525–535. [Google Scholar] [CrossRef]
- Lammer, J.; Malagari, K.; Vogl, T.; Pilleul, F.; Denys, A.; Watkinson, A.; Pitton, M.; Sergent, G.; Pfammatter, T.; Terraz, S.; et al. Prospective Randomized Study of Doxorubicin-Eluting-Bead Embolization in the Treatment of Hepatocellular Carcinoma: Results of the PRECISION V Study. Cardiovasc. Interv. Radiol. 2010, 33, 41–52. [Google Scholar] [CrossRef] [PubMed]
- Wang, E.A.; Stein, J.P.; Bellavia, R.J.; Broadwell, S.R. Treatment options for unresectable HCC with a focus on SIRT with Yttrium-90 resin microspheres. Int. J. Clin. Pract. 2017, 71, e12972. [Google Scholar] [CrossRef] [PubMed]
- Chang, Y.; Jeong, S.W.; Jang, J.Y.; Kim, Y.J. Recent Updates of Transarterial Chemoembolilzation in Hepatocellular Carcinoma. Int. J. Mol. Sci. 2020, 21, 8165. [Google Scholar] [CrossRef]
- Raoul, J.-L.; Forner, A.; Bolondi, L.; Cheung, T.T.; Kloeckner, R.; de Baere, T. Updated use of TACE for hepatocellular carcinoma treatment: How and when to use it based on clinical evidence. Cancer Treat. Rev. 2018, 72, 28–36. [Google Scholar] [CrossRef]
- Brown, K.T.; Do, R.K.; Gonen, M.; Covey, A.M.; Getrajdman, G.I.; Sofocleous, C.T.; Jarnagin, W.R.; D’Angelica, M.I.; Allen, P.J.; Erinjeri, J.P.; et al. Randomized Trial of Hepatic Artery Embolization for Hepatocellular Carcinoma Using Doxorubicin-Eluting Microspheres Compared With Embolization With Microspheres Alone. J. Clin. Oncol. 2016, 34, 2046–2053. [Google Scholar] [CrossRef]
- Guo, J.; Wang, W.; Zhang, Y.; Xu, L.; Kong, J. Comparison of initial tumor responses to transarterial bland embolization and drug-eluting beads-transarterial chemoembolization in the management of hepatocellular carcinoma: A propensity-score matching analysis. J. Gastrointest. Oncol. 2021, 12, 1838–1850. [Google Scholar] [CrossRef]
- Vilgrain, V.; Pereira, H.; Assenat, E.; Guiu, B.; Ilonca, A.D.; Pageaux, G.-P.; Sibert, A.; Bouattour, M.; Lebtahi, R.; Allaham, W.; et al. Efficacy and safety of selective internal radiotherapy with yttrium-90 resin microspheres compared with sorafenib in locally advanced and inoperable hepatocellular carcinoma (SARAH): An open-label randomised controlled phase 3 trial. Lancet Oncol. 2017, 18, 1624–1636. [Google Scholar] [CrossRef]
- Sangro, B.; Carpanese, L.; Cianni, R.; Golfieri, R.; Gasparini, D.; Ezziddin, S.; Paprottka, P.M.; Fiore, F.; Van Buskirk, M.; Bilbao, J.I.; et al. Survival after yttrium-90 resin microsphere radioembolization of hepatocellular carcinoma across Barcelona clinic liver cancer stages: A European evaluation. Hepatology 2011, 54, 868–878. [Google Scholar] [CrossRef] [PubMed]
- Brown, A.M.; Kassab, I.; Massani, M.; Townsend, W.; Singal, A.G.; Soydal, C.; Moreno-Luna, L.; Roberts, L.R.; Chen, V.L.; Parikh, N.D. TACE versus TARE for patients with hepatocellular carcinoma: Overall and individual patient level meta analysis. Cancer Med. 2022, 12, 2590–2599. [Google Scholar] [CrossRef] [PubMed]
- Chow, P.K.; Gandhi, M.; Tan, S.-B.; Khin, M.W.; Khasbazar, A.; Ong, J.; Choo, S.P.; Cheow, P.C.; Chotipanich, C.; Lim, K.; et al. SIRveNIB: Selective Internal Radiation Therapy Versus Sorafenib in Asia-Pacific Patients With Hepatocellular Carcinoma. J. Clin. Oncol. 2018, 36, 1913–1921. [Google Scholar] [CrossRef]
- Ricke, J.; Klümpen, H.J.; Amthauer, H.; Bargellini, I.; Bartenstein, P.; de Toni, E.N.; Gasbarrini, A.; Pech, M.; Peck-Radosavljevic, M.; Popovič, P.; et al. Impact of combined selective internal radiation therapy and sorafenib on survival in advanced hepatocellular carcinoma. J. Hepatol. 2019, 71, 1164–1174. [Google Scholar] [CrossRef]
- Wasan, H.S.; Gibbs, P.; Sharma, N.K.; Taieb, J.; Heinemann, V.; Ricke, J.; Peeters, M.; Findlay, M.; Weaver, A.; Mills, J.; et al. First-line selective internal radiotherapy plus chemotherapy versus chemotherapy alone in patients with liver metastases from colorectal cancer (FOXFIRE, SIRFLOX, and FOXFIRE-Global): A combined analysis of three multicentre, randomised, phase 3 trials. Lancet Oncol. 2017, 18, 1159–1171. [Google Scholar] [CrossRef] [PubMed]
- Kennedy, A.S.; Nutting, C.; Coldwell, D.; Gaiser, J.; Drachenberg, C. Pathologic response and microdosimetry of 90Y microspheres in man: Review of four explanted whole livers. Int. J. Radiat. Oncol. 2004, 60, 1552–1563. [Google Scholar] [CrossRef] [PubMed]
- Jackson, S.P.; Bartek, J. The DNA-damage response in human biology and disease. Nature 2009, 461, 1071–1078. [Google Scholar] [CrossRef]
- Kouloulias, V.; Mosa, E.; Georgakopoulos, I.; Platoni, K.; Brountzos, I.; Zygogianni, A.; Antypas, C.; Kosmidis, P.; Mystakidou, K.; Tolia, M.; et al. Three-Dimensional Conformal Radiotherapy for Hepatocellular Carcinoma in Patients Unfit for Resection, Ablation, or Chemotherapy: A Retrospective Study. Sci. World J. 2013, 2013, 780141. [Google Scholar] [CrossRef]
- Riou, O.; Moscardo, C.L.; Fenoglietto, P.; Deshayes, E.; Tetreau, R.; Molinier, J.; Lenglet, A.; Assenat, E.; Ychou, M.; Guiu, B.; et al. SBRT planning for liver metastases: A focus on immobilization, motion management and planning imaging techniques. Rep. Pract. Oncol. Radiother. 2017, 22, 103–110. [Google Scholar] [CrossRef]
- Lee, J.H.; Kim, N.H.; Ki, Y.K.; Nam, J.H.; Heo, J.; Woo, H.Y.; Kim, D.W.; Kim, W.T. Three-dimensional conformal radiotherapy for portal vein tumor thrombosis alone in advanced hepatocellular carcinoma. Radiat. Oncol. J. 2014, 32, 170–178. [Google Scholar] [CrossRef]
- Merle, P.; Mornex, F.; Trepo, C. Innovative therapy for hepatocellular carcinoma: Three-dimensional high-dose photon radiotherapy. Cancer Lett. 2009, 286, 129–133. [Google Scholar] [CrossRef]
- Su, F.; Chen, K.; Liang, Z.; Qu, S.; Li, L.; Chen, L.; Yang, Y.; Wu, C.; Liang, X.; Zhu, X. Survival benefit of higher fraction dose delivered by three-dimensional conformal radiotherapy in hepatocellular carcinoma smaller than 10 cm in size. Cancer Manag. Res. 2019, 11, 3791–3799. [Google Scholar] [CrossRef] [PubMed]
- Bae, S.H.; Jang, W.I.; Park, H.C. Intensity-modulated radiotherapy for hepatocellular carcinoma: Dosimetric and clinical results. Oncotarget 2017, 8, 59965–59976. [Google Scholar] [CrossRef] [PubMed]
- Galvin, J.M.; De Neve, W. Intensity Modulating and Other Radiation Therapy Devices for Dose Painting. J. Clin. Oncol. 2007, 25, 924–930. [Google Scholar] [CrossRef] [PubMed]
- Pyakuryal, A.; Pandit, S.; Narayanasamy, G.; Jang, S.; Lee, S.; Sio, T. Radio-Biologic Evaluation of Simultaneously Integrated Boost (SIB) IMRT Methods in Head and Neck Cancer: Multi-Institutional Study. Int. J. Radiat. Oncol. 2014, 90, S789–S790. [Google Scholar] [CrossRef]
- Nakamura, K.; Sasaki, T.; Ohga, S.; Yoshitake, T.; Terashima, K.; Asai, K.; Matsumoto, K.; Shioyama, Y.; Honda, H. Recent advances in radiation oncology: Intensity-modulated radiotherapy, a clinical perspective. Int. J. Clin. Oncol. 2014, 19, 564–569. [Google Scholar] [CrossRef]
- Manikandan, A.; Sarkar, B.; Holla, R.; Vivek, T.R.; Sujatha, N. Quality assurance of dynamic parameters in volumetric modulated arc therapy. Br. J. Radiol. 2012, 85, 1002–1010. [Google Scholar] [CrossRef] [PubMed]
- Teoh, M.; Clark, C.; Wood, K.; Whitaker, S.; Nisbet, A. Volumetric modulated arc therapy: A review of current literature and clinical use in practice. Br. J. Radiol. 2011, 84, 967–996. [Google Scholar] [CrossRef]
- Yoon, H.I.; Lee, I.J.; Han, K.-H.; Seong, J. Improved oncologic outcomes with image-guided intensity-modulated radiation therapy using helical tomotherapy in locally advanced hepatocellular carcinoma. J. Cancer Res. Clin. Oncol. 2014, 140, 1595–1605. [Google Scholar] [CrossRef]
- Ling, T.C.; Kang, J.I.; Bush, D.A.; Slater, J.D.; Yang, G.Y. Proton therapy for hepatocellular carcinoma. Chin. J. Cancer Res. 2012, 24, 361–367. [Google Scholar] [CrossRef][Green Version]
- Colbert, L.E.; Cloyd, J.M.; Koay, E.J.; Crane, C.H.; Vauthey, J.-N. Proton beam radiation as salvage therapy for bilateral colorectal liver metastases not amenable to second-stage hepatectomy. Surgery 2017, 161, 1543–1548. [Google Scholar] [CrossRef] [PubMed]
- Hong, T.S.; Wo, J.Y.; Yeap, B.Y.; Ben-Josef, E.; McDonnell, E.I.; Blaszkowsky, L.S.; Kwak, E.L.; Allen, J.N.; Clark, J.W.; Goyal, L.; et al. Multi-Institutional Phase II Study of High-Dose Hypofractionated Proton Beam Therapy in Patients with Localized, Unresectable Hepatocellular Carcinoma and Intrahepatic Cholangiocarcinoma. J. Clin. Oncol. 2016, 34, 460–468. [Google Scholar] [CrossRef] [PubMed]
- Bush, D.A.; Smith, J.C.; Slater, J.D.; Volk, M.L.; Reeves, M.E.; Cheng, J.; Grove, R.; de Vera, M.E. Randomized Clinical Trial Comparing Proton Beam Radiation Therapy with Transarterial Chemoembolization for Hepatocellular Carcinoma: Results of an Interim Analysis. Int. J. Radiat. Oncol. Biol. Phys. 2016, 95, 477–482. [Google Scholar] [CrossRef] [PubMed]
- Kim, T.H.; Koh, Y.H.; Kim, B.H.; Kim, M.J.; Lee, J.H.; Park, B.; Park, J.-W. Proton beam radiotherapy vs. radiofrequency ablation for recurrent hepatocellular carcinoma: A randomized phase III trial. J. Hepatol. 2020, 74, 603–612. [Google Scholar] [CrossRef]
- Kim, J.Y.; Lim, Y.K.; Kim, T.H.; Cho, K.H.; Choi, S.H.; Jeong, H.; Kim, D.W.; Park, J.H.; Shin, D.H.; Lee, S.B.; et al. Normal liver sparing by proton beam therapy for hepatocellular carcinoma: Comparison with helical intensity modulated radiotherapy and volumetric modulated arc therapy. Acta Oncol. 2015, 54, 1827–1832. [Google Scholar] [CrossRef] [PubMed]
- Sanford, N.N.; Pursley, J.; Noe, B.; Yeap, B.Y.; Goyal, L.; Clark, J.W.; Allen, J.N.; Blaszkowsky, L.S.; Ryan, D.P.; Ferrone, C.R.; et al. Protons versus Photons for Unresectable Hepatocellular Carcinoma: Liver Decompensation and Overall Survival. Int. J. Radiat. Oncol. 2019, 105, 64–72. [Google Scholar] [CrossRef]
- Narayanasamy, G.; Desai, D.; Maraboyina, S.; Penagaricano, J.; Zwicker, R.; Johnson, E.L. A dose falloff gradient study in RapidArc planning of lung stereotactic body radiation therapy. J. Med. Phys. 2018, 43, 147–154. [Google Scholar] [CrossRef]
- Kimura, T.; Doi, Y.; Takahashi, S.; Kubo, K.; Imano, N.; Takeuchi, Y.; Takahashi, I.; Nishibuchi, I.; Murakami, Y.; Kenjo, M.; et al. An overview of stereotactic body radiation therapy for hepatocellular carcinoma. Expert Rev. Gastroenterol. Hepatol. 2020, 14, 271–279. [Google Scholar] [CrossRef]
- Wang, P.-M.; Hsu, W.-C.; Chung, N.-N.; Chang, F.-L.; Jang, C.-J.; Fogliata, A.; Scorsetti, M.; Cozzi, L. Feasibility of stereotactic body radiation therapy with volumetric modulated arc therapy and high intensity photon beams for hepatocellular carcinoma patients. Radiat. Oncol. 2014, 9, 18. [Google Scholar] [CrossRef]
- Oldrini, G.; Taste-George, H.; Renard-Oldrini, S.; Baumann, A.-S.; Marchesi, V.; Troufléau, P.; Peiffert, D.; Didot-Moisei, A.; Boyer, B.; Grignon, B.; et al. Implantation of fiducial markers in the liver for stereotactic body radiation therapy: Feasibility and results. Diagn. Interv. Imaging 2015, 96, 589–592. [Google Scholar] [CrossRef]
- Heifferon, N. Triggered Imaging and Auto Beam Hold: Enhancing Lung SBRT; Varian: Palo Alto, CA, USA, 2018. [Google Scholar]
- Yu, J.B.; Cramer, L.D.; Herrin, J.; Soulos, P.R.; Potosky, A.L.; Gross, C.P. Stereotactic Body Radiation Therapy Versus Intensity-Modulated Radiation Therapy for Prostate Cancer: Comparison of Toxicity. J. Clin. Oncol. 2014, 32, 1195–1201. [Google Scholar] [CrossRef] [PubMed]
- Hilal, L.; Reyngold, M.; Wu, A.J.; Araji, A.; Abou-Alfa, G.K.; Jarnagin, W.; Harding, J.J.; Gambarin, M.; El Dika, I.; Brady, P.; et al. Ablative radiation therapy for hepatocellular carcinoma is associated with reduced treatment- and tumor-related liver failure and improved survival. J. Gastrointest. Oncol. 2021, 12, 1743–1752. [Google Scholar] [CrossRef] [PubMed]
- Tao, R.; Krishnan, S.; Bhosale, P.R.; Javle, M.M.; Aloia, T.A.; Shroff, R.T.; Kaseb, A.O.; Bishop, A.; Swanick, C.W.; Koay, E.J.; et al. Ablative Radiotherapy Doses Lead to a Substantial Prolongation of Survival in Patients With Inoperable Intrahepatic Cholangiocarcinoma: A Retrospective Dose Response Analysis. J. Clin. Oncol. 2016, 34, 219–226. [Google Scholar] [CrossRef] [PubMed]
- Crane, C.H.; Koay, E.J. Solutions that enable ablative radiotherapy for large liver tumors: Fractionated dose painting, simultaneous integrated protection, motion management, and computed tomography image guidance. Cancer 2016, 122, 1974–1986. [Google Scholar] [CrossRef]
- Li, L.-Q.; Zhou, Y.; Huang, Y.; Liang, P.; Liang, S.-X.; Su, T.-S. Stereotactic body radiotherapy versus intensity-modulated radiotherapy for hepatocellular carcinoma with portal vein tumor thrombosis. Hepatol. Int. 2021, 15, 630–641. [Google Scholar] [CrossRef] [PubMed]
- Lee, D.; Sohn, J.; Kirichenko, A. Quantifying Liver Heterogeneity via R2*-MRI with Super-Paramagnetic Iron Oxide Nanoparticles (SPION) to Characterize Liver Function and Tumor. Cancers 2022, 14, 5269. [Google Scholar] [CrossRef]
- Mannina, E.M.; Cardenes, H.R.; Lasley, F.D.; Goodman, B.; Zook, J.; Althouse, S.; Cox, J.A.; Saxena, R.; Tector, J.; Maluccio, M. Role of Stereotactic Body Radiation Therapy Before Orthotopic Liver Transplantation: Retrospective Evaluation of Pathologic Response and Outcomes. Int. J. Radiat. Oncol. 2017, 97, 931–938. [Google Scholar] [CrossRef]
- Berretta, M.; Rinaldi, L.; Di Benedetto, F.; Lleshi, A.; De Re, V.; Facchini, G.; De Paoli, P.; Di Francia, R. Angiogenesis Inhibitors for the Treatment of Hepatocellular Carcinoma. Front. Pharmacol. 2016, 7, 428. [Google Scholar] [CrossRef]
- Pardoll, D.M. The blockade of immune checkpoints in cancer immunotherapy. Nat. Rev. Cancer 2012, 12, 252–264. [Google Scholar] [CrossRef]
- Finn, R.S.; Kudo, M.; Merle, P.; Meyer, T.; Qin, S.; Ikeda, M.; Xu, R.; Edeline, J.; Ryoo, B.-Y.; Ren, Z.; et al. Llovet. LBA34—Primary Results from the Phase III LEAP-002 Study: Lenvatinib Plus Pembrolizumab versus Lenvatinib as First-Line (1L) Therapy for Advanced Hepatocellular Carcinoma (aHCC). 2022. Available online: https://oncologypro.esmo.org/meeting-resources/esmo-congress/primary-results-from-the-phase-iii-leap-002-study-lenvatinib-plus-pembrolizumab-versus-lenvatinib-as-first-line-1l-therapy-for-advanced-hepatoce (accessed on 25 September 2022).
- Lencioni, R.; Llovet, J.M.; Han, G.; Tak, W.Y.; Yang, J.; Guglielmi, A.; Paik, S.W.; Reig, M.; Kim, D.Y.; Chau, G.-Y.; et al. Sorafenib or placebo plus TACE with doxorubicin-eluting beads for intermediate stage HCC: The SPACE trial. J. Hepatol. 2016, 64, 1090–1098. [Google Scholar] [CrossRef]
- Meyer, T.; Fox, R.; Ma, Y.T.; Ross, P.J.; James, M.W.; Sturgess, R.; Stubbs, C.; Stocken, D.D.; Wall, L.; Watkinson, A.; et al. Sorafenib in combination with transarterial chemoembolisation in patients with unresectable hepatocellular carcinoma (TACE 2): A randomised placebo-controlled, double-blind, phase 3 trial. Lancet Gastroenterol. Hepatol. 2017, 2, 565–575. [Google Scholar] [CrossRef] [PubMed]
- Kudo, M.; Han, G.; Finn, R.S.; Poon, R.T.P.; Blanc, J.-F.; Yan, L.; Yang, J.; Lu, L.; Tak, W.Y.; Yu, X.; et al. Brivanib as adjuvant therapy to transarterial chemoembolization in patients with hepatocellular carcinoma: A randomized phase III trial. Hepatology 2014, 60, 1697–1707. [Google Scholar] [CrossRef] [PubMed]
- Kudo, M.; Cheng, A.-L.; Park, J.-W.; Park, J.H.; Liang, P.-C.; Hidaka, H.; Izumi, N.; Heo, J.; Lee, Y.J.; Sheen, I.-S.; et al. Orantinib versus placebo combined with transcatheter arterial chemoembolisation in patients with unresectable hepatocellular carcinoma (ORIENTAL): A randomised, double-blind, placebo-controlled, multicentre, phase 3 study. Lancet Gastroenterol. Hepatol. 2017, 3, 37–46. [Google Scholar] [CrossRef] [PubMed]
- Kudo, M.; Ueshima, K.; Ikeda, M.; Torimura, T.; Tanabe, N.; Aikata, H.; Izumi, N.; Yamasaki, T.; Nojiri, S.; Hino, K.; et al. Randomised, multicentre prospective trial of transarterial chemoembolisation (TACE) plus sorafenib as compared with TACE alone in patients with hepatocellular carcinoma: TACTICS trial. Gut 2019, 69, 1492–1501. [Google Scholar] [CrossRef] [PubMed]
- Duffy, A.G.; Ulahannan, S.V.; Makorova-Rusher, O.; Rahma, O.; Wedemeyer, H.; Pratt, D.; Davis, J.L.; Hughes, M.S.; Heller, T.; ElGindi, M.; et al. Tremelimumab in combination with ablation in patients with advanced hepatocellular carcinoma. J. Hepatol. 2016, 66, 545–551. [Google Scholar] [CrossRef]
- Harding, J.J.; Yarmohammadi, H.; Reiss, K.A.; Chou, J.F.; Capanu, M.; Do, R.K.G.; Khalil, D.; El Dika, I.H.; Ferrer, C.S.; Heffernan, O.; et al. Nivolumab (NIVO) and drug eluting bead transarterial chemoembolization (deb-TACE): Updated results from an ongoing phase 1 study of patients (pts) with liver limited hepatocellular carcinoma (HCC). J. Clin. Oncol. 2022, 40, 437. [Google Scholar] [CrossRef]
- Liu, B.; Zhang, Y.; Chen, H.; Li, W.; Tsochatzis, E. The combination of transcatheter arterial chemoembolisation (TACE) and thermal ablation versus TACE alone for hepatocellular carcinoma. Cochrane Database Syst. Rev. 2022, 1. [Google Scholar] [CrossRef]
- Jun, B.; Kim, S.G.; Kim, Y.D.; Cheon, G.J.; Han, K.H.; Yoo, J.-J.; Jeong, S.W.; Jang, J.Y.; Lee, S.H.; Park, S.; et al. Combined therapy of transarterial chemoembolization and stereotactic body radiation therapy versus transarterial chemoembolization for ≤5cm hepatocellular carcinoma: Propensity score matching analysis. PLoS ONE 2018, 13, e0206381. [Google Scholar] [CrossRef]
- Su, T.-S.; Lu, H.-Z.; Cheng, T.; Zhou, Y.; Huang, Y.; Gao, Y.-C.; Tang, M.-Y.; Jiang, H.-Y.; Lian, Z.-P.; Hou, E.-C.; et al. Long-term survival analysis in combined transarterial embolization and stereotactic body radiation therapy versus stereotactic body radiation monotherapy for unresectable hepatocellular carcinoma >5 cm. BMC Cancer 2016, 16, 834. [Google Scholar] [CrossRef]
- Shen, L.; Xi, M.; Zhao, L.; Zhang, X.; Wang, X.; Huang, Z.; Chen, Q.; Zhang, T.; Shen, J.; Liu, M.; et al. Combination Therapy after TACE for Hepatocellular Carcinoma with Macroscopic Vascular Invasion: Stereotactic Body Radiotherapy versus Sorafenib. Cancers 2018, 10, 516. [Google Scholar] [CrossRef]
- Dawson, L.; Winter, K.; Knox, J.; Zhu, A.; Krishnan, S.; Guha, C.; Kachnic, L.; Gillin, M.; Hong, T.; Craig, T.; et al. NRG/RTOG 1112: Randomized Phase III Study of Sorafenib vs. Stereotactic Body Radiation Therapy (SBRT) Followed by Sorafenib in Hepatocellular Carcinoma (HCC) (NCT01730937). Int. J. Radiat. Oncol. 2022, 114, 1057. [Google Scholar] [CrossRef]
- Conroy, R. Sorafenib Plus SBRT Yields Improved Survival vs Sorafenib Alone in Locally Advanced HCC; Cancer Network: Cranbury, NJ, USA, 2022. [Google Scholar]
- Meng, M.; Li, W.; Yang, X.; Huang, G.; Wei, Z.; Ni, Y.; Han, X.; Wang, J.; Ye, X. Transarterial chemoembolization, ablation, tyrosine kinase inhibitors, and immunotherapy (TATI): A novel treatment for patients with advanced hepatocellular carcinoma. J. Cancer Res. Ther. 2020, 16, 327–334. [Google Scholar] [CrossRef] [PubMed]
- Golfieri, R.; Giampalma, E.; Renzulli, M.; Cioni, R.; Bargellini, I.; Bartolozzi, C.; Breatta, A.D.; Gandini, G.; Nani, R.; et al.; on behalf of the Precision Italia Study Group Randomised controlled trial of doxorubicin-eluting beads vs conventional chemoembolisation for hepatocellular carcinoma. Br. J. Cancer 2014, 111, 255–264. [Google Scholar] [CrossRef] [PubMed]
- Pilones, K.A.; Vanpouille-Box, C.; Demaria, S. Combination of Radiotherapy and Immune Checkpoint Inhibitors. Semin. Radiat. Oncol. 2015, 25, 28–33. [Google Scholar] [CrossRef] [PubMed]
| BCLC Stage | Size [31] | Location Contraindications [15] | Presence of PVT [15] | |
|---|---|---|---|---|
| Ablation | A | ≤3 cm | Proximity to major bile ducts, large vessels, intra-abdominal organs and subcapsular regions | No |
| Arterially directed therapies | B | ≤8 cm (for RE) | Extensive bilobar involvement | No (TACE) Yes (RE) |
| Radiation | A or B | no limitation | Extrahepatic disease | Yes |
| Randomized Controlled Trial | Treatment Arms | Primary Endpoint | Outcomes | p-Value |
|---|---|---|---|---|
| SARAH [40] | SIRT-Y-90 (n = 237) vs. sorafenib (n = 222) | OS | 8.0 vs. 9.9 months | p = 0.18 |
| SIRveNIB [43] | SIRT-Y-90 (n = 182) vs. sorafenib (n = 178) | OS | 8.8 vs. 10.0 months | p = 0.36 |
| FOXFIRE, SIRFLOX, FOXFIRE-Global [45] | SIRT-Y-90 + FOLFOX (n = 554) vs. FOLFOX alone (n = 549) | OS | 22.6 vs. 23.3 months | p = 0.61 |
| SORAMIC [44] | SIRT-Y-90 + sorafenib (n = 216) vs. sorafenib (n = 208) | OS | 12.1 vs. 11.4 months | p = 0.9529 |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2023 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Chami, P.; Jarnagin, W.; Abou-Alfa, G.K.; Harding, J.; Kim, N.; Lin, H.; El Homsi, M.; Crane, C.; Hajj, C. Non-Surgical Locoregional Therapies Alone or in Combination with Systemic Therapy in Patients with Hepatocellular Carcinoma. Cancers 2023, 15, 1748. https://doi.org/10.3390/cancers15061748
Chami P, Jarnagin W, Abou-Alfa GK, Harding J, Kim N, Lin H, El Homsi M, Crane C, Hajj C. Non-Surgical Locoregional Therapies Alone or in Combination with Systemic Therapy in Patients with Hepatocellular Carcinoma. Cancers. 2023; 15(6):1748. https://doi.org/10.3390/cancers15061748
Chicago/Turabian StyleChami, Perla, William Jarnagin, Ghassan K. Abou-Alfa, James Harding, Neal Kim, Haibo Lin, Maria El Homsi, Christopher Crane, and Carla Hajj. 2023. "Non-Surgical Locoregional Therapies Alone or in Combination with Systemic Therapy in Patients with Hepatocellular Carcinoma" Cancers 15, no. 6: 1748. https://doi.org/10.3390/cancers15061748
APA StyleChami, P., Jarnagin, W., Abou-Alfa, G. K., Harding, J., Kim, N., Lin, H., El Homsi, M., Crane, C., & Hajj, C. (2023). Non-Surgical Locoregional Therapies Alone or in Combination with Systemic Therapy in Patients with Hepatocellular Carcinoma. Cancers, 15(6), 1748. https://doi.org/10.3390/cancers15061748





