Changes in the Acetylcholinesterase Enzymatic Activity in Tumor Development and Progression
Simple Summary
Abstract
1. Introduction
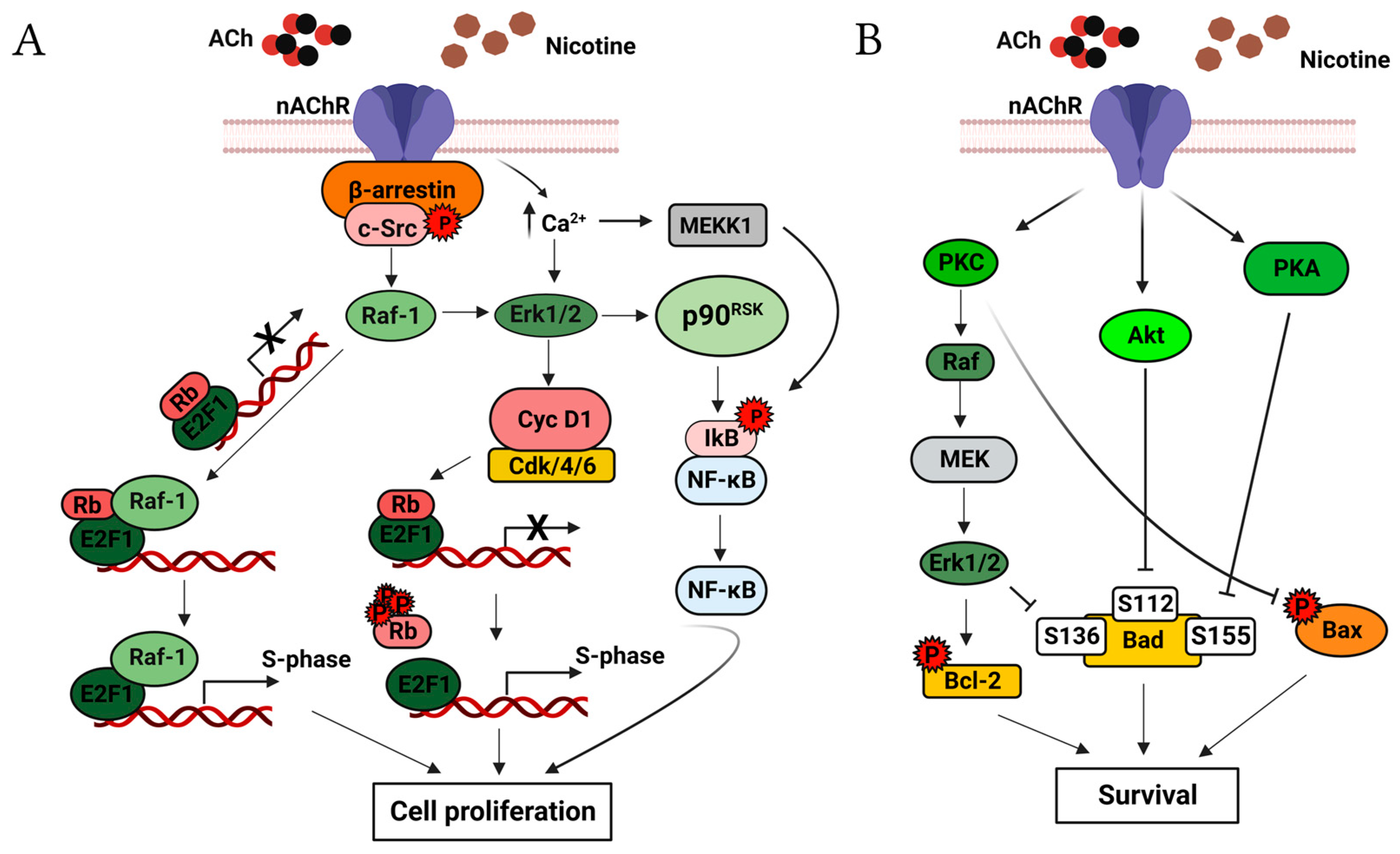
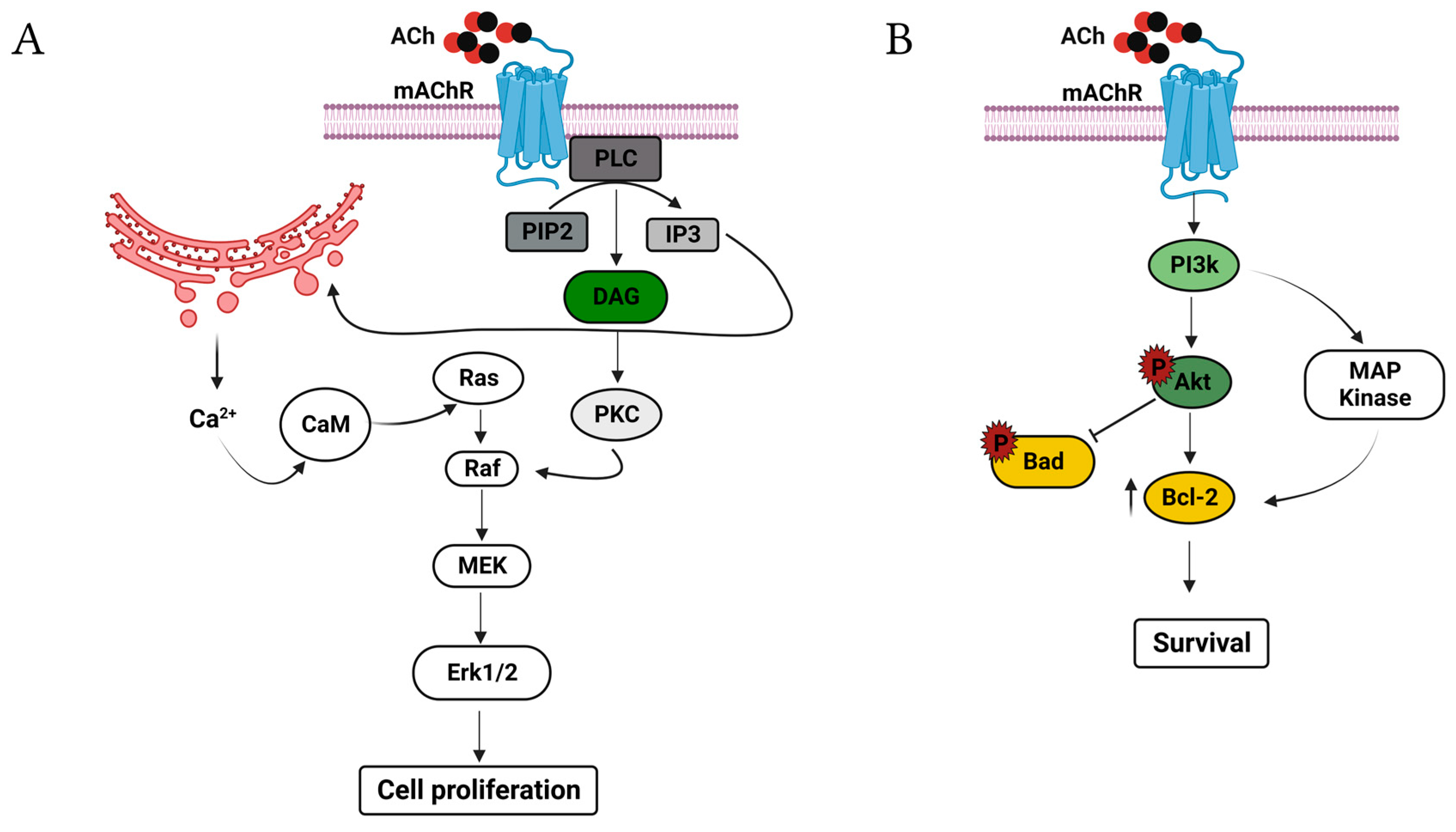
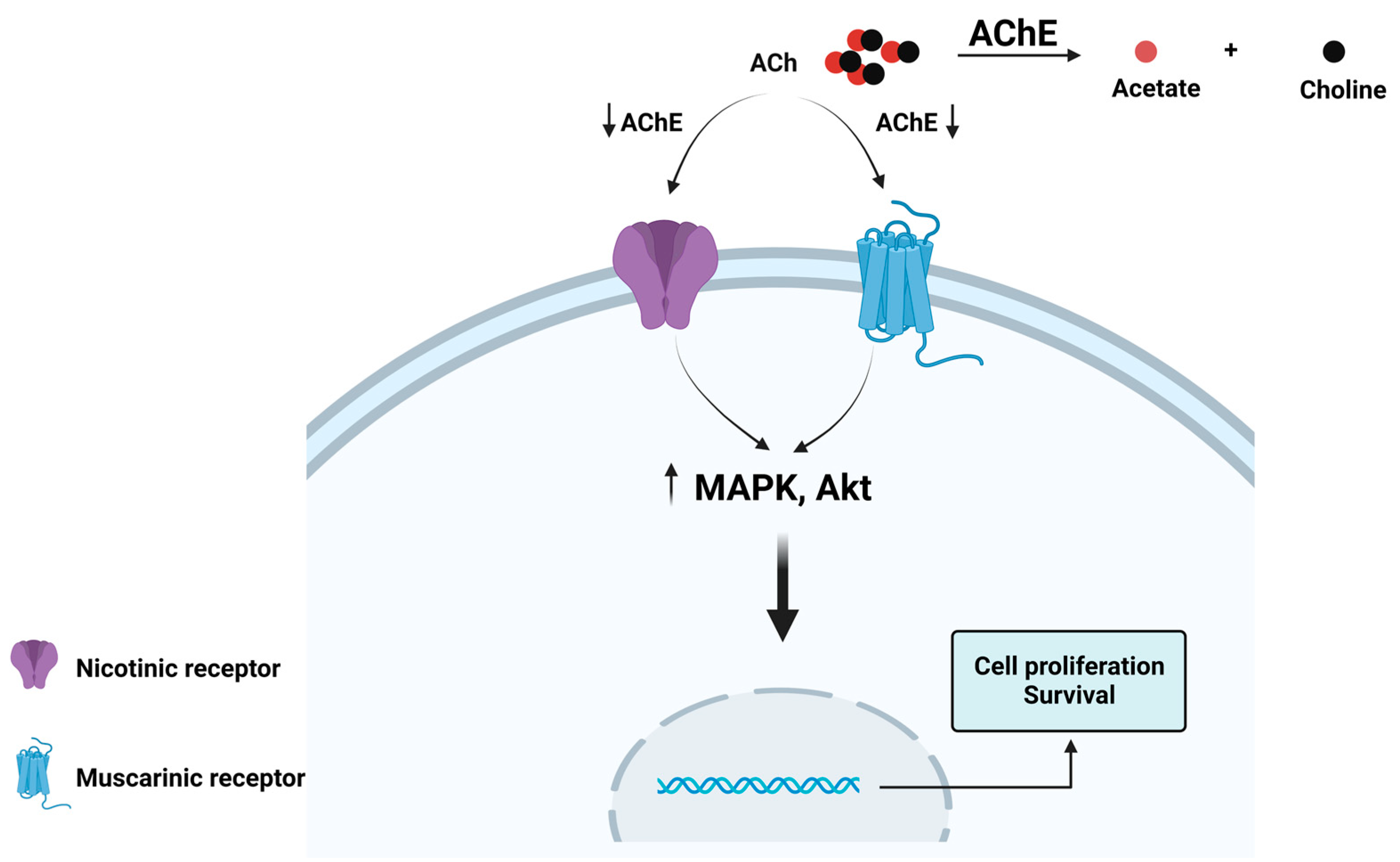
1.1. Acetylcholine as a Cell Proliferation Factor
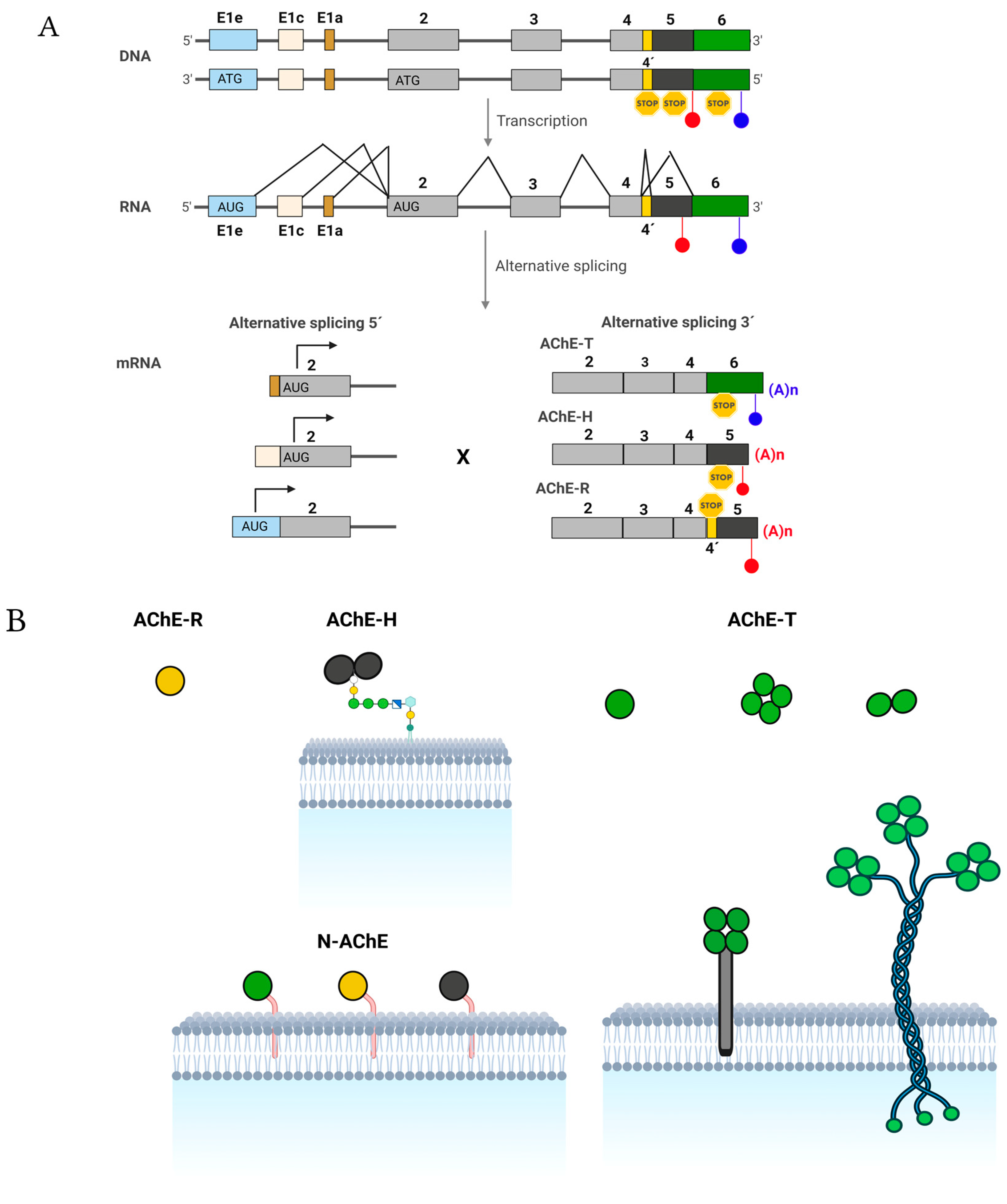
1.2. The Enzyme
2. The Implication of Acetylcholinesterase in Tumor Development
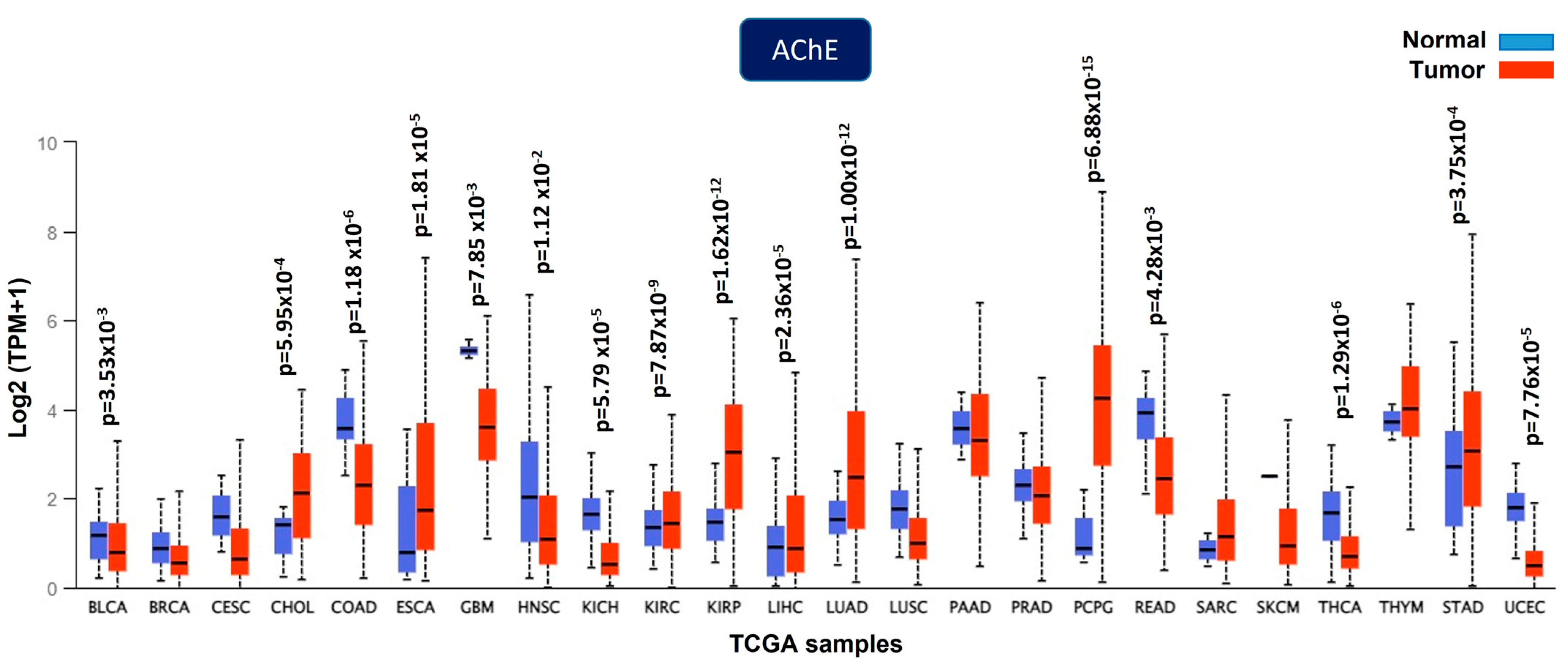
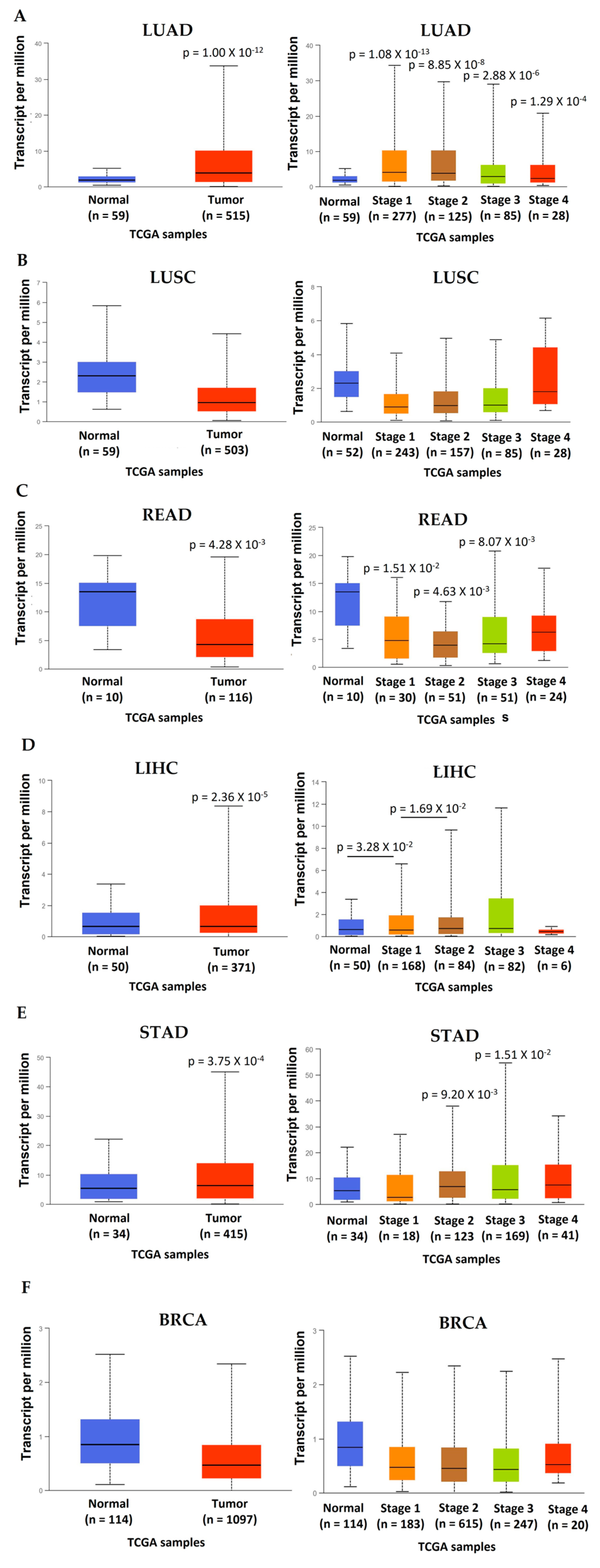
3. Acetylcholinesterase Activity in Tumors
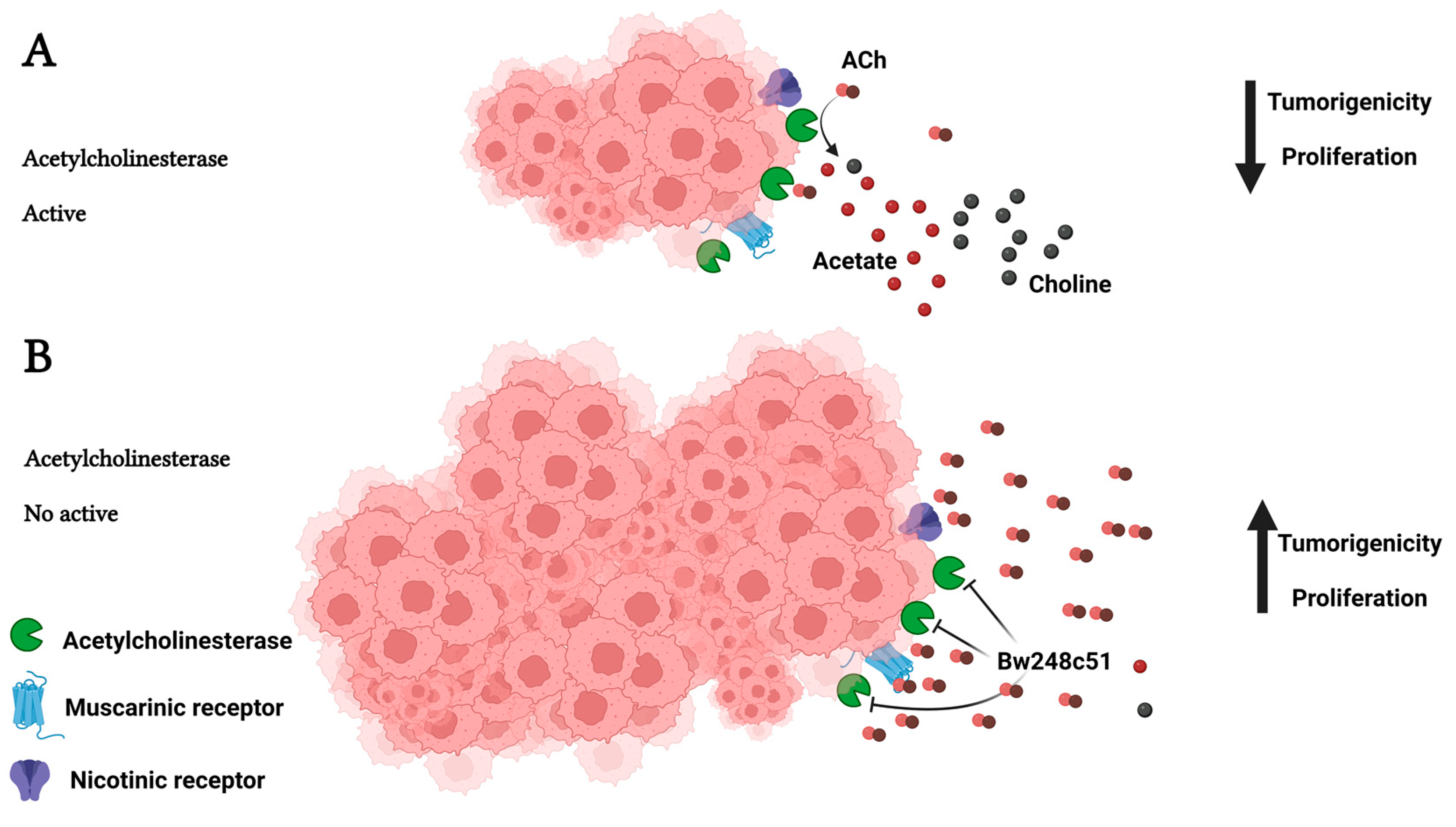
3.1. The Possible Role of Acetylcholinesterase in Tumors with Low Enzymatic Activity
Patterns of AChE Molecular Forms Expressed in Tumors with Low Enzymatic Activity
| Tumor Type | AChE Activity | Molecular Form | Reference(s) |
|---|---|---|---|
| Lung cancer | Low | G1A and G2A | [76,90] |
| High | - | - | |
| Colon cancer | Low | G1A and G2A G2H, G4A, G4H, and A4 (disappeared) | [75] |
| High | - | [119] | |
| Brain tumor | Low | G4 contains butyrylcholinesterase monomers | [91] |
| High | NA | [120] | |
| Liver cancer | Low | NA | [84,92] |
| High | - | - | |
| Gastric cancer | Low | NA | [85] |
| High | - | - | |
| Breast cancer | Low | G1A and G2A & G4H, A4 y A8 (disappeared) & | [93] &, [94] |
| High | G1A (low content) and G2A | [121] | |
| Head and neck carcinoma | Low | G1A and G2A (no enzymatic change) G4A (disappeared) | [86,87] |
| High | - | - | |
| Renal cancer | Low | - | - |
| High | G1A (no change) and G2A (high activity) | [77,122] | |
| Pancreatic cancer | Low | - | - |
| High | NA | [123] |
3.2. Enhanced Enzymatic Acetylcholinesterase Activity in Tumors
3.2.1. The Possible Function of Acetylcholinesterase in Tumors with High Enzymatic Activity
3.2.2. Patterns of Molecular Forms Expressed in Tumors with High Enzymatic Activity
4. Conclusions
Author Contributions
Funding
Conflicts of Interest
References
- Horiuchi, Y.; Kimura, R.; Kato, N.; Fujii, T.; Seki, M.; Endo, T.; Kato, T.; Kawashima, K. Evolutional Study on Acetylcholine Expression. Life Sci. 2003, 72, 1745–1756. [Google Scholar] [CrossRef] [PubMed]
- Pérez-Aguilar, B.; Vidal, C.J.; Gomez-Olivares, J.L.; Gerardo-Ramirez, M.; Gutiérrez-Ruiz, M.C.; Gomez-Quiroz, L.E. Acetylcholinesterase. In Encyclopedia of Signaling Molecules; Choi, S., Ed.; Springer International Publishing: Cham, Switzerland, 2018; pp. 91–101. ISBN 978-3-319-67199-4. [Google Scholar]
- Resende, R.R.; Alves, A.S.; Britto, L.R.G.; Ulrich, H. Role of Acetylcholine Receptors in Proliferation and Differentiation of P19 Embryonal Carcinoma Cells. Exp. Cell Res. 2008, 314, 1429–1443. [Google Scholar] [CrossRef] [PubMed]
- Yu, H.; Xia, H.; Tang, Q.; Xu, H.; Wei, G.; Chen, Y.; Dai, X.; Gong, Q.; Bi, F. Acetylcholine Acts through M3 Muscarinic Receptor to Activate the EGFR Signaling and Promotes Gastric Cancer Cell Proliferation. Sci. Rep. 2017, 7, 40802. [Google Scholar] [CrossRef]
- Cheng, K.; Samimi, R.; Xie, G.; Shant, J.; Drachenberg, C.; Wade, M.; Davis, R.J.; Nomikos, G.; Raufman, J.-P. Acetylcholine Release by Human Colon Cancer Cells Mediates Autocrine Stimulation of Cell Proliferation. Am. J. Physiol. Gastrointest. Liver Physiol. 2008, 295, G591–G597. [Google Scholar] [CrossRef] [PubMed]
- Pettersson, A.; Nilsson, L.; Nylund, G.; Khorram-Manesh, A.; Nordgren, S.; Delbro, D.S. Is Acetylcholine an Autocrine/Paracrine Growth Factor via the Nicotinic Alpha7-Receptor Subtype in the Human Colon Cancer Cell Line HT-29? Eur. J. Pharmacol. 2009, 609, 27–33. [Google Scholar] [CrossRef]
- Song, P.; Sekhon, H.S.; Jia, Y.; Keller, J.A.; Blusztajn, J.K.; Mark, G.P.; Spindel, E.R. Acetylcholine Is Synthesized by and Acts as an Autocrine Growth Factor for Small Cell Lung Carcinoma. Cancer Res. 2003, 63, 214–221. [Google Scholar]
- Sloniecka, M.; Backman, L.J.; Danielson, P. Antiapoptotic Effect of Acetylcholine in Fas-Induced Apoptosis in Human Keratocytes. Investig. Ophthalmol. Vis. Sci. 2016, 57, 5892–5902. [Google Scholar] [CrossRef]
- Lindenboim, L.; Pinkas-Kramarski, R.; Sokolovsky, M.; Stein, R. Activation of Muscarinic Receptors Inhibits Apoptosis in PC12M1 Cells. J. Neurochem. 1995, 64, 2491–2499. [Google Scholar] [CrossRef]
- Leloup, C.; Michaelson, D.M.; Fisher, A.; Hartmann, T.; Beyreuther, K.; Stein, R. M1 Muscarinic Receptors Block Caspase Activation by Phosphoinositide 3-Kinase- and MAPK/ERK-Independent Pathways. Cell Death Differ. 2000, 7, 825–833. [Google Scholar] [CrossRef][Green Version]
- Yan, G.M.; Lin, S.Z.; Irwin, R.P.; Paul, S.M. Activation of Muscarinic Cholinergic Receptors Blocks Apoptosis of Cultured Cerebellar Granule Neurons. Mol. Pharmacol. 1995, 47, 248–257. [Google Scholar]
- Wang, L.; Zhi, X.; Zhang, Q.; Wei, S.; Li, Z.; Zhou, J.; Jiang, J.; Zhu, Y.; Yang, L.; Xu, H.; et al. Muscarinic Receptor M3 Mediates Cell Proliferation Induced by Acetylcholine and Contributes to Apoptosis in Gastric Cancer. Tumour Biol. 2016, 37, 2105–2117. [Google Scholar] [CrossRef]
- Zeidler, R.; Albermann, K.; Lang, S. Nicotine and Apoptosis. Apoptosis 2007, 12, 1927–1943. [Google Scholar] [CrossRef]
- Mai, H.; May, W.S.; Gao, F.; Jin, Z.; Deng, X. A Functional Role for Nicotine in Bcl2 Phosphorylation and Suppression of Apoptosis. J. Biol. Chem. 2003, 278, 1886–1891. [Google Scholar] [CrossRef]
- Improgo, M.R.; Soll, L.G.; Tapper, A.R.; Gardner, P.D. Nicotinic Acetylcholine Receptors Mediate Lung Cancer Growth. Front. Physiol. 2013, 4, 251. [Google Scholar] [CrossRef]
- Wan, C.; Wu, M.; Zhang, S.; Chen, Y.; Lu, C. A7nAChR-mediated Recruitment of PP1γ Promotes TRAF6/NF-κB Cascade to Facilitate the Progression of Hepatocellular Carcinoma. Mol. Carcinog. 2018, 57, 1626–1639. [Google Scholar] [CrossRef]
- Chien, C.-Y.; Chen, Y.-C.; Hsu, C.-C.; Chou, Y.-T.; Shiah, S.-G.; Liu, S.-Y.; Hsieh, A.C.-T.; Yen, C.-Y.; Lee, C.-H.; Shieh, Y.-S. YAP-Dependent BiP Induction Is Involved in Nicotine-Mediated Oral Cancer Malignancy. Cells 2021, 10, 2080. [Google Scholar] [CrossRef]
- Paleari, L.; Grozio, A.; Cesario, A.; Russo, P. The Cholinergic System and Cancer. Semin. Cancer Biol. 2008, 18, 211–217. [Google Scholar] [CrossRef]
- Dasgupta, P.; Rastogi, S.; Pillai, S.; Ordonez-Ercan, D.; Morris, M.; Haura, E.; Chellappan, S. Nicotine Induces Cell Proliferation by Beta-Arrestin-Mediated Activation of Src and Rb-Raf-1 Pathways. J. Clin. Investig. 2006, 116, 2208–2217. [Google Scholar] [CrossRef]
- Dasgupta, P.; Chellappan, S.P. Nicotine-Mediated Cell Proliferation and Angiogenesis: New Twists to an Old Story. Cell Cycle 2006, 5, 2324–2328. [Google Scholar] [CrossRef]
- Trombino, S.; Cesario, A.; Margaritora, S.; Granone, P.; Motta, G.; Falugi, C.; Russo, P. Alpha7-Nicotinic Acetylcholine Receptors Affect Growth Regulation of Human Mesothelioma Cells: Role of Mitogen-Activated Protein Kinase Pathway. Cancer Res. 2004, 64, 135–145. [Google Scholar] [CrossRef]
- Jull, B.A.; Plummer, H.K.; Schuller, H.M. Nicotinic Receptor-Mediated Activation by the Tobacco-Specific Nitrosamine NNK of a Raf-1/MAP Kinase Pathway, Resulting in Phosphorylation of c-Myc in Human Small Cell Lung Carcinoma Cells and Pulmonary Neuroendocrine Cells. J. Cancer Res. Clin. Oncol. 2001, 127, 707–717. [Google Scholar] [CrossRef] [PubMed]
- Chu, M.; Guo, J.; Chen, C.-Y. Long-Term Exposure to Nicotine, via Ras Pathway, Induces Cyclin D1 to Stimulate G1 Cell Cycle Transition. J. Biol. Chem. 2005, 280, 6369–6379. [Google Scholar] [CrossRef] [PubMed]
- Schouten, G.J.; Vertegaal, A.C.; Whiteside, S.T.; Israël, A.; Toebes, M.; Dorsman, J.C.; van der Eb, A.J.; Zantema, A. IkappaB Alpha Is a Target for the Mitogen-Activated 90 KDa Ribosomal S6 Kinase. EMBO J. 1997, 16, 3133–3144. [Google Scholar] [CrossRef] [PubMed]
- Ghoda, L.; Lin, X.; Greene, W.C. The 90-KDa Ribosomal S6 Kinase (Pp90rsk) Phosphorylates the N-Terminal Regulatory Domain of IkappaBalpha and Stimulates Its Degradation in Vitro. J. Biol. Chem. 1997, 272, 21281–21288. [Google Scholar] [CrossRef]
- Xu, S.; Bayat, H.; Hou, X.; Jiang, B. Ribosomal S6 Kinase-1 Modulates Interleukin-1beta-Induced Persistent Activation of NF-KappaB through Phosphorylation of IkappaBbeta. Am. J. Physiol.-Cell Physiol. 2006, 291, C1336–C1345. [Google Scholar] [CrossRef]
- Lavoie, J.N.; L’Allemain, G.; Brunet, A.; Müller, R.; Pouysségur, J. Cyclin D1 Expression Is Regulated Positively by the P42/P44MAPK and Negatively by the P38/HOGMAPK Pathway. J. Biol. Chem. 1996, 271, 20608–20616. [Google Scholar] [CrossRef]
- Chambard, J.-C.; Lefloch, R.; Pouysségur, J.; Lenormand, P. ERK Implication in Cell Cycle Regulation. Biochim. Biophys. Acta (BBA)—Mol. Cell Res. 2007, 1773, 1299–1310. [Google Scholar] [CrossRef]
- Frödin, M.; Gammeltoft, S. Role and Regulation of 90 KDa Ribosomal S6 Kinase (RSK) in Signal Transduction. Mol. Cell. Endocrinol. 1999, 151, 65–77. [Google Scholar] [CrossRef]
- Lee, F.S.; Hagler, J.; Chen, Z.J.; Maniatis, T. Activation of the IkappaB Alpha Kinase Complex by MEKK1, a Kinase of the JNK Pathway. Cell 1997, 88, 213–222. [Google Scholar] [CrossRef]
- West, K.A.; Brognard, J.; Clark, A.S.; Linnoila, I.R.; Yang, X.; Swain, S.M.; Harris, C.; Belinsky, S.; Dennis, P.A. Rapid Akt Activation by Nicotine and a Tobacco Carcinogen Modulates the Phenotype of Normal Human Airway Epithelial Cells. J. Clin. Investig. 2003, 111, 81–90. [Google Scholar] [CrossRef]
- Jin, Z.; Gao, F.; Flagg, T.; Deng, X. Nicotine Induces Multi-Site Phosphorylation of Bad in Association with Suppression of Apoptosis. J. Biol. Chem. 2004, 279, 23837–23844. [Google Scholar] [CrossRef] [PubMed]
- Xin, M.; Deng, X. Nicotine Inactivation of the Proapoptotic Function of Bax through Phosphorylation. J. Biol. Chem. 2005, 280, 10781–10789. [Google Scholar] [CrossRef] [PubMed]
- Xin, M.; Gao, F.; May, W.S.; Flagg, T.; Deng, X. Protein Kinase Czeta Abrogates the Proapoptotic Function of Bax through Phosphorylation. J. Biol. Chem. 2007, 282, 21268–21277. [Google Scholar] [CrossRef] [PubMed]
- Español, A.J.; Sales, M.E. Different Muscarinc Receptors Are Involved in the Proliferation of Murine Mammary Adenocarcinoma Cell Lines. Int. J. Mol. Med. 2004, 13, 311–317. [Google Scholar]
- Felder, C.C. Muscarinic Acetylcholine Receptors: Signal Transduction through Multiple Effectors. FASEB J. 1995, 9, 619–625. [Google Scholar]
- Jiménez, E.; Montiel, M. Activation of MAP Kinase by Muscarinic Cholinergic Receptors Induces Cell Proliferation and Protein Synthesis in Human Breast Cancer Cells. J. Cell. Physiol. 2005, 204, 678–686. [Google Scholar] [CrossRef]
- Kolch, W.; Heidecker, G.; Kochs, G.; Hummel, R.; Vahidi, H.; Mischak, H.; Finkenzeller, G.; Marmé, D.; Rapp, U.R. Protein Kinase C Alpha Activates RAF-1 by Direct Phosphorylation. Nature 1993, 364, 249–252. [Google Scholar] [CrossRef]
- Li, B.S.; Ma, W.; Zhang, L.; Barker, J.L.; Stenger, D.A.; Pant, H.C. Activation of Phosphatidylinositol-3 Kinase (PI-3K) and Extracellular Regulated Kinases (Erk1/2) Is Involved in Muscarinic Receptor-Mediated DNA Synthesis in Neural Progenitor Cells. J. Neurosci. 2001, 21, 1569–1579. [Google Scholar]
- Iwasaki, H.; Shichiri, M.; Marumo, F.; Hirata, Y. Adrenomedullin Stimulates Proline-Rich Tyrosine Kinase 2 in Vascular Smooth Muscle Cells. Endocrinology 2001, 142, 564–572. [Google Scholar] [CrossRef]
- Della Rocca, G.J.; Mukhin, Y.V.; Garnovskaya, M.N.; Daaka, Y.; Clark, G.J.; Luttrell, L.M.; Lefkowitz, R.J.; Raymond, J.R. Serotonin 5-HT1A Receptor-Mediated Erk Activation Requires Calcium/Calmodulin-Dependent Receptor Endocytosis. J. Biol. Chem. 1999, 274, 4749–4753. [Google Scholar] [CrossRef]
- Schmitt, J.M.; Abell, E.; Wagner, A.; Davare, M.A. ERK Activation and Cell Growth Require CaM Kinases in MCF-7 Breast Cancer Cells. Mol. Cell. Biochem. 2010, 335, 155–171. [Google Scholar] [CrossRef] [PubMed][Green Version]
- Marte, B.M.; Downward, J. PKB/Akt: Connecting Phosphoinositide 3-Kinase to Cell Survival and Beyond. Trends Biochem. Sci. 1997, 22, 355–358. [Google Scholar] [CrossRef] [PubMed]
- Dudek, H.; Datta, S.R.; Franke, T.F.; Birnbaum, M.J.; Yao, R.; Cooper, G.M.; Segal, R.A.; Kaplan, D.R.; Greenberg, M.E. Regulation of Neuronal Survival by the Serine-Threonine Protein Kinase Akt. Science 1997, 275, 661–665. [Google Scholar] [CrossRef] [PubMed]
- Kulik, G.; Klippel, A.; Weber, M.J. Antiapoptotic Signalling by the Insulin-like Growth Factor I Receptor, Phosphatidylinositol 3-Kinase, and Akt. Mol. Cell. Biol. 1997, 17, 1595–1606. [Google Scholar] [CrossRef] [PubMed]
- Murga, C.; Laguinge, L.; Wetzker, R.; Cuadrado, A.; Gutkind, J.S. Activation of Akt/Protein Kinase B by G Protein-Coupled Receptors. A Role for Alpha and Beta Gamma Subunits of Heterotrimeric G Proteins Acting through Phosphatidylinositol-3-OH Kinasegamma. J. Biol. Chem. 1998, 273, 19080–19085. [Google Scholar] [CrossRef]
- Desdouits-Magnen, J.; Desdouits, F.; Takeda, S.; Syu, L.J.; Saltiel, A.R.; Buxbaum, J.D.; Czernik, A.J.; Nairn, A.C.; Greengard, P. Regulation of Secretion of Alzheimer Amyloid Precursor Protein by the Mitogen-Activated Protein Kinase Cascade. J. Neurochem. 1998, 70, 524–530. [Google Scholar] [CrossRef]
- Ueda, H.; Morishita, R.; Narumiya, S.; Kato, K.; Asano, T. Galphaq/11 Signaling Induces Apoptosis through Two Pathways Involving Reduction of Akt Phosphorylation and Activation of RhoA in HeLa Cells. Exp. Cell Res. 2004, 298, 207–217. [Google Scholar] [CrossRef]
- Budd, D.C.; Spragg, E.J.; Ridd, K.; Tobin, A.B. Signalling of the M3-Muscarinic Receptor to the Anti-Apoptotic Pathway. Biochem. J. 2004, 381, 43–49. [Google Scholar] [CrossRef]
- Cardone, M.H.; Roy, N.; Stennicke, H.R.; Salvesen, G.S.; Franke, T.F.; Stanbridge, E.; Frisch, S.; Reed, J.C. Regulation of Cell Death Protease Caspase-9 by Phosphorylation. Science 1998, 282, 1318–1321. [Google Scholar] [CrossRef]
- Page, C.; Lin, H.J.; Jin, Y.; Castle, V.P.; Nunez, G.; Huang, M.; Lin, J. Overexpression of Akt/AKT Can Modulate Chemotherapy-Induced Apoptosis. Anticancer Res. 2000, 20, 407–416. [Google Scholar]
- Henshall, D.C.; Araki, T.; Schindler, C.K.; Lan, J.-Q.; Tiekoter, K.L.; Taki, W.; Simon, R.P. Activation of Bcl-2-Associated Death Protein and Counter-Response of Akt within Cell Populations during Seizure-Induced Neuronal Death. J. Neurosci. 2002, 22, 8458–8465. [Google Scholar] [CrossRef]
- del Peso, L.; González-García, M.; Page, C.; Herrera, R.; Nuñez, G. Interleukin-3-Induced Phosphorylation of BAD through the Protein Kinase Akt. Science 1997, 278, 687–689. [Google Scholar] [CrossRef] [PubMed]
- Kennedy, S.G.; Wagner, A.J.; Conzen, S.D.; Jordán, J.; Bellacosa, A.; Tsichlis, P.N.; Hay, N. The PI 3-Kinase/Akt Signaling Pathway Delivers an Anti-Apoptotic Signal. Genes Dev. 1997, 11, 701–713. [Google Scholar] [CrossRef] [PubMed]
- Cui, Q.-L.; Fogle, E.; Almazan, G. Muscarinic Acetylcholine Receptors Mediate Oligodendrocyte Progenitor Survival through Src-like Tyrosine Kinases and PI3K/Akt Pathways. Neurochem. Int. 2006, 48, 383–393. [Google Scholar] [CrossRef]
- Quinn, D.M. Acetylcholinesterase: Enzyme Structure, Reaction Dynamics, and Virtual Transition States. Chem. Rev. 1987, 87, 955–979. [Google Scholar] [CrossRef]
- Taylor, P.; Radić, Z. The Cholinesterases: From Genes to Proteins. Annu. Rev. Pharmacol. Toxicol. 1994, 34, 281–320. [Google Scholar] [CrossRef]
- Getman, D.K.; Eubanks, J.H.; Camp, S.; Evans, G.A.; Taylor, P. The Human Gene Encoding Acetylcholinesterase Is Located on the Long Arm of Chromosome 7. Am. J. Hum. Genet. 1992, 51, 170–177. [Google Scholar]
- Bronicki, L.M.; Jasmin, B.J. Trans-Acting Factors Governing Acetylcholinesterase MRNA Metabolism in Neurons. Front. Mol. Neurosci. 2012, 5, 36. [Google Scholar] [CrossRef]
- Massoulié, J.; Anselmet, A.; Bon, S.; Krejci, E.; Legay, C.; Morel, N.; Simon, S. Acetylcholinesterase: C-Terminal Domains, Molecular Forms and Functional Localization. J. Physiol. Paris 1998, 92, 183–190. [Google Scholar] [CrossRef]
- Massoulié, J.; Pezzementi, L.; Bon, S.; Krejci, E.; Vallette, F.M. Molecular and Cellular Biology of Cholinesterases. Prog. Neurobiol. 1993, 41, 31–91. [Google Scholar] [CrossRef]
- Meshorer, E.; Soreq, H. Virtues and Woes of AChE Alternative Splicing in Stress-Related Neuropathologies. Trends Neurosci. 2006, 29, 216–224. [Google Scholar] [CrossRef] [PubMed]
- Nazim, M.; Masuda, A.; Rahman, M.A.; Nasrin, F.; Takeda, J.-I.; Ohe, K.; Ohkawara, B.; Ito, M.; Ohno, K. Competitive Regulation of Alternative Splicing and Alternative Polyadenylation by HnRNP H and CstF64 Determines Acetylcholinesterase Isoforms. Nucleic Acids Res. 2017, 45, 1455–1468. [Google Scholar] [CrossRef] [PubMed]
- Bon, S.; Massoulié, J. Quaternary Associations of Acetylcholinesterase: I. Oligomeric associations of T subunits with and without the amino-terminal domain of the collagen tail. J. Biol. Chem. 1997, 272, 3007–3015. [Google Scholar] [CrossRef]
- Perrier, A.L.; Massoulié, J.; Krejci, E. PRiMA: The Membrane Anchor of Acetylcholinesterase in the Brain. Neuron 2002, 33, 275–285. [Google Scholar] [CrossRef]
- Massoulié, J. The Origin of the Molecular Diversity and Functional Anchoring of Cholinesterases. Neurosignals 2002, 11, 130–143. [Google Scholar] [CrossRef] [PubMed]
- Coussen, F.; Ayon, A.; Le Goff, A.; Leroy, J.; Massoulié, J.; Bon, S. Addition of a Glycophosphatidylinositol to Acetylcholinesterase. Processing, Degradation, and Secretion. J. Biol. Chem. 2001, 276, 27881–27892. [Google Scholar] [CrossRef]
- Soreq, H.; Seidman, S. Acetylcholinesterase—New Roles for an Old Actor. Nat. Rev. Neurosci. 2001, 2, 294–302. [Google Scholar] [CrossRef]
- Meshorer, E.; Toiber, D.; Zurel, D.; Sahly, I.; Dori, A.; Cagnano, E.; Schreiber, L.; Grisaru, D.; Tronche, F.; Soreq, H. Combinatorial Complexity of 5′ Alternative Acetylcholinesterase Transcripts and Protein Products. J. Biol. Chem. 2004, 279, 29740–29751. [Google Scholar] [CrossRef]
- Zhang, X.J.; Yang, L.; Zhao, Q.; Caen, J.P.; He, H.Y.; Jin, Q.H.; Guo, L.H.; Alemany, M.; Zhang, L.Y.; Shi, Y.F. Induction of Acetylcholinesterase Expression during Apoptosis in Various Cell Types. Cell Death Differ. 2002, 9, 790–800. [Google Scholar] [CrossRef]
- Zhang, J.Y.; Jiang, H.; Gao, W.; Wu, J.; Peng, K.; Shi, Y.F.; Zhang, X.J. The JNK/AP1/ATF2 Pathway Is Involved in H2O2-Induced Acetylcholinesterase Expression during Apoptosis. Cell. Mol. Life Sci. 2008, 65, 1435–1445. [Google Scholar] [CrossRef]
- Bernardi, C.C.; Ribeiro, E.d.S.F.; Cavalli, I.J.; Chautard-Freire-Maia, E.A.; Souza, R.L.R. Amplification and Deletion of the ACHE and BCHE Cholinesterase Genes in Sporadic Breast Cancer. Cancer Genet. Cytogenet. 2010, 197, 158–165. [Google Scholar] [CrossRef] [PubMed]
- Boberg, D.R.; Batistela, M.S.; Pecharki, M.; Ribeiro, E.M.S.F.; Cavalli, I.J.; Lima, R.S.; Urban, C.A.; Furtado-Alle, L.; Souza, R.L.R. Copy Number Variation in ACHE/EPHB4 (7q22) and in BCHE/MME (3q26) Genes in Sporadic Breast Cancer. Chem. Biol. Interact. 2013, 203, 344–347. [Google Scholar] [CrossRef]
- Perry, C.; Sklan, E.H.; Birikh, K.; Shapira, M.; Trejo, L.; Eldor, A.; Soreq, H. Complex Regulation of Acetylcholinesterase Gene Expression in Human Brain Tumors. Oncogene 2002, 21, 8428–8441. [Google Scholar] [CrossRef]
- Montenegro, M.F.; Ruiz-Espejo, F.; Campoy, F.J.; Muñoz-Delgado, E.; de la Cadena, M.P.; Rodríguez-Berrocal, F.J.; Vidal, C.J. Cholinesterases Are Down-Expressed in Human Colorectal Carcinoma. Cell. Mol. Life Sci. 2006, 63, 2175–2182. [Google Scholar] [CrossRef] [PubMed]
- Martínez-Moreno, P.; Nieto-Cerón, S.; Torres-Lanzas, J.; Ruiz-Espejo, F.; Tovar-Zapata, I.; Martínez-Hernández, P.; Rodríguez-López, J.N.; Vidal, C.J.; Cabezas-Herrera, J. Cholinesterase Activity of Human Lung Tumours Varies According to Their Histological Classification. Carcinogenesis 2006, 27, 429–436. [Google Scholar] [CrossRef]
- Muñoz-Delgado, E.; Montenegro, M.F.; Campoy, F.J.; Moral-Naranjo, M.T.; Cabezas-Herrera, J.; Kovacs, G.; Vidal, C.J. Expression of Cholinesterases in Human Kidney and Its Variation in Renal Cell Carcinoma Types. FEBS J. 2010, 277, 4519–4529. [Google Scholar] [CrossRef]
- Qavi, H.; Al-Rajhi, A.A. Acetylcholinesterase and HHV-8 in Squamous Cell Carcinoma and Retinoblastoma. In Vivo 2009, 23, 679–683. [Google Scholar]
- Chandrashekar, D.S.; Bashel, B.; Balasubramanya, S.A.H.; Creighton, C.J.; Ponce-Rodriguez, I.; Chakravarthi, B.V.S.K.; Varambally, S. UALCAN: A Portal for Facilitating Tumor Subgroup Gene Expression and Survival Analyses. Neoplasia 2017, 19, 649–658. [Google Scholar] [CrossRef]
- Chandrashekar, D.S.; Karthikeyan, S.K.; Korla, P.K.; Patel, H.; Shovon, A.R.; Athar, M.; Netto, G.J.; Qin, Z.S.; Kumar, S.; Manne, U.; et al. UALCAN: An Update to the Integrated Cancer Data Analysis Platform. Neoplasia 2022, 25, 18–27. [Google Scholar] [CrossRef] [PubMed]
- Lánczky, A.; Győrffy, B. Web-Based Survival Analysis Tool Tailored for Medical Research (KMplot): Development and Implementation. J. Med. Internet Res. 2021, 23, e27633. [Google Scholar] [CrossRef]
- Cancer Today. Available online: http://gco.iarc.fr/today/home (accessed on 1 July 2022).
- Sung, H.; Ferlay, J.; Siegel, R.L.; Laversanne, M.; Soerjomataram, I.; Jemal, A.; Bray, F. Global Cancer Statistics 2020: GLOBOCAN Estimates of Incidence and Mortality Worldwide for 36 Cancers in 185 Countries. CA Cancer J. Clin. 2021, 71, 209–249. [Google Scholar] [CrossRef]
- Zhao, Y.; Wang, X.; Wang, T.; Hu, X.; Hui, X.; Yan, M.; Gao, Q.; Chen, T.; Li, J.; Yao, M.; et al. Acetylcholinesterase, a Key Prognostic Predictor for Hepatocellular Carcinoma, Suppresses Cell Growth and Induces Chemosensitization. Hepatology 2011, 53, 493–503. [Google Scholar] [CrossRef] [PubMed]
- Xu, H.; Shen, Z.; Xiao, J.; Yang, Y.; Huang, W.; Zhou, Z.; Shen, J.; Zhu, Y.; Liu, X.-Y.; Chu, L. Acetylcholinesterase Overexpression Mediated by Oncolytic Adenovirus Exhibited Potent Anti-Tumor Effect. BMC Cancer 2014, 14, 668. [Google Scholar] [CrossRef] [PubMed]
- Castillo-González, A.C.; Nieto-Cerón, S.; Pelegrín-Hernández, J.P.; Montenegro, M.F.; Noguera, J.A.; López-Moreno, M.F.; Rodríguez-López, J.N.; Vidal, C.J.; Hellín-Meseguer, D.; Cabezas-Herrera, J. Dysregulated Cholinergic Network as a Novel Biomarker of Poor Prognostic in Patients with Head and Neck Squamous Cell Carcinoma. BMC Cancer 2015, 15, 385. [Google Scholar] [CrossRef] [PubMed]
- Castillo-González, A.C.; Pelegrín-Hernández, J.P.; Nieto-Cerón, S.; Madrona, A.P.; Noguera, J.A.; López-Moreno, M.F.; Rodríguez-López, J.N.; Vidal, C.J.; Hellín-Meseguer, D.; Cabezas-Herrera, J. Unbalanced Acetylcholinesterase Activity in Larynx Squamous Cell Carcinoma. Int. Immunopharmacol. 2015, 29, 81–86. [Google Scholar] [CrossRef]
- Battisti, V.; Bagatini, M.D.; Maders, L.D.K.; Chiesa, J.; Santos, K.F.; Gonçalves, J.F.; Abdalla, F.H.; Battisti, I.E.; Schetinger, M.R.C.; Morsch, V.M. Cholinesterase Activities and Biochemical Determinations in Patients with Prostate Cancer: Influence of Gleason Score, Treatment and Bone Metastasis. Biomed. Pharmacother. 2012, 66, 249–255. [Google Scholar] [CrossRef]
- Nieto-Cerón, S.; Vargas-López, H.; Pérez-Albacete, M.; Tovar-Zapata, I.; Martínez-Hernández, P.; Rodríguez-López, J.N.; Cabezas-Herrera, J. Analysis of Cholinesterases in Human Prostate and Sperm: Implications in Cancer and Fertility. Chem. Biol. Interact. 2010, 187, 432–435. [Google Scholar] [CrossRef]
- Martínez-López de Castro, A.; Nieto-Cerón, S.; Aurelio, P.-C.; Galbis-Martínez, L.; Latour-Pérez, J.; Torres-Lanzas, J.; Tovar-Zapata, I.; Martínez-Hernández, P.; Rodríguez-López, J.N.; Cabezas-Herrera, J. Cancer-Associated Differences in Acetylcholinesterase Activity in Bronchial Aspirates from Patients with Lung Cancer. Clin. Sci. 2008, 115, 245–253. [Google Scholar] [CrossRef]
- Garcıa-Ayllón, M.S.; Sáez-Valero, J.; Muñoz-Delgado, E.; Vidal, C.J. Identification of Hybrid Cholinesterase Forms Consisting of Acetyl- and Butyrylcholinesterase Subunits in Human Glioma. Neuroscience 2001, 107, 199–208. [Google Scholar] [CrossRef]
- Pérez-Aguilar, B.; Vidal, C.J.; Palomec, G.; García-Dolores, F.; Gutiérrez-Ruiz, M.C.; Bucio, L.; Gómez-Olivares, J.L.; Gómez-Quiroz, L.E. Acetylcholinesterase Is Associated with a Decrease in Cell Proliferation of Hepatocellular Carcinoma Cells. Biochim. Biophys. Acta 2015, 1852, 1380–1387. [Google Scholar] [CrossRef]
- Ruiz-Espejo, F.; Cabezas-Herrera, J.; Illana, J.; Campoy, F.J.; Muñoz-Delgado, E.; Vidal, C.J. Breast Cancer Metastasis Alters Acetylcholinesterase Activity and the Composition of Enzyme Forms in Axillary Lymph Nodes. Breast Cancer Res. Treat. 2003, 80, 105–114. [Google Scholar] [CrossRef] [PubMed]
- Calaf, G.M.; Parra, E.; Garrido, F. Cell Proliferation and Tumor Formation Induced by Eserine, an Acetylcholinesterase Inhibitor, in Rat Mammary Gland. Oncol. Rep. 2007, 17, 25–33. [Google Scholar] [CrossRef] [PubMed][Green Version]
- Jing, P.; Jin, Q.; Wu, J.; Zhang, X.-J. GSK3beta Mediates the Induced Expression of Synaptic Acetylcholinesterase during Apoptosis. J. Neurochem. 2008, 104, 409–419. [Google Scholar] [CrossRef]
- Toiber, D.; Berson, A.; Greenberg, D.; Melamed-Book, N.; Diamant, S.; Soreq, H. N-Acetylcholinesterase-Induced Apoptosis in Alzheimer’s Disease. PLoS ONE 2008, 3, e3108. [Google Scholar] [CrossRef] [PubMed]
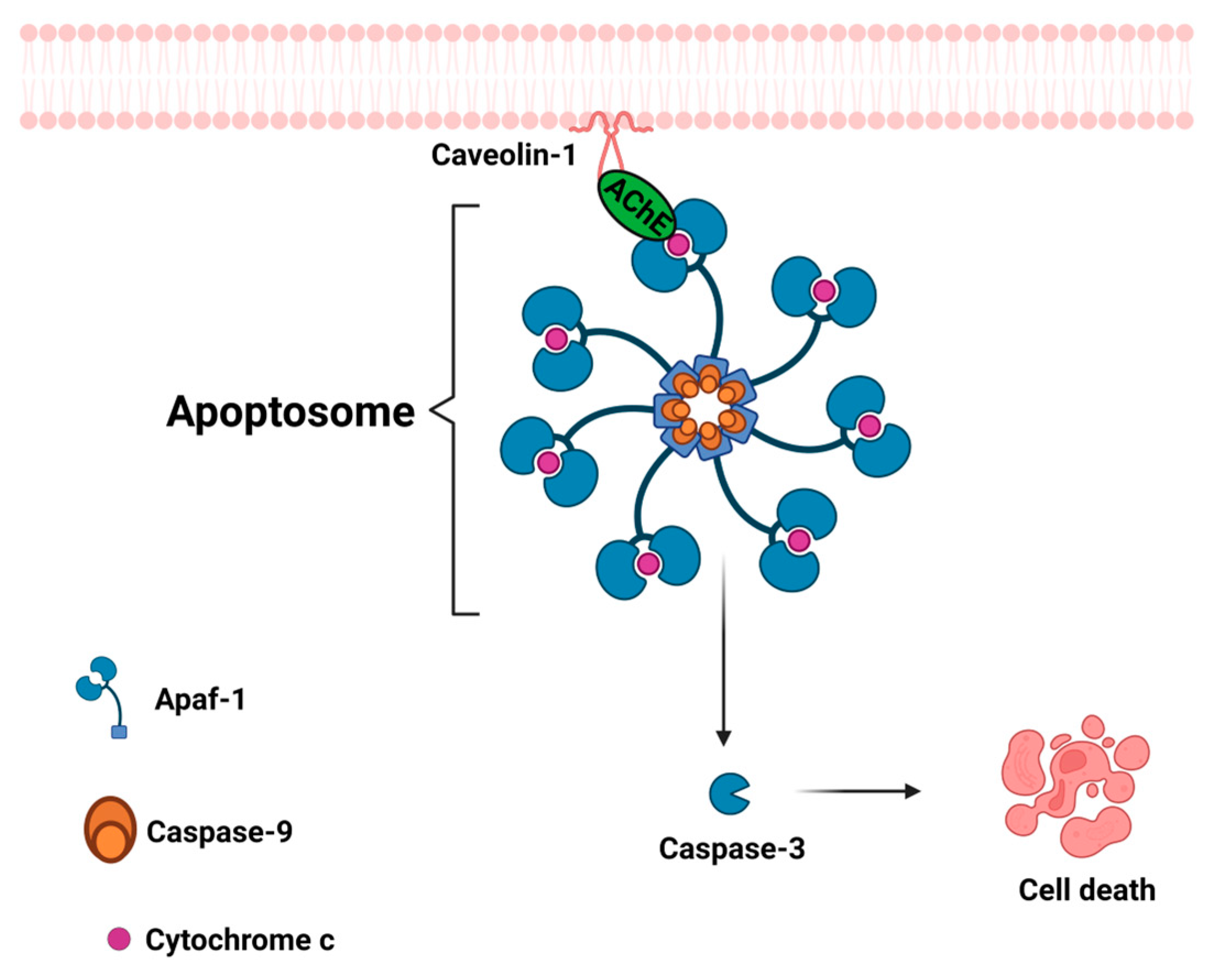
- Park, S.E.; Kim, N.D.; Yoo, Y.H. Acetylcholinesterase Plays a Pivotal Role in Apoptosome Formation. Cancer Res. 2004, 64, 2652–2655. [Google Scholar] [CrossRef] [PubMed]
- Park, S.E.; Jeong, S.H.; Yee, S.-B.; Kim, T.H.; Soung, Y.H.; Ha, N.C.; Kim, N.D.; Park, J.-Y.; Bae, H.R.; Park, B.S.; et al. Interactions of Acetylcholinesterase with Caveolin-1 and Subsequently with Cytochrome c Are Required for Apoptosome Formation. Carcinogenesis 2008, 29, 729–737. [Google Scholar] [CrossRef]
- Richbart, S.D.; Merritt, J.C.; Nolan, N.A.; Dasgupta, P. Acetylcholinesterase and Human Cancers. Adv. Cancer Res. 2021, 152, 1–66. [Google Scholar] [CrossRef]
- Cassiman, D.; Libbrecht, L.; Sinelli, N.; Desmet, V.; Denef, C.; Roskams, T. The Vagal Nerve Stimulates Activation of the Hepatic Progenitor Cell Compartment via Muscarinic Acetylcholine Receptor Type 3. Am. J. Pathol. 2002, 161, 521–530. [Google Scholar] [CrossRef] [PubMed]
- Nie, H.; Cao, Q.; Zhu, L.; Gong, Y.; Gu, J.; He, Z. Acetylcholine Acts on Androgen Receptor to Promote the Migration and Invasion but Inhibit the Apoptosis of Human Hepatocarcinoma. PLoS ONE 2013, 8, e61678. [Google Scholar] [CrossRef]
- Jiang, H.; Zhang, J.; Zhu, H.; Li, H.; Zhang, X. Nerve Growth Factor Prevents the Apoptosis-Associated Increase in Acetylcholinesterase Activity after Hydrogen Peroxide Treatment by Activating Akt. Acta Biochim. Biophys. Sin. 2007, 39, 46–56. [Google Scholar] [CrossRef]
- Noorolyai, S.; Shajari, N.; Baghbani, E.; Sadreddini, S.; Baradaran, B. The Relation between PI3K/AKT Signalling Pathway and Cancer. Gene 2019, 698, 120–128. [Google Scholar] [CrossRef] [PubMed]
- Fresno Vara, J.A.; Casado, E.; de Castro, J.; Cejas, P.; Belda-Iniesta, C.; González-Barón, M. PI3K/Akt Signalling Pathway and Cancer. Cancer Treat. Rev. 2004, 30, 193–204. [Google Scholar] [CrossRef] [PubMed]
- Qadir, X.V.; Han, C.; Lu, D.; Zhang, J.; Wu, T. MiR-185 Inhibits Hepatocellular Carcinoma Growth by Targeting the DNMT1/PTEN/Akt Pathway. Am. J. Pathol. 2014, 184, 2355–2364. [Google Scholar] [CrossRef]
- Bian, E.-B.; Huang, C.; Ma, T.-T.; Tao, H.; Zhang, H.; Cheng, C.; Lv, X.-W.; Li, J. DNMT1-Mediated PTEN Hypermethylation Confers Hepatic Stellate Cell Activation and Liver Fibrogenesis in Rats. Toxicol. Appl. Pharmacol. 2012, 264, 13–22. [Google Scholar] [CrossRef] [PubMed]
- Xi, Q.; Gao, N.; Yang, Y.; Ye, W.; Zhang, B.; Wu, J.; Jiang, G.; Zhang, X. Anticancer Drugs Induce Hypomethylation of the Acetylcholinesterase Promoter via a Phosphorylated-P38-DNMT1-AChE Pathway in Apoptotic Hepatocellular Carcinoma Cells. Int. J. Biochem. Cell Biol. 2015, 68, 21–32. [Google Scholar] [CrossRef]
- Saito, Y.; Kanai, Y.; Nakagawa, T.; Sakamoto, M.; Saito, H.; Ishii, H.; Hirohashi, S. Increased Protein Expression of DNA Methyltransferase (DNMT) 1 Is Significantly Correlated with the Malignant Potential and Poor Prognosis of Human Hepatocellular Carcinomas. Int. J. Cancer 2003, 105, 527–532. [Google Scholar] [CrossRef]
- Etoh, T.; Kanai, Y.; Ushijima, S.; Nakagawa, T.; Nakanishi, Y.; Sasako, M.; Kitano, S.; Hirohashi, S. Increased DNA Methyltransferase 1 (DNMT1) Protein Expression Correlates Significantly with Poorer Tumor Differentiation and Frequent DNA Hypermethylation of Multiple CpG Islands in Gastric Cancers. Am. J. Pathol. 2004, 164, 689–699. [Google Scholar] [CrossRef]
- Agoston, A.T.; Argani, P.; Yegnasubramanian, S.; De Marzo, A.M.; Ansari-Lari, M.A.; Hicks, J.L.; Davidson, N.E.; Nelson, W.G. Increased Protein Stability Causes DNA Methyltransferase 1 Dysregulation in Breast Cancer. J. Biol. Chem. 2005, 280, 18302–18310. [Google Scholar] [CrossRef]
- Kwon, Y.-M.; Park, J.H.; Kim, H.; Shim, Y.M.; Kim, J.; Han, J.; Park, J.; Kim, D.-H. Different Susceptibility of Increased DNMT1 Expression by Exposure to Tobacco Smoke According to Histology in Primary Non-Small Cell Lung Cancer. J. Cancer Res. Clin. Oncol. 2007, 133, 219–226. [Google Scholar] [CrossRef]
- Li, A.; Omura, N.; Hong, S.-M.; Goggins, M. Pancreatic Cancer DNMT1 Expression and Sensitivity to DNMT1 Inhibitors. Cancer Biol. Ther. 2010, 9, 321–329. [Google Scholar] [CrossRef]
- Rajendran, G.; Shanmuganandam, K.; Bendre, A.; Muzumdar, D.; Mujumdar, D.; Goel, A.; Shiras, A. Epigenetic Regulation of DNA Methyltransferases: DNMT1 and DNMT3B in Gliomas. J. Neurooncol. 2011, 104, 483–494. [Google Scholar] [CrossRef] [PubMed]
- Kullmann, K.; Deryal, M.; Ong, M.F.; Schmidt, W.; Mahlknecht, U. DNMT1 Genetic Polymorphisms Affect Breast Cancer Risk in the Central European Caucasian Population. Clin. Epigenetics 2013, 5, 7. [Google Scholar] [CrossRef] [PubMed]
- Cacan, E.; Ali, M.W.; Boyd, N.H.; Hooks, S.B.; Greer, S.F. Inhibition of HDAC1 and DNMT1 Modulate RGS10 Expression and Decrease Ovarian Cancer Chemoresistance. PLoS ONE 2014, 9, e87455. [Google Scholar] [CrossRef] [PubMed]
- Bottoni, P.; Giardina, B.; Vitali, A.; Boninsegna, A.; Scatena, R. A Proteomic Approach to Characterizing Ciglitazone-Induced Cancer Cell Differentiation in Hep-G2 Cell Line. Biochim. Biophys. Acta 2009, 1794, 615–626. [Google Scholar] [CrossRef] [PubMed]
- Layer, P.G.; Klaczinski, J.; Salfelder, A.; Sperling, L.E.; Thangaraj, G.; Tuschl, C.; Vogel-Höpker, A. Cholinesterases in Development: AChE as a Firewall to Inhibit Cell Proliferation and Support Differentiation. Chem. Biol. Interact. 2013, 203, 269–276. [Google Scholar] [CrossRef]
- Xiang, A.C.; Xie, J.; Zhang, X.J. Acetylcholinesterase in Intestinal Cell Differentiation Involves G2/M Cell Cycle Arrest. Cell. Mol. Life Sci. 2008, 65, 1768–1779. [Google Scholar] [CrossRef]
- Syed, M.; Fenoglio-Preiser, C.; Skau, K.A.; Weber, G.F. Acetylcholinesterase Supports Anchorage Independence in Colon Cancer. Clin. Exp. Metastasis 2008, 25, 787–798. [Google Scholar] [CrossRef]
- Barbosa, M.; Rios, O.; Velásquez, M.; Villalobos, J.; Ehrmanns, J. Acetylcholinesterase and Butyrylcholinesterase Histochemical Activities and Tumor Cell Growth in Several Brain Tumors. Surg. Neurol. 2001, 55, 106–112. [Google Scholar] [CrossRef]
- Ruiz-Espejo, F.; Cabezas-Herrera, J.; Illana, J.; Campoy, F.J.; Vidal, C.J. Cholinesterase Activity and Acetylcholinesterase Glycosylation Are Altered in Human Breast Cancer. Breast Cancer Res. Treat. 2002, 72, 11–22. [Google Scholar] [CrossRef]
- Muñoz-Delgado, E.; Montenegro, M.F.; Morote-García, J.C.; Campoy, F.J.; Cabezas-Herrera, J.; Kovacs, G.; Vidal, C.J. The Expression of Cholinesterases in Human Renal Tumours Varies According to Their Histological Types. Chem. Biol. Interact. 2008, 175, 340–342. [Google Scholar] [CrossRef]
- Pfitzinger, P.L.; Fangmann, L.; Wang, K.; Demir, E.; Gürlevik, E.; Fleischmann-Mundt, B.; Brooks, J.; D’Haese, J.G.; Teller, S.; Hecker, A.; et al. Indirect Cholinergic Activation Slows down Pancreatic Cancer Growth and Tumor-Associated Inflammation. J. Exp. Clin. Cancer Res. 2020, 39, 289. [Google Scholar] [CrossRef] [PubMed]
- Johnson, G.; Moore, S.W. Functional Idiotypic Mimicry of an Adhesion- and Differentiation-Promoting Site on Acetylcholinesterase. J. Cell. Biochem. 2004, 91, 999–1009. [Google Scholar] [CrossRef] [PubMed]
- Johnson, G.; Moore, S.W. The Adhesion Function on Acetylcholinesterase Is Located at the Peripheral Anionic Site. Biochem. Biophys. Res. Commun. 1999, 258, 758–762. [Google Scholar] [CrossRef]
- Johnson, G.; Moore, S.W. Cholinesterases Modulate Cell Adhesion in Human Neuroblastoma Cells in Vitro. Int. J. Dev. Neurosci. 2000, 18, 781–790. [Google Scholar] [CrossRef] [PubMed]
- Iwai, N.; Kitajima, K.; Sakai, K.; Kimura, T.; Nakano, T. Alteration of Cell Adhesion and Cell Cycle Properties of ES Cells by an Inducible Dominant Interfering Myb Mutant. Oncogene 2001, 20, 1425–1434. [Google Scholar] [CrossRef] [PubMed]
- Kawashima, K.; Yoshikawa, K.; Fujii, Y.X.; Moriwaki, Y.; Misawa, H. Expression and Function of Genes Encoding Cholinergic Components in Murine Immune Cells. Life Sci. 2007, 80, 2314–2319. [Google Scholar] [CrossRef] [PubMed]
- Bering, B.; Moises, H.W.; Müller, W.E. Muscarinic Cholinergic Receptors on Intact Human Lymphocytes. Properties and Subclass Characterization. Biol. Psychiatry 1987, 22, 1451–1458. [Google Scholar] [CrossRef] [PubMed]
- Kawashima, K.; Fujii, T. Expression of Non-Neuronal Acetylcholine in Lymphocytes and Its Contribution to the Regulation of Immune Function. Front. Biosci. 2004, 9, 2063–2085. [Google Scholar] [CrossRef] [PubMed]
- Razani-Boroujerdi, S.; Boyd, R.T.; Dávila-García, M.I.; Nandi, J.S.; Mishra, N.C.; Singh, S.P.; Pena-Philippides, J.C.; Langley, R.; Sopori, M.L. T Cells Express Alpha7-Nicotinic Acetylcholine Receptor Subunits That Require a Functional TCR and Leukocyte-Specific Protein Tyrosine Kinase for Nicotine-Induced Ca2+ Response. J. Immunol. 2007, 179, 2889–2898. [Google Scholar] [CrossRef]
- Mantovani, A.; Allavena, P.; Sica, A.; Balkwill, F. Cancer-Related Inflammation. Nature 2008, 454, 436–444. [Google Scholar] [CrossRef]
- Lin, W.-W.; Karin, M. A Cytokine-Mediated Link between Innate Immunity, Inflammation, and Cancer. J. Clin. Investig. 2007, 117, 1175–1183. [Google Scholar] [CrossRef] [PubMed]
- Mouton, C.; Ronson, A.; Razavi, D.; Delhaye, F.; Kupper, N.; Paesmans, M.; Moreau, M.; Nogaret, J.-M.; Hendlisz, A.; Gidron, Y. The Relationship between Heart Rate Variability and Time-Course of Carcinoembryonic Antigen in Colorectal Cancer. Auton. Neurosci. 2012, 166, 96–99. [Google Scholar] [CrossRef] [PubMed]
- De Couck, M.; van Brummelen, D.; Schallier, D.; De Grève, J.; Gidron, Y. The Relationship between Vagal Nerve Activity and Clinical Outcomes in Prostate and Non-Small Cell Lung Cancer Patients. Oncol. Rep. 2013, 30, 2435–2441. [Google Scholar] [CrossRef]
- Giese-Davis, J.; Wilhelm, F.H.; Tamagawa, R.; Palesh, O.; Neri, E.; Taylor, C.B.; Kraemer, H.C.; Spiegel, D. Higher Vagal Activity as Related to Survival in Patients with Advanced Breast Cancer: An Analysis of Autonomic Dysregulation. Psychosom. Med. 2015, 77, 346–355. [Google Scholar] [CrossRef]
- Offerhaus, G.J.; Tersmette, A.C.; Huibregtse, K.; van de Stadt, J.; Tersmette, K.W.; Stijnen, T.; Hoedemaeker, P.J.; Vandenbroucke, J.P.; Tytgat, G.N. Mortality Caused by Stomach Cancer after Remote Partial Gastrectomy for Benign Conditions: 40 Years of Follow up of an Amsterdam Cohort of 2633 Postgastrectomy Patients. Gut 1988, 29, 1588–1590. [Google Scholar] [CrossRef] [PubMed]
- Toftgaard, C. Gastric Cancer after Peptic Ulcer Surgery. A Historic Prospective Cohort Investigation. Ann. Surg. 1989, 210, 159–164. [Google Scholar] [CrossRef]
- Ahsberg, K.; Olsson, H.; Staël von Holstein, C. Increased Mortality in Prostate Carcinoma and Smoking-Related Disease after Parietal Cell Vagotomy: A Long-Term Follow-up Study. Scand. J. Gastroenterol. 2009, 44, 947–951. [Google Scholar] [CrossRef]
- Ekbom, A.; Lundegårdh, G.; McLaughlin, J.K.; Nyrén, O. Relation of Vagotomy to Subsequent Risk of Lung Cancer: Population Based Cohort Study. BMJ 1998, 316, 518–519. [Google Scholar] [CrossRef]
- Mantovani, A.; Sica, A.; Sozzani, S.; Allavena, P.; Vecchi, A.; Locati, M. The Chemokine System in Diverse Forms of Macrophage Activation and Polarization. Trends Immunol. 2004, 25, 677–686. [Google Scholar] [CrossRef]
- Mantovani, A.; Bottazzi, B.; Colotta, F.; Sozzani, S.; Ruco, L. The Origin and Function of Tumor-Associated Macrophages. Immunol. Today 1992, 13, 265–270. [Google Scholar] [CrossRef]
- Condeelis, J.; Pollard, J.W. Macrophages: Obligate Partners for Tumor Cell Migration, Invasion, and Metastasis. Cell 2006, 124, 263–266. [Google Scholar] [CrossRef]
- Murdoch, C.; Muthana, M.; Coffelt, S.B.; Lewis, C.E. The Role of Myeloid Cells in the Promotion of Tumour Angiogenesis. Nat. Rev. Cancer 2008, 8, 618–631. [Google Scholar] [CrossRef]
- Fei, R.; Zhang, Y.; Wang, S.; Xiang, T.; Chen, W. A7 Nicotinic Acetylcholine Receptor in Tumor-Associated Macrophages Inhibits Colorectal Cancer Metastasis through the JAK2/STAT3 Signaling Pathway. Oncol. Rep. 2017, 38, 2619–2628. [Google Scholar] [CrossRef]
- Liao, H.-J.; Carpenter, G. Role of the Sec61 Translocon in EGF Receptor Trafficking to the Nucleus and Gene Expression. Mol. Biol. Cell 2007, 18, 1064–1072. [Google Scholar] [CrossRef]
- Byun, H.; Gou, Y.; Zook, A.; Lozano, M.M.; Dudley, J.P. ERAD and How Viruses Exploit It. Front. Microbiol. 2014, 5, 330. [Google Scholar] [CrossRef]

Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2023 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Pérez-Aguilar, B.; Marquardt, J.U.; Muñoz-Delgado, E.; López-Durán, R.M.; Gutiérrez-Ruiz, M.C.; Gomez-Quiroz, L.E.; Gómez-Olivares, J.L. Changes in the Acetylcholinesterase Enzymatic Activity in Tumor Development and Progression. Cancers 2023, 15, 4629. https://doi.org/10.3390/cancers15184629
Pérez-Aguilar B, Marquardt JU, Muñoz-Delgado E, López-Durán RM, Gutiérrez-Ruiz MC, Gomez-Quiroz LE, Gómez-Olivares JL. Changes in the Acetylcholinesterase Enzymatic Activity in Tumor Development and Progression. Cancers. 2023; 15(18):4629. https://doi.org/10.3390/cancers15184629
Chicago/Turabian StylePérez-Aguilar, Benjamín, Jens U. Marquardt, Encarnación Muñoz-Delgado, Rosa María López-Durán, María Concepción Gutiérrez-Ruiz, Luis E. Gomez-Quiroz, and José Luis Gómez-Olivares. 2023. "Changes in the Acetylcholinesterase Enzymatic Activity in Tumor Development and Progression" Cancers 15, no. 18: 4629. https://doi.org/10.3390/cancers15184629
APA StylePérez-Aguilar, B., Marquardt, J. U., Muñoz-Delgado, E., López-Durán, R. M., Gutiérrez-Ruiz, M. C., Gomez-Quiroz, L. E., & Gómez-Olivares, J. L. (2023). Changes in the Acetylcholinesterase Enzymatic Activity in Tumor Development and Progression. Cancers, 15(18), 4629. https://doi.org/10.3390/cancers15184629








