Retroperitoneal Sarcoma Care in 2021
Abstract
Simple Summary
Abstract
1. Introduction
2. Anatomy
3. Histologic Subtypes
4. Genetics, and Familial Syndromes
4.1. Neurofibromatosis Type I (NF1, von Recklinghausen’s Disease)
4.2. TP53-Related Cancer Syndrome (hPT53c, Li–Fraumeni)
4.3. Hereditary Retinoblastoma
5. Additional Risk Factors
5.1. Radiation-Induced Sarcoma (RSTS)
5.2. Other Risk Factors
6. Clinical Presentation
7. Investigations
8. Percutaneous Biopsy
9. Staging and Nomograms
10. Multidisciplinary Care and International Collaborative
11. Management of Primary Retroperitoneal Sarcoma
11.1. Surgery for Locoregional Disease
11.2. Surgical Emergencies
11.3. Metastatic Disease
11.4. Palliative Resection of Local Disease
12. Management of Recurrent Sarcoma
12.1. Locoregional Recurrence
12.2. Metastatic Disease
13. Systemic Therapy
14. Radiation Therapy
15. Molecular Biology and Treatment Selection
16. Conclusions
Author Contributions
Funding
Conflicts of Interest
References
- Board WC of TE. Soft Tissue and Bone Tumours. Available online: https://publications.iarc.fr/Book-And-Report-Series/Who-Classification-Of-Tumours/Soft-Tissue-And-Bone-Tumours-2020 (accessed on 15 May 2021).
- Trans-Atlantic RPS Working Group Management of Primary Retroperitoneal Sarcoma (RPS) in the Adult: A Consensus Approach from the Trans-Atlantic RPS Working Group. Ann. Surg. Oncol. 2015, 22, 256–263. [CrossRef] [PubMed]
- Liles, J.S.; Tzeng, C.-W.D.; Short, J.J.; Kulesza, P.; Heslin, M.J. Retroperitoneal and Intra-Abdominal Sarcoma. Curr. Probl. Surg. 2009, 46, 445–503. [Google Scholar] [CrossRef] [PubMed]
- Tirkes, T.; Sandrasegaran, K.; Patel, A.A.; Hollar, M.A.; Tejada, J.G.; Tann, M.; Akisik, F.M.; Lappas, J.C. Peritoneal and Retroperitoneal Anatomy and Its Relevance for Cross-Sectional Imaging. RadioGraphics 2012, 32, 437–451. [Google Scholar] [CrossRef]
- Coffin, A.; Boulay-Coletta, I.; Sebbag-Sfez, D.; Zins, M. Radioanatomy of the retroperitoneal space. Diagn. Interv. Imaging 2015, 96, 171–186. [Google Scholar] [CrossRef] [PubMed]
- Dingley, B.; Fiore, M.; Gronchi, A. Personalizing surgical margins in retroperitoneal sarcomas: An update. Expert Rev. Anticancer Ther. 2019, 19, 613–631. [Google Scholar] [CrossRef]
- Callegaro, D.; Fiore, M.; Gronchi, A. Personalizing surgical margins in retroperitoneal sarcomas. Expert Rev. Anticancer Ther. 2015, 15, 553–567. [Google Scholar] [CrossRef] [PubMed]
- Sbaraglia, M.; Bellan, E.; Dei Tos, A.P. The 2020 WHO Classification of Soft Tissue Tumours: News and perspectives. Pathologica 2020, 113, 70–84. [Google Scholar] [CrossRef]
- Gronchi, A.; Strauss, D.C.; Miceli, R.; Bonvalot, S.; Swallow, C.J.; Hohenberger, P.; van Coevorden, F.; Rutkowski, P.; Callegaro, D.; Hayes, A.J.; et al. Variability in Patterns of Recurrence after Resection of Primary Retroperitoneal Sarcoma (RPS): A Report on 1007 Patients from the Multi-institutional Collaborative RPS Working Group. Ann. Surg. 2016, 263, 1002–1009. [Google Scholar] [CrossRef]
- Coindre, J.-M.; Mariani, O.; Chibon, F.; Mairal, A.; Somerhausen, N.D.S.A.; Favre-Guillevin, E.; Bui, N.B.; Stoeckle, E.; Hostein, I.; Aurias, A. Most Malignant Fibrous Histiocytomas Developed in the Retroperitoneum Are Dedifferentiated Liposarcomas: A Review of 25 Cases Initially Diagnosed as Malignant Fibrous Histiocytoma. Mod. Pathol. 2003, 16, 256–262. [Google Scholar] [CrossRef]
- Carbone, F.; Pizzolorusso, A.; Di Lorenzo, G.; Di Marzo, M.; Cannella, L.; Barretta, M.; Delrio, P.; Tafuto, S. Multidisciplinary Management of Retroperitoneal Sarcoma: Diagnosis, Prognostic Factors and Treatment. Cancers 2021, 13, 4016. [Google Scholar] [CrossRef]
- Gronchi, A.; Miceli, R.; Allard, M.A.; Callegaro, D.; Le Péchoux, C.; Fiore, M.; Honoré, C.; Sanfilippo, R.; Coppola, S.; Stacchiotti, S.; et al. Personalizing the approach to retroperitoneal soft tissue sarcoma: Histology-specific patterns of failure and postrelapse outcome after primary extended resection. Ann. Surg. Oncol. 2015, 22, 1447–1454. [Google Scholar] [CrossRef] [PubMed]
- Tyler, R.; Lee, M.; Ierodiakonou, V.; Hodson, J.; Taniere, P.; Almond, M.; Ford, S.; Desai, A. Prognostic implications of histological organ involvement in retroperitoneal sarcoma. BJS Open 2021, 5, zrab080. [Google Scholar] [CrossRef] [PubMed]
- Tan, M.C.B.; Brennan, M.F.; Kuk, D.; Agaram, N.P.; Antonescu, C.R.; Qin, L.-X.; Moraco, N.; Crago, A.M.; Singer, S. Histology-based Classification Predicts Pattern of Recurrence and Improves Risk Stratification in Primary Retroperitoneal Sarcoma. Ann. Surg. 2016, 263, 593–600. [Google Scholar] [CrossRef]
- Farid, M.; Ngeow, J. Sarcomas Associated with Genetic Cancer Predisposition Syndromes: A Review. Oncology 2016, 21, 1002–1013. [Google Scholar] [CrossRef] [PubMed]
- Ballinger, M.L.; Goode, D.L.; Ray-Coquard, I.; James, P.A.; Mitchell, G.; Niedermayr, E.; Puri, A.; Schiffman, J.D.; Dite, G.S.; Cipponi, A.; et al. Monogenic and polygenic determinants of sarcoma risk: An international genetic study. Lancet Oncol. 2016, 17, 1261–1271. [Google Scholar] [CrossRef]
- Chan, S.H.; Lim, W.K.; Ishak, N.D.B.; Li, S.-T.; Goh, W.L.; Tan, G.S.; Lim, K.H.; Teo, M.; Young, C.N.C.; Malik, S.; et al. Germline Mutations in Cancer Predisposition Genes are Frequent in Sporadic Sarcomas. Sci. Rep. 2017, 7, 10660. [Google Scholar] [CrossRef]
- Villani, A.; Tabori, U.; Schiffman, J.; Shlien, A.; Beyene, J.; Druker, H.; Novokmet, A.; Finlay, J.; Malkin, D. Biochemical and imaging surveillance in germline TP53 mutation carriers with Li–Fraumeni syndrome: A prospective observational study. Lancet Oncol. 2011, 12, 559–567. [Google Scholar] [CrossRef]
- Frebourg, T.; Genturis, T.E.R.N.; Lagercrantz, S.B.; Oliveira, C.; Magenheim, R.; Evans, D.G. Guidelines for the Li–Fraumeni and heritable TP53-related cancer syndromes. Eur. J. Hum. Genet. 2020, 28, 1379–1386. [Google Scholar] [CrossRef]
- Nieuwenhuis, M.H.; Lefevre, J.H.; Bülow, S.; Järvinen, H.; Bertario, L.; Kernéis, S.; Parc, Y.; Vasen, H.F.A. Family History, Surgery, and APC Mutation Are Risk Factors for Desmoid Tumors in Familial Adenomatous Polyposis: An International Cohort Study. Dis. Colon Rectum 2011, 54, 1229–1234. [Google Scholar] [CrossRef]
- Kaczmar, J.M.; Everett, J.; Ruth, K.; Stoffel, E.M.; Stoll, J.; Kupfer, S. Sarcoma: A Lynch syndrome (LS)-associated malignancy? JCO 2015, 33, 1516. [Google Scholar] [CrossRef]
- Bougeard, G.; Renaux-Petel, M.; Flaman, J.-M.; Charbonnier, C.; Fermey, P.; Belotti, M.; Gauthier-Villars, M.; Stoppa-Lyonnet, D.; Consolino, E.; Brugières, L.; et al. Revisiting Li–Fraumeni Syndrome from TP53 Mutation Carriers. J. Clin. Oncol. 2015, 33, 2345–2352. [Google Scholar] [CrossRef] [PubMed]
- Kleinerman, R.A.; Schonfeld, S.J.; Tucker, M.A. Sarcomas in hereditary retinoblastoma. Clin. Sarcoma Res. 2012, 2, 15. [Google Scholar] [CrossRef] [PubMed]
- Boyd, K.P.; Korf, B.R.; Theos, A. Neurofibromatosis type 1. J. Am. Acad. Dermatol. 2009, 61, 1–16. [Google Scholar] [CrossRef] [PubMed]
- Evans, D.G.; Baser, M.E.; McGaughran, J.; Sharif, S.; Howard, E. A Moran Malignant peripheral nerve sheath tumours in neurofibromatosis 1. J. Med. Genet. 2002, 39, 311–314. [Google Scholar] [CrossRef] [PubMed]
- De Raedt, T.; Brems, H.; Wolkenstein, P.; Vidaud, D.; Pilotti, S.; Perrone, F. Elevated Risk for MPNST in NF1 Microdeletion Patients. Am. J. Hum. Genet. 2003, 72, 1288–1292. [Google Scholar] [CrossRef]
- Daly, M.B.; Pal, T.; Berry, M.P.; Buys, S.S.; Dickson, P.; Domchek, S.M.; Elkhanany, A.; Freidman, A.; Goggins, M.; Hutton, M.L. Genetic/Familial High-Risk Assessment: Breast, Ovarian, and Pancreatic, Version 2.2021, NCCN Clinical Practice Guidelines in Oncology. J. Natl. Compr. Cancer Netw. 2021, 19, 77–102. [Google Scholar] [CrossRef]
- Marees, T.; Moll, A.C.; Imhof, S.M.; de Boer, M.; Ringens, P.J.; Van Leeuwen, F.E. Risk of Second Malignancies in Survivors of Retinoblastoma: More Than 40 Years of Follow-up. JNCI J. Natl. Cancer Inst. 2008, 100, 1771–1779. [Google Scholar] [CrossRef]
- Martland, H. Occupational poisoning in manufacture of luminous watch dials: General review of hazard caused by ingestion of luminous paint, with especial reference to the new jersey cases. J. Am. Med. Assoc. 1929, 92, 466–473. [Google Scholar] [CrossRef]
- Dineen, S.P.; Roland, C.L.; Feig, R.; May, C.; Zhou, S.; Demicco, E.; Al Sannaa, G.; Ingram, D.; Wang, W.; Ravi, V.; et al. Radiation-Associated Undifferentiated Pleomorphic Sarcoma is Associated with Worse Clinical Outcomes than Sporadic Lesions. Ann. Surg. Oncol. 2015, 22, 3913–3920. [Google Scholar]
- Cormier, J.N.; Pollock, R.E. Soft Tissue Sarcomas. CA A Cancer J. Clin. 2004, 54, 94–109. [Google Scholar] [CrossRef]
- Lahat, G.; Lazar, A.; Lev, D. Sarcoma Epidemiology and Etiology: Potential Environmental and Genetic Factors. Surg. Clin. N. Am. 2008, 88, 451–481. [Google Scholar] [CrossRef] [PubMed]
- Thijssens, K.M.J.; van Ginkel, R.J.; Suurmeijer, A.J.H.; Pras, E.; van der Graaf, W.T.A.; Hollander, M. Radiation-induced sarcoma: A challenge for the surgeon. Ann. Surg. Oncol. 2005, 12, 237–245. [Google Scholar] [PubMed]
- Spałek, M.; Czarnecka, A.; Rutkowski, P. The Management of Radiation-Induced Sarcomas: A Cohort Analysis from a Sarcoma Tertiary Center. J. Clin. Med. 2021, 10, 694. [Google Scholar] [CrossRef]
- Diessner, B.J.; Weigel, B.J.; Murugan, P.; Zhang, L.; Poynter, J.N.; Spector, L.G. Racial and Ethnic Differences in Sarcoma Incidence Are Independent of Census-Tract Socioeconomic Status. Cancer Epidemiol. Biomark. Prev. 2020, 29, 2141–2148. [Google Scholar] [CrossRef]
- Russell, M.; Mackay, G.; Hooshyari, A.; Meyer, J.A.; O’Hagan, L.; Cranshaw, I. Racial and ethnic differences in abdominal soft tissue sarcoma incidence in New Zealand: A retrospective audit. ANZ J. Surg. 2021, 92, 162–166. [Google Scholar] [CrossRef]
- Boyle, E.A.; Elliott, J.A.; McIntyre, T.V.; Barnes, M.E.; Donlon, N.E.; Umair, M.; Gillis, A.E.; Ridgway, P.F. Body composition is associated with operative and oncologic outcomes in the management of retroperitoneal and trunk soft tissue sarcoma. Am. J. Surg. 2021, in press. [Google Scholar] [CrossRef]
- Rives-Lange, C.; Poghosyan, T.; Dariane, C.; Douard, R.; Mongeois, E.; Boudaoud, A.A.; Barsamian, C.; Radu, A.; Lagorce, C.; Verkarre, V.; et al. Delayed retroperitoneal liposarcoma diagnosis and management in a patient with massive obesity. Eur. J. Clin. Nutr. 2021, 75, 1520–1522. [Google Scholar] [CrossRef]
- Recinos, L.M.; Mohapatra, S.; Santharaman, A.; Patel, N.; Broder, A. Retroperitoneal Liposarcoma Presenting with Malignant Gastric Outlet Obstruction and Acute Pancreatitis: A Case Report. Cureus 2021, 13, e12775. [Google Scholar] [CrossRef] [PubMed]
- Arakawa, Y.; Yoshioka, K.; Kamo, H.; Kawano, K.; Yamaguchi, T.; Sumise, Y.; Okitsu, N.; Ikeyama, S.; Morimoto, K.; Nakai, Y. Huge retroperitoneal dedifferentiated liposarcoma presented as acute pancreatitis: Report of a case. J. Med. Investig. 2013, 60, 164–168. [Google Scholar] [CrossRef][Green Version]
- Goh, T.L.; Lastik, J.; Schmigylski, R.; Murray, I.A. Ischaemic colitis secondary to retroperitoneal liposarcoma. BMJ Case Rep. 2021, 14, e245595. [Google Scholar] [CrossRef]
- Vishnoi, J.R.; Jain, A.; Misra, S.; Pareek, P.; Rao, M.; Sureka, B.; Puranik, A. Paraneoplastic Syndrome Associated with the Retroperitoneal Dedifferentiated Liposarcoma: An Atypical Presentation and Review of the Literature. Indian J. Surg. Oncol. 2019, 10, 703–707. [Google Scholar]
- Messiou, C.; Morosi, C. Imaging in retroperitoneal soft tissue sarcoma. J. Surg. Oncol. 2017, 117, 25–32. [Google Scholar] [CrossRef] [PubMed]
- White, L.M.; Wunder, J.S.; Bell, R.S.; O’Sullivan, B.; Catton, C.; Ferguson, P.; Blackstein, M.; Kandel, R.A. Histologic assessment of peritumoral edema in soft tissue sarcoma. Int. J. Radiat. Oncol. 2005, 61, 1439–1445. [Google Scholar] [CrossRef] [PubMed]
- Ioannidis, J.P.A.; Lau, J. 18F-FDG PET for the diagnosis and grading of soft-tissue sarcoma: A meta-analysis. J. Nucl. Med. 2003, 44, 717–724. [Google Scholar] [PubMed]
- Wakamatsu, T.; Imura, Y.; Tamiya, H.; Yagi, T.; Yasuda, N.; Nakai, S.; Nakai, T.; Outani, H.; Hamada, K.; Kakunaga, S. 18F-Fluorodeoxyglucose Positron Emission Tomography Is Useful in the Evaluation of Prognosis in Retroperitoneal Sarcoma. Cancers 2021, 13, 4611. [Google Scholar] [CrossRef]
- Alieva, M.; Van Rheenen, J.; Broekman, M.L.D. Potential impact of invasive surgical procedures on primary tumor growth and metastasis. Clin. Exp. Metastasis 2018, 35, 319–331. [Google Scholar] [CrossRef]
- Berger-Richardson, D.; Burtenshaw, S.M.; Ibrahim, A.M.; Gladdy, R.A.; Auer, R.; Beecroft, R.; Dickson, B.C.; Purgina, B.; Ambacher, K.; Nessim, C.; et al. Early and Late Complications of Percutaneous Core Needle Biopsy of Retroperitoneal Tumors at Two Tertiary Sarcoma Centers. Ann. Surg. Oncol. 2019, 26, 4692–4698. [Google Scholar] [CrossRef]
- Berger-Richardson, D.; Swallow, C.J. Needle tract seeding after percutaneous biopsy of sarcoma: Risk/benefit considerations. Cancer 2016, 123, 560–567. [Google Scholar] [CrossRef]
- Van Houdt, W.J.; Schrijver, A.M.; Cohen-Hallaleh, R.B.; Memos, N.; Fotiadis, N.; Smith, M.J.; Hayes, A.J.; Van Coevorden, F.; Strauss, D.C. Needle tract seeding following core biopsies in retroperitoneal sarcoma. Eur. J. Surg. Oncol. 2017, 43, 1740–1745. [Google Scholar] [CrossRef]
- Wilkinson, M.J.; Martin, J.L.; Khan, A.A.; Hayes, A.J.; Thomas, J.M.; Strauss, D.C. Percutaneous Core Needle Biopsy in Retroperitoneal Sarcomas Does Not Influence Local Recurrence or Overall Survival. Ann. Surg. Oncol. 2015, 22, 853–858. [Google Scholar] [CrossRef]
- Straker, R.J.; Song, Y.; Shannon, A.B.; Marcinak, C.T.; Miura, J.T.; Fraker, D.L.; Karakousis, G.C. Preoperative Biopsy in Patients with Retroperitoneal Sarcoma: Usage and Outcomes in a National Cohort. Ann. Surg. Oncol. 2021, 28, 6868–6879. [Google Scholar] [CrossRef]
- Casali, P.G.; Abecassis, N.; Bauer, S.; Biagini, R.; Bielack, S.; Bonvalot, S.; Boukovinas, I.; Bovee, J.V.M.G.; Brodowicz, T.; et al. Soft tissue and visceral sarcomas: ESMO–EURACAN Clinical Practice Guidelines for diagnosis, treatment and follow-up. Ann. Oncol. 2018, 29, 51–67. [Google Scholar] [CrossRef]
- Swallow, C.J.; Strauss, D.C.; Bonvalot, S.; Rutkowski, P.; Desai, A.; Gladdy, R.A.; Gonzalez, R.; Gyorki, D.E.; Fairweather, M.; van Houdt, W.J.; Stoeckle, E.; et al. Management of Primary Retroperitoneal Sarcoma (RPS) in the Adult: An Updated Consensus Approach from the Transatlantic Australasian RPS Working Group. Ann. Surg. Oncol. 2021, 14, 7873–7888. [Google Scholar] [CrossRef] [PubMed]
- von Mehren, M.; Kane, J.M.; Bui, M.M.; Choy, E.; Connelly, M.; Dry, S.; Ganjoo, K.N.; George, S.; Gonzalez, R.J.; Heslin, M.J.; et al. NCCN Guidelines Insights: Soft Tissue Sarcoma, Version 1.2021. J. Natl. Compr. Cancer Netw. 2020, 18, 1604–1612. [Google Scholar]
- Amin, M.B.; Edge, S.B. American Joint Committee on Cancer. In AJCC Cancer Staging Manual, 8th ed.; Springer: Cham, Switzerland, 2017. [Google Scholar]
- Huggett, B.D.; Cates, J.M.M. The Vanderbilt staging system for retroperitoneal sarcoma: A validation study of 6857 patients from the National Cancer Database. Mod. Pathol. 2018, 32, 539–545. [Google Scholar] [CrossRef] [PubMed]
- Tattersall, H.L.; Callegaro, D.; Ford, S.J.; Gronchi, A. Staging, nomograms and other predictive tools in retroperitoneal soft tissue sarcoma. Chin. Clin. Oncol. 2018, 7, 36. [Google Scholar] [CrossRef]
- Ye, L.; Hu, C.; Wang, C.; Yu, W.; Liu, F.; Chen, Z. Nomogram for predicting the overall survival and cancer-specific survival of patients with extremity liposarcoma: A population-based study. BMC Cancer 2020, 20, 889. [Google Scholar] [CrossRef] [PubMed]
- Callegaro, D.; Miceli, R.; Gladdy, R.A. Prognostic models for RPS patients—Attempting to predict patient outcomes. J. Surg. Oncol. 2018, 117, 69–78. [Google Scholar] [CrossRef]
- Zhuang, A.; Wu, Q.; Tong, H.; Zhang, Y.; Lu, W. Development and Validation of a Nomogram for Predicting Recurrence-Free Survival of Surgical Resected Retroperitoneal Liposarcoma. Cancer Manag. Res. 2021, 13, 6633–6639. [Google Scholar] [CrossRef]
- Kattan, M.W.; Leung, D.H.Y.; Brennan, M.F. Postoperative Nomogram for 12-Year Sarcoma-Specific Death. JCO 2002, 20, 791–796. [Google Scholar] [CrossRef]
- Gronchi, A.; Miceli, R.; Shurell, E.; Eilber, F.C.; Eilber, F.R.; Anaya, D.A.; Kattan, M.; Honoré, C.; Lev, D.C.; Colombo, C.; et al. Outcome Prediction in Primary Resected Retroperitoneal Soft Tissue Sarcoma: Histology-Specific Overall Survival and Disease-Free Survival Nomograms Built on Major Sarcoma Center Data Sets. J. Clin. Oncol. 2013, 31, 1649–1655. [Google Scholar] [CrossRef]
- Raut, C.P.; Miceli, R.; Strauss, D.C.; Swallow, C.J.; Hohenberger, P.; Van Coevorden, F.; Rutkowski, P.; Fiore, M.; Callegaro, D.; Casali, P.G.; et al. External validation of a multi-institutional retroperitoneal sarcoma nomogram. Cancer 2016, 122, 1417–1424. [Google Scholar] [CrossRef] [PubMed]
- SARCULATOR. Available online: https://www.sarculator.com/ (accessed on 15 May 2021).
- Raut, C.P.; Callegaro, D.; Miceli, R.; Barretta, F.; Rutkowski, P.; Blay, J.-Y.; Lahat, G.; Strauss, D.; Gonzalez, R.; Ahuja, N.; et al. Predicting Survival in Patients Under-going Resection for Locally Recurrent Retroperitoneal Sarcoma: A Study and Novel Nomogram from TARPSWG. Clin. Cancer Res. 2019, 25, 2664–2671. [Google Scholar]
- Blay, J.-Y.; Honoré, C.; Stoeckle, E.; Meeus, P.; Jafari, M.; Gouin, F.; Anract, P.; Ferron, G.; Rochwerger, A.; Ropars, M.; et al. Surgery in reference centers improves survival of sarcoma patients: A nationwide study. Ann. Oncol. 2019, 30, 1143–1153. [Google Scholar] [CrossRef] [PubMed]
- Jcf, W.; M von, S.; Cj, P.; Tr, G. Incidence, Treatment and Outcome of Patients with Retroperitoneal Soft-Tissue Sarcoma in Switzerland 2005–2015: A Population-Based Analysis. World J. Surg. 2022, 46, 461–468. [Google Scholar]
- Villano, A.M.; Zeymo, A.; Chan, K.S.; Unger, K.R.; Shara, N.; Al-Refaie, W.B. Variations in Retroperitoneal Soft Tissue Sarcoma Outcomes by Hospital Type: A National Cancer Database Analysis. JCO Oncol. Pract. 2020, 16, e991–e1003. [Google Scholar] [CrossRef]
- Schmitz, R.; Adam, M.A.; Blazer, D.G. Overcoming a travel burden to high-volume centers for treatment of retroperitoneal sarcomas is associated with improved survival. World J. Surg. Onc. 2019, 17, 1–8. [Google Scholar] [CrossRef]
- Villano, A.M.; Zeymo, A.; Chan, K.S.; Shara, N.; Al-Refaie, W.B. Identifying the Minimum Volume Threshold for Retroperitoneal Soft Tissue Sarcoma Resection: Merging National Data with Consensus Expert Opinion. J. Am. Coll. Surgeons. 2020, 230, 151–160. [Google Scholar] [CrossRef]
- Callegaro, D.; Raut, C.P.; Swallow, C.J.; Gronchi, A. Retroperitoneal sarcoma: The Transatlantic Australasian Retroperitoneal Sarcoma Working Group Program. Curr. Opin. Oncol. 2021, 33, 301–308. [Google Scholar] [CrossRef]
- Callegaro, D.; Swallow, C.J. ASO Author Reflections: Every Step Counts: Improved Survival of Retroperitoneal Sarcoma Patients During the Past 15 Years. Ann. Surg. Oncol. 2021, 28, 1710–1711. [Google Scholar] [CrossRef]
- Gronchi, A.; Lo Vullo, S.; Fiore, M.; Mussi, C.; Stacchiotti, S.; Collini, P. Aggressive surgical policies in a retrospectively reviewed single-institution case series of retroperitoneal soft tissue sarcoma patients. J. Clin. Oncol. 2009, 27, 24–30. [Google Scholar] [CrossRef]
- Bonvalot, S.; Rivoire, M.; Castaing, M.; Stoeckle, E.; Le Cesne, A.; Blay, J.Y.; Laplanche, A. Primary Retroperitoneal Sarcomas: A Multivariate Analysis of Surgical Factors Associated with Local Control. J. Clin. Oncol. 2009, 27, 31–37. [Google Scholar] [CrossRef] [PubMed]
- Bonvalot, S.; Raut, C.P.; Pollock, R.E.; Rutkowski, P.; Strauss, D.C.; Hayes, A.J.; Van Coevorden, F.; Fiore, M.; Stoeckle, E.; Hohenberger, P.; et al. Technical Considerations in Surgery for Retroperitoneal Sarcomas: Position Paper from E-Surge, a Master Class in Sarcoma Surgery, and EORTC–STBSG. Ann. Surg. Oncol. 2012, 19, 2981–2991. [Google Scholar]
- Nizri, E.; Fiore, M.; Barretta, F.; Colombo, C.; Radaelli, S.; Callegaro, D.; Sanfilippo, R.; Sangalli, C.; Collini, P.; Stacchiotti, S.; et al. Intraperitoneal Invasion of Retroperitoneal Sarcomas: A Risk Factor for Dismal Prognosis. Ann. Surg. Oncol. 2019, 26, 3535–3541. [Google Scholar]
- Cananzi, F.C.M.; Ruspi, L.; Fiore, M.; Sicoli, F.; Quagliuolo, V.; Gronchi, A. Major vascular resection in retroperitoneal sarcoma surgery. Surgery 2021, 170, 848–856. [Google Scholar] [CrossRef]
- MacNeill, A.J.; Gronchi, A.; Miceli, R.; Bonvalot, S.; Swallow, C.J.; Hohenberger, P.; Van Coevorden, F.; Rutkowski, P.; Callegaro, D.; Hayes, A.J.; et al. Postoperative Morbidity after Radical Resection of Primary Retroperitoneal Sarcoma: A Report from the Transatlantic RPS Working Group. Ann. Surg. 2018, 267, 959–964. [Google Scholar]
- Nessim, C.; Raut, C.P.; Callegaro, D.; Barretta, F.; Miceli, R.; Fairweather, M.; Rutkowski, P.; Blay, J.Y.; Strauss, D.; Gonzalez, R.; et al. Postoperative Morbidity after Resection of Recurrent Retroperitoneal Sarcoma: A Report from the Transatlantic Australasian RPS Working Group (TARPSWG). Ann. Surg. Oncol. 2021, 28, 2705–2714. [Google Scholar]
- Bagaria, S.P.; Swallow, C.; Suraweera, H.; Raut, C.P.; Fairweather, M.; Cananzi, F.; Quagliuolo, V.; Grignani, G.; Hompes, D.; Ford, S.J.; et al. Morbidity and Outcomes after Distal Pancreatectomy for Primary Retroperitoneal Sarcoma: An Analysis by the Trans-Atlantic Australasian Retroperitoneal Sarcoma Working Group. Ann. Surg. Oncol. 2021, 28, 6882–6889. [Google Scholar]
- Fairweather, M.; Lyu, H.; Conti, L.; Callegaro, D.; Radaelli, S.; Fiore, M.; Ng, D.; Swallow, C.; Gronchi, A.; Raut, C.P. Postnephrectomy outcomes following en bloc resection of primary retroperitoneal sarcoma: Multicentre study. Br. J. Surg. 2021, 109, 165–168. [Google Scholar] [CrossRef]
- Cruz, S.M.; Basmaci, U.N.; Bateni, C.P.; Darrow, M.A.; Judge, S.J.; Monjazeb, A.M.; Thorpe, S.W.; Humphries, M.D.; Canter, R.J. Surgical and oncologic outcomes following arterial resection and reconstruction for advanced solid tumors. J. Surg. Oncol. 2021, 124, 1251–1260. [Google Scholar]
- Spolverato, G.; Chiminazzo, V.; Lorenzoni, G.; Fiore, M.; Radaelli, S.; Sanfilippo, R.; Sangalli, C.; Barisella, M.; Callegaro, D.; Gronchi, A. Oncological outcomes after major vascular resections for primary retroperitoneal liposarcoma. Eur. J. Surg. Oncol. (EJSO) 2021, 47, 3004–3010. [Google Scholar] [CrossRef]
- Tirotta, F.; Parente, A.; Hodson, J.; Desai, A.; Almond, L.M.; Ford, S.J. Cumulative Burden of Postoperative Complications in Patients Undergoing Surgery for Primary Retroperitoneal Sarcoma. Ann. Surg. Oncol. 2021, 28, 7939–7949. [Google Scholar] [CrossRef]
- Samà, L.; Tzanis, D.; Bouhadiba, T.; Bonvalot, S. Emergency Retroperitoneal Sarcoma Surgery for Preoperative Rupture and Hemoperitoneum: A Case Report. Cureus 2021, 13, e13936. [Google Scholar] [CrossRef] [PubMed]
- Perera, G.B.; Wilson, S.E.; Barie, P.S.; Butler, J.A. Duodenocaval fistula: A late complication of retroperitoneal irradiation and vena cava replacement. Ann. Vasc. Surg. 2004, 18, 52–58. [Google Scholar] [CrossRef] [PubMed]
- Kopplin, L.; Kim, J. Retroperitoneal sarcoma: A rare cause of intestinal perforation in two cases. J. Surg. Case Rep. 2011, 2011, 3. [Google Scholar] [CrossRef]
- Attard, J.; Azzopardi, C.; Cortis, K.; Abela, J.E. A case of a large, painless retroperitoneal mass causing hydronephrosis and biliary obstruction. Case Rep. 2015, 2015, bcr2015212422. [Google Scholar]
- Trans-Atlantic Retroperitoneal Sarcoma Working Group (TARPSWG). Management of metastatic retroperitoneal sarcoma: A consensus approach from the Trans-Atlantic Retroperitoneal Sarcoma Working Group (TARPSWG). Ann. Oncol. 2018, 29, 857–871. [Google Scholar] [CrossRef]
- Zerhouni, S.; Coevorden, F.V.; Swallow, C.J. The role and outcomes of palliative surgery for retroperitoneal sarcoma. J. Surg. Oncol. 2018, 117, 105–110. [Google Scholar] [CrossRef]
- Yeh, J.J.; Singer, S.; Brennan, M.F.; Jaques, D.P. Effectiveness of Palliative Procedures for Intra-Abdominal Sarcomas. Ann. Surg. Oncol. 2005, 12, 1084–1089. [Google Scholar] [CrossRef]
- Thalji, S.Z.; Tsai, S.; Gamblin, T.C.; Clarke, C.; Christians, K.; Charlson, J.; Ethun, C.G.; Poultsides, G.; Grignol, V.P.; Roggin, K.K.; et al. Outcomes of palliative-intent surgery in retroperitoneal sarcoma—Results from the US Sarcoma Collaborative. J. Surg. Oncol. 2020, 121, 1140–1147. [Google Scholar] [CrossRef]
- Trans-Atlantic RPS Working Group. Management of Recurrent Retroperitoneal Sarcoma (RPS) in the Adult: A Consensus Approach from the Trans-Atlantic RPS Working Group. Ann. Surg. Oncol. 2016, 23, 3531–3540. [Google Scholar]
- Gyorki, D.E.; Brennan, M.F. Management of recurrent retroperitoneal sarcoma. J. Surg. Oncol. 2014, 109, 53–59. [Google Scholar] [CrossRef]
- Singer, S.; Antonescu, C.R.; Riedel, E.; Brennan, M.F. Histologic Subtype and Margin of Resection Predict Pattern of Recurrence and Survival for Retroperitoneal Liposarcoma. Ann. Surg. 2003, 238, 358–371. [Google Scholar] [CrossRef] [PubMed]
- MacNeill, A.J.; Miceli, R.; Strauss, D.C.; Bonvalot, S.; Hohenberger, P.; Van Coevorden, F.; Rutkowski, P.; Callegaro, D.; Hayes, A.J.; Honoré, C.; et al. Post-relapse outcomes after primary extended resection of retroperitoneal sarcoma: A report from the Trans-Atlantic RPS Working Group. Cancer 2017, 123, 1971–1978. [Google Scholar] [CrossRef] [PubMed]
- Nessim, C.; Raut, C.P.; Callegaro, D.; Barretta, F.; Miceli, R.; Fairweather, M.; Blay, J.-Y.; Strauss, D.; Rutkowski, P.; Ahuja, N.; et al. Analysis of Differentiation Changes and Outcomes at Time of First Recurrence of Retroperitoneal Liposarcoma by Transatlantic Australasian Retroperitoneal Sarcoma Working Group (TARPSWG). Ann. Surg. Oncol. 2021, 28, 7854–7863. [Google Scholar] [CrossRef] [PubMed]
- Ng, D.; Swallow, C.J. Decision-making for palliative versus curative intent treatment of retroperitoneal sarcoma (RPS). Chin. Clin. Oncol. 2018, 7, 40–40. [Google Scholar] [CrossRef] [PubMed]
- van Dalen, T.; Hoekstra, H.J.; van Geel, A.N.; van Coevorden, F.; Albus-Lutter, C.; Slootweg, P.J. Locoregional recurrence of retroperitoneal soft tissue sarcoma: Second chance of cure for selected patients. Eur. J. Surg. Oncol. 2001, 27, 564–568. [Google Scholar] [CrossRef]
- Evaluation of Preoperative Chemotherapy or Radiation and Overall Survival in Patients with Nonmetastatic, Resectable Retroperitoneal Sarcoma|Oncology|JAMA Network Open|JAMA Network. Available online: https://jamanetwork.com/journals/jamanetworkopen/fullarticle/2772797 (accessed on 25 July 2021).
- Almond, L.M.; Gronchi, A.; Strauss, D.; Jafri, M.; Ford, S.; Desai, A. Neoadjuvant and adjuvant strategies in retroperitoneal sarcoma. Eur. J. Surg. Oncol. 2018, 44, 571–579. [Google Scholar] [CrossRef]
- Bachmann, R.; Eckert, F.; Gelfert, D.; Strohäker, J.; Beltzer, C.; Ladurner, R. Perioperative strategy and outcome in giant retroperitoneal dedifferentiated liposarcoma—Results of a retrospective cohort study. World J. Surg. Oncol. 2020, 18, 1–7. [Google Scholar] [CrossRef]
- Issels, R.D.; Lindner, L.H.; Verweij, J.; Wessalowski, R.; Reichardt, P.; Wust, P.; Ghadjar, P.; Hohenberger, P.; Angele, M.; Salat, C.; et al. Effect of Neoadjuvant Chemo-therapy Plus Regional Hyperthermia on Long-term Outcomes Among Patients with Localized High-Risk Soft Tissue Sarcoma: The EORTC 62961-ESHO 95 Randomized Clinical Trial. JAMA Oncol. 2018, 4, 483. [Google Scholar]
- Birdi, H.K.; Jirovec, A.; Cortés-Kaplan, S.; Werier, J.; Nessim, C.; Diallo, J.-S.; Ardolino, M. Immunotherapy for sarcomas: New frontiers and unveiled opportunities. J. Immunother. Cancer 2021, 9, e001580. [Google Scholar] [CrossRef]
- Sindelar, W.F.; Kinsella, T.J.; Chen, P.W.; Delaney, T.F.; Tepper, J.E.; Rosenberg, S.A.; Glatstein, E. Intraoperative radiotherapy in retroperitoneal sarcomas. Final results of a prospective, randomized, clinical trial. Arch. Surg. 1993, 128, 402–410. [Google Scholar] [CrossRef]
- Bonvalot, S.; Gronchi, A.; Le Péchoux, C.; Swallow, C.J.; Strauss, D.; Meeus, P.; van Coevorden, F.; Stoldt, S.; Stoeckle, E.; Rutkowski, P.; et al. Preoperative radiotherapy plus surgery versus surgery alone for patients with primary retroperitoneal sarcoma (EORTC-62092: STRASS): A multi-centre, open-label, randomised, phase 3 trial. Lancet Oncol. 2020, 21, 1366–1377. [Google Scholar]
- Li, X.; Wu, T.; Xiao, M.; Wu, S.; Min, L.; Luo, C. Adjuvant therapy for retroperitoneal sarcoma: A meta-analysis. Radiat. Oncol. 2021, 16, 1–11. [Google Scholar] [CrossRef]
- Littau, M.J.; Kulshrestha, S.; Bunn, C.; Agnew, S.; Sweigert, P.; Luchette, F.A.; Baker, M.S. The importance of the margin of resection and radiotherapy in retroperitoneal liposarcoma. Am. J. Surg. 2020, 221, 554–560. [Google Scholar] [CrossRef]
- Lam, M.B.; Baldini, E.H.; Reijers, S.J.M.; Haas, R.L.; DeLaney, T.F. Role of Radiation Therapy for Newly Diagnosed Retroperitoneal Sarcoma. Curr. Treat. Options Oncol. 2021, 22, 75. [Google Scholar] [CrossRef] [PubMed]
- Salerno, K.E.; Alektiar, K.M.; Baldini, E.H.; Bedi, M.; Bishop, A.J.; Bradfield, L.; Chung, P.; DeLaney, T.F.; Folpe, A.; Kane, J.M.; et al. Radiation Therapy for Treatment of Soft Tissue Sarcoma in Adults: Executive Summary of an ASTRO Clinical Practice Guideline. Pract. Radiat. Oncol. 2021, 11, 339–351. [Google Scholar] [CrossRef] [PubMed]
- Grünewald, T.G.; Alonso, M.; Avnet, S.; Banito, A.; Burdach, S.; Cidre-Aranaz, F.; Di Pompo, G.; Distel, M.; Dorado-Garcia, H.; Garcia-Castro, J.; et al. Sarcoma treatment in the era of molecular medicine. EMBO Mol. Med. 2020, 12, e11131. [Google Scholar] [CrossRef]
- Pillozzi, S.; Bernini, A.; Palchetti, I.; Crociani, O.; Antonuzzo, L.; Campanacci, D.; Scoccianti,, G. Soft Tissue Sarcoma: An Insight on Biomarkers at Molecular, Metabolic and Cellular Level. Cancers 2021, 13, 3044. [Google Scholar]
- Sharma, S.R.; Paonessa, N.E.; Casadei, L.; Costas De Faria, F.; Pollock, R.E.; Grignol, V. Clinical biomarkers in soft tissue sarcoma A comprehensive review of current soft tissue sarcoma biomarkers. J. Surg. Oncol. 2022, 125, 239–245. [Google Scholar] [CrossRef]
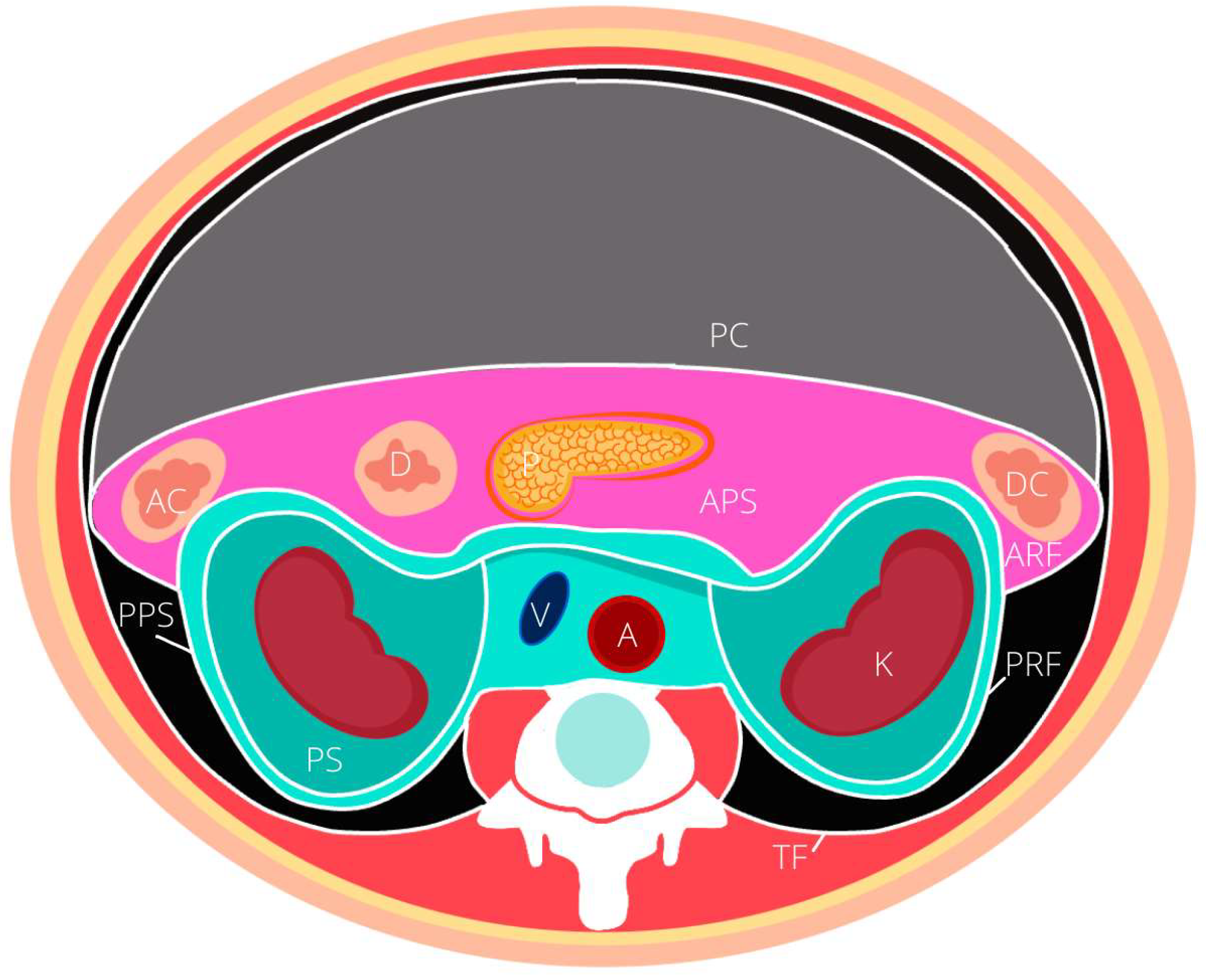

| Compartment | Space | Borders | Contents |
|---|---|---|---|
| Greater Vessel | Greater Vessel Space | Superior: posterior mediastinum Posterior: vertebral bodies, psoas muscle Lateral: perirenal spaces and ureters | Abdominal aorta Inferior vena cava Lymphatics |
| Posterior | Posterior Space | Anterior: transversalis fascia | Psoas muscle |
| Lateral | Anterior Pararenal Space (APS) | Anterior: Parietal peritoneum and intraperitoneal space Posterior: anterior renal fascia and perirenal space | Pancreas head and neck Duodenum (parts 2–4) Ascending Colon Descending Colon |
| Perirenal Space (PS) | Superior: diaphragm Anterior: Gerotas fascia and anterior pararenal space Posterior: Zuckerkandl fascia and posterior pararenal space | Adrenal gland Kidney Renal hilum with ureter, artery and vein | |
| Posterior Pararenal Space (PPS) | Lateral: lateroconal fascia Anterior: posterior renal fascia and perirenal space Posterior: Transversalis fascia | No major organs Fat pad ventral to quadratus lumborum |
| Familial Syndromes | Gene Mutation (Chromosome) | Associated Sarcomas |
|---|---|---|
| Neurofibromatosis type I (Von Recklinghausen’s disease) | NF1 (17q11.2) | GIST, RMS, MPNST |
| TP53-related cancer syndrome (Li–Fraumeni) | TP53 (17q13.1, 1q23), CHEK2 (22q12) | RMS, LMS, LPS, FHT [22] |
| Hereditary retinoblastoma | RB1 (13q14) | Bone and STS [23] |
| Familial rhabdoid predisposition syndrome I | SMARB1/INI1 (22q11.33) | MRT |
| Familial rhabdoid predisposition syndrome II | SMARCA4 (19q13.2) | MRT |
| Hereditary leiomyomatosis and renal cell cancer | FH (1q42) | Uterine LMS |
| Multiple osteochrondromas | EXT1 (8q24), EXT2 (11p11) | Chrondrosarcoma |
| Rubinstein–Taybi | CREBBP (16p13.1) | LMS |
| Tuberous sclerosis | TSC1 (9q34), TSC2 (16p13.3), TSC3 (12q22–24.1) | PEComa, chordoma |
| Mafucci syndrome | IDH1 (2q34), IDH2 (15q26.1) | Angiosarcoma, chondrosarcoma |
| Nijmegen breakage syndrome | NBN (8q21.3) | RMS |
| Sarcoma Subtype | Pattern of Spread | Mechanism of Failure (5-Year %) | Surgical Implications |
|---|---|---|---|
| WDLPS | Adipose infiltration Multilobulated Indistinct borders | LR (19–39%) >> MD (0%) | Extended en-bloc resection requiring ipsilateral retroperitoneal fat resection |
| DDLPS | Adipose and Visceral infiltration Multilobulated Indistinct borders | G2: LR (44%) > MD (10%) G3: LR (33%) << MD (44%) | Extended en-bloc resection requiring ipsilateral retroperitoneal fat resection |
| LMS | Distinct borders | LR (6–16%) << MD (55–56%) | En-bloc resection with vascular structures May preserve adjacent critical structures |
| MPNST | Distinct borders | LR (20–35%) > MD (12–13%) | En-bloc resection with associated neurovascular structures |
| SFT | Distinct borders | LR (4–8%) > MD (17%) | En-bloc resection May preserve adjacent critical structures |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2022 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Schmitz, E.; Nessim, C. Retroperitoneal Sarcoma Care in 2021. Cancers 2022, 14, 1293. https://doi.org/10.3390/cancers14051293
Schmitz E, Nessim C. Retroperitoneal Sarcoma Care in 2021. Cancers. 2022; 14(5):1293. https://doi.org/10.3390/cancers14051293
Chicago/Turabian StyleSchmitz, Erika, and Carolyn Nessim. 2022. "Retroperitoneal Sarcoma Care in 2021" Cancers 14, no. 5: 1293. https://doi.org/10.3390/cancers14051293
APA StyleSchmitz, E., & Nessim, C. (2022). Retroperitoneal Sarcoma Care in 2021. Cancers, 14(5), 1293. https://doi.org/10.3390/cancers14051293







