Current and Future Tools for Diagnosis of Kaposi’s Sarcoma
Simple Summary
Abstract
1. Introduction
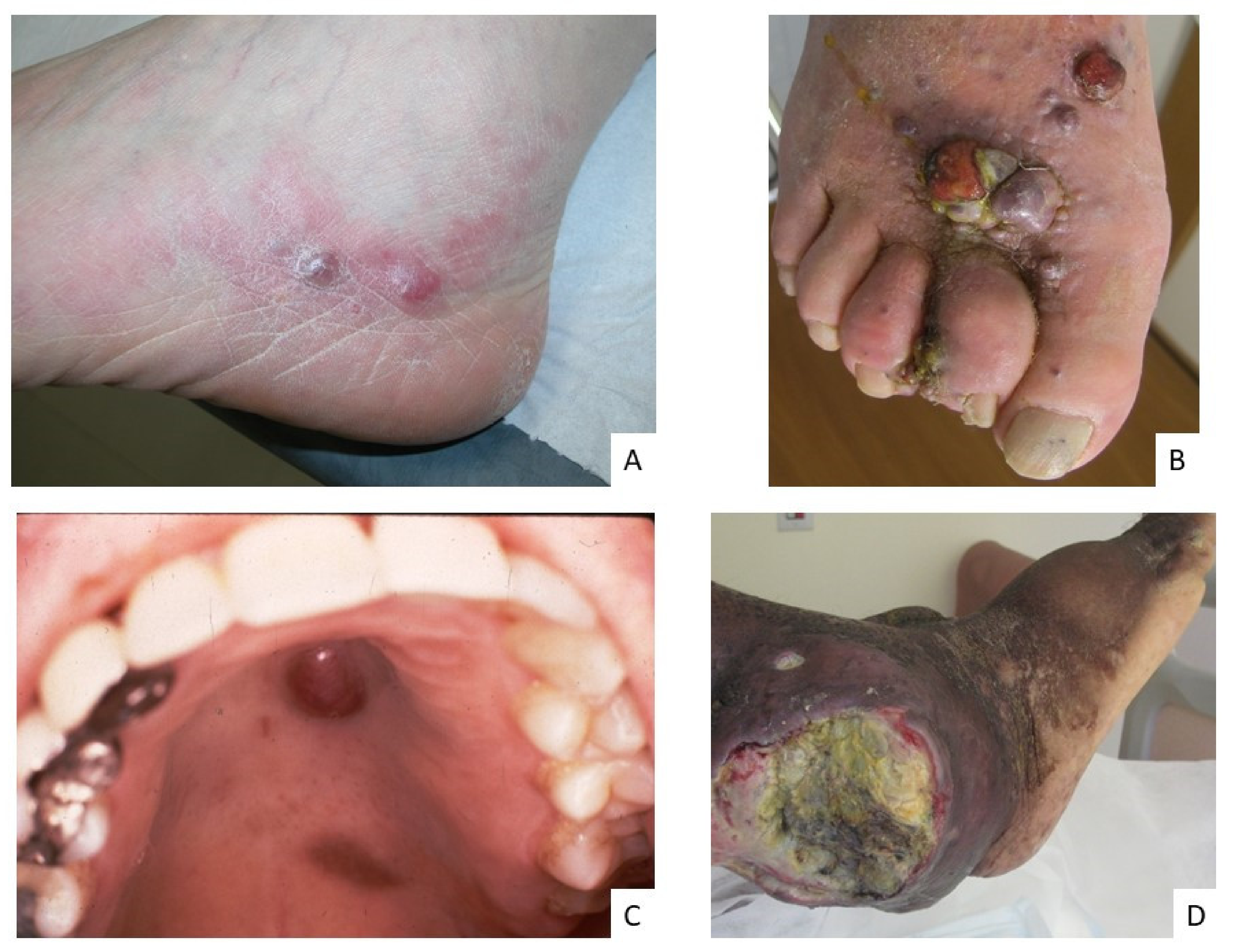
2. Staging of Kaposi’s Sarcoma
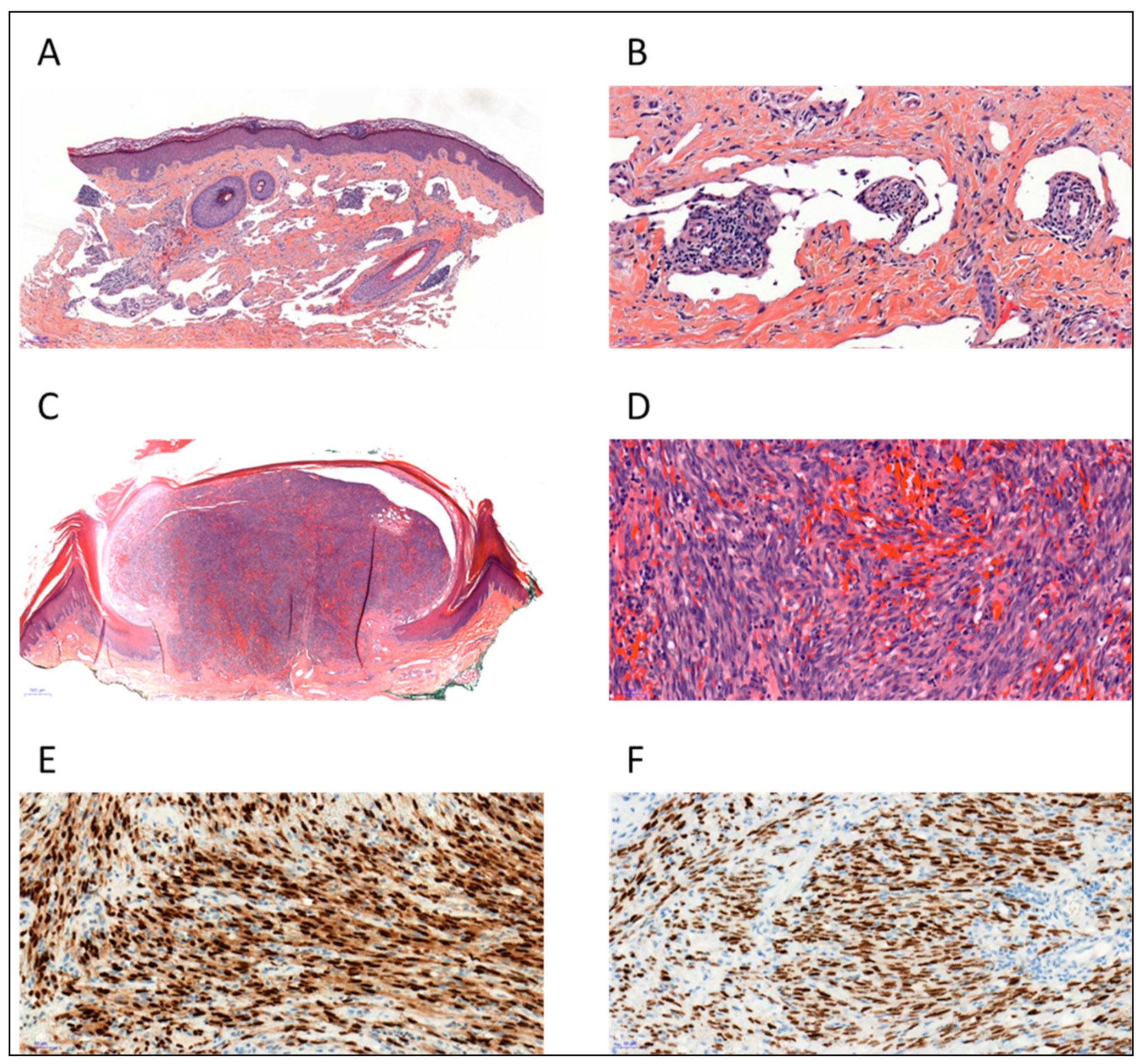
3. Histopathological Characteristics
4. Biological Diagnostic Tools
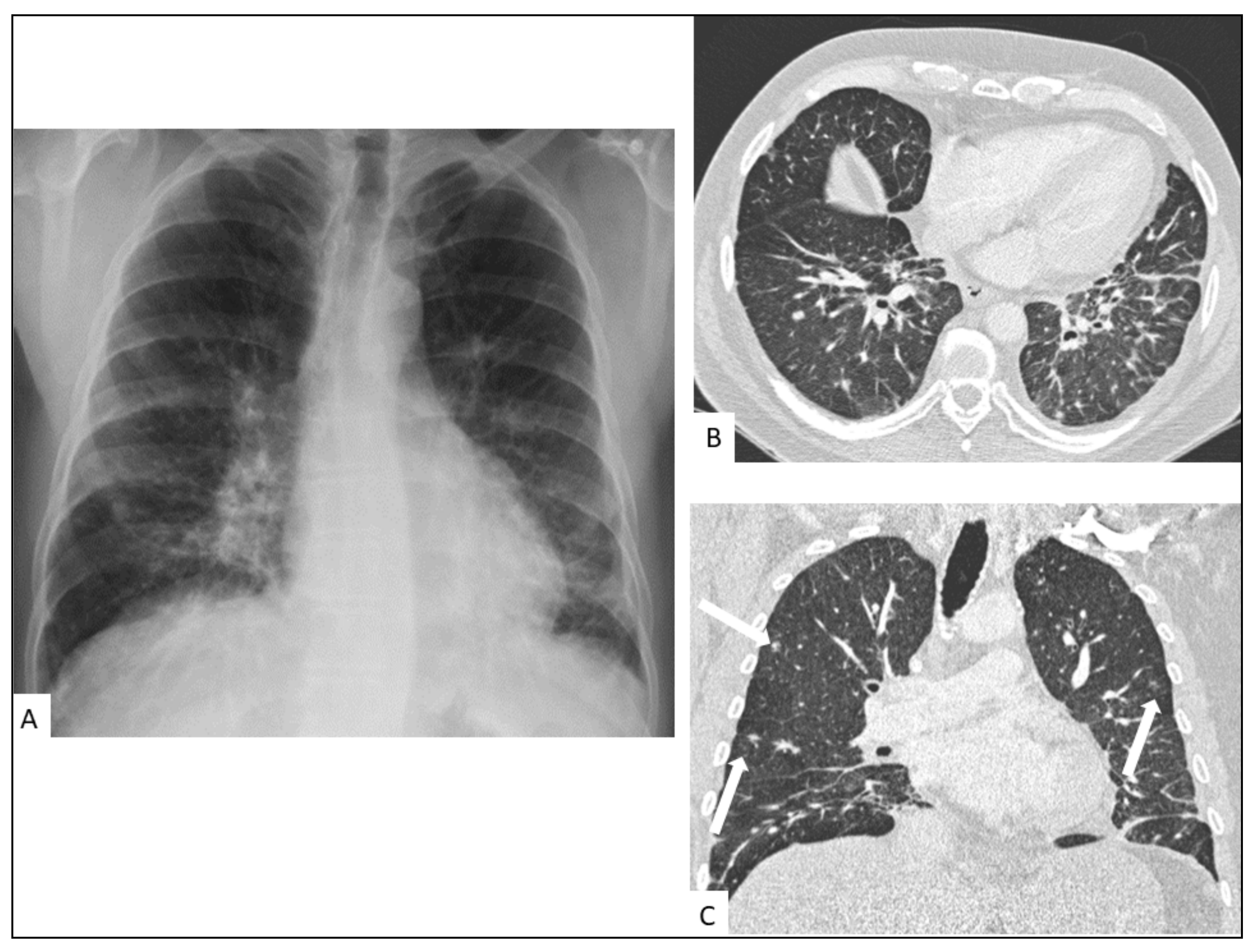
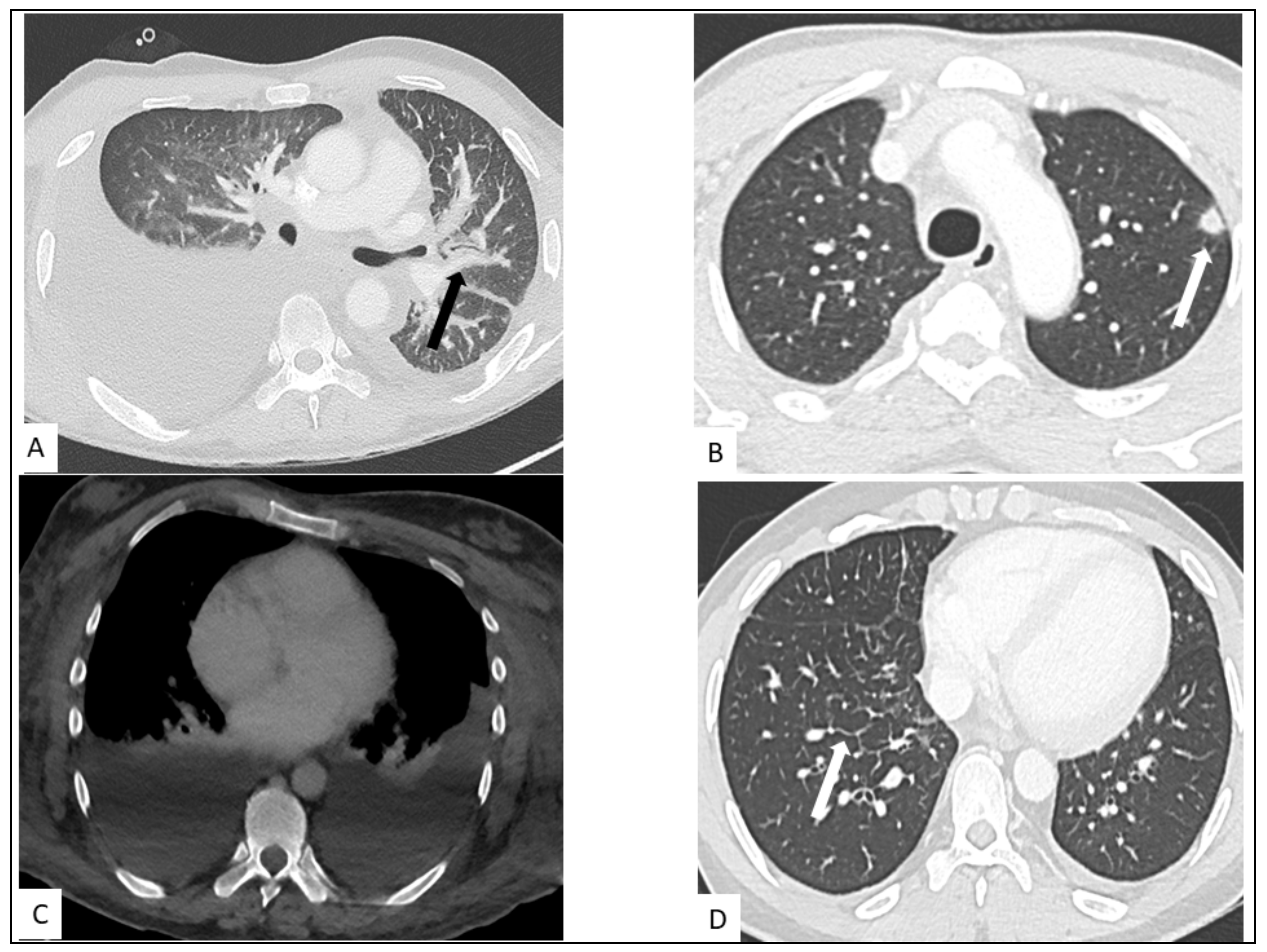
5. Radiological Presentation
5.1. Pulmonary KS
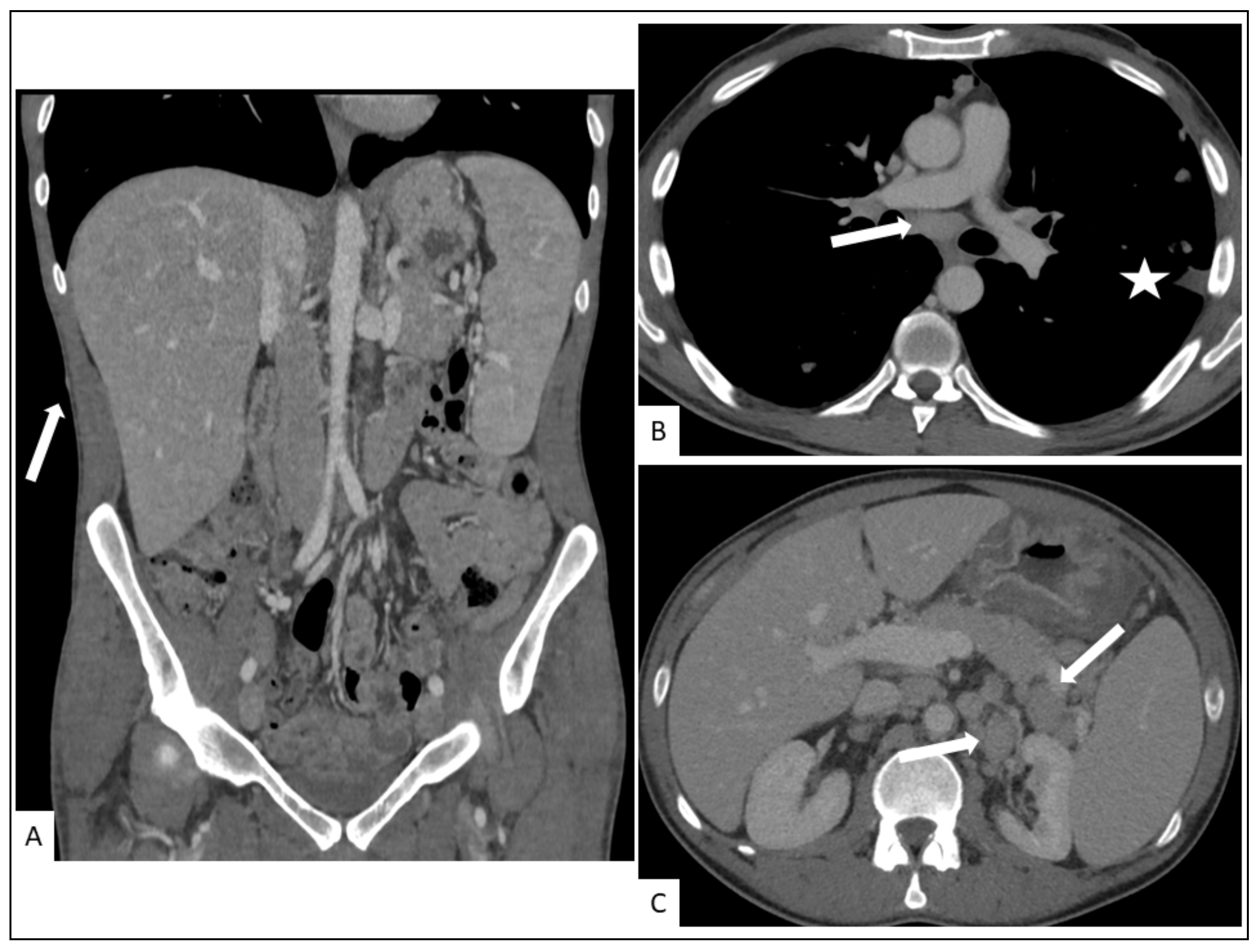
5.2. Hepato-Splenic KS
5.3. Other Visceral Involvement
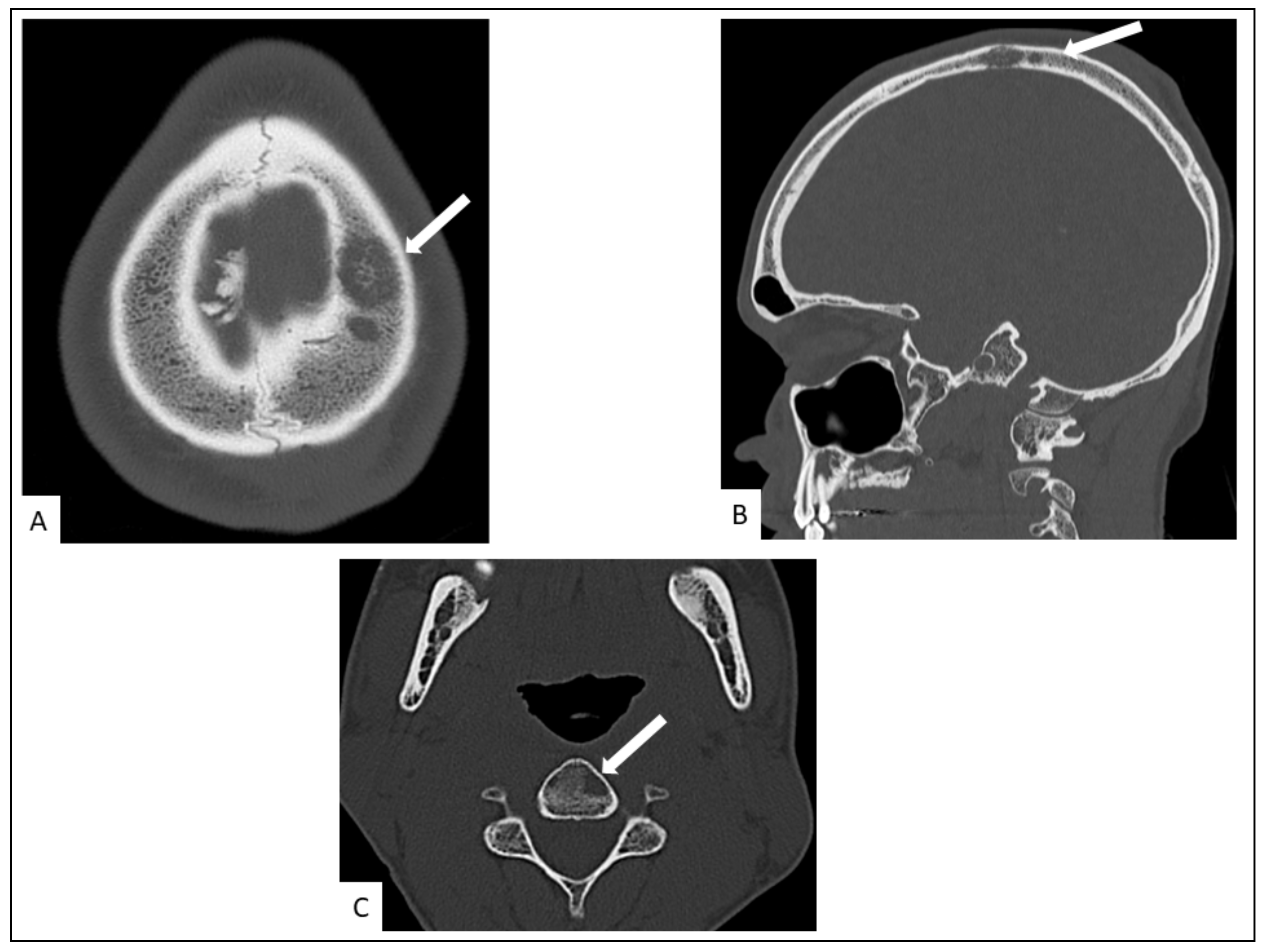
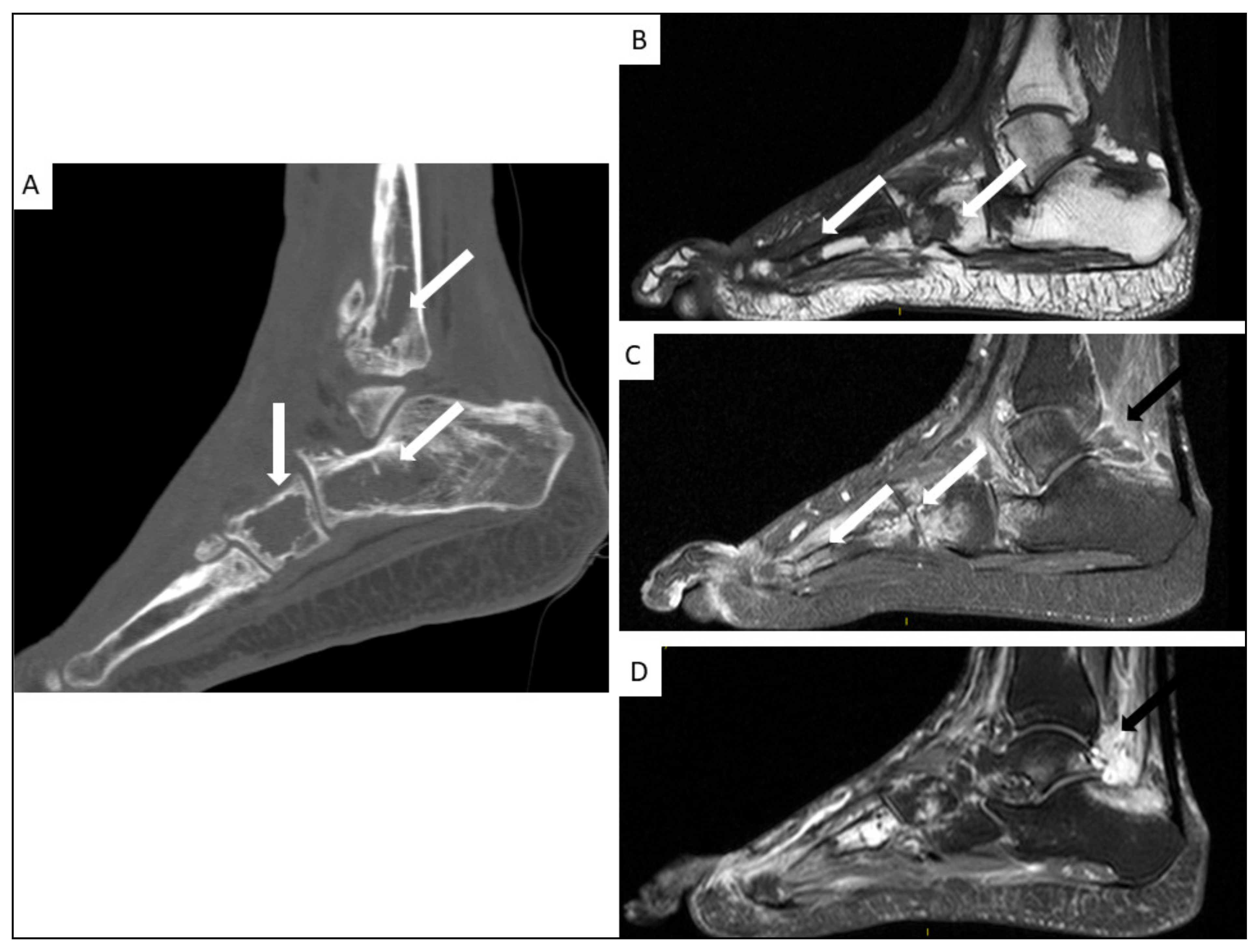
5.4. Musculo-Skeletal KS
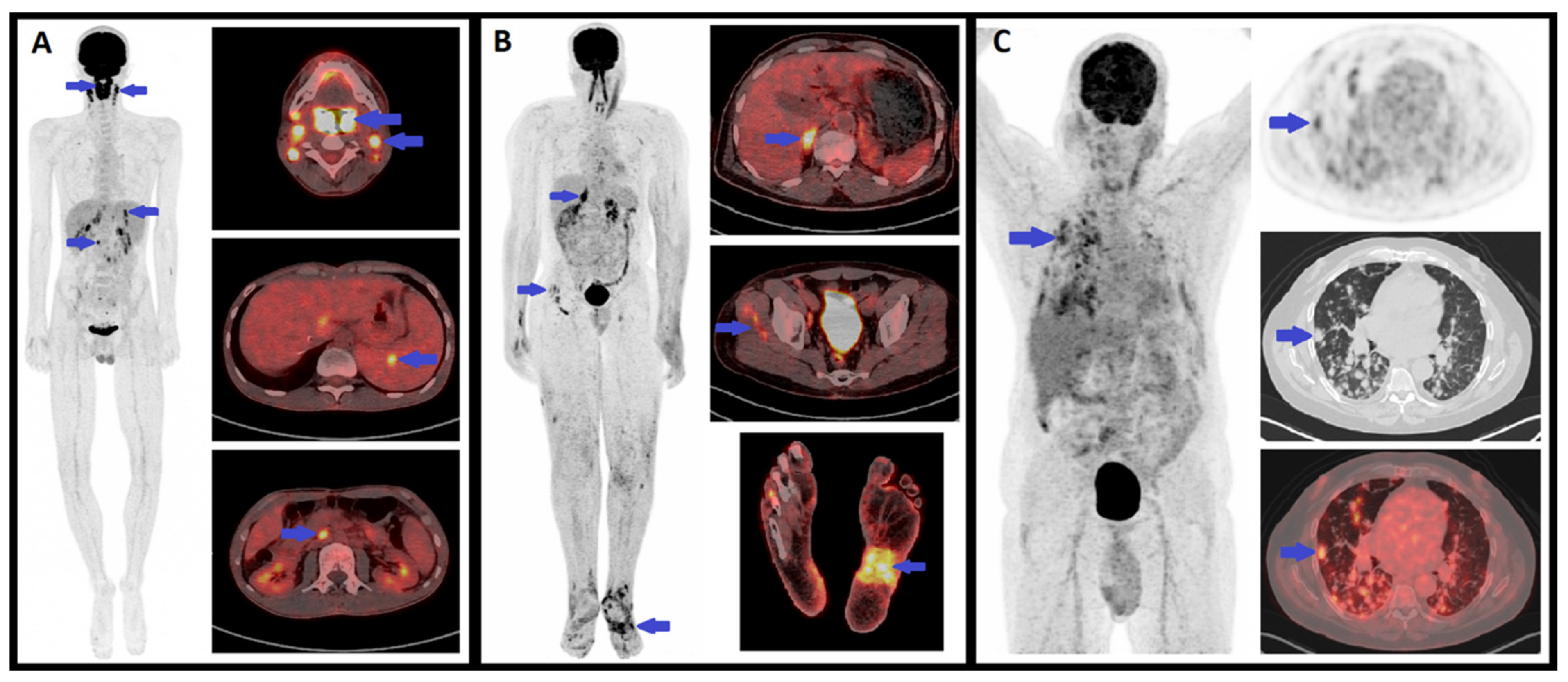
6. FDG-PET
7. Non-Invasive Imaging Tools
8. Conclusions
Author Contributions
Funding
Conflicts of Interest
References
- Tam, H.K.; Zhang, Z.-F.; Jacobson, L.P.; Margolick, J.B.; Chmiel, J.S.; Rinaldo, C.; Detels, R. Effect of Highly Active Antiretroviral Therapy on Survival among HIV-Infected Men with Kaposi Sarcoma or Non-Hodgkin Lymphoma. Int. J. Cancer 2002, 98, 916–922. [Google Scholar] [CrossRef] [PubMed]
- Grabar, S.; Abraham, B.; Mahamat, A.; Del Giudice, P.; Rosenthal, E.; Costagliola, D. Differential Impact of Combination Antiretroviral Therapy in Preventing Kaposi’s Sarcoma with and without Visceral Involvement. J. Clin. Oncol. Off. J. Am. Soc. Clin. Oncol. 2006, 24, 3408–3414. [Google Scholar] [CrossRef] [PubMed]
- Hernández-Ramírez, R.U.; Shiels, M.S.; Dubrow, R.; Engels, E.A. Cancer Risk in HIV-Infected People in the USA from 1996 to 2012: A Population-Based, Registry-Linkage Study. Lancet HIV 2017, 4, e495–e504. [Google Scholar] [CrossRef]
- Hleyhel, M.; Belot, A.; Bouvier, A.M.; Tattevin, P.; Pacanowski, J.; Genet, P.; De Castro, N.; Berger, J.-L.; Dupont, C.; Lavolé, A.; et al. Risk of AIDS-Defining Cancers among HIV-1-Infected Patients in France between 1992 and 2009: Results from the FHDH-ANRS CO4 Cohort. Clin. Infect. Dis. Off. Publ. Infect. Dis. Soc. Am. 2013, 57, 1638–1647. [Google Scholar] [CrossRef]
- Luo, Q.; Satcher Johnson, A.; Hall, H.I.; Cahoon, E.K.; Shiels, M. Kaposi Sarcoma Rates Among Persons Living With Human Immunodeficiency Virus in the United States: 2008–2016. Clin. Infect. Dis. Off. Publ. Infect. Dis. Soc. Am. 2021, 73, e2226–e2233. [Google Scholar] [CrossRef]
- Hengge, U.R.; Ruzicka, T.; Tyring, S.K.; Stuschke, M.; Roggendorf, M.; Schwartz, R.A.; Seeber, S. Update on Kaposi’s Sarcoma and Other HHV8 Associated Diseases. Part 1: Epidemiology, Environmental Predispositions, Clinical Manifestations, and Therapy. Lancet Infect. Dis. 2002, 2, 281–292. [Google Scholar] [CrossRef]
- Krown, S.E.; Metroka, C.; Wernz, J.C. Kaposi’s Sarcoma in the Acquired Immune Deficiency Syndrome: A Proposal for Uniform Evaluation, Response, and Staging Criteria. AIDS Clinical Trials Group Oncology Committee. J. Clin. Oncol. Off. J. Am. Soc. Clin. Oncol. 1989, 7, 1201–1207. [Google Scholar] [CrossRef]
- Krown, S.E.; Testa, M.A.; Huang, J. AIDS-Related Kaposi’s Sarcoma: Prospective Validation of the AIDS Clinical Trials Group Staging Classification. AIDS Clinical Trials Group Oncology Committee. J. Clin. Oncol. Off. J. Am. Soc. Clin. Oncol. 1997, 15, 3085–3092. [Google Scholar] [CrossRef]
- Krigel, R.L.; Laubenstein, L.J.; Muggia, F.M. Kaposi’s Sarcoma: A New Staging Classification. Cancer Treat. Rep. 1983, 67, 531–534. [Google Scholar]
- Brambilla, L.; Boneschi, V.; Taglioni, M.; Ferrucci, S. Staging of Classic Kaposi’s Sarcoma: A Useful Tool for Therapeutic Choices. Eur. J. Dermatol. EJD 2003, 13, 83–86. [Google Scholar]
- Lebbe, C.; Garbe, C.; Stratigos, A.J.; Harwood, C.; Peris, K.; Marmol, V.D.; Malvehy, J.; Zalaudek, I.; Hoeller, C.; Dummer, R.; et al. Diagnosis and Treatment of Kaposi’s Sarcoma: European Consensus-Based Interdisciplinary Guideline (EDF/EADO/EORTC). Eur. J. Cancer 2019, 114, 117–127. [Google Scholar] [CrossRef]
- Chapalain, M.; Goldman-Lévy, G.; Kramkimel, N.; Carlotti, A.; Franck, N.; Lheure, C.; Audard, V.; Avril, M.-F.; Marcelin, A.-G.; Damotte, D.; et al. Anaplastic Kaposi’s Sarcoma: 5 Cases of a Rare and Aggressive Type of Kaposi’s Sarcoma. Ann. Dermatol. Venereol. 2018, 145, 21–28. [Google Scholar] [CrossRef]
- Elder, D.E.; Massi, D.; Scolyer, R.A.; Willemze, R. WHO Classification of Skin Tumours; International Agency for Research on Cancer: Lyon, France, 2018; ISBN 928322440X. [Google Scholar]
- Grayson, W.; Pantanowitz, L. Histological Variants of Cutaneous Kaposi Sarcoma. Diagn. Pathol. 2008, 3, 31. [Google Scholar] [CrossRef]
- Tourlaki, A.; Recalcati, S.; Boneschi, V.; Gaiani, F.; Colombo, A.; Mancuso, R.; Brambilla, L. Anaplastic Kaposi’s Sarcoma: A Study of Eight Patients. Eur. J. Dermatol. 2013, 23, 382–386. [Google Scholar] [CrossRef]
- Chen, J.; Valle, L.D.; Lin, H.-Y.; Plaisance-Bonstaff, K.; Forrest, J.C.; Post, S.R.; Qin, Z. Expression of PD-1 and PD-Ls in Kaposi’s Sarcoma and Regulation by Oncogenic Herpesvirus Lytic Reactivation. Virology 2019, 536, 16–19. [Google Scholar] [CrossRef]
- Chen, B.J.; Chapuy, B.; Ouyang, J.; Sun, H.H.; Roemer, M.G.M.; Xu, M.L.; Yu, H.; Fletcher, C.D.M.; Freeman, G.J.; Shipp, M.A.; et al. PD-L1 Expression Is Characteristic of a Subset of Aggressive B-Cell Lymphomas and Virus-Associated Malignancies. Clin. Cancer Res. Off. J. Am. Assoc. Cancer Res. 2013, 19, 3462–3473. [Google Scholar] [CrossRef]
- Paydas, S.; Bagir, E.K.; Deveci, M.A.; Gonlusen, G. Clinical and Prognostic Significance of PD-1 and PD-L1 Expression in Sarcomas. Med. Oncol. Northwood Lond. Engl. 2016, 33, 93. [Google Scholar] [CrossRef]
- Mletzko, S.; Pinato, D.J.; Robey, R.C.; Dalla Pria, A.; Benson, P.; Imami, N.; Bower, M. Programmed Death Ligand 1 (PD-L1) Expression Influences the Immune-Tolerogenic Microenvironment in Antiretroviral Therapy-Refractory Kaposi’s Sarcoma: A Pilot Study. Oncoimmunology 2017, 6, e1304337. [Google Scholar] [CrossRef]
- Genovese, G.; Venegoni, L.; Fanoni, D.; Tourlaki, A.; Brambilla, L.; Berti, E. PD-L1 Expression in Tumour Microenvironment Supports the Rationale for Immune Checkpoint Blockade in Classic Kaposi’s Sarcoma. J. Eur. Acad. Dermatol. Venereol. 2019, 33, e269–e271. [Google Scholar] [CrossRef]
- Joest, B.; Kempf, W.; Berisha, A.; Peyk, P.; Tronnier, M.; Mitteldorf, C. Stage-Related PD-L1 Expression in Kaposi Sarcoma Tumor Microenvironment. J. Cutan. Pathol. 2020, 47, 888–895. [Google Scholar] [CrossRef]
- Kim, Y.J.; Jung, C.J.; Won, C.H.; Chang, S.E.; Lee, M.W.; Choi, J.H.; Lee, W.J. PD-1 and PD-L1 Expression in Kaposi Sarcoma: A Comparative Study According to the Pathological Stage and Clinical Characteristics. J. Cutan. Pathol. 2021, 48, 221–228. [Google Scholar] [CrossRef]
- Humar, A.; Michaels, M. AST ID Working Group on Infectious Disease Monitoring American Society of Transplantation Recommendations for Screening, Monitoring and Reporting of Infectious Complications in Immunosuppression Trials in Recipients of Organ Transplantation. Am. J. Transplant. 2006, 6, 262–274. [Google Scholar] [CrossRef]
- Moore, P.S.; Chang, Y. Detection of Herpesvirus-like DNA Sequences in Kaposi’s Sarcoma in Patients with and Those without HIV Infection. N. Engl. J. Med. 1995, 332, 1181–1185. [Google Scholar] [CrossRef]
- Maiorana, A.; Luppi, M.; Barozzi, P.; Collina, G.; Fano, R.A.; Torelli, G. Detection of Human Herpes Virus Type 8 DNA Sequences as a Valuable Aid in the Differential Diagnosis of Kaposi’s Sarcoma. Mod. Pathol. 1997, 10, 182–187. [Google Scholar]
- Asahi-Ozaki, Y.; Sato, Y.; Kanno, T.; Sata, T.; Katano, H. Quantitative Analysis of Kaposi Sarcoma-Associated Herpesvirus (KSHV) in KSHV-Associated Diseases. J. Infect. Dis. 2006, 193, 773–782. [Google Scholar] [CrossRef]
- Boivin, G.; Gaudreau, A.; Routy, J.P. Evaluation of the Human Herpesvirus 8 DNA Load in Blood and Kaposi’s Sarcoma Skin Lesions from AIDS Patients on Highly Active Antiretroviral Therapy. AIDS Lond. Engl. 2000, 14, 1907–1910. [Google Scholar] [CrossRef]
- Marcelin, A.-G.; Motol, J.; Guihot, A.; Caumes, E.; Viard, J.-P.; Dussaix, E.; Cadranel, J.; Frances, C.; Carcelain, G.; Calvez, V.; et al. Relationship between the Quantity of Kaposi Sarcoma-Associated Herpesvirus (KSHV) in Peripheral Blood and Effusion Fluid Samples and KSHV-Associated Disease. J. Infect. Dis. 2007, 196, 1163–1166. [Google Scholar] [CrossRef]
- Nsubuga, M.M.; Biggar, R.J.; Combs, S.; Marshall, V.; Mbisa, G.; Kambugu, F.; Mehta, M.; Biryahwaho, B.; Rabkin, C.S.; Whitby, D.; et al. Human Herpesvirus 8 Load and Progression of AIDS-Related Kaposi Sarcoma Lesions. Cancer Lett. 2008, 263, 182–188. [Google Scholar] [CrossRef][Green Version]
- Jary, A.; Leducq, V.; Palich, R.; Gothland, A.; Descamps, D.; Joly, V.; Lambert-Niclot, S.; Amiel, C.; Canestri, A.; Mirand, A.; et al. Usefulness of Kaposi’s Sarcoma-Associated Herpesvirus (KSHV) DNA Viral Load in Whole Blood for Diagnosis and Monitoring of KSHV-Associated Diseases. J. Clin. Microbiol. 2018, 56. [Google Scholar] [CrossRef]
- Duprez, R.; Kassa-Kelembho, E.; Plancoulaine, S.; Brière, J.; Fossi, M.; Kobangue, L.; Minsart, P.; Huerre, M.; Gessain, A. Human Herpesvirus 8 Serological Markers and Viral Load in Patients with AIDS-Associated Kaposi’s Sarcoma in Central African Republic. J. Clin. Microbiol. 2005, 43, 4840–4843. [Google Scholar] [CrossRef]
- Hosseinipour, M.C.; Sweet, K.M.; Xiong, J.; Namarika, D.; Mwafongo, A.; Nyirenda, M.; Chiwoko, L.; Kamwendo, D.; Hoffman, I.; Lee, J.; et al. Viral Profiling Identifies Multiple Subtypes of Kaposi’s Sarcoma. mBio 2014, 5, e01633-14. [Google Scholar] [CrossRef] [PubMed]
- Pellet, C.; Kerob, D.; Dupuy, A.; Carmagnat, M.V.; Mourah, S.; Podgorniak, M.-P.; Toledano, C.; Morel, P.; Vérola, O.; Dosquet, C.; et al. Kaposi’s Sarcoma-Associated Herpesvirus Viremia Is Associated with the Progression of Classic and Endemic Kaposi’s Sarcoma. J. Investig. Dermatol. 2006, 126, 621–627. [Google Scholar] [CrossRef] [PubMed]
- Quinlivan, E.B.; Zhang, C.; Stewart, P.W.; Komoltri, C.; Davis, M.G.; Wehbie, R.S. Elevated Virus Loads of Kaposi’s Sarcoma-Associated Human Herpesvirus 8 Predict Kaposi’s Sarcoma Disease Progression, but Elevated Levels of Human Immunodeficiency Virus Type 1 Do Not. J. Infect. Dis. 2002, 185, 1736–1744. [Google Scholar] [CrossRef] [PubMed]
- Laney, A.S.; Cannon, M.J.; Jaffe, H.W.; Offermann, M.K.; Ou, C.-Y.; Radford, K.W.; Patel, M.M.; Spira, T.J.; Gunthel, C.J.; Pellett, P.E.; et al. Human Herpesvirus 8 Presence and Viral Load Are Associated with the Progression of AIDS-Associated Kaposi’s Sarcoma. AIDS Lond. Engl. 2007, 21, 1541–1545. [Google Scholar] [CrossRef]
- Broccolo, F.; Tassan Din, C.; Viganò, M.G.; Rutigliano, T.; Esposito, S.; Lusso, P.; Tambussi, G.; Malnati, M.S. HHV-8 DNA Replication Correlates with the Clinical Status in AIDS-Related Kaposi’s Sarcoma. J. Clin. Virol. Off. Publ. Pan Am. Soc. Clin. Virol. 2016, 78, 47–52. [Google Scholar] [CrossRef]
- Tedeschi, R.; Enbom, M.; Bidoli, E.; Linde, A.; De Paoli, P.; Dillner, J. Viral Load of Human Herpesvirus 8 in Peripheral Blood of Human Immunodeficiency Virus-Infected Patients with Kaposi’s Sarcoma. J. Clin. Microbiol. 2001, 39, 4269–4273. [Google Scholar] [CrossRef]
- Martinelli, C.; Zazzi, M.; Ambu, S.; Bartolozzi, D.; Corsi, P.; Leoncini, F. Complete Regression of AIDS-Related Kaposi’s Sarcoma-Associated Human Herpesvirus-8 during Therapy with Indinavir. AIDS Lond. Engl. 1998, 12, 1717–1719. [Google Scholar]
- Marcelin, A.-G.; Grandadam, M.; Flandre, P.; Nicand, E.; Milliancourt, C.; Koeck, J.-L.; Philippon, M.; Teyssou, R.; Agut, H.; Dupin, N.; et al. Kaposi’s Sarcoma Herpesvirus and HIV-1 Seroprevalences in Prostitutes in Djibouti. J. Med. Virol. 2002, 68, 164–167. [Google Scholar] [CrossRef]
- Nascimento, M.C.; de Souza, V.A.; Sumita, L.M.; Freire, W.; Munoz, F.; Kim, J.; Pannuti, C.S.; Mayaud, P. Comparative Study of Kaposi’s Sarcoma-Associated Herpesvirus Serological Assays Using Clinically and Serologically Defined Reference Standards and Latent Class Analysis. J. Clin. Microbiol. 2007, 45, 715–720. [Google Scholar] [CrossRef]
- Goudsmit, J.; Renwick, N.; Dukers, N.H.; Coutinho, R.A.; Heisterkamp, S.; Bakker, M.; Schulz, T.F.; Cornelissen, M.; Weverling, G.J. Human Herpesvirus 8 Infections in the Amsterdam Cohort Studies (1984–1997): Analysis of Seroconversions to ORF65 and ORF. Proc. Natl. Acad. Sci. USA 2000, 97, 4838–4843. [Google Scholar] [CrossRef]
- Restrepo, C.S.; Martínez, S.; Lemos, J.A.; Carrillo, J.A.; Lemos, D.F.; Ojeda, P.; Koshy, P. Imaging Manifestations of Kaposi Sarcoma. Radiographics 2006, 26, 1169–1185. [Google Scholar] [CrossRef]
- Alwassia, A.; Alshathri, Z.; Khosla, R.; Spagnolo, S.V. Pulmonary Kaposi Sarcoma Presenting as Complete Lung Consolidation. BMJ Case Rep. 2017, 2017, bcr2016219048. [Google Scholar] [CrossRef]
- Traill, Z.C.; Miller, R.F.; Shaw, P.J. CT Appearances of Intrathoracic Kaposi’s Sarcoma in Patients with AIDS. Br. J. Radiol. 1996, 69, 1104–1107. [Google Scholar] [CrossRef]
- Khalil, A.M.; Carette, M.F.; Cadranel, J.L.; Mayaud, C.M.; Bigot, J.M. Intrathoracic Kaposi’s Sarcoma. CT Findings. Chest 1995, 108, 1622–1626. [Google Scholar] [CrossRef]
- Gasparetto, T.D.; Marchiori, E.; Lourenço, S.; Zanetti, G.; Vianna, A.D.; Santos, A.A.S.M.D.; Nobre, L.F. Pulmonary Involvement in Kaposi Sarcoma: Correlation between Imaging and Pathology. Orphanet J. Rare Dis. 2009, 4, 18. [Google Scholar] [CrossRef]
- Javadi, S.; Menias, C.O.; Karbasian, N.; Shaaban, A.; Shah, K.; Osman, A.; Jensen, C.T.; Lubner, M.G.; Gaballah, A.H.; Elsayes, K.M. HIV-Related Malignancies and Mimics: Imaging Findings and Management. Radiographics 2018, 38, 2051–2068. [Google Scholar] [CrossRef]
- Da Silva Filho, F.P.; Marchiori, E.; Valiante, P.M.; Escuissato, D.L.; Gasparetto, T.D. AIDS-Related Kaposi Sarcoma of the Lung Presenting with a "Crazy-Paving" Pattern on High-Resolution CT: Imaging and Pathologic Findings. J. Thorac. Imaging 2008, 23, 135–137. [Google Scholar] [CrossRef]
- Kaplan, L.D. Human Herpesvirus-8: Kaposi Sarcoma, Multicentric Castleman Disease, and Primary Effusion Lymphoma. Hematol. Am. Soc. Hematol. Educ. Program 2013, 2013, 103–108. [Google Scholar] [CrossRef]
- Allen, C.M.; Al-Jahdali, H.H.; Irion, K.L.; Al Ghanem, S.; Gouda, A.; Khan, A.N. Imaging Lung Manifestations of HIV/AIDS. Ann. Thorac. Med. 2010, 5, 201–216. [Google Scholar] [CrossRef]
- Gouny, P.; Lancelin, C.; Girard, P.M.; Hocquet-Cheynel, C.; Rozenbaum, W.; Nussaume, O. Pericardial Effusion and AIDS: Benefits of Surgical Drainage. Eur. J. Cardio-Thorac. Surg. Off. J. Eur. Assoc. Cardio-Thorac. Surg. 1998, 13, 165–169. [Google Scholar] [CrossRef][Green Version]
- Hussenet, C.; Calin, R.; Boussouar, S.; Londner, C.; Caby, F.; Tubiana, R.; Pourcher, V. Chylothorax as a complication of Kaposi’s sarcoma in an AIDS patient. Med. Mal. Infect. 2018, 48, 66–69. [Google Scholar] [CrossRef]
- Lababidi, M.H.; Alhawasli, H.; Iroegbu, N. Kaposi Sarcoma Can Also Involve the Heart. J. Community Hosp. Intern. Med. Perspect. 2015, 5, 29054. [Google Scholar] [CrossRef]
- Caponetti, G.; Dezube, B.J.; Restrepo, C.S.; Pantanowitz, L. Kaposi Sarcoma of the Musculoskeletal System: A Review of 66 Patients. Cancer 2007, 109, 1040–1052. [Google Scholar] [CrossRef]
- Ma, T.; Patel, H.; Babapoor-Farrokhran, S.; Franklin, R.; Semenza, G.L.; Sodhi, A.; Montaner, S. KSHV Induces Aerobic Glycolysis and Angiogenesis through HIF-1-Dependent Upregulation of Pyruvate Kinase 2 in Kaposi’s Sarcoma. Angiogenesis 2015, 18, 477–488. [Google Scholar] [CrossRef]
- Yogev, O.; Lagos, D.; Enver, T.; Boshoff, C. Kaposi’s Sarcoma Herpesvirus MicroRNAs Induce Metabolic Transformation of Infected Cells. PLoS Pathog. 2014, 10, e1004400. [Google Scholar] [CrossRef]
- Yogev, O.; Henderson, S.; Hayes, M.J.; Marelli, S.S.; Ofir-Birin, Y.; Regev-Rudzki, N.; Herrero, J.; Enver, T. Herpesviruses Shape Tumour Microenvironment through Exosomal Transfer of Viral MicroRNAs. PLoS Pathog. 2017, 13, e1006524. [Google Scholar] [CrossRef]
- Suzuki, J.; Sasahara, T.; Toshima, M.; Norizuki, M.; Onishi, T.; Okabe, T.; Minami, K.; Morisawa, Y. Usefulness of (18)F-Fluorodeoxyglucose-Position Emission Tomography with Computed Tomography and Gallium-67 Scintigraphy for Detection of Kaposi Sarcoma Lesions in a 40-Year-Old Japanese Man with AIDS. IDCases 2015, 2, 68–69. [Google Scholar] [CrossRef]
- Morooka, M.; Ito, K.; Kubota, K.; Minamimoto, R.; Shida, Y.; Hasuo, K.; Ito, T.; Tasato, D.; Honda, H.; Teruya, K.; et al. Whole-Body 18F-Fluorodeoxyglucose Positron Emission Tomography/Computed Tomography Images before and after Chemotherapy for Kaposi Sarcoma and Highly Active Antiretrovirus Therapy. Jpn. J. Radiol. 2010, 28, 759–762. [Google Scholar] [CrossRef]
- Mansfield, S.A.; Stawicki, S.P.A.; Forbes, R.C.; Papadimos, T.J.; Lindsey, D.E. Acute Upper Gastrointestinal Bleeding Secondary to Kaposi Sarcoma as Initial Presentation of HIV Infection. J. Gastrointest. Liver Dis. 2013, 22, 441–445. [Google Scholar]
- Morooka, M.; Ito, K.; Kubota, K.; Yanagisawa, K.; Teruya, K.; Hasuo, K.; Shida, Y.; Minamimoto, R.; Kikuchi, Y.; Oka, S. Usefulness of F-18 FDG PET/CT in a Case of Kaposi Sarcoma with an Unexpected Bone Lesion. Clin. Nucl. Med. 2011, 36, 231–234. [Google Scholar] [CrossRef]
- Yin, L.; Lin, Z.; Meng, Z. 18F-FDG PET/CT Findings in an HIV-Infected Patient with Systemic Kaposi Sarcoma. Pol. Arch. Intern. Med. 2021, 131, 78–80. [Google Scholar] [CrossRef] [PubMed]
- Mankia, S.K.; Miller, R.F.; Edwards, S.G.; Ramsay, A.; Lee, S.M. Highly Active Antiretroviral Therapy Alone Is an Effective Treatment for Lymphadenopathic Kaposi Sarcoma Demonstrated by a Clinical and F-18 FDG Positron Emission Tomography/Computed Tomography Response. Clin. Oncol. 2012, 24, 309–311. [Google Scholar] [CrossRef] [PubMed]
- Ozdemir, E.; Poyraz, N.Y.; Keskin, M.; Kandemir, Z.; Turkolmez, S. (18)F-FDG PET/CT Findings in a Case with HIV (-) Kaposi Sarcoma. Rev. Espanola Med. Nucl. E Imagen Mol. 2014, 33, 175–177. [Google Scholar] [CrossRef]
- Hwang, J.P.; Kim, J.; Park, J.M. Human Immunodeficiency Virus-Negative Multicentric Castleman’s Disease Coexistent with Kaposi’s Sarcoma on 18F-FDG PET/CT: A Case Report. Mol. Clin. Oncol. 2019, 10, 318–320. [Google Scholar] [CrossRef]
- Reuter, S.; Vrachimis, A.; Huss, S.; Wardelmann, E.; Weckesser, M.; Pavenstädt, H. A Challenging Case of Rapid Progressive Kaposi Sarcoma after Renal Transplantation: Diagnostics by FDG PET/CT. Medicine (Baltimore) 2014, 93, e67. [Google Scholar] [CrossRef]
- Delyon, J.; Bizot, A.; Battistella, M.; Madelaine, I.; Vercellino, L.; Lebbé, C. PD-1 Blockade with Nivolumab in Endemic Kaposi Sarcoma. Ann. Oncol. Off. J. Eur. Soc. Med. Oncol. 2018, 29, 1067–1069. [Google Scholar] [CrossRef]
- Cengiz, A.; Şavk, E.; Tataroğlu, C.; Yürekli, Y. 18F-Fluorodeoxyglucose Positron Emission Tomography/Computed Tomography Imaging in a Patient with HIV (-) Kaposi Sarcoma. Mol. Imaging Radionucl. Ther. 2016, 25, 140–142. [Google Scholar] [CrossRef]
- Sager, S.; Engin, B.; Kutlubay, Z.; Asa, S.; Sager, S.G.; Gucluer, B.; Kanmaz, B. PET/CT Imaging of HIV-Negative Kaposi’s Sarcoma. Ir. J. Med. Sci. 2013, 182, 745–746. [Google Scholar] [CrossRef]
- Jain, L.; Mackenzie, S.; Bomanji, J.B.; Shortman, R.; Noursadeghi, M.; Edwards, S.G.; Miller, R.F. 18F-Fluorodeoxyglucose Positron Emission Tomography-Computed Tomography Imaging in HIV-Infected Patients with Lymphadenopathy, with or without Fever and/or Splenomegaly. Int. J. STD AIDS 2018, 29, 691–694. [Google Scholar] [CrossRef]
- Hassan, M.; Little, R.F.; Vogel, A.; Aleman, K.; Wyvill, K.; Yarchoan, R.; Gandjbakhche, A.H. Quantitative Assessment of Tumor Vasculature and Response to Therapy in Kaposi’s Sarcoma Using Functional Noninvasive Imaging. Technol. Cancer Res. Treat. 2004, 3, 451–457. [Google Scholar] [CrossRef]
- Vogel, A.; Chernomordik, V.V.; Riley, J.D.; Hassan, M.; Amyot, F.; Dasgeb, B.; Demos, S.G.; Pursley, R.; Little, R.F.; Yarchoan, R.; et al. Using Noninvasive Multispectral Imaging to Quantitatively Assess Tissue Vasculature. J. Biomed. Opt. 2007, 12, 051604. [Google Scholar] [CrossRef][Green Version]
- Vogel, A.; Dasgeb, B.; Hassan, M.; Amyot, F.; Chernomordik, V.; Tao, Y.; Demos, S.G.; Wyvill, K.; Aleman, K.; Little, R.; et al. Using Quantitative Imaging Techniques to Assess Vascularity in AIDS-Related Kaposi’s Sarcoma. In Proceedings of the 2006 International Conference of the IEEE Engineering in Medicine and Biology Society, New York, NY, USA, 30 August–3 September 2006; IEEE: Piscataway Township, NJ, USA, 2006; pp. 232–235. [Google Scholar] [CrossRef]
- Gandjbakhche, A.; Vogel, A.; Amyot, F.; Chernomordik, V.; Hassan, M.; Demos, S.; Aleman, K.; Little, R.; Yarchoan, R. Noninvasive Multimodality Imaging Techniques to Assess Kaposi’s Sarcoma. In Proceedings of the 2005 IEEE Engineering in Medicine and Biology 27th Annual Conference, Shanghai, China, 17–18 January 2006; IEEE: Piscataway Township, NJ, USA, 2006; pp. 694–696. [Google Scholar] [CrossRef]
- Kainerstorfer, J.M.; Riley, J.D.; Ehler, M.; Najafizadeh, L.; Amyot, F.; Hassan, M.; Pursley, R.; Demos, S.G.; Chernomordik, V.; Pircher, M.; et al. Quantitative Principal Component Model for Skin Chromophore Mapping Using Multi-Spectral Images and Spatial Priors. Biomed. Opt. Express 2011, 2, 1040–1058. [Google Scholar] [CrossRef]
- Kainerstorfer, J.M.; Polizzotto, M.N.; Uldrick, T.S.; Rahman, R.; Hassan, M.; Najafizadeh, L.; Ardeshirpour, Y.; Wyvill, K.M.; Aleman, K.; Smith, P.D.; et al. Evaluation of Non-Invasive Multispectral Imaging as a Tool for Measuring the Effect of Systemic Therapy in Kaposi Sarcoma. PLoS ONE 2013, 8, e83887. [Google Scholar] [CrossRef]

| “TIS” Staging of KS | Good Risk (T0) | Poor Risk (T1) |
|---|---|---|
| Tumor | Confined to skin and/or lymph nodes, or minimal oral disease | Tumor-associated oedema or ulceration, extensive oral KS, gastrointestinal KS or KS in other non-nodal viscera |
| Immune status | CD4 cell count > 150/mm3 | CD4 cell count < 150/mm3 |
| Systemic illness | Karnofsky Performance Status > 70 | Karnofsky Performance Status < 70 or other HIV-related illness |
| Items | Classic/Endemic KS | AIDS-Associated KS | Iatrogenic KS |
|---|---|---|---|
| Clinical examination | ++ | ++ | ++ |
| HIV serology | ++ | ++ | ++ |
| Standard blood test | ++ | ++ | ++ |
| HHV-8 viremia | − | + | + |
| CD4 count | − | ++ | + |
| Histology | ++ | ++ | ++ |
| Total body CT-scan | +/− | + | + |
| Bronchoscopy | +/− | +/− | +/− |
| Esophago-gastro-duodenoscopy | +/− | +/− | +/− |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Dupin, N.; Jary, A.; Boussouar, S.; Syrykh, C.; Gandjbakhche, A.; Bergeret, S.; Palich, R. Current and Future Tools for Diagnosis of Kaposi’s Sarcoma. Cancers 2021, 13, 5927. https://doi.org/10.3390/cancers13235927
Dupin N, Jary A, Boussouar S, Syrykh C, Gandjbakhche A, Bergeret S, Palich R. Current and Future Tools for Diagnosis of Kaposi’s Sarcoma. Cancers. 2021; 13(23):5927. https://doi.org/10.3390/cancers13235927
Chicago/Turabian StyleDupin, Nicolas, Aude Jary, Samia Boussouar, Charlotte Syrykh, Amir Gandjbakhche, Sébastien Bergeret, and Romain Palich. 2021. "Current and Future Tools for Diagnosis of Kaposi’s Sarcoma" Cancers 13, no. 23: 5927. https://doi.org/10.3390/cancers13235927
APA StyleDupin, N., Jary, A., Boussouar, S., Syrykh, C., Gandjbakhche, A., Bergeret, S., & Palich, R. (2021). Current and Future Tools for Diagnosis of Kaposi’s Sarcoma. Cancers, 13(23), 5927. https://doi.org/10.3390/cancers13235927







