Simple Summary
The majority of patients with breast cancer are suitable for either breast-conserving therapy, consisting of breast-conserving surgery and radiation therapy, or mastectomy alone. In the present study, we compared survival outcomes in 1360 patients affected with early-stage breast cancer (stage I-IIA) according to the type of local treatment. We confirmed that patients treated with breast-conserving therapy had a lower rate of local, regional, and distant disease recurrences, and at least equivalent overall survival compared to those treated with mastectomy alone. Our results add to previous research showing a potential benefit of breast-conserving therapy when compared to mastectomy in patients suitable for both treatments at baseline.
Abstract
In the current study, we sought to compare survival outcomes after breast-conserving therapy (BCT) or mastectomy alone in patients with stage I-IIA breast cancer, whose tumors are typically suitable for both locoregional treatments. The study cohort consisted of 1360 patients with stage I-IIA (T1–2N0 or T0–1N1) breast cancer diagnosed between 2001 and 2013 and treated with either BCT (n = 1021, 75.1%) or mastectomy alone (n = 339, 24.9%). Median follow-ups for disease-free survival (DFS) and overall survival (OS) were 6.9 years (range, 0.3–15.9) and 7.5 years (range, 0.2–25.9), respectively. Fifteen (1.1%), 14 (1.0%) and 48 (3.5%) patients experienced local, regional, and distant relapse, respectively. For the whole cohort of patients, the estimated 5-year DFS and OS were 96% and 97%, respectively. After stratification based on the type of local treatment, the estimated 5-year DFS for BCT was 97%, while it was 91% (p < 0.001) for mastectomy-only treatment. Inverse probability of treatment weighting matching based on confounding confirmed that mastectomy was associated with worse DFS (HR 2.839, 95% CI 1.760–4.579, p < 0.0001), but not with OS (HR 1.455, 95% CI 0.844–2.511, p = 0.177). In our study, BCT was shown to have improved disease-specific outcomes compared to mastectomy alone, emphasizing the important role of adjuvant treatments, including postoperative radiation therapy, in patients with early-stage breast cancer at diagnosis.
1. Introduction
Long-term follow-up data from several randomized controlled trials undertaken to compare the efficacy of mastectomy with that of breast-conserving therapy (BCT) consisting of lumpectomy or quadrantectomy followed by postoperative radiotherapy showed no differences in terms of disease-free survival (DFS), distant-disease-free survival, and overall survival (OS) among the treatment groups [1,2,3,4,5]. The trials, conducted in the 1970s and 1980s, paved the way for the increased utilization of BCT for patients with stage I-II breast cancer [6]. Retrospective studies based on the analysis of large patient populations with early-stage breast cancer (EBC) treated in modern contexts indicate that BCT is at least comparable or even better in terms of breast-cancer-specific survival (BCSS) and OS compared to mastectomy without radiation therapy for early-stage breast cancer [7,8,9,10,11,12,13]. Improved DFS and OS rates were recently confirmed in smaller cohort studies [14,15,16,17,18,19,20] and were also observed in young women with EBC [21,22,23]. Based on older research, local recurrence is considered to be more common after BCT than after mastectomy. However, over the last 20 years, local recurrence rates after BCT have decreased substantially and are now shown to be as low as after mastectomy, most likely due to better understanding of breast cancer heterogeneity and consequently tailored systemic and radiation treatments [24,25].
For patients with breast cancer who are potentially suitable for both local treatments, BCT is suggested as the evidence-based primary local treatment [26]. Breast-conserving surgery is one of the major advances in the management of breast cancer. Nevertheless, breast-conserving surgery rates, as commonly reported, have reached a plateau in the last decade. In 2010–2011, breast-conserving surgery rates for the general population with unilateral EBC were 64.5–69% in the US [27,28,29], 73.3% in Europe [30], and 36.5–49.4% for patients younger than 50 years [28,31]. However, in some countries, the overall rate of breast-conserving surgery is lower than 50% [32,33].
The aim of BCT, as compared to mastectomy, is to achieve oncological safety with less extensive surgery, minimizing the psychosocial sequelae, and to obtain favorable cosmetic results with the use of oncoplastic techniques whenever possible. Most women feel negatively impacted by the scars resulting from breast cancer surgery, a consequence that particularly affects patients undergoing mastectomy [34]. When comparing long-term quality of life amongst patients treated with BCT or mastectomy, significantly lower scores for body image, role, and physical and sexual functioning, and more lifestyle disruptions were found for those treated with mastectomy. Conversely, psychosocial functioning slowly increased over time for women who underwent BCT, regardless of their age [35,36]. For patients undergoing mastectomy, access to breast reconstruction procedures is essential to increase positive body image and overall satisfaction and to maintain health-related quality of life [26,37]. However, barriers to immediate or delayed breast reconstruction exist on many levels, depending on the type of hospital (teaching vs. private), geographic location, reimbursement by insurance companies, lack of patient awareness, and the acceptability of the procedures by both physicians and patients [38]. In the past decade, the use of breast reconstruction has increased globally together with the indications for the use of postmastectomy irradiation for EBC [39,40]. It has been documented that the use of postmastectomy radiation therapy may be a negative outcome predictor for breast reconstruction [39]. On the other hand, opting for breast reconstruction may also influence clinical decision making in recommending postoperative radiation therapy due to the impact of radiation on long-term cosmetic results [39,41].
In the current study, we aimed to compare the outcomes of BCT and mastectomy-only treatment performed in the modern era in patients with stage I-IIA breast cancer, whose tumors are typically suitable for either BCT or mastectomy. The primary outcomes were DFS and OS, and secondary outcomes included any breast cancer recurrence (local, regional, and/or distant).
2. Materials and Methods
2.1. Study Cohort and Data Collection
For the present study, data were retrospectively collected and retrieved. The study cohort consisted of patients with stage I-IIA (T1–2N0 or T0–1N1) breast cancer diagnosed between 2001 and 2013 and treated with upfront BCT or mastectomy only with or without reconstruction, achieving clear resection margins in both cases. General patient demographic, histological characteristic, systemic therapy (chemotherapy, endocrine, or anti-HER2 therapies), and local treatment (surgery, radiotherapy) data were collected from individual clinical records. Clinical follow-up information for all patients was updated until 31 March 2021. For the purpose of this study, patient disease stage was classified based on medical records, according to breast carcinoma TNM Classification of Malignant Tumours (7th edition) [42]. Intrinsic subtypes of BC were defined as luminal A-like (estrogen-receptor positive, ER+; human epidermal growth factor receptor 2 negative, HER2−; Ki67 < 20%, progesterone receptor positive (PR+) with a cut-point of ≥20%); luminal B-like HER2-negative (ER+, HER2−, Ki67 ≥ 20%, or low PR+); luminal B-like HER2-positive (ER+, HER2+, any PR, any Ki67); HER2-positive (HER2+, PR−, ER−); and ‘Basal-like’ (ER−, PR−, HER2−) according to clinicopathological surrogate definitions as defined in the St Gallen International Expert Consensus on the primary therapy of EBC in 2013 [43].
2.2. Statistical Analysis
To compare clinical and tumor characteristics between the two groups (patients treated with BCT vs. those treated with mastectomy) we used independent-sample t-tests for continuous variables and Pearson’s χ2 or Fisher’s exact tests for categorical variables. Data were expressed as median with a sample range for continuous variables, and as counts with frequencies for categorical data. The Kaplan–Meier method was used to calculate estimated survival curves, and the log-rank test was used to compare the two groups. Univariate and multivariate Cox’s proportional hazards models were used to assess the effects of covariates on survival. The effect sizes were given as hazard ratios (HR) with 95% confidence intervals (CI). Overall survival (OS) was specified as the time of BC diagnosis to the date of death or last follow-up. Disease-free survival (DFS) was defined as time to disease recurrence (any type; local and/or regional and/or distant) after surgery. All tests were two-sided, and the statistical level of significance was set to p < 0.05. In addition, to reduce bias in our observational study and to analyze the cohort with a representative distribution of matching factors, we used a propensity-score-matched analysis with an inverse probability of treatment weighting (IPTW), calculating the reciprocal of the probability of receiving the treatment that the patient in fact received. We performed adjusted analyses using a multiple linear regression model and IPTW using the propensity score estimated via logistic regression. The outcome model used in the IPTW analysis was a linear regression of outcome on BCT or mastectomy, weighted by the estimated propensity score [44,45]. Covariate adjustment was based on age at diagnosis, pathological tumor and nodal stage, overall breast cancer stage group, tumor grade, type of axillary surgery, and the receipt of chemotherapy and/or endocrine therapy. Data were analyzed using IBM SPSS Statistics software version 26 (Statistical package for the Social Sciences Statistical Software, SPSS Inc, IBM Corporation, Armonk, NY, USA).
3. Results
In total, 1360 patients with stage I-IIA breast cancer treated with either BCT (n = 1021, 75.1%) or mastectomy only (n = 339, 24.9%) were included in the study. The median age at breast cancer diagnosis was 61 years in both groups (BCT range 23–87 and mastectomy range 27–91). The majority of breast tumors were sized ≤2 cm (n = 1100, 81.5%) and had positive estrogen or progesterone receptors (n = 1241, 92.3%). More than half of the patients had left-sided breast cancer (n = 729; 54.2%). Compared with patients receiving mastectomy only as local therapy, patients undergoing BCT were less likely to be younger than 50 or older than 70 years, less likely to have had more extensive axillary surgery, and more likely to have stage I breast cancer. We observed no differences in the two groups with respect to tumor grade, intrinsic subtype, and administration of endocrine or targeted therapy. However, more patients in the mastectomy group received adjuvant chemotherapy (Table 1).

Table 1.
Patients’ clinical, pathological, and treatment characteristics.
3.1. Surgery
Most patients received a limited axillary surgery (n = 1360, 81.3%). Data regarding breast reconstruction were known for 557 (41.0%) patients. Among the 62 patients receiving breast reconstruction, 4 had stage IA, 31 had stage IB, and 27 had stage IIA breast cancer.
3.2. Radiation Therapy
Out of the 1021 patients receiving radiotherapy, all following breast-conserving surgery, 495 (48.5%) were treated with conventional fractionation (median dose 50 Gy; range 28–50.4 Gy), 489 (47.9%) with moderate hypofractionated schedules (median dose 45 Gy; range 34.5–47.5), and 37 (3.6%) received one of the ultra-hypofractionated schedules (median dose 31.5 Gy; range 20–50 Gy). Additional dose to the tumor bed was received by 661 (64.7%) patients. Almost all patients received whole-breast radiotherapy only, excluding axillary or supraclavicular nodal volumes (n = 1014; 99.3%).
3.3. Systemic Treatment
Timing (preoperative versus postoperative) and type of systemic treatment are presented separately for both groups in Table 2. The receipt of taxane-based chemotherapy was more frequently observed in the mastectomy group, as compared to the BCT group (32.8% versus 24.7%; p < 0.0005).

Table 2.
Type and sequence of systemic treatment.
In total, 578 (45.1%) evaluated patients received endocrine therapy with aromatase inhibitors, 539 (42.0%) with tamoxifen, and 122 (12.9%) with treatment combinations (i.e., tamoxifen and aromatase inhibitors). Compared with patients treated with mastectomy only, patients undergoing BCT more often received adjuvant endocrine therapy with aromatase inhibitors (n = 141; 40.3% versus n = 437; 46.9%) and were less likely to receive adjuvant therapy with tamoxifen (152; 43.4% versus 387; 41.5%). The observed differences were statistically significant (p < 0.0005).
3.4. Outcome
Median follow-up for DFS and OS was 6.9 years (range: 0.3–15.9) and 7.5 years (range: 0.2–25.9), respectively. Overall, 86 (6.3%) patients experienced local (LR), regional (RR), or distant recurrence. We observed statistically meaningful differences across all recurrence types (Table 3). The cumulative incidences of 5-year LR and 10-year LR were 2.0% and 3.0% for the whole group, respectively. For the BCT group, the cumulative incidences of 5-year and 10-year LR were 1.0% and 3.0%; the corresponding cumulative incidences for the mastectomy group were 4% for both observed intervals. Observed absolute differences in cumulative incidence of recurrences between BCT and mastectomy groups were small, although statistically significant.

Table 3.
Cumulative incidence of local, regional, and distant recurrence for patients treated with breast-conserving therapy or with mastectomy.
For the whole cohort, the estimated 5-year and 10-year DFS were 96% and 95%, respectively. After stratification according to the type of local treatment, the estimated 5-year and 10-year DFS for the BCT group were 97% and 96%, and the estimated 5-year and 10-year DFS for the mastectomy-only group were 91% and 90% (log-rank; p < 0.001). In a univariate analysis, the following factors were associated with a decreased DFS: not receiving BCT, age > 70 years, tumor size ≥ 2 cm, stage IIA, tumor grade ≥ 2, and omission of endocrine adjuvant therapy. Upon multivariate Cox analysis, type of local treatment and tumor grade maintained statistical significance (Table 4).

Table 4.
Univariate and multivariate Cox regression analysis for 5-year disease-free survival.
The estimated 5-year and 10-year OS, calculated for the whole cohort, were 97% and 92%, respectively. Among patients treated with BCT, 5-year and 10-year OS estimates were 97% and 93%, and for those treated with mastectomy-only, 95% and 89%, respectively (log-rank; p = 0.045). Univariate and multivariate analyses were performed to analyze factors associated with worse survival outcomes. The use of mastectomy as the only local treatment was found to be correlated with worse OS in univariate analysis, but this finding was not confirmed in the multivariate Cox regression analysis (Table 5).

Table 5.
Univariate and multivariate Cox regression analysis for 5-year overall survival.
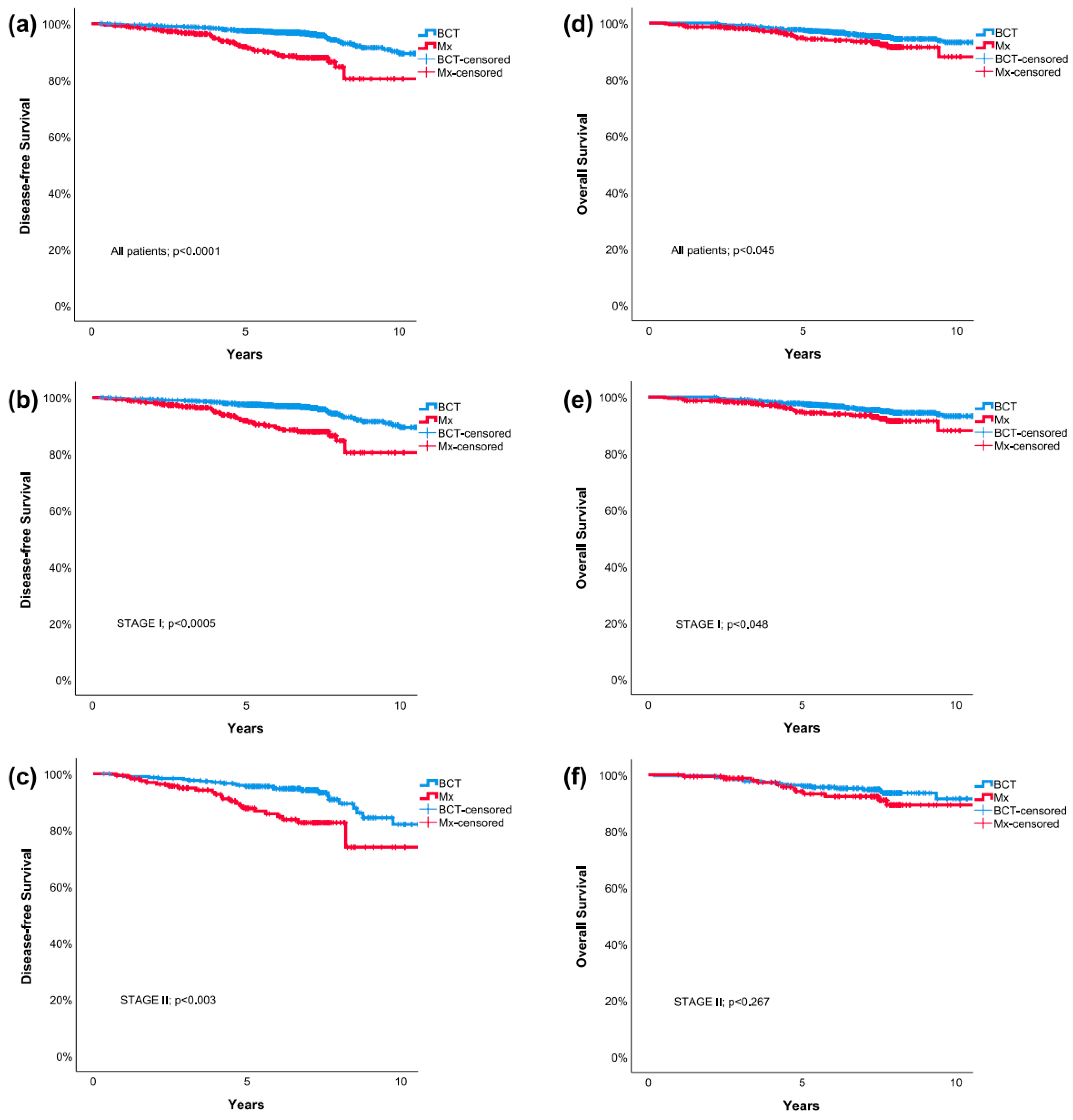
High tumor grade and the omission of systemic chemotherapy were the only two factors associated with poorer OS. The type of local treatment was not associated with improved OS using multivariable Cox regression. Kaplan–Meier survival curves for all included patients representing DFS and OS with respect to breast cancer stage group are presented in Figure 1.
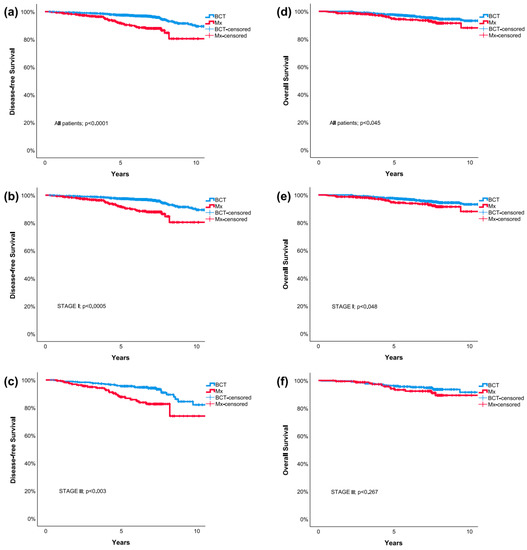
Figure 1.
Kaplan–Meier survival curves comparing breast conserving therapy and mastectomy: Disease-Free Survival for all included patients (a), patients with stage I (b) and stage II (c) breast cancer; Overall Survival for all included patients (d), patients with stage I (e) and stage II (f) breast cancer. BCT = breast-conserving therapy; Mx = mastectomy.
After IPTW matching based on confounding variables (age at diagnosis, pathological tumor and nodal stage, overall breast cancer stage group, tumor grade, type of axillary surgery, and the receipt of chemotherapy or endocrine therapy), and after excluding study subjects with extreme weights, 1343 patients were available for the analysis. Mastectomy was associated with worse DFS (HR 2.839, 95% CI 1.760–4.579, p < 0.0001). This finding was not confirmed for OS (HR 1.455, 95% CI 0.844–2.511, p = 0.177).
4. Discussion
In our patient cohort treated in the contemporary era, we evaluated the therapeutic outcomes in patients with stage I-IIA breast cancer treated with either conservative surgery combined with postoperative radiation therapy or with mastectomy alone. We demonstrated an outcome improvement associated with BCT in terms of both 5-year DFS and 5-year OS, with absolute differences of 6% and 2%, respectively. The observed differences were also consistent at 10 years. However, using multivariable Cox regression and after IPTW matching, the only outcome that was found to be significantly impacted by the type of local treatment (BCT compared to mastectomy) was DFS.
In our study, we observed very low LR, RR, and distant metastasis rates within the whole cohort. The cumulative in-breast/chest-wall failure rates at 10 years after treatment were 3.0% for the BCT group and 4.0% for the mastectomy group. Compared to historical series, reporting approximately 5–10% in-breast failures after 10 years from treatment, our results compare favorably [46,47]. This finding is in agreement with the reports of other studies, which are all convincing and uniformly show DFS and/or OS benefits for BCT compared to mastectomy in patients with stage I-II breast cancer (Table 6). Equivalent or improved outcomes with BCT as compared with mastectomy in terms of locoregional control, BCSS, DFS, or OS have been reported regardless of age [14,15], intrinsic breast cancer subtype [48,49,50,51], pathological tumor stage [11,14,15,51], overall breast cancer stage [52], and grade [51]. Recently, a Swedish cohort study using prospectively collected data of women with stage T1-2 N0-2 breast cancer confirmed better survival with BCT vs. mastectomy (irrespective of radiation therapy) even when taking into account comorbidity and socioeconomic status in both node-negative and node-positive disease, pointing out that offering more extensive surgery to patients who are suitable for either breast-conserving surgery or mastectomy is not saving lives [51].

Table 6.
Published studies comparing breast-conserving therapy with mastectomy for patients with stage I-II breast cancer.
Improved survival rates in patients with breast cancer over the past couple of decades are largely attributable to the use of breast cancer screening and better imaging, predictive biomarkers, and better understanding of breast cancer heterogeneity. New advances in the field of systemic treatments, including molecularly targeted therapies, endocrine therapy, taxane-based chemotherapy, and bisphosphonates have all effectively contributed to reduce the risk of distant and local breast cancer recurrence. Consequently, breast cancer mortality rates have declined in recent decades even in patients with a low risk of recurrence at baseline [53]. However, the contributions of a particular type of local treatment and new developments related to both surgical techniques and modern radiation therapy are frequently overlooked [54]. It is well known that prevention of locoregional recurrence reduces the risk of breast-cancer-specific death and is related to improvements in OS [55,56]. Many possible reasons for the better outcomes observed for patients with breast cancer undergoing lumpectomy combined with postoperative radiotherapy compared with mastectomy have been already elucidated [46,54,57,58]. Surgery does provide superior local control within resected tissue; however, with tangential radiotherapy techniques, the treated volume is larger (as compared to simple mastectomy) and typically includes unoperated breast tissue in its entirety, part of the muscle, regional lymphatics, draining lymphatics towards the axillary region, subcutaneous lymphatic plexus, and skin [46]. Incidental irradiation may potentially sterilize microscopic disease outside the breast tissue as it covers approximately 85% of axillary level I lymph nodes if the patient is treated in a supine position [59]. At the same time, radiotherapy techniques have improved in the past years, with three-dimensional treatment planning and heart-sparing techniques, including deep-inspiration breath-hold, prone-positioning, and partial breast irradiation substantially decreasing the dose to the heart and subsequently reducing mortality rate from the cardiac events [60].
The possibility of an anticancer immune response that can be elicited by radiotherapy outside of the radiation field, targeting micro- or macro-metastases, is also one of the postulated mechanisms of action. Abscopal effects have been demonstrated not only at higher doses per fraction but also at the lower dose per fraction (2.0–2.5 Gy) typically used in breast cancer postoperative radiotherapy [61]. Moreover, it is well known that postoperative radiotherapy not only reduces local recurrence, but also diminishes the risk of any recurrence type, including distant relapse, which could be explained by mechanisms such as the abscopal effect [62].
Omitting postoperative radiation therapy after mastectomy in patients undergoing breast reconstruction or in those with N1 disease may be a partial culprit of higher disease recurrence in these patients. In our study, 17.6% of patients had pathological N1 disease and the percentage of patients with pathological N1 disease did not differ between the groups. None of the patients with pathological N1 disease in the mastectomy group received postoperative radiation therapy. In a study by Sun et al., the authors analyzed the treatment outcomes of 4262 patients with clinical stage T1-2N1M0 breast cancer, and 832 (21.6%) of them received mastectomy and postoperative radiation therapy. In multivariate and propensity-score matching analyses, radiation therapy, but not type of surgical treatment, appeared to be an independent prognostic factor for improved OS, DFS, and loco-regional recurrence [19]. Although results from the meta-analysis of individual patient data clearly demonstrated a benefit in reducing both recurrence and breast cancer mortality in women with one to three positive lymph nodes, postmastectomy radiotherapy is less often routinely recommended than radiotherapy following breast-conserving surgery in patients with pathological N1 disease [46,62]. Patients who require post-mastectomy radiation therapy following immediate breast reconstruction are exposed to a detectably higher risk of post-reconstruction complications, including infection, implant removal, and capsular contracture in patients receiving implant-based reconstruction, and fat necrosis in those receiving autologous-tissue-based reconstruction [63]. Factors influencing the final cosmetic outcome and patients’ preferences may all affect the final decision to undergo postoperative chest-wall radiation therapy.
Despite the many benefits observed with BCT, the rates of unilateral or bilateral mastectomies for patients with unilateral breast cancer, who are candidates for BCT, are on the rise [29,64]. Perceived risks such as a fear of developing a second breast cancer, a historical belief that mastectomy is a safer option, possible avoidance of long-term breast cancer surveillance imaging, and the inconvenience of daily radiotherapy treatments may all have contributed to increasing mastectomy rates, which is of concern [53,65,66,67]. Nevertheless, it is important to note that different mastectomy and reconstruction techniques may lead to various amounts of remaining breast glandular tissue, potentially increasing the risk of breast cancer residual disease or recurrence [68].
As pointed out by Dodwell et al., women with screen-detected breast cancer are more likely to undergo BCT and mammographic screening confers a survival advantage compared to symptomatic presentation [69]. In our study, in which two-thirds of patients were aged between 50 and 70 years (n = 880, 64.7%) and a similar proportion had stage I disease (n = 891, 65.5%), individual data regarding screening status were missing.
The strengths of our study include a large patient cohort and thorough analysis with adjustments for confounding factors. Nevertheless, we acknowledge the limitations of our study and the difficulties in bias elimination in observational research. Our results may have been influenced by the retrospective nature of the study, as the quality of our data depend on reliable data collection. Additionally, follow-up was short and some of the data were not available at the time of the analysis. In our study, the impact of specific patient and tumor characteristics (e.g., age, tumor grade or size, lymph node status, and the receipt of endocrine therapy and systemic therapy) were adjusted with the use of a rigorous approach to reduce the effects of confounding in the estimation of the type of local treatment effect. However, we acknowledge the limitations of the propensity score analysis and IPTW-matching method, especially that there was no adjustment for the impact of all baseline characteristics [45]. In addition, a comparison of the results of patients with stage I-IIA EBC and treated with mastectomy followed by postoperative radiation therapy would certainly add value to our research.
5. Conclusions
Breast-conserving surgery followed by postoperative radiotherapy was shown in our study to have superior outcomes, including local, regional, and distant recurrence of the disease, and at least equivalent OS compared to mastectomy alone in patients with early-stage I-IIA breast cancer. The observed differences were statistically significant, but the clinical differences were relatively small. Nevertheless, it is essential that patients with EBC who are suitable for either BCT or mastectomy are well informed throughout the shared decision-making process about each locoregional treatment option and the corresponding long-term outcomes.
Author Contributions
Contributions are as follows for each author on this manuscript: Conceptualization, I.R. and P.F.; methodology, I.R., G.P., T.Z., P.F.; software, I.R., P.F., N.P.; validation, I.R., P.F., and A.P.; formal analysis, I.R. and P.F.; investigation, I.R. and P.F.; resources, I.R., P.F., N.P., A.P. and T.Z.; data curation, G.P., I.R., P.F., N.P. and T.Z.; writing—original draft preparation, I.R. and P.F.; writing—review and editing, I.R., P.F., G.P., N.P., T.Z. and A.P.; visualization, I.R. and P.F; supervision, P.F.; project administration, G.P., I.R., P.F., N.P., T.Z. and A.P. All authors have read and agreed to the published version of the manuscript.
Funding
The work was supported in part by ERA-NET within the framework of the call on “Translational research on tertiary prevention in cancer patients” (TRANSCAN), with funding from Ministry of Education, Science and Sport (MIZS), Slovenia.
Institutional Review Board Statement
This study was approved by the institutional review board and ethical committee (protocol code 92/04/15, approved on 23 April 2015). All procedures performed were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki Declaration and its later amendments or comparable ethical standards (N. INT 197/14).
Informed Consent Statement
Informed consent for using their data for retrospective study purposes at the start of their treatment was obtained from all individual participants included in the study.
Data Availability Statement
The data that support the findings of this study are not publicly available but can be requested from the corresponding author.
Conflicts of Interest
The authors declare no conflict of interest.
References
- Veronesi, U.; Cascinelli, N.; Mariani, L.; Greco, M.; Saccozzi, R.; Luini, A.; Aguilar, M.; Marubini, E. Twenty-year follow-up of a randomized study comparing breast-conserving surgery with radical mastectomy for early breast cancer. N. Engl. J. Med. 2002, 347, 1227–1232. [Google Scholar] [CrossRef]
- Fisher, B.; Anderson, S.; Bryant, J.; Margolese, R.G.; Deutsch, M.; Fisher, E.R.; Jeong, J.H.; Wolmark, N. Twenty-year follow-up of a randomized trial comparing total mastectomy, lumpectomy, and lumpectomy plus irradiation for the treatment of invasive breast cancer. N. Engl. J. Med. 2002, 347, 1233–1241. [Google Scholar] [CrossRef]
- Poggi, M.M.; Danforth, D.N.; Sciuto, L.C.; Smith, S.L.; Steinberg, S.M.; Liewehr, D.J.; Menard, C.; Lippman, M.E.; Lichter, A.S.; Altemus, R.M. Eighteen-year results in the treatment of early breast carcinoma with mastectomy versus breast conservation therapy: The National Cancer Institute randomized trial. Cancer 2003, 98, 697–702. [Google Scholar] [CrossRef]
- Blichert-Toft, M.; Nielsen, M.; Düring, M.; Møller, S.; Rank, F.; Overgaard, M.; Mouridsen, H.T. Long-term results of breast conserving surgery vs. mastectomy for early stage invasive breast cancer: 20-year follow-up of the Danish randomized DBCG-82TM protocol. Acta Oncol. 2008, 47, 672–681. [Google Scholar] [CrossRef]
- Litière, S.; Werutsky, G.; Fentiman, I.S.; Rutgers, E.; Christiaens, M.R.; Van Limbergen, E.; Baaijens, M.H.; Bogaerts, J.; Bartelink, H. Breast conserving therapy versus mastectomy for stage I-II breast cancer: 20-year follow-up of the EORTC 10801 phase 3 randomised trial. Lancet Oncol. 2012, 13, 412–419. [Google Scholar] [CrossRef]
- Lazovich, D.; Solomon, C.C.; Thomas, D.B.; Moe, R.E.; White, E. Breast conservation therapy in the United States following the 1990 National Institutes of Health Consensus Development Conference on the treatment of patients with early stage invasive breast carcinoma. Cancer 1999, 86, 628–637. [Google Scholar] [CrossRef]
- Lagendijk, M.; van Maaren, M.C.; Saadatmand, S.; Strobbe, L.J.A.; Poortmans, P.M.P.; Koppert, L.B.; Tilanus-Linthorst, M.M.A.; Siesling, S. Breast conserving therapy and mastectomy revisited: Breast cancer-specific survival and the influence of prognostic factors in 129,692 patients. Int. J. Cancer 2018, 142, 165–175. [Google Scholar] [CrossRef] [PubMed]
- Van Maaren, M.C.; de Munck, L.; Jobsen, J.J.; Poortmans, P.; de Bock, G.H.; Siesling, S.; Strobbe, L.J.A. Breast-conserving therapy versus mastectomy in T1-2N2 stage breast cancer: A population-based study on 10-year overall, relative, and distant metastasis-free survival in 3071 patients. Breast Cancer Res. Treat. 2016, 160, 511–521. [Google Scholar] [CrossRef][Green Version]
- Van Maaren, M.C.; de Munck, L.; de Bock, G.H.; Jobsen, J.J.; van Dalen, T.; Linn, S.C.; Poortmans, P.; Strobbe, L.J.A.; Siesling, S. 10-year survival after breast-conserving surgery plus radiotherapy compared with mastectomy in early breast cancer in The Netherlands: A population-based study. Lancet Oncol. 2016, 17, 1158–1170. [Google Scholar] [CrossRef]
- De Boniface, J.; Szulkin, R.; Johansson, A. Survival after breast conservation versus mastectomy adjusted for comorbidity and socioeconomic status: National 6-year follow-up on 48986 women. Breast 2021, 56, S69. [Google Scholar] [CrossRef]
- Agarwal, S.; Pappas, L.; Neumayer, L.; Kokeny, K.; Agarwal, J. Effect of breast conservation therapy vs mastectomy on disease-specific survival for early-stage breast cancer. JAMA Surg. 2014, 149, 267–274. [Google Scholar] [CrossRef] [PubMed]
- Wrubel, E.; Natwick, R.; Wright, G.P. Breast-Conserving Therapy is Associated with Improved Survival Compared with Mastectomy for Early-Stage Breast Cancer: A Propensity Score Matched Comparison Using the National Cancer Database. Ann. Surg. Oncol. 2021, 28, 914–919. [Google Scholar] [CrossRef]
- Almahariq, M.F.; Quinn, T.J.; Siddiqui, Z.; Jawad, M.S.; Chen, P.Y.; Gustafson, G.S.; Dilworth, J.T. Breast conserving therapy is associated with improved overall survival compared to mastectomy in early-stage, lymph node-negative breast cancer. Radiother Oncol. 2020, 142, 186–194. [Google Scholar] [CrossRef]
- Hartmann-Johnsen, O.J.; Kåresen, R.; Schlichting, E.; Nygård, J.F. Survival is Better after Breast Conserving Therapy than Mastectomy for Early Stage Breast Cancer: A Registry-Based Follow-up Study of Norwegian Women Primary Operated Between 1998 and 2008. Ann. Surg. Oncol. 2015, 22, 3836–3845. [Google Scholar] [CrossRef] [PubMed]
- Hartmann-Johnsen, O.J.; Kåresen, R.; Schlichting, E.; Nygård, J.F. Better survival after breast-conserving therapy compared to mastectomy when axillary node status is positive in early-stage breast cancer: A registry-based follow-up study of 6387 Norwegian women participating in screening, primarily operated between 1998 and 2009. World J. Surg. Oncol. 2017, 15, 118. [Google Scholar] [CrossRef] [PubMed]
- Wang, J.; Wang, S.; Tang, Y.; Jing, H.; Sun, G.; Jin, J.; Liu, Y.; Song, Y.; Wang, W.; Fang, H.; et al. Comparison of Treatment Outcomes With Breast-conserving Surgery Plus Radiotherapy Versus Mastectomy for Patients with Stage I Breast Cancer: A Propensity Score-matched Analysis. Clin. Breast Cancer 2018, 18, e975–e984. [Google Scholar] [CrossRef] [PubMed]
- Corradini, S.; Reitz, D.; Pazos, M.; Schönecker, S.; Braun, M.; Harbeck, N.; Matuschek, C.; Bölke, E.; Ganswindt, U.; Alongi, F.; et al. Mastectomy or breast-conserving therapy for early breast cancer in real-life clinical practice: Outcome comparison of 7565 cases. Cancers 2019, 11, 160. [Google Scholar] [CrossRef] [PubMed]
- Lan, X.W.; Wen, G.; He, Z.; Huang, J.H.; Zou, X.B.; Lin, X.; Tan, Y.T.; Huang, X.B. Comparison of long-term results between radiotherapy after breast-conserving surgery and postmastectomy radiotherapy in stage T1-2N1M0 breast cancer. Cancer Manag Res. 2019, 11, 6477–6487. [Google Scholar] [CrossRef] [PubMed]
- Sun, G.Y.; Wen, G.; Zhang, Y.J.; Tang, Y.; Jing, H.; Wang, J.Y.; Zhang, J.H.; Yang, Y.; Zhao, X.R.; Chen, S.Y.; et al. Radiotherapy plays an important role in improving the survival outcome in patients with T1–2N1M0 breast cancer—A joint analysis of 4262 real world cases from two institutions. BMC Cancer 2020, 20, 1155. [Google Scholar] [CrossRef]
- De Boniface, J.; Frisell, J.; Bergkvist, L.; Andersson, Y. Breast-conserving surgery followed by whole-breast irradiation offers survival benefits over mastectomy without irradiation. Br. J. Surg. 2018, 105, 1607–1614. [Google Scholar] [CrossRef]
- Mahmood, U.; Morris, C.; Neuner, G.; Koshy, M.; Kesmodel, S.; Buras, R.; Chumsri, S.; Bao, T.; Tkaczuk, K.; Feigenberg, S. Similar survival with breast conservation therapy or mastectomy in the management of young women with early-stage breast cancer. Int. J. Radiat. Oncol. Biol. Phys. 2012, 83, 1387–1393. [Google Scholar] [CrossRef]
- Frandsen, J.; Ly, D.; Cannon, G.; Suneja, G.; Matsen, C.; Gaffney, D.K.; Wright, M.; Kokeny, K.E.; Poppe, M.M. In the Modern Treatment Era, Is Breast Conservation Equivalent to Mastectomy in Women Younger Than 40 Years of Age? A Multi-Institution Study. Int. J. Radiat. Oncol. Biol. Phys. 2015, 93, 1096–1103. [Google Scholar] [CrossRef] [PubMed]
- Cao, J.Q.; Truong, P.T.; Olivotto, I.A.; Olson, R.; Coulombe, G.; Keyes, M.; Weir, L.; Gelmon, K.; Bernstein, V.; Woods, R.; et al. Should women younger than 40 years of age with invasive breast cancer have a mastectomy? 15-year outcomes in a population-based cohort. Int. J. Radiat. Oncol. Biol. Phys. 2014, 90, 509–517. [Google Scholar] [CrossRef]
- Mamtani, A.; Morrow, M. Why Are There So Many Mastectomies in the United States? Annu. Rev. Med. 2017, 68, 229–241. [Google Scholar] [CrossRef] [PubMed]
- Riedel, F.; Hennigs, A.; Hug, S.; Schaefgen, B.; Sohn, C.; Schuetz, F.; Golatta, M.; Heil, J. Is Mastectomy Oncologically Safer than Breast-Conserving Treatment in Early Breast Cancer. Breast Care 2017, 12, 385–390. [Google Scholar] [CrossRef]
- Cardoso, F.; Kyriakides, S.; Ohno, S.; Penault-Llorca, F.; Poortmans, P.; Rubio, I.T.; Zackrisson, S.; Senkus, E.; ESMO Guidelines Committee. Early breast cancer: ESMO Clinical Practice Guidelines for diagnosis, treatment and follow-up. Ann. Oncol. 2019, 30, 1194–1220. [Google Scholar] [CrossRef]
- Kummerow, K.L.; Du, L.; Penson, D.F.; Shyr, Y.; Hooks, M.A. Nationwide trends in mastectomy for early-stage breast cancer. JAMA Surg. 2015, 150, 9–16. [Google Scholar] [CrossRef]
- Pesce, C.E.; Liederbach, E.; Czechura, T.; Winchester, D.J.; Yao, K. Changing surgical trends in young patients with early stage breast cancer, 2003 to 2010: A report from the National Cancer Data Base. J. Am. Coll. Surg. 2014, 219, 19–28. [Google Scholar] [CrossRef]
- Baskin, A.S.; Wang, T.; Bredbeck, B.C.; Sinco, B.R.; Berlin, N.L.; Dossett, L.A. Trends in Contralateral Prophylactic Mastectomy Utilization for Small Unilateral Breast Cancer. J. Surg. Res. 2021, 262, 71–84. [Google Scholar] [CrossRef] [PubMed]
- Garcia-Etienne, C.A.; Tomatis, M.; Heil, J.; Friedrichs, K.; Kreienberg, R.; Denk, A.; Kiechle, M.; Lorenz-Salehi, F.; Kimmig, R.; Emons, G.; et al. Mastectomy trends for early-stage breast cancer: A report from the EUSOMA multi-institutional European database. Eur. J. Cancer 2012, 48, 1947–1956. [Google Scholar] [CrossRef] [PubMed]
- Sinnadurai, S.; Kwong, A.; Hartman, M.; Tan, E.Y.; Bhoo-Pathy, N.T.; Dahlui, M.; See, M.H.; Yip, C.H.; Taib, N.A.; Bhoo-Pathy, N. Breast-conserving surgery versus mastectomy in young women with breast cancer in Asian settings. BJS Open 2019, 3, 48–55. [Google Scholar] [CrossRef]
- Yu, L.-X.; Shi, P.; Tian, X.-S.; Yu, Z.-G. A multi-center investigation of breast-conserving surgery based on data from the Chinese Society of Breast Surgery (CSBrS-005). Chin. Med. J. 2020, 133, 2660–2664. [Google Scholar] [CrossRef]
- Hassan Ali, S.; Somashekhar, S.P.; Arun, K.N. Rate of Breast-Conserving Surgery vs Mastectomy in Breast Cancer: A Tertiary Care Centre Experience from South India. Indian J. Surg. Oncol. 2019, 10, 72–76. [Google Scholar] [CrossRef]
- Gass, J.; Mitchell, S.; Hanna, M. How do breast cancer surgery scars impact survivorship? Findings from a nationwide survey in the United States. BMC Cancer 2019, 19, 342. [Google Scholar] [CrossRef]
- Arndt, V.; Stegmaier, C.; Ziegler, H.; Brenner, H. Quality of life over 5 years in women with breast cancer after breast-conserving therapy versus mastectomy: A population-based study. J. Cancer Res. Clin. Oncol. 2008, 134, 1311–1318. [Google Scholar] [CrossRef]
- Engel, J.; Kerr, J.; Schlesinger-Raab, A.; Sauer, H.; Hölzel, D. Quality of life following breast-conserving therapy or mastectomy: Results of a 5-year prospective study. Breast J. 2004, 10, 223–231. [Google Scholar] [CrossRef]
- Zehra, S.; Doyle, F.; Barry, M.; Walsh, S.; Kell, M.R. Health-related quality of life following breast reconstruction compared to total mastectomy and breast-conserving surgery among breast cancer survivors: A systematic review and meta-analysis. Breast Cancer 2020, 27, 534–566. [Google Scholar] [CrossRef]
- Retrouvey, H.; Solaja, O.; Gagliardi, A.R.; Webster, F.; Zhong, T. Barriers of Access to Breast Reconstruction: A Systematic Review. Plast. Reconstr. Surg. 2019, 143, 465e–476e. [Google Scholar] [CrossRef] [PubMed]
- Frasier, L.L.; Holden, S.; Holden, T.; Schumacher, J.R.; Leverson, G.; Anderson, B.; Greenberg, C.C.; Neuman, H.B. Temporal trends in postmastectomy radiation therapy and breast reconstruction associated with changes in national comprehensive cancer network guidelines. JAMA Oncol. 2016, 2, 95–101. [Google Scholar] [CrossRef] [PubMed]
- Yang, R.L.; Newman, A.S.; Lin, I.C.; Reinke, C.E.; Karakousis, G.C.; Czerniecki, B.J.; Wu, L.C.; Kelz, R.R. Trends in immediate breast reconstruction across insurance groups after enactment of breast cancer legislation. Cancer 2013, 119, 2462–2468. [Google Scholar] [CrossRef] [PubMed]
- Jagsi, R.; Abrahamse, P.; Hawley, S.T.; Graff, J.J.; Hamilton, A.S.; Katz, S.J. Underascertainment of radiotherapy receipt in Surveillance, Epidemiology, and End Results registry data. Cancer 2012, 118, 333–341. [Google Scholar] [CrossRef] [PubMed]
- Sobin, L.H.; Gospodarowicz, M.K.; Wittekind, C. TNM Classification of Malignant Tumours, 7th ed.; International Union Against Cancer; John Wiley and Sons: Hoboken, NJ, USA, 2009. [Google Scholar]
- Goldhirsch, A.; Winer, E.P.; Coates, A.S.; Gelber, R.D.; Piccart-Gebhart, M.; Thürlimann, B.; Senn, H.J.; Panel Members. Personalizing the treatment of women with early breast cancer: Highlights of the St Gallen International Expert Consensus on the Primary Therapy of Early Breast Cancer 2013. Ann. Oncol. 2013, 24, 2206–2223. [Google Scholar] [CrossRef]
- Austin, P.C. Goodness-of-fit diagnostics for the propensity score model when estimating treatment effects using covariate adjustment with the propensity score. Pharmacoepidemiol. Drug Saf. 2008, 17, 1202–1217. [Google Scholar] [CrossRef]
- Lalani, N.; Jimenez, R.B.; Yeap, B. Understanding Propensity Score Analyses. Int. J. Radiat. Oncol. Biol. Phys. 2020, 107, 404–407. [Google Scholar] [CrossRef]
- Marks, L.B.; Gupta, G.P.; Muss, H.B.; Ollila, D.W. Mastectomy May Be an Inferior Oncologic Approach Compared to Breast Preservation. Int. J. Radiat. Oncol. Biol. Phys. 2019, 103, 78–80. [Google Scholar] [CrossRef] [PubMed]
- Early Breast Cancer Trialists’ Collaborative Group. Effects of Radiotherapy and Surgery in Early Breast Cancer. An Overview of the Randomized Trials. N. Engl. J. Med. 1995, 333, 1444–1455. [Google Scholar] [CrossRef]
- Zhang, J.; Yang, C.; Lei, C.; Zhang, Y.; Ji, F.; Gao, H.; Yang, M.; Zhang, L.; Li, J.; Zhu, T.; et al. Survival outcomes after breast-conserving therapy compared with mastectomy for patients with early-stage metaplastic breast cancer: A population-based study of 2412 patients. Breast 2021, 58, 10–17. [Google Scholar] [CrossRef] [PubMed]
- Abdulkarim, B.S.; Cuartero, J.; Hanson, J.; Deschênes, J.; Lesniak, D.; Sabri, S. Increased risk of locoregional recurrence for women with T1-2N0 triple-negative breast cancer treated with modified radical mastectomy without adjuvant radiation therapy compared with breast-conserving therapy. J. Clin. Oncol. 2011, 29, 2852–2858. [Google Scholar] [CrossRef]
- Zumsteg, Z.S.; Morrow, M.; Arnold, B.; Zheng, J.; Zhang, Z.; Robson, M.; Traina, T.; McCormick, B.; Powell, S.; Ho, A.Y. Breast-conserving therapy achieves locoregional outcomes comparable to mastectomy in women with T1-2N0 triple-negative breast cancer. Ann. Surg. Oncol. 2013, 20, 3469–3476. [Google Scholar] [CrossRef]
- De Boniface, J.; Szulkin, R.; Johansson, A.L.V. Survival after Breast Conservation vs Mastectomy Adjusted for Comorbidity and Socioeconomic Status: A Swedish National 6-Year Follow-up of 48986 Women. JAMA Surg 2021, 156, 628–637. [Google Scholar] [CrossRef]
- van Maaren, M.C.; le Cessie, S.; Strobbe, L.J.A.; Groothuis-Oudshoorn, C.G.M.; Poortmans, P.M.P.; Siesling, S. Different statistical techniques dealing with confounding in observational research: Measuring the effect of breast-conserving therapy and mastectomy on survival. J. Cancer Res. Clin. Oncol. 2019, 145, 1485–1493. [Google Scholar] [CrossRef]
- Anampa, J.; Makower, D.; Sparano, J.A. Progress in adjuvant chemotherapy for breast cancer: An overview. BMC Med. 2015, 13, 195. [Google Scholar] [CrossRef] [PubMed]
- Murphy, J.; Gandhi, A. Does Mastectomy Reduce Overall Survival in Early Stage Breast Cancer? Clin. Oncol. R. Coll. Radiol. 2021, 33, 440–447. [Google Scholar] [CrossRef]
- Clarke, M.; Collins, R.; Darby, S.; Davies, C.; Elphinstone, P.; Evans, V.; Godwin, J.; Gray, R.; Hicks, C.; James, S.; et al. Early Breast Cancer Trialists’ Collaborative Group (EBCTCG). Effects of radiotherapy and of differences in the extent of surgery for early breast cancer on local recurrence and 15-year survival: An overview of the randomised trials. Lancet 2005, 366, 2087–2106. [Google Scholar] [CrossRef]
- Sautter-Bihl, M.L.; Sedlmayer, F.; Budach, W.; Dunst, J.; Feyer, P.; Fietkau, R.; Haase, W.; Harms, W.; Rödel, C.; Souchon, R.; et al. One life saved by four prevented recurrences? Strahlenther. Onkol. 2012, 188, 461–463. [Google Scholar] [CrossRef] [PubMed]
- Gentilini, O.D.; Cardoso, M.-J.; Poortmans, P. Less is more. Breast conservation might be even better than mastectomy in early breast cancer patients. Breast 2017, 35, 32–33. [Google Scholar] [CrossRef]
- Van Maaren, M.C.; Poortmans, P.; Siesling, S. Breast-conserving therapy versus mastectomy. Oncoscience 2016, 3, 304–305. [Google Scholar] [CrossRef]
- Park, S.-H.; Kim, J.-C.; Lee, J.E.; Park, I.-K. Virtual lymph node analysis to evaluate axillary lymph node coverage provided by tangential breast irradiation. Radiat. Oncol. J. 2015, 33, 50–56. [Google Scholar] [CrossRef][Green Version]
- Haussmann, J.; Corradini, S.; Nestle-Kraemling, C.; Bölke, E.; Njanang, F.J.D.; Tamaskovics, B.; Orth, K.; Ruckhaeberle, E.; Fehm, T.; Mohrmann, S.; et al. Recent advances in radiotherapy of breast cancer. Radiat. Oncol. 2020, 15, 71. [Google Scholar] [CrossRef] [PubMed]
- Deutsch, E.; Chargari, C.; Galluzzi, L.; Kroemer, G. Optimising efficacy and reducing toxicity of anticancer radioimmunotherapy. Lancet Oncol. 2019, 20, e452–e463. [Google Scholar] [CrossRef]
- EBCTCG (Early Breast Cancer Trialists’ Collaborative Group); McGale, P.; Taylor, C.; Correa, C.; Cutter, D.; Duane, F.; Ewertz, M.; Gray, R.; Mannu, G.; Peto, R.; et al. Effect of radiotherapy after mastectomy and axillary surgery on 10-year recurrence and 20-year breast cancer mortality: Meta-analysis of individual patient data for 8135 women in 22 randomised trials. Lancet 2014, 383, 2127–2135. [Google Scholar] [CrossRef]
- Jagsi, R.; Jiang, J.; Momoh, A.O.; Alderman, A.; Giordano, S.H.; Buchholz, T.A.; Pierce, L.J.; Kronowitz, S.J.; Smith, B.D. Complications After Mastectomy and Immediate Breast Reconstruction for Breast Cancer: A Claims-Based Analysis. Ann. Surg. 2016, 263, 219–227. [Google Scholar] [CrossRef]
- Findlay-Shirras, L.; Lima, I.; Smith, G.; Clemons, M.; Arnaout, A. Canada follows the US in the rise of bilateral mastectomies for unilateral breast cancer: A 23-year population cohort study. Breast Cancer Res. Treat. 2021, 185, 517–525. [Google Scholar] [CrossRef]
- Wang, T.; Mott, N.; Miller, J.; Berlin, N.L.; Hawley, S.; Jagsi, R.; Dossett, L.A. Patient Perspectives on Treatment Options for Older Women with Hormone Receptor-Positive Breast Cancer: A Qualitative Study. JAMA Netw. Open 2020, 3, e2017129. [Google Scholar] [CrossRef] [PubMed]
- Nash, R.; Goodman, M.; Lin, C.C.; Freedman, R.A.; Dominici, L.S.; Ward, K.; Jemal, A. State Variation in the Receipt of a Contralateral Prophylactic Mastectomy Among Women Who Received a Diagnosis of Invasive Unilateral Early-Stage Breast Cancer in the United States, 2004–2012. JAMA Surg. 2017, 152, 648–657. [Google Scholar] [CrossRef]
- Hawley, S.T.; Jagsi, R.; Morrow, M.; Janz, N.K.; Hamilton, A.; Graff, J.J.; Katz, S.J. Social and Clinical Determinants of Contralateral Prophylactic Mastectomy. JAMA Surg. 2014, 149, 582–589. [Google Scholar] [CrossRef] [PubMed]
- Kaidar-Person, O.; Offersen, B.V.; Boersma, L.J.; de Ruysscher, D.; Tramm, T.; Kühn, T.; Gentilini, O.; Mátrai, Z.; Poortmans, P. A multidisciplinary view of mastectomy and breast reconstruction: Understanding the challenges. Breast 2021, 56, 42–52. [Google Scholar] [CrossRef]
- Dodwell, D.; Wheatley, D. Counterpoint: Does Mastectomy Reduce Overall Survival in Early Stage Breast Cancer? Clin. Oncol. 2021, 33, 448–450. [Google Scholar] [CrossRef] [PubMed]
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).