Improving Payload Capacity and Anti-Tumor Efficacy of Mesenchymal Stem Cells Using TAT Peptide Functionalized Polymeric Nanoparticles
Abstract
1. Introduction
2. Results
2.1. Synthesis of Thiolated TAT Peptide
2.2. Physicochemical Characterization of Nanoparticles
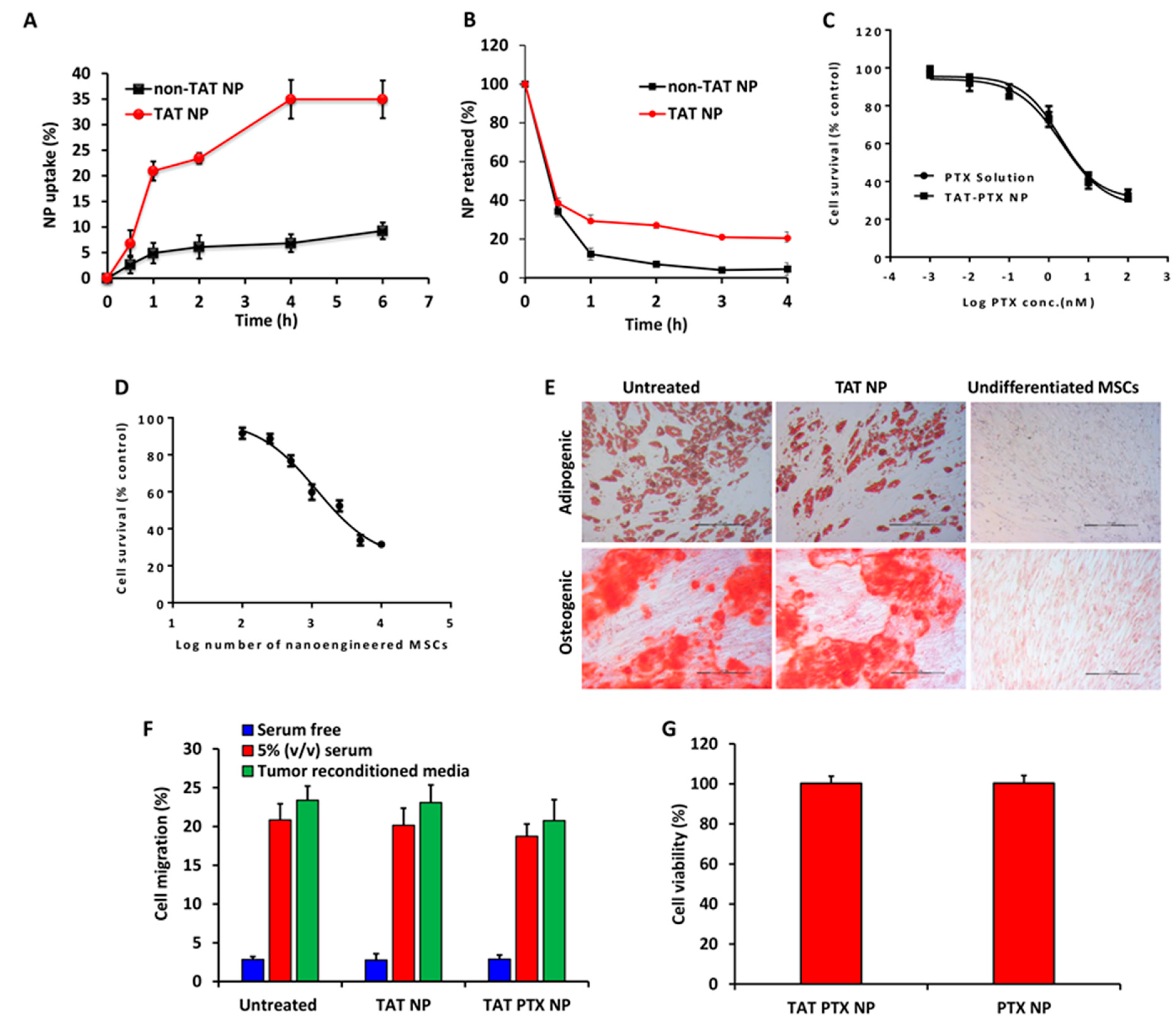
2.3. Nanoparticles Uptake and Retention in MSCs
2.4. In Vitro Cytotoxicity Studies
2.5. Characterization of Nano-Engineered MSCs
2.6. Cell Viability of Nano-Engineered MSCs
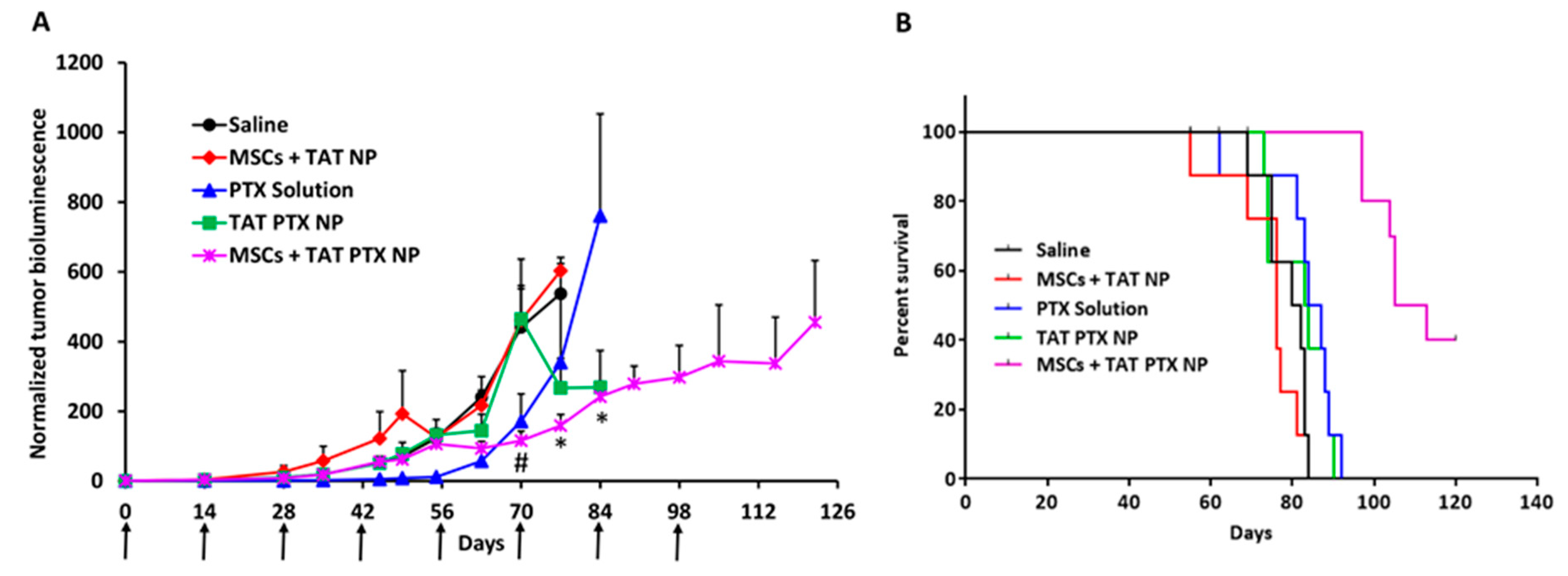
2.7. Therapeutic Efficacy of Nano-Engineered MSCs in Orthotopic Lung Tumor Model
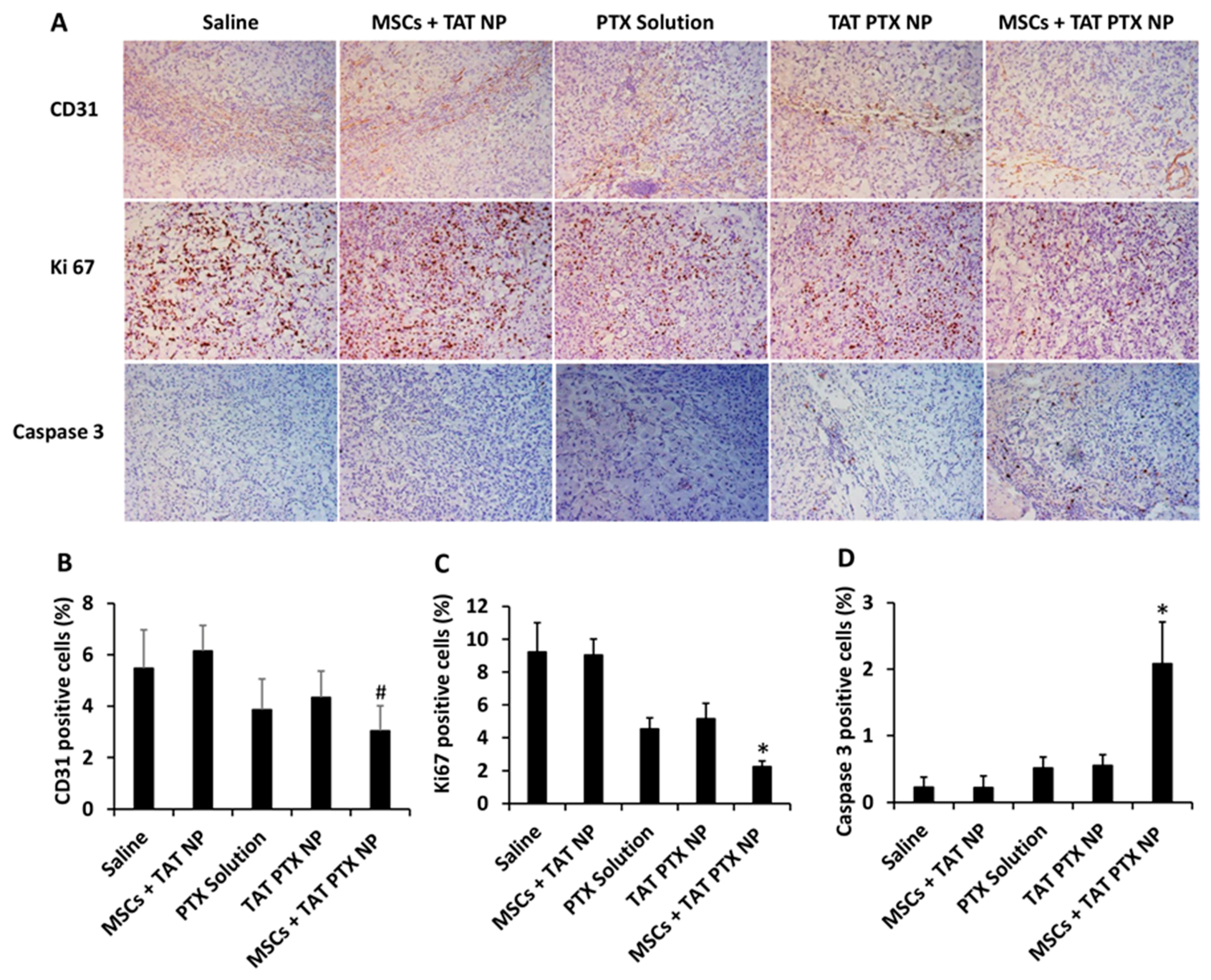
2.8. Immunohistological Staining of Lung Tumors
2.9. Toxicology Assessment of Nano-Engineered MSCs
3. Discussion
4. Materials and Methods
4.1. Materials
4.2. Synthesis of Sulfhydryl Activated TAT Peptide
4.3. Preparation of TAT-functionalized PLGA Nanoparticles
4.4. Characterization of Nanoparticles
4.5. Cell Culture
4.6. Nanoparticle Uptake and Retention in MSCs
4.7. Preparation of Nano-Engineered MSCs
4.8. In Vitro Migration Potential of Nano-Engineered MSCs
4.9. Effect of Nano-Engineering on MSC Viability
4.10. Differentiation Potential of Nano-Engineered MSCs
4.11. In Vitro Cell Growth Inhibition Studies
4.12. Therapeutic Efficacy of Nano-Engineered MSCs in Orthotopic Lung Tumor Model
4.13. Toxicology Assessment of Intravenously Administered Nano-Engineered MSCs
4.14. Immunohistological Staining of Lung Tumors
4.15. Statistical Analysis
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Acknowledgments
Conflicts of Interest
References
- Eberhard, A.; Kahlert, S.; Goede, V.; Hemmerlein, B.; Plate, K.H.; Augustin, H.G. Heterogeneity of angiogenesis and blood vessel maturation in human tumors: Implications for antiangiogenic tumor therapies. Cancer Res. 2000, 60, 1388–1393. [Google Scholar] [PubMed]
- Forster, J.C.; Harriss-Phillips, W.M.; Douglass, M.J.; Bezak, E. A review of the development of tumor vasculature and its effects on the tumor microenvironment. Hypoxia (Auckl) 2017, 5, 21–32. [Google Scholar] [CrossRef] [PubMed]
- Minchinton, A.I.; Tannock, I.F. Drug penetration in solid tumours. Nat. Rev. Cancer 2006, 6, 583–592. [Google Scholar] [CrossRef] [PubMed]
- Stylianopoulos, T.; Martin, J.D.; Chauhan, V.P.; Jain, S.R.; Diop-Frimpong, B.; Bardeesy, N.; Smith, B.L.; Ferrone, C.R.; Hornicek, F.J.; Boucher, Y.; et al. Causes, consequences, and remedies for growth-induced solid stress in murine and human tumors. Proc. Natl. Acad. Sci. USA 2012, 109, 15101–15108. [Google Scholar] [PubMed]
- Dewhirst, M.W.; Secomb, T.W. Transport of drugs from blood vessels to tumour tissue. Nat. Rev. Cancer 2017, 17, 738–750. [Google Scholar] [CrossRef]
- Nichols, J.W.; Sakurai, Y.; Harashima, H.; Bae, Y.H. Nano-sized drug carriers: Extravasation, intratumoral distribution, and their modeling. J. Control Release 2017, 267, 31–46. [Google Scholar] [CrossRef] [PubMed]
- Tan, Q.; Saggar, J.K.; Yu, M.; Wang, M.; Tannock, I.F. Mechanisms of Drug Resistance Related to the Microenvironment of Solid Tumors and Possible Strategies to Inhibit Them. Cancer J. 2015, 21, 254–262. [Google Scholar] [CrossRef] [PubMed]
- Agrahari, V.; Mitra, A.K. Next generation drug delivery: Circulatory cells-mediated nanotherapeutic approaches. Expert Opin. Drug Deliv. 2017, 14, 285–289. [Google Scholar] [CrossRef] [PubMed]
- Tan, S.; Wu, T.; Zhang, D.; Zhang, Z. Cell or cell membrane-based drug delivery systems. Theranostics 2015, 5, 863–881. [Google Scholar] [CrossRef] [PubMed]
- Villa, C.H.; Anselmo, A.C.; Mitragotri, S.; Muzykantov, V. Red blood cells: Supercarriers for drugs, biologicals, and nanoparticles and inspiration for advanced delivery systems. Adv. Drug Deliv. Rev. 2016, 106, 88–103. [Google Scholar] [CrossRef] [PubMed]
- Huang, B.; Abraham, W.D.; Zheng, Y.; Bustamante Lopez, S.C.; Luo, S.S.; Irvine, D.J. Active targeting of chemotherapy to disseminated tumors using nanoparticle-carrying T cells. Sci. Transl. Med. 2015, 7, 291ra294. [Google Scholar] [CrossRef] [PubMed]
- Pang, L.; Qin, J.; Han, L.; Zhao, W.; Liang, J.; Xie, Z.; Yang, P.; Wang, J. Exploiting macrophages as targeted carrier to guide nanoparticles into glioma. Oncotarget 2016, 7, 37081–37091. [Google Scholar] [CrossRef] [PubMed]
- Stuckey, D.W.; Shah, K. Stem cell-based therapies for cancer treatment: Separating hope from hype. Nat. Rev. Cancer 2014, 14, 683–691. [Google Scholar] [CrossRef] [PubMed]
- Bago, J.R.; Alfonso-Pecchio, A.; Okolie, O.; Dumitru, R.; Rinkenbaugh, A.; Baldwin, A.S.; Miller, C.R.; Magness, S.T.; Hingtgen, S.D. Therapeutically engineered induced neural stem cells are tumour-homing and inhibit progression of glioblastoma. Nat. Commun. 2016, 7, 10593. [Google Scholar] [CrossRef]
- Kim, S.W.; Lee, Y.K.; Hong, J.H.; Park, J.Y.; Choi, Y.A.; Lee, D.U.; Choi, J.; Sym, S.J.; Kim, S.H.; Khang, D. Mutual Destruction of Deep Lung Tumor Tissues by Nanodrug-Conjugated Stealth Mesenchymal Stem Cells. Adv. Sci. (Weinh) 2018, 5, 1700860. [Google Scholar] [CrossRef]
- Layek, B.; Sadhukha, T.; Panyam, J.; Prabha, S. Nano-Engineered Mesenchymal Stem Cells Increase Therapeutic Efficacy of Anticancer Drug Through True Active Tumor Targeting. Mol. Cancer 2018, 17, 1196–1206. [Google Scholar] [CrossRef] [PubMed]
- Zhao, Y.; Tang, S.; Guo, J.; Alahdal, M.; Cao, S.; Yang, Z.; Zhang, F.; Shen, Y.; Sun, M.; Mo, R.; et al. Targeted delivery of doxorubicin by nano-loaded mesenchymal stem cells for lung melanoma metastases therapy. Sci. Rep. 2017, 7, 44758. [Google Scholar] [CrossRef] [PubMed]
- Wang, F.; Wang, Y.; Zhang, X.; Zhang, W.; Guo, S.; Jin, F. Recent progress of cell-penetrating peptides as new carriers for intracellular cargo delivery. J. Control Release 2014, 174, 126–136. [Google Scholar] [CrossRef] [PubMed]
- Oh, N.; Park, J.-H. Endocytosis and exocytosis of nanoparticles in mammalian cells. Int. J. Nanomed. 2014, 9 (Suppl. 1), 51–63. [Google Scholar] [CrossRef]
- Guidotti, G.; Brambilla, L.; Rossi, D. Cell-Penetrating Peptides: From Basic Research to Clinics. Trends Pharm. Sci. 2017, 38, 406–424. [Google Scholar] [CrossRef] [PubMed]
- Silhol, M.; Tyagi, M.; Giacca, M.; Lebleu, B.; Vives, E. Different mechanisms for cellular internalization of the HIV-1 Tat-derived cell penetrating peptide and recombinant proteins fused to Tat. Eur. J. Biochem. 2002, 269, 494–501. [Google Scholar] [CrossRef] [PubMed]
- Brooks, H.; Lebleu, B.; Vives, E. Tat peptide-mediated cellular delivery: Back to basics. Adv. Drug Deliv. Rev. 2005, 57, 559–577. [Google Scholar] [CrossRef] [PubMed]
- Kang, H.J.; Choe, W.; Kim, B.M.; Chung, S.J. IgG Fc-binding peptide (FcBP)-tat conjugate as a smart antibody carrier into live cells. Macromol. Res. 2015, 23, 876–881. [Google Scholar] [CrossRef]
- Jo, J.; Hong, S.; Choi, W.Y.; Lee, D.R. Cell-penetrating peptide (CPP)-conjugated proteins is an efficient tool for manipulation of human mesenchymal stromal cells. Sci. Rep. 2014, 4, 4378. [Google Scholar] [CrossRef]
- Zeng, Z.; Han, S.; Hong, W.; Lang, Y.; Li, F.; Liu, Y.; Li, Z.; Wu, Y.; Li, W.; Zhang, X.; et al. A Tat-conjugated Peptide Nucleic Acid Tat-PNA-DR Inhibits Hepatitis B Virus Replication In Vitro and In Vivo by Targeting LTR Direct Repeats of HBV RNA. Mol. Nucleic Acids 2016, 5, e295. [Google Scholar] [CrossRef] [PubMed]
- Zhang, P.; Lock, L.L.; Cheetham, A.G.; Cui, H. Enhanced cellular entry and efficacy of tat conjugates by rational design of the auxiliary segment. Mol. Pharm. 2014, 11, 964–973. [Google Scholar] [CrossRef] [PubMed]
- Layek, B.; Lipp, L.; Singh, J. Cell Penetrating Peptide Conjugated Chitosan for Enhanced Delivery of Nucleic Acid. Int. J. Mol. Sci. 2015, 16, 28912–28930. [Google Scholar] [CrossRef] [PubMed]
- Majumder, P.; Bhunia, S.; Chaudhuri, A. A lipid-based cell penetrating nano-assembly for RNAi-mediated anti-angiogenic cancer therapy. Chem. Commun. (Camb.) 2018, 54, 1489–1492. [Google Scholar] [CrossRef] [PubMed]
- Trabulo, S.; Cardoso, A.L.; Mano, M.; De Lima, M.C.P. Cell-Penetrating Peptides-Mechanisms of Cellular Uptake and Generation of Delivery Systems. Pharmaceuticals (Basel) 2010, 3, 961–993. [Google Scholar] [CrossRef] [PubMed]
- Kauffman, W.B.; Fuselier, T.; He, J.; Wimley, W.C. Mechanism Matters: A Taxonomy of Cell Penetrating Peptides. Trends Biochem. Sci. 2015, 40, 749–764. [Google Scholar] [CrossRef] [PubMed]
- Kaplan, I.M.; Wadia, J.S.; Dowdy, S.F. Cationic TAT peptide transduction domain enters cells by macropinocytosis. J. Control. Release 2005, 102, 247–253. [Google Scholar] [CrossRef] [PubMed]
- Fittipaldi, A.; Ferrari, A.; Zoppé, M.; Arcangeli, C.; Pellegrini, V.; Beltram, F.; Giacca, M. Cell Membrane Lipid Rafts Mediate Caveolar Endocytosis of HIV-1 Tat Fusion Proteins. J. Biol. Chem. 2003, 278, 34141–34149. [Google Scholar] [CrossRef]
- Duchardt, F.; Fotin-Mleczek, M.; Schwarz, H.; Fischer, R.; Brock, R. A Comprehensive Model for the Cellular Uptake of Cationic Cell-penetrating Peptides. Traffic 2007, 8, 848–866. [Google Scholar] [CrossRef]
- Maiolo, J.R.; Ferrer, M.; Ottinger, E.A. Effects of cargo molecules on the cellular uptake of arginine-rich cell-penetrating peptides. Biochim. Biophys. Acta (Bba) Biomembr. 2005, 1712, 161–172. [Google Scholar] [CrossRef]
- Sadhukha, T.; O‘Brien, T.D.; Prabha, S. Nano-engineered mesenchymal stem cells as targeted therapeutic carriers. J. Control. Release 2014, 196, 243–251. [Google Scholar] [CrossRef] [PubMed]
- Zhang, P.; Zhang, G.; Liu, X.; Liu, H.; Yang, P.; Ma, L. Mesenchymal stem cells improve platelet counts in mice with immune thrombocytopenia. J. Cell. Biochem. 2019. [Google Scholar] [CrossRef] [PubMed]
- Gao, Z.; Zhang, L.; Hu, J.; Sun, Y. Mesenchymal stem cells: A potential targeted-delivery vehicle for anti-cancer drug loaded nanoparticles. Nanomed.: Nanotechnol. Biol. Med. 2013, 9, 174–184. [Google Scholar] [CrossRef]
- Layek, B.; Sadhukha, T.; Prabha, S. Glycoengineered mesenchymal stem cells as an enabling platform for two-step targeting of solid tumors. Biomaterials 2016, 88, 97–109. [Google Scholar] [CrossRef] [PubMed]
- Tripodo, G.; Chlapanidas, T.; Perteghella, S.; Vigani, B.; Mandracchia, D.; Trapani, A.; Galuzzi, M.; Tosca, M.C.; Antonioli, B.; Gaetani, P.; et al. Mesenchymal stromal cells loading curcumin-INVITE-micelles: A drug delivery system for neurodegenerative diseases. Colloids Surf. B Biointerfaces 2015, 125, 300–308. [Google Scholar] [CrossRef] [PubMed]
- Madeira, C.; Mendes, R.D.; Ribeiro, S.C.; Boura, J.S.; Aires-Barros, M.R.; da Silva, C.L.; Cabral, J.M.S. Nonviral gene delivery to mesenchymal stem cells using cationic liposomes for gene and cell therapy. J. Biomed. Biotechnol. 2010, 2010, 735349. [Google Scholar] [CrossRef] [PubMed]
- Zhang, X.; Yao, S.; Liu, C.; Jiang, Y. Tumor tropic delivery of doxorubicin-polymer conjugates using mesenchymal stem cells for glioma therapy. Biomaterials 2015, 39, 269–281. [Google Scholar] [CrossRef] [PubMed]
- Torchilin, V.P.; Rammohan, R.; Weissig, V.; Levchenko, T.S. TAT peptide on the surface of liposomes affords their efficient intracellular delivery even at low temperature and in the presence of metabolic inhibitors. Proc. Natl. Acad. Sci. USA 2001, 98, 8786–8791. [Google Scholar] [CrossRef]
- Feiner-Gracia, N.; Dols-Perez, A.; Royo, M.; Solans, C.; Garcia-Celma, M.J.; Fornaguera, C. Cell penetrating peptide grafting of PLGA nanoparticles to enhance cell uptake. Eur. Polym. J. 2018, 108, 429–438. [Google Scholar] [CrossRef]
- Alsharedi, M.; Gress, T.; Dotson, J.; Elmsherghi, N.; Tirona, M.T. Comparison of toxicity profile and tolerability between two standard of care paclitaxel-based adjuvant chemotherapy regimens in breast cancer. Med. Oncol. 2016, 33, 27. [Google Scholar] [CrossRef] [PubMed]
- Mandaliya, H.; Baghi, P.; Prawira, A.; George, M.K. A Rare Case of Paclitaxel and/or Trastuzumab Induced Acute Hepatic Necrosis. Case Rep. Oncol. Med. 2015, 2015, 825603. [Google Scholar] [CrossRef] [PubMed][Green Version]
- Patil, Y.; Sadhukha, T.; Ma, L.; Panyam, J. Nanoparticle-mediated simultaneous and targeted delivery of paclitaxel and tariquidar overcomes tumor drug resistance. J. Control Release 2009, 136, 21–29. [Google Scholar] [CrossRef] [PubMed]

| Parameters | Saline | MSCs + TAT NP | TAT PTX NP | MSCs + TAT PTX NP | ||||
|---|---|---|---|---|---|---|---|---|
| Day 7 | Day 18 | Day 7 | Day 18 | Day 7 | Day 18 | Day 7 | Day 18 | |
| ALT (U/L) | 33.0 ± 7.0 | 37.0 ± 5.3 | 33.5 ± 4.7 | 36.0 ± 5.4 | 32.5 ± 4.5 | 33.5 ± 5.5 | 35.8 ± 6.4 | 40.0 ± 4.4 |
| AST (U/L) | 80.7 ± 9.7 | 87.3 ± 13.1 | 85.8 ± 11.5 | 90.0 ± 10.8 | 85.7 ± 7.7 | 90.3 ± 10.0 | 84.8 ± 11.7 | 91.5 ± 5.8 |
| GGT(U/L) | 1.0 ± 0.0 | 1.0 ± 0.0 | 1.0 ± 0.0 | 1.0 ± 0.0 | 1.0 ± 0.0 | 1.0 ± 0.0 | 1.0 ± 0.0 | 1.0 ± 0.0 |
| ALP (U/L) | 94.3 ± 5.9 | 100.7 ± 7.1 | 90.3 ± 4.9 | 96.8 ± 11.0 | 95.5 ± 4.2 | 98.0 ± 16.5 | 95.0 ± 6.5 | 100.8 ± 10.3 |
| TP (g/dL) | 5.8 ± 0.2 | 5.4 ± 0.3 | 5.8 ± 0.3 | 5.9 ± 0.3 | 5.7 ± 0.2 | 5.5 ± 0.1 | 5.8 ± 0.2 | 5.3 ± 0.1 |
| ALB (g/dL) | 3.5 ± 0.1 | 3.2 ± 0.1 | 3.5 ± 0.2 | 3.4 ± 0.2 | 3.5 ± 0.1 | 3.4 ± 0.1 | 3.5 ± 0.1 | 3.4 ± 0.1 |
| GLOB (g/dL) | 2.3 ± 0.1 | 1.9 ± 0.1 | 2.3 ± 0.2 | 2.5 ± 0.2 | 2.1 ± 0.2 | 2.0 ± 0.1 | 2.3 ± 0.1 | 2.4 ± 0.0 |
| A/G | 1.5 ± 0.1 | 1.7 ± 0.1 | 1.6 ± 0.1 | 1.4 ± 0.1 | 1.7 ± 0.1 | 1.7 ± 0.1 | 1.5 ± 0.1 | 1.4 ± 0.0 |
| TBIL (mg/dL) | 0.3 ± 0.1 | 0.4 ± 0.1 | 0.3 ± 0.0 | 0.2 ± 0.0 | 0.3 ± 0.1 | 0.3 ± 0.0 | 0.2 ± 0.0 | 0.3 ± 0.1 |
| Parameters | Saline | MSCs + TAT NP | TAT PTX NP | MSCs + TAT PTX NP | ||||
|---|---|---|---|---|---|---|---|---|
| Day 7 | Day 18 | Day 7 | Day 18 | Day 7 | Day 18 | Day 7 | Day 18 | |
| WBC (×103 cells/µL) | 5.0 ± 1.4 | 6.3 ± 0.5 | 4.9 ± 0.8 | 5.0 ± 0.6 | 5.3 ± 0.6 | 4.4 ± 0.2 | 5.6 ± 1.2 | 4.7 ± 0.7 |
| RBC (×106 cells/µL) | 9.8 ± 0.3 | 9.7 ± 0.3 | 9.8 ± 0.2 | 9.5 ± 0.3 | 9.8 ± 0.1 | 9.1 ± 0.3 | 9.7 ± 0.2 | 9.1 ± 0.1 |
| HGB (g/dL) | 15.4 ± 0.4 | 15.5 ± 0.6 | 15.3 ± 0.3 | 15.0 ± 0.5 | 15.6 ± 0.2 | 14.8 ± 0.3 | 15.1 ± 0.3 | 14.3 ± 0.3 |
| HCT (%) | 50.9 ± 1.1 | 49.2 ± 1.7 | 50.2 ± 1.0 | 46.5 ± 1.6 | 51.4 ± 0.7 | 46.1 ± 1.5 | 49.5 ± 0.9 | 45.6 ± 0.9 |
| PLT (×103 cells/µL) | 840 ± 26 | 977 ± 50 | 1106 ± 224 | 1248 ± 131 | 914 ± 60 | 1060 ± 103 | 1349 ± 238 | 1234 ± 147 |
© 2019 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Moku, G.; Layek, B.; Trautman, L.; Putnam, S.; Panyam, J.; Prabha, S. Improving Payload Capacity and Anti-Tumor Efficacy of Mesenchymal Stem Cells Using TAT Peptide Functionalized Polymeric Nanoparticles. Cancers 2019, 11, 491. https://doi.org/10.3390/cancers11040491
Moku G, Layek B, Trautman L, Putnam S, Panyam J, Prabha S. Improving Payload Capacity and Anti-Tumor Efficacy of Mesenchymal Stem Cells Using TAT Peptide Functionalized Polymeric Nanoparticles. Cancers. 2019; 11(4):491. https://doi.org/10.3390/cancers11040491
Chicago/Turabian StyleMoku, Gopikrishna, Buddhadev Layek, Lana Trautman, Samuel Putnam, Jayanth Panyam, and Swayam Prabha. 2019. "Improving Payload Capacity and Anti-Tumor Efficacy of Mesenchymal Stem Cells Using TAT Peptide Functionalized Polymeric Nanoparticles" Cancers 11, no. 4: 491. https://doi.org/10.3390/cancers11040491
APA StyleMoku, G., Layek, B., Trautman, L., Putnam, S., Panyam, J., & Prabha, S. (2019). Improving Payload Capacity and Anti-Tumor Efficacy of Mesenchymal Stem Cells Using TAT Peptide Functionalized Polymeric Nanoparticles. Cancers, 11(4), 491. https://doi.org/10.3390/cancers11040491






